8b8f601347ab4e34f6e5223b47542cc8.ppt
- Количество слайдов: 46
 Mount Sinai ICU
Mount Sinai ICU
 Mount Sinai ICU Ø 16 bed medical-surgical ICU Ø Closed administration • countersign orders from outside services • notify referring services about all significant changes in their patients’ condition and in the event of a death of their patient
Mount Sinai ICU Ø 16 bed medical-surgical ICU Ø Closed administration • countersign orders from outside services • notify referring services about all significant changes in their patients’ condition and in the event of a death of their patient
 Attending Staff: • Tom Stewart (Physician in Chief) • Niall Ferguson (Director, Critical Care) • Stephen Lapinsky (Site Director & Education) • Geeta Mehta (Research Director) • Mike Christian (I. D. /Military medicine) • Eddy Fan • Christie Lee • Michael Detsky
Attending Staff: • Tom Stewart (Physician in Chief) • Niall Ferguson (Director, Critical Care) • Stephen Lapinsky (Site Director & Education) • Geeta Mehta (Research Director) • Mike Christian (I. D. /Military medicine) • Eddy Fan • Christie Lee • Michael Detsky
 Sources of consults / admissions Ø MSH inpatients Ø ACCESS Ø OR/PACU Ø emergency department Ø PMH inpatients Ø Criticall
Sources of consults / admissions Ø MSH inpatients Ø ACCESS Ø OR/PACU Ø emergency department Ø PMH inpatients Ø Criticall
 Daily schedule Ø 7: 45 sign over Ø 8: 00 allocate patients Ø 8: 00 - 8: 30 discharges, see patients Ø 8: 30 – 9: 00 rounds Ø 12: 00 teaching (post call residents welcome!) Ø Afternoon : see patients, procedures Ø Bullet rounds Tuesday 1 pm: multidisciplinary
Daily schedule Ø 7: 45 sign over Ø 8: 00 allocate patients Ø 8: 00 - 8: 30 discharges, see patients Ø 8: 30 – 9: 00 rounds Ø 12: 00 teaching (post call residents welcome!) Ø Afternoon : see patients, procedures Ø Bullet rounds Tuesday 1 pm: multidisciplinary
 Admit decisions Ø Assess patient, decide on ICU admission Ø Discuss with fellow, attending, charge nurse Ø if no resources available, speak to your attending staff Ø Do not refuse admission without discussing with attending
Admit decisions Ø Assess patient, decide on ICU admission Ø Discuss with fellow, attending, charge nurse Ø if no resources available, speak to your attending staff Ø Do not refuse admission without discussing with attending
 Admit decisions Ø If the unit is full: • this is the attending and NUA’s responsibility • Obligation to open 2 additional beds Ø Options: • Transfer a stable patient to the floor/SDU • Open beds in PACU or CCU. • Criticall to another hospital Ø We do not take responsibility for patients outside the unit except: • Patients transferred from ICU to PACU • ICU patients bedspaced in CCU
Admit decisions Ø If the unit is full: • this is the attending and NUA’s responsibility • Obligation to open 2 additional beds Ø Options: • Transfer a stable patient to the floor/SDU • Open beds in PACU or CCU. • Criticall to another hospital Ø We do not take responsibility for patients outside the unit except: • Patients transferred from ICU to PACU • ICU patients bedspaced in CCU
 Admission orders - preprinted
Admission orders - preprinted
 Admission orders – Medication reconciliation
Admission orders – Medication reconciliation
 Electronic order entry Ø ICU limited involvement in POE Ø ICU will only do Transfer orders online: • Checkbox Transfer orderset • Medication & fluids order entry • Education & support Ø New admissions: post-op orders check electronic orders, eg.
Electronic order entry Ø ICU limited involvement in POE Ø ICU will only do Transfer orders online: • Checkbox Transfer orderset • Medication & fluids order entry • Education & support Ø New admissions: post-op orders check electronic orders, eg.
 Discharge decision Ø make this decision as early as possible, preferably the night before Ø communicate this to the nurse in charge Ø Communicate with receiving service on the day of discharge Ø Prior to discharge to Medicine: • Assessed by Medical floor nurse • Assessed by GIM housestaff
Discharge decision Ø make this decision as early as possible, preferably the night before Ø communicate this to the nurse in charge Ø Communicate with receiving service on the day of discharge Ø Prior to discharge to Medicine: • Assessed by Medical floor nurse • Assessed by GIM housestaff
 Discharges Ø Dictate or web form: - discharges home - deaths - transfers to another hospital (eg. PMH) Ø Deaths: - complete yellow M&M form - consider organ donation, autopsy
Discharges Ø Dictate or web form: - discharges home - deaths - transfers to another hospital (eg. PMH) Ø Deaths: - complete yellow M&M form - consider organ donation, autopsy
 Dictation: web form Ø Discharge summary accessible via Powerchart Ø Name, MSID, Family doctor, attending, admission and discharge dates all populated
Dictation: web form Ø Discharge summary accessible via Powerchart Ø Name, MSID, Family doctor, attending, admission and discharge dates all populated
 Discharges Ø Discharge medications: • Confirm complete: • ICU flow sheet • ICU Cardex • Pharmacist admission notes • Check with pharmacist/nurse if unsure Ø Do not erase patient from signout • Change room number to “ACCESS”
Discharges Ø Discharge medications: • Confirm complete: • ICU flow sheet • ICU Cardex • Pharmacist admission notes • Check with pharmacist/nurse if unsure Ø Do not erase patient from signout • Change room number to “ACCESS”
 Deaths and Impending deaths Ø New requirement to inform Trillium Gift of Life Ø Inform charge nurse for who will make contact Ø TGOL will communicate with family if necessary Ø For: • Deaths • Impending deaths • Withdrawal of life-support Ø Further education to follow
Deaths and Impending deaths Ø New requirement to inform Trillium Gift of Life Ø Inform charge nurse for who will make contact Ø TGOL will communicate with family if necessary Ø For: • Deaths • Impending deaths • Withdrawal of life-support Ø Further education to follow
 ICU Surge Plan Ø Provincial requirement to increase capacity by 15% before transferring out via Criticall: • • • = 2 additional beds Usually to be located in the CCU (16 N), or PACU Managed by ICU medical and nursing staff Need to be clear under whose care patients are Keep on signout: eg. number “ 18 Bedspace CCU 7” Ø Additional surge will take over remainder of CCU beds -> 8 beds in total
ICU Surge Plan Ø Provincial requirement to increase capacity by 15% before transferring out via Criticall: • • • = 2 additional beds Usually to be located in the CCU (16 N), or PACU Managed by ICU medical and nursing staff Need to be clear under whose care patients are Keep on signout: eg. number “ 18 Bedspace CCU 7” Ø Additional surge will take over remainder of CCU beds -> 8 beds in total
 ACCESS team Ø Mount Sinai’s Critical Care Response Team • 24/7 service: Nurse 24 hrs, fellow, attending
ACCESS team Ø Mount Sinai’s Critical Care Response Team • 24/7 service: Nurse 24 hrs, fellow, attending
 Education sessions Ø Day 1: “Intensive Care University” • Full day teaching, simulation Ø teaching daily at noon – see schedule Ø attending rounds or mortality rounds on Tuesday noon Ø multidisciplinary teaching (RT, pharmacy, nutrition, research) on Friday noon Ø Simulation & practical sessions Ø Post-call residents are welcome!
Education sessions Ø Day 1: “Intensive Care University” • Full day teaching, simulation Ø teaching daily at noon – see schedule Ø attending rounds or mortality rounds on Tuesday noon Ø multidisciplinary teaching (RT, pharmacy, nutrition, research) on Friday noon Ø Simulation & practical sessions Ø Post-call residents are welcome!
 Daily rounds Ø Resident summarizes problems Ø Nursing report: head-to-toe Ø RT: mechanical ventilation Ø Pharmacist: medications Ø Labs Ø Management plan Ø Checklists: CRBSI, VAP
Daily rounds Ø Resident summarizes problems Ø Nursing report: head-to-toe Ø RT: mechanical ventilation Ø Pharmacist: medications Ø Labs Ø Management plan Ø Checklists: CRBSI, VAP
 Daily notes Ø Daily note: • • “ICU Rounds”: Problem list New issues Plan Ø Orders • Check/confirm at the end • Quality improvement checklists
Daily notes Ø Daily note: • • “ICU Rounds”: Problem list New issues Plan Ø Orders • Check/confirm at the end • Quality improvement checklists
 Quality Improvement data collection Ø Central line infections • Procedure checklist/note in central line insertion package • Daily data collection for CLI Ø Ventilator associated pneumonia • Checklist in nurses binder, reviewed by RT on rounds • Ventilated > CXR changes > check chart (WBC, sputum, etc) Ø Data is publicly reported
Quality Improvement data collection Ø Central line infections • Procedure checklist/note in central line insertion package • Daily data collection for CLI Ø Ventilator associated pneumonia • Checklist in nurses binder, reviewed by RT on rounds • Ventilated > CXR changes > check chart (WBC, sputum, etc) Ø Data is publicly reported
 Procedures – Procedure Note Ø Central line insertion kit contains drapes, cleaning material, gowns and Procedure Note/Checklist Ø To be completed by nurse and physician Ø White copy into chart (Progress notes section) Ø Yellow copy into tray at Ward Clerks desk Ø Acts as checklist, note and for QI data collection Ø Trial note: feedback is appreciated
Procedures – Procedure Note Ø Central line insertion kit contains drapes, cleaning material, gowns and Procedure Note/Checklist Ø To be completed by nurse and physician Ø White copy into chart (Progress notes section) Ø Yellow copy into tray at Ward Clerks desk Ø Acts as checklist, note and for QI data collection Ø Trial note: feedback is appreciated
 Procedures Ø central venous and arterial lines Ø Ultrasound: lines, chest, echo Ø PA catheters Ø intubation Ø Bronchoscopy Ø Intraosseus line insertion Ø Cardioversion Ø Chest tube insertion
Procedures Ø central venous and arterial lines Ø Ultrasound: lines, chest, echo Ø PA catheters Ø intubation Ø Bronchoscopy Ø Intraosseus line insertion Ø Cardioversion Ø Chest tube insertion
 Procedures Ø Simulation teaching Ø Supervision: by fellow or attending Ø Procedure notes: preprinted form Ø Procedure logging: POWER
Procedures Ø Simulation teaching Ø Supervision: by fellow or attending Ø Procedure notes: preprinted form Ø Procedure logging: POWER
 Procedures Ø Backup for procedures: Fellow and Attending Ø Don’t call anesthesia for routine intubations • They are very busy and it is not their responsibility • RT’s can intubate or support you • Anesthesia will be a backup if you have a problem • Make sure fellow/staff are involved
Procedures Ø Backup for procedures: Fellow and Attending Ø Don’t call anesthesia for routine intubations • They are very busy and it is not their responsibility • RT’s can intubate or support you • Anesthesia will be a backup if you have a problem • Make sure fellow/staff are involved
 Procedures Ø Wastage of supplies: • Most supplies taken into a room cannot be reused, even if not opened • Only take into room what you are about to use • This is a Patient safety and Economic issue!
Procedures Ø Wastage of supplies: • Most supplies taken into a room cannot be reused, even if not opened • Only take into room what you are about to use • This is a Patient safety and Economic issue!
 CCM Resident/Fellow Ø first line of consultation for the resident Ø when in doubt, consult with the attending Ø back up call 1: 3, may need to do 1 – 3 in-house calls Ø Teaching: fellow teaching, track formal rounds Ø Quality improvement: checklist, Safer. Healthcare. Now Ø M & M rounds
CCM Resident/Fellow Ø first line of consultation for the resident Ø when in doubt, consult with the attending Ø back up call 1: 3, may need to do 1 – 3 in-house calls Ø Teaching: fellow teaching, track formal rounds Ø Quality improvement: checklist, Safer. Healthcare. Now Ø M & M rounds
 M & M rounds last Tuesday of the month review monthly stats: Patrick Cheng present all deaths briefly categorise all deaths 1 – 5 for categories 4 and 5, detailed review, may go on to Quality of Care Committee Ø present autopsies if available Ø Ø Ø
M & M rounds last Tuesday of the month review monthly stats: Patrick Cheng present all deaths briefly categorise all deaths 1 – 5 for categories 4 and 5, detailed review, may go on to Quality of Care Committee Ø present autopsies if available Ø Ø Ø
 CCM Resident/Fellow Ø Fellow 1: • Runs rounds, Co-ordinates team Ø Fellow 2: • Support: transfers, discharges, procedures, resuscitation, nursing issues during rounds • Quality improvement • ACCESS (if no fellow 3) Ø Fellow 3: • ACCESS team • Quality improvement Ø (Fellow 4: Research, reading, QI)
CCM Resident/Fellow Ø Fellow 1: • Runs rounds, Co-ordinates team Ø Fellow 2: • Support: transfers, discharges, procedures, resuscitation, nursing issues during rounds • Quality improvement • ACCESS (if no fellow 3) Ø Fellow 3: • ACCESS team • Quality improvement Ø (Fellow 4: Research, reading, QI)
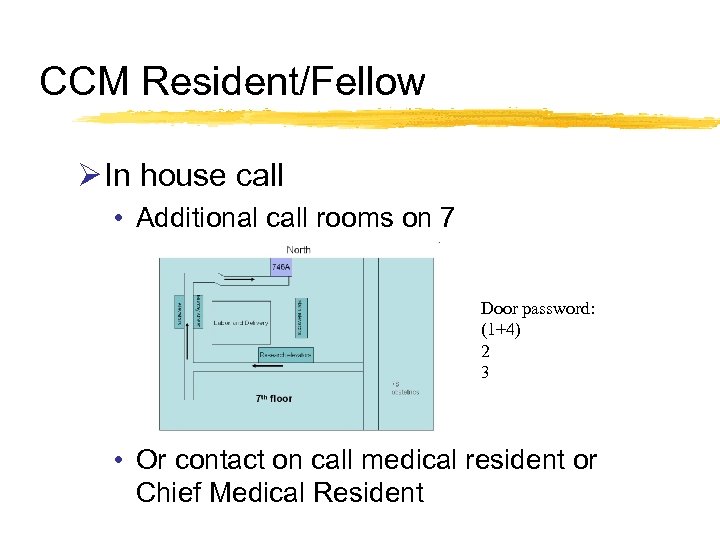 CCM Resident/Fellow Ø In house call • Additional call rooms on 7 Door password: (1+4) 2 3 • Or contact on call medical resident or Chief Medical Resident
CCM Resident/Fellow Ø In house call • Additional call rooms on 7 Door password: (1+4) 2 3 • Or contact on call medical resident or Chief Medical Resident
 CCM Resident/Fellow Ø Teaching: • Monday noon: responsible for resident teaching • Thursday am: present fellow-specific teaching • Evaluation on family meetings: twice per month
CCM Resident/Fellow Ø Teaching: • Monday noon: responsible for resident teaching • Thursday am: present fellow-specific teaching • Evaluation on family meetings: twice per month
 Resident Responsibilities Ø in-house call about 1: 4 Ø look after all patient care after hours, including consults • do not leave the unit unattended if there is an unstable situation ongoing inside the unit Ø hand-over at 7: 45 Monday – Friday Ø Weekends usually 8: 30 am
Resident Responsibilities Ø in-house call about 1: 4 Ø look after all patient care after hours, including consults • do not leave the unit unattended if there is an unstable situation ongoing inside the unit Ø hand-over at 7: 45 Monday – Friday Ø Weekends usually 8: 30 am
 Resident Responsibilities Ø Examine assigned patients, manage issues through the day Ø when in doubt, ask, listen to the nurse! Ø Code team leader: weekdays 8 – 5 only Ø Post-call morning: • order CXR for each patient where indicated • Order ECG for patients where indicated Ø write transfer orders and a transfer note for each patient being considered for transfer
Resident Responsibilities Ø Examine assigned patients, manage issues through the day Ø when in doubt, ask, listen to the nurse! Ø Code team leader: weekdays 8 – 5 only Ø Post-call morning: • order CXR for each patient where indicated • Order ECG for patients where indicated Ø write transfer orders and a transfer note for each patient being considered for transfer
 Infection Control Ø Consider MRSA & VRE precautions: • Hospital transfers • U. S. hospitals Ø Influenza precautions (in season) for: • Febrile respiratory illness requiring ICU • Fever & ARDS NYD • Droplet precautions + N 95, no negative pressure Ø Infection Control will assess and advise
Infection Control Ø Consider MRSA & VRE precautions: • Hospital transfers • U. S. hospitals Ø Influenza precautions (in season) for: • Febrile respiratory illness requiring ICU • Fever & ARDS NYD • Droplet precautions + N 95, no negative pressure Ø Infection Control will assess and advise
 Infection Control Ø Pseudomonas and Klebsiella oxytoca • Recent increase in incidence • Transmission from patients and basins • Multidrug resistance Ø Hand hygiene! Ø Hand audits being done intermittently Ø Daily allocation of “Hand hygiene monitor”
Infection Control Ø Pseudomonas and Klebsiella oxytoca • Recent increase in incidence • Transmission from patients and basins • Multidrug resistance Ø Hand hygiene! Ø Hand audits being done intermittently Ø Daily allocation of “Hand hygiene monitor”
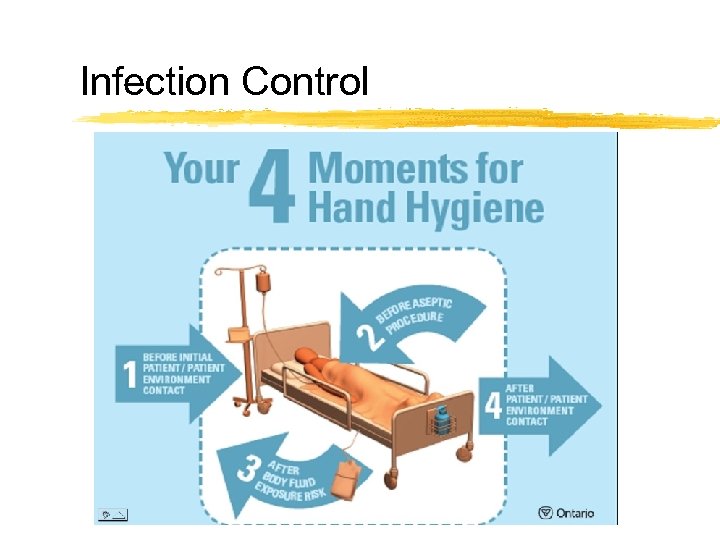 Infection Control
Infection Control
 Hand Hygiene
Hand Hygiene
 Antibiotic Stewardship Program Ø Dr. Andrew Morris - ID Physician Ø Dr. Sandra Nelson - ID Pharmacist Ø Optimize antibiotic utilization Ø Meet Mon, Wed, Fri after rounds: 10 min Ø Recommendations: • Improve patient care • Education • Cost savings
Antibiotic Stewardship Program Ø Dr. Andrew Morris - ID Physician Ø Dr. Sandra Nelson - ID Pharmacist Ø Optimize antibiotic utilization Ø Meet Mon, Wed, Fri after rounds: 10 min Ø Recommendations: • Improve patient care • Education • Cost savings
 Family contacts Ø daily contact is the standard Ø Initial meeting within 48 hr of admission (standardized format) Ø ensure that consistent communication, especially with regards to outside services Ø end of life discussions should always occur with the awareness/participation of referring services Ø Involve our social worker
Family contacts Ø daily contact is the standard Ø Initial meeting within 48 hr of admission (standardized format) Ø ensure that consistent communication, especially with regards to outside services Ø end of life discussions should always occur with the awareness/participation of referring services Ø Involve our social worker
 Research Opportunities Ø interested residents should speak to individual staff and/or Geeta Mehta Ø Many ongoing studies in the ICU Ø Unit research coordinators may approach you about studies
Research Opportunities Ø interested residents should speak to individual staff and/or Geeta Mehta Ø Many ongoing studies in the ICU Ø Unit research coordinators may approach you about studies
 Role of the Bedside Nurse Ø system review on a daily basis Ø co-ordinate communications Ø co-ordinates family meetings Ø reports to nurse in charge/nurse manager
Role of the Bedside Nurse Ø system review on a daily basis Ø co-ordinate communications Ø co-ordinates family meetings Ø reports to nurse in charge/nurse manager
 Role of the RT Ø airway management issues Ø mechanical ventilation issues Ø Bronchoscopy Ø Art line/ PA line setup Ø RT’s do one-on-one teaching on above:
Role of the RT Ø airway management issues Ø mechanical ventilation issues Ø Bronchoscopy Ø Art line/ PA line setup Ø RT’s do one-on-one teaching on above:
 Role of the Pharmacist Ø ensures routine prevention strategies for DVT, PUD Ø aware of important microbiologic data on each patient Ø Dose adjustment, eg. Renal failure Ø resource person for any other pharmacy related issue
Role of the Pharmacist Ø ensures routine prevention strategies for DVT, PUD Ø aware of important microbiologic data on each patient Ø Dose adjustment, eg. Renal failure Ø resource person for any other pharmacy related issue
 Role of the Dietician Ø recommends tube feeding and TPN formulas Ø advises management for tube feeding complications (e. g. diarrhea, high gastric residuals) Ø ensures appropriate diet and supplement orders Ø adjusts nutrition care based on swallowing assessments (e. g. appropriate p. o. initiation, modified diet education, calorie counts etc. )
Role of the Dietician Ø recommends tube feeding and TPN formulas Ø advises management for tube feeding complications (e. g. diarrhea, high gastric residuals) Ø ensures appropriate diet and supplement orders Ø adjusts nutrition care based on swallowing assessments (e. g. appropriate p. o. initiation, modified diet education, calorie counts etc. )
 Role of Chaplaincy Ø provides emotional and spiritual support to patient and family during ICU stay Ø available to attend family meetings, treatment decisions Ø provides/facilitates religious care Ø end of life care and bereavement support Ø available for staff support and debriefing (confidentiality observed) Ø past or current religious affiliation not required for chaplaincy support
Role of Chaplaincy Ø provides emotional and spiritual support to patient and family during ICU stay Ø available to attend family meetings, treatment decisions Ø provides/facilitates religious care Ø end of life care and bereavement support Ø available for staff support and debriefing (confidentiality observed) Ø past or current religious affiliation not required for chaplaincy support
 For further information Ø See intranet site: http: //info/intensivecare Ø Accessible from MSH, TGH, TWH, PMH
For further information Ø See intranet site: http: //info/intensivecare Ø Accessible from MSH, TGH, TWH, PMH


