7f53c9dc7230ed61c175abafce0408d9.ppt
- Количество слайдов: 34
 Pain and Addiction: Assessment Issues Russell K. Portenoy, MD Chairman, Dept of Pain Medicine and Palliative Care Beth Israel Medical Center New York, NY
Pain and Addiction: Assessment Issues Russell K. Portenoy, MD Chairman, Dept of Pain Medicine and Palliative Care Beth Israel Medical Center New York, NY
 Pain and Addiction: Assessment Issues • • Prevalence of chronic pain Populations with chronic pain and the importance of assessment Assessing the risk of substance abuse Elements of the comprehensive assessment
Pain and Addiction: Assessment Issues • • Prevalence of chronic pain Populations with chronic pain and the importance of assessment Assessing the risk of substance abuse Elements of the comprehensive assessment
 Pain and Addiction: Assessment Issues • Prevalence of chronic pain – – 2%-40% in a review of 15 populationbased surveys (Verhaak et al 1998) 22% in a WHO survey of 25, 916 primary care patients (Gureje et al 1998)
Pain and Addiction: Assessment Issues • Prevalence of chronic pain – – 2%-40% in a review of 15 populationbased surveys (Verhaak et al 1998) 22% in a WHO survey of 25, 916 primary care patients (Gureje et al 1998)
 Pain and Addiction: Assessment Issues – Telephone survey of community-dwelling adults in the U. S (Portenoy et al, in press) • • • Nationally representative sample: 454 Caucasians, 447 African Americans and 434 Hispanics Prevalence of chronic pain: 35% Caucasians, 39% African Americans, and 28% Hispanics Overall prevalence of “disabling pain: 35. 8%
Pain and Addiction: Assessment Issues – Telephone survey of community-dwelling adults in the U. S (Portenoy et al, in press) • • • Nationally representative sample: 454 Caucasians, 447 African Americans and 434 Hispanics Prevalence of chronic pain: 35% Caucasians, 39% African Americans, and 28% Hispanics Overall prevalence of “disabling pain: 35. 8%
 Pain and Addiction: Assessment Issues – Moderate to severe pain in the cancer population • • 1/3 of those with solid tumors during the period of active antineoplastic treatment 3/4 of those with advanced disease
Pain and Addiction: Assessment Issues – Moderate to severe pain in the cancer population • • 1/3 of those with solid tumors during the period of active antineoplastic treatment 3/4 of those with advanced disease
 Pain and Addiction: Assessment Issues Challenges in pain management – Heterogeneous disorders Headache Neck pain Polyneuropathy Central pain Somatoform disorders Low back pain Arthridites CRPS Myofascial pain Fibromyalgia Interstitial cystitis
Pain and Addiction: Assessment Issues Challenges in pain management – Heterogeneous disorders Headache Neck pain Polyneuropathy Central pain Somatoform disorders Low back pain Arthridites CRPS Myofascial pain Fibromyalgia Interstitial cystitis
 Pain and Addiction: Assessment Issues • Challenges in pain management – Heterogeneous pain-related outcomes • • • Physical Psychosocial Role functioning Family impact Economic impact
Pain and Addiction: Assessment Issues • Challenges in pain management – Heterogeneous pain-related outcomes • • • Physical Psychosocial Role functioning Family impact Economic impact
 Pain and Addiction: Assessment Issues • Challenges in pain management – Heterogeneous factors influencing pain experience and related outcomes • • • Personality Adaptation/coping Family response Past history Comorbidities
Pain and Addiction: Assessment Issues • Challenges in pain management – Heterogeneous factors influencing pain experience and related outcomes • • • Personality Adaptation/coping Family response Past history Comorbidities
 Pain and Addiction: Assessment Issues • Challenges in pain management – Heterogeneous comorbidities • • Physical/medical Psychiatric/psychosocial
Pain and Addiction: Assessment Issues • Challenges in pain management – Heterogeneous comorbidities • • Physical/medical Psychiatric/psychosocial
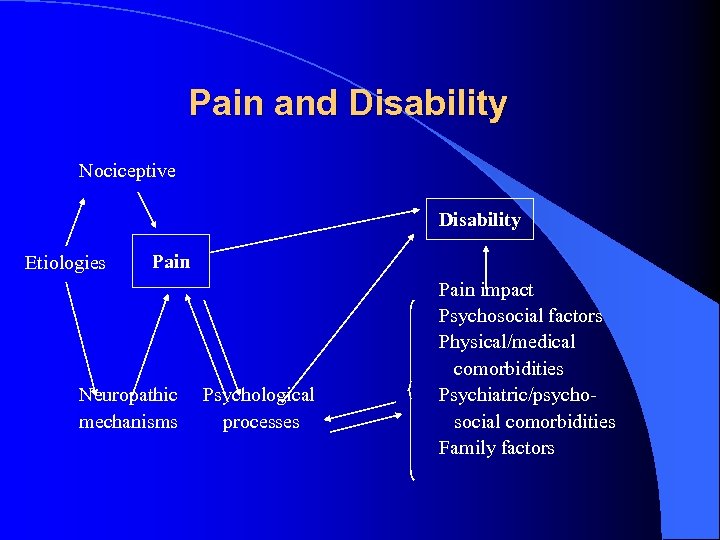 Pain and Disability Nociceptive Disability Etiologies Pain Neuropathic mechanisms Psychological processes Pain impact Psychosocial factors Physical/medical comorbidities Psychiatric/psychosocial comorbidities Family factors
Pain and Disability Nociceptive Disability Etiologies Pain Neuropathic mechanisms Psychological processes Pain impact Psychosocial factors Physical/medical comorbidities Psychiatric/psychosocial comorbidities Family factors
 Pain and Addiction: Assessment Issues • Challenges in pain management – Heterogeneous treatments Pharmacotherapy Rehabilitative Psychological Neurostimulatory Surgical Anesthesiologic CAM Lifestyle changes
Pain and Addiction: Assessment Issues • Challenges in pain management – Heterogeneous treatments Pharmacotherapy Rehabilitative Psychological Neurostimulatory Surgical Anesthesiologic CAM Lifestyle changes
 Pain and Addiction: Assessment Issues • Implications of heterogeneity – – – Few treatment standards Limited evidence - can guide therapy but does not capture complexity of practice Comprehensive assessment is the foundation for selection and implementation of treatments
Pain and Addiction: Assessment Issues • Implications of heterogeneity – – – Few treatment standards Limited evidence - can guide therapy but does not capture complexity of practice Comprehensive assessment is the foundation for selection and implementation of treatments
 Pain and Addiction: Assessment Issues 1. Example: Long-term opioid therapy – Evolving clinical use Consensus for use only in moderate-severe chronic pain due to cancer or AIDS, or life threatening illness 2. Expanding role in chronic noncancer pain, including populations with known histories of addiction 1.
Pain and Addiction: Assessment Issues 1. Example: Long-term opioid therapy – Evolving clinical use Consensus for use only in moderate-severe chronic pain due to cancer or AIDS, or life threatening illness 2. Expanding role in chronic noncancer pain, including populations with known histories of addiction 1.
 Pain and Addiction: Assessment Issues 1. Now may consider opioids for all with severe pain, but weigh the following: – – – What is conventional practice? Are opioids likely to work well? Are there alternatives with evidence of equal or better outcomes? Is the risk of toxicity increased? What is the likelihood of responsible drug use over time?
Pain and Addiction: Assessment Issues 1. Now may consider opioids for all with severe pain, but weigh the following: – – – What is conventional practice? Are opioids likely to work well? Are there alternatives with evidence of equal or better outcomes? Is the risk of toxicity increased? What is the likelihood of responsible drug use over time?
 Pain and Addiction: Assessment Issues • Optimal opioid use requires assessment in all populations – Must include evaluation of risk associated with misuse, abuse, addiction, diversion
Pain and Addiction: Assessment Issues • Optimal opioid use requires assessment in all populations – Must include evaluation of risk associated with misuse, abuse, addiction, diversion
 Pain and Addiction: Assessment Issues • Challenges in predicting drug-related problems during opioid therapy for pain – – – What is being predicted? What is the outcome worth predicting? Are predictive variables the same across populations?
Pain and Addiction: Assessment Issues • Challenges in predicting drug-related problems during opioid therapy for pain – – – What is being predicted? What is the outcome worth predicting? Are predictive variables the same across populations?
 Pain and Addiction: Assessment Issues • Factors identified by clinicians as potential predictors of substance abuse (Jovey 2002) – – Past history of drug abuse History of personality disorder associated with poor symptom control History of amplifying symptoms History of physical/sexual abuse
Pain and Addiction: Assessment Issues • Factors identified by clinicians as potential predictors of substance abuse (Jovey 2002) – – Past history of drug abuse History of personality disorder associated with poor symptom control History of amplifying symptoms History of physical/sexual abuse
 Pain and Addiction: Assessment Issues 1. Factors identified by clinicians as potential predictors of substance abuse (Jovey 2002) – – – History of using drugs to cope with stress History of severe depressive or anxiety disorder Regular contact with high risk people or high risk environments Current chaotic living environment History of criminal activity
Pain and Addiction: Assessment Issues 1. Factors identified by clinicians as potential predictors of substance abuse (Jovey 2002) – – – History of using drugs to cope with stress History of severe depressive or anxiety disorder Regular contact with high risk people or high risk environments Current chaotic living environment History of criminal activity
 Pain and Addiction: Assessment Issues • Factors identified by clinicians as potential predictors of substance abuse (Jovey 2002) – – Prior admission to drug rehabilitation Prior failed treatment at a pain management program Heavy tobacco use Heavy alcohol use
Pain and Addiction: Assessment Issues • Factors identified by clinicians as potential predictors of substance abuse (Jovey 2002) – – Prior admission to drug rehabilitation Prior failed treatment at a pain management program Heavy tobacco use Heavy alcohol use
 Pain and Addiction: Assessment Issues • Factors identified by clinicians as potential predictors of substance abuse (Jovey 2002) – – – Many automobile accidents Family history of severe depressive or anxiety disorder Family history of drug abuse
Pain and Addiction: Assessment Issues • Factors identified by clinicians as potential predictors of substance abuse (Jovey 2002) – – – Many automobile accidents Family history of severe depressive or anxiety disorder Family history of drug abuse
 Pain and Addiction: Assessment Issues • CAGE-AID screening tool (Brown & Rounds 1995) – – Tried to Cut down or Change your pattern of drinking or drug use? Been Annoyed or Angry by others’ concern about your drinking or drug use? Felt Guilty about the consequences of your drinking or drug use? Had a drink or used a drug in the morning (Eyeopener) to decrease hangover or withdrawal symptoms?
Pain and Addiction: Assessment Issues • CAGE-AID screening tool (Brown & Rounds 1995) – – Tried to Cut down or Change your pattern of drinking or drug use? Been Annoyed or Angry by others’ concern about your drinking or drug use? Felt Guilty about the consequences of your drinking or drug use? Had a drink or used a drug in the morning (Eyeopener) to decrease hangover or withdrawal symptoms?
 Pain and Addiction: Assessment Issues • CAGE-AID screening tool – – – Screens for ongoing abuse Ongoing abuse predicts future abuse Two or more positives has sensitivity of 6095% and specificity of 40 -95% for diagnosing alcohol or drug problems
Pain and Addiction: Assessment Issues • CAGE-AID screening tool – – – Screens for ongoing abuse Ongoing abuse predicts future abuse Two or more positives has sensitivity of 6095% and specificity of 40 -95% for diagnosing alcohol or drug problems
 Pain and Addiction: Assessment Issues • Screening Instrument For Substance Abuse Potential (SISAP) (Coambs et al 1996) – – High sensitivity/low specificity for problems during therapy Factors associated with increased risk • Heavy drinking • Marijuana use last year • Age <40 and a smoker
Pain and Addiction: Assessment Issues • Screening Instrument For Substance Abuse Potential (SISAP) (Coambs et al 1996) – – High sensitivity/low specificity for problems during therapy Factors associated with increased risk • Heavy drinking • Marijuana use last year • Age <40 and a smoker
 Pain and Addiction: Assessment Issues • Factors identified in veterans in a pain program as predictive of opioid abuse (Chabal et al 1997) – – – focus on opioids during clinic visits pattern of early refills or dose escalation multiple telephone calls or visits pertaining to opioid therapy other prescription problems obtaining opioids from other sources
Pain and Addiction: Assessment Issues • Factors identified in veterans in a pain program as predictive of opioid abuse (Chabal et al 1997) – – – focus on opioids during clinic visits pattern of early refills or dose escalation multiple telephone calls or visits pertaining to opioid therapy other prescription problems obtaining opioids from other sources
 Pain and Addiction: Assessment Issues • Factors identified in a pain clinic population as predictive of substance use disorder (Compton et al 1998) – – – tendency to increase the dose preference for a specific route of administration considering oneself addicted.
Pain and Addiction: Assessment Issues • Factors identified in a pain clinic population as predictive of substance use disorder (Compton et al 1998) – – – tendency to increase the dose preference for a specific route of administration considering oneself addicted.
 Pain and Addiction: Assessment Issues • Screening Tool for Addiction Risk (STAR) (Li et al 2001) – Factors distinguishing pain patients with history of substance abuse from others • prior treatment in a drug rehabilitation facility • nicotine use • feeling of excessive nicotine use
Pain and Addiction: Assessment Issues • Screening Tool for Addiction Risk (STAR) (Li et al 2001) – Factors distinguishing pain patients with history of substance abuse from others • prior treatment in a drug rehabilitation facility • nicotine use • feeling of excessive nicotine use
 Pain and Addiction: Assessment Issues • Predicting drug-related problems during opioid therapy: current status – – – Several questionnaires available and several others in development Varied predictor variables Variably predict aberrant drug-related behavior or substance use disorders
Pain and Addiction: Assessment Issues • Predicting drug-related problems during opioid therapy: current status – – – Several questionnaires available and several others in development Varied predictor variables Variably predict aberrant drug-related behavior or substance use disorders
 Pain and Addiction: Assessment Issues • Existing studies do not adequately clarify: – – What should be predicted? What are the best predictor variables? Can screening be done in a clinically feasible manner? Are the predictors generalizable across pain populations?
Pain and Addiction: Assessment Issues • Existing studies do not adequately clarify: – – What should be predicted? What are the best predictor variables? Can screening be done in a clinically feasible manner? Are the predictors generalizable across pain populations?
 Pain and Addiction: Assessment Issues • What to do? – – – Must assess risk even in the lack of conclusive information Substance use history is essential: nature of prior and current history of drug abuse likely to be important Other important factors (? ): major psychiatric pathology, age, family history
Pain and Addiction: Assessment Issues • What to do? – – – Must assess risk even in the lack of conclusive information Substance use history is essential: nature of prior and current history of drug abuse likely to be important Other important factors (? ): major psychiatric pathology, age, family history
 Pain and Addiction: Assessment Issues • What to do? – – – Based on this clinical assessment, categorize patient in terms of risk of problematic drugrelated behavior Categories of “high, ” “medium, ” and “low” can guide the structure of therapy Integrate this evaluation routinely into the pain assessment
Pain and Addiction: Assessment Issues • What to do? – – – Based on this clinical assessment, categorize patient in terms of risk of problematic drugrelated behavior Categories of “high, ” “medium, ” and “low” can guide the structure of therapy Integrate this evaluation routinely into the pain assessment
 Pain and Addiction: Assessment Issues • Process of assessment – – – Collect the data Integrate the findings Develop therapeutic strategy
Pain and Addiction: Assessment Issues • Process of assessment – – – Collect the data Integrate the findings Develop therapeutic strategy
 Pain and Addiction: Assessment Issues • Integrate the findings – Pain diagnoses • • • – – Etiology Pathophysiology Syndrome Impact of the pain Relevant comorbidities
Pain and Addiction: Assessment Issues • Integrate the findings – Pain diagnoses • • • – – Etiology Pathophysiology Syndrome Impact of the pain Relevant comorbidities
 Pain and Addiction: Assessment Issues • Develop a therapeutic strategy for pain and its comorbidities – – Primary treatment for underlying etiology, if appropriate Symptomatic therapies
Pain and Addiction: Assessment Issues • Develop a therapeutic strategy for pain and its comorbidities – – Primary treatment for underlying etiology, if appropriate Symptomatic therapies
 Pain and Addiction: Assessment Issues • Symptomatic therapy Pharmacotherapy Psychological Surgical CAM Rehabilitative Neurostimulatory Anesthesiologic Lifestyle changes
Pain and Addiction: Assessment Issues • Symptomatic therapy Pharmacotherapy Psychological Surgical CAM Rehabilitative Neurostimulatory Anesthesiologic Lifestyle changes


