a1f06ce0fdcac69c1a496da0ee3a6fa5.ppt
- Количество слайдов: 58
 PATOLOGIE TUMORALI ENDOCANALARI Dott. ssa Anna Pichiecchio U. O. Neuroradiologia Istituto Neurologico IRCCS Fondazione C. Mondino, Pavia
PATOLOGIE TUMORALI ENDOCANALARI Dott. ssa Anna Pichiecchio U. O. Neuroradiologia Istituto Neurologico IRCCS Fondazione C. Mondino, Pavia
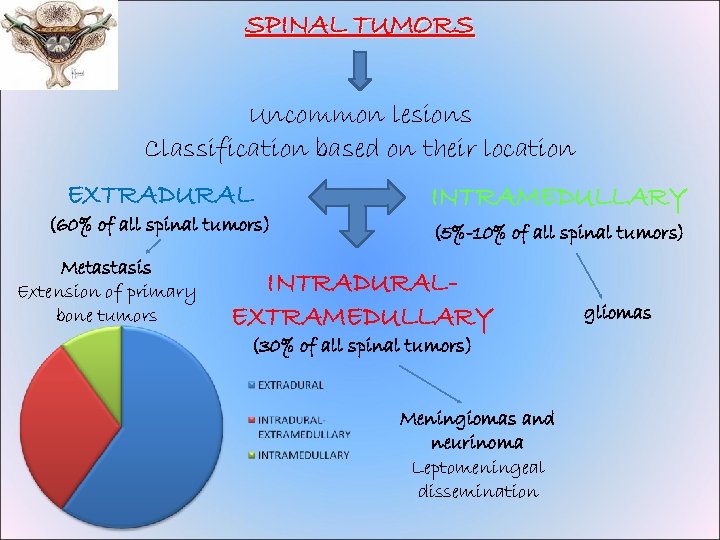 SPINAL TUMORS Uncommon lesions Classification based on their location EXTRADURAL (60% of all spinal tumors) Metastasis Extension of primary bone tumors INTRAMEDULLARY (5%-10% of all spinal tumors) INTRADURALEXTRAMEDULLARY (30% of all spinal tumors) Meningiomas and neurinoma Leptomeningeal dissemination gliomas
SPINAL TUMORS Uncommon lesions Classification based on their location EXTRADURAL (60% of all spinal tumors) Metastasis Extension of primary bone tumors INTRAMEDULLARY (5%-10% of all spinal tumors) INTRADURALEXTRAMEDULLARY (30% of all spinal tumors) Meningiomas and neurinoma Leptomeningeal dissemination gliomas
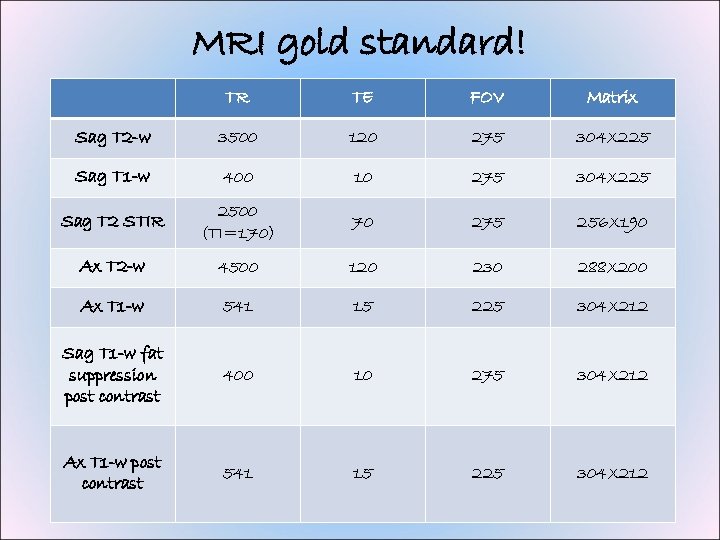 MRI gold standard! TR TE FOV Matrix Sag T 2 -w 3500 120 275 304 X 225 Sag T 1 -w 400 10 275 304 X 225 Sag T 2 STIR 2500 (TI=170) 70 275 256 X 190 Ax T 2 -w 4500 120 230 288 X 200 Ax T 1 -w 541 15 225 304 X 212 Sag T 1 -w fat suppression post contrast 400 10 275 304 X 212 Ax T 1 -w post contrast 541 15 225 304 X 212
MRI gold standard! TR TE FOV Matrix Sag T 2 -w 3500 120 275 304 X 225 Sag T 1 -w 400 10 275 304 X 225 Sag T 2 STIR 2500 (TI=170) 70 275 256 X 190 Ax T 2 -w 4500 120 230 288 X 200 Ax T 1 -w 541 15 225 304 X 212 Sag T 1 -w fat suppression post contrast 400 10 275 304 X 212 Ax T 1 -w post contrast 541 15 225 304 X 212
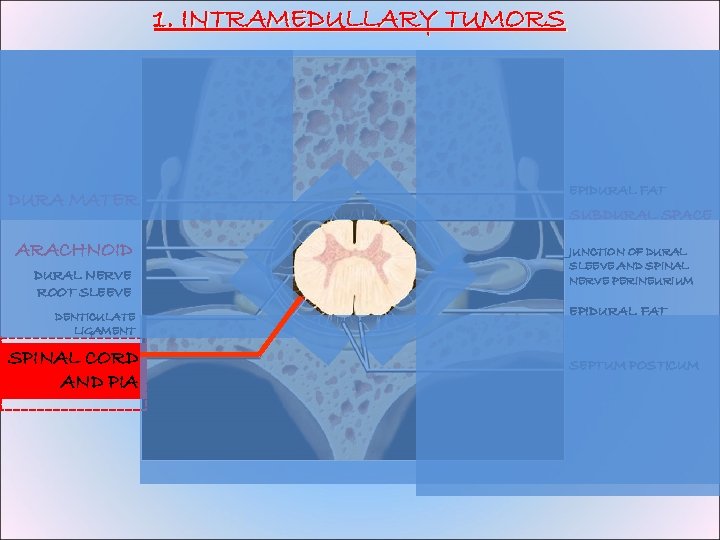 1. INTRAMEDULLARY TUMORS DURA MATER ARACHNOID DURAL NERVE ROOT SLEEVE DENTICULATE LIGAMENT SPINAL CORD AND PIA EPIDURAL FAT SUBDURAL SPACE JUNCTION OF DURAL SLEEVE AND SPINAL NERVE PERINEURIUM EPIDURAL FAT SEPTUM POSTICUM
1. INTRAMEDULLARY TUMORS DURA MATER ARACHNOID DURAL NERVE ROOT SLEEVE DENTICULATE LIGAMENT SPINAL CORD AND PIA EPIDURAL FAT SUBDURAL SPACE JUNCTION OF DURAL SLEEVE AND SPINAL NERVE PERINEURIUM EPIDURAL FAT SEPTUM POSTICUM
 Summary Three general characteristics: 1)they tend to enlarge the cord either focally or diffusely 2) on T 2 -w they produce high signal intensity 3) They enhance
Summary Three general characteristics: 1)they tend to enlarge the cord either focally or diffusely 2) on T 2 -w they produce high signal intensity 3) They enhance
 1. a. SPINAL CORD ASTROCYTOMA From astrocytes Most WHO I-II Most common in CHILDREN • 20% intraspinal neoplasms • 60% primary spinal cord tumors 80 -90% low grade üPilocitic üFibrillary subarachnoid dissemination may occur! Association with abnormalities of chromosome 17 p (TP 53 gene)
1. a. SPINAL CORD ASTROCYTOMA From astrocytes Most WHO I-II Most common in CHILDREN • 20% intraspinal neoplasms • 60% primary spinal cord tumors 80 -90% low grade üPilocitic üFibrillary subarachnoid dissemination may occur! Association with abnormalities of chromosome 17 p (TP 53 gene)
 General features A) Age: two peaks: 10 - 30 ys Demographic features: BEST DIAGNOSTIC CLUE LOCATION SIZE B) Gender: M > F (1, 3: 1); no gender difference in children! Enhancing infiltrating cord mass in child No capsule or cleavage Thoracic >Cervical > Lumbar Usually 1 -3 cm, less than 4 segments MORPHOLOGY fusiform expansion of cord, eccentric , posterior Risk in patients with Neurofibromatosis (NF 1 and NF 2)
General features A) Age: two peaks: 10 - 30 ys Demographic features: BEST DIAGNOSTIC CLUE LOCATION SIZE B) Gender: M > F (1, 3: 1); no gender difference in children! Enhancing infiltrating cord mass in child No capsule or cleavage Thoracic >Cervical > Lumbar Usually 1 -3 cm, less than 4 segments MORPHOLOGY fusiform expansion of cord, eccentric , posterior Risk in patients with Neurofibromatosis (NF 1 and NF 2)
 MR Findings T 1 -w: a) Cord expansion Usually < 4 segments Occasionally multisegmental (holocord more common with pilocytic astrocytomas) b) 40% cysts and syringohydromyelia c) Solid portion (hypo -isointense) CORD EXPANSION From Rossi et al 2007
MR Findings T 1 -w: a) Cord expansion Usually < 4 segments Occasionally multisegmental (holocord more common with pilocytic astrocytomas) b) 40% cysts and syringohydromyelia c) Solid portion (hypo -isointense) CORD EXPANSION From Rossi et al 2007
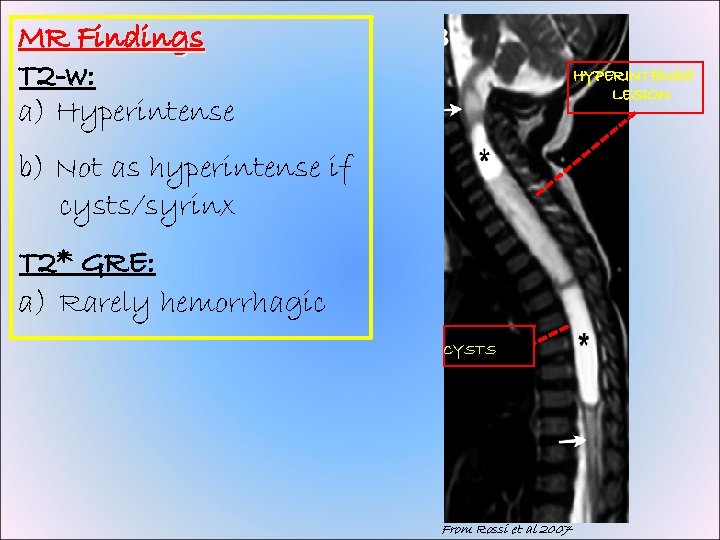 MR Findings T 2 -w: a) Hyperintense HYPERINTENSE LESION b) Not as hyperintense if cysts/syrinx T 2* GRE: a) Rarely hemorrhagic CYSTS From Rossi et al 2007
MR Findings T 2 -w: a) Hyperintense HYPERINTENSE LESION b) Not as hyperintense if cysts/syrinx T 2* GRE: a) Rarely hemorrhagic CYSTS From Rossi et al 2007
 RARELY HEMORRAGE CYSTS
RARELY HEMORRAGE CYSTS
 T 1 -w post-contrast: a) enhancement MODERATE C. E. ALWAYS!! From Rossi et al 2007
T 1 -w post-contrast: a) enhancement MODERATE C. E. ALWAYS!! From Rossi et al 2007
 DIFFERENTIAL DIAGNOSIS SARCOIDOSIS INTRAMEDULLARY EPENDYMOMA INTRAMEDULLARY HEMANGIOBLASTOMA From Baker et al 1999
DIFFERENTIAL DIAGNOSIS SARCOIDOSIS INTRAMEDULLARY EPENDYMOMA INTRAMEDULLARY HEMANGIOBLASTOMA From Baker et al 1999
 ARNOLD-CHIARI I MALFORMATION SYRINGOMYELIA
ARNOLD-CHIARI I MALFORMATION SYRINGOMYELIA
 1. b. SPINAL CORD EPENDYMOMA Cellular ependymomas (lining spinal cord central canal) Myxopapillary ependymomas (from ependymal cells of filum terminale)
1. b. SPINAL CORD EPENDYMOMA Cellular ependymomas (lining spinal cord central canal) Myxopapillary ependymomas (from ependymal cells of filum terminale)
 CELLULAR EPENDYMOMA Neoplasm of ependyma lining spinal cord central canal • Most common in ADULT (60%) in lower spine [ependymoma: 4% of all primary CNS tumors] • 2 nd most common in CHILDREN Associated with: • ESA • Superficial siderosis • NF 2 deletion or traslocation chr 22
CELLULAR EPENDYMOMA Neoplasm of ependyma lining spinal cord central canal • Most common in ADULT (60%) in lower spine [ependymoma: 4% of all primary CNS tumors] • 2 nd most common in CHILDREN Associated with: • ESA • Superficial siderosis • NF 2 deletion or traslocation chr 22
 General features A) Age: 40 yrs Demographic features: B) Gender: M: F=3: 1 C) Ethnicity: non racial predilection BEST DIAGNOSTIC CLUE LOCATION SIZE Circumscribed, enhancing cord mass with hemorrhage Conus> Cervico-Thoracic Multisegmental (typically 3 -4 segments) Well-circumscribed, symmetric cord expansion, MORPHOLOGY occasional exophytic component
General features A) Age: 40 yrs Demographic features: B) Gender: M: F=3: 1 C) Ethnicity: non racial predilection BEST DIAGNOSTIC CLUE LOCATION SIZE Circumscribed, enhancing cord mass with hemorrhage Conus> Cervico-Thoracic Multisegmental (typically 3 -4 segments) Well-circumscribed, symmetric cord expansion, MORPHOLOGY occasional exophytic component
 Radiological features MR Findings T 1 -w: a) Iso- or slightly hypointense to spinal cord b) Hemorrhage ISOHYPOINTENSE LESION
Radiological features MR Findings T 1 -w: a) Iso- or slightly hypointense to spinal cord b) Hemorrhage ISOHYPOINTENSE LESION
 Radiological features MR Findings T 2 -w: a)Hyperintense b) Polar (rostral or caudal) or intratumoral cysts (50 -90%) HEMOSIDERIN “CAP SIGN” Hemosiderin “Cap sign” c) Syrinx d) Focal hypointensity e) Surrounding cord oedema
Radiological features MR Findings T 2 -w: a)Hyperintense b) Polar (rostral or caudal) or intratumoral cysts (50 -90%) HEMOSIDERIN “CAP SIGN” Hemosiderin “Cap sign” c) Syrinx d) Focal hypointensity e) Surrounding cord oedema
 Radiological features HEMOSIDERIN “CAP SIGN” MR Findings STIR: a) Hyperintense T 1 -w post-contrast: a) Intense, welldelineated homogeneous c. e. (50%) b) Nodular, peripheral, heterogeneous c. e. c) Minimal or no c. e. rare C. E.
Radiological features HEMOSIDERIN “CAP SIGN” MR Findings STIR: a) Hyperintense T 1 -w post-contrast: a) Intense, welldelineated homogeneous c. e. (50%) b) Nodular, peripheral, heterogeneous c. e. c) Minimal or no c. e. rare C. E.
 ASTROCYTOMA EPENDYMOMA Astrocytoma cervical Eccentric posterior Infiltrative (poor borders) Ependymoma conus central hemorragic hyercellularity Pseudocapsule (plane)
ASTROCYTOMA EPENDYMOMA Astrocytoma cervical Eccentric posterior Infiltrative (poor borders) Ependymoma conus central hemorragic hyercellularity Pseudocapsule (plane)
 MYXOPAPILLARY EPENDYMOMA from ependymal cells of filum terminale ü 27 -30% of all ependymomas ü 90% of all filum terminale tumors
MYXOPAPILLARY EPENDYMOMA from ependymal cells of filum terminale ü 27 -30% of all ependymomas ü 90% of all filum terminale tumors
 Radiological features MR Findings T 1 -w: a) Usually Isointense with cord b) Hyperintensity (accumulation of mucin!) T 2 -w: a) Hyperintense b) Hypointensity at tumor margins (hemosiderin) STIR: a) Hyperintense T 1 -w post-contrast: a) Intense c. e. From Rossi et al 2007
Radiological features MR Findings T 1 -w: a) Usually Isointense with cord b) Hyperintensity (accumulation of mucin!) T 2 -w: a) Hyperintense b) Hypointensity at tumor margins (hemosiderin) STIR: a) Hyperintense T 1 -w post-contrast: a) Intense c. e. From Rossi et al 2007
 INTENSE C. E. From Rossi et al 2007
INTENSE C. E. From Rossi et al 2007
 DIFFERENTIAL DIAGNOSIS ARTERO-VENOUS FISTOLA
DIFFERENTIAL DIAGNOSIS ARTERO-VENOUS FISTOLA
 SPINAL MENINGIOMA From Rossi et al 2007 • Isointense with cord on T 1 -w and T 2 -w • More common in thoracic and cervical spine (conus and filum location unusual) • Hemorrhage uncommon • Bony changes rare
SPINAL MENINGIOMA From Rossi et al 2007 • Isointense with cord on T 1 -w and T 2 -w • More common in thoracic and cervical spine (conus and filum location unusual) • Hemorrhage uncommon • Bony changes rare
 1. c. SPINAL CORD HEMANGIOBLASTOMA Capillary rich neoplasms WHO I 1 -5% of all spinal cord neoplasms: • 75% sporadic • 25% associated with von Hippel-Lindau (VHL) • Autosomal dominant (chromosome 3 p) • Cerebellar hemangioblastomas, retinal angiomas, pheochromocytoma, renal cell carcinoma, angiomatous or cystic lesions of kidneys, pancreas and epididymis
1. c. SPINAL CORD HEMANGIOBLASTOMA Capillary rich neoplasms WHO I 1 -5% of all spinal cord neoplasms: • 75% sporadic • 25% associated with von Hippel-Lindau (VHL) • Autosomal dominant (chromosome 3 p) • Cerebellar hemangioblastomas, retinal angiomas, pheochromocytoma, renal cell carcinoma, angiomatous or cystic lesions of kidneys, pancreas and epididymis
 General features Demographic features: BEST DIAGNOSTIC CLUE LOCATION SIZE A) Age: mean age at presentation 30 ys B) Gender: M = F Intramedullary mass with serpentine “flow voids” Thoracic > Cervical Subpial (posterior, rarely anterior) often associated with intraspinal cysts Few mm to several cm MORPHOLOGY Round, well-defined margins
General features Demographic features: BEST DIAGNOSTIC CLUE LOCATION SIZE A) Age: mean age at presentation 30 ys B) Gender: M = F Intramedullary mass with serpentine “flow voids” Thoracic > Cervical Subpial (posterior, rarely anterior) often associated with intraspinal cysts Few mm to several cm MORPHOLOGY Round, well-defined margins
 Radiological features MR Findings T 1 -w: Small: a) Isointense b) Cyst!! (> 50%) Large: a) hypoisointense b) “flow voids” (lesion > 2, 5 cm) ISOHYPOINTENSE LESION + SYRINX
Radiological features MR Findings T 1 -w: Small: a) Isointense b) Cyst!! (> 50%) Large: a) hypoisointense b) “flow voids” (lesion > 2, 5 cm) ISOHYPOINTENSE LESION + SYRINX
 Radiological features MR Findings T 2 -w: a) Uniformly hyperintense (small lesions) mixed hyperintense (hemorrhage common) a) +/- peritumoral oedema b) Syrinx fluid HYPERINTENSE LESION + CYST
Radiological features MR Findings T 2 -w: a) Uniformly hyperintense (small lesions) mixed hyperintense (hemorrhage common) a) +/- peritumoral oedema b) Syrinx fluid HYPERINTENSE LESION + CYST
 Radiological features MR Findings T 1 -w post contrast: a) Subpial nodule Cyst/ Syrinx: Well-demarcated, no c. e. intense, homogeneous C. E. (often on surface of dorsal cord) SUBPIAL NODULE ON THE DORSAL SURFACE
Radiological features MR Findings T 1 -w post contrast: a) Subpial nodule Cyst/ Syrinx: Well-demarcated, no c. e. intense, homogeneous C. E. (often on surface of dorsal cord) SUBPIAL NODULE ON THE DORSAL SURFACE

 ARTERIOVENOUS MALFORMATION (AVM) CAVERNOUS MALFORMATION • Pattern of prior hemorrhage, hemosiderin rim • Minimal c. e. • Cord often normal/small, gliotic • focal nodule absent, dorsal veins prominent • M 50 -60 y insidious onset of lower extremities weakness From Chabert E et al. J Neuroradiol 1999; 26: 262 -268
ARTERIOVENOUS MALFORMATION (AVM) CAVERNOUS MALFORMATION • Pattern of prior hemorrhage, hemosiderin rim • Minimal c. e. • Cord often normal/small, gliotic • focal nodule absent, dorsal veins prominent • M 50 -60 y insidious onset of lower extremities weakness From Chabert E et al. J Neuroradiol 1999; 26: 262 -268
 Ependymoma metastasis mass centrally located Astrocytoma Crowley, Neurosurgery 2008 not hypervascular; peritumoral oedema common Renal cell carcinoma
Ependymoma metastasis mass centrally located Astrocytoma Crowley, Neurosurgery 2008 not hypervascular; peritumoral oedema common Renal cell carcinoma
 1)they tend to enlarge the cord either focally or diffusely 2) on T 2 -w they produce high signal intensity 3) They enhance
1)they tend to enlarge the cord either focally or diffusely 2) on T 2 -w they produce high signal intensity 3) They enhance
 Symptoms include pain, weakness and muscle atrophy Demylinating diseases Infections Inflammation Multiple Sclerosis ADEM Cord swelling from extramedullary infectious process (as meningitis producing vascular compromise) AIDS Sarcoid LES Syringohydromyelia Vascular lesions Causes of subacute necrotizing myelopahty Hemorrage Acute infarction Venous hypertension Cavernous angioma Arterovenous malformation ADEM Devic, MS HZV, Rubeola, Mononucleosis, mumps Toxo, TBC Lupus Spinal dural AVM Venous hypertension
Symptoms include pain, weakness and muscle atrophy Demylinating diseases Infections Inflammation Multiple Sclerosis ADEM Cord swelling from extramedullary infectious process (as meningitis producing vascular compromise) AIDS Sarcoid LES Syringohydromyelia Vascular lesions Causes of subacute necrotizing myelopahty Hemorrage Acute infarction Venous hypertension Cavernous angioma Arterovenous malformation ADEM Devic, MS HZV, Rubeola, Mononucleosis, mumps Toxo, TBC Lupus Spinal dural AVM Venous hypertension
 2. INTRADURAL EXTRAMEDULLARY TUMORS DURA MATER ARACHNOID DURAL NERVE ROOT SLEEVE DENTICULATE LIGAMENT SPINAL CORD AND PIA EPIDURAL FAT SUBDURAL SPACE JUNCTION OF DURAL SLEEVE AND SPINAL NERVE PERINEURIUM EPIDURAL FAT SEPTUM POSTICUM
2. INTRADURAL EXTRAMEDULLARY TUMORS DURA MATER ARACHNOID DURAL NERVE ROOT SLEEVE DENTICULATE LIGAMENT SPINAL CORD AND PIA EPIDURAL FAT SUBDURAL SPACE JUNCTION OF DURAL SLEEVE AND SPINAL NERVE PERINEURIUM EPIDURAL FAT SEPTUM POSTICUM
 Schwannoma, Neurinoma üArise from single nerve, from one side ü Typically dorsal root ü Schwann cells üDo NOT envelope the adiacent nerve root üLobulated üSingle Neurofibroma üSchwann cells and fibroblasts between dispersed nerve fibers, mps matrix üSpreads apart axons üDO envelope the adiacent nerve root üFusiform üMultiple
Schwannoma, Neurinoma üArise from single nerve, from one side ü Typically dorsal root ü Schwann cells üDo NOT envelope the adiacent nerve root üLobulated üSingle Neurofibroma üSchwann cells and fibroblasts between dispersed nerve fibers, mps matrix üSpreads apart axons üDO envelope the adiacent nerve root üFusiform üMultiple
 2. a. SCHWANNOMA Neoplasm of nerve sheath in PNS üMost common WHO grade I intradural extramedullary mass ü 30% primary spinal tumors • Mostly sporadic (inactivation of NF 2 gene) • Association with NF 2, bilateral multiple
2. a. SCHWANNOMA Neoplasm of nerve sheath in PNS üMost common WHO grade I intradural extramedullary mass ü 30% primary spinal tumors • Mostly sporadic (inactivation of NF 2 gene) • Association with NF 2, bilateral multiple
 General features A) Age: 40 ys Demographic features: B) Gender: M = F C) Ethnicity: no racial predilection BEST DIAGNOSTIC CLUE Well-circumscribed, “dumbbell” shaped, enhancing spinal mass Thoracic > Cervical = Lumbar LOCATION 70 -75% intradural extramedullary 15% completely extradural 15% “dumbbell” (both intra- and extradural) SIZE Few mm Giant schwannoma: > 2 vertebral segments MORPHOLOGY Round, lobulated
General features A) Age: 40 ys Demographic features: B) Gender: M = F C) Ethnicity: no racial predilection BEST DIAGNOSTIC CLUE Well-circumscribed, “dumbbell” shaped, enhancing spinal mass Thoracic > Cervical = Lumbar LOCATION 70 -75% intradural extramedullary 15% completely extradural 15% “dumbbell” (both intra- and extradural) SIZE Few mm Giant schwannoma: > 2 vertebral segments MORPHOLOGY Round, lobulated
 Radiological features T 1 -w: Isointense ISOINTENSE LESION T 2 -w: a) hyperintense b) 45%cyst 10% hemorrage c) “Target sign” HYPERINTENSE LESION WITH TARGET SIGN
Radiological features T 1 -w: Isointense ISOINTENSE LESION T 2 -w: a) hyperintense b) 45%cyst 10% hemorrage c) “Target sign” HYPERINTENSE LESION WITH TARGET SIGN
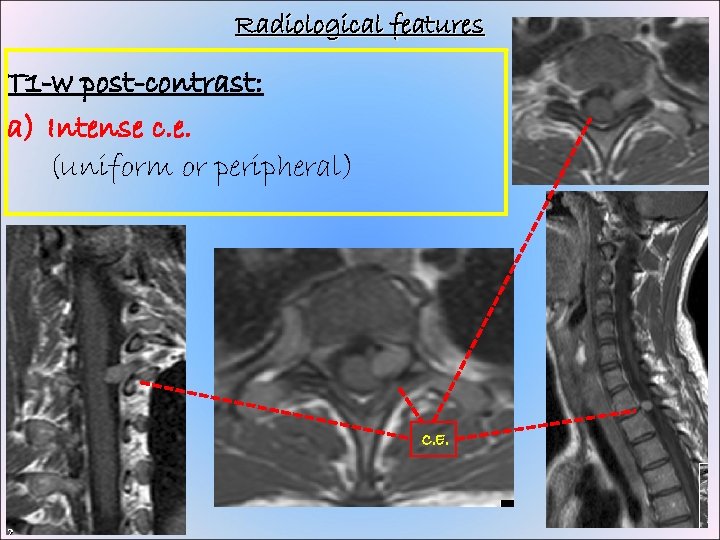 Radiological features T 1 -w post-contrast: a) Intense c. e. (uniform or peripheral) C. E.
Radiological features T 1 -w post-contrast: a) Intense c. e. (uniform or peripheral) C. E.
 2. b. NEUROFIBROMA Localized, diffuse or plexiform neoplasm of nerve sheath WHO grade III/IV • 5% of all benign soft tissue tumors • Association with neurofibromatosis 1 (NF 1) 13 -65% have spinal neurofibromas
2. b. NEUROFIBROMA Localized, diffuse or plexiform neoplasm of nerve sheath WHO grade III/IV • 5% of all benign soft tissue tumors • Association with neurofibromatosis 1 (NF 1) 13 -65% have spinal neurofibromas

 ISOINTENSE LESION HYPERINTENSE LESION + HYPOINTENSE SEPTATIONS C. E.
ISOINTENSE LESION HYPERINTENSE LESION + HYPOINTENSE SEPTATIONS C. E.
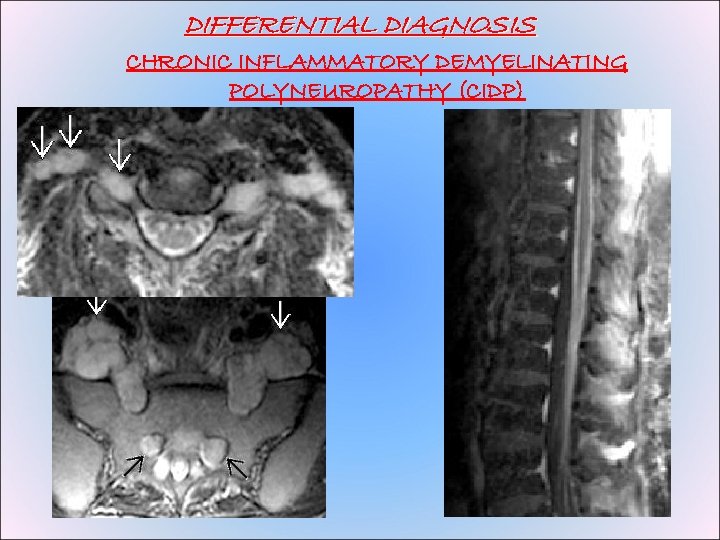 DIFFERENTIAL DIAGNOSIS CHRONIC INFLAMMATORY DEMYELINATING POLYNEUROPATHY (CIDP)
DIFFERENTIAL DIAGNOSIS CHRONIC INFLAMMATORY DEMYELINATING POLYNEUROPATHY (CIDP)
 2. c. MENINGIOMA Origin from arachnoid Attached to the dura mater for infiltration SECOND MOST COMMON INTRADURAL EXTRAMEDULLARY TUMOR > 25% WHO I üMeningothelial üFibroblastic üPsammomatous üangiomatous ü Genetic predisposition in women! • Almost all have chromosome 22 abnormalities • Association with neurofibromatosis 2 (NF 2) üSolitary
2. c. MENINGIOMA Origin from arachnoid Attached to the dura mater for infiltration SECOND MOST COMMON INTRADURAL EXTRAMEDULLARY TUMOR > 25% WHO I üMeningothelial üFibroblastic üPsammomatous üangiomatous ü Genetic predisposition in women! • Almost all have chromosome 22 abnormalities • Association with neurofibromatosis 2 (NF 2) üSolitary
 General features Demographic features: BEST DIAGNOSTIC CLUE LOCATION SIZE A) Age: 50 -60 yrs B) Gender: F: M=4: 1 (>70 -80% female!) Enhancing intradural extramedullary mass with “dural tail” Thoracic (80%)>> Cervical (16%) > Lumbar (4%) Typical intradural extramedullary Posterolateral (anterior cervical) Variable MORPHOLOGY Typically round with dural attachment, Ca ++ < 5%
General features Demographic features: BEST DIAGNOSTIC CLUE LOCATION SIZE A) Age: 50 -60 yrs B) Gender: F: M=4: 1 (>70 -80% female!) Enhancing intradural extramedullary mass with “dural tail” Thoracic (80%)>> Cervical (16%) > Lumbar (4%) Typical intradural extramedullary Posterolateral (anterior cervical) Variable MORPHOLOGY Typically round with dural attachment, Ca ++ < 5%
 Radiological features ISOINTENSE LESION WITH CALCIFICATION MR Findings T 1 -w: a) Isointense T 2 -w: b) Iso- hyperintense c) Hypointense (calcification)
Radiological features ISOINTENSE LESION WITH CALCIFICATION MR Findings T 1 -w: a) Isointense T 2 -w: b) Iso- hyperintense c) Hypointense (calcification)
 Radiological features C. E. T 1 -w post-contrast: a) Prominent c. e. b) May see enhancing “dural tail”
Radiological features C. E. T 1 -w post-contrast: a) Prominent c. e. b) May see enhancing “dural tail”
 Differential diagnosis NEURINOMA üMore anterior üVery hyperintense on T 2 -w with Target sign üCystic change, hemorrhage more common üNo dural attachment ü more frequent enlargment of neural foramen
Differential diagnosis NEURINOMA üMore anterior üVery hyperintense on T 2 -w with Target sign üCystic change, hemorrhage more common üNo dural attachment ü more frequent enlargment of neural foramen
 DROP METASTASIS
DROP METASTASIS
 3. EXTRADURAL TUMORS DURA MATER ARACHNOID DURAL NERVE ROOT SLEEVE DENTICULATE LIGAMENT SPINAL CORD AND PIA EPIDURAL FAT SUBDURAL SPACE JUNCTION OF DURAL SLEEVE AND SPINAL NERVE PERINEURIUM EPIDURAL FAT SEPTUM POSTICUM
3. EXTRADURAL TUMORS DURA MATER ARACHNOID DURAL NERVE ROOT SLEEVE DENTICULATE LIGAMENT SPINAL CORD AND PIA EPIDURAL FAT SUBDURAL SPACE JUNCTION OF DURAL SLEEVE AND SPINAL NERVE PERINEURIUM EPIDURAL FAT SEPTUM POSTICUM
 METASTASIS LYMPHOMA Female (breast and lung) Male (prostate and lung) Thoracic (70%)> lumbar (20%) > cervical (10%) From Thurner et al.
METASTASIS LYMPHOMA Female (breast and lung) Male (prostate and lung) Thoracic (70%)> lumbar (20%) > cervical (10%) From Thurner et al.
 DROP METASTASIS
DROP METASTASIS
 DIFFERENTIAL DIAGNOSIS ANGIOMIOLIPOMA
DIFFERENTIAL DIAGNOSIS ANGIOMIOLIPOMA
 DIFFERENTIAL DIAGNOSIS GRANULOMATOSIS
DIFFERENTIAL DIAGNOSIS GRANULOMATOSIS
 INTRADURAL ARACHNOID CYST EPIDURAL EMATOMA
INTRADURAL ARACHNOID CYST EPIDURAL EMATOMA
 Grazie per l’attenzione
Grazie per l’attenzione


