6743a9a61d93d9645ddd77caad5f5d82.ppt
- Количество слайдов: 78
 Mentorship: Colouring the context of clinical practice Welcome Mentor Preparation/ updates Newsletter Practice Facilitators Key contacts Forum Distance learning fairnessfainess FAIRNESSfairnessfairnessfai rness. FAIRNESSfairn essfairnessfairness Standards and learning Enter site Challenge and support Accountability and risk taking Credible assessment FAQ’s
Mentorship: Colouring the context of clinical practice Welcome Mentor Preparation/ updates Newsletter Practice Facilitators Key contacts Forum Distance learning fairnessfainess FAIRNESSfairnessfairnessfai rness. FAIRNESSfairn essfairnessfairness Standards and learning Enter site Challenge and support Accountability and risk taking Credible assessment FAQ’s
 Welcome Working in partnership How to navigate the mentor web pages… Welcome to the mentor pages of the Abertawe Bro Morgannwg University Health Board intranet site. The pages contain a wide range of information and materials relating to mentorship and the assessment of pre-registration student nurses in clinical practice. Click on the front page menu bar or whenever you see any coloured icons, pictures or text to take you to specific information. You can move forward and back and return to home at any point. fairness FAIRNE SSfairn NMC Standards and learning Challenge and support Accountability and risk taking Credible assessment welcome forward bac k hom e
Welcome Working in partnership How to navigate the mentor web pages… Welcome to the mentor pages of the Abertawe Bro Morgannwg University Health Board intranet site. The pages contain a wide range of information and materials relating to mentorship and the assessment of pre-registration student nurses in clinical practice. Click on the front page menu bar or whenever you see any coloured icons, pictures or text to take you to specific information. You can move forward and back and return to home at any point. fairness FAIRNE SSfairn NMC Standards and learning Challenge and support Accountability and risk taking Credible assessment welcome forward bac k hom e
 Welcome Working in partnership Partnership Support Achievement ABMU Health Board mission statement supports learning, teaching and assessment in order to: Develop mutually proactive mentorship between registered nurses and preregistration nursing students through partnership, support and achievement. Effective mentorship is highly prized in Abertawe Bro Morgannwg University Health Board. Both Swansea and Glamorgan University allocate pre-registration nursing students to clinical placements across nursing Directorates within the Health Board. The learning environment within these placements is continually monitored and measured against educational audit standards. Opportunities are available for student nurses within the context of inter professional learning and working in modern healthcare. fairness FAIRNE SSfairn forward back home
Welcome Working in partnership Partnership Support Achievement ABMU Health Board mission statement supports learning, teaching and assessment in order to: Develop mutually proactive mentorship between registered nurses and preregistration nursing students through partnership, support and achievement. Effective mentorship is highly prized in Abertawe Bro Morgannwg University Health Board. Both Swansea and Glamorgan University allocate pre-registration nursing students to clinical placements across nursing Directorates within the Health Board. The learning environment within these placements is continually monitored and measured against educational audit standards. Opportunities are available for student nurses within the context of inter professional learning and working in modern healthcare. fairness FAIRNE SSfairn forward back home
 Welcome Working in partnership Clarification: A ‘mentor’ is a registered nurse who supports pre-registration student nurses. All mentors will have completed a Nursing and Midwifery Council approved mentor preparation course and will meet the criteria to act as a mentor outlined in ‘Standards to support learning and assessment in practice’ (NMC 2008). A crucial aspect of contemporary student nurse training is mentorship. Each student is assigned a mentor (a registered nurse having undergone an NMC approved mentor preparation programme) in every clinical placement. The mentor acts as a role model and guide as well as being responsible together with colleagues for providing a credible assessment of students’ practice outcomes. A ‘preceptor’ has become associated with a registered nurse who supports a newly qualified nurse in their first year post qualification. Principle 8 of the current NMC review of pre-registration nursing is that a mandatory period of preceptorship will follow initial registration. fairness FAIRNE SSfairn forward back home
Welcome Working in partnership Clarification: A ‘mentor’ is a registered nurse who supports pre-registration student nurses. All mentors will have completed a Nursing and Midwifery Council approved mentor preparation course and will meet the criteria to act as a mentor outlined in ‘Standards to support learning and assessment in practice’ (NMC 2008). A crucial aspect of contemporary student nurse training is mentorship. Each student is assigned a mentor (a registered nurse having undergone an NMC approved mentor preparation programme) in every clinical placement. The mentor acts as a role model and guide as well as being responsible together with colleagues for providing a credible assessment of students’ practice outcomes. A ‘preceptor’ has become associated with a registered nurse who supports a newly qualified nurse in their first year post qualification. Principle 8 of the current NMC review of pre-registration nursing is that a mandatory period of preceptorship will follow initial registration. fairness FAIRNE SSfairn forward back home
 Welcome Working in partnership What is a mentor? A mentor is a registered nurse, midwife, health visitor, or specialist community public health nurse (registrant) who facilitates learning and supervises and assesses students in a practice setting. Mentors work alongside students in clinical areas helping them to develop their skills and apply their knowledge. By reflecting both in and on practice mentors help students to become confident and competent practitioners. Can anybody mentor students? It is recognised that staff of all grades across the full range of disciplines within the inter professional Team may be able to offer a valuable contribution to the students learning in practice. However a named mentor must facilitate this process and provide an assessment of the student’s completion of set outcomes as described in their programme. Can all nurses become mentors? All nurses can become mentors by undertaking an NMC approved mentor preparation programme. You would need to be qualified for a minimum of 12 months to be eligible for a place on such a programme. This is to allow registrants to consolidate their practice and to further develop their own skills and knowledge before passing them on to others. How do I become a mentor? To become a mentor you need to undertake an NMC approved mentor preparation programme. These are run in partnership with local universities (Swansea University and the University of Glamorgan) and involve 10 days of study, 5 days protected learning time and in practice. You may be eligible for a shorter course if you are granted accreditation for prior experiential learning, You would need to negotiate this before commencing the course. fairness FAIRNE SSfairn forward back home
Welcome Working in partnership What is a mentor? A mentor is a registered nurse, midwife, health visitor, or specialist community public health nurse (registrant) who facilitates learning and supervises and assesses students in a practice setting. Mentors work alongside students in clinical areas helping them to develop their skills and apply their knowledge. By reflecting both in and on practice mentors help students to become confident and competent practitioners. Can anybody mentor students? It is recognised that staff of all grades across the full range of disciplines within the inter professional Team may be able to offer a valuable contribution to the students learning in practice. However a named mentor must facilitate this process and provide an assessment of the student’s completion of set outcomes as described in their programme. Can all nurses become mentors? All nurses can become mentors by undertaking an NMC approved mentor preparation programme. You would need to be qualified for a minimum of 12 months to be eligible for a place on such a programme. This is to allow registrants to consolidate their practice and to further develop their own skills and knowledge before passing them on to others. How do I become a mentor? To become a mentor you need to undertake an NMC approved mentor preparation programme. These are run in partnership with local universities (Swansea University and the University of Glamorgan) and involve 10 days of study, 5 days protected learning time and in practice. You may be eligible for a shorter course if you are granted accreditation for prior experiential learning, You would need to negotiate this before commencing the course. fairness FAIRNE SSfairn forward back home
 Welcome Working in partnership Brief history of recent changes in nurse training The role of the mentor has gained ever more prominence in nursing in recent years. This reflects a major change in nurse education training. In 1999 a commissioned report by Sir Leonard Peach entitled ‘Fitness for Practice’ made recommendations including a need to focus attention on the accountability and credibility of mentors’ decision making. fairness FAIRNE SSfairn forward back home
Welcome Working in partnership Brief history of recent changes in nurse training The role of the mentor has gained ever more prominence in nursing in recent years. This reflects a major change in nurse education training. In 1999 a commissioned report by Sir Leonard Peach entitled ‘Fitness for Practice’ made recommendations including a need to focus attention on the accountability and credibility of mentors’ decision making. fairness FAIRNE SSfairn forward back home
 Welcome Working in partnership An expectation of adult learning between mentors and students Interpersonal skills which encourage students and mentors to reflect more closely on care events, becomes a way for both parties to describe, explore, evaluate or perhaps celebrate their roles in these encounters. The photograph of refracted images in water above is offered as an analogy for the multi-layered complexity of clinical experiences students and mentors encounter within practice settings. Each clinical episode brings with it a unique set of interpersonal relationships and attachments with patients and the wider care team. These multilayered ripples and connections leave enduring thoughts and feelings that all participants in those episodes attempt to make sense of. fairness FAIRNE SSfairn back Home
Welcome Working in partnership An expectation of adult learning between mentors and students Interpersonal skills which encourage students and mentors to reflect more closely on care events, becomes a way for both parties to describe, explore, evaluate or perhaps celebrate their roles in these encounters. The photograph of refracted images in water above is offered as an analogy for the multi-layered complexity of clinical experiences students and mentors encounter within practice settings. Each clinical episode brings with it a unique set of interpersonal relationships and attachments with patients and the wider care team. These multilayered ripples and connections leave enduring thoughts and feelings that all participants in those episodes attempt to make sense of. fairness FAIRNE SSfairn back Home
 Standards and learning Working in partnership How mentors interpret competence in their assessment of pre-registration student nurses has taken on increasingly significant importance in recent years. New ‘Standards to support learning and assessment in practice’ (NMC 2008) require that students on NMC approved pre-registration nursing education programmes, leading to registration on the nurses’ part of the register, must be supported and assessed by mentors who meet criteria for their role. This is vital when signing off proficiency at certain stages of students’ training. There will be a triennial review of nurses who are on the local register as a mentor, sign-off mentor or practice teacher. From September 2007 a ‘sign-off mentor’ who has met additional criteria must make the final assessment of practice and confirm to the NMC that the required proficiencies for entry to the register have been achieved. There are five underpinning principles and eight domains in the NMC Standards framework. Each with identified outcomes at four developmental stages for registrants, mentors, practice teachers and teachers. The domains are: 1 Establishing effective working relationships 2 Facilitation of learning 3 Assessment and accountability 4 Evaluation of learning 5 Creating an environment for learning 6 Context of practice 7 Evidence-based practice 8 Leadership Focus Download copy of NMC Standards to support learning and assessment in practice (2010) from Mentorship Categories page fairness FAIRNE SSfairn welcome home
Standards and learning Working in partnership How mentors interpret competence in their assessment of pre-registration student nurses has taken on increasingly significant importance in recent years. New ‘Standards to support learning and assessment in practice’ (NMC 2008) require that students on NMC approved pre-registration nursing education programmes, leading to registration on the nurses’ part of the register, must be supported and assessed by mentors who meet criteria for their role. This is vital when signing off proficiency at certain stages of students’ training. There will be a triennial review of nurses who are on the local register as a mentor, sign-off mentor or practice teacher. From September 2007 a ‘sign-off mentor’ who has met additional criteria must make the final assessment of practice and confirm to the NMC that the required proficiencies for entry to the register have been achieved. There are five underpinning principles and eight domains in the NMC Standards framework. Each with identified outcomes at four developmental stages for registrants, mentors, practice teachers and teachers. The domains are: 1 Establishing effective working relationships 2 Facilitation of learning 3 Assessment and accountability 4 Evaluation of learning 5 Creating an environment for learning 6 Context of practice 7 Evidence-based practice 8 Leadership Focus Download copy of NMC Standards to support learning and assessment in practice (2010) from Mentorship Categories page fairness FAIRNE SSfairn welcome home
 Challenge and support Working in partnership The mentor role is crucial in facilitating and guiding what otherwise might become introspective accounts of practice. In order to support such adult style learning, mentors are seen as needing to facilitate a climate that supports student’s personal growth. Mentor Toolkit This often depends on mentors’ qualities in providing opportunities that might challenge the resourcefulness of students, whilst at the same time making sure they are well supported and supervised. Trust, confidentiality and imagining novel solutions, characterise a mentor/student relationship that permits honest reflection in the messiness of practice, prompting students to actively engage in ‘live’ reflection and supervision with mentors. The degree of challenge and support between mentors and students has the potential therefore, to open up the learning experience as ‘a place of possibility’ (Gillespie 2005). This also depends on mentors being able to acknowledge and be comfortable about their own imperfections in becoming facilitators of learning as opposed to simply handing over expertise to students. Focus References Download copy of RCN toolkit (2007) from Mentorship Categories page fairness FAIRNE SSfairn welcome home
Challenge and support Working in partnership The mentor role is crucial in facilitating and guiding what otherwise might become introspective accounts of practice. In order to support such adult style learning, mentors are seen as needing to facilitate a climate that supports student’s personal growth. Mentor Toolkit This often depends on mentors’ qualities in providing opportunities that might challenge the resourcefulness of students, whilst at the same time making sure they are well supported and supervised. Trust, confidentiality and imagining novel solutions, characterise a mentor/student relationship that permits honest reflection in the messiness of practice, prompting students to actively engage in ‘live’ reflection and supervision with mentors. The degree of challenge and support between mentors and students has the potential therefore, to open up the learning experience as ‘a place of possibility’ (Gillespie 2005). This also depends on mentors being able to acknowledge and be comfortable about their own imperfections in becoming facilitators of learning as opposed to simply handing over expertise to students. Focus References Download copy of RCN toolkit (2007) from Mentorship Categories page fairness FAIRNE SSfairn welcome home
 Accountability and risk taking Working in partnership Nurses have a duty to teach and mentor others whilst also being accountable for their assessment decisions. Yet there have been some concerns that mentors are ‘failing to fail’ students. Competence has become especially significant to the achievement of clinical learning outcomes, as 50% of the current Fitness for Practice pre-registration nursing curriculum is now determined by mentors (UKCC 1999). From 2007, Nursing and Midwifery Council standards for placement learning have been further strengthened with an expectation that mentors will have developed their knowledge, skills and competence beyond registration in order to make credible decisions about the proficiency of students. ‘Sign-off’ mentors’ have been introduced who have ‘clinical currency and capability’ in their area of practice as well as an ‘in-depth understanding’ of their accountability for assessment decisions). Accountability and risk taking There a number of conflicts for students and mentors to negotiate therefore, not least in maintaining a fair and transparent assessment process. Focus Links: Ø Failing students NMC News Summary Mentors’ voices fairness FAIRNE SSfairn welcome home
Accountability and risk taking Working in partnership Nurses have a duty to teach and mentor others whilst also being accountable for their assessment decisions. Yet there have been some concerns that mentors are ‘failing to fail’ students. Competence has become especially significant to the achievement of clinical learning outcomes, as 50% of the current Fitness for Practice pre-registration nursing curriculum is now determined by mentors (UKCC 1999). From 2007, Nursing and Midwifery Council standards for placement learning have been further strengthened with an expectation that mentors will have developed their knowledge, skills and competence beyond registration in order to make credible decisions about the proficiency of students. ‘Sign-off’ mentors’ have been introduced who have ‘clinical currency and capability’ in their area of practice as well as an ‘in-depth understanding’ of their accountability for assessment decisions). Accountability and risk taking There a number of conflicts for students and mentors to negotiate therefore, not least in maintaining a fair and transparent assessment process. Focus Links: Ø Failing students NMC News Summary Mentors’ voices fairness FAIRNE SSfairn welcome home
 Credible assessment Working in partnership fairness fa. FAIRNESS fairness FAIRNESSai Nurses have struggled with the question whether it might be enough simply to have a ‘good heart’ to be a nurse. Yet clinical competence involves a sophisticated combination of theoretical knowledge, practical skill and humanistic endeavour. So how do mentors reach credible conclusions about students’ proficiency in clinical practice given the misgivings about failing to fail students (Duffy 2004)? The NMC have consulted on and published new standards for pre-registration nurse education 2010 detailing generic and field competences student nurses need to achieve. In part, credible assessment depends on mentors demonstrating a breadth of understanding of assessment strategies including ‘Clinical Practice Outcomes’ documentation and ‘Clinical Practice Assessment Criteria’ for each year of student training. Mentors’ documented assessment evidence needs to stand up to scrutiny. Credible assessment Links: Practice learning flow chart Equally importantly perhaps mentor/student relationships achieve the greatest credibility when student learning is situated in a holistic context of care, involving patients’ experiences and facilitated by reflective and inclusive mentors (Freshwater and Stickley 2004; Midgley 2005; Van Eps et al. 2006). In so doing, students’ learning experiences can become enriched by concentrating on the interrelatedness of knowledge, skills and attitudes. Focus The way students are included both ‘personally’ and ‘professionally’ into clinical teams during placements as well as the link between clinical practice, the University and assessment is vital therefore (Cope 2000). fairness FAIRNE SSfairn welcome home
Credible assessment Working in partnership fairness fa. FAIRNESS fairness FAIRNESSai Nurses have struggled with the question whether it might be enough simply to have a ‘good heart’ to be a nurse. Yet clinical competence involves a sophisticated combination of theoretical knowledge, practical skill and humanistic endeavour. So how do mentors reach credible conclusions about students’ proficiency in clinical practice given the misgivings about failing to fail students (Duffy 2004)? The NMC have consulted on and published new standards for pre-registration nurse education 2010 detailing generic and field competences student nurses need to achieve. In part, credible assessment depends on mentors demonstrating a breadth of understanding of assessment strategies including ‘Clinical Practice Outcomes’ documentation and ‘Clinical Practice Assessment Criteria’ for each year of student training. Mentors’ documented assessment evidence needs to stand up to scrutiny. Credible assessment Links: Practice learning flow chart Equally importantly perhaps mentor/student relationships achieve the greatest credibility when student learning is situated in a holistic context of care, involving patients’ experiences and facilitated by reflective and inclusive mentors (Freshwater and Stickley 2004; Midgley 2005; Van Eps et al. 2006). In so doing, students’ learning experiences can become enriched by concentrating on the interrelatedness of knowledge, skills and attitudes. Focus The way students are included both ‘personally’ and ‘professionally’ into clinical teams during placements as well as the link between clinical practice, the University and assessment is vital therefore (Cope 2000). fairness FAIRNE SSfairn welcome home
 Nurse education Working in partnership 1980’s Traditional training Up until the 1990’s nurse training was carried out within schools of nursing linked to hospitals. If you had been accepted to train as a nurse and lived in Bridgend for example, you would have been part of the Mid Glamorgan School of nursing. For adult nursing you would have received the taught part of your training at Quarella Rd nursing school Bridgend and most of your clinical experiences would have been within Bridgend General Hospital. Student nurses had four ‘one off’ assessments during their training including managing a shift, demonstrating total patient care, administering medication and performing an aseptic technique. Students would spend 12 weeks on a hospital ward and two weeks in the school of nursing. An emphasis was placed on clinical knowledge of disease and basic skills, hygiene and sterile technique as well as the safety and psychological comfort of patients. continue back home
Nurse education Working in partnership 1980’s Traditional training Up until the 1990’s nurse training was carried out within schools of nursing linked to hospitals. If you had been accepted to train as a nurse and lived in Bridgend for example, you would have been part of the Mid Glamorgan School of nursing. For adult nursing you would have received the taught part of your training at Quarella Rd nursing school Bridgend and most of your clinical experiences would have been within Bridgend General Hospital. Student nurses had four ‘one off’ assessments during their training including managing a shift, demonstrating total patient care, administering medication and performing an aseptic technique. Students would spend 12 weeks on a hospital ward and two weeks in the school of nursing. An emphasis was placed on clinical knowledge of disease and basic skills, hygiene and sterile technique as well as the safety and psychological comfort of patients. continue back home
 Challenge and support Working in partnership 1990’s Project 2000 In 1992 nurse training became associated with Higher Education Institutes rather than hospital based nursing schools. University affiliation and academic status were seen as strengthening the claim that nursing needed to become a ‘profession’ as well as a vocation. The new project 2000 curriculum had a common eighteen month foundation programme after which students would choose general nursing, children’s nursing mental health or learning disabilities training to complete their three year programme. Theoretical work was supplemented by practical experiences in a wide range of clinical settings. The expansion in community services also influenced the way training was developing. Nurse education explored ideas such as the process of daily living, the role of the nurse and the importance of self-awareness. Reflective practice became a central theme which extended into Post Registration Education and Practice (PREP) where nurses were and continue to be encouraged to keep a portfolio of their professional lives. By 1995 if you had been accepted for nurse training you would have received theoretical training in a University setting and had student status. You would have had a funding bursary and become supernumerary to the numbers in your clinical placements. continue back home
Challenge and support Working in partnership 1990’s Project 2000 In 1992 nurse training became associated with Higher Education Institutes rather than hospital based nursing schools. University affiliation and academic status were seen as strengthening the claim that nursing needed to become a ‘profession’ as well as a vocation. The new project 2000 curriculum had a common eighteen month foundation programme after which students would choose general nursing, children’s nursing mental health or learning disabilities training to complete their three year programme. Theoretical work was supplemented by practical experiences in a wide range of clinical settings. The expansion in community services also influenced the way training was developing. Nurse education explored ideas such as the process of daily living, the role of the nurse and the importance of self-awareness. Reflective practice became a central theme which extended into Post Registration Education and Practice (PREP) where nurses were and continue to be encouraged to keep a portfolio of their professional lives. By 1995 if you had been accepted for nurse training you would have received theoretical training in a University setting and had student status. You would have had a funding bursary and become supernumerary to the numbers in your clinical placements. continue back home
 Nurse education Working in partnership 2002 -present Fitness for Practice In 1999 the United Kingdom Central Council for Nursing, Midwifery and Health Visiting (now the Nursing and Midwifery Council) published a report about nurse training called ‘Fitness for Practice. ’ The report, chaired by Sir Leonard Peach, followed wide ranging discussion with many relevant groups including education and clinical representatives. The report made 33 recommendations, attempting to encourage ‘proficiency’ by enabling students to apply knowledge, understanding and skills in the safe delivery of care and to make the transition from student to registered nurse. In Wales, representatives from nursing and Higher Education Institutions considered the recommendations contained in the Fitness for Practice report on an all Wales basis. As a result each Higher Education Institute and NHS Trust in Wales are part of the All Wales Initiative. Because of this initiative nursing courses are run in very similar ways whether students embark on nurse training in the University of Glamorgan or the University of Bangor. The first students to experience the Fitness for Practice pre-registration programme qualified in March 2005. Students are now assessed on a continual basis throughout their training involving 50% theory and 50% practice. In order to progress to each successive year, students need to achieve all relevant academic work as well as practice outcomes assessed in clinical placements. They are also expected to complete a comprehensive personal portfolio detailing their progress. During the first year all students gain experience on a medical ward as well as experience of each of the four branch programmes. Importantly this includes experience of all branches of nursing (midwifery, child, mental health and learning disability services). back home
Nurse education Working in partnership 2002 -present Fitness for Practice In 1999 the United Kingdom Central Council for Nursing, Midwifery and Health Visiting (now the Nursing and Midwifery Council) published a report about nurse training called ‘Fitness for Practice. ’ The report, chaired by Sir Leonard Peach, followed wide ranging discussion with many relevant groups including education and clinical representatives. The report made 33 recommendations, attempting to encourage ‘proficiency’ by enabling students to apply knowledge, understanding and skills in the safe delivery of care and to make the transition from student to registered nurse. In Wales, representatives from nursing and Higher Education Institutions considered the recommendations contained in the Fitness for Practice report on an all Wales basis. As a result each Higher Education Institute and NHS Trust in Wales are part of the All Wales Initiative. Because of this initiative nursing courses are run in very similar ways whether students embark on nurse training in the University of Glamorgan or the University of Bangor. The first students to experience the Fitness for Practice pre-registration programme qualified in March 2005. Students are now assessed on a continual basis throughout their training involving 50% theory and 50% practice. In order to progress to each successive year, students need to achieve all relevant academic work as well as practice outcomes assessed in clinical placements. They are also expected to complete a comprehensive personal portfolio detailing their progress. During the first year all students gain experience on a medical ward as well as experience of each of the four branch programmes. Importantly this includes experience of all branches of nursing (midwifery, child, mental health and learning disability services). back home
 Standards and learning Working in partnership 2. 1. 1 Criteria for supporting learning and assessing in practice – mentors Registrants who intend to take on the role of mentor will be assessing that students have achieved NMC competencies/proficiency. They must fulfil the following criteria: Be registered in the same part or sub-part of the register as the student they are to assess and for the nurses’ part of the register be in the same field of practice (adult, mental health, learning disability or children’s). Have developed their own knowledge, skills and competence beyond registration i. e. been registered for at least one year. Have successfully completed an NMC approved mentor preparation programme (or a comparable programme which has been accredited by an AEI as meeting the NMC mentor requirements). Have the ability to select, support and assess a range of learning opportunities in their area of practice for students undertaking NMC approved programmes. Be able to support learning in an interprofessional environment – selecting and supporting a range of learning opportunities for students from other professions. Have the ability to contribute to the assessment of other professionals under the supervision of an experienced assessor from that profession Be able to make judgements about competence/proficiency of NMC students on the same part of the register, and in the same field of practice, and be accountable for such decisions. Be able to support other registrants in meeting CPD needs in accordance with The NMC code of professional conduct: standards for conduct, ethics and performance. back home
Standards and learning Working in partnership 2. 1. 1 Criteria for supporting learning and assessing in practice – mentors Registrants who intend to take on the role of mentor will be assessing that students have achieved NMC competencies/proficiency. They must fulfil the following criteria: Be registered in the same part or sub-part of the register as the student they are to assess and for the nurses’ part of the register be in the same field of practice (adult, mental health, learning disability or children’s). Have developed their own knowledge, skills and competence beyond registration i. e. been registered for at least one year. Have successfully completed an NMC approved mentor preparation programme (or a comparable programme which has been accredited by an AEI as meeting the NMC mentor requirements). Have the ability to select, support and assess a range of learning opportunities in their area of practice for students undertaking NMC approved programmes. Be able to support learning in an interprofessional environment – selecting and supporting a range of learning opportunities for students from other professions. Have the ability to contribute to the assessment of other professionals under the supervision of an experienced assessor from that profession Be able to make judgements about competence/proficiency of NMC students on the same part of the register, and in the same field of practice, and be accountable for such decisions. Be able to support other registrants in meeting CPD needs in accordance with The NMC code of professional conduct: standards for conduct, ethics and performance. back home
 Standards and learning Working in partnership Review and maintenance of mentor/practice teacher qualifications Mentors or practice teachers must demonstrate their knowledge, skills and competence on an ongoing basis. Placement providers must ensure that: Each mentor and practice teacher is reviewed every three years (triennial review) to ensure that only those who continue to meet the mentor/practice teacher requirements remain on the local register. Mentors who meet the criteria for signing-off proficiency in practice at the end of a programme are annotated on the local register. Practice teachers and midwife mentors will automatically be assigned this level of responsibility at the end of their preparation programme. Arrangements are in place for appraising mentor/practice teacher performance, addressing concern where appropriate, and for adding and removing individuals from the local register including mentors identified as having met the criteria to be able to sign-off proficiency. Triennial review of mentor and practice teacher The nature of the triennial review of mentors and practice teachers is for the placement providers to determine but may form part of an employer-led personal development appraisal. To be maintained on the local register the individual must have evidence of having: Mentored at least two students (practice teachers to supervise at least one student) with due regard (extenuating circumstances permitting) within the three year period. Participated in annual updating – to include an opportunity to meet and explore assessment and supervision issues with other mentors/practice teachers. Explored as a group activity the validity and reliability of judgements made when assessing practice in challenging circumstances. Mapped ongoing development in their role against the current NMC mentor/practice teacher standards. back home
Standards and learning Working in partnership Review and maintenance of mentor/practice teacher qualifications Mentors or practice teachers must demonstrate their knowledge, skills and competence on an ongoing basis. Placement providers must ensure that: Each mentor and practice teacher is reviewed every three years (triennial review) to ensure that only those who continue to meet the mentor/practice teacher requirements remain on the local register. Mentors who meet the criteria for signing-off proficiency in practice at the end of a programme are annotated on the local register. Practice teachers and midwife mentors will automatically be assigned this level of responsibility at the end of their preparation programme. Arrangements are in place for appraising mentor/practice teacher performance, addressing concern where appropriate, and for adding and removing individuals from the local register including mentors identified as having met the criteria to be able to sign-off proficiency. Triennial review of mentor and practice teacher The nature of the triennial review of mentors and practice teachers is for the placement providers to determine but may form part of an employer-led personal development appraisal. To be maintained on the local register the individual must have evidence of having: Mentored at least two students (practice teachers to supervise at least one student) with due regard (extenuating circumstances permitting) within the three year period. Participated in annual updating – to include an opportunity to meet and explore assessment and supervision issues with other mentors/practice teachers. Explored as a group activity the validity and reliability of judgements made when assessing practice in challenging circumstances. Mapped ongoing development in their role against the current NMC mentor/practice teacher standards. back home
 Sign-off mentor criteria Working in partnership Paragraph 2. 1. 3 Criteria for a sign-off mentor Criteria for sign-off mentors in the Standards are underpinned by principle A which states that: The NMC registrants who make judgements about whether a student has achieved the required standards of proficiency for safe and effective practice must be on the same part or sub-part of the register as those which the student is intending to enter. Only sign-off mentors and practice teachers that are on the same part of the register and in the same field of practice may confirm to the NMC that students have met the relevant standards of proficiency for the particular programme leading to registration or a qualification that is recordable on the NMC register. Placement providers must ensure that a registrant designated to sign-off proficiency for a particular student at the end of a programme is: Identified on the local register as a sign-off mentor or a practice teacher. Registered on the same part of the register. Working in the same field of practice as that in which the student intends to qualify. And additionally to be a sign-off mentor that they have: Clinical currency and capability in the field of practice in which the student is being assessed. Met the NMC requirements to remain on the local register. Been supervised on at least three occasions for signing off proficiency at the end of a final placement (or supervised practice placement) by an existing sign-off mentor or practice teacher. A working knowledge of current programme requirements, practice assessment strategies and relevant changes in education and practice for the student they are assessing. An understanding of the NMC registration requirements and the contribution they make to meeting these requirements. An in-depth understanding of their accountability to the NMC for the decision they make to pass or fail a student when assessing proficiency requirements at the end of a programme. back home
Sign-off mentor criteria Working in partnership Paragraph 2. 1. 3 Criteria for a sign-off mentor Criteria for sign-off mentors in the Standards are underpinned by principle A which states that: The NMC registrants who make judgements about whether a student has achieved the required standards of proficiency for safe and effective practice must be on the same part or sub-part of the register as those which the student is intending to enter. Only sign-off mentors and practice teachers that are on the same part of the register and in the same field of practice may confirm to the NMC that students have met the relevant standards of proficiency for the particular programme leading to registration or a qualification that is recordable on the NMC register. Placement providers must ensure that a registrant designated to sign-off proficiency for a particular student at the end of a programme is: Identified on the local register as a sign-off mentor or a practice teacher. Registered on the same part of the register. Working in the same field of practice as that in which the student intends to qualify. And additionally to be a sign-off mentor that they have: Clinical currency and capability in the field of practice in which the student is being assessed. Met the NMC requirements to remain on the local register. Been supervised on at least three occasions for signing off proficiency at the end of a final placement (or supervised practice placement) by an existing sign-off mentor or practice teacher. A working knowledge of current programme requirements, practice assessment strategies and relevant changes in education and practice for the student they are assessing. An understanding of the NMC registration requirements and the contribution they make to meeting these requirements. An in-depth understanding of their accountability to the NMC for the decision they make to pass or fail a student when assessing proficiency requirements at the end of a programme. back home
 Standards and learning Working in partnership Signing off practice proficiency In order to ensure public protection the NMC needs to be assured that students have been assessed and signed off as capable of safe and effective practice at the end of a programme. Additional criteria have been defined for the mentor to be able to sign-off proficiency in practice at the end of a programme paragraph 2. 1. 3). ( Placement providers will determine when a mentor has met the additional criteria and will be annotated as a sign-off mentor on the local register. The NMC statutory midwifery committee has decided that all midwife mentors must have met the additional criteria to be sign-off mentors. Confirmation of proficiency (Paragraph 3. 2. 6). The sign-off mentor, who has met the NMC additional criteria for assessing proficiency, is responsible and accountable for making the final sign-off in practice – confirming that a student has successfully completed all practice requirements. This confirmation will contribute to the portfolio of evidence considered by the Higher Education Institute’s examination or assessment board. The NMC requires mentors who have not yet met the additional criteria to be supported by a sign-off mentor or a practice teacher if it is the student’s final placement, or when failing a student. NMC requirements Advice and guidance Mentors should seek advice and guidance from a sign-off mentor or a practice teacher when dealing with failing students. Inexperienced mentors may require support from a signoff mentor or practice teacher when faced with a failing student to help them to communicate concerns, identify action and evaluate progress. back home
Standards and learning Working in partnership Signing off practice proficiency In order to ensure public protection the NMC needs to be assured that students have been assessed and signed off as capable of safe and effective practice at the end of a programme. Additional criteria have been defined for the mentor to be able to sign-off proficiency in practice at the end of a programme paragraph 2. 1. 3). ( Placement providers will determine when a mentor has met the additional criteria and will be annotated as a sign-off mentor on the local register. The NMC statutory midwifery committee has decided that all midwife mentors must have met the additional criteria to be sign-off mentors. Confirmation of proficiency (Paragraph 3. 2. 6). The sign-off mentor, who has met the NMC additional criteria for assessing proficiency, is responsible and accountable for making the final sign-off in practice – confirming that a student has successfully completed all practice requirements. This confirmation will contribute to the portfolio of evidence considered by the Higher Education Institute’s examination or assessment board. The NMC requires mentors who have not yet met the additional criteria to be supported by a sign-off mentor or a practice teacher if it is the student’s final placement, or when failing a student. NMC requirements Advice and guidance Mentors should seek advice and guidance from a sign-off mentor or a practice teacher when dealing with failing students. Inexperienced mentors may require support from a signoff mentor or practice teacher when faced with a failing student to help them to communicate concerns, identify action and evaluate progress. back home
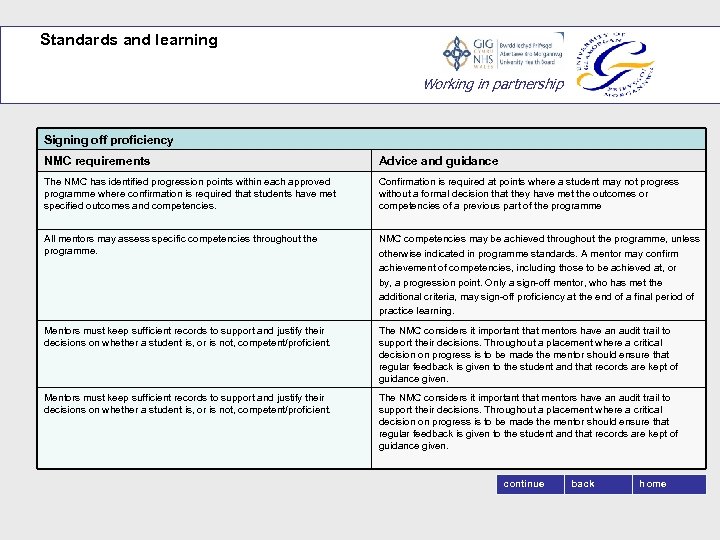 Standards and learning Working in partnership Signing off proficiency NMC requirements Advice and guidance The NMC has identified progression points within each approved programme where confirmation is required that students have met specified outcomes and competencies. Confirmation is required at points where a student may not progress without a formal decision that they have met the outcomes or competencies of a previous part of the programme All mentors may assess specific competencies throughout the programme. NMC competencies may be achieved throughout the programme, unless otherwise indicated in programme standards. A mentor may confirm achievement of competencies, including those to be achieved at, or by, a progression point. Only a sign-off mentor, who has met the additional criteria, may sign-off proficiency at the end of a final period of practice learning. Mentors must keep sufficient records to support and justify their decisions on whether a student is, or is not, competent/proficient. The NMC considers it important that mentors have an audit trail to support their decisions. Throughout a placement where a critical decision on progress is to be made the mentor should ensure that regular feedback is given to the student and that records are kept of guidance given. continue back home
Standards and learning Working in partnership Signing off proficiency NMC requirements Advice and guidance The NMC has identified progression points within each approved programme where confirmation is required that students have met specified outcomes and competencies. Confirmation is required at points where a student may not progress without a formal decision that they have met the outcomes or competencies of a previous part of the programme All mentors may assess specific competencies throughout the programme. NMC competencies may be achieved throughout the programme, unless otherwise indicated in programme standards. A mentor may confirm achievement of competencies, including those to be achieved at, or by, a progression point. Only a sign-off mentor, who has met the additional criteria, may sign-off proficiency at the end of a final period of practice learning. Mentors must keep sufficient records to support and justify their decisions on whether a student is, or is not, competent/proficient. The NMC considers it important that mentors have an audit trail to support their decisions. Throughout a placement where a critical decision on progress is to be made the mentor should ensure that regular feedback is given to the student and that records are kept of guidance given. continue back home
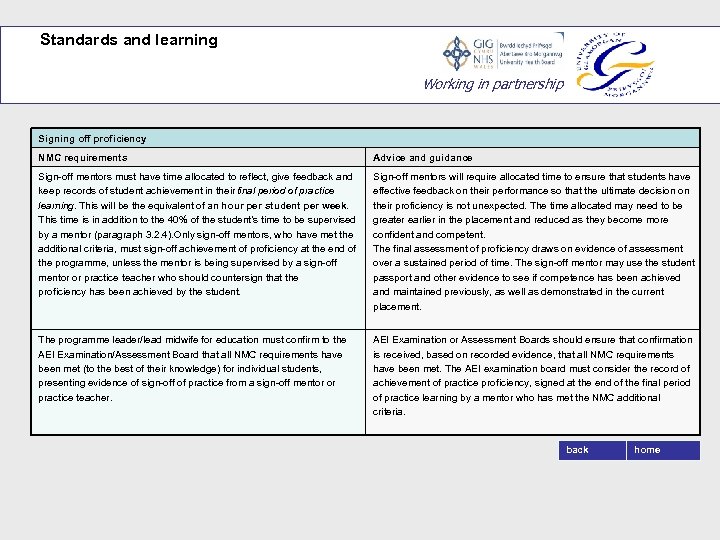 Standards and learning Working in partnership Signing off proficiency NMC requirements Advice and guidance Sign-off mentors must have time allocated to reflect, give feedback and keep records of student achievement in their final period of practice learning. This will be the equivalent of an hour per student per week. This time is in addition to the 40% of the student’s time to be supervised by a mentor (paragraph 3. 2. 4). Only sign-off mentors, who have met the additional criteria, must sign-off achievement of proficiency at the end of the programme, unless the mentor is being supervised by a sign-off mentor or practice teacher who should countersign that the proficiency has been achieved by the student. Sign-off mentors will require allocated time to ensure that students have effective feedback on their performance so that the ultimate decision on their proficiency is not unexpected. The time allocated may need to be greater earlier in the placement and reduced as they become more confident and competent. The final assessment of proficiency draws on evidence of assessment over a sustained period of time. The sign-off mentor may use the student passport and other evidence to see if competence has been achieved and maintained previously, as well as demonstrated in the current placement. The programme leader/lead midwife for education must confirm to the AEI Examination/Assessment Board that all NMC requirements have been met (to the best of their knowledge) for individual students, presenting evidence of sign-off of practice from a sign-off mentor or practice teacher. AEI Examination or Assessment Boards should ensure that confirmation is received, based on recorded evidence, that all NMC requirements have been met. The AEI examination board must consider the record of achievement of practice proficiency, signed at the end of the final period of practice learning by a mentor who has met the NMC additional criteria. back home
Standards and learning Working in partnership Signing off proficiency NMC requirements Advice and guidance Sign-off mentors must have time allocated to reflect, give feedback and keep records of student achievement in their final period of practice learning. This will be the equivalent of an hour per student per week. This time is in addition to the 40% of the student’s time to be supervised by a mentor (paragraph 3. 2. 4). Only sign-off mentors, who have met the additional criteria, must sign-off achievement of proficiency at the end of the programme, unless the mentor is being supervised by a sign-off mentor or practice teacher who should countersign that the proficiency has been achieved by the student. Sign-off mentors will require allocated time to ensure that students have effective feedback on their performance so that the ultimate decision on their proficiency is not unexpected. The time allocated may need to be greater earlier in the placement and reduced as they become more confident and competent. The final assessment of proficiency draws on evidence of assessment over a sustained period of time. The sign-off mentor may use the student passport and other evidence to see if competence has been achieved and maintained previously, as well as demonstrated in the current placement. The programme leader/lead midwife for education must confirm to the AEI Examination/Assessment Board that all NMC requirements have been met (to the best of their knowledge) for individual students, presenting evidence of sign-off of practice from a sign-off mentor or practice teacher. AEI Examination or Assessment Boards should ensure that confirmation is received, based on recorded evidence, that all NMC requirements have been met. The AEI examination board must consider the record of achievement of practice proficiency, signed at the end of the final period of practice learning by a mentor who has met the NMC additional criteria. back home
 Standards and learning Working in partnership Competence and outcomes for a mentor Page 1 of 2 Mentor competencies are achieved by successful completion of an NMC approved mentor preparation programme that achieves all of the outcomes of stage 2. These outcomes are as follows: 1. Establishing effective working relationships • Develop effective working relationships based on mutual trust and respect. • Demonstrate an understanding of factors that influence how students integrate into practice settings. • Provide ongoing and constructive support to facilitate transition from one learning environment to another. 2. Facilitation of learning • Use knowledge of the student’s stage of learning to select appropriate learning opportunities to meet their individual needs. • Facilitate selection of appropriate learning strategies to integrate learning from practice and academic experiences. • Support students in critically reflecting upon their learning experiences in order to enhance future learning. 3. Assessment and accountability • Foster professional growth, personal development and accountability through support of students in practice. • Demonstrate a breadth of understanding of assessment strategies and the ability to contribute to the total assessment process as part of the teaching team. • Provide constructive feedback to students and assist them in identifying future learning needs and actions. • Manage failing students so that they may either enhance their performance and capabilities for safe and effective practice or be able to understand their failure and the implications of this for their future. • Be accountable for confirming that students have met, or not met, the NMC competencies in practice. As a sign-off mentor confirm that students have met, or not met, the NMC standards of proficiency in practice and are capable of safe and effective practice. 4. Evaluation of learning • Contribute to evaluation of student learning and assessment experience proposing aspects for change as a result of such evaluation. • Participate in self and peer evaluation to facilitate personal development, and contribute to the development of others. continue back home
Standards and learning Working in partnership Competence and outcomes for a mentor Page 1 of 2 Mentor competencies are achieved by successful completion of an NMC approved mentor preparation programme that achieves all of the outcomes of stage 2. These outcomes are as follows: 1. Establishing effective working relationships • Develop effective working relationships based on mutual trust and respect. • Demonstrate an understanding of factors that influence how students integrate into practice settings. • Provide ongoing and constructive support to facilitate transition from one learning environment to another. 2. Facilitation of learning • Use knowledge of the student’s stage of learning to select appropriate learning opportunities to meet their individual needs. • Facilitate selection of appropriate learning strategies to integrate learning from practice and academic experiences. • Support students in critically reflecting upon their learning experiences in order to enhance future learning. 3. Assessment and accountability • Foster professional growth, personal development and accountability through support of students in practice. • Demonstrate a breadth of understanding of assessment strategies and the ability to contribute to the total assessment process as part of the teaching team. • Provide constructive feedback to students and assist them in identifying future learning needs and actions. • Manage failing students so that they may either enhance their performance and capabilities for safe and effective practice or be able to understand their failure and the implications of this for their future. • Be accountable for confirming that students have met, or not met, the NMC competencies in practice. As a sign-off mentor confirm that students have met, or not met, the NMC standards of proficiency in practice and are capable of safe and effective practice. 4. Evaluation of learning • Contribute to evaluation of student learning and assessment experience proposing aspects for change as a result of such evaluation. • Participate in self and peer evaluation to facilitate personal development, and contribute to the development of others. continue back home
 Standards and learning Working in partnership Competence and outcomes for a mentor Page 2 5. Creating an environment for learning • Support students to identify both learning needs and experiences that are appropriate to their level of learning. • Use a range of learning experiences, involving patients, clients, carers and the professional team, to meet defined learning needs. • Identify aspects of the learning environment which could be enhanced – negotiating with others to make appropriate changes. • Act as a resource to facilitate personal and professional development of others. 6. Context of practice • Contribute to the development of an environment in which effective practice is fostered, implemented, evaluated and disseminated. • Set and maintain professional boundaries that are sufficiently flexible for providing interprofessional care. • Initiate and respond to practice developments to ensure safe and effective care is achieved an effective learning environment is maintained. 7. Evidence-based practice • Identify and apply research and evidence-based practice to their area of practice. • Contribute to strategies to increase or review the evidence-base used to support practice. • Support students in applying an evidence base to their own practice. 8. Leadership • Plan a series of learning experiences that will meet students defined learning needs. • Be an advocate for students to support them accessing learning opportunities that meet their individual needs – involving a range of other professionals, patients, clients and carers. • Prioritise work to accommodate support of students within their practice roles. • Provide feedback about the effectiveness of learning and assessment in practice. back home
Standards and learning Working in partnership Competence and outcomes for a mentor Page 2 5. Creating an environment for learning • Support students to identify both learning needs and experiences that are appropriate to their level of learning. • Use a range of learning experiences, involving patients, clients, carers and the professional team, to meet defined learning needs. • Identify aspects of the learning environment which could be enhanced – negotiating with others to make appropriate changes. • Act as a resource to facilitate personal and professional development of others. 6. Context of practice • Contribute to the development of an environment in which effective practice is fostered, implemented, evaluated and disseminated. • Set and maintain professional boundaries that are sufficiently flexible for providing interprofessional care. • Initiate and respond to practice developments to ensure safe and effective care is achieved an effective learning environment is maintained. 7. Evidence-based practice • Identify and apply research and evidence-based practice to their area of practice. • Contribute to strategies to increase or review the evidence-base used to support practice. • Support students in applying an evidence base to their own practice. 8. Leadership • Plan a series of learning experiences that will meet students defined learning needs. • Be an advocate for students to support them accessing learning opportunities that meet their individual needs – involving a range of other professionals, patients, clients and carers. • Prioritise work to accommodate support of students within their practice roles. • Provide feedback about the effectiveness of learning and assessment in practice. back home
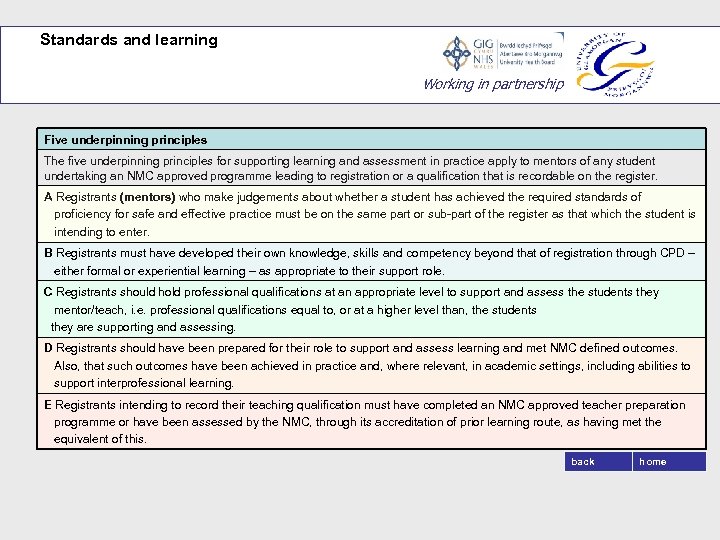 Standards and learning Working in partnership Five underpinning principles The five underpinning principles for supporting learning and assessment in practice apply to mentors of any student undertaking an NMC approved programme leading to registration or a qualification that is recordable on the register. A Registrants (mentors) who make judgements about whether a student has achieved the required standards of proficiency for safe and effective practice must be on the same part or sub-part of the register as that which the student is intending to enter. B Registrants must have developed their own knowledge, skills and competency beyond that of registration through CPD – either formal or experiential learning – as appropriate to their support role. C Registrants should hold professional qualifications at an appropriate level to support and assess the students they mentor/teach, i. e. professional qualifications equal to, or at a higher level than, the students they are supporting and assessing. D Registrants should have been prepared for their role to support and assess learning and met NMC defined outcomes. Also, that such outcomes have been achieved in practice and, where relevant, in academic settings, including abilities to support interprofessional learning. E Registrants intending to record their teaching qualification must have completed an NMC approved teacher preparation programme or have been assessed by the NMC, through its accreditation of prior learning route, as having met the equivalent of this. back home
Standards and learning Working in partnership Five underpinning principles The five underpinning principles for supporting learning and assessment in practice apply to mentors of any student undertaking an NMC approved programme leading to registration or a qualification that is recordable on the register. A Registrants (mentors) who make judgements about whether a student has achieved the required standards of proficiency for safe and effective practice must be on the same part or sub-part of the register as that which the student is intending to enter. B Registrants must have developed their own knowledge, skills and competency beyond that of registration through CPD – either formal or experiential learning – as appropriate to their support role. C Registrants should hold professional qualifications at an appropriate level to support and assess the students they mentor/teach, i. e. professional qualifications equal to, or at a higher level than, the students they are supporting and assessing. D Registrants should have been prepared for their role to support and assess learning and met NMC defined outcomes. Also, that such outcomes have been achieved in practice and, where relevant, in academic settings, including abilities to support interprofessional learning. E Registrants intending to record their teaching qualification must have completed an NMC approved teacher preparation programme or have been assessed by the NMC, through its accreditation of prior learning route, as having met the equivalent of this. back home
 Adult learning Working in partnership Encouraging patients to make informed decisions, the development of person-centred planning systems and a holistic approach to health promotion, have become central goals within humanistic health care (Siddell et al 2003; Priest and Gibbs 2004). These philosophical changes have been mirrored in nurse education, notably influenced by humanistic psychology (Rogers 1969, Mezirow 1981) with adult style learning founded in self direction, creativity and personal discovery. Students are viewed as autonomous individuals taking responsibility for their own ongoing learning (Knowles 1984). In this sense, the process of learning becomes worthy of examination as much as learning as an end product. (Morton-Cooper and Palmer (2000). Perhaps the value of this learning is in the balance between students’ personal reflections and engaging in a critical dialogue with mentors? back home
Adult learning Working in partnership Encouraging patients to make informed decisions, the development of person-centred planning systems and a holistic approach to health promotion, have become central goals within humanistic health care (Siddell et al 2003; Priest and Gibbs 2004). These philosophical changes have been mirrored in nurse education, notably influenced by humanistic psychology (Rogers 1969, Mezirow 1981) with adult style learning founded in self direction, creativity and personal discovery. Students are viewed as autonomous individuals taking responsibility for their own ongoing learning (Knowles 1984). In this sense, the process of learning becomes worthy of examination as much as learning as an end product. (Morton-Cooper and Palmer (2000). Perhaps the value of this learning is in the balance between students’ personal reflections and engaging in a critical dialogue with mentors? back home
 Mentor qualities Working in partnership Despite the pressures mentors may face there is reassuring evidence that mentors are enthusiastic to work with students and keen to support a learning culture within clinical settings (Gillespie 2005). Landmark et al. ’s (2003) focus group interviews with mentors highlight the benefits of shared learning within student/mentor relationships including increased self-confidence, achieving personal learning goals and a deepening understanding of nursing. Establishing a dialogue with students Just as people with blue eyes will each have a different coloured hue, people will experience learning situations in a very individual way. Positive mentor attributes have been identified as professionalism, expert knowledge, good communication skills and the motivation to teach and support students (Neary 2000). Key elements of the role are seen as including teaching, support and assessment of student performance. Darling (1984) identified other aspects of an effective mentor as ‘inspirer, ’ ‘investor’ and ‘supporter’ as well as being a role model, energizer, door-opener, idea bouncer, challenger, problem-solver and career counsellor. Effective mentorship is also seen as identifying every opportunity to create and maximize learning opportunities. Yet being an effective mentor has a number of challenges particularly in allocating time to students given the busyness of many clinical settings. There is a tightrope that mentors need to negotiate therefore between providing pastoral support and being a clinical assessor. back home
Mentor qualities Working in partnership Despite the pressures mentors may face there is reassuring evidence that mentors are enthusiastic to work with students and keen to support a learning culture within clinical settings (Gillespie 2005). Landmark et al. ’s (2003) focus group interviews with mentors highlight the benefits of shared learning within student/mentor relationships including increased self-confidence, achieving personal learning goals and a deepening understanding of nursing. Establishing a dialogue with students Just as people with blue eyes will each have a different coloured hue, people will experience learning situations in a very individual way. Positive mentor attributes have been identified as professionalism, expert knowledge, good communication skills and the motivation to teach and support students (Neary 2000). Key elements of the role are seen as including teaching, support and assessment of student performance. Darling (1984) identified other aspects of an effective mentor as ‘inspirer, ’ ‘investor’ and ‘supporter’ as well as being a role model, energizer, door-opener, idea bouncer, challenger, problem-solver and career counsellor. Effective mentorship is also seen as identifying every opportunity to create and maximize learning opportunities. Yet being an effective mentor has a number of challenges particularly in allocating time to students given the busyness of many clinical settings. There is a tightrope that mentors need to negotiate therefore between providing pastoral support and being a clinical assessor. back home
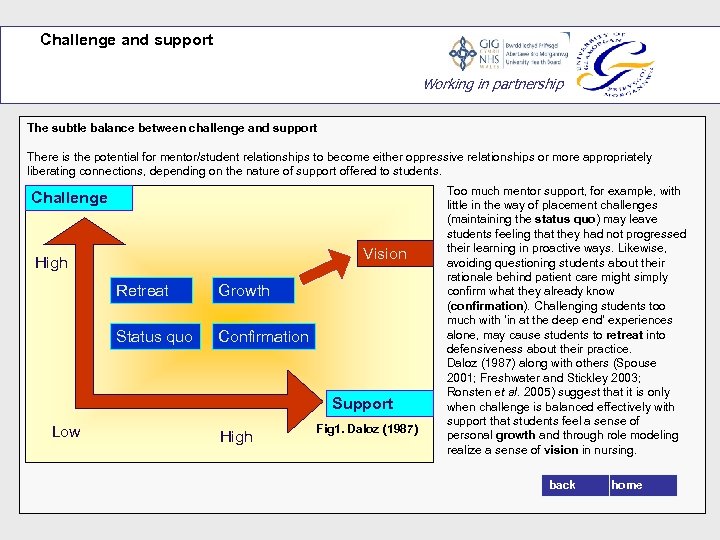 Challenge and support Working in partnership The subtle balance between challenge and support There is the potential for mentor/student relationships to become either oppressive relationships or more appropriately liberating connections, depending on the nature of support offered to students. Challenge Vision High Retreat Growth Status quo Confirmation Support Low High Fig 1. Daloz (1987) Too much mentor support, for example, with little in the way of placement challenges (maintaining the status quo) may leave students feeling that they had not progressed their learning in proactive ways. Likewise, avoiding questioning students about their rationale behind patient care might simply confirm what they already know (confirmation). Challenging students too much with ‘in at the deep end’ experiences alone, may cause students to retreat into defensiveness about their practice. Daloz (1987) along with others (Spouse 2001; Freshwater and Stickley 2003; Ronsten et al. 2005) suggest that it is only when challenge is balanced effectively with support that students feel a sense of personal growth and through role modeling realize a sense of vision in nursing. back home
Challenge and support Working in partnership The subtle balance between challenge and support There is the potential for mentor/student relationships to become either oppressive relationships or more appropriately liberating connections, depending on the nature of support offered to students. Challenge Vision High Retreat Growth Status quo Confirmation Support Low High Fig 1. Daloz (1987) Too much mentor support, for example, with little in the way of placement challenges (maintaining the status quo) may leave students feeling that they had not progressed their learning in proactive ways. Likewise, avoiding questioning students about their rationale behind patient care might simply confirm what they already know (confirmation). Challenging students too much with ‘in at the deep end’ experiences alone, may cause students to retreat into defensiveness about their practice. Daloz (1987) along with others (Spouse 2001; Freshwater and Stickley 2003; Ronsten et al. 2005) suggest that it is only when challenge is balanced effectively with support that students feel a sense of personal growth and through role modeling realize a sense of vision in nursing. back home
 NMC Press release 2004 Working in partnership Failing to fail students? ‘NMC funded research has strongly criticised nurse mentors for not failing students when they show a lack of clinical competence on placements. The report, entitled 'Failing Students', was written by Kathleen Duffy, a lecturer at Glasgow Caledonian University. The main findings of the report are that Mentors pass student nurses’ clinical assessments even when there are doubts about their performance. Weak students who often had a history of problems in clinical practice have been given the benefit of the doubt. The report also found that Mentors are too ready to allow failing students' personal problems to influence their judgements. The report says that mentors need to be prepared to fail students as well as to pass them. Duffy also calls for improved mentor preparation programmes and for further research into this area. She says that mentors should contact teaching staff with their concerns at an early stage and in writing. Failure to voice concerns in writing often means that no action is taken. The report also points out that responsibility for the problem also lies with lecturers. Kathleen Duffy said: "The research show that Mentors find it difficult to fail students. Preparing mentors for their role and responsibility in a fail scenario is vital and must be backed up with adequate support from both education and practice. " Janice Gosby, NMC professional advisor, said: "This report provides important insights into the reasons why students are not failed in practice and gives a number of recommendations that the Council may wish to implement. Mentors are accountable for their decisions on fitness for practice that enable entry to the register, and it is the quality of these decisions that protects the public from incompetent practitioners" back home
NMC Press release 2004 Working in partnership Failing to fail students? ‘NMC funded research has strongly criticised nurse mentors for not failing students when they show a lack of clinical competence on placements. The report, entitled 'Failing Students', was written by Kathleen Duffy, a lecturer at Glasgow Caledonian University. The main findings of the report are that Mentors pass student nurses’ clinical assessments even when there are doubts about their performance. Weak students who often had a history of problems in clinical practice have been given the benefit of the doubt. The report also found that Mentors are too ready to allow failing students' personal problems to influence their judgements. The report says that mentors need to be prepared to fail students as well as to pass them. Duffy also calls for improved mentor preparation programmes and for further research into this area. She says that mentors should contact teaching staff with their concerns at an early stage and in writing. Failure to voice concerns in writing often means that no action is taken. The report also points out that responsibility for the problem also lies with lecturers. Kathleen Duffy said: "The research show that Mentors find it difficult to fail students. Preparing mentors for their role and responsibility in a fail scenario is vital and must be backed up with adequate support from both education and practice. " Janice Gosby, NMC professional advisor, said: "This report provides important insights into the reasons why students are not failed in practice and gives a number of recommendations that the Council may wish to implement. Mentors are accountable for their decisions on fitness for practice that enable entry to the register, and it is the quality of these decisions that protects the public from incompetent practitioners" back home
 Frequently asked questions Working in partnership Frequently asked questions Q 1. Why should mentors assess students in practice? An assessment of student competence needs to be made at strategic points during their training. 50% is assessed through students’ academic work and 50% during their clinical practice placements. Mentors are best placed to assess competence in practice because of their close supervision of students. Ultimately this is about the safety of patients and the protection of the public. Q 2. What should I do if I feel uncertain of what is required of me as a mentor? Contact a Practice Facilitator in the Trust. They will discuss any concerns you may have or help you map out your training needs. Q 3. How often should students work with their mentor? Nursing and Midwifery Standards to support learning and assessment in practice advise students and mentors to spend at least 40% of placement time working together. In order for mentors to be effective role models and get to know the student well enough to make an accurate assessment of their performance mentors should work with students for the equivalent of 3 shifts a week. The amount of time however, needs to be balanced with a number of considerations both students and mentors may have including the: -Student’s level of competence and their need for support. -Need to get feedback from others about the student’s performance. -Multidisciplinary nature of the placement environment. Next question back home -Range of teaching and learning opportunities available.
Frequently asked questions Working in partnership Frequently asked questions Q 1. Why should mentors assess students in practice? An assessment of student competence needs to be made at strategic points during their training. 50% is assessed through students’ academic work and 50% during their clinical practice placements. Mentors are best placed to assess competence in practice because of their close supervision of students. Ultimately this is about the safety of patients and the protection of the public. Q 2. What should I do if I feel uncertain of what is required of me as a mentor? Contact a Practice Facilitator in the Trust. They will discuss any concerns you may have or help you map out your training needs. Q 3. How often should students work with their mentor? Nursing and Midwifery Standards to support learning and assessment in practice advise students and mentors to spend at least 40% of placement time working together. In order for mentors to be effective role models and get to know the student well enough to make an accurate assessment of their performance mentors should work with students for the equivalent of 3 shifts a week. The amount of time however, needs to be balanced with a number of considerations both students and mentors may have including the: -Student’s level of competence and their need for support. -Need to get feedback from others about the student’s performance. -Multidisciplinary nature of the placement environment. Next question back home -Range of teaching and learning opportunities available.
 Frequently asked questions Working in partnership Frequently asked questions Q 4. What can we do to make sure our team is ready to accept students? Check to see if your educational audit is current. The audit document will highlight how many students your team should have at any one time and at what stage of their training. The document also includes a range of Standard statements to measure yourselves against as a placement team. Contact a Practice Facilitator or Link Tutor from the University for any assistance with your educational audit. Q 5. What can I do to prepare for a student? As an individual mentor you can firstly make sure you feel comfortable about acting in this capacity by mapping yourself against the criteria for being a mentor. It is also good practice to check your rota for the duration of the student’s placement. If you know you are on annual leave for a proportion of the student’s allocation, make some arrangements with colleagues to cover this period. Collect some helpful documentation ready for the student on their first day. This will normally be contained within a Student nurse induction pack available within your clinical setting. Construct a loose timetable for the student. This might include particular clinics, teaching sessions or other learning opportunities occurring regularly in your clinical area which would be valuable for the student to experience. There is a balance of course as a mentor between enabling a student to experience a variety of learning opportunities yet ensuring they spend enough time with you for you to make a credible assessment of their competence. The RCN have produced a helpful checklist for mentors in preparation for students. Next question back home
Frequently asked questions Working in partnership Frequently asked questions Q 4. What can we do to make sure our team is ready to accept students? Check to see if your educational audit is current. The audit document will highlight how many students your team should have at any one time and at what stage of their training. The document also includes a range of Standard statements to measure yourselves against as a placement team. Contact a Practice Facilitator or Link Tutor from the University for any assistance with your educational audit. Q 5. What can I do to prepare for a student? As an individual mentor you can firstly make sure you feel comfortable about acting in this capacity by mapping yourself against the criteria for being a mentor. It is also good practice to check your rota for the duration of the student’s placement. If you know you are on annual leave for a proportion of the student’s allocation, make some arrangements with colleagues to cover this period. Collect some helpful documentation ready for the student on their first day. This will normally be contained within a Student nurse induction pack available within your clinical setting. Construct a loose timetable for the student. This might include particular clinics, teaching sessions or other learning opportunities occurring regularly in your clinical area which would be valuable for the student to experience. There is a balance of course as a mentor between enabling a student to experience a variety of learning opportunities yet ensuring they spend enough time with you for you to make a credible assessment of their competence. The RCN have produced a helpful checklist for mentors in preparation for students. Next question back home
 Frequently asked questions Working in partnership Frequently asked questions Q 6. What should I expect a student to have prepared prior to a placement? Before each placement students complete a Self-Assessment and Action Plan. These identify a student’s concerns and expectations about forthcoming placements as well as their individual strengths and weaknesses. As their mentor you can ask a student to share these reflections about themselves at the beginning of a placement. There may be particular skills or needs a student might have highlighted that they need to work on during the placement. Q 7. What should happen on the student’s first day in a placement? Make them feel welcome. A consistent theme from students’ evaluations of placements is the value of a warm welcome in setting the climate for effective learning. The way a student is introduced to team members, orientated to the environment of the clinical area, allocated their pattern of work and shown where they can change or leave personal belongings can go a long way to lessening any anxiety students’ may feel. Ideally the mentor and the student should set time aside on the first day (certainly within the first three days) to discuss their expectations for the placement. Next question back home
Frequently asked questions Working in partnership Frequently asked questions Q 6. What should I expect a student to have prepared prior to a placement? Before each placement students complete a Self-Assessment and Action Plan. These identify a student’s concerns and expectations about forthcoming placements as well as their individual strengths and weaknesses. As their mentor you can ask a student to share these reflections about themselves at the beginning of a placement. There may be particular skills or needs a student might have highlighted that they need to work on during the placement. Q 7. What should happen on the student’s first day in a placement? Make them feel welcome. A consistent theme from students’ evaluations of placements is the value of a warm welcome in setting the climate for effective learning. The way a student is introduced to team members, orientated to the environment of the clinical area, allocated their pattern of work and shown where they can change or leave personal belongings can go a long way to lessening any anxiety students’ may feel. Ideally the mentor and the student should set time aside on the first day (certainly within the first three days) to discuss their expectations for the placement. Next question back home
 Frequently asked questions Working in partnership Frequently asked questions Q 8. What do I do if there is a lack of co-operation from the student? Initially discuss this issue with the student. It may be that the reason for the student’s uncooperativeness is due to shyness or anxiety as much as it may be due to lack of interest or de-motivation. Once the motives for the lack of co-operation have been established an action plan can be developed with the student. Nevertheless, as the mentor you have a right to expect a student’s co-operation within your agreed learning plan. If this situation is not resolved within the placement by discussions with colleagues during the early stages of the placement you might want to contact a Practice Facilitator or the student’s personal tutor. Q 9. Are students accountable for their actions? Pre-registration students are not professionally accountable for their actions to the NMC. As far as the NMC are concerned it is the registered nurse working with the student who is professionally responsible for the consequences of any acts or omissions students might make. Students should only work within their level of understanding and competence and always under the supervision of a registered nurse. Students do need to be continually mindful of their professionalism however as the public will expect this of nurses. Students can be called to account by the University or by the law for the consequences of their acts or omissions as a pre-registration student. Next question back home
Frequently asked questions Working in partnership Frequently asked questions Q 8. What do I do if there is a lack of co-operation from the student? Initially discuss this issue with the student. It may be that the reason for the student’s uncooperativeness is due to shyness or anxiety as much as it may be due to lack of interest or de-motivation. Once the motives for the lack of co-operation have been established an action plan can be developed with the student. Nevertheless, as the mentor you have a right to expect a student’s co-operation within your agreed learning plan. If this situation is not resolved within the placement by discussions with colleagues during the early stages of the placement you might want to contact a Practice Facilitator or the student’s personal tutor. Q 9. Are students accountable for their actions? Pre-registration students are not professionally accountable for their actions to the NMC. As far as the NMC are concerned it is the registered nurse working with the student who is professionally responsible for the consequences of any acts or omissions students might make. Students should only work within their level of understanding and competence and always under the supervision of a registered nurse. Students do need to be continually mindful of their professionalism however as the public will expect this of nurses. Students can be called to account by the University or by the law for the consequences of their acts or omissions as a pre-registration student. Next question back home
 Frequently asked questions Working in partnership Frequently asked questions Q 10. What should I do if I have concerns about a student’s competence? Firstly discuss these concerns with the student. This might be sensitively discussed as part of the learning contract middle interview. Document your concerns. This is a good point to involve a Practice Facilitator. They can help set up an Action Plan to document students’ progress and meet with you and the student at regular intervals. The Practice Facilitator will also act as a bridge between your placement and key people in the University. Q 11. How can I celebrate a student’s exceptional performance? Each individual student should be recognised for their own personal skills and qualities. Whilst students can never be compared to one another (hence the ‘Clinical Practice Assessment Criteria’ mentors use to measure students’ performance) there may be occasions when mentors want to recognise a student’s exceptional effort and achievement. Personal praise and recognition can be extremely motivating to students, some of whom may undersell themselves. You could also document these views about a student in the learning contract ‘Statement of Achievement’ or provide the student with an additional ‘testimonial’ which they can add to their personal portfolio. back home
Frequently asked questions Working in partnership Frequently asked questions Q 10. What should I do if I have concerns about a student’s competence? Firstly discuss these concerns with the student. This might be sensitively discussed as part of the learning contract middle interview. Document your concerns. This is a good point to involve a Practice Facilitator. They can help set up an Action Plan to document students’ progress and meet with you and the student at regular intervals. The Practice Facilitator will also act as a bridge between your placement and key people in the University. Q 11. How can I celebrate a student’s exceptional performance? Each individual student should be recognised for their own personal skills and qualities. Whilst students can never be compared to one another (hence the ‘Clinical Practice Assessment Criteria’ mentors use to measure students’ performance) there may be occasions when mentors want to recognise a student’s exceptional effort and achievement. Personal praise and recognition can be extremely motivating to students, some of whom may undersell themselves. You could also document these views about a student in the learning contract ‘Statement of Achievement’ or provide the student with an additional ‘testimonial’ which they can add to their personal portfolio. back home
 Frequently asked questions Working in partnership Frequently asked questions Q 12. What can mentors use as evidence of their updateness? There are many activities mentors engage in that constitute mentoring activity in addition to acting as a mentor for pre-registration student nurses. It may be that as a mentor you work as a co mentor, support a student during a shift, involve yourself in reviewing your clinical area’s student nurse induction pack or educational audit. You may attend mentor updates, a mentor link forum meeting or mentor conference, or engage in ongoing dialogue about students within your clinical setting with other nurse mentors. You may have completed additional learning about mentorship either within an academic qualification or distance learning material. You may also have documented some reflections about your role as a mentor. All of these activities are legitimate mentoring activities and can be reflected in a portfolio of evidence (you are invited to use the mentor portfolio on offer within ABM University Health Board) and discuss this updateness at your annual PDR review in line with NMC Standards to maintain you status as a mentor. back home
Frequently asked questions Working in partnership Frequently asked questions Q 12. What can mentors use as evidence of their updateness? There are many activities mentors engage in that constitute mentoring activity in addition to acting as a mentor for pre-registration student nurses. It may be that as a mentor you work as a co mentor, support a student during a shift, involve yourself in reviewing your clinical area’s student nurse induction pack or educational audit. You may attend mentor updates, a mentor link forum meeting or mentor conference, or engage in ongoing dialogue about students within your clinical setting with other nurse mentors. You may have completed additional learning about mentorship either within an academic qualification or distance learning material. You may also have documented some reflections about your role as a mentor. All of these activities are legitimate mentoring activities and can be reflected in a portfolio of evidence (you are invited to use the mentor portfolio on offer within ABM University Health Board) and discuss this updateness at your annual PDR review in line with NMC Standards to maintain you status as a mentor. back home
 Frequently asked questions Working in partnership Frequently asked questions Q 13. How much information should be passed on from one placement to another about a student who is on the borderline of achievement in clinical practice? A great deal of care and sensitivity is needed in these circumstances. Students who may be underperforming in practice have the right to opportunities within each academic year to achieve practice outcomes (as long as their performance does not constitute a serious breach of safety of patient care). At the same time mentors are accountable for the delegation of work to students. Here lies the tension for mentors and students in offering opportunities to engage in clinical nursing activities whilst carrying out credible student assessment. Other information about a student’s underperformance may act to prejudice future mentors and so should not be passed on wholesale between clinical areas. There may well be a history and context to a student’s developing needs such as issues relating to individual learning styles or perhaps associated with dyslexia or disability. It would be advisable to contact a Practice Facilitator should mentors be faced with assessing a student who there are doubts about. They are in a position to liaise with key University personnel and also provide direct support to student and mentors in these circumstances. back home
Frequently asked questions Working in partnership Frequently asked questions Q 13. How much information should be passed on from one placement to another about a student who is on the borderline of achievement in clinical practice? A great deal of care and sensitivity is needed in these circumstances. Students who may be underperforming in practice have the right to opportunities within each academic year to achieve practice outcomes (as long as their performance does not constitute a serious breach of safety of patient care). At the same time mentors are accountable for the delegation of work to students. Here lies the tension for mentors and students in offering opportunities to engage in clinical nursing activities whilst carrying out credible student assessment. Other information about a student’s underperformance may act to prejudice future mentors and so should not be passed on wholesale between clinical areas. There may well be a history and context to a student’s developing needs such as issues relating to individual learning styles or perhaps associated with dyslexia or disability. It would be advisable to contact a Practice Facilitator should mentors be faced with assessing a student who there are doubts about. They are in a position to liaise with key University personnel and also provide direct support to student and mentors in these circumstances. back home
 Frequently asked questions Working in partnership Frequently asked questions Q 14. How do we know that reliable assessment decisions are being made between different mentors? Given that mentors use their subjectivity as part of the assessment of student nurses’ competence there is a need to ensure that mentors are assessing students in consistent ways. A number of studies have concentrated on the impact of this aspect of the mentoring role when making decisions about student competence (Jones 2004; Kneafsey 2007); the inter rater reliability between mentors in their assessment strategies (Brown 2000; Seldomridge and Walsh 2006; Mc. Carthy and Murphy 2008), the difficult process of giving accurate feedback to students (Clynes 2008) and the way key personnel make decisions about the capacity of clinical placements to support student learning in practice (Pulsford et al. 2002; Hutchings et al. 2005). An influential study by Duffy (2003) found that competence assessment was complicated by mentors not addressing problems early enough in placements and being swayed by the idea of giving novice students the benefit of the doubt. The emotional trauma experienced by some mentors at having to fail a student was a significant finding. back home
Frequently asked questions Working in partnership Frequently asked questions Q 14. How do we know that reliable assessment decisions are being made between different mentors? Given that mentors use their subjectivity as part of the assessment of student nurses’ competence there is a need to ensure that mentors are assessing students in consistent ways. A number of studies have concentrated on the impact of this aspect of the mentoring role when making decisions about student competence (Jones 2004; Kneafsey 2007); the inter rater reliability between mentors in their assessment strategies (Brown 2000; Seldomridge and Walsh 2006; Mc. Carthy and Murphy 2008), the difficult process of giving accurate feedback to students (Clynes 2008) and the way key personnel make decisions about the capacity of clinical placements to support student learning in practice (Pulsford et al. 2002; Hutchings et al. 2005). An influential study by Duffy (2003) found that competence assessment was complicated by mentors not addressing problems early enough in placements and being swayed by the idea of giving novice students the benefit of the doubt. The emotional trauma experienced by some mentors at having to fail a student was a significant finding. back home
 Frequently asked questions Working in partnership Frequently asked questions Q 15. What affects mentors ability to supervise students for at least 40% of the time during clinical placements? An examination of the mentorship literature identifies a number of issues which may potentially compromise nurses’ role as mentors. Depending on the clinical setting time may become an important factor when supporting and assessing the learning of pre-registration students. The demands of clinical work for the registered nurse mentor may limit their ability to spend as much time as they might like with students. The student/mentor relationship appears to be heavily influenced by the quality of this bond (Andrews and Chilton 2000; Jones et al. 2001; Koskinen and Tossavainen 2003), the frequency of contact between student and mentor (Lloyd Jones et al. 2001; Wood 2005) and the confidence mentors have in their own assessment decision-making (Bray and Nettleton 2007; Webb and Shakespeare 2008). Clearly, the quality of mentorship and inspirational role modelling student nurses’ experience throughout their training is critical (Neary 2000), as is the standard and availability of mentor preparation programmes (Finnerty et al. 2006; Clemow 2007). back home
Frequently asked questions Working in partnership Frequently asked questions Q 15. What affects mentors ability to supervise students for at least 40% of the time during clinical placements? An examination of the mentorship literature identifies a number of issues which may potentially compromise nurses’ role as mentors. Depending on the clinical setting time may become an important factor when supporting and assessing the learning of pre-registration students. The demands of clinical work for the registered nurse mentor may limit their ability to spend as much time as they might like with students. The student/mentor relationship appears to be heavily influenced by the quality of this bond (Andrews and Chilton 2000; Jones et al. 2001; Koskinen and Tossavainen 2003), the frequency of contact between student and mentor (Lloyd Jones et al. 2001; Wood 2005) and the confidence mentors have in their own assessment decision-making (Bray and Nettleton 2007; Webb and Shakespeare 2008). Clearly, the quality of mentorship and inspirational role modelling student nurses’ experience throughout their training is critical (Neary 2000), as is the standard and availability of mentor preparation programmes (Finnerty et al. 2006; Clemow 2007). back home
 Failing to fail Working in partnership Kathleen Duffy received a UKCC scholarship in 2001 to study the issue of failing students. The results of her research are summarised in this article. A copy of Kathleen Duffy’s full report is available on the NMC website. The following is reproduced from NMC News July 2004 Number 8. Page 1 of 2… ‘In your role as a mentor have you ever had concerns about a student nurse or a student midwife’s clinical performance and been caught in the dilemma of whether or not to fail them? The decision isn’t always as straightforward as it might seem. Kathleen Duffy’s study showed that most mentors are well prepared and carefully consider the assessment decisions they make for the students they support, but some of the mentors interviewed had given a pass despite having concerns about a student’s clinical performance. Several reasons were identified as to why students passed when their performance was not up to scratch. Some mentors disclosed that they had not failed students who were early on in the training programme as they felt that they needed time to learn and should be given the ‘benefit of the doubt’. Mentors felt that the student would pick up the necessary skills in future placements. Other mentors felt that it wasn’t their responsibility to fail students and that it was sufficient for them to raise concerns about a student’s clinical performance to lecturing staff. Many felt uncomfortable ‘putting pen to paper’ - either because they found the clinical assessment document full of jargon that they could not translate into practice, or they were worried about repercussions from the university of failing a student. Other mentors in the study saw failing a student as an uncaring practice. One mentor had given a third year student, who was close to qualifying, the ‘benefit of the doubt’ because she did not want to jeopardise the student’s future when they were so close to finishing their course. Another allowed a student’s personal problems and circumstances to influence her judgement. Some mentors felt they had no choice but to pass a student. As an example, one mentor found that, despite asking, no support was provided from education staff and she did not feel able to fail the student. Others were told by lecturers that they could not fail a student because they had not followed the correct procedures to do so. forward home
Failing to fail Working in partnership Kathleen Duffy received a UKCC scholarship in 2001 to study the issue of failing students. The results of her research are summarised in this article. A copy of Kathleen Duffy’s full report is available on the NMC website. The following is reproduced from NMC News July 2004 Number 8. Page 1 of 2… ‘In your role as a mentor have you ever had concerns about a student nurse or a student midwife’s clinical performance and been caught in the dilemma of whether or not to fail them? The decision isn’t always as straightforward as it might seem. Kathleen Duffy’s study showed that most mentors are well prepared and carefully consider the assessment decisions they make for the students they support, but some of the mentors interviewed had given a pass despite having concerns about a student’s clinical performance. Several reasons were identified as to why students passed when their performance was not up to scratch. Some mentors disclosed that they had not failed students who were early on in the training programme as they felt that they needed time to learn and should be given the ‘benefit of the doubt’. Mentors felt that the student would pick up the necessary skills in future placements. Other mentors felt that it wasn’t their responsibility to fail students and that it was sufficient for them to raise concerns about a student’s clinical performance to lecturing staff. Many felt uncomfortable ‘putting pen to paper’ - either because they found the clinical assessment document full of jargon that they could not translate into practice, or they were worried about repercussions from the university of failing a student. Other mentors in the study saw failing a student as an uncaring practice. One mentor had given a third year student, who was close to qualifying, the ‘benefit of the doubt’ because she did not want to jeopardise the student’s future when they were so close to finishing their course. Another allowed a student’s personal problems and circumstances to influence her judgement. Some mentors felt they had no choice but to pass a student. As an example, one mentor found that, despite asking, no support was provided from education staff and she did not feel able to fail the student. Others were told by lecturers that they could not fail a student because they had not followed the correct procedures to do so. forward home
 Failing to fail Working in partnership Page 2… Although these reasons are understandable, the consequences of not failing a student can be very serious. Passing students in the hope that they will improve later in the course has consequences for patients, clients, students and future mentors. Lecturers who were interviewed during the study indicated that some students were reaching their third year before failing clinical assessments. The students themselves felt devastated at being failed at this late stage, while mentors involved in failing them highlighted that it was a ‘horrendous, emotionally draining and time consuming’ process. There was some anger that colleagues in earlier placements had ‘passed the buck’. Failing to tell students that they have not reached the required standards also has consequences for the professions. Lecturers talked about students who had qualified despite having a history of problems. Passing students who should have failed does not protect the interests of the public and puts the patients who will be under their care at risk. This is not a new problem but one which, as professionals, we need to acknowledge, discuss and debate. The reality of being a mentor is that it is a complex and demanding role. Add in the issue of a problematic student and it can be overwhelming. Mentors need effective preparation and support to deal with under-performing students. Initial mentorship preparation programmes need to address the issue of failing students, highlighting issues of accountability, as well as the emotional impact and practical aspects of the process. When faced with a problematic student, mentors need extra time and guidance to fulfil their professional responsibility; help from experienced mentors and lecturers; and strong line management support. The NMC standards for the preparation of mentors provides a tool for preparation, but it is the mentor’s knowledge, skills and competence in effectively carrying out their role that protects the public by ensuring that students who are lacking in competence do not progress to become registered nurses or midwives. Most importantly there has to be the recognition that some students need to fail. So if you are thinking of giving a student the ‘benefit of the doubt’ then you should consider whether it is in the best interests of the patients, your clients, the student, subsequent mentors and the profession as a whole. ’ Kathleen Duffy Lecturer, School of Nursing, Midwifery and Community Health, Glasgow Caledonian University e-mail: k. duffy@gcal. ac. uk back home
Failing to fail Working in partnership Page 2… Although these reasons are understandable, the consequences of not failing a student can be very serious. Passing students in the hope that they will improve later in the course has consequences for patients, clients, students and future mentors. Lecturers who were interviewed during the study indicated that some students were reaching their third year before failing clinical assessments. The students themselves felt devastated at being failed at this late stage, while mentors involved in failing them highlighted that it was a ‘horrendous, emotionally draining and time consuming’ process. There was some anger that colleagues in earlier placements had ‘passed the buck’. Failing to tell students that they have not reached the required standards also has consequences for the professions. Lecturers talked about students who had qualified despite having a history of problems. Passing students who should have failed does not protect the interests of the public and puts the patients who will be under their care at risk. This is not a new problem but one which, as professionals, we need to acknowledge, discuss and debate. The reality of being a mentor is that it is a complex and demanding role. Add in the issue of a problematic student and it can be overwhelming. Mentors need effective preparation and support to deal with under-performing students. Initial mentorship preparation programmes need to address the issue of failing students, highlighting issues of accountability, as well as the emotional impact and practical aspects of the process. When faced with a problematic student, mentors need extra time and guidance to fulfil their professional responsibility; help from experienced mentors and lecturers; and strong line management support. The NMC standards for the preparation of mentors provides a tool for preparation, but it is the mentor’s knowledge, skills and competence in effectively carrying out their role that protects the public by ensuring that students who are lacking in competence do not progress to become registered nurses or midwives. Most importantly there has to be the recognition that some students need to fail. So if you are thinking of giving a student the ‘benefit of the doubt’ then you should consider whether it is in the best interests of the patients, your clients, the student, subsequent mentors and the profession as a whole. ’ Kathleen Duffy Lecturer, School of Nursing, Midwifery and Community Health, Glasgow Caledonian University e-mail: k. duffy@gcal. ac. uk back home
 ‘Live’ supervision Working in partnership This event involves a client (Jack), a Ward manager, a second year Adult branch student (Lisa) and a mentor (Emma), in her role as community nurse. Personal details have been disguised. Page 1 of 3… Jack has a mild learning disability and had been admitted to a medical ward because of respiratory problems. There was going to be a delay in Jack’s discharge back to the community group home where he lived. The problem had arisen because of funding issues relating to Jack’s challenging needs. Delivering this bad news to Jack needed to be sensitively managed as he was expecting to be discharged shortly. Emma invited Lisa to be a part of this process. The Ward manager, Lisa and Emma discussed when and where to talk to Jack about the delay. It was decided that Emma would lead this process. Although by telling Jack the truth, therapeutic value of hope might be compromised, withholding news about the funding would only delay his inevitable increased anxiety when his anticipated discharge date came and went. Emma suggested they went into a side room as a venue for the conversation with Jack. She was aware that responding to Jack in a supportive and attentive way was made more difficult being the bearer of bad news. Yet at the same time, Emma felt that she was considered in her approach to Jack especially with her non-verbal behaviour and the words that she used. Lisa also made some important contributions. At first, Jack appeared receptive to communication. He seemed to take the news surprisingly well and thanked everyone for being frank with him. Emma repeated the information again, but Jack seemed comfortable with the idea of a delay and asked to go for a cup of tea. Initially, Emma and Lisa felt some relief that Jack had apparently accepted his position following their conversation. At the same time, both the Ward manager and Emma felt uncomfortable about Jack’s reaction, as his passive response seemed out of place with the personal consequences of the information. forward back home
‘Live’ supervision Working in partnership This event involves a client (Jack), a Ward manager, a second year Adult branch student (Lisa) and a mentor (Emma), in her role as community nurse. Personal details have been disguised. Page 1 of 3… Jack has a mild learning disability and had been admitted to a medical ward because of respiratory problems. There was going to be a delay in Jack’s discharge back to the community group home where he lived. The problem had arisen because of funding issues relating to Jack’s challenging needs. Delivering this bad news to Jack needed to be sensitively managed as he was expecting to be discharged shortly. Emma invited Lisa to be a part of this process. The Ward manager, Lisa and Emma discussed when and where to talk to Jack about the delay. It was decided that Emma would lead this process. Although by telling Jack the truth, therapeutic value of hope might be compromised, withholding news about the funding would only delay his inevitable increased anxiety when his anticipated discharge date came and went. Emma suggested they went into a side room as a venue for the conversation with Jack. She was aware that responding to Jack in a supportive and attentive way was made more difficult being the bearer of bad news. Yet at the same time, Emma felt that she was considered in her approach to Jack especially with her non-verbal behaviour and the words that she used. Lisa also made some important contributions. At first, Jack appeared receptive to communication. He seemed to take the news surprisingly well and thanked everyone for being frank with him. Emma repeated the information again, but Jack seemed comfortable with the idea of a delay and asked to go for a cup of tea. Initially, Emma and Lisa felt some relief that Jack had apparently accepted his position following their conversation. At the same time, both the Ward manager and Emma felt uncomfortable about Jack’s reaction, as his passive response seemed out of place with the personal consequences of the information. forward back home
 ‘Live’ supervision Working in partnership ‘Live’ supervision continued Page 2… They both sensed that Jack’s reaction did not fit with previous conversations where he had been consumed with an eagerness to be discharged. Despite a temptation to leave the ward as it was now approaching the end of their shift, Emma, Lisa and the Ward manager felt that they needed to give Jack more time to digest the information they had discussed with him. They discussed some of the reasons for these intuitive feelings. There are indications, for example, that nurses overestimate the comprehensive skills of people with learning disabilities in deciphering more complex issues (Banat et al 2002), that people with learning disabilities may not be able to recognise the impact of emotionally charged messages and have a tendency towards compliance during questioning (Richardson 2000). Emma and Lisa felt that some of these issues may have influenced their discussion with Jack. The Ward manager, Lisa and Emma had a pertinent discussion about the difficulties of power distinctions between patients and nurses and how this may have been particularly relevant to Jack’s interactions with us, given historical patterns of institutionalised relationships between people with learning disabilities and professionals. Lisa drew on the point that wearing her uniform might have subtly reinforced this power discrepancy, contributing to Jack’s seemingly passive acceptance of significant information. He later became more agitated about his situation. Of particular concern during the episode was the tension between ‘relief’ that Jack had apparently accepted the bad news, yet intuitive feelings that he had not fully comprehended his position. forward back home
‘Live’ supervision Working in partnership ‘Live’ supervision continued Page 2… They both sensed that Jack’s reaction did not fit with previous conversations where he had been consumed with an eagerness to be discharged. Despite a temptation to leave the ward as it was now approaching the end of their shift, Emma, Lisa and the Ward manager felt that they needed to give Jack more time to digest the information they had discussed with him. They discussed some of the reasons for these intuitive feelings. There are indications, for example, that nurses overestimate the comprehensive skills of people with learning disabilities in deciphering more complex issues (Banat et al 2002), that people with learning disabilities may not be able to recognise the impact of emotionally charged messages and have a tendency towards compliance during questioning (Richardson 2000). Emma and Lisa felt that some of these issues may have influenced their discussion with Jack. The Ward manager, Lisa and Emma had a pertinent discussion about the difficulties of power distinctions between patients and nurses and how this may have been particularly relevant to Jack’s interactions with us, given historical patterns of institutionalised relationships between people with learning disabilities and professionals. Lisa drew on the point that wearing her uniform might have subtly reinforced this power discrepancy, contributing to Jack’s seemingly passive acceptance of significant information. He later became more agitated about his situation. Of particular concern during the episode was the tension between ‘relief’ that Jack had apparently accepted the bad news, yet intuitive feelings that he had not fully comprehended his position. forward back home
 ‘Live’ supervision Working in partnership ‘Live’ supervision continued Page 3… Emma and Lisa talked about how their feelings of anxiety might have been alleviated had they left the ward, which they were entitled to do as it was the end of their shift (self-interest). Yet, this was balanced with a sense of moral duty to see the situation through partly because of consistency and Emma’s prior involvement with Jack, but also because of a beneficent feeling of ‘doing right by him’ (selfless obligation). Emma and Lisa made some analogies about how virtue ethics were influencing the situation with Jack (‘what kind of people were we being at this moment’), whilst also acknowledging that these principles were fundamental in most nursing situations. Through her participation in these discussions and in the episode as it was happening, Lisa was attempting to advance her ‘knowledge in waiting’ into ‘knowledge in use’ (Schön 1987). This encounter approaches what Rolfe et al (2001) describe as a ‘reflexive practicum, ’ where reflection in the moment of messy practice situations becomes visible as a learning experience. In this sense, reflection-in-action stimulates a continual reframing and re-evaluation of the event, prompting further action and new reflection. For each person involved in delivering the bad news to Jack, whether as the main actor or legitimate partner members, there was a need to act (sensitive discussion with Jack), reflect on what was happening (respond to Jack’s need for attentiveness and to be left alone) and to reflect on how the unfolding episode was being dealt with (continually noticing the impact of our presence on Jack’s assimilation of bad news). As a legitimate partner, Lisa was able to experience some of the contextual realities involved in the episode such as enabling patient’s autonomous decision-making. The situation may also have helped Lisa identify the process of being an ‘internal supervisor’ of your own practice (Casement 1985), by tracking the evolution of the episode from initial strategy decisions to ending the contact with Jack. back home
‘Live’ supervision Working in partnership ‘Live’ supervision continued Page 3… Emma and Lisa talked about how their feelings of anxiety might have been alleviated had they left the ward, which they were entitled to do as it was the end of their shift (self-interest). Yet, this was balanced with a sense of moral duty to see the situation through partly because of consistency and Emma’s prior involvement with Jack, but also because of a beneficent feeling of ‘doing right by him’ (selfless obligation). Emma and Lisa made some analogies about how virtue ethics were influencing the situation with Jack (‘what kind of people were we being at this moment’), whilst also acknowledging that these principles were fundamental in most nursing situations. Through her participation in these discussions and in the episode as it was happening, Lisa was attempting to advance her ‘knowledge in waiting’ into ‘knowledge in use’ (Schön 1987). This encounter approaches what Rolfe et al (2001) describe as a ‘reflexive practicum, ’ where reflection in the moment of messy practice situations becomes visible as a learning experience. In this sense, reflection-in-action stimulates a continual reframing and re-evaluation of the event, prompting further action and new reflection. For each person involved in delivering the bad news to Jack, whether as the main actor or legitimate partner members, there was a need to act (sensitive discussion with Jack), reflect on what was happening (respond to Jack’s need for attentiveness and to be left alone) and to reflect on how the unfolding episode was being dealt with (continually noticing the impact of our presence on Jack’s assimilation of bad news). As a legitimate partner, Lisa was able to experience some of the contextual realities involved in the episode such as enabling patient’s autonomous decision-making. The situation may also have helped Lisa identify the process of being an ‘internal supervisor’ of your own practice (Casement 1985), by tracking the evolution of the episode from initial strategy decisions to ending the contact with Jack. back home
 Reflecting in practice Working in partnership ‘Reflection in the messiness of practice Page 1 of 2… Simply to ‘possess’ skills and abilities in nursing devoid of a rationale for your actions, may lead to nursing activities being carried out in efficient but unquestioning ways (Biggs 2005). For example, in one seemingly simple activity such as helping an older vulnerable person have a bath, a complex world of needs, sensitivities and implications exists in which nursing care amounts to more than a series of tasks or procedures. Integrating theory and practice in nursing situations can be seen as requiring a therapeutic blend of technical skills and intuitive responses to solve particular problems. Perhaps this ‘craft knowledge’ Titchen & Ersser (2001), where nurses are able to apply such therapeutic blends in clinical practice is worthy of further exploration. Examining the ideas student and mentors may hold about their practice through reflection becomes significant therefore, especially as nursing actions are inevitably influenced by private, cultural or educational experience. forward back home
Reflecting in practice Working in partnership ‘Reflection in the messiness of practice Page 1 of 2… Simply to ‘possess’ skills and abilities in nursing devoid of a rationale for your actions, may lead to nursing activities being carried out in efficient but unquestioning ways (Biggs 2005). For example, in one seemingly simple activity such as helping an older vulnerable person have a bath, a complex world of needs, sensitivities and implications exists in which nursing care amounts to more than a series of tasks or procedures. Integrating theory and practice in nursing situations can be seen as requiring a therapeutic blend of technical skills and intuitive responses to solve particular problems. Perhaps this ‘craft knowledge’ Titchen & Ersser (2001), where nurses are able to apply such therapeutic blends in clinical practice is worthy of further exploration. Examining the ideas student and mentors may hold about their practice through reflection becomes significant therefore, especially as nursing actions are inevitably influenced by private, cultural or educational experience. forward back home
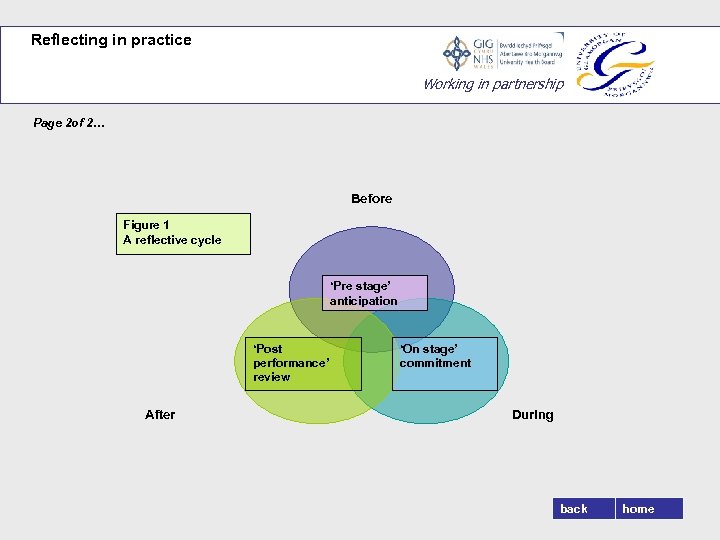 Reflecting in practice Working in partnership Page 2 of 2… Before Figure 1 A reflective cycle ‘Pre stage’ anticipation ‘Post performance’ review After ‘On stage’ commitment During back home
Reflecting in practice Working in partnership Page 2 of 2… Before Figure 1 A reflective cycle ‘Pre stage’ anticipation ‘Post performance’ review After ‘On stage’ commitment During back home
 Practice Facilitators Working in partnership There are 3 Practice Facilitators working within East Abertawe Bro Morgannwg NHS Trust: Simon Cassidy (RMN; RNLD; Bsc (Hons); Dip HE Prof Prac; PGCE) qualified as a mental health nurse in 1984 and subsequently as a Registered nurse for people with learning disabilities. He has worked extensively within residential and community health settings. Based at Princess of Wales Hospital Bridgend, Simon is responsible for mentorship issues within Surgical Specialities, Anaesthetics & Critical Care, Mental Health & Forensics and Learning Disability Services (Bridgend area). Simon has an interest in qualitative research about how mentors’ interpret competence in their assessment of pre-registration student nurses who are on the borderline of achievement in practice. He is due to commence an MPhil/Phd in October 2008 to pursue this topic. Contact: Tel : 01656 752557/8 Simon. Cassidy@wales. nhs. uk Kay Jones RGN, BSc(Hons), Dip N, PGCE(Pc. ET) qualified as a general Nurse in 1993. She has a wide range of experience which includes medicine, palliative care, HDU/ITU and Practice Nursing. In 2004 she became one of a team of 4 manual handling trainers for ABM (Bro Morgannwg) and helped to launch the All Wales Manual Handling Training Passport across the Trust. This sparked her interest in teaching and education. She soon went on to complete the PGCE in 2007. At present her post is on secondment basis as a Practice Facilitator for ABM. Contact: Tel: 01656 752557/8 kay. jones@wales. nhs. uk Download a copy of the Practice Facilitators Annual Report 2009/2010 From Mentorship Categories page home
Practice Facilitators Working in partnership There are 3 Practice Facilitators working within East Abertawe Bro Morgannwg NHS Trust: Simon Cassidy (RMN; RNLD; Bsc (Hons); Dip HE Prof Prac; PGCE) qualified as a mental health nurse in 1984 and subsequently as a Registered nurse for people with learning disabilities. He has worked extensively within residential and community health settings. Based at Princess of Wales Hospital Bridgend, Simon is responsible for mentorship issues within Surgical Specialities, Anaesthetics & Critical Care, Mental Health & Forensics and Learning Disability Services (Bridgend area). Simon has an interest in qualitative research about how mentors’ interpret competence in their assessment of pre-registration student nurses who are on the borderline of achievement in practice. He is due to commence an MPhil/Phd in October 2008 to pursue this topic. Contact: Tel : 01656 752557/8 Simon. Cassidy@wales. nhs. uk Kay Jones RGN, BSc(Hons), Dip N, PGCE(Pc. ET) qualified as a general Nurse in 1993. She has a wide range of experience which includes medicine, palliative care, HDU/ITU and Practice Nursing. In 2004 she became one of a team of 4 manual handling trainers for ABM (Bro Morgannwg) and helped to launch the All Wales Manual Handling Training Passport across the Trust. This sparked her interest in teaching and education. She soon went on to complete the PGCE in 2007. At present her post is on secondment basis as a Practice Facilitator for ABM. Contact: Tel: 01656 752557/8 kay. jones@wales. nhs. uk Download a copy of the Practice Facilitators Annual Report 2009/2010 From Mentorship Categories page home
 Mentor training Working in partnership Please contact Simon or Kay about Mentor Preparation courses or Mentor Update courses in the Bridgend areas of the Health Board. Simon Cassidy Contact: Tel : 01656 752557/8 email: simon. cassidy@wales. nhs. uk Kay Jones Contact: Tel: 01656 752557/8 email: kay. jones@wales. nhs. uk mentor preparation dates mentor update sessions back home
Mentor training Working in partnership Please contact Simon or Kay about Mentor Preparation courses or Mentor Update courses in the Bridgend areas of the Health Board. Simon Cassidy Contact: Tel : 01656 752557/8 email: simon. cassidy@wales. nhs. uk Kay Jones Contact: Tel: 01656 752557/8 email: kay. jones@wales. nhs. uk mentor preparation dates mentor update sessions back home
 Mentor training Working in partnership MENTORSHIP PREPARATION 2009 (For nurses never having undertaken mentor training before). All sessions are held in the Nurse Education Centre Princess of Wales Hospital and start at 9. 30 am. For nurses wishing to commence Mentor Preparation training an Introductory letter of invitation from ABM Mentorship Categories section which explains the structure of the course. Download a copy Overall learning outcomes indicate the content of the preparation programme which includes learning in academic and practice settings. Click to book Book a place back home
Mentor training Working in partnership MENTORSHIP PREPARATION 2009 (For nurses never having undertaken mentor training before). All sessions are held in the Nurse Education Centre Princess of Wales Hospital and start at 9. 30 am. For nurses wishing to commence Mentor Preparation training an Introductory letter of invitation from ABM Mentorship Categories section which explains the structure of the course. Download a copy Overall learning outcomes indicate the content of the preparation programme which includes learning in academic and practice settings. Click to book Book a place back home
 Mentor training Working in partnership Venue: Multi Professional Education Centre POW Times: 9. 30 -4 pm These sessions are designed for nurses registered for at least one year who wish to become mentors. 2011 Cohort dates: Mentorship advice and support is available for Registered nurses and pre-registration students from: Simon Cassidy Practice Facilitator Multi professional Education Centre Princess of Wales Hospital Tel: 01656 75(2557) email: simon. cassidy@wales. nhs. uk Dec 2 nd (2010) March 23 rd (2011) Seminar room 9 March 24 th June 17 th Seminar room 8 June 16 th Sept 23 rd Seminar room 8 Sept 22 nd Dec 1 st March 20 th Book a Seminar room 8 place Book a place Seminar room 8 back home
Mentor training Working in partnership Venue: Multi Professional Education Centre POW Times: 9. 30 -4 pm These sessions are designed for nurses registered for at least one year who wish to become mentors. 2011 Cohort dates: Mentorship advice and support is available for Registered nurses and pre-registration students from: Simon Cassidy Practice Facilitator Multi professional Education Centre Princess of Wales Hospital Tel: 01656 75(2557) email: simon. cassidy@wales. nhs. uk Dec 2 nd (2010) March 23 rd (2011) Seminar room 9 March 24 th June 17 th Seminar room 8 June 16 th Sept 23 rd Seminar room 8 Sept 22 nd Dec 1 st March 20 th Book a Seminar room 8 place Book a place Seminar room 8 back home
 Mentor training Working in partnership MENTORSHIP UPDATES 2011 (For nurses having undertaken mentor preparation training but who want to revisit key aspects of mentorship). All sessions are held in the Multi Professional Education Centre Princess of Wales Hospital. Mentor Update sessions (Recap): These sessions are designed for existing mentors who have a working familiarity with assessment processes but who need to recap on current mentorship issues. Click to book Mentor Update sessions (Extended): These sessions are designed for existing mentors who want extended opportunity for exploration of mentorship issues. Click to book Book a place back home
Mentor training Working in partnership MENTORSHIP UPDATES 2011 (For nurses having undertaken mentor preparation training but who want to revisit key aspects of mentorship). All sessions are held in the Multi Professional Education Centre Princess of Wales Hospital. Mentor Update sessions (Recap): These sessions are designed for existing mentors who have a working familiarity with assessment processes but who need to recap on current mentorship issues. Click to book Mentor Update sessions (Extended): These sessions are designed for existing mentors who want extended opportunity for exploration of mentorship issues. Click to book Book a place back home
 Mentor training Working in partnership Venue: Multi Professional Education Centre POW All sessions in Seminar room 8 Times: 2 -3. 30 pm These sessions are designed for existing mentors who have a working familiarity with assessment processes but who need to recap on current mentorship issues. Mentorship advice and support is available for Registered nurses and pre-registration students from: Simon Cassidy Practice Facilitator Multi professional Education Centre Princess of Wales Hospital Tel: 01656 75(2557) email: simon. cassidy@wales. nhs. uk 2011 dates: January February March April May June July September October November 11 th / 18 th / 22 nd 5 th / 12 th 3 rd / 17 th / 21 st 5 th / 12 th 13 th / 14 th 11 th / 18 th 15 th / 22 nd Book a place back home
Mentor training Working in partnership Venue: Multi Professional Education Centre POW All sessions in Seminar room 8 Times: 2 -3. 30 pm These sessions are designed for existing mentors who have a working familiarity with assessment processes but who need to recap on current mentorship issues. Mentorship advice and support is available for Registered nurses and pre-registration students from: Simon Cassidy Practice Facilitator Multi professional Education Centre Princess of Wales Hospital Tel: 01656 75(2557) email: simon. cassidy@wales. nhs. uk 2011 dates: January February March April May June July September October November 11 th / 18 th / 22 nd 5 th / 12 th 3 rd / 17 th / 21 st 5 th / 12 th 13 th / 14 th 11 th / 18 th 15 th / 22 nd Book a place back home
 Mentor training Working in partnership Venue: Multi Professional Education Centre POW All sessions in Seminar room 8 Times: 9. 30 -12. 30 These sessions are designed for existing mentors who want extended opportunity for exploration of mentorship issues. Mentorship advice and support is available for Registered nurses and pre-registration students from: Simon Cassidy Practice Facilitator Multi professional Education Centre Princess of Wales Hospital Tel: 01656 75(2557) email: simon. cassidy@wales. nhs. uk 2011 dates: January February March April May June July September October November 14 th 11 th 15 th 20 th 10 th 8 th 16 th 14 th 18 th Book a place back home
Mentor training Working in partnership Venue: Multi Professional Education Centre POW All sessions in Seminar room 8 Times: 9. 30 -12. 30 These sessions are designed for existing mentors who want extended opportunity for exploration of mentorship issues. Mentorship advice and support is available for Registered nurses and pre-registration students from: Simon Cassidy Practice Facilitator Multi professional Education Centre Princess of Wales Hospital Tel: 01656 75(2557) email: simon. cassidy@wales. nhs. uk 2011 dates: January February March April May June July September October November 14 th 11 th 15 th 20 th 10 th 8 th 16 th 14 th 18 th Book a place back home
 Distance learning menu Working in partnership The distance learning material contained here can be used in a variety of ways. The menu enables nurses new to mentorship as well as those who have supervised students on numerous occasions to choose from a range of refresher topics. In the spirit of adult learning individuals are invited to work through any aspect of the material enclosed here. Completion of any part of the distance learning material can also be documented in a Mentor Portfolio format as evidence of annual and triennial updating. Download a portfolio from Mentorship Categories page , save the portfolio to your desktop and you will be able to enter information to add to your evidence of annual updatedness. As well as providing information about current mentorship issues, distance learning material also sparks discussion about student assessment that spills over into clinical placement areas. In this way more contentious issues might be explored as a group activity. This is particularly the case when examining the validity and reliability of judgements made when assessing practice in challenging circumstances. Click here for learning menu back home
Distance learning menu Working in partnership The distance learning material contained here can be used in a variety of ways. The menu enables nurses new to mentorship as well as those who have supervised students on numerous occasions to choose from a range of refresher topics. In the spirit of adult learning individuals are invited to work through any aspect of the material enclosed here. Completion of any part of the distance learning material can also be documented in a Mentor Portfolio format as evidence of annual and triennial updating. Download a portfolio from Mentorship Categories page , save the portfolio to your desktop and you will be able to enter information to add to your evidence of annual updatedness. As well as providing information about current mentorship issues, distance learning material also sparks discussion about student assessment that spills over into clinical placement areas. In this way more contentious issues might be explored as a group activity. This is particularly the case when examining the validity and reliability of judgements made when assessing practice in challenging circumstances. Click here for learning menu back home
 Distance learning menu Working in partnership Units 1 -5 Mentorship Preparation Distance Learning material Download Units from Mentorship categories page Content description: The Unit s focus on interpersonal skills required for promoting effective interactions between students and mentors. Includes key factors that create an effective learning environment. Enabling Mentorship Activities This workbook has been designed for you to complete within your clinical area. The activities can be completed separately or in their entirety over a period of time by dipping in and out of the workbook exercises. Download the Workbook from Mentorship Categories page Reflective practice NMC Standards to support learning and assessment in practice This presentation explains the main elements of the Nursing and Midwifery Council standards to support learning and assessment in practice. There is a detailed comparison between the NMC Standards framework and what the processes of student nurse assessment as it currently exists in Wales. Assessment documentation quiz: This quiz asks 10 questions about student documentation such as: -What is the purpose of the Professional Attitudes scale? - Where does the mentor sign when there is progress towards achievement of practice outcome, but this has not been achieved fully? Questions and responses Completing student assessment documentation This presentation explains where mentors need to place signatures in order to sign student documentation. There is also an explanation of the assessment strategies mentors use to interpret students’ performance. If you feel you need a more in depth explanation and analysis of student documentation you might want to attend a mentor update session. back home
Distance learning menu Working in partnership Units 1 -5 Mentorship Preparation Distance Learning material Download Units from Mentorship categories page Content description: The Unit s focus on interpersonal skills required for promoting effective interactions between students and mentors. Includes key factors that create an effective learning environment. Enabling Mentorship Activities This workbook has been designed for you to complete within your clinical area. The activities can be completed separately or in their entirety over a period of time by dipping in and out of the workbook exercises. Download the Workbook from Mentorship Categories page Reflective practice NMC Standards to support learning and assessment in practice This presentation explains the main elements of the Nursing and Midwifery Council standards to support learning and assessment in practice. There is a detailed comparison between the NMC Standards framework and what the processes of student nurse assessment as it currently exists in Wales. Assessment documentation quiz: This quiz asks 10 questions about student documentation such as: -What is the purpose of the Professional Attitudes scale? - Where does the mentor sign when there is progress towards achievement of practice outcome, but this has not been achieved fully? Questions and responses Completing student assessment documentation This presentation explains where mentors need to place signatures in order to sign student documentation. There is also an explanation of the assessment strategies mentors use to interpret students’ performance. If you feel you need a more in depth explanation and analysis of student documentation you might want to attend a mentor update session. back home
 References page 1 Working in partnership Banat, D. Summers S. Pring T. (2002) An investigation into carers perceptions of the verbal ability of adults with severe learning disabilities. British Journal of Learning Disabilities 30: 78 -81. Biggs, J (2005) Student Learning Research and Theory – where do we currently stand? Available from: http: //www. londonmet. ac. uk/deliberations/ocsid-publications. [Accessed on 5. 9. 06. ] Casement, P. (1985) On Learning form the Patient. London. Routledge. Daloz, L. A. (1987) Effective Teaching and Mentoring. San Fransisco. Jossey-Bass. Darling, L. A. W. (1986) What to do about toxic mentors Nurse Educator 11(2): 29 -30 Freshwater, D. and Stickley, T. (2004) The heart of the art: emotional intelligence in nurse education. Nurse Inquiry 11(2): 9198. Gillespie, M. (2005) Student-teacher connection: a place of possibility. Journal of Advanced Nursing 52(2) 211 -219. Knowles, M. (1984) The Adult Learner. A Neglected Species (3 rd edn) Houston. Gulf. Landmark, B. Hansen, G. S. Bjones, I. Bohler, A. (2003) Clinical supervision – factors defined by nurses as influential upon the development of competence and skills in supervision. Journal of Clinical Nursing 12: 834 -841. Mezirow, J. (1990) Fostering Critical Reflection in Adulthood. San Fransisco. Jossey-Bass. forward back home
References page 1 Working in partnership Banat, D. Summers S. Pring T. (2002) An investigation into carers perceptions of the verbal ability of adults with severe learning disabilities. British Journal of Learning Disabilities 30: 78 -81. Biggs, J (2005) Student Learning Research and Theory – where do we currently stand? Available from: http: //www. londonmet. ac. uk/deliberations/ocsid-publications. [Accessed on 5. 9. 06. ] Casement, P. (1985) On Learning form the Patient. London. Routledge. Daloz, L. A. (1987) Effective Teaching and Mentoring. San Fransisco. Jossey-Bass. Darling, L. A. W. (1986) What to do about toxic mentors Nurse Educator 11(2): 29 -30 Freshwater, D. and Stickley, T. (2004) The heart of the art: emotional intelligence in nurse education. Nurse Inquiry 11(2): 9198. Gillespie, M. (2005) Student-teacher connection: a place of possibility. Journal of Advanced Nursing 52(2) 211 -219. Knowles, M. (1984) The Adult Learner. A Neglected Species (3 rd edn) Houston. Gulf. Landmark, B. Hansen, G. S. Bjones, I. Bohler, A. (2003) Clinical supervision – factors defined by nurses as influential upon the development of competence and skills in supervision. Journal of Clinical Nursing 12: 834 -841. Mezirow, J. (1990) Fostering Critical Reflection in Adulthood. San Fransisco. Jossey-Bass. forward back home
 References Page 2 Working in partnership Morton-Cooper, A. Palmer, A. (2005) Mentoring, Preceptorship and Clinical Supervision. London. Blackwell Publishing. Neary, M. (2000) Responsive assessment: assessing student nurses’ clinical competence. Nurse Education Today 21: 3 -17. Priest, H. Gibbs, M. (2004) Mental Health Care For People With Learning Disabilities. London. Churchill Livingstone. Richardson, M. (2000) How we live: participatory research with six people with learning difficulties. Journal of Advanced Nursing 32 (6) 1383 -1395. Rolfe, G. Freshwater, D. Jasper, M. (2001) Critical reflection for nursing and the helping professions. Bristol. Palgrave Macmillan. Ronsten, B. Andersson, E. Gustafsson, B. (2005) Confirming mentorship. Journal of Nursing Management 13: 312 -321. Schön, D. (1987) Educating the Reflective Practitioner. San Francisco. Jossey-Bass. Siddell, M. Jones, L. Katz, J. Peberdy, A. Douglas, J. (2003) Debates and Dilemmas in health promotion-a reader. Basingstoke. Palgrave. Spouse, J. (2001) Bridging theory and practice in the supervisory relationship: a sociocultural perspective. Journal of Advanced Nursing 33(4): 512 -522. Titchen, A. and Ersser, S. (2001) Explicating, creating and validating professional craft knowledge. In: Higgs, J. Titchen, A. (eds) Practice Knowledge and Expertise in the Health Professions. Oxford. Butterworth Heinmann. back home
References Page 2 Working in partnership Morton-Cooper, A. Palmer, A. (2005) Mentoring, Preceptorship and Clinical Supervision. London. Blackwell Publishing. Neary, M. (2000) Responsive assessment: assessing student nurses’ clinical competence. Nurse Education Today 21: 3 -17. Priest, H. Gibbs, M. (2004) Mental Health Care For People With Learning Disabilities. London. Churchill Livingstone. Richardson, M. (2000) How we live: participatory research with six people with learning difficulties. Journal of Advanced Nursing 32 (6) 1383 -1395. Rolfe, G. Freshwater, D. Jasper, M. (2001) Critical reflection for nursing and the helping professions. Bristol. Palgrave Macmillan. Ronsten, B. Andersson, E. Gustafsson, B. (2005) Confirming mentorship. Journal of Nursing Management 13: 312 -321. Schön, D. (1987) Educating the Reflective Practitioner. San Francisco. Jossey-Bass. Siddell, M. Jones, L. Katz, J. Peberdy, A. Douglas, J. (2003) Debates and Dilemmas in health promotion-a reader. Basingstoke. Palgrave. Spouse, J. (2001) Bridging theory and practice in the supervisory relationship: a sociocultural perspective. Journal of Advanced Nursing 33(4): 512 -522. Titchen, A. and Ersser, S. (2001) Explicating, creating and validating professional craft knowledge. In: Higgs, J. Titchen, A. (eds) Practice Knowledge and Expertise in the Health Professions. Oxford. Butterworth Heinmann. back home
 Key contacts Working in partnership Abertawe Bro Morgannwg University NHS Trust has identified education leads within each Directorate. The group is managed by the Senior Nurse for Education. Lynne Jones Neath and Port Talbot Hospital, Baglan, Port Talbot. Lynne. Jones 3@wales. nhs. uk Tel: 01639 683172 University contacts: Jill Kneath-Jones is the pre-registration nursing course leader for the University of Glamorgan: Jill Kneath-Jones Pre-registration nursing course leader University of Glamorgan Faculty of Health and Sports Science Glyntaf Campus Pontypridd CF 37 1 DL Tel: 01443 480480 jkneathj@glam. ac. uk home
Key contacts Working in partnership Abertawe Bro Morgannwg University NHS Trust has identified education leads within each Directorate. The group is managed by the Senior Nurse for Education. Lynne Jones Neath and Port Talbot Hospital, Baglan, Port Talbot. Lynne. Jones 3@wales. nhs. uk Tel: 01639 683172 University contacts: Jill Kneath-Jones is the pre-registration nursing course leader for the University of Glamorgan: Jill Kneath-Jones Pre-registration nursing course leader University of Glamorgan Faculty of Health and Sports Science Glyntaf Campus Pontypridd CF 37 1 DL Tel: 01443 480480 jkneathj@glam. ac. uk home
 Focus Working in partnership How do we know that reliable assessment decisions are being made between different mentors? Click for further discussion fairness FAIRNE SSfairn NMC Standards and learning Challenge and support Accountability and risk taking Credible assessment back hom e
Focus Working in partnership How do we know that reliable assessment decisions are being made between different mentors? Click for further discussion fairness FAIRNE SSfairn NMC Standards and learning Challenge and support Accountability and risk taking Credible assessment back hom e
 Focus Working in partnership What can mentors use as evidence of their updateness as a mentor? Click for further discussion fairness FAIRNE SSfairn NMC Standards and learning Challenge and support Accountability and risk taking Credible assessment bac k hom e
Focus Working in partnership What can mentors use as evidence of their updateness as a mentor? Click for further discussion fairness FAIRNE SSfairn NMC Standards and learning Challenge and support Accountability and risk taking Credible assessment bac k hom e
 Focus Working in partnership How much information should be passed on from one placement to another about a student who may be on the borderline of achievement in practice? Click for further discussion fairness FAIRNE SSfairn NMC Standards and learning Challenge and support Accountability and risk taking Credible assessment welcome forward bac k hom e
Focus Working in partnership How much information should be passed on from one placement to another about a student who may be on the borderline of achievement in practice? Click for further discussion fairness FAIRNE SSfairn NMC Standards and learning Challenge and support Accountability and risk taking Credible assessment welcome forward bac k hom e
 Focus Working in partnership What affects mentors ability to supervise students for at least 40% of the time during clinical placements? Click for further discussion fairness FAIRNE SSfairn NMC Standards and learning Challenge and support Accountability and risk taking Credible assessment welcome forward bac k hom e
Focus Working in partnership What affects mentors ability to supervise students for at least 40% of the time during clinical placements? Click for further discussion fairness FAIRNE SSfairn NMC Standards and learning Challenge and support Accountability and risk taking Credible assessment welcome forward bac k hom e
 Which Practice outcome is this? I wish my wife was here The pressure is getting to me “Minds are like parachutes, they work best when open” Sir Thomas Dewar (1864 -1930) bac k hom e
Which Practice outcome is this? I wish my wife was here The pressure is getting to me “Minds are like parachutes, they work best when open” Sir Thomas Dewar (1864 -1930) bac k hom e
 I had this feeling that if I didn’t express my concerns about the student I wouldn’t only be failing them but also other mentors I looked very carefully at the standards about being a third year nurse. At the same time I had this urge to think well would I want this person to nurse me or my relatives There are these windows of opportunity, these six weeks where I need to get to know the student well enough to give a credible assessment I did question myself at the time. I felt as though it was me. Maybe I had too high expectations of the student? There was a sense that I had failed the student I found the process intense but throughout it all I knew I had support from my colleagues. That helped me feel more comfortable in giving constructive criticism to the student fairness FAIRNE SSfairn NMC Standards and learning Challenge and support Accountability and risk taking Credible assessment bac k hom e
I had this feeling that if I didn’t express my concerns about the student I wouldn’t only be failing them but also other mentors I looked very carefully at the standards about being a third year nurse. At the same time I had this urge to think well would I want this person to nurse me or my relatives There are these windows of opportunity, these six weeks where I need to get to know the student well enough to give a credible assessment I did question myself at the time. I felt as though it was me. Maybe I had too high expectations of the student? There was a sense that I had failed the student I found the process intense but throughout it all I knew I had support from my colleagues. That helped me feel more comfortable in giving constructive criticism to the student fairness FAIRNE SSfairn NMC Standards and learning Challenge and support Accountability and risk taking Credible assessment bac k hom e
 What is meant by competence? The term competence refers to the overarching set of knowledge, skills and attitudes required to practise safely and effectively without direct supervision. It has been defined as ‘the combination of skills, knowledge and attitudes, values and technical abilities that underpin safe and effective nursing practice and interventions’ (adapted from Queensland Nursing Council 2009). The NMC specifies competence as a requirement for entry to the NMC register. Both generic competence and field-specific competence are required to practise in a specific field. The term competencies replaces the term ‘proficiencies’ that describe the criteria students must meet in order to complete their programme successfully and apply for registration. The various competencies are acquired in stages during the pre-registration nursing programme. Evidence that all competencies have been acquired is used to determine whether a nursing student is competent to practise as a nurse (NMC Standards for pre-registration 2010) fairness FAIRNE SSfairn NMC Standards and learning Challenge and support Accountability and risk taking Credible assessment bac k hom e
What is meant by competence? The term competence refers to the overarching set of knowledge, skills and attitudes required to practise safely and effectively without direct supervision. It has been defined as ‘the combination of skills, knowledge and attitudes, values and technical abilities that underpin safe and effective nursing practice and interventions’ (adapted from Queensland Nursing Council 2009). The NMC specifies competence as a requirement for entry to the NMC register. Both generic competence and field-specific competence are required to practise in a specific field. The term competencies replaces the term ‘proficiencies’ that describe the criteria students must meet in order to complete their programme successfully and apply for registration. The various competencies are acquired in stages during the pre-registration nursing programme. Evidence that all competencies have been acquired is used to determine whether a nursing student is competent to practise as a nurse (NMC Standards for pre-registration 2010) fairness FAIRNE SSfairn NMC Standards and learning Challenge and support Accountability and risk taking Credible assessment bac k hom e
 Overall Learning Outcomes Working in partnership Theoretical learning outcomes: • Discuss the implications of mentoring pre-registration student nurses in a current health care context. • Drawing on theories of education, examine the qualities involved in positive mentorship when supporting preregistration student nurses. • Given practice assessment documentation, explain how accurate completion of competency outcomes can assist students in developing their personal learning. • Using research literature and case scenarios, examine ways mentors can manage placement experiences when supporting failing students. Clinical learning outcomes: • Describe the integration of mentorship principles in the practice of supporting pre-registration student nurses in clinical experiences. • Reflect on the use of mentoring skills in practice, including identifying any limitations in discussions with course supervisor/ clinical mentor. fairness FAIRNE SSfairn NMC Standards and learning Challenge and support Accountability and risk taking Credible assessment bac k hom e
Overall Learning Outcomes Working in partnership Theoretical learning outcomes: • Discuss the implications of mentoring pre-registration student nurses in a current health care context. • Drawing on theories of education, examine the qualities involved in positive mentorship when supporting preregistration student nurses. • Given practice assessment documentation, explain how accurate completion of competency outcomes can assist students in developing their personal learning. • Using research literature and case scenarios, examine ways mentors can manage placement experiences when supporting failing students. Clinical learning outcomes: • Describe the integration of mentorship principles in the practice of supporting pre-registration student nurses in clinical experiences. • Reflect on the use of mentoring skills in practice, including identifying any limitations in discussions with course supervisor/ clinical mentor. fairness FAIRNE SSfairn NMC Standards and learning Challenge and support Accountability and risk taking Credible assessment bac k hom e
 Documentation quiz Working in partnership Mentorship documentation. 1. How far into the placement should the statement of intent be completed? 2. What essential elements should be included in the ‘Statement of intent? ’ 3. What is the purpose of the middle progress statement? 4. What would you include in the Statement of Progress/ Achievement at the end of the placement? 5. What length of placement requires a ‘short placement record? ’ 6. What is the purpose of the Professional Attitudes scale? 7. During a 6 week placement, how often would the Assessment of Professional Attitudes scale be completed? 8. When completing the Attitudes scale, how does the student and the mentor record levels of achievement? 9. What level of supervision do the following students require? 1 st year? 2 nd year? 3 rd year? 10. Where does the mentor sign when the practice outcome has been achieved? 11. Where does the mentor sign when there is progress towards achievement of practice outcome, but this has not been achieved fully? Suggested 12. What additional support is available for mentors? responses fairness FAIRNE SSfairn NMC Standards and learning Challenge and support Accountability and risk taking Credible assessment bac k hom e
Documentation quiz Working in partnership Mentorship documentation. 1. How far into the placement should the statement of intent be completed? 2. What essential elements should be included in the ‘Statement of intent? ’ 3. What is the purpose of the middle progress statement? 4. What would you include in the Statement of Progress/ Achievement at the end of the placement? 5. What length of placement requires a ‘short placement record? ’ 6. What is the purpose of the Professional Attitudes scale? 7. During a 6 week placement, how often would the Assessment of Professional Attitudes scale be completed? 8. When completing the Attitudes scale, how does the student and the mentor record levels of achievement? 9. What level of supervision do the following students require? 1 st year? 2 nd year? 3 rd year? 10. Where does the mentor sign when the practice outcome has been achieved? 11. Where does the mentor sign when there is progress towards achievement of practice outcome, but this has not been achieved fully? Suggested 12. What additional support is available for mentors? responses fairness FAIRNE SSfairn NMC Standards and learning Challenge and support Accountability and risk taking Credible assessment bac k hom e
 Documentation quiz responses Working in partnership 1. How far into the placement should the statement of intent be completed? Within 3 days. Importance of initial interview providing a foundation for the placement. Set dates for the middle and end interview. 2. What essential elements should be included in the ‘Statement of intent? ’ Clarification of learning opportunities in the Practice learning Environment in relation to the student’s expectations. Draw on the student’s prepared Self Assessment and Individual Action Plan in their Ongoing Record of Achievement. 3. What is the purpose of the middle progress statement? To provide constructive feedback as to how the student is progressing, clarify areas to work on for underachieving student as well as celebrating the work of students who are performing well. 4. What would you include in the Statement of Progress/ Achievement at the end of the placement? Telling the story of how the student has performed. Be specific rather than flowery. How has student functioned as a team member / towards patients, clients, service users / their professional behaviour. fairness FAIRNE SSfairn NMC Standards and learning Challenge and support Accountability and risk taking Credible assessment Next question bac k hom e
Documentation quiz responses Working in partnership 1. How far into the placement should the statement of intent be completed? Within 3 days. Importance of initial interview providing a foundation for the placement. Set dates for the middle and end interview. 2. What essential elements should be included in the ‘Statement of intent? ’ Clarification of learning opportunities in the Practice learning Environment in relation to the student’s expectations. Draw on the student’s prepared Self Assessment and Individual Action Plan in their Ongoing Record of Achievement. 3. What is the purpose of the middle progress statement? To provide constructive feedback as to how the student is progressing, clarify areas to work on for underachieving student as well as celebrating the work of students who are performing well. 4. What would you include in the Statement of Progress/ Achievement at the end of the placement? Telling the story of how the student has performed. Be specific rather than flowery. How has student functioned as a team member / towards patients, clients, service users / their professional behaviour. fairness FAIRNE SSfairn NMC Standards and learning Challenge and support Accountability and risk taking Credible assessment Next question bac k hom e
 Documentation quiz responses Working in partnership 5. What length of placement requires a ‘short placement record? ’ Currently three weeks and below. 6. What is the purpose of the Professional Attitudes scale? Assessing communication / Team working / Responding to individual needs. 7. During a 6 week placement, how often would the Assessment of Professional Attitudes scale be completed? Once mid way and once at the end of placement. 8. When completing the Attitudes scale, how does the student and the mentor record levels of achievement? Student completes with cross / mentor with a tick. Red pen for midway scoring and blue for end of placement. 9. What level of supervision do the following students require? 1 st year? Direct supervision / Demonstrate an understanding of rationales / using appropriate communication skills/ performing basic skills safely on the instruction of others. 2 nd year? Under supervision / Demonstrate initiative and confidence in performing nursing skills / increased problem solving skills / Communicating and reporting effectively. 3 rd year? Minimum supervision / Selecting and performing complex skills fairness FAIRNE consistently and safely / identifying more complex aspects of nursing care / articulating rationales SSfairn and justifying decisions. Next bac hom NMC Standards Challenge and Accountability Credible k e question and learning support and risk taking assessment
Documentation quiz responses Working in partnership 5. What length of placement requires a ‘short placement record? ’ Currently three weeks and below. 6. What is the purpose of the Professional Attitudes scale? Assessing communication / Team working / Responding to individual needs. 7. During a 6 week placement, how often would the Assessment of Professional Attitudes scale be completed? Once mid way and once at the end of placement. 8. When completing the Attitudes scale, how does the student and the mentor record levels of achievement? Student completes with cross / mentor with a tick. Red pen for midway scoring and blue for end of placement. 9. What level of supervision do the following students require? 1 st year? Direct supervision / Demonstrate an understanding of rationales / using appropriate communication skills/ performing basic skills safely on the instruction of others. 2 nd year? Under supervision / Demonstrate initiative and confidence in performing nursing skills / increased problem solving skills / Communicating and reporting effectively. 3 rd year? Minimum supervision / Selecting and performing complex skills fairness FAIRNE consistently and safely / identifying more complex aspects of nursing care / articulating rationales SSfairn and justifying decisions. Next bac hom NMC Standards Challenge and Accountability Credible k e question and learning support and risk taking assessment
 Documentation quiz responses Working in partnership 10. Where does the mentor sign when the practice outcome has been achieved? All relevant shaded boxes and the end box. 11. Where does the mentor sign when there is progress towards achievement of practice outcome, but this has not been achieved fully? Sign under ‘Progress towards but not achieved’ and complete progression statement. Sign and date. Importance of this in relation to overall record of achievement for student. 12. What additional support is available for mentors? Immediate colleagues within Practice Learning Environment Practice Facilitators Link tutor Link mentor fairness FAIRNE SSfairn NMC Standards and learning Challenge and support Accountability and risk taking Credible assessment bac k hom e
Documentation quiz responses Working in partnership 10. Where does the mentor sign when the practice outcome has been achieved? All relevant shaded boxes and the end box. 11. Where does the mentor sign when there is progress towards achievement of practice outcome, but this has not been achieved fully? Sign under ‘Progress towards but not achieved’ and complete progression statement. Sign and date. Importance of this in relation to overall record of achievement for student. 12. What additional support is available for mentors? Immediate colleagues within Practice Learning Environment Practice Facilitators Link tutor Link mentor fairness FAIRNE SSfairn NMC Standards and learning Challenge and support Accountability and risk taking Credible assessment bac k hom e
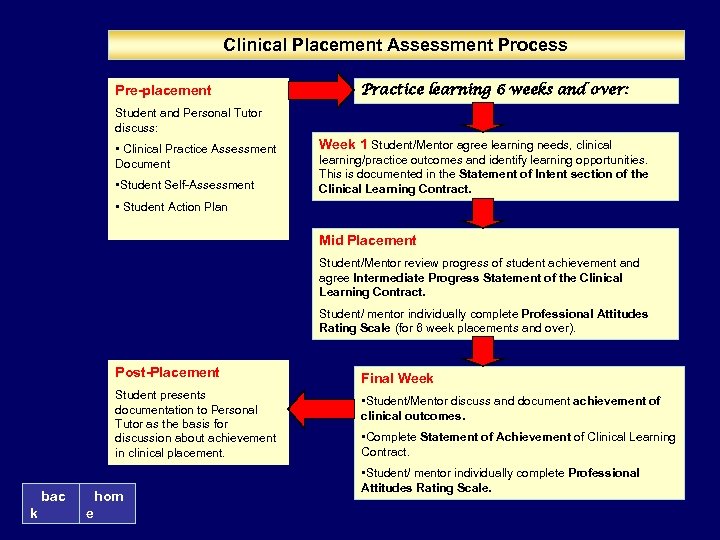 Clinical Placement Assessment Process Pre-placement Practice learning 6 weeks and over: Student and Personal Tutor discuss: • Clinical Practice Assessment Document • Student Self-Assessment Week 1 Student/Mentor agree learning needs, clinical learning/practice outcomes and identify learning opportunities. This is documented in the Statement of Intent section of the Clinical Learning Contract. • Student Action Plan Mid Placement Student/Mentor review progress of student achievement and agree Intermediate Progress Statement of the Clinical Learning Contract. Student/ mentor individually complete Professional Attitudes Rating Scale (for 6 week placements and over). Post-Placement Student presents documentation to Personal Tutor as the basis for discussion about achievement in clinical placement. bac k Final Week • Student/Mentor discuss and document achievement of clinical outcomes. hom e • Complete Statement of Achievement of Clinical Learning Contract. • Student/ mentor individually complete Professional Attitudes Rating Scale.
Clinical Placement Assessment Process Pre-placement Practice learning 6 weeks and over: Student and Personal Tutor discuss: • Clinical Practice Assessment Document • Student Self-Assessment Week 1 Student/Mentor agree learning needs, clinical learning/practice outcomes and identify learning opportunities. This is documented in the Statement of Intent section of the Clinical Learning Contract. • Student Action Plan Mid Placement Student/Mentor review progress of student achievement and agree Intermediate Progress Statement of the Clinical Learning Contract. Student/ mentor individually complete Professional Attitudes Rating Scale (for 6 week placements and over). Post-Placement Student presents documentation to Personal Tutor as the basis for discussion about achievement in clinical placement. bac k Final Week • Student/Mentor discuss and document achievement of clinical outcomes. hom e • Complete Statement of Achievement of Clinical Learning Contract. • Student/ mentor individually complete Professional Attitudes Rating Scale.
 A dialogue Working in partnership A reconstructed narrative presented here, identifies ‘counselling skills’ to assist another individual orientate themselves to the issues they are conveying. Despite not expressly promoting therapeutic healing, the dialogue nevertheless incorporates important aspects of counselling. Although set up as a real conversation the narrative is reconstructed from an unpremeditated interaction between a Practice Facilitator and a nurse mentor. This reconstruction followed shortly after the actual discussion with the mentor as part of the author’s ongoing reflective practice. Whilst this does not allow for a literal reproduction of what was said, key words and phrases convey a representation of important moments in the dialogue. The narrative acts as a platform to explore the intricacies of assessment decision making occurring within clinical nursing settings. All contextual information has been disguised to protect any possible compromise of anonymity of individuals concerned. Likewise, permission was sought and granted from the mentor to reproduce this version of the conversation. Continued fairness FAIRNE SSfairn NMC Standards and learning Challenge and support Accountability and risk taking Credible assessment bac k hom e
A dialogue Working in partnership A reconstructed narrative presented here, identifies ‘counselling skills’ to assist another individual orientate themselves to the issues they are conveying. Despite not expressly promoting therapeutic healing, the dialogue nevertheless incorporates important aspects of counselling. Although set up as a real conversation the narrative is reconstructed from an unpremeditated interaction between a Practice Facilitator and a nurse mentor. This reconstruction followed shortly after the actual discussion with the mentor as part of the author’s ongoing reflective practice. Whilst this does not allow for a literal reproduction of what was said, key words and phrases convey a representation of important moments in the dialogue. The narrative acts as a platform to explore the intricacies of assessment decision making occurring within clinical nursing settings. All contextual information has been disguised to protect any possible compromise of anonymity of individuals concerned. Likewise, permission was sought and granted from the mentor to reproduce this version of the conversation. Continued fairness FAIRNE SSfairn NMC Standards and learning Challenge and support Accountability and risk taking Credible assessment bac k hom e
 A dialogue continued……. Working in partnership Also, the narrative spotlights one part of an ongoing support network involving relevant Higher Education Institution personnel, the author, mentors and students. The discussion leads to a suggestion that making sense of mentoring experiences by examining personal counselling skills helps establish connections between what may otherwise remain disparate narratives (Rashotte, 2005). Hence, the process of dissection and reassembly of unique personal stories co-constructed with others assists those involved in reframing their personal approach. The dialogue highlighted here, focuses on strategies that may assist mentors and other key players enhance the validity and reliability of their assessment decisions…………………. . Continued fairness FAIRNE SSfairn NMC Standards and learning Challenge and support Accountability and risk taking Credible assessment bac k hom e
A dialogue continued……. Working in partnership Also, the narrative spotlights one part of an ongoing support network involving relevant Higher Education Institution personnel, the author, mentors and students. The discussion leads to a suggestion that making sense of mentoring experiences by examining personal counselling skills helps establish connections between what may otherwise remain disparate narratives (Rashotte, 2005). Hence, the process of dissection and reassembly of unique personal stories co-constructed with others assists those involved in reframing their personal approach. The dialogue highlighted here, focuses on strategies that may assist mentors and other key players enhance the validity and reliability of their assessment decisions…………………. . Continued fairness FAIRNE SSfairn NMC Standards and learning Challenge and support Accountability and risk taking Credible assessment bac k hom e
![A dialogue continued……. Working in partnership Mentor [Sue]: ‘‘I really need to speak to A dialogue continued……. Working in partnership Mentor [Sue]: ‘‘I really need to speak to](https://present5.com/presentation/6743a9a61d93d9645ddd77caad5f5d82/image-71.jpg) A dialogue continued……. Working in partnership Mentor [Sue]: ‘‘I really need to speak to you about one of the students. It’s a bit delicate. ’’ Practice Facilitator: ”I can see you’re worried Sue. Is there somewhere private we can go? ’’ The dialogue is set in a bathroom area. The bathroom is commonly used for ward handovers as the office is compact and interruptions more likely. Whilst it might have been logical to arrange another mutually convenient time and though somewhat unusual, the decision to carry on the conversation in the bathroom is made more pertinent by Sue’s frustration. PF ‘‘I bet you never thought when you did your nurse training that you would be in a bathroom talking about the finer points of student assessment? ’’ Sue: ‘‘I’ve been in a lot worse places during my nursing career!’’ PF: ‘‘I suppose that’s what makes nursing so different from other types of training. There’s something about having to make pragmatic decisions in order to get things done. Sue: ‘‘Yeah, I feel a bit like that having drawn the short straw being the mentor for this particular student. . . It’s like we’re sitting on the edge of the bath hoping neither of us falls in. ’’ PF: ‘‘I’m not sure if I will have any easy solutions to the concerns you may have Sue, but I want you to know that I am a willing participant here. I’m offering to help as a confidential listener and supporter in your role as a mentor…………. ’’ Continued fairness FAIRNE SSfairn NMC Standards and learning Challenge and support Accountability and risk taking Credible assessment bac k hom e
A dialogue continued……. Working in partnership Mentor [Sue]: ‘‘I really need to speak to you about one of the students. It’s a bit delicate. ’’ Practice Facilitator: ”I can see you’re worried Sue. Is there somewhere private we can go? ’’ The dialogue is set in a bathroom area. The bathroom is commonly used for ward handovers as the office is compact and interruptions more likely. Whilst it might have been logical to arrange another mutually convenient time and though somewhat unusual, the decision to carry on the conversation in the bathroom is made more pertinent by Sue’s frustration. PF ‘‘I bet you never thought when you did your nurse training that you would be in a bathroom talking about the finer points of student assessment? ’’ Sue: ‘‘I’ve been in a lot worse places during my nursing career!’’ PF: ‘‘I suppose that’s what makes nursing so different from other types of training. There’s something about having to make pragmatic decisions in order to get things done. Sue: ‘‘Yeah, I feel a bit like that having drawn the short straw being the mentor for this particular student. . . It’s like we’re sitting on the edge of the bath hoping neither of us falls in. ’’ PF: ‘‘I’m not sure if I will have any easy solutions to the concerns you may have Sue, but I want you to know that I am a willing participant here. I’m offering to help as a confidential listener and supporter in your role as a mentor…………. ’’ Continued fairness FAIRNE SSfairn NMC Standards and learning Challenge and support Accountability and risk taking Credible assessment bac k hom e
 A dialogue continued……. Working in partnership Sue: ‘‘I appreciate that but I just feel I’ve been given this student because no-one else wants to act as the mentor. Lisa [student] is not performing to the level you would expect of someone who is due to qualify in a couple of months. She has come to me because the mentor who was assigned to her at the beginning of the placement has gone sick and the Ward Sister felt I was the most experienced to take her on. ’’ PF: ‘‘I get a sense that you are a bit disgruntled at being given the mentor role having drawn the ‘short straw’ as you put it. Do you want to say a bit more about that Sue? ’’ Sue: ‘‘It’s not that I shy away from giving honest appraisal to students. I realise the importance of being accountable for my decisions as a mentor and I will go out of my way to support students. I’m just not sure about Lisa’s attitude to the rest of the team and I’m worried there is not a lot of time left to assess her properly. ’’ PF: ‘‘Uh hmm. . Go on. ’’ Sue: ‘‘Well, she’s safe enough administering medication and is dedicated towards the patients, she just seems so sure of herself. It’s like she knows everything. If I check with her that she has completed a certain task she immediately becomes defensive, even hostile. ’’ PF: ‘‘Hostile……………? ’’ Continued fairness FAIRNE SSfairn NMC Standards and learning Challenge and support Accountability and risk taking Credible assessment bac k hom e
A dialogue continued……. Working in partnership Sue: ‘‘I appreciate that but I just feel I’ve been given this student because no-one else wants to act as the mentor. Lisa [student] is not performing to the level you would expect of someone who is due to qualify in a couple of months. She has come to me because the mentor who was assigned to her at the beginning of the placement has gone sick and the Ward Sister felt I was the most experienced to take her on. ’’ PF: ‘‘I get a sense that you are a bit disgruntled at being given the mentor role having drawn the ‘short straw’ as you put it. Do you want to say a bit more about that Sue? ’’ Sue: ‘‘It’s not that I shy away from giving honest appraisal to students. I realise the importance of being accountable for my decisions as a mentor and I will go out of my way to support students. I’m just not sure about Lisa’s attitude to the rest of the team and I’m worried there is not a lot of time left to assess her properly. ’’ PF: ‘‘Uh hmm. . Go on. ’’ Sue: ‘‘Well, she’s safe enough administering medication and is dedicated towards the patients, she just seems so sure of herself. It’s like she knows everything. If I check with her that she has completed a certain task she immediately becomes defensive, even hostile. ’’ PF: ‘‘Hostile……………? ’’ Continued fairness FAIRNE SSfairn NMC Standards and learning Challenge and support Accountability and risk taking Credible assessment bac k hom e
 A dialogue continued……. Working in partnership Sue: ‘‘Yes, I’ve wondered if it’s that Lisa is afraid of making a mistake, as though she needs to be some kind of perfect nurse and that’s why she reacts badly when people ask her to clarify things about her practice. ’’ PF: ‘‘I’m hesitating to jump to any conclusions Sue, but something that really strikes me are your thoughts about Lisa aspiring to perfection and that this might be a reason for her defensiveness. It’s a tempting theory, almost as if her own anxieties about needing to be seen to be doing well are actually acting as a barrier to her learning. ’’ Sue: ‘‘Maybe. I’m not sure. You see she does do many things very well. The main concerns are about how she will be able to work with others should she qualify. It’s not just knowing about the technical stuff in nursing that’s important. ’’ PF: ‘‘Yes. . . no easy answers. ’’ Sue: ‘‘I wish there were some. ’’ PF: ‘‘You’ve covered a lot of ground in our conversation already Sue. What does shine through though is your dedication to Lisa despite the difficulties you have. ” fairness FAIRNE SSfairn NMC Standards and learning Challenge and support Accountability and risk taking Credible assessment bac k hom e
A dialogue continued……. Working in partnership Sue: ‘‘Yes, I’ve wondered if it’s that Lisa is afraid of making a mistake, as though she needs to be some kind of perfect nurse and that’s why she reacts badly when people ask her to clarify things about her practice. ’’ PF: ‘‘I’m hesitating to jump to any conclusions Sue, but something that really strikes me are your thoughts about Lisa aspiring to perfection and that this might be a reason for her defensiveness. It’s a tempting theory, almost as if her own anxieties about needing to be seen to be doing well are actually acting as a barrier to her learning. ’’ Sue: ‘‘Maybe. I’m not sure. You see she does do many things very well. The main concerns are about how she will be able to work with others should she qualify. It’s not just knowing about the technical stuff in nursing that’s important. ’’ PF: ‘‘Yes. . . no easy answers. ’’ Sue: ‘‘I wish there were some. ’’ PF: ‘‘You’ve covered a lot of ground in our conversation already Sue. What does shine through though is your dedication to Lisa despite the difficulties you have. ” fairness FAIRNE SSfairn NMC Standards and learning Challenge and support Accountability and risk taking Credible assessment bac k hom e
 Newsletter Partnership Accountability Credibility Trust Working in partnership Mentorship Matters: A quarterly newsletter for mentors Issue Sept 2010 Welcome to the September edition of our quarterly newsletter. Our aim is to provide forum where we can share news, advice and support with mentors across the ABM University Trust. Please contact us with your news and ideas. Difficult times The current financial climate for ABM University Trust has produced particular challenges for nurses to maintain high standards of care, teaching and assessment. Mentorship of student nurses remains a crucial aspect for the future workforce of nursing, yet the commitment, time and investment required of mentors is a challenge given present resource pressures. At the same time there is substantial evidence (student evaluations, practice facilitator observations, mentor discussions) that despite current difficulties, mentors continue to have a positive view of mentorship across all Directorates, want to do right by students and that students are still receiving high quality mentorship. This is to be commended in a time of increased challenges. fairness FAIRNE SSfairn NMC Standards and learning Challenge and support Accountability and risk taking Credible assessment Forward bac k hom e
Newsletter Partnership Accountability Credibility Trust Working in partnership Mentorship Matters: A quarterly newsletter for mentors Issue Sept 2010 Welcome to the September edition of our quarterly newsletter. Our aim is to provide forum where we can share news, advice and support with mentors across the ABM University Trust. Please contact us with your news and ideas. Difficult times The current financial climate for ABM University Trust has produced particular challenges for nurses to maintain high standards of care, teaching and assessment. Mentorship of student nurses remains a crucial aspect for the future workforce of nursing, yet the commitment, time and investment required of mentors is a challenge given present resource pressures. At the same time there is substantial evidence (student evaluations, practice facilitator observations, mentor discussions) that despite current difficulties, mentors continue to have a positive view of mentorship across all Directorates, want to do right by students and that students are still receiving high quality mentorship. This is to be commended in a time of increased challenges. fairness FAIRNE SSfairn NMC Standards and learning Challenge and support Accountability and risk taking Credible assessment Forward bac k hom e
 Newsletter Partnership Accountability Credibility Trust Working in partnership NMC Standards The NMC standards to support learning & assessment in practice are now in place. These standards have introduce some key changes to the way in which nurses meet and maintain their status as mentors for pre-registration nursing and midwifery students. Since the original introduction of the standards there have been some revisions in the form of NMC circulars. These are now incorporated into a revised document with a different cover. The Standards can be accessed via the NMC web site or on the Mentor intranet site of ABM NHS Trust (see below). Significant elements of the Standards include mentors needing to update themselves on an annual basis, a revised system of mentor preparation and the introduction of ‘sign-off’ mentors to support students in the last three months of their nurse training. The Health Board has developed a portfolio to support mentors in recording their mentorship activity, copies of which are available from Practice Facilitators (see contact details below) or from the ABM University Health Board mentor intranet site. fairness FAIRNE SSfairn NMC Standards and learning Challenge and support Accountability and risk taking Credible assessment Forward bac k hom e
Newsletter Partnership Accountability Credibility Trust Working in partnership NMC Standards The NMC standards to support learning & assessment in practice are now in place. These standards have introduce some key changes to the way in which nurses meet and maintain their status as mentors for pre-registration nursing and midwifery students. Since the original introduction of the standards there have been some revisions in the form of NMC circulars. These are now incorporated into a revised document with a different cover. The Standards can be accessed via the NMC web site or on the Mentor intranet site of ABM NHS Trust (see below). Significant elements of the Standards include mentors needing to update themselves on an annual basis, a revised system of mentor preparation and the introduction of ‘sign-off’ mentors to support students in the last three months of their nurse training. The Health Board has developed a portfolio to support mentors in recording their mentorship activity, copies of which are available from Practice Facilitators (see contact details below) or from the ABM University Health Board mentor intranet site. fairness FAIRNE SSfairn NMC Standards and learning Challenge and support Accountability and risk taking Credible assessment Forward bac k hom e
 Newsletter Partnership Accountability Credibility Trust Working in partnership Creating a learning environment & educational audit It is good practice to educationally audit your areas on an annual basis. Audits are formally required every three years. Should your area be due an educational audit and you are unfamiliar with the process, please contact a Practice Facilitator who will guide you through the process. Could you put your hand on your educational audit? The Educational Audit document needs to be reviewed by a Link Tutor from the University of Glamorgan every 3 years. This document details the numbers of students coming to your clinical area and what stage of their training they are placed with you. There also a number of educational standards which act as a benchmark of educational quality. Mentor Intranet Site. The Mentor site is now available on the Trust intranet system (Home page below). The mentor pages contain a wide range of information and materials relating to registered nurse mentor assessment of pre-registration student nurses and midwives in clinical practice. Training dates for mentor updates and mentor preparation courses for 2010 are on the site together with distance learning activities related directly to mentorship. fairness FAIRNE SSfairn NMC Standards and learning Challenge and support Accountability and risk taking Credible assessment Forward bac k hom e
Newsletter Partnership Accountability Credibility Trust Working in partnership Creating a learning environment & educational audit It is good practice to educationally audit your areas on an annual basis. Audits are formally required every three years. Should your area be due an educational audit and you are unfamiliar with the process, please contact a Practice Facilitator who will guide you through the process. Could you put your hand on your educational audit? The Educational Audit document needs to be reviewed by a Link Tutor from the University of Glamorgan every 3 years. This document details the numbers of students coming to your clinical area and what stage of their training they are placed with you. There also a number of educational standards which act as a benchmark of educational quality. Mentor Intranet Site. The Mentor site is now available on the Trust intranet system (Home page below). The mentor pages contain a wide range of information and materials relating to registered nurse mentor assessment of pre-registration student nurses and midwives in clinical practice. Training dates for mentor updates and mentor preparation courses for 2010 are on the site together with distance learning activities related directly to mentorship. fairness FAIRNE SSfairn NMC Standards and learning Challenge and support Accountability and risk taking Credible assessment Forward bac k hom e
 Newsletter Partnership Accountability Credibility Trust Working in partnership Mentor Intranet Site. The Mentor site is now available on the Trust intranet system (Home page below). The mentor pages contain a wide range of information and materials relating to registered nurse mentor assessment of preregistration student nurses and midwives in clinical practice. Training dates for mentor updates and mentor preparation courses for 2010 are on the site together with distance learning activities related directly to mentorship. Notice Board A notice board is also now located at the entrance to the Oasis restaurant on the top corridor of the Princess of Wales Hospital containing information about available support and advice for mentors as well as training dates. Contacts Each clinical area has a designated Practice Facilitator. They provide the link between the Higher Education Institutes and the practice placements. They provide direct advice and support when there are issues about students who are on the borderline of achievement. Contact Simon Cassidy and Kay Jones Based at Office 4 Multi Professional Education Centre Princess of Wales Hospital Tel 01656 722557 e-mail: simon. cassidy@wales. nhs. uk ; kay. jones@wales. nhs. uk fairness FAIRNE SSfairn NMC Standards and learning Challenge and support Accountability and risk taking Credible assessment bac k hom e
Newsletter Partnership Accountability Credibility Trust Working in partnership Mentor Intranet Site. The Mentor site is now available on the Trust intranet system (Home page below). The mentor pages contain a wide range of information and materials relating to registered nurse mentor assessment of preregistration student nurses and midwives in clinical practice. Training dates for mentor updates and mentor preparation courses for 2010 are on the site together with distance learning activities related directly to mentorship. Notice Board A notice board is also now located at the entrance to the Oasis restaurant on the top corridor of the Princess of Wales Hospital containing information about available support and advice for mentors as well as training dates. Contacts Each clinical area has a designated Practice Facilitator. They provide the link between the Higher Education Institutes and the practice placements. They provide direct advice and support when there are issues about students who are on the borderline of achievement. Contact Simon Cassidy and Kay Jones Based at Office 4 Multi Professional Education Centre Princess of Wales Hospital Tel 01656 722557 e-mail: simon. cassidy@wales. nhs. uk ; kay. jones@wales. nhs. uk fairness FAIRNE SSfairn NMC Standards and learning Challenge and support Accountability and risk taking Credible assessment bac k hom e
 Forum Partnership Accountability Credibility Trust Working in partnership Download a copy of the latest Mentor Link Forum on the Mentorship categories page fairness FAIRNE SSfairn NMC Standards and learning Challenge and support Accountability and risk taking Credible assessment bac k hom e
Forum Partnership Accountability Credibility Trust Working in partnership Download a copy of the latest Mentor Link Forum on the Mentorship categories page fairness FAIRNE SSfairn NMC Standards and learning Challenge and support Accountability and risk taking Credible assessment bac k hom e


