4554760fde66b79201663e715cfae9aa.ppt
- Количество слайдов: 13
 OR Culture Part II If culture is the problem, what is the solution? Dr. Mark Fleming Mark. fleming@smu. ca
OR Culture Part II If culture is the problem, what is the solution? Dr. Mark Fleming Mark. fleming@smu. ca
 Outline • Where are we? (Cultural typology) • Improvement strategies – Engagement – Spread – Improvement • Assessment and improvement tools – Surveys – Team training
Outline • Where are we? (Cultural typology) • Improvement strategies – Engagement – Spread – Improvement • Assessment and improvement tools – Surveys – Team training
 Safety Culture A culture of safety can be defined as an integrated pattern of individual and organizational behavior, based upon shared beliefs and values, that continuously seeks to minimize patient harm that may result from the processes of care delivery (Kizer, 1999).
Safety Culture A culture of safety can be defined as an integrated pattern of individual and organizational behavior, based upon shared beliefs and values, that continuously seeks to minimize patient harm that may result from the processes of care delivery (Kizer, 1999).
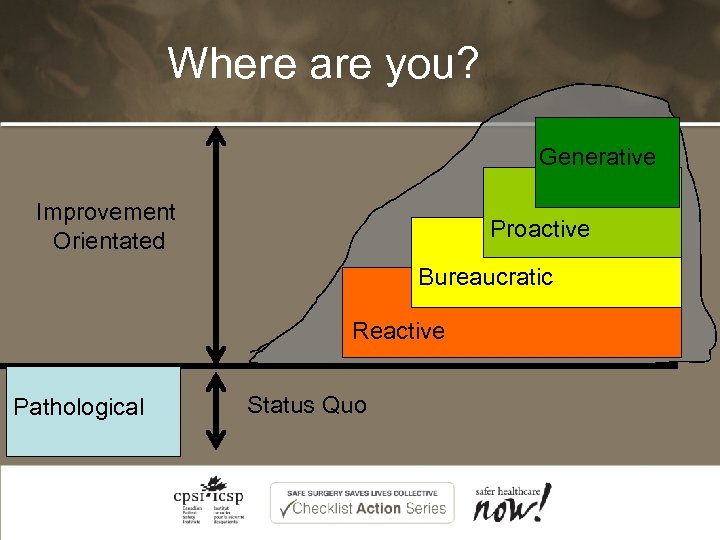 Where are you? Generative Safety Proactive mountain Improvement Orientated Bureaucratic Reactive Pathological Status Quo
Where are you? Generative Safety Proactive mountain Improvement Orientated Bureaucratic Reactive Pathological Status Quo
 What level are you at? • Pathological – Toxic environment (shoot the messenger), people actively do not want to improve • Reactive – Passive ignoring of improvement initiatives, until something bad happens • Bureaucratic – Willing adoption of proven safety interventions • Proactive – Active development and evaluation of new safety interventions • Generative
What level are you at? • Pathological – Toxic environment (shoot the messenger), people actively do not want to improve • Reactive – Passive ignoring of improvement initiatives, until something bad happens • Bureaucratic – Willing adoption of proven safety interventions • Proactive – Active development and evaluation of new safety interventions • Generative
 Engagement • Identify one (or more) supportive Physician to pilot checklist and promote benefits to colleagues • Highlight need to change by identifying failures that could have been prevented • Conduct team survey to highlight communication problems
Engagement • Identify one (or more) supportive Physician to pilot checklist and promote benefits to colleagues • Highlight need to change by identifying failures that could have been prevented • Conduct team survey to highlight communication problems
 Spread • Track levels of checklist use • Ask those who are not using the checklist why they are not using it • Get current users to present benefits to colleagues (e. g. grand rounds) • Create information sheet promoting benefits • Get supportive dept heads to discuss checklist use with non users
Spread • Track levels of checklist use • Ask those who are not using the checklist why they are not using it • Get current users to present benefits to colleagues (e. g. grand rounds) • Create information sheet promoting benefits • Get supportive dept heads to discuss checklist use with non users
 Improvement • Develop quality audit – Develop checklist of key behaviours (timing, attention of team members etc) – Develop schedule to observe each physician using audit – Provide individual and group feedback • Survey staff groups about how the audit is being used
Improvement • Develop quality audit – Develop checklist of key behaviours (timing, attention of team members etc) – Develop schedule to observe each physician using audit – Provide individual and group feedback • Survey staff groups about how the audit is being used
 Surveys • Modified Stanford Instrument – Used by accreditation Canada, – Does not measure team work • Map. Sa. F – Developed for use in NHS, not sure about copyright issues for use in Canada • ORMAQ – Items are published, includes teamwork
Surveys • Modified Stanford Instrument – Used by accreditation Canada, – Does not measure team work • Map. Sa. F – Developed for use in NHS, not sure about copyright issues for use in Canada • ORMAQ – Items are published, includes teamwork
 ORMAQ teamwork items 17. The only people qualified to give me feedback are members of my own profession. 18. It is better to agree with the operating theatre team members than to voice a different opinion. 22. The doctor’s responsibilities include co-ordination between his or her work team and other support areas. 25. Operating theatre team members share responsibilities for prioritizing activities in high workload situations. 31. I enjoy working as part of a team. 44. To resolve conflicts, team members should openly discuss their differences with each other. 48. All members of the operating theatre team are qualified to give me feedback. 54. The concept of all operating theatre personnel working as a team does not work at this hospital. 56. Effective operating theatre team co-ordination requires members to take into account the personalities of other team members.
ORMAQ teamwork items 17. The only people qualified to give me feedback are members of my own profession. 18. It is better to agree with the operating theatre team members than to voice a different opinion. 22. The doctor’s responsibilities include co-ordination between his or her work team and other support areas. 25. Operating theatre team members share responsibilities for prioritizing activities in high workload situations. 31. I enjoy working as part of a team. 44. To resolve conflicts, team members should openly discuss their differences with each other. 48. All members of the operating theatre team are qualified to give me feedback. 54. The concept of all operating theatre personnel working as a team does not work at this hospital. 56. Effective operating theatre team co-ordination requires members to take into account the personalities of other team members.
 Team Training • Dr. Donald Moorman (Beth Israel Deaconness Hospital in Boston) developed a 3 hour knowledge based team training program, based on CRM • There is some evidence that it is effective – Reduction in errors and adverse events – Increase in teamwork behaviours • Adapted for Canadian teams with permission by: – Mark Taylor, Lesia Yasinski and Mike Rodgers
Team Training • Dr. Donald Moorman (Beth Israel Deaconness Hospital in Boston) developed a 3 hour knowledge based team training program, based on CRM • There is some evidence that it is effective – Reduction in errors and adverse events – Increase in teamwork behaviours • Adapted for Canadian teams with permission by: – Mark Taylor, Lesia Yasinski and Mike Rodgers
 References • Kizer, K. W. 1999. Large system change and a culture of safety. In: Enhancing Patient Safety and Reducing Errors in Health Care. Chicago, IL: National Patient Safety Foundation. • Manchester Patient Safety Framework (Ma. PSa. F) http: //www. nrls. npsa. nhs. uk/resources/? entryid 45=59796 • Sexton J, Helmreich RL, Thomas E. Error, stress and teamwork in medicine and aviation: cross sectional surveys. BMJ 2000; 320: 745 -50 • Fleming, M. , Smith, S. Slaunwhite, J. & Sullivan, J. (2006). Investigating interpersonal competencies in cardiac surgery teams. Canadian Journal of Surgery, Vol 49 No 1. • Team Training materials files. me. com/markfleming/u 3 l 77 t
References • Kizer, K. W. 1999. Large system change and a culture of safety. In: Enhancing Patient Safety and Reducing Errors in Health Care. Chicago, IL: National Patient Safety Foundation. • Manchester Patient Safety Framework (Ma. PSa. F) http: //www. nrls. npsa. nhs. uk/resources/? entryid 45=59796 • Sexton J, Helmreich RL, Thomas E. Error, stress and teamwork in medicine and aviation: cross sectional surveys. BMJ 2000; 320: 745 -50 • Fleming, M. , Smith, S. Slaunwhite, J. & Sullivan, J. (2006). Investigating interpersonal competencies in cardiac surgery teams. Canadian Journal of Surgery, Vol 49 No 1. • Team Training materials files. me. com/markfleming/u 3 l 77 t
 Team training video links • • • files. me. com/markfleming/4 xvafh files. me. com/markfleming/9 pp 0 b 6 files. me. com/markfleming/cm 7 cfk files. me. com/markfleming/dwoxeo files. me. com/markfleming/13 b 8 vo files. me. com/markfleming/qcu 7 gr
Team training video links • • • files. me. com/markfleming/4 xvafh files. me. com/markfleming/9 pp 0 b 6 files. me. com/markfleming/cm 7 cfk files. me. com/markfleming/dwoxeo files. me. com/markfleming/13 b 8 vo files. me. com/markfleming/qcu 7 gr


