f86d1ace6d042dd30df4712e80fdb0b0.ppt
- Количество слайдов: 42

Obesity in Adults: Treatment and Management Gary D. Foster, Ph. D Clinical Director, Weight and Eating Disorders Program Assistant Professor, Department of Psychiatry University of Pennsylvania School of Medicine © 2000 University of Pennsylvania School of Medicine

Objectives · Describe the efficacy of the following for the treatment of obesity: Ø Behavioral methods Ø Pharmacological therapy Ø Surgical approaches · Identify the pros and cons of self-help diets for the treatment of obesity. · Review new guidelines for successful outcomes in obesity treatment. © 2000 University of Pennsylvania School of Medicine

Treatment of Obesity · Behavioral · Pharmacological · Surgical · Self help programs and books © 2000 University of Pennsylvania School of Medicine

Behavioral Treatment Philosophy · Consists of a set of principles and techniques to modify eating and activity habits. · Emphasizes small and sustainable changes. © 2000 University of Pennsylvania School of Medicine

Behavioral Treatment Methods Identifying Patterns · Buy chips · Leaves chips on table · Come home from work, tired and hungry · See kids eating chips · Eat several handfuls of chips standing up · Feel guilty · Finish bag of chips © 2000 University of Pennsylvania School of Medicine

Behavioral Treatment Methods · Self-monitoring Ø Recording food intake/evaluating nutrients Ø Recording physical activity · Stimulus control techniques Ø Time Ø Place Ø Activity Ø Sight/smell Ø Emotions © 2000 University of Pennsylvania School of Medicine

Behavioral Treatment Methods Rationale for Increasing Physical Activity · Associated with significant health benefits. · Single best predictor of weight maintenance. · Not associated with short-term weight loss. © 2000 University of Pennsylvania School of Medicine

Behavioral Treatment Methods Increasing Physical Activity · Identify barriers Ø Lack of time Ø Lack of motivation Ø Increased safety concerns · Prescribe small changes Ø Take the stairs Ø Gardening Ø Walking during work © 2000 University of Pennsylvania School of Medicine

Behavioral Treatment Results · 10% reduction over 20 to 24 weeks · 33% regain at one year · More weight regained over time © 2000 University of Pennsylvania School of Medicine

Improving Weight-loss Maintenance · Continued care · Sustaining dietary changes · Exercise · Pharmacotherapy © 2000 University of Pennsylvania School of Medicine

Treatment of Obesity Pharmacological Therapy · Pharmacological interventions to facilitate weight loss and behavior change include: Ø Enhancing satiety Ø Decreasing fat absorption Ø Increasing energy expenditure Ø Decrease appetite © 2000 University of Pennsylvania School of Medicine

Sibutramine (Meridia) Mechanism of Action · Serotonin and norepinephrine re-uptake inhibitor (SNRI). · Animal research data shows drug reduces body weight by: Ø Decreasing food intake in rats Ø Stimulates thermogenesis in rats © 2000 University of Pennsylvania School of Medicine

Sibutramine (Meridia) Summary of Research Findings · 6% to 8% weight loss with 10 to 15 mg/day. · 2% weight loss with placebo. · Published data available up to one year. © 2000 University of Pennsylvania School of Medicine

Sibutramine (Meridia) Summary of Reported Adverse Event Percent (%) of Patients Adverse Event Placebo (n = 884) Sibutramine (n=2068) Dry mouth 4 17 Anorexia 4 13 Constipation 6 12 Insomnia 5 11 Appetite increase 3 9 Dizziness 4 7 Nausea 3 6 Package insert data, Sibutramine, 1998. © 2000 University of Pennsylvania School of Medicine

Sibutramine (Meridia) Prescribing Information · For patients with BMI > 30 or > 27 in the presence of risk factors. · 5 to 15 mg per day. · Not for patients on SSRIs (e. g. Paxil, Zoloft, Prozac) · Not for patients with poorly controlled hypertension, history of coronary artery disease, CHF, arrhythmia or stroke. · Regular BP and heart rate monitoring required. © 2000 University of Pennsylvania School of Medicine

Orlistat (Xenical): Mechanism of Action · Activity occurs in the stomach and small intestine. · Inhibits gastric and pancreatic lipases. · 30% of ingested fat is unabsorbed and excreted. · Minimal systemic absorption. · Low-fat diet ( 30%) required to minimize side effects. © 2000 University of Pennsylvania School of Medicine
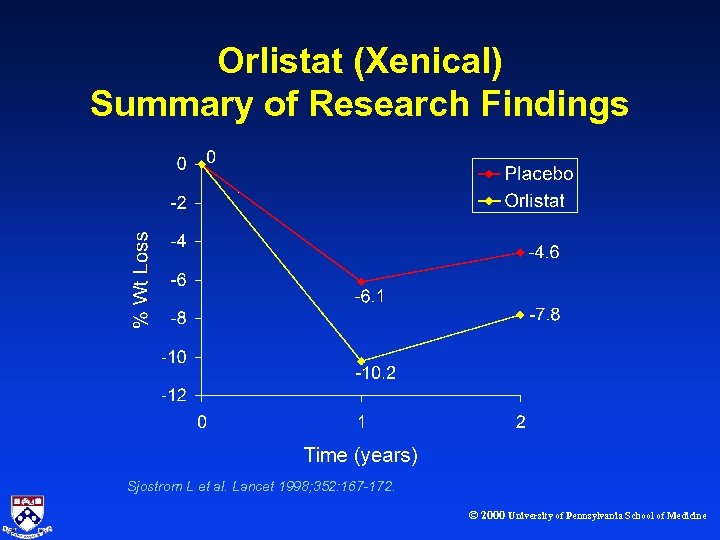
Orlistat (Xenical) Summary of Research Findings Sjostrom L et al. Lancet 1998; 352: 167 -172. © 2000 University of Pennsylvania School of Medicine

Orlistat (Xenical) Summary of Reported Adverse Events Overall Incidence (% of Patients) Oily spotting 26. 6 Flatus with discharge 23. 9 Fecal urgency 22. 1 Oily stool 20. 0 Oily evacuation 11. 9 Increased defecation 10. 8 Fecal incontinence 7. 7 Package insert data, Orlistat, 1998. © 2000 University of Pennsylvania School of Medicine

Orlistat (Xenical) Prescribing Information · 120 mg TID with meals containing fat. · Patients should be on a nutritionally balanced, low-fat diet (< 30%) to minimize side effects. · Prescribe multivitamin to be taken at least two hours before or after the medication. · Orlistat is contraindicated for pregnant or lactating women, and those with chronic malabsorption syndromes or cholestasis. © 2000 University of Pennsylvania School of Medicine

Chronic Pharmacological Treatment and Challenges · Similar to pharmacotherapy of other chronic conditions. · Consistent weight gain seen when medications are discontinued. · Requires intensive risk/benefit analysis and careful patient selection. · Safe and effective medications. © 2000 University of Pennsylvania School of Medicine

Surgical Treatment of Obesity · Patient selection criteria Ø BMI > 40 or > 35 for those with weight related co-morbidities. Ø History of failed conservative weight loss approaches. Ø No substance abuse and/or psychiatric disorders. · Surgical options Ø Vertical banded gastroplasty (VBG) Ø Gastric bypass (GBP) · Outcomes Ø Weight loss is 25% to 35% of initial weight. Ø Weight loss is generally well maintained. Ø Significant improvement in co-morbidities. © 2000 University of Pennsylvania School of Medicine

Surgical Treatment of Obesity Vertical Banded Gastroplasty (VBG) Staple Line Ø Formation of small proximal gastric pouch. Ø Restricts amount of food without bypassing the gut. Ø Delays gastric emptying. Ø Creates feeling of early satiety. Pouch Band Fundus © 2000 University of Pennsylvania School of Medicine

Surgical Treatment of Obesity Gastric Bypass Ø Ø Delays gastric emptying. Ø Interferes with absorption of nutrients. Ø May induce dumping syndrome after high carbohydrate meal. Staple Line Formation of 20 -30 ml proximal gastric pouch. Pouch Fundus Jejunum © 2000 University of Pennsylvania School of Medicine

Treatment of Obesity Popular Weight Loss Diets · Low-calorie diets Ø Calorie deficit allows for 1 to 2 pound weight loss/week Ø Nutritionally balanced food plan (15% protein, 30% fat, 55% carbohydrate) Ø Weight Watchers, Jenny Craig · High protein, low carbohydrate diets Ø Emphasis can vary between unrestricted sources of protein and consumption of only lean sources (chicken, fish). Ø Dr. Atkins’ New Diet Revolution, The Zone, Sugar Busters. © 2000 University of Pennsylvania School of Medicine

Treatment of Obesity Popular Weight Loss Diets · Low-calorie diets Ø Weight Watchers Ø Jenny Craig · Low-carbohydrate diets Ø Dr. Atkins’ New Diet Revolution Ø The Zone Ø Sugar Busters © 2000 University of Pennsylvania School of Medicine

Low-Calorie Diets · Usually provide a total calorie deficit to allow for 1 to 1 1/2 pounds of weight loss per week. · Rely on use of fat-free and low-fat foods. · Balanced nutritional food plan. (15% protein, 30% fat, 55% carbohydrate) · Mulitvitamin/mineral supplement recommended. © 2000 University of Pennsylvania School of Medicine

Commercial Programs Weight Watchers · Traditional program includes a balanced low calorie diet containing 1200 calories per day for women; 1800 calories for men. · Offers a flexible 1 -2 -3 program which enables you to eat whatever you want using a point system which are determined based on your weight loss goals. · Priced reasonably; approximately $12. 00 per visit. · Weekly “weigh-ins” and purchasing your own food. · Group meetings lead by successful program graduates which provide support and advice on behavior modification, exercise, and nutrition. © 2000 University of Pennsylvania School of Medicine

Commercial Programs Jenny Craig · Offers several programs to meet individual needs · Provides weekly planned menus which are nutritionally balanced · Menus feature Jenny Craig packaged foods which can cost approximately $65 - $75 per week · Offers convenience for the person who does not cook · Calorie levels range from 1000 - 2300 calories/day · Provides basic strategies for managing stress and physical activity · Staff not medically trained © 2000 University of Pennsylvania School of Medicine

Dr Atkins’ Diet Book • High protein diet. • To identify methods to assess the nutritional status of healthy patients as well as those with acute or chronic illness. • To identify risk factors and usual physical findings associated with malnutrition and determine who would benefit from additional nutrition counseling. © 2000 University of Pennsylvania School of Medicine

Atkins Diet: The Rules of the Induction Diet (14 days) • Diet consists of pure proteins and fat with < 20 grams carbohydrates per day. • Sample menu: Ø Breakfast: Ham, cheese, mushroom omelet with bacon or smoked fish with cream cheese. Ø Lunch: Chef salad with ham, chicken, cheese, eggs, creamy Italian dressing or bacon cheeseburger- no bun. Ø Dinner: rack of lamb, salmon or chicken and salad. Ø Dessert: assorted cheeses or diet Jello with heavy cream. © 2000 University of Pennsylvania School of Medicine

Biochemical Aspects of the Atkin’s Diet • No more than 20 grams of carbohydrates/day so that insulin levels are decreased. • Low insulin/glucagon (IG) ratio results in fatty acid oxidation and gluconeogenesis for energy. • Goal is to achieve ketosis/lipolysis. • High protein diet needed to preserve lean body mass (muscle protein) however there is always a state of low protein synthesis due to low IG ratio. © 2000 University of Pennsylvania School of Medicine

Metabolic Effects of Low Carbohydrate Diets · Significant reduction in caloric intake. · Significant reduction in B vitamins and fiber intake. · Increased ketone formation if severe CHO restriction. · High saturated fat diet clearly shown to increase serum LDL levels and risk of CVD. · No long-term studies on weight change (-/+) or effects on serum glucose or LDL levels. © 2000 University of Pennsylvania School of Medicine

Zone Diet Book by Barry Zears, Ph. D • Ideal ratio of carbohydrate, fat, and protein is 40, 30, respectively. • All meals and snacks should be composed of this nutrient ratio. • Can purchase meals, beverages, snack bars providing correct nutrient ratio. • Based on the fact that carbohydrates stimulate insulin secretion which in turn causes excess calories to be converted to fat. • Emphasizes low fat proteins such as chicken and fish. • Avoidance of caffeine is recommended. • Calculating correct amount of protein, fat, and carbohydrate per meal can be time consuming. © 2000 University of Pennsylvania School of Medicine

Sugar Busters Drs. Rachael and Richard Heller • Follows the basic diet plan of Dr. Atkins’ high protein, low carbohydrate diet, emphasizing lean meats. • Focus is on avoiding refined carbohydrates such as sugar and white rice. • Diet allows one reward meal each day in which carbohydrates are permitted. • Avoids food eaten in combination (i. e. fruits should not be eaten with meat dishes). © 2000 University of Pennsylvania School of Medicine

Improving Weight-loss Maintenance · Continued care · Exercise · Pharmacotherapy · Other © 2000 University of Pennsylvania School of Medicine

Weight Change: Former Criteria for Success · Reduction to ideal body weight. · Reduction of 50% of excess weight. · Reduction to upper limit of “normal” body fat © 2000 University of Pennsylvania School of Medicine

Reasons for Abandoning Ideal Weight with Significantly Overweight People · Most cannot achieve ideal weight, even with most aggressive approaches. · Most cannot maintain losses >15% of initial body weight without surgery. · Losses of 5% to 10% of body weight are associated with significant health improvements. © 2000 University of Pennsylvania School of Medicine

Weight Change New Criteria for Success · According to the Institute of Medicine’s report, Weighing the Options: Ø Successful long-term weight control by our definition means losing at least 5% of body weight and keeping it below our definition of significant weight loss for at least one year. Ø Weight loss of only 5% to 10% of body weight may improve many of the problems associated with overweight, such as high blood pressure and diabetes. Thomas P (ed). Weighing the Options. Washington, DC: IOM, National Academy Press, 1995. © 2000 University of Pennsylvania School of Medicine

What Is A Reasonable Weight Loss ? Patients’ Expectations and Evaluations of Obesity Treatment and Outcome · Study design Ø 60 obese women, age 40 + 8. 7 yrs. Ø BMI 36. 3 + 4. 3 kg/m 2 · Subjects questioned about their goal weight Ø Dream weight Ø Happy weight Ø Acceptable weight Ø Disappointed weight Foster GD, et al. J Consult Clin Psychol 1997; 65: 79 -85. © 2000 University of Pennsylvania School of Medicine

Results Defined Weights % Reduction Dream 38% Happy 31% Acceptable 25% Disappointed 17% Foster GD, et al. J Consult Clin Psychol 1997; 65: 79 -85. © 2000 University of Pennsylvania School of Medicine
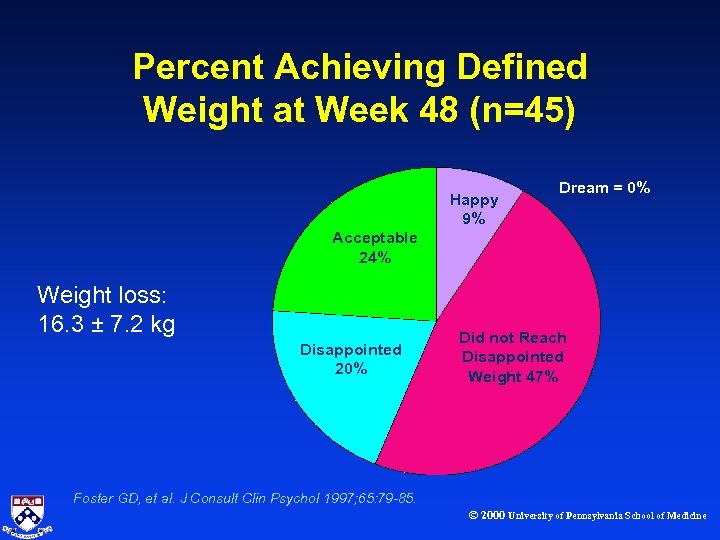
Percent Achieving Defined Weight at Week 48 (n=45) Happy 9% Dream = 0% Acceptable 24% Weight loss: 16. 3 ± 7. 2 kg Disappointed 20% Did not Reach Disappointed Weight 47% Foster GD, et al. J Consult Clin Psychol 1997; 65: 79 -85. © 2000 University of Pennsylvania School of Medicine

Helping Patients Accepts More Modest Weight Loss · Be clear about what treatment can and cannot do. · Discuss biological limits. · Focus on non-weight outcomes. · Be empathic about dissatisfaction with weight and shape. © 2000 University of Pennsylvania School of Medicine
f86d1ace6d042dd30df4712e80fdb0b0.ppt