944c27e2794220f5db355491bbdbdc2f.ppt
- Количество слайдов: 56
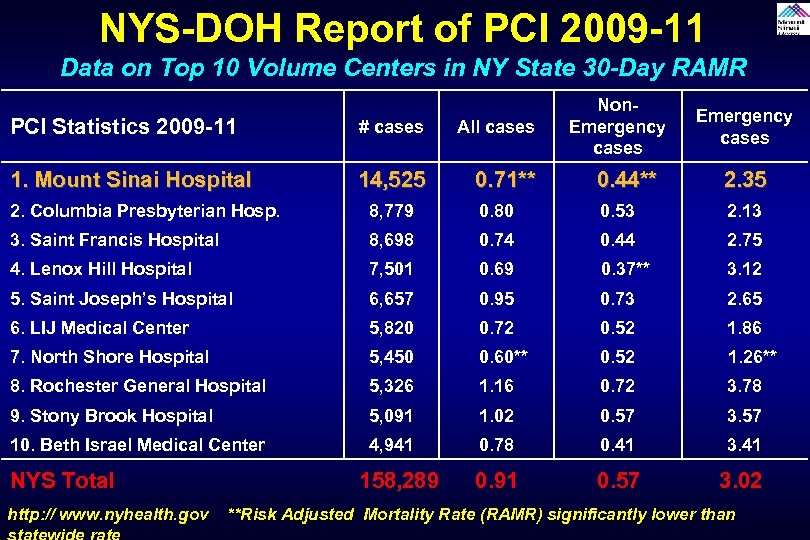 NYS-DOH Report of PCI 2009 -11 Data on Top 10 Volume Centers in NY State 30 -Day RAMR Non. Emergency cases PCI Statistics 2009 -11 # cases All cases 1. Mount Sinai Hospital 14, 525 0. 71** 0. 44** 2. 35 2. Columbia Presbyterian Hosp. 8, 779 0. 80 0. 53 2. 13 3. Saint Francis Hospital 8, 698 0. 74 0. 44 2. 75 4. Lenox Hill Hospital 7, 501 0. 69 0. 37** 3. 12 5. Saint Joseph’s Hospital 6, 657 0. 95 0. 73 2. 65 6. LIJ Medical Center 5, 820 0. 72 0. 52 1. 86 7. North Shore Hospital 5, 450 0. 60** 0. 52 1. 26** 8. Rochester General Hospital 5, 326 1. 16 0. 72 3. 78 9. Stony Brook Hospital 5, 091 1. 02 0. 57 3. 57 10. Beth Israel Medical Center 4, 941 0. 78 0. 41 3. 41 0. 91 0. 57 3. 02 NYS Total http: // www. nyhealth. gov 158, 289 **Risk Adjusted Mortality Rate (RAMR) significantly lower than
NYS-DOH Report of PCI 2009 -11 Data on Top 10 Volume Centers in NY State 30 -Day RAMR Non. Emergency cases PCI Statistics 2009 -11 # cases All cases 1. Mount Sinai Hospital 14, 525 0. 71** 0. 44** 2. 35 2. Columbia Presbyterian Hosp. 8, 779 0. 80 0. 53 2. 13 3. Saint Francis Hospital 8, 698 0. 74 0. 44 2. 75 4. Lenox Hill Hospital 7, 501 0. 69 0. 37** 3. 12 5. Saint Joseph’s Hospital 6, 657 0. 95 0. 73 2. 65 6. LIJ Medical Center 5, 820 0. 72 0. 52 1. 86 7. North Shore Hospital 5, 450 0. 60** 0. 52 1. 26** 8. Rochester General Hospital 5, 326 1. 16 0. 72 3. 78 9. Stony Brook Hospital 5, 091 1. 02 0. 57 3. 57 10. Beth Israel Medical Center 4, 941 0. 78 0. 41 3. 41 0. 91 0. 57 3. 02 NYS Total http: // www. nyhealth. gov 158, 289 **Risk Adjusted Mortality Rate (RAMR) significantly lower than
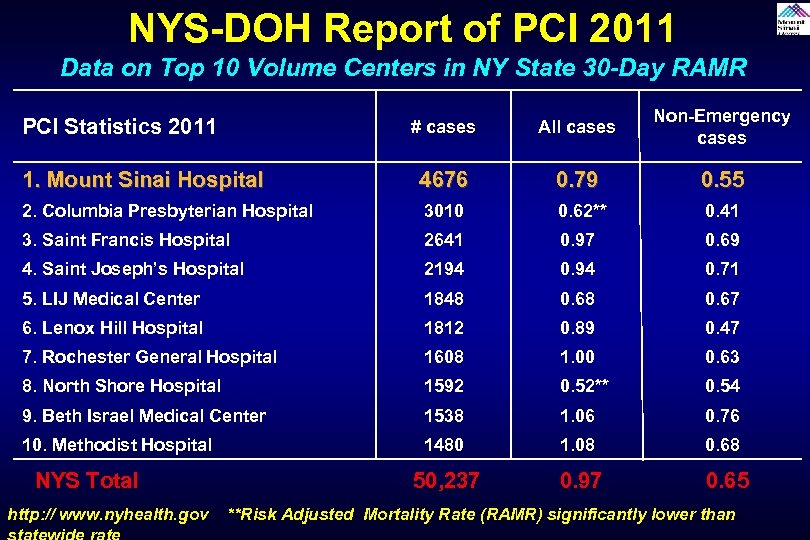 NYS-DOH Report of PCI 2011 Data on Top 10 Volume Centers in NY State 30 -Day RAMR # cases All cases Non-Emergency cases 1. Mount Sinai Hospital 4676 0. 79 0. 55 2. Columbia Presbyterian Hospital 3010 0. 62** 0. 41 3. Saint Francis Hospital 2641 0. 97 0. 69 4. Saint Joseph’s Hospital 2194 0. 71 5. LIJ Medical Center 1848 0. 67 6. Lenox Hill Hospital 1812 0. 89 0. 47 7. Rochester General Hospital 1608 1. 00 0. 63 8. North Shore Hospital 1592 0. 52** 0. 54 9. Beth Israel Medical Center 1538 1. 06 0. 76 10. Methodist Hospital 1480 1. 08 0. 68 50, 237 0. 97 0. 65 PCI Statistics 2011 NYS Total http: // www. nyhealth. gov **Risk Adjusted Mortality Rate (RAMR) significantly lower than
NYS-DOH Report of PCI 2011 Data on Top 10 Volume Centers in NY State 30 -Day RAMR # cases All cases Non-Emergency cases 1. Mount Sinai Hospital 4676 0. 79 0. 55 2. Columbia Presbyterian Hospital 3010 0. 62** 0. 41 3. Saint Francis Hospital 2641 0. 97 0. 69 4. Saint Joseph’s Hospital 2194 0. 71 5. LIJ Medical Center 1848 0. 67 6. Lenox Hill Hospital 1812 0. 89 0. 47 7. Rochester General Hospital 1608 1. 00 0. 63 8. North Shore Hospital 1592 0. 52** 0. 54 9. Beth Israel Medical Center 1538 1. 06 0. 76 10. Methodist Hospital 1480 1. 08 0. 68 50, 237 0. 97 0. 65 PCI Statistics 2011 NYS Total http: // www. nyhealth. gov **Risk Adjusted Mortality Rate (RAMR) significantly lower than
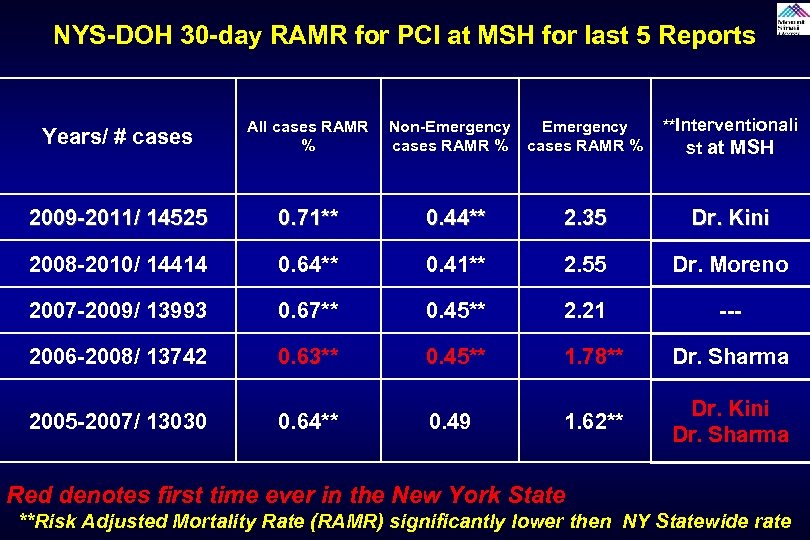 NYS-DOH 30 -day RAMR for PCI at MSH for last 5 Reports Years/ # cases 2009 -2011/ 14525 0. 71** 0. 44** 2. 35 Dr. Kini 2008 -2010/ 14414 0. 64** 0. 41** 2. 55 Dr. Moreno 2007 -2009/ 13993 0. 67** 0. 45** 2. 21 --- 2006 -2008/ 13742 0. 63** 0. 45** 1. 78** Dr. Sharma 1. 62** Dr. Kini Dr. Sharma 2005 -2007/ 13030 0. 64** Non-Emergency cases RAMR % **Interventionali All cases RAMR % 0. 49 st at MSH Red denotes first time ever in the New York State **Risk Adjusted Mortality Rate (RAMR) significantly lower then NY Statewide rate
NYS-DOH 30 -day RAMR for PCI at MSH for last 5 Reports Years/ # cases 2009 -2011/ 14525 0. 71** 0. 44** 2. 35 Dr. Kini 2008 -2010/ 14414 0. 64** 0. 41** 2. 55 Dr. Moreno 2007 -2009/ 13993 0. 67** 0. 45** 2. 21 --- 2006 -2008/ 13742 0. 63** 0. 45** 1. 78** Dr. Sharma 1. 62** Dr. Kini Dr. Sharma 2005 -2007/ 13030 0. 64** Non-Emergency cases RAMR % **Interventionali All cases RAMR % 0. 49 st at MSH Red denotes first time ever in the New York State **Risk Adjusted Mortality Rate (RAMR) significantly lower then NY Statewide rate
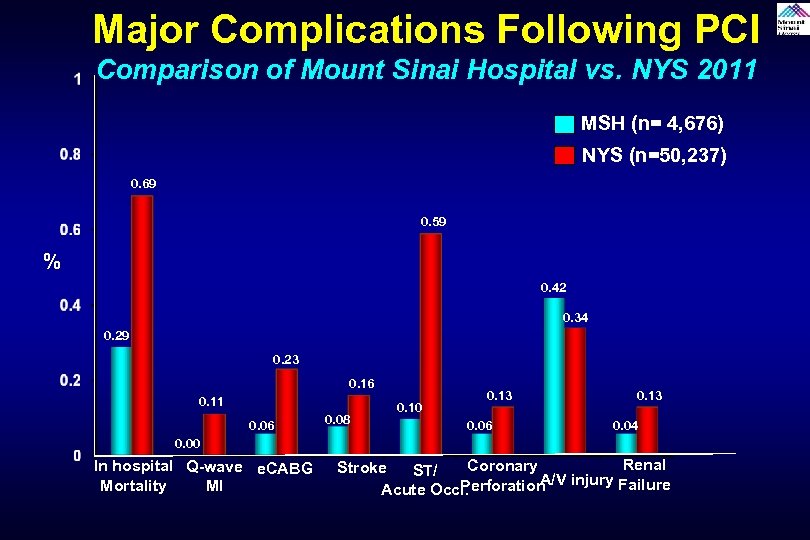 Major Complications Following PCI Comparison of Mount Sinai Hospital vs. NYS 2011 MSH (n= 4, 676) NYS (n=50, 237) 0. 69 0. 59 % 0. 42 0. 34 0. 29 0. 23 0. 16 0. 11 0. 06 0. 08 0. 10 0. 13 0. 06 0. 13 0. 04 0. 00 In hospital Q-wave e. CABG Mortality MI Renal Coronary Stroke ST/ A/V injury Failure Perforation Acute Occl.
Major Complications Following PCI Comparison of Mount Sinai Hospital vs. NYS 2011 MSH (n= 4, 676) NYS (n=50, 237) 0. 69 0. 59 % 0. 42 0. 34 0. 29 0. 23 0. 16 0. 11 0. 06 0. 08 0. 10 0. 13 0. 06 0. 13 0. 04 0. 00 In hospital Q-wave e. CABG Mortality MI Renal Coronary Stroke ST/ A/V injury Failure Perforation Acute Occl.
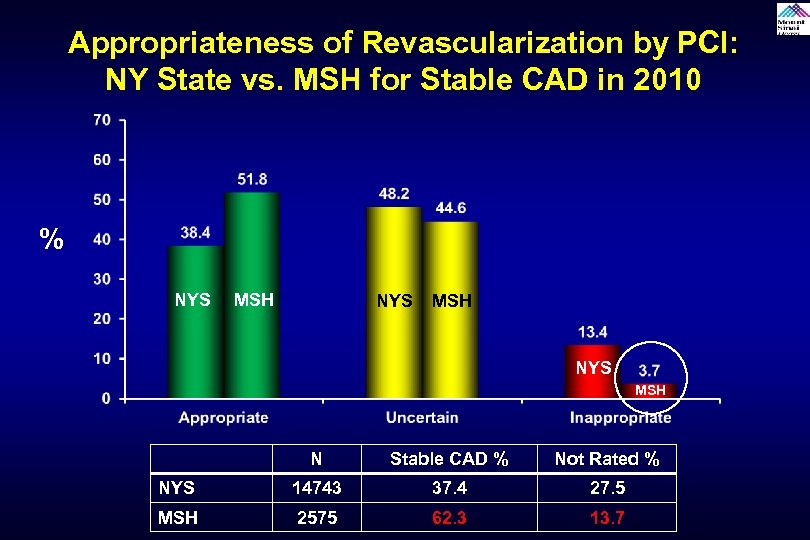 Appropriateness of Revascularization by PCI: NY State vs. MSH for Stable CAD in 2010 % NYS MSH N Stable CAD % Not Rated % NYS 14743 37. 4 27. 5 MSH 2575 62. 3 13. 7
Appropriateness of Revascularization by PCI: NY State vs. MSH for Stable CAD in 2010 % NYS MSH N Stable CAD % Not Rated % NYS 14743 37. 4 27. 5 MSH 2575 62. 3 13. 7
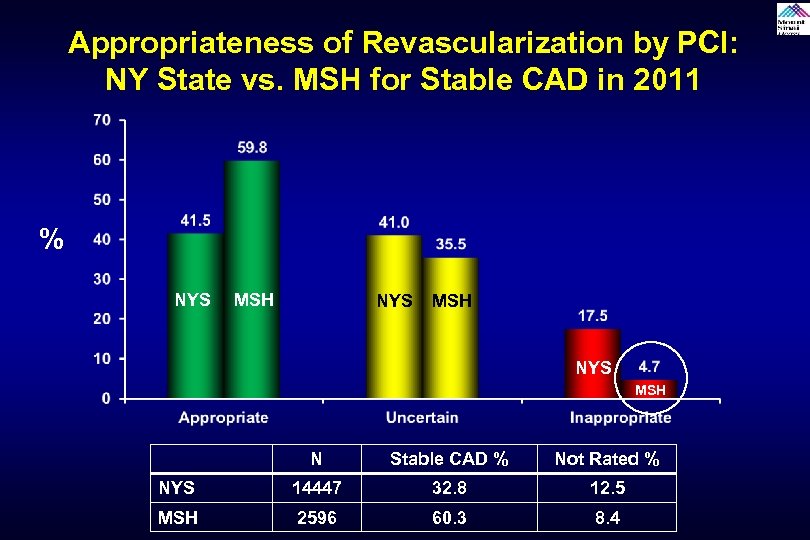 Appropriateness of Revascularization by PCI: NY State vs. MSH for Stable CAD in 2011 % NYS MSH N Stable CAD % Not Rated % NYS 14447 32. 8 12. 5 MSH 2596 60. 3 8. 4
Appropriateness of Revascularization by PCI: NY State vs. MSH for Stable CAD in 2011 % NYS MSH N Stable CAD % Not Rated % NYS 14447 32. 8 12. 5 MSH 2596 60. 3 8. 4
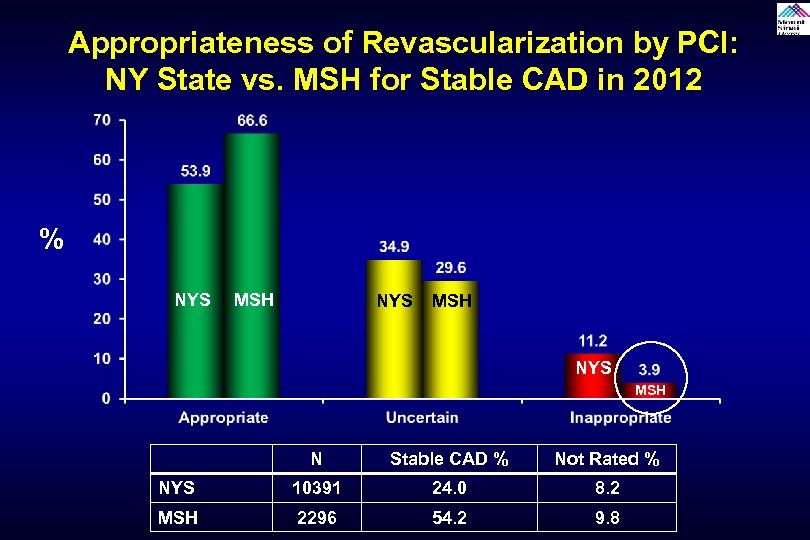 Appropriateness of Revascularization by PCI: NY State vs. MSH for Stable CAD in 2012 % NYS MSH N Stable CAD % Not Rated % NYS 10391 24. 0 8. 2 MSH 2296 54. 2 9. 8
Appropriateness of Revascularization by PCI: NY State vs. MSH for Stable CAD in 2012 % NYS MSH N Stable CAD % Not Rated % NYS 10391 24. 0 8. 2 MSH 2296 54. 2 9. 8
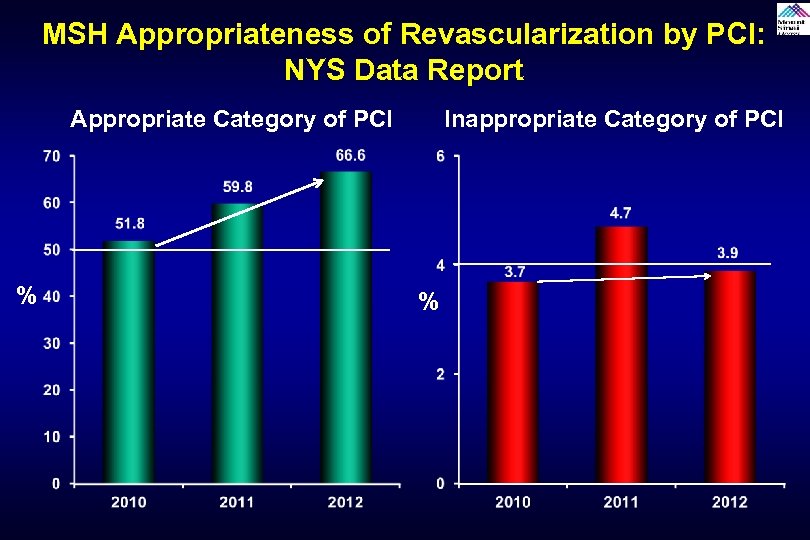 MSH Appropriateness of Revascularization by PCI: NYS Data Report Appropriate Category of PCI % Inappropriate Category of PCI %
MSH Appropriateness of Revascularization by PCI: NYS Data Report Appropriate Category of PCI % Inappropriate Category of PCI %
 Complex Coronary Cases Supported by: • Abbott Vascular • Boston Scientific Corp • Maquet Inc • CSI
Complex Coronary Cases Supported by: • Abbott Vascular • Boston Scientific Corp • Maquet Inc • CSI
 Disclosures Samin K. Sharma, MBBS, FACC Speaker’s Bureau – Boston Scientific Corporation, Abbott Vascular Inc, Angio. Score, DSI/Lilly Inc. , ABIOMED, CSI Annapoorna S. Kini, MBBS, FACC Nothing to disclose Sameer Mehta, MBBS, FACC Consulting Fees – The Medicines Company
Disclosures Samin K. Sharma, MBBS, FACC Speaker’s Bureau – Boston Scientific Corporation, Abbott Vascular Inc, Angio. Score, DSI/Lilly Inc. , ABIOMED, CSI Annapoorna S. Kini, MBBS, FACC Nothing to disclose Sameer Mehta, MBBS, FACC Consulting Fees – The Medicines Company
 July 15 th 2014 Case #61: MF, 86 yr M Presentation: Patient presented on July 7 th 2014 with cresendo angina, CCS class III and stress MPI + for moderate anterior and mild lateral ischemia with TID and LVEF 50%. A cardiac cath done @OSH revealed 90% calcific distal left main bifurcation CAD with patent prior stent sites in LAD and RCA. Echo revealed LVEF 50% and normal functioning aortic tilting disc prosthesis. Pt was referred to CT surgery but declined due to redo-CABG and old age. Pt continued to be symptomatic. Prior History: Hypertension, Hyperlipidemia, AAA, s/p mechanical AVR 1997 Medications: All once daily dosage Metoprolol XL 50 mg, Amlodipine 2. 5 mg, Amiodarone 200 mg, Dabigatran 150 mg, ASA 81 mg, Rosuvastatin 5 mg, Pantoprazole
July 15 th 2014 Case #61: MF, 86 yr M Presentation: Patient presented on July 7 th 2014 with cresendo angina, CCS class III and stress MPI + for moderate anterior and mild lateral ischemia with TID and LVEF 50%. A cardiac cath done @OSH revealed 90% calcific distal left main bifurcation CAD with patent prior stent sites in LAD and RCA. Echo revealed LVEF 50% and normal functioning aortic tilting disc prosthesis. Pt was referred to CT surgery but declined due to redo-CABG and old age. Pt continued to be symptomatic. Prior History: Hypertension, Hyperlipidemia, AAA, s/p mechanical AVR 1997 Medications: All once daily dosage Metoprolol XL 50 mg, Amlodipine 2. 5 mg, Amiodarone 200 mg, Dabigatran 150 mg, ASA 81 mg, Rosuvastatin 5 mg, Pantoprazole
 Case# 61: cont… SYNTAX Score: 19 Cardiac Cath 7/7/2014: Right Dominance LM CAD normal aortic tilting disc prosthesis RCA: mild diffuse disease with patent DES in mid LM: 80% calcific distal bifurcation LAD: 30% prox lesion with patent DES in prox-mid segment LCx: 50% calcific proximal lesion, distal mild diffuse disease Plan Today: - PCI of calcific distal LM bifurcation lesion using atherectomy (OA or RA) with possible IABP assist
Case# 61: cont… SYNTAX Score: 19 Cardiac Cath 7/7/2014: Right Dominance LM CAD normal aortic tilting disc prosthesis RCA: mild diffuse disease with patent DES in mid LM: 80% calcific distal bifurcation LAD: 30% prox lesion with patent DES in prox-mid segment LCx: 50% calcific proximal lesion, distal mild diffuse disease Plan Today: - PCI of calcific distal LM bifurcation lesion using atherectomy (OA or RA) with possible IABP assist
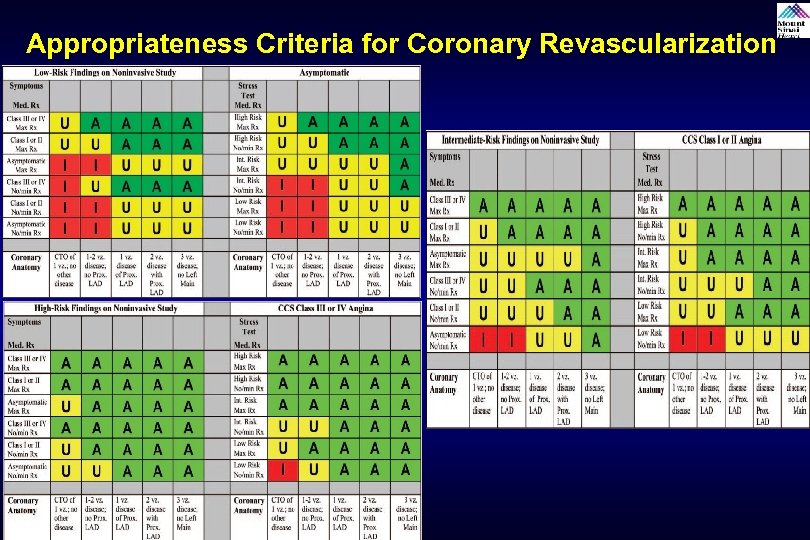 Appropriateness Criteria for Coronary Revascularization
Appropriateness Criteria for Coronary Revascularization
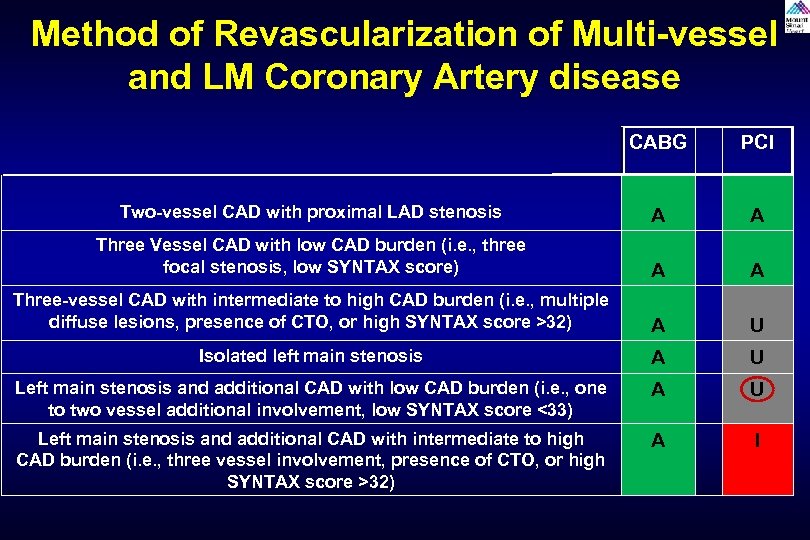 Method of Revascularization of Multi-vessel and LM Coronary Artery disease CABG PCI Two-vessel CAD with proximal LAD stenosis A A Three Vessel CAD with low CAD burden (i. e. , three focal stenosis, low SYNTAX score) A A Three-vessel CAD with intermediate to high CAD burden (i. e. , multiple diffuse lesions, presence of CTO, or high SYNTAX score >32) A U Isolated left main stenosis A U Left main stenosis and additional CAD with low CAD burden (i. e. , one to two vessel additional involvement, low SYNTAX score <33) A U Left main stenosis and additional CAD with intermediate to high CAD burden (i. e. , three vessel involvement, presence of CTO, or high SYNTAX score >32) A I
Method of Revascularization of Multi-vessel and LM Coronary Artery disease CABG PCI Two-vessel CAD with proximal LAD stenosis A A Three Vessel CAD with low CAD burden (i. e. , three focal stenosis, low SYNTAX score) A A Three-vessel CAD with intermediate to high CAD burden (i. e. , multiple diffuse lesions, presence of CTO, or high SYNTAX score >32) A U Isolated left main stenosis A U Left main stenosis and additional CAD with low CAD burden (i. e. , one to two vessel additional involvement, low SYNTAX score <33) A U Left main stenosis and additional CAD with intermediate to high CAD burden (i. e. , three vessel involvement, presence of CTO, or high SYNTAX score >32) A I
 Issues Involving The Case • Role of IVUS during PCI with DES • Update in ULM Revascularization
Issues Involving The Case • Role of IVUS during PCI with DES • Update in ULM Revascularization
 Issues Involving The Case • Role of IVUS during PCI with DES • Update in ULM Revascularization
Issues Involving The Case • Role of IVUS during PCI with DES • Update in ULM Revascularization

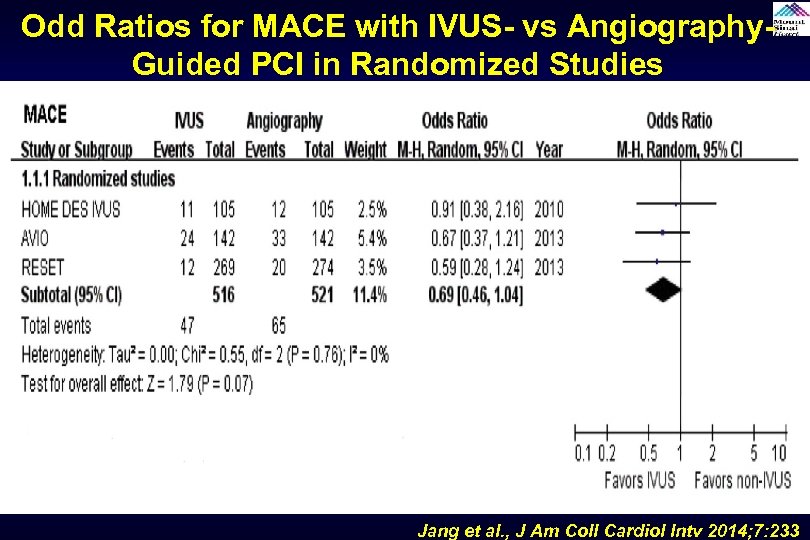 Odd Ratios for MACE with IVUS- vs Angiography. Guided PCI in Randomized Studies Jang et al. , J Am Coll Cardiol Intv 2014; 7: 233
Odd Ratios for MACE with IVUS- vs Angiography. Guided PCI in Randomized Studies Jang et al. , J Am Coll Cardiol Intv 2014; 7: 233
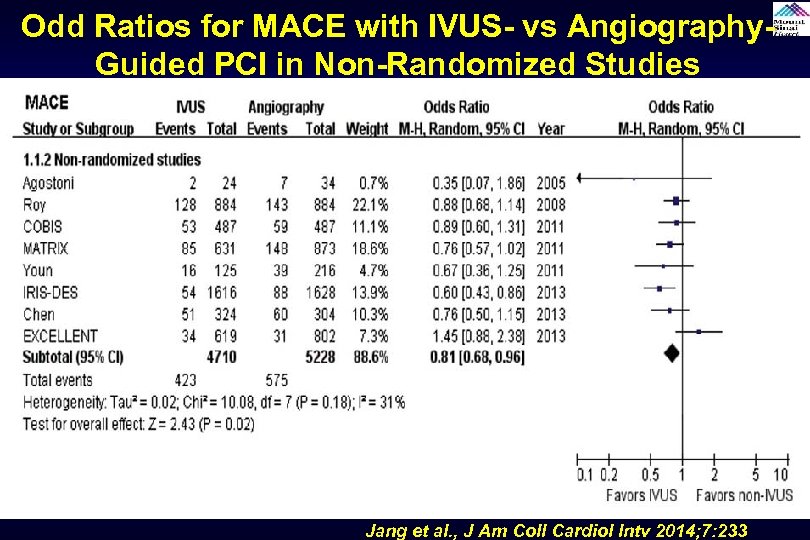 Odd Ratios for MACE with IVUS- vs Angiography. Guided PCI in Non-Randomized Studies Jang et al. , J Am Coll Cardiol Intv 2014; 7: 233
Odd Ratios for MACE with IVUS- vs Angiography. Guided PCI in Non-Randomized Studies Jang et al. , J Am Coll Cardiol Intv 2014; 7: 233
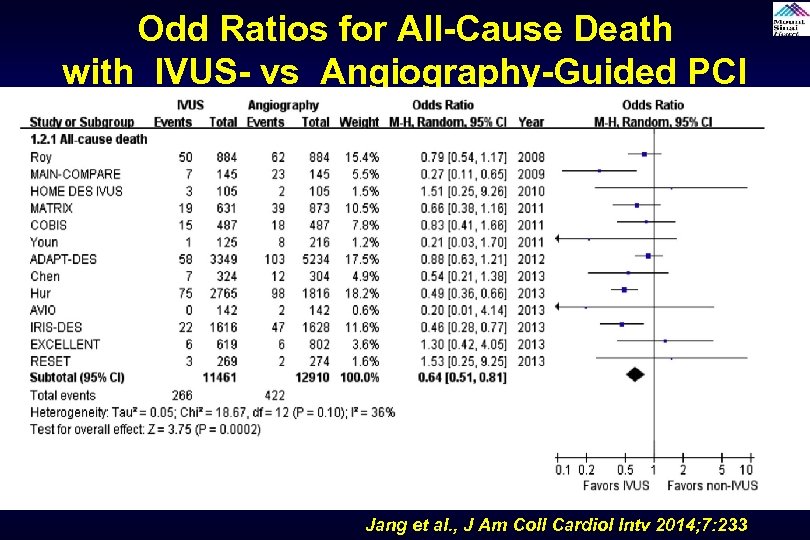 Odd Ratios for All-Cause Death with IVUS- vs Angiography-Guided PCI Jang et al. , J Am Coll Cardiol Intv 2014; 7: 233
Odd Ratios for All-Cause Death with IVUS- vs Angiography-Guided PCI Jang et al. , J Am Coll Cardiol Intv 2014; 7: 233
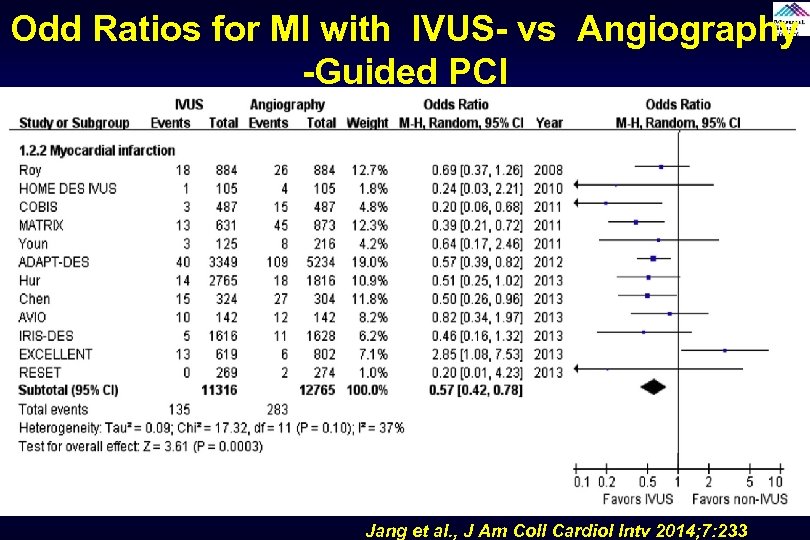 Odd Ratios for MI with IVUS- vs Angiography -Guided PCI Jang et al. , J Am Coll Cardiol Intv 2014; 7: 233
Odd Ratios for MI with IVUS- vs Angiography -Guided PCI Jang et al. , J Am Coll Cardiol Intv 2014; 7: 233
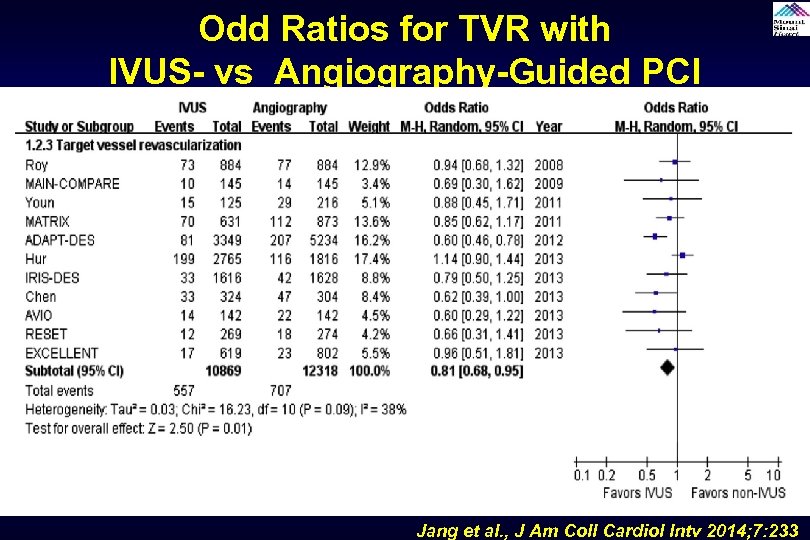 Odd Ratios for TVR with IVUS- vs Angiography-Guided PCI Jang et al. , J Am Coll Cardiol Intv 2014; 7: 233
Odd Ratios for TVR with IVUS- vs Angiography-Guided PCI Jang et al. , J Am Coll Cardiol Intv 2014; 7: 233
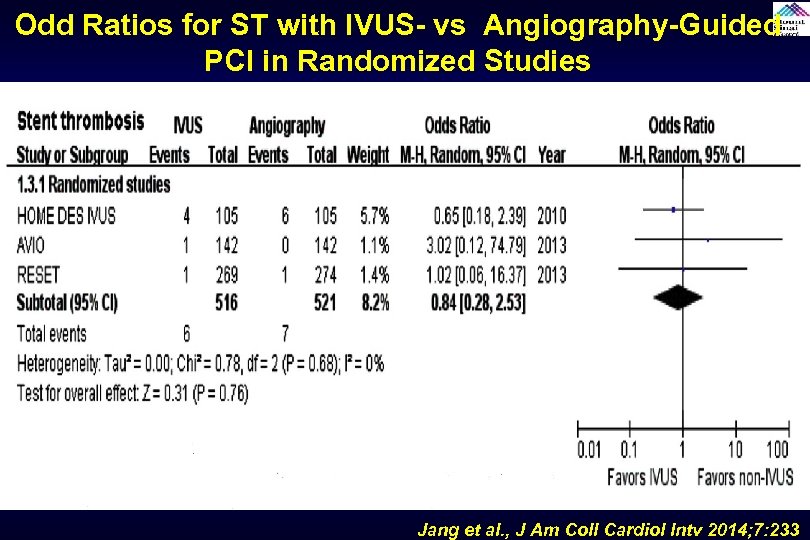 Odd Ratios for ST with IVUS- vs Angiography-Guided PCI in Randomized Studies Jang et al. , J Am Coll Cardiol Intv 2014; 7: 233
Odd Ratios for ST with IVUS- vs Angiography-Guided PCI in Randomized Studies Jang et al. , J Am Coll Cardiol Intv 2014; 7: 233
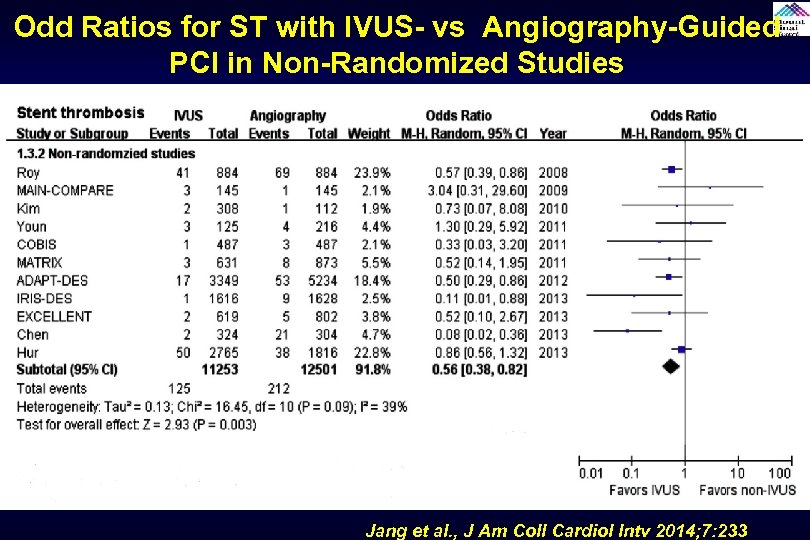 Odd Ratios for ST with IVUS- vs Angiography-Guided PCI in Non-Randomized Studies Jang et al. , J Am Coll Cardiol Intv 2014; 7: 233
Odd Ratios for ST with IVUS- vs Angiography-Guided PCI in Non-Randomized Studies Jang et al. , J Am Coll Cardiol Intv 2014; 7: 233
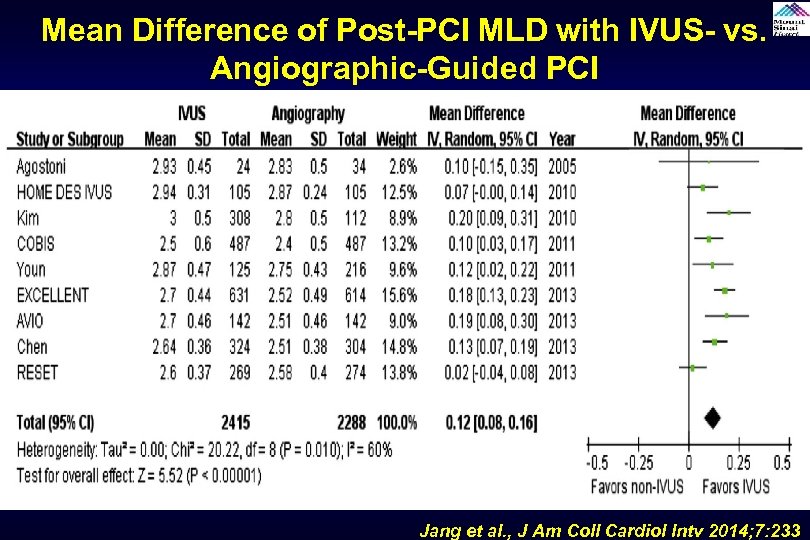 Mean Difference of Post-PCI MLD with IVUS- vs. Angiographic-Guided PCI Jang et al. , J Am Coll Cardiol Intv 2014; 7: 233
Mean Difference of Post-PCI MLD with IVUS- vs. Angiographic-Guided PCI Jang et al. , J Am Coll Cardiol Intv 2014; 7: 233
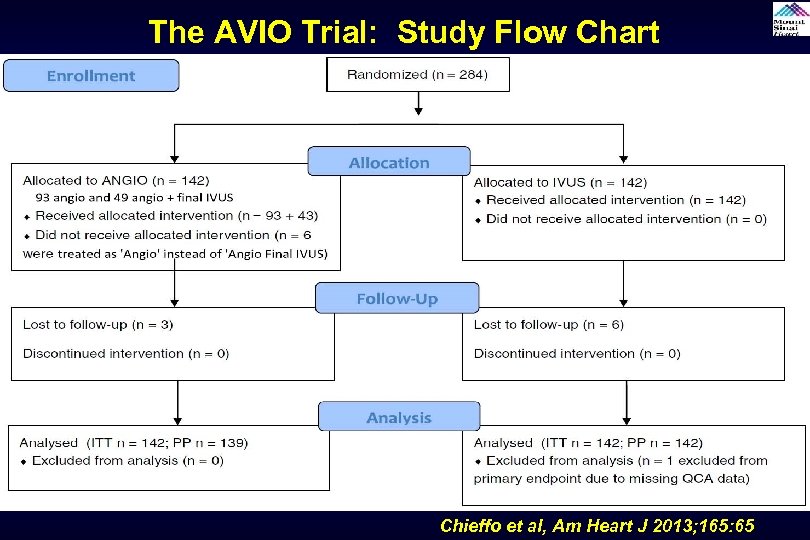 The AVIO Trial: Study Flow Chart Chieffo et al, Am Heart J 2013; 165: 65
The AVIO Trial: Study Flow Chart Chieffo et al, Am Heart J 2013; 165: 65
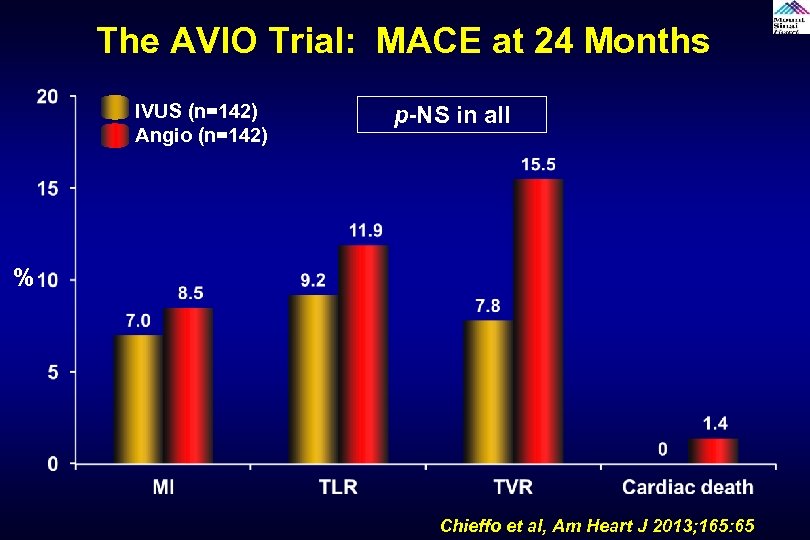 The AVIO Trial: MACE at 24 Months IVUS (n=142) Angio (n=142) p-NS in all % Chieffo et al, Am Heart J 2013; 165: 65
The AVIO Trial: MACE at 24 Months IVUS (n=142) Angio (n=142) p-NS in all % Chieffo et al, Am Heart J 2013; 165: 65

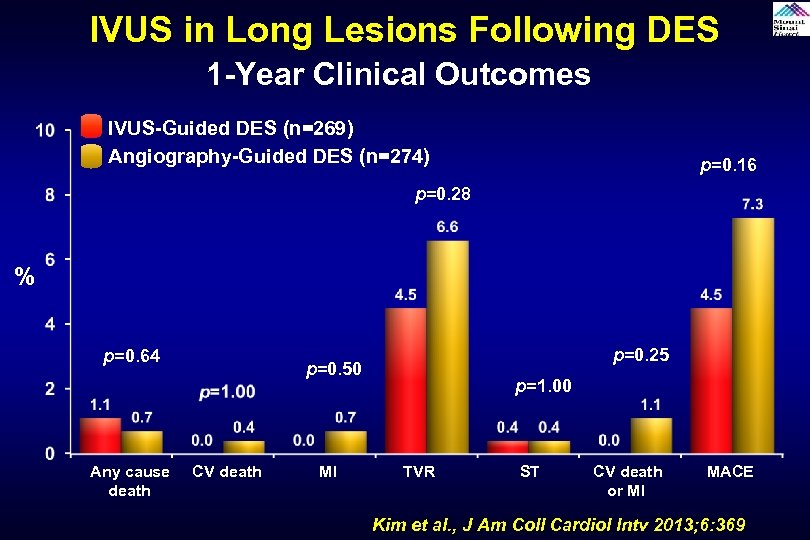 IVUS in Long Lesions Following DES 1 -Year Clinical Outcomes IVUS-Guided DES (n=269) Angiography-Guided DES (n=274) p=0. 16 p=0. 28 % p=0. 64 Any cause death p=0. 25 p=0. 50 CV death MI p=1. 00 TVR ST CV death or MI MACE Kim et al. , J Am Coll Cardiol Intv 2013; 6: 369
IVUS in Long Lesions Following DES 1 -Year Clinical Outcomes IVUS-Guided DES (n=269) Angiography-Guided DES (n=274) p=0. 16 p=0. 28 % p=0. 64 Any cause death p=0. 25 p=0. 50 CV death MI p=1. 00 TVR ST CV death or MI MACE Kim et al. , J Am Coll Cardiol Intv 2013; 6: 369

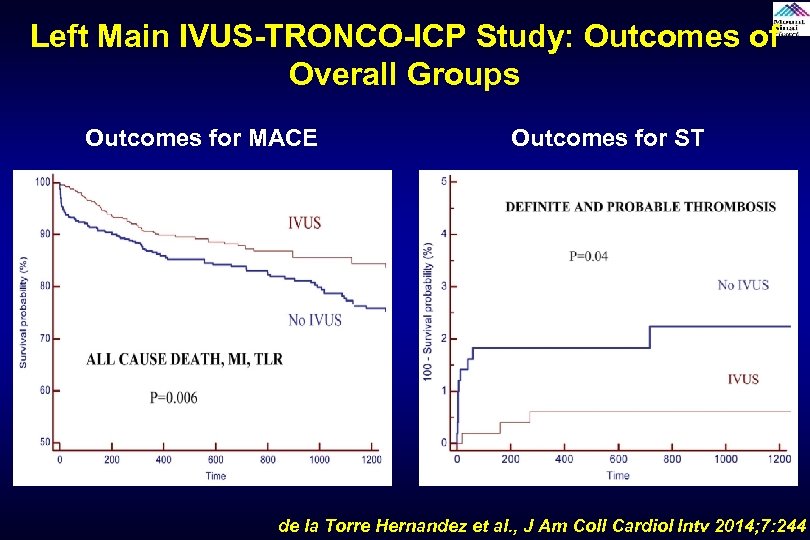 Left Main IVUS-TRONCO-ICP Study: Outcomes of Overall Groups Outcomes for MACE Outcomes for ST de la Torre Hernandez et al. , J Am Coll Cardiol Intv 2014; 7: 244
Left Main IVUS-TRONCO-ICP Study: Outcomes of Overall Groups Outcomes for MACE Outcomes for ST de la Torre Hernandez et al. , J Am Coll Cardiol Intv 2014; 7: 244
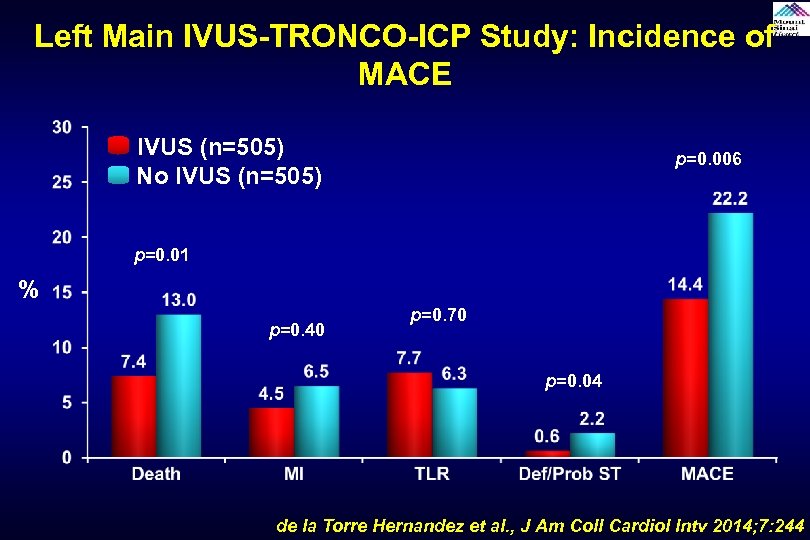 Left Main IVUS-TRONCO-ICP Study: Incidence of MACE IVUS (n=505) No IVUS (n=505) p=0. 006 p=0. 01 % p=0. 40 p=0. 70 p=0. 04 de la Torre Hernandez et al. , J Am Coll Cardiol Intv 2014; 7: 244
Left Main IVUS-TRONCO-ICP Study: Incidence of MACE IVUS (n=505) No IVUS (n=505) p=0. 006 p=0. 01 % p=0. 40 p=0. 70 p=0. 04 de la Torre Hernandez et al. , J Am Coll Cardiol Intv 2014; 7: 244
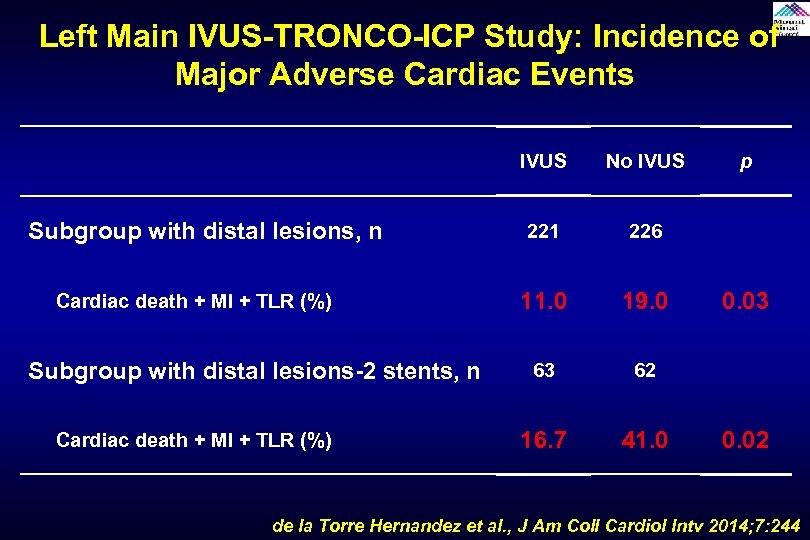 Left Main IVUS-TRONCO-ICP Study: Incidence of Major Adverse Cardiac Events IVUS Subgroup with distal lesions, n Cardiac death + MI + TLR (%) Subgroup with distal lesions-2 stents, n Cardiac death + MI + TLR (%) No IVUS 221 226 11. 0 19. 0 63 62 16. 7 41. 0 p 0. 03 0. 02 de la Torre Hernandez et al. , J Am Coll Cardiol Intv 2014; 7: 244
Left Main IVUS-TRONCO-ICP Study: Incidence of Major Adverse Cardiac Events IVUS Subgroup with distal lesions, n Cardiac death + MI + TLR (%) Subgroup with distal lesions-2 stents, n Cardiac death + MI + TLR (%) No IVUS 221 226 11. 0 19. 0 63 62 16. 7 41. 0 p 0. 03 0. 02 de la Torre Hernandez et al. , J Am Coll Cardiol Intv 2014; 7: 244
 Issues Involving The Case • Role of IVUS during PCI with DES • Update in ULM Revascularization
Issues Involving The Case • Role of IVUS during PCI with DES • Update in ULM Revascularization
 LMCA Stenosis Location X About two third of LMCA 66% Lesions include distal Bifurcation rd LC LMCA D LA 26% 8% Ostium Body-Shaft bifurcation; 1/3 are ostial/shaft lesions
LMCA Stenosis Location X About two third of LMCA 66% Lesions include distal Bifurcation rd LC LMCA D LA 26% 8% Ostium Body-Shaft bifurcation; 1/3 are ostial/shaft lesions
 PCI (1 st Gen DES) vs. CABG for LM Disease Meta-Analysis of 4 RCTs (N=1, 611) 1 -Year Outcomes PCI Death 3. 0% MI Stroke OR (95%CI) CABG OR (95%CI) p-Value 4. 1% 0. 74 (0. 43 -1. 28) 0. 29 2. 8% 2. 9% 0. 98 (0. 54 -1. 78) 0. 95 0. 1% 1. 7% 0. 15 (0. 03 -0. 67) 0. 01 Death, MI, or stroke 5. 3% 6. 8% 0. 77 (0. 48 -1. 22) 0. 26 Repeat Revasc 11. 4% 5. 4% 2. 25 (1. 54 -3. 28) <0. 001 MACCE 14. 5% 11. 8% 1. 28 (0. 95 -1. 72) 0. 01 0. 1 Favors PCI 1 10 0. 11 100 Favors CABG Capodanno et al. J Am Coll Cardiol 2011; 58: 14262
PCI (1 st Gen DES) vs. CABG for LM Disease Meta-Analysis of 4 RCTs (N=1, 611) 1 -Year Outcomes PCI Death 3. 0% MI Stroke OR (95%CI) CABG OR (95%CI) p-Value 4. 1% 0. 74 (0. 43 -1. 28) 0. 29 2. 8% 2. 9% 0. 98 (0. 54 -1. 78) 0. 95 0. 1% 1. 7% 0. 15 (0. 03 -0. 67) 0. 01 Death, MI, or stroke 5. 3% 6. 8% 0. 77 (0. 48 -1. 22) 0. 26 Repeat Revasc 11. 4% 5. 4% 2. 25 (1. 54 -3. 28) <0. 001 MACCE 14. 5% 11. 8% 1. 28 (0. 95 -1. 72) 0. 01 0. 1 Favors PCI 1 10 0. 11 100 Favors CABG Capodanno et al. J Am Coll Cardiol 2011; 58: 14262
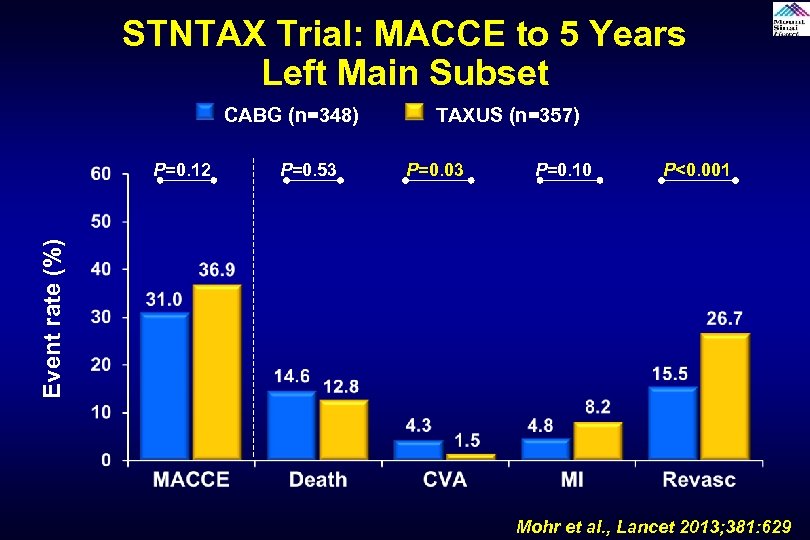 STNTAX Trial: MACCE to 5 Years Left Main Subset CABG (n=348) P=0. 53 P=0. 03 P=0. 10 P<0. 001 Event rate (%) P=0. 12 TAXUS (n=357) Mohr et al. , Lancet 2013; 381: 629
STNTAX Trial: MACCE to 5 Years Left Main Subset CABG (n=348) P=0. 53 P=0. 03 P=0. 10 P<0. 001 Event rate (%) P=0. 12 TAXUS (n=357) Mohr et al. , Lancet 2013; 381: 629
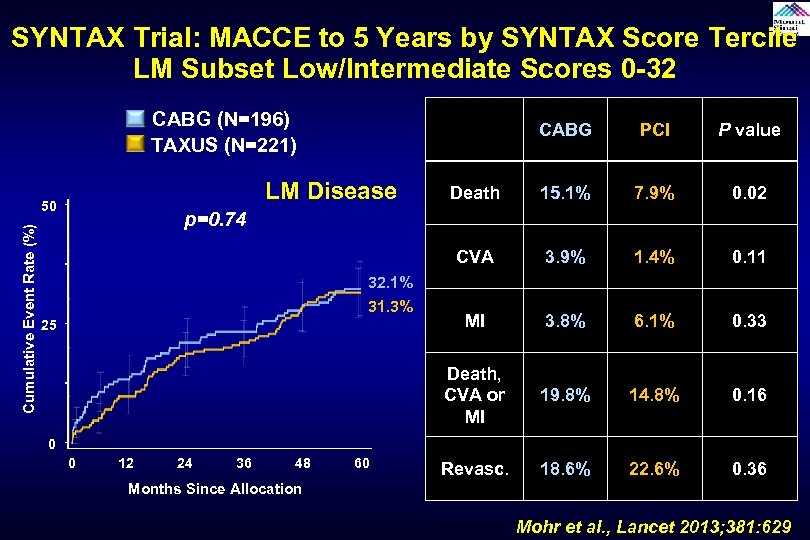 SYNTAX Trial: MACCE to 5 Years by SYNTAX Score Tercile LM Subset Low/Intermediate Scores 0 -32 CABG (N=196) TAXUS (N=221) PCI P value Death 15. 1% 7. 9% 0. 02 CVA 3. 9% 1. 4% 0. 11 MI 3. 8% 6. 1% 0. 33 Death, CVA or MI LM Disease 50 Cumulative Event Rate (%) CABG 19. 8% 14. 8% 0. 16 Revasc. 18. 6% 22. 6% 0. 36 p=0. 74 32. 1% 31. 3% 25 0 0 12 24 36 48 60 Months Since Allocation Mohr et al. , Lancet 2013; 381: 629
SYNTAX Trial: MACCE to 5 Years by SYNTAX Score Tercile LM Subset Low/Intermediate Scores 0 -32 CABG (N=196) TAXUS (N=221) PCI P value Death 15. 1% 7. 9% 0. 02 CVA 3. 9% 1. 4% 0. 11 MI 3. 8% 6. 1% 0. 33 Death, CVA or MI LM Disease 50 Cumulative Event Rate (%) CABG 19. 8% 14. 8% 0. 16 Revasc. 18. 6% 22. 6% 0. 36 p=0. 74 32. 1% 31. 3% 25 0 0 12 24 36 48 60 Months Since Allocation Mohr et al. , Lancet 2013; 381: 629
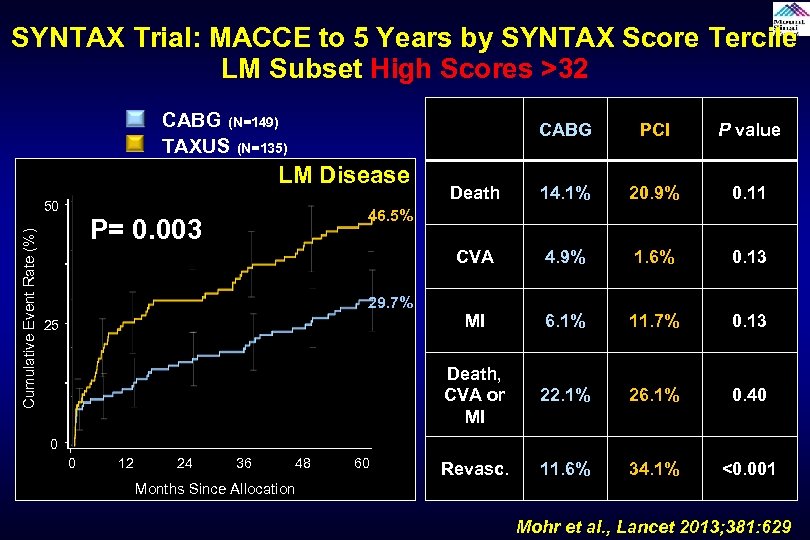 SYNTAX Trial: MACCE to 5 Years by SYNTAX Score Tercile LM Subset High Scores >32 CABG (N=149) TAXUS (N=135) CABG Cumulative Event Rate (%) Death 14. 1% 20. 9% 0. 11 4. 9% 1. 6% 0. 13 MI 6. 1% 11. 7% 0. 13 Death, CVA or MI 50 P value CVA LM Disease PCI 22. 1% 26. 1% 0. 40 Revasc. 11. 6% 34. 1% <0. 001 46. 5% P= 0. 003 29. 7% 25 0 0 12 24 36 48 60 Months Since Allocation Mohr et al. , Lancet 2013; 381: 629
SYNTAX Trial: MACCE to 5 Years by SYNTAX Score Tercile LM Subset High Scores >32 CABG (N=149) TAXUS (N=135) CABG Cumulative Event Rate (%) Death 14. 1% 20. 9% 0. 11 4. 9% 1. 6% 0. 13 MI 6. 1% 11. 7% 0. 13 Death, CVA or MI 50 P value CVA LM Disease PCI 22. 1% 26. 1% 0. 40 Revasc. 11. 6% 34. 1% <0. 001 46. 5% P= 0. 003 29. 7% 25 0 0 12 24 36 48 60 Months Since Allocation Mohr et al. , Lancet 2013; 381: 629

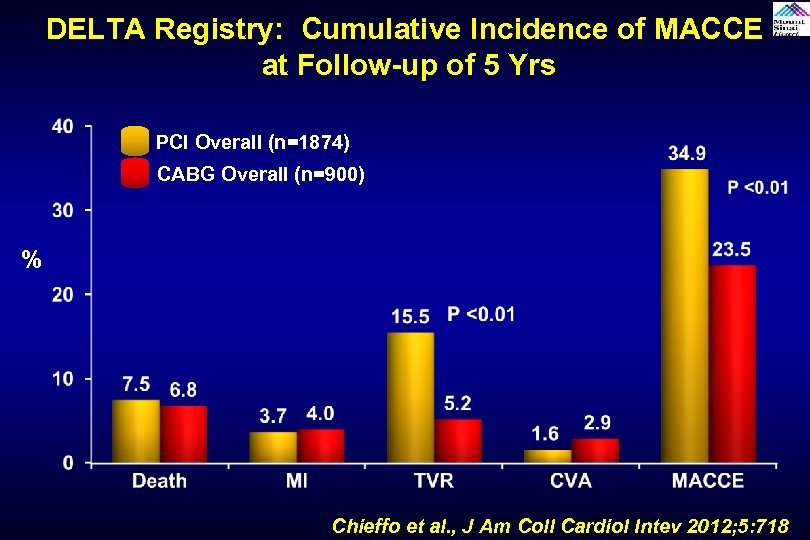 DELTA Registry: Cumulative Incidence of MACCE at Follow-up of 5 Yrs PCI Overall (n=1874) CABG Overall (n=900) % Chieffo et al. , J Am Coll Cardiol Intev 2012; 5: 718
DELTA Registry: Cumulative Incidence of MACCE at Follow-up of 5 Yrs PCI Overall (n=1874) CABG Overall (n=900) % Chieffo et al. , J Am Coll Cardiol Intev 2012; 5: 718
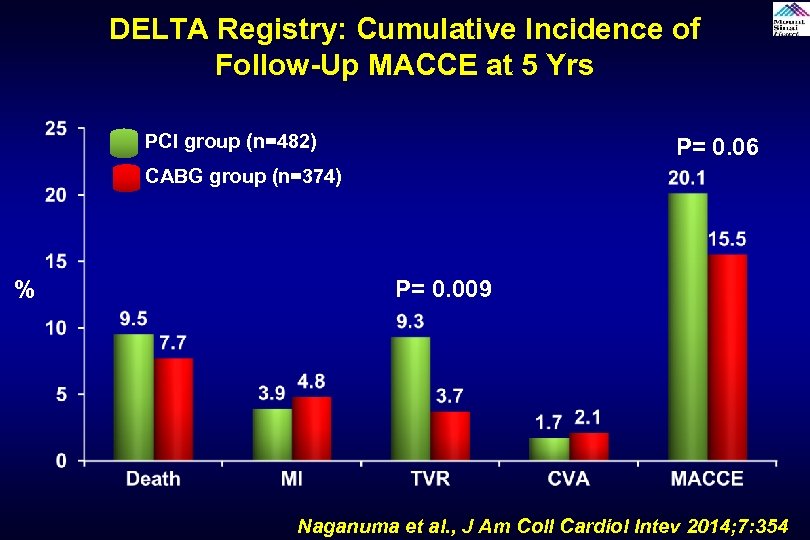 DELTA Registry: Cumulative Incidence of Follow-Up MACCE at 5 Yrs PCI group (n=482) P= 0. 06 CABG group (n=374) % P= 0. 009 Naganuma et al. , J Am Coll Cardiol Intev 2014; 7: 354
DELTA Registry: Cumulative Incidence of Follow-Up MACCE at 5 Yrs PCI group (n=482) P= 0. 06 CABG group (n=374) % P= 0. 009 Naganuma et al. , J Am Coll Cardiol Intev 2014; 7: 354
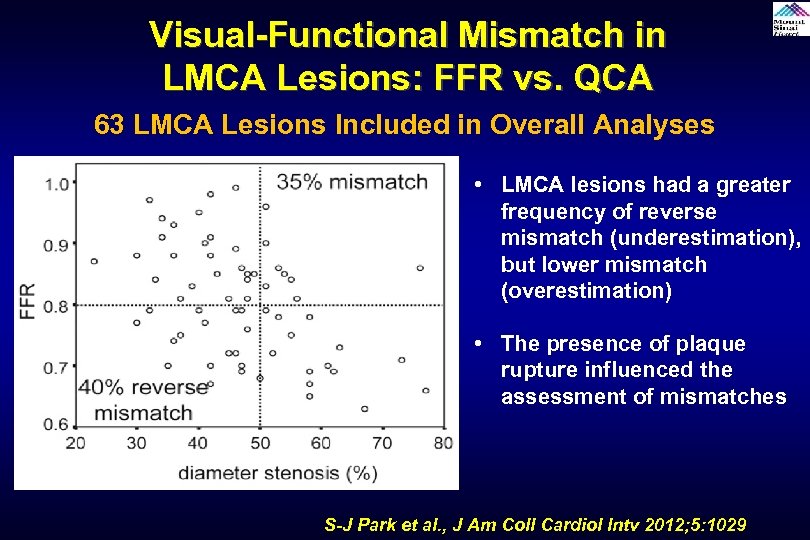 Visual-Functional Mismatch in LMCA Lesions: FFR vs. QCA 63 LMCA Lesions Included in Overall Analyses • LMCA lesions had a greater frequency of reverse mismatch (underestimation), but lower mismatch (overestimation) • The presence of plaque rupture influenced the assessment of mismatches S-J Park et al. , J Am Coll Cardiol Intv 2012; 5: 1029
Visual-Functional Mismatch in LMCA Lesions: FFR vs. QCA 63 LMCA Lesions Included in Overall Analyses • LMCA lesions had a greater frequency of reverse mismatch (underestimation), but lower mismatch (overestimation) • The presence of plaque rupture influenced the assessment of mismatches S-J Park et al. , J Am Coll Cardiol Intv 2012; 5: 1029
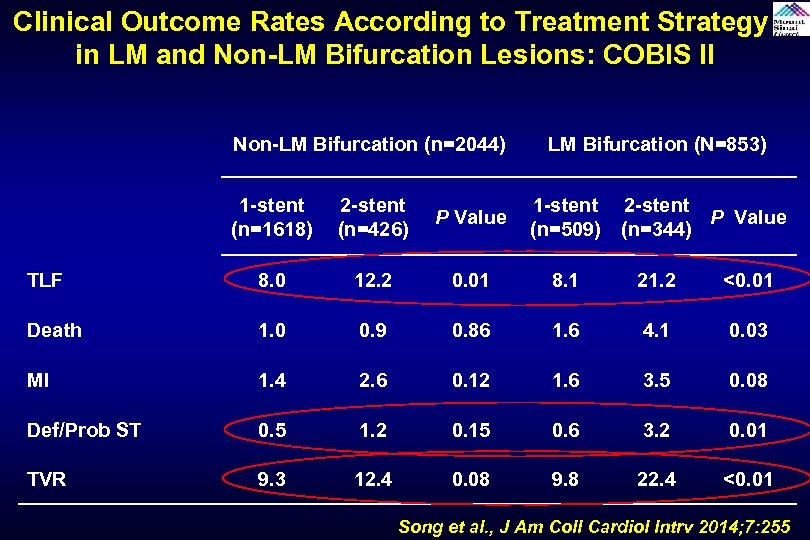 Clinical Outcome Rates According to Treatment Strategy in LM and Non-LM Bifurcation Lesions: COBIS II Non-LM Bifurcation (n=2044) LM Bifurcation (N=853) 1 -stent (n=1618) 2 -stent (n=426) P Value 1 -stent (n=509) 2 -stent P Value (n=344) TLF 8. 0 12. 2 0. 01 8. 1 21. 2 <0. 01 Death 1. 0 0. 9 0. 86 1. 6 4. 1 0. 03 MI 1. 4 2. 6 0. 12 1. 6 3. 5 0. 08 Def/Prob ST 0. 5 1. 2 0. 15 0. 6 3. 2 0. 01 TVR 9. 3 12. 4 0. 08 9. 8 22. 4 <0. 01 Song et al. , J Am Coll Cardiol Intrv 2014; 7: 255
Clinical Outcome Rates According to Treatment Strategy in LM and Non-LM Bifurcation Lesions: COBIS II Non-LM Bifurcation (n=2044) LM Bifurcation (N=853) 1 -stent (n=1618) 2 -stent (n=426) P Value 1 -stent (n=509) 2 -stent P Value (n=344) TLF 8. 0 12. 2 0. 01 8. 1 21. 2 <0. 01 Death 1. 0 0. 9 0. 86 1. 6 4. 1 0. 03 MI 1. 4 2. 6 0. 12 1. 6 3. 5 0. 08 Def/Prob ST 0. 5 1. 2 0. 15 0. 6 3. 2 0. 01 TVR 9. 3 12. 4 0. 08 9. 8 22. 4 <0. 01 Song et al. , J Am Coll Cardiol Intrv 2014; 7: 255
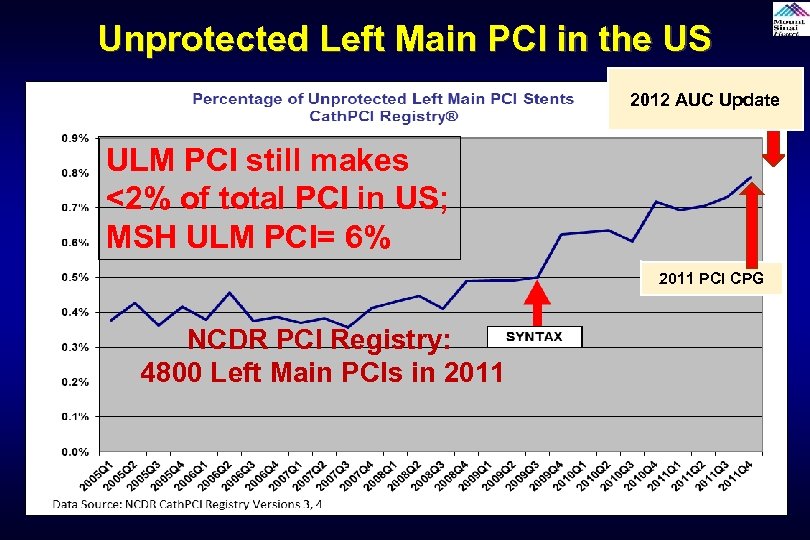 Unprotected Left Main PCI in the US 2012 AUC Update ULM PCI still makes <2% of total PCI in US; MSH ULM PCI= 6% 2011 PCI CPG NCDR PCI Registry: 4800 Left Main PCIs in 2011
Unprotected Left Main PCI in the US 2012 AUC Update ULM PCI still makes <2% of total PCI in US; MSH ULM PCI= 6% 2011 PCI CPG NCDR PCI Registry: 4800 Left Main PCIs in 2011
 Steps to Improve Left Main PCI Outcomes ¡ ¡ Use best DES Optimal pharmacotherapy • 2 nd and 3 rd Generation DES ¡ ¡ IVUS/FFR to assess intermediate LM lesion ¡ FFR to avoid unnecessary stenting ¡ IVUS guided LM stenting Thienopyridine pre-loading; PRU Statin pre-loading Bivalirudin anticoagulation ¡ IVUS for LM Bifurcation FFR for isolated lesion ¡ Especially of Side Branch ¡ ¡ Especially in LM bifurcation/ 2 stents ¡ One DES use; avoid 2 -stents Lesion preparation; Debulking Hemodynamic support; Impella Staging additional lesions ? Angiographic F/U in complex LM ¡ ¡ Optimal LM stent technique ¡ ¡ ¡
Steps to Improve Left Main PCI Outcomes ¡ ¡ Use best DES Optimal pharmacotherapy • 2 nd and 3 rd Generation DES ¡ ¡ IVUS/FFR to assess intermediate LM lesion ¡ FFR to avoid unnecessary stenting ¡ IVUS guided LM stenting Thienopyridine pre-loading; PRU Statin pre-loading Bivalirudin anticoagulation ¡ IVUS for LM Bifurcation FFR for isolated lesion ¡ Especially of Side Branch ¡ ¡ Especially in LM bifurcation/ 2 stents ¡ One DES use; avoid 2 -stents Lesion preparation; Debulking Hemodynamic support; Impella Staging additional lesions ? Angiographic F/U in complex LM ¡ ¡ Optimal LM stent technique ¡ ¡ ¡
 EXCEL Trial (Evaluation of Xience Prime vs. CABG for Examination of LM Disease) LM disease (± 1, 2 or 3 vessel disease) and SYNTAX score of ≤ 32 Randomize 2600 pts Trial finished enrollment after 1800 cases ABBOTT Vascular XIENCE Prime stent CABG • The primary endpoint is the composite incidence of death, large MI or stroke at a median FU duration of 3 years, powered for sequential non-inferiority and superiority testing. • The major secondary endpoint is the composite incidence of death, MI, stroke or unplanned repeat revascularization. All patients will be followed for 5 years total.
EXCEL Trial (Evaluation of Xience Prime vs. CABG for Examination of LM Disease) LM disease (± 1, 2 or 3 vessel disease) and SYNTAX score of ≤ 32 Randomize 2600 pts Trial finished enrollment after 1800 cases ABBOTT Vascular XIENCE Prime stent CABG • The primary endpoint is the composite incidence of death, large MI or stroke at a median FU duration of 3 years, powered for sequential non-inferiority and superiority testing. • The major secondary endpoint is the composite incidence of death, MI, stroke or unplanned repeat revascularization. All patients will be followed for 5 years total.
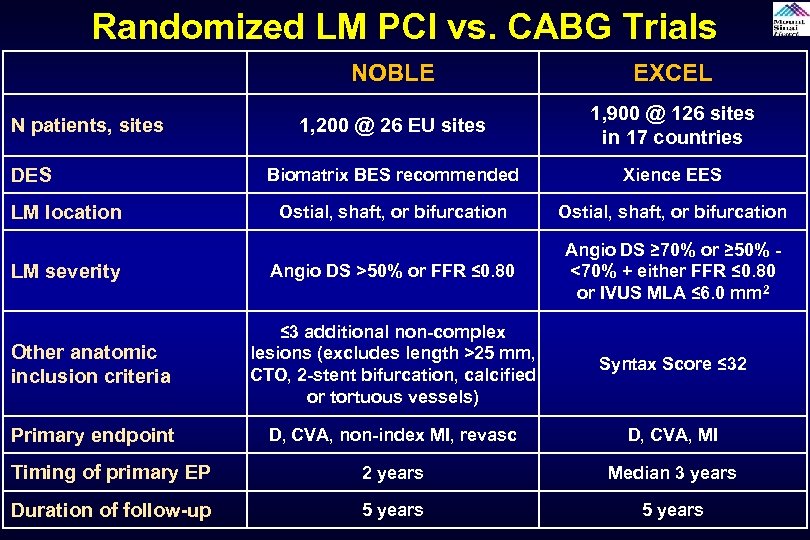 Randomized LM PCI vs. CABG Trials NOBLE EXCEL 1, 200 @ 26 EU sites 1, 900 @ 126 sites in 17 countries Biomatrix BES recommended Xience EES Ostial, shaft, or bifurcation Angio DS >50% or FFR ≤ 0. 80 Angio DS ≥ 70% or ≥ 50% <70% + either FFR ≤ 0. 80 or IVUS MLA ≤ 6. 0 mm 2 Other anatomic inclusion criteria ≤ 3 additional non-complex lesions (excludes length >25 mm, CTO, 2 -stent bifurcation, calcified or tortuous vessels) Syntax Score ≤ 32 Primary endpoint D, CVA, non-index MI, revasc D, CVA, MI Timing of primary EP 2 years Median 3 years Duration of follow-up 5 years N patients, sites DES LM location LM severity
Randomized LM PCI vs. CABG Trials NOBLE EXCEL 1, 200 @ 26 EU sites 1, 900 @ 126 sites in 17 countries Biomatrix BES recommended Xience EES Ostial, shaft, or bifurcation Angio DS >50% or FFR ≤ 0. 80 Angio DS ≥ 70% or ≥ 50% <70% + either FFR ≤ 0. 80 or IVUS MLA ≤ 6. 0 mm 2 Other anatomic inclusion criteria ≤ 3 additional non-complex lesions (excludes length >25 mm, CTO, 2 -stent bifurcation, calcified or tortuous vessels) Syntax Score ≤ 32 Primary endpoint D, CVA, non-index MI, revasc D, CVA, MI Timing of primary EP 2 years Median 3 years Duration of follow-up 5 years N patients, sites DES LM location LM severity
 CABG vs. PCI for Complex/LM CAD
CABG vs. PCI for Complex/LM CAD
 Take Home Message: Role of IVUS in DES PCI and Update in ULM PCI ü Contemporary randomized trials and registries of IVUS guided PCI has shown to have lower MACE rates including lower mortality, TVR (trend) and stent thrombosis. Benefit is more pronounced in distal LM lesions and with use of 2 stents ü Outcomes of ULM PCI in low-intermediate risk (SYNTAX score <32 ) have shown long-term outcomes to be similar to the CABG cohort while distal bifurcation lesions and high SYNTAX score (>32) pts have higher MACE rates and hence should undergo CABG. Heart Team discussion before proceeding for ULM revascularization should be routine.
Take Home Message: Role of IVUS in DES PCI and Update in ULM PCI ü Contemporary randomized trials and registries of IVUS guided PCI has shown to have lower MACE rates including lower mortality, TVR (trend) and stent thrombosis. Benefit is more pronounced in distal LM lesions and with use of 2 stents ü Outcomes of ULM PCI in low-intermediate risk (SYNTAX score <32 ) have shown long-term outcomes to be similar to the CABG cohort while distal bifurcation lesions and high SYNTAX score (>32) pts have higher MACE rates and hence should undergo CABG. Heart Team discussion before proceeding for ULM revascularization should be routine.
 Question # 1 Following is the false statements regarding use of IVUS during DES PCI: A. IVUS use is associated with higher dissections B. IVUS use is associated with higher MLD C. IVUS use is not associated with lower ST D. IVUS use is associated with lower mortality in ULM lesions E. A and C
Question # 1 Following is the false statements regarding use of IVUS during DES PCI: A. IVUS use is associated with higher dissections B. IVUS use is associated with higher MLD C. IVUS use is not associated with lower ST D. IVUS use is associated with lower mortality in ULM lesions E. A and C
 Question # 2 Following is the true statement of 5 year F/U of SYNTAX trial comparing TAXUS DES PCI to CABG for ULM in low-intermediate score (<33): A. PCI is associated with significantly higher CVA B. PCI is associated with significantly lower MI C. PCI is associated with significantly higher TVR D. PCI is associated with significantly lower Death E. None of the above
Question # 2 Following is the true statement of 5 year F/U of SYNTAX trial comparing TAXUS DES PCI to CABG for ULM in low-intermediate score (<33): A. PCI is associated with significantly higher CVA B. PCI is associated with significantly lower MI C. PCI is associated with significantly higher TVR D. PCI is associated with significantly lower Death E. None of the above
 Question # 3 COBIS II Registry of LM and non-LM bifurcation lesion analysis revealed the following true statement for LM bifurcation lesion PCI; A. 2 stent approach is associated with higher MI B. 2 stent approach is associated with higher death C. 2 stent approach is associated with higher MACE D. 2 stent approach is associated with higher ST E. All of the above
Question # 3 COBIS II Registry of LM and non-LM bifurcation lesion analysis revealed the following true statement for LM bifurcation lesion PCI; A. 2 stent approach is associated with higher MI B. 2 stent approach is associated with higher death C. 2 stent approach is associated with higher MACE D. 2 stent approach is associated with higher ST E. All of the above
 Question # 1 Following is the false statements regarding use of IVUS during DES PCI: A. IVUS use is associated with higher dissections B. IVUS use is associated with higher MLD C. IVUS use is not associated with lower ST D. IVUS use is associated with lower mortality in ULM lesions E. A and C The correct answer is E as all others are true Jang et al. , J Am Coll Cardiol Intv 2014; 7: 233
Question # 1 Following is the false statements regarding use of IVUS during DES PCI: A. IVUS use is associated with higher dissections B. IVUS use is associated with higher MLD C. IVUS use is not associated with lower ST D. IVUS use is associated with lower mortality in ULM lesions E. A and C The correct answer is E as all others are true Jang et al. , J Am Coll Cardiol Intv 2014; 7: 233
 Question # 2 Following is the true statement of 5 year F/U of SYNTAX trial comparing TAXUS DES PCI to CABG for ULM in low-intermediate score (<33): A. PCI is associated with significantly higher CVA B. PCI is associated with significantly lower MI C. PCI is associated with significantly higher TVR D. PCI is associated with significantly lower Death E. None of the above The correct answer is D as all others are not true Mohr et al. , Lancet 2013; 381: 629
Question # 2 Following is the true statement of 5 year F/U of SYNTAX trial comparing TAXUS DES PCI to CABG for ULM in low-intermediate score (<33): A. PCI is associated with significantly higher CVA B. PCI is associated with significantly lower MI C. PCI is associated with significantly higher TVR D. PCI is associated with significantly lower Death E. None of the above The correct answer is D as all others are not true Mohr et al. , Lancet 2013; 381: 629
 Question # 3 COBIS II Registry of LM and non-LM bifurcation lesion analysis revealed the following true statement for LM bifurcation lesion PCI; A. 2 stent approach is associated with higher MI B. 2 stent approach is associated with higher death C. 2 stent approach is associated with higher MACE D. 2 stent approach is associated with higher ST E. All of the above The correct answer is E as all are true Song et al. , J Am Coll Cardiol Intrv 2014; 7: 255
Question # 3 COBIS II Registry of LM and non-LM bifurcation lesion analysis revealed the following true statement for LM bifurcation lesion PCI; A. 2 stent approach is associated with higher MI B. 2 stent approach is associated with higher death C. 2 stent approach is associated with higher MACE D. 2 stent approach is associated with higher ST E. All of the above The correct answer is E as all are true Song et al. , J Am Coll Cardiol Intrv 2014; 7: 255


