1eaf951938f6b3c6a1d13ee277282af1.ppt
- Количество слайдов: 51
Outline 29. 1 Body Water and Its Solutes 29. 2 Fluid Balance 29. 3 Blood 29. 4 Plasma Proteins, White Blood Cells, and Immunity 29. 5 Blood Clotting 29. 6 Red Blood Cells and Blood Gases 29. 7 The Kidney and Urine Formation 29. 8 Urine Composition and Function

Goals 1. How are body fluids classified? Be able to describe the major categories of body fluids, their general composition, and the exchange of solutes between them. 2. What are the roles of blood in maintaining homeostasis? Be able to explain the composition and functions of blood. 3. How do blood components participate in the body’s defense mechanisms? Be able to identify and describe the roles of blood components that participate in inflammation, the immune response, and blood clotting. 4. How do red blood cells participate in the transport of blood gases? Be able to explain the relationships among O 2 and CO 2 transport, and acid–base balance. 5. How is the composition of urine controlled? Be able to describe the transfer of water and solutes during urine formation, and give an overview of the composition of urine.

29. 1 Body Water and Its Solutes • Extracellular fluid includes blood plasma (the fluid portion of blood), interstitial fluid (the fluid that fills the spaces between cells), lymph, cerebrospinal fluid, and the fluid that lubricates joints (synovial fluid).

29. 1 Body Water and Its Solutes • To be soluble in water, a substance must be an ion, a gas, a small polar molecule, or a large molecule having many polar, hydrophilic (water loving) or ionic groups on its surface. • All four types of solutes are present in body fluids. • Although these fluids have different compositions, their osmolarities are the same.

29. 1 Body Water and Its Solutes • Electrolytes are major contributors to the osmolarity of body fluids, and move about as necessary to maintain charge balance. • Water soluble proteins make up a large proportion of the solutes in blood plasma and intracellular fluid. • Blood gases (oxygen and carbon dioxide), along with glucose, amino acids, and the by products of protein catabolism, are the major small molecules in body fluids.
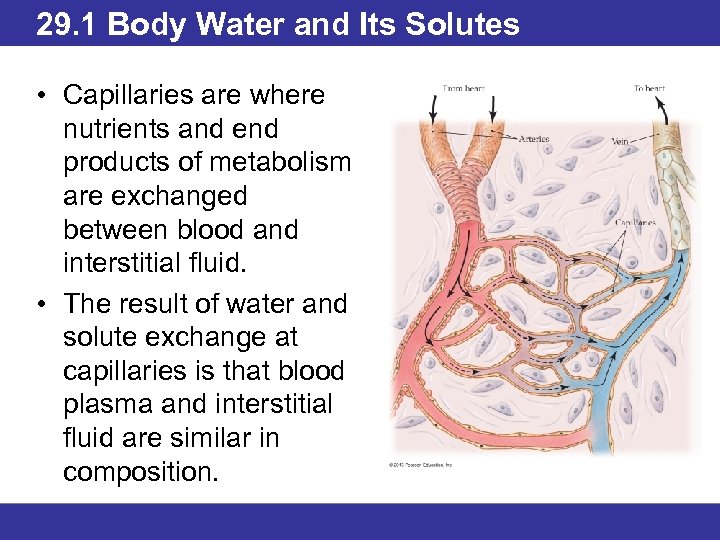
29. 1 Body Water and Its Solutes • Capillaries are where nutrients and end products of metabolism are exchanged between blood and interstitial fluid. • The result of water and solute exchange at capillaries is that blood plasma and interstitial fluid are similar in composition.

29. 1 Body Water and Its Solutes • Peripheral tissue is networked with lymph capillaries. • The lymphatic system collects excess interstitial fluid, debris from cellular breakdown, and proteins and lipid droplets too large to pass through capillary walls. • Lymph enters the bloodstream at the thoracic duct. • Exchange of solutes between the interstitial fluid and the intracellular fluid occurs by active transport (transport requiring energy). • Sodium ion concentration is high in extracellular fluids and low in intracellular fluids; potassium ion concentrations are high inside cells and low outside cells.

29. 2 Fluid Balance • Preserving fluid balance is crucial in maintaining physiological homeostasis. • During the course of an endurance event, fluid loss occurs with minimal fluid intake. • Physiologists consider 4% body mass loss to be the “danger zone. ” • Both intake and output of water are controlled by hormones.

29. 2 Fluid Balance • A 2% change in osmolarity causes adjustment in hormone secretion. • When blood osmolarity rises, secretion of antidiuretic hormone (vasopressin) increases. • The kidneys keep water and electrolytes in balance by increasing or decreasing the amounts eliminated. In the kidney, antidiuretic hormone causes a decrease in the water content of the urine.

29. 2 Fluid Balance • Osmoreceptors in the hypothalamus and baroreceptors in the heart and blood vessels activate thirst mechanism. • Both oversecretion and undersecretion of antidiuretic hormone (ADH) can lead to serious disease states. – When ADH secretion is too high, the kidney excretes too little water, the water content of body compartments increases, and serum concentrations of electrolytes drop. – In diabetes insipidus, too little ADH is secreted and up to 15 L of dilute urine are excreted each day.

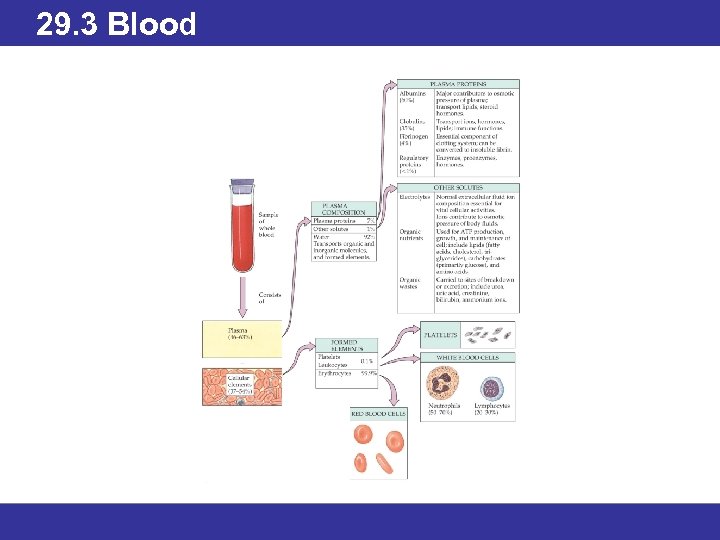
29. 3 Blood • About 55% of blood is plasma; the remaining 45% is a mixture of red blood cells, platelets, and white blood cells (leukocytes). • Plasma and cells together make up whole blood. • Blood serum is the fluid remaining after blood has completely clotted. • Blood serum composition is not the same as that of blood plasma.

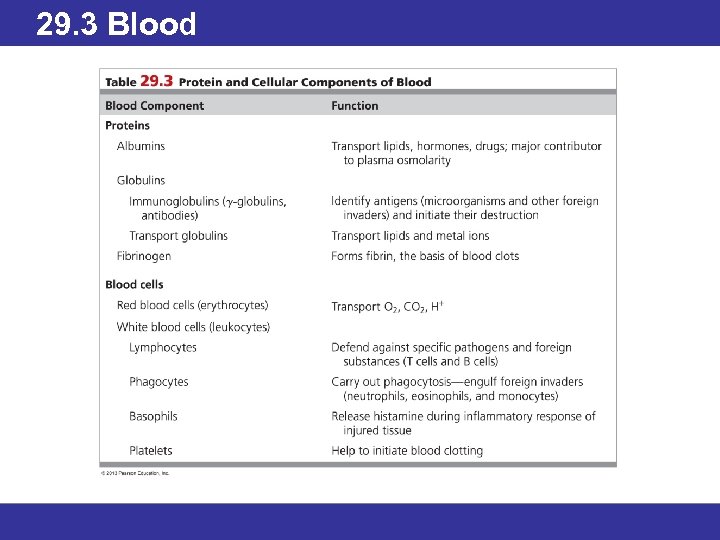
29. 3 Blood Major Functions of Blood • Transport—Oxygen and carbon dioxide are carried to and from by red blood cells. Nutrients are carried from the intestine to the sites of their catabolism. Waste products of metabolism are carried to the kidneys. Hormones from endocrine glands are delivered to their target tissues.

29. 3 Blood Major Functions of Blood • Regulation—Blood distributes body heat, participating in regulation of body temperature. It also picks up or delivers water and electrolytes as needed. Blood buffers are essential to maintenance of acid–base balance. • Defense—Blood carries the molecules and cells needed for two major defense mechanisms: (1) the immune response, which destroys foreign invaders; and (2) blood clotting, which prevents blood loss and begins healing of wounds.
29. 3 Blood

29. 3 Blood

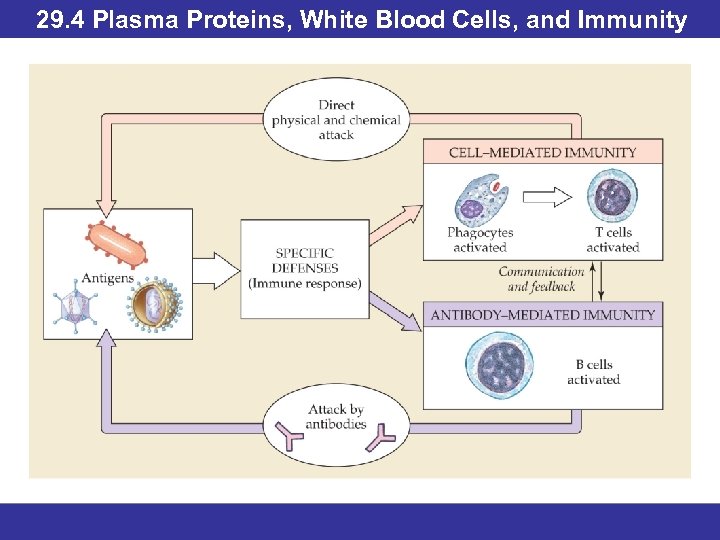
29. 4 Plasma Proteins, White Blood Cells, and Immunity • An antigen is any molecule or portion of a molecule recognized by the body as a foreign invader. • Antigens can also be haptens: recognized as antigens after they have bonded to carrier proteins. • Recognition of an antigen can initiate three responses: inflammation, cell mediated response, and antibody mediated immune response.
29. 4 Plasma Proteins, White Blood Cells, and Immunity
29. 4 Plasma Proteins, White Blood Cells, and Immunity Inflammatory Response • Inflammation is a nonspecific defense mechanism in which chemical messengers (histidine) direct inflammatory response. It includes swelling, redness, warmth, and pain. • Histamine causes dilation of capillaries and increases permeability of capillary walls, increasing blood flow. • Plasma carrying blood clotting factors, defensive proteins, and white blood cells enter the intercellular space. • Antigens are destroyed by phagocytes. • Inflammation caused by a wound will heal completely only after all infectious agents, dead cells and other debris have been absorbed into the lymph system.
29. 4 Plasma Proteins, White Blood Cells, and Immunity The Blood–Brain Barrier • The brain is rigorously isolated from variations in blood composition. • The endothelial cells that form the walls of brain capillaries form a series of continuous tight junctions so that nothing can pass between them. • The blood–brain barrier (BBB) serves as internal protection for the brain. • Glucose and certain amino acids are brought across the cell membranes by transport mechanisms specific to each nutrient. • Substances soluble in membrane lipids readily breach the blood–brain barrier. Among such substances are nicotine, caffeine, codeine, diazepam (Valium, an antidepressant), and heroin.

29. 4 Plasma Proteins, White Blood Cells, and Immunity Cell-mediated Immune Response • Cell mediated immune response is under the control of T lymphocytes, or T cells. • It principally guards against abnormal cells and bacteria or viruses that have entered normal cells. It also guards against the invasion of some cancer cells and causes the rejection of transplanted organs. • The result of T cell recognition of an antigen is production of cytotoxic, or killer, T cells that can destroy the invader, helper T cells that enhance the body’s defenses, and memory T cells that will immediately generate killer T cells if the same pathogen reappears.

29. 4 Plasma Proteins, White Blood Cells, and Immunity Antibody-Mediated Immune Response • B cells identify antigens adrift in body fluids. • A B cell is activated when it first bonds to an antigen and then encounters a helper T cell that recognizes the same antigen. • This activation often occurs in lymph nodes, tonsils, or the spleen, which have large concentrations of lymphocytes. • Once activated, B cells divide to form plasma cells that secrete antibodies specific to the antigen.

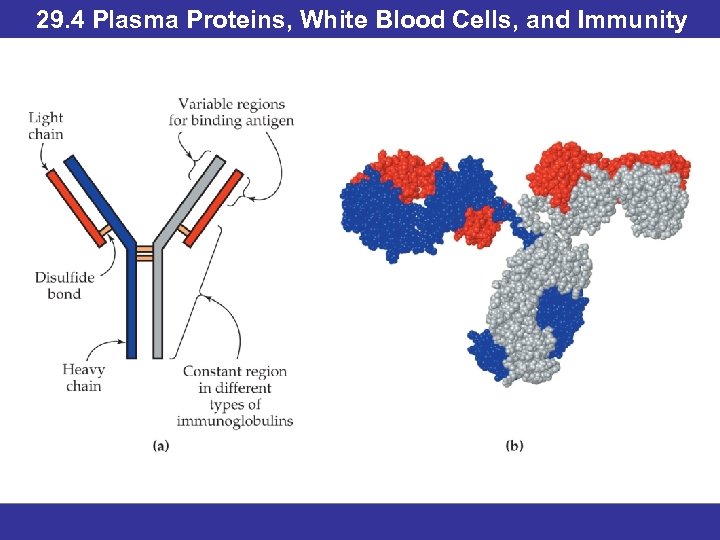
29. 4 Plasma Proteins, White Blood Cells, and Immunity Antibody-Mediated Immune Response • Antibodies are immunoglobulins. • The body contains up to 10, 000 different immunoglobulins at any given time. • They are glycoproteins composed of two “heavy” polypeptide chains and two “light” polypeptide chains joined by disulfide bonds. • The variable regions are sequences of amino acids that will bind a specific antigen. • Once synthesized, antibodies spread out to find their antigens.
29. 4 Plasma Proteins, White Blood Cells, and Immunity

29. 4 Plasma Proteins, White Blood Cells, and Immunity Antibody-Mediated Immune Response • Formation of an antigen–antibody complex inactivates the antigen. • Activated B cell division also yields memory cells. • Immunoglobulin G antibodies (gamma globulins), protect against viruses and bacteria. • Allergies and asthma are caused by an oversupply of immunoglobulin E. • Autoimmune diseases include attack on connective tissue in rheumatoid arthritis, attack on pancreatic islet cells in diabetes mellitus, and a generalized attack on nucleic acids and blood components in systemic lupus erythematosus.
29. 5 Blood Clotting • A blood clot consists of blood cells trapped in a mesh of the insoluble fibrous protein known as fibrin. • Clot formation is a multiple step process requiring participation of 12 clotting factors. – Calcium ion is one of the clotting factors. – Others, most of which are glycoproteins, are synthesized in the liver by pathways that require vitamin K as a coenzyme.

29. 5 Blood Clotting • A deficiency of vitamin K, a competitive inhibitor of vitamin K, or deficiency of a clotting factor can cause excessive bleeding from even minor tissue damage. • Hemophilia is caused by an inherited genetic defect that results in the absence of one or more of the clotting factors. • Hemophilia occurs in 10, 000 individuals, with 80– 90% of hemophiliacs being male.
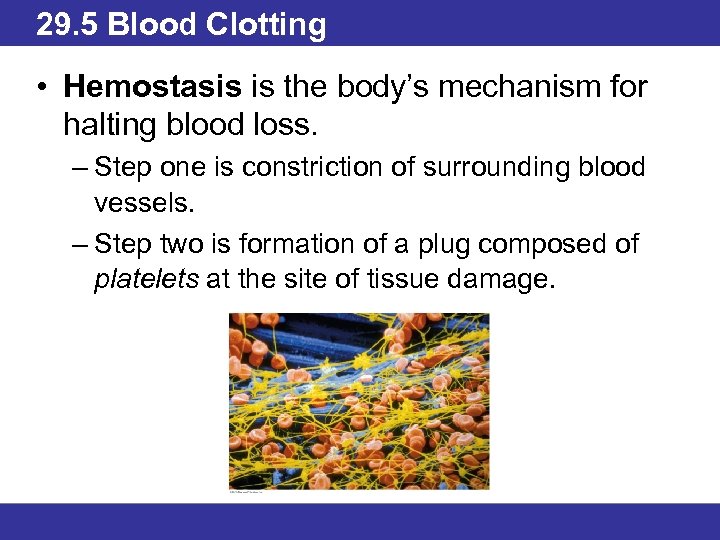
29. 5 Blood Clotting • Hemostasis is the body’s mechanism for halting blood loss. – Step one is constriction of surrounding blood vessels. – Step two is formation of a plug composed of platelets at the site of tissue damage.
29. 5 Blood Clotting • A blood clot is formed in a process that is triggered by two pathways. – The intrinsic pathway begins when blood makes contact with the negatively charged surface of the fibrous protein collagen, which is exposed at the site of tissue damage. – The extrinsic pathway begins when damaged tissue releases an integral membrane glycoprotein known as tissue factor.

29. 5 Blood Clotting • A cascade of reactions is initiated when an inactive clotting factor (a zymogen) is converted to its active form. • The newly activated enzyme then catalyzes the activation of the next factor in the cascade. • In the final step of the common pathway, thrombin catalyzes cleavage of small polypeptides from the soluble plasma protein fibrinogen.

29. 5 Blood Clotting • Negatively charged groups make fibrinogen soluble and keep the molecules apart. • Once these polypeptides are removed, fibrin molecules associate with each other by noncovalent interactions. • They are bound into fibers by formation of amide cross links between lysine and glutamine side chains in a reaction catalyzed by another clotting factor.
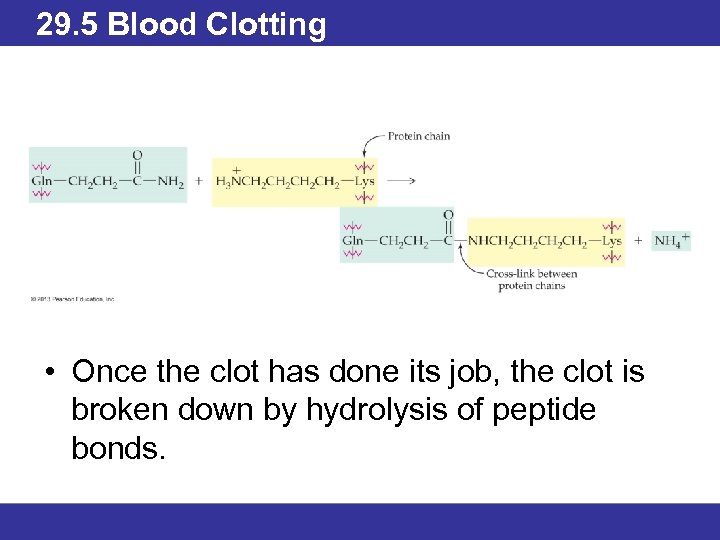
29. 5 Blood Clotting • Once the clot has done its job, the clot is broken down by hydrolysis of peptide bonds.

29. 6 Red Blood Cells and Blood Gases • Erythrocytes transport blood gases. • Erythrocytes in mammals have no nuclei or ribosomes and cannot replicate. • They must obtain glucose from plasma. • 95% of the protein in an erythrocyte is hemoglobin. • Hemoglobin (Hb) is composed of four polypeptide chains with central heme groups. • Each heme can combine with one O 2 molecule.

29. 6 Red Blood Cells and Blood Gases Oxygen Transport • The iron(II) ion, Fe 2+ sits in the center of each heme and binds O 2. • Hemoglobin (Hb) carrying four oxygens (oxyhemoglobin) is bright red. Hemoglobin that has lost one or more oxygens (deoxyhemoglobin) is dark red purple. • The color of arterial blood carrying oxygen is used in pulse oximetry. • Percent saturation, is dependent on the partial pressure of oxygen in surrounding tissues. • Oxygen is more readily released to tissues where the partial pressure of oxygen is low.

29. 6 Red Blood Cells and Blood Gases Carbon Dioxide Transport, Acidosis and Alkylosis • The relationships among H+ and HCO 3– concentrations and O 2 and CO 2 partial pressures are essential to maintaining electrolyte and acid–base balance. • Carbon dioxide diffuses into interstitial fluid and then into capillaries, where it is transported in blood three ways: (1) as dissolved CO 2 (2) bonded to Hb, or (3) as HCO 3— in solution. • Most of the CO 2 is converted to bicarbonate ion within erythrocytes, which contain a large concentration of carbonic anhydrase.
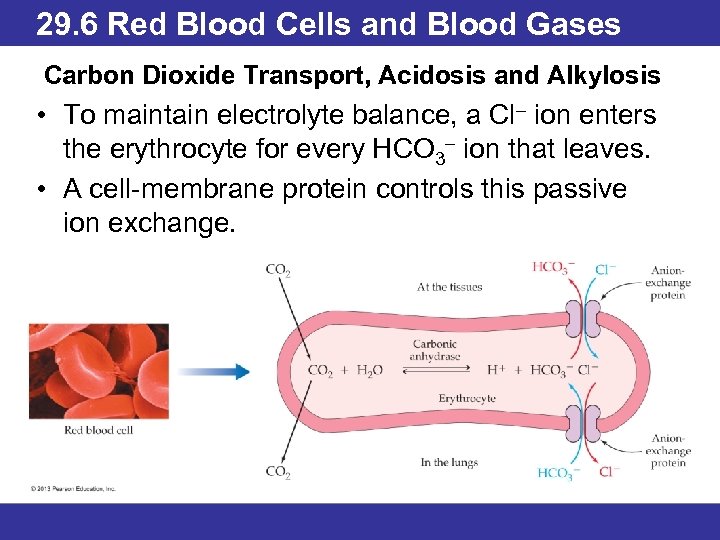
29. 6 Red Blood Cells and Blood Gases Carbon Dioxide Transport, Acidosis and Alkylosis • To maintain electrolyte balance, a Cl– ion enters the erythrocyte for every HCO 3– ion that leaves. • A cell membrane protein controls this passive ion exchange.

29. 6 Red Blood Cells and Blood Gases Carbon Dioxide Transport, Acidosis and Alkylosis • To counteract the acidity increases caused by carbonic anhydrase, hemoglobin reversibly binds hydrogen ions. • Oxygen is held more firmly when the hydrogen ion concentration decreases. • Homeostasis requires a blood p. H between 7. 35 and 7. 45. A p. H outside this range creates either acidosis or alkalosis. • The wide variety of conditions that cause acidosis or alkalosis are divided between respiratory and metabolic malfunctions.
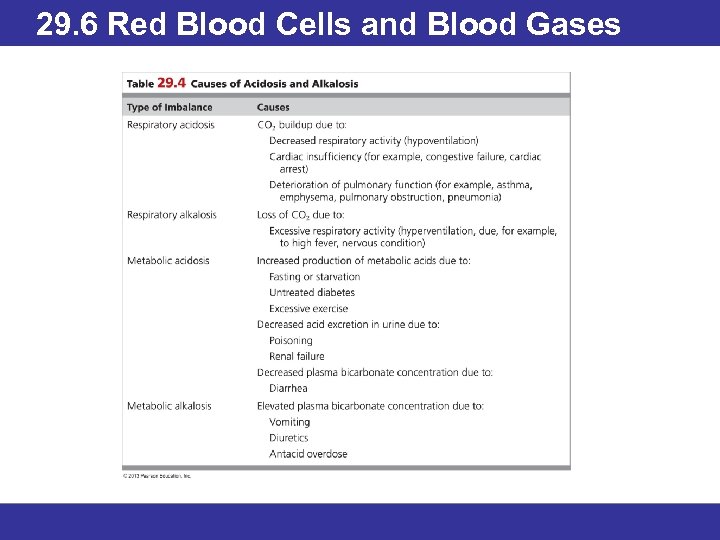
29. 6 Red Blood Cells and Blood Gases
29. 7 The Kidney and Urine Formation • The kidneys bear the major responsibility for maintaining a constant internal environment in the body. • About 25% of the blood pumped from the heart goes directly to the kidneys, where the functional units are the nephrons. • Blood enters a nephron at a glomerulus, a tangle of capillaries surrounded by a fluid filled space. • Filtration occurs here.
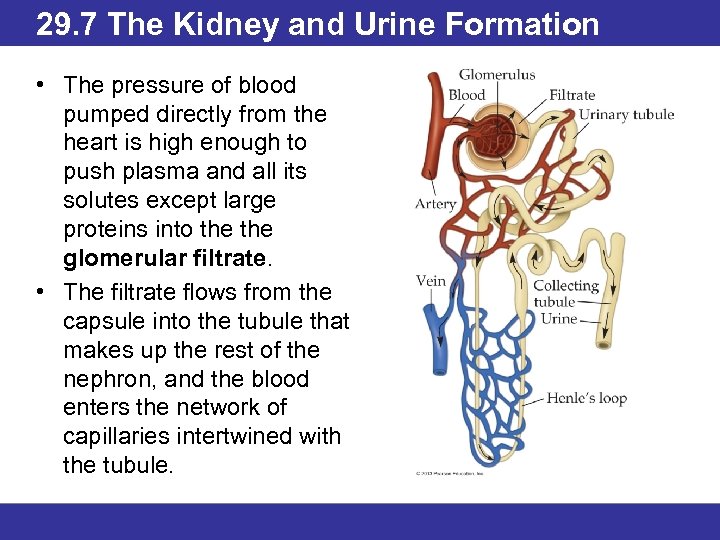
29. 7 The Kidney and Urine Formation • The pressure of blood pumped directly from the heart is high enough to push plasma and all its solutes except large proteins into the glomerular filtrate. • The filtrate flows from the capsule into the tubule that makes up the rest of the nephron, and the blood enters the network of capillaries intertwined with the tubule.

29. 7 The Kidney and Urine Formation • About 125 m. L of filtrate per minute enters the kidneys. • They produce 180 L of filtrate per day, but excrete only about 1. 4 L of urine. • Another important function of the kidneys is reabsorption. • More of certain solutes must be excreted than are present in the filtrate. This situation is dealt with by secretion—the transfer of solutes into the kidney tubule.

29. 8 Urine Composition and Function • Urine contains the products of glomerular filtration minus the substances reabsorbed in the tubules, plus the substances secreted in the tubules. • About 50 g of solids (in solution) are excreted every day—about 20 g of electrolytes and 30 g of nitrogen containing wastes. • Normal urine composition is usually reported as the quantity of solute excreted per day. • Laboratory urinalysis often requires collection of all urine excreted during a 24 hour period.

29. 8 Urine Composition and Function

29. 8 Urine Composition and Function Acid–Base Balance • Respiration, buffers, and excretion of hydrogen ions in urine combine to maintain acid–base balance. • The H+ to be eliminated is produced by the reaction of CO 2 with water in the cells lining the tubules of the nephrons.

29. 8 Urine Composition and Function • • • Automated Clinical Laboratory Analysis When a physician orders chemical tests of blood, urine, or spinal fluid, the sample goes to a clinical chemistry laboratory where most tests are done by automated clinical chemistry analyzers. There are two types of chemical analysis, one for the quantity of a chemical and the other for the quantity of an enzyme. Many chemical components are measured directly by mixing a reagent with the sample—the analyte—and noting the quantity of a colored product formed by using a photometer. Many analytes are also substrates for enzyme catalyzed reactions. Analysis of the substrate concentration is therefore often made possible by treating the analyte with appropriate enzymes. Determination of the quantity of a specific enzyme or the ratio of two or more enzymes, is invaluable in detecting organ damage that allows enzymes to leak into body fluids. Automated analyzers rely on premixed reagents and automatic division of a fluid sample into small portions for each test.

29. 8 Urine Composition and Function Fluid And Na+ Balance • The amount of water reabsorbed is dependent on the osmolarity of the fluid passing through the kidneys, the antidiuretic hormone–controlled permeability of the collecting duct membrane, and the amount of Na+ actively reabsorbed. • Increased sodium reabsorption means higher interstitial osmolarity, greater water reabsorption, and decreased urine volume. • Decreased sodium reabsorption means less water is reabsorbed and urine volume increases.

29. 8 Urine Composition and Function Fluid And Na+ Balance • Reabsorption of Na+ is normally under the control of the steroid hormone aldosterone. • The arrival of chemical messengers signaling a decrease in total blood plasma volume accelerates the secretion of aldosterone. • The result is increased Na+ reabsorption in the kidney tubules accompanied by increased water reabsorption.

Chapter Summary 1. How are body fluids classified? • Body fluids are either intracellular or extracellular. • Extracellular fluid includes blood plasma (the fluid part of blood) and interstitial fluid. • Blood serum is the fluid remaining after blood has clotted. • Solutes in body fluids include blood gases, electrolytes, metabolites, and proteins. Solutes are carried throughout the body in blood and lymph. • Exchange of solutes between blood and interstitial fluid occurs at the network of capillaries in peripheral tissues. Exchange of solutes between interstitial fluid and intracellular fluid occurs by passage across cell membranes.

Chapter Summary, Continued 2. What are the roles of blood in maintaining homeostasis? • The principal functions of blood are (1) transport of solutes and blood gases, (2) regulation, including regulation of heat and acid–base balance, and (3) defense, which includes the immune response and blood clotting. • In addition to plasma and proteins, blood is composed of red blood cells (erythrocytes), which transport oxygen; white blood cells (leukocytes), for defense functions; and platelets, which participate in blood clotting.

Chapter Summary, Continued 3. • • • How do blood components participate in the body’s defense mechanisms? The presence of an antigen (a substance foreign to the body) initiates (1) the inflammatory response, (2) the cell mediated immune response, and (3) the antibody mediated immune response. The inflammatory response is initiated by histamine and accompanied by the destruction of invaders by phagocytes. The cell-mediated response is effected by T cells that can, for example, release a toxic protein that kills invaders. The antibody-mediated response is effected by B cells, which generates antibodies (immunoglobulins), proteins that complex with antigens and destroy them. Blood clotting occurs in a cascade of reactions in which a series of zymogens are activated, ultimately resulting in the formation of a clot composed of fibrin and platelets.

Chapter Summary, Continued 4. • • • How do red blood cells participate in the transport of blood gases? Oxygen is transported bonded to Fe 2+ ions in hemoglobin. The percent saturation of hemoglobin with oxygen is governed by the partial pressure of oxygen in surrounding tissues and allosteric variations in hemoglobin structure. Carbon dioxide is transported in blood as a solute, bonded to hemoglobin, or in solution as bicarbonate ion. In peripheral tissues, carbon dioxide diffuses into red blood cells, where it is converted to bicarbonate ion. Acid–base balance is controlled as hydrogen ions generated by bicarbonate formation are bound by hemoglobin. At the lungs, oxygen enters the cells, and bicarbonate and hydrogen ions leave. A blood p. H outside the normal range of 7. 35– 7. 45 can be caused by respiratory or metabolic imbalance, resulting in the potentially serious conditions of acidosis or alkalosis.

Chapter Summary, Continued 5. How is the composition of urine controlled? • The first essential kidney function is filtration, in which plasma and most of its solute cross capillary membranes and enter the glomerular filtrate. Water and essential solutes are then reabsorbed, whereas additional solutes for elimination are secreted into the filtrate. • Urine is thus composed of the products of filtration, minus the substances reabsorbed, plus the secreted substances. It is composed of water, nitrogen containing wastes, and electrolytes that are excreted to help to maintain acid– base balance. The balance between water and Na+ excreted or absorbed is governed by the osmolarity of fluid in the kidney, the hormone aldosterone, and various chemical messengers.
1eaf951938f6b3c6a1d13ee277282af1.ppt