eccc75a98108c3d8bdb45ed470fd2957.ppt
- Количество слайдов: 32

 Pain Management- An integral aspect of Wound Care. n Glenn Bruce. n Clinical Nurse Specialist for in-patient pain management. Taunton & Somerset NHS Trust. http: //www. gb 42. com/Exeter. html
Pain Management- An integral aspect of Wound Care. n Glenn Bruce. n Clinical Nurse Specialist for in-patient pain management. Taunton & Somerset NHS Trust. http: //www. gb 42. com/Exeter. html
 What is pain? “Pain is what Sister says it is, and only exists when Sister says it does!”
What is pain? “Pain is what Sister says it is, and only exists when Sister says it does!”
 What is pain? “Pain is what Matron says it is, and only exists when Matron says it does!”
What is pain? “Pain is what Matron says it is, and only exists when Matron says it does!”
 What is pain? n 'an unpleasant sensory and emotional experience associated with actual or potential tissue damage, or described in terms of such damage' The International Association for the Study of Pain. (1986)
What is pain? n 'an unpleasant sensory and emotional experience associated with actual or potential tissue damage, or described in terms of such damage' The International Association for the Study of Pain. (1986)
 Pain, is pain, is pain…. n Acute pain. n Short duration. (<3 months) n A response to tissue damage. n Pain decreases/resolves as tissues heal. n Responds well to ‘medical model’ Rx.
Pain, is pain, is pain…. n Acute pain. n Short duration. (<3 months) n A response to tissue damage. n Pain decreases/resolves as tissues heal. n Responds well to ‘medical model’ Rx.
 Pain, is pain, is pain…. n Chronic pain.
Pain, is pain, is pain…. n Chronic pain.
 Pain, is pain, is pain…. n Chronic persistent pain. n n n Longer duration (>3 months) Not always in response to tissue damage. Persists after tissue healing. Pain management, not pain relief may be the goal. Multidimensional Responds to Bio-psychosocial model
Pain, is pain, is pain…. n Chronic persistent pain. n n n Longer duration (>3 months) Not always in response to tissue damage. Persists after tissue healing. Pain management, not pain relief may be the goal. Multidimensional Responds to Bio-psychosocial model
 Nociceptive pain n A normal physiological response to tissue damage Responds well to ‘traditional’ analgesics Normally ‘time-limited’
Nociceptive pain n A normal physiological response to tissue damage Responds well to ‘traditional’ analgesics Normally ‘time-limited’
 Neuropathic pain n n Pain experienced as a result of injury to, or malfunction of, the nervous system. May follow tissue damage. May be of unknown aetiology. Often responds poorly to ‘traditional’ analgesics. May respond to anti-depressants or anti-epileptic drugs (e. g. amitriptyline, gabapentin, lyrica)
Neuropathic pain n n Pain experienced as a result of injury to, or malfunction of, the nervous system. May follow tissue damage. May be of unknown aetiology. Often responds poorly to ‘traditional’ analgesics. May respond to anti-depressants or anti-epileptic drugs (e. g. amitriptyline, gabapentin, lyrica)
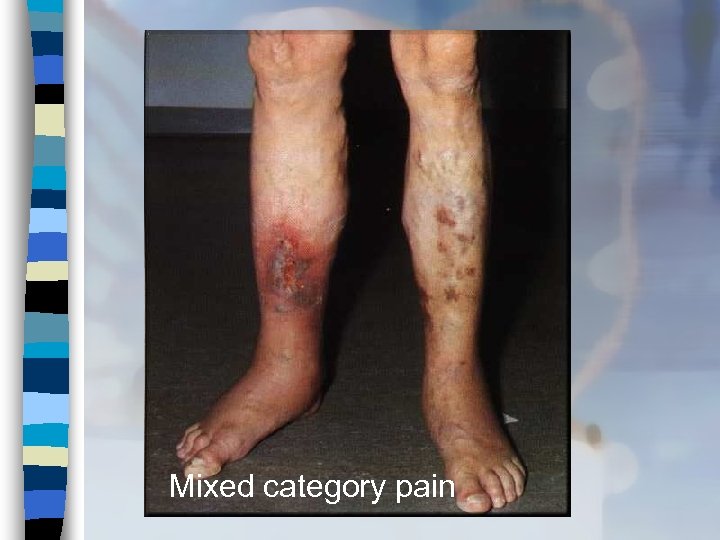 Mixed category pain
Mixed category pain
 n. Leg Ulcers 83% of patients with arterial ulcers had pain (Lindholm 1999) 65% of patients with venous leg ulcers had pain (Ryan et al 2003, Briggs and Nelson, Cochrane Review 2003). n. Diabetic Foot Ulcers 48% patients reported pain (Ebbeskog et al 1996) n. Pressure Ulcers 59% patients report pain (Dallum 1995), nearly half of patients with Stage 3, 4 ulcers had pain (Lindholm 1999) n. Fungating Wounds 38% patients report pain (Naylor 2001)
n. Leg Ulcers 83% of patients with arterial ulcers had pain (Lindholm 1999) 65% of patients with venous leg ulcers had pain (Ryan et al 2003, Briggs and Nelson, Cochrane Review 2003). n. Diabetic Foot Ulcers 48% patients reported pain (Ebbeskog et al 1996) n. Pressure Ulcers 59% patients report pain (Dallum 1995), nearly half of patients with Stage 3, 4 ulcers had pain (Lindholm 1999) n. Fungating Wounds 38% patients report pain (Naylor 2001)
 What are the dangers of poor pain relief? • Anxiety and insomnia • Delayed healing • Atelectasis and hypoxia • Retained secretions and pneumonia • Increased myocardial work • Delayed gastric emptying • Increased cortisol & reduced insulin secretion
What are the dangers of poor pain relief? • Anxiety and insomnia • Delayed healing • Atelectasis and hypoxia • Retained secretions and pneumonia • Increased myocardial work • Delayed gastric emptying • Increased cortisol & reduced insulin secretion
 What are the causes of poor pain relief? • Poor pain assessment • Poor analgesia choice • Incorrect dose • Wrong frequency • Wrong mode of delivery
What are the causes of poor pain relief? • Poor pain assessment • Poor analgesia choice • Incorrect dose • Wrong frequency • Wrong mode of delivery
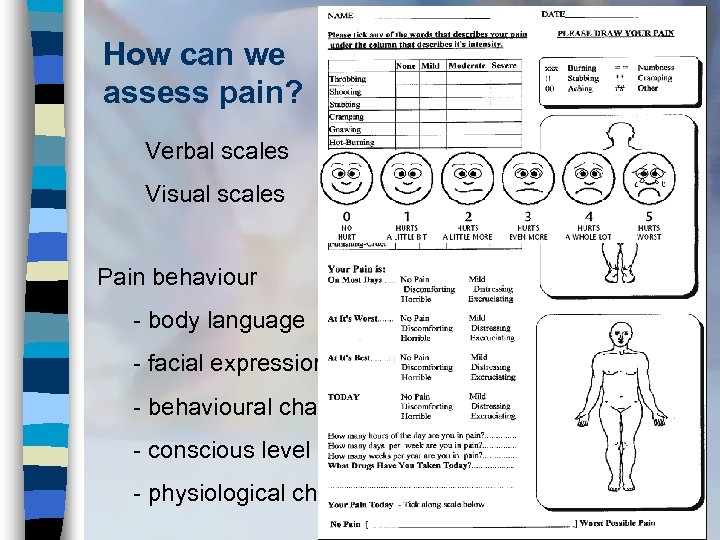 How can we assess pain? Verbal scales Visual scales Pain behaviour - body language - facial expression - behavioural changes - conscious level - physiological changes
How can we assess pain? Verbal scales Visual scales Pain behaviour - body language - facial expression - behavioural changes - conscious level - physiological changes
 What routes of analgesia are there? • Inhalation • Sublingual • Oral • Intramuscular • Intravenous bolus/infusion/PCA • Spinal or epidural • Rectal • Transdermal • Topical
What routes of analgesia are there? • Inhalation • Sublingual • Oral • Intramuscular • Intravenous bolus/infusion/PCA • Spinal or epidural • Rectal • Transdermal • Topical
 What options are there for analgesia? n n n Opiates ‘Moderate’ analgesics: e. g. codeine, tramadol ‘Mild’ analgesics: paracetamol NSAIDS Other drugs Non drug treatments.
What options are there for analgesia? n n n Opiates ‘Moderate’ analgesics: e. g. codeine, tramadol ‘Mild’ analgesics: paracetamol NSAIDS Other drugs Non drug treatments.
 Where do we, as nurses come in? n Pain assessment. n Record keeping. n Pre-emptive analgesia administration. n Explanations and reassurance. n Distraction. n Dressing technique & dressing choice.
Where do we, as nurses come in? n Pain assessment. n Record keeping. n Pre-emptive analgesia administration. n Explanations and reassurance. n Distraction. n Dressing technique & dressing choice.
 Dressing technique & dressing choice. n Traditional dressings, cleaning solutions and tapes have been shown to damage healing tissue. n Dressings such as hydrocolloids, gels, alginates and foams are less traumatic for the patient. n But the best dressing may not be the one that causes least pain! n Local infiltration, anaesthetic gels, analgesic dressings.
Dressing technique & dressing choice. n Traditional dressings, cleaning solutions and tapes have been shown to damage healing tissue. n Dressings such as hydrocolloids, gels, alginates and foams are less traumatic for the patient. n But the best dressing may not be the one that causes least pain! n Local infiltration, anaesthetic gels, analgesic dressings.
 Some points to ponder…. . . When is pain present? . Is neuropathic pain a factor? Twenty of 39 . Aggravating factors participants reported phantom sensations. . Relieving factors Nine of the participants with phantom sensations . Pain intensity experienced phantom . Analgesia choice pain and 11 non-painful phantom sensations. (Rothemund 2004)
Some points to ponder…. . . When is pain present? . Is neuropathic pain a factor? Twenty of 39 . Aggravating factors participants reported phantom sensations. . Relieving factors Nine of the participants with phantom sensations . Pain intensity experienced phantom . Analgesia choice pain and 11 non-painful phantom sensations. (Rothemund 2004)
 Analgesia Choice n n n Regular analgesia is more effective than PRN Pre-emptive analgesia is more effective than reactive analgesia For nociceptive pain follow the W. H. O analgesia ladder For neuropathic pain consider antidepressants or anti-epileptics. Be prepared to balance effects/side-effects.
Analgesia Choice n n n Regular analgesia is more effective than PRN Pre-emptive analgesia is more effective than reactive analgesia For nociceptive pain follow the W. H. O analgesia ladder For neuropathic pain consider antidepressants or anti-epileptics. Be prepared to balance effects/side-effects.
 The analgesia ladder
The analgesia ladder
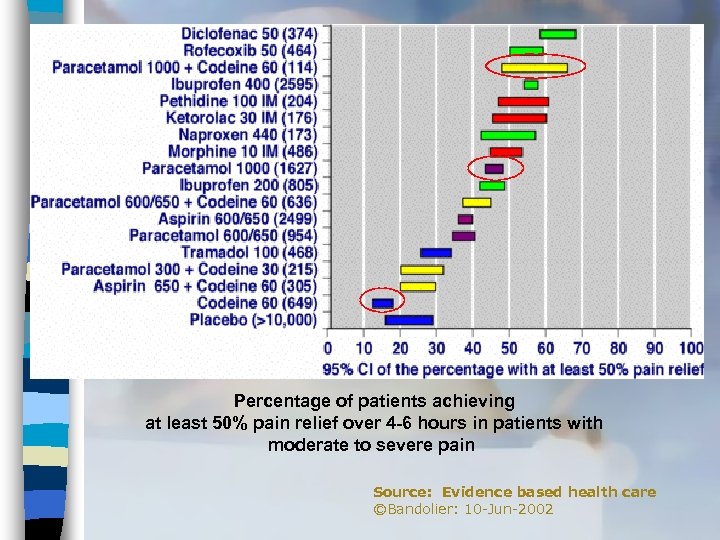 Percentage of patients achieving at least 50% pain relief over 4 -6 hours in patients with moderate to severe pain Source: Evidence based health care ©Bandolier: 10 -Jun-2002
Percentage of patients achieving at least 50% pain relief over 4 -6 hours in patients with moderate to severe pain Source: Evidence based health care ©Bandolier: 10 -Jun-2002
 Neuropathic pain n Amitriptyline n Increasing by 10 mg every third day in the absence of effect/unacceptable side-effects up to a maximum of 100 mg nocte. n Gabapentin n 10 mg nocte 100 mg T. D. S Increasing by 100 -300 mg every third day in the absence of effect/unacceptable side-effects up to a typical maximum of 1800 mg/day (3600 mg absolute max. )
Neuropathic pain n Amitriptyline n Increasing by 10 mg every third day in the absence of effect/unacceptable side-effects up to a maximum of 100 mg nocte. n Gabapentin n 10 mg nocte 100 mg T. D. S Increasing by 100 -300 mg every third day in the absence of effect/unacceptable side-effects up to a typical maximum of 1800 mg/day (3600 mg absolute max. )
 Pain Relief Ask the following questions: • Is effective analgesia prescribed? • Is effective analgesia being given? • Is the treatment safe and appropriate for the patient? • Is it working?
Pain Relief Ask the following questions: • Is effective analgesia prescribed? • Is effective analgesia being given? • Is the treatment safe and appropriate for the patient? • Is it working?
 Further reading: The Best Practice statement on Pain & Trauma in wound management (Cooper et al. 2004) www. tvna. org Pain at wound dressing-related procedures: a template for assessment. (Hollingworth 2005) www. worldwidewounds. com
Further reading: The Best Practice statement on Pain & Trauma in wound management (Cooper et al. 2004) www. tvna. org Pain at wound dressing-related procedures: a template for assessment. (Hollingworth 2005) www. worldwidewounds. com
 Further reading: The management of patients’ pain in wound care (Hollingworth 2005) www. nursing-standard. co. uk Pain Talk (www. pain-talk. org. uk) The national discussion forum and community for UK Healthcare Professionals with an interest in acute, chronic, or palliative Pain Management.
Further reading: The management of patients’ pain in wound care (Hollingworth 2005) www. nursing-standard. co. uk Pain Talk (www. pain-talk. org. uk) The national discussion forum and community for UK Healthcare Professionals with an interest in acute, chronic, or palliative Pain Management.
 Further reading: Pain and quality of life for patients with venous leg ulcers: proof of concept of the efficacy of Biatain®-Ibu, a new pain reducing wound dressing Authors: Jørgensen, Bo; Friis, Gitte Juel; Gottrup, Finn Source: Wound Repair and Regeneration, Volume 14, Number 3, May-June 2006 , pp. 233 -239(7) Publisher: Blackwell Publishing
Further reading: Pain and quality of life for patients with venous leg ulcers: proof of concept of the efficacy of Biatain®-Ibu, a new pain reducing wound dressing Authors: Jørgensen, Bo; Friis, Gitte Juel; Gottrup, Finn Source: Wound Repair and Regeneration, Volume 14, Number 3, May-June 2006 , pp. 233 -239(7) Publisher: Blackwell Publishing
 Pain Management- An integral aspect of Wound Care. n Clinical Nurse Specialist for in-patient pain management. Taunton & Somerset NHS Trust.
Pain Management- An integral aspect of Wound Care. n Clinical Nurse Specialist for in-patient pain management. Taunton & Somerset NHS Trust.
 http: //www. gb 42. com/Exeter. html
http: //www. gb 42. com/Exeter. html



