4cdac41a0d5e958483866ca5a101fb5b.ppt
- Количество слайдов: 64
 Post Arthroplasty Review Clinic
Post Arthroplasty Review Clinic
 The Post Arthroplasty Review (PAR) Clinic 2009 -10
The Post Arthroplasty Review (PAR) Clinic 2009 -10
 Why? • Current orthopaedic post operative outpatient review clinic was not achieving organisation KPI’s – Demand for review appointments > number of appointments available – Only 41% of requests for 12 month post op reviews from Jan 08 – Jun 08 met the KPI. – KPI for priority 1 and 2 urgent NP appointments not being met 2008 – 09 • Evaluation of patient outcomes post surgery currently not possible – documentation not consistent and often incomplete – Patient Outcome measures not used
Why? • Current orthopaedic post operative outpatient review clinic was not achieving organisation KPI’s – Demand for review appointments > number of appointments available – Only 41% of requests for 12 month post op reviews from Jan 08 – Jun 08 met the KPI. – KPI for priority 1 and 2 urgent NP appointments not being met 2008 – 09 • Evaluation of patient outcomes post surgery currently not possible – documentation not consistent and often incomplete – Patient Outcome measures not used
 Department of Health Grant: The PAR clinic 2009 -10 Scoping Phase PROJECT AIM: • To investigate the potential of introducing an advanced practice musculoskeletal physiotherapist to review patients following hip or knee arthroplasty in the orthopaedic outpatient clinic • To improve the experience & outcomes for orthopaedic outpatients following hip or knee arthroplasty • To optimise utilisation of the orthopaedic surgeon’s time & expertise
Department of Health Grant: The PAR clinic 2009 -10 Scoping Phase PROJECT AIM: • To investigate the potential of introducing an advanced practice musculoskeletal physiotherapist to review patients following hip or knee arthroplasty in the orthopaedic outpatient clinic • To improve the experience & outcomes for orthopaedic outpatients following hip or knee arthroplasty • To optimise utilisation of the orthopaedic surgeon’s time & expertise
 Method: • Working party established – Miss Sue Liew, Claire Sage, Paula Harding • Arthroplasty patients selected b/c: – Low infection and complication rate – Large amount of surgeon time required due to regular scheduling of reviews • New clinic proposed named Physiotherapy Arthroplasty Review Clinic (PAR) clinic • Guidelines and framework of new model of care discussed with and final proposal presented to the Orthopaedic Surgeons • Support achieved from majority of surgeons (exception of 1) • Support achieved from other key stakeholders : Outpatients, Radiology, IT
Method: • Working party established – Miss Sue Liew, Claire Sage, Paula Harding • Arthroplasty patients selected b/c: – Low infection and complication rate – Large amount of surgeon time required due to regular scheduling of reviews • New clinic proposed named Physiotherapy Arthroplasty Review Clinic (PAR) clinic • Guidelines and framework of new model of care discussed with and final proposal presented to the Orthopaedic Surgeons • Support achieved from majority of surgeons (exception of 1) • Support achieved from other key stakeholders : Outpatients, Radiology, IT
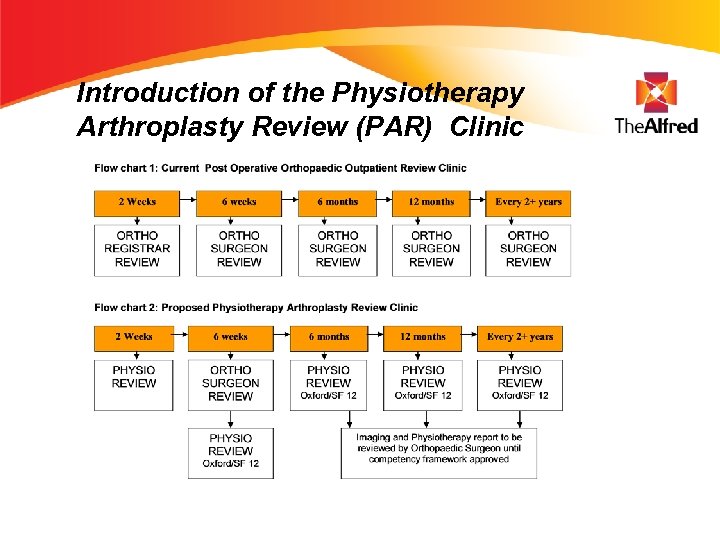 Introduction of the Physiotherapy Arthroplasty Review (PAR) Clinic
Introduction of the Physiotherapy Arthroplasty Review (PAR) Clinic
 PAR Clinic Pilot • 10 patients weekly • X 2 Mon am in the Physio ED #/trauma r/v clinic 4 C (15 min reviews) for 2 weeks post op X 4 Thurs and Fri am 8. 30 – 9. 30 (15 min reviews) for 6 week, 6 and 12 month, 2 yearly reviews (before screening clinic) Days allocated according to operating surgeon Patients attend Xray either Wed prior to appointment or at 8. 00 on the day of appointment Appointment letter to be sent to patients advising them they will be seeing a physiotherapist. Patient focused objective outcome measures SF 12 and Oxford hip and knee scale to be collected at each review • • •
PAR Clinic Pilot • 10 patients weekly • X 2 Mon am in the Physio ED #/trauma r/v clinic 4 C (15 min reviews) for 2 weeks post op X 4 Thurs and Fri am 8. 30 – 9. 30 (15 min reviews) for 6 week, 6 and 12 month, 2 yearly reviews (before screening clinic) Days allocated according to operating surgeon Patients attend Xray either Wed prior to appointment or at 8. 00 on the day of appointment Appointment letter to be sent to patients advising them they will be seeing a physiotherapist. Patient focused objective outcome measures SF 12 and Oxford hip and knee scale to be collected at each review • • •
 Felice Rosemary Lloyd Travel Scholarship CANADA Hotel Dieu Hospital, Kingston, Ontario Holland Orthopaedic and Arthritic Centre, Toronto, Ontario UNITED KINGDOM Edinburgh Royal Infirmary Wrightington Hospital, Wigan The Royal Derby Hospital, Derby Broadgreen NHS, Liverpool
Felice Rosemary Lloyd Travel Scholarship CANADA Hotel Dieu Hospital, Kingston, Ontario Holland Orthopaedic and Arthritic Centre, Toronto, Ontario UNITED KINGDOM Edinburgh Royal Infirmary Wrightington Hospital, Wigan The Royal Derby Hospital, Derby Broadgreen NHS, Liverpool
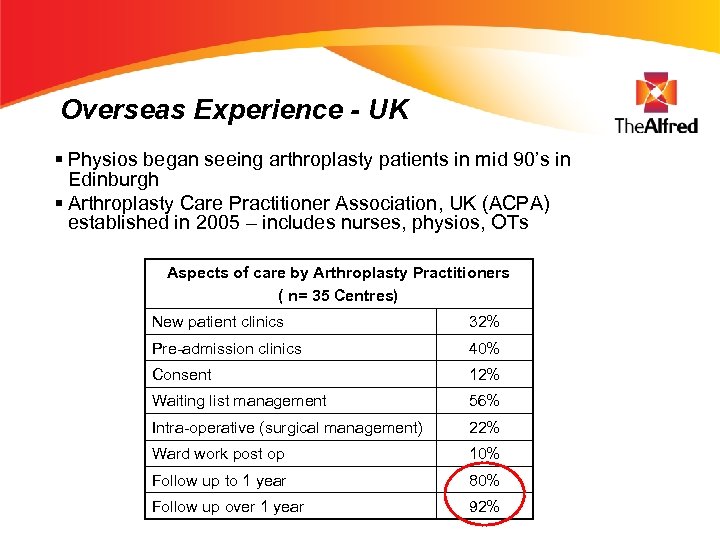 Overseas Experience - UK § Physios began seeing arthroplasty patients in mid 90’s in Edinburgh § Arthroplasty Care Practitioner Association, UK (ACPA) established in 2005 – includes nurses, physios, OTs Aspects of care by Arthroplasty Practitioners ( n= 35 Centres) New patient clinics 32% Pre-admission clinics 40% Consent 12% Waiting list management 56% Intra-operative (surgical management) 22% Ward work post op 10% Follow up to 1 year 80% Follow up over 1 year 92%
Overseas Experience - UK § Physios began seeing arthroplasty patients in mid 90’s in Edinburgh § Arthroplasty Care Practitioner Association, UK (ACPA) established in 2005 – includes nurses, physios, OTs Aspects of care by Arthroplasty Practitioners ( n= 35 Centres) New patient clinics 32% Pre-admission clinics 40% Consent 12% Waiting list management 56% Intra-operative (surgical management) 22% Ward work post op 10% Follow up to 1 year 80% Follow up over 1 year 92%
 Overseas Experience- Canada § Not as widespread as UK § Physios started in arthroplasty role about 5 years ago § Aitken et al, 2007: § 40 TKA and 40 THA seen by orthopaedic surgeon and physiotherapist § Harris Hip Score § Physio within 5 points of surgeon for 90% of cases § 4/80 patients recommended by surgeon to have required surgical review – physio also identified these 4 patients for surgical review
Overseas Experience- Canada § Not as widespread as UK § Physios started in arthroplasty role about 5 years ago § Aitken et al, 2007: § 40 TKA and 40 THA seen by orthopaedic surgeon and physiotherapist § Harris Hip Score § Physio within 5 points of surgeon for 90% of cases § 4/80 patients recommended by surgeon to have required surgical review – physio also identified these 4 patients for surgical review
 Aitken et al, 2007 § Authors concluded that: “a physiotherapist could effectively manage these patients for orthopaedic surgeons and this model of care could allow surgeons to spend more time in the operating room or assessing new patients with the potential to decrease waiting lists”
Aitken et al, 2007 § Authors concluded that: “a physiotherapist could effectively manage these patients for orthopaedic surgeons and this model of care could allow surgeons to spend more time in the operating room or assessing new patients with the potential to decrease waiting lists”
 Department of Health Grant: The PAR clinic 2010 Implementation phase OBJECTIVES: • To establish a pilot clinic concurrently with the Orthopaedic Outpatient Clinic called the Physiotherapy Arthroplasty Review (PAR) Clinic • To establish a process to measure & report on patient outcomes post routine orthopaedic surgery
Department of Health Grant: The PAR clinic 2010 Implementation phase OBJECTIVES: • To establish a pilot clinic concurrently with the Orthopaedic Outpatient Clinic called the Physiotherapy Arthroplasty Review (PAR) Clinic • To establish a process to measure & report on patient outcomes post routine orthopaedic surgery
 Implementation Phase: 2010 Inclusion Criteria: • Primary THA/TKA Any red flags identified on assessment must be discussed with surgeon Exclusion Criteria: • Revision surgery • Intra-operative fracture • Wound infections • Post-op complications • Primary Dx: Tumor, Paget's etc. • Complicated co-morbidities • Any other patient as identified by the ortho consultant at the time of surgery • Any patient requesting not to be seen in the PAR Clinic
Implementation Phase: 2010 Inclusion Criteria: • Primary THA/TKA Any red flags identified on assessment must be discussed with surgeon Exclusion Criteria: • Revision surgery • Intra-operative fracture • Wound infections • Post-op complications • Primary Dx: Tumor, Paget's etc. • Complicated co-morbidities • Any other patient as identified by the ortho consultant at the time of surgery • Any patient requesting not to be seen in the PAR Clinic
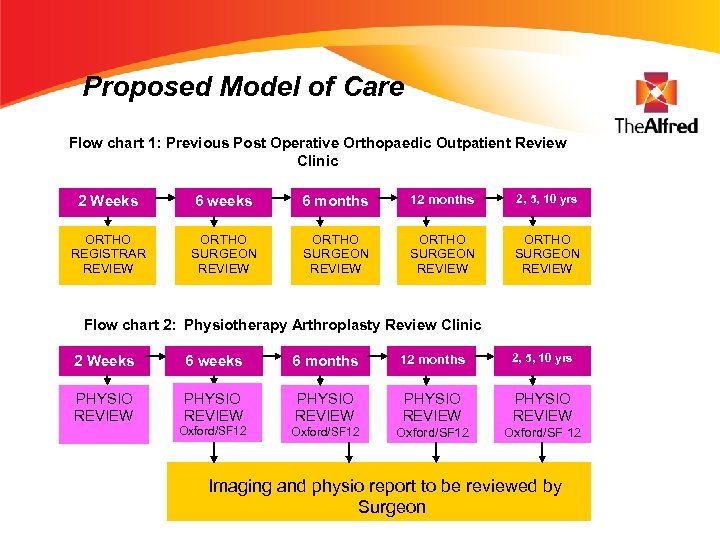 Proposed Model of Care Flow chart 1: Previous Post Operative Orthopaedic Outpatient Review Clinic 2 Weeks 6 weeks 6 months 12 months 2, 5, 10 yrs ORTHO REGISTRAR REVIEW ORTHO SURGEON REVIEW Flow chart 2: Physiotherapy Arthroplasty Review Clinic 2 Weeks 6 weeks 6 months 12 months 2, 5, 10 yrs PHYSIO REVIEW PHYSIO REVIEW Oxford/SF 12 Imaging and physio report to be reviewed by Surgeon
Proposed Model of Care Flow chart 1: Previous Post Operative Orthopaedic Outpatient Review Clinic 2 Weeks 6 weeks 6 months 12 months 2, 5, 10 yrs ORTHO REGISTRAR REVIEW ORTHO SURGEON REVIEW Flow chart 2: Physiotherapy Arthroplasty Review Clinic 2 Weeks 6 weeks 6 months 12 months 2, 5, 10 yrs PHYSIO REVIEW PHYSIO REVIEW Oxford/SF 12 Imaging and physio report to be reviewed by Surgeon
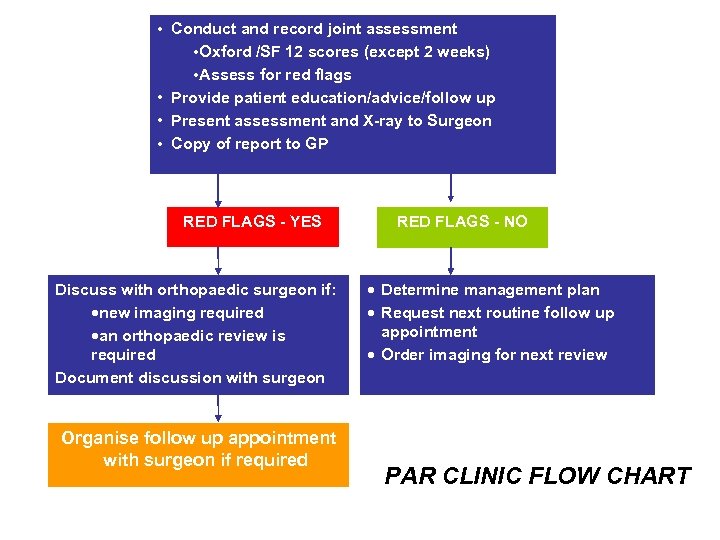 • Conduct and record joint assessment • Oxford /SF 12 scores (except 2 weeks) • Assess for red flags • Provide patient education/advice/follow up • Present assessment and X-ray to Surgeon • Copy of report to GP RED FLAGS - YES Discuss with orthopaedic surgeon if: ·new imaging required ·an orthopaedic review is required Document discussion with surgeon Organise follow up appointment with surgeon if required RED FLAGS - NO · Determine management plan · Request next routine follow up appointment · Order imaging for next review PAR CLINIC FLOW CHART
• Conduct and record joint assessment • Oxford /SF 12 scores (except 2 weeks) • Assess for red flags • Provide patient education/advice/follow up • Present assessment and X-ray to Surgeon • Copy of report to GP RED FLAGS - YES Discuss with orthopaedic surgeon if: ·new imaging required ·an orthopaedic review is required Document discussion with surgeon Organise follow up appointment with surgeon if required RED FLAGS - NO · Determine management plan · Request next routine follow up appointment · Order imaging for next review PAR CLINIC FLOW CHART
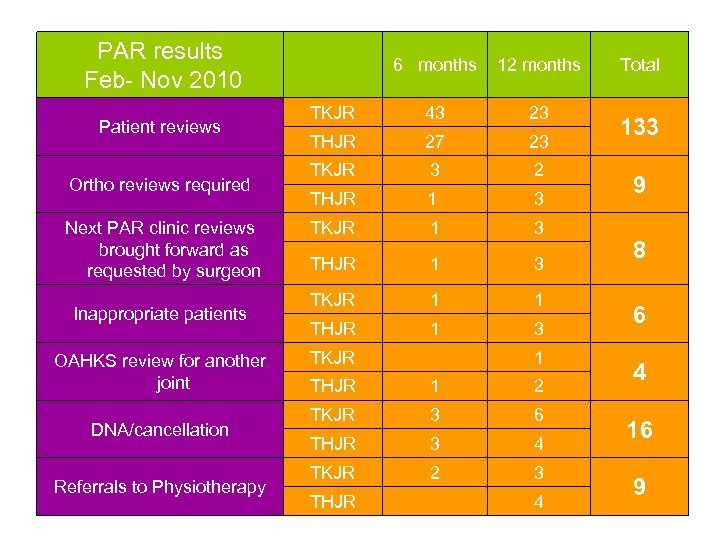 PAR results Feb- Nov 2010 Patient reviews Ortho reviews required Next PAR clinic reviews brought forward as requested by surgeon Inappropriate patients OAHKS review for another joint DNA/cancellation Referrals to Physiotherapy 6 months 12 months TKJR 43 23 THJR 27 23 TKJR 3 2 THJR 1 3 TKJR 1 3 THJR 1 3 TKJR 1 1 THJR 1 3 TKJR 1 THJR 1 2 TKJR 3 6 THJR 3 4 TKJR 2 3 THJR 4 Total 133 9 8 6 4 16 9
PAR results Feb- Nov 2010 Patient reviews Ortho reviews required Next PAR clinic reviews brought forward as requested by surgeon Inappropriate patients OAHKS review for another joint DNA/cancellation Referrals to Physiotherapy 6 months 12 months TKJR 43 23 THJR 27 23 TKJR 3 2 THJR 1 3 TKJR 1 3 THJR 1 3 TKJR 1 1 THJR 1 3 TKJR 1 THJR 1 2 TKJR 3 6 THJR 3 4 TKJR 2 3 THJR 4 Total 133 9 8 6 4 16 9
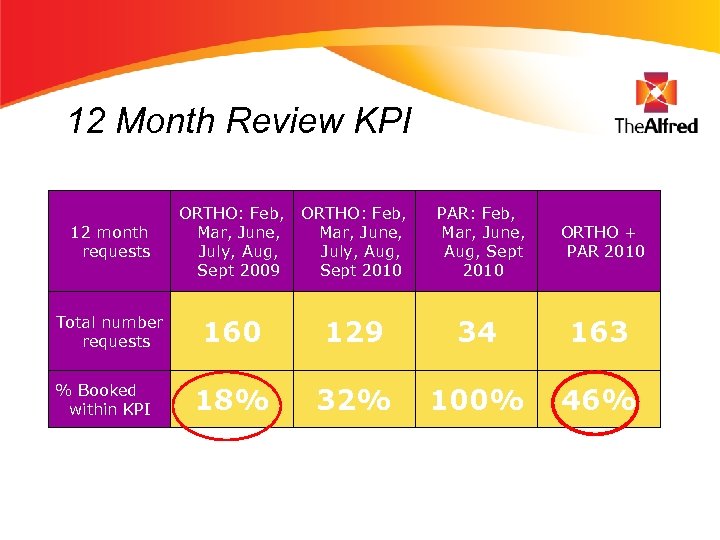 12 Month Review KPI 12 month requests ORTHO: Feb, Mar, June, July, Aug, Sept 2009 ORTHO: Feb, Mar, June, July, Aug, Sept 2010 PAR: Feb, Mar, June, Aug, Sept 2010 ORTHO + PAR 2010 Total number requests 160 129 34 163 18% 32% 100% 46% % Booked within KPI
12 Month Review KPI 12 month requests ORTHO: Feb, Mar, June, July, Aug, Sept 2009 ORTHO: Feb, Mar, June, July, Aug, Sept 2010 PAR: Feb, Mar, June, Aug, Sept 2010 ORTHO + PAR 2010 Total number requests 160 129 34 163 18% 32% 100% 46% % Booked within KPI
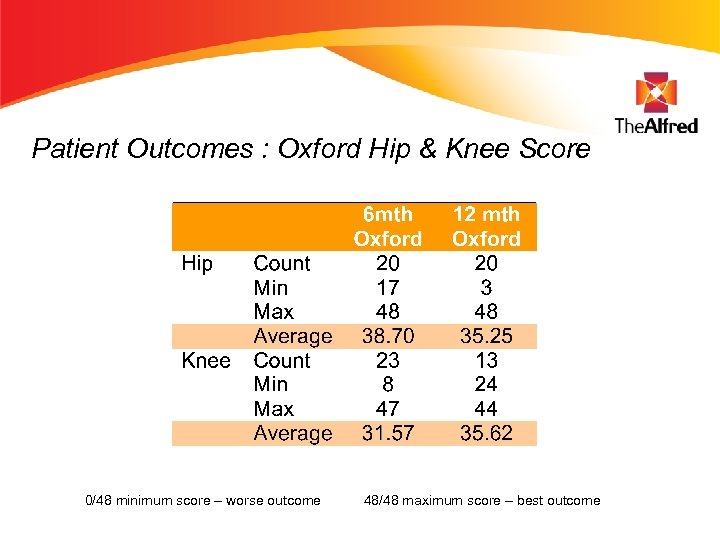 Patient Outcomes : Oxford Hip & Knee Score 0/48 minimum score – worse outcome 48/48 maximum score – best outcome
Patient Outcomes : Oxford Hip & Knee Score 0/48 minimum score – worse outcome 48/48 maximum score – best outcome
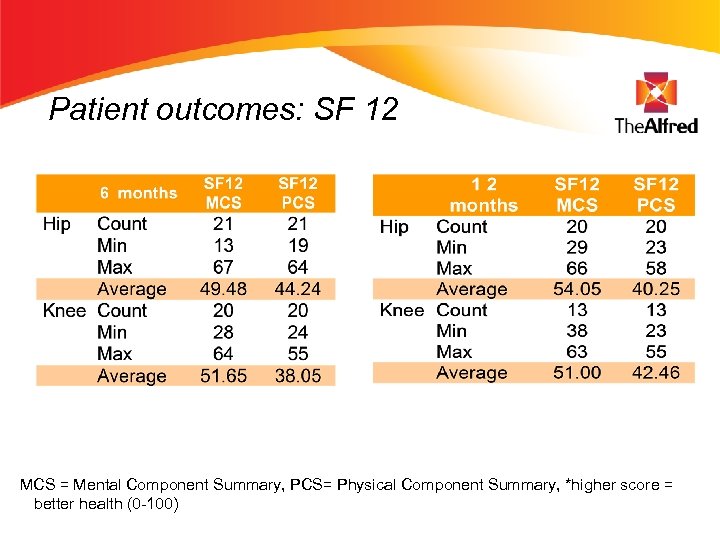 Patient outcomes: SF 12 MCS = Mental Component Summary, PCS= Physical Component Summary, *higher score = better health (0 -100)
Patient outcomes: SF 12 MCS = Mental Component Summary, PCS= Physical Component Summary, *higher score = better health (0 -100)
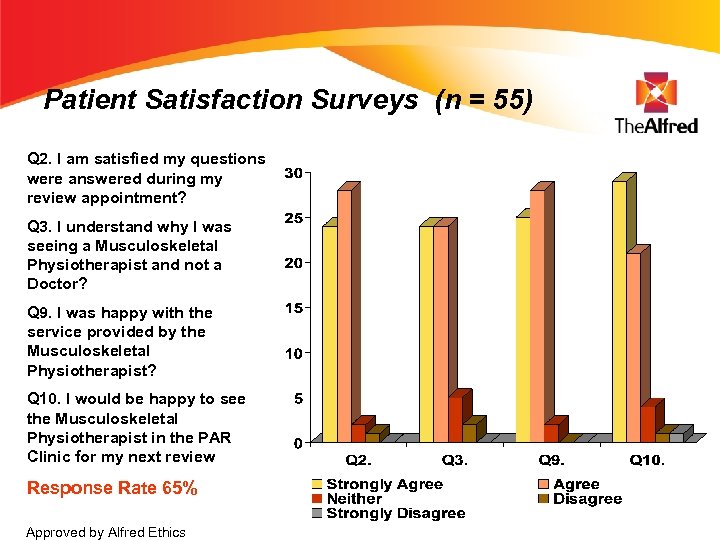 Patient Satisfaction Surveys (n = 55) Q 2. I am satisfied my questions were answered during my review appointment? Q 3. I understand why I was seeing a Musculoskeletal Physiotherapist and not a Doctor? Q 9. I was happy with the service provided by the Musculoskeletal Physiotherapist? Q 10. I would be happy to see the Musculoskeletal Physiotherapist in the PAR Clinic for my next review Response Rate 65% Approved by Alfred Ethics
Patient Satisfaction Surveys (n = 55) Q 2. I am satisfied my questions were answered during my review appointment? Q 3. I understand why I was seeing a Musculoskeletal Physiotherapist and not a Doctor? Q 9. I was happy with the service provided by the Musculoskeletal Physiotherapist? Q 10. I would be happy to see the Musculoskeletal Physiotherapist in the PAR Clinic for my next review Response Rate 65% Approved by Alfred Ethics
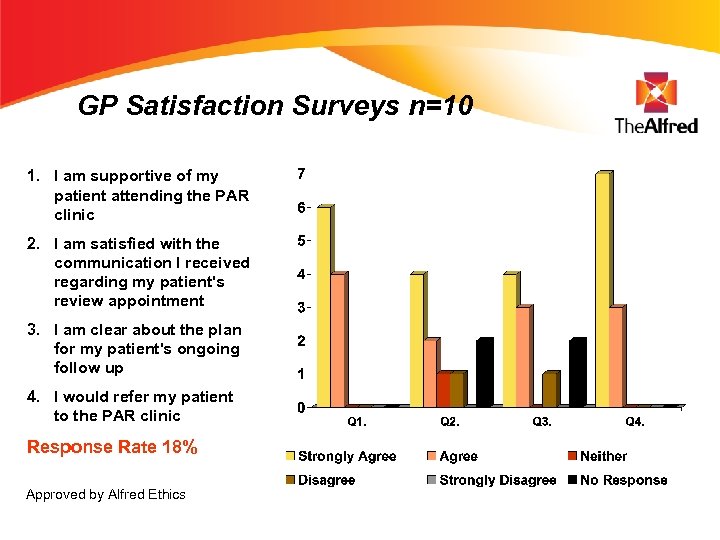 GP Satisfaction Surveys n=10 1. I am supportive of my patient attending the PAR clinic 2. I am satisfied with the communication I received regarding my patient's review appointment 3. I am clear about the plan for my patient's ongoing follow up 4. I would refer my patient to the PAR clinic Response Rate 18% Approved by Alfred Ethics
GP Satisfaction Surveys n=10 1. I am supportive of my patient attending the PAR clinic 2. I am satisfied with the communication I received regarding my patient's review appointment 3. I am clear about the plan for my patient's ongoing follow up 4. I would refer my patient to the PAR clinic Response Rate 18% Approved by Alfred Ethics
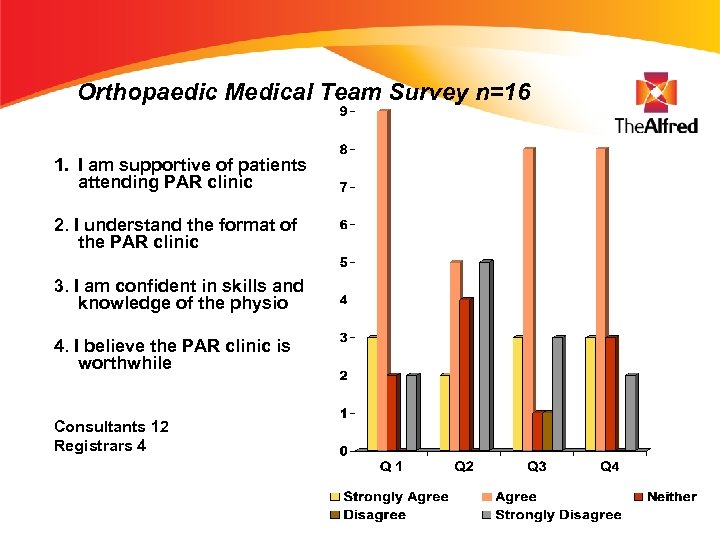 Orthopaedic Medical Team Survey n=16 1. I am supportive of patients attending PAR clinic 2. I understand the format of the PAR clinic 3. I am confident in skills and knowledge of the physio 4. I believe the PAR clinic is worthwhile Consultants 12 Registrars 4
Orthopaedic Medical Team Survey n=16 1. I am supportive of patients attending PAR clinic 2. I understand the format of the PAR clinic 3. I am confident in skills and knowledge of the physio 4. I believe the PAR clinic is worthwhile Consultants 12 Registrars 4
 Thank you
Thank you
 POST ARTHROPLASTY REVIEW CLINIC
POST ARTHROPLASTY REVIEW CLINIC
 Introduction • Commenced March 2009 (5 years) • Innovation grant Do. H • Need: ESAS program at St Vincent’s allowed good access to surgery but difficulty getting new patients in for initial appointment as 75% of surgeons list were review appointments. Two new operating theatres being built to further improve surgical throughput. • Supported and encouraged by Head of Orthopaedics.
Introduction • Commenced March 2009 (5 years) • Innovation grant Do. H • Need: ESAS program at St Vincent’s allowed good access to surgery but difficulty getting new patients in for initial appointment as 75% of surgeons list were review appointments. Two new operating theatres being built to further improve surgical throughput. • Supported and encouraged by Head of Orthopaedics.
 Structure of Clinic Vital that it is co-located but SPACE always an issue
Structure of Clinic Vital that it is co-located but SPACE always an issue
 Solution 730 am Monday morning so there would be a cross over with surgeons prior to them starting at 9: 00 am.
Solution 730 am Monday morning so there would be a cross over with surgeons prior to them starting at 9: 00 am.
 Framework of clinic • Time points to review patients • Exclusion and Inclusion • Key stake holders • X-ray: when, where and review • Establish Pathways for patients requiring immediate/review specialist consult • Administration: appointments, histories, questionnaires • Data collection: for whom and why • Documentation: patient records, letters to GP and other such as physiotherapy
Framework of clinic • Time points to review patients • Exclusion and Inclusion • Key stake holders • X-ray: when, where and review • Establish Pathways for patients requiring immediate/review specialist consult • Administration: appointments, histories, questionnaires • Data collection: for whom and why • Documentation: patient records, letters to GP and other such as physiotherapy
 THJR and TKJR 6 weeks : with surgeon (request for physio to see this cohort) 3 months: can be missed but must have a 6 month review 6 months: can be missed but must have had a 3 month review 12 months: standard review 3 yrs, 5 yrs and 10 yrs: standard reviews 10 plus: only if concerns (can be discharged at 10 yrs)
THJR and TKJR 6 weeks : with surgeon (request for physio to see this cohort) 3 months: can be missed but must have a 6 month review 6 months: can be missed but must have had a 3 month review 12 months: standard review 3 yrs, 5 yrs and 10 yrs: standard reviews 10 plus: only if concerns (can be discharged at 10 yrs)
 Framework of clinic • Time points to review patients • Exclusion and Inclusion • Identify keystake holders • X-ray: when, where and review • Establish Pathways for patients requiring immediate/review specialist consult • Administration: appointments, histories, questionnaires • Data collection: for whom and why • Documentation: patient records, letters to GP and other such as physiotherapy
Framework of clinic • Time points to review patients • Exclusion and Inclusion • Identify keystake holders • X-ray: when, where and review • Establish Pathways for patients requiring immediate/review specialist consult • Administration: appointments, histories, questionnaires • Data collection: for whom and why • Documentation: patient records, letters to GP and other such as physiotherapy
 Triaging referrals Inclusion criteria Exclusion criteria Knee Arthroplasty Tumour Hip Arthroplasty Pathological Fracture/Prothesis Normal Pathway Revision (early) Infection (acute) Intra-operative fracture
Triaging referrals Inclusion criteria Exclusion criteria Knee Arthroplasty Tumour Hip Arthroplasty Pathological Fracture/Prothesis Normal Pathway Revision (early) Infection (acute) Intra-operative fracture
 Framework of clinic • Time points to review patients • Exclusion and Inclusion • Key stake holders • X-ray: when, where and review • Establish Pathways for patients requiring immediate/review specialist consult • Administration: appointments, histories, questionnaires • Documentation: patient records, letters to GP and other such as physiotherapy • Data collection: for whom and why
Framework of clinic • Time points to review patients • Exclusion and Inclusion • Key stake holders • X-ray: when, where and review • Establish Pathways for patients requiring immediate/review specialist consult • Administration: appointments, histories, questionnaires • Documentation: patient records, letters to GP and other such as physiotherapy • Data collection: for whom and why
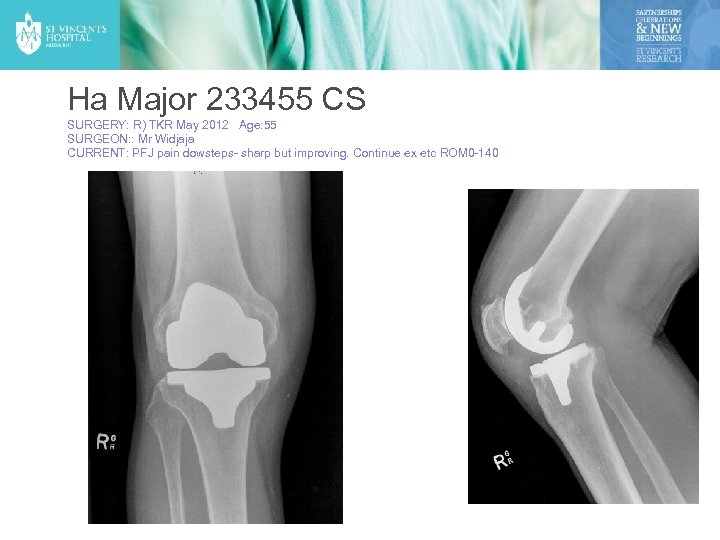 Ha Major 233455 CS SURGERY: R) TKR May 2012 Age: 55 SURGEON: : Mr Widjaja CURRENT: PFJ pain dowsteps- sharp but improving. Continue ex etc ROM 0 -140
Ha Major 233455 CS SURGERY: R) TKR May 2012 Age: 55 SURGEON: : Mr Widjaja CURRENT: PFJ pain dowsteps- sharp but improving. Continue ex etc ROM 0 -140
 Framework of clinic • Time points to review patients • Exclusion and Inclusion • Identify key stake holders • X-ray: when, where and review • Establish Pathways for patients requiring immediate/review specialist consult • Administration: appointments, histories, questionnaires • Documentation: patient records, letters to GP and other such as physiotherapy • Data collection: for whom and why
Framework of clinic • Time points to review patients • Exclusion and Inclusion • Identify key stake holders • X-ray: when, where and review • Establish Pathways for patients requiring immediate/review specialist consult • Administration: appointments, histories, questionnaires • Documentation: patient records, letters to GP and other such as physiotherapy • Data collection: for whom and why
 Evaluation Initial data was collected on the prospective patients suitable for the clinic. This data included the specific surgical technique and prosthesis, complications and comorbidities. Functional outcomes (SF 12), quality of life and physical measures (international knee society scores/harris hip scores and SF-12) are routinely collected on all patients. This information is recorded on the Orthopaedic database at St Vincent’s Hospital. Patient satisfaction questionnaires were collected during the implementation period on all patients and matched with a control group of patients who attended the routine Orthopaedic surgeon-led clinic. The aim of the questionnaire was to collect information on clinic processes and perceived outcomes from all patients and to enable a comparison between the two groups.
Evaluation Initial data was collected on the prospective patients suitable for the clinic. This data included the specific surgical technique and prosthesis, complications and comorbidities. Functional outcomes (SF 12), quality of life and physical measures (international knee society scores/harris hip scores and SF-12) are routinely collected on all patients. This information is recorded on the Orthopaedic database at St Vincent’s Hospital. Patient satisfaction questionnaires were collected during the implementation period on all patients and matched with a control group of patients who attended the routine Orthopaedic surgeon-led clinic. The aim of the questionnaire was to collect information on clinic processes and perceived outcomes from all patients and to enable a comparison between the two groups.
 Comparison: surgeon & physio led clinic HIPS: No significant differences between patients who attended the surgeon-led clinic and the physiotherapy-led clinic at 12 month review. KNEES: There were significant differences in the 12 month outcome measures. The IKS was significantly higher and the physical component of the SF-12 was significantly higher in the physiotherapy-led clinic group.
Comparison: surgeon & physio led clinic HIPS: No significant differences between patients who attended the surgeon-led clinic and the physiotherapy-led clinic at 12 month review. KNEES: There were significant differences in the 12 month outcome measures. The IKS was significantly higher and the physical component of the SF-12 was significantly higher in the physiotherapy-led clinic group.
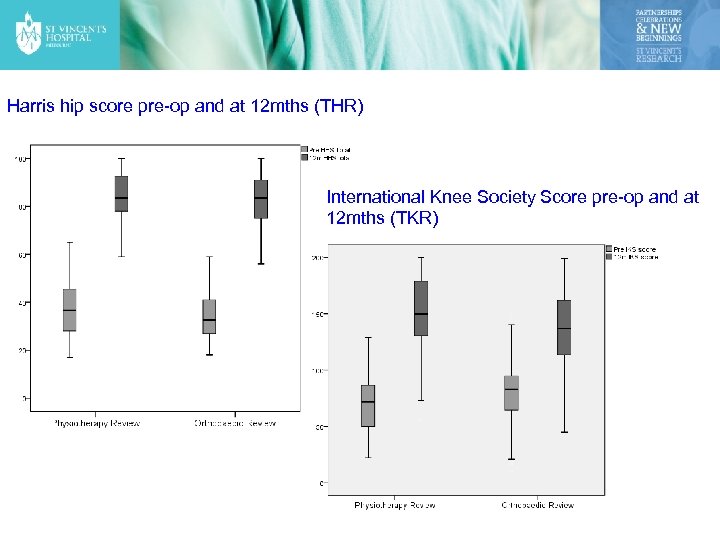 Harris hip score pre-op and at 12 mths (THR) International Knee Society Score pre-op and at 12 mths (TKR)
Harris hip score pre-op and at 12 mths (THR) International Knee Society Score pre-op and at 12 mths (TKR)

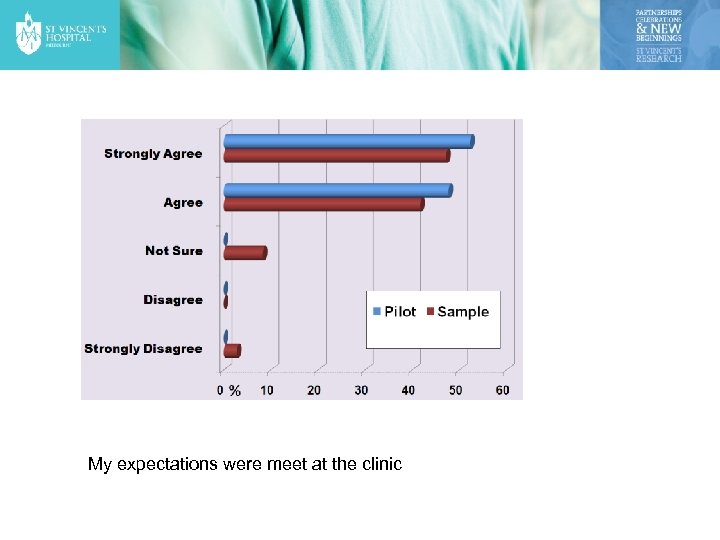 My expectations were meet at the clinic
My expectations were meet at the clinic
 Barriers to clinic • Being accepted (Orthopaedic surgeon, GP, nursing, executive, administration) as a useful and important team member in that role. • Establishing the best system/framework: this takes time • Space and administration for long term success • Barriers to quick access to orthopaedic surgeons or other health providers. • Physiotherapist can order plan X-rays but need sign off for ordering blood test and other imaging such as white blood cell nuclear bone scan. • Succession planning: training and maintaining an excellent level of skill
Barriers to clinic • Being accepted (Orthopaedic surgeon, GP, nursing, executive, administration) as a useful and important team member in that role. • Establishing the best system/framework: this takes time • Space and administration for long term success • Barriers to quick access to orthopaedic surgeons or other health providers. • Physiotherapist can order plan X-rays but need sign off for ordering blood test and other imaging such as white blood cell nuclear bone scan. • Succession planning: training and maintaining an excellent level of skill
 Time…….
Time…….
 Neurosurgery Screening clinic
Neurosurgery Screening clinic
 Physiotherapy Led Neurosurgery Spine Clinic at Melbourne Health Samantha Plumb / Uyen Phan
Physiotherapy Led Neurosurgery Spine Clinic at Melbourne Health Samantha Plumb / Uyen Phan
 Melbourne Health • MH provides services to the population in our primary and secondary catchment areas: > 1 million people
Melbourne Health • MH provides services to the population in our primary and secondary catchment areas: > 1 million people
 Neurosurgery Department • Conservatively driven organisation • Services are provided to the broader Victorian community and interstate • International reputation • Trauma and tumours a large focus • LBP a small component
Neurosurgery Department • Conservatively driven organisation • Services are provided to the broader Victorian community and interstate • International reputation • Trauma and tumours a large focus • LBP a small component
 Physiotherapy • 80 EFT across the acute and subacute sites • Musc team at both sites • Advanced clinics currently at the acute site • 6 advanced practice physios, casuals
Physiotherapy • 80 EFT across the acute and subacute sites • Musc team at both sites • Advanced clinics currently at the acute site • 6 advanced practice physios, casuals
 Advanced Practice Clinics • • ED 2004 OAHKS 2006 Orthopaedic Spine 2006 STI 2007 Shoulder 2008 JRS 2009 Neurosurgery 2009
Advanced Practice Clinics • • ED 2004 OAHKS 2006 Orthopaedic Spine 2006 STI 2007 Shoulder 2008 JRS 2009 Neurosurgery 2009
 Neurosurgery Clinic drivers for change • • • Applies to all advanced practice roles Low back pain (condition) common High number of patient referrals Waitlist and access issues Low conversion rate to surgery Majority haven’t trialled conservative options • Model successful in other clinics
Neurosurgery Clinic drivers for change • • • Applies to all advanced practice roles Low back pain (condition) common High number of patient referrals Waitlist and access issues Low conversion rate to surgery Majority haven’t trialled conservative options • Model successful in other clinics
 Implementation of the Physiotherapy Led Neurosurgical Clinic at MH Do. H funded 1 year trial - July 2009 - 2010 - Developed inclusion and exclusion criteria - 3 clinics: 10 new and 8 review appointments per week - 2 physio training up at the same time - Both had post grad qualifications
Implementation of the Physiotherapy Led Neurosurgical Clinic at MH Do. H funded 1 year trial - July 2009 - 2010 - Developed inclusion and exclusion criteria - 3 clinics: 10 new and 8 review appointments per week - 2 physio training up at the same time - Both had post grad qualifications
 Patient Selection Neurosurgery Outpatient Clinic Urgent or Next Available (N/A) Physiotherapy-Led Clinic* Mechanical spinal pain +/- limb pain Absence of neurological signs Likelihood of surgery is low * No previous input from Neurosurgery unit
Patient Selection Neurosurgery Outpatient Clinic Urgent or Next Available (N/A) Physiotherapy-Led Clinic* Mechanical spinal pain +/- limb pain Absence of neurological signs Likelihood of surgery is low * No previous input from Neurosurgery unit
 Clinic Procedure Routine assessment including: Red flag screening questionnaire Neurological testing: Reflexes, sensation, strength Radiological imaging: Relevance to the clinical picture Management plan including patient education Letters: GP, Community Physiotherapist Review 3 -6 months
Clinic Procedure Routine assessment including: Red flag screening questionnaire Neurological testing: Reflexes, sensation, strength Radiological imaging: Relevance to the clinical picture Management plan including patient education Letters: GP, Community Physiotherapist Review 3 -6 months
 Key Points for implementation • • • Identified need for change eg: waitlist/access Support from key stakeholders Collaboration with neurosurgeons Change management strategies Collection of data during implementation phase, important for Do. H final report, clinic evaluation and sustainability (business case) and growth for other APP clinics • Process maps
Key Points for implementation • • • Identified need for change eg: waitlist/access Support from key stakeholders Collaboration with neurosurgeons Change management strategies Collection of data during implementation phase, important for Do. H final report, clinic evaluation and sustainability (business case) and growth for other APP clinics • Process maps
 Process maps
Process maps
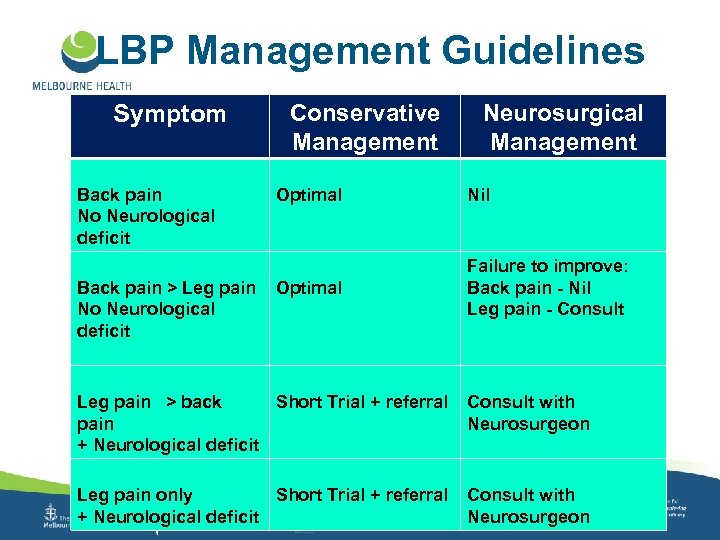 LBP Management Guidelines Symptom Back pain No Neurological deficit Back pain > Leg pain No Neurological deficit Conservative Management Neurosurgical Management Optimal Nil Optimal Failure to improve: Back pain - Nil Leg pain - Consult Leg pain > back Short Trial + referral pain + Neurological deficit Consult with Neurosurgeon Leg pain only Short Trial + referral + Neurological deficit Consult with Neurosurgeon
LBP Management Guidelines Symptom Back pain No Neurological deficit Back pain > Leg pain No Neurological deficit Conservative Management Neurosurgical Management Optimal Nil Optimal Failure to improve: Back pain - Nil Leg pain - Consult Leg pain > back Short Trial + referral pain + Neurological deficit Consult with Neurosurgeon Leg pain only Short Trial + referral + Neurological deficit Consult with Neurosurgeon
 Key Points for Implementation • • Triage process Exclusion/inclusion criteria Red and yellow flags Orientation Management guidelines
Key Points for Implementation • • Triage process Exclusion/inclusion criteria Red and yellow flags Orientation Management guidelines
 Orientation Management Guidelines
Orientation Management Guidelines
 Key points for Implementation • Business case submitted to MH following 1 year pilot • Exec supported the need for new models of care, 2 ongoing clinics per week supported
Key points for Implementation • Business case submitted to MH following 1 year pilot • Exec supported the need for new models of care, 2 ongoing clinics per week supported
 Key Considerations • • • Variability amongst surgeons Succession planning (nsurg) Leave management Space Admin support for dictation Access to surgeons for opinions, spread the load Register of radiology requests for each patient Register of credentialing Lack of and variable quality/availability of community resources
Key Considerations • • • Variability amongst surgeons Succession planning (nsurg) Leave management Space Admin support for dictation Access to surgeons for opinions, spread the load Register of radiology requests for each patient Register of credentialing Lack of and variable quality/availability of community resources
 Successes • Resource to surgeon for non surgical options including physio and a whole management plan (other AH) • Networking and advocacy for profession, community physio • Improved understanding of physiotherapy • Collaboration with Western Health for similar clinic
Successes • Resource to surgeon for non surgical options including physio and a whole management plan (other AH) • Networking and advocacy for profession, community physio • Improved understanding of physiotherapy • Collaboration with Western Health for similar clinic
 Successes • • • Developed triage guidelines Developed procedure (CPGs nsurg) Developed clinical protocols Education for GPs referring in Clinical governance (eg: peer review process) • WBA for credentialling process
Successes • • • Developed triage guidelines Developed procedure (CPGs nsurg) Developed clinical protocols Education for GPs referring in Clinical governance (eg: peer review process) • WBA for credentialling process
 Management Guidelines for GPs
Management Guidelines for GPs
 Neurosurgery Clinical Practice Guideline
Neurosurgery Clinical Practice Guideline
 What could have been done better • Succession planning • Establishing better links with community services • Limited internal outpatient services to support APP clinics (city, parking, high demand for services, focus on acute – chronic patients) • Think about patient journey and options for management
What could have been done better • Succession planning • Establishing better links with community services • Limited internal outpatient services to support APP clinics (city, parking, high demand for services, focus on acute – chronic patients) • Think about patient journey and options for management
 Moving Forward • Currently in collaboration with 2 community health centres and INWML to develop an interface clinic set in subacute / community to manage back pain • Referrals for rheum, ortho and nsurg combined • “One stop shop”
Moving Forward • Currently in collaboration with 2 community health centres and INWML to develop an interface clinic set in subacute / community to manage back pain • Referrals for rheum, ortho and nsurg combined • “One stop shop”


