9a7ab7ba2e7920c0d3f94a25afd84b5d.ppt
- Количество слайдов: 52

NEWBORN INFANT SCREENING AND ASSESSMENT: Emerging Technologies and Protocols James W. Hall III, Ph. D. Clinical Professor and Chair Department of Communicative Disorders College of Health Professions University of Florida Gainesville, Florida 32610 -0174 Jhall@hp. ufl. edu
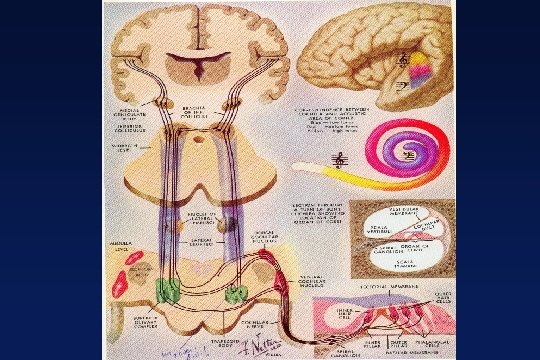

Marion Downs “Grandmother of Newborn Hearing Screening”

Year 2000 JCIH Position Statement: Principles and Guidelines for Early Hearing Detection and Intervention Programs q JCIH = Joint Committee on Infant Hearing q Published in: l Audiology Today (Special Issue): August 2000, pp. 6 -27 l American Journal of Audiology 9: 9 -29, 2000. l www. audiology. org q Member organizations: l American Academy of Audiology & ASHA l American Academy of Otolaryngology-Head & Neck Surgery l American Academy of Pediatrics l Council on Education of the Deaf l Directors of Speech and Hearing Programs in State and Welfare Agencies

JCIH Risk Indicators for Hearing Impairment: Birth to 29 Days q Illness or condition requiring admission of > 48 hours to an NICU. q Stigmata or other findings associated with a syndrome known to include a sensorineural or conductive hearing loss. q Family history of permanent childhood sensorineural hearing loss q Craniofacial anomalies, including those with morphological abnormalities of pinna and ear canal q In-utero infection such as cytomegalovirus, herpes, toxoplasmosis, or rubella

JCIH Risk Indicators for Hearing Impairment: 29 Days to 2 Years (1) q Parental or caregiver concern regarding hearing, speech, language, and or developmental delay q Family history of permanent childhood hearing loss q Stigmata or other findings associated with a syndrome known to include a sensorineural or conductive hearing loss. q Postnatal infections associated with sensorineural hearing loss including bacterial meningitis q In-utero infection such as cytomegalovirus, herpes, toxoplasmosis, rubella, syphilis

JCIH Risk Indicators for Hearing Impairment: 29 Days to 2 Years (2) q Neonatal indicators, specifically hyperbilirubinemia at a serum level requiring exchange transfusion, persistent pulmonary hypertension of the newborn associated with mechanical ventilation, and conditions requiring extracorporeal membrane oxygenation q Syndromes associated with progressive hearing loss, such as neurofibromatosis, osteopetrosis, and Usher’s syndrome q Neurodegenerative disorders, such as Hunter syndrome, or sensory motor neuropathies, such as Friedreich’s ataxia q Head trauma q Recurrent or persistent otitis media with effusion for at least 3 months
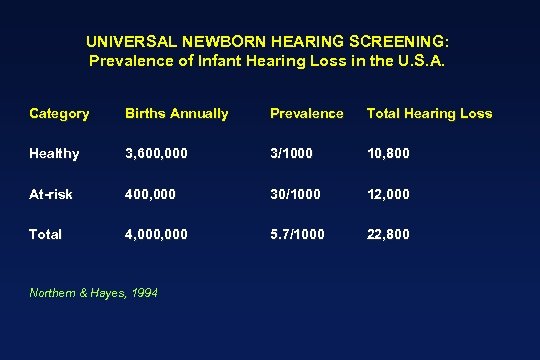
UNIVERSAL NEWBORN HEARING SCREENING: Prevalence of Infant Hearing Loss in the U. S. A. Category Births Annually Prevalence Total Hearing Loss Healthy 3, 600, 000 3/1000 10, 800 At-risk 400, 000 30/1000 12, 000 Total 4, 000 5. 7/1000 22, 800 Northern & Hayes, 1994

Universal Newborn Hearing Screening: Turning Point in the United States of America

UNIVERSAL NEWBORN HEARING SCREENING: Recent Events in the U. S. A. q 1975 -1985: Hearing screening of at risk infants with ABR q 1993: National Institutes of Health Consensus Conference on Early Identification of Hearing Impairment in Children q 1994: Joint Committee on Infant Hearing (JCIH) Position Statement (recommending ABR and OAE techniques) q 1998: Yoshinaga-Itano et al. Language of early and later identified children with hearing loss. Pediatrics 102. q 1999: American Academy of Pediatrics Task Force on Newborn and Infant Hearing Screening: Diagnosis and intervention. Pediatrics 103. q 2000: JCIH Position Statement. Principles and Guidelines for Early Hearing Detection & Intervention Programs.

UNIVERSAL NEWBORN HEARING SCREENING: Converging Trends in 1990 s q Automated OAE and ABR devices manufactured for newborn hearing screening q Evidence of low “refer” rates (< 4%) q Evidence of low false-positive rates (< 2%) q Documentation of benefits of early intervention (before 6 months) q Successful implementation of UNHS in selected states

EARLY IDENTIFICATION OF AND INTERVENTION FOR HEARING IMPAIRMENT IN CHILDREN q "Hearing loss of 30 d. B HL and greater in the frequency region important for speech recognition will interfere with the normal development of speech and language. q "Techniques used to assess hearing of infants must be capable of detecting hearing loss of this degree in infants by age three months and younger. q Of the various approaches to newborn hearing assessment currently available, two physiologic measures. . . auditory brainstem response (ABR) and otoacoustic emissions (OAE). . . show good promise for achieving this goal" Joint Committee on Infant Hearing 1994 Position Statement
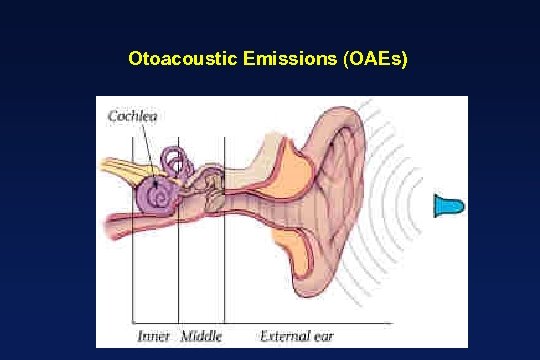
Otoacoustic Emissions (OAEs)
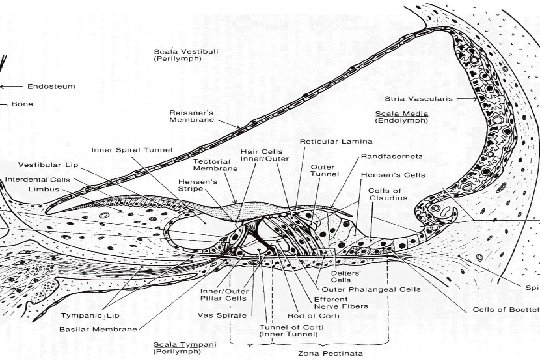
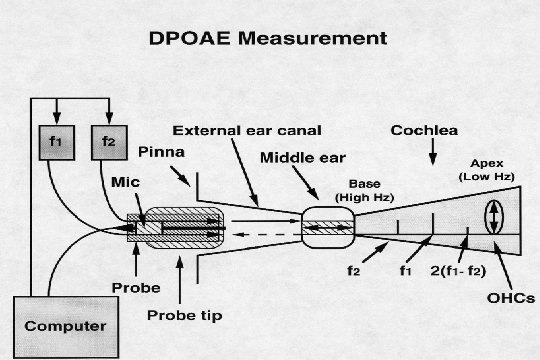
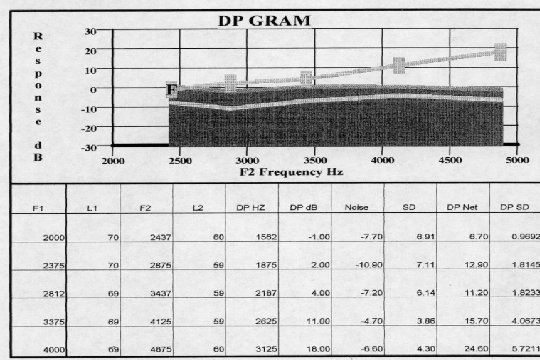

NEWBORN HEARING SCREENING: OTOACOUSTIC EMISSIONS q Vohr et al. The Rhode Island Hearing Assessment Program: Experience with statewide hearing screening (1993 -1996). Journal of Pediatrics 133: 353 -357, 1998 l 53, 121 babies underwent screening (NICU =5130) l average initial failure rate = 10% l failure rate for rescreens at 2 to 6 weeks = 14. 7% l over failure (refer) rate = 1. 2% l 111 infants identified with permanent hearing loss l average of intervention (amplification) = 5. 7 months

Auditory Brainstem Response (ABR)
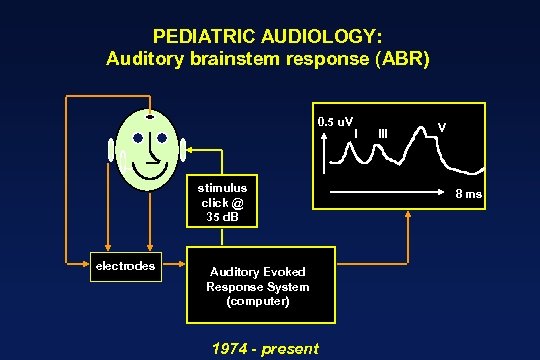
PEDIATRIC AUDIOLOGY: Auditory brainstem response (ABR) 0. 5 u. V stimulus click @ 35 d. B electrodes Auditory Evoked Response System (computer) 1974 - present I III V 8 ms

UNIVERSAL NEWBORN HEARING SCREENING WITH AUTOMATED AUDITORY BRAINSTEM RESPONSE (AABR): A MULTI-SITE INVESTIGATION J Perinatology 20 ((8): S 128, December 2000. James W. Hall III, Ph. D. University of Florida Gainesville, Florida, U. S. A. Dan Stewart, M. D. Kosair Children’s Hospital Louisville, Kentucky Albert Mehl, M. D. Boulder Community Hospital Boulder, Colorado Mark Carroll, M. S. E. N. T. Associates Huntsville, Alabama Vicki Thomson, M. A. Boulder Community Hospital Boulder, Colorado James Hamlett, M. D. Baptist Memorial Hospital East Memphis, Tennessee
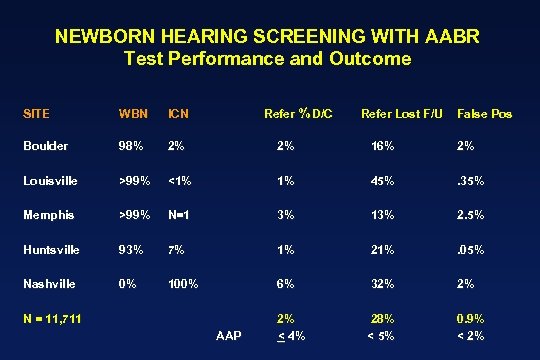
NEWBORN HEARING SCREENING WITH AABR Test Performance and Outcome Refer % D/C SITE WBN ICN Boulder 98% 2% 2% 16% 2% Louisville >99% <1% 1% 45% . 35% Memphis >99% N=1 3% 13% 2. 5% Huntsville 93% 7% 1% 21% . 05% Nashville 0% 100% 6% 32% 2% 2% < 4% 28% < 5% 0. 9% < 2% N = 11, 711 AAP Refer Lost F/U False Pos
Combination Device for Newborn Hearing Screening and Diagnosis with OAEs and ABR: Audio. Screener by Grason Stadler

Rationale for Combined OAE/ABR Screening q In ear calibration of signal intensity (OAE and ABR) q Lower refer (< 2%) and false-positive rates (< 0. 2%) q Minimal parental anxiety q Fewer diagnostic follow-ups with lower costs q Less hearing impaired infants lost to follow-up q Differentiation of conductive vs. sensory vs. neural auditory dysfunction q Quicker and more appropriate management q Identification of auditory neuropathy q Earlier identification of hearing impairment
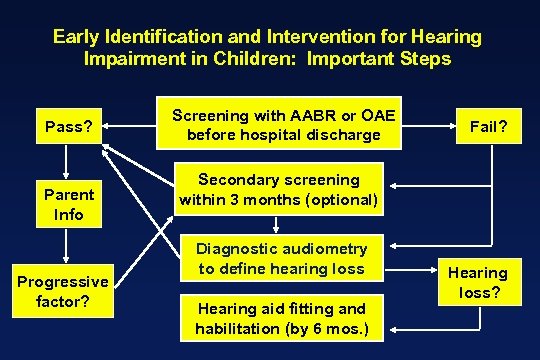
Early Identification and Intervention for Hearing Impairment in Children: Important Steps Pass? Parent Info Progressive factor? Screening with AABR or OAE before hospital discharge Fail? Secondary screening within 3 months (optional) Diagnostic audiometry to define hearing loss Hearing aid fitting and habilitation (by 6 mos. ) Hearing loss?

Year 2000 JCIH Position Statement: Protocol for Confirmation of Hearing Loss In Infants and Toddlers (0 to 6 months) q Child and family history q Otoacoustic emissions q ABR during initial evaluation to confirm type, degree & configuration of hearing loss (ASSR? ) q Acoustic immittance measures (including acoustic reflexes) q Behavioral response audiometry (if feasible) üVisual reinforcement audiometry or üConditioned play audiometry üSpeech detection and recognition q Parental report of auditory & visual behaviors q Screening of infant’s communication milestones

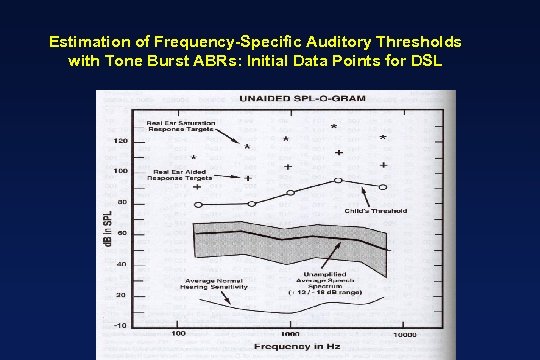
Estimation of Frequency-Specific Auditory Thresholds with Tone Burst ABRs: Initial Data Points for DSL
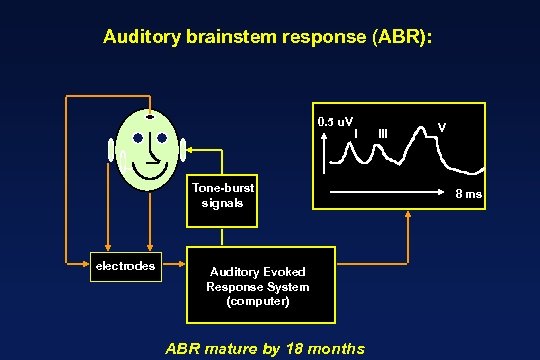
Auditory brainstem response (ABR): 0. 5 u. V I Tone-burst signals electrodes Auditory Evoked Response System (computer) ABR mature by 18 months III V 8 ms
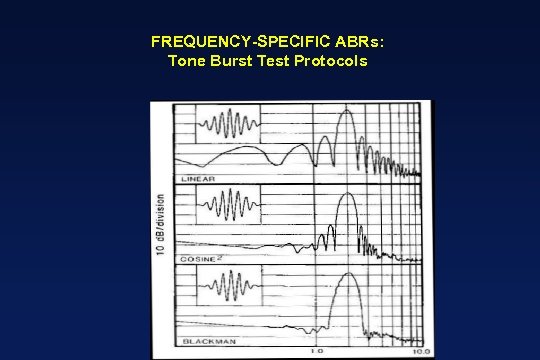
FREQUENCY-SPECIFIC ABRs: Tone Burst Test Protocols
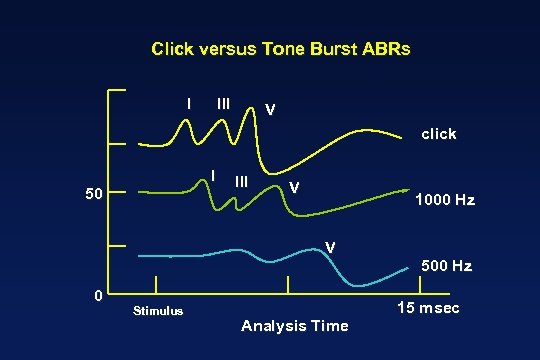
Click versus Tone Burst ABRs I III V click I 50 III V 1000 Hz V 0 Stimulus Analysis Time 500 Hz 15 msec
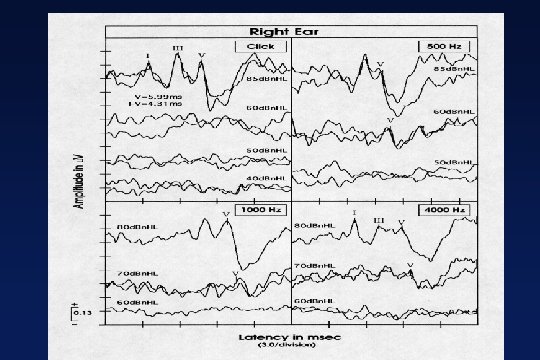
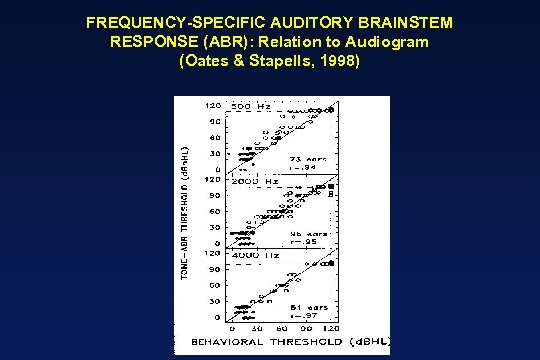
FREQUENCY-SPECIFIC AUDITORY BRAINSTEM RESPONSE (ABR): Relation to Audiogram (Oates & Stapells, 1998)
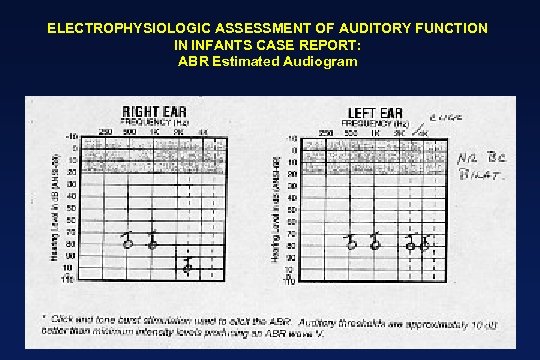
ELECTROPHYSIOLOGIC ASSESSMENT OF AUDITORY FUNCTION IN INFANTS CASE REPORT: ABR Estimated Audiogram
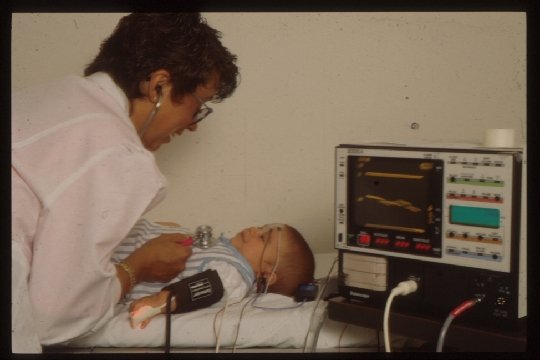

Auditory Steady-State Response (ASSR): General Principles q An electrophysiologic response, similar to ABR. q Instrumentation includes: l Insert earphones l Surface electrodes l Averaging computer q Stimuli are pure tones (frequency specific, steady state signals) activating cochlea and CNS q ASSR is generated by rapid modulation of “carrier” pure tone amplitude (AM) or frequency (FM). q Signal intensity can be as high as 120 d. B HL q ASSR phase or frequency is detected automatically (vs. visual detection)

Auditory Steady State Response (ASSR): Clinical Devices q GSI VIASYS l Audera l Descendant of Melbourne Australia system Field (Rickards, Gary Rance, Barbara Cone-Wesson, et al) q Bio-Logic Systems Inc. l. MASTER l. Descendent of Canadian system (Terry Picton et al)


ASSR: 2000 Hz tone modulated at rate of 100 Hz
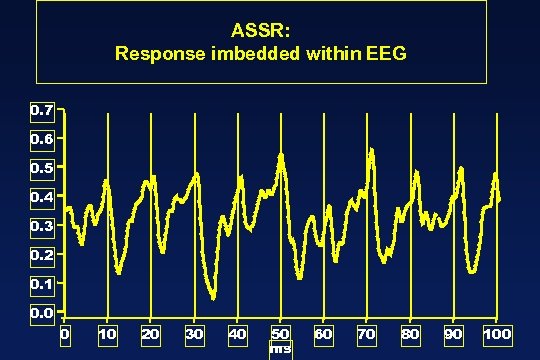
ASSR: Response imbedded within EEG 0. 7 0. 6 0. 5 0. 4 0. 3 0. 2 0. 1 0. 0 0 10 20 30 40 50 ms 60 70 80 90 100
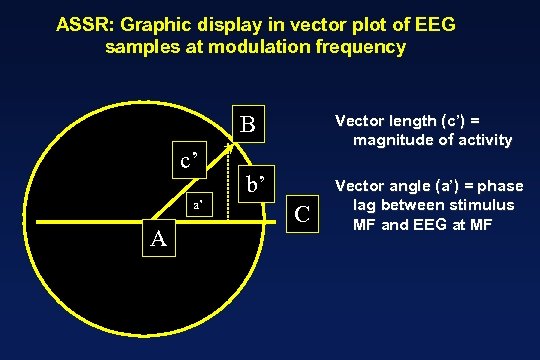
ASSR: Graphic display in vector plot of EEG samples at modulation frequency B c’ a’ A Vector length (c’) = magnitude of activity b’ C Vector angle (a’) = phase lag between stimulus MF and EEG at MF
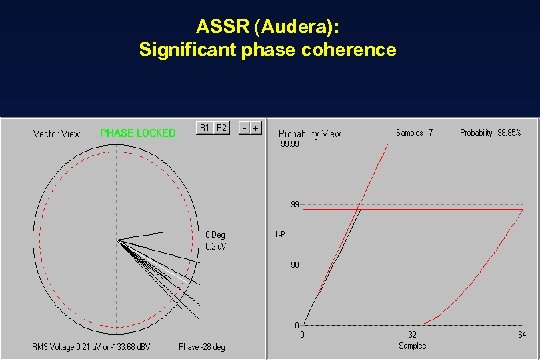
ASSR (Audera): Significant phase coherence
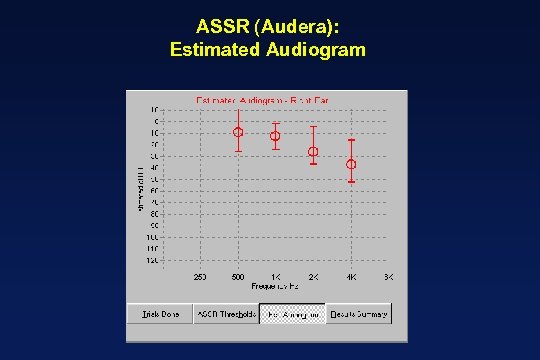
ASSR (Audera): Estimated Audiogram
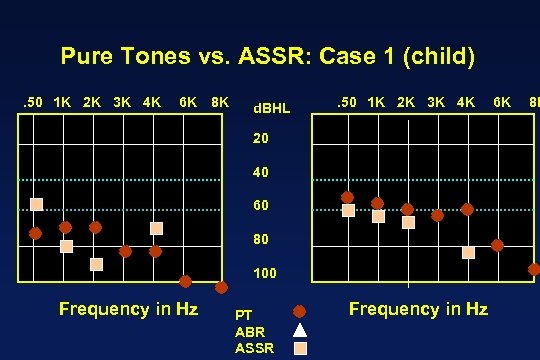
Pure Tones vs. ASSR: Case 1 (child). 50 1 K 2 K 3 K 4 K 6 K 8 K d. BHL . 50 1 K 2 K 3 K 4 K 20 40 60 80 100 Frequency in Hz PT ABR ASSR Frequency in Hz 6 K 8 K
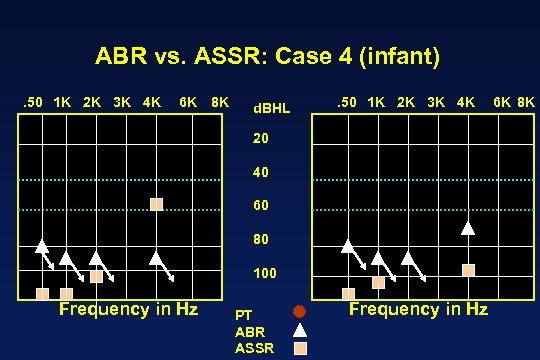
ABR vs. ASSR: Case 4 (infant). 50 1 K 2 K 3 K 4 K 6 K 8 K d. BHL . 50 1 K 2 K 3 K 4 K 20 40 60 80 100 Frequency in Hz PT ABR ASSR Frequency in Hz 6 K 8 K
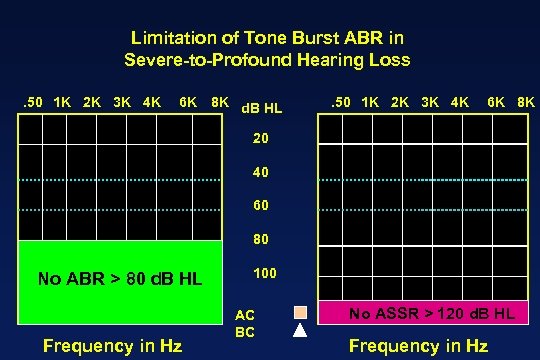
Limitation of Tone Burst ABR in Severe-to-Profound Hearing Loss. 50 1 K 2 K 3 K 4 K 6 K 8 K d. B HL . 50 1 K 2 K 3 K 4 K 6 K 8 K 20 40 60 80 No ABR > 80 d. B HL Frequency in Hz 100 AC BC No ASSR > 120 d. B HL Frequency in Hz
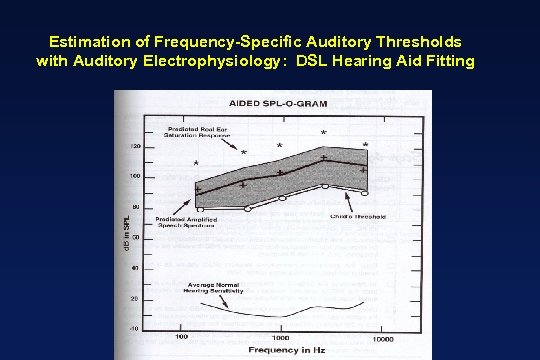
Estimation of Frequency-Specific Auditory Thresholds with Auditory Electrophysiology: DSL Hearing Aid Fitting


Early Intervention for Infant Hearing Impairment: Amplification
Management of Infant Hearing Loss: Cochlear Implants

Newborn Hearing Screening and Assessment: Conclusions q Universal newborn hearing screening is feasible with automated OAE and ABR technology q Estimation of hearing thresholds (audiogram) is possible in infants with electrophysiologic techniques l. ABRs evoked by tone burst stimuli l. Auditory steady-state response (ASSR) q Intervention with hearing aids can be implemented early (before 6 months) q Cochlear implant candidacy can be determined during infancy q Early intervention leads to normal language development
9a7ab7ba2e7920c0d3f94a25afd84b5d.ppt