86487bf5c5b2e73717e331402e4d19ef.ppt
- Количество слайдов: 46
 National QOF Consultation Developing the Quality and Outcomes Framework: Proposals for a new, independent process Tuesday 6 th January, Birmingham
National QOF Consultation Developing the Quality and Outcomes Framework: Proposals for a new, independent process Tuesday 6 th January, Birmingham
 Welcome & Introduction Graham Urwin, Chief Executive, Stoke on Trent PCT
Welcome & Introduction Graham Urwin, Chief Executive, Stoke on Trent PCT
 National QOF Consultation Developing the Quality and Outcomes Framework: Proposals for a new, independent process Tuesday 6 th January, Birmingham
National QOF Consultation Developing the Quality and Outcomes Framework: Proposals for a new, independent process Tuesday 6 th January, Birmingham
 Background to the Consultation Ben Dyson, Director of Primary Care, Department of Health
Background to the Consultation Ben Dyson, Director of Primary Care, Department of Health
 High quality care for all is at the heart of the NHS Stage Review Final Report • Help to stay healthy • Empowering patients • Most effective • Raising standards Quality at the heart of the NHS treatments for all • Stronger involvement of clinicians in decision making at every level of the NHS • Fostering a pioneering NHS • Keeping patients as Primary Medical Care safe as possible High quality care for all High quality care for patients and the public • Empowering Freedom to focus on quality frontline staff to lead change that improves quality for patients • Valuing the work of NHS staff
High quality care for all is at the heart of the NHS Stage Review Final Report • Help to stay healthy • Empowering patients • Most effective • Raising standards Quality at the heart of the NHS treatments for all • Stronger involvement of clinicians in decision making at every level of the NHS • Fostering a pioneering NHS • Keeping patients as Primary Medical Care safe as possible High quality care for all High quality care for patients and the public • Empowering Freedom to focus on quality frontline staff to lead change that improves quality for patients • Valuing the work of NHS staff
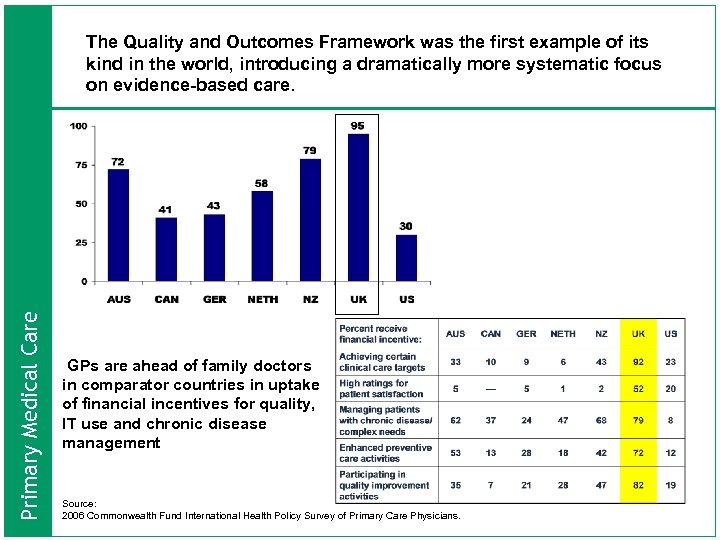 Primary Medical Care The Quality and Outcomes Framework was the first example of its kind in the world, introducing a dramatically more systematic focus on evidence-based care. GPs are ahead of family doctors in comparator countries in uptake of financial incentives for quality, IT use and chronic disease management Source: 2006 Commonwealth Fund International Health Policy Survey of Primary Care Physicians.
Primary Medical Care The Quality and Outcomes Framework was the first example of its kind in the world, introducing a dramatically more systematic focus on evidence-based care. GPs are ahead of family doctors in comparator countries in uptake of financial incentives for quality, IT use and chronic disease management Source: 2006 Commonwealth Fund International Health Policy Survey of Primary Care Physicians.
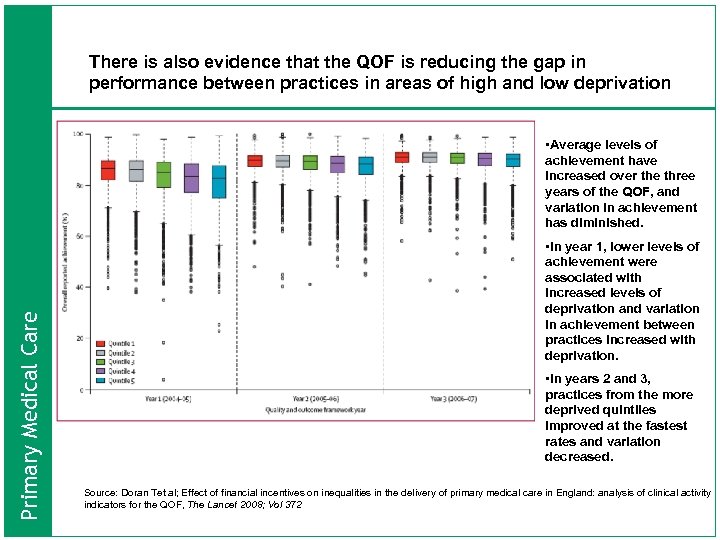 There is also evidence that the QOF is reducing the gap in performance between practices in areas of high and low deprivation Primary Medical Care • Average levels of achievement have increased over the three years of the QOF, and variation in achievement has diminished. • In year 1, lower levels of achievement were associated with increased levels of deprivation and variation in achievement between practices increased with deprivation. • In years 2 and 3, practices from the more deprived quintiles improved at the fastest rates and variation decreased. Source: Doran Tet al; Effect of financial incentives on inequalities in the delivery of primary medical care in England: analysis of clinical activity indicators for the QOF, The Lancet 2008; Vol 372
There is also evidence that the QOF is reducing the gap in performance between practices in areas of high and low deprivation Primary Medical Care • Average levels of achievement have increased over the three years of the QOF, and variation in achievement has diminished. • In year 1, lower levels of achievement were associated with increased levels of deprivation and variation in achievement between practices increased with deprivation. • In years 2 and 3, practices from the more deprived quintiles improved at the fastest rates and variation decreased. Source: Doran Tet al; Effect of financial incentives on inequalities in the delivery of primary medical care in England: analysis of clinical activity indicators for the QOF, The Lancet 2008; Vol 372
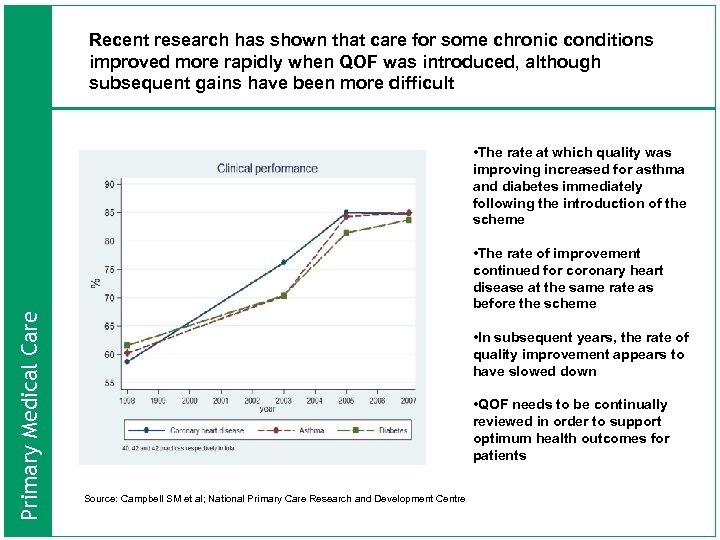 Recent research has shown that care for some chronic conditions improved more rapidly when QOF was introduced, although subsequent gains have been more difficult Primary Medical Care • The rate at which quality was improving increased for asthma and diabetes immediately following the introduction of the scheme • The rate of improvement continued for coronary heart disease at the same rate as before the scheme • In subsequent years, the rate of quality improvement appears to have slowed down • QOF needs to be continually reviewed in order to support optimum health outcomes for patients Source: Campbell SM et al; National Primary Care Research and Development Centre
Recent research has shown that care for some chronic conditions improved more rapidly when QOF was introduced, although subsequent gains have been more difficult Primary Medical Care • The rate at which quality was improving increased for asthma and diabetes immediately following the introduction of the scheme • The rate of improvement continued for coronary heart disease at the same rate as before the scheme • In subsequent years, the rate of quality improvement appears to have slowed down • QOF needs to be continually reviewed in order to support optimum health outcomes for patients Source: Campbell SM et al; National Primary Care Research and Development Centre
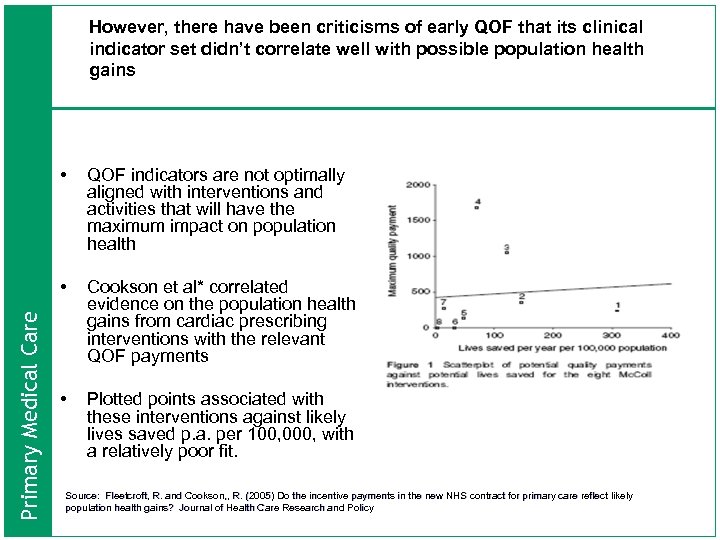 However, there have been criticisms of early QOF that its clinical indicator set didn’t correlate well with possible population health gains QOF indicators are not optimally aligned with interventions and activities that will have the maximum impact on population health • Primary Medical Care • Cookson et al* correlated evidence on the population health gains from cardiac prescribing interventions with the relevant QOF payments • Plotted points associated with these interventions against likely lives saved p. a. per 100, 000, with a relatively poor fit. Source: Fleetcroft, R. and Cookson, , R. (2005) Do the incentive payments in the new NHS contract for primary care reflect likely population health gains? Journal of Health Care Research and Policy
However, there have been criticisms of early QOF that its clinical indicator set didn’t correlate well with possible population health gains QOF indicators are not optimally aligned with interventions and activities that will have the maximum impact on population health • Primary Medical Care • Cookson et al* correlated evidence on the population health gains from cardiac prescribing interventions with the relevant QOF payments • Plotted points associated with these interventions against likely lives saved p. a. per 100, 000, with a relatively poor fit. Source: Fleetcroft, R. and Cookson, , R. (2005) Do the incentive payments in the new NHS contract for primary care reflect likely population health gains? Journal of Health Care Research and Policy
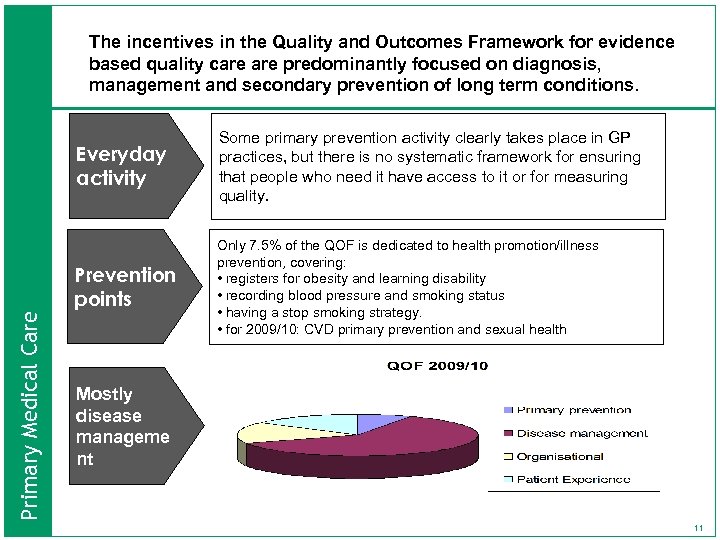 The incentives in the Quality and Outcomes Framework for evidence based quality care predominantly focused on diagnosis, management and secondary prevention of long term conditions. Prevention points Primary Medical Care Everyday activity Some primary prevention activity clearly takes place in GP practices, but there is no systematic framework for ensuring that people who need it have access to it or for measuring quality. Only 7. 5% of the QOF is dedicated to health promotion/illness prevention, covering: • registers for obesity and learning disability • recording blood pressure and smoking status • having a stop smoking strategy. • for 2009/10: CVD primary prevention and sexual health Mostly disease manageme nt 11
The incentives in the Quality and Outcomes Framework for evidence based quality care predominantly focused on diagnosis, management and secondary prevention of long term conditions. Prevention points Primary Medical Care Everyday activity Some primary prevention activity clearly takes place in GP practices, but there is no systematic framework for ensuring that people who need it have access to it or for measuring quality. Only 7. 5% of the QOF is dedicated to health promotion/illness prevention, covering: • registers for obesity and learning disability • recording blood pressure and smoking status • having a stop smoking strategy. • for 2009/10: CVD primary prevention and sexual health Mostly disease manageme nt 11
 National Audit Office Report on GP contract modernisation Recommendations to the Department of Health • Develop a long term strategy to support yearly negotiations on the QOF and develop the QOF based on patient needs and in a transparent way Primary Medical Care • Base the strategy more on outcomes and cost effectiveness • Agree to allocate a proportion of QOF indicators for local negotiation at Strategic Health Authority (SHA) or PCT level • Consider the case for time-limiting QOF points.
National Audit Office Report on GP contract modernisation Recommendations to the Department of Health • Develop a long term strategy to support yearly negotiations on the QOF and develop the QOF based on patient needs and in a transparent way Primary Medical Care • Base the strategy more on outcomes and cost effectiveness • Agree to allocate a proportion of QOF indicators for local negotiation at Strategic Health Authority (SHA) or PCT level • Consider the case for time-limiting QOF points.
 Aims and objectives of the new process • all stakeholders have a clear opportunity to contribute to the development of indicators; • indicators should address topics of importance to patients, professionals and the health of the public and help professionals; • Indicators should address inequalities in health; Primary Medical Care • indicators proposed for inclusion are based on evidence of clinical and cost effectiveness and make the best use of NHS resources; • there is an objective and transparent system for setting the value of a QOF indicator; • existing indicators are reviewed regularly; • potential new indicators are tested through piloting and considered in terms of whether they are workable; • all processes and methods are inclusive, open, transparent and consistently applied; • there appropriate governance structures and clear working arrangements with other relevant parties.
Aims and objectives of the new process • all stakeholders have a clear opportunity to contribute to the development of indicators; • indicators should address topics of importance to patients, professionals and the health of the public and help professionals; • Indicators should address inequalities in health; Primary Medical Care • indicators proposed for inclusion are based on evidence of clinical and cost effectiveness and make the best use of NHS resources; • there is an objective and transparent system for setting the value of a QOF indicator; • existing indicators are reviewed regularly; • potential new indicators are tested through piloting and considered in terms of whether they are workable; • all processes and methods are inclusive, open, transparent and consistently applied; • there appropriate governance structures and clear working arrangements with other relevant parties.
 Why should NICE lead the process? NICE is an independent body with statutory responsibility for providing guidance to the NHS based on evidence of clinical effectiveness and cost effectiveness. The aim is for new QOF indicators to be underpinned by NICE evidence-based clinical and public health recommendations relevant to primary care. • NICE currently has a very high degree of operational independence from the Department of Health and is responsible for developing its methodology and guidance independently. • Primary Medical Care • NICE already produces guidance aimed at general practice. It has a well established track record in producing evidence-based guidance and consults widely. • Asking NICE to manage the new process will build on the excellent work of the current QOF expert panel, whilst also ensuring that the assessment of evidence is clearly seen to be independent of the subsequent process for negotiating and approving changes to the QOF. • NICE’s guidance is based on a rigorous assessment of the best available evidence and involves wide consultation with stakeholders and an independent appeals process.
Why should NICE lead the process? NICE is an independent body with statutory responsibility for providing guidance to the NHS based on evidence of clinical effectiveness and cost effectiveness. The aim is for new QOF indicators to be underpinned by NICE evidence-based clinical and public health recommendations relevant to primary care. • NICE currently has a very high degree of operational independence from the Department of Health and is responsible for developing its methodology and guidance independently. • Primary Medical Care • NICE already produces guidance aimed at general practice. It has a well established track record in producing evidence-based guidance and consults widely. • Asking NICE to manage the new process will build on the excellent work of the current QOF expert panel, whilst also ensuring that the assessment of evidence is clearly seen to be independent of the subsequent process for negotiating and approving changes to the QOF. • NICE’s guidance is based on a rigorous assessment of the best available evidence and involves wide consultation with stakeholders and an independent appeals process.
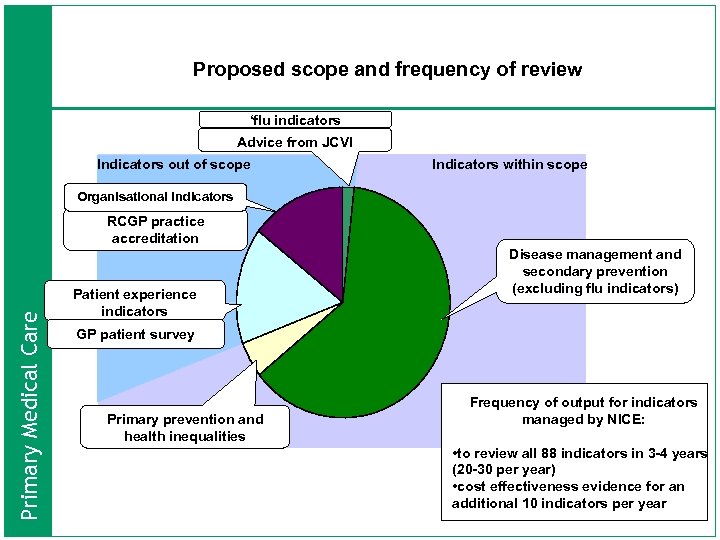 Proposed scope and frequency of review ‘flu indicators Advice from JCVI Indicators out of scope Indicators within scope Organisational indicators Primary Medical Care RCGP practice accreditation Patient experience indicators Disease management and secondary prevention (excluding flu indicators) GP patient survey Primary prevention and health inequalities Frequency of output for indicators managed by NICE: • to review all 88 indicators in 3 -4 years (20 -30 per year) • cost effectiveness evidence for an additional 10 indicators per year
Proposed scope and frequency of review ‘flu indicators Advice from JCVI Indicators out of scope Indicators within scope Organisational indicators Primary Medical Care RCGP practice accreditation Patient experience indicators Disease management and secondary prevention (excluding flu indicators) GP patient survey Primary prevention and health inequalities Frequency of output for indicators managed by NICE: • to review all 88 indicators in 3 -4 years (20 -30 per year) • cost effectiveness evidence for an additional 10 indicators per year
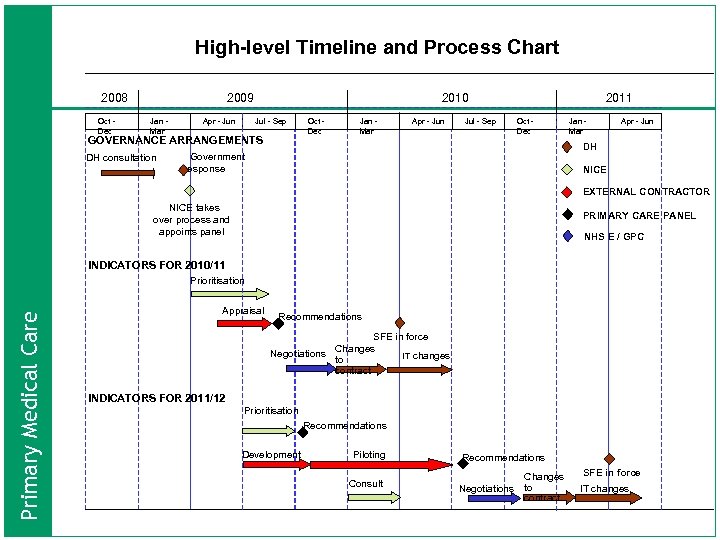 High-level Timeline and Process Chart 2008 Oct Dec 2009 Jan Mar Apr - Jun 2010 Jul - Sep GOVERNANCE ARRANGEMENTS DH consultation Oct Dec Jan Mar Apr - Jun Jul - Sep 2011 Oct Dec Jan Mar Apr - Jun DH Government response NICE EXTERNAL CONTRACTOR NICE takes over process and appoints panel PRIMARY CARE PANEL NHS E / GPC INDICATORS FOR 2010/11 Primary Medical Care Prioritisation Appraisal Recommendations SFE in force Changes Negotiations IT changes to contract INDICATORS FOR 2011/12 Prioritisation Recommendations Development Piloting Consult Recommendations Negotiations Changes to contract SFE in force IT changes
High-level Timeline and Process Chart 2008 Oct Dec 2009 Jan Mar Apr - Jun 2010 Jul - Sep GOVERNANCE ARRANGEMENTS DH consultation Oct Dec Jan Mar Apr - Jun Jul - Sep 2011 Oct Dec Jan Mar Apr - Jun DH Government response NICE EXTERNAL CONTRACTOR NICE takes over process and appoints panel PRIMARY CARE PANEL NHS E / GPC INDICATORS FOR 2010/11 Primary Medical Care Prioritisation Appraisal Recommendations SFE in force Changes Negotiations IT changes to contract INDICATORS FOR 2011/12 Prioritisation Recommendations Development Piloting Consult Recommendations Negotiations Changes to contract SFE in force IT changes
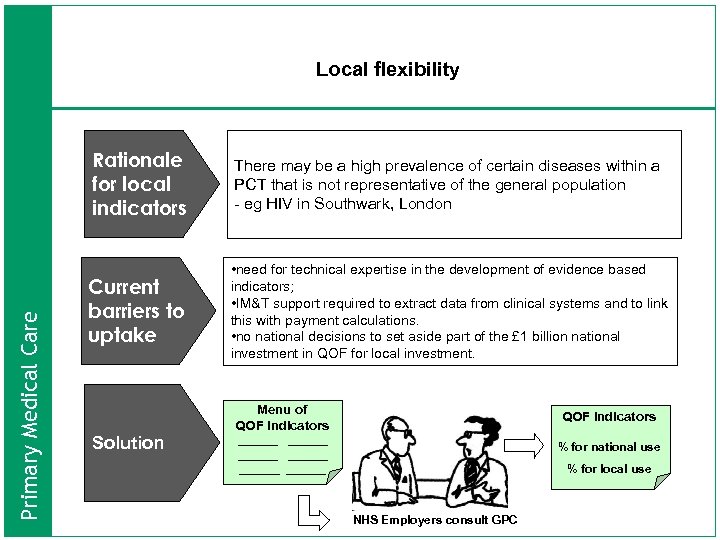 Local flexibility Primary Medical Care Rationale for local indicators There may be a high prevalence of certain diseases within a PCT that is not representative of the general population - eg HIV in Southwark, London Current barriers to uptake • need for technical expertise in the development of evidence based indicators; • IM&T support required to extract data from clinical systems and to link this with payment calculations. • no national decisions to set aside part of the £ 1 billion national investment in QOF for local investment. Menu of QOF indicators Solution QOF indicators ______ ______ % for national use % for local use NHS Employers consult GPC
Local flexibility Primary Medical Care Rationale for local indicators There may be a high prevalence of certain diseases within a PCT that is not representative of the general population - eg HIV in Southwark, London Current barriers to uptake • need for technical expertise in the development of evidence based indicators; • IM&T support required to extract data from clinical systems and to link this with payment calculations. • no national decisions to set aside part of the £ 1 billion national investment in QOF for local investment. Menu of QOF indicators Solution QOF indicators ______ ______ % for national use % for local use NHS Employers consult GPC
 UK collaboration • Our aim is for a collaborative approach to developing and reviewing indicators across the four UK countries. Primary Medical Care • Each of the four countries could remain within a UK framework, with local flexibility according to specific health needs. • NICE is responsible for evidence based guidelines for England, Wales and Northern Ireland. • There is already good collaboration between NICE and NHS Quality Improvement Scotland. In the future, NICE could use guidance developed from other sources, including SIGN guidance, subject to the availability of cost effectiveness information.
UK collaboration • Our aim is for a collaborative approach to developing and reviewing indicators across the four UK countries. Primary Medical Care • Each of the four countries could remain within a UK framework, with local flexibility according to specific health needs. • NICE is responsible for evidence based guidelines for England, Wales and Northern Ireland. • There is already good collaboration between NICE and NHS Quality Improvement Scotland. In the future, NICE could use guidance developed from other sources, including SIGN guidance, subject to the availability of cost effectiveness information.
 Developing the Quality and Outcomes Framework: Proposals for a new, independent process Responding to the consultation QOFConsultation@dh. gsi. gov. uk Primary Medical Care Quality Team, Primary Medical Care, Room 2 E 56, Quarry House, Quarry Hill, Leeds LS 2 7 UE http: //www. dh. gov. uk/en/Consultations/Liveconsultations/DH_089778
Developing the Quality and Outcomes Framework: Proposals for a new, independent process Responding to the consultation QOFConsultation@dh. gsi. gov. uk Primary Medical Care Quality Team, Primary Medical Care, Room 2 E 56, Quarry House, Quarry Hill, Leeds LS 2 7 UE http: //www. dh. gov. uk/en/Consultations/Liveconsultations/DH_089778
 National QOF Consultation Developing the Quality and Outcomes Framework: Proposals for a new, independent process Tuesday 6 th January, Birmingham
National QOF Consultation Developing the Quality and Outcomes Framework: Proposals for a new, independent process Tuesday 6 th January, Birmingham
 Outline Process for Developing Indicators Dr Gillian Leng, Chief Operating Officer for NHS Evidence and Deputy Chief Executive, National Institute of Clinical Excellence
Outline Process for Developing Indicators Dr Gillian Leng, Chief Operating Officer for NHS Evidence and Deputy Chief Executive, National Institute of Clinical Excellence
 Outline of process for developing indicators for the Quality and Outcomes Framework National Institute for Health and Clinical Excellence (NICE)
Outline of process for developing indicators for the Quality and Outcomes Framework National Institute for Health and Clinical Excellence (NICE)
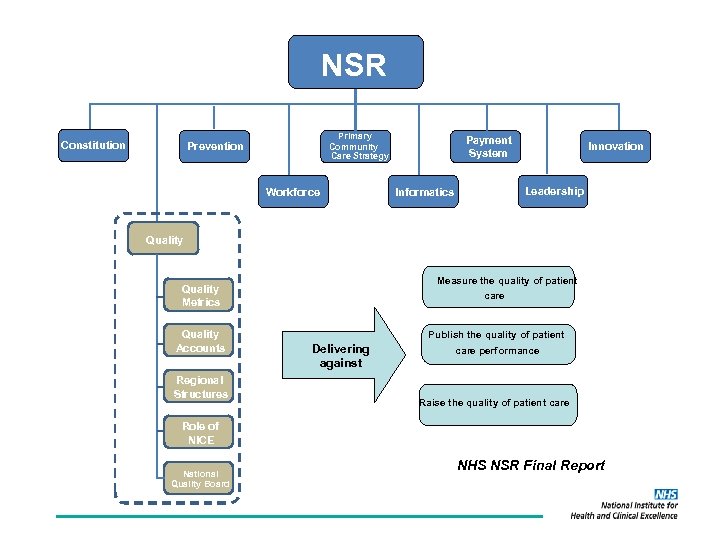 NSR NHS Constitution Primary Community Care Strategy Prevention Workforce Payment System Informatics Innovation Leadership Quality Measure the quality of patient care Quality Metrics Quality Accounts Regional Structures Publish the quality of patient Delivering against care performance Raise the quality of patient care Role of NICE National Quality Board NHS NSR Final Report
NSR NHS Constitution Primary Community Care Strategy Prevention Workforce Payment System Informatics Innovation Leadership Quality Measure the quality of patient care Quality Metrics Quality Accounts Regional Structures Publish the quality of patient Delivering against care performance Raise the quality of patient care Role of NICE National Quality Board NHS NSR Final Report
 Expanded role for NICE • Response to ‘the Darzi Review’ – More/faster TAs – Devices and diagnostics – NICE Fellows – More Clinical Guidelines/Public Health guidance – National Quality Standards – NHS Evidence – Quality and Outcomes Framework
Expanded role for NICE • Response to ‘the Darzi Review’ – More/faster TAs – Devices and diagnostics – NICE Fellows – More Clinical Guidelines/Public Health guidance – National Quality Standards – NHS Evidence – Quality and Outcomes Framework
 Core principles for development of NICE products • • Comprehensive evidence base Expert input • Patient and carer involvement • Independent advisory Committees • • Genuine consultation and contestability Regular review • Open and transparent process
Core principles for development of NICE products • • Comprehensive evidence base Expert input • Patient and carer involvement • Independent advisory Committees • • Genuine consultation and contestability Regular review • Open and transparent process
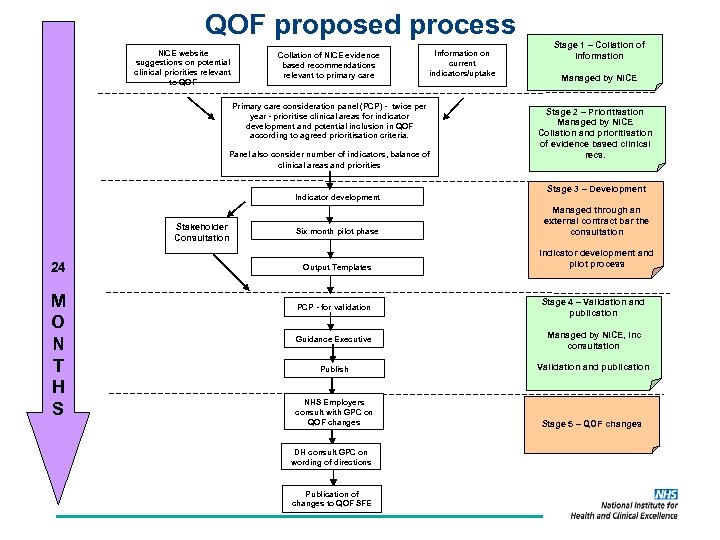 QOF proposed process NICE website suggestions on potential clinical priorities relevant to QOF Collation of NICE evidence based recommendations relevant to primary care Information on current indicators/uptake Primary care consideration panel (PCP) - twice per year - prioritise clinical areas for indicator development and potential inclusion in QOF according to agreed prioritisation criteria. Panel also consider number of indicators, balance of clinical areas and priorities Indicator development Stakeholder Consultation 24 M O N T H S Stage 1 – Collation of information Managed by NICE Stage 2 – Prioritisation Managed by NICE Collation and prioritisation of evidence based clinical recs. Stage 3 – Development Six month pilot phase Managed through an external contract bar the consultation Output Templates Indicator development and pilot process PCP - for validation Stage 4 – Validation and publication Guidance Executive Managed by NICE, inc consultation Publish Validation and publication NHS Employers consult with GPC on QOF changes Stage 5 – QOF changes DH consult GPC on wording of directions Publication of changes to QOF SFE
QOF proposed process NICE website suggestions on potential clinical priorities relevant to QOF Collation of NICE evidence based recommendations relevant to primary care Information on current indicators/uptake Primary care consideration panel (PCP) - twice per year - prioritise clinical areas for indicator development and potential inclusion in QOF according to agreed prioritisation criteria. Panel also consider number of indicators, balance of clinical areas and priorities Indicator development Stakeholder Consultation 24 M O N T H S Stage 1 – Collation of information Managed by NICE Stage 2 – Prioritisation Managed by NICE Collation and prioritisation of evidence based clinical recs. Stage 3 – Development Six month pilot phase Managed through an external contract bar the consultation Output Templates Indicator development and pilot process PCP - for validation Stage 4 – Validation and publication Guidance Executive Managed by NICE, inc consultation Publish Validation and publication NHS Employers consult with GPC on QOF changes Stage 5 – QOF changes DH consult GPC on wording of directions Publication of changes to QOF SFE
 Process for developing indicators • Stage 1 – Collation of information E IC N Y B ED G – Collation of evidence based recommendations NA A M relevant to primary care – NICE website suggestions on potential clinical priorities relevant to QOF – Information on current indicators uptake
Process for developing indicators • Stage 1 – Collation of information E IC N Y B ED G – Collation of evidence based recommendations NA A M relevant to primary care – NICE website suggestions on potential clinical priorities relevant to QOF – Information on current indicators uptake
 Process for developing indicators • Stage 2 – Prioritisation of areas for indicator development E IC N Y B ED G - Primary Care Consideration Panel will meet twice a year NA A M using prioritisation criteria - Decisions made - Prioritisation of new areas for the development of indicators and process for dealing with current indicators - Panel consider numbers of indicators, balance of clinical areas and priorities.
Process for developing indicators • Stage 2 – Prioritisation of areas for indicator development E IC N Y B ED G - Primary Care Consideration Panel will meet twice a year NA A M using prioritisation criteria - Decisions made - Prioritisation of new areas for the development of indicators and process for dealing with current indicators - Panel consider numbers of indicators, balance of clinical areas and priorities.
 Primary Care Consideration Panel • Chaired by an acknowledged expert in primary medical care • Formal Advisory Body status • Meet twice a year • Approximately 30 individuals • Range of experts and representatives of primary care workforce – GPs, patients or carers, commissioners, practice nurses social care professionals from countries taking part and health economists and information specialists
Primary Care Consideration Panel • Chaired by an acknowledged expert in primary medical care • Formal Advisory Body status • Meet twice a year • Approximately 30 individuals • Range of experts and representatives of primary care workforce – GPs, patients or carers, commissioners, practice nurses social care professionals from countries taking part and health economists and information specialists
 Process for developing indicators LY AL • Stage 3 – Indicator Development (managed through external contract bar consultation step) RN E XT E - Current indicators reviewed and cost effectiveness ED applied methodology G A N A - Piloting of indicators M - New indicators developed - External stakeholder consultation run by NICE
Process for developing indicators LY AL • Stage 3 – Indicator Development (managed through external contract bar consultation step) RN E XT E - Current indicators reviewed and cost effectiveness ED applied methodology G A N A - Piloting of indicators M - New indicators developed - External stakeholder consultation run by NICE
 Assessing cost effectiveness. General principles • An indicator is cost effective where net benefit >0 Net benefit = (monetised benefit – delivery cost) – QOF payment • Delivery cost is the cost to deliver the treatment/intervention offset by any savings where new treatments replace older treatments • Monetised benefit is derived from the expected increase in quality adjusted life year (QALY). NICE will need to identify an appropriate QALY threshold cost, which is expected to be within the range £ 20, 000£ 30, 000 • QOF payment is an initial incentive to embed within general practice best evidence-based care that will continue to improve patients’ care and health
Assessing cost effectiveness. General principles • An indicator is cost effective where net benefit >0 Net benefit = (monetised benefit – delivery cost) – QOF payment • Delivery cost is the cost to deliver the treatment/intervention offset by any savings where new treatments replace older treatments • Monetised benefit is derived from the expected increase in quality adjusted life year (QALY). NICE will need to identify an appropriate QALY threshold cost, which is expected to be within the range £ 20, 000£ 30, 000 • QOF payment is an initial incentive to embed within general practice best evidence-based care that will continue to improve patients’ care and health
 Process for developing indicators • Stage 4 – Validation and Publication E IC N Y B ED and information - Menu of new G indicators about current indicators NA A - Recommendations about review dates -M Potential upper and lower thresholds - Validation and publication of outputs via NICE website - Assessment of evidence on cost-effectiveness to inform decisions on the value of indicators
Process for developing indicators • Stage 4 – Validation and Publication E IC N Y B ED and information - Menu of new G indicators about current indicators NA A - Recommendations about review dates -M Potential upper and lower thresholds - Validation and publication of outputs via NICE website - Assessment of evidence on cost-effectiveness to inform decisions on the value of indicators
 Process for developing indicators • Stage 5 – QOF changes DHinto - Indicators published on NICE website fed Y B DH for negotiation ED - NHS Employers consult with AG General Practice. N A Committee (GPC) on QOF changes M - DH consult with GPC on wording of directions - Publication of changes to QOF Statement of Financial Entitlements
Process for developing indicators • Stage 5 – QOF changes DHinto - Indicators published on NICE website fed Y B DH for negotiation ED - NHS Employers consult with AG General Practice. N A Committee (GPC) on QOF changes M - DH consult with GPC on wording of directions - Publication of changes to QOF Statement of Financial Entitlements
 Next steps • Tender process for external contractor currently running – At consultation events, a record of questions is being kept and will be communicated to all interested parties as part of the tender procedure – Should anyone be considering bidding, any discussion in response to the questions raised at the events will not constitute the office tender view • Timelines – Offers submitted by 6 th February 2009 – Interviews to be held between 9 -13 th March 2009 – Contract to be in place by the start of April 2009
Next steps • Tender process for external contractor currently running – At consultation events, a record of questions is being kept and will be communicated to all interested parties as part of the tender procedure – Should anyone be considering bidding, any discussion in response to the questions raised at the events will not constitute the office tender view • Timelines – Offers submitted by 6 th February 2009 – Interviews to be held between 9 -13 th March 2009 – Contract to be in place by the start of April 2009
 Next steps • Recruiting to Primary Care Consideration Panel early 2009 • Setting up internal project management structures • Proposed process for indicator development will be subject to consultation in 2009
Next steps • Recruiting to Primary Care Consideration Panel early 2009 • Setting up internal project management structures • Proposed process for indicator development will be subject to consultation in 2009
 National QOF Consultation Developing the Quality and Outcomes Framework: Proposals for a new, independent process Tuesday 6 th January, Birmingham
National QOF Consultation Developing the Quality and Outcomes Framework: Proposals for a new, independent process Tuesday 6 th January, Birmingham
 Panel Q & A § Please wait for a microphone before asking your question § Please state your name and organisation § Please keep your questions in the context of the Consultation
Panel Q & A § Please wait for a microphone before asking your question § Please state your name and organisation § Please keep your questions in the context of the Consultation
 National QOF Consultation Developing the Quality and Outcomes Framework: Proposals for a new, independent process Tuesday 6 th January, Birmingham
National QOF Consultation Developing the Quality and Outcomes Framework: Proposals for a new, independent process Tuesday 6 th January, Birmingham
 Workshop Briefing
Workshop Briefing
 Refreshments Please be ready to start Workshop Session One at 12. 00
Refreshments Please be ready to start Workshop Session One at 12. 00
 Workshop Sessions Criteria for selection process Room: Orchid QOF cost effectiveness methodology Room: Palm Room
Workshop Sessions Criteria for selection process Room: Orchid QOF cost effectiveness methodology Room: Palm Room
 Draft selection criteria for areas for developing indicators for the quality and outcomes framework Primary Medical Care Remit 1. Is the proposed topic within NICE’s remit? 2. Has NICE already provided guidance or is NICE developing guidance on the proposed topic? 3. Is the topic one where GPs can have a significant contribution to make in terms of improving patients’ health? Health improvement and reduction of health inequalities 1. Do the proposed indicators relate to an NHS clinical priority areas, or to other health-related government priorities? 2. Do the proposed indicators address an area of action where introduction of evidence-based indicators in primary medical care would lead to cost effective improvements in the delivery of health care? 3. Are the consequences understood? Are the costs for other sectors proportionate? Are they affordable and deliverable in the short term? 4. For public health topics, do the indicators address an area of public health action that promotes population health? 5. For clinical topics, do the indicators address a condition which is associated with significant morbidity or mortality?
Draft selection criteria for areas for developing indicators for the quality and outcomes framework Primary Medical Care Remit 1. Is the proposed topic within NICE’s remit? 2. Has NICE already provided guidance or is NICE developing guidance on the proposed topic? 3. Is the topic one where GPs can have a significant contribution to make in terms of improving patients’ health? Health improvement and reduction of health inequalities 1. Do the proposed indicators relate to an NHS clinical priority areas, or to other health-related government priorities? 2. Do the proposed indicators address an area of action where introduction of evidence-based indicators in primary medical care would lead to cost effective improvements in the delivery of health care? 3. Are the consequences understood? Are the costs for other sectors proportionate? Are they affordable and deliverable in the short term? 4. For public health topics, do the indicators address an area of public health action that promotes population health? 5. For clinical topics, do the indicators address a condition which is associated with significant morbidity or mortality?
 Draft selection criteria for areas for developing indicators for the quality and outcomes framework Primary Medical Care Effect of intervention Do the indicators: 1. significantly improve patients’ or carers’ quality of life; and/or 2. reduce avoidable morbidity; and/or 3. reduce avoidable premature mortality; and/or 4. reduce inequalities in health relative to current standard practice if used more extensively or more appropriately? Timeliness 1. Is this an area of QOF where existing indicators are coming up for review? 2. Would new indicators support implementation of new NICE guidance or National Service Frameworks which are in development or recently published? 3. Is there emerging evidence for developing new indicators with direct health benefit where there are currently no indicators or where existing indicators do not measure direct health benefit? 4. Is there a degree of urgency for introducing indicators caused by factors other than those listed above, for example, significant public concern, a new disease, an important new area for public health action? 5. Would the indicators still be relevant and timely at the expected date of use?
Draft selection criteria for areas for developing indicators for the quality and outcomes framework Primary Medical Care Effect of intervention Do the indicators: 1. significantly improve patients’ or carers’ quality of life; and/or 2. reduce avoidable morbidity; and/or 3. reduce avoidable premature mortality; and/or 4. reduce inequalities in health relative to current standard practice if used more extensively or more appropriately? Timeliness 1. Is this an area of QOF where existing indicators are coming up for review? 2. Would new indicators support implementation of new NICE guidance or National Service Frameworks which are in development or recently published? 3. Is there emerging evidence for developing new indicators with direct health benefit where there are currently no indicators or where existing indicators do not measure direct health benefit? 4. Is there a degree of urgency for introducing indicators caused by factors other than those listed above, for example, significant public concern, a new disease, an important new area for public health action? 5. Would the indicators still be relevant and timely at the expected date of use?
 National QOF Consultation Developing the Quality and Outcomes Framework: Proposals for a new, independent process Tuesday 6 th January, Birmingham
National QOF Consultation Developing the Quality and Outcomes Framework: Proposals for a new, independent process Tuesday 6 th January, Birmingham
 Feedback, Other Issues & Next Steps Graham Urwin, Chief Executive, Stoke on Trent PCT
Feedback, Other Issues & Next Steps Graham Urwin, Chief Executive, Stoke on Trent PCT
 Event Close • Thank you for attending • Please remember to hand in your delegate badge for recycling
Event Close • Thank you for attending • Please remember to hand in your delegate badge for recycling
 Developing the Quality and Outcomes Framework: Proposals for a new, independent process Responding to the consultation QOFConsultation@dh. gsi. gov. uk Primary Medical Care Quality Team, Primary Medical Care, Room 2 E 56, Quarry House, Quarry Hill, Leeds LS 2 7 UE http: //www. dh. gov. uk/en/Consultations/Liveconsultations/DH_089778
Developing the Quality and Outcomes Framework: Proposals for a new, independent process Responding to the consultation QOFConsultation@dh. gsi. gov. uk Primary Medical Care Quality Team, Primary Medical Care, Room 2 E 56, Quarry House, Quarry Hill, Leeds LS 2 7 UE http: //www. dh. gov. uk/en/Consultations/Liveconsultations/DH_089778


