71dc591ea73e2a7722ca9d28e3b532a8.ppt
- Количество слайдов: 37

Overview of Medical Acupuncture Robert B. Kelly, MD, MS Associate Director & Curriculum Coordinator Fairview Hospital / Cleveland Clinic Family Medicine Residency

Objectives • Traditional Chinese Medicine vs Medical Acupuncture • Traditional and modern understandings of how acupuncture works • Methods and application of Medical Acupuncture • Training and professional certification • Example patients; content of 3 years experience with 170 patients; 1000 treatments given

What is Acupuncture? • Therapeutic insertion of solid needles in various combinations and patterns • Traditional patterns based on principles of encouraging flow of Qi in classical channels • Medical Acupuncture means that treatment is done by a physician; traditional acupuncture is usually combined with nontraditional methods to a minor or major degree

Traditional Chinese Medicine • • Chinese herbs Acupuncture and Moxibustion Massage and manipulation Breathing exercises Pulse and tongue diagnosis Non-western model of health and illness Constitutional factors and types Pathogens - Cold, Heat, Damp, Dry, Wind

Medical Acupuncture • • • Traditional acupuncture, plus Electro-acupuncture PENS (percutaneous electrical nerve stimulation) Periosteal stimulation IMS (intramuscular stimulation) Auricular acupuncture (french, chinese) Scalp acupuncture (chinese, japanese) Non-traditional acupuncture points or “areas” Baldry, Seem, Gokavi, Wong, etc. techniques
Yang Yin

Basic TCM Concepts • Illness caused by interruption of flow of Qi or depletion of Qi with resulting energetic or structural damage • Related concepts of Blood, Shen, Types of Qi • Acupuncture and/or herbs can help restore flow of Qi, renew depleted Qi, thereby relieving symptoms of illness and restoring “organ” function • Diagnoses: “Blood stagnation”, “ Kidney Yin deficiency”, “rising Liver Fire”, Wei Qi deficiency

Medical Acupuncture • Local Effects – Blood flow; increased circulation; temperature – Muscle relaxation, microinjury • Remote Effects – Neurohumoral changes (endorphins and others) – Brain activation (limbic, thalamic, cortical) – Sympathetic and parasympathetic effects • Longer-term Effects – Pain threshold; Nervous system “plasticity” – Improved autonomic function

When Acupuncture Works • • • Problem was going to get better anyway “Placebo” effect Local effect Nonspecific effect (put needles anywhere) Specific effect (it mattered that needles were placed in particular points) • Cumulative specific effect • Combinations of these effects

What patient can expect • More likely than not it will help • Weekly treatment initially; response in chronic problems usually evident after 3 to 6 treatments • Maximum improvement usually evident after 6 -9 treatments • Once maximum improvement is seen, treatment interval can be lengthened • Patient will either need maintenance treatment (most likely) or will have permanent change without further need for treatment (less likely)

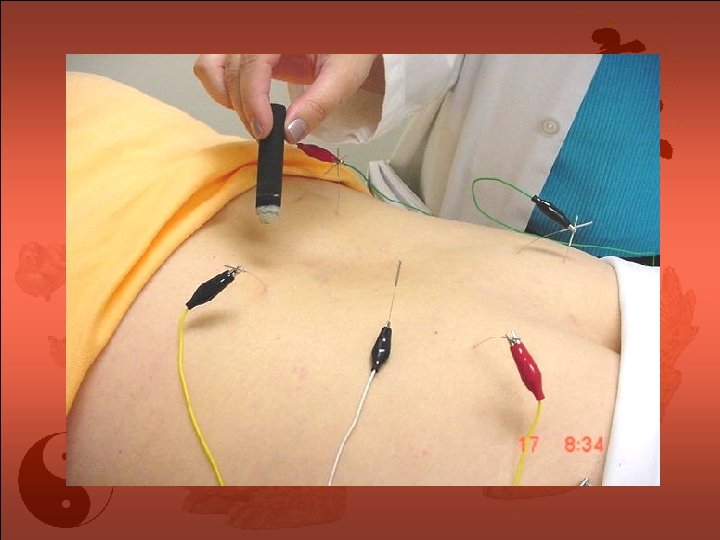
Typical Medical Acupuncture • Pick a principal meridian subcircuit that makes sense for the patient’s problem • Tonify this PM using points below knees and below elbows bilaterally to move Qi in this circuit; electroacupuncture at 2 -4 Hz is commonly used • A local focusing treatment; this varies by problem; may involve more electroacupuncture; 4 -10 Hz can be used if it is PENS or “two-needle” technique • Moxibustion if it makes sense • Reinforcing auricular acupuncture using specific areas or “master points”
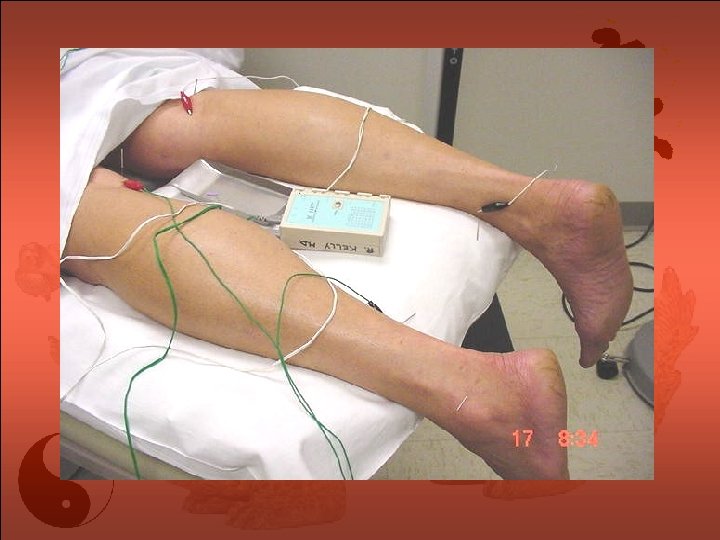
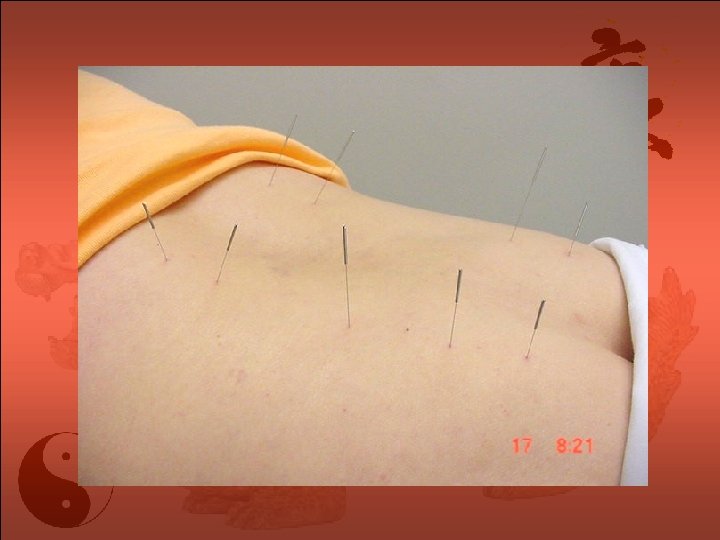
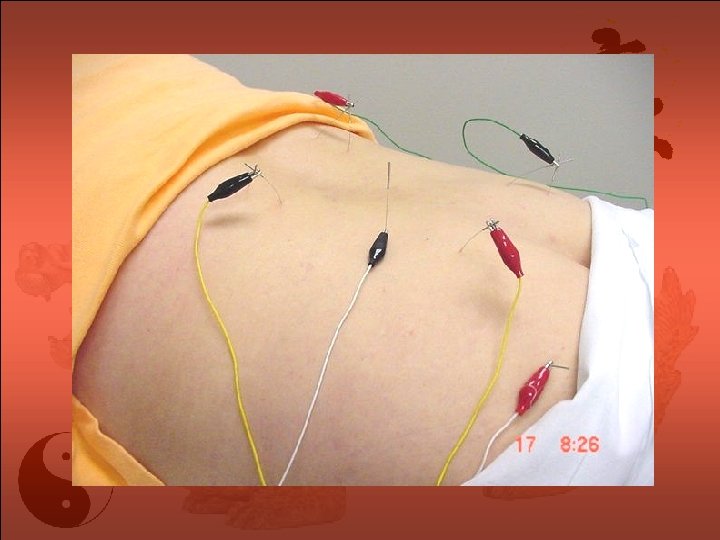
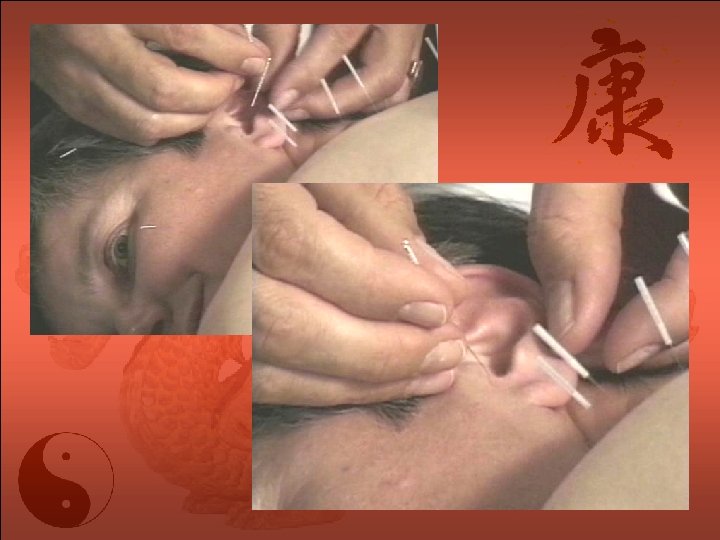
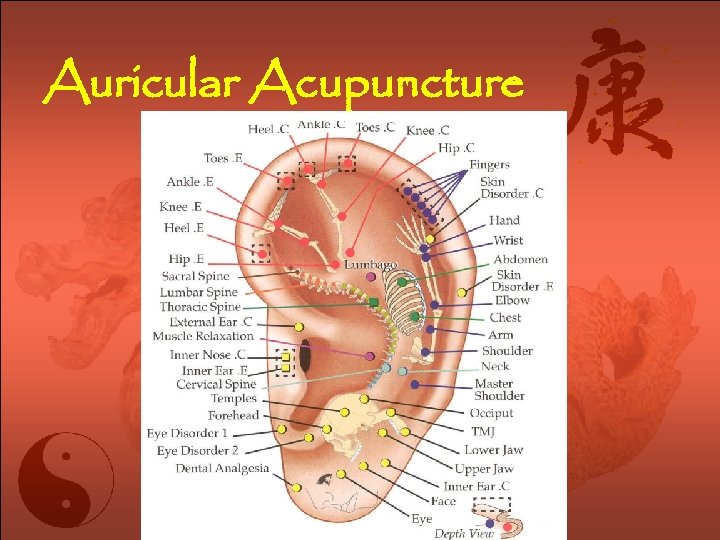
Auricular Acupuncture

Adverse Effects • • • Minor bleeding Needle shock Chondritis Pneumothorax Organ penetration Infection
Uses of Acupuncture • Musculoskeletal pain – Acute: soft tissue contusions, sprains, strains – Chronic: carpal tunnel, tennis elbow, myofascial pain, TMJ, tension headaches, neck pain, degenerative disk disease, sciatica, other LBP • Post operative pain; postop illeus • Nausea of pregnancy, chemotherapy • Boost immune system function – Less well studied and proven; defensive Qi

Uses of Acupuncture • • Addictions – drugs, cigarettes Recurrent sinusitis, URIs, bronchitis Fatigue, mild anxiety, sleep disturbance Irritable bowel, prostatitis, cystitis Dysmenorrhea, infertility Osteoarthritis, bursitis Fibromyalgia, chronic fatigue

Less useful for • Severe, chronic inflammatory conditions, eg, rheumatoid arthritis, collagen vascular disease • Weight loss, obesity • Neurologic problems: migraine, seizures, stroke, dementia

Acupuncture for neck disorders Cochrane Database Syst Rev. 2006 Jul 19; 3: CD 004870. • CONCLUSIONS: There is moderate evidence that acupuncture relieves pain better than some sham treatments, measured at the end of the treatment. There is moderate evidence that those who received acupuncture reported less pain at short term follow-up than those on a waiting list. There is also moderate evidence that acupuncture is more effective than inactive treatments for relieving pain posttreatment and this is maintained at short-term follow-up.

Acupuncture and knee osteoarthritis: A three-armed randomized trial Ann Intern Med. 2006 Jul 4; 145(1): 12 -20. • CONCLUSIONS: Compared with physiotherapy and as-needed anti-inflammatory drugs, addition of either traditional chinese acupuncture (TCA) or sham acupuncture led to greater improvement in Western Ontario and Mc. Master Universities Osteoarthritis Index (WOMAC) score at 26 weeks. No statistically significant difference was observed between TCA and sham acupuncture, suggesting that the observed differences could be due to placebo effects, differences in intensity of provider contact, or a physiologic effect of needling regardless of whether it is done according to TCA principles.

Acupuncture in patients with chronic low back pain: A randomized controlled trial. Arch Intern Med. 2006 Feb 27; 166(4): 450 -7. • METHODS: Patients were randomized to treatment with acupuncture, minimal acupuncture (superficial needling at nonacupuncture points), or a waiting list control. Acupuncture consisted of 12 sessions per patient over 8 weeks. The primary outcome variable was the change in low back pain intensity from baseline to the end of week 8, as determined on a visual analog scale (range, 0 -100 mm). • RESULTS: In 298 patients pain intensity decreased by a mean of 28. 7 mm in the acupuncture group, 23. 6 mm in the minimal acupuncture group, and 6. 9 mm in the waiting list group. The difference for the acupuncture vs minimal acupuncture group was 5. 1 mm (P =. 26), and the difference for the acupuncture vs waiting list group was 21. 7 mm (P<. 001). • CONCLUSION: Acupuncture was more effective in improving pain than no acupuncture treatment in patients with chronic low back pain, whereas there were no significant differences between acupuncture and minimal acupuncture.

Pragmatic randomized trial evaluating the clinical and economic effectiveness of acupuncture for chronic low back pain. Am J Epidemiol. 2006 Sep 1; 164(5): 487 -96. • At 3 months, back function improved by 12. 1 (standard error (SE), 0. 4) to 74. 5 (SE, 0. 4) points in the acupuncture group and by 2. 7 (SE, 0. 4) to 65. 1 (SE, 0. 4) points among controls (difference=9. 4 points (95% confidence interval 8. 3, 10. 5); p<0. 001). Nonrandomized patients had more severe symptoms at baseline and showed improvements in back function similar to those seen in randomized patients. The incremental cost-effectiveness ratio was euro 10, 526 (euros) per quality-adjusted life year. Acupuncture plus routine care was associated with marked clinical improvements in these patients and was relatively cost-effective.

Improvement in fibromyalgia symptoms with acupuncture: Results of a randomized controlled trial. Mayo Clin Proc. 2006 Jun; 81(6): 749 -57. • Total fibromyalgia symptoms, as measured by the Fibromyalgia Impact Questionnaire (FIQ), were significantly improved in the acupuncture group compared with the control group during the study period (P =. 01). The largest difference in mean FIQ total scores was observed at 1 month (42. 2 vs 34. 8 in the control and acupuncture groups, respectively; P =. 007). Fatigue and anxiety were the most significantly improved symptoms during the follow-up period. However, activity and physical function levels did not change. Acupuncture was well tolerated, with minimal adverse effects. • We found that acupuncture significantly improved symptoms of fibromyalgia. Symptomatic improvement was not restricted to pain relief and was most significant for fatigue and anxiety.

A multicentral randomized control study on clinical acupuncture treatment of Bell's palsy. J Tradit Chin Med. 2006 Mar; 26(1): 3 -7. • Patients were randomly divided into the following 3 groups, a control group(treated with prednisone, vitamin B 12 and dibazol), an acu-moxibustion group (treated with filiform needle plus moxibustion), and a basic treatment plus acu-moxibustion group (treated with oral medicine, acupuncture, and moxibustion). The treatment course lasted 4 weeks. The therapeutic effects were evaluated according to the House-Brackmann grading scale and facial disability indexes(FDI). • Therapeutic effects of the two treatment groups were better than the control group (respectively P < 0. 01 and P < 0. 05).

Effect of acupuncture on the outcome of in vitro fertilization and intracytoplasmic sperm injection: a randomized, prospective, controlled clinical study. Fertil Steril. 2006 May; 85(5): 1347 -51. • OBJECTIVE: To determine the effect of luteal-phase acupuncture on the outcome of IVF/intracytoplasmic sperm injection (ICSI). • DESIGN: Randomized, prospective, controlled clinical study. • SETTING: University IVF center. • PATIENT(S): 225 infertile patients undergoing IVF/ICSI. • INTERVENTION(S): In group I, 116 patients received luteal-phase acupuncture according to the principles of traditional Chinese medicine. In group II, 109 patients received placebo acupuncture. • MAIN OUTCOME MEASURE(S): Clinical and ongoing pregnancy rates. RESULT(S): In group I, the clinical pregnancy rate and ongoing pregnancy rate (33. 6% and 28. 4%, respectively) were significantly higher than in group II (15. 6% and 13. 8%). • CONCLUSION(S): Luteal-phase acupuncture has a positive effect on the outcome of IVF/ICSI.

Training & Professional Associations / Boards • Helms Medical Institute “Medical Acupuncture for Physicians” course (UCLA School of Medicine affiliation) • American Academy of Medical Acupuncture – requires minimum of 200 hours training • American Board of Medical Acupuncture requires approved training, successful examination score, and a minimum of 500 treatments over at least two years in practice


Example Patients • E. G. , a 70 year old woman • 6 treatments (March 2006 to May 2006) • Variant of IBS (? ) with prominent chronic nausea (2+ years), as well as chronic insomnia. • Result: Has GI symptom improvement with essentially complete resolution of nausea; much less need for medications to help sleep. • Has not required any ongoing treatment to maintain benefit. Now beginning treatment for hip pain, seemingly a trochanteric bursitis

Example Patients • B. B. , a 44 year old man • 8 treatments (Feb 2006 to present) • Cryptogenic severe L ear and L facial pain episodes of several days’ duration ranging from q 2 months to q 2 weeks for several years, very incapacitating when they occur • Result: No episodes since beginning acupuncture • Has not wanted to stop treatments for fear his pattern will return. On quarterly maintenance.

Example Patients • L. S. , a 54 yo woman • 22 treatments (December 2004 -present) • Daily chronic low back left-sided sciatic pain with L 4 -L 5 and L 5 -S 1 level narrowing; limits activities and exercise. • Result: Has better mobility, ADL function, and ability to exercise. • Requires every 6 week maintenance treatment to maintain the benefits of acupuncture.

Example Patients • R. B. , a 63 year old man • 8 treatments (January 2005 to May 2005) • Chronic lower left jaw trigeminal neuralgia pain. Prior to acupuncture, symptoms controlled with daily medication in fairly high doses (tegretol and gabapentin) and with undesirable side effects. • Result: Reduced need for medication (from 11 to 2 pills/day) with good control of symptoms • No ongoing treatment needed in more than 1 year.

First Two Years, 120 patients • • 37 - Mechanical Back / Neck pain 22 – Joint pain, eg. Knee / Hip / Shoulder 13 - Neuralgia / Neuropathic pain 12 - Tendonitis / Carpal tunnel 11 - Fibromyalgia / Myofascial pain 10 - Gastrointestinal / Digestion / IBS 9 - Fatigue / CFS / Autonomic Dysfunction 6 - Allergy / Sinus / Asthma • Misc. : Migraine HA, Tinnitus, Bell’s Palsy, Obesity, Depression, Smoking, Infertility, ED, Incontinence, Insomnia, Anxiety
71dc591ea73e2a7722ca9d28e3b532a8.ppt