d2bf07be0cc0714b573b7d7f82194aea.ppt
- Количество слайдов: 13

Noninvasive brain stimulation in neurorehabilitation Disclosures Roy Hamilton, MD, MS • Medical consultant for Neuronix, Assistant Professor of Neurology & LTD, Israel Physical Medicine & Rehabilitation • Funding from NIH/NINDS, Director, Laboratory for Cognition & NIH/NIDCD, RWJF, Neural Stimulation Dana Foundation University of Pennsylvania

NIBS in post-stroke neurorehabilitation Post-Stroke Motor & Cognitive Deficits Visuospatial • Common and debilitating Neglect • Current therapies: Ineffective (at typical doses) • Recovery depends on network reorganization Aphasia Paresis

How do intact cognitive systems work? Reorganized How do. Systems injured systems differ from normal systems? NIBS in cognitive neurorehabilitation: Normal Systems a model system in translational Cognitive Outcomes Cancognitivereorganization of injured neural systems? we facilitate neuroscience Does it work? * Hypothesis-guided Opinions in Neurobiology, 2014 Poeppel D. , Current Neuromodulation et al. Neurology, 2011 Turkeltaub
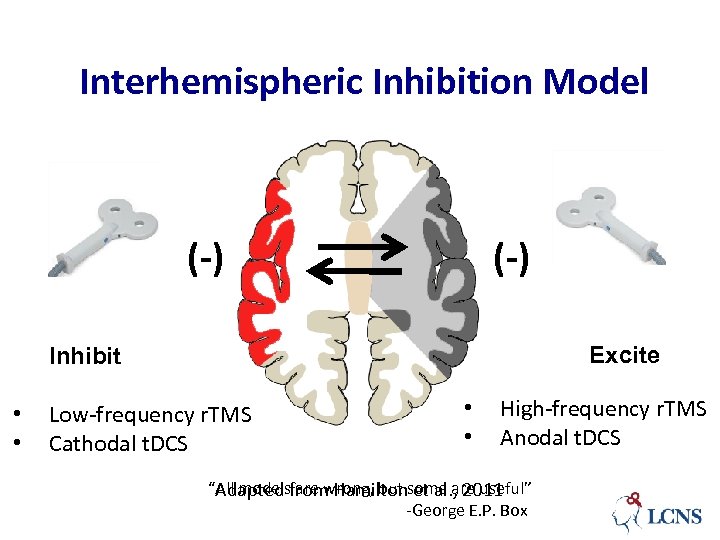
Interhemispheric Inhibition Model (-) Excite Inhibit • • Low-frequency r. TMS Cathodal t. DCS • • High-frequency r. TMS Anodal t. DCS “All modelsfrom Hamiltonsome are useful” Adapted are wrong, but et al. , 2011 -George E. P. Box
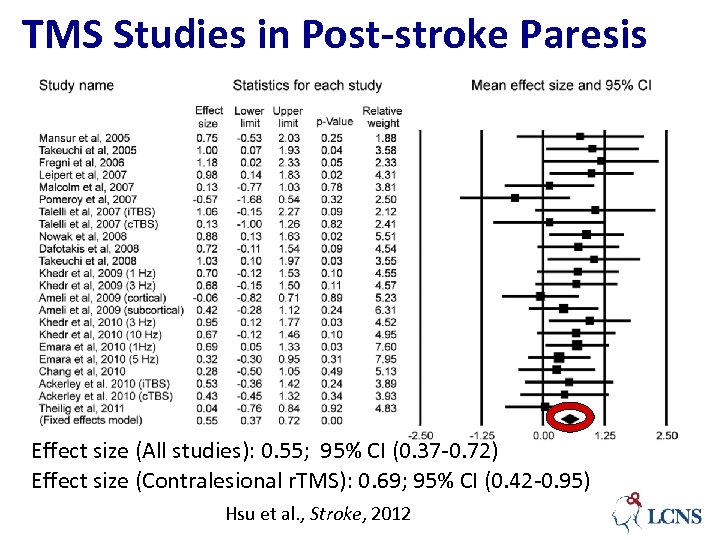
TMS Studies in Post-stroke Paresis Effect size (All studies): 0. 55; 95% CI (0. 37 -0. 72) Effect size (Contralesional r. TMS): 0. 69; 95% CI (0. 42 -0. 95) Hsu et al. , Stroke, 2012
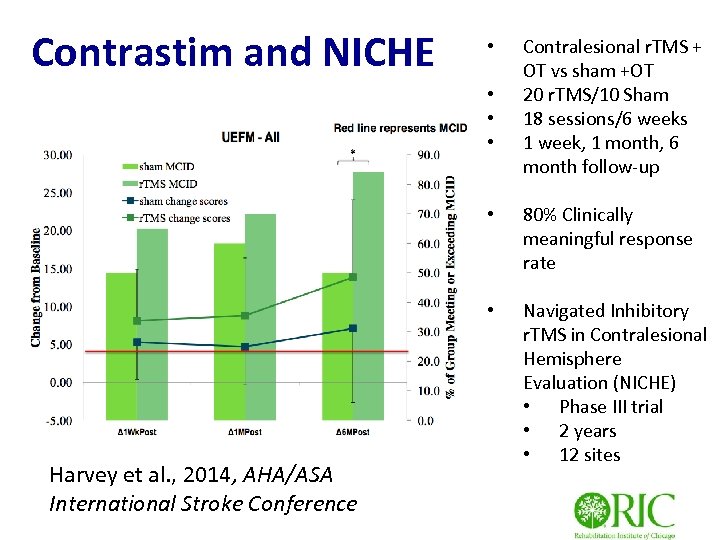
Contrastim and NICHE • • Contralesional r. TMS + OT vs sham +OT 20 r. TMS/10 Sham 18 sessions/6 weeks 1 week, 1 month, 6 month follow-up • • Harvey et al. , 2014, AHA/ASA International Stroke Conference 80% Clinically meaningful response rate Navigated Inhibitory r. TMS in Contralesional Hemisphere Evaluation (NICHE) • Phase III trial • 2 years • 12 sites
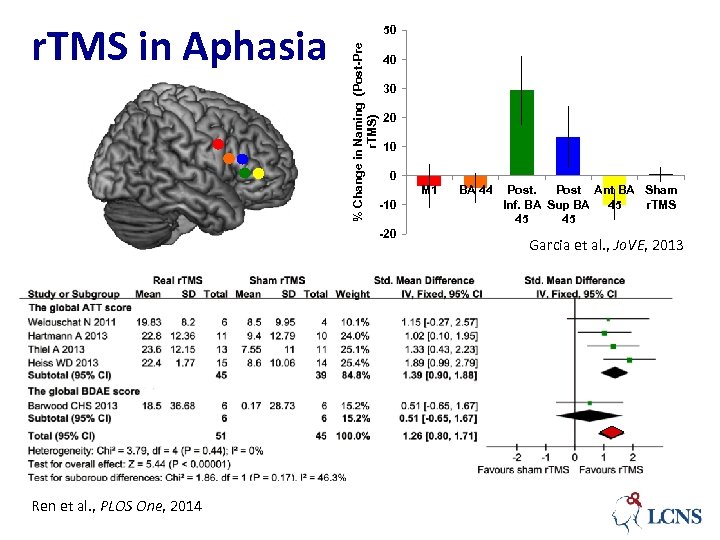
% Change in Naming (Post-Pre r. TMS) r. TMS in Aphasia 50 40 30 20 10 0 M 1 -10 -20 Ren et al. , PLOS One, 2014 BA 44 Post Ant BA Sham Inf. BA Sup BA 45 r. TMS 45 45 Garcia et al. , Jo. VE, 2013
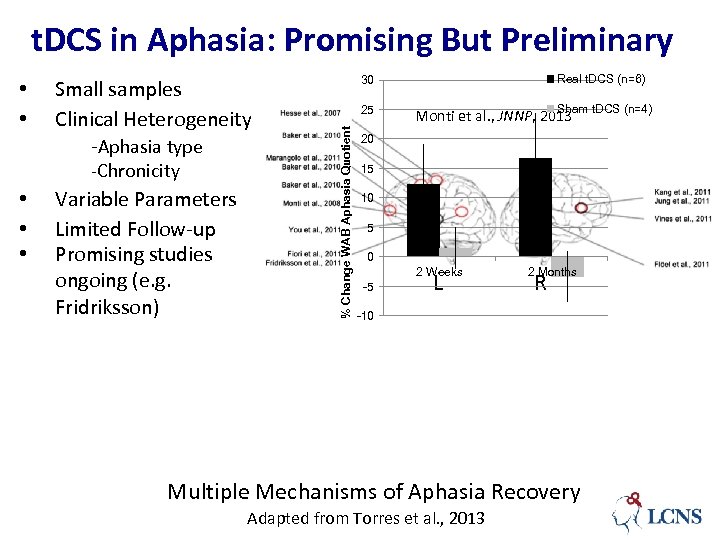
t. DCS in Aphasia: Promising But Preliminary Small samples Clinical Heterogeneity -Aphasia type -Chronicity • • • Variable Parameters Limited Follow-up Promising studies ongoing (e. g. Fridriksson) 25 % Change WAB Aphasia Quotient • • Real t. DCS (n=6) 30 Sham Monti et al. , JNNP, 2013 t. DCS (n=4) 20 15 10 5 0 2 Weeks -5 L 2 Months R -10 Multiple Mechanisms of Aphasia Recovery Adapted from Torres et al. , 2013
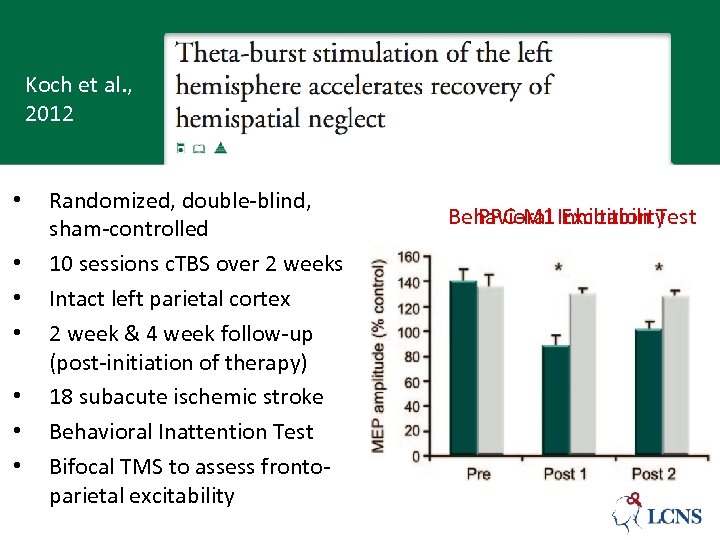
Koch et al. , 2012 • • Randomized, double-blind, sham-controlled 10 sessions c. TBS over 2 weeks Intact left parietal cortex 2 week & 4 week follow-up (post-initiation of therapy) 18 subacute ischemic stroke Behavioral Inattention Test Bifocal TMS to assess frontoparietal excitability PPC-M 1 Excitability Behavioral Inhibition Test
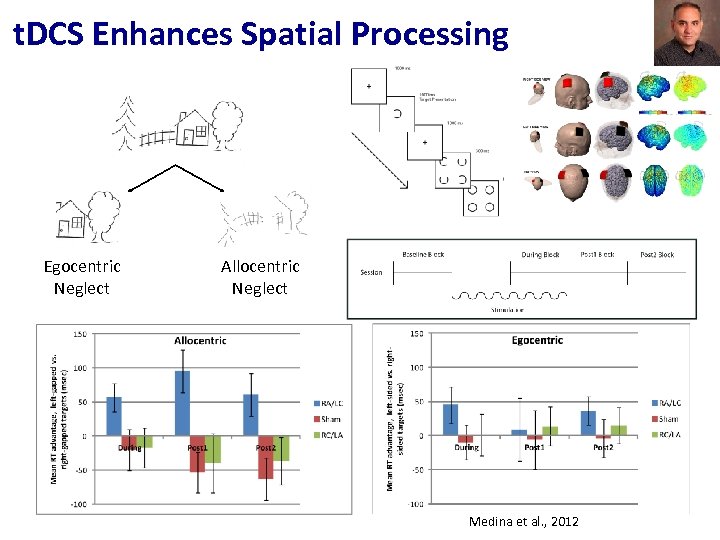
t. DCS Enhances Spatial Processing Egocentric Neglect Allocentric Neglect Medina et al. , 2012

Challenges to NIBS in Rehab • No FDA-approved rehab indications to date • Much research at proof-of-concept stage Challenges to clinical development of TMS/t. DCS • Phase I: • Dose-effect relationships • Testing of potentially risky populations • Phase II/III: • Recruitment/eligibility challenges • Heterogeneous patient populations • Multiple sessions & attrition • Phase III: • Control group and blinding issues • Heterogeneity of approaches • Small sample sizes/single sites FDA Clinical Trial Phases: Phase I: Screening for safety Phase II: Smaller, controlled trials of efficacy Phase III: Pivotal larger studies of safety and efficacy* *Two positive phase III trials are required for FDA approval.

Other applications in brain injury • TMS as a prognostic indicator of stroke outcomes – Motor tract patency – Marker of plasticity • TMS pre-surgical mapping of motor function and language • NIBs to treat motor, cognitive, neuropsychological disorders associated with TBI

Faculty Roy Hamilton, MD, MS H. Branch Coslett, MD Sudha Kessler, MD Postdoctoral Fellows Rachel Wurzman, Ph. D Denise Harvey, Ph. D John Megdaglia, Ph. D Students Perelman School Of Medicine Catherine Norise Harrison Mc. Adams Penn School of Nursing Darina Petrovsky, MSN Undergraduates Jay Gill Jill Sorcher Trevin Glasgow Menvekeh Daramay Follow us on Twitter @Penn. Med. LCNS email: braintms@mail. med. upenn. edu LCNS website: http: //www. med. upenn. edu/lcns Collaborators Priyanka Shah-Basak, Ph. D Peter Turkeltaub, MD, Ph. D (Georgetown) Jared Medina, Ph. D (U. Delaware) Margaret Naeser, Ph. D (Boston University) Alvaro Pascual-Leone, MD, Ph. D (Harvard) Research Staff Olufunsho Faseyitan, MS Daniela Sacchetti, MS Juliann Purcell, MSc Felix Gervits, MA
d2bf07be0cc0714b573b7d7f82194aea.ppt