615e79a837f42393df18e86ff1689728.ppt
- Количество слайдов: 38
 Pediatric Anti-Retroviral Drug Formulary 2004 Celia DC Christie CHART Conference Montego Bay, Jamaica July 18, 2004
Pediatric Anti-Retroviral Drug Formulary 2004 Celia DC Christie CHART Conference Montego Bay, Jamaica July 18, 2004
 Pediatric HIV in the Caribbean • 3% women in Antenatal Clinics are HIV+ • 2, 600 - 4, 000 children born to HIV+ Moms, with 1, 070 newly infected children annually • HIV/AIDS leading cause of death in 1 -4 yr group • Transmission - MTCT, breast feeding, abuse • With low cost ART’s becoming available, we need to know how to use them to improve morbidity and mortality in children with HIV/AIDS
Pediatric HIV in the Caribbean • 3% women in Antenatal Clinics are HIV+ • 2, 600 - 4, 000 children born to HIV+ Moms, with 1, 070 newly infected children annually • HIV/AIDS leading cause of death in 1 -4 yr group • Transmission - MTCT, breast feeding, abuse • With low cost ART’s becoming available, we need to know how to use them to improve morbidity and mortality in children with HIV/AIDS
 Caribbean Diversity • Wide diversity – Expertise – Health care facilities – Lab diagnostic capacity – Treatment options • p. ARV monitored by pediatricians with – Expertise in treating p. HIV, OI’s, using ARV’s
Caribbean Diversity • Wide diversity – Expertise – Health care facilities – Lab diagnostic capacity – Treatment options • p. ARV monitored by pediatricians with – Expertise in treating p. HIV, OI’s, using ARV’s
 Purpose • Principles of anti-retroviral therapy (p. ARV) – Whom should we treat – First line and second line ARVs – Monitoring of p. ARVs, clinical and lab – Reasons for changing HAART • Pediatric ARV formulary for Caribbean • Special issues in Children • Case histories and prognosis
Purpose • Principles of anti-retroviral therapy (p. ARV) – Whom should we treat – First line and second line ARVs – Monitoring of p. ARVs, clinical and lab – Reasons for changing HAART • Pediatric ARV formulary for Caribbean • Special issues in Children • Case histories and prognosis
 Principles of p. ART • MTCT HIV progresses more rapidly in infants and children that HIV in adults • 10 yrs post infection 50% adults AIDS • 3 years post infection 50% kids AIDS • Rapid, slow and no disease progression • CNS damage common in infants • Viral load and CD 4 counts are not as predictive of outcome in 1 st year vs. later
Principles of p. ART • MTCT HIV progresses more rapidly in infants and children that HIV in adults • 10 yrs post infection 50% adults AIDS • 3 years post infection 50% kids AIDS • Rapid, slow and no disease progression • CNS damage common in infants • Viral load and CD 4 counts are not as predictive of outcome in 1 st year vs. later
 NIH’s ART Treatment Decisions • We SHOULD treat: – All HIV-infected children < 1 year, regardless of clinical, immunologic, or virologic status – All HIV infected children > 1 year if, recent symptoms of ongoing HIV infection, or significant immune suppression, or viral load suggests disease progression, ie. , viral load > 100, 000 copies/ml • Delay ART if stable, or non-compliance
NIH’s ART Treatment Decisions • We SHOULD treat: – All HIV-infected children < 1 year, regardless of clinical, immunologic, or virologic status – All HIV infected children > 1 year if, recent symptoms of ongoing HIV infection, or significant immune suppression, or viral load suggests disease progression, ie. , viral load > 100, 000 copies/ml • Delay ART if stable, or non-compliance
 WHO’s treatment decisions • < 18 months: if virologically proven, or CD 4 available – All clinical AIDS, stage 3 – All stage 2, with CD 4 < 20% – All symptomatic stage 1, with CD 4 < 20% • > 18 months and HIV positive – All clinical AIDS, stage 3 – All stage 2 HIV, CD 4 + < 15% assist decision – All stage 1, CD 4 and < 15% (asymptomatic)
WHO’s treatment decisions • < 18 months: if virologically proven, or CD 4 available – All clinical AIDS, stage 3 – All stage 2, with CD 4 < 20% – All symptomatic stage 1, with CD 4 < 20% • > 18 months and HIV positive – All clinical AIDS, stage 3 – All stage 2 HIV, CD 4 + < 15% assist decision – All stage 1, CD 4 and < 15% (asymptomatic)
 Goals of Therapy • Achieve and maintain HIV viral load = zero – Prevents disease progression – Optimizes recovery – Prevents ART drug resistance • Temporary partial suppression of viral replication leads to resistance and limits future treatment options
Goals of Therapy • Achieve and maintain HIV viral load = zero – Prevents disease progression – Optimizes recovery – Prevents ART drug resistance • Temporary partial suppression of viral replication leads to resistance and limits future treatment options
 Individualize Treatment Plans • • Clinical considerations Drug side effects, interactions Patient convenience Drug availability and cost
Individualize Treatment Plans • • Clinical considerations Drug side effects, interactions Patient convenience Drug availability and cost
 Adherence Treatment failures from non-adherence – Establish trust, mutually acceptable goals for care – Evaluate nursing, social, behavioral assessments – Obtaining, storing, administering medications – Who is responsible and how dosing is done? – Intensive family education and medication training before initiating treatment
Adherence Treatment failures from non-adherence – Establish trust, mutually acceptable goals for care – Evaluate nursing, social, behavioral assessments – Obtaining, storing, administering medications – Who is responsible and how dosing is done? – Intensive family education and medication training before initiating treatment
 Teaching Pill-swallowing • Children 3 years of age can be pill-trained • No unpleasant experiences with pill-taking and no behavior problems • Relax, give child increasing sizes of placebo, encourage to swallow with water • Encourage with minimal extrinsic rewards • Once child starts taking ART’s, he cannot be allowed to refuse meds • Disallow any other activity until ART’s are taken
Teaching Pill-swallowing • Children 3 years of age can be pill-trained • No unpleasant experiences with pill-taking and no behavior problems • Relax, give child increasing sizes of placebo, encourage to swallow with water • Encourage with minimal extrinsic rewards • Once child starts taking ART’s, he cannot be allowed to refuse meds • Disallow any other activity until ART’s are taken
 WHO’s 1 st Line Regimen Zidovudine/ Retrovir / AZT or Stavudine/ Zerit/ D 4 T Plus Lamivudine /Epivir / 3 TC Plus Nevirapine/ Viramune /NVP, or Efavirenz/ Sustiva /EFV NB: If age < 3, weight < 10 kg use NVP If age > 3 y, weight > 10 kg use NVP/EFV
WHO’s 1 st Line Regimen Zidovudine/ Retrovir / AZT or Stavudine/ Zerit/ D 4 T Plus Lamivudine /Epivir / 3 TC Plus Nevirapine/ Viramune /NVP, or Efavirenz/ Sustiva /EFV NB: If age < 3, weight < 10 kg use NVP If age > 3 y, weight > 10 kg use NVP/EFV
 1 st Line Therapy if TB likely Zidovudine/ Retrovir /AZT Plus Lamivudine/ Epivir /3 TC Plus Abacavir/ Ziagen /ABC NB: ARV therapy should be deferred for at last 2 months after anti-TB medications have been commenced
1 st Line Therapy if TB likely Zidovudine/ Retrovir /AZT Plus Lamivudine/ Epivir /3 TC Plus Abacavir/ Ziagen /ABC NB: ARV therapy should be deferred for at last 2 months after anti-TB medications have been commenced
 Other 1 st Line Options Zidovudine/ AZT + Lamivudine /3 TC + Nelfinavir/ NLF, or Ritonavir/ RTV
Other 1 st Line Options Zidovudine/ AZT + Lamivudine /3 TC + Nelfinavir/ NLF, or Ritonavir/ RTV
 Other Monitors • Intensive follow-up to support and educate family, monitor adherence, viral response – Viral loads monthly, until undetectable, then three monthly visits – Pharmacy refills, pill counts, medication intolerance, dosing difficulties, inconvenience – CBC, electrolytes, urea, LFT’s, lipid panels – Failure should prompt evaluation of adherence and potential drug resistance
Other Monitors • Intensive follow-up to support and educate family, monitor adherence, viral response – Viral loads monthly, until undetectable, then three monthly visits – Pharmacy refills, pill counts, medication intolerance, dosing difficulties, inconvenience – CBC, electrolytes, urea, LFT’s, lipid panels – Failure should prompt evaluation of adherence and potential drug resistance
 Treatment Failure – Clinical • Lack of growth – after an initial growth response • Decline in growth – after an initial response • Loss of neuro-developmental milestones • Development of encephalopathy • New opportunistic infection, or malignancy – signifying clinical disease progression
Treatment Failure – Clinical • Lack of growth – after an initial growth response • Decline in growth – after an initial response • Loss of neuro-developmental milestones • Development of encephalopathy • New opportunistic infection, or malignancy – signifying clinical disease progression
 Treatment Failure - Immunological • Return of CD 4 count, or if age < 6 yrs, of CD 4 percentage to pre-baseline or below • > 50% fall from peak level on therapy of CD 4 cell percentage without obvious cause
Treatment Failure - Immunological • Return of CD 4 count, or if age < 6 yrs, of CD 4 percentage to pre-baseline or below • > 50% fall from peak level on therapy of CD 4 cell percentage without obvious cause
 Preventing Resistance • Replicating virus in presence of drug promotes resistance • Treatment must achieve suppression of viral load to zero to prevent resistance • Non-adherence or resistance must be considered if viral load does not decay rapidly to undetectable
Preventing Resistance • Replicating virus in presence of drug promotes resistance • Treatment must achieve suppression of viral load to zero to prevent resistance • Non-adherence or resistance must be considered if viral load does not decay rapidly to undetectable
 Changing ART Regimen • Do not change ART’s until you have ruled out non-adherence • Confirm viral load that suggest a change is needed • Because of limited treatment options, better to accept a suboptimal response than to change to a new regimen that may not control viral replication
Changing ART Regimen • Do not change ART’s until you have ruled out non-adherence • Confirm viral load that suggest a change is needed • Because of limited treatment options, better to accept a suboptimal response than to change to a new regimen that may not control viral replication
 WHO’s 2 nd Line ARV’s Abacavir/ Ziagen/ ABC plus Didanosine/ Videx/ dd. I plus PI Lopinavir/ritonavir/ Kaletra/ LPV/r or Saquinavir/ Fortovase/ SQVr
WHO’s 2 nd Line ARV’s Abacavir/ Ziagen/ ABC plus Didanosine/ Videx/ dd. I plus PI Lopinavir/ritonavir/ Kaletra/ LPV/r or Saquinavir/ Fortovase/ SQVr
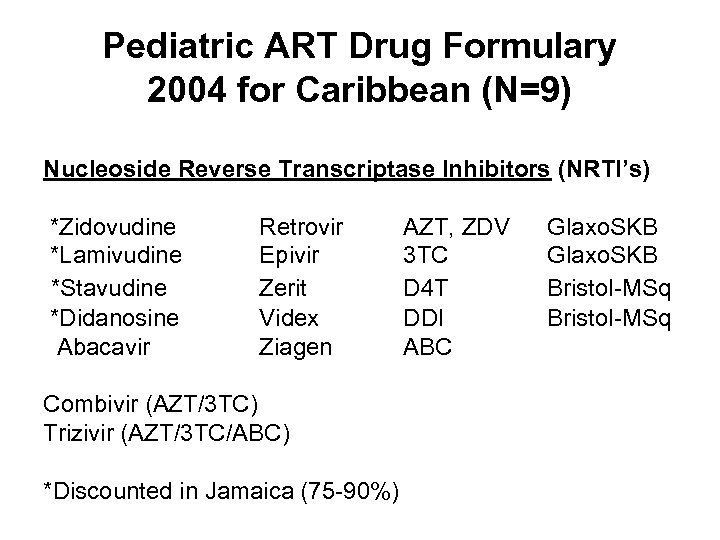 Pediatric ART Drug Formulary 2004 for Caribbean (N=9) Nucleoside Reverse Transcriptase Inhibitors (NRTI’s) *Zidovudine *Lamivudine *Stavudine *Didanosine Abacavir Retrovir Epivir Zerit Videx Ziagen Combivir (AZT/3 TC) Trizivir (AZT/3 TC/ABC) *Discounted in Jamaica (75 -90%) AZT, ZDV 3 TC D 4 T DDI ABC Glaxo. SKB Bristol-MSq
Pediatric ART Drug Formulary 2004 for Caribbean (N=9) Nucleoside Reverse Transcriptase Inhibitors (NRTI’s) *Zidovudine *Lamivudine *Stavudine *Didanosine Abacavir Retrovir Epivir Zerit Videx Ziagen Combivir (AZT/3 TC) Trizivir (AZT/3 TC/ABC) *Discounted in Jamaica (75 -90%) AZT, ZDV 3 TC D 4 T DDI ABC Glaxo. SKB Bristol-MSq
 Pediatric ART Drug Formulary 2004 for Caribbean (N=9) Non-nucleoside reverse transcriptase inhibitor (NNRTI) **Nevirapine *Efavirenz Viramune Sustiva *Discounted in Jamaica (75 -90%) **Free in Jamaica for MTCT NVP EFV Dupont
Pediatric ART Drug Formulary 2004 for Caribbean (N=9) Non-nucleoside reverse transcriptase inhibitor (NNRTI) **Nevirapine *Efavirenz Viramune Sustiva *Discounted in Jamaica (75 -90%) **Free in Jamaica for MTCT NVP EFV Dupont
 Pediatric ART Drug Formulary 2004 for Caribbean (N=9) Protease Inhibitor (PI) Nelfinavir Lopinavir/Ritonavir Viracept NFV Kaletra LPV/r
Pediatric ART Drug Formulary 2004 for Caribbean (N=9) Protease Inhibitor (PI) Nelfinavir Lopinavir/Ritonavir Viracept NFV Kaletra LPV/r
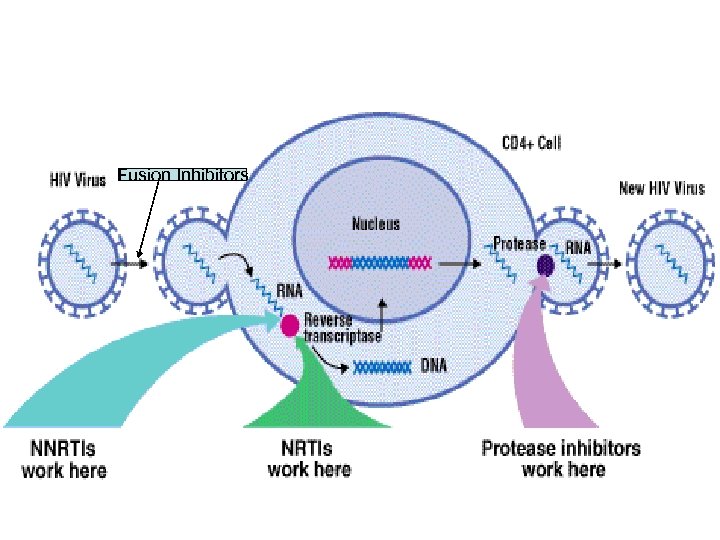 Fusion Inhibitors
Fusion Inhibitors
 Special Issues in Children • Growth failure and CNS disease – ARV’s that penetrate CNS • No good tasting ARV’s – especially, RTV, NLF • Regimens should be twice daily – EFV once daily • > 3 ARV’s should be given • Toxicity
Special Issues in Children • Growth failure and CNS disease – ARV’s that penetrate CNS • No good tasting ARV’s – especially, RTV, NLF • Regimens should be twice daily – EFV once daily • > 3 ARV’s should be given • Toxicity
 More Issues • Pharmacokinetics – Different drug distribution, metabolism, clearance, dosing (weight, BMI), side effects • Ensure health and well-being of caregiver – Grandparents, elderly guardians • Disclosure, adolescents and sexuality • Stigma and severe poverty contribute to non-adherence
More Issues • Pharmacokinetics – Different drug distribution, metabolism, clearance, dosing (weight, BMI), side effects • Ensure health and well-being of caregiver – Grandparents, elderly guardians • Disclosure, adolescents and sexuality • Stigma and severe poverty contribute to non-adherence
 Pediatric HIV Clinics, Kingston Sept. 1, 2002 – June 11, 2004 (21 mos) Health Institutions ## University Hospital Spanish Town Hospital Comprehensive Clinic Bustamante Hospital Victoria Jubilee Hospital 125 80 81 60 8 Total 354
Pediatric HIV Clinics, Kingston Sept. 1, 2002 – June 11, 2004 (21 mos) Health Institutions ## University Hospital Spanish Town Hospital Comprehensive Clinic Bustamante Hospital Victoria Jubilee Hospital 125 80 81 60 8 Total 354
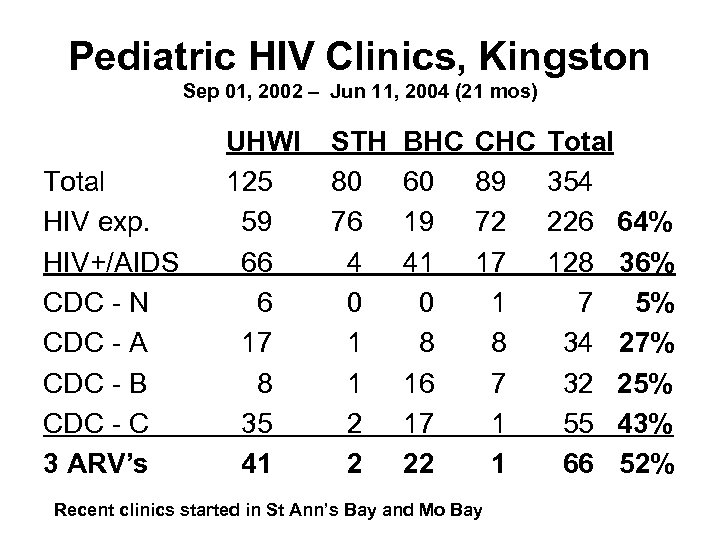 Pediatric HIV Clinics, Kingston Sep 01, 2002 – Jun 11, 2004 (21 mos) Total HIV exp. HIV+/AIDS CDC - N CDC - A CDC - B CDC - C 3 ARV’s UHWI 125 59 66 6 17 8 35 41 STH 80 76 4 0 1 1 2 2 BHC 60 19 41 0 8 16 17 22 CHC 89 72 17 1 8 7 1 1 Recent clinics started in St Ann’s Bay and Mo Bay Total 354 226 64% 128 36% 7 5% 34 27% 32 25% 55 43% 66 52%
Pediatric HIV Clinics, Kingston Sep 01, 2002 – Jun 11, 2004 (21 mos) Total HIV exp. HIV+/AIDS CDC - N CDC - A CDC - B CDC - C 3 ARV’s UHWI 125 59 66 6 17 8 35 41 STH 80 76 4 0 1 1 2 2 BHC 60 19 41 0 8 16 17 22 CHC 89 72 17 1 8 7 1 1 Recent clinics started in St Ann’s Bay and Mo Bay Total 354 226 64% 128 36% 7 5% 34 27% 32 25% 55 43% 66 52%
 TB and HIV Co-infection in Jamaican Children at UHWI Active TB +HIV 1999 2 2 2000 0 0 2001 9 3 2002 14 7 ---------------------------Total 25 12 Trend analysis -- P < 0. 05
TB and HIV Co-infection in Jamaican Children at UHWI Active TB +HIV 1999 2 2 2000 0 0 2001 9 3 2002 14 7 ---------------------------Total 25 12 Trend analysis -- P < 0. 05
 Whom do we treat? • No access to CD 4, viral loads, genotyping, so treatment decisions and followup are clinical – – – – All tuberculosis Failure to thrive Hospitalized CDC category C, then B Any HIV-infected child aged < one year Affordability of drugs and care Adherence/ access to meds and care
Whom do we treat? • No access to CD 4, viral loads, genotyping, so treatment decisions and followup are clinical – – – – All tuberculosis Failure to thrive Hospitalized CDC category C, then B Any HIV-infected child aged < one year Affordability of drugs and care Adherence/ access to meds and care
 Clinical Monitoring • Reduced hospitalizations • Increased appetite, weight, height • Improved brain growth, neurodevelopment affect, head circumference • Reduced morbidity, opportunistic infections, minor co-morbid illnesses, – papular prurigo, otitis media, oral thrush, URIs
Clinical Monitoring • Reduced hospitalizations • Increased appetite, weight, height • Improved brain growth, neurodevelopment affect, head circumference • Reduced morbidity, opportunistic infections, minor co-morbid illnesses, – papular prurigo, otitis media, oral thrush, URIs
 ARV’s prevent hospitalization • SH - infected at birth by blood transfusion • Admitted @ 6 months, severe malnutrition, encephalopathy, PCP pneumonitis • Several hospitalizations for LIP, LRTI’s, dyskinetic cerebral palsy, neuro-developmental delay, CD 4 565, HIV viral load 221, 000 c/ml • Commenced AZT, 3 TC, ABC and prednisone – No hospitalizations > 3 years – Excellent growth and developmental improvement – Great school performance
ARV’s prevent hospitalization • SH - infected at birth by blood transfusion • Admitted @ 6 months, severe malnutrition, encephalopathy, PCP pneumonitis • Several hospitalizations for LIP, LRTI’s, dyskinetic cerebral palsy, neuro-developmental delay, CD 4 565, HIV viral load 221, 000 c/ml • Commenced AZT, 3 TC, ABC and prednisone – No hospitalizations > 3 years – Excellent growth and developmental improvement – Great school performance
 ARV’s improve growth • SF – HIV via MTCT, symptomatic at age 10 mos, with recurrent otitis media, sinusitis, chronic diarrhea, LRTI’s, cryptosporidiosis, salmonella UTI’s, failure to thrive, thrombocytopenia • Commenced AZT, 3 TC, NVP • Voracious appetite, weight gain, no more infections
ARV’s improve growth • SF – HIV via MTCT, symptomatic at age 10 mos, with recurrent otitis media, sinusitis, chronic diarrhea, LRTI’s, cryptosporidiosis, salmonella UTI’s, failure to thrive, thrombocytopenia • Commenced AZT, 3 TC, NVP • Voracious appetite, weight gain, no more infections
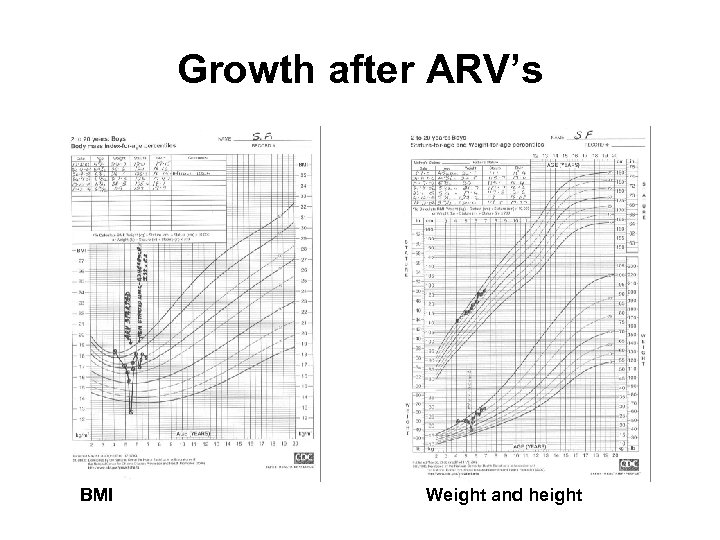 Growth after ARV’s BMI Weight and height
Growth after ARV’s BMI Weight and height
 TB Co-infection cured • • SP, 6 yo F with HIV MTCT TB with recurrent RUL pneumonia CD 4 -154 Treated with INH, RIF, PZA and ETH x 2 mos then INH and RIF x 10 mos • AZT, 3 TC and ABC • TB cured and good growth
TB Co-infection cured • • SP, 6 yo F with HIV MTCT TB with recurrent RUL pneumonia CD 4 -154 Treated with INH, RIF, PZA and ETH x 2 mos then INH and RIF x 10 mos • AZT, 3 TC and ABC • TB cured and good growth
 HIV and TB Co-infections Outcomes at UHWI • Mortality, morbidity and hospital stay longer in HIV and TB co-infections • Children treated with anti-TB drugs alone – Get better in hospital then die – Get better in hospital, then deteriorate during outpatient follow-up • Children treated with anti-TB meds AND anti retrovirals (ARTs) are usually cured
HIV and TB Co-infections Outcomes at UHWI • Mortality, morbidity and hospital stay longer in HIV and TB co-infections • Children treated with anti-TB drugs alone – Get better in hospital then die – Get better in hospital, then deteriorate during outpatient follow-up • Children treated with anti-TB meds AND anti retrovirals (ARTs) are usually cured
 Summary • Pediatric HIV/AIDS is being diagnosed • ARV’s are now available for management • ARV’s can only control but not cure this devastating chronic disease • Children are growing up to consider a university education, buy a house, marry and even have children • While p. MTCT HIV, prognoses for pediatric HIV/AIDS can be excellent, long-term
Summary • Pediatric HIV/AIDS is being diagnosed • ARV’s are now available for management • ARV’s can only control but not cure this devastating chronic disease • Children are growing up to consider a university education, buy a house, marry and even have children • While p. MTCT HIV, prognoses for pediatric HIV/AIDS can be excellent, long-term
 WEST INDIAN MEDICAL JOURNAL - SPECIAL ISSUE Pediatric and Perinatal HIV/AIDS in Jamaica Supported in part by the Elizabeth Glaser Pediatric AIDS Foundation Pfizer Foundation (Pharmaceuticals), the University of the West Indies and the Jamaican Ministry Health.
WEST INDIAN MEDICAL JOURNAL - SPECIAL ISSUE Pediatric and Perinatal HIV/AIDS in Jamaica Supported in part by the Elizabeth Glaser Pediatric AIDS Foundation Pfizer Foundation (Pharmaceuticals), the University of the West Indies and the Jamaican Ministry Health.


