5cc22053d7862fdbca366d60fafa41d6.ppt
- Количество слайдов: 19
 Morning Report Anne Lachiewicz January 25, 2010
Morning Report Anne Lachiewicz January 25, 2010
 Mycobacteria Except for MTB & M. leprae, generally free-living orgs ubiquitous in the environment n Recovered from water, soil, domestic/wild animals, milk, and food n >100 species in the genus n Species vary by geography n
Mycobacteria Except for MTB & M. leprae, generally free-living orgs ubiquitous in the environment n Recovered from water, soil, domestic/wild animals, milk, and food n >100 species in the genus n Species vary by geography n
 Mycobacteria Acid fast bacillus = mycobacterium (ex for Nocardia, weakly or variably AF) n Refractile GP or gram neutral rods “gram variable rods” n Slightly bent, often beaded rods 2 -4 microns long under 100 x n Over the past 15 years, labs are isolating less MTB & more NTM n
Mycobacteria Acid fast bacillus = mycobacterium (ex for Nocardia, weakly or variably AF) n Refractile GP or gram neutral rods “gram variable rods” n Slightly bent, often beaded rods 2 -4 microns long under 100 x n Over the past 15 years, labs are isolating less MTB & more NTM n
 Mycobacteria n n Isolate rates n NTM isolates are more common than MTB isolates n Report rates of isolates are not verified with clinical significant of the report Disease rates n NTM dz is not communicable thus not reportable n In industrialized countries: 11. 8/100, 000 of NTM disease vs. 3. 5/100, 000 of active MTB
Mycobacteria n n Isolate rates n NTM isolates are more common than MTB isolates n Report rates of isolates are not verified with clinical significant of the report Disease rates n NTM dz is not communicable thus not reportable n In industrialized countries: 11. 8/100, 000 of NTM disease vs. 3. 5/100, 000 of active MTB
 Mycobacteria n n 4 groups of human pathogens n MTB complex n M. leprae n Slow growing NTM n Rapidly growing NTM IFN-g & IL-12 control mycobacteria via up-regulation of TNF-a from monocytes/macrophages
Mycobacteria n n 4 groups of human pathogens n MTB complex n M. leprae n Slow growing NTM n Rapidly growing NTM IFN-g & IL-12 control mycobacteria via up-regulation of TNF-a from monocytes/macrophages
 The most common disease causing NTM in the US are MAC & M. kansasii.
The most common disease causing NTM in the US are MAC & M. kansasii.
 NTM – 4 clinical syndromes n n Pulmonary disease (75 -94%) n Older persons +/- underlying lung dz n CF patients n MAC, M. kansasii Disseminated disease (5%) n Severely immunocompromised n MAC, RGM spp. (M. abscesses, M. fortuitum, M. chelonae) Skin & soft tissue infection (2 -3%) n Direct inoculation n M. marinum, M. ulcerans n RGM spp. (may be nosocomial, surgical site infections) Superficial lymphadenitis, esp. cervical (0. 4 -3%) n Children n MAC, M. scrofulaceum
NTM – 4 clinical syndromes n n Pulmonary disease (75 -94%) n Older persons +/- underlying lung dz n CF patients n MAC, M. kansasii Disseminated disease (5%) n Severely immunocompromised n MAC, RGM spp. (M. abscesses, M. fortuitum, M. chelonae) Skin & soft tissue infection (2 -3%) n Direct inoculation n M. marinum, M. ulcerans n RGM spp. (may be nosocomial, surgical site infections) Superficial lymphadenitis, esp. cervical (0. 4 -3%) n Children n MAC, M. scrofulaceum
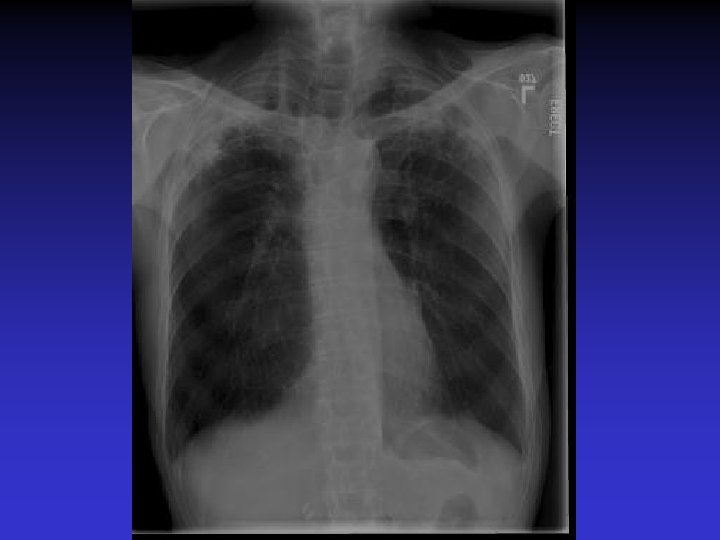
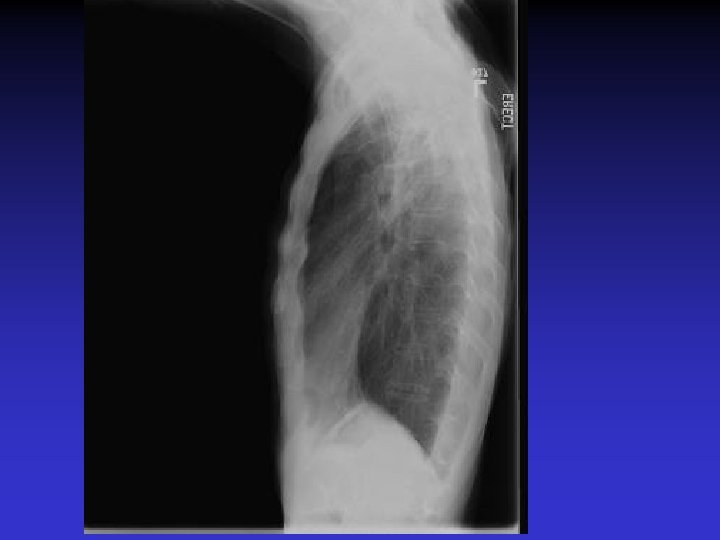
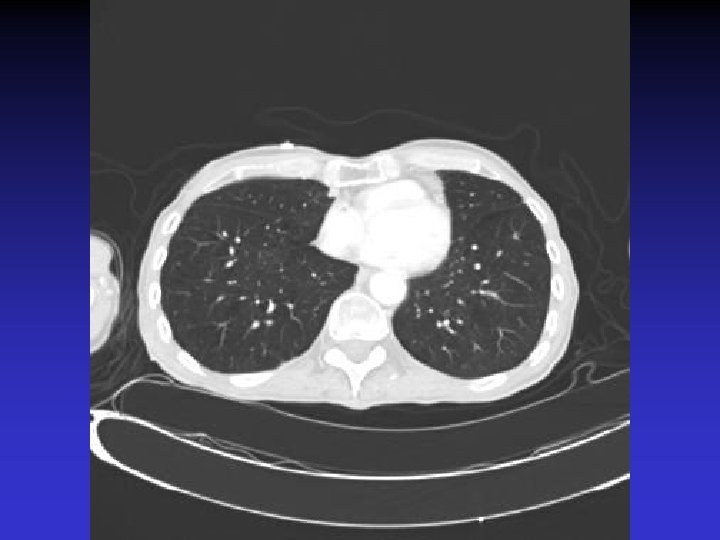
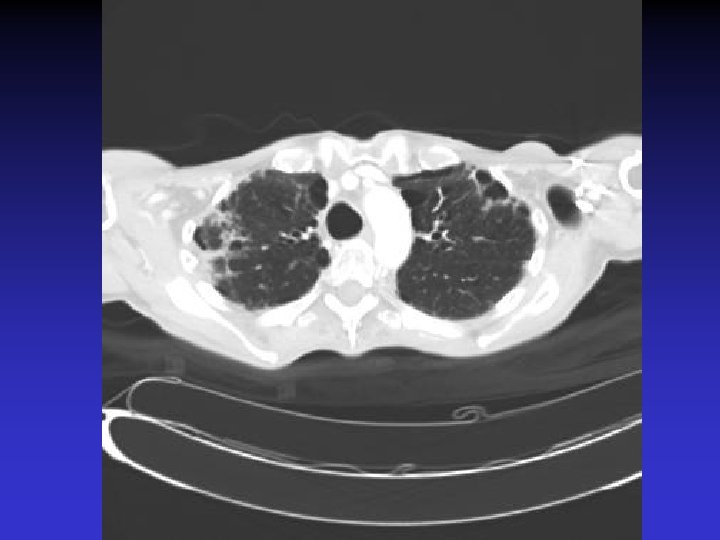
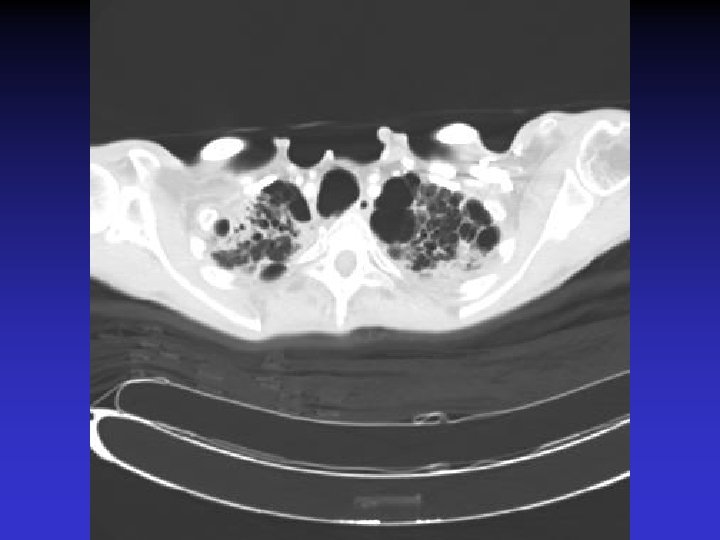
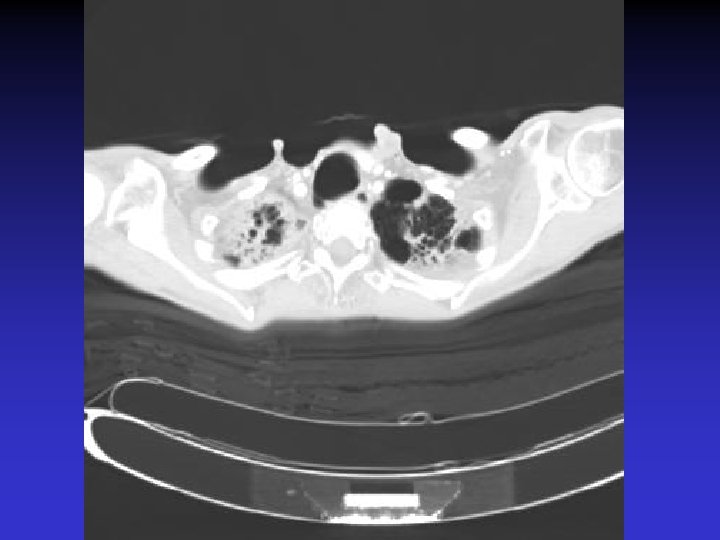
 NTM lung disease n n MAC, M. kansasii, M. abscessus >50 years, ? M vs. F Symptoms n variable, nonspecific n chronic or reoccurring cough n sputum production, fatigue, malaise, dyspnea, fever, hemoptysis, chest pain, wt loss n more constitutional symptoms with advancing disease n evaluation complicated by sx of coexisting lung disease CXR n Fibrocavitary – often like MTB, but may be dense airspace dz or solitary cavity w/o cavitation n Nodular/bronchietatic – typical MAC, usu. mid-lower lung fields, +/- cavitation
NTM lung disease n n MAC, M. kansasii, M. abscessus >50 years, ? M vs. F Symptoms n variable, nonspecific n chronic or reoccurring cough n sputum production, fatigue, malaise, dyspnea, fever, hemoptysis, chest pain, wt loss n more constitutional symptoms with advancing disease n evaluation complicated by sx of coexisting lung disease CXR n Fibrocavitary – often like MTB, but may be dense airspace dz or solitary cavity w/o cavitation n Nodular/bronchietatic – typical MAC, usu. mid-lower lung fields, +/- cavitation

 Treatment of NTM lung dz n n Indications for treatment 1. Compatible respiratory or constitutional sx w/ XR abnormalities n Plus EITHER n Consistent isolation of NTM in modhigh numbers from more than one specimen of pulmonary secretions n lsolation from >1 specimen if there is histological evidence of pulm parenchymal involvement Susceptibility testing & treament recs vary by species
Treatment of NTM lung dz n n Indications for treatment 1. Compatible respiratory or constitutional sx w/ XR abnormalities n Plus EITHER n Consistent isolation of NTM in modhigh numbers from more than one specimen of pulmonary secretions n lsolation from >1 specimen if there is histological evidence of pulm parenchymal involvement Susceptibility testing & treament recs vary by species
 M. simiae n n n n Clustered in Israel, Cuba, SW US Found in local tap water. Recent pseudo-outbreak in an urban Texas hospital from a contaminated water supply Usually a contaminant. Causes clinical disease in 9 -21% of pts. Immunocompromised pts: AIDS, underlying lung disease Usually pulmonary dz, rare intraabdominal infections, and disseminated dz in AIDS Difficult to treat: No predictably effective drug combos & in vivo response may not correlate with in vitro response ? ATS recs clarithromycin and a fluoroquinolone (moxifloxaxin preferred). Linezolid, SMX may work
M. simiae n n n n Clustered in Israel, Cuba, SW US Found in local tap water. Recent pseudo-outbreak in an urban Texas hospital from a contaminated water supply Usually a contaminant. Causes clinical disease in 9 -21% of pts. Immunocompromised pts: AIDS, underlying lung disease Usually pulmonary dz, rare intraabdominal infections, and disseminated dz in AIDS Difficult to treat: No predictably effective drug combos & in vivo response may not correlate with in vitro response ? ATS recs clarithromycin and a fluoroquinolone (moxifloxaxin preferred). Linezolid, SMX may work
 M. simiae n n M. simiae may be confused with MTB as it is the only niacin-positive NTM Maoz et al. compared pts in Israel with M. simiae vs MTB. Pts with M. simiae: n More females, older age n Higher rates of smoking, COPD, other dz (DM, CAD, cancer), immunosuppressive drugs n Less HIV n Blunted symptoms n More noncavitary infiltrates in middle/lower lobes Most M. simiae isolates were contaminants Treatment with clarithromycin, ethambutol, rifabutin, and streptomycin (with modification for sensitivities)
M. simiae n n M. simiae may be confused with MTB as it is the only niacin-positive NTM Maoz et al. compared pts in Israel with M. simiae vs MTB. Pts with M. simiae: n More females, older age n Higher rates of smoking, COPD, other dz (DM, CAD, cancer), immunosuppressive drugs n Less HIV n Blunted symptoms n More noncavitary infiltrates in middle/lower lobes Most M. simiae isolates were contaminants Treatment with clarithromycin, ethambutol, rifabutin, and streptomycin (with modification for sensitivities)
 References n n n Griffith, DE et al. An offical ATS/IDSA statement: Diagnosis, treatment, and prevention of nontuberculous mycobacterial diseases. Am J Respir Crit Care Med. 2007; 175: 367 -416. Griffith, DE and Wallace, RJ. Microbiology of nontuberculous mycobacteria. In: Up. To. Date, Basow, DS (Ed), Up. To. Date, Waltham, MA, 2009. Griffith, DE and Wallace, RJ. Overview of nontuberculous mycobacterial infections in HIV-negative patients. In: Up. To. Date, Basow, DS (Ed), Up. To. Date, Waltham, MA, 2009. Griffith, DE and Wallace, RJ. Treatment of nontuberculous mycobacterial infections of the lung in HIV-negative patients. In: Up. To. Date, Basow, DS (Ed), Up. To. Date, Waltham, MA, 2009. Maoz, C et al. Pulmonary Mycobacterium simiae infection: comparison with pulmonary tuberculosis. Eur J Clin Infect Dis. 2008; 27, 945 -950. Samra, Z et al. Emergence of Mycobacterium simiae in respiratory specimens. Scan Infect Dis. 2005; 37: 838 -841.
References n n n Griffith, DE et al. An offical ATS/IDSA statement: Diagnosis, treatment, and prevention of nontuberculous mycobacterial diseases. Am J Respir Crit Care Med. 2007; 175: 367 -416. Griffith, DE and Wallace, RJ. Microbiology of nontuberculous mycobacteria. In: Up. To. Date, Basow, DS (Ed), Up. To. Date, Waltham, MA, 2009. Griffith, DE and Wallace, RJ. Overview of nontuberculous mycobacterial infections in HIV-negative patients. In: Up. To. Date, Basow, DS (Ed), Up. To. Date, Waltham, MA, 2009. Griffith, DE and Wallace, RJ. Treatment of nontuberculous mycobacterial infections of the lung in HIV-negative patients. In: Up. To. Date, Basow, DS (Ed), Up. To. Date, Waltham, MA, 2009. Maoz, C et al. Pulmonary Mycobacterium simiae infection: comparison with pulmonary tuberculosis. Eur J Clin Infect Dis. 2008; 27, 945 -950. Samra, Z et al. Emergence of Mycobacterium simiae in respiratory specimens. Scan Infect Dis. 2005; 37: 838 -841.


