480e9598c53787f7b8131ce4c9e8ca42.ppt
- Количество слайдов: 31
 Multi-center Assessment of the Utilization of SPECT Myocardial Perfusion Imaging Using the ACCF Appropriateness Criteria: The ACCF and United Healthcare SPECT Pilot Study Robert C. Hendel, Manual Cerqueira, Kathleen Hewitt, Karen Caruth, Joseph Allen, Neil Jensen, Michael Wolk, Pamela S. Douglas, Ralph Brindis, American College of Cardiology Foundation, Washington, DC, United. Healthcare, Minneapolis, MN Robert C. Hendel, MD, FACC Midwest Heart Specialists Winfield, IL Chairman, ACCF/UHC SPECT-MPI Pilot Study Late Breaking Clinical Trials American College of Cardiology Scientific Sessions 2009 March 29, 2009
Multi-center Assessment of the Utilization of SPECT Myocardial Perfusion Imaging Using the ACCF Appropriateness Criteria: The ACCF and United Healthcare SPECT Pilot Study Robert C. Hendel, Manual Cerqueira, Kathleen Hewitt, Karen Caruth, Joseph Allen, Neil Jensen, Michael Wolk, Pamela S. Douglas, Ralph Brindis, American College of Cardiology Foundation, Washington, DC, United. Healthcare, Minneapolis, MN Robert C. Hendel, MD, FACC Midwest Heart Specialists Winfield, IL Chairman, ACCF/UHC SPECT-MPI Pilot Study Late Breaking Clinical Trials American College of Cardiology Scientific Sessions 2009 March 29, 2009
 Presenter Disclosure Information Robert C. Hendel, MD The following relationships exist related to this presentation: Consulting PGx Health Astellas Pharma GE Healthcare Modest Research support Astellas GE Healthcare Modest Organizational ACC (Appropriate Use Criteria Task Force)
Presenter Disclosure Information Robert C. Hendel, MD The following relationships exist related to this presentation: Consulting PGx Health Astellas Pharma GE Healthcare Modest Research support Astellas GE Healthcare Modest Organizational ACC (Appropriate Use Criteria Task Force)
 BACKGROUND • Growth and cost of CV imaging has placed renewed attention on proper/optimal test ordering • True nature of utilization unknown –Overuse/underuse/appropriate use • Development and publication of SPECT-MPI appropriate use criteria (AUC) in 2005 –Subsequent AUC for echo, CT, CMR –SPECT MPI revision 2009 • Criteria widely available and increasingly being adopted, but evaluation in community practice settings required
BACKGROUND • Growth and cost of CV imaging has placed renewed attention on proper/optimal test ordering • True nature of utilization unknown –Overuse/underuse/appropriate use • Development and publication of SPECT-MPI appropriate use criteria (AUC) in 2005 –Subsequent AUC for echo, CT, CMR –SPECT MPI revision 2009 • Criteria widely available and increasingly being adopted, but evaluation in community practice settings required
 GOALS OF STUDY • Assess feasibility of tracking AUC –Point-of-service data collection –Computer derived indication assignment • Determine patterns of use for SPECT MPI in clinical practice • Evaluate the impact of referral source • Identify selected areas (indications) for quality improvement
GOALS OF STUDY • Assess feasibility of tracking AUC –Point-of-service data collection –Computer derived indication assignment • Determine patterns of use for SPECT MPI in clinical practice • Evaluate the impact of referral source • Identify selected areas (indications) for quality improvement
 METHODS • Sites selected by ACC from potential locations provided by UHC • Data collection instrument and web-based entry system developed • Automated algorithm created • Audit of automated indication assignments • On-demand reports • Periodic overall and site-specific summaries provided
METHODS • Sites selected by ACC from potential locations provided by UHC • Data collection instrument and web-based entry system developed • Automated algorithm created • Audit of automated indication assignments • On-demand reports • Periodic overall and site-specific summaries provided
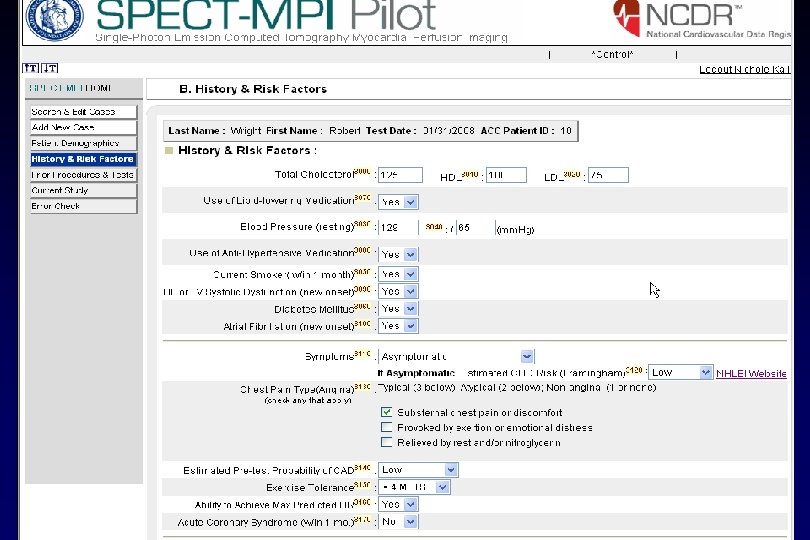
 DATA COLLECTION FORM • Front page – Patient Demographics – History & Risk Factors, – Prior procedures & Tests • Back page – Current Study – Reference section • Designed to be completed in one minute or less
DATA COLLECTION FORM • Front page – Patient Demographics – History & Risk Factors, – Prior procedures & Tests • Back page – Current Study – Reference section • Designed to be completed in one minute or less
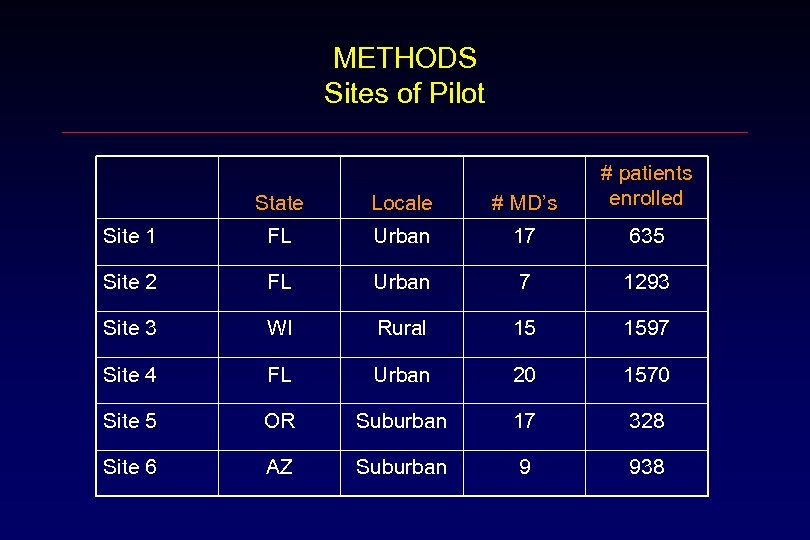 METHODS Sites of Pilot State Locale # MD’s # patients enrolled Site 1 FL Urban 17 635 Site 2 FL Urban 7 1293 Site 3 WI Rural 15 1597 Site 4 FL Urban 20 1570 Site 5 OR Suburban 17 328 Site 6 AZ Suburban 9 938
METHODS Sites of Pilot State Locale # MD’s # patients enrolled Site 1 FL Urban 17 635 Site 2 FL Urban 7 1293 Site 3 WI Rural 15 1597 Site 4 FL Urban 20 1570 Site 5 OR Suburban 17 328 Site 6 AZ Suburban 9 938
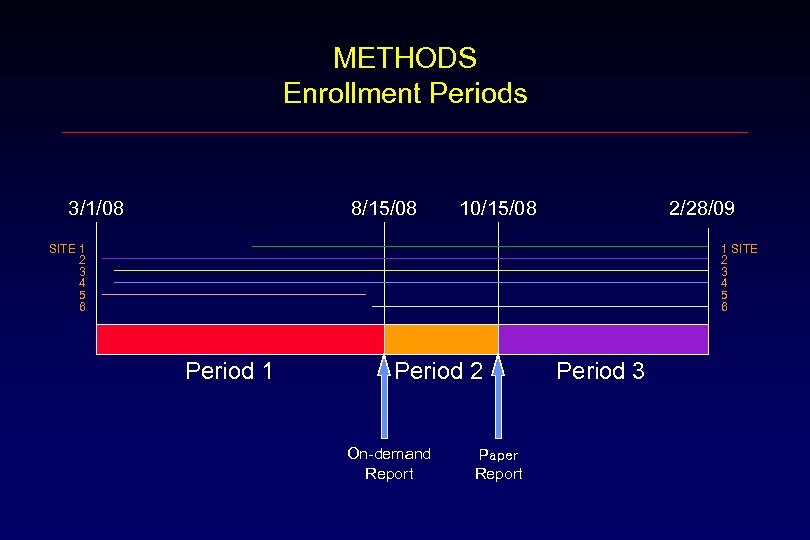 METHODS Enrollment Periods 3/1/08 8/15/08 10/15/08 2/28/09 SITE 1 2 3 4 5 6 1 SITE 2 3 4 5 6 Period 1 Period 2 On-demand Report Paper Report Period 3
METHODS Enrollment Periods 3/1/08 8/15/08 10/15/08 2/28/09 SITE 1 2 3 4 5 6 1 SITE 2 3 4 5 6 Period 1 Period 2 On-demand Report Paper Report Period 3
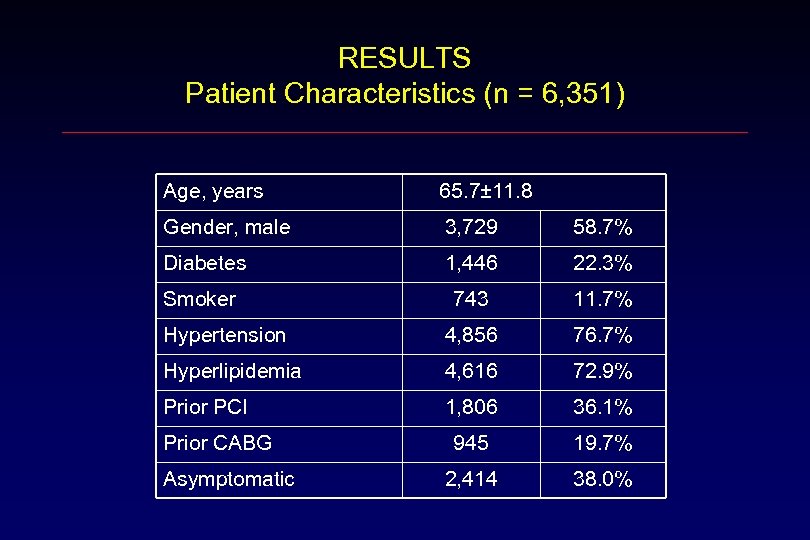 RESULTS Patient Characteristics (n = 6, 351) Age, years 65. 7± 11. 8 Gender, male 3, 729 58. 7% Diabetes 1, 446 22. 3% Smoker 743 11. 7% Hypertension 4, 856 76. 7% Hyperlipidemia 4, 616 72. 9% Prior PCI 1, 806 36. 1% 945 19. 7% 2, 414 38. 0% Prior CABG Asymptomatic
RESULTS Patient Characteristics (n = 6, 351) Age, years 65. 7± 11. 8 Gender, male 3, 729 58. 7% Diabetes 1, 446 22. 3% Smoker 743 11. 7% Hypertension 4, 856 76. 7% Hyperlipidemia 4, 616 72. 9% Prior PCI 1, 806 36. 1% 945 19. 7% 2, 414 38. 0% Prior CABG Asymptomatic
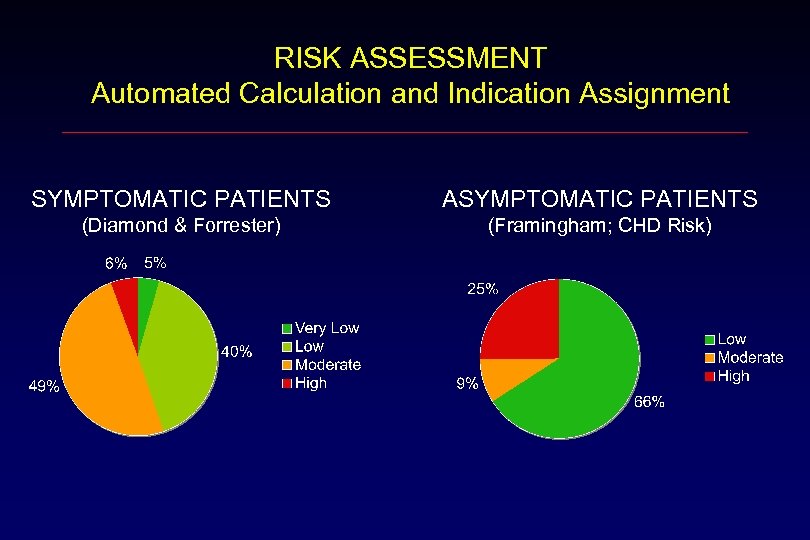 RISK ASSESSMENT Automated Calculation and Indication Assignment SYMPTOMATIC PATIENTS ASYMPTOMATIC PATIENTS (Diamond & Forrester) (Framingham; CHD Risk)
RISK ASSESSMENT Automated Calculation and Indication Assignment SYMPTOMATIC PATIENTS ASYMPTOMATIC PATIENTS (Diamond & Forrester) (Framingham; CHD Risk)
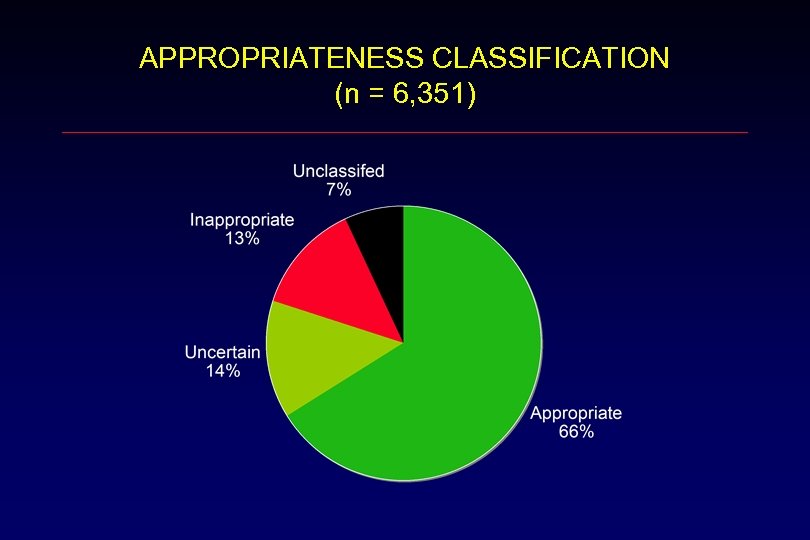 APPROPRIATENESS CLASSIFICATION (n = 6, 351)
APPROPRIATENESS CLASSIFICATION (n = 6, 351)
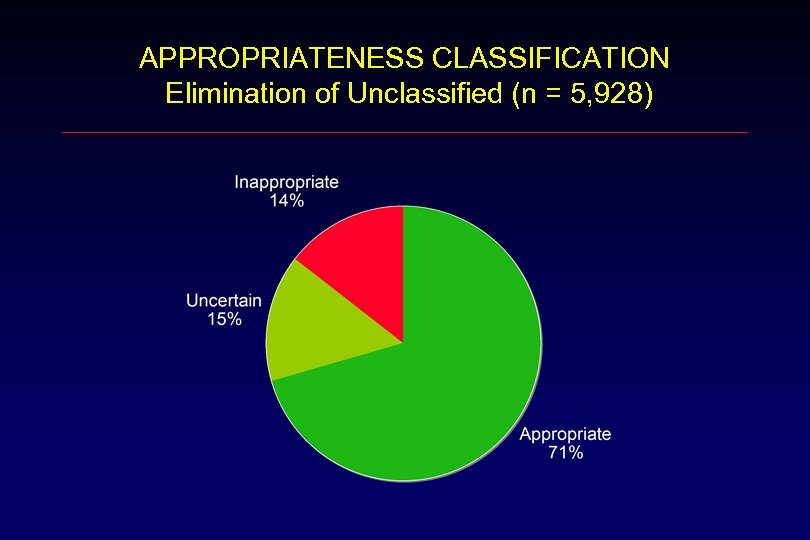 APPROPRIATENESS CLASSIFICATION Elimination of Unclassified (n = 5, 928)
APPROPRIATENESS CLASSIFICATION Elimination of Unclassified (n = 5, 928)
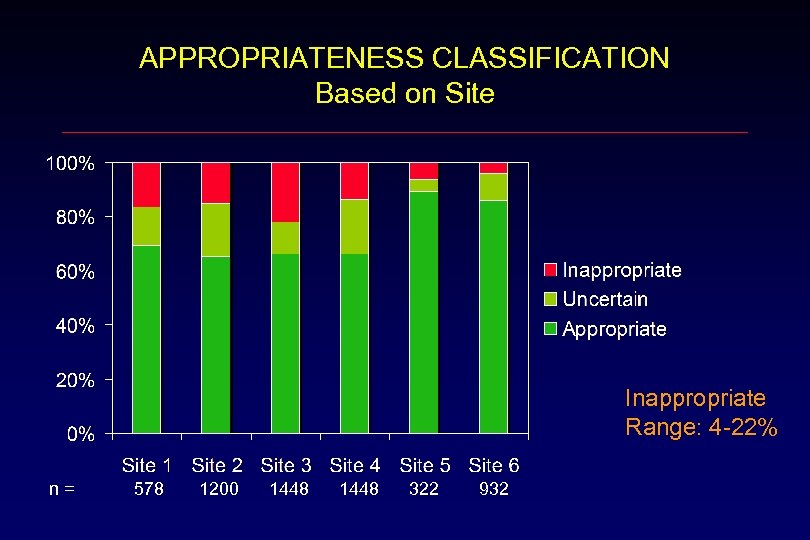 APPROPRIATENESS CLASSIFICATION Based on Site Inappropriate Range: 4 -22% n= 578 1200 1448 322 932
APPROPRIATENESS CLASSIFICATION Based on Site Inappropriate Range: 4 -22% n= 578 1200 1448 322 932
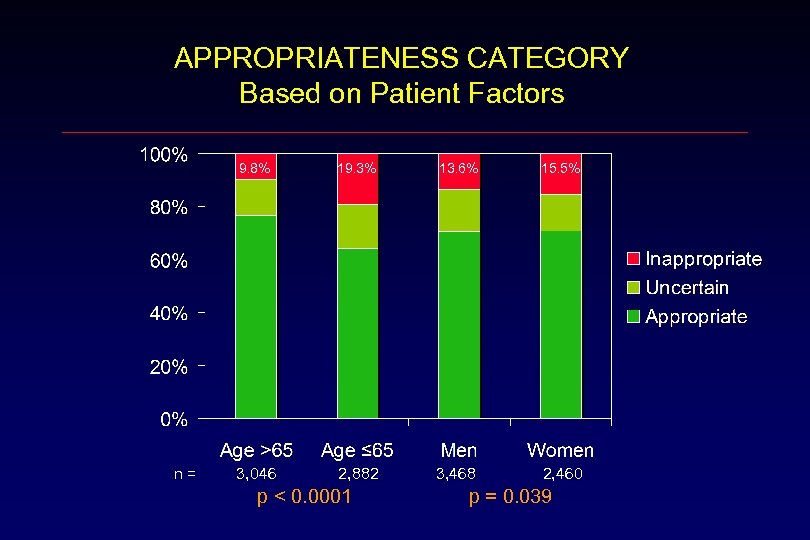 APPROPRIATENESS CATEGORY Based on Patient Factors 9. 8% n= 19. 3% 13. 6% 15. 5% 3, 046 2, 882 3, 468 2, 460 p < 0. 0001 p = 0. 039
APPROPRIATENESS CATEGORY Based on Patient Factors 9. 8% n= 19. 3% 13. 6% 15. 5% 3, 046 2, 882 3, 468 2, 460 p < 0. 0001 p = 0. 039
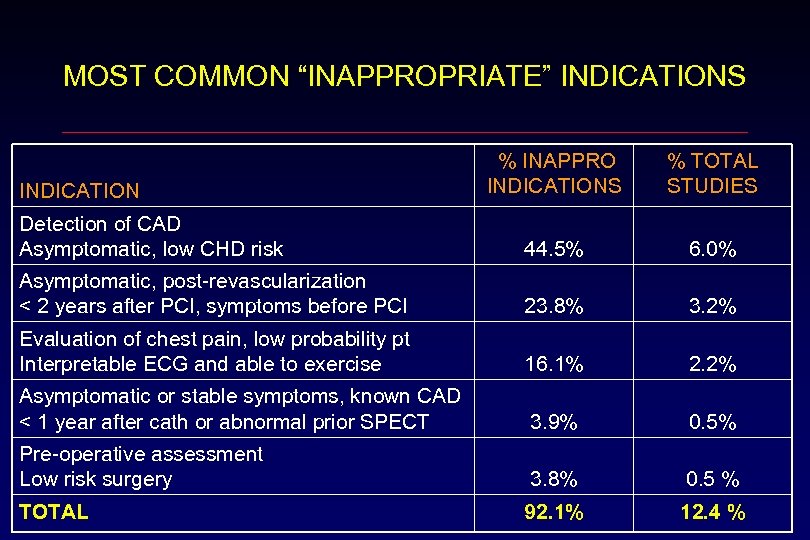 MOST COMMON “INAPPROPRIATE” INDICATIONS % INAPPRO INDICATIONS % TOTAL STUDIES Detection of CAD Asymptomatic, low CHD risk 44. 5% 6. 0% Asymptomatic, post-revascularization < 2 years after PCI, symptoms before PCI 23. 8% 3. 2% Evaluation of chest pain, low probability pt Interpretable ECG and able to exercise 16. 1% 2. 2% Asymptomatic or stable symptoms, known CAD < 1 year after cath or abnormal prior SPECT 3. 9% 0. 5% Pre-operative assessment Low risk surgery 3. 8% 0. 5 % TOTAL 92. 1% 12. 4 % INDICATION
MOST COMMON “INAPPROPRIATE” INDICATIONS % INAPPRO INDICATIONS % TOTAL STUDIES Detection of CAD Asymptomatic, low CHD risk 44. 5% 6. 0% Asymptomatic, post-revascularization < 2 years after PCI, symptoms before PCI 23. 8% 3. 2% Evaluation of chest pain, low probability pt Interpretable ECG and able to exercise 16. 1% 2. 2% Asymptomatic or stable symptoms, known CAD < 1 year after cath or abnormal prior SPECT 3. 9% 0. 5% Pre-operative assessment Low risk surgery 3. 8% 0. 5 % TOTAL 92. 1% 12. 4 % INDICATION
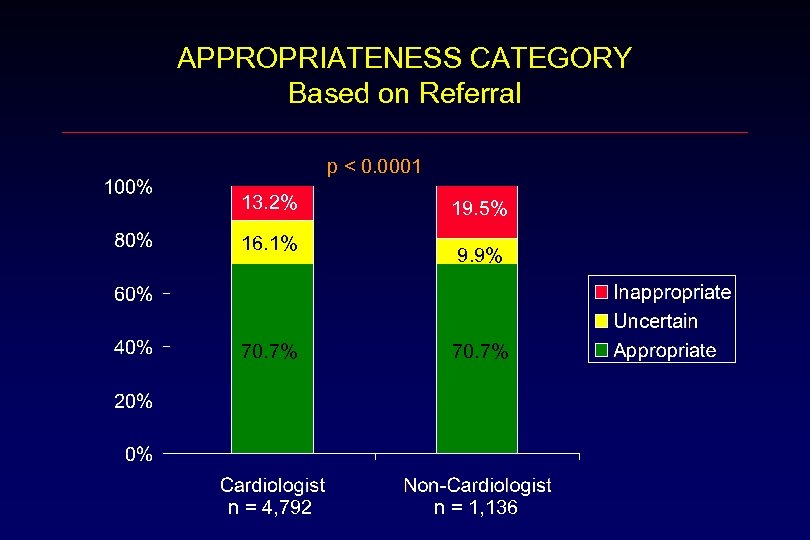 APPROPRIATENESS CATEGORY Based on Referral p < 0. 0001 13. 2% 16. 1% 19. 5% 9. 9% 70. 7% n = 4, 792 n = 1, 136
APPROPRIATENESS CATEGORY Based on Referral p < 0. 0001 13. 2% 16. 1% 19. 5% 9. 9% 70. 7% n = 4, 792 n = 1, 136
 APPROPRIATENESS CATEGORY Based on Referral p < 0. 0001 13. 2% 16. 0% 20. 1% 10. 1% 70. 9% 69. 8% n = 4, 881 n = 1, 047
APPROPRIATENESS CATEGORY Based on Referral p < 0. 0001 13. 2% 16. 0% 20. 1% 10. 1% 70. 9% 69. 8% n = 4, 881 n = 1, 047
 FEEDBACK TO SITES
FEEDBACK TO SITES
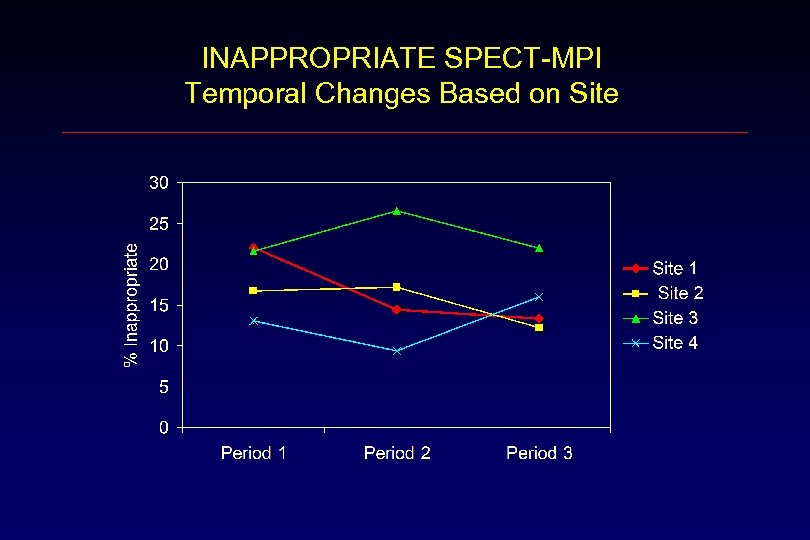 INAPPROPRIATE SPECT-MPI Temporal Changes Based on Site
INAPPROPRIATE SPECT-MPI Temporal Changes Based on Site
 CONCLUSIONS • Data collection and analysis regarding appropriate use of SPECT imaging is feasible in busy community practice environment –Easy to use, point-of-ordering tool with web-based data entry –Automated determination of appropriateness –On-demand, benchmarked reports • Variable rates of test appropriateness • Consistent inappropriate indications –Asymptomatic, low risk patient are most frequent • Feedback/education may influence on practice habits • Less inappropriate testing from cardiologists than non-cardiologists
CONCLUSIONS • Data collection and analysis regarding appropriate use of SPECT imaging is feasible in busy community practice environment –Easy to use, point-of-ordering tool with web-based data entry –Automated determination of appropriateness –On-demand, benchmarked reports • Variable rates of test appropriateness • Consistent inappropriate indications –Asymptomatic, low risk patient are most frequent • Feedback/education may influence on practice habits • Less inappropriate testing from cardiologists than non-cardiologists
 IMPLICATIONS • Physicians and other health care professionals, working with medical societies, recognize the current healthcare environment –Active measures to optimize performance and cost-effectiveness –Preserve patient access to evaluation and treatment • The development and implementation of appropriate use criteria may offer an alternative to prior authorization/pre-certification approaches –Transparency –Expanded information regarding practice habits –Facilitation of on-going quality improvement –Movement toward point-of-order application –Potential for wide-scale utilization • Establishment of partnership between ACC, subspeciality societies, and health plans regarding responsible approach to medical imaging and continued emphasis on improving the quality of care
IMPLICATIONS • Physicians and other health care professionals, working with medical societies, recognize the current healthcare environment –Active measures to optimize performance and cost-effectiveness –Preserve patient access to evaluation and treatment • The development and implementation of appropriate use criteria may offer an alternative to prior authorization/pre-certification approaches –Transparency –Expanded information regarding practice habits –Facilitation of on-going quality improvement –Movement toward point-of-order application –Potential for wide-scale utilization • Establishment of partnership between ACC, subspeciality societies, and health plans regarding responsible approach to medical imaging and continued emphasis on improving the quality of care
 ACKNOWLEDGMENTS • American Society of Nuclear Cardiology (ASNC) • United. Healthcare • Leadership of ACC –Especially Douglas Weaver, Ralph Brindis, Michael Wolk, Pamela Douglas, Jack Lewin, and Janet Wright • Staff from ACC, NCDR, and DCRI –Notably Joseph Allen, Karen Caruth, Wenqin Pan, and Nichole Kallas
ACKNOWLEDGMENTS • American Society of Nuclear Cardiology (ASNC) • United. Healthcare • Leadership of ACC –Especially Douglas Weaver, Ralph Brindis, Michael Wolk, Pamela Douglas, Jack Lewin, and Janet Wright • Staff from ACC, NCDR, and DCRI –Notably Joseph Allen, Karen Caruth, Wenqin Pan, and Nichole Kallas
 LIMITATIONS • Non-evaluable data –Missing information –Conflicting indications • Rolling recruitment with inconsistent time periods • Lack of validation of computer-assigned indications –Multiple indications –Audits reveal variance • Educational initiatives inconsistently applied • Non-adjudicated SPECT interpretations
LIMITATIONS • Non-evaluable data –Missing information –Conflicting indications • Rolling recruitment with inconsistent time periods • Lack of validation of computer-assigned indications –Multiple indications –Audits reveal variance • Educational initiatives inconsistently applied • Non-adjudicated SPECT interpretations
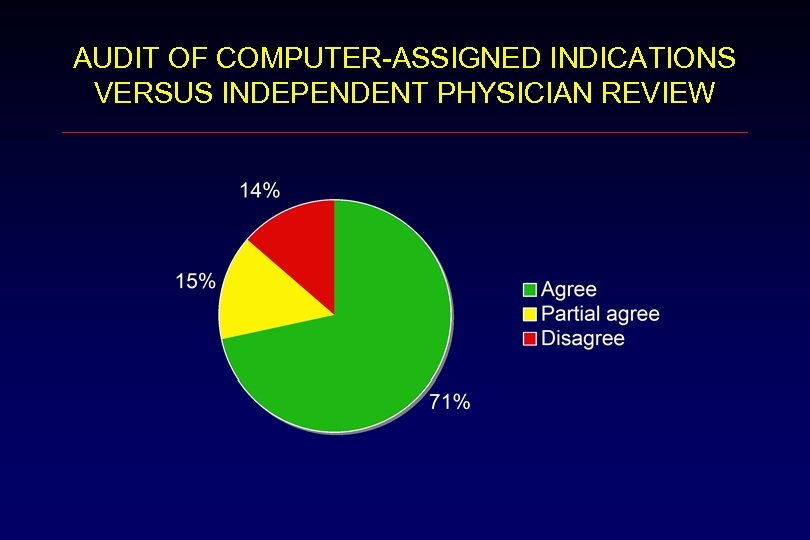 AUDIT OF COMPUTER-ASSIGNED INDICATIONS VERSUS INDEPENDENT PHYSICIAN REVIEW
AUDIT OF COMPUTER-ASSIGNED INDICATIONS VERSUS INDEPENDENT PHYSICIAN REVIEW
 SPECT RESULTS Based on Appropriateness Category APPROPRIATE UNCERTAIN INAPPROPRIATE p < 0. 0003
SPECT RESULTS Based on Appropriateness Category APPROPRIATE UNCERTAIN INAPPROPRIATE p < 0. 0003
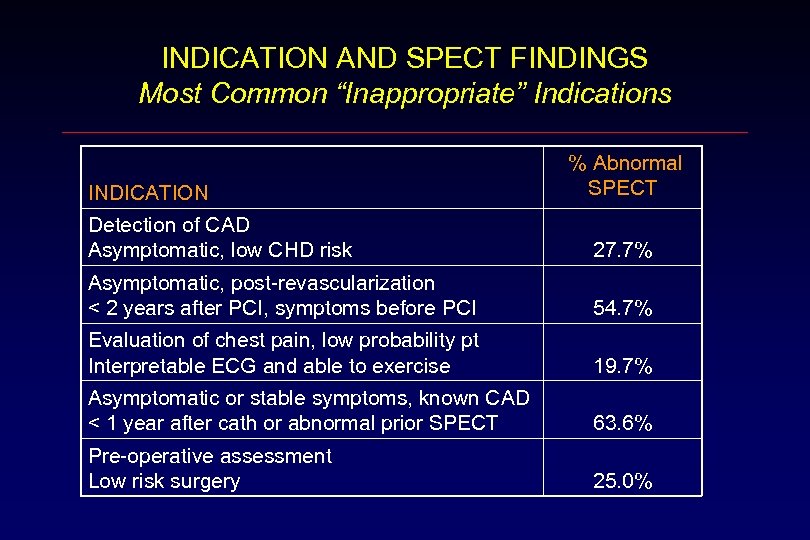 INDICATION AND SPECT FINDINGS Most Common “Inappropriate” Indications INDICATION % Abnormal SPECT Detection of CAD Asymptomatic, low CHD risk 27. 7% Asymptomatic, post-revascularization < 2 years after PCI, symptoms before PCI 54. 7% Evaluation of chest pain, low probability pt Interpretable ECG and able to exercise 19. 7% Asymptomatic or stable symptoms, known CAD < 1 year after cath or abnormal prior SPECT 63. 6% Pre-operative assessment Low risk surgery 25. 0%
INDICATION AND SPECT FINDINGS Most Common “Inappropriate” Indications INDICATION % Abnormal SPECT Detection of CAD Asymptomatic, low CHD risk 27. 7% Asymptomatic, post-revascularization < 2 years after PCI, symptoms before PCI 54. 7% Evaluation of chest pain, low probability pt Interpretable ECG and able to exercise 19. 7% Asymptomatic or stable symptoms, known CAD < 1 year after cath or abnormal prior SPECT 63. 6% Pre-operative assessment Low risk surgery 25. 0%
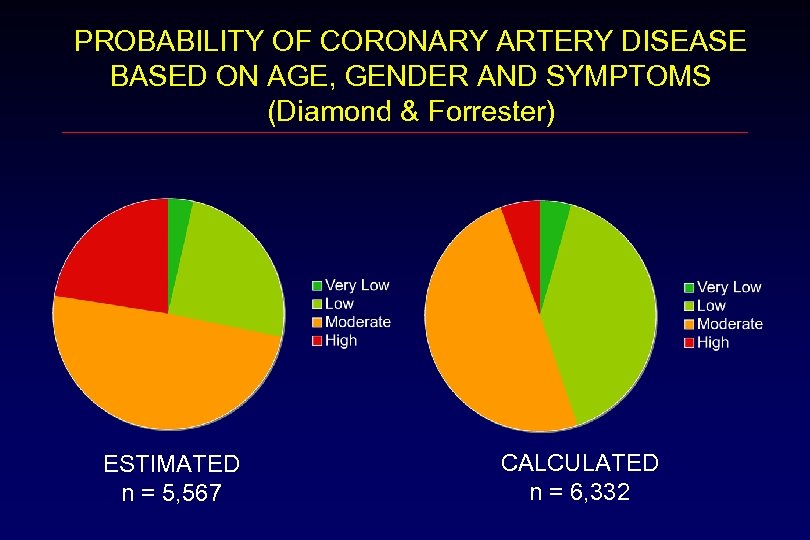 PROBABILITY OF CORONARY ARTERY DISEASE BASED ON AGE, GENDER AND SYMPTOMS (Diamond & Forrester) ESTIMATED n = 5, 567 CALCULATED n = 6, 332
PROBABILITY OF CORONARY ARTERY DISEASE BASED ON AGE, GENDER AND SYMPTOMS (Diamond & Forrester) ESTIMATED n = 5, 567 CALCULATED n = 6, 332
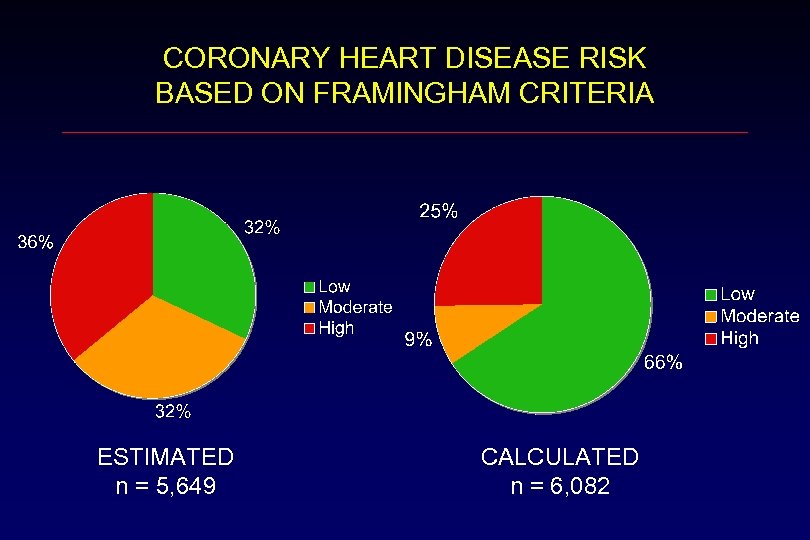 CORONARY HEART DISEASE RISK BASED ON FRAMINGHAM CRITERIA ESTIMATED n = 5, 649 CALCULATED n = 6, 082
CORONARY HEART DISEASE RISK BASED ON FRAMINGHAM CRITERIA ESTIMATED n = 5, 649 CALCULATED n = 6, 082
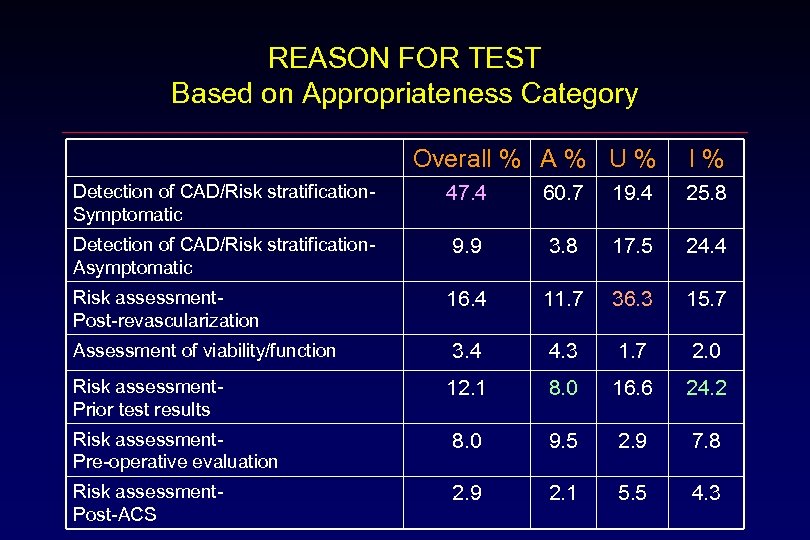 REASON FOR TEST Based on Appropriateness Category Overall % A % U % I% Detection of CAD/Risk stratification. Symptomatic 47. 4 60. 7 19. 4 25. 8 Detection of CAD/Risk stratification. Asymptomatic 9. 9 3. 8 17. 5 24. 4 16. 4 11. 7 36. 3 15. 7 3. 4 4. 3 1. 7 2. 0 12. 1 8. 0 16. 6 24. 2 Risk assessment. Pre-operative evaluation 8. 0 9. 5 2. 9 7. 8 Risk assessment. Post-ACS 2. 9 2. 1 5. 5 4. 3 Risk assessment. Post-revascularization Assessment of viability/function Risk assessment. Prior test results
REASON FOR TEST Based on Appropriateness Category Overall % A % U % I% Detection of CAD/Risk stratification. Symptomatic 47. 4 60. 7 19. 4 25. 8 Detection of CAD/Risk stratification. Asymptomatic 9. 9 3. 8 17. 5 24. 4 16. 4 11. 7 36. 3 15. 7 3. 4 4. 3 1. 7 2. 0 12. 1 8. 0 16. 6 24. 2 Risk assessment. Pre-operative evaluation 8. 0 9. 5 2. 9 7. 8 Risk assessment. Post-ACS 2. 9 2. 1 5. 5 4. 3 Risk assessment. Post-revascularization Assessment of viability/function Risk assessment. Prior test results
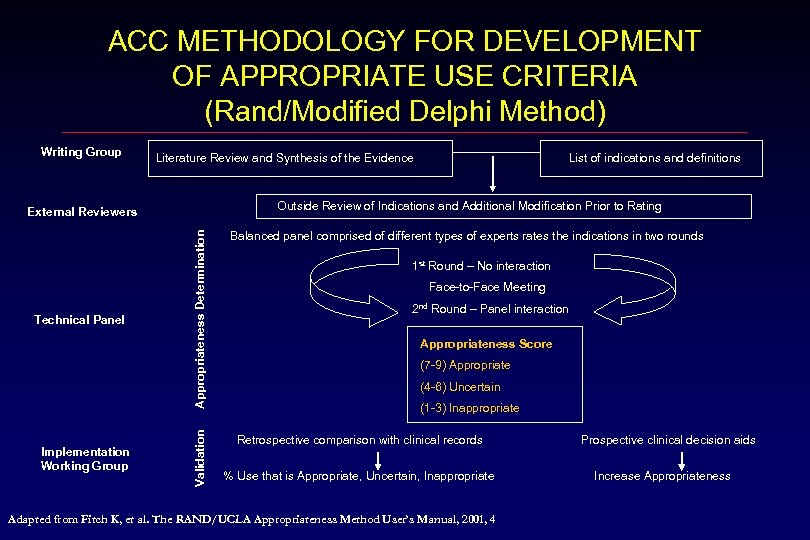 ACC METHODOLOGY FOR DEVELOPMENT OF APPROPRIATE USE CRITERIA (Rand/Modified Delphi Method) Writing Group Literature Review and Synthesis of the Evidence Outside Review of Indications and Additional Modification Prior to Rating Validation Implementation Working Group Appropriateness Determination External Reviewers Technical Panel List of indications and definitions Balanced panel comprised of different types of experts rates the indications in two rounds 1 st Round – No interaction Face-to-Face Meeting 2 nd Round – Panel interaction Appropriateness Score (7 -9) Appropriate (4 -6) Uncertain (1 -3) Inappropriate Retrospective comparison with clinical records % Use that is Appropriate, Uncertain, Inappropriate Adapted from Fitch K, et al. The RAND/UCLA Appropriateness Method User’s Manual, 2001, 4 Prospective clinical decision aids Increase Appropriateness
ACC METHODOLOGY FOR DEVELOPMENT OF APPROPRIATE USE CRITERIA (Rand/Modified Delphi Method) Writing Group Literature Review and Synthesis of the Evidence Outside Review of Indications and Additional Modification Prior to Rating Validation Implementation Working Group Appropriateness Determination External Reviewers Technical Panel List of indications and definitions Balanced panel comprised of different types of experts rates the indications in two rounds 1 st Round – No interaction Face-to-Face Meeting 2 nd Round – Panel interaction Appropriateness Score (7 -9) Appropriate (4 -6) Uncertain (1 -3) Inappropriate Retrospective comparison with clinical records % Use that is Appropriate, Uncertain, Inappropriate Adapted from Fitch K, et al. The RAND/UCLA Appropriateness Method User’s Manual, 2001, 4 Prospective clinical decision aids Increase Appropriateness


