163c2bac42b5dfd78997e0162fc0e3ed.ppt
- Количество слайдов: 43
 Palliative Care Home Visit Curriculum Department of Family Medicine Mayo Clinic Florida 2008 -2010
Palliative Care Home Visit Curriculum Department of Family Medicine Mayo Clinic Florida 2008 -2010
 Overview Importance of Home Visits/Palliative Medicine for Family Medicine Home Visit Checklist Documenting and Coding Fast Facts Resources
Overview Importance of Home Visits/Palliative Medicine for Family Medicine Home Visit Checklist Documenting and Coding Fast Facts Resources
 Why Home Visits? Provides a unique perspective on your patient and their health. Allows you to get out of the office. The ACGME requires it! For More Information on Home Visits and Family Medicine: – “The Home Visit” American Family Physician October 1, 1999. http: //www. aafp. org/afp/991001 ap/1481. html – “House Calls: Taking the Practice to the Patient” Family Practice Management June 2000. http: //www. aafp. org/fpm/20000600/49 hous. html
Why Home Visits? Provides a unique perspective on your patient and their health. Allows you to get out of the office. The ACGME requires it! For More Information on Home Visits and Family Medicine: – “The Home Visit” American Family Physician October 1, 1999. http: //www. aafp. org/afp/991001 ap/1481. html – “House Calls: Taking the Practice to the Patient” Family Practice Management June 2000. http: //www. aafp. org/fpm/20000600/49 hous. html
 Why Palliative Medicine? The Home Visit provides the ideal setting for learning Palliative Medicine principles because the majority of end-of-life care occurs in the home setting.
Why Palliative Medicine? The Home Visit provides the ideal setting for learning Palliative Medicine principles because the majority of end-of-life care occurs in the home setting.
 Home Visit Checklist I Immobility N Nutrition H Housing O Other People M Medications E Examination S Safety S Spiritual Health S Services by Home Health Agencies http: //www. aafp. org/afp/991001 ap/1481. html
Home Visit Checklist I Immobility N Nutrition H Housing O Other People M Medications E Examination S Safety S Spiritual Health S Services by Home Health Agencies http: //www. aafp. org/afp/991001 ap/1481. html
 Immobility Activities of Daily Living Evaluate Functional Activities Getting In and Out of Car Opening Pill Bottle Opening Front Door
Immobility Activities of Daily Living Evaluate Functional Activities Getting In and Out of Car Opening Pill Bottle Opening Front Door
 Katz’s Functional Status Basic ADL’s – – – Bathing Dressing Toileting Transfers Continence Feeding Instrumental ADL’s – – – – Travel Shopping Meal Preparation Housekeeping Laundry Managing Money Telephone Use Taking Medicine
Katz’s Functional Status Basic ADL’s – – – Bathing Dressing Toileting Transfers Continence Feeding Instrumental ADL’s – – – – Travel Shopping Meal Preparation Housekeeping Laundry Managing Money Telephone Use Taking Medicine
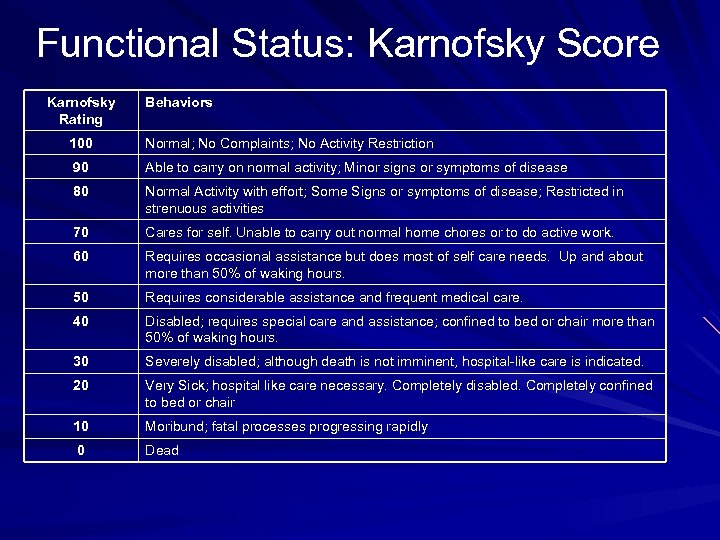 Functional Status: Karnofsky Score Karnofsky Rating Behaviors 100 Normal; No Complaints; No Activity Restriction 90 Able to carry on normal activity; Minor signs or symptoms of disease 80 Normal Activity with effort; Some Signs or symptoms of disease; Restricted in strenuous activities 70 Cares for self. Unable to carry out normal home chores or to do active work. 60 Requires occasional assistance but does most of self care needs. Up and about more than 50% of waking hours. 50 Requires considerable assistance and frequent medical care. 40 Disabled; requires special care and assistance; confined to bed or chair more than 50% of waking hours. 30 Severely disabled; although death is not imminent, hospital-like care is indicated. 20 Very Sick; hospital like care necessary. Completely disabled. Completely confined to bed or chair 10 Moribund; fatal processes progressing rapidly 0 Dead
Functional Status: Karnofsky Score Karnofsky Rating Behaviors 100 Normal; No Complaints; No Activity Restriction 90 Able to carry on normal activity; Minor signs or symptoms of disease 80 Normal Activity with effort; Some Signs or symptoms of disease; Restricted in strenuous activities 70 Cares for self. Unable to carry out normal home chores or to do active work. 60 Requires occasional assistance but does most of self care needs. Up and about more than 50% of waking hours. 50 Requires considerable assistance and frequent medical care. 40 Disabled; requires special care and assistance; confined to bed or chair more than 50% of waking hours. 30 Severely disabled; although death is not imminent, hospital-like care is indicated. 20 Very Sick; hospital like care necessary. Completely disabled. Completely confined to bed or chair 10 Moribund; fatal processes progressing rapidly 0 Dead
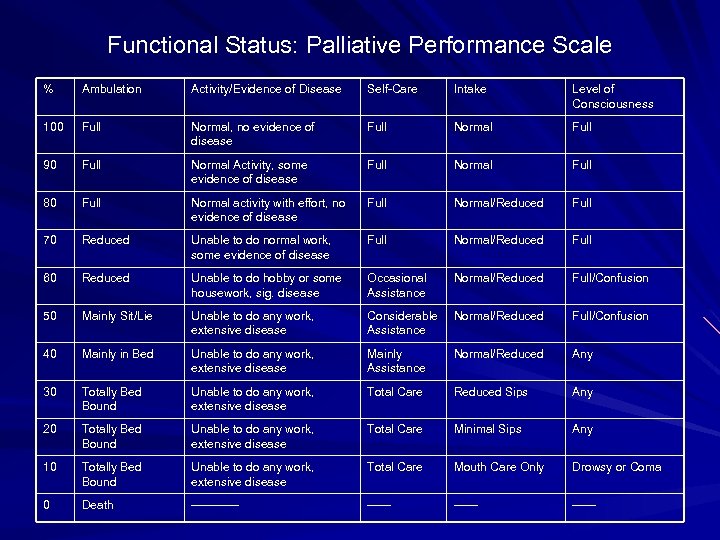 Functional Status: Palliative Performance Scale % Ambulation Activity/Evidence of Disease Self-Care Intake Level of Consciousness 100 Full Normal, no evidence of disease Full Normal Full 90 Full Normal Activity, some evidence of disease Full Normal Full 80 Full Normal activity with effort, no evidence of disease Full Normal/Reduced Full 70 Reduced Unable to do normal work, some evidence of disease Full Normal/Reduced Full 60 Reduced Unable to do hobby or some housework, sig. disease Occasional Assistance Normal/Reduced Full/Confusion 50 Mainly Sit/Lie Unable to do any work, extensive disease Considerable Normal/Reduced Assistance Full/Confusion 40 Mainly in Bed Unable to do any work, extensive disease Mainly Assistance Normal/Reduced Any 30 Totally Bed Bound Unable to do any work, extensive disease Total Care Reduced Sips Any 20 Totally Bed Bound Unable to do any work, extensive disease Total Care Minimal Sips Any 10 Totally Bed Bound Unable to do any work, extensive disease Total Care Mouth Care Only Drowsy or Coma 0 Death ------ ------
Functional Status: Palliative Performance Scale % Ambulation Activity/Evidence of Disease Self-Care Intake Level of Consciousness 100 Full Normal, no evidence of disease Full Normal Full 90 Full Normal Activity, some evidence of disease Full Normal Full 80 Full Normal activity with effort, no evidence of disease Full Normal/Reduced Full 70 Reduced Unable to do normal work, some evidence of disease Full Normal/Reduced Full 60 Reduced Unable to do hobby or some housework, sig. disease Occasional Assistance Normal/Reduced Full/Confusion 50 Mainly Sit/Lie Unable to do any work, extensive disease Considerable Normal/Reduced Assistance Full/Confusion 40 Mainly in Bed Unable to do any work, extensive disease Mainly Assistance Normal/Reduced Any 30 Totally Bed Bound Unable to do any work, extensive disease Total Care Reduced Sips Any 20 Totally Bed Bound Unable to do any work, extensive disease Total Care Minimal Sips Any 10 Totally Bed Bound Unable to do any work, extensive disease Total Care Mouth Care Only Drowsy or Coma 0 Death ------ ------
 Functional Status Function recapitulates prognosis In patients with advanced cancer, a Karnofsky score <40 roughly correlates with a median survival of 3 months* *http: //www. eperc. mcw. edu/fast. Fact/ff_013. htm
Functional Status Function recapitulates prognosis In patients with advanced cancer, a Karnofsky score <40 roughly correlates with a median survival of 3 months* *http: //www. eperc. mcw. edu/fast. Fact/ff_013. htm
 Nutrition Eating Behaviors Food Preferences Pantry/Refrigerator Survey – Diabetics – CHF patients --Malnourished patients How Do Your Grocery Shopping?
Nutrition Eating Behaviors Food Preferences Pantry/Refrigerator Survey – Diabetics – CHF patients --Malnourished patients How Do Your Grocery Shopping?
 Nutrition: Feeding Issues Reversible Causes of Anorexia A Aches and pains N Nausea and gastrointestinal dysfunction O Oral Candidiasis R Reactive (or organic) depression E Evacuation problems (constipation, retention) X Xerostomia (dry mouth) I Iatrogenic (radiation, chemotherapy, drugs) A Acid-related problems (gastritis, peptic ulcers)
Nutrition: Feeding Issues Reversible Causes of Anorexia A Aches and pains N Nausea and gastrointestinal dysfunction O Oral Candidiasis R Reactive (or organic) depression E Evacuation problems (constipation, retention) X Xerostomia (dry mouth) I Iatrogenic (radiation, chemotherapy, drugs) A Acid-related problems (gastritis, peptic ulcers)
 Oral Hygiene Risk Factors – – – – – Debility Reduced oral intake Unable to brush teeth Dehydration Saliva-reducing drugs Chemotherapy Radiotherapy Mouth breathing Oxygen therapy Prevention – Regular tooth and denture brushing twice daily – Regular use of antibacterial and anti-fungal mouthwash – Check fit of dentures, remembering nightly soak – Regular dental checks – Regular mouth care: frequency dictated following assessment, e. g. for general care treat Q 612 hours, for at risk patients treat Q 2 hours, for high risk patients or for serious problems treat hourly
Oral Hygiene Risk Factors – – – – – Debility Reduced oral intake Unable to brush teeth Dehydration Saliva-reducing drugs Chemotherapy Radiotherapy Mouth breathing Oxygen therapy Prevention – Regular tooth and denture brushing twice daily – Regular use of antibacterial and anti-fungal mouthwash – Check fit of dentures, remembering nightly soak – Regular dental checks – Regular mouth care: frequency dictated following assessment, e. g. for general care treat Q 612 hours, for at risk patients treat Q 2 hours, for high risk patients or for serious problems treat hourly
 Oral Hygiene: Common Problems and Solutions Dry mouth – Frequent sips or sprays of water, use of artificial saliva (but avoid acidic solutions), ensure frequent mouthcare, vaseline to lips, iced drinks, ice cubes, pineapple juice. Chewing gum helps some patients. Pilocarpine 5 mg Q 8 hours helps some patients Dirty mouth – Remove dentures if used and soak/clean accordingly. if they have their own teeth, regular brushing is important. Alternatively, clean the mouth with sponge swabs or gauze over a gloved finger Candida – Ketaconazole (200 mg once daily for 5 days), fluconazole (150 mg as single dose), nystatin (2 mls Q 6 hours for at least 10 days) Ulceration and infection – Viral infection: acyclovir 200 mg Q 4 hours for 1 week (400 mg if immunosuppressed) Apthous ulcers – Topical corticosteroid (triamcinalone in Orabase or betamethasone tablets), or tetracyline suspension mouthwash (disperse a 250 mg capsule in water and rinse in the mouth for 2 minutes then swallow Q 6 hours) Malignant ulcers – If anaerobic infection present (i. e. foul smell) use systemic metronidazole Q 12 hours 500 mg PO or 1 g PR, or use 1% topical gel if not tolerated systemically (topical gel is expensive) Sore mouth – Sucralfate suspension mouthwash, benzocaine lozenges (100 mg sucked as required) or a lidocaine spray
Oral Hygiene: Common Problems and Solutions Dry mouth – Frequent sips or sprays of water, use of artificial saliva (but avoid acidic solutions), ensure frequent mouthcare, vaseline to lips, iced drinks, ice cubes, pineapple juice. Chewing gum helps some patients. Pilocarpine 5 mg Q 8 hours helps some patients Dirty mouth – Remove dentures if used and soak/clean accordingly. if they have their own teeth, regular brushing is important. Alternatively, clean the mouth with sponge swabs or gauze over a gloved finger Candida – Ketaconazole (200 mg once daily for 5 days), fluconazole (150 mg as single dose), nystatin (2 mls Q 6 hours for at least 10 days) Ulceration and infection – Viral infection: acyclovir 200 mg Q 4 hours for 1 week (400 mg if immunosuppressed) Apthous ulcers – Topical corticosteroid (triamcinalone in Orabase or betamethasone tablets), or tetracyline suspension mouthwash (disperse a 250 mg capsule in water and rinse in the mouth for 2 minutes then swallow Q 6 hours) Malignant ulcers – If anaerobic infection present (i. e. foul smell) use systemic metronidazole Q 12 hours 500 mg PO or 1 g PR, or use 1% topical gel if not tolerated systemically (topical gel is expensive) Sore mouth – Sucralfate suspension mouthwash, benzocaine lozenges (100 mg sucked as required) or a lidocaine spray
 Home Environment Allow Privacy – Bedside commode is nearby but some privacy measures in place Social Interaction Safe Neighborhood Proximity to Services No Assumptions on Environment
Home Environment Allow Privacy – Bedside commode is nearby but some privacy measures in place Social Interaction Safe Neighborhood Proximity to Services No Assumptions on Environment
 Other People Social Support System Clarify Roles/Concerns Emergency Help Healthcare Surrogate for the Patient Medical Power Of Attorney/Living Will – 5 Wishes www. agingwithdignity. org
Other People Social Support System Clarify Roles/Concerns Emergency Help Healthcare Surrogate for the Patient Medical Power Of Attorney/Living Will – 5 Wishes www. agingwithdignity. org
 Medications Evaluate Type, Amount & Frequency Methods of Delivery – Organization System i. e. Pillboxes ALL Meds Including OTC’s Estimate of Patient Compliance Doctor Shopping Remedy POLYPHARMACY
Medications Evaluate Type, Amount & Frequency Methods of Delivery – Organization System i. e. Pillboxes ALL Meds Including OTC’s Estimate of Patient Compliance Doctor Shopping Remedy POLYPHARMACY
 Examination Vital Signs including Pain Score – If Weight cannot be obtained, consider obtaining a mid-upper arm circumference Directed Physical Exam – Nutritional Status: temporal muscle wasting, poor fitting clothing, oral hygiene, dysphagia-aspiration risk – Look for evidence of pressure ulcers Document stage and size of wound Assess Function – Rate with Karnofsky or Palliative Performance Index
Examination Vital Signs including Pain Score – If Weight cannot be obtained, consider obtaining a mid-upper arm circumference Directed Physical Exam – Nutritional Status: temporal muscle wasting, poor fitting clothing, oral hygiene, dysphagia-aspiration risk – Look for evidence of pressure ulcers Document stage and size of wound Assess Function – Rate with Karnofsky or Palliative Performance Index
 Decubitus Ulcers: Prevention Turning and Positioning Schedule Other off-loading strategies: wheelchair pads, heel protectors, pressure reduction mattress Ointments such as zinc, lantiseptic, antifungal cream Incontinence control Keep skin clean and dry; clean all wounds with specialized wound cleansers
Decubitus Ulcers: Prevention Turning and Positioning Schedule Other off-loading strategies: wheelchair pads, heel protectors, pressure reduction mattress Ointments such as zinc, lantiseptic, antifungal cream Incontinence control Keep skin clean and dry; clean all wounds with specialized wound cleansers
 Decubitus Ulcers: Products Aquacel®: A dressing that becomes gel-like upon contact with an exudate, and keeps exudate away from wound Aquacel AG®: Same as above, with silver which has antimicrobial properties Duoderm®: A hydrocolloid dressing that provides a waterproof barrier to outside, has foam layer for mechanical protection Combiderm®: Similar to Duoderm®, but has an absorbent pad for better absorption of exudates Note: There are many similar products on the market; these products are used by Community Hospice through contracts with Conva. Tec; the authors of this presentation have no financial interests with Conva. Tec
Decubitus Ulcers: Products Aquacel®: A dressing that becomes gel-like upon contact with an exudate, and keeps exudate away from wound Aquacel AG®: Same as above, with silver which has antimicrobial properties Duoderm®: A hydrocolloid dressing that provides a waterproof barrier to outside, has foam layer for mechanical protection Combiderm®: Similar to Duoderm®, but has an absorbent pad for better absorption of exudates Note: There are many similar products on the market; these products are used by Community Hospice through contracts with Conva. Tec; the authors of this presentation have no financial interests with Conva. Tec
 Decubitus Ulcers Stage 1: – Nonblanchable erythema of intact skin, in heavily pigmented skin areas will appear dark. Does not go away when pressure is relieved. High Friction Areas: Apply Duo. Derm® change Q 3 -5 days Incontinence: Apply lantiseptic skin cream Denuded Skin: Apply zinc oxide Fungal Rash: Apply antifungal ointment
Decubitus Ulcers Stage 1: – Nonblanchable erythema of intact skin, in heavily pigmented skin areas will appear dark. Does not go away when pressure is relieved. High Friction Areas: Apply Duo. Derm® change Q 3 -5 days Incontinence: Apply lantiseptic skin cream Denuded Skin: Apply zinc oxide Fungal Rash: Apply antifungal ointment
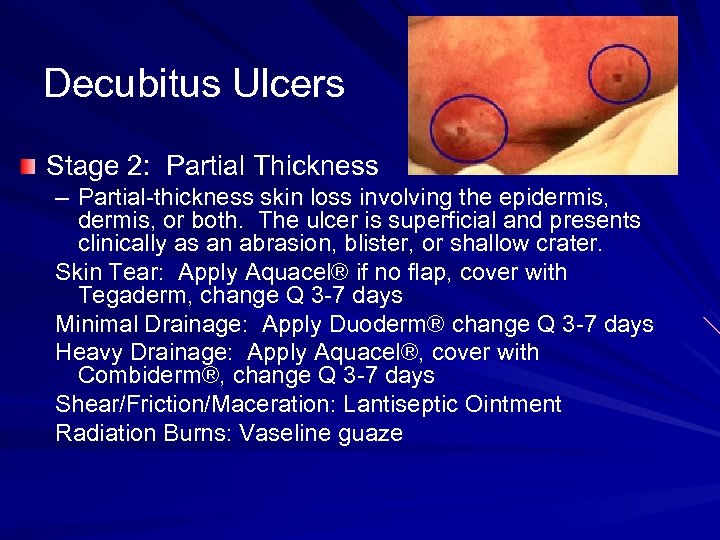 Decubitus Ulcers Stage 2: Partial Thickness – Partial-thickness skin loss involving the epidermis, or both. The ulcer is superficial and presents clinically as an abrasion, blister, or shallow crater. Skin Tear: Apply Aquacel® if no flap, cover with Tegaderm, change Q 3 -7 days Minimal Drainage: Apply Duoderm® change Q 3 -7 days Heavy Drainage: Apply Aquacel®, cover with Combiderm®, change Q 3 -7 days Shear/Friction/Maceration: Lantiseptic Ointment Radiation Burns: Vaseline guaze
Decubitus Ulcers Stage 2: Partial Thickness – Partial-thickness skin loss involving the epidermis, or both. The ulcer is superficial and presents clinically as an abrasion, blister, or shallow crater. Skin Tear: Apply Aquacel® if no flap, cover with Tegaderm, change Q 3 -7 days Minimal Drainage: Apply Duoderm® change Q 3 -7 days Heavy Drainage: Apply Aquacel®, cover with Combiderm®, change Q 3 -7 days Shear/Friction/Maceration: Lantiseptic Ointment Radiation Burns: Vaseline guaze
 Decubitus Ulcers Stage 3: Full Thickness – Full-thickness skin loss involving damage or necrosis of subcutaneous tissue, which may extend down to but not through underlying fascia. The ulcer may contain undermining to adjacent tissue. Minimal Drainage: Apply moistened (with normal saline) Aquacel® then Duoderm®, change Q 3 -7 days Moderate Drainage: Apply non-moistened Aquacel® then cover with Combiderm®, change Q 3 -7 days Infection: Apply Aquacel AG® and cover with Combiderm®, change Q 2 -3 days
Decubitus Ulcers Stage 3: Full Thickness – Full-thickness skin loss involving damage or necrosis of subcutaneous tissue, which may extend down to but not through underlying fascia. The ulcer may contain undermining to adjacent tissue. Minimal Drainage: Apply moistened (with normal saline) Aquacel® then Duoderm®, change Q 3 -7 days Moderate Drainage: Apply non-moistened Aquacel® then cover with Combiderm®, change Q 3 -7 days Infection: Apply Aquacel AG® and cover with Combiderm®, change Q 2 -3 days
 Decubitus Ulcers Stage 4: Full Thickness – Full-thickness skin loss with extensive destruction, tissue necrosis, or damage to muscle, bone or supporting structures (such as tendon, or joint capsule). The ulcer may contain undermining or tunneling. Minimal Drainage: Same as stage 3, but insert fluffed gauze between Aquacel® and Duoderm® Moderate/High Drainage: Same as stage 3, but insert fluffed gauze between Aquacel® and Combiderm® Infection/Odor: Same as stage 3, but insert fluffed gauze between Aquacel AG® and Combiderm®
Decubitus Ulcers Stage 4: Full Thickness – Full-thickness skin loss with extensive destruction, tissue necrosis, or damage to muscle, bone or supporting structures (such as tendon, or joint capsule). The ulcer may contain undermining or tunneling. Minimal Drainage: Same as stage 3, but insert fluffed gauze between Aquacel® and Duoderm® Moderate/High Drainage: Same as stage 3, but insert fluffed gauze between Aquacel® and Combiderm® Infection/Odor: Same as stage 3, but insert fluffed gauze between Aquacel AG® and Combiderm®
 Safety Comfortable Furniture Placement Throw Rugs Tap Water Temp Water Heater Setting Stairs Electrical Cords Smoking/Oxygen Use Emergency Numbers Emergency Route Lighting Night Lights Pets Bathroom Safety Smoke Detectors Oxygen Tubing Physician Personal Safety: It is strongly advised that you check out the area ahead of time (at least on Mapquest). Take your cell phone with you. If you feel unsafe in the area, keep on driving!
Safety Comfortable Furniture Placement Throw Rugs Tap Water Temp Water Heater Setting Stairs Electrical Cords Smoking/Oxygen Use Emergency Numbers Emergency Route Lighting Night Lights Pets Bathroom Safety Smoke Detectors Oxygen Tubing Physician Personal Safety: It is strongly advised that you check out the area ahead of time (at least on Mapquest). Take your cell phone with you. If you feel unsafe in the area, keep on driving!
 Spiritual Health “The spiritual dimension cannot be ignored, for it is what makes us human. ” Victor Frankl Observe for Religious Objects Reading Material Ask About the Influence of Spiritual Beliefs – Can use FICA tool Spirituality for Coping/Healing
Spiritual Health “The spiritual dimension cannot be ignored, for it is what makes us human. ” Victor Frankl Observe for Religious Objects Reading Material Ask About the Influence of Spiritual Beliefs – Can use FICA tool Spirituality for Coping/Healing
 Spiritual Health: FICA tool Faith: “Do you consider yourself spiritual or religious? ” or “Do you have spiritual beliefs that help you cope with stress? ” If “no” “What gives your life meaning? ” Importance and Influence: “What importance does your faith or belief have in your life? Have your beliefs influenced you in how you handle stress? Do you have specific beliefs that might influence your healthcare decisions? ” Community: “Are you a part of a spiritual or religious community? Is this of support to you and how? Is there a group of people you really love or who are important to you? ” Address/Action in Care: “How should the healthcare provider address these issues in your healthcare? ”
Spiritual Health: FICA tool Faith: “Do you consider yourself spiritual or religious? ” or “Do you have spiritual beliefs that help you cope with stress? ” If “no” “What gives your life meaning? ” Importance and Influence: “What importance does your faith or belief have in your life? Have your beliefs influenced you in how you handle stress? Do you have specific beliefs that might influence your healthcare decisions? ” Community: “Are you a part of a spiritual or religious community? Is this of support to you and how? Is there a group of people you really love or who are important to you? ” Address/Action in Care: “How should the healthcare provider address these issues in your healthcare? ”
 Services Having Members Present from Other Agencies Increase Communication/Coordination Clarify Orders Perspectives on Care Can be Elicited If Other Services are Not Present, Call the Services and Share the Information
Services Having Members Present from Other Agencies Increase Communication/Coordination Clarify Orders Perspectives on Care Can be Elicited If Other Services are Not Present, Call the Services and Share the Information
 Local Services Mayo Clinic Memory Disorders Caregiver Educational Series and Support Group – Provides monthly educational sessions – 904 953 7103 Mayo Clinic Cancer Resource and Support Group – Sessions held twice a month – 904 953 6807 Jewish Family & Community Services – Medical Advocate Program – 904 394 5777 Community Hospice NE Florida – www. communityhospice. com – 904 407 6500
Local Services Mayo Clinic Memory Disorders Caregiver Educational Series and Support Group – Provides monthly educational sessions – 904 953 7103 Mayo Clinic Cancer Resource and Support Group – Sessions held twice a month – 904 953 6807 Jewish Family & Community Services – Medical Advocate Program – 904 394 5777 Community Hospice NE Florida – www. communityhospice. com – 904 407 6500
 Documenting the Home Visit For Medicare Reimbursement: Requires documentation of need for home visit – Patient home bound – Office visit would require ambulance transport – Office visit requires excessive effort or pain – http: //www. aafp. org/fpm/20070600/coding. html
Documenting the Home Visit For Medicare Reimbursement: Requires documentation of need for home visit – Patient home bound – Office visit would require ambulance transport – Office visit requires excessive effort or pain – http: //www. aafp. org/fpm/20070600/coding. html
 Coding: New Patient* 99341: Straightforward Decision – Problem Focused Hx/Exam – 20 minutes: $57. 67 99342: Low Complexity Decision – Expanded Problem Focused Hx/Exam – 30 minutes: $84. 26 99343: Moderate Complexity – Detailed History & Detailed Exam – 45 minutes: $133. 30 *2008 Medicare Reimbursement
Coding: New Patient* 99341: Straightforward Decision – Problem Focused Hx/Exam – 20 minutes: $57. 67 99342: Low Complexity Decision – Expanded Problem Focused Hx/Exam – 30 minutes: $84. 26 99343: Moderate Complexity – Detailed History & Detailed Exam – 45 minutes: $133. 30 *2008 Medicare Reimbursement
 Coding: New Patient* 99344: Moderate Complexity – Comprehensive History – Comprehensive EXAM – 60 minutes: $174. 55 99345: High Complexity – Comprehensive History – Comprehensive Exam – 75 minutes: $210. 00 *2008 Medicare Reimbursement
Coding: New Patient* 99344: Moderate Complexity – Comprehensive History – Comprehensive EXAM – 60 minutes: $174. 55 99345: High Complexity – Comprehensive History – Comprehensive Exam – 75 minutes: $210. 00 *2008 Medicare Reimbursement
 Coding: Established Patient* 99347: Straightforward – Problem Focused History – Problem Focused Exam – 15 Minutes: $55. 09 99348: Low Complexity – Expanded Problem Focus History – Expanded Problem Focus Exam – 25 Minutes: $82. 94 *2008 Medicare Reimbursement
Coding: Established Patient* 99347: Straightforward – Problem Focused History – Problem Focused Exam – 15 Minutes: $55. 09 99348: Low Complexity – Expanded Problem Focus History – Expanded Problem Focus Exam – 25 Minutes: $82. 94 *2008 Medicare Reimbursement
 Coding: Established Patient* 99349: Moderate Complexity – Detailed Interval History – Detailed Exam – 40 Minutes: $121. 29 99350: High Complexity – Comprehensive History – Comprehensive Exam – 60 Minutes: $170. 03 *2008 Medicare Reimbursement
Coding: Established Patient* 99349: Moderate Complexity – Detailed Interval History – Detailed Exam – 40 Minutes: $121. 29 99350: High Complexity – Comprehensive History – Comprehensive Exam – 60 Minutes: $170. 03 *2008 Medicare Reimbursement
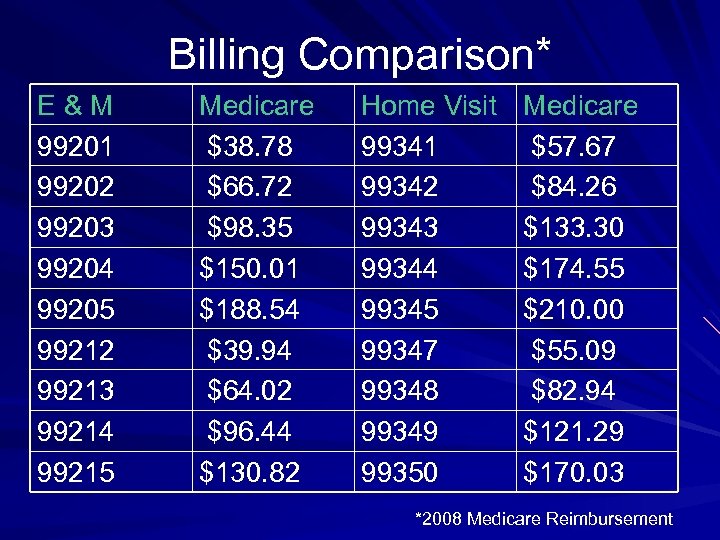 Billing Comparison* E & M 99201 99202 99203 99204 99205 99212 99213 99214 99215 Medicare $38. 78 $66. 72 $98. 35 $150. 01 $188. 54 $39. 94 $64. 02 $96. 44 $130. 82 Home Visit 99341 99342 99343 99344 99345 99347 99348 99349 99350 Medicare $57. 67 $84. 26 $133. 30 $174. 55 $210. 00 $55. 09 $82. 94 $121. 29 $170. 03 *2008 Medicare Reimbursement
Billing Comparison* E & M 99201 99202 99203 99204 99205 99212 99213 99214 99215 Medicare $38. 78 $66. 72 $98. 35 $150. 01 $188. 54 $39. 94 $64. 02 $96. 44 $130. 82 Home Visit 99341 99342 99343 99344 99345 99347 99348 99349 99350 Medicare $57. 67 $84. 26 $133. 30 $174. 55 $210. 00 $55. 09 $82. 94 $121. 29 $170. 03 *2008 Medicare Reimbursement
 Billing with Hospice When you refer a patient to hospice, you can continue to see and care for the patient as their attending physician. The attending physician can bill Medicare (GV modifier) and other insurance providers for regular visits related to the hospice plan of care.
Billing with Hospice When you refer a patient to hospice, you can continue to see and care for the patient as their attending physician. The attending physician can bill Medicare (GV modifier) and other insurance providers for regular visits related to the hospice plan of care.
 Fast Facts Developed at Medical University of Wisconsin Provide quick summaries of hundreds of topics relevant to hospice/palliative medicine Be prepared to present a Fast Fact during your precept time (hopefully one that is relevant to your patient!) http: //www. eperc. mcw. edu/ look for fast facts link on the left side of screen
Fast Facts Developed at Medical University of Wisconsin Provide quick summaries of hundreds of topics relevant to hospice/palliative medicine Be prepared to present a Fast Fact during your precept time (hopefully one that is relevant to your patient!) http: //www. eperc. mcw. edu/ look for fast facts link on the left side of screen
 Fast Fact: #042: Broaching the Topic of a Palliative Care Consultation Palliative care consultative services are becoming commonplace in academic and community hospitals. Patients and families often, although not always, have negative perceptions of palliative care and hospice, viewing such a discussion as signaling that the physician is “giving up on the patient” and that the reality of impending death must be faced. For the attending physician, the decision to convey to a patient and family that a consultation is needed can provoke anxiety; physicians may fear such a discussion will provoke anxiety, anger or a sense of hopelessness. This Fast Fact provides tips for beginning a discussion leading to a visit by a palliative care consultation team. First, decide why you want assistance from the palliative care team; typically, physicians seek assistance in four domains: 1) pain and nonpain symptom assessment and management; 2) assistance in making difficult decisions, usually about continued use or withdrawal of technological treatments such as feeding tubes, antibiotics, dialysis, or ventilators; 3) assistance in planning for the most appropriate care setting and care givers to meet patient/family goals for end-of-life care; and 4) providing psychological support to patients, families and the health care team.
Fast Fact: #042: Broaching the Topic of a Palliative Care Consultation Palliative care consultative services are becoming commonplace in academic and community hospitals. Patients and families often, although not always, have negative perceptions of palliative care and hospice, viewing such a discussion as signaling that the physician is “giving up on the patient” and that the reality of impending death must be faced. For the attending physician, the decision to convey to a patient and family that a consultation is needed can provoke anxiety; physicians may fear such a discussion will provoke anxiety, anger or a sense of hopelessness. This Fast Fact provides tips for beginning a discussion leading to a visit by a palliative care consultation team. First, decide why you want assistance from the palliative care team; typically, physicians seek assistance in four domains: 1) pain and nonpain symptom assessment and management; 2) assistance in making difficult decisions, usually about continued use or withdrawal of technological treatments such as feeding tubes, antibiotics, dialysis, or ventilators; 3) assistance in planning for the most appropriate care setting and care givers to meet patient/family goals for end-of-life care; and 4) providing psychological support to patients, families and the health care team.
 Fast Fact: #042: Broaching the Topic of a Palliative Care Consultation Second, contact the palliative care team; discuss your reason(s) for consultation along with pertinent details of the patient’s history and family support structure. Describe both what your goals are for the consultation, as well as what the family’s/patient’s goals may be. This is a good time to discuss any concerns you have about using the term palliative care with the patient or family. While remaining sensitive to the patient and family’s value. Palliative care guides the patient and family as they face disease progression and changing goals of care, and helps those who wish to address issues of life completion and life closure.
Fast Fact: #042: Broaching the Topic of a Palliative Care Consultation Second, contact the palliative care team; discuss your reason(s) for consultation along with pertinent details of the patient’s history and family support structure. Describe both what your goals are for the consultation, as well as what the family’s/patient’s goals may be. This is a good time to discuss any concerns you have about using the term palliative care with the patient or family. While remaining sensitive to the patient and family’s value. Palliative care guides the patient and family as they face disease progression and changing goals of care, and helps those who wish to address issues of life completion and life closure.
 Fast Fact: #042: Broaching the Topic of a Palliative Care Consultation Third, engage the patient/family in a discussion of the current medical condition and goals of care. (see FF # 38 Discussing Hospice Care). Introduce the topic of a consultation by saying: To best meet some of the goals we’ve been discussing (fill in with the goals mentioned by the family/patient) I’d like to have some consultants from the Palliative Care Team visit with you. You can follow this by saying, They are experts in treating the symptoms you are experiencing (fill in symptom); They are also good at helping your family deal with all the changes brought on by your illness; they can answer your questions about (fill in previously discussed patient questions). You should not say that the reason you are asking Palliative care to be involved is “that there is nothing more to do” or because “I have nothing more to offer. ” Talk about the positive goals Palliative care can help you and the patient achieve.
Fast Fact: #042: Broaching the Topic of a Palliative Care Consultation Third, engage the patient/family in a discussion of the current medical condition and goals of care. (see FF # 38 Discussing Hospice Care). Introduce the topic of a consultation by saying: To best meet some of the goals we’ve been discussing (fill in with the goals mentioned by the family/patient) I’d like to have some consultants from the Palliative Care Team visit with you. You can follow this by saying, They are experts in treating the symptoms you are experiencing (fill in symptom); They are also good at helping your family deal with all the changes brought on by your illness; they can answer your questions about (fill in previously discussed patient questions). You should not say that the reason you are asking Palliative care to be involved is “that there is nothing more to do” or because “I have nothing more to offer. ” Talk about the positive goals Palliative care can help you and the patient achieve.
 Fast Fact: #042: Broaching the Topic of a Palliative Care Consultation Finally, emphasize your continued involvement: You and I will talk about the recommendations of the palliative care experts. I'll make sure all your questions are answered. This can help relieve fears of abandonment. If a patient or family reacts negatively to the suggestion for a consultation, you might explore their concerns. Someone may have mentioned palliative care and this may have negative connotations to them. Ask, What experience do you have with hospice/palliative care? What are your concerns? It may be important to discuss that palliative care is compatible with aggressively treating the underlying disease. Emphasize the positive aspects of what palliative care can do, rather than focusing on how the palliative care team will help them accept death and dying. After all, the goal of palliative care is to achieve the best possible quality of life through relief of suffering, control of symptoms and restoration of functional capacity,
Fast Fact: #042: Broaching the Topic of a Palliative Care Consultation Finally, emphasize your continued involvement: You and I will talk about the recommendations of the palliative care experts. I'll make sure all your questions are answered. This can help relieve fears of abandonment. If a patient or family reacts negatively to the suggestion for a consultation, you might explore their concerns. Someone may have mentioned palliative care and this may have negative connotations to them. Ask, What experience do you have with hospice/palliative care? What are your concerns? It may be important to discuss that palliative care is compatible with aggressively treating the underlying disease. Emphasize the positive aspects of what palliative care can do, rather than focusing on how the palliative care team will help them accept death and dying. After all, the goal of palliative care is to achieve the best possible quality of life through relief of suffering, control of symptoms and restoration of functional capacity,
 References “The Home Visit” American Family Physician October 1, 1999. – http: //www. aafp. org/afp/991001 ap/1481. html “House Calls: Taking the Practice to the Patient” Family Practice Management June 2000. – http: //www. aafp. org/fpm/20000600/49 hous. html Policzer, Joel and Jason Sobel. Unipac 4: Management of Selected Nonpain Symptoms of Life-Limiting Illness. American Academy of Hospice and Palliative Medicine: 2008. pp 27. Current Learning in Palliative Care; Help the Hospices. Last accessed 10/12/08 – http: //www. helpthehospices. org. uk/elearning/index. asp http: //www. aafp. org/fpm/20070600/coding. html http: //www. eperc. mcw. edu/ Pressure Ulcer Images: www. pele. com. tw/pressure_ulcers. htm last accessed 10/12/08 Community Hospice Wound Management Guide Conva. Tec USA: http: //www. convatec. com/en/cvtus-homeus/cvt-home/0/393/0/default. html last accessed 10/12/08
References “The Home Visit” American Family Physician October 1, 1999. – http: //www. aafp. org/afp/991001 ap/1481. html “House Calls: Taking the Practice to the Patient” Family Practice Management June 2000. – http: //www. aafp. org/fpm/20000600/49 hous. html Policzer, Joel and Jason Sobel. Unipac 4: Management of Selected Nonpain Symptoms of Life-Limiting Illness. American Academy of Hospice and Palliative Medicine: 2008. pp 27. Current Learning in Palliative Care; Help the Hospices. Last accessed 10/12/08 – http: //www. helpthehospices. org. uk/elearning/index. asp http: //www. aafp. org/fpm/20070600/coding. html http: //www. eperc. mcw. edu/ Pressure Ulcer Images: www. pele. com. tw/pressure_ulcers. htm last accessed 10/12/08 Community Hospice Wound Management Guide Conva. Tec USA: http: //www. convatec. com/en/cvtus-homeus/cvt-home/0/393/0/default. html last accessed 10/12/08
 References Billings, J Andrew et. al “The Role of Palliative Care in the Home in Medical Education: Report from a National Consensus Conference” Journal of Palliative Medicine. Vol. 4, No 3. 2001; pp 361 -371. Puchalski CM. “Taking a Spiritual History: FICA. ” Spirituality and Medicine Connection 1999. Frankl, Victor. Man’s Search for Meaning. Simon and Schuster: 1984; p 134.
References Billings, J Andrew et. al “The Role of Palliative Care in the Home in Medical Education: Report from a National Consensus Conference” Journal of Palliative Medicine. Vol. 4, No 3. 2001; pp 361 -371. Puchalski CM. “Taking a Spiritual History: FICA. ” Spirituality and Medicine Connection 1999. Frankl, Victor. Man’s Search for Meaning. Simon and Schuster: 1984; p 134.


