3eac85a91b274e1b7887c15b92042561.ppt
- Количество слайдов: 167
 Patient versus Professional Autonomy: So Whose Life is it Anyway? Dennise Krencicki, PT, DPT, MA APTANJ January 2014
Patient versus Professional Autonomy: So Whose Life is it Anyway? Dennise Krencicki, PT, DPT, MA APTANJ January 2014
 Course Objectives Explore various roles of health care professionals relating to health care decision-making and its impact on patient autonomy Discuss potential areas of conflict within decisionmaking locus of authority Identify and discuss issues of patient competence, cultural competency and informed consent on patient decision making Analyze, using the RIPS Model, case scenarios to allow participants to explore ethical problems relating to patient versus health care practitioner autonomy
Course Objectives Explore various roles of health care professionals relating to health care decision-making and its impact on patient autonomy Discuss potential areas of conflict within decisionmaking locus of authority Identify and discuss issues of patient competence, cultural competency and informed consent on patient decision making Analyze, using the RIPS Model, case scenarios to allow participants to explore ethical problems relating to patient versus health care practitioner autonomy
 Review methods to access the NJ Physical Therapy Practice Act and related documents
Review methods to access the NJ Physical Therapy Practice Act and related documents
 But before we do that Let’s review the RIPS Model
But before we do that Let’s review the RIPS Model
 The RIPS Model Realm Individual Process Issue or problem Individual (relationship between individuals) Organizational/Institution al (good of the organization) Societal (Common good) Ethical Situation Moral Sensitivity (recognize there is a situation) Moral Judgment (right or wrong) Moral Motivation (moral values above other values) Moral Courage (implement action) (values are challenged) Distress (Right course of action blocked by a barrier) Dilemma (right vs. right decision) Temptation (right vs. . wrong situation) Silence (values are challenged but no one is addressing it), Kirsch 5
The RIPS Model Realm Individual Process Issue or problem Individual (relationship between individuals) Organizational/Institution al (good of the organization) Societal (Common good) Ethical Situation Moral Sensitivity (recognize there is a situation) Moral Judgment (right or wrong) Moral Motivation (moral values above other values) Moral Courage (implement action) (values are challenged) Distress (Right course of action blocked by a barrier) Dilemma (right vs. right decision) Temptation (right vs. . wrong situation) Silence (values are challenged but no one is addressing it), Kirsch 5
 Realm-Individual Process-Situation (RIPS) Model of Ethical Decision Making Step I: Recognize and define the ethical issues Realm Individual Process Situation Swisher, Nordrum, Kirsch, 2009 6
Realm-Individual Process-Situation (RIPS) Model of Ethical Decision Making Step I: Recognize and define the ethical issues Realm Individual Process Situation Swisher, Nordrum, Kirsch, 2009 6
 Realm Individual - between individuals Organizational - good of the organization Societal - common good Swisher, Nordrum, Kirsch, 2009 7
Realm Individual - between individuals Organizational - good of the organization Societal - common good Swisher, Nordrum, Kirsch, 2009 7
 Individual Processes Moral Sensitivity- recognize a situation exists Moral Judgment- judge between right and wrong Moral Motivation- moral values above other values Moral Courage – implement action Swisher, Nordrum, Kirsch, 2009 8
Individual Processes Moral Sensitivity- recognize a situation exists Moral Judgment- judge between right and wrong Moral Motivation- moral values above other values Moral Courage – implement action Swisher, Nordrum, Kirsch, 2009 8
 Situation Issue or problem Dilemma Distress Temptation Silence Swisher, Nordrum, Kirsch, 2009 9
Situation Issue or problem Dilemma Distress Temptation Silence Swisher, Nordrum, Kirsch, 2009 9
 Problems / Challenges Presents challenges or threats to moral duties and values Causes need for reflection on course of action Questions of conduct Relatively straightforward Temporary Readily resolvable Kirsch (2003) 10
Problems / Challenges Presents challenges or threats to moral duties and values Causes need for reflection on course of action Questions of conduct Relatively straightforward Temporary Readily resolvable Kirsch (2003) 10
 Ethical Distress Know which course of action should take, but there is a structural barrier
Ethical Distress Know which course of action should take, but there is a structural barrier
 Ethical Dilemma Between a rock and a hard place
Ethical Dilemma Between a rock and a hard place
 Ethical Dilemma Two values conflict There is more than one course of action, each of which is right or wrong. No matter choice, something of value is compromised Act on one – the other eliminated Between the devil and the deep blue sea
Ethical Dilemma Two values conflict There is more than one course of action, each of which is right or wrong. No matter choice, something of value is compromised Act on one – the other eliminated Between the devil and the deep blue sea
 Dilemmas fall into broad patterns Truth versus Loyalty Individual versus Community Short Term versus Long Term Justice versus Mercy Kidder(2005)
Dilemmas fall into broad patterns Truth versus Loyalty Individual versus Community Short Term versus Long Term Justice versus Mercy Kidder(2005)
 Truth versus Loyalty “Honesty or integrity versus Commitment, responsibility , or promise-keeping” Kidder (2005)
Truth versus Loyalty “Honesty or integrity versus Commitment, responsibility , or promise-keeping” Kidder (2005)
 Individual vs Community “Us versus them Self versus others Smaller versus the larger group” Kidder (2005)
Individual vs Community “Us versus them Self versus others Smaller versus the larger group” Kidder (2005)
 Short Term versus Long Term “Now versus then” “Reflects difficulties arising when immediate needs or desires run counter to future goals or prospects” Kidder (2005)
Short Term versus Long Term “Now versus then” “Reflects difficulties arising when immediate needs or desires run counter to future goals or prospects” Kidder (2005)
 Justice versus Mercy “fairness, equity, and even-handed application of the law often conflict with compassion, empathy and love. ” Kidder (2005)
Justice versus Mercy “fairness, equity, and even-handed application of the law often conflict with compassion, empathy and love. ” Kidder (2005)
 Temptation “Choice between right and a wrong and in which you may stand to profit from doing the wrong thing: Swisher, et al (2005) 19
Temptation “Choice between right and a wrong and in which you may stand to profit from doing the wrong thing: Swisher, et al (2005) 19
 Silence “Ethical values are challenged but no one is speaking about this challenge to values. ” Swisher et al (2005) 20
Silence “Ethical values are challenged but no one is speaking about this challenge to values. ” Swisher et al (2005) 20
 Step II What are the relevant facts and contextual information? Who are the major stakeholders? What are the possible consequences (intended and unintended)? What are the relevant laws, duties, obligations, and ethical principles? What professional resources speak to this situation? Are any of the five tests for right versus wrong situation positive (legal test, stench test, front-page test, Mom test, professional ethics test)? Swisher, Nordrum, Kirsch, 2009 21
Step II What are the relevant facts and contextual information? Who are the major stakeholders? What are the possible consequences (intended and unintended)? What are the relevant laws, duties, obligations, and ethical principles? What professional resources speak to this situation? Are any of the five tests for right versus wrong situation positive (legal test, stench test, front-page test, Mom test, professional ethics test)? Swisher, Nordrum, Kirsch, 2009 21
 Step III – Decide the right think to do Approach to resolve issue: Rule-based- follow the rules, duties, obligations, or ethical principles already in place Ends-based- determine the consequences or outcomes of alternative actions and the good or harm that will result for all of the stakeholders Care-based- resolve dilemmas according relationships and concern for others Swisher, Nordrum, Kirsch, 2009 22
Step III – Decide the right think to do Approach to resolve issue: Rule-based- follow the rules, duties, obligations, or ethical principles already in place Ends-based- determine the consequences or outcomes of alternative actions and the good or harm that will result for all of the stakeholders Care-based- resolve dilemmas according relationships and concern for others Swisher, Nordrum, Kirsch, 2009 22
 the ethical approach used to solve a dilemma can change the conclusion reached
the ethical approach used to solve a dilemma can change the conclusion reached
 Heinz Dilemma Heinz Steals the Drug In Europe, a woman was near death from a special kind of cancer. There was one drug that the doctors thought might save her. It was a form of radium that a druggist in the same town had recently discovered. The drug was expensive to make, but the druggist was charging ten times what the drug cost him to make. He paid $200 for the radium and charged $2, 000 for a small dose of the drug. The sick woman's husband, Heinz, went to everyone he knew to borrow the money, but he could only get together about $ 1, 000 which is half of what it cost. He told the druggist that his wife was dying and asked him to sell it cheaper or let him pay later. But the druggist said: "No, I discovered the drug and I'm going to make money from it. " So Heinz got desperate and broke into the man's store to steal the drug-for his wife. Should the husband have done that? (Kohlberg, 1963) W. C. Crain (1985) Theories of Development. Prentice-Hall. Pgs 118 -136 Accessed at http: //faculty. plts. edu/gpence/html/kohlberg. htm
Heinz Dilemma Heinz Steals the Drug In Europe, a woman was near death from a special kind of cancer. There was one drug that the doctors thought might save her. It was a form of radium that a druggist in the same town had recently discovered. The drug was expensive to make, but the druggist was charging ten times what the drug cost him to make. He paid $200 for the radium and charged $2, 000 for a small dose of the drug. The sick woman's husband, Heinz, went to everyone he knew to borrow the money, but he could only get together about $ 1, 000 which is half of what it cost. He told the druggist that his wife was dying and asked him to sell it cheaper or let him pay later. But the druggist said: "No, I discovered the drug and I'm going to make money from it. " So Heinz got desperate and broke into the man's store to steal the drug-for his wife. Should the husband have done that? (Kohlberg, 1963) W. C. Crain (1985) Theories of Development. Prentice-Hall. Pgs 118 -136 Accessed at http: //faculty. plts. edu/gpence/html/kohlberg. htm
 Step IV: Implement, evaluate, re-assess What did you as a professional learn from this situation? What are your strengths and weaknesses in terms of the four individual processes? Is there a need to plan professional activities to grow in moral sensitivity, judgment, motivation, or courage? Swisher, Nordrum, Kirsch, 2009 25
Step IV: Implement, evaluate, re-assess What did you as a professional learn from this situation? What are your strengths and weaknesses in terms of the four individual processes? Is there a need to plan professional activities to grow in moral sensitivity, judgment, motivation, or courage? Swisher, Nordrum, Kirsch, 2009 25
 Health Care Principles Autonomy Beneficence Nonmaleficence Justice
Health Care Principles Autonomy Beneficence Nonmaleficence Justice
 Ethics of health care provider /patient relationships are historically rooted in the ethical principles of Beneficence Nonmaleficence Physician knows best – paternalism (Clawson, 1994)
Ethics of health care provider /patient relationships are historically rooted in the ethical principles of Beneficence Nonmaleficence Physician knows best – paternalism (Clawson, 1994)
 Paternalism Occurs when one fails to respect another’s autonomy and acts with disregard that individual rights. Substitute own beliefs, opinions and judgment for the patients’ Justify by saying that they acted in best interest of the patient - beneficence
Paternalism Occurs when one fails to respect another’s autonomy and acts with disregard that individual rights. Substitute own beliefs, opinions and judgment for the patients’ Justify by saying that they acted in best interest of the patient - beneficence
 Shift from paternalism toward respect for patient autonomy as core value in physicianpatient relationship
Shift from paternalism toward respect for patient autonomy as core value in physicianpatient relationship
 Autonomy Personal self-determination Moral right to make choices and decisions about one’s own course of action Considered by some as the principle to follow when no other is clearly applicable 1891 US Supreme Court “no right is held more sacred, or is more carefully guarded by the common law, than the right of every individual to the possession and control of his (or her) own person, free from all restraint or interference of others, unless by clear and unquestionable authority of law. ” As quoted in Miller, R. Problems in Health Care Law. Ninth Ed. Jones and Bartlett, Sudbury MA
Autonomy Personal self-determination Moral right to make choices and decisions about one’s own course of action Considered by some as the principle to follow when no other is clearly applicable 1891 US Supreme Court “no right is held more sacred, or is more carefully guarded by the common law, than the right of every individual to the possession and control of his (or her) own person, free from all restraint or interference of others, unless by clear and unquestionable authority of law. ” As quoted in Miller, R. Problems in Health Care Law. Ninth Ed. Jones and Bartlett, Sudbury MA
 Conflicting Authorities Physician vs. Other HC Providers vs. HC Providers HC Provider vs. Patients HC Provider vs. Administration HC Provider vs. Insurance Carrier Family member vs. family member Patient vs. family member 32
Conflicting Authorities Physician vs. Other HC Providers vs. HC Providers HC Provider vs. Patients HC Provider vs. Administration HC Provider vs. Insurance Carrier Family member vs. family member Patient vs. family member 32
 Patient versus Practitioner Autonomy
Patient versus Practitioner Autonomy
 Contexts Therapeutic relationship dedicated to fostering health and best interests of patient Roberts, LW. www. medscape. com/viewarticle/460483 Downloaded April 7, 2010
Contexts Therapeutic relationship dedicated to fostering health and best interests of patient Roberts, LW. www. medscape. com/viewarticle/460483 Downloaded April 7, 2010
 Patient Autonomy Informed consent Requires that competent individual is encouraged to actively participate in planning and selection of activities that affect their care 35
Patient Autonomy Informed consent Requires that competent individual is encouraged to actively participate in planning and selection of activities that affect their care 35
 What is informed consent? Informed consent is the process by which a fully informed patient can participate in choices about her health care. It originates from the legal and ethical right the patient has to direct what happens to her body and from the ethical duty of the physician to involve the patient in her health care. http: //depts. washington. edu/bioethx/topics/consent. html
What is informed consent? Informed consent is the process by which a fully informed patient can participate in choices about her health care. It originates from the legal and ethical right the patient has to direct what happens to her body and from the ethical duty of the physician to involve the patient in her health care. http: //depts. washington. edu/bioethx/topics/consent. html
 Informed Consent Directly related to autonomy, as stated By Caplan: “the doctrine that had emerged as the guarantee of individual patient autonomy…is informed consent. Patients have the absolute right to make informed choices about the kind and degree of care they wish to receive: (Caplan, et al, 1987) (Clawson, 1994)
Informed Consent Directly related to autonomy, as stated By Caplan: “the doctrine that had emerged as the guarantee of individual patient autonomy…is informed consent. Patients have the absolute right to make informed choices about the kind and degree of care they wish to receive: (Caplan, et al, 1987) (Clawson, 1994)
 How do you provide informed consent to your patients? What do you include?
How do you provide informed consent to your patients? What do you include?
 Informed Consent World Confederation for Physical Therapy states: “Competent individuals should be provided with adequate, intelligible information about the proposed physical therapy. This information should include a clear explanation of: the planned examination/assessment the evaluation, diagnosis, and prognosis/plan the intervention/treatment to be provided
Informed Consent World Confederation for Physical Therapy states: “Competent individuals should be provided with adequate, intelligible information about the proposed physical therapy. This information should include a clear explanation of: the planned examination/assessment the evaluation, diagnosis, and prognosis/plan the intervention/treatment to be provided
 Informed Consent the risks which may be associated with the intervention the expected benefits of the intervention the anticipated time frames the anticipated costs any reasonable alternatives to the recommended intervention http: //www. wcpt. org/policy/ps-consent accessed 9 -28 -11
Informed Consent the risks which may be associated with the intervention the expected benefits of the intervention the anticipated time frames the anticipated costs any reasonable alternatives to the recommended intervention http: //www. wcpt. org/policy/ps-consent accessed 9 -28 -11
 Elements of Informed Consent the nature of the decision/procedure reasonable alternatives to the proposed intervention the relevant risks, benefits, and uncertainties related to each alternative assessment of patient understanding the acceptance of the intervention by the patient http: //depts. washington. edu/bioethx/topics/consent. html
Elements of Informed Consent the nature of the decision/procedure reasonable alternatives to the proposed intervention the relevant risks, benefits, and uncertainties related to each alternative assessment of patient understanding the acceptance of the intervention by the patient http: //depts. washington. edu/bioethx/topics/consent. html
 Issues in Informed Consent Oral vs. written How much information to give Patient competence Who decides if patient incompetent (Clawson , 1994)
Issues in Informed Consent Oral vs. written How much information to give Patient competence Who decides if patient incompetent (Clawson , 1994)
 Determination of Ability to Give Informed Consent Legal capacity standards vary across jurisdictions Competence – Clinical judgment by provider of patient’s ability to give informed consent Not necessarily function of psychiatrist In most states, presumption of continued competence If disagree, must prove otherwise Direction by patients when they have decision making capacity should be followed after they lose capacity
Determination of Ability to Give Informed Consent Legal capacity standards vary across jurisdictions Competence – Clinical judgment by provider of patient’s ability to give informed consent Not necessarily function of psychiatrist In most states, presumption of continued competence If disagree, must prove otherwise Direction by patients when they have decision making capacity should be followed after they lose capacity
 Decision Making Capacity In US, individuals are adults for most purposes on 18 th birthday Able to make own medical decisions Able to make decisions Not declared incompetent by court Capable of understanding consequences or alternatives NOT the degree to which it agrees with provider’s recommendations Miller, Problems in Health Care Law
Decision Making Capacity In US, individuals are adults for most purposes on 18 th birthday Able to make own medical decisions Able to make decisions Not declared incompetent by court Capable of understanding consequences or alternatives NOT the degree to which it agrees with provider’s recommendations Miller, Problems in Health Care Law
 Capacity To Consent for Treatment Generally include “Abilities to communicate a choice” “Understand relevant information” “Appreciate medical consequences” “Reason about treatment choices” In question, generally decided in court Appelbaum, P. S. “Assessment of patients’ competence to consent to treatment. ” NEJM 357: 18, pages 1834 -1840.
Capacity To Consent for Treatment Generally include “Abilities to communicate a choice” “Understand relevant information” “Appreciate medical consequences” “Reason about treatment choices” In question, generally decided in court Appelbaum, P. S. “Assessment of patients’ competence to consent to treatment. ” NEJM 357: 18, pages 1834 -1840.
 Mental Capacity Pelligrino 1. Can communicate 2. Able to understand comprehend gravity of situation 3. Able to make decision which is reasoned Follow from set of values
Mental Capacity Pelligrino 1. Can communicate 2. Able to understand comprehend gravity of situation 3. Able to make decision which is reasoned Follow from set of values
 4. Patient must persist in decision for a reasonable amount of time 5. Must be authentic In keeping with previous lifestyle and decisions Can change mind
4. Patient must persist in decision for a reasonable amount of time 5. Must be authentic In keeping with previous lifestyle and decisions Can change mind
 Patient’s Clinical Competence Exception: Dementia Depression Unsound mind Under age Not legal definition
Patient’s Clinical Competence Exception: Dementia Depression Unsound mind Under age Not legal definition
 Adolescents and Consent Legal/ age of majority in NJ – 18 years Vote Jury Military Marry Consent to medical treatment 17 years of age - drive 21 years of age – drinking age
Adolescents and Consent Legal/ age of majority in NJ – 18 years Vote Jury Military Marry Consent to medical treatment 17 years of age - drive 21 years of age – drinking age
 Rights of Minors in NJ Consent to any medical treatment Are or ever have been married Who are parents (both for their own and for their children’s care In military service Emancipated http: //www. aclu-nj. org/downloads/2008 minorsrights. pdf
Rights of Minors in NJ Consent to any medical treatment Are or ever have been married Who are parents (both for their own and for their children’s care In military service Emancipated http: //www. aclu-nj. org/downloads/2008 minorsrights. pdf
 Without parental consent Receive family planning services and contraceptives Emergency contraception Pregnancy testing Prenatal care HIV testing and treatment STD testing and treatment Treatment for drug use or dependency Alcohol dependency http: //www. aclu-nj. org/downloads/2008 minorsrights. pdf
Without parental consent Receive family planning services and contraceptives Emergency contraception Pregnancy testing Prenatal care HIV testing and treatment STD testing and treatment Treatment for drug use or dependency Alcohol dependency http: //www. aclu-nj. org/downloads/2008 minorsrights. pdf
 Making Your Wishes Known Advanced Directives Living Wills Special Health Care Power of Attorney DNR Orders POLST
Making Your Wishes Known Advanced Directives Living Wills Special Health Care Power of Attorney DNR Orders POLST
 Advanced Directive Legal document Written directions prepared in advance that states what medical care you want in the event you become unable to make decisions for yourself (Advanced Directives for Health Care; a publication of the State of NJ Commission of Legal and Ethical Problems in the Delivery of Health Care, © 1991)
Advanced Directive Legal document Written directions prepared in advance that states what medical care you want in the event you become unable to make decisions for yourself (Advanced Directives for Health Care; a publication of the State of NJ Commission of Legal and Ethical Problems in the Delivery of Health Care, © 1991)
 Three Kinds of Advanced Directives Proxy Directives – designates a person and gives them the legal authority to make decisions for you when you cannot – Power of Attorney for Health Care Instruction Directives – statement of your medical treatment preferences – Living will Combined Directives – single document combining both proxy and instruction directives (Advanced Directives for Health Care; a publication of the State of NJ Commission of Legal and Ethical Problems in the Delivery of Health Care, © 1991)
Three Kinds of Advanced Directives Proxy Directives – designates a person and gives them the legal authority to make decisions for you when you cannot – Power of Attorney for Health Care Instruction Directives – statement of your medical treatment preferences – Living will Combined Directives – single document combining both proxy and instruction directives (Advanced Directives for Health Care; a publication of the State of NJ Commission of Legal and Ethical Problems in the Delivery of Health Care, © 1991)
 Living Wills Explains the care you do or do not want CPR Feeding Ventilator Test, medicines, surgery Blood Transfusion (Medline. Plus - Advanced Directives)
Living Wills Explains the care you do or do not want CPR Feeding Ventilator Test, medicines, surgery Blood Transfusion (Medline. Plus - Advanced Directives)
 Do Not Resuscitate Request not to have Cardiopulmonary resuscitation Two general situations arise which justify withholding CPR: when CPR is judged to be of no medical benefit - also known as "medical futility“ Patient/designee decides http: //depts. washington. edu/bioethx/topics/dnr. html
Do Not Resuscitate Request not to have Cardiopulmonary resuscitation Two general situations arise which justify withholding CPR: when CPR is judged to be of no medical benefit - also known as "medical futility“ Patient/designee decides http: //depts. washington. edu/bioethx/topics/dnr. html
 NJ Advanced Directives for Health Care Act N. J. Stat 26: 2 H-53 (2009) Right to control decisions about own health care should not be lost if unable to participate Right to life-sustaining measures not absolute Societal interest in preserving human life preserving life of individual patient preserving sanctity of all human life as enduring social value Protection of individuals from direct and purposeful self destruction Protection of innocent third parties who may be harmed by patient’s decision Rejects on moral and legal grounds active euthanasia
NJ Advanced Directives for Health Care Act N. J. Stat 26: 2 H-53 (2009) Right to control decisions about own health care should not be lost if unable to participate Right to life-sustaining measures not absolute Societal interest in preserving human life preserving life of individual patient preserving sanctity of all human life as enduring social value Protection of individuals from direct and purposeful self destruction Protection of innocent third parties who may be harmed by patient’s decision Rejects on moral and legal grounds active euthanasia
 POLST Practitioner Orders for Life-Sustaining Treatment “A set of medical orders that help give seriously ill or frail elderly patients more control over their end –of life- care Specifies the types of medical treatment that a patient wishes to receive Complements an Advanced Directive , is not intended to replace it
POLST Practitioner Orders for Life-Sustaining Treatment “A set of medical orders that help give seriously ill or frail elderly patients more control over their end –of life- care Specifies the types of medical treatment that a patient wishes to receive Complements an Advanced Directive , is not intended to replace it
 POLST Includes: Goals of care Preferences regarding CPR Preferences regarding use of intubation and mechanical ventilation for respiratory failure Preferences for artificially administered nutrition and hydration Other specific medical interventions that are desired or declined
POLST Includes: Goals of care Preferences regarding CPR Preferences regarding use of intubation and mechanical ventilation for respiratory failure Preferences for artificially administered nutrition and hydration Other specific medical interventions that are desired or declined
 Differences Between Advanced Directive and POLST Advanced Directive Not a medical Order Communicates treatment preferences and designates proxy Recommended for all adults with decision making capacity POLST Is a medical Order Reflects individual’s goals of care and wishes for care at end of life and transforms them into actionable orders that must be followed Recommends for individuals with advances illness, frailty or strong preference about metical intervention
Differences Between Advanced Directive and POLST Advanced Directive Not a medical Order Communicates treatment preferences and designates proxy Recommended for all adults with decision making capacity POLST Is a medical Order Reflects individual’s goals of care and wishes for care at end of life and transforms them into actionable orders that must be followed Recommends for individuals with advances illness, frailty or strong preference about metical intervention
 Professional Autonomy
Professional Autonomy
 Professional Autonomy R. Sandstrom(2007) Physical Therapy 87(1), 98 -110 “Professional autonomy , or the ability to control the conditions of one’s work” Social contract based on public trust “is an outcome of a trust relationship established between a profession and the society” Privilege Advocate Patient Society
Professional Autonomy R. Sandstrom(2007) Physical Therapy 87(1), 98 -110 “Professional autonomy , or the ability to control the conditions of one’s work” Social contract based on public trust “is an outcome of a trust relationship established between a profession and the society” Privilege Advocate Patient Society
 can be weakened and limited by relationship with another profession, other social institutions and internal disposition of profession itself PT autonomy has increased as medical dominance declined (Sandstrom, 2007)
can be weakened and limited by relationship with another profession, other social institutions and internal disposition of profession itself PT autonomy has increased as medical dominance declined (Sandstrom, 2007)
 Autonomous Practice J. Rothstein(2002) Physical Therapy 82(8), 750 -751 Direct and unrestricted access Ability to refer to other HC providers Ability to refer to other professionals Ability to refer for diagnostic tests
Autonomous Practice J. Rothstein(2002) Physical Therapy 82(8), 750 -751 Direct and unrestricted access Ability to refer to other HC providers Ability to refer to other professionals Ability to refer for diagnostic tests
 Autonomous Physical Therapist Practice HOD P 06 -06 -18 -11 Physical Therapists have the responsibility to practice autonomously in all settings, practice environments and employment relationships. Autonomous physical therapist practice is characterized by: 65
Autonomous Physical Therapist Practice HOD P 06 -06 -18 -11 Physical Therapists have the responsibility to practice autonomously in all settings, practice environments and employment relationships. Autonomous physical therapist practice is characterized by: 65
 Independent, self determined professional judgment within one’s scope of practice, consistent with the profession's Codes and Standards and in the patient's /client’s best interest Responsibility and acceptance of risk for all aspects of the physical therapist patient /client management 66
Independent, self determined professional judgment within one’s scope of practice, consistent with the profession's Codes and Standards and in the patient's /client’s best interest Responsibility and acceptance of risk for all aspects of the physical therapist patient /client management 66
 Ability to refer and collaborate with health care providers and other to enhance the physical therapist patient / client management Recognition of circumstances that necessitate a request for consultation and initiation of such consultation when in the best interest of the patient / client 67
Ability to refer and collaborate with health care providers and other to enhance the physical therapist patient / client management Recognition of circumstances that necessitate a request for consultation and initiation of such consultation when in the best interest of the patient / client 67
 Clinical decision making independent of external financial considerations Physical therapist governance and control of physical therapy practice in all settings
Clinical decision making independent of external financial considerations Physical therapist governance and control of physical therapy practice in all settings
 WHAT IS IT NOT? Independent Alone Unaligned with other health care practitioners Maybe it is the wrong word
WHAT IS IT NOT? Independent Alone Unaligned with other health care practitioners Maybe it is the wrong word
 when considering heath care provider autonomy, need to distinguish between Individual/personal values Professional values
when considering heath care provider autonomy, need to distinguish between Individual/personal values Professional values
 Shared Decision Making Patients and professionals share evidence Access to info via internet, etc. Patients supported to consider options to achieve preferences Versus clinicians making decision on behalf of patient Paternalism Elwyn, Frosch, Thomson, Joseph-Williams, Lloyd, Kinnersley, Cording, Tomson, Dodd, Rollnick, Edwards &v. Barr (2012)
Shared Decision Making Patients and professionals share evidence Access to info via internet, etc. Patients supported to consider options to achieve preferences Versus clinicians making decision on behalf of patient Paternalism Elwyn, Frosch, Thomson, Joseph-Williams, Lloyd, Kinnersley, Cording, Tomson, Dodd, Rollnick, Edwards &v. Barr (2012)
 Shared Decision Making Patients have preferences based on their values and beliefs Situations can change with illness Patient may not know what they want, may lack understanding , or have competing values Health Care providers have a duty to elicit those preferences and respect them Help patients to understand what they want Provide information May include challenging patient choices (Crib & Entwistle, 2011)
Shared Decision Making Patients have preferences based on their values and beliefs Situations can change with illness Patient may not know what they want, may lack understanding , or have competing values Health Care providers have a duty to elicit those preferences and respect them Help patients to understand what they want Provide information May include challenging patient choices (Crib & Entwistle, 2011)
 Conflicts in Patient versus Professional Autonomy EXAMPLES Patient refuses treatment When patient values conflict with practitioners values Patient chooses non-traditional/unproven treatment Patient makes irrational choices Patient requests unnecessary treatment Patient choice places burden/risk on others Patient non-compliance
Conflicts in Patient versus Professional Autonomy EXAMPLES Patient refuses treatment When patient values conflict with practitioners values Patient chooses non-traditional/unproven treatment Patient makes irrational choices Patient requests unnecessary treatment Patient choice places burden/risk on others Patient non-compliance
 To what extent does practitioner personal integrity place limits on the types of care they provide? Do practitioners have obligation to provide care they do not feel is optimal? To provide care they believe is morally wrong? To provide care they believe may be harmful? To withhold care necessary care at the request of the patient?
To what extent does practitioner personal integrity place limits on the types of care they provide? Do practitioners have obligation to provide care they do not feel is optimal? To provide care they believe is morally wrong? To provide care they believe may be harmful? To withhold care necessary care at the request of the patient?
 When a patient makes choices that appear irrational or harmful to themselves
When a patient makes choices that appear irrational or harmful to themselves
 Patient with Body Dysmorphic Disorder Obsessed with body image and perceived defects Body Integrity Identity Disorder Part of body doesn’t belong
Patient with Body Dysmorphic Disorder Obsessed with body image and perceived defects Body Integrity Identity Disorder Part of body doesn’t belong
 What would you do Patient requests that you tatoo him as follows: Would you consent? How far would you go?
What would you do Patient requests that you tatoo him as follows: Would you consent? How far would you go?
 When patient refuses treatment
When patient refuses treatment
 Patient Autonomy A competent adult patient has moral and legal right to refuse treatment (Baily, 2011)
Patient Autonomy A competent adult patient has moral and legal right to refuse treatment (Baily, 2011)
 Case of Dax Cowart “The case of Dax Cowart illustrates the complexity of issues such as autonomy, paternalism, and quality of life. As the result of a freak accident in the summer of 1973, 25 year-old Dax Cowart was badly burned over 65% of his body. Both eyes, both ears and both hands were damaged beyond repair. Large doses of narcotics were required for minimal pain relief. He pleaded with his caregivers to be allowed to die, and also stated several times that he wanted to kill himself. The physicians at Parkland Hospital in Texas turned to his mother to obtain consent for all his treatments, even though she was not appointed his legal guardian and even though Dax was determined by psychiatric evaluation to have full decision-making capacity. ” http: //www. ascensionhealth. org/index. php? option=com_content&view=article&id=244&It emid=173
Case of Dax Cowart “The case of Dax Cowart illustrates the complexity of issues such as autonomy, paternalism, and quality of life. As the result of a freak accident in the summer of 1973, 25 year-old Dax Cowart was badly burned over 65% of his body. Both eyes, both ears and both hands were damaged beyond repair. Large doses of narcotics were required for minimal pain relief. He pleaded with his caregivers to be allowed to die, and also stated several times that he wanted to kill himself. The physicians at Parkland Hospital in Texas turned to his mother to obtain consent for all his treatments, even though she was not appointed his legal guardian and even though Dax was determined by psychiatric evaluation to have full decision-making capacity. ” http: //www. ascensionhealth. org/index. php? option=com_content&view=article&id=244&It emid=173
 Do you agree with the physician’s course of action and the decisions made?
Do you agree with the physician’s course of action and the decisions made?
 “There was a constant struggle of will between Dax and his mother. Ultimately, he recovered from the burns, albeit severely mutilated. He successfully sued the oil company responsible for his burns, which left him financially secure. Later, he attended law school at Baylor University. He attempted suicide twice after his rehabilitation period. He eventually finished law school and married. He now apparently is happy, but still believes the doctors were wrong to follow his mother’s wishes over his. The case advanced respect for patient autonomy all around the country. ” http: //www. ascensionhealth. org/index. php? option=co m_content&view=article&id=244&Itemid=173
“There was a constant struggle of will between Dax and his mother. Ultimately, he recovered from the burns, albeit severely mutilated. He successfully sued the oil company responsible for his burns, which left him financially secure. Later, he attended law school at Baylor University. He attempted suicide twice after his rehabilitation period. He eventually finished law school and married. He now apparently is happy, but still believes the doctors were wrong to follow his mother’s wishes over his. The case advanced respect for patient autonomy all around the country. ” http: //www. ascensionhealth. org/index. php? option=co m_content&view=article&id=244&Itemid=173
 Parental / Guardian Autonomy When parent/guardian is making decisions for a minor Parents have a right to the direct care, control, and upbringing of their children while they are still minors, according to Find. Law. They also have the right to make various decisions on behalf of their child, including what medical treatment can be used. http: //philadelphiapersonalinjuryblog. com/2011/02/judge-rules-mazeratti-mitchell-must-be-treatedby-doctors. html
Parental / Guardian Autonomy When parent/guardian is making decisions for a minor Parents have a right to the direct care, control, and upbringing of their children while they are still minors, according to Find. Law. They also have the right to make various decisions on behalf of their child, including what medical treatment can be used. http: //philadelphiapersonalinjuryblog. com/2011/02/judge-rules-mazeratti-mitchell-must-be-treatedby-doctors. html
 Mazeratti Mitchell suffered a spinal injury during a wrestling practice in January after he crashed head-on into another wrestler. He has been bedridden at Thomas Jefferson University Hospital since the incident, and doctors have said his spine needs to be stabilized with pins and plates for it to heal properly. But Mazeratti Mitchell's parents argued that they should be permitted to treat their son with other alternative medicines and non-invasive techniques. Erline Aguiluz
Mazeratti Mitchell suffered a spinal injury during a wrestling practice in January after he crashed head-on into another wrestler. He has been bedridden at Thomas Jefferson University Hospital since the incident, and doctors have said his spine needs to be stabilized with pins and plates for it to heal properly. But Mazeratti Mitchell's parents argued that they should be permitted to treat their son with other alternative medicines and non-invasive techniques. Erline Aguiluz
 What would you decide? Delaware County Judge Mary Alice Brennan recently ruled that the teen, an injured wrestler from Chichester High School, will have to receive treatment from doctors. The judge's decision overrode the wishes of the teen's parents to have their son treated at home without surgery or the use of any drugs. http: //philadelphiapersonalinjuryblog. com/2011/02/judge-rules-mazeratti-mitchell-must -be-treated-by-doctors. html
What would you decide? Delaware County Judge Mary Alice Brennan recently ruled that the teen, an injured wrestler from Chichester High School, will have to receive treatment from doctors. The judge's decision overrode the wishes of the teen's parents to have their son treated at home without surgery or the use of any drugs. http: //philadelphiapersonalinjuryblog. com/2011/02/judge-rules-mazeratti-mitchell-must -be-treated-by-doctors. html
 WHY? ? ? Although the state does not normally interfere with these decisions, courts can step in and overrule the choices of parents when the situation is extreme or life-threatening. http: //philadelphiapersonalinjuryblog. com/2011/02/judge-rules-mazeratti-mitchell -must-be-treated-by-doctors. html
WHY? ? ? Although the state does not normally interfere with these decisions, courts can step in and overrule the choices of parents when the situation is extreme or life-threatening. http: //philadelphiapersonalinjuryblog. com/2011/02/judge-rules-mazeratti-mitchell -must-be-treated-by-doctors. html
 When Values are Different
When Values are Different
 When patient and practitioner values conflict, can create a conflict in practitioner to do what is best for patient to achieve best medical outcome (beneficence) versus allowing patient to make best personal decision (autonomy)
When patient and practitioner values conflict, can create a conflict in practitioner to do what is best for patient to achieve best medical outcome (beneficence) versus allowing patient to make best personal decision (autonomy)
 Ethic of Diversity is the norm Ethical decision making requires recognition, acknowledgement and consideration of cultures of all involved Patient/client Practitioner Setting Profession Purtilo , Jensen and Royseen. 2005. Education for Moral Action, FA Davis, Philadelphia, PA.
Ethic of Diversity is the norm Ethical decision making requires recognition, acknowledgement and consideration of cultures of all involved Patient/client Practitioner Setting Profession Purtilo , Jensen and Royseen. 2005. Education for Moral Action, FA Davis, Philadelphia, PA.
 Ethical Relativism “Moral values are relative to a particular culture or individual” “Cannot be judged outside that culture” When society has multiple, overlapping cultures, that can lead to conflict – do we allow others to live in ways we believe are morally unacceptable? Purtilo , Jensen and Royseen. 2005. Education for Moral Action, FA Davis, Philadelphia, PA.
Ethical Relativism “Moral values are relative to a particular culture or individual” “Cannot be judged outside that culture” When society has multiple, overlapping cultures, that can lead to conflict – do we allow others to live in ways we believe are morally unacceptable? Purtilo , Jensen and Royseen. 2005. Education for Moral Action, FA Davis, Philadelphia, PA.
 Cultural Competency Need to consider the cultural background of the patient May complicate and interfere with provision of care and patient satisfaction , especially in those cultures where family or social unit plays a more important role making treatment decisions. (Rihnke, Wilson, Akamatsu, Kinoue, Takashima, Goldstein, Koenig, Hornberger, Raffin, 2000)
Cultural Competency Need to consider the cultural background of the patient May complicate and interfere with provision of care and patient satisfaction , especially in those cultures where family or social unit plays a more important role making treatment decisions. (Rihnke, Wilson, Akamatsu, Kinoue, Takashima, Goldstein, Koenig, Hornberger, Raffin, 2000)
 Respect – “involves sensitivity to individual and group differences” Respect ≠ respectful interaction Need to consider how people interpret facial expressions, choice of words and other forms of communication that are influenced by their culture and past experience
Respect – “involves sensitivity to individual and group differences” Respect ≠ respectful interaction Need to consider how people interpret facial expressions, choice of words and other forms of communication that are influenced by their culture and past experience
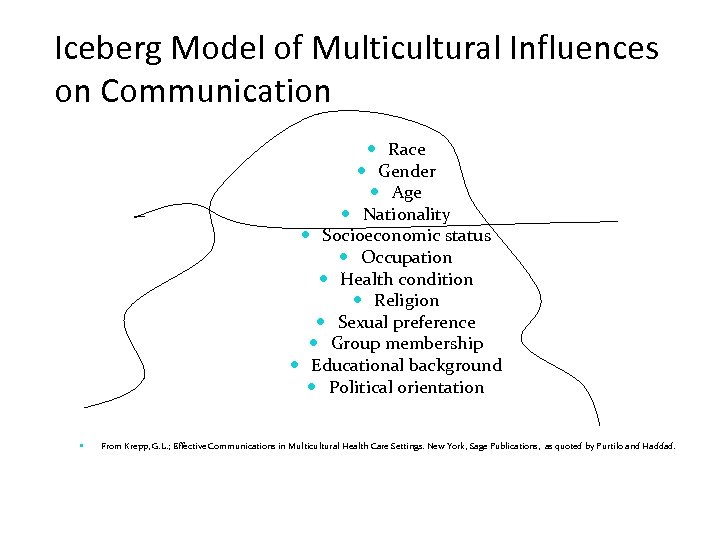 Iceberg Model of Multicultural Influences on Communication Race Gender Age Nationality Socioeconomic status Occupation Health condition Religion Sexual preference Group membership Educational background Political orientation From Krepp, G. L. ; Effective Communications in Multicultural Health Care Settings. New York, Sage Publications, as quoted by Purtilo and Haddad.
Iceberg Model of Multicultural Influences on Communication Race Gender Age Nationality Socioeconomic status Occupation Health condition Religion Sexual preference Group membership Educational background Political orientation From Krepp, G. L. ; Effective Communications in Multicultural Health Care Settings. New York, Sage Publications, as quoted by Purtilo and Haddad.
 Cultural Bias Interpreting based on cultural meaning Personal Bias Interpreting based on personal significance
Cultural Bias Interpreting based on cultural meaning Personal Bias Interpreting based on personal significance
 Da. Vinci Code Symbols White hood KKK vs. robes of priests Pitchfork Devil vs. Poseidon Mother and child statute Ancient Egyptian vs. Pieta Swastika Evil vs. Good Luck
Da. Vinci Code Symbols White hood KKK vs. robes of priests Pitchfork Devil vs. Poseidon Mother and child statute Ancient Egyptian vs. Pieta Swastika Evil vs. Good Luck
 Need to understand influence of these biases and cultural differences in health care and their effect on health care issues Pain Communication of bad news Management of chronic illness and disability Issues of death Methods of treatment Attitudes toward Health Care System Beliefs in other healing methods Putilo and Haddad, Health Professional and Patient Interaction
Need to understand influence of these biases and cultural differences in health care and their effect on health care issues Pain Communication of bad news Management of chronic illness and disability Issues of death Methods of treatment Attitudes toward Health Care System Beliefs in other healing methods Putilo and Haddad, Health Professional and Patient Interaction
 Provider Biases Important contributor to health care disparities HC provides hold stereotypes based on patient race, class, sex, etc, that influence their interpretation or behaviors and symptoms and their clinical decisions Application of these stereotypes frequently occurs outside conscious awareness Providers interact less effectively with minority than with white patients Burgess, D. , van. Ryan, M. , Dovidio, J. & Saha, S. (2007). Reducing racial bias among health care providers: lessons from social-cognitive psychology. Journal of General Internal Medicine(22), 882 -887.
Provider Biases Important contributor to health care disparities HC provides hold stereotypes based on patient race, class, sex, etc, that influence their interpretation or behaviors and symptoms and their clinical decisions Application of these stereotypes frequently occurs outside conscious awareness Providers interact less effectively with minority than with white patients Burgess, D. , van. Ryan, M. , Dovidio, J. & Saha, S. (2007). Reducing racial bias among health care providers: lessons from social-cognitive psychology. Journal of General Internal Medicine(22), 882 -887.
 Obese Patients When Your Doctor Makes You Feel Fat Multiple studies have found that health care professionals routinely stereotype heavy patients Quotes 2003 Research from University of Pennsylvania that found half of 620 primary-care doctors characterized obese patients as Awkward, unattractive, ugly, noncompliant Weak-willed, sloppy, lazy http: //www. prevention. com/print/22527
Obese Patients When Your Doctor Makes You Feel Fat Multiple studies have found that health care professionals routinely stereotype heavy patients Quotes 2003 Research from University of Pennsylvania that found half of 620 primary-care doctors characterized obese patients as Awkward, unattractive, ugly, noncompliant Weak-willed, sloppy, lazy http: //www. prevention. com/print/22527
 But what is of value to the patient? Quality of life is defined differently by individuals Does it mean that when most people would disagree, that patient choice is ignored? “a person who enjoys a meaningful and productive life despite being ventilator dependent should not have to fear being denied life-saving cancer treatment simply because others cannot imagine that life on a ventilator could be worth living” (Baily, 2011)
But what is of value to the patient? Quality of life is defined differently by individuals Does it mean that when most people would disagree, that patient choice is ignored? “a person who enjoys a meaningful and productive life despite being ventilator dependent should not have to fear being denied life-saving cancer treatment simply because others cannot imagine that life on a ventilator could be worth living” (Baily, 2011)
 Video: “The Courage of One’s Conviction”
Video: “The Courage of One’s Conviction”
 What happens when a patient holds with what is considered by practitioner offensive or objectionable personal beliefs seeks care
What happens when a patient holds with what is considered by practitioner offensive or objectionable personal beliefs seeks care
 Patient with objectionable tatoos “A new patient came in for low back pain. He is a male in his 30 s. When he removed his shirt for the exam he had several tattoos of offensive nature. Across his back in large print was “White Power”. Also, on his back, was a grim reaper, holding by the hair the cut off head of a Black person. On his chest was a swastika and “SS”. The treating therapist and the aide assisting her found this extremely offensive and have refused to treat the patient further. The otherapists and staff also do not wish to take over his care due to the above and I cannot fault them… Do we have the right to refuse to treat him since he offends everything we believe is morally correct? ”
Patient with objectionable tatoos “A new patient came in for low back pain. He is a male in his 30 s. When he removed his shirt for the exam he had several tattoos of offensive nature. Across his back in large print was “White Power”. Also, on his back, was a grim reaper, holding by the hair the cut off head of a Black person. On his chest was a swastika and “SS”. The treating therapist and the aide assisting her found this extremely offensive and have refused to treat the patient further. The otherapists and staff also do not wish to take over his care due to the above and I cannot fault them… Do we have the right to refuse to treat him since he offends everything we believe is morally correct? ”
 Does the practitioner have a right to refuse care in this situation?
Does the practitioner have a right to refuse care in this situation?
 Boston Marathon Bombing What is the obligation of doctors who may have treated the injured to the care of the accused bombers?
Boston Marathon Bombing What is the obligation of doctors who may have treated the injured to the care of the accused bombers?
 “widely accepted that the primary responsibility of a physician to promote the good of the patient… doctors are professionally bound to provide medical care to their patients to the best of their abilities regardless of their appealing, unappealing, or even repugnant characteristics” (Capozzi, Rhodes, & Gantsoudes, 2008)
“widely accepted that the primary responsibility of a physician to promote the good of the patient… doctors are professionally bound to provide medical care to their patients to the best of their abilities regardless of their appealing, unappealing, or even repugnant characteristics” (Capozzi, Rhodes, & Gantsoudes, 2008)
 What happens when patient make poor choices?
What happens when patient make poor choices?
 Case Study Mary is a 67 yo female referred to rehabilitation following a AKA (R). Her past medical history is significant for a 20 year history of DM, HTN, and PVD. Following 3 weeks of rehabilitation, she is ambulating with a temporary prosthesis using a walker and close supervision for 25 ft. She is unable to stand for a period longer than 5 minutes due to fatigue. 107
Case Study Mary is a 67 yo female referred to rehabilitation following a AKA (R). Her past medical history is significant for a 20 year history of DM, HTN, and PVD. Following 3 weeks of rehabilitation, she is ambulating with a temporary prosthesis using a walker and close supervision for 25 ft. She is unable to stand for a period longer than 5 minutes due to fatigue. 107
 She lives alone in a two story home with the bed and bath on the second floor. She has a daughter who lives nearby, but who works full time and has two young children. The rehab team has meet with Mary to discuss her discharge plan. Mary insists on going home. The team wants Mary to enter a nursing home as they feel she is unable to care for herself at home. 108
She lives alone in a two story home with the bed and bath on the second floor. She has a daughter who lives nearby, but who works full time and has two young children. The rehab team has meet with Mary to discuss her discharge plan. Mary insists on going home. The team wants Mary to enter a nursing home as they feel she is unable to care for herself at home. 108
 What Is Your Decision? 109
What Is Your Decision? 109
 What happens when the health care provider does not believe that the care is appropriate will not work not proper use of provider’s skills not consistent with standard of care will harm
What happens when the health care provider does not believe that the care is appropriate will not work not proper use of provider’s skills not consistent with standard of care will harm
 You MUST let my bedsores kill me. You MUST! The case of the patient who refused to be turned in bed. Caplan, A. (2012). You must let my bedsores kill me. You must! Medscape, Nov 29, 2012. Accessed 12/5/12 at www. medscape. com
You MUST let my bedsores kill me. You MUST! The case of the patient who refused to be turned in bed. Caplan, A. (2012). You must let my bedsores kill me. You must! Medscape, Nov 29, 2012. Accessed 12/5/12 at www. medscape. com
 Patient Against Society Health care provider as a double agent Advocate for patient vs. advocating for society But patient is part of society Rationing of health care
Patient Against Society Health care provider as a double agent Advocate for patient vs. advocating for society But patient is part of society Rationing of health care
 Patient Decisions Difference between Refusing medical care AND Demanding medical care
Patient Decisions Difference between Refusing medical care AND Demanding medical care
 “Refusing to let people do things to you is one thing, but demanding that people do things for you is quite another. Patients may well have some positive moral or legal rights to health care, but such rights cannot be unlimited. Other people deserve to have their autonomy respected also, and to make their own decisions about what they will or will not do. ” (Baily, M A. 2011)
“Refusing to let people do things to you is one thing, but demanding that people do things for you is quite another. Patients may well have some positive moral or legal rights to health care, but such rights cannot be unlimited. Other people deserve to have their autonomy respected also, and to make their own decisions about what they will or will not do. ” (Baily, M A. 2011)
 Right to demand care cannot be unlimited
Right to demand care cannot be unlimited
 Patient decision can place burdens on family members in Time Energy Psychological trauma Financial costs (Baily, 2011)
Patient decision can place burdens on family members in Time Energy Psychological trauma Financial costs (Baily, 2011)
 Case Scenario Patient is an 18 yo female diagnosed 2 yrs ago with Lyme's Disease. She has undergone 1 year of PT for strengthening and pain control. At this time she is independent in her exercise program and administration of Tens. The PT has decided to terminate her PT. The decision is discussed with the patient who raised no objections. However, the next day the PT received a call from the patient’s physician who states the patient contacted him distressed that her PT was being discontinued. He agrees with the patient and requests that therapy continue.
Case Scenario Patient is an 18 yo female diagnosed 2 yrs ago with Lyme's Disease. She has undergone 1 year of PT for strengthening and pain control. At this time she is independent in her exercise program and administration of Tens. The PT has decided to terminate her PT. The decision is discussed with the patient who raised no objections. However, the next day the PT received a call from the patient’s physician who states the patient contacted him distressed that her PT was being discontinued. He agrees with the patient and requests that therapy continue.
 When the PT explains that all therapy goals have been met, the physician states that he will then send the patient to a gym to continue her program. The PT is concerned with this plan, as the patient could be harmed if the exercise is too strenuous. The PT is also concerned as the MD is a very influential member of the hospital’s medical staff and would not hesitate to contact the administration to demand continued care for his patient. It should also be noted that the patient has spent the last 2 years home tutored due to the effects of the Lyme’s Disease. She has lost contact with most of her friends and has developed a strong dependency on the rehab staff for her socialization and as her support system.
When the PT explains that all therapy goals have been met, the physician states that he will then send the patient to a gym to continue her program. The PT is concerned with this plan, as the patient could be harmed if the exercise is too strenuous. The PT is also concerned as the MD is a very influential member of the hospital’s medical staff and would not hesitate to contact the administration to demand continued care for his patient. It should also be noted that the patient has spent the last 2 years home tutored due to the effects of the Lyme’s Disease. She has lost contact with most of her friends and has developed a strong dependency on the rehab staff for her socialization and as her support system.
 The PT must make a decision – should he continue to treat the patient as requested by the patient and MD? Will termination of the care impact the patient’s physical and/or psychological health? If the MD goes to the administration and demands the care be continued, it could threaten the PT’s continued employment and the MD’s patient referrals which are a substantial portion of the department's revenue base.
The PT must make a decision – should he continue to treat the patient as requested by the patient and MD? Will termination of the care impact the patient’s physical and/or psychological health? If the MD goes to the administration and demands the care be continued, it could threaten the PT’s continued employment and the MD’s patient referrals which are a substantial portion of the department's revenue base.
 What would you do? What does you practice act say about this? 13: 39 A-3. 6 Prohibition on excessive fees; overutilization (c) A licensed physical therapist shall not provide intervention or conduct testing which in light of the patient's history and findings are unwarranted and unnecessary. (d) A licensed physical therapist shall not charge a fee to a patient or a third party payer for an intervention or other physical therapy which is unwarranted and unnecessary.
What would you do? What does you practice act say about this? 13: 39 A-3. 6 Prohibition on excessive fees; overutilization (c) A licensed physical therapist shall not provide intervention or conduct testing which in light of the patient's history and findings are unwarranted and unnecessary. (d) A licensed physical therapist shall not charge a fee to a patient or a third party payer for an intervention or other physical therapy which is unwarranted and unnecessary.
 13: 39 A-3. 8 Violative acts; professional misconduct (a)6. Rendering an intervention when, in the exercise of his or her professional judgment, the licensed physical therapist may deem such intervention to be unnecessary. When appropriate, the licensed physical therapist shall Notify the referring professional in writing that the intervention to be terminated and the reason(s) for such termination;
13: 39 A-3. 8 Violative acts; professional misconduct (a)6. Rendering an intervention when, in the exercise of his or her professional judgment, the licensed physical therapist may deem such intervention to be unnecessary. When appropriate, the licensed physical therapist shall Notify the referring professional in writing that the intervention to be terminated and the reason(s) for such termination;
 When considering how to spend limited health care dollars. . How Much is Too Much?
When considering how to spend limited health care dollars. . How Much is Too Much?
 “it is in the long-term interest of insured patients to have reasonable limits on their treatment choices so that premiums and taxes need not rise to unreasonable levels. ” “With no limits at all, there will be fewer resources available for health care earlier in life or for other important goods. ” “ a cost conscious standard of care does not mean having no choice: it just means not having unlimited choice at the expense of other people. ” (Baily, 2011)
“it is in the long-term interest of insured patients to have reasonable limits on their treatment choices so that premiums and taxes need not rise to unreasonable levels. ” “With no limits at all, there will be fewer resources available for health care earlier in life or for other important goods. ” “ a cost conscious standard of care does not mean having no choice: it just means not having unlimited choice at the expense of other people. ” (Baily, 2011)
 Patient Non-compliance Beneficence versus Autonomy Non-maleficence Best outcome may not always be the best medical outcome Does not always mean there is a problem Compliance is not always the solution Should be viewed as a potential outcome of a competent patient making an autonomous decision Should a patient be coerced or deceived in order to achieve the practitioner’s choice of outcome
Patient Non-compliance Beneficence versus Autonomy Non-maleficence Best outcome may not always be the best medical outcome Does not always mean there is a problem Compliance is not always the solution Should be viewed as a potential outcome of a competent patient making an autonomous decision Should a patient be coerced or deceived in order to achieve the practitioner’s choice of outcome
 Terminating the Physician. Patient Relationship Capozzi et al (2008) raise the questions “When does the failure of a patient to so what he or she should do release the physician from professional responsibility? ” If patient has ongoing medical needs, MD has ongoing duty to provider care “What are the physician’s professional limitations with regard to promoting the good of the patient? ” It depends- if good of patient is promoted by medical care, professional responsibility is involved
Terminating the Physician. Patient Relationship Capozzi et al (2008) raise the questions “When does the failure of a patient to so what he or she should do release the physician from professional responsibility? ” If patient has ongoing medical needs, MD has ongoing duty to provider care “What are the physician’s professional limitations with regard to promoting the good of the patient? ” It depends- if good of patient is promoted by medical care, professional responsibility is involved
 Case Study 54 yo female suffered right CVA and has been receiving PT Increased ms tone is developing in left UE making ROM painful She is getting good neurological return in LE and is now able to ambulate with CG Pt begins to refuse PROM due to pain. Her mother sustained a CVA and had no functional return in UE , so patient expects the same
Case Study 54 yo female suffered right CVA and has been receiving PT Increased ms tone is developing in left UE making ROM painful She is getting good neurological return in LE and is now able to ambulate with CG Pt begins to refuse PROM due to pain. Her mother sustained a CVA and had no functional return in UE , so patient expects the same
 Therapist explains importance of treatment, not just to facilitate fictional return but also for prevention of severe contractures Patient continues to refuse Therapist believes patient does not understand long term implication of her decision and proceeds with PROM exercises, telling the patient ‘it’s for your own good. In the future, you will understand why I have to do this” Patient cries through the session and tries to push therapist away (Coy, 1989)
Therapist explains importance of treatment, not just to facilitate fictional return but also for prevention of severe contractures Patient continues to refuse Therapist believes patient does not understand long term implication of her decision and proceeds with PROM exercises, telling the patient ‘it’s for your own good. In the future, you will understand why I have to do this” Patient cries through the session and tries to push therapist away (Coy, 1989)
 Is therapist justified in forcing the services on the patient?
Is therapist justified in forcing the services on the patient?
 So, are there ways you might approach a patient differently in the future when they don’t agree with you?
So, are there ways you might approach a patient differently in the future when they don’t agree with you?
 Accessing the New Jersey Physical Therapy Practice Act
Accessing the New Jersey Physical Therapy Practice Act
 Law “System of principles and processes by which people who live in a society attempt to control human conduct, to facilitate cooperative enterprise, and to minimize the use of force in resolving conflict” Society specifies standards of behavior Miller, Robert D. Problems in Health Care Law
Law “System of principles and processes by which people who live in a society attempt to control human conduct, to facilitate cooperative enterprise, and to minimize the use of force in resolving conflict” Society specifies standards of behavior Miller, Robert D. Problems in Health Care Law
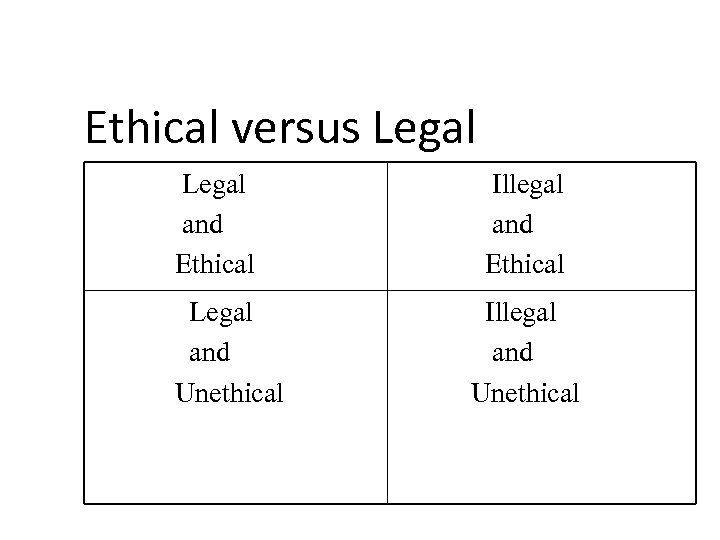 Ethical versus Legal and Ethical Legal and Unethical Illegal and Ethical Illegal and Unethical
Ethical versus Legal and Ethical Legal and Unethical Illegal and Ethical Illegal and Unethical
 Purpose of Regulation To protect the public
Purpose of Regulation To protect the public
 The Legislature finds and declares that the public interest requires the regulation of the practice of physical therapy and the establishment of clear licensure standards for physical therapists; and that the health and welfare of the citizens of this State will be protected by identifying to the public those individuals who are qualified and legally authorized to practice physical therapy
The Legislature finds and declares that the public interest requires the regulation of the practice of physical therapy and the establishment of clear licensure standards for physical therapists; and that the health and welfare of the citizens of this State will be protected by identifying to the public those individuals who are qualified and legally authorized to practice physical therapy
 Why Important? Ignorance of the law is no defense!
Why Important? Ignorance of the law is no defense!
 Sources of Law Constitutional Statutes Administrative Court Decisions
Sources of Law Constitutional Statutes Administrative Court Decisions
 Branches of Government Legislative – enact and amend law Executive – enforce and administer law Judicial – decide disputes Separation of Powers No one dominant Each can effect and limit the others
Branches of Government Legislative – enact and amend law Executive – enforce and administer law Judicial – decide disputes Separation of Powers No one dominant Each can effect and limit the others
 Federal versus State Congress – has powers delegated by Constitution State – all powers not denied by Constitution, federal law or state constitution Practice Acts are state laws Local Law – power granted by state
Federal versus State Congress – has powers delegated by Constitution State – all powers not denied by Constitution, federal law or state constitution Practice Acts are state laws Local Law – power granted by state
 Criminal Law “Legal actions brought on behalf of society for violations of its criminal laws against a defendant or multiple defendants” Scott, Ronald (1997). Promoting Legal Awareness in Physical and Occupational Therapy, St. Louis, Mo. Mosby. page 7
Criminal Law “Legal actions brought on behalf of society for violations of its criminal laws against a defendant or multiple defendants” Scott, Ronald (1997). Promoting Legal Awareness in Physical and Occupational Therapy, St. Louis, Mo. Mosby. page 7
 Civil Law “Encompasses private legal actions brought by one or more private defendants” Tort = Wrong Health Care Malpractice Scott, Ronald (1997). Promoting Legal Awareness in Physical and Occupational Therapy, St. Louis, Mo. Mosby. page 7 Compensate monetarily for losses that should have been prevented Miller, Robert D (2006). Problems in Health Care Law, Sudbury, MA. Jones and Bartlett.
Civil Law “Encompasses private legal actions brought by one or more private defendants” Tort = Wrong Health Care Malpractice Scott, Ronald (1997). Promoting Legal Awareness in Physical and Occupational Therapy, St. Louis, Mo. Mosby. page 7 Compensate monetarily for losses that should have been prevented Miller, Robert D (2006). Problems in Health Care Law, Sudbury, MA. Jones and Bartlett.
 Licensure A form of credentialing, established by statute and intended to protect the public, that regulates the practice of a trade or profession by specifying who may practice and what duties they may perform. Most restrictive form of governmental credentialing Legal Considerations in Sports Medicine
Licensure A form of credentialing, established by statute and intended to protect the public, that regulates the practice of a trade or profession by specifying who may practice and what duties they may perform. Most restrictive form of governmental credentialing Legal Considerations in Sports Medicine
 Laws and Regulations In NJ New Jersey Statutes – Chapter 45 Physical Therapist Licensing Act of 1983 Uniform Enforcement Act (NJ) Uniform Regulations: Duty to Cooperate Administrative Code – Chapter 39 Others Insurance Regulations(DOBI - NJ) CMS: Medicare & Medicaid (Federal)
Laws and Regulations In NJ New Jersey Statutes – Chapter 45 Physical Therapist Licensing Act of 1983 Uniform Enforcement Act (NJ) Uniform Regulations: Duty to Cooperate Administrative Code – Chapter 39 Others Insurance Regulations(DOBI - NJ) CMS: Medicare & Medicaid (Federal)
 Health Care Professional Responsibility Reporting Oct 2005 New Rules Adopted Jan 31, 2011 Applies to any health care professional board Creates Clearing House Coordinator within Department of Consumer Affairs “health care entity shall notify the division in writing if a health care professional who is employed by, under contract to render professional services to, or has privileges granted by, that health care entity, or who provides such services pursuant to an agreement with a health care services firm or staffing registry”
Health Care Professional Responsibility Reporting Oct 2005 New Rules Adopted Jan 31, 2011 Applies to any health care professional board Creates Clearing House Coordinator within Department of Consumer Affairs “health care entity shall notify the division in writing if a health care professional who is employed by, under contract to render professional services to, or has privileges granted by, that health care entity, or who provides such services pursuant to an agreement with a health care services firm or staffing registry”
 For reasons relating to the health care professional’s impairment, incompetency or professional misconduct, which incompetency or professional misconduct relates adversely to patient care or safety: Privileges revoked or suspended Discharged / terminated Conditions placed on practice Voluntarily resign while under review Party to malpractice suit
For reasons relating to the health care professional’s impairment, incompetency or professional misconduct, which incompetency or professional misconduct relates adversely to patient care or safety: Privileges revoked or suspended Discharged / terminated Conditions placed on practice Voluntarily resign while under review Party to malpractice suit
 Also required criminal background check for new licensees
Also required criminal background check for new licensees
 Uniform Enforcement Act Authorized boards to adopt rules and regulations to serve the public health, safety and welfare Establishes powers of the Attorney General to implement and administer law enforcement activities of boards
Uniform Enforcement Act Authorized boards to adopt rules and regulations to serve the public health, safety and welfare Establishes powers of the Attorney General to implement and administer law enforcement activities of boards
 Provides for power by of the boards to investigate any act or practice deemed unlawful by statute or regulation administered by the board Ability to discipline licensee Suspend/Revoke licensure Civil penalties Mandatory continuing education Compels compliance by licensees and others in investigative process Access to premises Provide testimony Provide documentation
Provides for power by of the boards to investigate any act or practice deemed unlawful by statute or regulation administered by the board Ability to discipline licensee Suspend/Revoke licensure Civil penalties Mandatory continuing education Compels compliance by licensees and others in investigative process Access to premises Provide testimony Provide documentation
 Provides Governor with the authority to appointment members of named boards Specifically calls for appointment of two public members Provides for the reimbursement of expenses and compensation for Board members Established a 2 -year licensure period
Provides Governor with the authority to appointment members of named boards Specifically calls for appointment of two public members Provides for the reimbursement of expenses and compensation for Board members Established a 2 -year licensure period
 Establishes unlicensed practice 30 days after license expires License suspended pursuant to this section can be reinstated within 5 years of expiration with renewal application and additional fees After 5 years – requirement to complete examination
Establishes unlicensed practice 30 days after license expires License suspended pursuant to this section can be reinstated within 5 years of expiration with renewal application and additional fees After 5 years – requirement to complete examination
 Claims for Third Party Payment Licensed health care provider is responsible for filing claims to third party payers for health care services provided by licensee that are eligible for third party payment Within 60 days of last day of service If payment assigned to provider, within 180 days Standard form Establishes fees for noncompliance
Claims for Third Party Payment Licensed health care provider is responsible for filing claims to third party payers for health care services provided by licensee that are eligible for third party payment Within 60 days of last day of service If payment assigned to provider, within 180 days Standard form Establishes fees for noncompliance
 Uniform Regulations Requires cooperation by a licensee in any inquiry, inspection or investigation by or on behalf of a board, Director of Consumer Affairs or licensing agency into a licensee’s conduct, fitness or capacity to engage in a licensed profession or occupation
Uniform Regulations Requires cooperation by a licensee in any inquiry, inspection or investigation by or on behalf of a board, Director of Consumer Affairs or licensing agency into a licensee’s conduct, fitness or capacity to engage in a licensed profession or occupation
 Failure to cooperate , absent good cause or bona fide claim of privilege, may be constitute professional misconduct and thereby subject a licensee to disciplinary action
Failure to cooperate , absent good cause or bona fide claim of privilege, may be constitute professional misconduct and thereby subject a licensee to disciplinary action
 Failure to Cooperate Failure to respond timely to an inquiry to provide information in response to a complaint concerning licensee conduct Failure to provide records Failure to attend hearing Failure to provide board with timely notice of change of address
Failure to Cooperate Failure to respond timely to an inquiry to provide information in response to a complaint concerning licensee conduct Failure to provide records Failure to attend hearing Failure to provide board with timely notice of change of address
 History of Physical Therapy Regulation in New Jersey 1963 1983 2003
History of Physical Therapy Regulation in New Jersey 1963 1983 2003
 Physical Therapist Licensing Act of 1983 Statutes enacted by New Jersey State Legislature as “the legislature finds and declares that the public interest requires the regulation of the practice of physical therapy and the establishment of clear licensure standards for physical therapists”
Physical Therapist Licensing Act of 1983 Statutes enacted by New Jersey State Legislature as “the legislature finds and declares that the public interest requires the regulation of the practice of physical therapy and the establishment of clear licensure standards for physical therapists”
 “And that the health and welfare of the citizens of this state will be protected by identifying to the public those individuals who are qualified and legally authorized to practice physical therapy”
“And that the health and welfare of the citizens of this state will be protected by identifying to the public those individuals who are qualified and legally authorized to practice physical therapy”
 State Board of Physical Therapy Examiners Governor Appointment 11 members – residents of state 6 PT – actively engaged on practice for at least 5 years immediately preceding appointment 1 PTA – actively engaged on practice for at least 5 years immediately preceding appointment 1 licensed physician 2 public members 1 state executive department member
State Board of Physical Therapy Examiners Governor Appointment 11 members – residents of state 6 PT – actively engaged on practice for at least 5 years immediately preceding appointment 1 PTA – actively engaged on practice for at least 5 years immediately preceding appointment 1 licensed physician 2 public members 1 state executive department member
 Duties of SBPTE Administer and enforce law Establish procedures for licensure Establish standards for examination Review and pass upon qualifications of applicants Establish disciplinary procedures Maintain record of all licensees Conduct hearing into allegations of misconduct Establish continuing education requirements
Duties of SBPTE Administer and enforce law Establish procedures for licensure Establish standards for examination Review and pass upon qualifications of applicants Establish disciplinary procedures Maintain record of all licensees Conduct hearing into allegations of misconduct Establish continuing education requirements
 APTA VERSUS SBPTE So Who’s Who ?
APTA VERSUS SBPTE So Who’s Who ?
 What’s the Difference? SBPTE APTA Legally Binding Defines Current Practice Positions and policies not legally binding Recommends and advocates for practice change Nationwide Voluntary Promotion of profession, licensees and patients/clients By State Covers all licensees Public Protection
What’s the Difference? SBPTE APTA Legally Binding Defines Current Practice Positions and policies not legally binding Recommends and advocates for practice change Nationwide Voluntary Promotion of profession, licensees and patients/clients By State Covers all licensees Public Protection
 Physical Therapist Licensing Act of 1983 New Jersey State Board of Physical Therapy Examiners http: //www. njconsumeraffairs. gov/pt
Physical Therapist Licensing Act of 1983 New Jersey State Board of Physical Therapy Examiners http: //www. njconsumeraffairs. gov/pt
 REFERENCES *Physical Therapist Licensing Act of 1983: Physical Therapy Regulations 45: 9 -37. 11 -45: 9 -37. 34 e *Chapter 39 A, State Board of Physical Therapy; Administrative Rules *Uniform Enforcement Act, Professions and Occupations Title 45: 1 -1 – 45: 1 -41 (L. 2005, c. 83, s. 19) *Uniform Regulations, Chapter 45 C, ( Authority N. J. S. A. 5: 8 -30. 2, 45: 1 -17(b) and 52: 17 B-122) Capozzi, J. D. , Rhodes, R. & Gantsoudes, G. (2008). Terminating the physician-patient relationship. J Bone Joint Surg Am, 90, pg 208 -210. Saunders, J. (2006), Ethical decision-making in professional bodies. Clinical Medicine: 6(1), 13 -15. Greenfield, B. H. (2006). The meaning of caring in five experienced physical therapists. Physiotherapy Theory and Practice: 22(4), 175 -187. Hurst, S. A. , Du. Val. G & Danis, M. (2008). How physicians face ethical difficulties: a qualitative analysis. J. Med Ethics: 31, pgs 7 -14.
REFERENCES *Physical Therapist Licensing Act of 1983: Physical Therapy Regulations 45: 9 -37. 11 -45: 9 -37. 34 e *Chapter 39 A, State Board of Physical Therapy; Administrative Rules *Uniform Enforcement Act, Professions and Occupations Title 45: 1 -1 – 45: 1 -41 (L. 2005, c. 83, s. 19) *Uniform Regulations, Chapter 45 C, ( Authority N. J. S. A. 5: 8 -30. 2, 45: 1 -17(b) and 52: 17 B-122) Capozzi, J. D. , Rhodes, R. & Gantsoudes, G. (2008). Terminating the physician-patient relationship. J Bone Joint Surg Am, 90, pg 208 -210. Saunders, J. (2006), Ethical decision-making in professional bodies. Clinical Medicine: 6(1), 13 -15. Greenfield, B. H. (2006). The meaning of caring in five experienced physical therapists. Physiotherapy Theory and Practice: 22(4), 175 -187. Hurst, S. A. , Du. Val. G & Danis, M. (2008). How physicians face ethical difficulties: a qualitative analysis. J. Med Ethics: 31, pgs 7 -14.
 References Detert, J. R. & Trevino, L. K. (2008). Moral Disengagement in ethical decision making: A study of antecedents and outcomes. Journal of Applied Psychology: 93(2), 374 -391 Numminen, O. H. & Leino-Kilpi. H. (2007). Nursing students’ ethical; decision-making: a review of the literature. Nurse Education Today: 27, pg 796 -807. *Kirsch, N. (2011). Patient presents with troubling autonomy. PT in Motion 2011(5). Accessed at http: //www. apta. org/PTin. Motion/2011/5/Ethicsin. Practice/, on 6/24/11. Bennett, J. (2007). Informed consent: tips and caveats for PTs. PT in Motion 2007(12). Accessed at http: //www. apta. org/PTin. Motion/2007/12/Liability. Awareness , on June 24. 2011. Kirsch, N (2008). Confidentiality issues: analysis. PT in Motion 2008, Vol. 11. Accessed at http: //www. apta. org/PTin. MOtion/2008/11/ethicsin. Action/, on June 24, 2011. Kirsch, N (2006). Ethical decision making: terminology and context. PT in Motion 2006, Vol. 2. Accessed at http: //www. apta. org. PTin. Motion/2006/2/Ethicsin. Action/, on June 24, 2011.
References Detert, J. R. & Trevino, L. K. (2008). Moral Disengagement in ethical decision making: A study of antecedents and outcomes. Journal of Applied Psychology: 93(2), 374 -391 Numminen, O. H. & Leino-Kilpi. H. (2007). Nursing students’ ethical; decision-making: a review of the literature. Nurse Education Today: 27, pg 796 -807. *Kirsch, N. (2011). Patient presents with troubling autonomy. PT in Motion 2011(5). Accessed at http: //www. apta. org/PTin. Motion/2011/5/Ethicsin. Practice/, on 6/24/11. Bennett, J. (2007). Informed consent: tips and caveats for PTs. PT in Motion 2007(12). Accessed at http: //www. apta. org/PTin. Motion/2007/12/Liability. Awareness , on June 24. 2011. Kirsch, N (2008). Confidentiality issues: analysis. PT in Motion 2008, Vol. 11. Accessed at http: //www. apta. org/PTin. MOtion/2008/11/ethicsin. Action/, on June 24, 2011. Kirsch, N (2006). Ethical decision making: terminology and context. PT in Motion 2006, Vol. 2. Accessed at http: //www. apta. org. PTin. Motion/2006/2/Ethicsin. Action/, on June 24, 2011.
 References Brock, D. , and Wartman, S. (1990). When competent patients make irrational choices. New England Journal of Medicine 1990 Vol. 32, 1595 – 1599. Accessed at http: //www. nejm. org. libproxy. umsnj. edu/doi/full/10. 1056/NEJM 199005313222209? view. Type=Print on June 24, 2011 Capozzi, . . Rhodes, R. , Gantsoudes, G. (2008). Terminatig the Capozzi, J. D. , Lowenstein, G. , Brennan, T. , & Volpp. K. (2007). Asymmetric paternalism to improve health behaviors: commentary. Journal of the American Medical Association, 2007, Vol. 298(20), 2415 – 2417. Accessed at jama. org at University of Medicine & Dentistry on NJ on June 24, 2100. Swindell, J. , Mc. Guire, A. , & Halpern, S. (2010). Beneficent Persuasion: techniques and ethical guidelines to improve patients' decisions. Annals of Family Medicine, Vol. 8(3). Accessed at www. annfammed. org on June 24, 2011 Kirsch, N. (2009). New and improved: updated ethics documents for PTs and PTAs. PT in Motion, 2009, Vol. 11. Accessed at http: //www. apta. org/PTin. Motion/2009/11/Ethicsin. Practice on June 24, 2011. Kirsch, N. (2011). The parent trap. PT in Motion, 2011, Vol. 4. Accessed at http: //www. apta. org/PTin. Motion/2011/4/Ethicsin. Practice, on June 24, 2011. Dockter, L. (2009). Confidentiality issues: legal analysis. PT in Motion, 2008, Vol. 12. Accessed at http: www. apta. org/PTin. Motion/2008/12/Ethicsin. Action on June 24, 2011. *Sandstrom, R. (2007). The Meanings of autonomy for physical therapy. Physical Therapy Journal, Vol. 87(1), 98 – 110. Accessed at http: //www. apta. org on June 24, 2011.
References Brock, D. , and Wartman, S. (1990). When competent patients make irrational choices. New England Journal of Medicine 1990 Vol. 32, 1595 – 1599. Accessed at http: //www. nejm. org. libproxy. umsnj. edu/doi/full/10. 1056/NEJM 199005313222209? view. Type=Print on June 24, 2011 Capozzi, . . Rhodes, R. , Gantsoudes, G. (2008). Terminatig the Capozzi, J. D. , Lowenstein, G. , Brennan, T. , & Volpp. K. (2007). Asymmetric paternalism to improve health behaviors: commentary. Journal of the American Medical Association, 2007, Vol. 298(20), 2415 – 2417. Accessed at jama. org at University of Medicine & Dentistry on NJ on June 24, 2100. Swindell, J. , Mc. Guire, A. , & Halpern, S. (2010). Beneficent Persuasion: techniques and ethical guidelines to improve patients' decisions. Annals of Family Medicine, Vol. 8(3). Accessed at www. annfammed. org on June 24, 2011 Kirsch, N. (2009). New and improved: updated ethics documents for PTs and PTAs. PT in Motion, 2009, Vol. 11. Accessed at http: //www. apta. org/PTin. Motion/2009/11/Ethicsin. Practice on June 24, 2011. Kirsch, N. (2011). The parent trap. PT in Motion, 2011, Vol. 4. Accessed at http: //www. apta. org/PTin. Motion/2011/4/Ethicsin. Practice, on June 24, 2011. Dockter, L. (2009). Confidentiality issues: legal analysis. PT in Motion, 2008, Vol. 12. Accessed at http: www. apta. org/PTin. Motion/2008/12/Ethicsin. Action on June 24, 2011. *Sandstrom, R. (2007). The Meanings of autonomy for physical therapy. Physical Therapy Journal, Vol. 87(1), 98 – 110. Accessed at http: //www. apta. org on June 24, 2011.
 References Brock, D. , and Wartman, S. (1990). When competent patients make irrational choices. New England Journal of Medicine 1990 Vol. 32, 1595 – 1599. Accessed at http: //www. nejm. org. libproxy. umsnj. edu/doi/full/10. 1056/NEJM 199005313222209? view. Type=Print on June 24, 2011 Capozzi, J. F. , Rhodes, R. , Gantsoudes, G. (2008). Terminating the physician=patient relationship. J Bone Joint Surg AM, 90, 208 -210. Lowenstein, G. , Brennan, T. , & Volpp. K. (2007). Asymmetric paternalism to improve health behaviors: commentary. Journal of the American Medical Association, 2007, Vol. 298(20), 2415 – 2417. Accessed at jama. org at University of Medicine & Dentistry on NJ on June 24, 2100. Swindell, J. , Mc. Guire, A. , & Halpern, S. (2010). Beneficent Persuasion: techniques and ethical guidelines to improve patients' decisions. Annals of Family Medicine, Vol. 8(3). Accessed at www. annfammed. org on June 24, 2011 Kirsch, N. (2009). New and improved: updated ethics documents for PTs and PTAs. PT in Motion, 2009, Vol. 11. Accessed at http: //www. apta. org/PTin. Motion/2009/11/Ethicsin. Practice on June 24, 2011. Kirsch, N. (2011). The parent trap. PT in Motion, 2011, Vol. 4. Accessed at http: //www. apta. org/PTin. Motion/2011/4/Ethicsin. Practice, on June 24, 2011. Dockter, L. (2009). Confidentiality issues: legal analysis. PT in Motion, 2008, Vol. 12. Accessed at http: www. apta. org/PTin. Motion/2008/12/Ethicsin. Action on June 24, 2011. *Sandstrom, R. (2007). The Meanings of autonomy for physical therapy. Physical Therapy Journal, Vol. 87(1), 98 – 110. Accessed at http: //www. apta. org on June 24, 2011.
References Brock, D. , and Wartman, S. (1990). When competent patients make irrational choices. New England Journal of Medicine 1990 Vol. 32, 1595 – 1599. Accessed at http: //www. nejm. org. libproxy. umsnj. edu/doi/full/10. 1056/NEJM 199005313222209? view. Type=Print on June 24, 2011 Capozzi, J. F. , Rhodes, R. , Gantsoudes, G. (2008). Terminating the physician=patient relationship. J Bone Joint Surg AM, 90, 208 -210. Lowenstein, G. , Brennan, T. , & Volpp. K. (2007). Asymmetric paternalism to improve health behaviors: commentary. Journal of the American Medical Association, 2007, Vol. 298(20), 2415 – 2417. Accessed at jama. org at University of Medicine & Dentistry on NJ on June 24, 2100. Swindell, J. , Mc. Guire, A. , & Halpern, S. (2010). Beneficent Persuasion: techniques and ethical guidelines to improve patients' decisions. Annals of Family Medicine, Vol. 8(3). Accessed at www. annfammed. org on June 24, 2011 Kirsch, N. (2009). New and improved: updated ethics documents for PTs and PTAs. PT in Motion, 2009, Vol. 11. Accessed at http: //www. apta. org/PTin. Motion/2009/11/Ethicsin. Practice on June 24, 2011. Kirsch, N. (2011). The parent trap. PT in Motion, 2011, Vol. 4. Accessed at http: //www. apta. org/PTin. Motion/2011/4/Ethicsin. Practice, on June 24, 2011. Dockter, L. (2009). Confidentiality issues: legal analysis. PT in Motion, 2008, Vol. 12. Accessed at http: www. apta. org/PTin. Motion/2008/12/Ethicsin. Action on June 24, 2011. *Sandstrom, R. (2007). The Meanings of autonomy for physical therapy. Physical Therapy Journal, Vol. 87(1), 98 – 110. Accessed at http: //www. apta. org on June 24, 2011.
 References Coy, J. (1989). Autonomy-based informed consent: ethical implications for patient noncompliance. Physical Therapy Journal, 1989, Vol. 69(10), 826 -833. Accessed at http: //www. apta. org on June 24, 2011. Bruckner, J. (1987). Physical therapists as double agents: ethical dilemmas of divided loyalties. Physical Therapy Journal, 1987, Vol. 67(3), 383 – 387. Accessed at http: //www. apte. org on June 24, 2011. Caplan, A. (2012). You must let my bedsores kill me. You must! Medscape, Nov 29, 2012. Accessed 12/5/12 at www. medscape. com Nalette, E, (2010). Constrained physical therapist practice: an ethical case analysis of recommending discharge placement from the acute care setting. Physical Therapy Journal, 2010, Vol. 90(6), 939 – 952. Accessed ay http: //www. apta. org on June 24, 2011. Greenfield, B. & Jensen, G. (2010). Understanding the lived experiences of patients: application of a phenomenological approach to ethics. Physical Therapy Journal 2010 Vol. 90(8), 1185 -1197. Accessed at http: //ptjournal. apta. org/content/90/8/1185. fill. pdf%20 html? sid=fbc 20 a 6 c-3 f 7 b-4 b 87 -b 2 cc 7 c 8 e 385 d 65 db on June 24, 2011 Purtilo , Jensen and Royseen. 2005. Education for Moral Action, FA Davis, Philadelphia, PA.
References Coy, J. (1989). Autonomy-based informed consent: ethical implications for patient noncompliance. Physical Therapy Journal, 1989, Vol. 69(10), 826 -833. Accessed at http: //www. apta. org on June 24, 2011. Bruckner, J. (1987). Physical therapists as double agents: ethical dilemmas of divided loyalties. Physical Therapy Journal, 1987, Vol. 67(3), 383 – 387. Accessed at http: //www. apte. org on June 24, 2011. Caplan, A. (2012). You must let my bedsores kill me. You must! Medscape, Nov 29, 2012. Accessed 12/5/12 at www. medscape. com Nalette, E, (2010). Constrained physical therapist practice: an ethical case analysis of recommending discharge placement from the acute care setting. Physical Therapy Journal, 2010, Vol. 90(6), 939 – 952. Accessed ay http: //www. apta. org on June 24, 2011. Greenfield, B. & Jensen, G. (2010). Understanding the lived experiences of patients: application of a phenomenological approach to ethics. Physical Therapy Journal 2010 Vol. 90(8), 1185 -1197. Accessed at http: //ptjournal. apta. org/content/90/8/1185. fill. pdf%20 html? sid=fbc 20 a 6 c-3 f 7 b-4 b 87 -b 2 cc 7 c 8 e 385 d 65 db on June 24, 2011 Purtilo , Jensen and Royseen. 2005. Education for Moral Action, FA Davis, Philadelphia, PA.
 References NJ Advanced Directive in Health Care Act Accessed at http: //www. nj. gov/health/advanced directive/documents/njsa_26. 2 h. 53. pdf When your doctor makes you feel fat. Prevention Accessed 12/5/13 @ http: //www. prevention. com/print/22527 ETHICS IN MEDICINE University of Washington School of Medicine accessed 12/4/2013 at http: //depts. washington. edu/bioethx/topics/dnr. html
References NJ Advanced Directive in Health Care Act Accessed at http: //www. nj. gov/health/advanced directive/documents/njsa_26. 2 h. 53. pdf When your doctor makes you feel fat. Prevention Accessed 12/5/13 @ http: //www. prevention. com/print/22527 ETHICS IN MEDICINE University of Washington School of Medicine accessed 12/4/2013 at http: //depts. washington. edu/bioethx/topics/dnr. html


