f7da7cf199448c7b20c7f8996e91e976.ppt
- Количество слайдов: 138
 Overview of High Consequence Livestock Pathogens For veterinarians Center for Food Security and Public Health Iowa State University 2004
Overview of High Consequence Livestock Pathogens For veterinarians Center for Food Security and Public Health Iowa State University 2004
 USDA High Consequence Livestock Pathogens and Toxins Center for Food Security and Public Health Iowa State University 2004
USDA High Consequence Livestock Pathogens and Toxins Center for Food Security and Public Health Iowa State University 2004
 Disease Awareness Veterinarians recognize animal diseases at the local level • Prepare by knowing • − Typical signs of diseases − Basic disease etiology − Economic and trade impact − How to report suspected cases • Disseminate knowledge Center for Food Security and Public Health Iowa State University 2004
Disease Awareness Veterinarians recognize animal diseases at the local level • Prepare by knowing • − Typical signs of diseases − Basic disease etiology − Economic and trade impact − How to report suspected cases • Disseminate knowledge Center for Food Security and Public Health Iowa State University 2004
 Overview Importance of agriculture and livestock to U. S. economy • High consequence livestock pathogens • − CDC’s Category A, B, C Bioterrorism Agent List − Additional diseases • Veterinarian’s responsibilities Center for Food Security and Public Health Iowa State University 2004
Overview Importance of agriculture and livestock to U. S. economy • High consequence livestock pathogens • − CDC’s Category A, B, C Bioterrorism Agent List − Additional diseases • Veterinarian’s responsibilities Center for Food Security and Public Health Iowa State University 2004
 Importance of Agriculture & Livestock Center for Food Security and Public Health Iowa State University 2004
Importance of Agriculture & Livestock Center for Food Security and Public Health Iowa State University 2004
 U. S. Agriculture • Exports are our lifeblood − 2003, $56. 2 billion exported in agricultural commodities § • $12. 2 billion from animal/animal products Some diseases reportable to the OIE − Trade • could be halted Negative effect on economy, livestock/grain producers, and employment rate Center for Food Security and Public Health Iowa State University 2004
U. S. Agriculture • Exports are our lifeblood − 2003, $56. 2 billion exported in agricultural commodities § • $12. 2 billion from animal/animal products Some diseases reportable to the OIE − Trade • could be halted Negative effect on economy, livestock/grain producers, and employment rate Center for Food Security and Public Health Iowa State University 2004
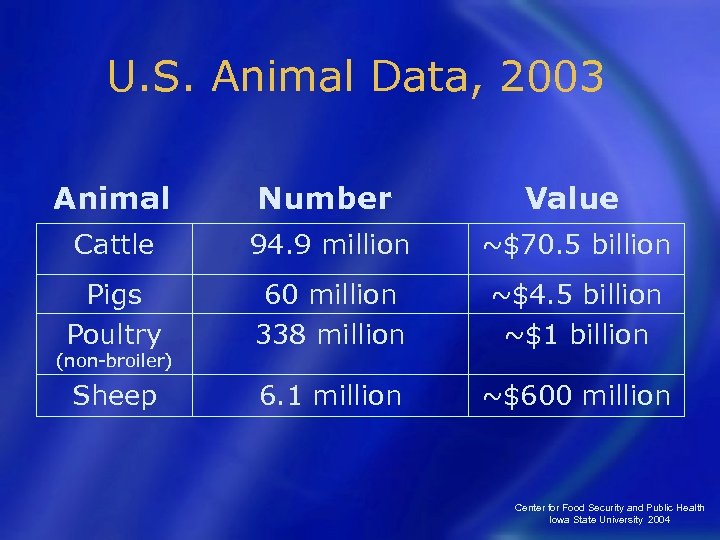 U. S. Animal Data, 2003 Animal Number Value Cattle 94. 9 million ~$70. 5 billion Pigs Poultry 60 million 338 million ~$4. 5 billion ~$1 billion Sheep 6. 1 million ~$600 million (non-broiler) Center for Food Security and Public Health Iowa State University 2004
U. S. Animal Data, 2003 Animal Number Value Cattle 94. 9 million ~$70. 5 billion Pigs Poultry 60 million 338 million ~$4. 5 billion ~$1 billion Sheep 6. 1 million ~$600 million (non-broiler) Center for Food Security and Public Health Iowa State University 2004
 Some Agents are Zoonotic Disease may be seen in animals before humans • Animals are sentinels • − Pets, livestock, wildlife Protect yourself • Educate your clients about the risks • Center for Food Security and Public Health Iowa State University 2004
Some Agents are Zoonotic Disease may be seen in animals before humans • Animals are sentinels • − Pets, livestock, wildlife Protect yourself • Educate your clients about the risks • Center for Food Security and Public Health Iowa State University 2004
 Biosecurity: Veterinarians Disinfect your clothes, boots, equipment between farms • Avoid vehicle contamination • Follow biosecurity guidelines set forth by species-specific associations • Center for Food Security and Public Health Iowa State University 2004
Biosecurity: Veterinarians Disinfect your clothes, boots, equipment between farms • Avoid vehicle contamination • Follow biosecurity guidelines set forth by species-specific associations • Center for Food Security and Public Health Iowa State University 2004
 CDC Category ABC Agent Overview Center for Food Security and Public Health Iowa State University 2004
CDC Category ABC Agent Overview Center for Food Security and Public Health Iowa State University 2004
 Classification Prepared by the CDC’s Bioterrorism Preparedness and Response Office • Category A: Highest priority • Category B: Second highest priority • Category C: Third highest priority • Center for Food Security and Public Health Iowa State University 2004
Classification Prepared by the CDC’s Bioterrorism Preparedness and Response Office • Category A: Highest priority • Category B: Second highest priority • Category C: Third highest priority • Center for Food Security and Public Health Iowa State University 2004
 CDC Category ABC Agents Category A • Anthrax • Botulism • Tularemia Category B • Brucellosis • Glanders • Melioidosis • Q Fever • Viral encephalitis • Toxins Category C • Nipah Center for Food Security and Public Health Iowa State University 2004
CDC Category ABC Agents Category A • Anthrax • Botulism • Tularemia Category B • Brucellosis • Glanders • Melioidosis • Q Fever • Viral encephalitis • Toxins Category C • Nipah Center for Food Security and Public Health Iowa State University 2004
 “Weaponization” of Agents • Alter characteristics of a pathogen to make it a more effective weapon − Enhance transmission − Increase virulence − Resistant to antibiotics − Evade vaccine protection − Alter clinical signs Center for Food Security and Public Health Iowa State University 2004
“Weaponization” of Agents • Alter characteristics of a pathogen to make it a more effective weapon − Enhance transmission − Increase virulence − Resistant to antibiotics − Evade vaccine protection − Alter clinical signs Center for Food Security and Public Health Iowa State University 2004
 Note to presenter As time allows select diseases you would like to review. • The CDC Category A, B, C diseases are listed first, and then you will see the additional High Consequence Livestock Pathogens. • The disease coverage is brief. If you would like more information on a disease, refer to the fact sheet or to the disease specific presentation. • Center for Food Security and Public Health Iowa State University 2004
Note to presenter As time allows select diseases you would like to review. • The CDC Category A, B, C diseases are listed first, and then you will see the additional High Consequence Livestock Pathogens. • The disease coverage is brief. If you would like more information on a disease, refer to the fact sheet or to the disease specific presentation. • Center for Food Security and Public Health Iowa State University 2004
 CDC Category A Anthrax Botulism Tularemia Center for Food Security and Public Health Iowa State University 2004
CDC Category A Anthrax Botulism Tularemia Center for Food Security and Public Health Iowa State University 2004
 Anthrax: The Agent Bacillus anthracis – Gram positive spore-forming bacteria • Forms spores • Human disease • − Skin − Intestinal − Pulmonary • Animal disease − Septicemia and rapid death Center for Food Security and Public Health Iowa State University 2004
Anthrax: The Agent Bacillus anthracis – Gram positive spore-forming bacteria • Forms spores • Human disease • − Skin − Intestinal − Pulmonary • Animal disease − Septicemia and rapid death Center for Food Security and Public Health Iowa State University 2004
 Anthrax: The Bioweapon • • History Available & easily produced Spores infective Aerosolization Low lethal dose High mortality Person-to-person transmission rare Center for Food Security and Public Health Iowa State University 2004
Anthrax: The Bioweapon • • History Available & easily produced Spores infective Aerosolization Low lethal dose High mortality Person-to-person transmission rare Center for Food Security and Public Health Iowa State University 2004
 Anthrax: The Response • Vaccine − Humans − Animals • Antibiotics − Treatment − Prophylaxis • Disinfection − Sporicidal agents, sterilization Center for Food Security and Public Health Iowa State University 2004
Anthrax: The Response • Vaccine − Humans − Animals • Antibiotics − Treatment − Prophylaxis • Disinfection − Sporicidal agents, sterilization Center for Food Security and Public Health Iowa State University 2004
 Botulism: The Agent Clostridium botulinum – Gram positive, spore-forming bacteria • 7 different neurotoxins • − Types • A-G Clinical signs − Flaccid paralysis − Pigs, dogs, and cats fairly resistant Center for Food Security and Public Health Iowa State University 2004
Botulism: The Agent Clostridium botulinum – Gram positive, spore-forming bacteria • 7 different neurotoxins • − Types • A-G Clinical signs − Flaccid paralysis − Pigs, dogs, and cats fairly resistant Center for Food Security and Public Health Iowa State University 2004
 Botulism: The Bioweapon • • • Used by Aum Shinrikyo cult in Japan Aerosolized Easy to produce and transport Potent and lethal Most poisonous substance known Center for Food Security and Public Health Iowa State University 2004
Botulism: The Bioweapon • • • Used by Aum Shinrikyo cult in Japan Aerosolized Easy to produce and transport Potent and lethal Most poisonous substance known Center for Food Security and Public Health Iowa State University 2004
 Botulism: The Response Toxoids for high risk people • Antitoxin available • − Case-by-case • basis Botulinum toxins are easily inactivated with many disinfectants and heat Center for Food Security and Public Health Iowa State University 2004
Botulism: The Response Toxoids for high risk people • Antitoxin available • − Case-by-case • basis Botulinum toxins are easily inactivated with many disinfectants and heat Center for Food Security and Public Health Iowa State University 2004
 Tularemia: The Agent Francisella tularensis • Transmitted by ingestion, inhalation, vectors, direct contact through skin • Six clinical forms in humans • Glandular Ulceroglandular Center for Food Security and Public Health Iowa State University 2004
Tularemia: The Agent Francisella tularensis • Transmitted by ingestion, inhalation, vectors, direct contact through skin • Six clinical forms in humans • Glandular Ulceroglandular Center for Food Security and Public Health Iowa State University 2004
 Tularemia: The Agent • Sheep, young pigs, horses, dogs, cats • Sudden fever, lethargy, stiffness, prostration, and death • Wildlife • Usually find dead • Rabbits behave strangely • Cattle, older pigs resistant Center for Food Security and Public Health Iowa State University 2004
Tularemia: The Agent • Sheep, young pigs, horses, dogs, cats • Sudden fever, lethargy, stiffness, prostration, and death • Wildlife • Usually find dead • Rabbits behave strangely • Cattle, older pigs resistant Center for Food Security and Public Health Iowa State University 2004
 Tularemia: The Bioweapon • • • Stable Aerosolized Low infective dose via inhalation Case fatality: 30 -60% (untreated) WHO estimation: 1970 − 50 kg agent: City population 5 million § 250, 000 ill § 19, 000 deaths Center for Food Security and Public Health Iowa State University 2004
Tularemia: The Bioweapon • • • Stable Aerosolized Low infective dose via inhalation Case fatality: 30 -60% (untreated) WHO estimation: 1970 − 50 kg agent: City population 5 million § 250, 000 ill § 19, 000 deaths Center for Food Security and Public Health Iowa State University 2004
 Tularemia: The Response Person-to-person transmission not documented • Antibiotics effective, if early or prophylactic • Vaccine • − For high risk individuals − Unknown efficacy against inhalational tularemia Center for Food Security and Public Health Iowa State University 2004
Tularemia: The Response Person-to-person transmission not documented • Antibiotics effective, if early or prophylactic • Vaccine • − For high risk individuals − Unknown efficacy against inhalational tularemia Center for Food Security and Public Health Iowa State University 2004
 CDC Category B Brucellosis Q Fever Glanders. Toxins Melioidosis Viral Encephalitis Center for Food Security and Public Health Iowa State University 2004
CDC Category B Brucellosis Q Fever Glanders. Toxins Melioidosis Viral Encephalitis Center for Food Security and Public Health Iowa State University 2004
 Brucellosis: The Agent Gram-negative bacteria • Ingestion, inhalation, or direct contact • Clinical signs • − Humans: cyclic fever and flu-like symptoms − Animals: reproductive signs Center for Food Security and Public Health Iowa State University 2004
Brucellosis: The Agent Gram-negative bacteria • Ingestion, inhalation, or direct contact • Clinical signs • − Humans: cyclic fever and flu-like symptoms − Animals: reproductive signs Center for Food Security and Public Health Iowa State University 2004
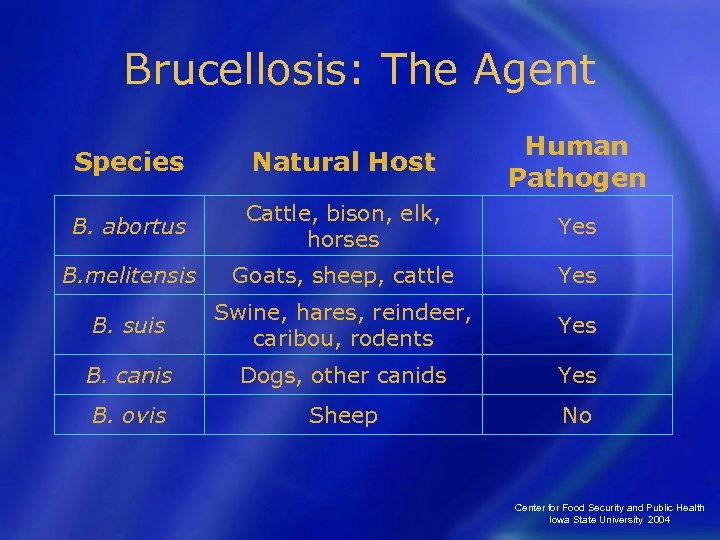 Brucellosis: The Agent Species Natural Host Human Pathogen B. abortus Cattle, bison, elk, horses Yes B. melitensis Goats, sheep, cattle Yes B. suis Swine, hares, reindeer, caribou, rodents Yes B. canis Dogs, other canids Yes B. ovis Sheep No Center for Food Security and Public Health Iowa State University 2004
Brucellosis: The Agent Species Natural Host Human Pathogen B. abortus Cattle, bison, elk, horses Yes B. melitensis Goats, sheep, cattle Yes B. suis Swine, hares, reindeer, caribou, rodents Yes B. canis Dogs, other canids Yes B. ovis Sheep No Center for Food Security and Public Health Iowa State University 2004
 Brucellosis: The Bioweapon • • • History Highly infectious Easily aerosolized Stable Prolonged incubation period − May • make diagnosis difficult Person-to-person unlikely Center for Food Security and Public Health Iowa State University 2004
Brucellosis: The Bioweapon • • • History Highly infectious Easily aerosolized Stable Prolonged incubation period − May • make diagnosis difficult Person-to-person unlikely Center for Food Security and Public Health Iowa State University 2004
 Brucellosis: The Response • • • Long term antibiotics generally effective Vaccinate calves, no human vaccine Eliminate reservoir Standard precaution to avoid exposure Thorough disinfection Center for Food Security and Public Health Iowa State University 2004
Brucellosis: The Response • • • Long term antibiotics generally effective Vaccinate calves, no human vaccine Eliminate reservoir Standard precaution to avoid exposure Thorough disinfection Center for Food Security and Public Health Iowa State University 2004
 Glanders: The Agent Burkholderia mallei: Gram-negative • Transmission by ingestion, inhalation, or direct contact • − Animal-to-human transmission is inefficient • Clinical signs − Humans & horses: cutaneous & pulmonary lesions, rapidly fatal illness Center for Food Security and Public Health Iowa State University 2004
Glanders: The Agent Burkholderia mallei: Gram-negative • Transmission by ingestion, inhalation, or direct contact • − Animal-to-human transmission is inefficient • Clinical signs − Humans & horses: cutaneous & pulmonary lesions, rapidly fatal illness Center for Food Security and Public Health Iowa State University 2004
 Glanders: The Bioweapon • History − WWI Russian horses − WWII Chinese civilians, horses, POW’s Easy to produce • Aerosolized, highly infectious • Mortality high in chronic form • − 50 -70% • Person to person transmission: Rare Center for Food Security and Public Health Iowa State University 2004
Glanders: The Bioweapon • History − WWI Russian horses − WWII Chinese civilians, horses, POW’s Easy to produce • Aerosolized, highly infectious • Mortality high in chronic form • − 50 -70% • Person to person transmission: Rare Center for Food Security and Public Health Iowa State University 2004
 Glanders: The Response No vaccine • Antibiotic therapy likely effective • Destroyed by various chemicals • Center for Food Security and Public Health Iowa State University 2004
Glanders: The Response No vaccine • Antibiotic therapy likely effective • Destroyed by various chemicals • Center for Food Security and Public Health Iowa State University 2004
 Melioidosis: The Agent Burkholderia pseudomallei: Gram-negative • Transmission: Contact, ingestion, inhalation • Clinical signs: Humans, sheep, goats, and pigs • − Asymptomatic to pneumonia, lung and wound abscesses Center for Food Security and Public Health Iowa State University 2004
Melioidosis: The Agent Burkholderia pseudomallei: Gram-negative • Transmission: Contact, ingestion, inhalation • Clinical signs: Humans, sheep, goats, and pigs • − Asymptomatic to pneumonia, lung and wound abscesses Center for Food Security and Public Health Iowa State University 2004
 Melioidosis: The Bioweapon • • • Easy to produce Available Aerosolization High mortality: 90% Person-to-person (rare) Animal-to-person (rare) Center for Food Security and Public Health Iowa State University 2004
Melioidosis: The Bioweapon • • • Easy to produce Available Aerosolization High mortality: 90% Person-to-person (rare) Animal-to-person (rare) Center for Food Security and Public Health Iowa State University 2004
 Melioidosis: The Response Long-term, multiple antibiotics effective • Vaccines available: not in U. S. • Easily destroyed by disinfectants • Center for Food Security and Public Health Iowa State University 2004
Melioidosis: The Response Long-term, multiple antibiotics effective • Vaccines available: not in U. S. • Easily destroyed by disinfectants • Center for Food Security and Public Health Iowa State University 2004
 Toxins: The Agents Staphylococcal enterotoxin B (SEB) • Ricin toxin from castor plant • Clostridium perfringens epsilon toxin • Center for Food Security and Public Health Iowa State University 2004
Toxins: The Agents Staphylococcal enterotoxin B (SEB) • Ricin toxin from castor plant • Clostridium perfringens epsilon toxin • Center for Food Security and Public Health Iowa State University 2004
 SEB: The Agent Staphylococcal enterotoxin B (SEB) • A common cause of food poisoning • Clinical signs: Humans • − Fever, chills, headache, myalgia − Non-productive cough if inhaled − GI signs if swallowed • Animals: Likely similar to human Center for Food Security and Public Health Iowa State University 2004
SEB: The Agent Staphylococcal enterotoxin B (SEB) • A common cause of food poisoning • Clinical signs: Humans • − Fever, chills, headache, myalgia − Non-productive cough if inhaled − GI signs if swallowed • Animals: Likely similar to human Center for Food Security and Public Health Iowa State University 2004
 Ricin: The Agent Ricin toxin from bean of castor plant • Available worldwide • Clinical signs • − Acute onset of fever, chest tightness, cough, dyspnea, nausea Center for Food Security and Public Health Iowa State University 2004
Ricin: The Agent Ricin toxin from bean of castor plant • Available worldwide • Clinical signs • − Acute onset of fever, chest tightness, cough, dyspnea, nausea Center for Food Security and Public Health Iowa State University 2004
 Epsilon Toxin: The Agent Clostridium perfringens type B and D • Increases intestinal and vascular permeability, liver and neurological damage • Clinical signs • − Calves: Diarrhea, abdominal pain, listlessness, neurologic − Sheep, goats: Watery to bloody diarrhea, neurologic − Humans: Little information Center for Food Security and Public Health Iowa State University 2004
Epsilon Toxin: The Agent Clostridium perfringens type B and D • Increases intestinal and vascular permeability, liver and neurological damage • Clinical signs • − Calves: Diarrhea, abdominal pain, listlessness, neurologic − Sheep, goats: Watery to bloody diarrhea, neurologic − Humans: Little information Center for Food Security and Public Health Iowa State University 2004
 Toxins: The Bioweapon • • • History Aerosolized: SEB, ricin Available worldwide Easy to produce, stable Many species affected No person-to-person transmission Center for Food Security and Public Health Iowa State University 2004
Toxins: The Bioweapon • • • History Aerosolized: SEB, ricin Available worldwide Easy to produce, stable Many species affected No person-to-person transmission Center for Food Security and Public Health Iowa State University 2004
 Toxins: The Response Supportive care • No vaccines currently available for SEB or ricin • Vaccines for animals for clostridial disease • Toxins are inactivated with common disinfectants • Center for Food Security and Public Health Iowa State University 2004
Toxins: The Response Supportive care • No vaccines currently available for SEB or ricin • Vaccines for animals for clostridial disease • Toxins are inactivated with common disinfectants • Center for Food Security and Public Health Iowa State University 2004
 Viral Encephalitis: The Agent The Alphaviruses: EEE, WEE, and VEE • Transmitted via mosquito • Clinical signs • − Humans, horses, donkeys, mules: Often asymptomatic to flu-like − Encephalitis in small proportions • Birds are asymptomatic carriers, act as sentinels Center for Food Security and Public Health Iowa State University 2004
Viral Encephalitis: The Agent The Alphaviruses: EEE, WEE, and VEE • Transmitted via mosquito • Clinical signs • − Humans, horses, donkeys, mules: Often asymptomatic to flu-like − Encephalitis in small proportions • Birds are asymptomatic carriers, act as sentinels Center for Food Security and Public Health Iowa State University 2004
 Viral Encephalitis: The Bioweapon Easy to produce • Aerosolization • High rate of infection • Person-to-person transmission possible • Center for Food Security and Public Health Iowa State University 2004
Viral Encephalitis: The Bioweapon Easy to produce • Aerosolization • High rate of infection • Person-to-person transmission possible • Center for Food Security and Public Health Iowa State University 2004
 Viral Encephalitis: The Response Supportive care • Vaccine • • Virus unstable in environment − Equine − Human: High risk Center for Food Security and Public Health Iowa State University 2004
Viral Encephalitis: The Response Supportive care • Vaccine • • Virus unstable in environment − Equine − Human: High risk Center for Food Security and Public Health Iowa State University 2004
 CDC Category C Nipah Center for Food Security and Public Health Iowa State University 2004
CDC Category C Nipah Center for Food Security and Public Health Iowa State University 2004
 Nipah Virus: The Agent Paramyxovirus • Fruit bat reservoir • Clinical signs • − Humans: Encephalitis − Pigs: Respiratory, neurological − Dogs and cats: “Distemper” Center for Food Security and Public Health Iowa State University 2004
Nipah Virus: The Agent Paramyxovirus • Fruit bat reservoir • Clinical signs • − Humans: Encephalitis − Pigs: Respiratory, neurological − Dogs and cats: “Distemper” Center for Food Security and Public Health Iowa State University 2004
 Nipah Virus: The Bioweapon Aerosolization potential • Wide host range • No person-to-person transmission expected • High morbidity and mortality • Center for Food Security and Public Health Iowa State University 2004
Nipah Virus: The Bioweapon Aerosolization potential • Wide host range • No person-to-person transmission expected • High morbidity and mortality • Center for Food Security and Public Health Iowa State University 2004
 Nipah Virus: The Response Avoid contact with all infected animals and fluids • Vaccine being researched • Call authorities immediately • Center for Food Security and Public Health Iowa State University 2004
Nipah Virus: The Response Avoid contact with all infected animals and fluids • Vaccine being researched • Call authorities immediately • Center for Food Security and Public Health Iowa State University 2004
 Other Important Diseases Rift Valley Fever • Hendra Virus • Center for Food Security and Public Health Iowa State University 2004
Other Important Diseases Rift Valley Fever • Hendra Virus • Center for Food Security and Public Health Iowa State University 2004
 Rift Valley Fever: The Agent Phlebovirus in family Bunyaviridae • Transmission: Mosquito, inhalation, contact with infected body fluids • Clinical signs • − Humans: headache § Flu-like, fever, Severe disease: Retinitis, hemorrhagic fever − Animals: Abortions, death in neonates Center for Food Security and Public Health Iowa State University 2004
Rift Valley Fever: The Agent Phlebovirus in family Bunyaviridae • Transmission: Mosquito, inhalation, contact with infected body fluids • Clinical signs • − Humans: headache § Flu-like, fever, Severe disease: Retinitis, hemorrhagic fever − Animals: Abortions, death in neonates Center for Food Security and Public Health Iowa State University 2004
 Rift Valley Fever: The Bioweapon • WHO estimate: 1970 − 50 kg of virus aerosolized − 35, 000 incapacitated − 400 deaths (1% mortality) Stable at most temperatures • Inactivated by various chemicals • Center for Food Security and Public Health Iowa State University 2004
Rift Valley Fever: The Bioweapon • WHO estimate: 1970 − 50 kg of virus aerosolized − 35, 000 incapacitated − 400 deaths (1% mortality) Stable at most temperatures • Inactivated by various chemicals • Center for Food Security and Public Health Iowa State University 2004
 Rift Valley Fever: The Response Vaccinate ruminants in endemic areas • Control mosquitoes • Avoid contact with infected tissues & blood • − Wear • protective clothing No person-to-person transmission Center for Food Security and Public Health Iowa State University 2004
Rift Valley Fever: The Response Vaccinate ruminants in endemic areas • Control mosquitoes • Avoid contact with infected tissues & blood • − Wear • protective clothing No person-to-person transmission Center for Food Security and Public Health Iowa State University 2004
 Hendra Virus: The Agent • Newly discovered − Australia Fruit bats • Transmission: Urine, body fluids • Humans • − Flu-like • illness, respiratory failure Horses, cats − Acute respiratory signs, nasal discharge, fever, encephalitis, sudden death Center for Food Security and Public Health Iowa State University 2004
Hendra Virus: The Agent • Newly discovered − Australia Fruit bats • Transmission: Urine, body fluids • Humans • − Flu-like • illness, respiratory failure Horses, cats − Acute respiratory signs, nasal discharge, fever, encephalitis, sudden death Center for Food Security and Public Health Iowa State University 2004
 Hendra Virus: The Response Little is known about disease • Highest level of security to work with the agent • Potentially serious consequences • − High mortality rate − Lack of treatment Center for Food Security and Public Health Iowa State University 2004
Hendra Virus: The Response Little is known about disease • Highest level of security to work with the agent • Potentially serious consequences • − High mortality rate − Lack of treatment Center for Food Security and Public Health Iowa State University 2004
 Additional High Consequence Livestock Pathogens Center for Food Security and Public Health Iowa State University 2004
Additional High Consequence Livestock Pathogens Center for Food Security and Public Health Iowa State University 2004
 Additional High Consequence Livestock Pathogens • • • African horse sickness African swine fever Akabane Avian influenza (HP) Bluetongue BSE Classical swine fever Coccidioidomycosis Contagious bovine pleuropneumonia Contagious caprine pleuropneumonia Foot and mouth disease • • • Heartwater Japanese encephalitis Lumpy skin disease Malignant catarrhal fever Menangle Newcastle disease Peste des petit ruminants Rinderpest Screwworm myiasis Sheep/goat pox Swine vesicular disease Vesicular stomatitis Center for Food Security and Public Health Iowa State University 2004
Additional High Consequence Livestock Pathogens • • • African horse sickness African swine fever Akabane Avian influenza (HP) Bluetongue BSE Classical swine fever Coccidioidomycosis Contagious bovine pleuropneumonia Contagious caprine pleuropneumonia Foot and mouth disease • • • Heartwater Japanese encephalitis Lumpy skin disease Malignant catarrhal fever Menangle Newcastle disease Peste des petit ruminants Rinderpest Screwworm myiasis Sheep/goat pox Swine vesicular disease Vesicular stomatitis Center for Food Security and Public Health Iowa State University 2004
 World Organisation for Animal Health Early Warning System • Disease reported within 24 hours • Informs countries at risk • Trade shut down until further notice • Center for Food Security and Public Health Iowa State University 2004
World Organisation for Animal Health Early Warning System • Disease reported within 24 hours • Informs countries at risk • Trade shut down until further notice • Center for Food Security and Public Health Iowa State University 2004
 African Horse Sickness Viral infection • Horses, mules, donkeys • − Lethal • disease Arthropod-borne − Culicoides sp. (biting midges) Endemic in sub-Saharan Africa • Peak: Late summer - early autumn • − Prevalence influenced by climate Center for Food Security and Public Health Iowa State University 2004
African Horse Sickness Viral infection • Horses, mules, donkeys • − Lethal • disease Arthropod-borne − Culicoides sp. (biting midges) Endemic in sub-Saharan Africa • Peak: Late summer - early autumn • − Prevalence influenced by climate Center for Food Security and Public Health Iowa State University 2004
 AHS: The Disease • Incubation period: 2 -14 days − Clinical • signs typically seen in 5 -7 days Four forms of the disease − Pulmonary § Mortality 100% − Cardiac § Mortality 50 -70% − Mixed-pulmonary and cardiac − Horsesickness fever § Rarely fatal Center for Food Security and Public Health Iowa State University 2004
AHS: The Disease • Incubation period: 2 -14 days − Clinical • signs typically seen in 5 -7 days Four forms of the disease − Pulmonary § Mortality 100% − Cardiac § Mortality 50 -70% − Mixed-pulmonary and cardiac − Horsesickness fever § Rarely fatal Center for Food Security and Public Health Iowa State University 2004
 AHS: Impact & Response • 1989: Portugal outbreak − Eradication • cost $1. 9 million U. S. Horse Industry − Inventory: 5. 25 million horses − Value of sales: $1. 75 billion Vaccine available in endemic areas • No natural human infection • Vector control imperative to disease control • Center for Food Security and Public Health Iowa State University 2004
AHS: Impact & Response • 1989: Portugal outbreak − Eradication • cost $1. 9 million U. S. Horse Industry − Inventory: 5. 25 million horses − Value of sales: $1. 75 billion Vaccine available in endemic areas • No natural human infection • Vector control imperative to disease control • Center for Food Security and Public Health Iowa State University 2004
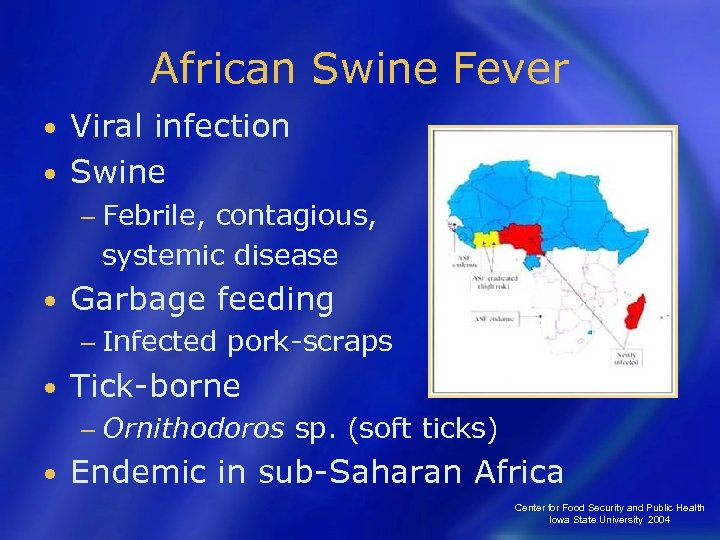 African Swine Fever Viral infection • Swine • − Febrile, contagious, systemic disease • Garbage feeding − Infected • pork-scraps Tick-borne − Ornithodoros • sp. (soft ticks) Endemic in sub-Saharan Africa Center for Food Security and Public Health Iowa State University 2004
African Swine Fever Viral infection • Swine • − Febrile, contagious, systemic disease • Garbage feeding − Infected • pork-scraps Tick-borne − Ornithodoros • sp. (soft ticks) Endemic in sub-Saharan Africa Center for Food Security and Public Health Iowa State University 2004
 ASF: The Disease Incubation period: 48 -72 hours • Chronic infection • − Low fever, multi-focal erythema (raised and necrotic), pneumonia, swelling of joints • painless High virulence (100% mortality) − High fever, recumbency, erythema, anorexia, death • Low virulence (seroconversion) Center for Food Security and Public Health Iowa State University 2004
ASF: The Disease Incubation period: 48 -72 hours • Chronic infection • − Low fever, multi-focal erythema (raised and necrotic), pneumonia, swelling of joints • painless High virulence (100% mortality) − High fever, recumbency, erythema, anorexia, death • Low virulence (seroconversion) Center for Food Security and Public Health Iowa State University 2004
 ASF: Impact and Response • Morbidity approaches 100% − Mortality • varies with virulence (0 -100%) Import/export ban of hogs − Isolation and slaughter required for eradication − Huge economic impact No treatment or vaccine • Humans not susceptible to disease • Center for Food Security and Public Health Iowa State University 2004
ASF: Impact and Response • Morbidity approaches 100% − Mortality • varies with virulence (0 -100%) Import/export ban of hogs − Isolation and slaughter required for eradication − Huge economic impact No treatment or vaccine • Humans not susceptible to disease • Center for Food Security and Public Health Iowa State University 2004
 Akabane Viral infection • Cattle, sheep, goats • − Reproductive disorders − Asymptomatic dams Mosquitoes, biting midges • Tropics and subtropics • − Australia, Japan, Israel, Korea − Incidence related to climate, season Center for Food Security and Public Health Iowa State University 2004
Akabane Viral infection • Cattle, sheep, goats • − Reproductive disorders − Asymptomatic dams Mosquitoes, biting midges • Tropics and subtropics • − Australia, Japan, Israel, Korea − Incidence related to climate, season Center for Food Security and Public Health Iowa State University 2004
 Akabane: The Disease Viremia: 1 -6 days infection • Adults asymptomatic • Pregnant ruminants post- • − Abortion and stillbirths − Dystocia • Congenital abnormalities − Varies with stage of gestation Center for Food Security and Public Health Iowa State University 2004
Akabane: The Disease Viremia: 1 -6 days infection • Adults asymptomatic • Pregnant ruminants post- • − Abortion and stillbirths − Dystocia • Congenital abnormalities − Varies with stage of gestation Center for Food Security and Public Health Iowa State University 2004
 Akabane: Impact and Response • 2002 U. S. livestock statistics − Calves: 38. 2 million head − Lambs: 4. 36 million head − U. S. livestock naïve No effective treatment • No natural human infection • Potential vectors found in U. S. • − Control • vector to control disease Vaccine used in Japan Center for Food Security and Public Health Iowa State University 2004
Akabane: Impact and Response • 2002 U. S. livestock statistics − Calves: 38. 2 million head − Lambs: 4. 36 million head − U. S. livestock naïve No effective treatment • No natural human infection • Potential vectors found in U. S. • − Control • vector to control disease Vaccine used in Japan Center for Food Security and Public Health Iowa State University 2004
 Avian Influenza, Highly Pathogenic Type A virus • Domestic and wild birds • Humans • Reservoir: Migratory water fowl • − Aerosols, contaminated drinking water Infected flock- source of virus for life • Worldwide distribution • Center for Food Security and Public Health Iowa State University 2004
Avian Influenza, Highly Pathogenic Type A virus • Domestic and wild birds • Humans • Reservoir: Migratory water fowl • − Aerosols, contaminated drinking water Infected flock- source of virus for life • Worldwide distribution • Center for Food Security and Public Health Iowa State University 2004
 HPAI: The Disease Incubation period: 3 -14 days • Birds • − Sudden death − Egg production drops − Neurological signs • Humans − Conjunctivitis and respiratory signs − Death possible Center for Food Security and Public Health Iowa State University 2004
HPAI: The Disease Incubation period: 3 -14 days • Birds • − Sudden death − Egg production drops − Neurological signs • Humans − Conjunctivitis and respiratory signs − Death possible Center for Food Security and Public Health Iowa State University 2004
 HPAI: Impact and Response • Direct losses Depopulation and disposal − High morbidity and mortality − Quarantine and surveillance − Indemnities − • 2003: European outbreak (H 7 N 7) − 30 million birds destroyed − Estimated at $338 million USD • 2004: Asian outbreak (H 5 N 1) Center for Food Security and Public Health Iowa State University 2004
HPAI: Impact and Response • Direct losses Depopulation and disposal − High morbidity and mortality − Quarantine and surveillance − Indemnities − • 2003: European outbreak (H 7 N 7) − 30 million birds destroyed − Estimated at $338 million USD • 2004: Asian outbreak (H 5 N 1) Center for Food Security and Public Health Iowa State University 2004
 HPAI: Impact and Response • Treatment − Poultry- none − Humans- antivirals Control outbreak through depopulation/disinfection • Prompt response to MP AI outbreak • Vaccine • − Poultry: Expensive, no cross protection − Human: No cross protection Center for Food Security and Public Health Iowa State University 2004
HPAI: Impact and Response • Treatment − Poultry- none − Humans- antivirals Control outbreak through depopulation/disinfection • Prompt response to MP AI outbreak • Vaccine • − Poultry: Expensive, no cross protection − Human: No cross protection Center for Food Security and Public Health Iowa State University 2004
 Bluetongue Viral disease • Ruminants: Primarily sheep • 24 serotypes worldwide • − 5 • isolated in the U. S. Vector-borne − Culicoides • (biting midge) Worldwide distribution − Mediterranean outbreak, 1997 -2002 Center for Food Security and Public Health Iowa State University 2004
Bluetongue Viral disease • Ruminants: Primarily sheep • 24 serotypes worldwide • − 5 • isolated in the U. S. Vector-borne − Culicoides • (biting midge) Worldwide distribution − Mediterranean outbreak, 1997 -2002 Center for Food Security and Public Health Iowa State University 2004
 Bluetongue: The Disease Incubation period: 5 -20 days • Sheep • − Salivation, facial swelling, nasal discharge − Cyanotic (blue) tongue − Reproductive disorders • Cattle, goats − Subclinical; • possible mild hyperemia Wildlife − Hemorrhages, sudden death Center for Food Security and Public Health Iowa State University 2004
Bluetongue: The Disease Incubation period: 5 -20 days • Sheep • − Salivation, facial swelling, nasal discharge − Cyanotic (blue) tongue − Reproductive disorders • Cattle, goats − Subclinical; • possible mild hyperemia Wildlife − Hemorrhages, sudden death Center for Food Security and Public Health Iowa State University 2004
 Bluetongue: Impact and Response • Affects cattle industry − $125 million per year in lost trade and animal testing No treatment; supportive care • Vector control • Vaccine available • − Serotype • specific, adverse effects Humans: Low risk of infection Center for Food Security and Public Health Iowa State University 2004
Bluetongue: Impact and Response • Affects cattle industry − $125 million per year in lost trade and animal testing No treatment; supportive care • Vector control • Vaccine available • − Serotype • specific, adverse effects Humans: Low risk of infection Center for Food Security and Public Health Iowa State University 2004
 Bovine Spongiform Encephalopathy Prions • Cattle and humans • − Progressively fatal neurologic disease • Transmission − Consumption of -infected feed − Spontaneous mutation • scrapie Worldwide distribution Center for Food Security and Public Health Iowa State University 2004
Bovine Spongiform Encephalopathy Prions • Cattle and humans • − Progressively fatal neurologic disease • Transmission − Consumption of -infected feed − Spontaneous mutation • scrapie Worldwide distribution Center for Food Security and Public Health Iowa State University 2004
 BSE: The Disease • Cattle (BSE) − Incubation period: 2 -8 yrs − Initial signs subtle − Final stages § • Excitable, hypermetria, ataxic, tremors, loss of condition, death Humans (v. CJD) − Incubation unknown − Neurological signs progressing to death − 28 years old (mean age at death) Center for Food Security and Public Health Iowa State University 2004
BSE: The Disease • Cattle (BSE) − Incubation period: 2 -8 yrs − Initial signs subtle − Final stages § • Excitable, hypermetria, ataxic, tremors, loss of condition, death Humans (v. CJD) − Incubation unknown − Neurological signs progressing to death − 28 years old (mean age at death) Center for Food Security and Public Health Iowa State University 2004
 BSE: Impact and Response • United Kingdom − £ 3. 7 billion by end of 2001/02 financial year No effective treatment or vaccine • Surveillance program • Restrictions in place • − Import, animal feeds, slaughter, mammalian products • Very resistant Center for Food Security and Public Health Iowa State University 2004
BSE: Impact and Response • United Kingdom − £ 3. 7 billion by end of 2001/02 financial year No effective treatment or vaccine • Surveillance program • Restrictions in place • − Import, animal feeds, slaughter, mammalian products • Very resistant Center for Food Security and Public Health Iowa State University 2004
 Classical Swine Fever Viral infection • Pigs and wild boars • − Highly • contagious reservoir Transmission − Oral (contaminated garbage), direct contact, aerosol, vertical, insects, fomites • Worldwide distribution Center for Food Security and Public Health Iowa State University 2004
Classical Swine Fever Viral infection • Pigs and wild boars • − Highly • contagious reservoir Transmission − Oral (contaminated garbage), direct contact, aerosol, vertical, insects, fomites • Worldwide distribution Center for Food Security and Public Health Iowa State University 2004
 CSF: The Disease Incubation period: 2 -14 days • Variable clinical signs • − Acute to asymptomatic Fever, weakness, anorexia, discoloration of ears/thighs § Chronic infection fatal § purplish − Strain of virus − Susceptibility of pigs − Indistinguishable from ASF Center for Food Security and Public Health Iowa State University 2004
CSF: The Disease Incubation period: 2 -14 days • Variable clinical signs • − Acute to asymptomatic Fever, weakness, anorexia, discoloration of ears/thighs § Chronic infection fatal § purplish − Strain of virus − Susceptibility of pigs − Indistinguishable from ASF Center for Food Security and Public Health Iowa State University 2004
 CSF: Impact and Response Mortality approaches 100% in acute/chronic infections • Ban on import/export of pigs/products • − Huge economic impact No treatment • Control through quarantine, slaughter • Vaccine in endemic countries • Humans not susceptible to disease • Center for Food Security and Public Health Iowa State University 2004
CSF: Impact and Response Mortality approaches 100% in acute/chronic infections • Ban on import/export of pigs/products • − Huge economic impact No treatment • Control through quarantine, slaughter • Vaccine in endemic countries • Humans not susceptible to disease • Center for Food Security and Public Health Iowa State University 2004
 Coccidioidomycosis • Dimorphic fungus − Saprophytic phase and parasitic Dogs, cats, horses, humans • From soil or dust • − Arthroconidia become airborne, inhaled • Endemic in southwest U. S. , northern Mexico, Argentina Center for Food Security and Public Health Iowa State University 2004
Coccidioidomycosis • Dimorphic fungus − Saprophytic phase and parasitic Dogs, cats, horses, humans • From soil or dust • − Arthroconidia become airborne, inhaled • Endemic in southwest U. S. , northern Mexico, Argentina Center for Food Security and Public Health Iowa State University 2004
 Coccidioidomycosis: The Disease Incubation period: 1 -3 weeks • Disease varies in severity and species affected • Asymptomatic to disseminated • Primary form • − Fever, • lethargy, dry/harsh cough Disseminate form − Lameness, joint swelling, abscesses and draining skin lesions Center for Food Security and Public Health Iowa State University 2004
Coccidioidomycosis: The Disease Incubation period: 1 -3 weeks • Disease varies in severity and species affected • Asymptomatic to disseminated • Primary form • − Fever, • lethargy, dry/harsh cough Disseminate form − Lameness, joint swelling, abscesses and draining skin lesions Center for Food Security and Public Health Iowa State University 2004
 Coccidioidomycosis: Impact and Response • Infection is costly − 1990: Kern County, CA § Cost more than $66 million − Can be widespread in livestock Not communicable or zoonotic • Anti-fungal treatment • No vaccine • Prevent exposure to dust in endemic areas • Center for Food Security and Public Health Iowa State University 2004
Coccidioidomycosis: Impact and Response • Infection is costly − 1990: Kern County, CA § Cost more than $66 million − Can be widespread in livestock Not communicable or zoonotic • Anti-fungal treatment • No vaccine • Prevent exposure to dust in endemic areas • Center for Food Security and Public Health Iowa State University 2004
 Contagious Bovine Pleuropneumonia (CBPP) • Bacteria − Mycoplasma mycoides − Small colony type Bovine and zebu • Transmission via close contact (inhalation); transplacental • Endemic in Africa • − Eradicated in Western Hemisphere Center for Food Security and Public Health Iowa State University 2004
Contagious Bovine Pleuropneumonia (CBPP) • Bacteria − Mycoplasma mycoides − Small colony type Bovine and zebu • Transmission via close contact (inhalation); transplacental • Endemic in Africa • − Eradicated in Western Hemisphere Center for Food Security and Public Health Iowa State University 2004
 CBPP: The Disease Incubation period: 20 -123 days • Respiratory signs • − Cough, • broad stance Chronic infections − Depressed, thin, polyarthritis − 25% Subclinical carriers Morbidity ~100% • Mortality 10 -70% • Center for Food Security and Public Health Iowa State University 2004
CBPP: The Disease Incubation period: 20 -123 days • Respiratory signs • − Cough, • broad stance Chronic infections − Depressed, thin, polyarthritis − 25% Subclinical carriers Morbidity ~100% • Mortality 10 -70% • Center for Food Security and Public Health Iowa State University 2004
 CBPP: Impact and Response • High economic, social impact − Zambia, Tanzania, Botswana − Drought leading to spread of disease • Treatment not always effective − Organism • Vaccine available in endemic areas − Not • sequestered always economically feasible Humans not susceptible Center for Food Security and Public Health Iowa State University 2004
CBPP: Impact and Response • High economic, social impact − Zambia, Tanzania, Botswana − Drought leading to spread of disease • Treatment not always effective − Organism • Vaccine available in endemic areas − Not • sequestered always economically feasible Humans not susceptible Center for Food Security and Public Health Iowa State University 2004
 Contagious Caprine Pleuropneumonia (CCPP) • Bacteria − Mycoplasma capricolum − Mycoplasma mycoides capri Goats • Transmission by direct contact • − inhalation • Africa, Middle East, Eastern Europe, Soviet Union, Far East Center for Food Security and Public Health Iowa State University 2004
Contagious Caprine Pleuropneumonia (CCPP) • Bacteria − Mycoplasma capricolum − Mycoplasma mycoides capri Goats • Transmission by direct contact • − inhalation • Africa, Middle East, Eastern Europe, Soviet Union, Far East Center for Food Security and Public Health Iowa State University 2004
 CCPP: The Disease Incubation period: 6 -28 days • Mycoplasma F 38 strain • − Respiratory § Coughing, labored respiration, nasal discharge, − Chronic • symptoms cases: Carriers M. mycoides capri − Septicemia, reproductive, GI, respiratory symptoms • Morbidity 100%; Mortality 60 -100% Center for Food Security and Public Health Iowa State University 2004
CCPP: The Disease Incubation period: 6 -28 days • Mycoplasma F 38 strain • − Respiratory § Coughing, labored respiration, nasal discharge, − Chronic • symptoms cases: Carriers M. mycoides capri − Septicemia, reproductive, GI, respiratory symptoms • Morbidity 100%; Mortality 60 -100% Center for Food Security and Public Health Iowa State University 2004
 CCPP: Impact and Response • Africa and Asia − Goats § • essential to economics Meat, milk, hides Treatment with antibiotics possible early − Newly infected countries: Slaughter recommended Vaccine available in some countries • Humans not susceptible • Center for Food Security and Public Health Iowa State University 2004
CCPP: Impact and Response • Africa and Asia − Goats § • essential to economics Meat, milk, hides Treatment with antibiotics possible early − Newly infected countries: Slaughter recommended Vaccine available in some countries • Humans not susceptible • Center for Food Security and Public Health Iowa State University 2004
 Foot and Mouth Disease: FMD • Viral infection − Highly • contagious Cloven-hooved animals − Not horses Transmission: Direct contact, aerosol, fomites • Worldwide distribution • − Eradicated from U. S. in 1929 Center for Food Security and Public Health Iowa State University 2004
Foot and Mouth Disease: FMD • Viral infection − Highly • contagious Cloven-hooved animals − Not horses Transmission: Direct contact, aerosol, fomites • Worldwide distribution • − Eradicated from U. S. in 1929 Center for Food Security and Public Health Iowa State University 2004
 Foot-and-Mouth Disease Distribution and Recent Activity Free Present Recent Activity (Rev. 3 -25 -01) Center for Food Security and Public Health Iowa State University 2004
Foot-and-Mouth Disease Distribution and Recent Activity Free Present Recent Activity (Rev. 3 -25 -01) Center for Food Security and Public Health Iowa State University 2004
 FMD: The Disease Incubation period: 2 -12 days • Cattle • Indicator host − Fever, vesicles, salivation, lameness − • Sheep and goats Maintenance hosts − Mild clinical signs − • Pigs: Amplifying host − Lameness predominant sign Center for Food Security and Public Health Iowa State University 2004
FMD: The Disease Incubation period: 2 -12 days • Cattle • Indicator host − Fever, vesicles, salivation, lameness − • Sheep and goats Maintenance hosts − Mild clinical signs − • Pigs: Amplifying host − Lameness predominant sign Center for Food Security and Public Health Iowa State University 2004
 FMD: Impact and Response • 2001, U. K. Outbreak − Total USD • billion 6 million animals slaughtered − FMD • costs over $18 free in less than 1 year Public perception − Animal welfare − Smoke pollution Center for Food Security and Public Health Iowa State University 2004
FMD: Impact and Response • 2001, U. K. Outbreak − Total USD • billion 6 million animals slaughtered − FMD • costs over $18 free in less than 1 year Public perception − Animal welfare − Smoke pollution Center for Food Security and Public Health Iowa State University 2004
 FMD: Impact and Response • • • Most important livestock disease in the world USDA upgrading safeguarding measures Quarantine, depopulation, disinfection Vaccination – complex decision Extremely rare, mild symptoms in people Center for Food Security and Public Health Iowa State University 2004
FMD: Impact and Response • • • Most important livestock disease in the world USDA upgrading safeguarding measures Quarantine, depopulation, disinfection Vaccination – complex decision Extremely rare, mild symptoms in people Center for Food Security and Public Health Iowa State University 2004
 Heartwater Rickettsial bacterium • Cattle, sheep, goats, and water buffalo • − Severe • disease Arthropod-borne − Amblyomma • sp. Endemic in Africa and Caribbean islands Center for Food Security and Public Health Iowa State University 2004
Heartwater Rickettsial bacterium • Cattle, sheep, goats, and water buffalo • − Severe • disease Arthropod-borne − Amblyomma • sp. Endemic in Africa and Caribbean islands Center for Food Security and Public Health Iowa State University 2004
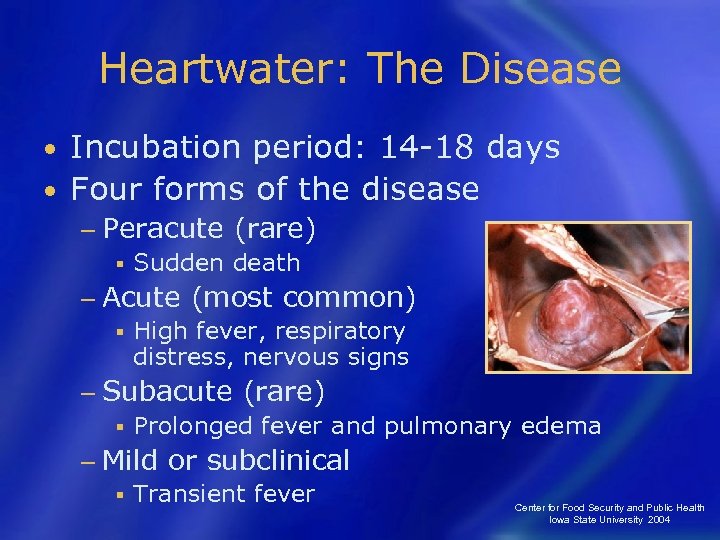 Heartwater: The Disease Incubation period: 14 -18 days • Four forms of the disease • − Peracute (rare) § Sudden death − Acute (most common) § High fever, respiratory distress, nervous signs − Subacute (rare) § Prolonged fever and pulmonary edema − Mild or subclinical § Transient fever Center for Food Security and Public Health Iowa State University 2004
Heartwater: The Disease Incubation period: 14 -18 days • Four forms of the disease • − Peracute (rare) § Sudden death − Acute (most common) § High fever, respiratory distress, nervous signs − Subacute (rare) § Prolonged fever and pulmonary edema − Mild or subclinical § Transient fever Center for Food Security and Public Health Iowa State University 2004
 Heartwater: Impact and Response • Zimbabwe national losses − $56 • million Potential outbreak in U. S. − Estimated mortality 40– 100% Treat with tetracycline • Vaccine is available • Vector control • Center for Food Security and Public Health Iowa State University 2004
Heartwater: Impact and Response • Zimbabwe national losses − $56 • million Potential outbreak in U. S. − Estimated mortality 40– 100% Treat with tetracycline • Vaccine is available • Vector control • Center for Food Security and Public Health Iowa State University 2004
 Japanese Encephalitis Viral infection • Humans, pigs, and other domestic species • Arthropod-borne • − Culex • sp. Endemic in temperate and tropical Asia Center for Food Security and Public Health Iowa State University 2004
Japanese Encephalitis Viral infection • Humans, pigs, and other domestic species • Arthropod-borne • − Culex • sp. Endemic in temperate and tropical Asia Center for Food Security and Public Health Iowa State University 2004
 JE: The Disease Incubation period: 6 -10 days • Horses • − Fever • and neurologic signs Swine − Stillbirths • Humans − Fever, headache − Fatal encephalitis possible Center for Food Security and Public Health Iowa State University 2004
JE: The Disease Incubation period: 6 -10 days • Horses • − Fever • and neurologic signs Swine − Stillbirths • Humans − Fever, headache − Fatal encephalitis possible Center for Food Security and Public Health Iowa State University 2004
 JE: Impact and Response High financial loss in pigs • No effective treatment • − Supportive care Vector control measures • Vaccine • − Horses and swine − Humans Center for Food Security and Public Health Iowa State University 2004
JE: Impact and Response High financial loss in pigs • No effective treatment • − Supportive care Vector control measures • Vaccine • − Horses and swine − Humans Center for Food Security and Public Health Iowa State University 2004
 Lumpy Skin Disease Viral infection • Cattle • Arthropod vector • − Mosquitoes biting flies and Endemic in sub-Saharan Africa • Peak: Rainy season • Center for Food Security and Public Health Iowa State University 2004
Lumpy Skin Disease Viral infection • Cattle • Arthropod vector • − Mosquitoes biting flies and Endemic in sub-Saharan Africa • Peak: Rainy season • Center for Food Security and Public Health Iowa State University 2004
 Lumpy Skin Disease: The Disease Incubation period: -5 weeks • Fever, abortions, decreased milk production • 2 − Nodules typically appear 10 days later • Mortality rates vary − 2 -85% Center for Food Security and Public Health Iowa State University 2004
Lumpy Skin Disease: The Disease Incubation period: -5 weeks • Fever, abortions, decreased milk production • 2 − Nodules typically appear 10 days later • Mortality rates vary − 2 -85% Center for Food Security and Public Health Iowa State University 2004
 Lumpy Skin Disease: Impact and Response Severe economic losses due to decreased animal production • Control secondary infections • Attenuated LSD vaccine • − South • Africa Sheep and goat pox vaccine − Kenya, Egypt Center for Food Security and Public Health Iowa State University 2004
Lumpy Skin Disease: Impact and Response Severe economic losses due to decreased animal production • Control secondary infections • Attenuated LSD vaccine • − South • Africa Sheep and goat pox vaccine − Kenya, Egypt Center for Food Security and Public Health Iowa State University 2004
 Malignant Catarrhal Fever Viral infection • Wildebeest- Africa • Sheep/goats- N. America • Susceptible species: Cattle, bison, other wild ruminants • − Dead-end • hosts Aerosol or mechanical transmission Center for Food Security and Public Health Iowa State University 2004
Malignant Catarrhal Fever Viral infection • Wildebeest- Africa • Sheep/goats- N. America • Susceptible species: Cattle, bison, other wild ruminants • − Dead-end • hosts Aerosol or mechanical transmission Center for Food Security and Public Health Iowa State University 2004
 MCF: The Disease Incubation period: 9 -77 days • Four clinical forms • − Acute Sudden death − Head and eye § Fever, necrotic lesions − Intestinal § Severe diarrhea − Mild § Center for Food Security and Public Health Iowa State University 2004
MCF: The Disease Incubation period: 9 -77 days • Four clinical forms • − Acute Sudden death − Head and eye § Fever, necrotic lesions − Intestinal § Severe diarrhea − Mild § Center for Food Security and Public Health Iowa State University 2004
 MCF: Impact and Response High economic losses in exotics • Mortality near 100% in clinically ill animals • No effective treatment • − Supportive therapy No current vaccine • Human disease not documented • Center for Food Security and Public Health Iowa State University 2004
MCF: Impact and Response High economic losses in exotics • Mortality near 100% in clinically ill animals • No effective treatment • − Supportive therapy No current vaccine • Human disease not documented • Center for Food Security and Public Health Iowa State University 2004
 Menangle virus • Viral infection − Recently discovered Swine reproductive disease • Humans infected • Not highly contagious • Fruit bat reservoir • − Fecal-oral • or urinary-oral Single outbreak − New South Wales, Australia Center for Food Security and Public Health Iowa State University 2004
Menangle virus • Viral infection − Recently discovered Swine reproductive disease • Humans infected • Not highly contagious • Fruit bat reservoir • − Fecal-oral • or urinary-oral Single outbreak − New South Wales, Australia Center for Food Security and Public Health Iowa State University 2004
 Menangle: The Disease • Incubation period: Unknown − Pigs • seroconvert in 10 -14 days Disease in developing fetuses − Mummification − Stillbirth − Deformities Decreased farrowing rate • No signs in postnatal pigs • Center for Food Security and Public Health Iowa State University 2004
Menangle: The Disease • Incubation period: Unknown − Pigs • seroconvert in 10 -14 days Disease in developing fetuses − Mummification − Stillbirth − Deformities Decreased farrowing rate • No signs in postnatal pigs • Center for Food Security and Public Health Iowa State University 2004
 Menangle: Impact and Response Great economic impact in naïve swine populations • 1977 outbreak • − Farrowing rate decreased 44% − Decreased litter size − Strong immunity after infection No vaccine • Humans • − Malaise, fever, chills − Full recovery Center for Food Security and Public Health Iowa State University 2004
Menangle: Impact and Response Great economic impact in naïve swine populations • 1977 outbreak • − Farrowing rate decreased 44% − Decreased litter size − Strong immunity after infection No vaccine • Humans • − Malaise, fever, chills − Full recovery Center for Food Security and Public Health Iowa State University 2004
 Exotic Newcastle Disease (END) • Virus affecting poultry − Four • pathotypes Migratory birds − Secondary human spread Feral pigeons • Psittacines shed virus for >1 year • v. ND endemic in Asia, Middle East, Africa, Central/ South America • Center for Food Security and Public Health Iowa State University 2004
Exotic Newcastle Disease (END) • Virus affecting poultry − Four • pathotypes Migratory birds − Secondary human spread Feral pigeons • Psittacines shed virus for >1 year • v. ND endemic in Asia, Middle East, Africa, Central/ South America • Center for Food Security and Public Health Iowa State University 2004
 END: The Disease • • • Incubation period: 2 -15 days Drop in egg production, neurological damage, GI signs, respiratory distress Numerous deaths within 24 -48 hours Deaths continue for 7 -10 days Morbidity 100%, mortality 90% Center for Food Security and Public Health Iowa State University 2004
END: The Disease • • • Incubation period: 2 -15 days Drop in egg production, neurological damage, GI signs, respiratory distress Numerous deaths within 24 -48 hours Deaths continue for 7 -10 days Morbidity 100%, mortality 90% Center for Food Security and Public Health Iowa State University 2004
 END: Impact and Response Most costly poultry disease worldwide • 2002 -2003: California outbreak • − $160 • million impact Developing countries − Affects quality and quantity of dietary protein Vaccine available • Human’s can acquire eye infections from contact with virus • Center for Food Security and Public Health Iowa State University 2004
END: Impact and Response Most costly poultry disease worldwide • 2002 -2003: California outbreak • − $160 • million impact Developing countries − Affects quality and quantity of dietary protein Vaccine available • Human’s can acquire eye infections from contact with virus • Center for Food Security and Public Health Iowa State University 2004
 Peste des Petits Ruminants Viral infection • Goats and sheep • Close contact • − Aerosol, fomites? Morbidity and mortality up to 100% • Africa, the Middle East, India • Center for Food Security and Public Health Iowa State University 2004
Peste des Petits Ruminants Viral infection • Goats and sheep • Close contact • − Aerosol, fomites? Morbidity and mortality up to 100% • Africa, the Middle East, India • Center for Food Security and Public Health Iowa State University 2004
 Peste des Petits Ruminants: The Disease Incubation period: 3 -10 days • Sudden onset • − Fever, erosive stomatitis, conjunctivitis, pneumonia − More severe in young − Abortions − Diarrhea, dehydration and death • Prognosis correlated with extent of mouth lesions Center for Food Security and Public Health Iowa State University 2004
Peste des Petits Ruminants: The Disease Incubation period: 3 -10 days • Sudden onset • − Fever, erosive stomatitis, conjunctivitis, pneumonia − More severe in young − Abortions − Diarrhea, dehydration and death • Prognosis correlated with extent of mouth lesions Center for Food Security and Public Health Iowa State University 2004
 Peste des Petits Ruminants: Impact and Response • Ecomonic losses − Loss of production, death, abortion − Limit trade, export − Constraints on availability of protein for human consumption No specific treatment • Rinderpest vaccine • − Protects for 12 months − Hinders rinderpest campaign in Africa Center for Food Security and Public Health Iowa State University 2004
Peste des Petits Ruminants: Impact and Response • Ecomonic losses − Loss of production, death, abortion − Limit trade, export − Constraints on availability of protein for human consumption No specific treatment • Rinderpest vaccine • − Protects for 12 months − Hinders rinderpest campaign in Africa Center for Food Security and Public Health Iowa State University 2004
 Rinderpest Viral infection • Highly contagious • Cattle, domestic buffalo • − Other • ungulates can carry disease Direct or close contact − Also contaminated food, water, fomites • East Africa, possibly Asia Center for Food Security and Public Health Iowa State University 2004
Rinderpest Viral infection • Highly contagious • Cattle, domestic buffalo • − Other • ungulates can carry disease Direct or close contact − Also contaminated food, water, fomites • East Africa, possibly Asia Center for Food Security and Public Health Iowa State University 2004
 Rinderpest: The Disease • Incubation period − 3 -15 • days Four forms − Classical: Fever, diarrhea, nasal/ocular discharge, oral erosions − Peracute: Young animals, rapidly fatal − Subacute: Mild signs, low mortality − Atypical: Irregular fever, mild diarrhea Center for Food Security and Public Health Iowa State University 2004
Rinderpest: The Disease • Incubation period − 3 -15 • days Four forms − Classical: Fever, diarrhea, nasal/ocular discharge, oral erosions − Peracute: Young animals, rapidly fatal − Subacute: Mild signs, low mortality − Atypical: Irregular fever, mild diarrhea Center for Food Security and Public Health Iowa State University 2004
 Rinderpest: Impact and Response • • • Africa: 1982 -84 outbreak cost $500 million $100 million spent annually on vaccination world-wide Diagnosis usually means slaughter Vaccine offers life-long immunity Humans not susceptible to disease Center for Food Security and Public Health Iowa State University 2004
Rinderpest: Impact and Response • • • Africa: 1982 -84 outbreak cost $500 million $100 million spent annually on vaccination world-wide Diagnosis usually means slaughter Vaccine offers life-long immunity Humans not susceptible to disease Center for Food Security and Public Health Iowa State University 2004
 Screwworm Myiasis • • • Larvae of the Family Calliphoridae All warm-blooded animals Humans and animals infected when female fly deposits eggs into wound Morbidity variable, can reach 100% Tropical regions Center for Food Security and Public Health Iowa State University 2004
Screwworm Myiasis • • • Larvae of the Family Calliphoridae All warm-blooded animals Humans and animals infected when female fly deposits eggs into wound Morbidity variable, can reach 100% Tropical regions Center for Food Security and Public Health Iowa State University 2004
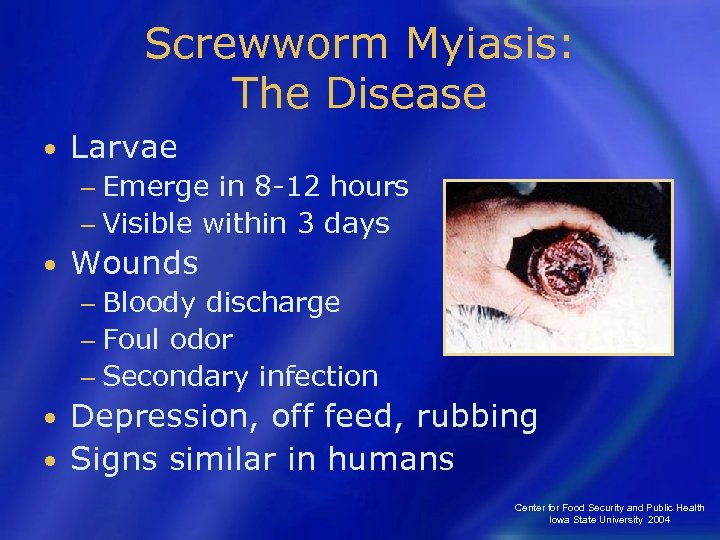 Screwworm Myiasis: The Disease • Larvae − Emerge in 8 -12 hours − Visible within 3 days • Wounds − Bloody discharge − Foul odor − Secondary infection Depression, off feed, rubbing • Signs similar in humans • Center for Food Security and Public Health Iowa State University 2004
Screwworm Myiasis: The Disease • Larvae − Emerge in 8 -12 hours − Visible within 3 days • Wounds − Bloody discharge − Foul odor − Secondary infection Depression, off feed, rubbing • Signs similar in humans • Center for Food Security and Public Health Iowa State University 2004
 Screwworm Myiasis: Impact and Response • Estimated losses if reintroduced − $540 million annually − $1. 27 billion for eradication • Treatment − Removal of larvae − Topical larvicide 2 -3 days • Sterile fly technique − U. S. free in 1966 − Mexico free in 1991 Center for Food Security and Public Health Iowa State University 2004
Screwworm Myiasis: Impact and Response • Estimated losses if reintroduced − $540 million annually − $1. 27 billion for eradication • Treatment − Removal of larvae − Topical larvicide 2 -3 days • Sterile fly technique − U. S. free in 1966 − Mexico free in 1991 Center for Food Security and Public Health Iowa State University 2004
 Sheep and Goat Pox • Viral infection − Capripoxvirus − Contagious Most important pox disease of domestic animals • Direct contact • − Inhalation, • insects? Parts of Africa, Asia, India, and the Middle East Center for Food Security and Public Health Iowa State University 2004
Sheep and Goat Pox • Viral infection − Capripoxvirus − Contagious Most important pox disease of domestic animals • Direct contact • − Inhalation, • insects? Parts of Africa, Asia, India, and the Middle East Center for Food Security and Public Health Iowa State University 2004
 Sheep and Goat Pox: The Disease Incubation period: 4 -13 days • Clinical signs include • − Fever, conjunctivitis, dyspnea − Skin lesions take up to 6 weeks to heal • Mortality − 50% in susceptible flock − 100% in young • No chronic carriers Center for Food Security and Public Health Iowa State University 2004
Sheep and Goat Pox: The Disease Incubation period: 4 -13 days • Clinical signs include • − Fever, conjunctivitis, dyspnea − Skin lesions take up to 6 weeks to heal • Mortality − 50% in susceptible flock − 100% in young • No chronic carriers Center for Food Security and Public Health Iowa State University 2004
 Sheep and Goat Pox: Impact and Response Infection can limit trade of live animals and product • Treat secondary infections • Vaccination • − Endemic areas with attenuated virus Slaughter should be considered • Humans not susceptible • Center for Food Security and Public Health Iowa State University 2004
Sheep and Goat Pox: Impact and Response Infection can limit trade of live animals and product • Treat secondary infections • Vaccination • − Endemic areas with attenuated virus Slaughter should be considered • Humans not susceptible • Center for Food Security and Public Health Iowa State University 2004
 Swine Vesicular Disease • Viral infection − Resistant to heat, p. H, curing − Moderately contagious Swine and humans • Ingestion or close contact • Previously Europe and Hong Kong • − Only in Italy as of 2002 Center for Food Security and Public Health Iowa State University 2004
Swine Vesicular Disease • Viral infection − Resistant to heat, p. H, curing − Moderately contagious Swine and humans • Ingestion or close contact • Previously Europe and Hong Kong • − Only in Italy as of 2002 Center for Food Security and Public Health Iowa State University 2004
 SVD: The Disease • Incubation period: − Ingestion: 2 -5 days − Direct contact: 2 -7 days Clinically resembles FMD • Fever, salivation, lameness • Vesicles • − Snout, mammary gland, coronary band • Mortality low Center for Food Security and Public Health Iowa State University 2004
SVD: The Disease • Incubation period: − Ingestion: 2 -5 days − Direct contact: 2 -7 days Clinically resembles FMD • Fever, salivation, lameness • Vesicles • − Snout, mammary gland, coronary band • Mortality low Center for Food Security and Public Health Iowa State University 2004
 SVD: Impact and Response • • • Control measures costly Export restrictions Supportive care Vaccine not commercially available Human infection not common − Incubation period: 1 -5 weeks − Mild influenza-like symptoms − Vesicular lesions not seen Center for Food Security and Public Health Iowa State University 2004
SVD: Impact and Response • • • Control measures costly Export restrictions Supportive care Vaccine not commercially available Human infection not common − Incubation period: 1 -5 weeks − Mild influenza-like symptoms − Vesicular lesions not seen Center for Food Security and Public Health Iowa State University 2004
 Vesicular Stomatitis • • • Viral infection Horses, donkeys, cattle, swine, South American camelids Arthropod-borne, direct contact, aerosol Morbidity 90%, mortality low Southwest United States Center for Food Security and Public Health Iowa State University 2004
Vesicular Stomatitis • • • Viral infection Horses, donkeys, cattle, swine, South American camelids Arthropod-borne, direct contact, aerosol Morbidity 90%, mortality low Southwest United States Center for Food Security and Public Health Iowa State University 2004
 VSV: The Disease • Animals − Incubation period 3 -5 days − Oral/mammary/coronary band lesions, salivation, lameness § Resembles FMD − Recovery • in 2 weeks Humans − Incubation period 1 -6 days − Influenza-like symptoms, rarely oral vesicles − Self limiting Center for Food Security and Public Health Iowa State University 2004
VSV: The Disease • Animals − Incubation period 3 -5 days − Oral/mammary/coronary band lesions, salivation, lameness § Resembles FMD − Recovery • in 2 weeks Humans − Incubation period 1 -6 days − Influenza-like symptoms, rarely oral vesicles − Self limiting Center for Food Security and Public Health Iowa State University 2004
 VSV: Impact and Response • • • Outbreaks every 10 years in the U. S 1982 and 1995: $53 -$202 per head lost on cattle 1998: Equine outbreak Supportive treatment Vaccines available during an outbreak Center for Food Security and Public Health Iowa State University 2004
VSV: Impact and Response • • • Outbreaks every 10 years in the U. S 1982 and 1995: $53 -$202 per head lost on cattle 1998: Equine outbreak Supportive treatment Vaccines available during an outbreak Center for Food Security and Public Health Iowa State University 2004
 The Veterinarian’s Responsibility Center for Food Security and Public Health Iowa State University 2004
The Veterinarian’s Responsibility Center for Food Security and Public Health Iowa State University 2004
 The Veterinarian’s Responsibility • • • Guardian of animal and public health Sharpen awareness of disease agents Alert officials early Be involved with emergency response plans at all levels You are the expert − Provide leadership and input to clients and community Center for Food Security and Public Health Iowa State University 2004
The Veterinarian’s Responsibility • • • Guardian of animal and public health Sharpen awareness of disease agents Alert officials early Be involved with emergency response plans at all levels You are the expert − Provide leadership and input to clients and community Center for Food Security and Public Health Iowa State University 2004
 Contacts • Phone numbers to know − State Veterinarian − State Public Health Veterinarian − APHIS- Area Veterinarian in Charge − Public Health Officials Center for Food Security and Public Health Iowa State University 2004
Contacts • Phone numbers to know − State Veterinarian − State Public Health Veterinarian − APHIS- Area Veterinarian in Charge − Public Health Officials Center for Food Security and Public Health Iowa State University 2004
 Conclusion Center for Food Security and Public Health Iowa State University 2004
Conclusion Center for Food Security and Public Health Iowa State University 2004
 Summary Importance of agriculture and livestock • Specific disease agents on high consequence livestock pathogen list • − Zoonotic potential Veterinarian’s responsibilities • Awareness education imperative • Center for Food Security and Public Health Iowa State University 2004
Summary Importance of agriculture and livestock • Specific disease agents on high consequence livestock pathogen list • − Zoonotic potential Veterinarian’s responsibilities • Awareness education imperative • Center for Food Security and Public Health Iowa State University 2004
 Conclusion “The best prescription, is knowledge. ” Dr. C. Everett Koop Former U. S. Surgeon General Center for Food Security and Public Health Iowa State University 2004
Conclusion “The best prescription, is knowledge. ” Dr. C. Everett Koop Former U. S. Surgeon General Center for Food Security and Public Health Iowa State University 2004
 Acknowledgments Development of this presentation was funded by a grant from the Centers for Disease Control and Prevention to the Center for Food Security and Public Health at Iowa State University. Center for Food Security and Public Health Iowa State University 2004
Acknowledgments Development of this presentation was funded by a grant from the Centers for Disease Control and Prevention to the Center for Food Security and Public Health at Iowa State University. Center for Food Security and Public Health Iowa State University 2004
 Acknowledgments Author: Danelle Bickett-Weddle, DVM, MPH Co-author: Katie Steneroden, DVM, MPH Stacy Holzbauer, DVM Reviewer: James Roth, DVM, Ph. D Glenda Dvorak, DVM, MS, MPH Center for Food Security and Public Health Iowa State University 2004
Acknowledgments Author: Danelle Bickett-Weddle, DVM, MPH Co-author: Katie Steneroden, DVM, MPH Stacy Holzbauer, DVM Reviewer: James Roth, DVM, Ph. D Glenda Dvorak, DVM, MS, MPH Center for Food Security and Public Health Iowa State University 2004


