d1c8425a4bc6b54c00ecf06a95bada8a.ppt
- Количество слайдов: 101
 Mitchell Wilson, MD Associate Professor of Medicine Physician Advisor, University of North Carolina Hospitals Medical Director, Department of Clinical Care Management Section Chief of Hospital Medicine Medical Director, First. Health of the Carolinas Hospitalist Services Member, Society of Hospital Medicine Board of Directors
Mitchell Wilson, MD Associate Professor of Medicine Physician Advisor, University of North Carolina Hospitals Medical Director, Department of Clinical Care Management Section Chief of Hospital Medicine Medical Director, First. Health of the Carolinas Hospitalist Services Member, Society of Hospital Medicine Board of Directors
 Integrating Non-Physician Providers into Hospital Medicine Services Mitchell J. Wilson, M. D. Member, SHM Board of Directors
Integrating Non-Physician Providers into Hospital Medicine Services Mitchell J. Wilson, M. D. Member, SHM Board of Directors
 Learning Objectives Ø To understand how Non-Physician Providers can add value to hospitalist programs Ø To describe how integrating Non. Physician Providers can impact the delivery of care
Learning Objectives Ø To understand how Non-Physician Providers can add value to hospitalist programs Ø To describe how integrating Non. Physician Providers can impact the delivery of care
 Learning Objectives Ø To explore how a collaborative team approach influences program development Ø Examine the potential advantages and disadvantages of integrating Non. Physician Providers into hospitalist programs
Learning Objectives Ø To explore how a collaborative team approach influences program development Ø Examine the potential advantages and disadvantages of integrating Non. Physician Providers into hospitalist programs
 Learning Objectives Ø To examine (by audience selection) some key components of NPPs in hospitalist practices: • • • Academics: NPPs as substitute house staff Advantages and disadvantages Billing for services Credentialing, privileges and duties Demographics Education and training
Learning Objectives Ø To examine (by audience selection) some key components of NPPs in hospitalist practices: • • • Academics: NPPs as substitute house staff Advantages and disadvantages Billing for services Credentialing, privileges and duties Demographics Education and training
 Learning Objectives ØParticipate in an interactive discussion to share and learn from other’s experiences And PLEASE Interject questions and redirect content to suit your individual needs
Learning Objectives ØParticipate in an interactive discussion to share and learn from other’s experiences And PLEASE Interject questions and redirect content to suit your individual needs
 What’s an “APRN” Ø Umbrella title for RNs who are: • • CRNA CNM CNS NPs Ø Requires completion of an advanced formal education AND certification
What’s an “APRN” Ø Umbrella title for RNs who are: • • CRNA CNM CNS NPs Ø Requires completion of an advanced formal education AND certification
 Why Integrate Physician Assistants, Nurse Practitioners, Clinical Care Coordinators, and Clinical Pharmacists into Hospitalist Practices?
Why Integrate Physician Assistants, Nurse Practitioners, Clinical Care Coordinators, and Clinical Pharmacists into Hospitalist Practices?
 The Greatest Force… Value
The Greatest Force… Value
 Physician Assistants and Nurse Practitioners What’s the Evidence for Their Value
Physician Assistants and Nurse Practitioners What’s the Evidence for Their Value
 PAs and NPs What’s the Evidence for Their Value? Some Elements of Value: Structure: Denotes the attributes of the setting “How is care organized” Process: Denotes action in giving & receiving care “What is done” Outcome: Denotes the effects of care on health “What Happened”
PAs and NPs What’s the Evidence for Their Value? Some Elements of Value: Structure: Denotes the attributes of the setting “How is care organized” Process: Denotes action in giving & receiving care “What is done” Outcome: Denotes the effects of care on health “What Happened”
 Hospitalists Non-hospitalists Slower traffic Keep right
Hospitalists Non-hospitalists Slower traffic Keep right
 The Health Care Value Cascade Value = Quality / Cost Health Care = Clinical quality x Satisfaction Quality Clinical Quality = structure, process, outcomes structure Wachter, "Hospital Medicine" p. 33, Donabedian , "JAMA" 1988
The Health Care Value Cascade Value = Quality / Cost Health Care = Clinical quality x Satisfaction Quality Clinical Quality = structure, process, outcomes structure Wachter, "Hospital Medicine" p. 33, Donabedian , "JAMA" 1988
 PAs and NPs What’s the Evidence for Their Value? Value: Structure Processes Value = Outcomes x Satisfaction Cost Wachter, Donabedian
PAs and NPs What’s the Evidence for Their Value? Value: Structure Processes Value = Outcomes x Satisfaction Cost Wachter, Donabedian
 PAs and NPs What’s the Evidence for Their Value? Value: Evidence: Studies, Experience Structure Processes Outcomes Value = Clin. Qual x Satisfaction Cost
PAs and NPs What’s the Evidence for Their Value? Value: Evidence: Studies, Experience Structure Processes Outcomes Value = Clin. Qual x Satisfaction Cost
 PAs and NPs What’s the Evidence for Their Value? Value: Evidence: Studies, Experience Patient/Family Provider: Inpatient Attending, PCP Staff Administration Value = Clin. Qual x Satisfaction Cost Provider mix: MD & NPP Effect on ALOS, resource utilization, readmissions, COC, M & M Enhanced productivity or market share (pt census)
PAs and NPs What’s the Evidence for Their Value? Value: Evidence: Studies, Experience Patient/Family Provider: Inpatient Attending, PCP Staff Administration Value = Clin. Qual x Satisfaction Cost Provider mix: MD & NPP Effect on ALOS, resource utilization, readmissions, COC, M & M Enhanced productivity or market share (pt census)
 The Mantra of Hospitalists The purpose of admitting patients to the hospital is to discharge them Discharge planning begins at the moment of admission The average length of stay for most patients should not exceed three (3) days.
The Mantra of Hospitalists The purpose of admitting patients to the hospital is to discharge them Discharge planning begins at the moment of admission The average length of stay for most patients should not exceed three (3) days.
 Fo llo vis w u its p A dm iss io ns Procedures The conundrum of competing Family conferences congruent contemporaneous O care processes ve ICU rn ig ht ha n do ff s Administrative duties es g ar h Consults D sc i
Fo llo vis w u its p A dm iss io ns Procedures The conundrum of competing Family conferences congruent contemporaneous O care processes ve ICU rn ig ht ha n do ff s Administrative duties es g ar h Consults D sc i
 The Competition for provider time… delays the continuum of care that culminates in the patient’s (un)timely discharge
The Competition for provider time… delays the continuum of care that culminates in the patient’s (un)timely discharge
 Competition for Provider Time: The Ivory Tower Solution Academia &Residents !Interns Students
Competition for Provider Time: The Ivory Tower Solution Academia &Residents !Interns Students
 Competition for Provider Time: A non-housestaff Solution Integrating PAs, NPs and RN CCCs in Acute Care The integrated model of medical practice, in which the patient care team is led by the medical manager (MD or DO), assisted by the patient care manager (PA or NP), and clinically coordinated by the CCC (RN) is one solution to the competition for care processes in the management of inpatients.
Competition for Provider Time: A non-housestaff Solution Integrating PAs, NPs and RN CCCs in Acute Care The integrated model of medical practice, in which the patient care team is led by the medical manager (MD or DO), assisted by the patient care manager (PA or NP), and clinically coordinated by the CCC (RN) is one solution to the competition for care processes in the management of inpatients.
 Competition for Provider Time: A non-housestaff Solution Integrating PAs, NPs and RN CCCs in Acute Care Physician (medical manager) makes key medical decisions & follows medical progress NPP (patient care manager) implements decisions (dependent & independent), monitors care Nurse CCC coordinates the clinical care processes culminating in discharge
Competition for Provider Time: A non-housestaff Solution Integrating PAs, NPs and RN CCCs in Acute Care Physician (medical manager) makes key medical decisions & follows medical progress NPP (patient care manager) implements decisions (dependent & independent), monitors care Nurse CCC coordinates the clinical care processes culminating in discharge
 Fo llo vis w u its p A dm iss io ns Procedures Family conferences O ve rn ig ht ha n Administrative duties es g Dr Wilson do ff s ar h D sc i
Fo llo vis w u its p A dm iss io ns Procedures Family conferences O ve rn ig ht ha n Administrative duties es g Dr Wilson do ff s ar h D sc i
 A dm iss io ns Procedures Fo llo vis w u its p Family conferences Administrative duties O ve rn ig ht ha n es g ar h do ff s Consults isc D
A dm iss io ns Procedures Fo llo vis w u its p Family conferences Administrative duties O ve rn ig ht ha n es g ar h do ff s Consults isc D
 Learning Objectives Ø To understand how Non-Physician Providers can add value to hospitalist programs Ø To describe how integrating Non. Physician Providers can impact the delivery of care
Learning Objectives Ø To understand how Non-Physician Providers can add value to hospitalist programs Ø To describe how integrating Non. Physician Providers can impact the delivery of care
 Learning Objectives Ø To explore how a collaborative team approach influences program development Ø Examine the potential advantages and disadvantages of integrating PAs, NPs, RN CCCs, and Clinical Pharmacists into hospitalist programs
Learning Objectives Ø To explore how a collaborative team approach influences program development Ø Examine the potential advantages and disadvantages of integrating PAs, NPs, RN CCCs, and Clinical Pharmacists into hospitalist programs
 Learning Objectives Ø To examine (by audience selection) some key components of NPPs in hospitalist practices: • • • Academics: NPPs as substitute house staff Advantages and disadvantages Billing for services Credentialing, privileges and duties Demographics Education and training
Learning Objectives Ø To examine (by audience selection) some key components of NPPs in hospitalist practices: • • • Academics: NPPs as substitute house staff Advantages and disadvantages Billing for services Credentialing, privileges and duties Demographics Education and training
 Disadvantages PAs and NPs in Acute Care
Disadvantages PAs and NPs in Acute Care
 Disadvantages Ø More expensive than residents Ø Loss of Medicare DME & IME Ø May cost upwards of $85, 000 (includes benefits, recruitment, admin overhead, CME) Ø Medical liability Ø ? ? Decreased “face time”? ? Ø Potential redundancy Ø Competition Russell, et. al. , Cawley, et. al. , Med. Econ. April 2000,
Disadvantages Ø More expensive than residents Ø Loss of Medicare DME & IME Ø May cost upwards of $85, 000 (includes benefits, recruitment, admin overhead, CME) Ø Medical liability Ø ? ? Decreased “face time”? ? Ø Potential redundancy Ø Competition Russell, et. al. , Cawley, et. al. , Med. Econ. April 2000,
 Advantages PAs and NPs in Acute Care
Advantages PAs and NPs in Acute Care
 Substituting for Residents: Advantages of PAs and NPs Ø Greater consistency of ability Ø More clinical experience Ø Diminished supervision Ø Better “systems” managers Ø Enhanced efficiency Ø Stronger staff affiliations Ø Higher visibility and availability Ø Improved continuity of care Silver et. al. , Cawley et. al. , Frick et. al. , Jones et. al.
Substituting for Residents: Advantages of PAs and NPs Ø Greater consistency of ability Ø More clinical experience Ø Diminished supervision Ø Better “systems” managers Ø Enhanced efficiency Ø Stronger staff affiliations Ø Higher visibility and availability Ø Improved continuity of care Silver et. al. , Cawley et. al. , Frick et. al. , Jones et. al.
 Integrated Hospitalist Teams: Advantages of PAs and NPs Ø Cost less than M. D. F. T. E. Ø Manage the care of patients not requiring direct physician care time Ø Provide high-quality care Ø Facilitate and coordinate care processes Ø Enhance efficiency Ø Augment practice productivity Ø Serve most specialties Ø Perform procedures Economics 1990 Beck LC, Medical
Integrated Hospitalist Teams: Advantages of PAs and NPs Ø Cost less than M. D. F. T. E. Ø Manage the care of patients not requiring direct physician care time Ø Provide high-quality care Ø Facilitate and coordinate care processes Ø Enhance efficiency Ø Augment practice productivity Ø Serve most specialties Ø Perform procedures Economics 1990 Beck LC, Medical
 Integrated Hospitalist Teams: Advantages of PAs and NPs Ø Spend more time with patients, especially w. r. t. education, prevention, health maintenance Ø Interface with ancillary services and consultants Ø Write prescriptions Ø May lessen the liability risk Ø Services reimbursed by Medicare, Insurers Beck LC, Medical Economics 1990
Integrated Hospitalist Teams: Advantages of PAs and NPs Ø Spend more time with patients, especially w. r. t. education, prevention, health maintenance Ø Interface with ancillary services and consultants Ø Write prescriptions Ø May lessen the liability risk Ø Services reimbursed by Medicare, Insurers Beck LC, Medical Economics 1990
 Physician Assistants and Nurse Practitioners Evidence for Their Value “As these two major national advisory groups (Institute of Medicine and Pew Health Professions Commission) and other policy analysts have concluded, it is the integration of care using a team of providers, not the fragmentation of care through the proliferation of independent providers, that will be the model of high-quality and cost-effective health care in the future. ” link Crane, S. , "Physician Executive" 1995
Physician Assistants and Nurse Practitioners Evidence for Their Value “As these two major national advisory groups (Institute of Medicine and Pew Health Professions Commission) and other policy analysts have concluded, it is the integration of care using a team of providers, not the fragmentation of care through the proliferation of independent providers, that will be the model of high-quality and cost-effective health care in the future. ” link Crane, S. , "Physician Executive" 1995
 The Bottom Line
The Bottom Line
 Non. Physician Providers Billing for Services
Non. Physician Providers Billing for Services
 Billing Medicare: Hospital Settings Generally, all services for which Medicare would pay if provided by a physician are also covered when performed by an NPP. Medicare Part A (hospital insurance) covers facility fees, supply costs Medicare Part B (supplemental medical insurance) covers professional services and DME
Billing Medicare: Hospital Settings Generally, all services for which Medicare would pay if provided by a physician are also covered when performed by an NPP. Medicare Part A (hospital insurance) covers facility fees, supply costs Medicare Part B (supplemental medical insurance) covers professional services and DME
 Billing Medicare: Hospital Settings Medicare gives two options as to how billing should occur for hospital-employed NPPs. Salaries may: 1) Be included in the hospital’s cost report and “covered” in the facility’s Part A payment OR 2) NOT be included in the cost report, allowing each covered service by the NPP to be billed under Part B HCFA, AAPA 44
Billing Medicare: Hospital Settings Medicare gives two options as to how billing should occur for hospital-employed NPPs. Salaries may: 1) Be included in the hospital’s cost report and “covered” in the facility’s Part A payment OR 2) NOT be included in the cost report, allowing each covered service by the NPP to be billed under Part B HCFA, AAPA 44
 Billing Medicare r No separate payment may be made to NPPs when a facility or other provider payment or charge is also made for such professional services Par t. B Part A STOP HCFA-Pub. 60 AB 45
Billing Medicare r No separate payment may be made to NPPs when a facility or other provider payment or charge is also made for such professional services Par t. B Part A STOP HCFA-Pub. 60 AB 45
 Billing Medicare: Hospital Settings INCIDENT TO
Billing Medicare: Hospital Settings INCIDENT TO
 Billing Medicare: Hospital Settings Hospital Employees Part B services must be billed under the NPPs provider identification number (PIN) to be reimbursed at: · 85% of the physician fee schedule, without direct, documented physician involvement Part B services are billed under the physician’s PIN and reimbursed at: · 100% based on the physician’s level of personal, hands-on care, as documented on the patient’s chart HCFA letter to ACEP, AAPA publication 47
Billing Medicare: Hospital Settings Hospital Employees Part B services must be billed under the NPPs provider identification number (PIN) to be reimbursed at: · 85% of the physician fee schedule, without direct, documented physician involvement Part B services are billed under the physician’s PIN and reimbursed at: · 100% based on the physician’s level of personal, hands-on care, as documented on the patient’s chart HCFA letter to ACEP, AAPA publication 47
 Billing Medicare: Hospital Settings Hospital Employees The service is not automatically billed at 85% just because the NPP participated in the patient’s care The service could be billed by the physician if the NPP were to take the history and assist the physician in the physical exam… HCFA letter to ACEP, AAPA publication 48
Billing Medicare: Hospital Settings Hospital Employees The service is not automatically billed at 85% just because the NPP participated in the patient’s care The service could be billed by the physician if the NPP were to take the history and assist the physician in the physical exam… HCFA letter to ACEP, AAPA publication 48
 Billing Medicare: Hospital Settings The service is not automatically billed at 85% just because the NPP participated in the patient’s care The service could be billed by the physician at 100% if the criteria for a “shared visit” are met* *October 25, 2002 Medicare Transmittal 1776
Billing Medicare: Hospital Settings The service is not automatically billed at 85% just because the NPP participated in the patient’s care The service could be billed by the physician at 100% if the criteria for a “shared visit” are met* *October 25, 2002 Medicare Transmittal 1776
 Billing Medicare: Hospital Settings Shared Visits*: Physician Assistants ü The PA & physician must work for the same employer, practice or hospital ü The physician must provide some faceto-face portion of the E/M encounter ØSimply reviewing or signing the patient’s chart is not sufficient ØIf no physician “face time” then bill under the PAs PIN @ 85% (on-site physician presence NOT required) *October 25, 2002 Medicare Transmittal 1776
Billing Medicare: Hospital Settings Shared Visits*: Physician Assistants ü The PA & physician must work for the same employer, practice or hospital ü The physician must provide some faceto-face portion of the E/M encounter ØSimply reviewing or signing the patient’s chart is not sufficient ØIf no physician “face time” then bill under the PAs PIN @ 85% (on-site physician presence NOT required) *October 25, 2002 Medicare Transmittal 1776
 Billing Medicare: Hospital Settings Shared Visits*: Physician Assistants ü Does NOT apply to procedures (applies to hospital E/M services only) ØBill for the practitioner who does the majority of the procedure ü Does not apply to initial consults ü The physician co-documents their involvement in a “shared-visit” *October 25, 2002 Medicare Transmittal 1776
Billing Medicare: Hospital Settings Shared Visits*: Physician Assistants ü Does NOT apply to procedures (applies to hospital E/M services only) ØBill for the practitioner who does the majority of the procedure ü Does not apply to initial consults ü The physician co-documents their involvement in a “shared-visit” *October 25, 2002 Medicare Transmittal 1776
 Billing Medicare: Hospital Settings Documenting Shared Visits*: Physician Assistants First document: “I have personally shared in the visit of Mr/s. ____ along with ____PA—C providing face-to-face (or bedside) participation in the evaluation and management. I _______ (document something you actually did)” *October 25, 2002 Medicare Transmittal 1776
Billing Medicare: Hospital Settings Documenting Shared Visits*: Physician Assistants First document: “I have personally shared in the visit of Mr/s. ____ along with ____PA—C providing face-to-face (or bedside) participation in the evaluation and management. I _______ (document something you actually did)” *October 25, 2002 Medicare Transmittal 1776
 Billing Medicare: Hospital Settings Documenting Shared Visits*: Physician Assistants Then document: ü That you “agree with the E/M as documented” and then co-sign the note Or ü Key elements you wish to elaborate upon Or ü Additional elements you wish to combine with the PA note to increase the E/M code *October 25, 2002 Medicare Transmittal 1776
Billing Medicare: Hospital Settings Documenting Shared Visits*: Physician Assistants Then document: ü That you “agree with the E/M as documented” and then co-sign the note Or ü Key elements you wish to elaborate upon Or ü Additional elements you wish to combine with the PA note to increase the E/M code *October 25, 2002 Medicare Transmittal 1776
 Billing Medicare: Hospital Settings Shared Visits*: Physician Assistants Remember the “ 3 Sames and a Some” rule: ü Same employer ü Same patient ü Same day ü Some face-to-face time with the patient
Billing Medicare: Hospital Settings Shared Visits*: Physician Assistants Remember the “ 3 Sames and a Some” rule: ü Same employer ü Same patient ü Same day ü Some face-to-face time with the patient
 Billing Medicare: Hospital Settings Shared Visits: Nurse Practitioners The service could be billed by the physician at 100% if the NP provided the E/M service and the physician (same day/visit): ü personally reviewed the history ü examined the patient ü made the medical treatment decisions ü documented involvement
Billing Medicare: Hospital Settings Shared Visits: Nurse Practitioners The service could be billed by the physician at 100% if the NP provided the E/M service and the physician (same day/visit): ü personally reviewed the history ü examined the patient ü made the medical treatment decisions ü documented involvement
 Billing Medicare: Non-Hospital Employees Independent Hospitalist practices All services are billed under Part B: · 85% of the physician fee schedule without direct, documented physician involvement, using the NPPs PIN · 100% based on the physician’s level of personal, hands-on care, as documented on the patient’s chart, using the physician’s PIN
Billing Medicare: Non-Hospital Employees Independent Hospitalist practices All services are billed under Part B: · 85% of the physician fee schedule without direct, documented physician involvement, using the NPPs PIN · 100% based on the physician’s level of personal, hands-on care, as documented on the patient’s chart, using the physician’s PIN
 To scribe or not to… “Yes, it’s OK to use a scribe, ” says HCFA As long as the scribe writes “in the presence of (Dr’s name) I am taking down these notes, ” and the physician signs them “A scribe can write if the doctor is involved, and says so. ”—HCFA official Part B News, Gosfield & Assoc. , Philadelphia 57
To scribe or not to… “Yes, it’s OK to use a scribe, ” says HCFA As long as the scribe writes “in the presence of (Dr’s name) I am taking down these notes, ” and the physician signs them “A scribe can write if the doctor is involved, and says so. ”—HCFA official Part B News, Gosfield & Assoc. , Philadelphia 57
 To scribe or not to… One approach The NPP scribes: “This note is transcribed in the presence of/for Dr. X who has seen and examined this patient with me, and has directed the patient’s care. ” The physician writes (after the above note): “I have personally interviewed and examined Mr. /s. Y along with the PA-C/NP who has transcribed the full note for me from my Hx/ROS, PE findings, and medical decision making. I personally directed her/his evaluation and management. ” Supplemental Narrative documenting involvement
To scribe or not to… One approach The NPP scribes: “This note is transcribed in the presence of/for Dr. X who has seen and examined this patient with me, and has directed the patient’s care. ” The physician writes (after the above note): “I have personally interviewed and examined Mr. /s. Y along with the PA-C/NP who has transcribed the full note for me from my Hx/ROS, PE findings, and medical decision making. I personally directed her/his evaluation and management. ” Supplemental Narrative documenting involvement
 Private Insurance s Enrolling new products with an existing NPP s Bringing an NPP into existing products Contact the payor and obtain in writing: · · · The representative’s name The written policy or contract Specific reimbursement issues:
Private Insurance s Enrolling new products with an existing NPP s Bringing an NPP into existing products Contact the payor and obtain in writing: · · · The representative’s name The written policy or contract Specific reimbursement issues:
 Private Insurance · Specific reimbursement issues: · · Requirements on supervision Limitations on services provided Inpatient/hospital setting How to submit billing, by NPP or physician provider number Covers services for authorized providers
Private Insurance · Specific reimbursement issues: · · Requirements on supervision Limitations on services provided Inpatient/hospital setting How to submit billing, by NPP or physician provider number Covers services for authorized providers
 The Bottom Line: Costs & Reimbursements
The Bottom Line: Costs & Reimbursements
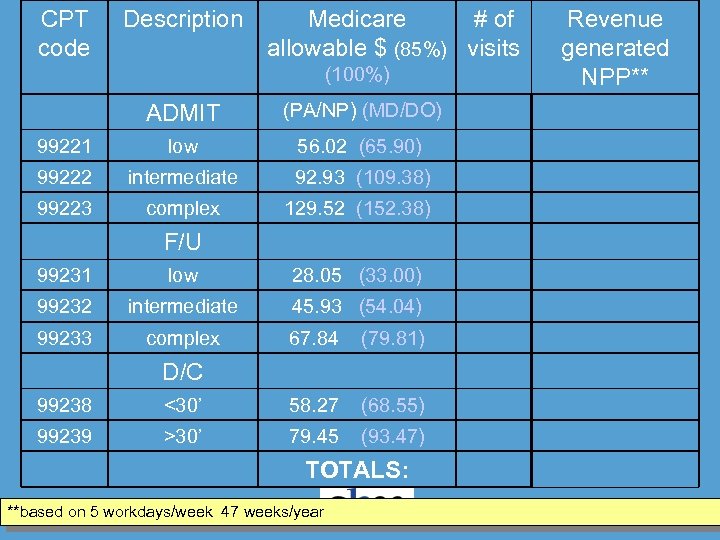 CPT code Description Medicare # of allowable $ (85%) visits (100%) ADMIT (PA/NP) (MD/DO) 99221 low 56. 02 (65. 90) 99222 intermediate 92. 93 (109. 38) 99223 complex 129. 52 (152. 38) F/U 99231 low 28. 05 (33. 00) 99232 intermediate 45. 93 (54. 04) 99233 complex 67. 84 (79. 81) D/C 99238 <30’ 58. 27 (68. 55) 99239 >30’ 79. 45 (93. 47) TOTALS: **based on 5 workdays/week 47 weeks/year Revenue generated NPP**
CPT code Description Medicare # of allowable $ (85%) visits (100%) ADMIT (PA/NP) (MD/DO) 99221 low 56. 02 (65. 90) 99222 intermediate 92. 93 (109. 38) 99223 complex 129. 52 (152. 38) F/U 99231 low 28. 05 (33. 00) 99232 intermediate 45. 93 (54. 04) 99233 complex 67. 84 (79. 81) D/C 99238 <30’ 58. 27 (68. 55) 99239 >30’ 79. 45 (93. 47) TOTALS: **based on 5 workdays/week 47 weeks/year Revenue generated NPP**
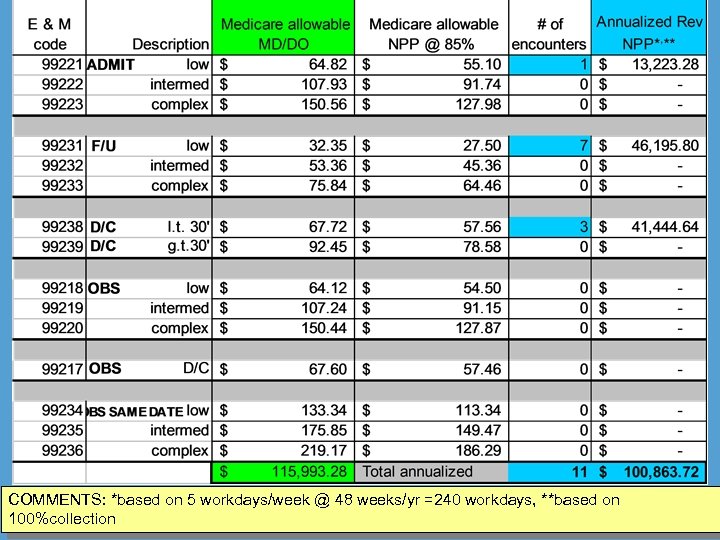 COMMENTS: *based on 5 workdays/week @ 48 weeks/yr =240 workdays, **based on 100%collection
COMMENTS: *based on 5 workdays/week @ 48 weeks/yr =240 workdays, **based on 100%collection
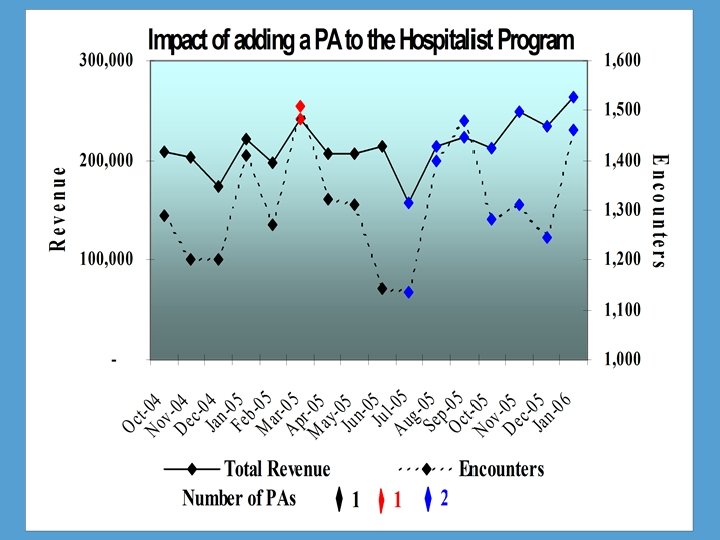
 The Bottom Line: Costs & Reimbursements Rev. per Day NP PA Cost per Day Net Rev. per Day $528 $263 $265 $826 $254 $572 Allied Consulting Inc. from MGMA Phys Comp & Prod Survey: 1998 Report Based on 1997 Data
The Bottom Line: Costs & Reimbursements Rev. per Day NP PA Cost per Day Net Rev. per Day $528 $263 $265 $826 $254 $572 Allied Consulting Inc. from MGMA Phys Comp & Prod Survey: 1998 Report Based on 1997 Data
 The Bottom Line: Costs & Reimbursements Median Gross Charges NP PA $206, 821 $395, 635 Physician Compensation and Production Survey: 1999 Report based on 1998 Data, MGMA
The Bottom Line: Costs & Reimbursements Median Gross Charges NP PA $206, 821 $395, 635 Physician Compensation and Production Survey: 1999 Report based on 1998 Data, MGMA
 Credentialing, Privileges and Guidelines Delineating Duties
Credentialing, Privileges and Guidelines Delineating Duties
 Hospital Credentialing Ø Based on state statutes regarding licensure and certification Ø Institutional guidelines typically developed by the credentials committee of the medical staff through amendments to the medical staff bylaws Ø Specifies types of educational and professional qualifications required for privileges Cawley, et. al. , AAPA
Hospital Credentialing Ø Based on state statutes regarding licensure and certification Ø Institutional guidelines typically developed by the credentials committee of the medical staff through amendments to the medical staff bylaws Ø Specifies types of educational and professional qualifications required for privileges Cawley, et. al. , AAPA
 Hospital Credentialing Ø A typical candidate is required to: ¤ Be a graduate of a CAHEA or NLN accredited program ¤ Be eligible for or have passed the national certifying exam by the NCCPA, or various nursing specialty boards ¤ Be properly registered with the state’s medical or nursing licensing board Cawley, et. al. , AAPA, NLN
Hospital Credentialing Ø A typical candidate is required to: ¤ Be a graduate of a CAHEA or NLN accredited program ¤ Be eligible for or have passed the national certifying exam by the NCCPA, or various nursing specialty boards ¤ Be properly registered with the state’s medical or nursing licensing board Cawley, et. al. , AAPA, NLN
 Hospital Privileges Ø Most hospitals use the same process for NPPs that they use for physicians, including provisional or courtesy status Ø Upon approval, “limited” medical staff privileges are granted—“staff affiliate” or “associate staff” Ø Guidance available from AAPA, JCAHO, AHA, HCFA, state agencies Ø Delineation of duties JCAHO, HCFA AAPA,
Hospital Privileges Ø Most hospitals use the same process for NPPs that they use for physicians, including provisional or courtesy status Ø Upon approval, “limited” medical staff privileges are granted—“staff affiliate” or “associate staff” Ø Guidance available from AAPA, JCAHO, AHA, HCFA, state agencies Ø Delineation of duties JCAHO, HCFA AAPA,
 Guidelines Delineating Duties Ø Evaluate adequacy of training and qualifications of the NPP for anticipated duties Ø Review specific needs and requirements of the medical attending staff Ø Provide for supervision and monitoring of performance Ø Delineate expected clinical duties the NPP will perform Cawley, et. al. , AAPA
Guidelines Delineating Duties Ø Evaluate adequacy of training and qualifications of the NPP for anticipated duties Ø Review specific needs and requirements of the medical attending staff Ø Provide for supervision and monitoring of performance Ø Delineate expected clinical duties the NPP will perform Cawley, et. al. , AAPA
 Guidelines Delineating Duties Ø Job description outlining both common tasks and specific duties Ø AMA-defined categories of clinical services: Evaluation ¤ Monitoring ¤ Diagnostics ¤ Therapeutics ¤ Counseling ¤ Referral ¤ Cawley, et. al. , AMA, Patient Care Jan. 1995
Guidelines Delineating Duties Ø Job description outlining both common tasks and specific duties Ø AMA-defined categories of clinical services: Evaluation ¤ Monitoring ¤ Diagnostics ¤ Therapeutics ¤ Counseling ¤ Referral ¤ Cawley, et. al. , AMA, Patient Care Jan. 1995
 Guidelines Delineating Duties Ø Specify tasks or actions beyond the institutional scope of practice Ø Opportunities for “extended” privileges beyond the basic job description ¤Seniority and advancement ¤Additional proficiency ¤Specialty roles Cawley, et. al. , AAPA, JCAHO
Guidelines Delineating Duties Ø Specify tasks or actions beyond the institutional scope of practice Ø Opportunities for “extended” privileges beyond the basic job description ¤Seniority and advancement ¤Additional proficiency ¤Specialty roles Cawley, et. al. , AAPA, JCAHO
 Summary Recommendations Adding NPPs to the Hospitalist Mix 1) “Institutional commitment to an MLP program is vital. ” 2) “Local history and circumstance must be considered in MLP program design and implementation. ” 3) “The PAs and residents have to be portrayed to the attending physician staff, and to each other, as partners, not competitors. ” Russell et. al. , Acad Med 1999; 74(6)
Summary Recommendations Adding NPPs to the Hospitalist Mix 1) “Institutional commitment to an MLP program is vital. ” 2) “Local history and circumstance must be considered in MLP program design and implementation. ” 3) “The PAs and residents have to be portrayed to the attending physician staff, and to each other, as partners, not competitors. ” Russell et. al. , Acad Med 1999; 74(6)
 Summary Recommendations Adding NPPs to the Hospitalist Mix 4) “Using an educational model for the PA program can be worthwhile. ” 5) “Implement a comprehensive PA program. ” 6) “A comprehensive PA program requires effective leadership. ” Russell et. al. , Acad Med 1999; 74(6)
Summary Recommendations Adding NPPs to the Hospitalist Mix 4) “Using an educational model for the PA program can be worthwhile. ” 5) “Implement a comprehensive PA program. ” 6) “A comprehensive PA program requires effective leadership. ” Russell et. al. , Acad Med 1999; 74(6)
 Summary Recommendations Adding NPPs to the Hospitalist Mix 7) On screening candidates: a. Verify credentials b. Get the “right” people: i. There’s no “I” in TEAM ii. Techno-savvy iii. Adaptable iv. Interdependent roles
Summary Recommendations Adding NPPs to the Hospitalist Mix 7) On screening candidates: a. Verify credentials b. Get the “right” people: i. There’s no “I” in TEAM ii. Techno-savvy iii. Adaptable iv. Interdependent roles
 Summary Recommendations Adding NPPs to the Hospitalist Mix 8) Know the rules: a. State regulations, registration, certification b. Institutional bylaws and privileges c. Documentation, billing, reimbursement 9) Write specific practice guidelines 10) Provide a career path and incentives
Summary Recommendations Adding NPPs to the Hospitalist Mix 8) Know the rules: a. State regulations, registration, certification b. Institutional bylaws and privileges c. Documentation, billing, reimbursement 9) Write specific practice guidelines 10) Provide a career path and incentives
 On-line Resources Ø www. aapa. org Ø www. aanp. org Ø www. nurse. org/acnp
On-line Resources Ø www. aapa. org Ø www. aanp. org Ø www. nurse. org/acnp
 DEMOGRAPHICS A National Overview
DEMOGRAPHICS A National Overview
 Demographics: Physician Assistants AAPA Survey says: Ø Nationwide, 66, 483 graduates eligible to practice as PAs, 58, 665 in actual practice Ø 89% PAs in clinical practice Ø 36% of practicing PAs listed the hospital setting as their primary setting 2005 AAPA Census
Demographics: Physician Assistants AAPA Survey says: Ø Nationwide, 66, 483 graduates eligible to practice as PAs, 58, 665 in actual practice Ø 89% PAs in clinical practice Ø 36% of practicing PAs listed the hospital setting as their primary setting 2005 AAPA Census
 Demographics: Physician Assistants AAPA Survey says: Ø Of the 36 % listing the hospital as their primary unit, 9. 3% are employed full time in an inpatient unit of the hospital: • Outpatient unit 7. 0% • OR 7. 0% 2005 AAPA Census • ED 9. 0%
Demographics: Physician Assistants AAPA Survey says: Ø Of the 36 % listing the hospital as their primary unit, 9. 3% are employed full time in an inpatient unit of the hospital: • Outpatient unit 7. 0% • OR 7. 0% 2005 AAPA Census • ED 9. 0%
 Demographics: Physician Assistants Survey continues: Ø 37% manage the care of patients in an inpatient setting Ø 22. 4 % are employed by hospitals Ø 40% see some inpatients in their job Ø Of the 22, 502 respondents asked to define the subpopulation they care for 920 or 4. 1% were determined to “likely function in a hospitalist role. ” Ø If this projects out, then of the 58, 665 practicing PAs, we might assume there are 2, 405 “Hospitalist PAs” in circulation nationwide. 2005 AAPA Census
Demographics: Physician Assistants Survey continues: Ø 37% manage the care of patients in an inpatient setting Ø 22. 4 % are employed by hospitals Ø 40% see some inpatients in their job Ø Of the 22, 502 respondents asked to define the subpopulation they care for 920 or 4. 1% were determined to “likely function in a hospitalist role. ” Ø If this projects out, then of the 58, 665 practicing PAs, we might assume there are 2, 405 “Hospitalist PAs” in circulation nationwide. 2005 AAPA Census
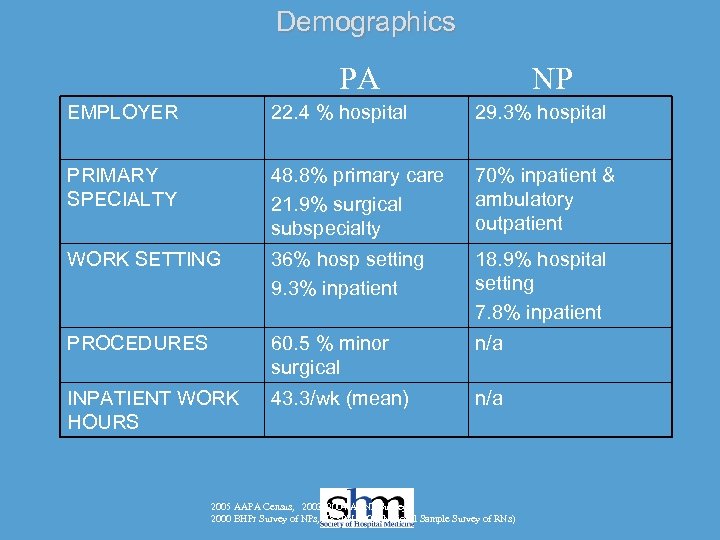 Demographics PA NP EMPLOYER 22. 4 % hospital 29. 3% hospital PRIMARY SPECIALTY 48. 8% primary care 21. 9% surgical subspecialty 70% inpatient & ambulatory outpatient WORK SETTING 36% hosp setting 9. 3% inpatient 18. 9% hospital setting 7. 8% inpatient PROCEDURES 60. 5 % minor surgical n/a INPATIENT WORK HOURS 43. 3/wk (mean) n/a 2005 AAPA Census, 2003, 2004 ACNP Survey, 2000 BHPr Survey of NPs, NSSRN 2000 (National Sample Survey of RNs)
Demographics PA NP EMPLOYER 22. 4 % hospital 29. 3% hospital PRIMARY SPECIALTY 48. 8% primary care 21. 9% surgical subspecialty 70% inpatient & ambulatory outpatient WORK SETTING 36% hosp setting 9. 3% inpatient 18. 9% hospital setting 7. 8% inpatient PROCEDURES 60. 5 % minor surgical n/a INPATIENT WORK HOURS 43. 3/wk (mean) n/a 2005 AAPA Census, 2003, 2004 ACNP Survey, 2000 BHPr Survey of NPs, NSSRN 2000 (National Sample Survey of RNs)
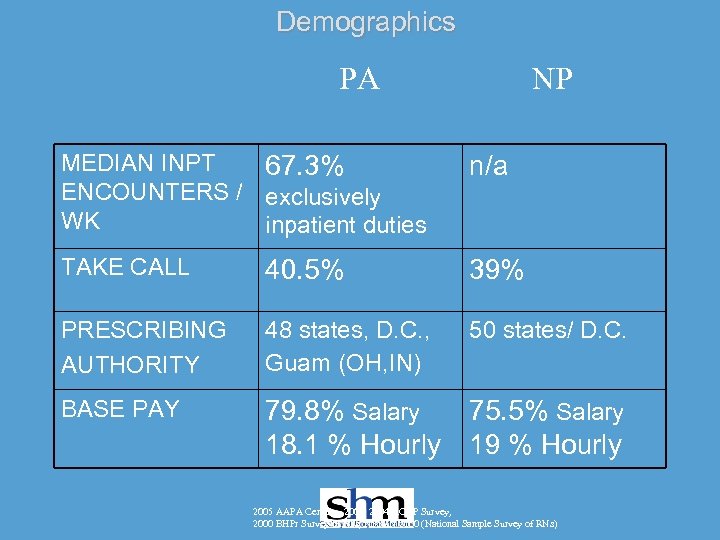 Demographics PA NP MEDIAN INPT 67. 3% ENCOUNTERS / exclusively WK inpatient duties n/a TAKE CALL 40. 5% 39% PRESCRIBING AUTHORITY 48 states, D. C. , Guam (OH, IN) 50 states/ D. C. BASE PAY 79. 8% Salary 18. 1 % Hourly 75. 5% Salary 19 % Hourly 2005 AAPA Census, 2003, 2004 ACNP Survey, 2000 BHPr Survey of NPs, NSSRN 2000 (National Sample Survey of RNs)
Demographics PA NP MEDIAN INPT 67. 3% ENCOUNTERS / exclusively WK inpatient duties n/a TAKE CALL 40. 5% 39% PRESCRIBING AUTHORITY 48 states, D. C. , Guam (OH, IN) 50 states/ D. C. BASE PAY 79. 8% Salary 18. 1 % Hourly 75. 5% Salary 19 % Hourly 2005 AAPA Census, 2003, 2004 ACNP Survey, 2000 BHPr Survey of NPs, NSSRN 2000 (National Sample Survey of RNs)
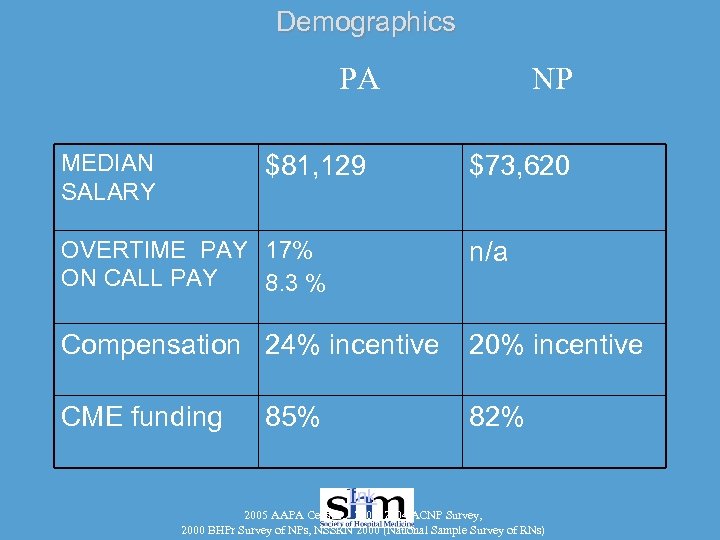 Demographics PA MEDIAN SALARY $81, 129 NP $73, 620 OVERTIME PAY 17% ON CALL PAY 8. 3 % n/a Compensation 24% incentive 20% incentive CME funding 82% 85% link 2005 AAPA Census, 2003, 2004 ACNP Survey, 2000 BHPr Survey of NPs, NSSRN 2000 (National Sample Survey of RNs)
Demographics PA MEDIAN SALARY $81, 129 NP $73, 620 OVERTIME PAY 17% ON CALL PAY 8. 3 % n/a Compensation 24% incentive 20% incentive CME funding 82% 85% link 2005 AAPA Census, 2003, 2004 ACNP Survey, 2000 BHPr Survey of NPs, NSSRN 2000 (National Sample Survey of RNs)
 Non. Physician Providers THE EDUCATION AND TRAINING OF PHYSICIAN ASSISTANTS AND NURSE PRACTITIONERS
Non. Physician Providers THE EDUCATION AND TRAINING OF PHYSICIAN ASSISTANTS AND NURSE PRACTITIONERS
 The Education and Training of Physician Assistants G 120 programs accredited currently, several pending G Program accreditation by the Accreditation Review Committee-Physician Assistant (ARC -PA); necessary for: & eligibility for federal Title VII grant funding & graduates to qualify (along with passage of the Physician Assistant National Certifying Exam [PANCE]) to practice in most states
The Education and Training of Physician Assistants G 120 programs accredited currently, several pending G Program accreditation by the Accreditation Review Committee-Physician Assistant (ARC -PA); necessary for: & eligibility for federal Title VII grant funding & graduates to qualify (along with passage of the Physician Assistant National Certifying Exam [PANCE]) to practice in most states
 The Education and Training of Physician Assistants G ARC-PA is sponsored by: & American Academy of Family Physicians & American Academy of Pediatrics & American Academy of Physician Assistants & American College of Physicians & American College of Surgeons & AMA & Association of Physician Assistant Programs
The Education and Training of Physician Assistants G ARC-PA is sponsored by: & American Academy of Family Physicians & American Academy of Pediatrics & American Academy of Physician Assistants & American College of Physicians & American College of Surgeons & AMA & Association of Physician Assistant Programs
 The Education and Training of Physician Assistants G First program at Duke Universitycompetency-based, generalist program with specific curricula addressing the most frequently encountered clinical problems G Curricula addressed outpatient primary care, emphasis on underserved areas G Program innovations now include inpatient and subspecialty care, more in line with traditional medical model
The Education and Training of Physician Assistants G First program at Duke Universitycompetency-based, generalist program with specific curricula addressing the most frequently encountered clinical problems G Curricula addressed outpatient primary care, emphasis on underserved areas G Program innovations now include inpatient and subspecialty care, more in line with traditional medical model
 The Education and Training of Physician Assistants G Typical applicant has obtained bachelor’s degree and has at least 4 years health care experience G Average PA program curriculum is 111 weeks (24 -26 months) G Credential awarded varies from certificate only (rare), to Bachelor or a Master’s degree
The Education and Training of Physician Assistants G Typical applicant has obtained bachelor’s degree and has at least 4 years health care experience G Average PA program curriculum is 111 weeks (24 -26 months) G Credential awarded varies from certificate only (rare), to Bachelor or a Master’s degree
 The Education and Training of Physician Assistants G Format of the typical PA program educates the student in primary care: ***regional differences & Approximately 10 -12 months for didactic instruction in the basic and clinical sciences & Followed by a similar period of rotating clerkships and preceptorships in all major clinical disciplines
The Education and Training of Physician Assistants G Format of the typical PA program educates the student in primary care: ***regional differences & Approximately 10 -12 months for didactic instruction in the basic and clinical sciences & Followed by a similar period of rotating clerkships and preceptorships in all major clinical disciplines
 The Education and Training of Physician Assistants G Didactic courses include: & anatomy & pathophysiology & microbiology & biochemistry & pharmacology
The Education and Training of Physician Assistants G Didactic courses include: & anatomy & pathophysiology & microbiology & biochemistry & pharmacology
 The Education and Training of Physician Assistants & behavioral/social sciences, including: health promotion/disease prevention bioethics medical sociology death and dying cross cultural medicine
The Education and Training of Physician Assistants & behavioral/social sciences, including: health promotion/disease prevention bioethics medical sociology death and dying cross cultural medicine
 The Education and Training of Physician Assistants GClinical course work includes & history & physical examination & clinical diagnosis & communication and interpersonal skills & epidemiology and preventative medicine & clinical procedures and surgical skills, and & interpretation of laboratory tests and imaging studies
The Education and Training of Physician Assistants GClinical course work includes & history & physical examination & clinical diagnosis & communication and interpersonal skills & epidemiology and preventative medicine & clinical procedures and surgical skills, and & interpretation of laboratory tests and imaging studies
 The Education and Training of Physician Assistants & Clinical rotations: inpatient medicine primary care/ambulatory medicine pediatrics obstetrics and gynecology psychiatry emergency medicine Radiology and imaging sciences & Final surgery preceptorship in primary care or a subspecialty
The Education and Training of Physician Assistants & Clinical rotations: inpatient medicine primary care/ambulatory medicine pediatrics obstetrics and gynecology psychiatry emergency medicine Radiology and imaging sciences & Final surgery preceptorship in primary care or a subspecialty
 The Education and Training of Physician Assistants G Postgraduate residency programs: 1 yr intense supervised clinical experience in specialty disciplines &Surgery &Pediatrics/Neonatology &Emergency Medicine &Occupational Medicine &Primary Care
The Education and Training of Physician Assistants G Postgraduate residency programs: 1 yr intense supervised clinical experience in specialty disciplines &Surgery &Pediatrics/Neonatology &Emergency Medicine &Occupational Medicine &Primary Care
 The Education and Training of Physician Assistants G Licensure and scope of practice defined by licensure statutes/state practice acts G Renewal q 2 yrs for most states G Certification by national examination PANCE, with recertification every 6 years G CME mandatory to maintain license, with minimum # of hours per state and national boards
The Education and Training of Physician Assistants G Licensure and scope of practice defined by licensure statutes/state practice acts G Renewal q 2 yrs for most states G Certification by national examination PANCE, with recertification every 6 years G CME mandatory to maintain license, with minimum # of hours per state and national boards
 Non. Physician Providers NURSE PRACTITIONERS
Non. Physician Providers NURSE PRACTITIONERS
 The Education and Training of Nurse Practitioners G Over 400 NP programs currently G Accreditation of programs by National League of Nursing G Must have a professional nursing degree prior to entrance into program G Degree awarded may be certificate only, or Master’s G Program generally full time 2 yrs
The Education and Training of Nurse Practitioners G Over 400 NP programs currently G Accreditation of programs by National League of Nursing G Must have a professional nursing degree prior to entrance into program G Degree awarded may be certificate only, or Master’s G Program generally full time 2 yrs
 The Education and Training of Nurse Practitioners GTypes of programs: & Family NP & Adult NP & Pediatric NP & School NP & Geriatric NP & Acute Care NP
The Education and Training of Nurse Practitioners GTypes of programs: & Family NP & Adult NP & Pediatric NP & School NP & Geriatric NP & Acute Care NP
 The Education and Training of Nurse Practitioners G Basic NP program: & pharmacology & pathophysiology & research & health promotion and disease prevention & differential diagnosis and disease management & ethics & advanced health assessment & with min clinical hours 500+
The Education and Training of Nurse Practitioners G Basic NP program: & pharmacology & pathophysiology & research & health promotion and disease prevention & differential diagnosis and disease management & ethics & advanced health assessment & with min clinical hours 500+
 The Education and Training of Nurse Practitioners G ACNP: curricula includes above with the specialty’s emphasis on pathophysiology, differential diagnoses, pharmacology G Clinical rotations on general wards, surgery, emergency medicine, and units specific to the specialty
The Education and Training of Nurse Practitioners G ACNP: curricula includes above with the specialty’s emphasis on pathophysiology, differential diagnoses, pharmacology G Clinical rotations on general wards, surgery, emergency medicine, and units specific to the specialty
 The Education and Training of Nurse Practitioners GLicensure and scope of practice set by the individual states’ Board of Nursing (BON) GCertification by national exam not required by all states but is recommended by the AANP and ACNP GCNE required for license renewal and regulated by state’s BON link
The Education and Training of Nurse Practitioners GLicensure and scope of practice set by the individual states’ Board of Nursing (BON) GCertification by national exam not required by all states but is recommended by the AANP and ACNP GCNE required for license renewal and regulated by state’s BON link
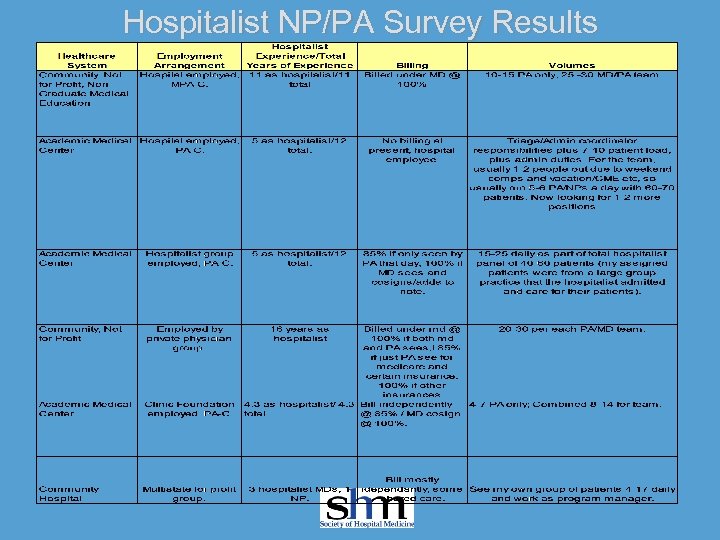 Hospitalist NP/PA Survey Results
Hospitalist NP/PA Survey Results
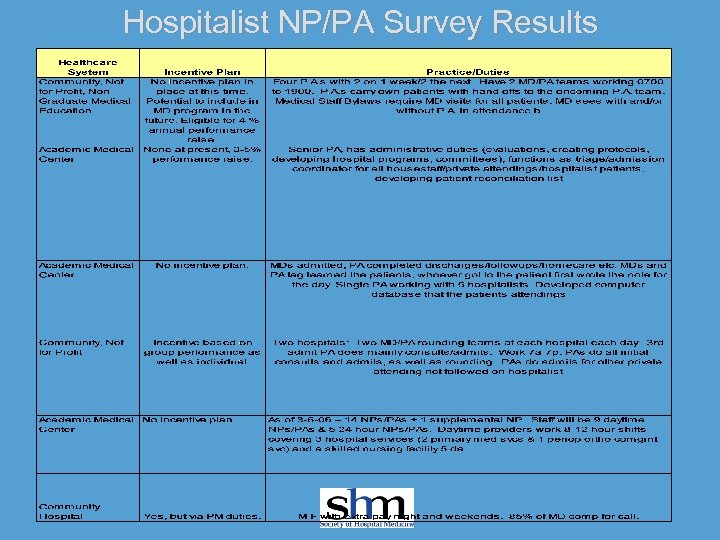 Hospitalist NP/PA Survey Results
Hospitalist NP/PA Survey Results
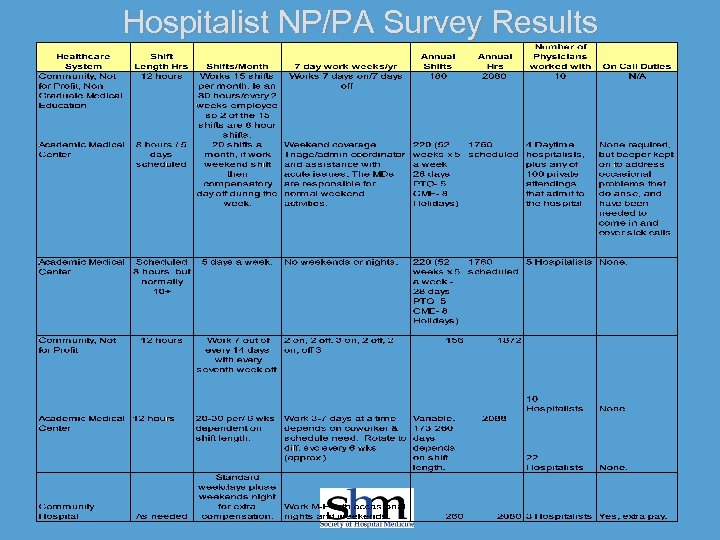 Hospitalist NP/PA Survey Results
Hospitalist NP/PA Survey Results
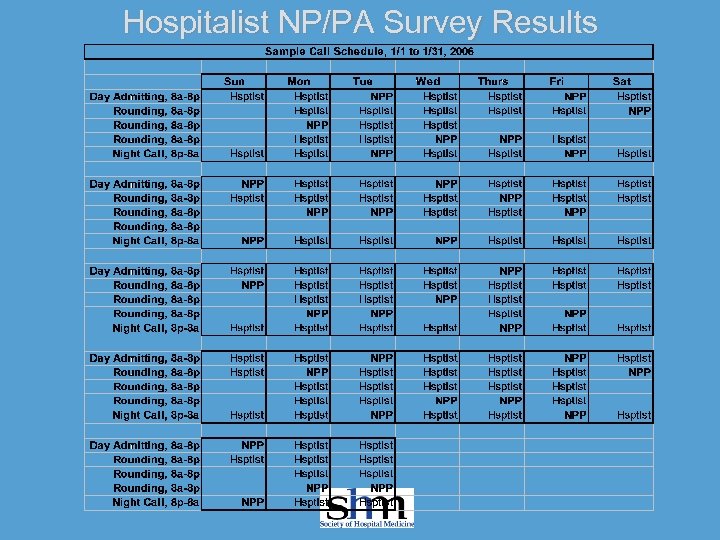 Hospitalist NP/PA Survey Results
Hospitalist NP/PA Survey Results


