bb6195e252519a9cb60457ae5ef2417a.ppt
- Количество слайдов: 53

NPf. IT: The Biggest Computer Programme in the World Ever ! Sean Brennan Clinical Matrix

Why do the cows in the Isle of Man have better computers that the NHS?

But…………………. . • Daisy’s Record is a by-product. • The Primary objective is to milk her.

Why does my dog have a better electronic health record than I have?
Doggie Health Record Clinical History

So why do we need clinical IT?

Today in the NHS (England) • Will spend £ 170 million • £ 2000 every second • £ 10 million settling litigation claims • 110 people will die due to ‘adverse events’ • 1230 people will suffer an adverse event • 270 people will catch a hospital acquired infection • £ 2. 8 million on treating patients who have MRSA • £ 1. 3 million on treating patients who have had an adverse drug event

Today in the NHS (England) • 200, 000 people will get help in their home from the NHS • 1. 2 million will visit their GP’s • 160, 000 will be treated in NHS Outpatients • 140, 000 will visit an NHS dentist • Over 1400 babies will be born • NHS Direct will receive 3, 500 calls seeking advice • Labs will perform millions of tests The NHS is a very BUSY organisation. • 3 million critical processes each and every day. • If totally supported by electronic records that would be approx 30 MILLION new transactions each day!

So • Computerising the NHS is a very big and very difficult project. • But lets NOT just add technology to existing workflow……. Isn’t there a better way?

Spanish Brasero – wasted opportunity?

“Here is Edward Bear, coming downstairs now, bump, on the back of his head, behind Christopher Robin. It is, as far as he knows, the only way of coming downstairs, but sometimes he feels that there really is another way, if only he could stop bumping for a moment and think of it” A. A. Milne 1926 Illustration E. H. Shepard 192614

It’s about change • We need to change the way care is delivered • IT enables change to happen • The current model is no longer appropriate
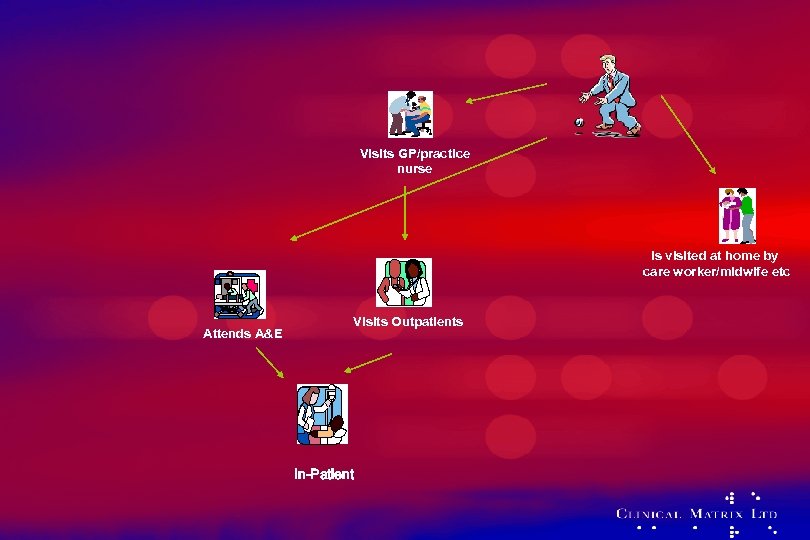
Visits GP/practice nurse Is visited at home by care worker/midwife etc Attends A&E Visits Outpatients In-Patient
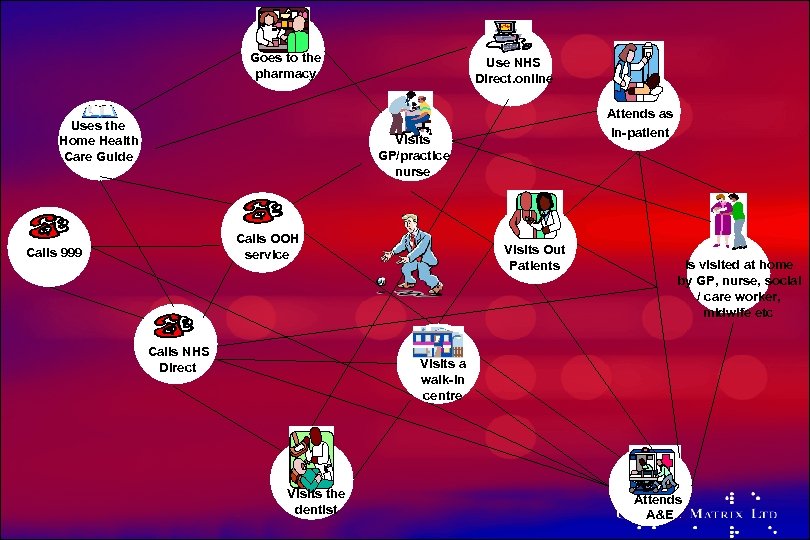
Goes to the pharmacy Uses the Home Health Care Guide Use NHS Direct. online Attends as in-patient Visits GP/practice nurse Calls OOH service Calls 999 Calls NHS Direct Visits Out Patients Is visited at home by GP, nurse, social / care worker, midwife etc Visits a walk-in centre Visits the dentist Attends A&E

We must use technology to support change Not just add technology to existing ways of working
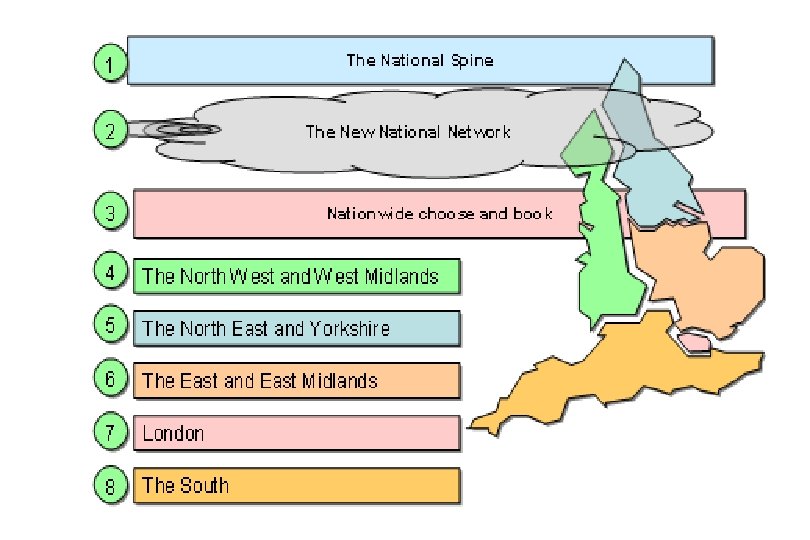
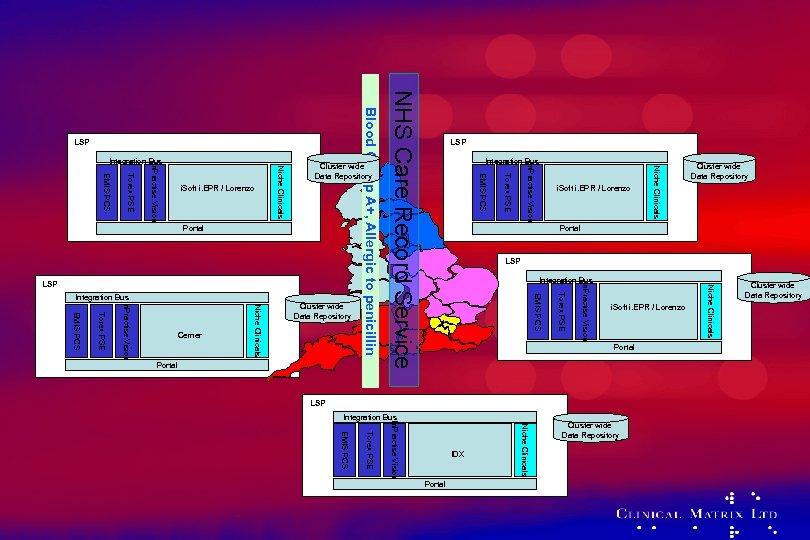
Niche Clinicals i. Soft i. EPR / Lorenzo Portal LSP IDX Portal Niche Clinicals Torex PSE EMIS PCS In. Practise Vision Integration Bus Cluster wide Data Repository Niche Clinicals Integration Bus In. Practise Vision Portal LSP Torex PSE Cluster wide Data Repository i. Soft i. EPR / Lorenzo Cluster wide Data Repository Portal EMIS PCS Cerner Niche Clinicals Torex PSE EMIS PCS In. Practise Vision Integration Bus In. Practise Vision LSP Integration Bus Torex PSE Portal LSP EMIS PCS Cluster wide Data Repository NHS Care Record Service i. Soft i. EPR / Lorenzo Niche Clinicals Torex PSE EMIS PCS In. Practise Vision Integration Bus Blood Group A+, Allergic to penicillin LSP Cluster wide Data Repository
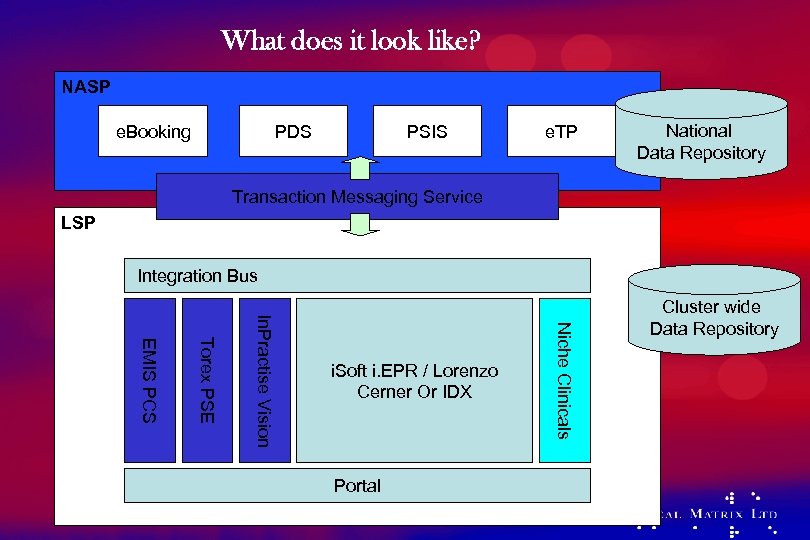
What does it look like? NASP e. Booking PDS PSIS e. TP National Data Repository Transaction Messaging Service LSP Integration Bus Portal Niche Clinicals In. Practise Vision Torex PSE EMIS PCS i. Soft i. EPR / Lorenzo Cerner Or IDX Cluster wide Data Repository
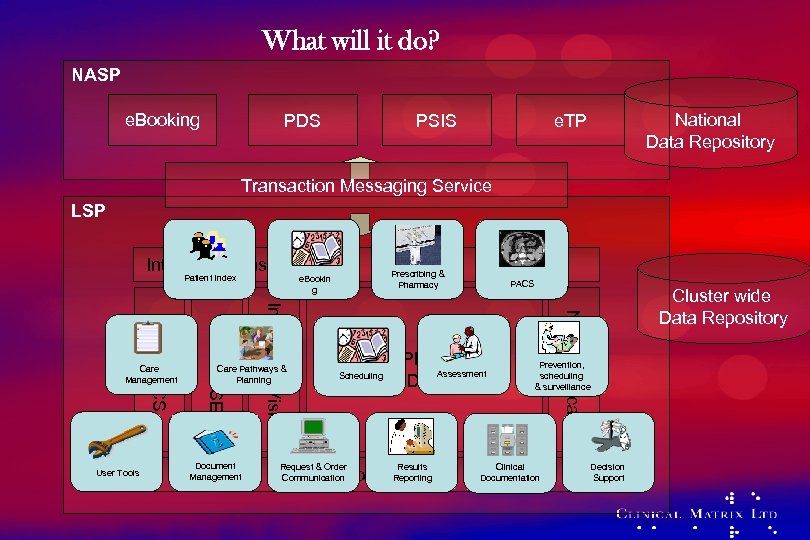
What will it do? NASP e. Booking PDS PSIS National Data Repository e. TP Transaction Messaging Service LSP Integration Bus Patient Index Care Pathways & Planning Document Management PACS i. Soft i. EPR / Lorenzo Assessment or IDX or ? Scheduling Request & Order Communication Results Portal Reporting Cluster wide Data Repository Niche Clinicals In. Practise Vision User Tools Torex PSE EMIS PCS Care Management Prescribing & Pharmacy e. Bookin g Prevention, scheduling & surveillance Clinical Documentation Decision Support

So what’s in it for you and your patients? • This is the biggest national clinical change programme ever carried out in the NHS • It will affect you and all your clinical colleagues • It will impact the way that you practice and improve the way you treat your patients by: – Ensuring that the right information is always available at the point of care – Making it easier and faster to book appointments order tests and see results, anywhere – Helping to ensure consistent good practice treatments – Reducing prescribing errors – Stops the paper chase. Making huge savings on the 30% of all NHS costs that are associated with recording, transporting, storing, and looking for information!

OK – so what do I get out of it? • Access to knowledge/guidelines • Real-time decision support • Access to ALL the patients information • Reduction in administrative data collection • Provide clinical information for secondary analysis • Reduce inappropriate referrals • Plan discharge • Opportunities to re-design the service

NCRS: What are the benefits?

Benefits………. • Access to clinical knowledge • Access to all the patients information • Better communications • Decision support • Easier ordering and prescribing • Access to digital images (X-Rays) • Care pathways and protocols • Quality clinical information for audit and research

Hospital discharge letters • Illegible • Written in haste • Arrive two weeks after discharge

Benefits: Access to knowledge

T’Internet The Good, the Bad and the Ugly

Benefits Reduce Illegibility

Illegible Writing kills Patients! • Doctors writing illegibly are still killing patients Advise doctors to write in CAPITAL LETTERS • It is writing in lower case in a hurry which causes mistakes Medical Defense Union in BMJ 1992; 305: 604

Benefits Decision Support

Prescription Error Rate Admission Drugs - 24% patients had 1 error (or more) - - 2 items in error per patient Discharge Drugs - 19% discharge prescriptions had error - - 1. 4 items in error per patient - 21. 5% patients had error in prescription on admission / discharge - 1. 7 items in error per patient Total Error Rate

Drug Errors: Causes • Human Factors • Labelling • Communication • Name Confusion • Package Design 42% 20% 19% 13% 6%

Advantages of Electronic Medicines Administration • Clarity • Schedule compliance • Audit trail • Alerts/Warnings

But……. . • Computer errors on the increase! – 46% errors in transcription and documentation phase – 36% errors at drug dispensing – 13% errors at prescription phase – 4% errors at drug administration • Automation does not equal safety. Training is an issue • Don Detmer: Properly structured automated systems can reduce error rates substantially. However, simply installing an automated system will not magically eliminate errors.

Benefits: Warnings

Useful Warnings ! • The drug you are about to give the patient will react with one they are already on. • The dose you are about to give the patient is incorrect for their body mass. • On bottom of Coke bottles – – Open other end

What will make it work? • What’s in it for me ? – Benefits to me as a clinician – Benefits to my patients – Benefits to my organisation • Is it easy to use? • Is it responsive? (i. e. quick!)

Making it easy to use The Interface: The London Underground

Ways to improve clinical data capture

User Interface • Touch Screens • Handwriting Recognition • Bar Codes • OCR Forms • Light Pens • Voice Recognition

Touch Screens for clinicians • In certain conditions excellent – Operating Theatres – Sterile Stores – Reception areas

Bar Codes • Invented in 1948 by Bernard Silver and Norman Woodland • 1949 first patent issued 1952 • Trial by Bar Codes? • But……. was it the Irish who invented it?

Bar Codes: Uses in healthcare • Drugs • Laboratories • Meals • Fluids • Positive Patient ID • X-Ray films

Light Pens • Rapid • Easy to use • Used at Wirral • Removes need for keyboard • Rapid (Did I say rapid? )

Optical Character Recognition • Useful for patients use – Complete data before consultation • Good for surveys • Where multiple data items are collected – Anaesthetic information in theatre • Paper is good !

Voice Recognition • Opportunities – Radiology – Pathology – Clinician Reporting • Discharge letters • Outpatient letters

1992 NHS IM&T Strategy Haven’t we been promised all this before? Why should we believe it this time?

This time…. . • Top of the office commitment • Huge increase in resources • Tight contracts • Buying a service not a single system • Local Service Providers accountable • Recognition that it is NOT just an IT project

But………………. . • Local Vs. . National • We MUST engage clinicians • We MUST be open and honest about timetable • We MUST acknowledge it is difficult AND different • We SHOULD ensure we have the right focus • We MUST learn from history

What annoys clinicians? • Change for the sake of change • Dodgy evidence • Quicker doesn’t always mean better • Systems that don’t fit clinical workflow • Feeding the beast • Slow systems • Not enough workstations • Interfering computers • Too many alerts • Complicated systems/poor user interface

Thank You Merry Christmas & Happy New year sean. brennan@clinicalmatrix. com
bb6195e252519a9cb60457ae5ef2417a.ppt