b50c0198ef051738e59a6a405a80d5c3.ppt
- Количество слайдов: 49

Pharmacokinetics of antibiotics in burn patients 台大醫院藥劑部 吳建志藥師

Outline 1. Basic concepts of pharmacokinetics(PK) 2. Antibiotic PK principle in critically ill patients 3. PK/PD study in burn patients 4. Approaches to improve antibiotics effect in burn patients 2

1. Basic concepts of pharmacokinetics(PK)

Termination • Pharmacokinetics (PK) – Absorption, distribution, elimination (excretion and metabolism) • Clinical pharmacokinetics – Application of pharmacokinetic methods in drug therapy – Various disease status influence drug PK • Pharmacodynamics (PD) – Relationship between the drug concentration at the site of action and pharmacologic effect 4

Distribution – volume of distribution (Vd) • Describing the relationship between the dose of a drug and resulting serum concentration • No exact physiologic meaning • In a 70 kg person, Vd = 15 -18 L (extracellular fluid), 40 L (total body water), > 40 -50 L (tissue) • Affect loading dose (Vd↑; LD↑) Tissue Interstitial fluid (21%) Total body water (60%) Plasma (4%) Extracellular fluid (25%) Intracellular fluid (35%) 5
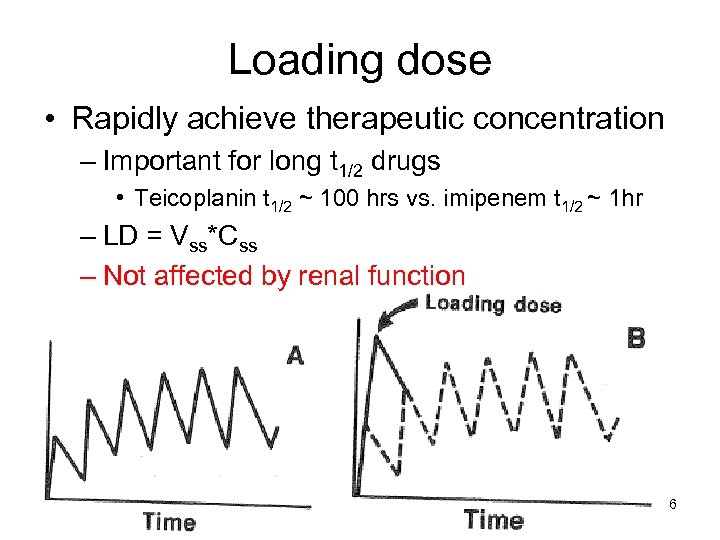
Loading dose • Rapidly achieve therapeutic concentration – Important for long t 1/2 drugs • Teicoplanin t 1/2 ~ 100 hrs vs. imipenem t 1/2 ~ 1 hr – LD = Vss*Css – Not affected by renal function 6

Distribution – protein binding • Only unbound or free drugs exert pharmacological effect • High protein binding: ≥ 70% • Hypoalbuminemia (<2. 5 g/d. L) is meaningful for high protein binding agents – Free drug (Fu) ↑, Vd ↑, CL ↑ • High protein binding antibiotics – Ceftriaxone, ertapenem, teicoplanin, daptomycin etc. Protein Normal conc. (g/d. L) Type of drug bound Burn Albumin 3. 5 -4. 5 acidic ↓ α-1 acid glycoprotein 0. 4 -1. 0 basic ↑ 7 Ibrahim RB. Seminars in Dialysis 2012; 25: 176 -89.
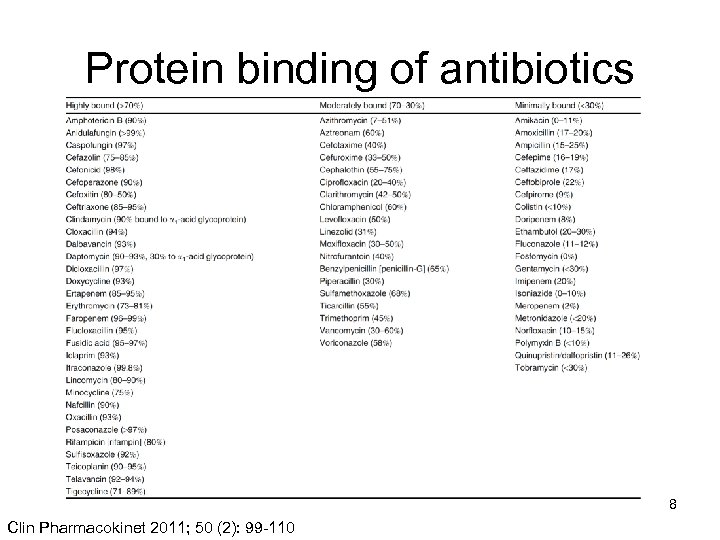
Protein binding of antibiotics 8 Clin Pharmacokinet 2011; 50 (2): 99 -110

Excretion • Cpt = D(1 -e-ktin) e-kτ/(tin x CL) • Glomerular filtration rate (GFR) is the primary mechanism responsible for the renal drug clearance of most drugs. – Normal GFR: 125 m. L/min • CLR > 125 m. L/min → active tubular secretion • CLR < 125 m. L/min → re-absorption • Cockcroft-Gault equation for GFR estimation – Most common use for dose adjustment – Only accurate in stable patients – Not correlate well in critically ill patient 9 CL: clearance, D: dose, tin = infusion time, τ: dosing interval, k: elimination rate constant
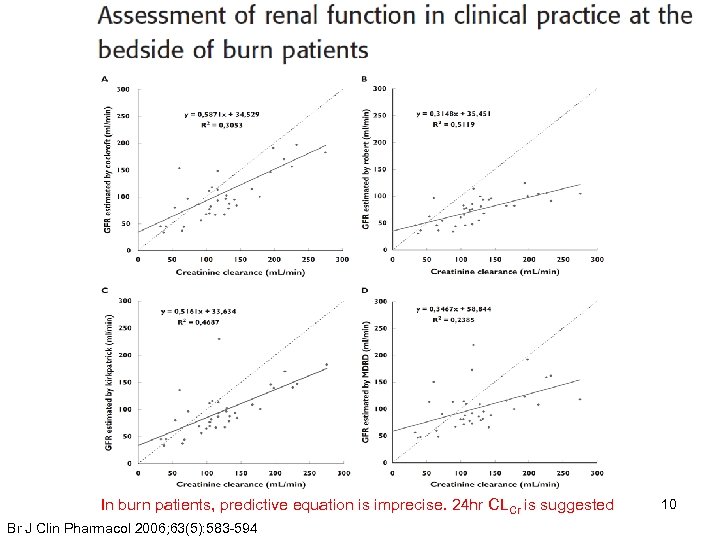
In burn patients, predictive equation is imprecise. 24 hr CLCr is suggested Br J Clin Pharmacol 2006; 63(5): 583 -594 10

2. Antibiotic PK principle in critically ill patients
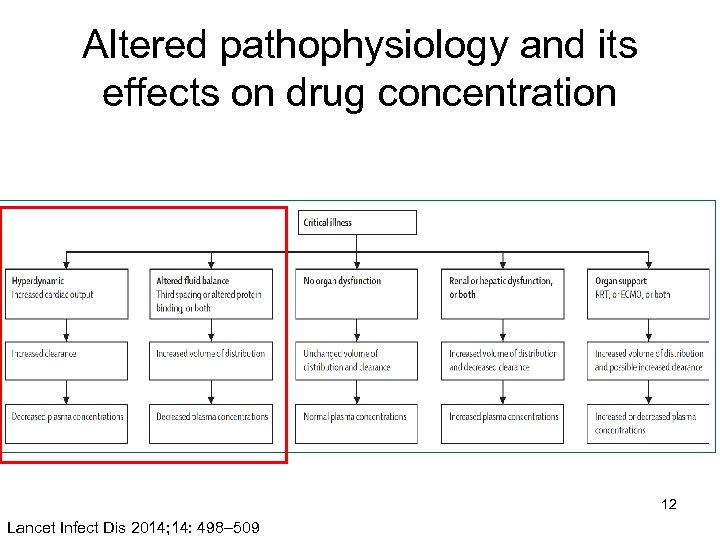
Altered pathophysiology and its effects on drug concentration 12 Lancet Infect Dis 2014; 14: 498– 509
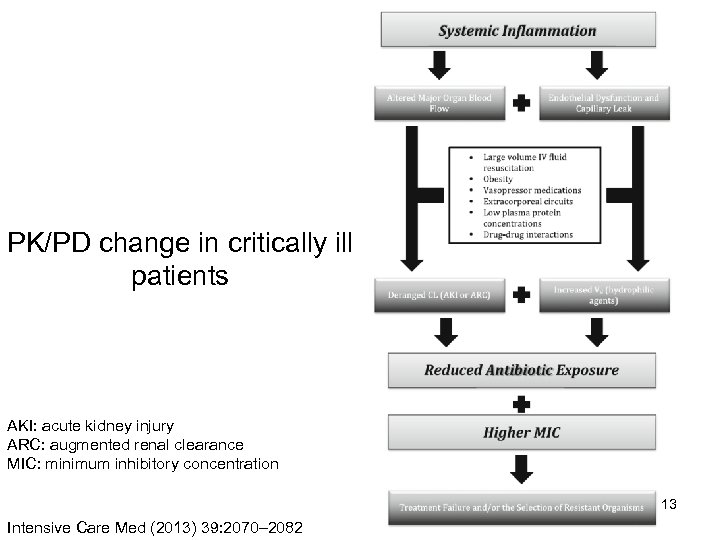
PK/PD change in critically ill patients AKI: acute kidney injury ARC: augmented renal clearance MIC: minimum inhibitory concentration 13 Intensive Care Med (2013) 39: 2070– 2082
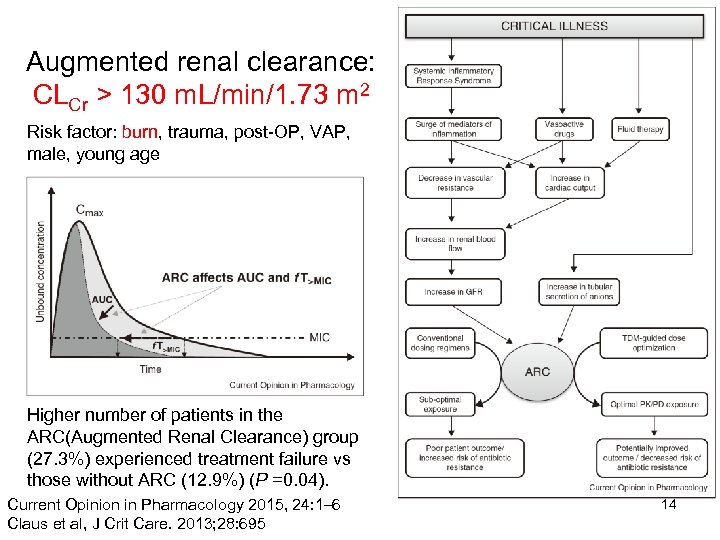
Augmented renal clearance: CLCr > 130 m. L/min/1. 73 m 2 Risk factor: burn, trauma, post-OP, VAP, male, young age Higher number of patients in the ARC(Augmented Renal Clearance) group (27. 3%) experienced treatment failure vs those without ARC (12. 9%) (P =0. 04). Current Opinion in Pharmacology 2015, 24: 1– 6 Claus et al, J Crit Care. 2013; 28: 695 14
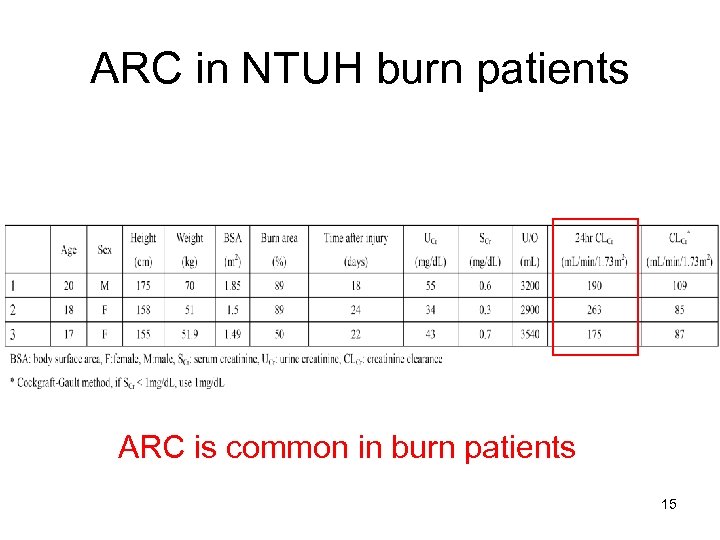
ARC in NTUH burn patients ARC is common in burn patients 15

Potential solution for altered antibiotics PK/PD in critical illness For time-dependent antibiotics Intermittent infusion: <2 hrs Extended infusion: 2 -4 hrs Continuous infusion: 24 hrs 16 Intensive Care Med 2013; 39: 2070– 2082
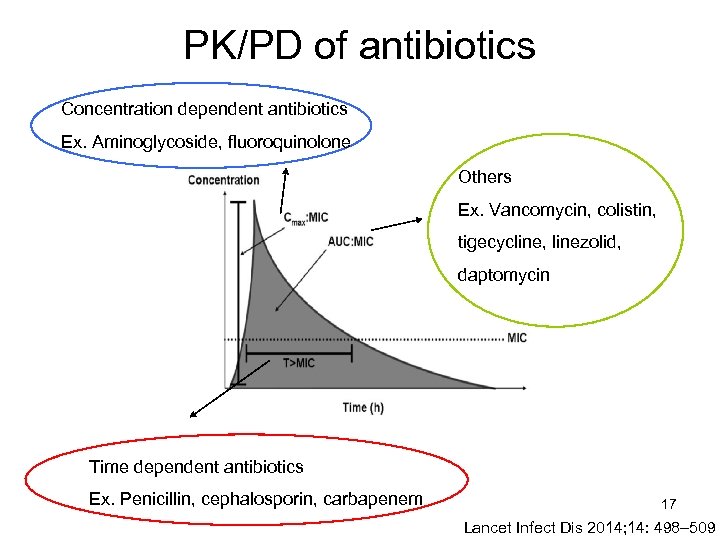
PK/PD of antibiotics Concentration dependent antibiotics Ex. Aminoglycoside, fluoroquinolone Others Ex. Vancomycin, colistin, tigecycline, linezolid, daptomycin Time dependent antibiotics Ex. Penicillin, cephalosporin, carbapenem 17 Lancet Infect Dis 2014; 14: 498– 509
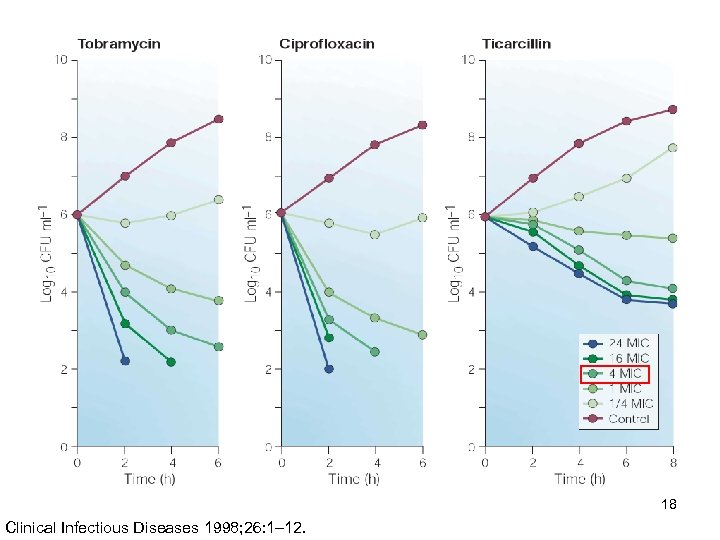
18 Clinical Infectious Diseases 1998; 26: 1– 12.

PK/PD of β-lactam • Time-dependent characteristic – The best predictor of bacterial killing: % f T>MIC • >4×MIC higher is better • The longer f T>MIC, the better the outcome Lodise TP et al. Pharmacotherapy 2006; 26: 1320. Nicolau DP. Critical care 2008; 12 Suppl 4: S 2. 19
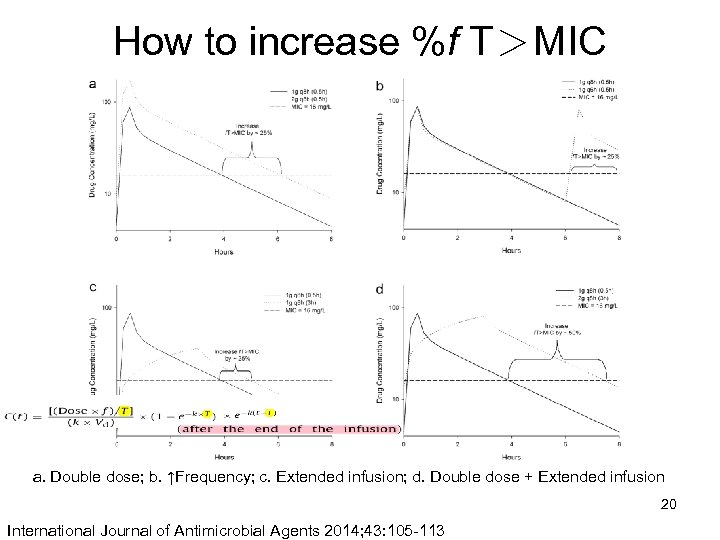
How to increase %f T>MIC a. Double dose; b. ↑Frequency; c. Extended infusion; d. Double dose + Extended infusion 20 International Journal of Antimicrobial Agents 2014; 43: 105 -113
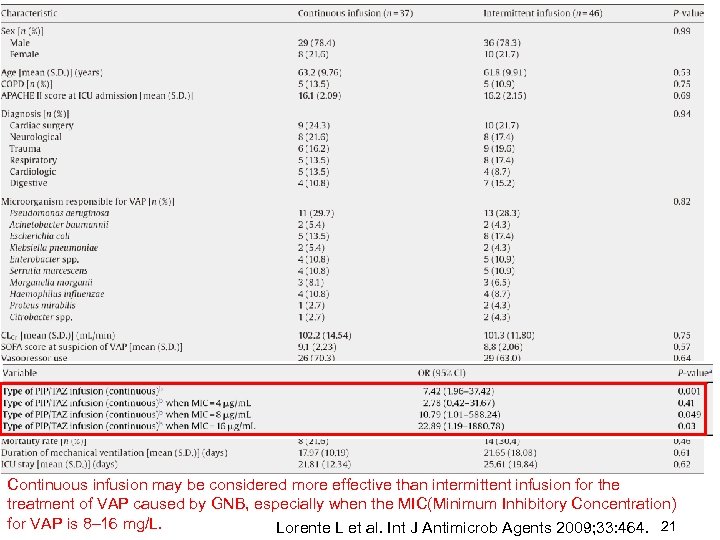
Continuous infusion may be considered more effective than intermittent infusion for the treatment of VAP caused by GNB, especially when the MIC(Minimum Inhibitory Concentration) for VAP is 8– 16 mg/L. Lorente L et al. Int J Antimicrob Agents 2009; 33: 464. 21
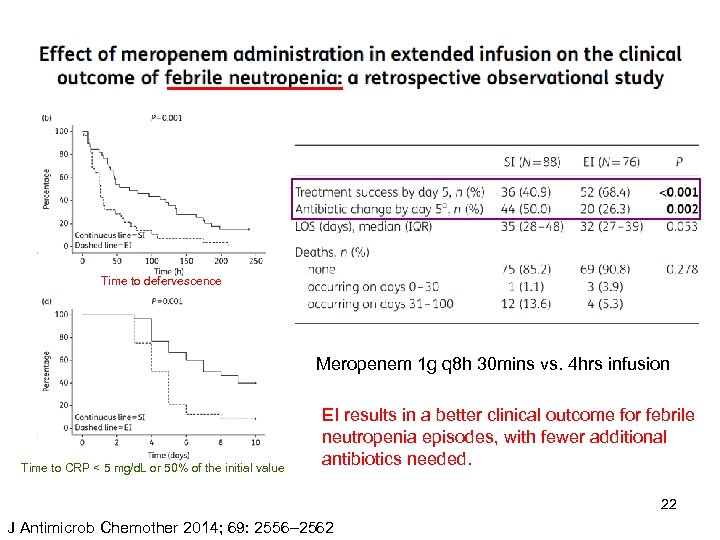
Time to defervescence Meropenem 1 g q 8 h 30 mins vs. 4 hrs infusion Time to CRP < 5 mg/d. L or 50% of the initial value EI results in a better clinical outcome for febrile neutropenia episodes, with fewer additional antibiotics needed. 22 J Antimicrob Chemother 2014; 69: 2556– 2562
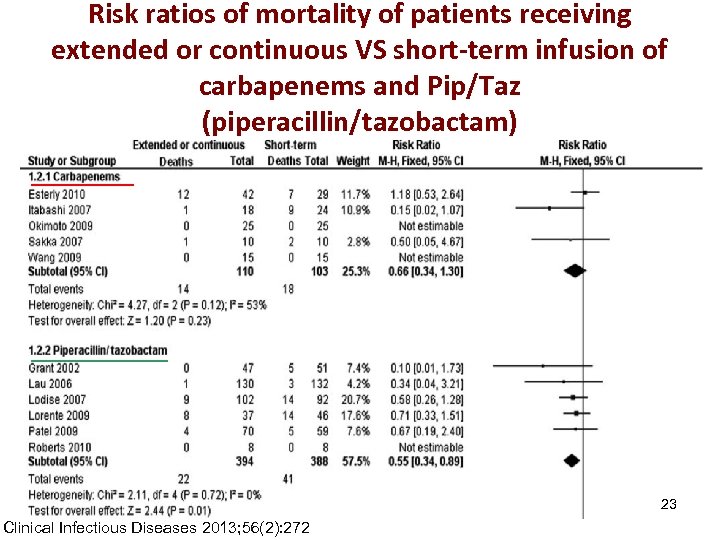
Risk ratios of mortality of patients receiving extended or continuous VS short-term infusion of carbapenems and Pip/Taz (piperacillin/tazobactam) 23 Clinical Infectious Diseases 2013; 56(2): 272
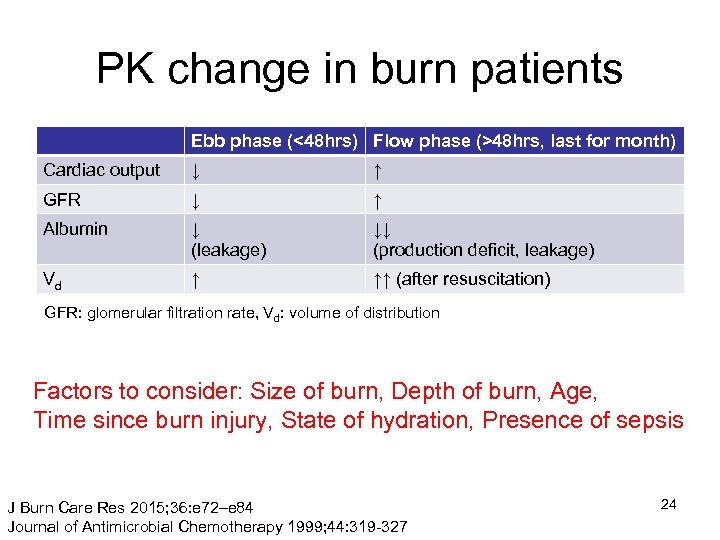

PK change in burn patients Ebb phase (<48 hrs) Flow phase (>48 hrs, last for month) Cardiac output ↓ ↑ GFR ↓ ↑ Albumin ↓ (leakage) ↓↓ (production deficit, leakage) Vd ↑ ↑↑ (after resuscitation) GFR: glomerular filtration rate, Vd: volume of distribution Factors to consider: Size of burn, Depth of burn, Age, Time since burn injury, State of hydration, Presence of sepsis J Burn Care Res 2015; 36: e 72–e 84 Journal of Antimicrobial Chemotherapy 1999; 44: 319 -327 24
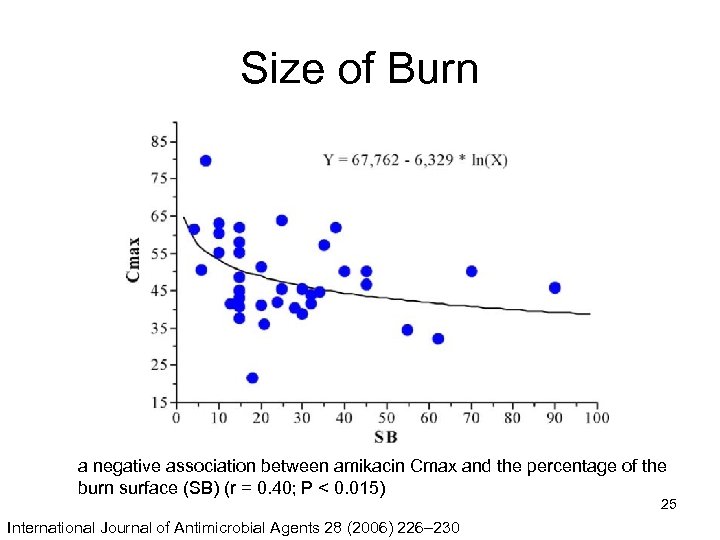
Size of Burn a negative association between amikacin Cmax and the percentage of the burn surface (SB) (r = 0. 40; P < 0. 015) 25 International Journal of Antimicrobial Agents 28 (2006) 226– 230
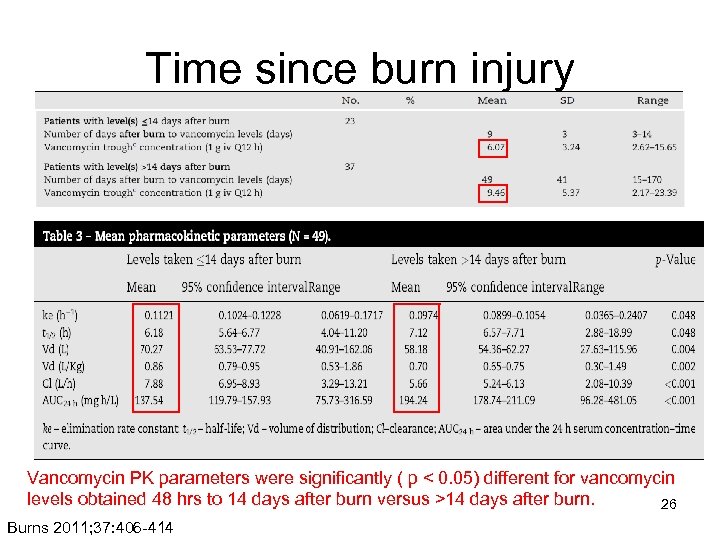

Time since burn injury Vancomycin PK parameters were significantly ( p < 0. 05) different for vancomycin levels obtained 48 hrs to 14 days after burn versus >14 days after burn. 26 Burns 2011; 37: 406 -414
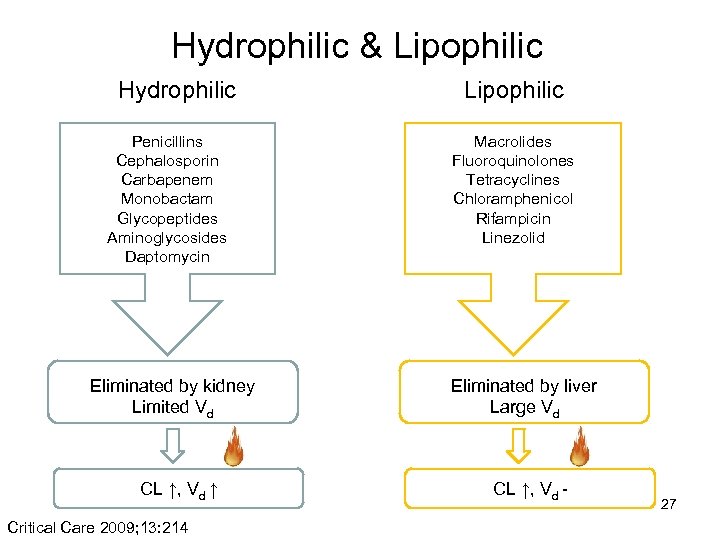
Hydrophilic & Lipophilic Hydrophilic Penicillins Cephalosporin Carbapenem Monobactam Glycopeptides Aminoglycosides Daptomycin Eliminated by kidney Limited Vd CL ↑, Vd ↑ Critical Care 2009; 13: 214 Lipophilic Macrolides Fluoroquinolones Tetracyclines Chloramphenicol Rifampicin Linezolid Eliminated by liver Large Vd CL ↑, Vd - 27

3. PK/PD study in burn patients

Summary of antibiotics PK study in burn patients • PK studies in burn patients showed discrepancy – Small sample size – Variability across PK/PD methods, as well as soft-wares – Different burn factors • Vd and CL were higher than healthy population – High dose of antibiotics was suggested for burn patients without renal failure – Therapeutic drug monitoring(TDM) is important • Studies focused on aminoglycosides, β-lactams, glycopeptides. Lack of data of colistin and tigecycline J Burn Care Res 2015; 36: e 194–e 211; J Burn Care Res 2015; 36: e 72–e 84 Clin Pharmacokinet 2008; 47 (10): 635 -654 29
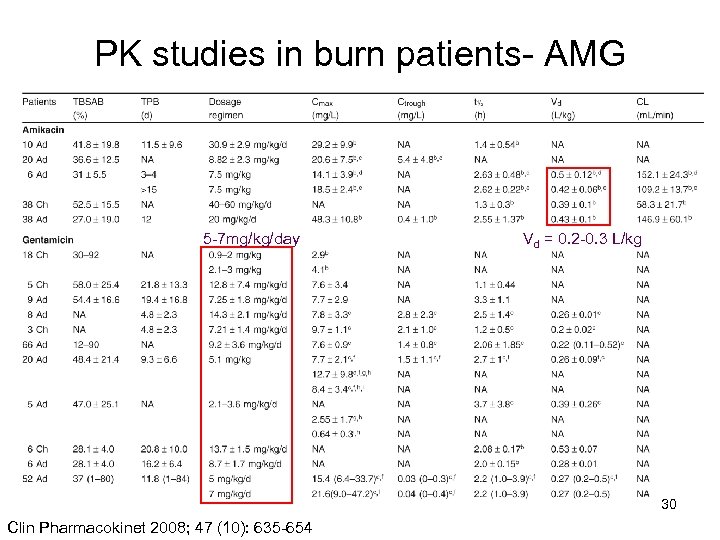
PK studies in burn patients- AMG 5 -7 mg/kg/day Vd = 0. 2 -0. 3 L/kg 30 Clin Pharmacokinet 2008; 47 (10): 635 -654
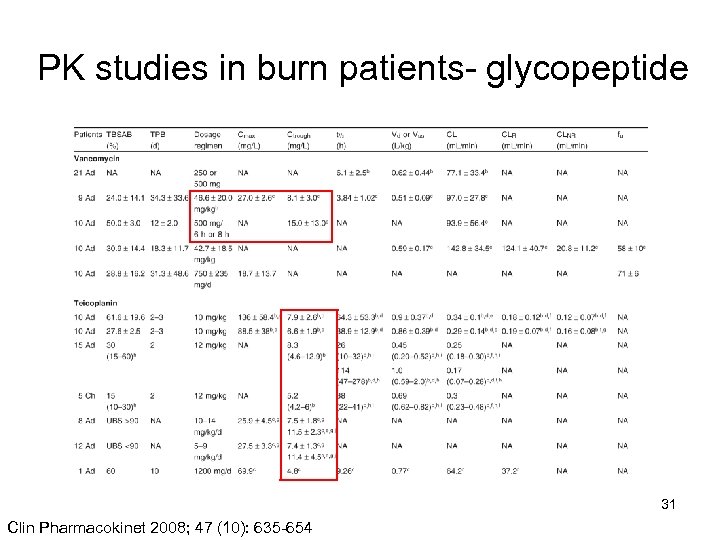
PK studies in burn patients- glycopeptide 31 Clin Pharmacokinet 2008; 47 (10): 635 -654

Vancomycin dosing regimen in burn Only 20 -25% could achieve trough target based on this regimen, TDM is mandated in burn patients , and two serum level is suggested Burns 2011; 3 7: 406 -414 32
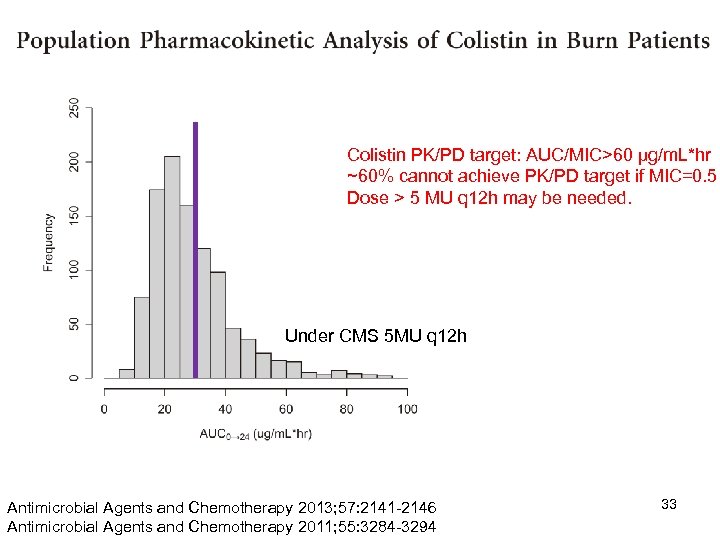
Colistin PK/PD target: AUC/MIC>60 μg/m. L*hr ~60% cannot achieve PK/PD target if MIC=0. 5 Dose > 5 MU q 12 h may be needed. Under CMS 5 MU q 12 h Antimicrobial Agents and Chemotherapy 2013; 57: 2141 -2146 Antimicrobial Agents and Chemotherapy 2011; 55: 3284 -3294 33
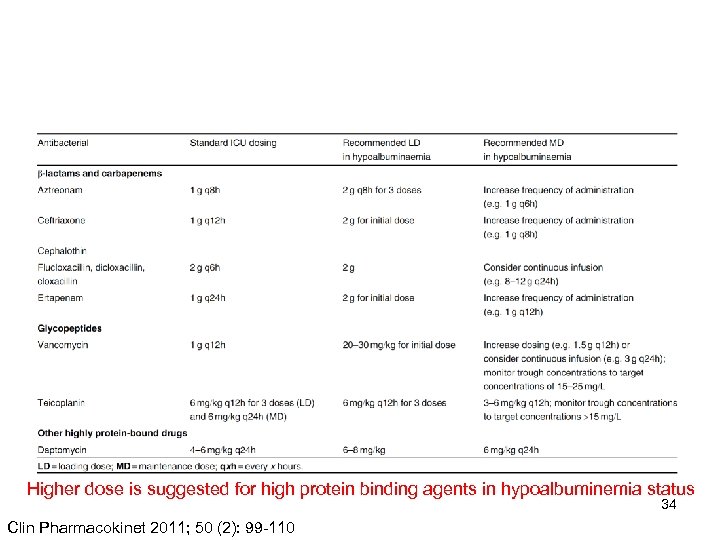
Higher dose is suggested for high protein binding agents in hypoalbuminemia status 34 Clin Pharmacokinet 2011; 50 (2): 99 -110

4. Approaches to improve antibiotics effect in burn patients

Approaches to improve antibiotics effect • Vd ↑ = ↑ Loading dose – Amikacin once daily dose: 25 mg/kg – Vancomycin loading dose: 25 -30 mg/kg • CL ↑ = ↑ daily dose – Time-dependent antibiotics = extended infusion or continuous infusion • Therapeutic drug monitoring (TDM) – AMG, vancomycin = 2 serum levels for individual PK data – β-lactam, future development 36
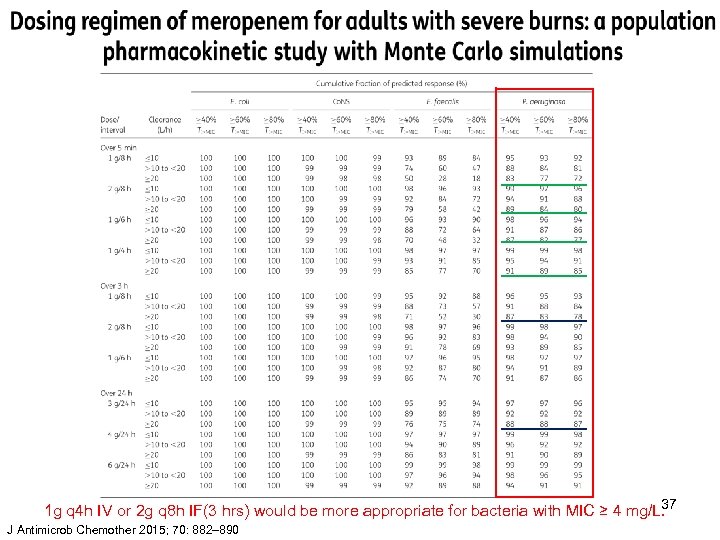
37 1 g q 4 h IV or 2 g q 8 h IF(3 hrs) would be more appropriate for bacteria with MIC ≥ 4 mg/L. J Antimicrob Chemother 2015; 70: 882– 890

TDM for AMG and vancomycin • Follow up 2 serum level was suggested – Applied Sawchuk and Zaske method for PK parameter such as K, Vd, CL, AUC etc. • Sawchuk and Zaske method – Cpt = Cp 0 x e-kt – At steady state Cpt = D x e-kt /[Vd(1 -e-k )] – T 1/2 = 0. 693/K – CL (L/hr) = K*Vd t: time between Cp 0 and Cpt, D: dose, Vd: volume of distribution, = dosing interval, CL: clearance, k: elimination constant, AUC: area under curve 38
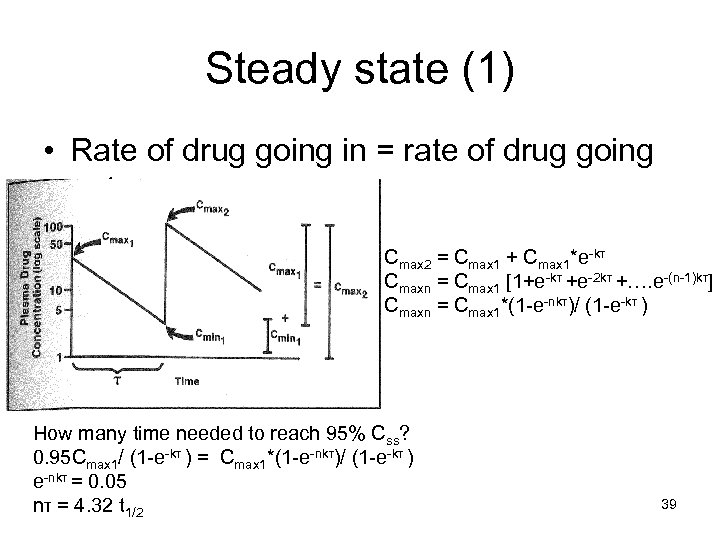
Steady state (1) • Rate of drug going in = rate of drug going out Cmax 2 = Cmax 1 + Cmax 1*e-kτ Cmaxn = Cmax 1 [1+e-kτ +e-2 kτ +…. e-(n-1)kτ] Cmaxn = Cmax 1*(1 -e-nkτ)/ (1 -e-kτ ) How many time needed to reach 95% Css? 0. 95 Cmax 1/ (1 -e-kτ ) = Cmax 1*(1 -e-nkτ)/ (1 -e-kτ ) e-nkτ = 0. 05 nτ = 4. 32 t 1/2 39
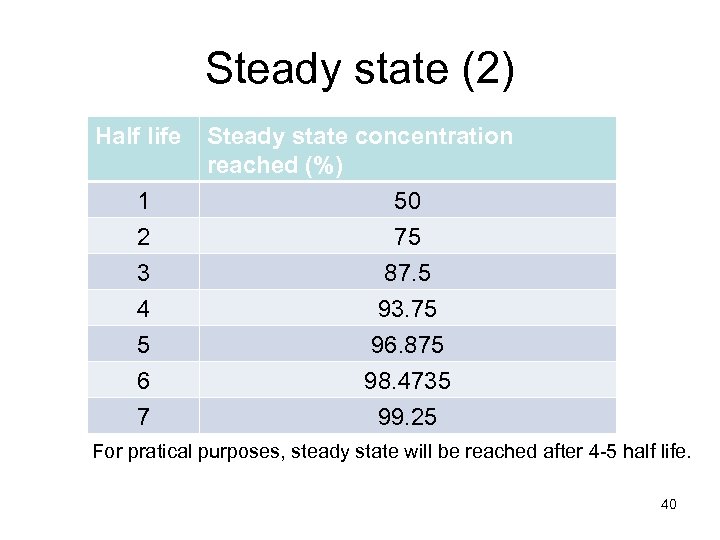
Steady state (2) Half life 1 2 3 4 5 6 7 Steady state concentration reached (%) 50 75 87. 5 93. 75 96. 875 98. 4735 99. 25 For pratical purposes, steady state will be reached after 4 -5 half life. 40
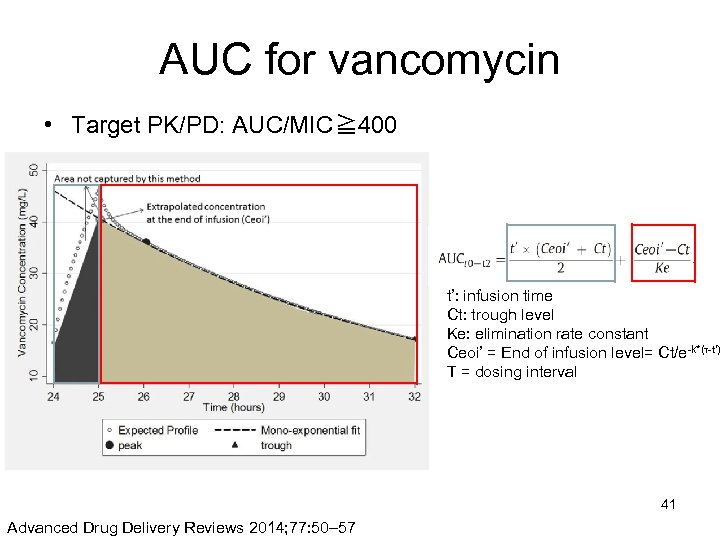
AUC for vancomycin • Target PK/PD: AUC/MIC≧ 400 t’: infusion time Ct: trough level Ke: elimination rate constant Ceoi’ = End of infusion level= Ct/e-k*(τ-t’) Τ = dosing interval 41 Advanced Drug Delivery Reviews 2014; 77: 50– 57

Example • 20 y/o male, 180 cm/83. 1 kg, SCr: 0. 7 mg/d. L • Vancomycin was used to cover gram positive pathogen empirically • LD: 2000 mg; MD: 1000 mg q 8 h • Infusion time: 5: 00 -7: 00 • Level 1 time: 10: 30, Level 1 = 10. 82 mg/L • Level 2 time: 13: 00, Level 2 = 4. 44 mg/L • What is the k, t 1/2, Vd, CL, and AUC? 42
![Answer • K = ln[(10. 82/4. 44)/2. 5] = 0. 35 hr-1 • T Answer • K = ln[(10. 82/4. 44)/2. 5] = 0. 35 hr-1 • T](https://present5.com/presentation/b50c0198ef051738e59a6a405a80d5c3/image-43.jpg)
Answer • K = ln[(10. 82/4. 44)/2. 5] = 0. 35 hr-1 • T 1/2 = 0. 693/K = 1. 98 hr • Cpt = D x e-kt /[Vd(1 -e-k )], D=1000 mg, t=8 hr, Cpt=4. 44 mg/L – Vd = 14. 58 L • CL = K* Vd = 5. 1 L/hr • AUC = 405 mg*hr/L – Ceoi = 37. 17 mg/L, [(37. 17+4. 44)+(37. 174. 44)/0. 35]*3 = 405 43
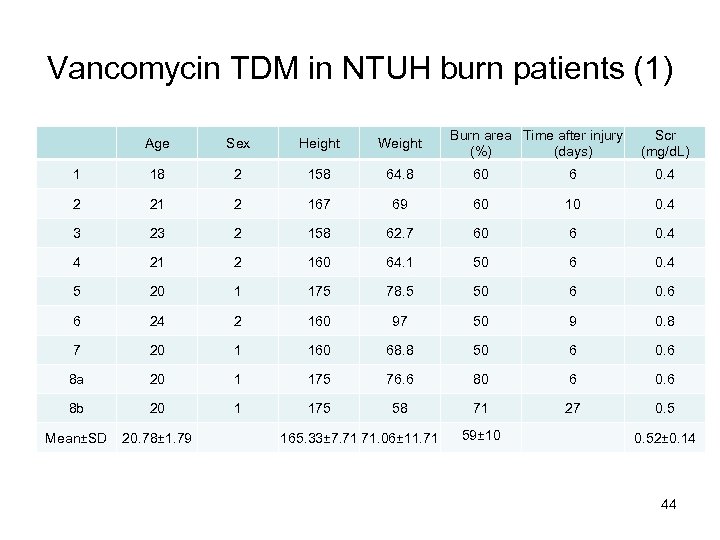
Vancomycin TDM in NTUH burn patients (1) Burn area Time after injury (%) (days) Scr (mg/d. L) Age Sex Height Weight 1 18 2 158 64. 8 60 6 0. 4 2 21 2 167 69 60 10 0. 4 3 23 2 158 62. 7 60 6 0. 4 4 21 2 160 64. 1 50 6 0. 4 5 20 1 175 78. 5 50 6 0. 6 6 24 2 160 97 50 9 0. 8 7 20 1 160 68. 8 50 6 0. 6 8 a 20 1 175 76. 6 80 6 0. 6 8 b 20 1 175 58 71 27 0. 5 Mean±SD 20. 78± 1. 79 165. 33± 7. 71 71. 06± 11. 71 59± 10 0. 52± 0. 14 44
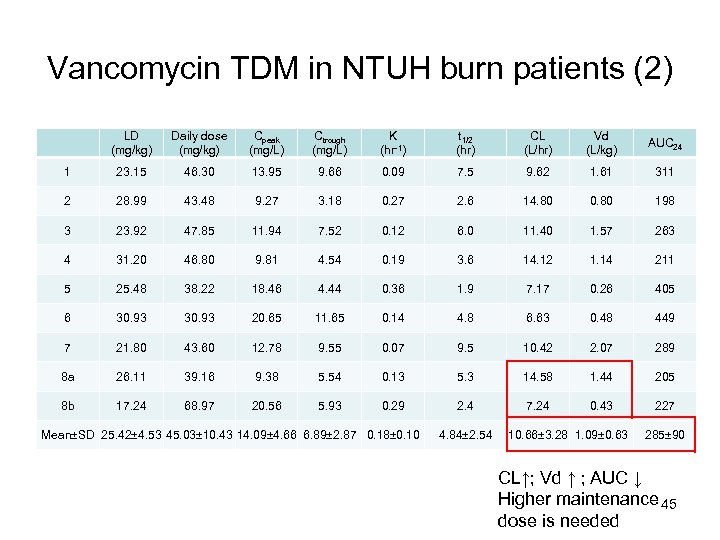
Vancomycin TDM in NTUH burn patients (2) LD (mg/kg) Daily dose (mg/kg) Cpeak (mg/L) Ctrough (mg/L) K (hr-1) t 1/2 (hr) CL (L/hr) Vd (L/kg) AUC 24 1 23. 15 46. 30 13. 95 9. 66 0. 09 7. 5 9. 62 1. 61 311 2 28. 99 43. 48 9. 27 3. 18 0. 27 2. 6 14. 80 0. 80 198 3 23. 92 47. 85 11. 94 7. 52 0. 12 6. 0 11. 40 1. 57 263 4 31. 20 46. 80 9. 81 4. 54 0. 19 3. 6 14. 12 1. 14 211 5 25. 48 38. 22 18. 46 4. 44 0. 36 1. 9 7. 17 0. 26 405 6 30. 93 20. 65 11. 65 0. 14 4. 8 6. 63 0. 48 449 7 21. 80 43. 60 12. 78 9. 55 0. 07 9. 5 10. 42 2. 07 289 8 a 26. 11 39. 16 9. 38 5. 54 0. 13 5. 3 14. 58 1. 44 205 8 b 17. 24 68. 97 20. 56 5. 93 0. 29 2. 4 7. 24 0. 43 227 Mean±SD 25. 42± 4. 53 45. 03± 10. 43 14. 09± 4. 66 6. 89± 2. 87 0. 18± 0. 10 4. 84± 2. 54 10. 66± 3. 28 1. 09± 0. 63 285± 90 CL↑; Vd ↑ ; AUC ↓ Higher maintenance 45 dose is needed

• Benefit for population with unpredictable PK parameters – Critically ill (burn), the obese, the elderly and those with cystic fibrosis. • Target: 100% f. T>MIC • Only available in 30 hospitals in the world • Obstacle for this service – HPLC(High Performance Liquid Chromatography), longer turnaround time (624 hrs), higher cost 46 J Antimicrob Chemother 2015; doi: 10. 1093/jac/dkv 201

Similar numbers of inappropriate meropenem trough levels (30. 4%) were below and above the upper limit. Burns 2015; 41: 956 -968 47

Take home message • Vd and CL of antibiotics increase in burn patients, and this results in higher loading and maintenance dose for this population. • TDM is the best approach to optimize antibiotic treatment • Still lack of PK data of many antibiotics in this field 48

Thank you for your attention
b50c0198ef051738e59a6a405a80d5c3.ppt