ed2de6bfb102dfaadccba8104d82d407.ppt
- Количество слайдов: 77
 Pierce County Health. Watch June 26, 2014 Mike Rust, Chief Operating Officer ABC for Rural Health, Inc. 100 Polk County Plaza, Suite 180 Balsam Lake, WI 54810 (715) 485 -8525 miker@co. polk. wi. us 3/17/2018 1
Pierce County Health. Watch June 26, 2014 Mike Rust, Chief Operating Officer ABC for Rural Health, Inc. 100 Polk County Plaza, Suite 180 Balsam Lake, WI 54810 (715) 485 -8525 miker@co. polk. wi. us 3/17/2018 1
 ABC for Rural Health, Inc. A Wisconsin-based nonprofit public interest law firm dedicated to linking children and families, particularly those with special health care needs, to health care benefits and services. 3/17/2018 2
ABC for Rural Health, Inc. A Wisconsin-based nonprofit public interest law firm dedicated to linking children and families, particularly those with special health care needs, to health care benefits and services. 3/17/2018 2
 Patient Protection and Affordable Care Act 3/17/2018 3
Patient Protection and Affordable Care Act 3/17/2018 3
 Affordable Care Act • Open Enrollment – 11/15/2014 – 2/15/2015 • SEP’s – Loss of Minimum Essential Coverage – Changes in life circumstances – Enrollment problems – Exceptional circumstances 3/17/2018 4
Affordable Care Act • Open Enrollment – 11/15/2014 – 2/15/2015 • SEP’s – Loss of Minimum Essential Coverage – Changes in life circumstances – Enrollment problems – Exceptional circumstances 3/17/2018 4
 Loss of Minimum Essential Coverage • MEC is cancelled, involuntarily terminated, or ends before January 2015 • Loss of job is common • Must be involuntary • MEC includes Medicaid and Badger. Care • New coverage must begin on the 1 st day of the month after MEC ended 3/17/2018 5
Loss of Minimum Essential Coverage • MEC is cancelled, involuntarily terminated, or ends before January 2015 • Loss of job is common • Must be involuntary • MEC includes Medicaid and Badger. Care • New coverage must begin on the 1 st day of the month after MEC ended 3/17/2018 5
 Changes in Life Circumstances • Turning 26 • Moving to where the plans are different • Adding a dependent (marriage, birth, adoption, foster care placement) – In the last 3, new coverage must start the date of that event, regardless of plan enrollment date • Divorce or death must also include loss of MEC 3/17/2018 6
Changes in Life Circumstances • Turning 26 • Moving to where the plans are different • Adding a dependent (marriage, birth, adoption, foster care placement) – In the last 3, new coverage must start the date of that event, regardless of plan enrollment date • Divorce or death must also include loss of MEC 3/17/2018 6
 Enrollment Problems • Unable to enroll • Error, misrepresentation, or inaction of an official or agent, misconduct, material violation of the contract by a plan • Individuals who were « in line » • Individuals who were denied Medicaid, but notified until after open enrollment 3/17/2018 7
Enrollment Problems • Unable to enroll • Error, misrepresentation, or inaction of an official or agent, misconduct, material violation of the contract by a plan • Individuals who were « in line » • Individuals who were denied Medicaid, but notified until after open enrollment 3/17/2018 7
 Exceptional Circumstances Losing eligibility for a hardship exemption Surviving domestic violence (until May 30) Loss of HIRSP (Until May 1) Seeking to terminate COBRA (until July 1) Loss of an individual plan outside of open enrollment • Service in Ameri. Corps, VISTA, NCCC • • • 3/17/2018 8
Exceptional Circumstances Losing eligibility for a hardship exemption Surviving domestic violence (until May 30) Loss of HIRSP (Until May 1) Seeking to terminate COBRA (until July 1) Loss of an individual plan outside of open enrollment • Service in Ameri. Corps, VISTA, NCCC • • • 3/17/2018 8
 Other Examples • Unexpected hospitalization or temporary cognitive disability • Natural disaster • Technical error between Marketplace and plan • Immigration system error • Display of incorrect plan data 3/17/2018 9
Other Examples • Unexpected hospitalization or temporary cognitive disability • Natural disaster • Technical error between Marketplace and plan • Immigration system error • Display of incorrect plan data 3/17/2018 9
 System Appeals • • • Whether you’re eligible to buy a Marketplace plan Whether you can enroll in a Marketplace plan outside the regular open enrollment period Whether you’re eligible for lower costs based on your income The amount of savings you’re eligible for Whether you’re eligible for Medicaid or the Children’s Health Insurance Program (CHIP) Whether you are eligible for an exemption from the individual responsibility requirement 3/17/2018 10
System Appeals • • • Whether you’re eligible to buy a Marketplace plan Whether you can enroll in a Marketplace plan outside the regular open enrollment period Whether you’re eligible for lower costs based on your income The amount of savings you’re eligible for Whether you’re eligible for Medicaid or the Children’s Health Insurance Program (CHIP) Whether you are eligible for an exemption from the individual responsibility requirement 3/17/2018 10
 System Appeals • Send a letter or a Wisconsin appeal form to – Health Insurance Marketplace 465 Industrial Blvd. London, KY 40750 -0061 • Wisconsin appeal form location – https: //www. healthcare. gov/downloads/market place-appeal-request-form-a. pdf – Appeals may be expedited. You may ask for representation. Should be done in 90 days. 3/17/2018 11
System Appeals • Send a letter or a Wisconsin appeal form to – Health Insurance Marketplace 465 Industrial Blvd. London, KY 40750 -0061 • Wisconsin appeal form location – https: //www. healthcare. gov/downloads/market place-appeal-request-form-a. pdf – Appeals may be expedited. You may ask for representation. Should be done in 90 days. 3/17/2018 11
 Plan Appeals • Your insurer must notify you of denials in writing and explain why: – Within 15 days if you’re seeking prior authorization for a treatment – Within 30 days for medical services already received – Within 72 hours for urgent care cases 3/17/2018 12
Plan Appeals • Your insurer must notify you of denials in writing and explain why: – Within 15 days if you’re seeking prior authorization for a treatment – Within 30 days for medical services already received – Within 72 hours for urgent care cases 3/17/2018 12
 Internal Appeals • Must file internal appeal within 180 days • Appeal must be decided within 30 days if you have not received the service and 60 days if you have received the service • Then you may seek external appeal • You may request an expedited appeal for urgent situations 3/17/2018 13
Internal Appeals • Must file internal appeal within 180 days • Appeal must be decided within 30 days if you have not received the service and 60 days if you have received the service • Then you may seek external appeal • You may request an expedited appeal for urgent situations 3/17/2018 13
 OCI RE: Training • Nonnavigator assisters, including certified application counselors, are required to complete 8 hours of health insurance continuing education training annually. • Entities must attest to training on an OCI attestation form by October 1 annually • This guidance does not apply to navigators. 3/17/2018 14
OCI RE: Training • Nonnavigator assisters, including certified application counselors, are required to complete 8 hours of health insurance continuing education training annually. • Entities must attest to training on an OCI attestation form by October 1 annually • This guidance does not apply to navigators. 3/17/2018 14
 Required Topics 1. Principles of health insurance 2. Wisconsin health insurance laws and regulations 3. Public health program law, regulations and guidance including Badger. Care and Medicare 4. Federal Affordable Care Act law, regulations and guidance 5. Privacy and Security Guidelines - Personally Identifiable Information (PII) 3/17/2018 15
Required Topics 1. Principles of health insurance 2. Wisconsin health insurance laws and regulations 3. Public health program law, regulations and guidance including Badger. Care and Medicare 4. Federal Affordable Care Act law, regulations and guidance 5. Privacy and Security Guidelines - Personally Identifiable Information (PII) 3/17/2018 15
 3/17/2018 16
3/17/2018 16
 ACA Discussion • • • Provider network issues Outreach, Education and Enrollment Review Plans for now and for next open enrollment Problems Training and resource needs 3/17/2018 17
ACA Discussion • • • Provider network issues Outreach, Education and Enrollment Review Plans for now and for next open enrollment Problems Training and resource needs 3/17/2018 17
 Paul Wellstone and Pete Domenici Mental Health Parity and Addiction Equity Act of 2008 (MHPAEA) 3/17/2018 18
Paul Wellstone and Pete Domenici Mental Health Parity and Addiction Equity Act of 2008 (MHPAEA) 3/17/2018 18
 MHPAEA Basic Requirement • A plan may not apply any financial requirement or treatment limitation to mental health or substance use disorder benefits in any classification that is more restrictive than the predominant financial requirement or treatment limitation applied to substantially all medical/surgical benefits in the same classification 3/17/2018 19
MHPAEA Basic Requirement • A plan may not apply any financial requirement or treatment limitation to mental health or substance use disorder benefits in any classification that is more restrictive than the predominant financial requirement or treatment limitation applied to substantially all medical/surgical benefits in the same classification 3/17/2018 19
 MHPAEA Categories • Financial requirements – e. g. , deductibles, copayments, coinsurance, out-of-pocket maximums • Treatment limitations – limit benefits based on frequency of treatment, number of visits, days of coverage, days in a waiting period, and “other similar limits on the scope and duration of treatment”. – Quantitative treatment limitation – expressed numerically, e. g. , annual limit of 50 outpatient visits – Nonquantitative treatment limitation – not expressed numerically but otherwise limits the scope or duration of benefits 3/17/2018 20
MHPAEA Categories • Financial requirements – e. g. , deductibles, copayments, coinsurance, out-of-pocket maximums • Treatment limitations – limit benefits based on frequency of treatment, number of visits, days of coverage, days in a waiting period, and “other similar limits on the scope and duration of treatment”. – Quantitative treatment limitation – expressed numerically, e. g. , annual limit of 50 outpatient visits – Nonquantitative treatment limitation – not expressed numerically but otherwise limits the scope or duration of benefits 3/17/2018 20
 Quantitative • A particular type of financial requirement or QTL must apply to substantially all (2/3) of med-surg benefits in a classification before it may be applied to MH/SUD benefits. • If requirement applies to 2/3, then permissible level of that limit is set by predominant level that applies to 50% 3/17/2018 21
Quantitative • A particular type of financial requirement or QTL must apply to substantially all (2/3) of med-surg benefits in a classification before it may be applied to MH/SUD benefits. • If requirement applies to 2/3, then permissible level of that limit is set by predominant level that applies to 50% 3/17/2018 21
 Non-Quantifiable (NQTL’s) • Any non-numerical limits to scope or duration of treatment (processes, strategies, evidentiary standards or other factors) used in applying an NQTL to MH/SUD benefits must be applied comparably and no more stringently than those are applied to medicalsurgical benefits 3/17/2018 22
Non-Quantifiable (NQTL’s) • Any non-numerical limits to scope or duration of treatment (processes, strategies, evidentiary standards or other factors) used in applying an NQTL to MH/SUD benefits must be applied comparably and no more stringently than those are applied to medicalsurgical benefits 3/17/2018 22
 Sample NQTL’s • • • Medical management standards Prescription drug formulary designs Standards for provider admission to a network Determination of UCR amounts Requirements to use less costly first Requirements to complete a course of treatment 3/17/2018 23
Sample NQTL’s • • • Medical management standards Prescription drug formulary designs Standards for provider admission to a network Determination of UCR amounts Requirements to use less costly first Requirements to complete a course of treatment 3/17/2018 23
 6 Benefit Classifications • • • Inpatient, in-network Inpatient, out-of-network Outpatient*, in-network Outpatient*, out-of-network Emergency care Prescription drugs *May use sub-classifications of office visits vs all other care 3/17/2018 24
6 Benefit Classifications • • • Inpatient, in-network Inpatient, out-of-network Outpatient*, in-network Outpatient*, out-of-network Emergency care Prescription drugs *May use sub-classifications of office visits vs all other care 3/17/2018 24
 Parity Scope & Timeline • Applies to both mental health and substance use disorder (MH/SUD) benefits • Generally effective for plan years after October 3, 2009. Fully effective 1/1/11. • Interim Final Rules issued February 2, 2010 • Final Rules issued November 13, 2013 • Final rules apply first plan year after 7/1/14 3/17/2018 25
Parity Scope & Timeline • Applies to both mental health and substance use disorder (MH/SUD) benefits • Generally effective for plan years after October 3, 2009. Fully effective 1/1/11. • Interim Final Rules issued February 2, 2010 • Final Rules issued November 13, 2013 • Final rules apply first plan year after 7/1/14 3/17/2018 25
 General Applicablity • Covers – Fully insured & self-funded large group plans (>50 employees) – Non-federal government plans over 100 (may request exemption) – Individual & small group plans sold on and off the Marketplace • Increased cost exemption 3/17/2018 26
General Applicablity • Covers – Fully insured & self-funded large group plans (>50 employees) – Non-federal government plans over 100 (may request exemption) – Individual & small group plans sold on and off the Marketplace • Increased cost exemption 3/17/2018 26
 Specific Applicability • Newly eligible in Medicaid expansion states • Incorporated by reference into MA for managed care (state plan) and CHIP (EPSDT) • Not applicable to Medicare except for outpatient co-pays (20%) • Church plans exempt unless purchase Marketplace plan or state-regulated plan • Federal Employee HBP covered • Tri. Care not covered • Does not supersede more stringent state parity laws (WI – eg. , autism mandate) 3/17/2018 27
Specific Applicability • Newly eligible in Medicaid expansion states • Incorporated by reference into MA for managed care (state plan) and CHIP (EPSDT) • Not applicable to Medicare except for outpatient co-pays (20%) • Church plans exempt unless purchase Marketplace plan or state-regulated plan • Federal Employee HBP covered • Tri. Care not covered • Does not supersede more stringent state parity laws (WI – eg. , autism mandate) 3/17/2018 27
 Final Rule Clarifications 3/17/2018 28
Final Rule Clarifications 3/17/2018 28
 Intermediate Care • Parity applies to intermediate levels of care received in residential treatment and intensive outpatient settings – Intermediate care for MH/SUD treatment services must be assigned to the same classification that plans or issuers assign residential treatment for medical-surgical care. 3/17/2018 29
Intermediate Care • Parity applies to intermediate levels of care received in residential treatment and intensive outpatient settings – Intermediate care for MH/SUD treatment services must be assigned to the same classification that plans or issuers assign residential treatment for medical-surgical care. 3/17/2018 29
 Transparency • Upon request of a participant or contracting provider, plan administrators must disclose the criteria for medical necessity. • Plan documents must be provided within 30 days of a request. • The reason for any denial of benefits must be made available automatically and free of charge. 3/17/2018 30
Transparency • Upon request of a participant or contracting provider, plan administrators must disclose the criteria for medical necessity. • Plan documents must be provided within 30 days of a request. • The reason for any denial of benefits must be made available automatically and free of charge. 3/17/2018 30
 Scope of Services • Parity requirements for NQTLs are expanded to include restrictions on geographic location, facility type, provider specialty and other criteria that limit the scope or duration of benefits for services (including access to intermediate levels of care, out of state care). 3/17/2018 31
Scope of Services • Parity requirements for NQTLs are expanded to include restrictions on geographic location, facility type, provider specialty and other criteria that limit the scope or duration of benefits for services (including access to intermediate levels of care, out of state care). 3/17/2018 31
 Provider Rates • The final rule confirms that provider reimbursement rates are a form of NQTL • All rate-setting factors must be applied comparably and no more stringently on MH/SUD providers. 3/17/2018 32
Provider Rates • The final rule confirms that provider reimbursement rates are a form of NQTL • All rate-setting factors must be applied comparably and no more stringently on MH/SUD providers. 3/17/2018 32
 Items • The final regulations clarify that mental health benefits, medical/surgical benefits and substance use disorder benefits each include benefits for items as well as for services. 3/17/2018 33
Items • The final regulations clarify that mental health benefits, medical/surgical benefits and substance use disorder benefits each include benefits for items as well as for services. 3/17/2018 33
 Cumulative Requirements • Definitions: – Cumulative financial requirements – e. g. , deductibles (excludes lifetime and annual dollar limits) – Cumulative quantitative treatment limitations – e. g. , annual or lifetime day or visit limits • MH/SUD and medical/surgical benefits must accumulate toward the same, combined deductible (or other cumulative requirement/limit) within a classification – In other words, separate but equal deductibles are not allowed (even if a plan uses more than one service provider) 3/17/2018 34
Cumulative Requirements • Definitions: – Cumulative financial requirements – e. g. , deductibles (excludes lifetime and annual dollar limits) – Cumulative quantitative treatment limitations – e. g. , annual or lifetime day or visit limits • MH/SUD and medical/surgical benefits must accumulate toward the same, combined deductible (or other cumulative requirement/limit) within a classification – In other words, separate but equal deductibles are not allowed (even if a plan uses more than one service provider) 3/17/2018 34
 ACA & MHPAEA • Expands MHPAEA to individual and small group market • Requires coverage of MH/SUD services as one of the ten essential health benefits • Prohibits annual or lifetime dollar limits on the 10 EHB’s • Preventive services (alcohol misuse screening and counseling, depression counseling, and tobacco use screening) are free of cost-sharing • Prohibits certain kinds of discrimination 3/17/2018 35
ACA & MHPAEA • Expands MHPAEA to individual and small group market • Requires coverage of MH/SUD services as one of the ten essential health benefits • Prohibits annual or lifetime dollar limits on the 10 EHB’s • Preventive services (alcohol misuse screening and counseling, depression counseling, and tobacco use screening) are free of cost-sharing • Prohibits certain kinds of discrimination 3/17/2018 35
 ACA Discrimination • § 300 gg– 5. Non-discrimination in health care – A group health plan and a health insurance issuer offering group or individual health insurance coverage shall not discriminate with respect to participation under the plan or coverage against any health care provider who is acting within the scope of that provider’s license or certification under applicable State law. This section shall not require that a group health plan or health insurance issuer contract with any health care provider willing to abide by the terms and conditions for participation established by the plan or issuer. Nothing in this section shall be construed as preventing a group health plan, a health insurance issuer, or the Secretary from establishing varying reimbursement rates based on quality or performance measures. 3/17/2018 36
ACA Discrimination • § 300 gg– 5. Non-discrimination in health care – A group health plan and a health insurance issuer offering group or individual health insurance coverage shall not discriminate with respect to participation under the plan or coverage against any health care provider who is acting within the scope of that provider’s license or certification under applicable State law. This section shall not require that a group health plan or health insurance issuer contract with any health care provider willing to abide by the terms and conditions for participation established by the plan or issuer. Nothing in this section shall be construed as preventing a group health plan, a health insurance issuer, or the Secretary from establishing varying reimbursement rates based on quality or performance measures. 3/17/2018 36
 Case Example 3/17/2018 37
Case Example 3/17/2018 37
 MHPAEA & PPACA • MHPAEA or PPACA solution? – Patients had been seeing QTT’s – Large corporation employers – New plan with major national carrier denied QTT network access • “Both providers are deemed non-participating, ineligible provider and at this time claims will process as non-participating, ineligible provider. • Under ***** policy only licensed practitioners are accepted. Practitioners with a training certificate will not be added. ***** also does not currently recognize the specialty of Advanced Practice Social Worker as a reimbursable provider” 3/17/2018 38
MHPAEA & PPACA • MHPAEA or PPACA solution? – Patients had been seeing QTT’s – Large corporation employers – New plan with major national carrier denied QTT network access • “Both providers are deemed non-participating, ineligible provider and at this time claims will process as non-participating, ineligible provider. • Under ***** policy only licensed practitioners are accepted. Practitioners with a training certificate will not be added. ***** also does not currently recognize the specialty of Advanced Practice Social Worker as a reimbursable provider” 3/17/2018 38
 SPD General Exclusion – Treatment or services provided by a non-licensed Provider, or that do not require a license to provide: services that consist of supervision by a Provider of a non-licensed person; services performed by a relative of a Member for which, in the absence of any health benefits coverage, no charge would be made; services provided to the Member by a local, state, or federal government agency, or by a public school system or school district, except when the plan’s benefits must be provided by law, services if the Member is not required to pay for them or they are provided to the Member for free 3/17/2018 39
SPD General Exclusion – Treatment or services provided by a non-licensed Provider, or that do not require a license to provide: services that consist of supervision by a Provider of a non-licensed person; services performed by a relative of a Member for which, in the absence of any health benefits coverage, no charge would be made; services provided to the Member by a local, state, or federal government agency, or by a public school system or school district, except when the plan’s benefits must be provided by law, services if the Member is not required to pay for them or they are provided to the Member for free 3/17/2018 39
 Internal Guidance for Behavioral Health • The Behavioral Health provider types that we credential are those licensed by the state. The three digit codes found at the end of the Wisconsin license number are: • • • 123 - LCSW (Licensed Clinical Social Worker) 124 - LMFT (Licensed Marriage and Family Therapist) 125 - LPC (Licensed Professional Counselor) 057 - Ph. D, Psy. D, and Ed. D (Licensed Psychologist) 020 - MD (Psychiatrist) • Only licensed practitioners are accepted. Practitioners with a training certificate' will not be added. 3/17/2018 40
Internal Guidance for Behavioral Health • The Behavioral Health provider types that we credential are those licensed by the state. The three digit codes found at the end of the Wisconsin license number are: • • • 123 - LCSW (Licensed Clinical Social Worker) 124 - LMFT (Licensed Marriage and Family Therapist) 125 - LPC (Licensed Professional Counselor) 057 - Ph. D, Psy. D, and Ed. D (Licensed Psychologist) 020 - MD (Psychiatrist) • Only licensed practitioners are accepted. Practitioners with a training certificate' will not be added. 3/17/2018 40
 Analysis • QTT’s are licensed in Wisconsin • The SPD does not restrict licensure with reference to training or supervision • Restriction here disagrees with the SPD • May also be problem with Parity if there is no equivalent Internal Guidance for Medical. Surgical Care 3/17/2018 41
Analysis • QTT’s are licensed in Wisconsin • The SPD does not restrict licensure with reference to training or supervision • Restriction here disagrees with the SPD • May also be problem with Parity if there is no equivalent Internal Guidance for Medical. Surgical Care 3/17/2018 41
 MHPAEA Financial Impact 3/17/2018 42
MHPAEA Financial Impact 3/17/2018 42
 Inpatient • 10% of large plans out of compliance in 2010 • Virtually none in 2011 • 2009 – 2011 higher copays and deductibles for MH/SUD decreased rapidly • For mid-sized employers, between 10% & 16% out of compliance before MHPAEA, and less than 7% after 3/17/2018 43
Inpatient • 10% of large plans out of compliance in 2010 • Virtually none in 2011 • 2009 – 2011 higher copays and deductibles for MH/SUD decreased rapidly • For mid-sized employers, between 10% & 16% out of compliance before MHPAEA, and less than 7% after 3/17/2018 43
 Outpatient • 30% of large plans out of compliance in 2010 • In 2011, fewer plans out of compliance, but 20% retained higher outpatient, in-network copays for MH/SUD benefits • Between 2009 and 2011, dramatic decline in more restrictive copays & coinsurance • Before MHPAEA, 50% of mid-size business plans out of compliance. 40% after MHPAEA 3/17/2018 44
Outpatient • 30% of large plans out of compliance in 2010 • In 2011, fewer plans out of compliance, but 20% retained higher outpatient, in-network copays for MH/SUD benefits • Between 2009 and 2011, dramatic decline in more restrictive copays & coinsurance • Before MHPAEA, 50% of mid-size business plans out of compliance. 40% after MHPAEA 3/17/2018 44
 ER & Rx • In 2010 vast majority of large plans complied with parity in Rx • 20% higher cost-sharing for MH/SUD ER • By 2011, virtually all plans complied with both ER & Rx 3/17/2018 45
ER & Rx • In 2010 vast majority of large plans complied with parity in Rx • 20% higher cost-sharing for MH/SUD ER • By 2011, virtually all plans complied with both ER & Rx 3/17/2018 45
 MHPAEA Quantitative Impact 3/17/2018 46
MHPAEA Quantitative Impact 3/17/2018 46
 Inpatient • In 2010 nearly all large plans compliant on MH • 20% more restrictive for SUD • By 2011, no unequal dollar limits & 8% unequal day limits (both MH and SUD) • 2009 – 2011 dramatic decline in unequal limits • Largest drop in unequal day limits (50% - 10%) 3/17/2018 47
Inpatient • In 2010 nearly all large plans compliant on MH • 20% more restrictive for SUD • By 2011, no unequal dollar limits & 8% unequal day limits (both MH and SUD) • 2009 – 2011 dramatic decline in unequal limits • Largest drop in unequal day limits (50% - 10%) 3/17/2018 47
 Outpatient • 50% of large plans had unequal visit limits for MH/SUD in 2010 • Less than 7% in 2011 • 30% unequal dollar limits in 2010 • Virtually none in 2011 • Mid-sized employers, 81% out of compliance in 2008. Down to 13% in 2011. 3/17/2018 48
Outpatient • 50% of large plans had unequal visit limits for MH/SUD in 2010 • Less than 7% in 2011 • 30% unequal dollar limits in 2010 • Virtually none in 2011 • Mid-sized employers, 81% out of compliance in 2008. Down to 13% in 2011. 3/17/2018 48
 MHPAEA NQTL Impact 3/17/2018 49
MHPAEA NQTL Impact 3/17/2018 49
 Non-Quantifiable Treatment Limitations • In 2010, most plans still used more restrictive NQTLs for MH/SUD • Most common: – Precertification requirements – Medical necessity criteria – Routine retrospective reviews for MH/SUD – Reimbursement on lower % of UCR 3/17/2018 50
Non-Quantifiable Treatment Limitations • In 2010, most plans still used more restrictive NQTLs for MH/SUD • Most common: – Precertification requirements – Medical necessity criteria – Routine retrospective reviews for MH/SUD – Reimbursement on lower % of UCR 3/17/2018 50
 MAPP • Medicaid eligibility for disabled individuals – Household income under 250% FPL – Applicant-only assets under $15, 000 – $0 Premium if applicant income under 150% – Must have one work experience/month for “something of value” in return 3/17/2018 51
MAPP • Medicaid eligibility for disabled individuals – Household income under 250% FPL – Applicant-only assets under $15, 000 – $0 Premium if applicant income under 150% – Must have one work experience/month for “something of value” in return 3/17/2018 51
 Badger. Care Plus 3/17/2018 53
Badger. Care Plus 3/17/2018 53
 Badger. Care • NEW Basic Financial Eligibility Limits – Children (defined as up to age 18) • Up to 306% FPL – Pregnant women • Up to 306% FPL – Adults • • • Up to 100% FPL Parents may have Medicare Childless Adults may not have Medicare – Certain former foster care youth 3/17/2018 54
Badger. Care • NEW Basic Financial Eligibility Limits – Children (defined as up to age 18) • Up to 306% FPL – Pregnant women • Up to 306% FPL – Adults • • • Up to 100% FPL Parents may have Medicare Childless Adults may not have Medicare – Certain former foster care youth 3/17/2018 54
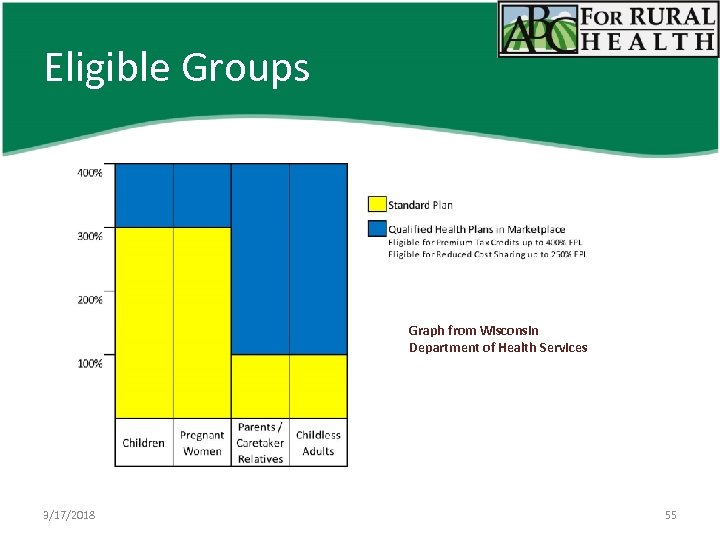 Eligible Groups Graph from Wisconsin Department of Health Services 3/17/2018 55
Eligible Groups Graph from Wisconsin Department of Health Services 3/17/2018 55
 MAGI Income Under MAGI, countable income = taxable income. This includes (but is not limited to): – Taxable Earned Income, – Taxable Net Self-Employment Income, – Unemployment Compensation, – Alimony/Spousal Maintenance, and – Social Security Income. 3/17/2018 56
MAGI Income Under MAGI, countable income = taxable income. This includes (but is not limited to): – Taxable Earned Income, – Taxable Net Self-Employment Income, – Unemployment Compensation, – Alimony/Spousal Maintenance, and – Social Security Income. 3/17/2018 56
 Plus • After arriving at your Adjusted Gross Income, the next step in calculating your MAGI is to add back certain types of income: – Non-taxable Social Security benefits (Line 20 a minus 20 b on a Form 1040) • For Social Security Benefits include disability payments (SSDI), but exclude Supplemental Security Income (SSI), – Tax-exempt interest (Line 8 b on a Form 1040) – Foreign earned income & housing expenses for Americans living abroad (calculated on a Form 2555) 3/17/2018 57
Plus • After arriving at your Adjusted Gross Income, the next step in calculating your MAGI is to add back certain types of income: – Non-taxable Social Security benefits (Line 20 a minus 20 b on a Form 1040) • For Social Security Benefits include disability payments (SSDI), but exclude Supplemental Security Income (SSI), – Tax-exempt interest (Line 8 b on a Form 1040) – Foreign earned income & housing expenses for Americans living abroad (calculated on a Form 2555) 3/17/2018 57
 MAGI Pre-tax deductions • The following deductions will be allowed if the payments are taken out of the individual’s paycheck on a pre-tax basis. (Will be on the pay stub) – – – 3/17/2018 Health Insurance Premiums Health Savings Account Retirement Contributions Parking & Transit Costs Child Care Savings Account Group Life Insurance 58
MAGI Pre-tax deductions • The following deductions will be allowed if the payments are taken out of the individual’s paycheck on a pre-tax basis. (Will be on the pay stub) – – – 3/17/2018 Health Insurance Premiums Health Savings Account Retirement Contributions Parking & Transit Costs Child Care Savings Account Group Life Insurance 58
 MAGI Tax Deductions • Tax deductions listed on page 1 of form 1040. – Student Loan Interest (capped at $208/month) – Higher Education Expenses – tuition, school fees, room & board, supplies, books, etc. (capped at $333) – Self-Employment Tax Deduction – Spousal Support/Alimony (court ordered amount) – Teachers’ Tax-Deductible Expenses (capped at $21/month) – Out-of-pocket Costs for a Job-Related Move – Loss from Sale of Business Property • Itemized deductions are not allowed. 3/17/2018 59
MAGI Tax Deductions • Tax deductions listed on page 1 of form 1040. – Student Loan Interest (capped at $208/month) – Higher Education Expenses – tuition, school fees, room & board, supplies, books, etc. (capped at $333) – Self-Employment Tax Deduction – Spousal Support/Alimony (court ordered amount) – Teachers’ Tax-Deductible Expenses (capped at $21/month) – Out-of-pocket Costs for a Job-Related Move – Loss from Sale of Business Property • Itemized deductions are not allowed. 3/17/2018 59
 New Income Counted by MAGI – Financial aid, if used for living expenses. – All Tribal per capita payments from gaming revenue. – Ameri. Corps income. – Taxable retirement, pension and annuities. – Interest & dividends. – Lump sum income counted in month received. 3/17/2018 60
New Income Counted by MAGI – Financial aid, if used for living expenses. – All Tribal per capita payments from gaming revenue. – Ameri. Corps income. – Taxable retirement, pension and annuities. – Interest & dividends. – Lump sum income counted in month received. 3/17/2018 60
 MAGI Exempt Income • Some common income types that will NOT be counted for Badger. Care Plus eligibility include: – Child Support, – Supplemental Security Income (SSI), – Workers’ Compensation, and – Veterans Benefits. 3/17/2018 61
MAGI Exempt Income • Some common income types that will NOT be counted for Badger. Care Plus eligibility include: – Child Support, – Supplemental Security Income (SSI), – Workers’ Compensation, and – Veterans Benefits. 3/17/2018 61
 Whose Income is Counted? • In general, everyone in an assistance group will have their income counted. • In some cases, children and tax dependents’ income will not be counted, if their income is so low that they are not required to file taxes. 3/17/2018 62
Whose Income is Counted? • In general, everyone in an assistance group will have their income counted. • In some cases, children and tax dependents’ income will not be counted, if their income is so low that they are not required to file taxes. 3/17/2018 62
 Reminder – “Expect to…” • For MAGI questions, ACCESS will ask about what individuals are planning to do for the current tax year in which they are applying, not the previous year. • Example: If applying for benefits in March 2014, ACCESS will ask about the taxes that the individual expects to file in 2015 for income that he or she has in 2014. 3/17/2018 63
Reminder – “Expect to…” • For MAGI questions, ACCESS will ask about what individuals are planning to do for the current tax year in which they are applying, not the previous year. • Example: If applying for benefits in March 2014, ACCESS will ask about the taxes that the individual expects to file in 2015 for income that he or she has in 2014. 3/17/2018 63
 Who is Subject to MAGI Rules? • Badger. Care Plus Members: – Children, – Parents and caretaker relatives, – Pregnant women, and – Adults with no dependent children. • Family Planning Only Services (FPOS) members will be subject to MAGI income rules, but always with a group size of one. 3/17/2018 64
Who is Subject to MAGI Rules? • Badger. Care Plus Members: – Children, – Parents and caretaker relatives, – Pregnant women, and – Adults with no dependent children. • Family Planning Only Services (FPOS) members will be subject to MAGI income rules, but always with a group size of one. 3/17/2018 64
 Who is Not Subject to MAGI Rules? MAGI rules do not apply to: • • • Elderly, blind and disabled groups Elderly, Blind and Disabled (EBD) Medicaid Long-Term Care (LTC) Waiver Enrollees Senior. Care QMB, SLMB+ MAPP Well Woman Medicaid Categorically eligible populations Former Foster Care Youth 3/17/2018 65
Who is Not Subject to MAGI Rules? MAGI rules do not apply to: • • • Elderly, blind and disabled groups Elderly, Blind and Disabled (EBD) Medicaid Long-Term Care (LTC) Waiver Enrollees Senior. Care QMB, SLMB+ MAPP Well Woman Medicaid Categorically eligible populations Former Foster Care Youth 3/17/2018 65
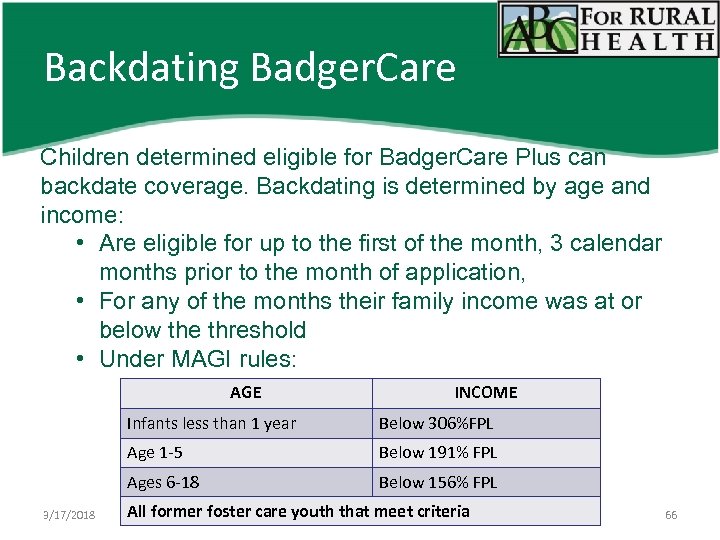 Backdating Badger. Care Children determined eligible for Badger. Care Plus can backdate coverage. Backdating is determined by age and income: • Are eligible for up to the first of the month, 3 calendar months prior to the month of application, • For any of the months their family income was at or below the threshold • Under MAGI rules: AGE INCOME Infants less than 1 year Age 1 -5 Below 191% FPL Ages 6 -18 3/17/2018 Below 306%FPL Below 156% FPL All former foster care youth that meet criteria 66
Backdating Badger. Care Children determined eligible for Badger. Care Plus can backdate coverage. Backdating is determined by age and income: • Are eligible for up to the first of the month, 3 calendar months prior to the month of application, • For any of the months their family income was at or below the threshold • Under MAGI rules: AGE INCOME Infants less than 1 year Age 1 -5 Below 191% FPL Ages 6 -18 3/17/2018 Below 306%FPL Below 156% FPL All former foster care youth that meet criteria 66
 Backdating Rules for Pregnant Women: • All pregnant women, except those eligible under the BC+ Prenatal program, may have their eligibility backdated to whichever is more recent: – The first of the month in which the pregnancy began -or– The first of the month, three months prior to the month of application. 3/17/2018 67
Backdating Rules for Pregnant Women: • All pregnant women, except those eligible under the BC+ Prenatal program, may have their eligibility backdated to whichever is more recent: – The first of the month in which the pregnancy began -or– The first of the month, three months prior to the month of application. 3/17/2018 67
 Backdating Rules for Family Planning Only Services (FPOS): • Eligibility for FPOS begins on the first of the month of application, if all non-financial and financial eligibility requirements are met. • FPOS may be backdated up to three months from the month of application. 3/17/2018 68
Backdating Rules for Family Planning Only Services (FPOS): • Eligibility for FPOS begins on the first of the month of application, if all non-financial and financial eligibility requirements are met. • FPOS may be backdated up to three months from the month of application. 3/17/2018 68
 Backdating Rules for Parents & Caretakers • All non-pregnant, non-disabled parents and caretakers may have their eligibility backdated up to the first of the month, three calendar months prior to the month of application for any of the months in which their family income was at or below 100% FPL 3/17/2018 69
Backdating Rules for Parents & Caretakers • All non-pregnant, non-disabled parents and caretakers may have their eligibility backdated up to the first of the month, three calendar months prior to the month of application for any of the months in which their family income was at or below 100% FPL 3/17/2018 69
 Backdating Rules for Childless Adults • Childless adults with assistance group income under 100% FPL will be eligible for backdating for up to the first of the month, three calendar months prior to the month of application. • However, retroactive coverage cannot begin prior to April 1, 2014. • As a result, a childless adult could not be eligible for the full three calendar months period of backdating until July 1, 2014. 3/17/2018 70
Backdating Rules for Childless Adults • Childless adults with assistance group income under 100% FPL will be eligible for backdating for up to the first of the month, three calendar months prior to the month of application. • However, retroactive coverage cannot begin prior to April 1, 2014. • As a result, a childless adult could not be eligible for the full three calendar months period of backdating until July 1, 2014. 3/17/2018 70
 Badger. Care Plus Crowd Out Rules • Affects children based on age relative to household income: – < 1 year old = no effect on eligibility – Age 1 to 6 th b-day = check insurance access if income > 191% FPL (185%) – Age 6 to 18 th b-day = check insurance access if income > 156% FPL (150%) • May be denied eligibility if: – Employer contribution is at least 80% of total premium cost; and, • Are currently enrolled in employer plan, or • Failed to enroll in employer plan offered any time in the last 12 months, or • Have current ability to enroll in coverage that will start within three months, or • Employer coverage was dropped during previous three months * “Good Cause” exceptions may apply 3/17/2018 71
Badger. Care Plus Crowd Out Rules • Affects children based on age relative to household income: – < 1 year old = no effect on eligibility – Age 1 to 6 th b-day = check insurance access if income > 191% FPL (185%) – Age 6 to 18 th b-day = check insurance access if income > 156% FPL (150%) • May be denied eligibility if: – Employer contribution is at least 80% of total premium cost; and, • Are currently enrolled in employer plan, or • Failed to enroll in employer plan offered any time in the last 12 months, or • Have current ability to enroll in coverage that will start within three months, or • Employer coverage was dropped during previous three months * “Good Cause” exceptions may apply 3/17/2018 71
 Separated, Divorced, Unmarried Parents • Only one parent can include the child in the household for purposes of determining income eligibility for Marketplace financial assistance and Badger. Care – Alternating dependent exemptions can cause children to have to switch coverage from year to year if: • Parents live in different geographic locations not served by same plan network • One parent has Marketplace coverage and the other has BC+/Medicaid – Can also cause parents with income near 100% FPL to churn between Marketplace and Badger. Care 3/17/2018 72
Separated, Divorced, Unmarried Parents • Only one parent can include the child in the household for purposes of determining income eligibility for Marketplace financial assistance and Badger. Care – Alternating dependent exemptions can cause children to have to switch coverage from year to year if: • Parents live in different geographic locations not served by same plan network • One parent has Marketplace coverage and the other has BC+/Medicaid – Can also cause parents with income near 100% FPL to churn between Marketplace and Badger. Care 3/17/2018 72
 Location & Access • Geographic location and network access – Children may be eligible for Marketplace financial assistance if they do not have meaningful access to the provider network of a parent’s insurance plan even if they technically could be enrolled in coverage that meets minimum essential coverage standards 3/17/2018 73
Location & Access • Geographic location and network access – Children may be eligible for Marketplace financial assistance if they do not have meaningful access to the provider network of a parent’s insurance plan even if they technically could be enrolled in coverage that meets minimum essential coverage standards 3/17/2018 73
 COBRA – In many cases, spouses who previously would have had to rely on former spouse’s continuation coverage will be eligible for Marketplace coverage at lower cost. – COBRA election is no longer the only option – Forgoing COBRA election does not disqualify individual for APTC/CSR – COBRA coverage is retroactive from date of notice to election date – COBRA election deadline is at least 60 days – Election deadline is 30 days for plans governed by Wisconsin insurance law (e. g. very small group and some 3/17/2018 church plans) 74
COBRA – In many cases, spouses who previously would have had to rely on former spouse’s continuation coverage will be eligible for Marketplace coverage at lower cost. – COBRA election is no longer the only option – Forgoing COBRA election does not disqualify individual for APTC/CSR – COBRA coverage is retroactive from date of notice to election date – COBRA election deadline is at least 60 days – Election deadline is 30 days for plans governed by Wisconsin insurance law (e. g. very small group and some 3/17/2018 church plans) 74
 Maximizing Coverage • Commercial insurance coverage does not necessarily preclude using public benefits for ‘wraparound’ coverage. • Children can use Badger. Care as secondary coverage as long as they are not subject to insurance crowd out rules. • Adults under 100% FPL are exempt from crowd out rules and can have Badger. Care as secondary coverage on top of any other insurance (except Medicare). • Crowd out rules do not apply to disability based Medicaid programs • Medicaid enrolled provider may not balance bill for Medicaid covered services, including copays not covered by other insurance • Secondary coverage may pay deductible expenses 3/17/2018 75
Maximizing Coverage • Commercial insurance coverage does not necessarily preclude using public benefits for ‘wraparound’ coverage. • Children can use Badger. Care as secondary coverage as long as they are not subject to insurance crowd out rules. • Adults under 100% FPL are exempt from crowd out rules and can have Badger. Care as secondary coverage on top of any other insurance (except Medicare). • Crowd out rules do not apply to disability based Medicaid programs • Medicaid enrolled provider may not balance bill for Medicaid covered services, including copays not covered by other insurance • Secondary coverage may pay deductible expenses 3/17/2018 75
 MAPP • Medicaid eligibility for disabled individuals – Household income under 250% FPL – Applicant-only assets under $15, 000 – $0 Premium if applicant income under 150% – Must have one work experience/month for “something of value” in return 3/17/2018 76
MAPP • Medicaid eligibility for disabled individuals – Household income under 250% FPL – Applicant-only assets under $15, 000 – $0 Premium if applicant income under 150% – Must have one work experience/month for “something of value” in return 3/17/2018 76
 One Final Hitch… • DHS uses the current year’s federal poverty level to determine Badger. Care and Medicaid eligibility • Until next open enrollment, the Marketplace will use 2013 federal poverty levels to determine eligibility for APTC and CSR 3/17/2018 77
One Final Hitch… • DHS uses the current year’s federal poverty level to determine Badger. Care and Medicaid eligibility • Until next open enrollment, the Marketplace will use 2013 federal poverty levels to determine eligibility for APTC and CSR 3/17/2018 77
 Health. Watch 3/17/2018 78
Health. Watch 3/17/2018 78


