b2557e63772280e751a9d1e78dbde4b8.ppt
- Количество слайдов: 37
 New challenges and opportunities in organ donation Dr Paul Murphy National Clinical Lead for Organ Donation NHS Blood and Transplant 1
New challenges and opportunities in organ donation Dr Paul Murphy National Clinical Lead for Organ Donation NHS Blood and Transplant 1
 Outline • Performance 2013/14 • Updates – – – Ante mortem interventions DCD heart retrieval Extended DCD Anencephaly Neurological determination of death in infants < 2 months – Challenges to neurological determination of death • Current strategies – – Family refusal DCD triage Organ utilisation Regional Collaboratives
Outline • Performance 2013/14 • Updates – – – Ante mortem interventions DCD heart retrieval Extended DCD Anencephaly Neurological determination of death in infants < 2 months – Challenges to neurological determination of death • Current strategies – – Family refusal DCD triage Organ utilisation Regional Collaboratives
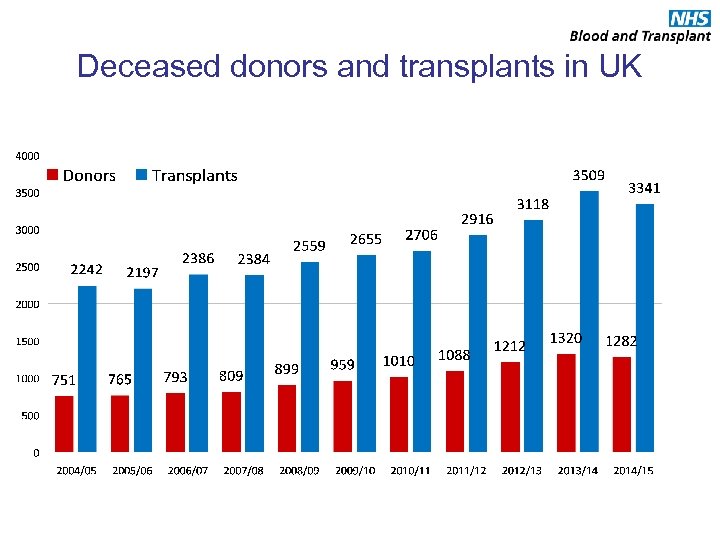 Deceased donors and transplants in UK
Deceased donors and transplants in UK
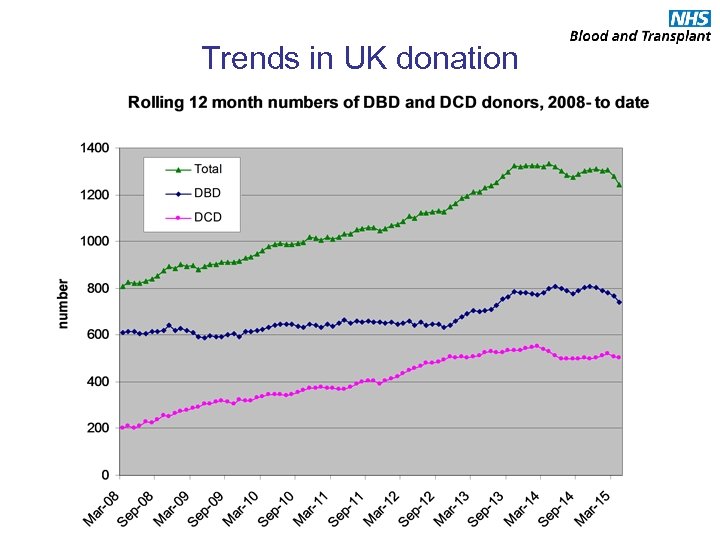 Trends in UK donation
Trends in UK donation
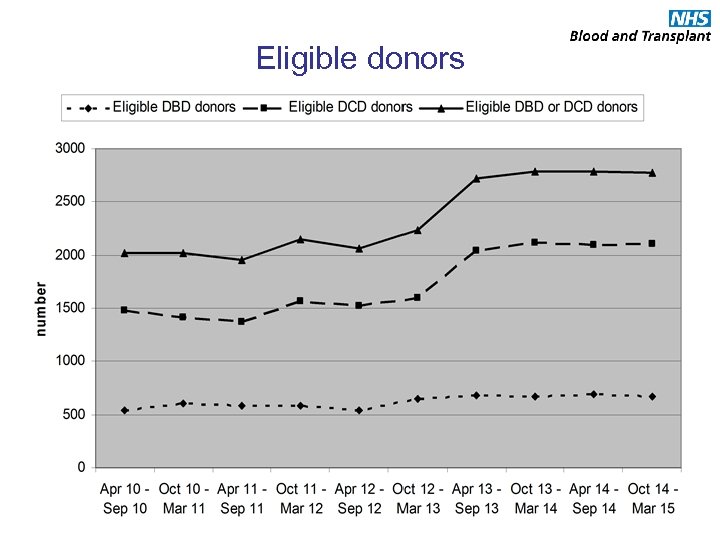 Eligible donors
Eligible donors
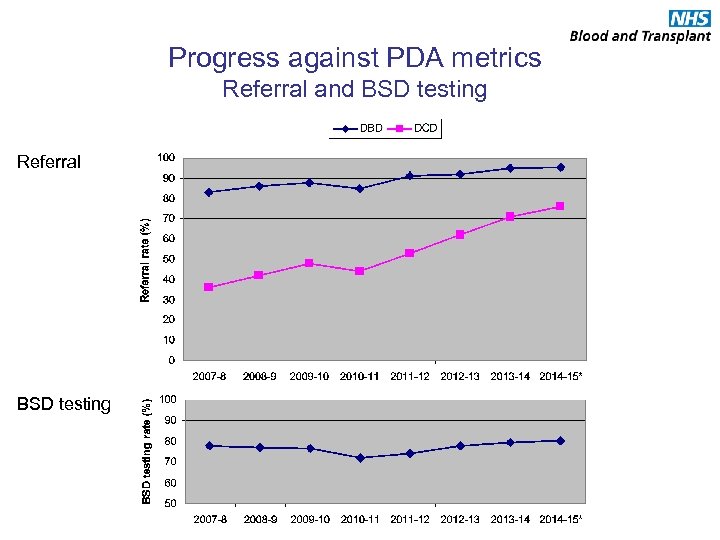 Progress against PDA metrics Referral and BSD testing Referral BSD testing
Progress against PDA metrics Referral and BSD testing Referral BSD testing
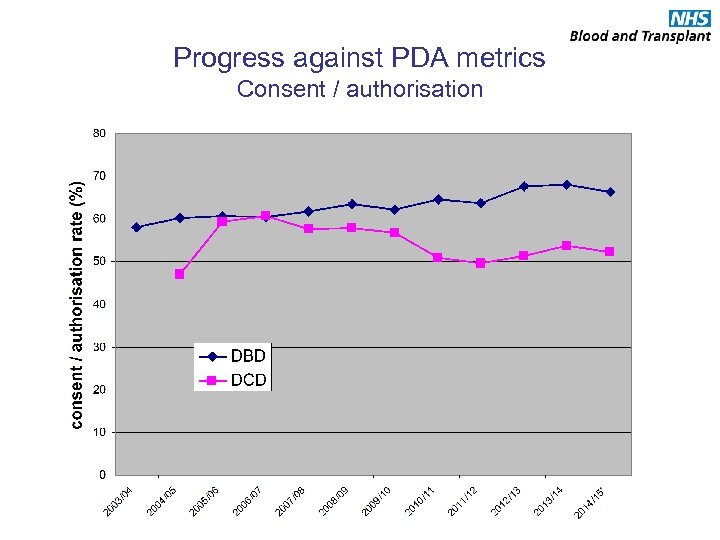 Progress against PDA metrics Consent / authorisation
Progress against PDA metrics Consent / authorisation
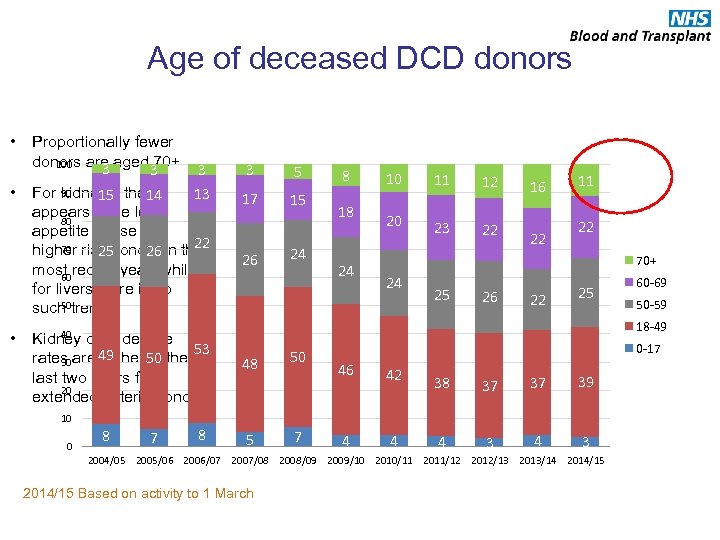 Age of deceased DCD donors • • • Proportionally fewer donors are aged 70+ 100 3 3 3 For 90 kidneys, there 13 14 15 appears to be less 80 appetite to use the 22 70 higher risk donors in the 26 25 most recent year, while 60 for livers there is no 50 such trend. 3 5 17 15 26 24 8 18 24 10 11 12 20 23 22 16 22 11 22 70+ 24 25 26 22 25 10 0 8 7 8 50 -59 18 -49 40 Kidney offer decline 53 rates are 49 higher 50 the in 30 last two years for 20 extended criteria donors. 60 -69 48 5 50 7 0 -17 46 42 38 37 37 39 4 4 4 3 2004/05 2005/06 2006/07 2007/08 2008/09 2009/10 2010/11 2011/12 2012/13 2013/14 2014/15 Based on activity to 1 March
Age of deceased DCD donors • • • Proportionally fewer donors are aged 70+ 100 3 3 3 For 90 kidneys, there 13 14 15 appears to be less 80 appetite to use the 22 70 higher risk donors in the 26 25 most recent year, while 60 for livers there is no 50 such trend. 3 5 17 15 26 24 8 18 24 10 11 12 20 23 22 16 22 11 22 70+ 24 25 26 22 25 10 0 8 7 8 50 -59 18 -49 40 Kidney offer decline 53 rates are 49 higher 50 the in 30 last two years for 20 extended criteria donors. 60 -69 48 5 50 7 0 -17 46 42 38 37 37 39 4 4 4 3 2004/05 2005/06 2006/07 2007/08 2008/09 2009/10 2010/11 2011/12 2012/13 2013/14 2014/15 Based on activity to 1 March
 Some features of current position • 7% fall in donor numbers from peak – Both DBD and DCD • No substantial deterioration in donor pool, referral or testing – Possible small fall in DBD pool – 25% of potential DCD not referred • Little progress with consent / authorisation – Slight fall in both DBD and DCD in 2014/15 • More cautious approach to older / higher risk kidney donors – Kidney offer decline rates are higher in the last two years for extended criteria donors DRAFT
Some features of current position • 7% fall in donor numbers from peak – Both DBD and DCD • No substantial deterioration in donor pool, referral or testing – Possible small fall in DBD pool – 25% of potential DCD not referred • Little progress with consent / authorisation – Slight fall in both DBD and DCD in 2014/15 • More cautious approach to older / higher risk kidney donors – Kidney offer decline rates are higher in the last two years for extended criteria donors DRAFT
 Update: ante mortem interventions in DCD • Legal guidance issued in 2009 - 11 – Conservative – Effective prohibition on ante-mortem heparin • Call for revision in 2012 / 2013 by UK DEC – Generic overarching guidance – Separate documents covering specific interventions (e. g. heparin, extubation) – Specific recommendations regarding heparin • Further evidence required by Department of Health – Risks and benefits – Clinical and public acceptability – NHSBT asked to conduct this review
Update: ante mortem interventions in DCD • Legal guidance issued in 2009 - 11 – Conservative – Effective prohibition on ante-mortem heparin • Call for revision in 2012 / 2013 by UK DEC – Generic overarching guidance – Separate documents covering specific interventions (e. g. heparin, extubation) – Specific recommendations regarding heparin • Further evidence required by Department of Health – Risks and benefits – Clinical and public acceptability – NHSBT asked to conduct this review
 Physiological changes following treatment withdrawal • Can a point of ‘no-return’ be identified following treatment withdrawal? – Does the patient always die if BP goes below a certain level? – Does donation always happen if BP goes below a certain level? • Is there time to give heparin once point of no return is identified for it to have a systemic effect? • What happens to non-proceeding DCD donors? – Do all potential DCD donors die following treatment withdrawal?
Physiological changes following treatment withdrawal • Can a point of ‘no-return’ be identified following treatment withdrawal? – Does the patient always die if BP goes below a certain level? – Does donation always happen if BP goes below a certain level? • Is there time to give heparin once point of no return is identified for it to have a systemic effect? • What happens to non-proceeding DCD donors? – Do all potential DCD donors die following treatment withdrawal?
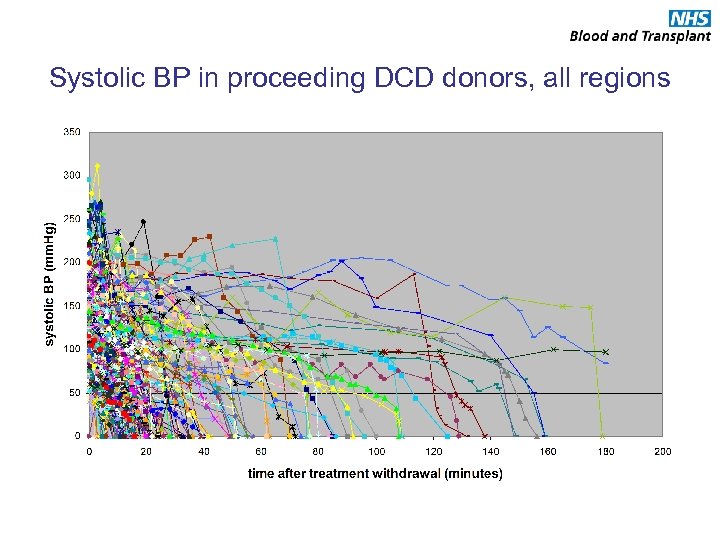 Systolic BP in proceeding DCD donors, all regions
Systolic BP in proceeding DCD donors, all regions
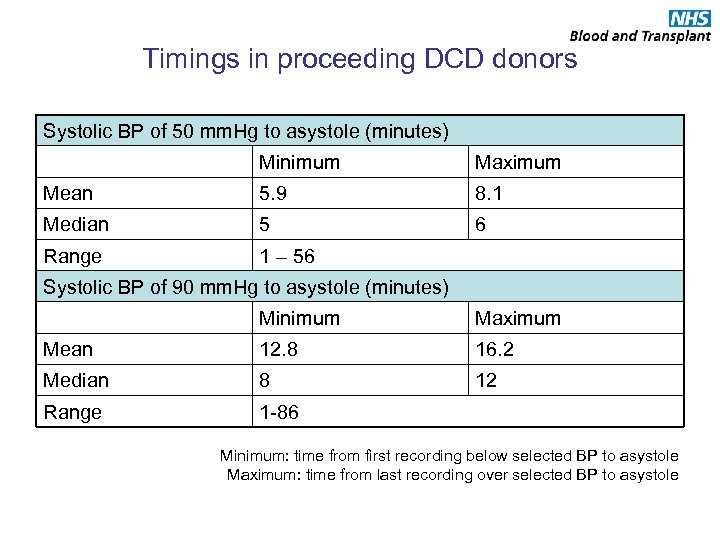 Timings in proceeding DCD donors Systolic BP of 50 mm. Hg to asystole (minutes) Minimum Maximum Mean 5. 9 8. 1 Median 5 6 Range 1 – 56 Systolic BP of 90 mm. Hg to asystole (minutes) Minimum Maximum Mean 12. 8 16. 2 Median 8 12 Range 1 -86 Minimum: time from first recording below selected BP to asystole Maximum: time from last recording over selected BP to asystole
Timings in proceeding DCD donors Systolic BP of 50 mm. Hg to asystole (minutes) Minimum Maximum Mean 5. 9 8. 1 Median 5 6 Range 1 – 56 Systolic BP of 90 mm. Hg to asystole (minutes) Minimum Maximum Mean 12. 8 16. 2 Median 8 12 Range 1 -86 Minimum: time from first recording below selected BP to asystole Maximum: time from last recording over selected BP to asystole
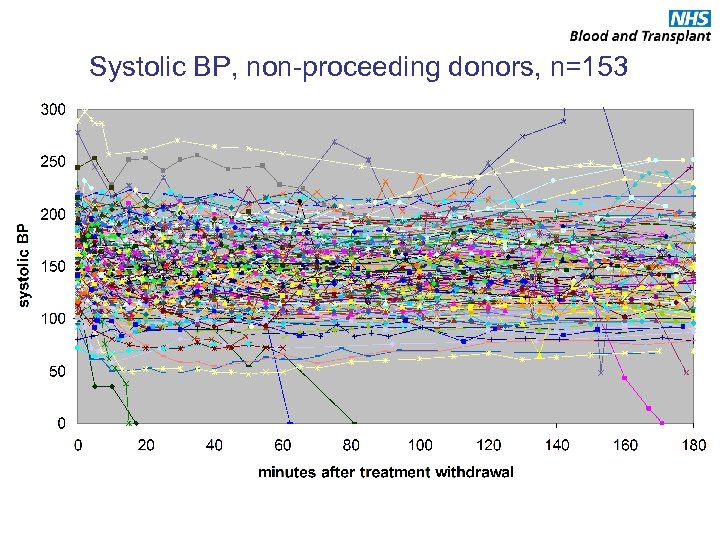 Systolic BP, non-proceeding donors, n=153
Systolic BP, non-proceeding donors, n=153
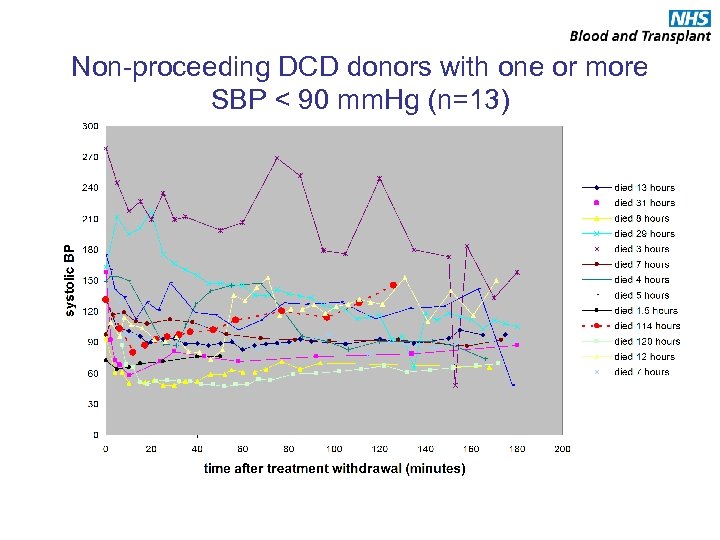 Non-proceeding DCD donors with one or more SBP < 90 mm. Hg (n=13)
Non-proceeding DCD donors with one or more SBP < 90 mm. Hg (n=13)
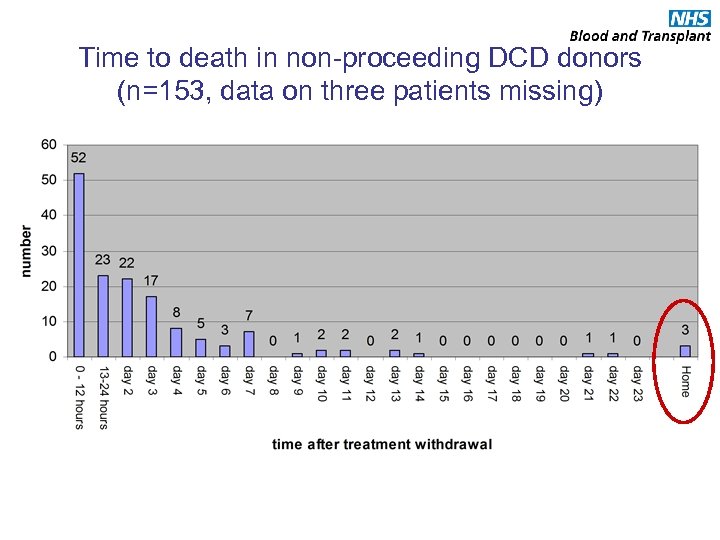 Time to death in non-proceeding DCD donors (n=153, data on three patients missing)
Time to death in non-proceeding DCD donors (n=153, data on three patients missing)
 Update: Heart retrieval from DCD donors UK pilots • 2 pilots • Normothermic regional perfusion assisted – Papworth – 3 centres in Eastern region – 2 successful transplants to date • Standard DCD retrieval – Papworth and Harefield – Eastern and South East regions – Transthoracic echo (Harefield)
Update: Heart retrieval from DCD donors UK pilots • 2 pilots • Normothermic regional perfusion assisted – Papworth – 3 centres in Eastern region – 2 successful transplants to date • Standard DCD retrieval – Papworth and Harefield – Eastern and South East regions – Transthoracic echo (Harefield)
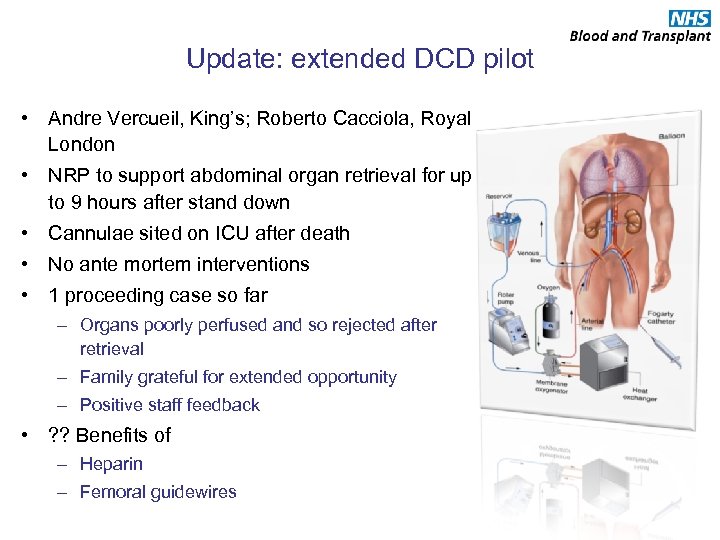 Update: extended DCD pilot • Andre Vercueil, King’s; Roberto Cacciola, Royal London • NRP to support abdominal organ retrieval for up to 9 hours after stand down • Cannulae sited on ICU after death • No ante mortem interventions • 1 proceeding case so far – Organs poorly perfused and so rejected after retrieval – Family grateful for extended opportunity – Positive staff feedback • ? ? Benefits of – Heparin – Femoral guidewires
Update: extended DCD pilot • Andre Vercueil, King’s; Roberto Cacciola, Royal London • NRP to support abdominal organ retrieval for up to 9 hours after stand down • Cannulae sited on ICU after death • No ante mortem interventions • 1 proceeding case so far – Organs poorly perfused and so rejected after retrieval – Family grateful for extended opportunity – Positive staff feedback • ? ? Benefits of – Heparin – Femoral guidewires
 Update: organ donation from babies with anencephaly • Twin pregnancy • Successful donation of kidneys and heart valves from an anencephalic infant in April 14 • Delivery ≡ treatment withdrawal • Baby died after 100 minutes – Death diagnosed after 5 minutes asystole • Assessment of renal function limited to size on USS and lack of oligohydramnios • Media coverage at baby’s anniversary – c. 15 000 on-line registrations National CLOD in Big Brother Chair
Update: organ donation from babies with anencephaly • Twin pregnancy • Successful donation of kidneys and heart valves from an anencephalic infant in April 14 • Delivery ≡ treatment withdrawal • Baby died after 100 minutes – Death diagnosed after 5 minutes asystole • Assessment of renal function limited to size on USS and lack of oligohydramnios • Media coverage at baby’s anniversary – c. 15 000 on-line registrations National CLOD in Big Brother Chair
 Update: organ donation from babies with anencephaly • Twin pregnancy • Successful donation of kidneys and heart valves from an anencephalic infant in April 14 • Delivery ≡ treatment withdrawal • Baby died after 100 minutes – Death diagnosed after 5 minutes asystole • Assessment of renal function limited to size on USS and lack of oligohydramnios • Media coverage at baby’s anniversary – c. 15 000 on-line registrations
Update: organ donation from babies with anencephaly • Twin pregnancy • Successful donation of kidneys and heart valves from an anencephalic infant in April 14 • Delivery ≡ treatment withdrawal • Baby died after 100 minutes – Death diagnosed after 5 minutes asystole • Assessment of renal function limited to size on USS and lack of oligohydramnios • Media coverage at baby’s anniversary – c. 15 000 on-line registrations
 Update: diagnosis of death by neurological criteria in infants < 2 months • Ao. MRC (2008) applies from 37 weeks gestation to 2 months, with two additional cautions • Available at http: //www. rcpch. ac. uk/system/files/ protected/page/DNC%20 Guide%20 FINAL. pdf
Update: diagnosis of death by neurological criteria in infants < 2 months • Ao. MRC (2008) applies from 37 weeks gestation to 2 months, with two additional cautions • Available at http: //www. rcpch. ac. uk/system/files/ protected/page/DNC%20 Guide%20 FINAL. pdf
 Update: DNC in infants < 2 months Additional cautions • In post-asphyxiated infants, or those receiving intensive care after resuscitation, a period of at least 24 hours of observation during which the preconditions necessary for assessment for DNC should be continuously present, should elapse before clinical testing for DNC. If there are concerns about residual drug-induced sedation, then this period of observation may need to be extended • A stronger hypercarbic stimulus is used to establish respiratory unresponsiveness. Specifically, there should be a clear rise in Pa. CO 2 levels of >2. 7 k. Pa (>20 mm Hg) above the base line with no respiratory response at that level.
Update: DNC in infants < 2 months Additional cautions • In post-asphyxiated infants, or those receiving intensive care after resuscitation, a period of at least 24 hours of observation during which the preconditions necessary for assessment for DNC should be continuously present, should elapse before clinical testing for DNC. If there are concerns about residual drug-induced sedation, then this period of observation may need to be extended • A stronger hypercarbic stimulus is used to establish respiratory unresponsiveness. Specifically, there should be a clear rise in Pa. CO 2 levels of >2. 7 k. Pa (>20 mm Hg) above the base line with no respiratory response at that level.
 Update: challenges to neurological determination of death by organ retrieval teams • 6 incidents reported Nov 14 – Feb 15 • Nature – – Apnoea test (starting CO 2) Hypernatraeamia Interval between testing Lack of microbiological characterisation • Outcome – Retrieval delayed until tests repeated – Considerable distress in donor hospitals • Root cause analysis – Education and training deficits – Variation in practice in critical care – Issues with documentation
Update: challenges to neurological determination of death by organ retrieval teams • 6 incidents reported Nov 14 – Feb 15 • Nature – – Apnoea test (starting CO 2) Hypernatraeamia Interval between testing Lack of microbiological characterisation • Outcome – Retrieval delayed until tests repeated – Considerable distress in donor hospitals • Root cause analysis – Education and training deficits – Variation in practice in critical care – Issues with documentation
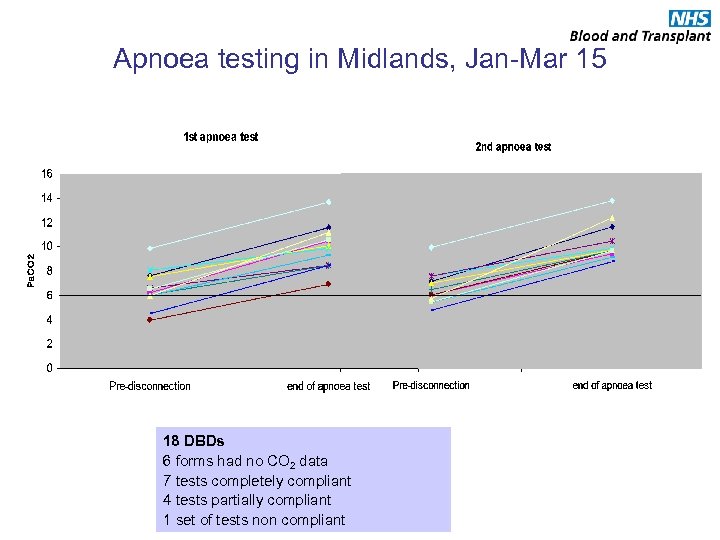 Apnoea testing in Midlands, Jan-Mar 15 18 DBDs 6 forms had no CO 2 data 7 tests completely compliant 4 tests partially compliant 1 set of tests non compliant
Apnoea testing in Midlands, Jan-Mar 15 18 DBDs 6 forms had no CO 2 data 7 tests completely compliant 4 tests partially compliant 1 set of tests non compliant
 National Standards for Organ Retrieval 5. 11 Before embarking on the retrieval operation, the lead retrieval surgeons must review the patient’s medical notes. In particular they must: • Have a clear understanding of the donor information prior to the start of the retrieval; • Check the identity, blood group and virology status of the donor; • Check that brain stem death or confirmation of cardiac death has been confirmed and documented correctly; • Check that appropriate consent/authorisation has been documented for the organs and tissues to be retrieved;
National Standards for Organ Retrieval 5. 11 Before embarking on the retrieval operation, the lead retrieval surgeons must review the patient’s medical notes. In particular they must: • Have a clear understanding of the donor information prior to the start of the retrieval; • Check the identity, blood group and virology status of the donor; • Check that brain stem death or confirmation of cardiac death has been confirmed and documented correctly; • Check that appropriate consent/authorisation has been documented for the organs and tissues to be retrieved;
 Interim proposal • Additional form • Completed by ICU consultant • Confirmation that death has been diagnosed and confirmed by neurological criteria • Cause, time and place of death • No other clinical information • Supported by NODC and NRG • Consulting HTA
Interim proposal • Additional form • Completed by ICU consultant • Confirmation that death has been diagnosed and confirmed by neurological criteria • Cause, time and place of death • No other clinical information • Supported by NODC and NRG • Consulting HTA
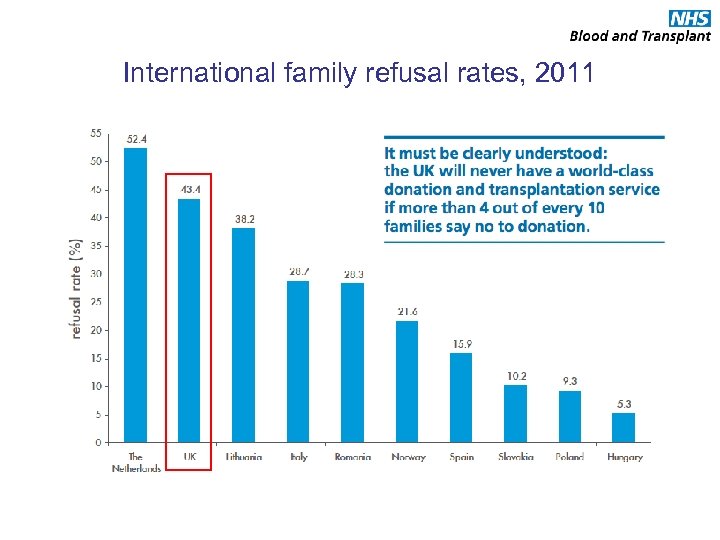 International family refusal rates, 2011
International family refusal rates, 2011
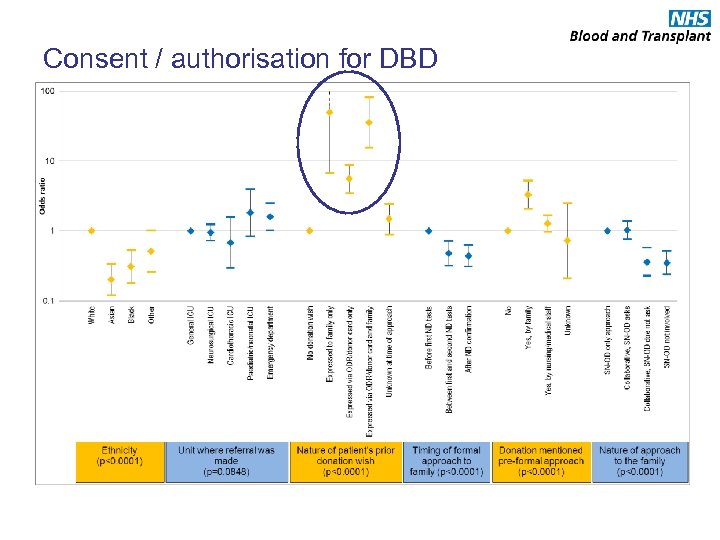 Consent / authorisation for DBD
Consent / authorisation for DBD
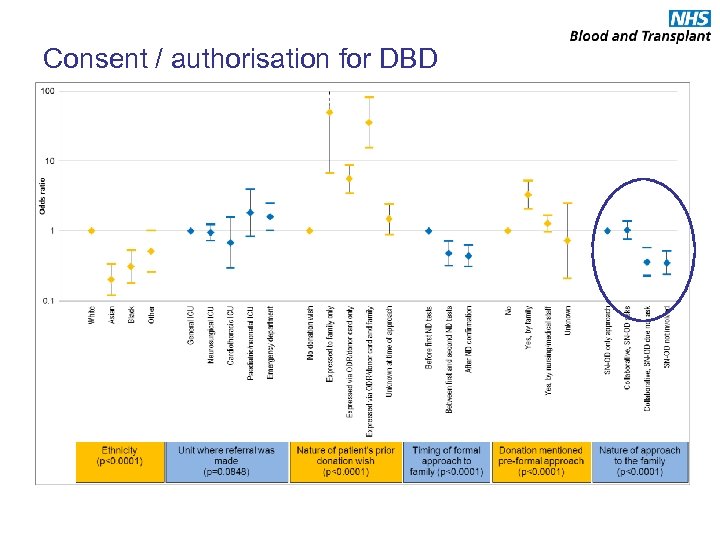 Consent / authorisation for DBD
Consent / authorisation for DBD
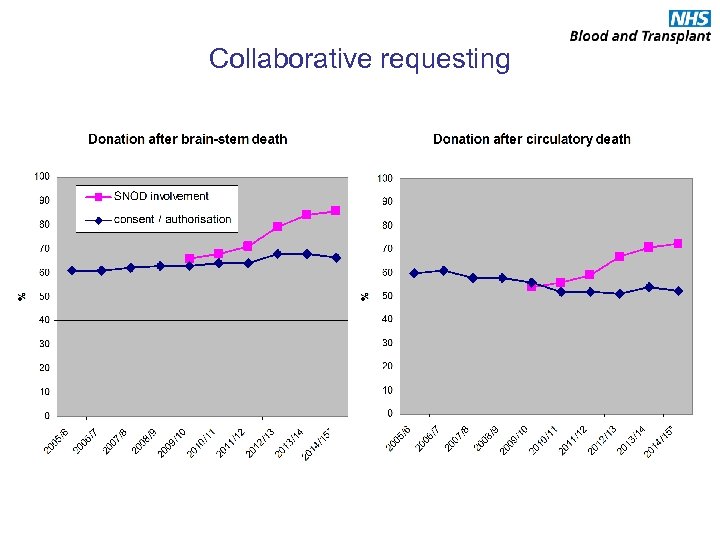 Collaborative requesting
Collaborative requesting
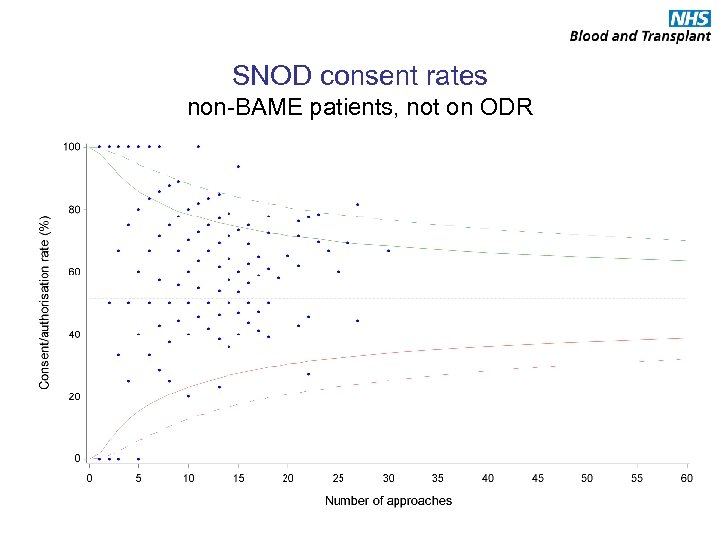 SNOD consent rates non-BAME patients, not on ODR
SNOD consent rates non-BAME patients, not on ODR
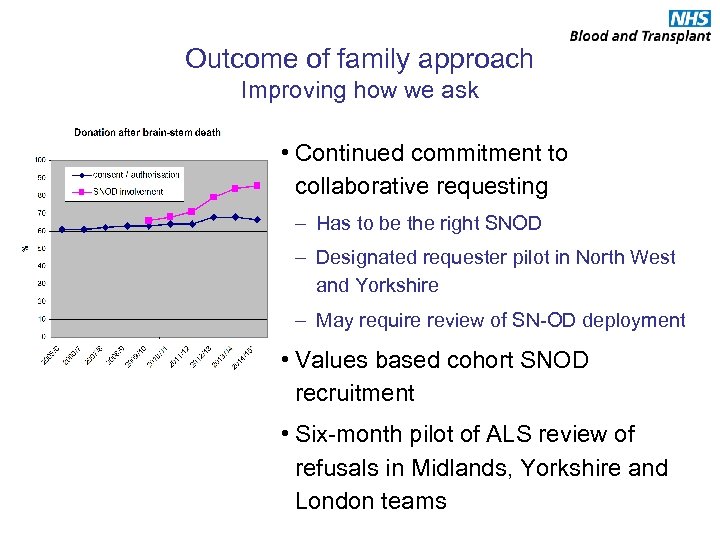 Outcome of family approach Improving how we ask • Continued commitment to collaborative requesting – Has to be the right SNOD – Designated requester pilot in North West and Yorkshire – May require review of SN-OD deployment • Values based cohort SNOD recruitment • Six-month pilot of ALS review of refusals in Midlands, Yorkshire and London teams
Outcome of family approach Improving how we ask • Continued commitment to collaborative requesting – Has to be the right SNOD – Designated requester pilot in North West and Yorkshire – May require review of SN-OD deployment • Values based cohort SNOD recruitment • Six-month pilot of ALS review of refusals in Midlands, Yorkshire and London teams
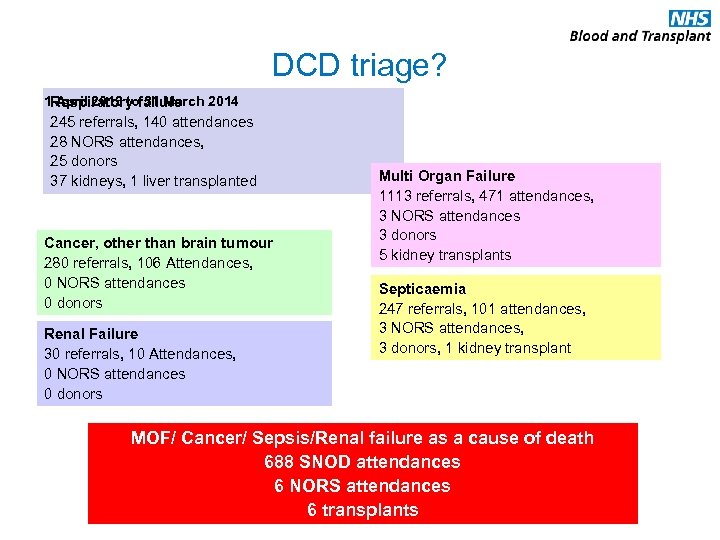 DCD triage? 1 Respiratory failure April 2013 to 31 March 2014 245 referrals, 140 attendances 28 NORS attendances, 25 donors 37 kidneys, 1 liver transplanted Cancer, other than brain tumour 280 referrals, 106 Attendances, 0 NORS attendances 0 donors Renal Failure 30 referrals, 10 Attendances, 0 NORS attendances 0 donors Multi Organ Failure 1113 referrals, 471 attendances, 3 NORS attendances 3 donors 5 kidney transplants Septicaemia 247 referrals, 101 attendances, 3 NORS attendances, 3 donors, 1 kidney transplant MOF/ Cancer/ Sepsis/Renal failure as a cause of death 688 SNOD attendances 6 NORS attendances 6 transplants
DCD triage? 1 Respiratory failure April 2013 to 31 March 2014 245 referrals, 140 attendances 28 NORS attendances, 25 donors 37 kidneys, 1 liver transplanted Cancer, other than brain tumour 280 referrals, 106 Attendances, 0 NORS attendances 0 donors Renal Failure 30 referrals, 10 Attendances, 0 NORS attendances 0 donors Multi Organ Failure 1113 referrals, 471 attendances, 3 NORS attendances 3 donors 5 kidney transplants Septicaemia 247 referrals, 101 attendances, 3 NORS attendances, 3 donors, 1 kidney transplant MOF/ Cancer/ Sepsis/Renal failure as a cause of death 688 SNOD attendances 6 NORS attendances 6 transplants
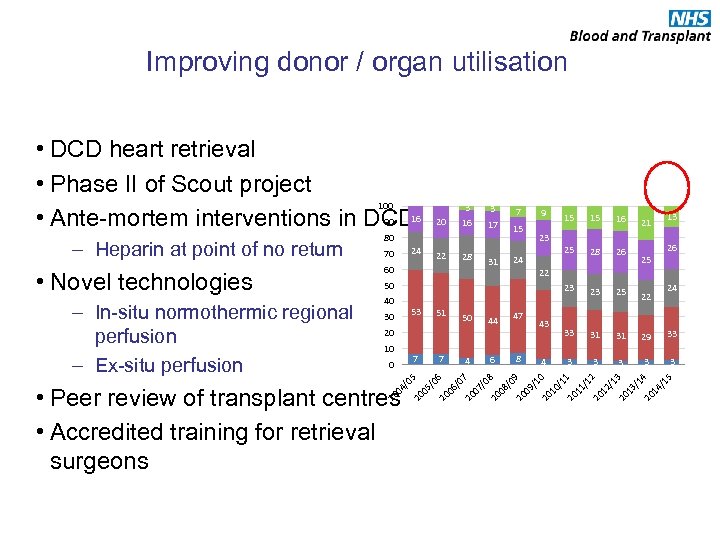 Improving donor / organ utilisation • DCD heart retrieval • Phase II of Scout project 100 90 • Ante-mortem interventions in DCD 16 • Novel technologies – In-situ normothermic regional perfusion – Ex-situ perfusion 3 7 17 15 9 13 80 24 70 22 28 60 31 23 24 53 30 51 50 44 47 20 10 7 4 6 15 16 25 28 26 23 25 22 33 31 31 29 33 3 3 21 25 26 22 50 40 15 23 20 8 43 4 24 /0 20 5 05 /0 20 6 06 /0 20 7 07 /0 20 8 08 /0 20 9 09 /1 20 0 10 /1 20 1 11 /1 20 2 12 /1 20 3 13 /1 20 4 14 /1 5 – Heparin at point of no return 3 16 20 04 • Peer review of transplant centres • Accredited training for retrieval surgeons DRAFT
Improving donor / organ utilisation • DCD heart retrieval • Phase II of Scout project 100 90 • Ante-mortem interventions in DCD 16 • Novel technologies – In-situ normothermic regional perfusion – Ex-situ perfusion 3 7 17 15 9 13 80 24 70 22 28 60 31 23 24 53 30 51 50 44 47 20 10 7 4 6 15 16 25 28 26 23 25 22 33 31 31 29 33 3 3 21 25 26 22 50 40 15 23 20 8 43 4 24 /0 20 5 05 /0 20 6 06 /0 20 7 07 /0 20 8 08 /0 20 9 09 /1 20 0 10 /1 20 1 11 /1 20 2 12 /1 20 3 13 /1 20 4 14 /1 5 – Heparin at point of no return 3 16 20 04 • Peer review of transplant centres • Accredited training for retrieval surgeons DRAFT
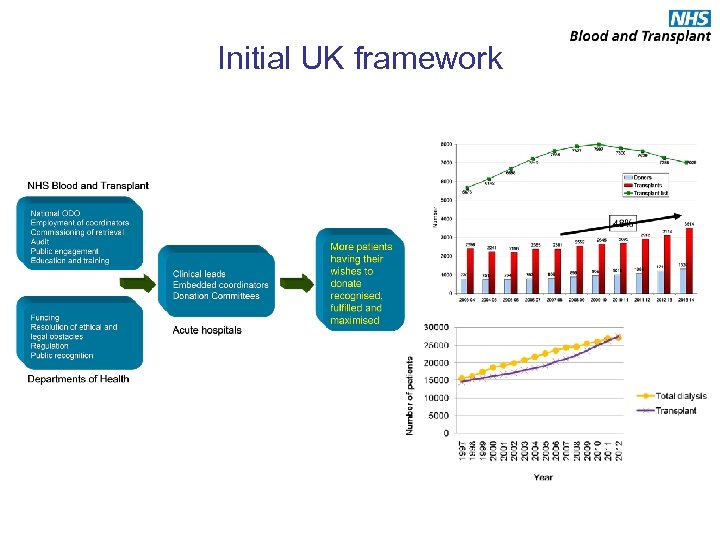 Initial UK framework
Initial UK framework
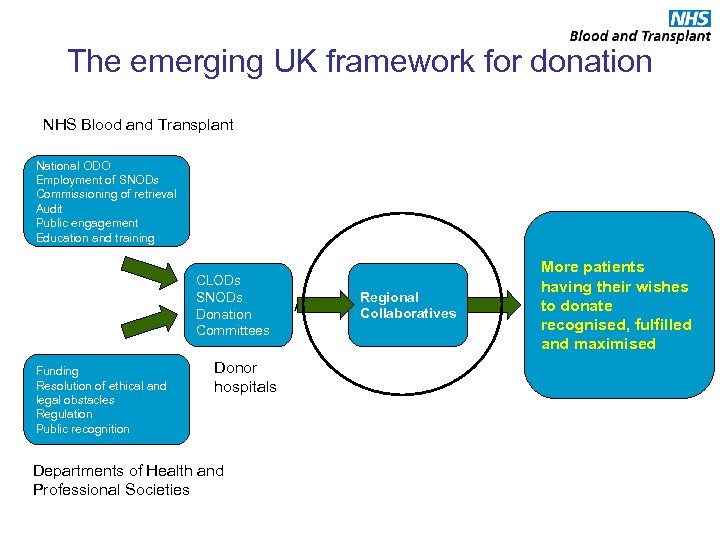 The emerging UK framework for donation NHS Blood and Transplant National ODO Employment of SNODs Commissioning of retrieval Audit Public engagement Education and training CLODs SNODs Donation Committees Funding Resolution of ethical and legal obstacles Regulation Public recognition Donor hospitals Departments of Health and Professional Societies Regional Acute hospitals Collaboratives More patients having their wishes to donate recognised, fulfilled and maximised
The emerging UK framework for donation NHS Blood and Transplant National ODO Employment of SNODs Commissioning of retrieval Audit Public engagement Education and training CLODs SNODs Donation Committees Funding Resolution of ethical and legal obstacles Regulation Public recognition Donor hospitals Departments of Health and Professional Societies Regional Acute hospitals Collaboratives More patients having their wishes to donate recognised, fulfilled and maximised
 Service improvement in deceased donation • Timely identification and referral – Emergency Department • Brain-stem death testing • Collaborative requesting • Streamlining DCD • Physiological optimisation of the DBD donor
Service improvement in deceased donation • Timely identification and referral – Emergency Department • Brain-stem death testing • Collaborative requesting • Streamlining DCD • Physiological optimisation of the DBD donor


