Neuro Potpourri.pptx
- Количество слайдов: 48
 Neuro Potpourri Gerald F. Smith, MPH, MS, PA-C Neurology and Neurophysiology Associates Philadelphia University Spring 2015
Neuro Potpourri Gerald F. Smith, MPH, MS, PA-C Neurology and Neurophysiology Associates Philadelphia University Spring 2015
 Brain trick
Brain trick
 Neuro goes to the movies
Neuro goes to the movies
 Neuro Potporrui Myasthenia Gravis Neuropathies ALS Restless Legs Syndrome
Neuro Potporrui Myasthenia Gravis Neuropathies ALS Restless Legs Syndrome
 Myasthenia Gravis Chronic autoimmune neuromuscular disease Characterized by varying degrees of weakness of skeletal muscles Name literally means “grave muscle weakness”
Myasthenia Gravis Chronic autoimmune neuromuscular disease Characterized by varying degrees of weakness of skeletal muscles Name literally means “grave muscle weakness”
 Myasthenia Gravis Prevalence estimated at 14 -20 cases per 100, 000 population (36, 000 -60, 000 cases) Most likely underdiagnosed Age of onset in females typically between age 20 -30; males 70 -80, with more males affected
Myasthenia Gravis Prevalence estimated at 14 -20 cases per 100, 000 population (36, 000 -60, 000 cases) Most likely underdiagnosed Age of onset in females typically between age 20 -30; males 70 -80, with more males affected
 Myasthenia Gravis Caused by defective neuromuscular transmission Acetylcholine is the neurotransmitter involved Both anatomic and physiologic changes involved
Myasthenia Gravis Caused by defective neuromuscular transmission Acetylcholine is the neurotransmitter involved Both anatomic and physiologic changes involved
 Myasthenia Gravis In normal neuromuscular transmission, Ach released from motor nerve terminal in quanta Travel across neuromuscular junction to receptors Binding to receptors causes muscle contraction
Myasthenia Gravis In normal neuromuscular transmission, Ach released from motor nerve terminal in quanta Travel across neuromuscular junction to receptors Binding to receptors causes muscle contraction
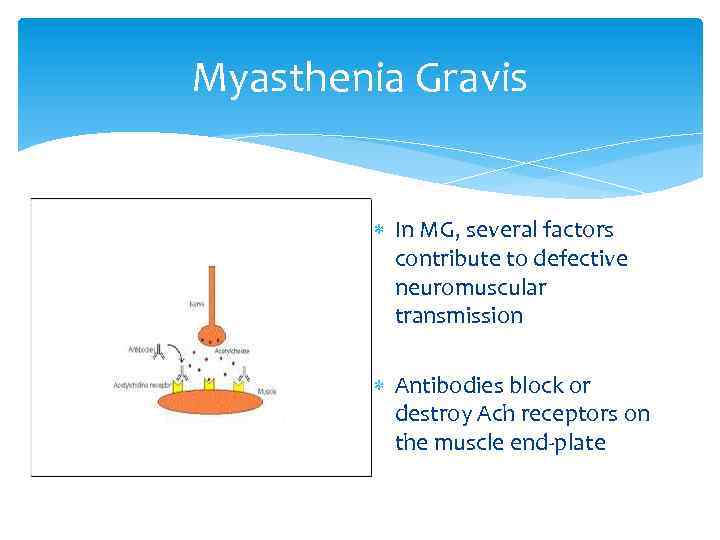 Myasthenia Gravis In MG, several factors contribute to defective neuromuscular transmission Antibodies block or destroy Ach receptors on the muscle end-plate
Myasthenia Gravis In MG, several factors contribute to defective neuromuscular transmission Antibodies block or destroy Ach receptors on the muscle end-plate
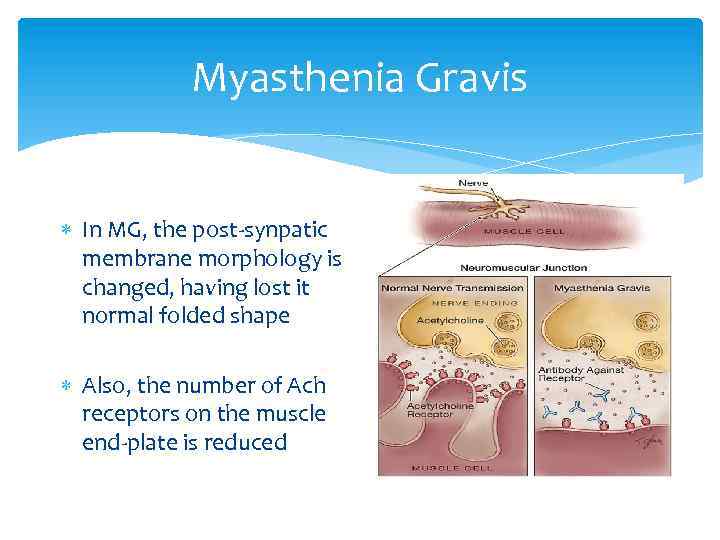 Myasthenia Gravis In MG, the post-synpatic membrane morphology is changed, having lost it normal folded shape Also, the number of Ach receptors on the muscle end-plate is reduced
Myasthenia Gravis In MG, the post-synpatic membrane morphology is changed, having lost it normal folded shape Also, the number of Ach receptors on the muscle end-plate is reduced
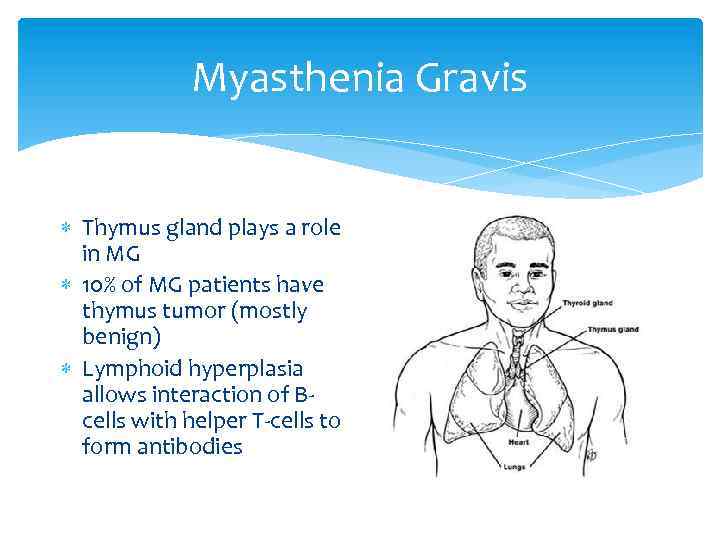 Myasthenia Gravis Thymus gland plays a role in MG 10% of MG patients have thymus tumor (mostly benign) Lymphoid hyperplasia allows interaction of Bcells with helper T-cells to form antibodies
Myasthenia Gravis Thymus gland plays a role in MG 10% of MG patients have thymus tumor (mostly benign) Lymphoid hyperplasia allows interaction of Bcells with helper T-cells to form antibodies
 Myasthenia Gravis As a result of these changes to the postsynaptic membrane, the effect of Ach is reduced Resultant effect is greatly reduced or blocked stimulation of muscle contraction
Myasthenia Gravis As a result of these changes to the postsynaptic membrane, the effect of Ach is reduced Resultant effect is greatly reduced or blocked stimulation of muscle contraction
 Myasthenia Gravis Unusual distribution of symptoms often presents puzzling clinical picture Classic symptoms include: drooping of eyelids, diplopia, dysphagia, and dysarthria These symptoms are sometimes pursued as intracranial in origin
Myasthenia Gravis Unusual distribution of symptoms often presents puzzling clinical picture Classic symptoms include: drooping of eyelids, diplopia, dysphagia, and dysarthria These symptoms are sometimes pursued as intracranial in origin
 Myasthenia Gravis Muscle weakness, particularly in the extremities, is a common symptom The muscle weakness becomes more severe as the day progresses Rest will often temporarily improve muscle weakness
Myasthenia Gravis Muscle weakness, particularly in the extremities, is a common symptom The muscle weakness becomes more severe as the day progresses Rest will often temporarily improve muscle weakness
 Myasthenia Gravis Muscles which control breathing, swallowing (bulbar) may be affected Myasthenic crisis occurs when these muscles weaken to the point where ventilation or eating/drinking is impaired Crisis can be triggered by infection, fever, or drugs
Myasthenia Gravis Muscles which control breathing, swallowing (bulbar) may be affected Myasthenic crisis occurs when these muscles weaken to the point where ventilation or eating/drinking is impaired Crisis can be triggered by infection, fever, or drugs
 Myasthenia Gravis Several classes of ABX: aminoglycosides, quinolones, macrolides Antihypertensives: Bblockers and CCB Lithium Magnesium (including Maalox, Mylanta)
Myasthenia Gravis Several classes of ABX: aminoglycosides, quinolones, macrolides Antihypertensives: Bblockers and CCB Lithium Magnesium (including Maalox, Mylanta)
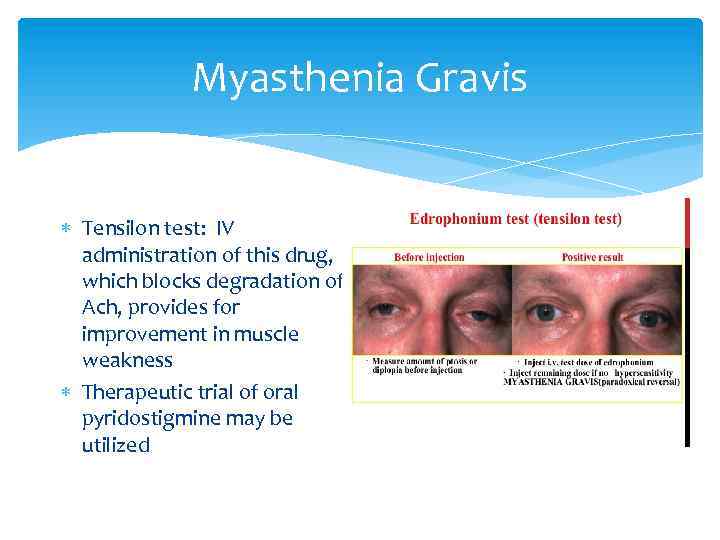 Myasthenia Gravis Tensilon test: IV administration of this drug, which blocks degradation of Ach, provides for improvement in muscle weakness Therapeutic trial of oral pyridostigmine may be utilized
Myasthenia Gravis Tensilon test: IV administration of this drug, which blocks degradation of Ach, provides for improvement in muscle weakness Therapeutic trial of oral pyridostigmine may be utilized
 Myasthenia Gravis Antibody testing is utilized to detect Anti-Ach receptor antibodies Nearly 75% of patients with generalized MG have serum antibodies to Ach receptors Antibody concentration may be increased in SLE, ALS, and inflammatory neuropathy
Myasthenia Gravis Antibody testing is utilized to detect Anti-Ach receptor antibodies Nearly 75% of patients with generalized MG have serum antibodies to Ach receptors Antibody concentration may be increased in SLE, ALS, and inflammatory neuropathy
 Myasthenia Gravis EMG testing, using repetitive nerve stimulation, shows decremental change in amplitude of muscle response Not specific to MG May be normal in mild cases
Myasthenia Gravis EMG testing, using repetitive nerve stimulation, shows decremental change in amplitude of muscle response Not specific to MG May be normal in mild cases
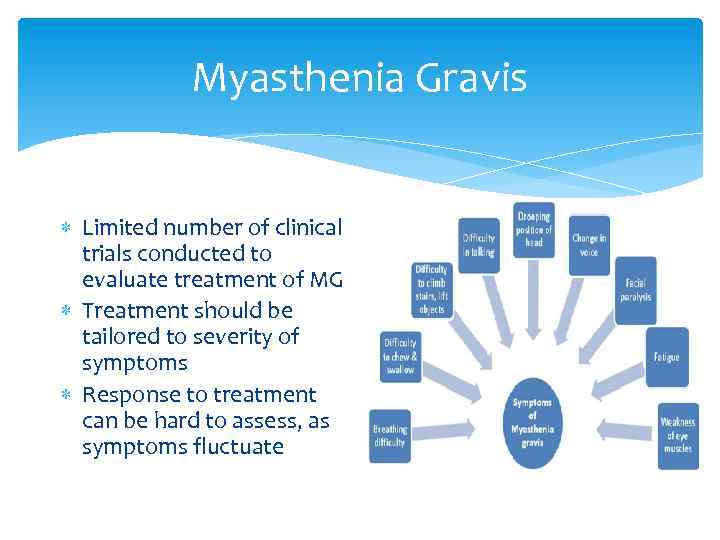 Myasthenia Gravis Limited number of clinical trials conducted to evaluate treatment of MG Treatment should be tailored to severity of symptoms Response to treatment can be hard to assess, as symptoms fluctuate
Myasthenia Gravis Limited number of clinical trials conducted to evaluate treatment of MG Treatment should be tailored to severity of symptoms Response to treatment can be hard to assess, as symptoms fluctuate
 Myasthenia Gravis Anticholinesterase drugs impair the degradation of Ach (Mestinon) Allow Ach to accumulate at the neuromuscular junction Response is variable GI side effects common CNS effects rare
Myasthenia Gravis Anticholinesterase drugs impair the degradation of Ach (Mestinon) Allow Ach to accumulate at the neuromuscular junction Response is variable GI side effects common CNS effects rare
 Myasthenia Gravis Prednisone often provides rapid improvement in symptoms Most effective in patients with recent onset of symptoms Approx. 1/3 of patients will become weaker initially
Myasthenia Gravis Prednisone often provides rapid improvement in symptoms Most effective in patients with recent onset of symptoms Approx. 1/3 of patients will become weaker initially
 Myasthenia Gravis Immunosuppresive drugs may be considered when otherapies have produced sub-optimal responses Azathioprine, Cyclosporine, and Cyclophosphamide have been used with varying levels of success Cost and side effects related to these agents are important considerations
Myasthenia Gravis Immunosuppresive drugs may be considered when otherapies have produced sub-optimal responses Azathioprine, Cyclosporine, and Cyclophosphamide have been used with varying levels of success Cost and side effects related to these agents are important considerations
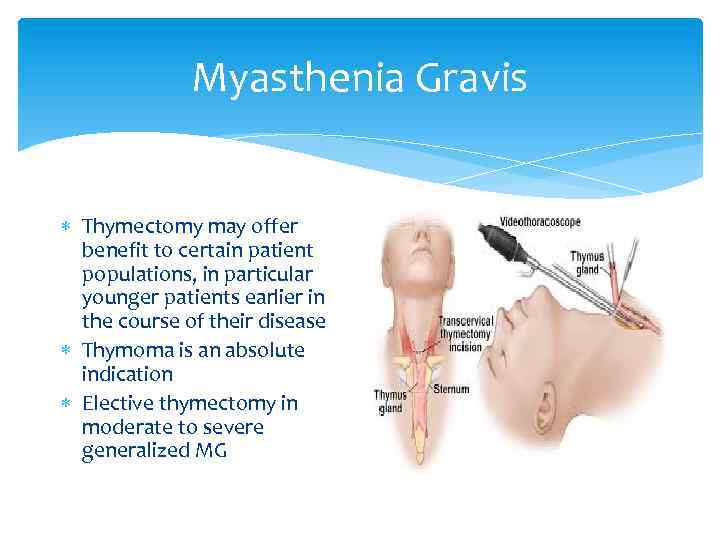 Myasthenia Gravis Thymectomy may offer benefit to certain patient populations, in particular younger patients earlier in the course of their disease Thymoma is an absolute indication Elective thymectomy in moderate to severe generalized MG
Myasthenia Gravis Thymectomy may offer benefit to certain patient populations, in particular younger patients earlier in the course of their disease Thymoma is an absolute indication Elective thymectomy in moderate to severe generalized MG
 Neuropathy Peripheral neuropathies can be subdivided broadly into mononeuropathies and polyneuropathies Mononeuropathies result from injury to nerve along its course or by compression, angulation or stretching of the nerve Entrapment neuropathies occur when the nerve course passes through a narrow anatomical space
Neuropathy Peripheral neuropathies can be subdivided broadly into mononeuropathies and polyneuropathies Mononeuropathies result from injury to nerve along its course or by compression, angulation or stretching of the nerve Entrapment neuropathies occur when the nerve course passes through a narrow anatomical space
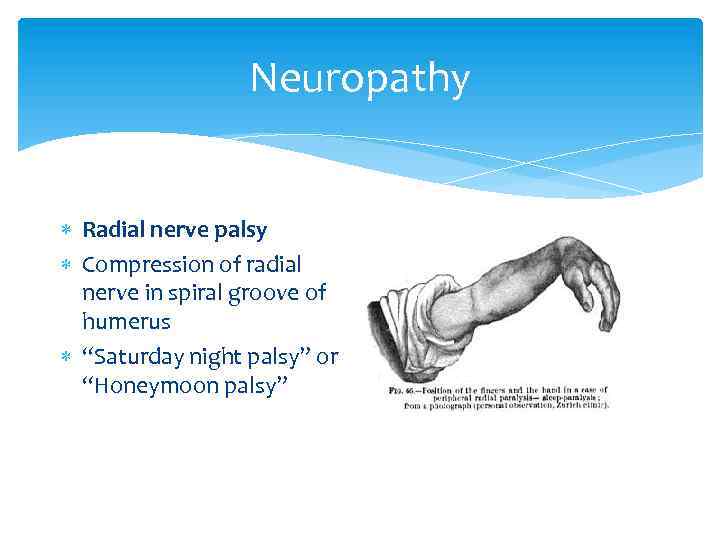 Neuropathy Radial nerve palsy Compression of radial nerve in spiral groove of humerus “Saturday night palsy” or “Honeymoon palsy”
Neuropathy Radial nerve palsy Compression of radial nerve in spiral groove of humerus “Saturday night palsy” or “Honeymoon palsy”
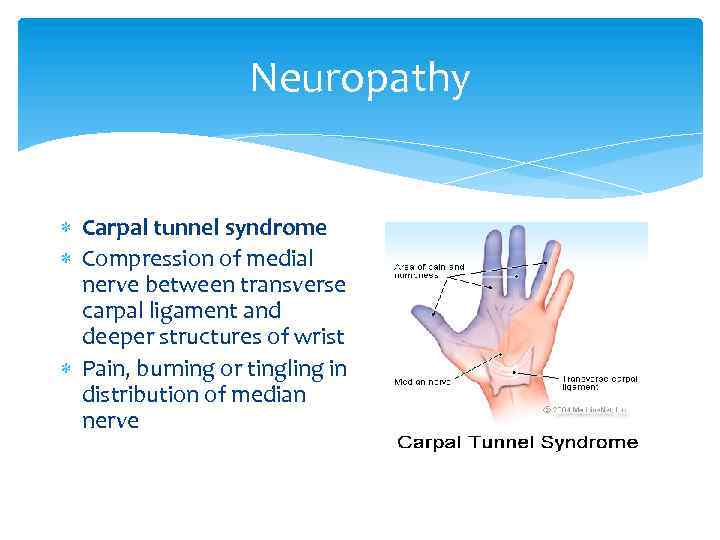 Neuropathy Carpal tunnel syndrome Compression of medial nerve between transverse carpal ligament and deeper structures of wrist Pain, burning or tingling in distribution of median nerve
Neuropathy Carpal tunnel syndrome Compression of medial nerve between transverse carpal ligament and deeper structures of wrist Pain, burning or tingling in distribution of median nerve
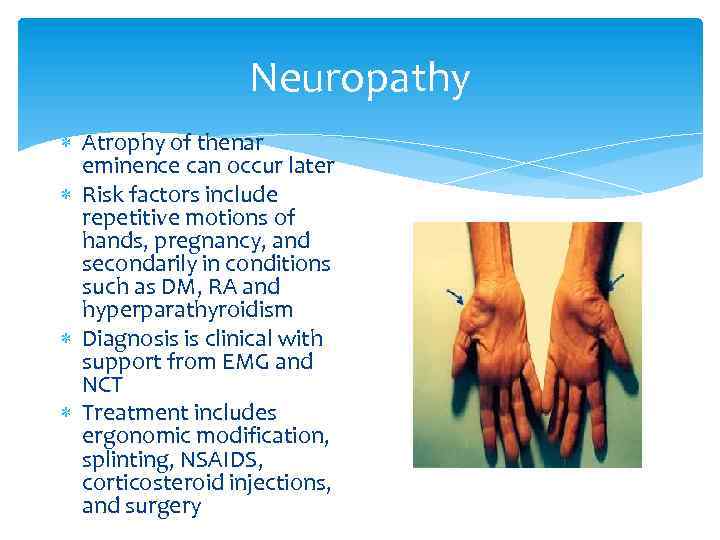 Neuropathy Atrophy of thenar eminence can occur later Risk factors include repetitive motions of hands, pregnancy, and secondarily in conditions such as DM, RA and hyperparathyroidism Diagnosis is clinical with support from EMG and NCT Treatment includes ergonomic modification, splinting, NSAIDS, corticosteroid injections, and surgery
Neuropathy Atrophy of thenar eminence can occur later Risk factors include repetitive motions of hands, pregnancy, and secondarily in conditions such as DM, RA and hyperparathyroidism Diagnosis is clinical with support from EMG and NCT Treatment includes ergonomic modification, splinting, NSAIDS, corticosteroid injections, and surgery
 Neuropathy Polyneuropathies lead to symmetric sensory, motor or mixed deficit Most prominent distally May be broadly classified as hereditary, metabolic or toxic Pain may be prominent symptom In approximately 50% no specific cause is identified
Neuropathy Polyneuropathies lead to symmetric sensory, motor or mixed deficit Most prominent distally May be broadly classified as hereditary, metabolic or toxic Pain may be prominent symptom In approximately 50% no specific cause is identified
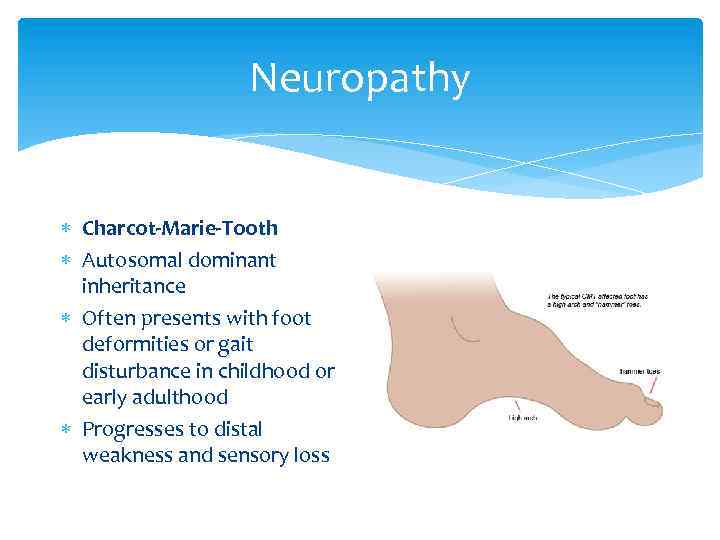 Neuropathy Charcot-Marie-Tooth Autosomal dominant inheritance Often presents with foot deformities or gait disturbance in childhood or early adulthood Progresses to distal weakness and sensory loss
Neuropathy Charcot-Marie-Tooth Autosomal dominant inheritance Often presents with foot deformities or gait disturbance in childhood or early adulthood Progresses to distal weakness and sensory loss
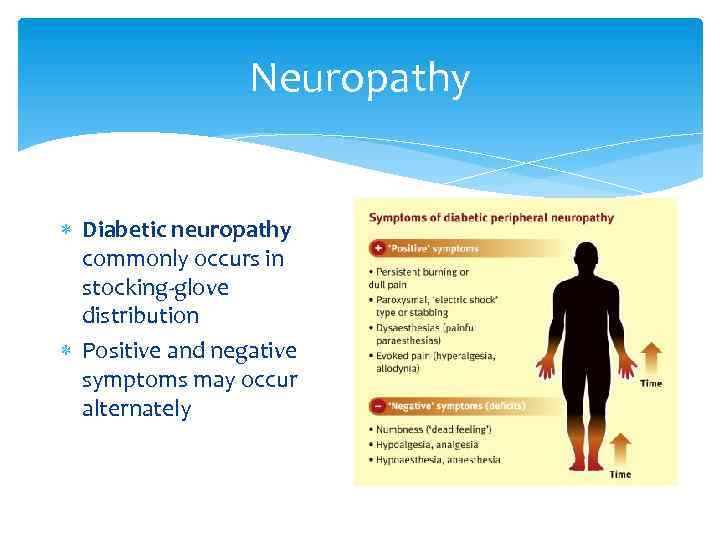 Neuropathy Diabetic neuropathy commonly occurs in stocking-glove distribution Positive and negative symptoms may occur alternately
Neuropathy Diabetic neuropathy commonly occurs in stocking-glove distribution Positive and negative symptoms may occur alternately
 Neuropathy Toxic neuropathies may result from exposure to various agents, including organophosphates, heavy metals, and certain drugs (phenytoin, isoniazid, nitrofurantoin) Occupational history and identification of clusters may help in diagnosis
Neuropathy Toxic neuropathies may result from exposure to various agents, including organophosphates, heavy metals, and certain drugs (phenytoin, isoniazid, nitrofurantoin) Occupational history and identification of clusters may help in diagnosis
 Neuropathy Aside from a thorough history, serologic studies are an important part of the work-up of polyneuropathies GTT ANA ACE B 6, B 12, folate Copper Lyme titer HIV RPR SS-A, SS-B, C-ANCA, P-ANCA Heavy metals (if suspected)
Neuropathy Aside from a thorough history, serologic studies are an important part of the work-up of polyneuropathies GTT ANA ACE B 6, B 12, folate Copper Lyme titer HIV RPR SS-A, SS-B, C-ANCA, P-ANCA Heavy metals (if suspected)
 Neuropathy Treatment involves addressing underlying cause Pharmacologic treatment can involve: Ø NSAIDS Ø Antidepressants (Effexor, Cymbalta, amitriptyline) Ø Anti-epileptics (Neurontin, Lyrica, carbamazepine) Ø Opioids in severe pain
Neuropathy Treatment involves addressing underlying cause Pharmacologic treatment can involve: Ø NSAIDS Ø Antidepressants (Effexor, Cymbalta, amitriptyline) Ø Anti-epileptics (Neurontin, Lyrica, carbamazepine) Ø Opioids in severe pain
 Guillain-Barré Syndrome Acute or subacute, progressive polyradiculoneuropathy, often preceded by an infection, immunization or surgery Associated with Campylobacter jejuni enteritis. Inflammatory response that affects the spinal root, peripheral & extra axial cranial nerves Exact mechanism is unclear
Guillain-Barré Syndrome Acute or subacute, progressive polyradiculoneuropathy, often preceded by an infection, immunization or surgery Associated with Campylobacter jejuni enteritis. Inflammatory response that affects the spinal root, peripheral & extra axial cranial nerves Exact mechanism is unclear
 Guillain-Barré Syndrome Diagnosis Ascending weakness, primarily motor symptoms Muscles of respiration and deglutition may be affected Autonomic component (tachy, hypo/HTN) Elevated protein level in the CSF EMG – axonal loss, delayed F-waves CXR, stool cultures
Guillain-Barré Syndrome Diagnosis Ascending weakness, primarily motor symptoms Muscles of respiration and deglutition may be affected Autonomic component (tachy, hypo/HTN) Elevated protein level in the CSF EMG – axonal loss, delayed F-waves CXR, stool cultures
 Guillain-Barré Syndrome Treatment Close monitoring of respiratory function Preventive measures – wound care & DVT/PE prophylaxis Plasma exchange & IV immunoglobulins Prognosis 75% completely recover within 3 -6 months 20% with permanent deficit
Guillain-Barré Syndrome Treatment Close monitoring of respiratory function Preventive measures – wound care & DVT/PE prophylaxis Plasma exchange & IV immunoglobulins Prognosis 75% completely recover within 3 -6 months 20% with permanent deficit
 Bell’s Palsy Sudden onset of facial paresis caused by an inflammatory response involving the facial nerve Idiopathic, although theorized to be caused by reactivation of HSV type 1 or varicella virus More common in patients with DM and in pregnancy
Bell’s Palsy Sudden onset of facial paresis caused by an inflammatory response involving the facial nerve Idiopathic, although theorized to be caused by reactivation of HSV type 1 or varicella virus More common in patients with DM and in pregnancy
 Bell’s Palsy Abrupt facial paralysis that gradually worsens Ear pain on the affected side Numbness sensation Difficulty eating Excessive tearing Difficulty closing ipsilateral eye Poor fine facial movements
Bell’s Palsy Abrupt facial paralysis that gradually worsens Ear pain on the affected side Numbness sensation Difficulty eating Excessive tearing Difficulty closing ipsilateral eye Poor fine facial movements
 Bell’s Palsy Routine labs or diagnostic imaging not necessary for diagnosis unless clinical suspicion of underlying cause (herpes zoster, Lyme Disease, HIV, tumor) Treatment is controversial, as 60% of patients resolve completely without it Steroids may have an impact: 2 week taper Antivirals? Eye drops and patching
Bell’s Palsy Routine labs or diagnostic imaging not necessary for diagnosis unless clinical suspicion of underlying cause (herpes zoster, Lyme Disease, HIV, tumor) Treatment is controversial, as 60% of patients resolve completely without it Steroids may have an impact: 2 week taper Antivirals? Eye drops and patching
 Amyotrophic Lateral Sclerosis Amyotrophic lateral sclerosis (ALS) "Lou Gehrig's disease" A-myo-trophic=no muscle nourishment: leads to atrophy Lateral: area of spinal cord where portions of the nerve cells that signal and control the muscles are located Sclerosis: As this area degenerates it leads to scarring Progressive neurodegenerative disease that affects motor neurons in the brain and the spinal cord. The progressive degeneration of the motor neurons in ALS eventually lead to their death. Death of motor neurons causes loss of ability of the brain to initiate and control muscle movement
Amyotrophic Lateral Sclerosis Amyotrophic lateral sclerosis (ALS) "Lou Gehrig's disease" A-myo-trophic=no muscle nourishment: leads to atrophy Lateral: area of spinal cord where portions of the nerve cells that signal and control the muscles are located Sclerosis: As this area degenerates it leads to scarring Progressive neurodegenerative disease that affects motor neurons in the brain and the spinal cord. The progressive degeneration of the motor neurons in ALS eventually lead to their death. Death of motor neurons causes loss of ability of the brain to initiate and control muscle movement
 ALS Incidence higher in men Onset from teenage years to eight decade; average 60 in sporadic; 50 in inherited Estimated lifetime risk for men 1 in 350, 1 in 420 for women Paradoxically, earlier diagnosis more likely to lead to long-term survival
ALS Incidence higher in men Onset from teenage years to eight decade; average 60 in sporadic; 50 in inherited Estimated lifetime risk for men 1 in 350, 1 in 420 for women Paradoxically, earlier diagnosis more likely to lead to long-term survival
 ALS Increasing muscle weakness, especially involving the arms and legs Difficulty with speech, swallowing or breathing (bulbar) Atrophy of affected limbs Progresses to complete paralysis Cognitive decline, pseudobulbar affect and parkinsonism may occur.
ALS Increasing muscle weakness, especially involving the arms and legs Difficulty with speech, swallowing or breathing (bulbar) Atrophy of affected limbs Progresses to complete paralysis Cognitive decline, pseudobulbar affect and parkinsonism may occur.
 ALS Riluzole is only available treatment; it may slow progression (2 -3 mos) Supportive care, therapy are mainstays of treatment Life expectancy 2 -5 years from diagnosis
ALS Riluzole is only available treatment; it may slow progression (2 -3 mos) Supportive care, therapy are mainstays of treatment Life expectancy 2 -5 years from diagnosis
 Restless Legs Syndrome May occur as a primary (idiopathic) disorder Occurs secondarily in pregnancy, Fe deficiency anemia, peripheral neuropathy Restlessness and sensory disturbance lead to irresistible urge to move legs, especially during periods of relaxation Disturbed nocturnal sleep and excessive daytime somnolence may result
Restless Legs Syndrome May occur as a primary (idiopathic) disorder Occurs secondarily in pregnancy, Fe deficiency anemia, peripheral neuropathy Restlessness and sensory disturbance lead to irresistible urge to move legs, especially during periods of relaxation Disturbed nocturnal sleep and excessive daytime somnolence may result
 RLS Incidence twice as high in females Can occur at any age; most common in middle age Typically bilateral Can affect arms, trunk and head, but less commonly ETOH can exacerbate problem
RLS Incidence twice as high in females Can occur at any age; most common in middle age Typically bilateral Can affect arms, trunk and head, but less commonly ETOH can exacerbate problem
 RLS Thought to have genetic component Dopamine is thought to play a role, as RLS is often seen in PD, which effects basal ganglia (dopamine dependent) Typically progresses in severity over time Patients may experience periods of remission
RLS Thought to have genetic component Dopamine is thought to play a role, as RLS is often seen in PD, which effects basal ganglia (dopamine dependent) Typically progresses in severity over time Patients may experience periods of remission
 RLS Avoidance of caffeine, nicotine, ETOH Treat deficiencies (Fe, Mg, folate) Sleep hygiene Exercise Massage Pharmacotherapy with dopaminergics (Mirapex, Requip)
RLS Avoidance of caffeine, nicotine, ETOH Treat deficiencies (Fe, Mg, folate) Sleep hygiene Exercise Massage Pharmacotherapy with dopaminergics (Mirapex, Requip)


