208725678998d9ca56bc629b67056c60.ppt
- Количество слайдов: 51

OFFICE OF TRAUMA REPORT October 29, 2010

Recognition State Trauma Medical Director Karanbir Gill, M. D. State Trauma Medical Advisor Patricia Byers, M. D.

2010 Session Trauma System Legislative Update

2010 Session Trauma System Legislative Update • SB 768 Enrolled Relating to Luis Rivera Ortega Street Racing Act Status: Signed by the Governor on 6/3/2010.

Trauma System Legislative Update • HB 325 Enrolled Uniform Traffic Control/Mark Wandall Traffic Safety Program – Traffic Infraction Detectors Status: The bill was signed in to law by the Governor on 5/13/2010. This bill provides additional funding for Florida’s Trauma Centers. Rule Hearing scheduled for October 13, 2010.

Trauma System Legislative Update Continued HB 5311 Enrolled - Relating to Department of Health Reorganization and Conforming Bill Status: Approved by Governor on 5/28/2010. Office of Trauma staff have been working with the department leadership with specific assignments related to restructuring and reorganization.

Rule Promulgation • Apportionment of Trauma Centers within a Trauma Service Area (TSA) – 64 J-2. 010, F. A. C. –. C. Rule hearing held October 13, 2010 • Surgical and Nonsurgical Specialists- Rule development workshop held August , 2010 • Future rule development workshops to be held: Trauma Center Application- 64 J-2010, F. A. C. Rule language being developed

2010 Trauma Center Application Process Applications Submitted 4/1/10 • Bay Medical Center, Level II (Withdrawn 9/2010) • University of Miami Hospital, Level II (Withdrawn 4/12/10) • Kendal Regional Medical Center, Level II • Orange Park Medical Center, Level II • Blake Medical Center, Level II • Fort Walton Medical Center, Level II (Withdrawn 9/2010) • Regional Medical Center Bayonette Point, Level II

Letter of Intent, Effective 10/1/10 Delray Medical Center – Level I Saint Mary’s Medical Center- Level l Bay Medical Center – Level ll Ft Walton Beach Medical Center- Level ll

Major Accomplishments 1998 - Present Injury Prevention: • 282 prevention and outreach programs • EMS grant funding was renewed to continue implementing Walk. Safe™, an evidenced based program Outcome: 21 trauma centers participated • “Prom Night, ” “Prom-Promise, ” and Shattered Dreams” Outcome: • In 1998, there were 50 deaths statewide on prom night. • In 2006, 2007, 2008, 2009 and 2010 there were no deaths.

Major Accomplishments 1998 – Present continued Research: Currently, there approximately 235 research projects, including pharmaceutical clinical trials; Total: $288 M

Major Accomplishments 1998 – Present continued New Programs and Studies: • First Ventilator-Dependent Rehabilitation Program May 2008 • Implementation of the Preventive Ulcer Program standards in all 21 trauma centers 2009 – Present • BSCIP Standards for Preventative Ulcer Program (PUP) implemented – April 2009 Outcome: Third quarter statistics in 2010 with the implementation of the program for Trauma and BSCIP patients indicated a 10% decrease in pressure ulcers of spinal cord patients. Adopted in Rule – April, 2010

Major Accomplishments 1998 – Present Continued • Diaphragmatic Pacer Program Outcome: First Diaphragmatic Pacing Surgery in Florida. Implemented May 2009 YTD – 9 patients on program

Major Accomplishments 1998 – Present Continued • Trauma Centers Verified - two additional trauma centers were verified in 2009 and 2010 • Legislatively Mandated Trauma Center Payments • Funding Source - From 2005 to December 31, 2009, the Office of Trauma had distributed a total of $20. 6 million to Florida’s trauma centers • Improving Trauma Center Compliance - In 2007, the Office of Trauma and the Brain and Spinal Cord Injury Program conducted eight combined site surveys in 2007. These combined surveys delivered a cost savings of $45, 000 per survey for the residents of Florida.

Major Accomplishments 1998 – Present Continued • Traumatic Brain Injury Grant Outcomes - Number of registered nurses and other healthcare professionals educated on the Mild TBI Curriculum from March 2004 to December 2009: 8, 100 • Mass Casualty Events and Mild TBI Grant Outcomes From the implementation of this grant in 2005 to December 31, 2009, 4, 125 emergency room nurses from acute care hospitals and trauma centers have received the training

Major Accomplishments 1998 – Present Continued HRSA / ASPR Burn Care Grants • Bombs, Burns and Blast DVD Second Education - As of December 2009, the 21 trauma centers and 60 nontrauma centers have used this DVD to train a total of 48, 000 EMTs and paramedics, and 26, 000 healthcare providers. • Phase II Burn Grant for Physician Training • Phase III - Web-Based Training Program “Burn Center” - Since the release of “Burn Center” video game in mid. October 2008, over 260 trauma physicians, residents/fellows, and trauma nurses have completed the training

Major Accomplishments 1998 – Present Continued Florida Trauma Telemedicine Networks Implemented • Phase I: In FY 2008 -2009 - Phase I was completed in 2009, which linked two Level I trauma centers (Jackson Memorial Hospital/Ryder Trauma Center and the Shands at the University of Florida in Gainesville) with community and rural hospital emergency rooms in each of their respective trauma service areas

Major Accomplishments 1998 – Present Continued Florida Trauma Telemedicine Networks Implemented • Phase II - Orlando Regional Medical Center, Sacred Heart Hospital and Tampa General Hospital are participating trauma telemedicine centers in FY 2009 -2010. This grant also provided some limited sustainment funds for the current participating facilities. Phase II has been implemented in the Phase II trauma centers and in additional rural facilities to each of the participating pilot trauma centers established in Phase I

Major Accomplishments 1998 – Present Continued Florida Trauma Telemedicine Networks Implemented • Phase III - Link Lee Memorial, Tallahassee Memorial Healthcare, and Holmes Regional Medical Center trauma centers with their satellite community or rural hospitals

Major Accomplishments 1998 – Present Continued • American College of Surgeons’ Disaster Management Course Implemented - Since the initiation of the course in 2007, there have been a total of 18 classes conducted throughout the state, educating approximately 450 health care providers from the 21 trauma centers, and approximately 19 other hospitals • Trauma Transport Protocols Reviewed Annually – No adverse outcomes from 2007 to 10/10

Major Accomplishments 1998 – Present Continued • Florida Department of Transportation Motorcycle Safety Grant - The Office of Trauma was the recipient of a $250, 000 Florida Department of Transportation grant for a statewide motorcycle safety education project through the Florida's trauma centers from 10/10 through 10/11

Strategic Plan • As of June, 2010, approximately 90% of the goals and objectives of the current five-year strategic plan have been accomplished • Recognized the “Florida Trauma System Plan Committee” to include additional partners and stakeholders needed to complete the current plan and develop the next five-year strategic plan • Completed SWOT analysis – November 2009 • Strategic Planning Session was held on February 25, 2010 • Conference calls have been held from April – June to review each goal, objectives, and strategies • Strategic Plan reviewed and approved June 30, 2010

Sterling Scorecard Evaluations • The Office of Trauma staff has initiated benchmarks for evaluating effectiveness based on Sterling models. • These benchmarks include the following: • product service outcomes • access to trauma care • trauma centers’ mandated quarterly data • customer focused results • financial market results • human resources • organizational effectiveness • leadership and social responsibility

Indicators Access to Trauma Care: • Increase access to a trauma center for definitive trauma care within the “Golden Hour” to 99% of Florida’s population by 2010

Indicators Continued Trauma Centers’ Mandated Quarterly Data: • The number of deaths. Outcome- Florida’s mortality rate has decreased from 6% in • • 2004 to 4. 8 % in 2009. The number of unplanned, trauma-related re-admissions to the hospital within 30 days of discharge Outcome: JCAHO standard 3 -4%, from -2007 -2009 - range 1. 7%- 1. 6% The number of unplanned admissions or re-admissions to an intensive care unit Outcome: JCAHO standard 4 -5%, from 2007 -2009 - range 2. 6 -1. 7% Customer Focused Results: • % satisfaction with site visit process – trauma centers (CEO, TMD, TPM) • Outcome: overall satisfaction 95%, major request for change process included electronic presurvey questionnaire was needed. This has been developed, and implemented 8/2010. • # complaints regarding trauma office 1/2010 - present, no complaints reported

Indicators Continued Financial Market Results: • Notification of spending plan completion • % prompt payments - 99% - Office of Trauma Human Resources: • Turnover rate- 5% Organizational Effectiveness • % of trauma centers in compliance with standards (21 trauma centers) • Registry minimum data set quality/completeness (DOH staff send quarterly reports and reviews with trauma center staff)

Indicators Continued Leadership and Social Responsibility • % compliance with strategic action plans (90%) • % compliance with fiscal audits (100%) • FDOT Grant of $107, 000 deliverables for Motorcycle Safety and Injury Prevention (100% compliance) • ASPR funding for telemedicine , OR supplies/equipment and ACS Disaster Course (100% compliance) • HRSA Rural Health Grant for ACS Rural Health Course ( 100% Compliance)

Disaster Response Operation Haiti

Disaster Response Operation Haiti Lessons Learned • Telemedicine was effective and efficient for patient transport • 519 patients transported from Haiti to trauma centers and acute care hospitals • No reported patient deaths while being transported

Contact Information Office of Trauma Website: http: //www. doh. state. fl. us/demo/Trauma

State Trauma Medical Director: Karanbir Gill, M. D. , F. A. C. S. 2005 – 2010 Trauma State Plan update reports by planning teams

Goal 1 Leadership Executive Committee of the Florida Trauma System Plan Committee Membership DOH Trauma Leadership Team State Trauma Medical Director State Trauma Medical Advisor Chair (FTSPC) Vice Chair (FTSPC) Planning team leads

Goal 2 Injury Prevention and Control Lead: Olumide Sobowale, M. D.

Goal 3 Disaster Response: Emergency/ Disaster Preparedness Planning Lead: Dr. John Armstrong – MCI Co-Leads: Dr. Eric Frykberg - Mass Casualty & Training Dr. David Mozingo - Burn Care Dr. Antonio Marttos - Telemedicine

Goal 4 Pre-Hospital Care and Transport Co-Leads: Dr. Joseph Nelson, Dr. Laurie Romig, and Dr. Andrew Kerwin

Goal 5 Trauma Center Care Lead: Patricia Byers, M. D. Standards Lead: Ernest Block, M. D.

Goal 6 Rehabilitation: Medical Rehabilitation for Trauma Patients Co-Leads: Dr. Gillian Hotz Dr. Cynthia Beaulieu Dr. John Kuluz

Goal 7 Quality Improvement Lead: Lianne Brown, R. N. , M. B. A. Staff Liaisons Dianna Liebnitzky Michael Lo Carma Harvey

Goal 8 System Evaluation Leads: Dr. Rodney Durham – Systems Evaluations Dr. Lawrence Lottenberg – Systems Evaluations Dr. Karanbir Gill – Rural Trauma Health Dr. Winston Richards – Hand Surgery

Goal 9 Trauma Registry/Research Co-Leads: Dr. Joseph Tepas Dr. Drew Mikulaschek Dr. Carl Schulman Trauma Registry Consultants: Barbara Orban, Ph. D. , Etienne Pracht, Ph. D, and Pam Pieper, Ph. D.

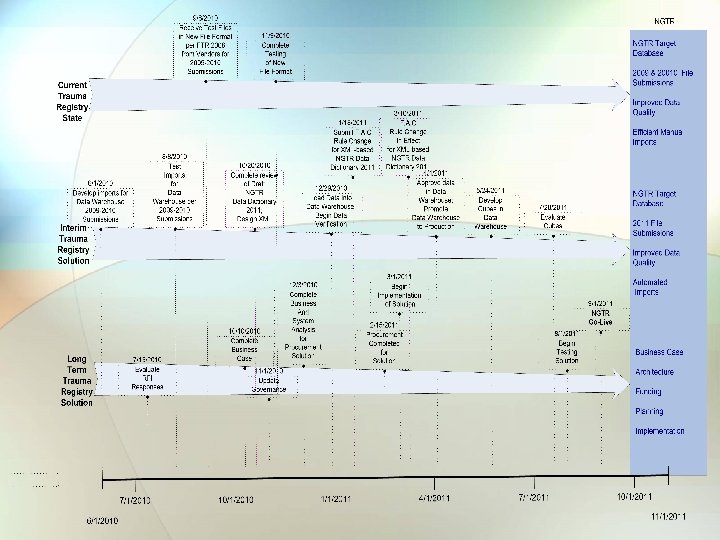
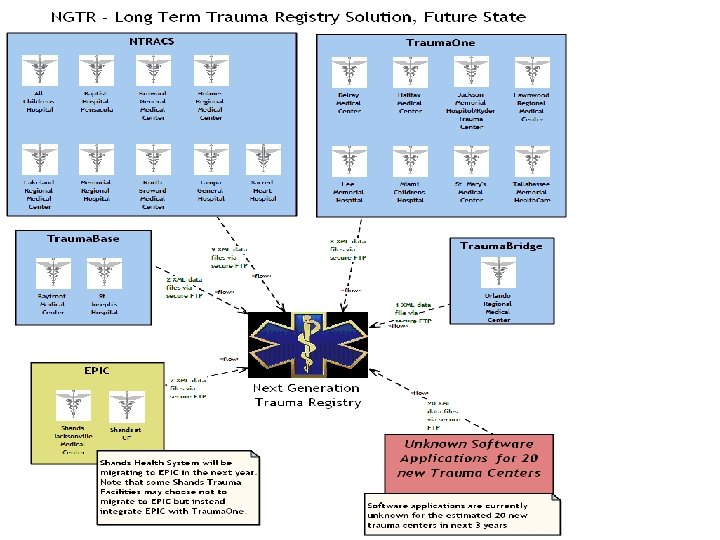
Next Generation Trauma Registry (NGTR) Project Update

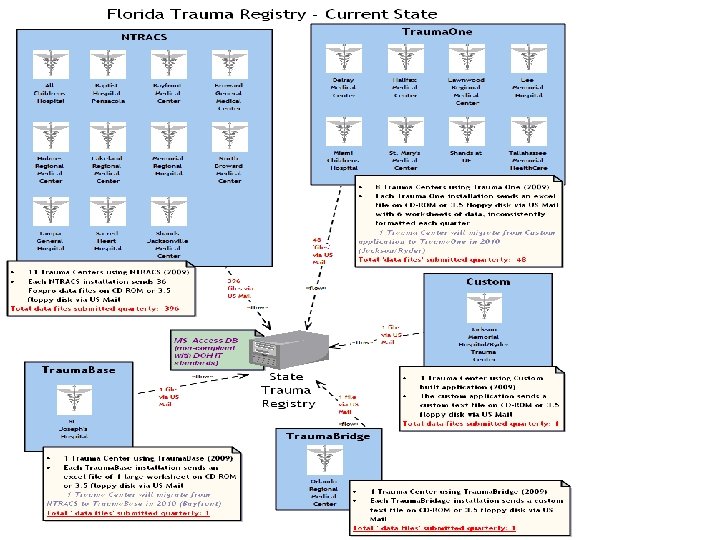
Current State • Current Pain Points – Lack of standardization of file formats between: • • • NTRACS (11 trauma centers) Trauma. One (8 trauma centers) Trauma. Base (1 trauma center) Trauma. Bridge (1 trauma center) Custom (1 trauma center) – Overwhelming number of files to integrate each year • NTRACS: __T, __PRE, __DAG, __USE, etc. x 11 TC x 4 quarters • Trauma. One: up 5 Excel tabs in state dumps x 8 TC x 4 quarters • Patient Age, LOS, etc. can be numeric in one quarter, alpha in another – these fields must be standardized before integration • Pain Points must be addressed to enable: – More efficient calculation of ICISS for payments – Release of raw data for research/analysis, QI, grants, etc – Linkage to other data: EMS, BSCIP, AHCA, DHSMV, etc.

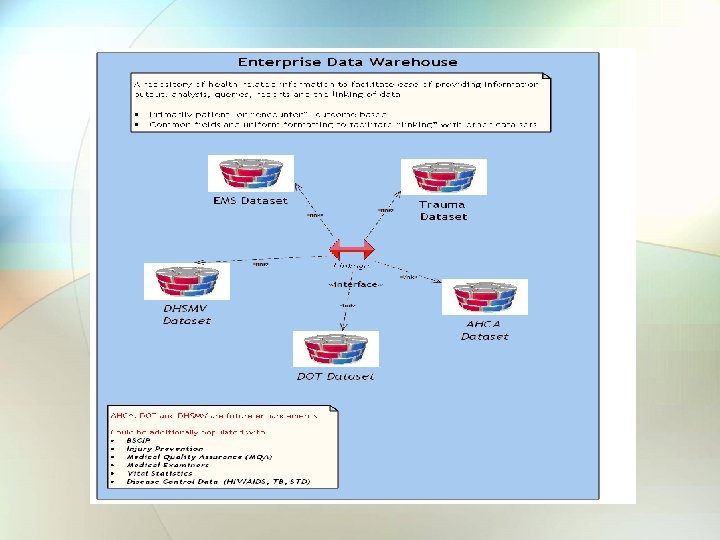
Major Actions/Accomplishments • Since July 2010: – Interim Solution (to address current pain points) • Performed initial testing of standardized file submission formats for files submitted in 2009 and 2010 from vendors/TC • Completed review of sections within draft of FL Trauma Registry (FTR) Data Dictionary 2011 with FL Trauma Data Group • Designed NGTR SQL database in DOH DEMO Enterprise Data Warehouse • Developed imports of files into DOH DEMO Enterprise Data Warehouse for each file format (NTRACS, Trauma. One, etc. ) – Long-Term Solution (to better meet trauma needs) • Buy vs. Build: Determination to Buy the Solution – Evaluated vendor responses to Request for Information (RFI) for potential trauma registry software applications for NGTR – Reviewed software product demonstrations by vendors – Contacted peer state organizations for advice/vendor references • Completed initial draft of core Business Case for review and approval by DOH IT Governance Committee

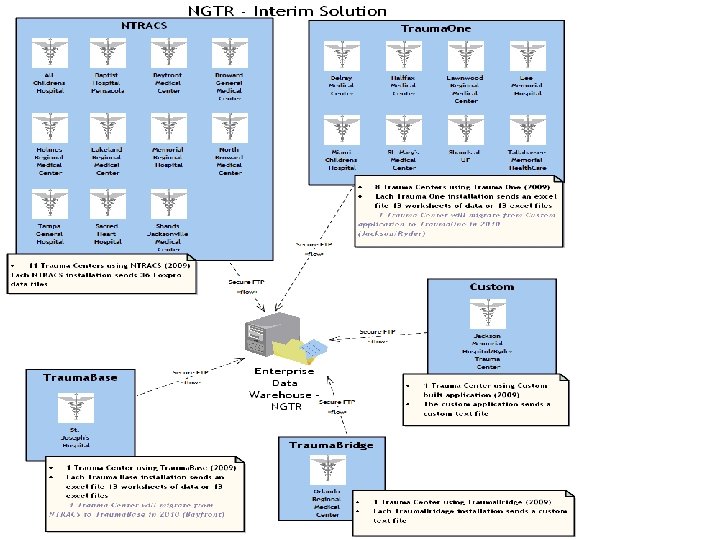
Interim Solution • Scope of 1 st phase (Development) – In-Progress • Integration and testing of imports • Basic validation reports • Estimated completion: January 2011 • Scope of 2 nd phase (Linkage evaluation - Not yet started) • • • Evaluation of data quality Analysis of linkage to EMS Development of linkage reports and cubes for aggregate reporting Development of imports for NGTR XML files to be submitted in 2011 Estimated completion: July 2011

Long-Term Solution • Planning Phase – In-Progress • Completion of Business and System analysis for Business Case • Development of Invitation to Negotiate (ITN) requirements • Estimated Completion of Planning Phase: May 2011

Next Steps • October 2010 – Imports for 2009 -2010 data completed for DOH DEMO Enterprise Data Warehouse • January 2011 – Trauma data loaded for 2009 -2010 DOH DEMO Enterprise Data Warehouse • Testing of imports – Design of XML schema for FTR 2011 XML Data Dictionary – ITN advertised • March 2011 – ITN awarded – Rule change completed for FTR 2011 XML Data Dictionary
208725678998d9ca56bc629b67056c60.ppt