1c0bd76edff9832a56d90d3836411edb.ppt
- Количество слайдов: 51

partment of habilitation Medicine oul National University llege of Medicine Rehabilitation of Myelodysplasia Moon Suk Bang, MD Department of Rehabilitation Medicine, Seoul National University College of Medicine
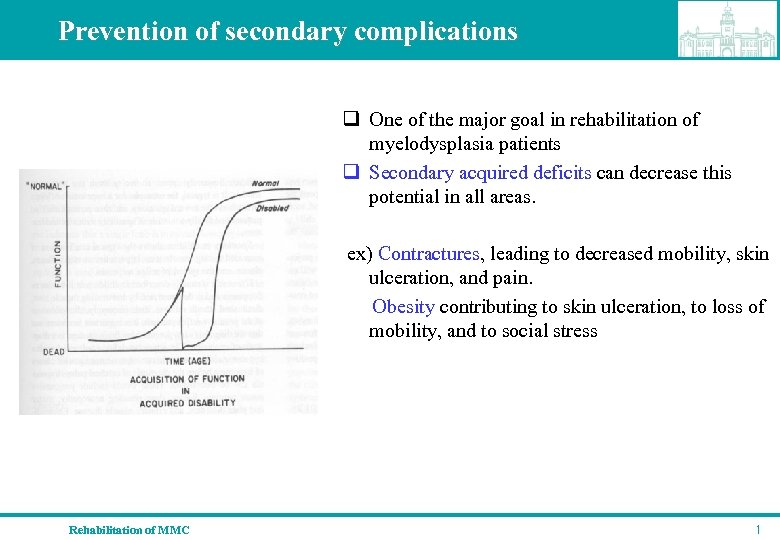
Prevention of secondary complications q One of the major goal in rehabilitation of myelodysplasia patients q Secondary acquired deficits can decrease this potential in all areas. ex) Contractures, leading to decreased mobility, skin ulceration, and pain. Obesity contributing to skin ulceration, to loss of mobility, and to social stress Rehabilitation of MMC 1

Rehabilitation approach q Comprehensive care; must begin when children with MMC are young q Individualized approach q Team approach; physical therapy, occupational therapy, proper orthosis and assistive device prescription, special education and etc. q Goal-directed approach should base on accurate evaluation; physical, exam, imaging, electrophysiologic study Rehabilitation of MMC 2
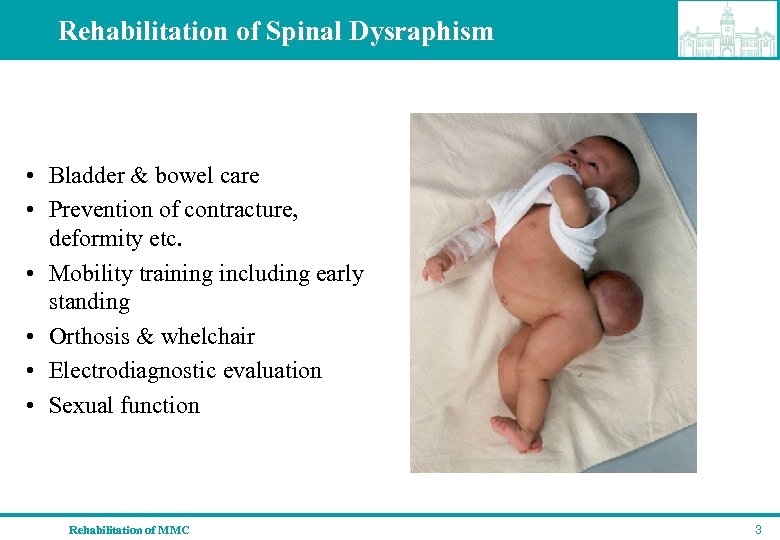
Rehabilitation of Spinal Dysraphism • Bladder & bowel care • Prevention of contracture, deformity etc. • Mobility training including early standing • Orthosis & whelchair • Electrodiagnostic evaluation • Sexual function Rehabilitation of MMC 3
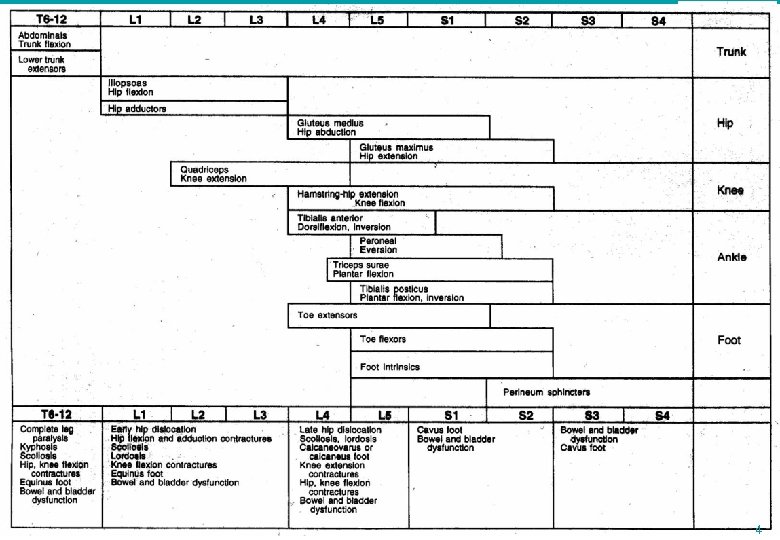
Rehabilitation of MMC 4

Clinical sign and course -motor paralysis- usually lower motor neuron type. combination of flaccid and spastic type; 10~40% two types of joint abnormalities (1) static, rigid deformities at birth (2) deformity developing over the years as a result of neurogenic muscle imbalance or improper positioning Rehabilitation of MMC 5

Motor paralysis q early accurate neurologic evaluation including diagnostic imaging study and electrophysiologic study(prerequisite for prognostic evaluation) q electrophysiologic study; more informative (NCS, needle EMG, SEP, BCRL) q both motor and sensory deficit may be different, incomplete, or asymmetric. Rehabilitation of MMC 6

Clinical signs by spinal level -thoracic lesionq intact upper extremity function q intercostals, abdominal, and back muscle weakness q kyphosis or kyphoscoliosis q often spastic lower extremity q partial hip external rotation, abduction, ankle plantar flexion from supine position q hip, knee flexion, and equinus foot deformities from sitting Rehabilitation of MMC 7
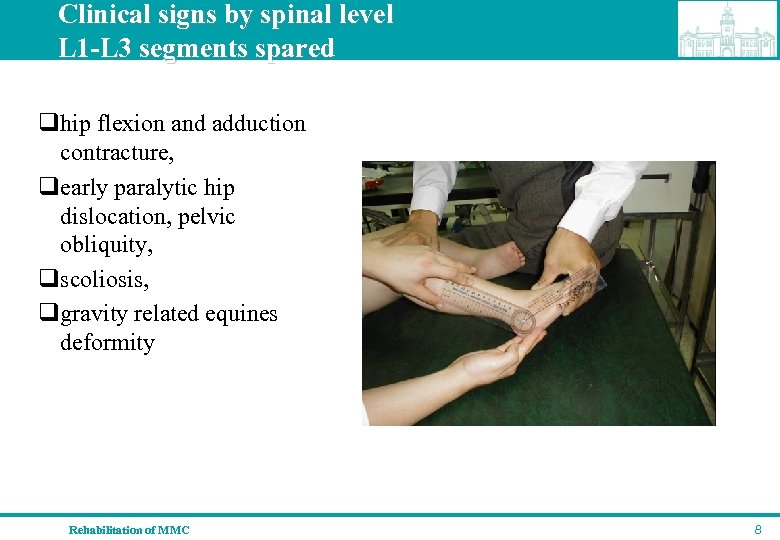
Clinical signs by spinal level L 1 -L 3 segments spared qhip flexion and adduction contracture, qearly paralytic hip dislocation, pelvic obliquity, qscoliosis, qgravity related equines deformity Rehabilitation of MMC 8
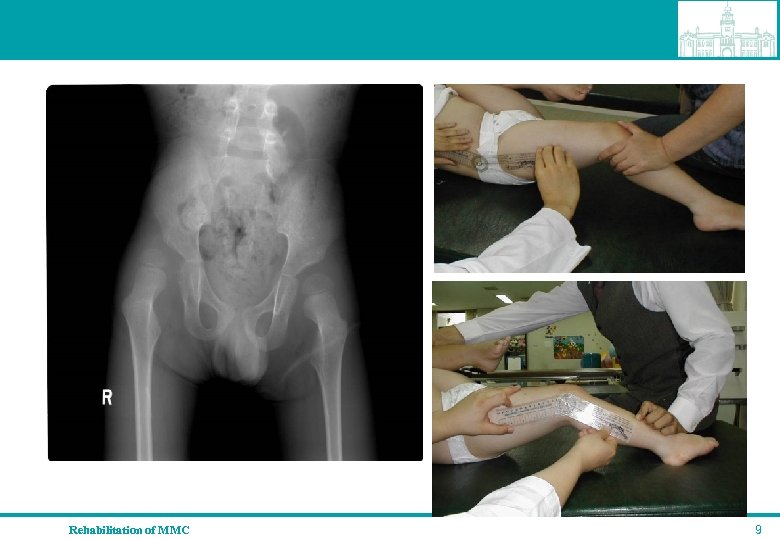
Rehabilitation of MMC 9
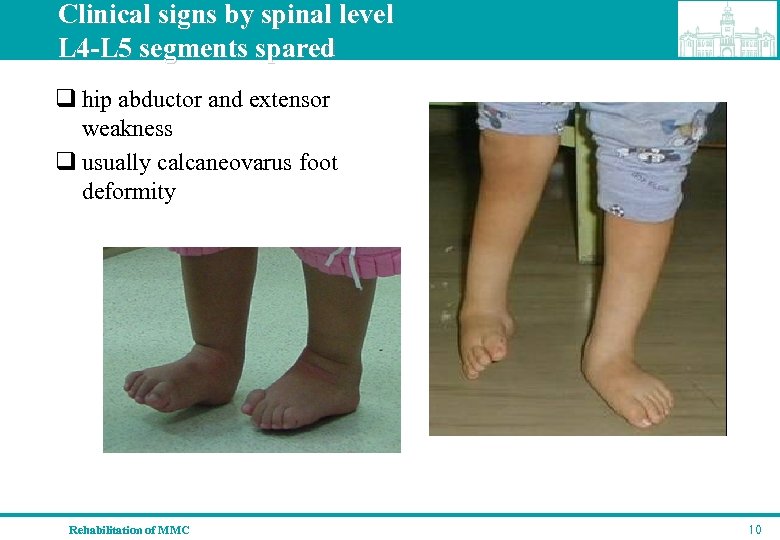
Clinical signs by spinal level L 4 -L 5 segments spared q hip abductor and extensor weakness q usually calcaneovarus foot deformity Rehabilitation of MMC 10
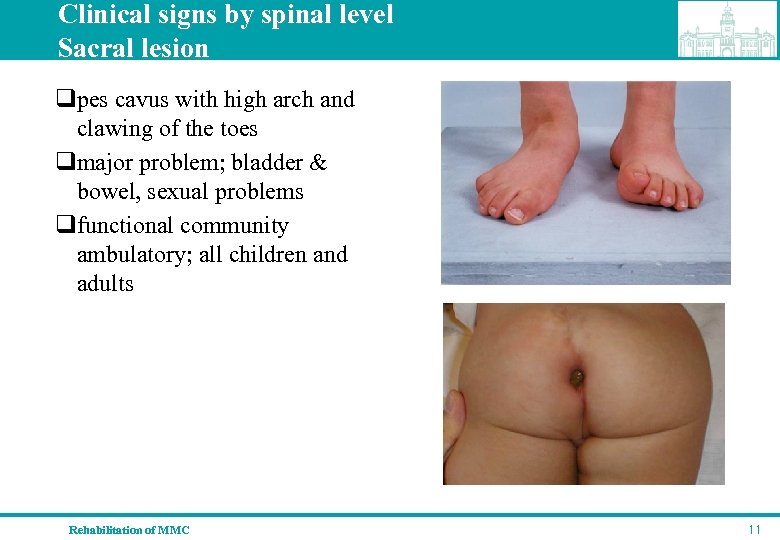
Clinical signs by spinal level Sacral lesion qpes cavus with high arch and clawing of the toes qmajor problem; bladder & bowel, sexual problems qfunctional community ambulatory; all children and adults Rehabilitation of MMC 11

consequences of denervation qvasomotor dysfunction decreased skin temperature over the involved area qasymmetric lower extremity growth qneuropathic charcot joint qosteoporosis; prevention; weight bearing by passive standing Rehabilitation of MMC 12
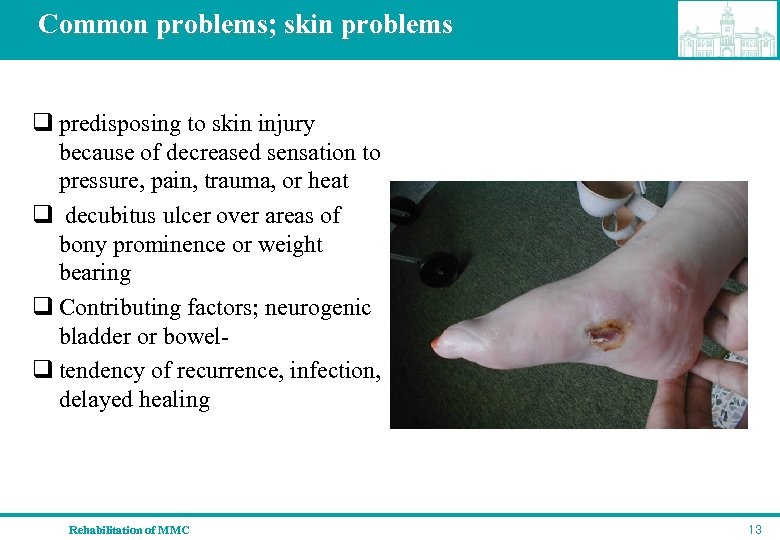
Common problems; skin problems q predisposing to skin injury because of decreased sensation to pressure, pain, trauma, or heat q decubitus ulcer over areas of bony prominence or weight bearing q Contributing factors; neurogenic bladder or bowel- q tendency of recurrence, infection, delayed healing Rehabilitation of MMC 13

skin problems qneurotrophic factor; healing of chronic wound after release of tethered cord qacute or chronic osteomyelitis qeducation of children and parents; touching with hand first, careful daily inspection, pressure relief qmost common complaints among patients with orthoses Rehabilitation of MMC 14

Influencing factor; obesity q short stature, short lower extremities as well as scoliosis and at times vertebral anomalies q heights; at or below the fifth percentile for age, weights; approximately the fiftieth percentile, weight-height ratio above the ninety-fifth percentile Rehabilitation of MMC 15

Obesity qin children with L 1–L 3 lesions; obesity; critical factor in the loss of ambulation qsecondary to decreased energy expenditure among non-ambulatory patients qhypothalamic-pituitary dysfunction may also play a role. Rehabilitation of MMC 16

Rehabilitation Therapy q. Physical therapy and occupational therapy; one of the first educational processes for a parent of an infant with spina bifida Rehabilitation of MMC 17

positioning and range of motion exercises q goals of positioning; to promote development and to prevent contractures q goal of maintaining functional joint range of motion; education pf parents from hospital, promotion of equilibrium responses and righting reactions. Rehabilitation of MMC 18

Rehabilitation therapy q developmental stimulation therapy; for the development of fine and gross motor skills, including coordination, designed to assist with both general childhood activities of daily living as well as mobility. q mobility training including crawling or scooting; depending on a child’s motor abilities, and progression to an upright mobility approach Rehabilitation of MMC 19

Self-care q self care including activity of daily living (ADL) should be monitored and encouraged q delay in ADL ; occupational therapy evaluation q OT sessions include training the children as well as parents q OT; necessary in extensive lower extremity paralysis and thoracic lesion to learn technique of dressing and other ADLs adapted to the home environment and other functional situation Rehabilitation of MMC 20

Orthotics in MMC q. Often without objective evidence of efficacy q. Influenced by practice pattern of geographic area (early instruction for walking) Rehabilitation of MMC 21

Principles of L/E orthotics 1. 2. 3. 4. Prevent deformity Support normal joint alignment and mechanics Provide variable range of motion when appropriate Facilitate function Rehabilitation of MMC 22

Standing frame q. Parapodium q. Swievel walker; for C 6 injured child Rehabilitation of MMC 23
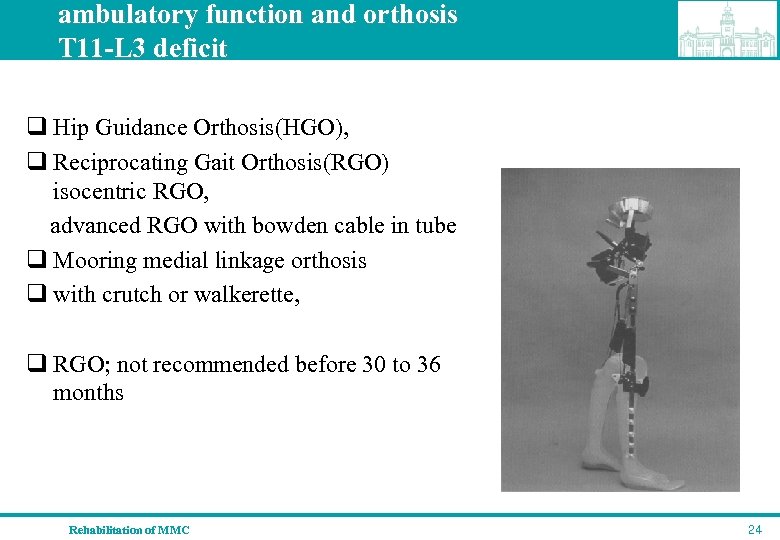
ambulatory function and orthosis T 11 -L 3 deficit q Hip Guidance Orthosis(HGO), q Reciprocating Gait Orthosis(RGO) isocentric RGO, advanced RGO with bowden cable in tube q Mooring medial linkage orthosis q with crutch or walkerette, q RGO; not recommended before 30 to 36 months Rehabilitation of MMC 24
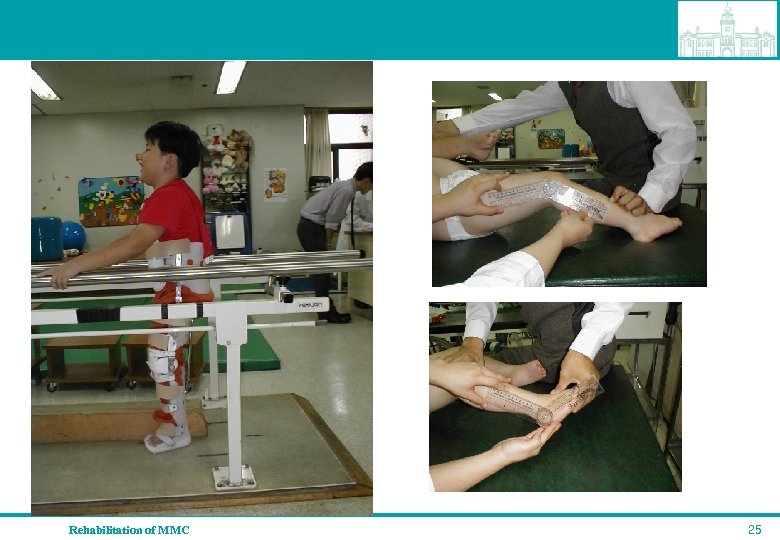
Rehabilitation of MMC 25
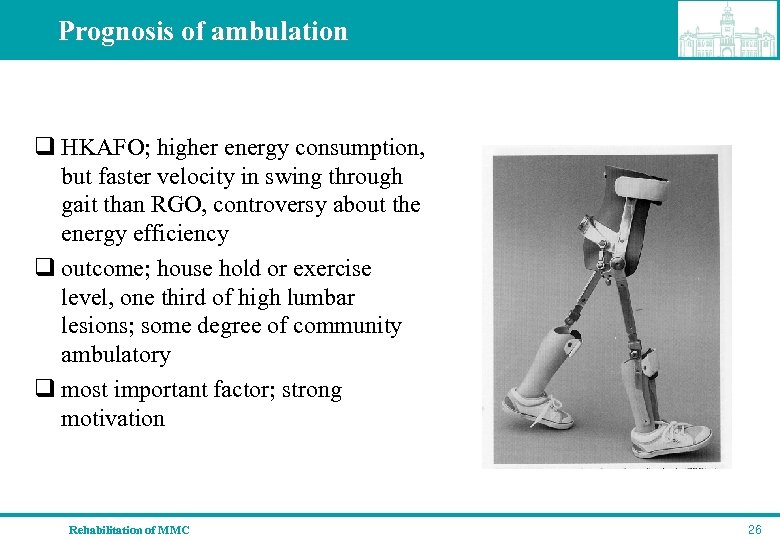
Prognosis of ambulation q HKAFO; higher energy consumption, but faster velocity in swing through gait than RGO, controversy about the energy efficiency q outcome; house hold or exercise level, one third of high lumbar lesions; some degree of community ambulatory q most important factor; strong motivation Rehabilitation of MMC 26

Effects of walking q. Subjects who walked as children fewer fractures & pressure ulcer more independent, better able to transfer than wheelchair user from early in life Rehabilitation of MMC 27
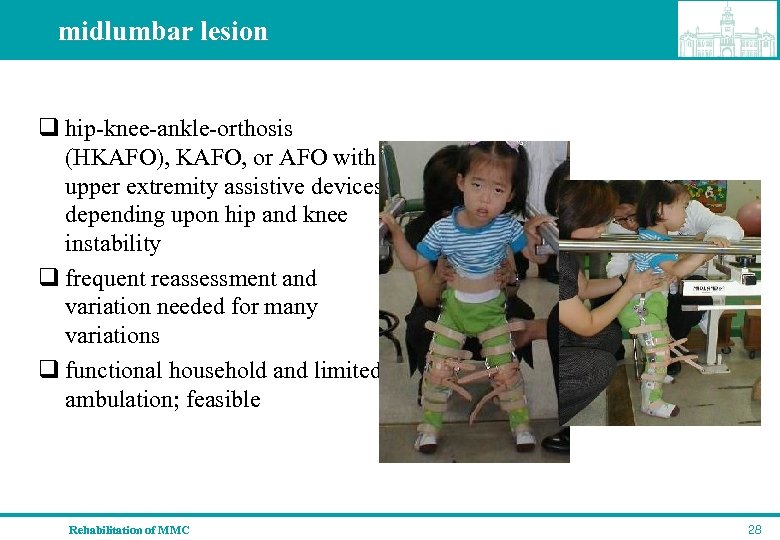
midlumbar lesion q hip-knee-ankle-orthosis (HKAFO), KAFO, or AFO with upper extremity assistive devices depending upon hip and knee instability q frequent reassessment and variation needed for many variations q functional household and limited ambulation; feasible Rehabilitation of MMC 28
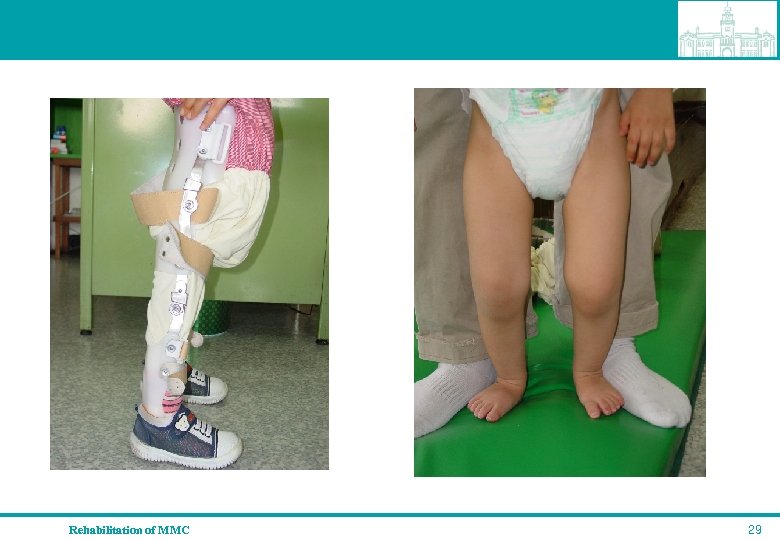
Rehabilitation of MMC 29
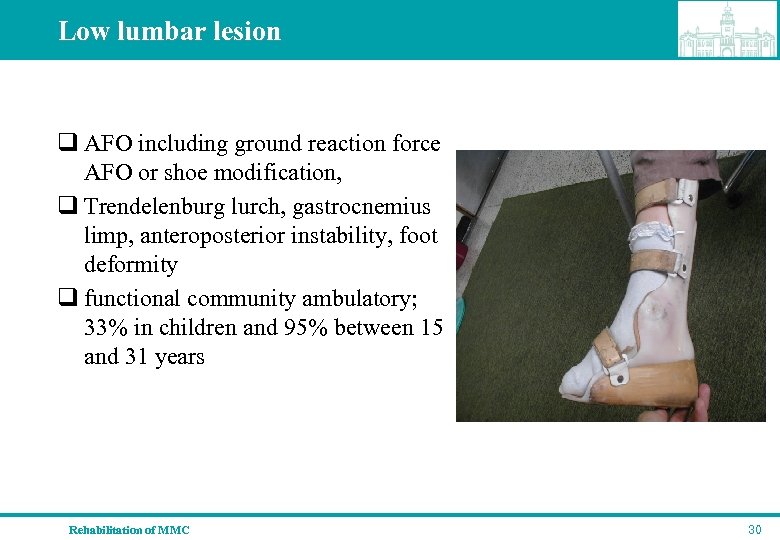
Low lumbar lesion q AFO including ground reaction force AFO or shoe modification, q Trendelenburg lurch, gastrocnemius limp, anteroposterior instability, foot deformity q functional community ambulatory; 33% in children and 95% between 15 and 31 years Rehabilitation of MMC 30

5 key componets of ankle & foot support q. Control of the subtalar joint q. Control of the mid tarsaljoint q. High(flexible) medial & lateral wall q. Toe elecation; intrsic or extrinsic q. Transmetatarsal arch Rehabilitation of MMC 31

AFO q. Conventional metal type q. Plastic type since 70’s good for molding medial or lateral wedge inserts Rehabilitation of MMC 32

AFO q. Common benefits improving knee(reduced excessive knee flexion) improving ankle(reduced excessive dorsiflexion) Park et al(1997) use of AFO decreased prolongation duration of muscle activity of knee extensor in stance phase(24 S level patients) – by gait analysis(surface EMG) Rehabilitation of MMC 33
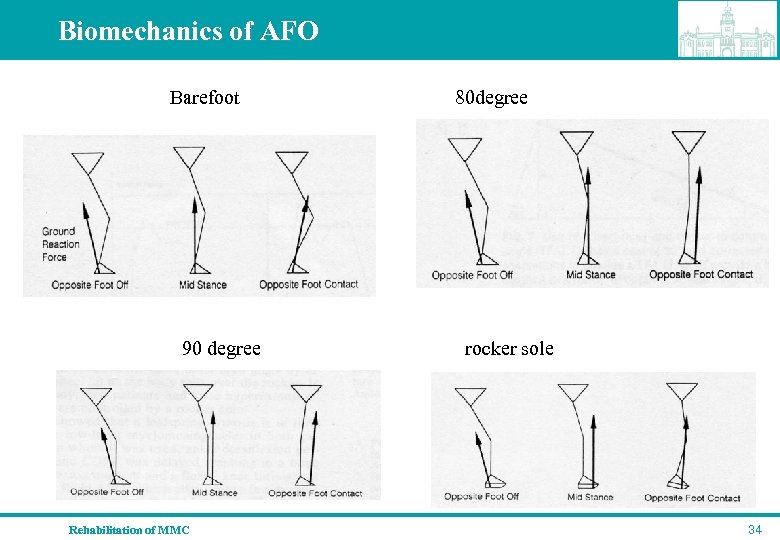
Biomechanics of AFO Barefoot 80 degree 90 degree rocker sole Rehabilitation of MMC 34
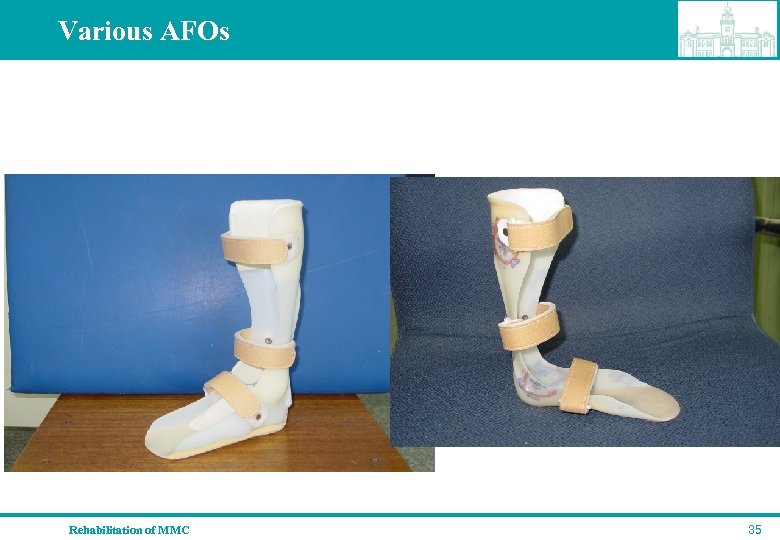
Various AFOs Rehabilitation of MMC 35

Various AFOs Rehabilitation of MMC 36

Various AFOs Rehabilitation of MMC 37
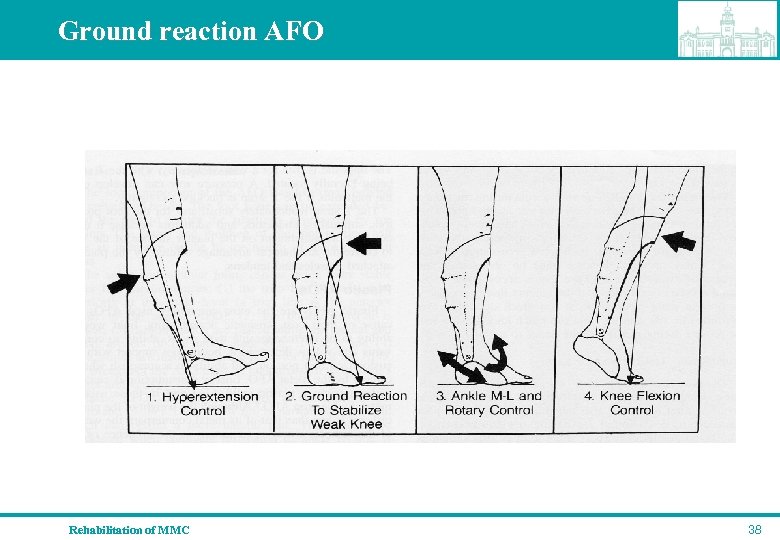
Ground reaction AFO Rehabilitation of MMC 38
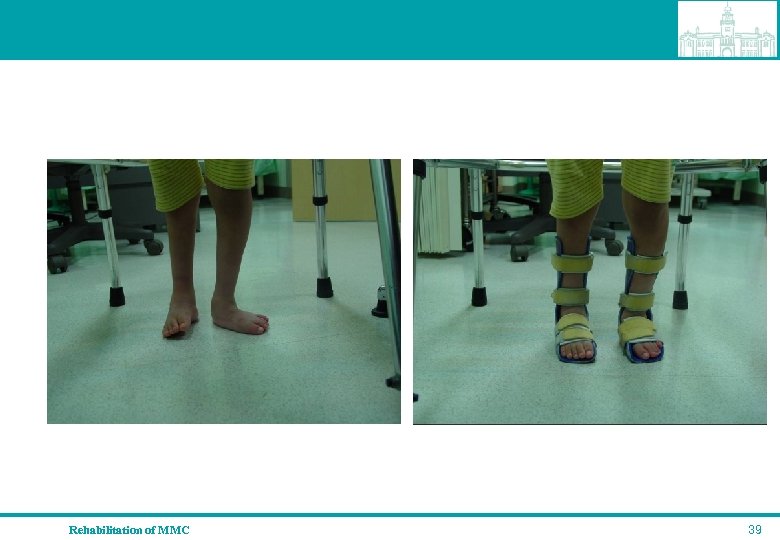
Rehabilitation of MMC 39
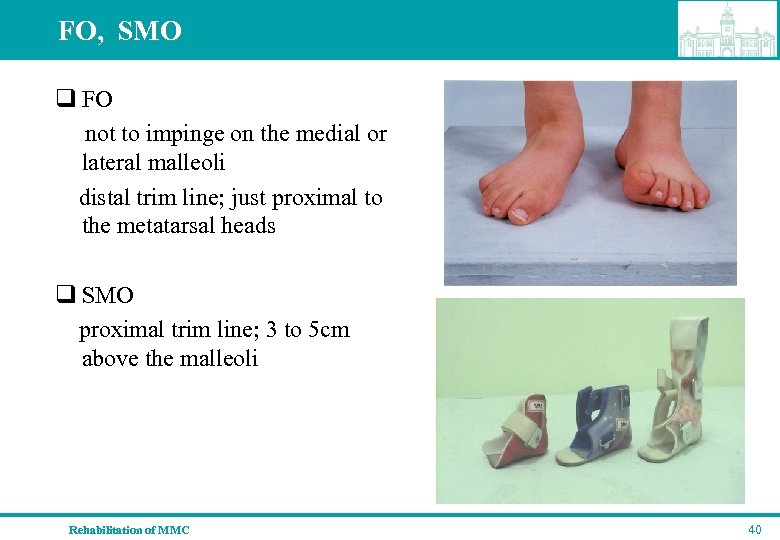
FO, SMO q FO not to impinge on the medial or lateral malleoli distal trim line; just proximal to the metatarsal heads q SMO proximal trim line; 3 to 5 cm above the malleoli Rehabilitation of MMC 40
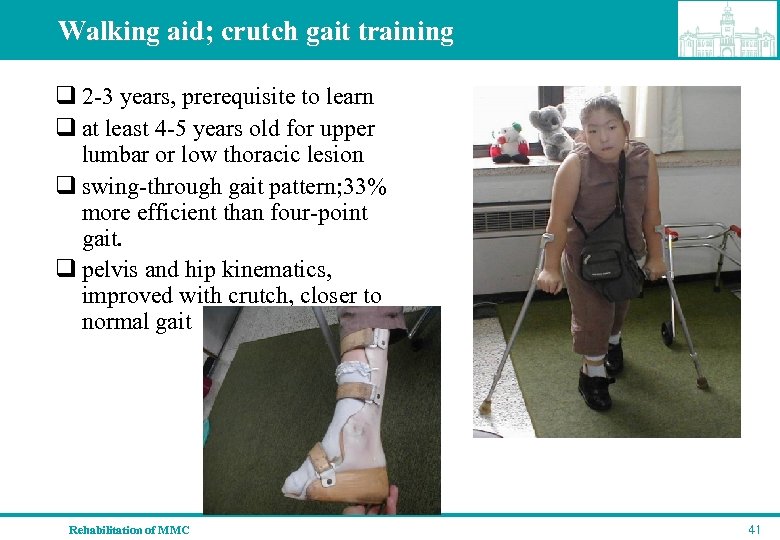
Walking aid; crutch gait training q 2 -3 years, prerequisite to learn q at least 4 -5 years old for upper lumbar or low thoracic lesion q swing-through gait pattern; 33% more efficient than four-point gait. q pelvis and hip kinematics, improved with crutch, closer to normal gait Rehabilitation of MMC 41
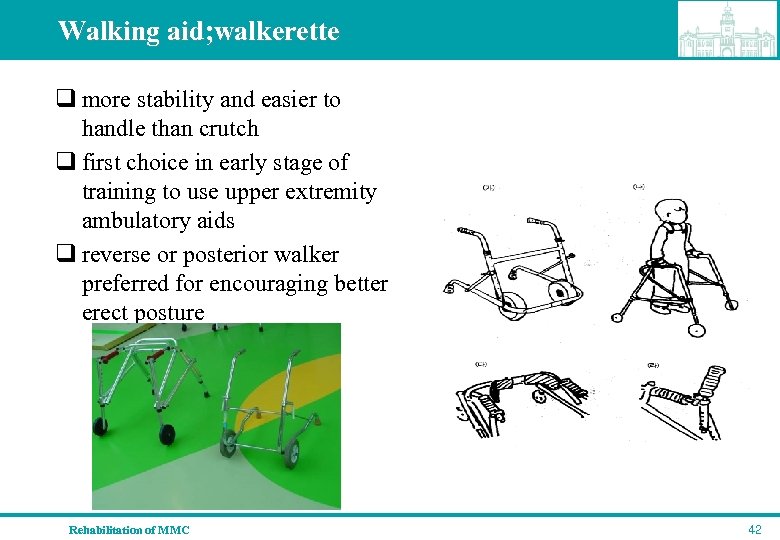
Walking aid; walkerette q more stability and easier to handle than crutch q first choice in early stage of training to use upper extremity ambulatory aids q reverse or posterior walker preferred for encouraging better erect posture Rehabilitation of MMC 42

Wheelchair use q may partial ambulators eventually give up walking for full time wheelchair use around adolescence q faster and more convenient for mobility q wheelchair training; beginning at age 2 q special seating support for anesthetic skin, useful for sports activity Rehabilitation of MMC 43

qmobility training including crawling or scooting; depending on a child’s motor abilities, and progression to an upright mobility approach Rehabilitation of MMC 44

Factors determining ambulatory function qneurologic level and active muscle activity, commonly the quadriceps qother important factors obesity, contractures or deformity(esp. hip), age, cognitive status, motivation qtype of spina bifida and other factors qearly predictors of walking; sitting balance and motor level qunfavorable factors; deformity of spine and obesity Rehabilitation of MMC 45

Reason for stop walking q. Neurologic deterioration q. Spasticity q. Knee & hip contracture q. Low back pain q. Lack of motivation q. Serious major medical events Rehabilitation of MMC 46

Spinal orthosis - goals of spine treatment - qmaintenance of a balanced trunk and pelvis to help maintain a seating position prevention of skin problems qpreservation of respiratory function and maximal trunk height Rehabilitation of MMC 47

Treatment of scoliosis: qbracing; with a curve of 20 degrees and progression of 5 degrees per year or more qpotential problems with bracing; compromised pulmonary function, skin problems, qand potential rib deformity qcustom-molded thoracolumbosacral orthosis; most common, then Boston brace Rehabilitation of MMC 48

Congenital kyphosis(gibbus) Incidence; approximately 10% in patients with MMC Problems caused by kyphosis qskin ulceration at the most prominent portion qrespiratory difficulty due to decreased lung cavity size qcompression of abdominal contents qseating problems qdecreased urologic function qdecreased ability to use the hands well secondary to requiring increased use of the hands for balance Rehabilitation of MMC 49

Cogenital Kyphosis Bracing impractical for long-term care because of skin ulceration and compression of abdominal structures Goals of surgery skin protection, improved sitting posture, and increased upper-extremity use, along with preservation of pulmonary and abdominal cavity area. Rehabilitation of MMC 50
1c0bd76edff9832a56d90d3836411edb.ppt