76bedf2f09a1be2d4d00a34625f72f86.ppt
- Количество слайдов: 23
 Palliative Care in CKD Patients Peenida Skulratanasak Division of Nephrology, Siriraj hospital
Palliative Care in CKD Patients Peenida Skulratanasak Division of Nephrology, Siriraj hospital
 Therapeutic Options in CKD Renal replacement therapy Hemodialysis Peritoneal dialysis Kidney transplantation Vascular access TK insertion LRKT/DDKT
Therapeutic Options in CKD Renal replacement therapy Hemodialysis Peritoneal dialysis Kidney transplantation Vascular access TK insertion LRKT/DDKT
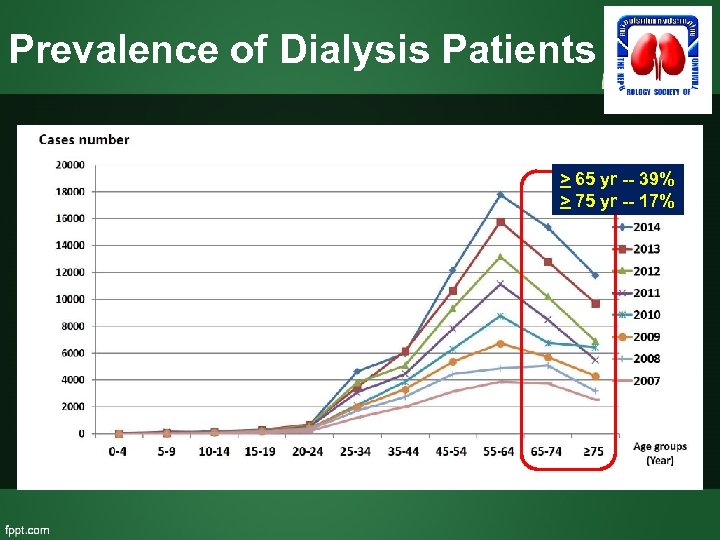 Prevalence of Dialysis Patients > 65 yr -- 39% > 75 yr -- 17%
Prevalence of Dialysis Patients > 65 yr -- 39% > 75 yr -- 17%
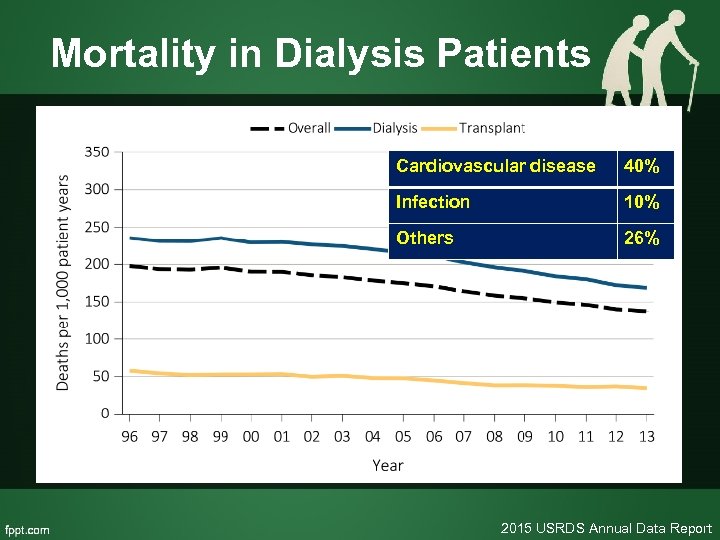 Mortality in Dialysis Patients Cardiovascular disease 40% Infection 10% Others 26% 2015 USRDS Annual Data Report
Mortality in Dialysis Patients Cardiovascular disease 40% Infection 10% Others 26% 2015 USRDS Annual Data Report
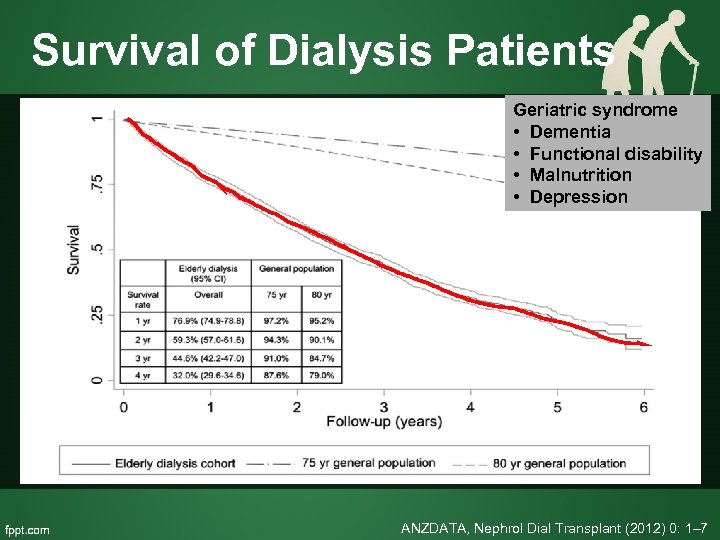 Survival of Dialysis Patients Geriatric syndrome • Dementia • Functional disability • Malnutrition • Depression ANZDATA, Nephrol Dial Transplant (2012) 0: 1– 7
Survival of Dialysis Patients Geriatric syndrome • Dementia • Functional disability • Malnutrition • Depression ANZDATA, Nephrol Dial Transplant (2012) 0: 1– 7
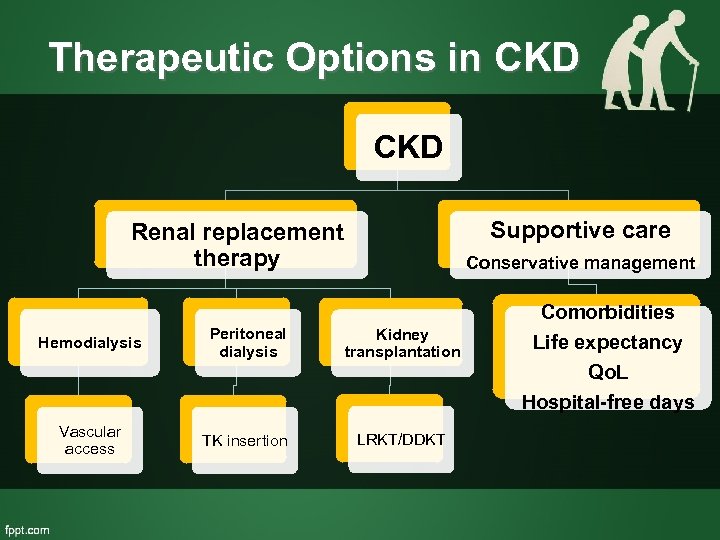 Therapeutic Options in CKD Supportive care Renal replacement therapy Hemodialysis Peritoneal dialysis Conservative management Kidney transplantation Comorbidities Life expectancy Qo. L Hospital-free days Vascular access TK insertion LRKT/DDKT
Therapeutic Options in CKD Supportive care Renal replacement therapy Hemodialysis Peritoneal dialysis Conservative management Kidney transplantation Comorbidities Life expectancy Qo. L Hospital-free days Vascular access TK insertion LRKT/DDKT
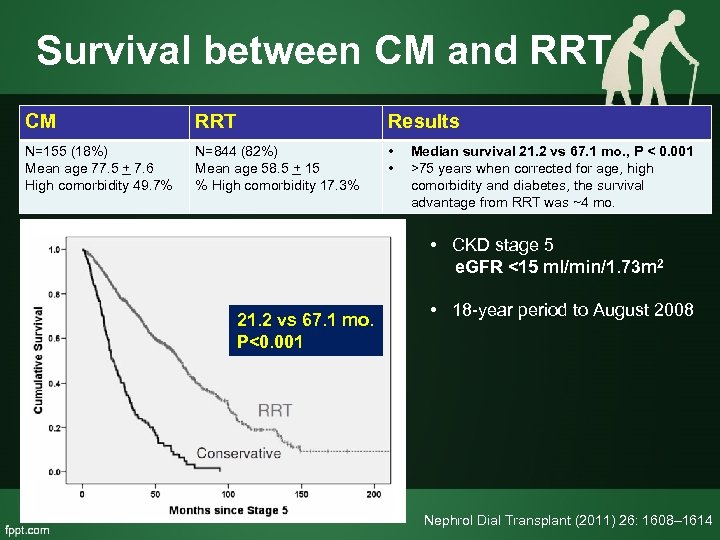 Survival between CM and RRT CM RRT Results N=155 (18%) Mean age 77. 5 + 7. 6 High comorbidity 49. 7% N=844 (82%) Mean age 58. 5 + 15 % High comorbidity 17. 3% • • Median survival 21. 2 vs 67. 1 mo. , P < 0. 001 >75 years when corrected for age, high comorbidity and diabetes, the survival advantage from RRT was ~4 mo. • CKD stage 5 e. GFR <15 ml/min/1. 73 m 2 21. 2 vs 67. 1 mo. P<0. 001 • 18 -year period to August 2008 Nephrol Dial Transplant (2011) 26: 1608– 1614
Survival between CM and RRT CM RRT Results N=155 (18%) Mean age 77. 5 + 7. 6 High comorbidity 49. 7% N=844 (82%) Mean age 58. 5 + 15 % High comorbidity 17. 3% • • Median survival 21. 2 vs 67. 1 mo. , P < 0. 001 >75 years when corrected for age, high comorbidity and diabetes, the survival advantage from RRT was ~4 mo. • CKD stage 5 e. GFR <15 ml/min/1. 73 m 2 21. 2 vs 67. 1 mo. P<0. 001 • 18 -year period to August 2008 Nephrol Dial Transplant (2011) 26: 1608– 1614
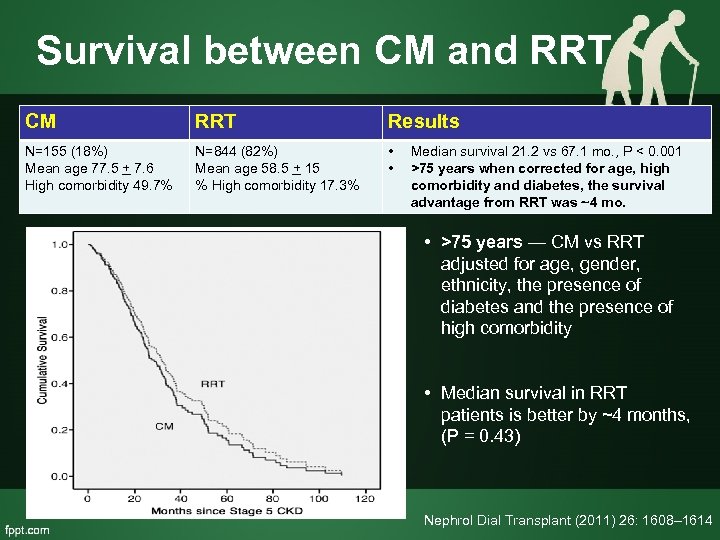 Survival between CM and RRT CM RRT Results N=155 (18%) Mean age 77. 5 + 7. 6 High comorbidity 49. 7% N=844 (82%) Mean age 58. 5 + 15 % High comorbidity 17. 3% • • Median survival 21. 2 vs 67. 1 mo. , P < 0. 001 >75 years when corrected for age, high comorbidity and diabetes, the survival advantage from RRT was ~4 mo. • >75 years — CM vs RRT adjusted for age, gender, ethnicity, the presence of diabetes and the presence of high comorbidity • Median survival in RRT patients is better by ~4 months, (P = 0. 43) Nephrol Dial Transplant (2011) 26: 1608– 1614
Survival between CM and RRT CM RRT Results N=155 (18%) Mean age 77. 5 + 7. 6 High comorbidity 49. 7% N=844 (82%) Mean age 58. 5 + 15 % High comorbidity 17. 3% • • Median survival 21. 2 vs 67. 1 mo. , P < 0. 001 >75 years when corrected for age, high comorbidity and diabetes, the survival advantage from RRT was ~4 mo. • >75 years — CM vs RRT adjusted for age, gender, ethnicity, the presence of diabetes and the presence of high comorbidity • Median survival in RRT patients is better by ~4 months, (P = 0. 43) Nephrol Dial Transplant (2011) 26: 1608– 1614
 Prognostic Tools for Elderly • Hemodialysis Mortality Predictor – Touchcalc • Charlson Comorbidity Index • Karnofsky Performance Status • WHO Performance Status
Prognostic Tools for Elderly • Hemodialysis Mortality Predictor – Touchcalc • Charlson Comorbidity Index • Karnofsky Performance Status • WHO Performance Status
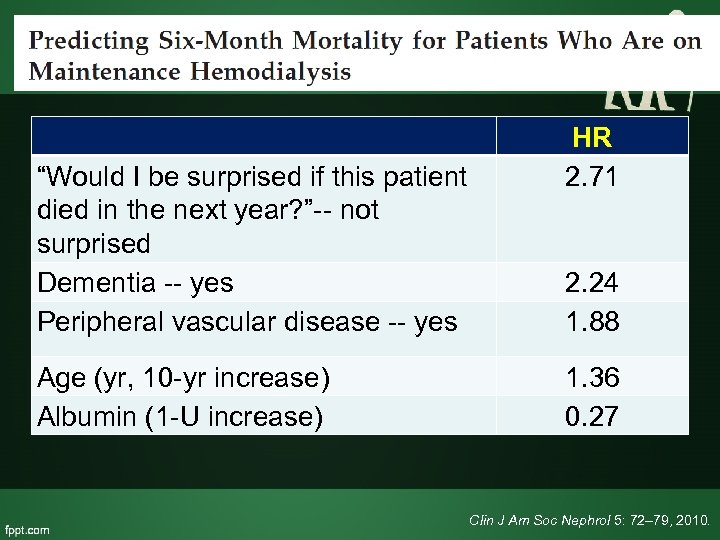 “Would I be surprised if this patient died in the next year? ”-- not surprised Dementia -- yes Peripheral vascular disease -- yes Age (yr, 10 -yr increase) Albumin (1 -U increase) HR 2. 71 2. 24 1. 88 1. 36 0. 27 Clin J Am Soc Nephrol 5: 72– 79, 2010.
“Would I be surprised if this patient died in the next year? ”-- not surprised Dementia -- yes Peripheral vascular disease -- yes Age (yr, 10 -yr increase) Albumin (1 -U increase) HR 2. 71 2. 24 1. 88 1. 36 0. 27 Clin J Am Soc Nephrol 5: 72– 79, 2010.
 HD Mortality Predictor http: //touchcalc. com/c alculators/sq Clin J Am Soc Nephrol 2010; 5: 72 -9
HD Mortality Predictor http: //touchcalc. com/c alculators/sq Clin J Am Soc Nephrol 2010; 5: 72 -9
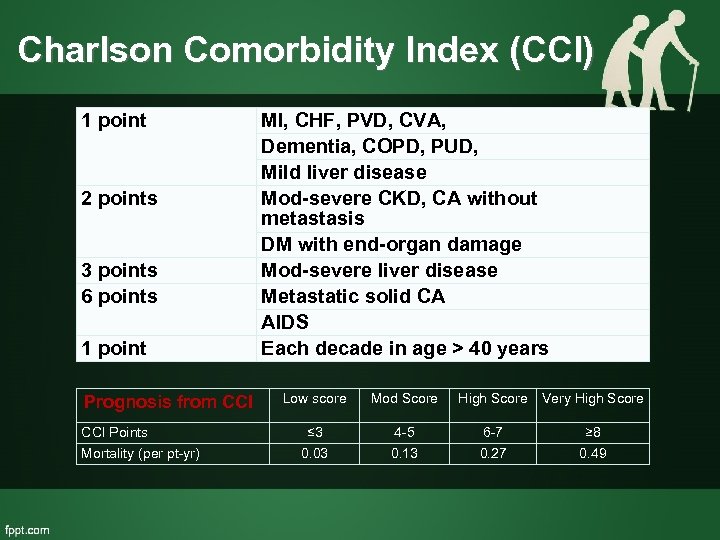 Charlson Comorbidity Index (CCI) 1 point 2 points 3 points 6 points 1 point Prognosis from CCI Points Mortality (per pt-yr) MI, CHF, PVD, CVA, Dementia, COPD, PUD, Mild liver disease Mod-severe CKD, CA without metastasis DM with end-organ damage Mod-severe liver disease Metastatic solid CA AIDS Each decade in age > 40 years Low score Mod Score High Score Very High Score ≤ 3 0. 03 4 -5 0. 13 6 -7 0. 27 ≥ 8 0. 49
Charlson Comorbidity Index (CCI) 1 point 2 points 3 points 6 points 1 point Prognosis from CCI Points Mortality (per pt-yr) MI, CHF, PVD, CVA, Dementia, COPD, PUD, Mild liver disease Mod-severe CKD, CA without metastasis DM with end-organ damage Mod-severe liver disease Metastatic solid CA AIDS Each decade in age > 40 years Low score Mod Score High Score Very High Score ≤ 3 0. 03 4 -5 0. 13 6 -7 0. 27 ≥ 8 0. 49
 Charlson Comorbidity Index (CCI) 1 point MI, CHF, PVD, CVA, Dementia, COPD, PUD, Mild liver disease 2 points Mod-severe CKD, CA without metastasis DM with end-organ damage 3 points Mod-severe liver disease 6 points Metastatic solid CA AIDS 1 point Each decade in age > 40 years Female 75 years old with underlying disease - DM with diabetic nephropathy - Chronic kidney disease - History of CVA Age – 3 points DM – 2 points CKD – 2 points CVA – 1 point CCI – 8 points
Charlson Comorbidity Index (CCI) 1 point MI, CHF, PVD, CVA, Dementia, COPD, PUD, Mild liver disease 2 points Mod-severe CKD, CA without metastasis DM with end-organ damage 3 points Mod-severe liver disease 6 points Metastatic solid CA AIDS 1 point Each decade in age > 40 years Female 75 years old with underlying disease - DM with diabetic nephropathy - Chronic kidney disease - History of CVA Age – 3 points DM – 2 points CKD – 2 points CVA – 1 point CCI – 8 points
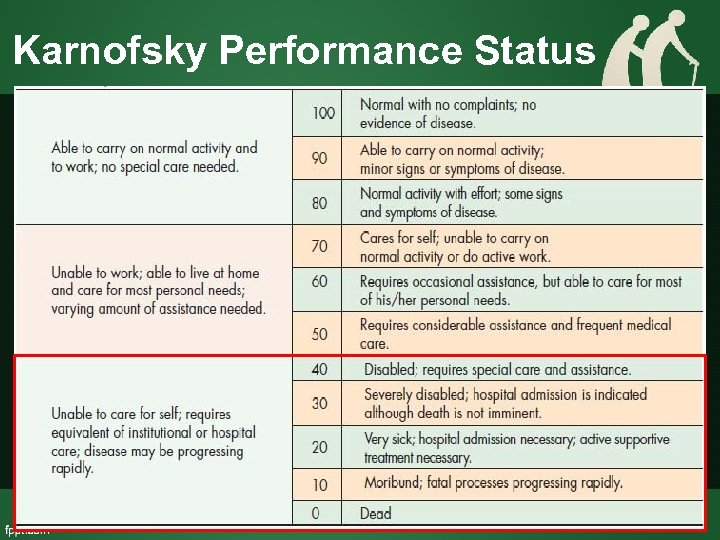 Karnofsky Performance Status
Karnofsky Performance Status
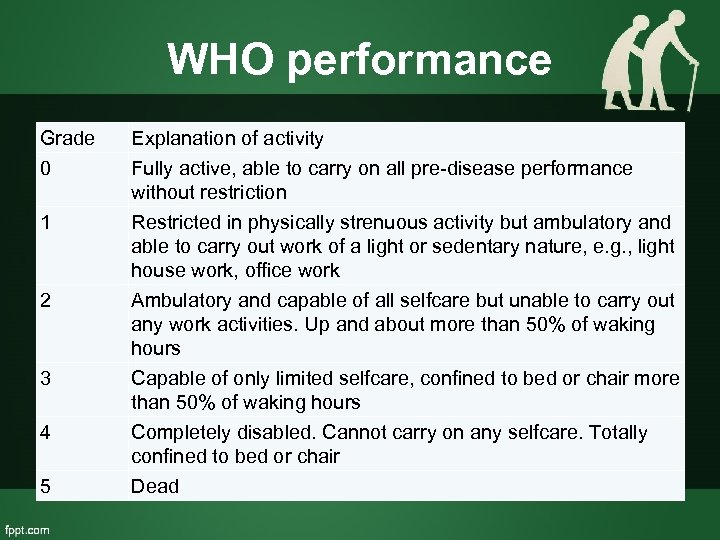 WHO performance Grade 0 1 2 3 4 5 Explanation of activity Fully active, able to carry on all pre-disease performance without restriction Restricted in physically strenuous activity but ambulatory and able to carry out work of a light or sedentary nature, e. g. , light house work, office work Ambulatory and capable of all selfcare but unable to carry out any work activities. Up and about more than 50% of waking hours Capable of only limited selfcare, confined to bed or chair more than 50% of waking hours Completely disabled. Cannot carry on any selfcare. Totally confined to bed or chair Dead
WHO performance Grade 0 1 2 3 4 5 Explanation of activity Fully active, able to carry on all pre-disease performance without restriction Restricted in physically strenuous activity but ambulatory and able to carry out work of a light or sedentary nature, e. g. , light house work, office work Ambulatory and capable of all selfcare but unable to carry out any work activities. Up and about more than 50% of waking hours Capable of only limited selfcare, confined to bed or chair more than 50% of waking hours Completely disabled. Cannot carry on any selfcare. Totally confined to bed or chair Dead
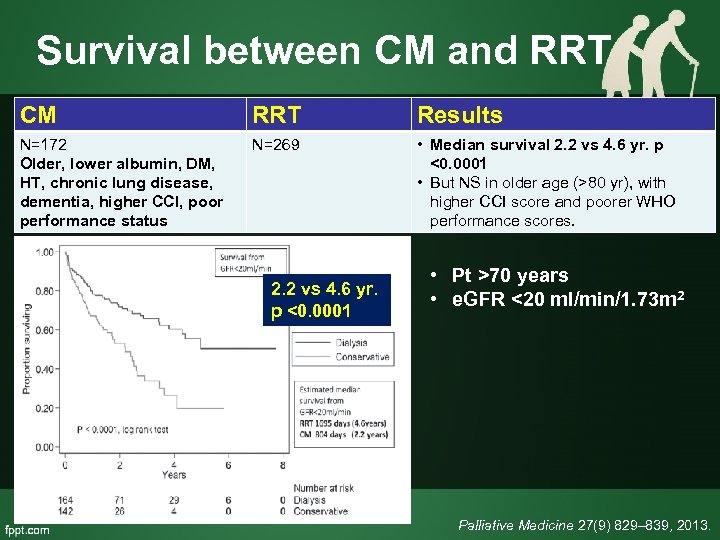 Survival between CM and RRT CM RRT Results N=172 Older, lower albumin, DM, HT, chronic lung disease, dementia, higher CCI, poor performance status N=269 • Median survival 2. 2 vs 4. 6 yr. p <0. 0001 • But NS in older age (>80 yr), with higher CCI score and poorer WHO performance scores. 2. 2 vs 4. 6 yr. p <0. 0001 • Pt >70 years • e. GFR <20 ml/min/1. 73 m 2 Palliative Medicine 27(9) 829– 839, 2013.
Survival between CM and RRT CM RRT Results N=172 Older, lower albumin, DM, HT, chronic lung disease, dementia, higher CCI, poor performance status N=269 • Median survival 2. 2 vs 4. 6 yr. p <0. 0001 • But NS in older age (>80 yr), with higher CCI score and poorer WHO performance scores. 2. 2 vs 4. 6 yr. p <0. 0001 • Pt >70 years • e. GFR <20 ml/min/1. 73 m 2 Palliative Medicine 27(9) 829– 839, 2013.
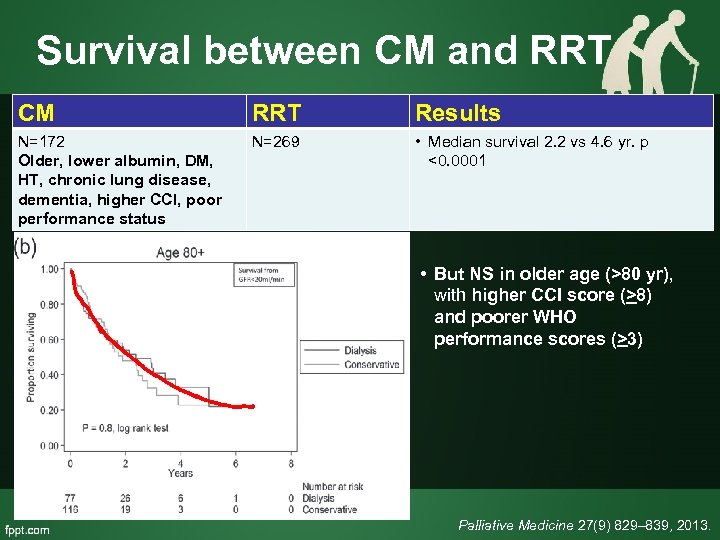 Survival between CM and RRT CM RRT Results N=172 Older, lower albumin, DM, HT, chronic lung disease, dementia, higher CCI, poor performance status N=269 • Median survival 2. 2 vs 4. 6 yr. p <0. 0001 • But NS in older age (>80 yr), with higher CCI score (>8) and poorer WHO performance scores (>3) Palliative Medicine 27(9) 829– 839, 2013.
Survival between CM and RRT CM RRT Results N=172 Older, lower albumin, DM, HT, chronic lung disease, dementia, higher CCI, poor performance status N=269 • Median survival 2. 2 vs 4. 6 yr. p <0. 0001 • But NS in older age (>80 yr), with higher CCI score (>8) and poorer WHO performance scores (>3) Palliative Medicine 27(9) 829– 839, 2013.
 • • Optimize Qo. L Avoid unnecessary hospitalizations Hospital-free day Control symptoms • A prospective study from the UK – Conservative management – Patient survival of 1. 95 years, with a 1 year survival rate of 65% – 60% of these patients did not have any hospital admissions over the 3 -year follow-up Ren. Fail. 29(6), 653– 659 (2007)
• • Optimize Qo. L Avoid unnecessary hospitalizations Hospital-free day Control symptoms • A prospective study from the UK – Conservative management – Patient survival of 1. 95 years, with a 1 year survival rate of 65% – 60% of these patients did not have any hospital admissions over the 3 -year follow-up Ren. Fail. 29(6), 653– 659 (2007)
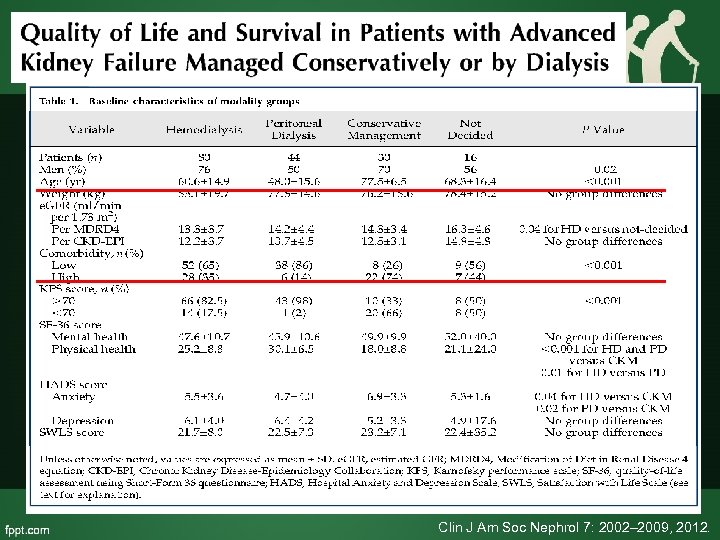 • Quality of life assessment – SF-36 mental health and physical health – HADS: Hospital anxiety and depression scale – SWLS: Satisfaction with life scale Clin J Am Soc Nephrol 7: 2002– 2009, 2012.
• Quality of life assessment – SF-36 mental health and physical health – HADS: Hospital anxiety and depression scale – SWLS: Satisfaction with life scale Clin J Am Soc Nephrol 7: 2002– 2009, 2012.
 • Multilevel growth models demonstrated no serial change in quality-of-life measures • Starting dialysis led to a significant decrease in the SWLS score Clin J Am Soc Nephrol 7: 2002– 2009, 2012.
• Multilevel growth models demonstrated no serial change in quality-of-life measures • Starting dialysis led to a significant decrease in the SWLS score Clin J Am Soc Nephrol 7: 2002– 2009, 2012.
 Comorbidities Performance status Age Survival Quality of life Hospitalization
Comorbidities Performance status Age Survival Quality of life Hospitalization
 Elderly Population in the Future Elderly people 30% 21 million people Present – Dialysis pt. 1, 200 pmp In 2574 – Predicted dialysis pt. 3, 325 pmp -- Predicted elderly dialysis pt. 1, 330 pmp สำนกงานคณะกรรมการพฒนาเศรษฐกจและสงคมแหงชาต
Elderly Population in the Future Elderly people 30% 21 million people Present – Dialysis pt. 1, 200 pmp In 2574 – Predicted dialysis pt. 3, 325 pmp -- Predicted elderly dialysis pt. 1, 330 pmp สำนกงานคณะกรรมการพฒนาเศรษฐกจและสงคมแหงชาต
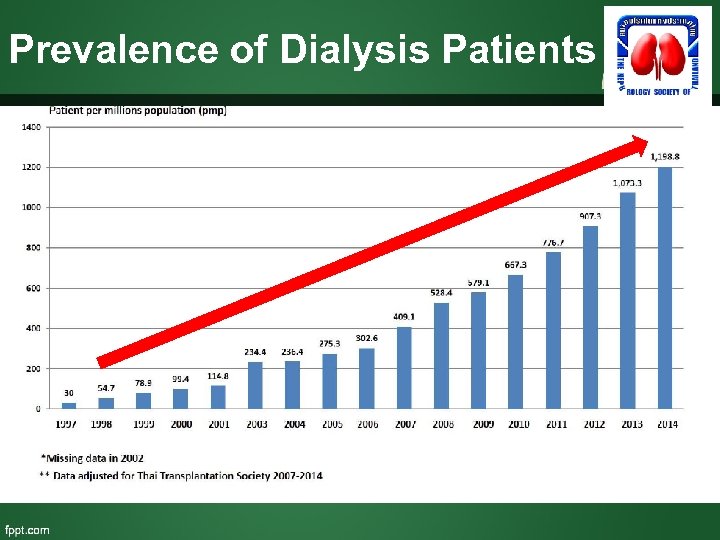 Prevalence of Dialysis Patients
Prevalence of Dialysis Patients


