8d9571bef80ed41152e63e47547656ba.ppt
- Количество слайдов: 72
 Nutrition Therapy in the ICU: The Clock is Ticking! Daren K. Heyland Professor of Medicine Queen’s University, Kingston General Hospital Kingston, ON Canada
Nutrition Therapy in the ICU: The Clock is Ticking! Daren K. Heyland Professor of Medicine Queen’s University, Kingston General Hospital Kingston, ON Canada
 Case Scenario • • Mr KT 76 per’d diverticulum Septic shock, ARDS, MODS Day 1 - high NG drainage, distended abdomen Day 3 - trickle feeds Feeds on and off again for whole first week No PN, no small bowel feeds, no specialized nutrients
Case Scenario • • Mr KT 76 per’d diverticulum Septic shock, ARDS, MODS Day 1 - high NG drainage, distended abdomen Day 3 - trickle feeds Feeds on and off again for whole first week No PN, no small bowel feeds, no specialized nutrients
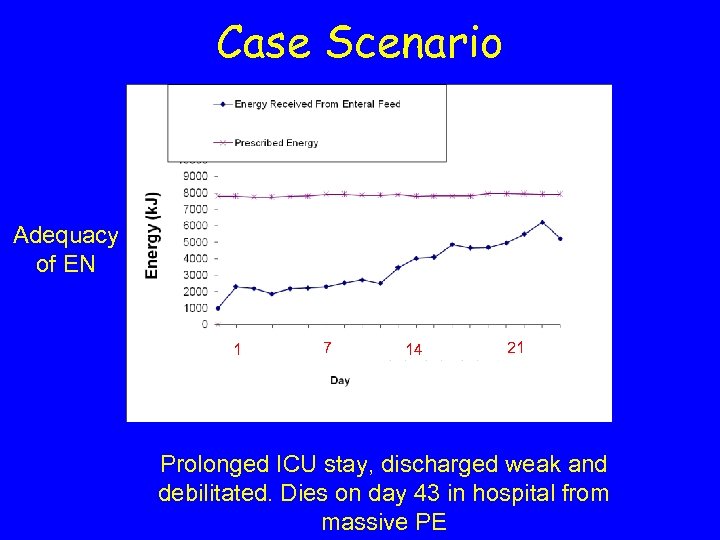 Case Scenario Adequacy of EN 1 7 14 21 Prolonged ICU stay, discharged weak and debilitated. Dies on day 43 in hospital from massive PE
Case Scenario Adequacy of EN 1 7 14 21 Prolonged ICU stay, discharged weak and debilitated. Dies on day 43 in hospital from massive PE
 To what extent did nutrition therapy (or lack thereof) play a role in this patient’s demise?
To what extent did nutrition therapy (or lack thereof) play a role in this patient’s demise?
 Conclusions (1) Nutrition is therapy that modulates the underlying disease process Adjunctive Supportive Care Proactive Primary Therapy
Conclusions (1) Nutrition is therapy that modulates the underlying disease process Adjunctive Supportive Care Proactive Primary Therapy
 Conclusions (2) Nutrition therapy impacts clinical outcomes Adjunctive Supportive Care Proactive Primary Therapy
Conclusions (2) Nutrition therapy impacts clinical outcomes Adjunctive Supportive Care Proactive Primary Therapy
 Conclusions (3) Timeliness of administration of nutrition therapy matters! Adjunctive Supportive Care Proactive Primary Therapy
Conclusions (3) Timeliness of administration of nutrition therapy matters! Adjunctive Supportive Care Proactive Primary Therapy
 Conclusions (4) Quantity of nutrition therapy matters! Adjunctive Supportive Care Proactive Primary Therapy
Conclusions (4) Quantity of nutrition therapy matters! Adjunctive Supportive Care Proactive Primary Therapy
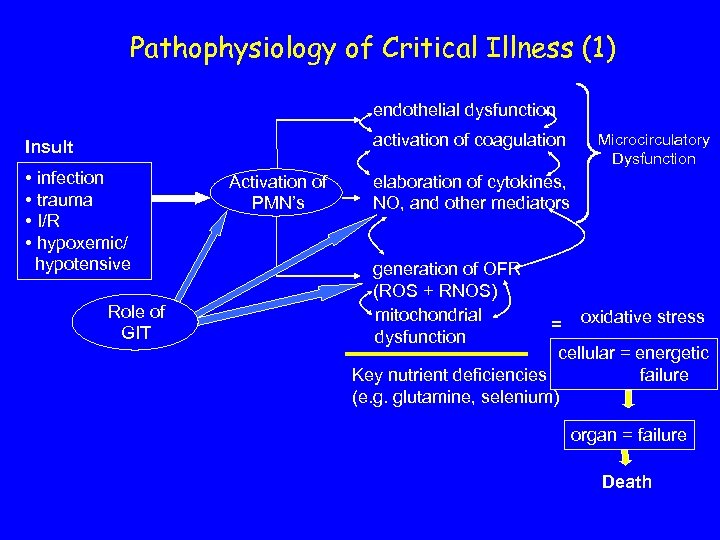 Pathophysiology of Critical Illness (1) endothelial dysfunction activation of coagulation Insult • infection • trauma • I/R • hypoxemic/ hypotensive Role of GIT Activation of PMN’s Microcirculatory Dysfunction elaboration of cytokines, NO, and other mediators generation of OFR (ROS + RNOS) mitochondrial dysfunction = oxidative stress cellular = energetic failure Key nutrient deficiencies (e. g. glutamine, selenium) organ = failure Death
Pathophysiology of Critical Illness (1) endothelial dysfunction activation of coagulation Insult • infection • trauma • I/R • hypoxemic/ hypotensive Role of GIT Activation of PMN’s Microcirculatory Dysfunction elaboration of cytokines, NO, and other mediators generation of OFR (ROS + RNOS) mitochondrial dysfunction = oxidative stress cellular = energetic failure Key nutrient deficiencies (e. g. glutamine, selenium) organ = failure Death
 Arginine-supplemented diets?
Arginine-supplemented diets?
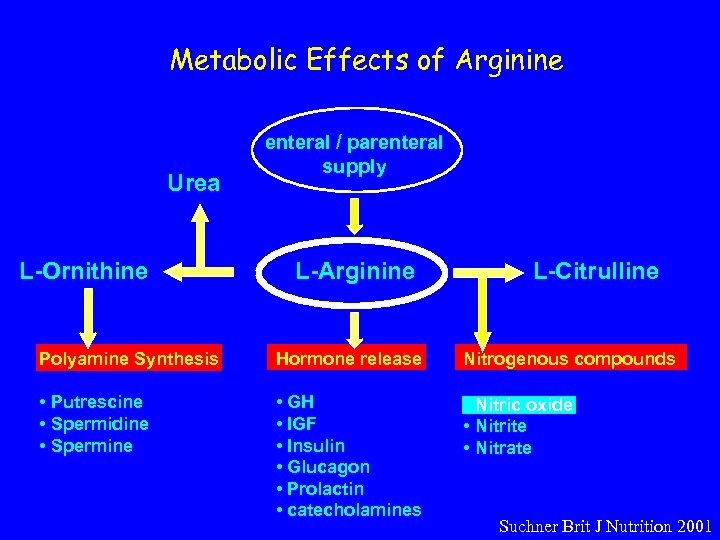 Metabolic Effects of Arginine Urea L-Ornithine enteral / parenteral supply L-Arginine L-Citrulline Polyamine Synthesis Hormone release Nitrogenous compounds • Putrescine • Spermidine • Spermine • GH • IGF • Insulin • Glucagon • Prolactin • catecholamines • Nitric oxide • Nitrite • Nitrate Suchner Brit J Nutrition 2001
Metabolic Effects of Arginine Urea L-Ornithine enteral / parenteral supply L-Arginine L-Citrulline Polyamine Synthesis Hormone release Nitrogenous compounds • Putrescine • Spermidine • Spermine • GH • IGF • Insulin • Glucagon • Prolactin • catecholamines • Nitric oxide • Nitrite • Nitrate Suchner Brit J Nutrition 2001
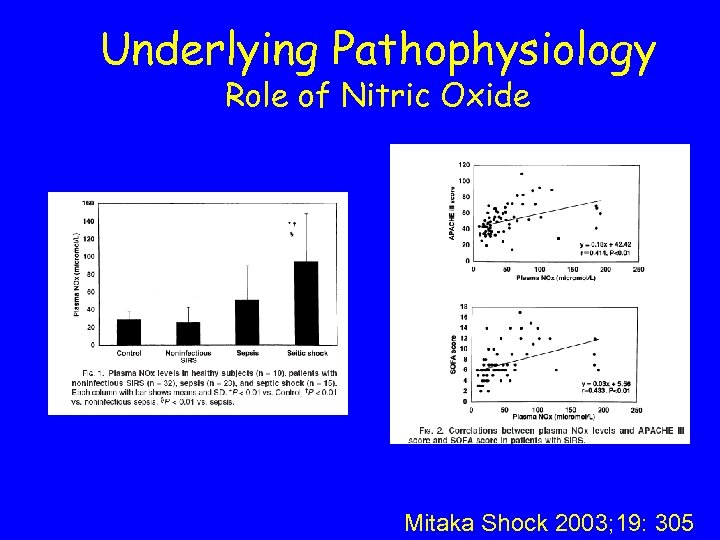 Underlying Pathophysiology Role of Nitric Oxide Mitaka Shock 2003; 19: 305
Underlying Pathophysiology Role of Nitric Oxide Mitaka Shock 2003; 19: 305
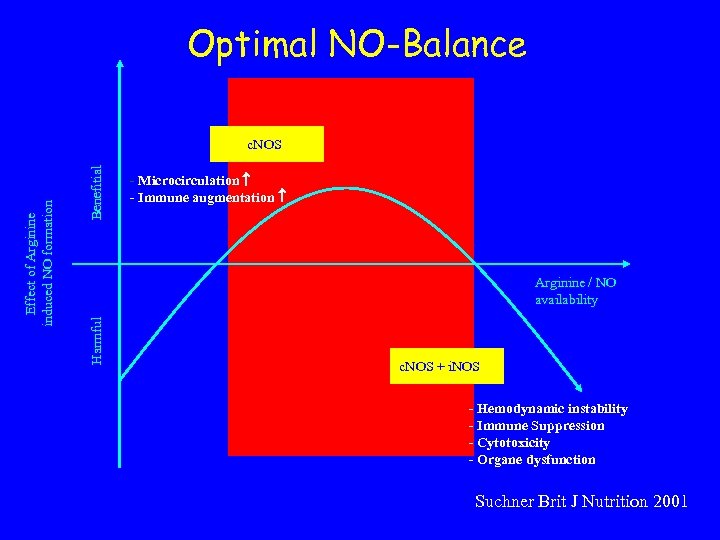 Optimal NO-Balance Benefitial - Microcirculation - Immune augmentation Arginine / NO availability Harmful Effect of Arginine induced NO formation c. NOS + i. NOS - Hemodynamic instability - Immune Suppression - Cytotoxicity - Organe dysfunction Suchner Brit J Nutrition 2001
Optimal NO-Balance Benefitial - Microcirculation - Immune augmentation Arginine / NO availability Harmful Effect of Arginine induced NO formation c. NOS + i. NOS - Hemodynamic instability - Immune Suppression - Cytotoxicity - Organe dysfunction Suchner Brit J Nutrition 2001
 Is it plausible that Argininesupplemented diets may do harm? Ø Randomized, double blind, placebo-controlled Ø Beagles Ø Parenteral L-arginine (+ NAC) vs placebo Ø Canine model of E. coli peritonitis Kalil Crit Care Med 2006; 34: 2719
Is it plausible that Argininesupplemented diets may do harm? Ø Randomized, double blind, placebo-controlled Ø Beagles Ø Parenteral L-arginine (+ NAC) vs placebo Ø Canine model of E. coli peritonitis Kalil Crit Care Med 2006; 34: 2719
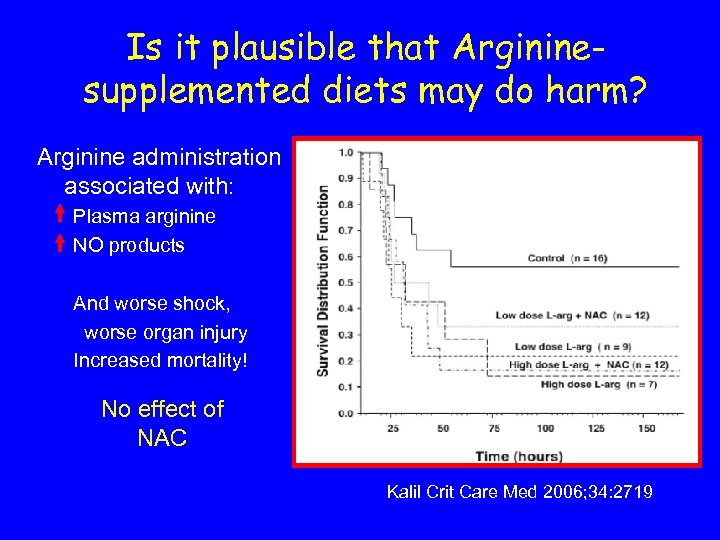 Is it plausible that Argininesupplemented diets may do harm? Arginine administration associated with: Plasma arginine NO products And worse shock, worse organ injury Increased mortality! No effect of NAC Kalil Crit Care Med 2006; 34: 2719
Is it plausible that Argininesupplemented diets may do harm? Arginine administration associated with: Plasma arginine NO products And worse shock, worse organ injury Increased mortality! No effect of NAC Kalil Crit Care Med 2006; 34: 2719
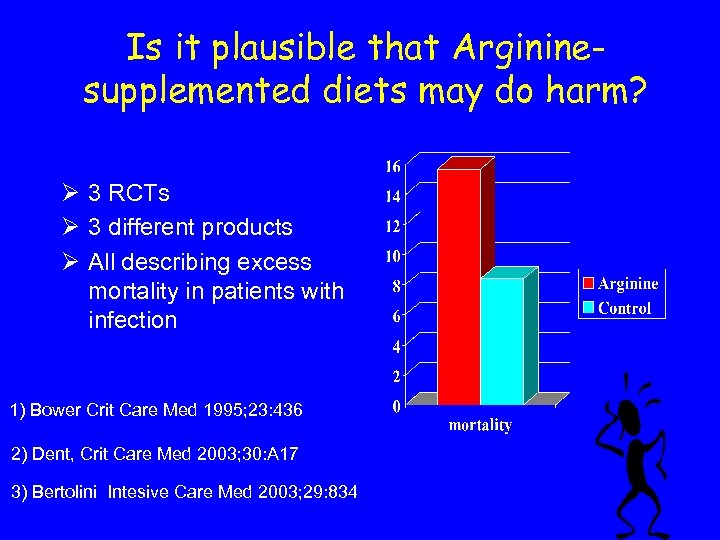 Is it plausible that Argininesupplemented diets may do harm? Ø 3 RCTs Ø 3 different products Ø All describing excess mortality in patients with infection 1) Bower Crit Care Med 1995; 23: 436 2) Dent, Crit Care Med 2003; 30: A 17 3) Bertolini Intesive Care Med 2003; 29: 834
Is it plausible that Argininesupplemented diets may do harm? Ø 3 RCTs Ø 3 different products Ø All describing excess mortality in patients with infection 1) Bower Crit Care Med 1995; 23: 436 2) Dent, Crit Care Med 2003; 30: A 17 3) Bertolini Intesive Care Med 2003; 29: 834
 Fish Oil supplemented diets?
Fish Oil supplemented diets?
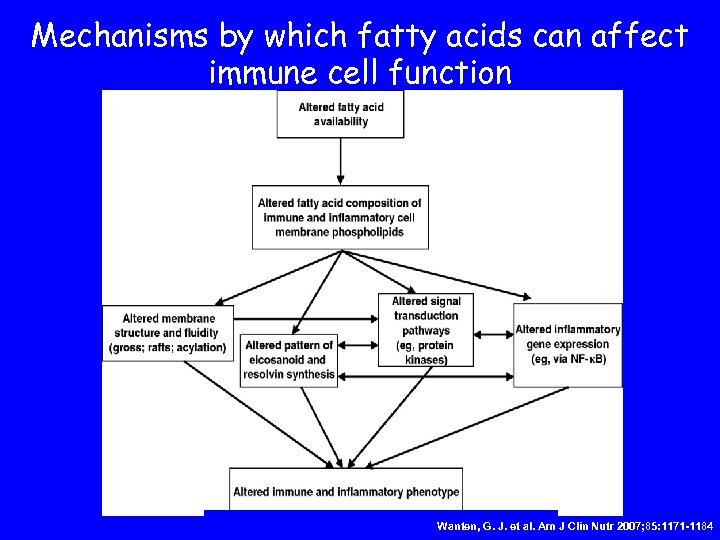 Mechanisms by which fatty acids can affect immune cell function Wanten, G. J. Copyright © 2007 The American Society for Nutrition et al. Am J Clin Nutr 2007; 85: 1171 -1184
Mechanisms by which fatty acids can affect immune cell function Wanten, G. J. Copyright © 2007 The American Society for Nutrition et al. Am J Clin Nutr 2007; 85: 1171 -1184
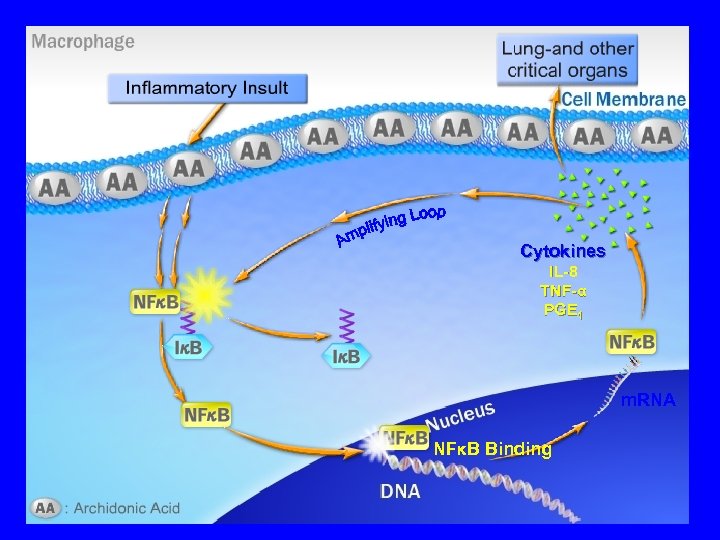 Cytokines IL-8 TNF-α PGE 1 m. RNA NFκB Binding
Cytokines IL-8 TNF-α PGE 1 m. RNA NFκB Binding
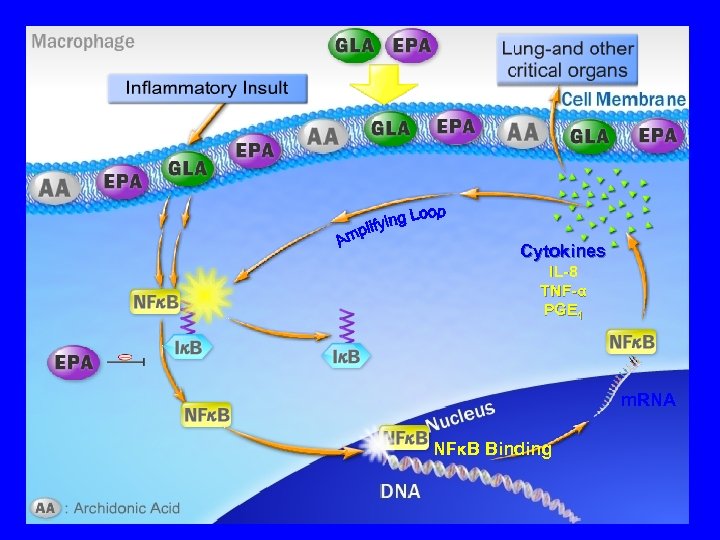 Cytokines IL-8 TNF-α PGE 1 m. RNA NFκB Binding
Cytokines IL-8 TNF-α PGE 1 m. RNA NFκB Binding
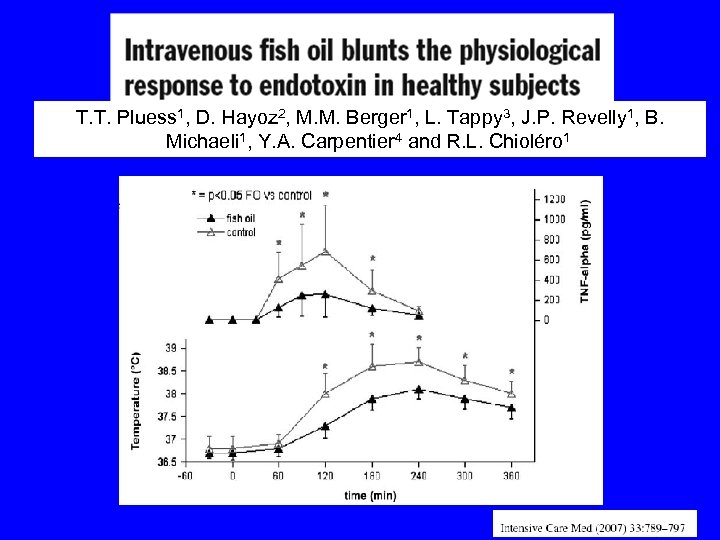 T. T. Pluess 1, D. Hayoz 2, M. M. Berger 1, L. Tappy 3, J. P. Revelly 1, B. Michaeli 1, Y. A. Carpentier 4 and R. L. Chioléro 1
T. T. Pluess 1, D. Hayoz 2, M. M. Berger 1, L. Tappy 3, J. P. Revelly 1, B. Michaeli 1, Y. A. Carpentier 4 and R. L. Chioléro 1
 • 21 patients with sepsis requiring TPN • Randomized to recieve PN with an n-3 or n 6 lipid emulsion for 5 days • Dose: 350 ml og s 10% n-3 lipid emulsion (Omegevan) Am J Respir Crit Care Med 2003; 167: 1321
• 21 patients with sepsis requiring TPN • Randomized to recieve PN with an n-3 or n 6 lipid emulsion for 5 days • Dose: 350 ml og s 10% n-3 lipid emulsion (Omegevan) Am J Respir Crit Care Med 2003; 167: 1321
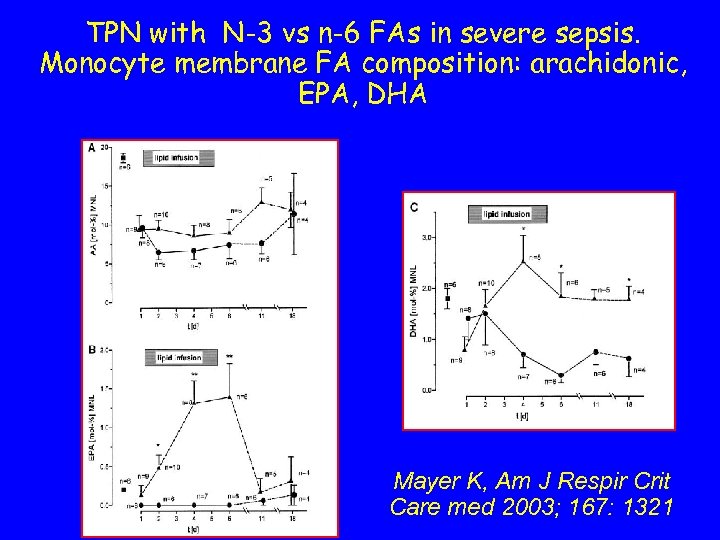 TPN with N-3 vs n-6 FAs in severe sepsis. Monocyte membrane FA composition: arachidonic, EPA, DHA Mayer K, Am J Respir Crit Care med 2003; 167: 1321
TPN with N-3 vs n-6 FAs in severe sepsis. Monocyte membrane FA composition: arachidonic, EPA, DHA Mayer K, Am J Respir Crit Care med 2003; 167: 1321
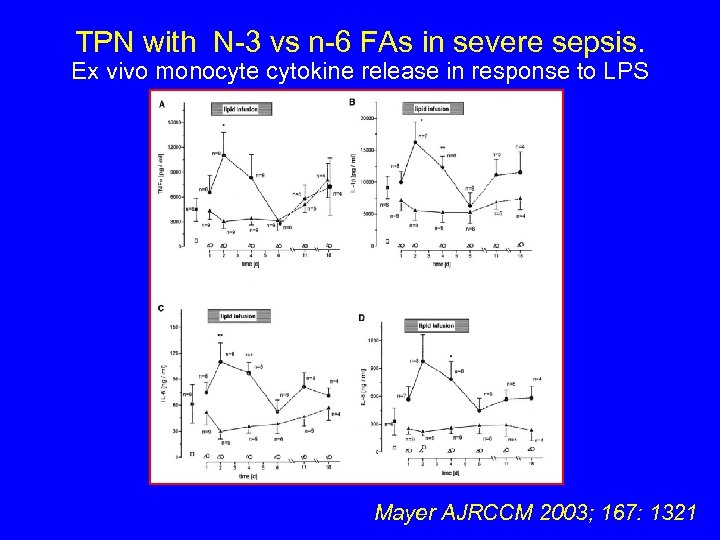 TPN with N-3 vs n-6 FAs in severe sepsis. Ex vivo monocyte cytokine release in response to LPS Mayer AJRCCM 2003; 167: 1321
TPN with N-3 vs n-6 FAs in severe sepsis. Ex vivo monocyte cytokine release in response to LPS Mayer AJRCCM 2003; 167: 1321
 • 47 Patients with severe acute pancreatitis • Randomized, double blind study of PN • N-3 lipid emulsion (omegaven 10%) vs. Soybean emulsion with TPNx 5 days • Dose of fish oils: 0. 15 -0. 20 g/kg/d • Patients comparable at baseline • Control group mortality 10%; no deaths in FO group Wang JPEN 2008; 32: 236
• 47 Patients with severe acute pancreatitis • Randomized, double blind study of PN • N-3 lipid emulsion (omegaven 10%) vs. Soybean emulsion with TPNx 5 days • Dose of fish oils: 0. 15 -0. 20 g/kg/d • Patients comparable at baseline • Control group mortality 10%; no deaths in FO group Wang JPEN 2008; 32: 236
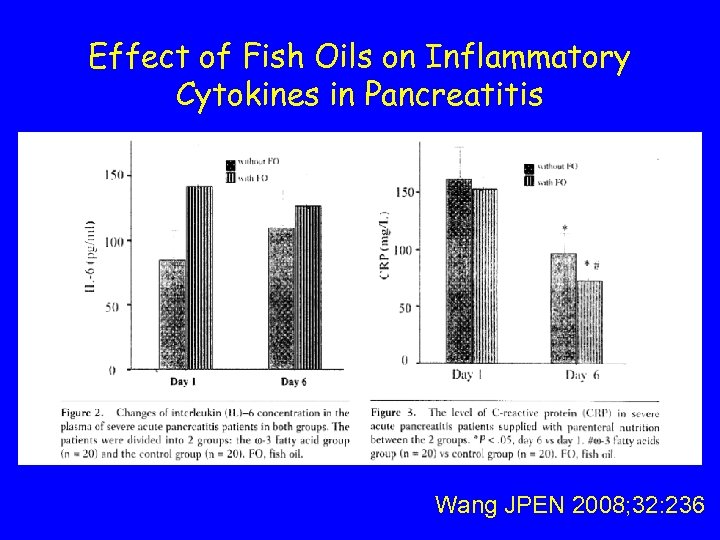 Effect of Fish Oils on Inflammatory Cytokines in Pancreatitis • Put figure 2 and 3 Wang JPEN 2008; 32: 236
Effect of Fish Oils on Inflammatory Cytokines in Pancreatitis • Put figure 2 and 3 Wang JPEN 2008; 32: 236
 Effect of Enteral Fish Oils/Borage Oils and antioxidants in Critically Ill with ALI • RCT of 146 critically ill patients with ALI and BAL+ for WBCs • Double-blinded; ITT • Experimental: Oxepa® • Control: high fat diet • Groups well matched at baseline After 3 -4 days • Reduction in AA and increase in EPA in lung and alveolar macrophage • Decrease in neutrophils recovered in BAL fluid • Improved oxygenation Gadek Crit Care Med 1999; 27: 1409
Effect of Enteral Fish Oils/Borage Oils and antioxidants in Critically Ill with ALI • RCT of 146 critically ill patients with ALI and BAL+ for WBCs • Double-blinded; ITT • Experimental: Oxepa® • Control: high fat diet • Groups well matched at baseline After 3 -4 days • Reduction in AA and increase in EPA in lung and alveolar macrophage • Decrease in neutrophils recovered in BAL fluid • Improved oxygenation Gadek Crit Care Med 1999; 27: 1409
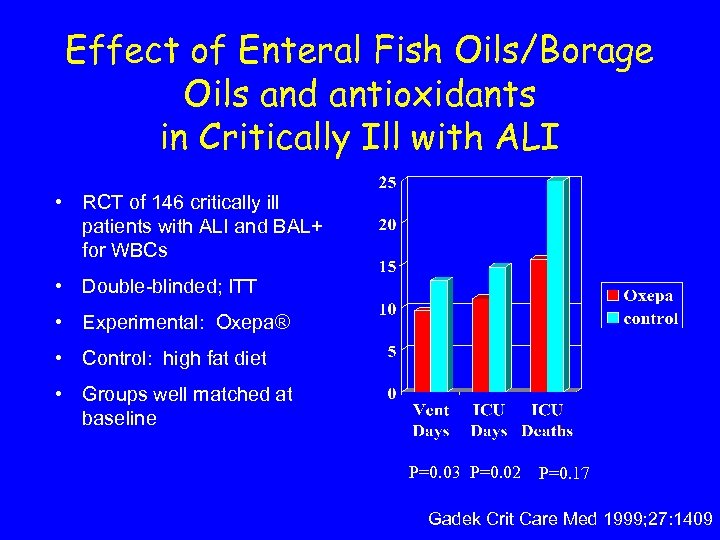 Effect of Enteral Fish Oils/Borage Oils and antioxidants in Critically Ill with ALI • RCT of 146 critically ill patients with ALI and BAL+ for WBCs • Double-blinded; ITT • Experimental: Oxepa® • Control: high fat diet • Groups well matched at baseline P=0. 03 P=0. 02 P=0. 17 Gadek Crit Care Med 1999; 27: 1409
Effect of Enteral Fish Oils/Borage Oils and antioxidants in Critically Ill with ALI • RCT of 146 critically ill patients with ALI and BAL+ for WBCs • Double-blinded; ITT • Experimental: Oxepa® • Control: high fat diet • Groups well matched at baseline P=0. 03 P=0. 02 P=0. 17 Gadek Crit Care Med 1999; 27: 1409
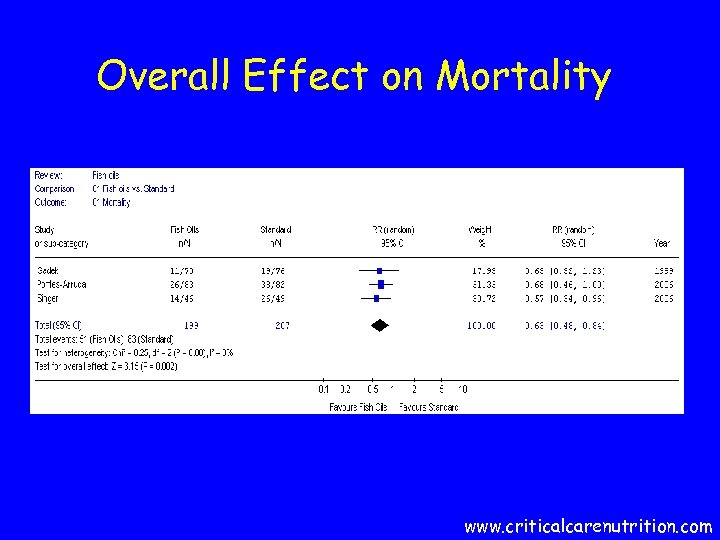 Overall Effect on Mortality www. criticalcarenutrition. com
Overall Effect on Mortality www. criticalcarenutrition. com
 Glutamine supplementation?
Glutamine supplementation?
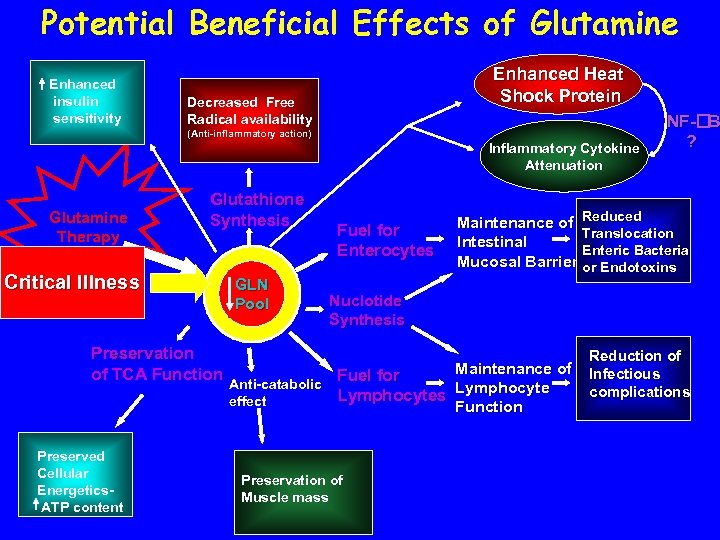 Potential Beneficial Effects of Glutamine Enhanced insulin sensitivity Enhanced Heat Shock Protein Decreased Free Radical availability (Anti-inflammatory action) Inflammatory Cytokine Attenuation Glutamine Therapy Glutathione Synthesis Critical Illness Preservation of TCA Function Preserved Cellular Energetics. ATP content GLN Pool pool Fuel for Enterocytes NF- B ? Maintenance of Reduced Translocation Intestinal Enteric Bacteria Mucosal Barrier or Endotoxins Nuclotide Synthesis Maintenance of Fuel for Anti-catabolic Lymphocytes effect Function Preservation of Muscle mass Reduction of Infectious complications
Potential Beneficial Effects of Glutamine Enhanced insulin sensitivity Enhanced Heat Shock Protein Decreased Free Radical availability (Anti-inflammatory action) Inflammatory Cytokine Attenuation Glutamine Therapy Glutathione Synthesis Critical Illness Preservation of TCA Function Preserved Cellular Energetics. ATP content GLN Pool pool Fuel for Enterocytes NF- B ? Maintenance of Reduced Translocation Intestinal Enteric Bacteria Mucosal Barrier or Endotoxins Nuclotide Synthesis Maintenance of Fuel for Anti-catabolic Lymphocytes effect Function Preservation of Muscle mass Reduction of Infectious complications
 Effect of Glutamine: A Systematic Review of the Literature Infectious Complications www. criticalcarenutrition. com
Effect of Glutamine: A Systematic Review of the Literature Infectious Complications www. criticalcarenutrition. com
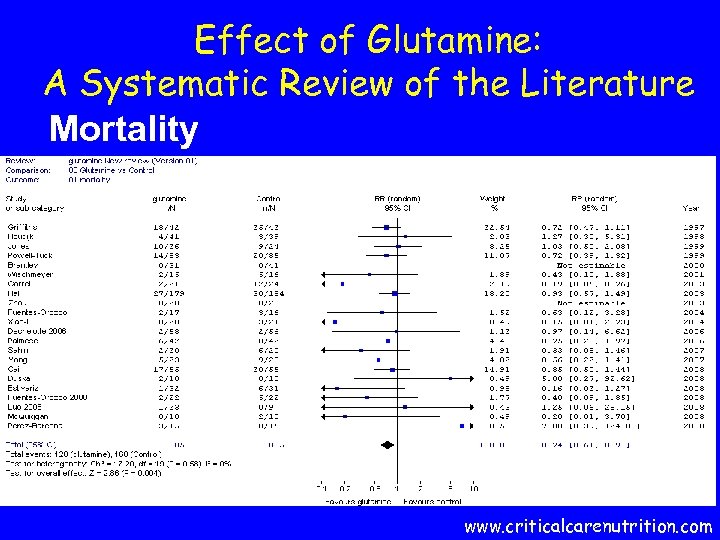 Effect of Glutamine: A Systematic Review of the Literature Mortality www. criticalcarenutrition. com
Effect of Glutamine: A Systematic Review of the Literature Mortality www. criticalcarenutrition. com
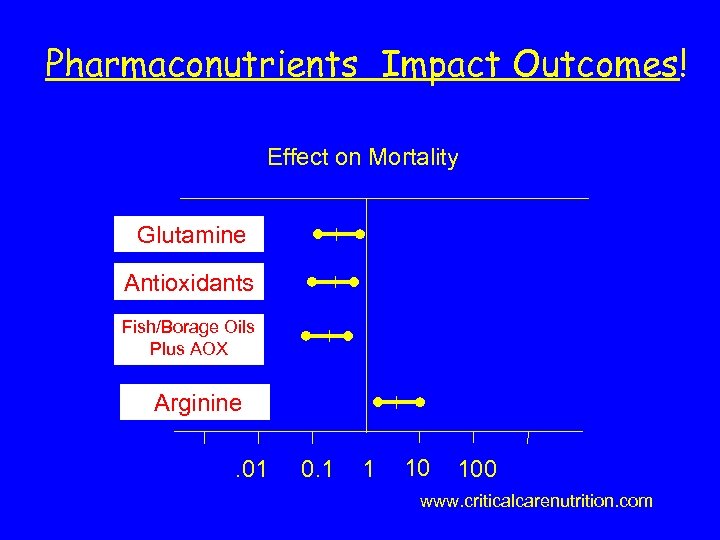 Pharmaconutrients Impact Outcomes! Effect on Mortality Glutamine Antioxidants Fish/Borage Oils Plus AOX Arginine. 01 0. 1 1 10 100 www. criticalcarenutrition. com
Pharmaconutrients Impact Outcomes! Effect on Mortality Glutamine Antioxidants Fish/Borage Oils Plus AOX Arginine. 01 0. 1 1 10 100 www. criticalcarenutrition. com
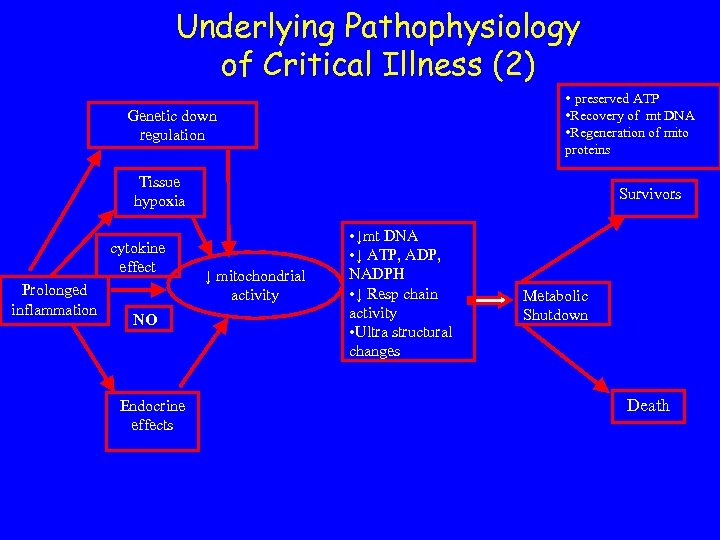 Underlying Pathophysiology of Critical Illness (2) • preserved ATP Genetic down regulation • Recovery of mt DNA • Regeneration of mito proteins Tissue hypoxia cytokine effect Prolonged inflammation NO Endocrine effects Survivors ↓ mitochondrial activity • ↓mt DNA • ↓ ATP, ADP, NADPH • ↓ Resp chain activity • Ultra structural changes Metabolic Shutdown Death
Underlying Pathophysiology of Critical Illness (2) • preserved ATP Genetic down regulation • Recovery of mt DNA • Regeneration of mito proteins Tissue hypoxia cytokine effect Prolonged inflammation NO Endocrine effects Survivors ↓ mitochondrial activity • ↓mt DNA • ↓ ATP, ADP, NADPH • ↓ Resp chain activity • Ultra structural changes Metabolic Shutdown Death
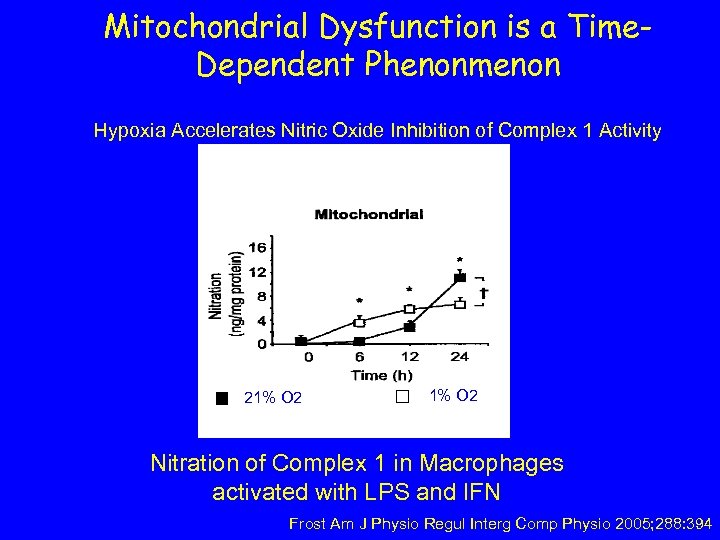 Mitochondrial Dysfunction is a Time. Dependent Phenonmenon Hypoxia Accelerates Nitric Oxide Inhibition of Complex 1 Activity 21% O 2 Nitration of Complex 1 in Macrophages activated with LPS and IFN Frost Am J Physio Regul Interg Comp Physio 2005; 288: 394
Mitochondrial Dysfunction is a Time. Dependent Phenonmenon Hypoxia Accelerates Nitric Oxide Inhibition of Complex 1 Activity 21% O 2 Nitration of Complex 1 in Macrophages activated with LPS and IFN Frost Am J Physio Regul Interg Comp Physio 2005; 288: 394
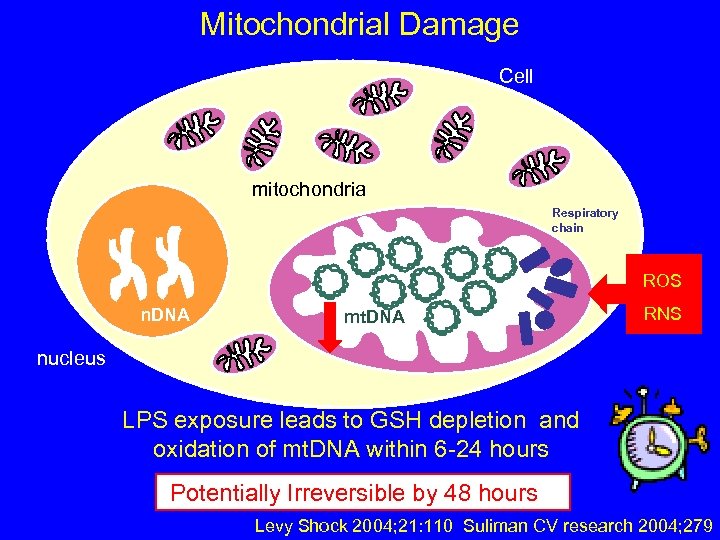 Mitochondrial Damage Cell mitochondria Respiratory chain ROS n. DNA mt. DNA RNS nucleus LPS exposure leads to GSH depletion and oxidation of mt. DNA within 6 -24 hours Potentially Irreversible by 48 hours Levy Shock 2004; 21: 110 Suliman CV research 2004; 279
Mitochondrial Damage Cell mitochondria Respiratory chain ROS n. DNA mt. DNA RNS nucleus LPS exposure leads to GSH depletion and oxidation of mt. DNA within 6 -24 hours Potentially Irreversible by 48 hours Levy Shock 2004; 21: 110 Suliman CV research 2004; 279
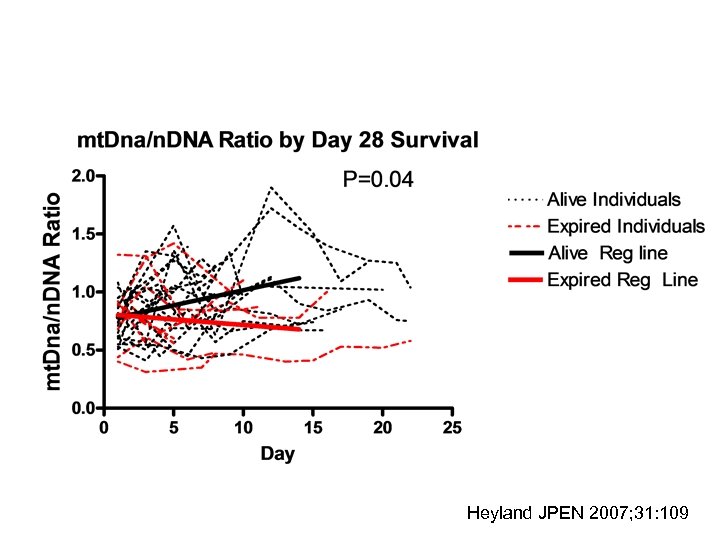 Heyland JPEN 2007; 31: 109
Heyland JPEN 2007; 31: 109
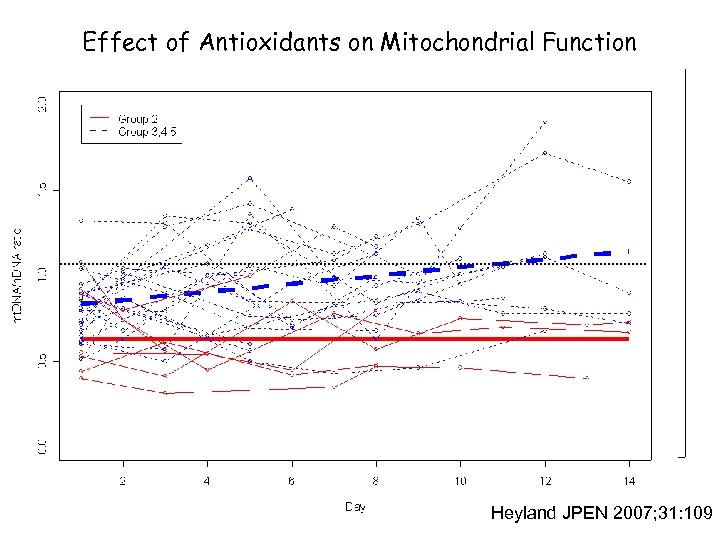 Effect of Antioxidants on Mitochondrial Function Heyland JPEN 2007; 31: 109
Effect of Antioxidants on Mitochondrial Function Heyland JPEN 2007; 31: 109
 Smallest Randomized Trial of Selenium in Sepsis § Single center RCT § double-blinded § ITT analysis § 40 patients with severe sepsis § Mean APACHE II 18 § Primary endpoint: need for RRT § standard nutrition plus 474 ug x 3 days, 316 ug x 3 days; 31. 6 ug thereafter vs 31. 6 ug/day in control Mishra Clinical Nutrition 2007; 26: 41 -50
Smallest Randomized Trial of Selenium in Sepsis § Single center RCT § double-blinded § ITT analysis § 40 patients with severe sepsis § Mean APACHE II 18 § Primary endpoint: need for RRT § standard nutrition plus 474 ug x 3 days, 316 ug x 3 days; 31. 6 ug thereafter vs 31. 6 ug/day in control Mishra Clinical Nutrition 2007; 26: 41 -50
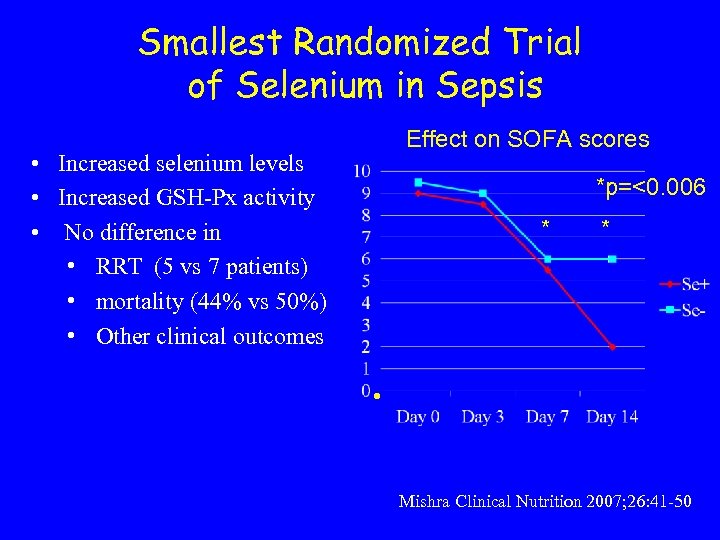 Smallest Randomized Trial of Selenium in Sepsis Effect on SOFA scores • Increased selenium levels • Increased GSH-Px activity • No difference in • RRT (5 vs 7 patients) • mortality (44% vs 50%) • Other clinical outcomes *p=<0. 006 * * • Mishra Clinical Nutrition 2007; 26: 41 -50
Smallest Randomized Trial of Selenium in Sepsis Effect on SOFA scores • Increased selenium levels • Increased GSH-Px activity • No difference in • RRT (5 vs 7 patients) • mortality (44% vs 50%) • Other clinical outcomes *p=<0. 006 * * • Mishra Clinical Nutrition 2007; 26: 41 -50
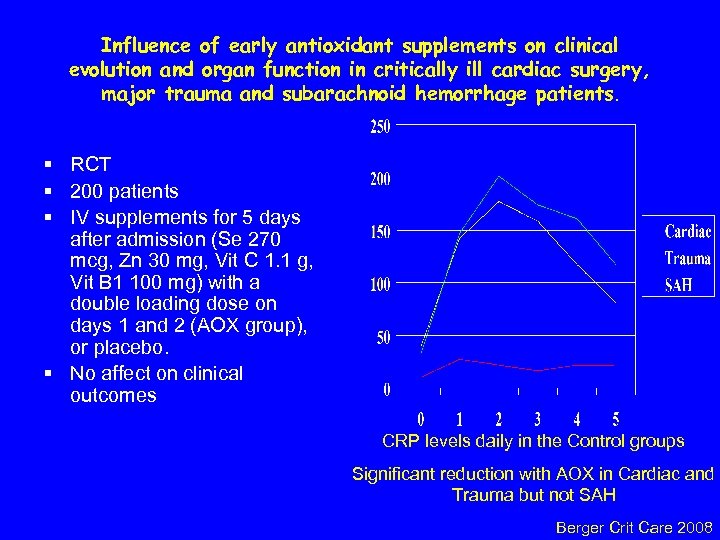 Influence of early antioxidant supplements on clinical evolution and organ function in critically ill cardiac surgery, major trauma and subarachnoid hemorrhage patients. § RCT § 200 patients § IV supplements for 5 days after admission (Se 270 mcg, Zn 30 mg, Vit C 1. 1 g, Vit B 1 100 mg) with a double loading dose on days 1 and 2 (AOX group), or placebo. § No affect on clinical outcomes CRP levels daily in the Control groups Significant reduction with AOX in Cardiac and Trauma but not SAH Berger Crit Care 2008
Influence of early antioxidant supplements on clinical evolution and organ function in critically ill cardiac surgery, major trauma and subarachnoid hemorrhage patients. § RCT § 200 patients § IV supplements for 5 days after admission (Se 270 mcg, Zn 30 mg, Vit C 1. 1 g, Vit B 1 100 mg) with a double loading dose on days 1 and 2 (AOX group), or placebo. § No affect on clinical outcomes CRP levels daily in the Control groups Significant reduction with AOX in Cardiac and Trauma but not SAH Berger Crit Care 2008
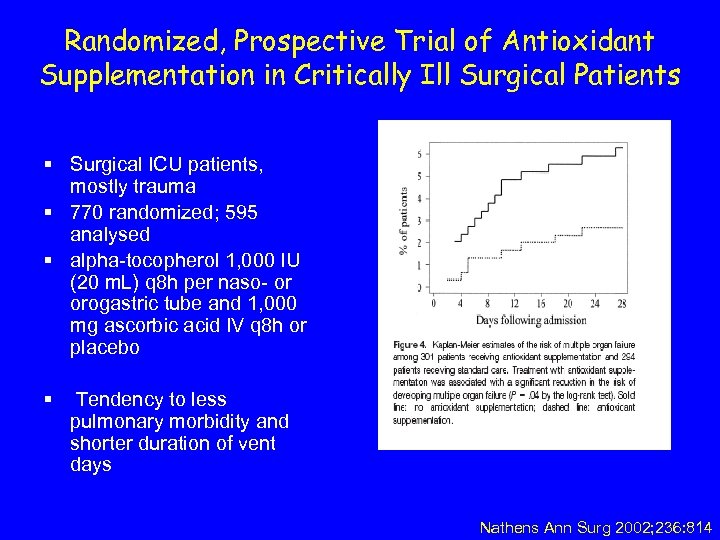 Randomized, Prospective Trial of Antioxidant Supplementation in Critically Ill Surgical Patients § Surgical ICU patients, mostly trauma § 770 randomized; 595 analysed § alpha-tocopherol 1, 000 IU (20 m. L) q 8 h per naso- or orogastric tube and 1, 000 mg ascorbic acid IV q 8 h or placebo § Tendency to less pulmonary morbidity and shorter duration of vent days Nathens Ann Surg 2002; 236: 814
Randomized, Prospective Trial of Antioxidant Supplementation in Critically Ill Surgical Patients § Surgical ICU patients, mostly trauma § 770 randomized; 595 analysed § alpha-tocopherol 1, 000 IU (20 m. L) q 8 h per naso- or orogastric tube and 1, 000 mg ascorbic acid IV q 8 h or placebo § Tendency to less pulmonary morbidity and shorter duration of vent days Nathens Ann Surg 2002; 236: 814
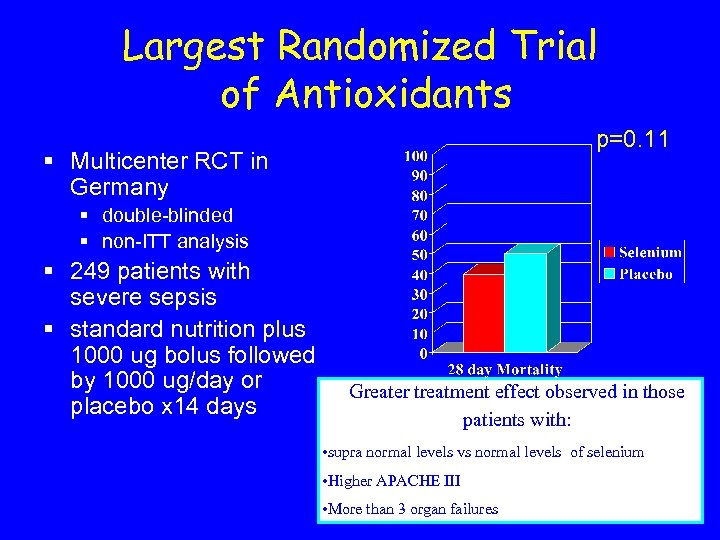 Largest Randomized Trial of Antioxidants p=0. 11 § Multicenter RCT in Germany § double-blinded § non-ITT analysis § 249 patients with severe sepsis § standard nutrition plus 1000 ug bolus followed by 1000 ug/day or placebo x 14 days Greater treatment effect observed in those patients with: • supra normal levels vs normal levels of selenium • Higher APACHE III • More than 3 organ failures Crit Care Med 2007; 135: 1
Largest Randomized Trial of Antioxidants p=0. 11 § Multicenter RCT in Germany § double-blinded § non-ITT analysis § 249 patients with severe sepsis § standard nutrition plus 1000 ug bolus followed by 1000 ug/day or placebo x 14 days Greater treatment effect observed in those patients with: • supra normal levels vs normal levels of selenium • Higher APACHE III • More than 3 organ failures Crit Care Med 2007; 135: 1
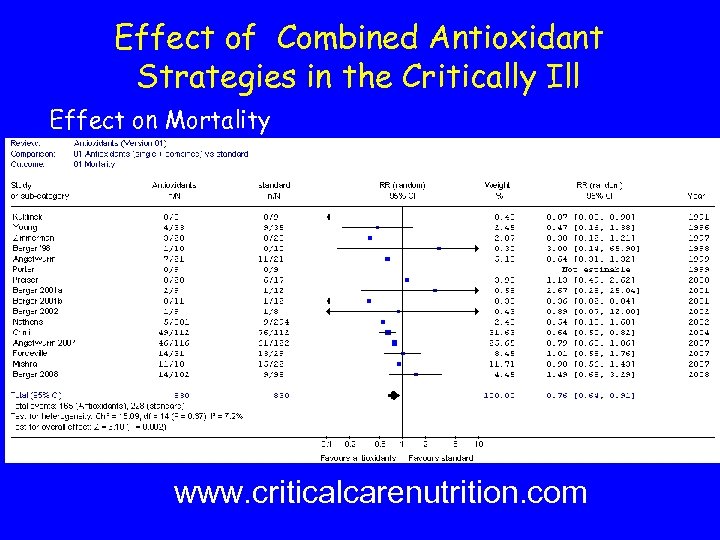 Effect of Combined Antioxidant Strategies in the Critically Ill Effect on Mortality www. criticalcarenutrition. com
Effect of Combined Antioxidant Strategies in the Critically Ill Effect on Mortality www. criticalcarenutrition. com
 Biological Plausibility! Mitochondrial dysfunction Antioxidants Inflammation/oxidative stress Antioxidants Organ dysfunction Antioxidants
Biological Plausibility! Mitochondrial dysfunction Antioxidants Inflammation/oxidative stress Antioxidants Organ dysfunction Antioxidants
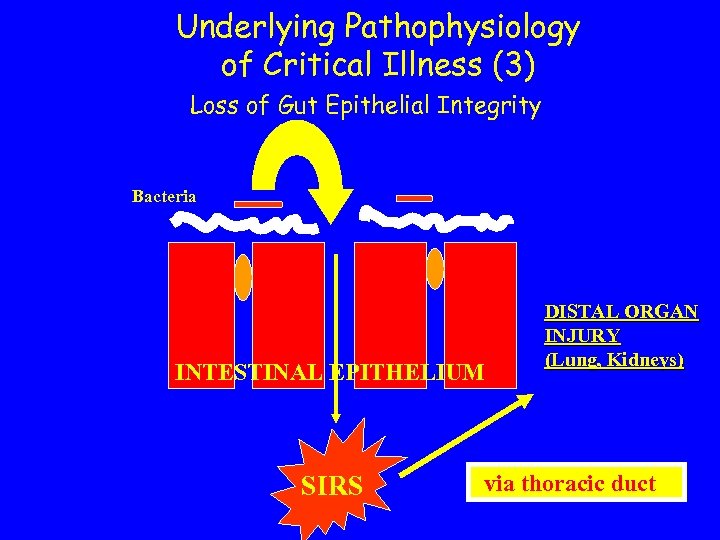 Underlying Pathophysiology of Critical Illness (3) Loss of Gut Epithelial Integrity Bacteria INTESTINAL EPITHELIUM SIRS DISTAL ORGAN INJURY (Lung, Kidneys) via thoracic duct
Underlying Pathophysiology of Critical Illness (3) Loss of Gut Epithelial Integrity Bacteria INTESTINAL EPITHELIUM SIRS DISTAL ORGAN INJURY (Lung, Kidneys) via thoracic duct
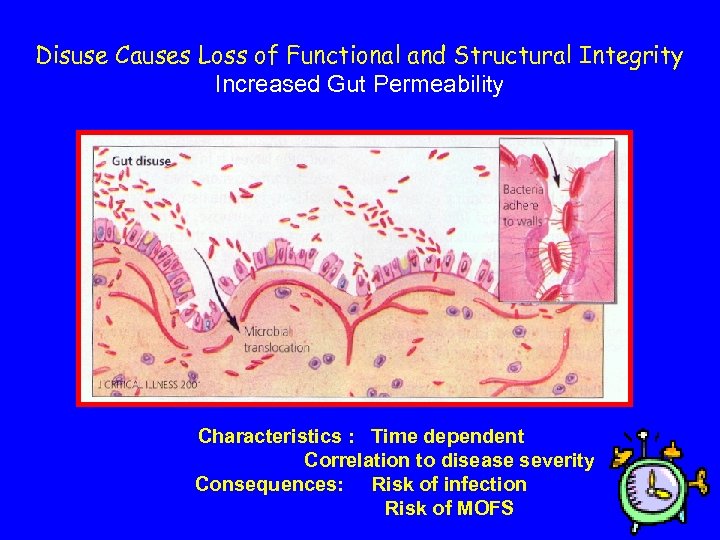 Disuse Causes Loss of Functional and Structural Integrity Increased Gut Permeability Characteristics : Time dependent Correlation to disease severity Consequences: Risk of infection Risk of MOFS
Disuse Causes Loss of Functional and Structural Integrity Increased Gut Permeability Characteristics : Time dependent Correlation to disease severity Consequences: Risk of infection Risk of MOFS
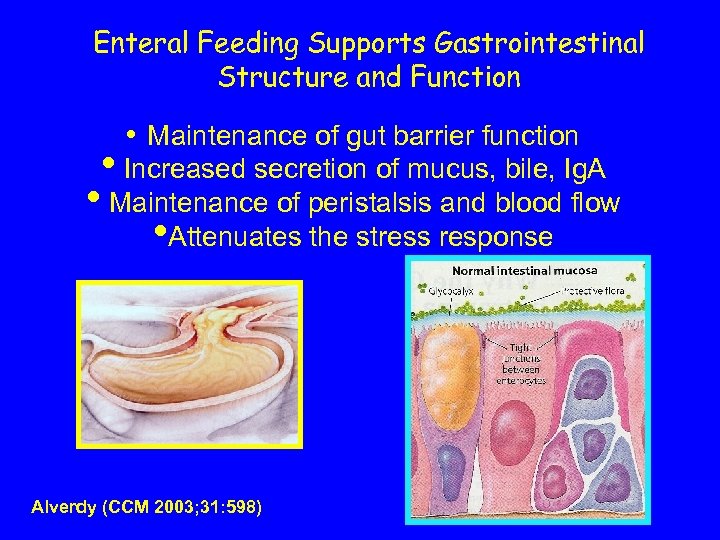 Enteral Feeding Supports Gastrointestinal Structure and Function • Maintenance of gut barrier function • Increased secretion of mucus, bile, Ig. A • Maintenance of peristalsis and blood flow • Attenuates the stress response Alverdy (CCM 2003; 31: 598)
Enteral Feeding Supports Gastrointestinal Structure and Function • Maintenance of gut barrier function • Increased secretion of mucus, bile, Ig. A • Maintenance of peristalsis and blood flow • Attenuates the stress response Alverdy (CCM 2003; 31: 598)
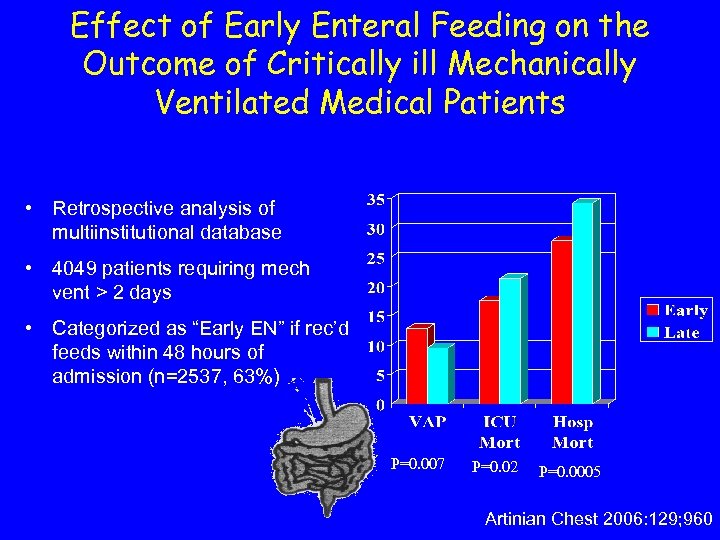 Effect of Early Enteral Feeding on the Outcome of Critically ill Mechanically Ventilated Medical Patients • Retrospective analysis of multiinstitutional database • 4049 patients requiring mech vent > 2 days • Categorized as “Early EN” if rec’d feeds within 48 hours of admission (n=2537, 63%) P=0. 007 P=0. 02 P=0. 0005 Artinian Chest 2006: 129; 960
Effect of Early Enteral Feeding on the Outcome of Critically ill Mechanically Ventilated Medical Patients • Retrospective analysis of multiinstitutional database • 4049 patients requiring mech vent > 2 days • Categorized as “Early EN” if rec’d feeds within 48 hours of admission (n=2537, 63%) P=0. 007 P=0. 02 P=0. 0005 Artinian Chest 2006: 129; 960
 Early vs. Delayed EN: Effect on Infectious Complications www. criticalcarenutrition. com
Early vs. Delayed EN: Effect on Infectious Complications www. criticalcarenutrition. com
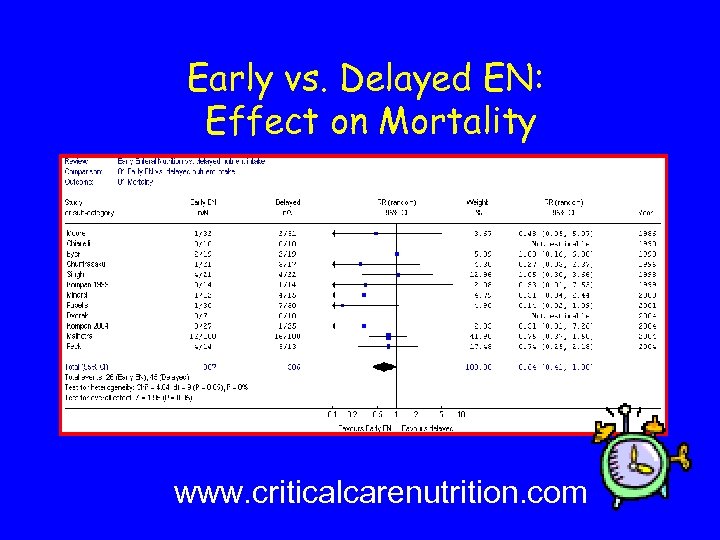 Early vs. Delayed EN: Effect on Mortality www. criticalcarenutrition. com
Early vs. Delayed EN: Effect on Mortality www. criticalcarenutrition. com
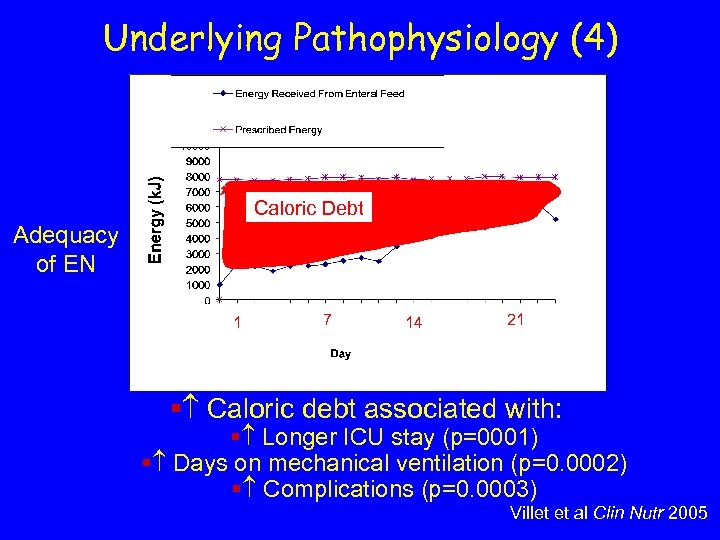 Underlying Pathophysiology (4) Caloric Debt Adequacy of EN 1 7 14 21 § Caloric debt associated with: § Longer ICU stay (p=0001) § Days on mechanical ventilation (p=0. 0002) § Complications (p=0. 0003) Villet et al Clin Nutr 2005
Underlying Pathophysiology (4) Caloric Debt Adequacy of EN 1 7 14 21 § Caloric debt associated with: § Longer ICU stay (p=0001) § Days on mechanical ventilation (p=0. 0002) § Complications (p=0. 0003) Villet et al Clin Nutr 2005
 2007 International Nutrition Practice Survey • Point prevalence survey of nutrition practices in ICU’s around the world conducted Jan. 27, 2007 • Enrolled 2772 patients from 158 ICU’s over 5 continents • Included ventilated adult patients who remained in ICU >72 hours
2007 International Nutrition Practice Survey • Point prevalence survey of nutrition practices in ICU’s around the world conducted Jan. 27, 2007 • Enrolled 2772 patients from 158 ICU’s over 5 continents • Included ventilated adult patients who remained in ICU >72 hours
 Hypothesis • There is a relationship between amount of energy and protein received and clinical outcomes (mortality and # of days on ventilator) • The relationship is influenced by nutritional risk • BMI is used to define chronic nutritional risk
Hypothesis • There is a relationship between amount of energy and protein received and clinical outcomes (mortality and # of days on ventilator) • The relationship is influenced by nutritional risk • BMI is used to define chronic nutritional risk
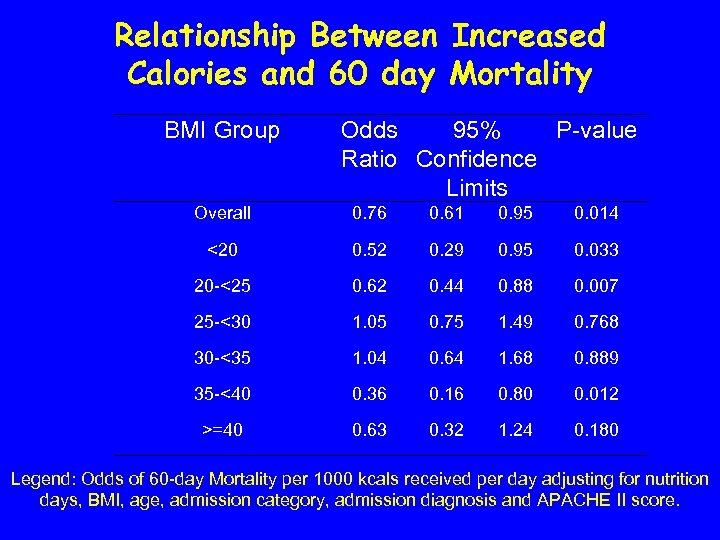 Relationship Between Increased Calories and 60 day Mortality BMI Group Odds 95% P-value Ratio Confidence Limits Overall 0. 76 0. 61 0. 95 0. 014 <20 0. 52 0. 29 0. 95 0. 033 20 -<25 0. 62 0. 44 0. 88 0. 007 25 -<30 1. 05 0. 75 1. 49 0. 768 30 -<35 1. 04 0. 64 1. 68 0. 889 35 -<40 0. 36 0. 16 0. 80 0. 012 >=40 0. 63 0. 32 1. 24 0. 180 Legend: Odds of 60 -day Mortality per 1000 kcals received per day adjusting for nutrition days, BMI, age, admission category, admission diagnosis and APACHE II score.
Relationship Between Increased Calories and 60 day Mortality BMI Group Odds 95% P-value Ratio Confidence Limits Overall 0. 76 0. 61 0. 95 0. 014 <20 0. 52 0. 29 0. 95 0. 033 20 -<25 0. 62 0. 44 0. 88 0. 007 25 -<30 1. 05 0. 75 1. 49 0. 768 30 -<35 1. 04 0. 64 1. 68 0. 889 35 -<40 0. 36 0. 16 0. 80 0. 012 >=40 0. 63 0. 32 1. 24 0. 180 Legend: Odds of 60 -day Mortality per 1000 kcals received per day adjusting for nutrition days, BMI, age, admission category, admission diagnosis and APACHE II score.
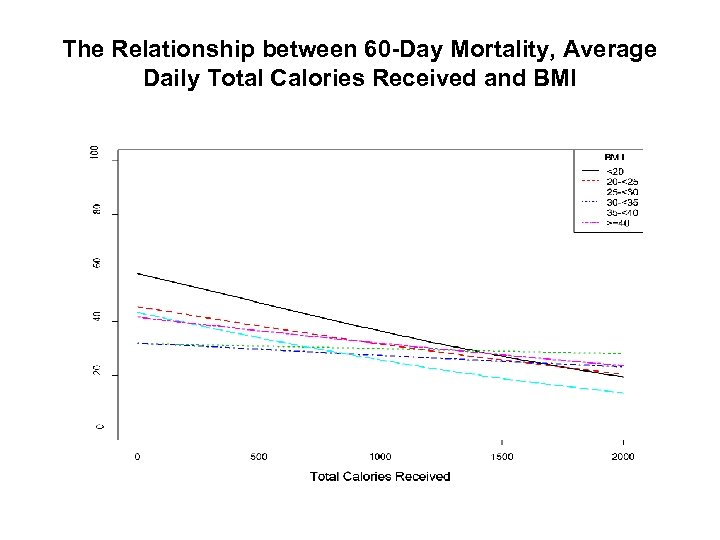 The Relationship between 60 -Day Mortality, Average Daily Total Calories Received and BMI
The Relationship between 60 -Day Mortality, Average Daily Total Calories Received and BMI
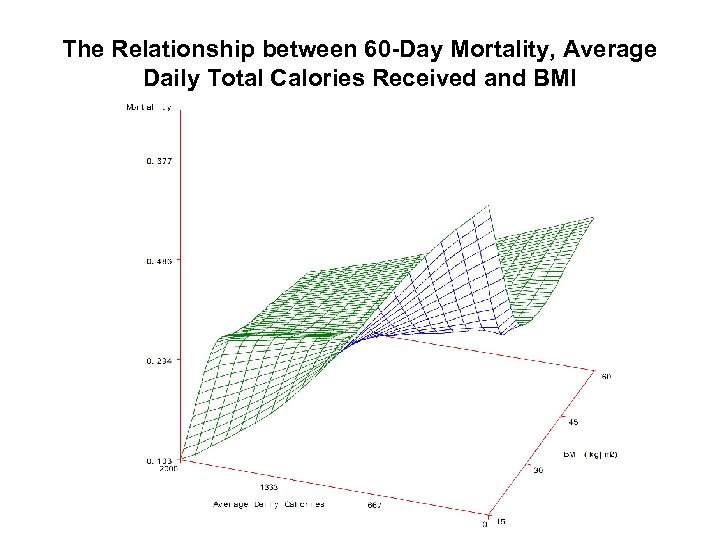 The Relationship between 60 -Day Mortality, Average Daily Total Calories Received and BMI
The Relationship between 60 -Day Mortality, Average Daily Total Calories Received and BMI
 ICU patients are not all created equal…should we expect the impact of nutrition therapy to be the same across all patients?
ICU patients are not all created equal…should we expect the impact of nutrition therapy to be the same across all patients?
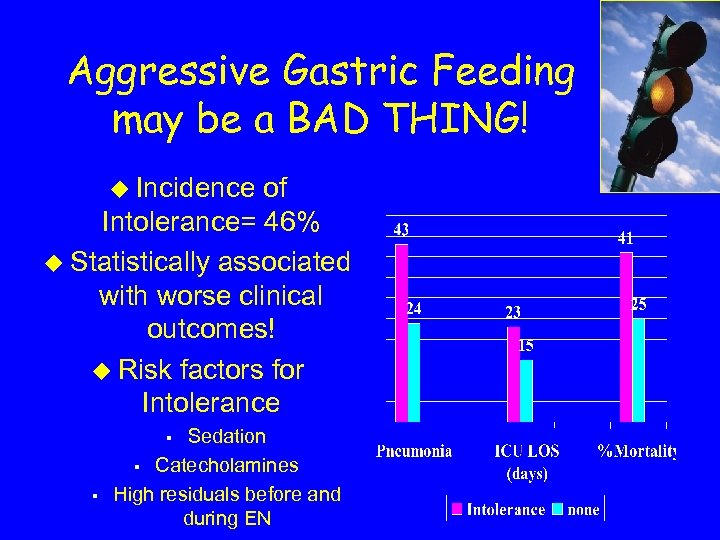 Aggressive Gastric Feeding may be a BAD THING! u Incidence of Intolerance= 46% u Statistically associated with worse clinical outcomes! u Risk factors for Intolerance Sedation § Catecholamines High residuals before and during EN § §
Aggressive Gastric Feeding may be a BAD THING! u Incidence of Intolerance= 46% u Statistically associated with worse clinical outcomes! u Risk factors for Intolerance Sedation § Catecholamines High residuals before and during EN § §
 Strategies to Maximize the Benefits and Minimize the Risks of EN • • • concentrated feeding formulas feeding protocols motility agents elevation of HOB small bowel feeds weak evidence stronger evidence Canadian CPGs www. criticalcarenutrition. com
Strategies to Maximize the Benefits and Minimize the Risks of EN • • • concentrated feeding formulas feeding protocols motility agents elevation of HOB small bowel feeds weak evidence stronger evidence Canadian CPGs www. criticalcarenutrition. com
 What if you can’t provide adequate nutrition enterally? … to TPN or not to TPN, that is the question!
What if you can’t provide adequate nutrition enterally? … to TPN or not to TPN, that is the question!
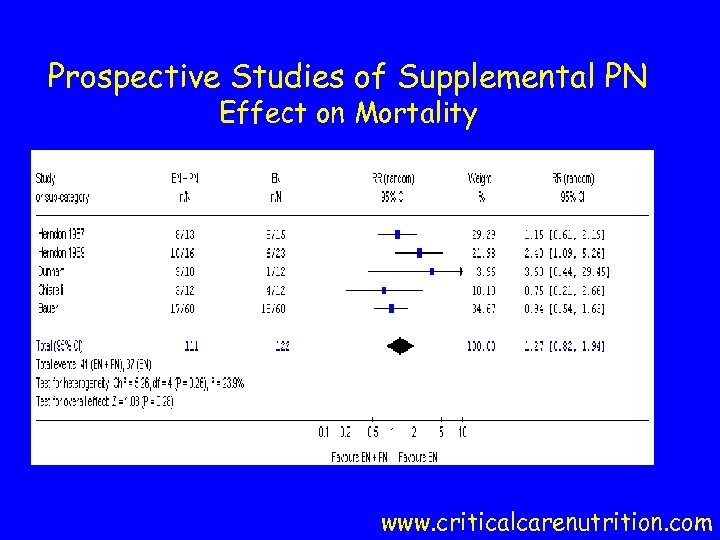 Prospective Studies of Supplemental PN Effect on Mortality www. criticalcarenutrition. com
Prospective Studies of Supplemental PN Effect on Mortality www. criticalcarenutrition. com
 What if you can’t provide adequate nutrition enterally? … to TPN or not to TPN, that is the question! Maximize EN delivery prior to initiating PN
What if you can’t provide adequate nutrition enterally? … to TPN or not to TPN, that is the question! Maximize EN delivery prior to initiating PN
 Summary • Nutrients/Nutritional strategies – Modulate underlying pathphysiological processes – Improve clinical outcomes – Disease processes and treatment effects are time dependent – Quantity of nutrition therapy associated with outcomes, particularly in low and high BMI patients
Summary • Nutrients/Nutritional strategies – Modulate underlying pathphysiological processes – Improve clinical outcomes – Disease processes and treatment effects are time dependent – Quantity of nutrition therapy associated with outcomes, particularly in low and high BMI patients
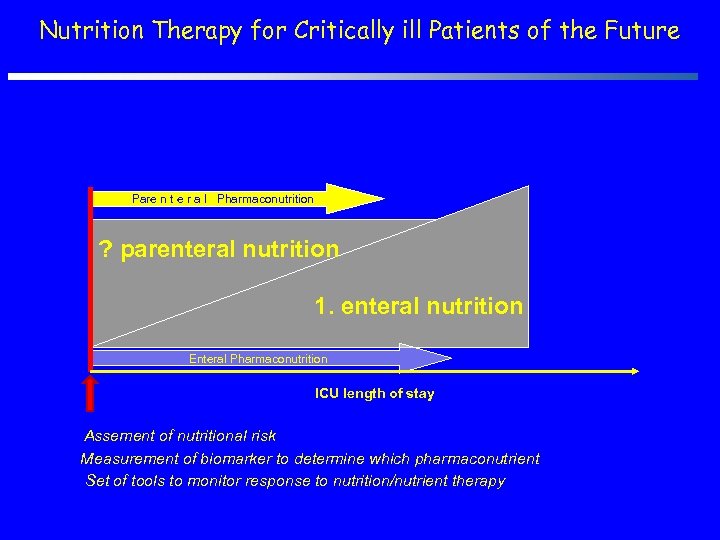 Nutrition Therapy for Critically ill Patients of the Future Pare n t e r a l Pharmaconutrition ? parenteral nutrition 1. enteral nutrition Enteral Pharmaconutrition ICU length of stay Assement of nutritional risk Measurement of biomarker to determine which pharmaconutrient Set of tools to monitor response to nutrition/nutrient therapy
Nutrition Therapy for Critically ill Patients of the Future Pare n t e r a l Pharmaconutrition ? parenteral nutrition 1. enteral nutrition Enteral Pharmaconutrition ICU length of stay Assement of nutritional risk Measurement of biomarker to determine which pharmaconutrient Set of tools to monitor response to nutrition/nutrient therapy
 Case Scenario • • Mr KT 76 per’d diverticulum Septic shock, ARDS, MODS Day 1 - high NG drainage, distended abdomen Day 3 - trickle feeds Feeds on and off again for whole first week No PN, no small bowel feeds, no specialized nutrients
Case Scenario • • Mr KT 76 per’d diverticulum Septic shock, ARDS, MODS Day 1 - high NG drainage, distended abdomen Day 3 - trickle feeds Feeds on and off again for whole first week No PN, no small bowel feeds, no specialized nutrients
 Case Scenario • Treatment effect function of timeliness – Early goal resuscitation – Appropriate antibiotics – Use of Activated Protein C – Hydrocortisone AND Early Pharmaconutrients Early EN
Case Scenario • Treatment effect function of timeliness – Early goal resuscitation – Appropriate antibiotics – Use of Activated Protein C – Hydrocortisone AND Early Pharmaconutrients Early EN
 How long do we allow the status quo remain? How many more Mr. KTs have to die before we do something to improve practice? Remember, the clock is ticking…
How long do we allow the status quo remain? How many more Mr. KTs have to die before we do something to improve practice? Remember, the clock is ticking…
 www. criticalcarenutrition. com
www. criticalcarenutrition. com
 Questions?
Questions?


