e3a83b3f0ffd2fb6cfcde548c48641f3.ppt
- Количество слайдов: 17
 Population Trends in the Incidence and Outcomes of Acute Myocardial Infarction Robert W. Yeh, MD MSc Massachusetts General Hospital Alan S. Go, MD Kaiser Division of Research University of California, San Francisco
Population Trends in the Incidence and Outcomes of Acute Myocardial Infarction Robert W. Yeh, MD MSc Massachusetts General Hospital Alan S. Go, MD Kaiser Division of Research University of California, San Francisco
 BACKGROUND The “Ecosystem” of Acute Myocardial Infarction Widespread use of statins Obese population rising DM & HTN increasing Population at Risk for Myocardial Infarction Better antiplatelet therapy More use of beta blockers and ACE-I Aging of the population Increased use of smoking cessation programs NET EFFECT?
BACKGROUND The “Ecosystem” of Acute Myocardial Infarction Widespread use of statins Obese population rising DM & HTN increasing Population at Risk for Myocardial Infarction Better antiplatelet therapy More use of beta blockers and ACE-I Aging of the population Increased use of smoking cessation programs NET EFFECT?
 Existing Recent Literature on Myocardial Infarction Incidence - Mostly limited to trends prior to 2002 - Focused on groups with limited diversity with respect to race and ethnic group, age and sex - Have not distinguished ST and non-ST-elevation MI - Have not examined trends in improvements in outpatient cardiovascular medication use
Existing Recent Literature on Myocardial Infarction Incidence - Mostly limited to trends prior to 2002 - Focused on groups with limited diversity with respect to race and ethnic group, age and sex - Have not distinguished ST and non-ST-elevation MI - Have not examined trends in improvements in outpatient cardiovascular medication use
 OBJECTIVE Goals of Proposed Research To provide a comprehensive, contemporary assessment of the epidemiology of STEMI and NSTEMI in a large population-based sample between 1999 and 2008 • An evaluation of progress in the care of MI patients • A test of the true impact of medical and public health interventions • Suggestions for more optimal health resource allocation
OBJECTIVE Goals of Proposed Research To provide a comprehensive, contemporary assessment of the epidemiology of STEMI and NSTEMI in a large population-based sample between 1999 and 2008 • An evaluation of progress in the care of MI patients • A test of the true impact of medical and public health interventions • Suggestions for more optimal health resource allocation
 Kaiser Permanente of Northern California • Integrated health care delivery system providing comprehensive care of ~3. 3 million persons • 20 medical centers + large set of ambulatory practices • Diverse population representative of northern California and statewide • Low churn rate
Kaiser Permanente of Northern California • Integrated health care delivery system providing comprehensive care of ~3. 3 million persons • 20 medical centers + large set of ambulatory practices • Diverse population representative of northern California and statewide • Low churn rate
 METHODS Incidence of Myocardial Infarction Incidence rates of STEMI and NSTEMI calculated for each year – All Kaiser members age ≥ 30 – Numerator: Hospitalized admission for MI based on ICD-9 -CM primary discharge diagnosis. • STEMI: 4101 – 410. 6, 410. 8 • NSTEMI 410. 7, 410. 9 • Codes validated by detailed chart review in a random sample of 800 MI admissions. – Denominator: Person-months, annualized, based on monthly updated membership status. – Direct Age-Sex adjustment
METHODS Incidence of Myocardial Infarction Incidence rates of STEMI and NSTEMI calculated for each year – All Kaiser members age ≥ 30 – Numerator: Hospitalized admission for MI based on ICD-9 -CM primary discharge diagnosis. • STEMI: 4101 – 410. 6, 410. 8 • NSTEMI 410. 7, 410. 9 • Codes validated by detailed chart review in a random sample of 800 MI admissions. – Denominator: Person-months, annualized, based on monthly updated membership status. – Direct Age-Sex adjustment
 Comprehensive Clinical and Administrative Electronic Databases Health plan databases capture the large majority of aspects of clinical care and linked through single medical record number • Detailed demographic information • Multiple data sources to ascertain comorbid conditions • Longitudinal outpatient prescription medication use before and after incident MI • Outcomes – detailed discharge and billing codes with access to medical records; linked to state death files and Social Security Administration vital status data
Comprehensive Clinical and Administrative Electronic Databases Health plan databases capture the large majority of aspects of clinical care and linked through single medical record number • Detailed demographic information • Multiple data sources to ascertain comorbid conditions • Longitudinal outpatient prescription medication use before and after incident MI • Outcomes – detailed discharge and billing codes with access to medical records; linked to state death files and Social Security Administration vital status data
 Outcomes Cardiac Biomarkers – Peak CK-MB and MB fraction ascertained for all identified MI admissions Mortality – 30 -day all-cause mortality ascertained from linked health plan administrative databases, proxy information, Social Security Administration vital status files, and California state death certificate information – Logistic regression using generalized estimating equations to account for facility-based clustering used to examine trends in yearly adjusted mortality.
Outcomes Cardiac Biomarkers – Peak CK-MB and MB fraction ascertained for all identified MI admissions Mortality – 30 -day all-cause mortality ascertained from linked health plan administrative databases, proxy information, Social Security Administration vital status files, and California state death certificate information – Logistic regression using generalized estimating equations to account for facility-based clustering used to examine trends in yearly adjusted mortality.
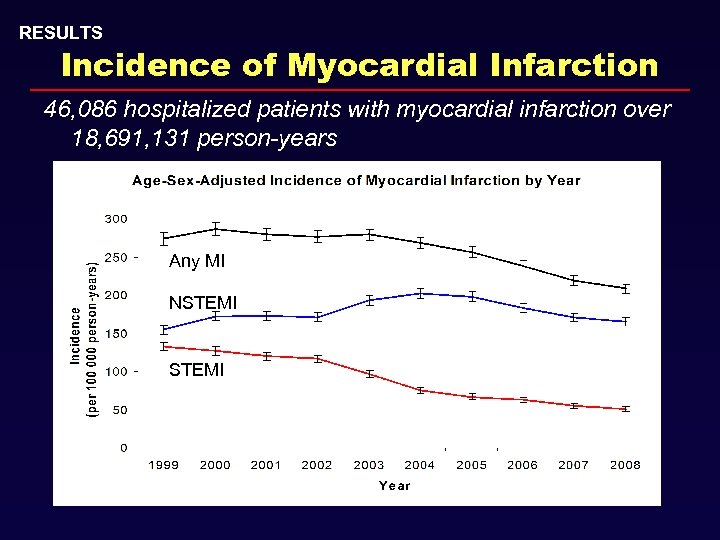 RESULTS Incidence of Myocardial Infarction 46, 086 hospitalized patients with myocardial infarction over 18, 691, 131 person-years Any MI NSTEMI
RESULTS Incidence of Myocardial Infarction 46, 086 hospitalized patients with myocardial infarction over 18, 691, 131 person-years Any MI NSTEMI
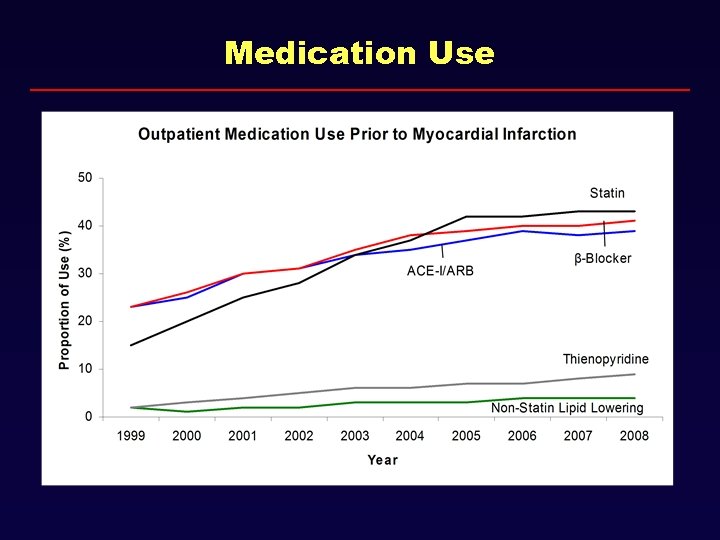 Medication Use
Medication Use
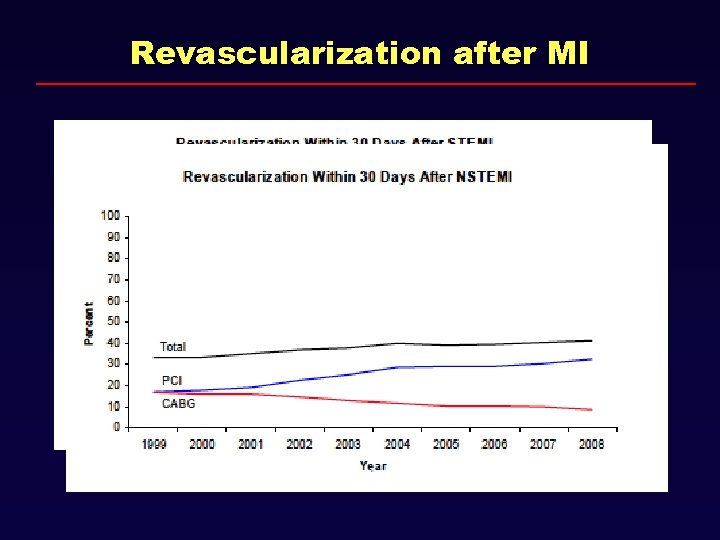 Revascularization after MI
Revascularization after MI
 Biomarkers • Troponin I testing increased from 53% in 1999 to 84% in 2004 – Stable testing rates after 2004 • Peak CK-MB and CK-MB fraction decreased significantly over time for all MI and for NSTEMI. • No change in biomarker peak levels over time after STEMI
Biomarkers • Troponin I testing increased from 53% in 1999 to 84% in 2004 – Stable testing rates after 2004 • Peak CK-MB and CK-MB fraction decreased significantly over time for all MI and for NSTEMI. • No change in biomarker peak levels over time after STEMI
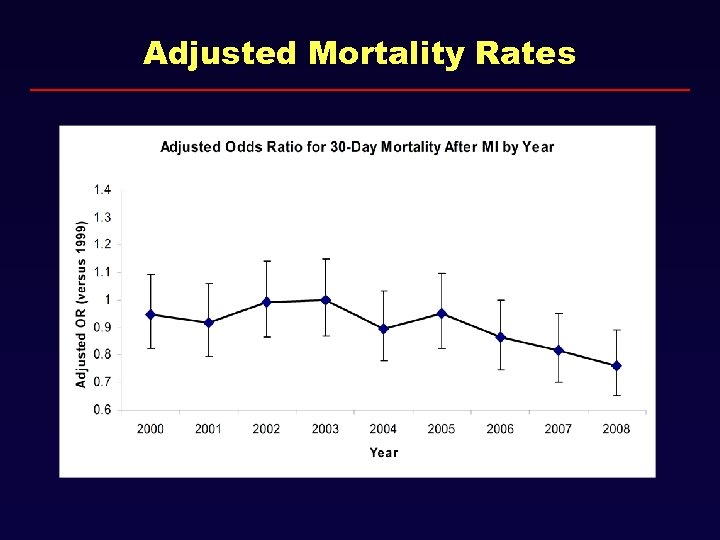 Adjusted Mortality Rates
Adjusted Mortality Rates
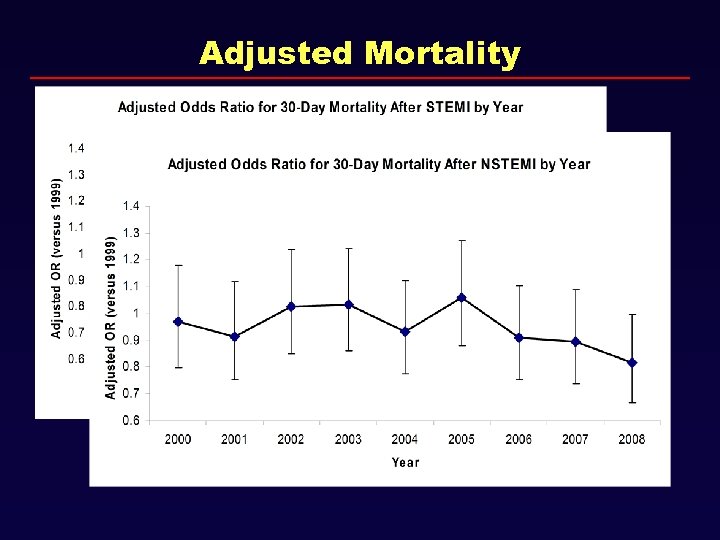 Adjusted Mortality
Adjusted Mortality
 Conclusions • There has been a 24% decline in the incidence of MI since 2000, with steep decline in STEMI incidence throughout time period. • Significant improvements in the outpatient use of cardiovascular medications including statins and beta blockers have occurred, which may, in part, explain declines in MI incidence. • Lower severity NSTEMI have been detected over time, coinciding with increased use of troponin. • Improvements in adjusted mortality have been modest, and are likely driven by in part by increased ascertainment of low-acuity NSTEMI
Conclusions • There has been a 24% decline in the incidence of MI since 2000, with steep decline in STEMI incidence throughout time period. • Significant improvements in the outpatient use of cardiovascular medications including statins and beta blockers have occurred, which may, in part, explain declines in MI incidence. • Lower severity NSTEMI have been detected over time, coinciding with increased use of troponin. • Improvements in adjusted mortality have been modest, and are likely driven by in part by increased ascertainment of low-acuity NSTEMI
 Limitations • Reliance on diagnosis codes – Sensitivity analyses that broadened the definition of MI to include other codes showed similar trends. – Trends in STEMI and NSTEMI were similar at 95% confidence limits of positive predictive value of codes based on validation. • Large, diverse population but may not be completely generalizable to all health care settings and populations Whether declines in MI incidence have occurred similarly in other geographic regions is not known.
Limitations • Reliance on diagnosis codes – Sensitivity analyses that broadened the definition of MI to include other codes showed similar trends. – Trends in STEMI and NSTEMI were similar at 95% confidence limits of positive predictive value of codes based on validation. • Large, diverse population but may not be completely generalizable to all health care settings and populations Whether declines in MI incidence have occurred similarly in other geographic regions is not known.
 Thank You
Thank You


