St P Lecture.ppt
- Количество слайдов: 53

Physiotherapy in Mental Health St. Petersburg May 2016 Josephine Bell Clinical Specialist Physiotherapist South West London & St. George’s Mental Health NHS Trust

Objectives To gain an awareness of the most common mental health problems and how people are affected by them To develop and understanding of how a physiotherapist can adapt their treatment to help people with significant mental health problems

Mental illness is distinct from learning disability (although there may be some overlap) What types of problems are classed as mental health conditions?

A brief history of mental health in the United Kingdom Prior to the 19 th © most people with mental illness were cared for either by their families or the local parish, or they resorted to begging. Later they were assigned to the ‘Poorhouses’. There were a few private ‘madhouses’ but these were only for the privileged few and they were run by businessman for profit.

In 1845 the Lunatics Act decreed that a ‘lunatic asylum’ be built in each county. This terminology is no longer used and today we refer to ‘mental health hospitals’.



Initially people were “ committed “ to an asylum by family members or people of authority It was not until the ‘Mental Treatment Act’ of 1930 that voluntary admission became possible However informal admission did not become the norm until the 1960 s
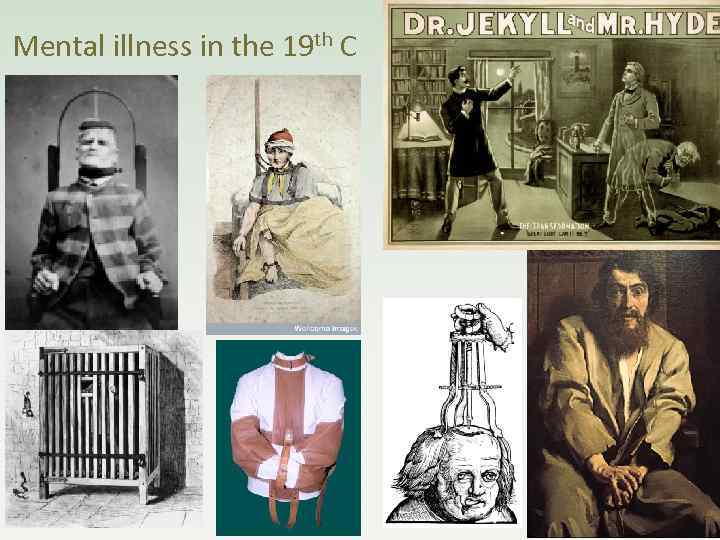
Mental illness in the 19 th C
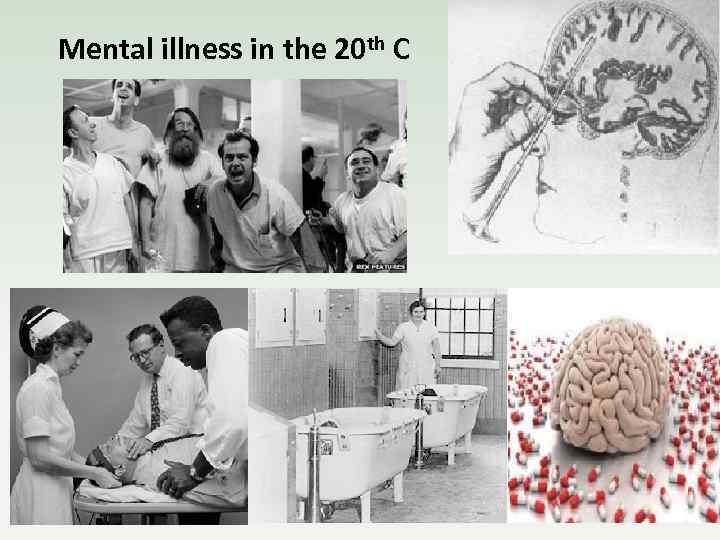
Mental illness in the 20 th C



Is mental illness in the 21 st C more fluffy?

Anyone can be affected by mental health issues

1 person in 4 in Britain will experience some kind of mental health problem in the course of a year 90% are treated locally by their local doctors The remaining 10% will require specialist services
Mental state consists of: Thoughts Cognitions Feelings Perceptions Behaviours

Why do we need perceptions? They are the means by which we experience and make sense of the world about us: vision hearing touch taste smell kinaesthesis

Examples of disorders of perception Auditory hallucinations (noises, music, voices heard in the absence of external stimulus – strongly associated with schizophrenia) Visual hallucinations (should suggest the possibility of an organic disorder but also can occur with severe depression or schizophrenia) Tactile hallucinations (e. g. of insects crawling under the skin: common in cocaine abuse and sometimes schizophrenia) Hallucinations of taste and smell (less common in mental health conditions. May occur with temporal lobe epilepsy)

Thoughts Ideas Concepts Internal dialogue

Feelings Subjective emotional states that have psychological and physiological aspects e. g. happiness sadness paranoia anger fear
Cognitions Memory Orientation Attention and concentration Calculation Language (insight)

Behaviours What we do: our ‘external’ actions in relation to the world about us (the physical and social world)

Signs and symptoms of mental disorder Disordered perception (Auditory, visual or tactile hallucinations) Disordered thinking (as in Schizophrenia, OCD & psychotic depression) Disordered mood (anxiety, depression, phobia, mania) Disordered body image (Anorexia Nervosa and Body Dysmorphic Disorder)

Depression Affects 1 in 6 people, most commonly from 25 – 44 years of age The Science of Depression: https: //www. youtube. com/watch? v=GOK 1 KFFIQI

Signs and symptoms of depression 1. Persistent sad, anxious or “empty” mood 2. Loss of interest or pleasure in activities that were previously enjoyed And possibly also: - Weight loss or weight gain - Insomnia or hypersomnia - Agitation or slowing down - Poor concentration - Feelings of worthlessness - Thoughts of death or suicide

Bipolar affective Disorder Affects about 1 in 100 adults As well as becoming low in mood, some people can also become ‘high’ as in bipolar affective disorder, the signs and symptoms of which are: - Elated or exalted mood - Reduced need for sleep - Increased energy and ideas - Racing and/or grandiose thoughts - Rapid talking - Irritability - Increased sexual desire - Inappropriate social behaviour (disinhibition)

Re. Bipolar Affective Disorder:

Anxiety Disorders 1 in 10 people suffer a ‘Disabling Anxiety Disorder’ at some time in their lives Some examples are: - Generalised Anxiety Disorder - Phobia (e. g. agoraphobia, social or specific phobia) - Panic attacks / panic Disorder - Obsessive-compulsive Disorder - Post Traumatic Stress Disorder - Eating Disorder

Anxiety - Characterised by anxious and avoidant behaviour - Sometimes there is a disturbance of mood or distortion of body image - Reality testing is intact (actions recognised as one’s own) - There is no organic aetiology - Behaviour does not generally violate social norms ( It can be ‘understood’) Often overlaps with physical illness. It may also mimic physical disease, resulting in diagnostic difficulty

Physiological signs of anxiety Increased muscle tension - including tension headaches, restlessness and tremor Autonomic arousal with a release of Adrenaline leading to: - Raised heart rate/palpitations - Increased perspiration - Raised heart rate/palpitation - Raised respiratory rate - Dryness of mouth, loss of appetite - Bowel/bladder over-activity

Psychosis Affects 1 in 100 people at some time in their lives with 10 -15% developing long term difficulties (enduring mental illness, usually Schizophrenia) The most difficult of all syndromes to describe and define: - The definition has varied and is still under some dispute - Not a ‘split personality’ or ‘multiple personalities’ - Many varieties of clinical picture - A change in chemical messengers in the brain results in thought, mood, perception and behavioural disturbance - It is an episodic condition that usually fluctuates - Many patients are not aware/do not accept that they are unwell

Symptoms are divided into positive & negative Positive Negative - Disordered thinking - Poor motivation - Delusions - Hallucinations - Agitation - Preoccupation or agitation - Depression - Low self-esteem - Social withdrawal - Self-neglect

What images do you get if you Google Schizophrenia in the UK?

Mental illness is controversial: The topics of mental health and illness have always roused controversy and raised many questions. Questions such as : - What behaviour is ‘normal’? - What is being ‘rational’? - Are problems biological or functional? - Should we treat patterns of thinking and behaviour as medical problems? Opinions have, and probably always will, vary about the best way to define and treat mental health problems

Mental illness is almost always multifactorial in nature Physiological Psychological Social, cultural & economic factors All need to be considered !

This fits well with the bio-psycho-social model adopted by physiotherapists. . . and allows for a holistic approach

Stigma and discrimination Many people in the UK with mental health problems report experiencing stigma and discrimination from society, friends, family and health care professionals Stigma and discrimination have a negative impact on mental health problems and can trap people in a cycle of illness However progress is being made and people are becoming more willing to disclose, talk about and seek treatment for mental health problems

The best way to challenge stereotypes is through first hand contact with people with mental health problems

People with severe and enduring mental illness have poor physical health compared to the wider population Their life expectancy is ~ 10 - 20 years less than the average

Physical health problems Twice as likely to die from coronary heart disease as the general population Four times more likely to die from respiratory disease Twice as likely to have Diabetes (many people with Schizophrenia have multiple risk factors for type 2 Diabetes such as a family history of Diabetes, obesity, sedentary lifestyle and smoking) They also suffer more from hypertension, CVA, obesity and infections

Why is this so?

The inequalities cannot be explained by the mental health problem alone. The reasons are complex!
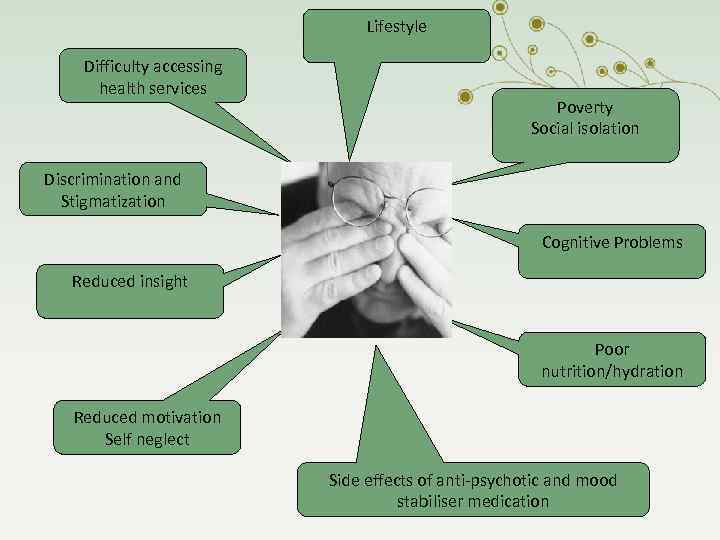
Lifestyle Difficulty accessing health services Poverty Social isolation Discrimination and Stigmatization Cognitive Problems Reduced insight Poor nutrition/hydration Reduced motivation Self neglect Side effects of anti-psychotic and mood stabiliser medication

There are many problems secondary to mental illness that may challenge physiotherapeutic intervention

• • • • Poor motivation Anxiety/fear avoidance Obsessions/compulsions Low self esteem Irritability/aggression Reduced concentration or poor cognition Distraction due to hallucinations, delusions or mania Altered body image Deliberate self harm Fatigue/decreased energy /apathy Obesity or extreme low weight Alcohol or drug abuse/dependence High smoking rates • Extra pyramidal side effects of medication (EPSE) • Motor symptoms: tics, stereotypies, posturing • Loss of strength or decreased conditioning • ? Altered pain perception • Somatic symptoms/Medically unexplained symptoms • Lack of insight


The broad role of physio in Mental Healthcare • • • Base-line physical assessment Assessment & rehabilitation of neuromusculoskeletal problems Pain management Management of respiratory and long term conditions Advice to MDT and carers on management of physical problems Walking aid provision and assessment/referral for wheelchairs Advice to families on moving and handling Advice on return to work Advice on accessing local services Prevention of injuries and chronic problems Managing continence Health promotion and healthy lifestyle advice

How do we adapt ? • • • Provide a private and informal, but safe environment Try to build a therapeutic relationship based on honesty and trust Non judgemental and empathic approach Flexible appointment times and location Flexible DNA/discharge policy Longer/shorter treatment sessions, as needed Adapt for cognitive factors: memory, attention etc. Consider motivation, self esteem, insight Adapt assessment and treatment techniques

Engagement • • • Engagement is always a priority Use effective and sensitive communication Initial aim is to ‘hear about their story’ Facilitate them to set their own goals and own their treatment programme Facilitate motivation by demonstrating interest and making them feel valued Make it informal: show empathy, curiosity Assess in a ‘chatty’ style but help them to stay focussed Make them feel understood and taken seriously Cease if necessary (e. g. insufficient attention, irritability or aggression) Don’t take rejection personally Adopt a truly holistic approach
Some suggested reading/videos/resources: Facts and figures about Mental health 2015 https: //www. mentalhealth. org. uk/publications/fundamental-facts-about-mental-health-2015 Organisations: http: //www. mind. org. uk/ http: //www. who. int/mental_health/evidence/en/ http: //www. mentalhealth. org. uk/help-information/ http: //www. rcpsych. ac. uk/healthadvice/problemsdisorders. aspx http: //www. time-to-change. org. uk/ Guide to mental health services in England: http: //www. nhs. uk/NHSEngland/About. NHSservices/mental-health-servicesexplained/Pages/accessing%20 services. aspx “Recovery letters”: http: //therecoveryletters. com/


St P Lecture.ppt