Amenorrhoea Dr Fida.pptx
- Количество слайдов: 52
 Menstrual cycle and Amenorrhea Dr Fida Al-Asali
Menstrual cycle and Amenorrhea Dr Fida Al-Asali
 Menstrual cycle: Regular occurrence of ovulation throughout a woman’s reproductive cycle which is: Predictable - Cyclic- Spontaneous Regulated by complex interactions of: Hypothalamic/pituitary axis – Ovaries -Genital tract
Menstrual cycle: Regular occurrence of ovulation throughout a woman’s reproductive cycle which is: Predictable - Cyclic- Spontaneous Regulated by complex interactions of: Hypothalamic/pituitary axis – Ovaries -Genital tract
 Length of cycle The mean length of the cycle is 28 days ± 7 days • Polymenorrhoea: cycles that occur at short intervals (less than 21 days) • Oligomenorrhoea: cycles that occur at long intervals (more than 35 days) • Menstrual cycles are most irregular during times of anovulation (2 years after menarche and 3 years before manopause)
Length of cycle The mean length of the cycle is 28 days ± 7 days • Polymenorrhoea: cycles that occur at short intervals (less than 21 days) • Oligomenorrhoea: cycles that occur at long intervals (more than 35 days) • Menstrual cycles are most irregular during times of anovulation (2 years after menarche and 3 years before manopause)
 Classic phases of the menstrual cycles • Proliferative(Follicular) • Secretory(luteal) • Menstrual
Classic phases of the menstrual cycles • Proliferative(Follicular) • Secretory(luteal) • Menstrual
 Follicular (proliferative) phase • Lasts from 1 st day of menses until ovulation • Endometrial glands proliferate under influence of oestrogen
Follicular (proliferative) phase • Lasts from 1 st day of menses until ovulation • Endometrial glands proliferate under influence of oestrogen
 Luteal (secretory) phase • Extends from ovulation until the onset of menses • Endometrial glands develop secretory status necessary for implantation of the embryo under influence of progesterone
Luteal (secretory) phase • Extends from ovulation until the onset of menses • Endometrial glands develop secretory status necessary for implantation of the embryo under influence of progesterone
 Cycle interaction Gn. RH Gonadotropins - FSH - LH Sex steroids -Androstenedione - Esradiol - Estrone - Progesterone
Cycle interaction Gn. RH Gonadotropins - FSH - LH Sex steroids -Androstenedione - Esradiol - Estrone - Progesterone
 Normal menstrual cycle • • • Count from 1 st day of flow Normal 21 -35 days The perfect 28 days in only 15% Duration of blood flow 4 -6 days (2 -8 days) Average blood loss 30 ml >80 ml menorrhagia Constant 14 day luteal phase Most of anovulatory cycles <20 or >40 yr age Amount of flow dependent on how rapid endometrium sheds
Normal menstrual cycle • • • Count from 1 st day of flow Normal 21 -35 days The perfect 28 days in only 15% Duration of blood flow 4 -6 days (2 -8 days) Average blood loss 30 ml >80 ml menorrhagia Constant 14 day luteal phase Most of anovulatory cycles <20 or >40 yr age Amount of flow dependent on how rapid endometrium sheds
 Amenorrhea Definitions
Amenorrhea Definitions
 Definitions Primary Secondary Absence of No menstruation menses for 6 by age 14 years No menstruation months (or greater accompanied by by age 16 when than 3 times the failure to grow previous cycle growth and sexual properly or intervals) in a development are develop secondary women who has normal sexual menstruated characteristics before
Definitions Primary Secondary Absence of No menstruation menses for 6 by age 14 years No menstruation months (or greater accompanied by by age 16 when than 3 times the failure to grow previous cycle growth and sexual properly or intervals) in a development are develop secondary women who has normal sexual menstruated characteristics before
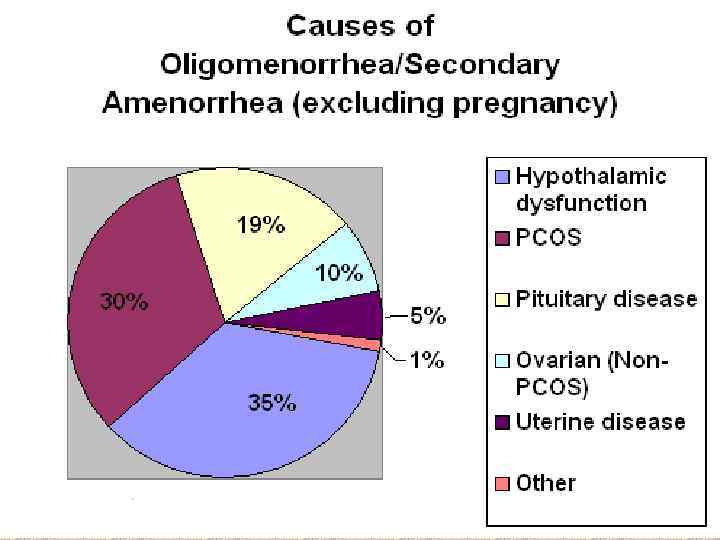
 Causes
Causes
 Causes of primary amenorrhoea Chromosomal XO- Tuner syndrome 46, XY DSD Ovotesticular DSD Hypothalamic Physiological delay Weight loss/ anorexia/ heavy exercise Isolated Gn. RH deficiency Congenital CNS defects Intracranial tumours Pituitary Partial/ total hypopituitarism Hyperproalactinaemia Pituitary adenoma Empty sella syndrome Trauma/ surgery
Causes of primary amenorrhoea Chromosomal XO- Tuner syndrome 46, XY DSD Ovotesticular DSD Hypothalamic Physiological delay Weight loss/ anorexia/ heavy exercise Isolated Gn. RH deficiency Congenital CNS defects Intracranial tumours Pituitary Partial/ total hypopituitarism Hyperproalactinaemia Pituitary adenoma Empty sella syndrome Trauma/ surgery
 Causes of primary amenorrhoea (continued) Ovarian True agenesis Premature ovarian failure Radiation/ chemotherapy/ autoimmune Polycystic ovaries Virilizing ovarian tumours Other endocrine Primary hypothyroidism Adrenal hyperplasia Adrenal tumour Uterine/ vaginal Imperforate hymen Uterovaginal agenesis
Causes of primary amenorrhoea (continued) Ovarian True agenesis Premature ovarian failure Radiation/ chemotherapy/ autoimmune Polycystic ovaries Virilizing ovarian tumours Other endocrine Primary hypothyroidism Adrenal hyperplasia Adrenal tumour Uterine/ vaginal Imperforate hymen Uterovaginal agenesis
 Causes of secondary amenorrhoea Physiological Pregnancy Lactation Menopause Hypothalamic Weight loss/ anorexia Heavy exercise Stress Pituitary Hyperproalactinaemia Partial/ total hypopituitarism Sheehan’s syndrome Trauma/ surgery
Causes of secondary amenorrhoea Physiological Pregnancy Lactation Menopause Hypothalamic Weight loss/ anorexia Heavy exercise Stress Pituitary Hyperproalactinaemia Partial/ total hypopituitarism Sheehan’s syndrome Trauma/ surgery
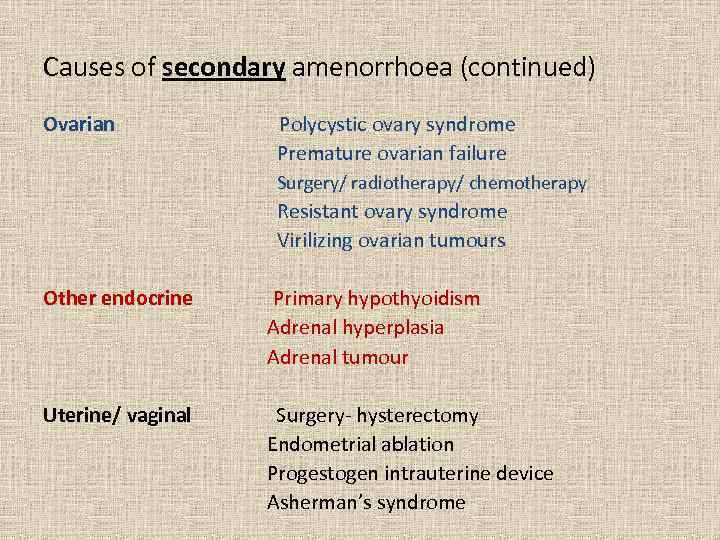 Causes of secondary amenorrhoea (continued) Ovarian Polycystic ovary syndrome Premature ovarian failure Surgery/ radiotherapy/ chemotherapy Resistant ovary syndrome Virilizing ovarian tumours Other endocrine Primary hypothyoidism Adrenal hyperplasia Adrenal tumour Uterine/ vaginal Surgery- hysterectomy Endometrial ablation Progestogen intrauterine device Asherman’s syndrome
Causes of secondary amenorrhoea (continued) Ovarian Polycystic ovary syndrome Premature ovarian failure Surgery/ radiotherapy/ chemotherapy Resistant ovary syndrome Virilizing ovarian tumours Other endocrine Primary hypothyoidism Adrenal hyperplasia Adrenal tumour Uterine/ vaginal Surgery- hysterectomy Endometrial ablation Progestogen intrauterine device Asherman’s syndrome
 Disorders of outflow tract and/or uterus Disorders of the ovary Causes Disorders of the hypothalamus Disorders of the anterior pituitary
Disorders of outflow tract and/or uterus Disorders of the ovary Causes Disorders of the hypothalamus Disorders of the anterior pituitary
 Disorders of outflow tract and/or uterus
Disorders of outflow tract and/or uterus
 Cryptomenorroea Absence or hypoplasia of vagina Testicular feminisation Asherman’s syndrome Infections
Cryptomenorroea Absence or hypoplasia of vagina Testicular feminisation Asherman’s syndrome Infections
 Cryptomenorrhoea • Vaginal atresia or an imperforate hymen prevents menstrual loss • Features; primary amenorrhoea in a teenage girl with normal sexual development complaining of; - intermittent abdominal pain - difficulty with micturition - palpable lower abdominal swelling - bulging, bluish membrane at lower vagina • Management: Incise membrane under aseptic conditions
Cryptomenorrhoea • Vaginal atresia or an imperforate hymen prevents menstrual loss • Features; primary amenorrhoea in a teenage girl with normal sexual development complaining of; - intermittent abdominal pain - difficulty with micturition - palpable lower abdominal swelling - bulging, bluish membrane at lower vagina • Management: Incise membrane under aseptic conditions
 Absence or hypoplasia of vagina • Features; - growth, development and ovarian function are usually normal - uterus is usually absent (if only lower 1/3 of vagina has developed) but maybe normal or rudimentary - renal anomalies (30%) - skeletal defects (10%) • Management; a functional vagina can be created by surgery or dilators
Absence or hypoplasia of vagina • Features; - growth, development and ovarian function are usually normal - uterus is usually absent (if only lower 1/3 of vagina has developed) but maybe normal or rudimentary - renal anomalies (30%) - skeletal defects (10%) • Management; a functional vagina can be created by surgery or dilators
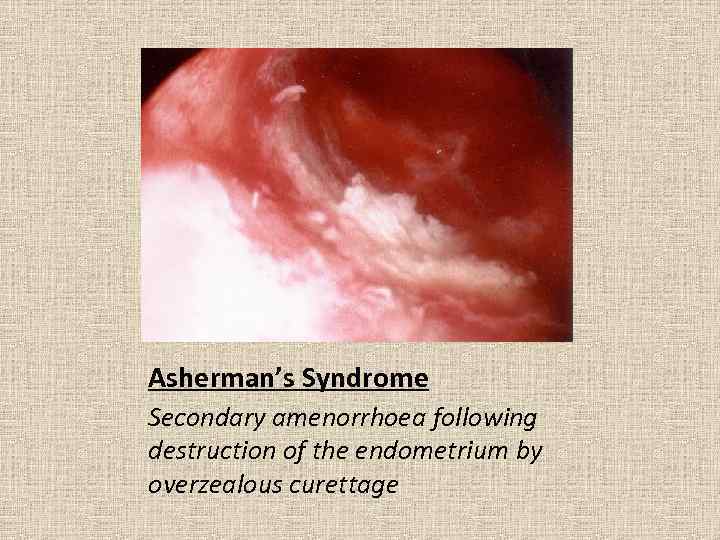 Asherman’s Syndrome Secondary amenorrhoea following destruction of the endometrium by overzealous curettage
Asherman’s Syndrome Secondary amenorrhoea following destruction of the endometrium by overzealous curettage
 Multiple synechiae show up on hysterography
Multiple synechiae show up on hysterography
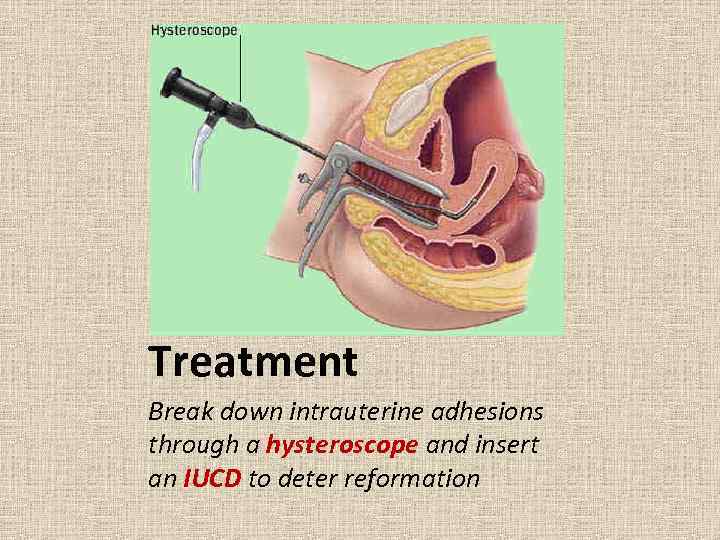 Treatment Break down intrauterine adhesions through a hysteroscope and insert an IUCD to deter reformation
Treatment Break down intrauterine adhesions through a hysteroscope and insert an IUCD to deter reformation
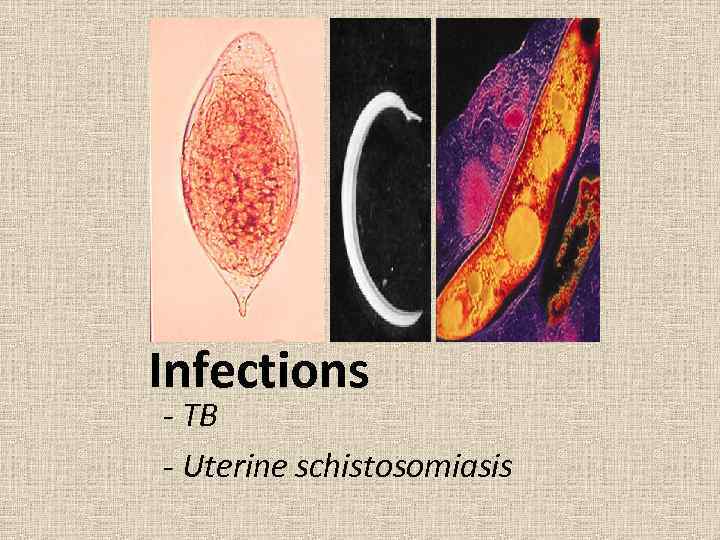 Infections - TB - Uterine schistosomiasis
Infections - TB - Uterine schistosomiasis
 Disorders of the ovary
Disorders of the ovary
 Disorders of the ovary 1. Chromosomal abnormalities 2. Failure of gonadal development 3. Resistant ovary syndrome 4. Premature menopause
Disorders of the ovary 1. Chromosomal abnormalities 2. Failure of gonadal development 3. Resistant ovary syndrome 4. Premature menopause
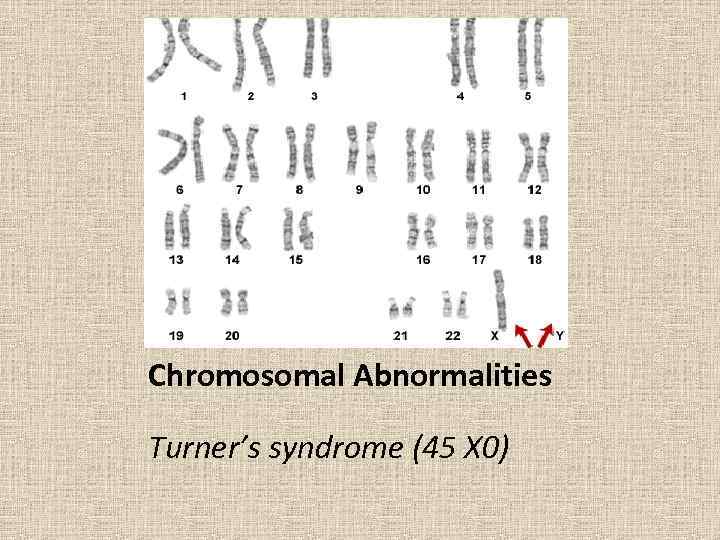 Chromosomal Abnormalities Turner’s syndrome (45 X 0)
Chromosomal Abnormalities Turner’s syndrome (45 X 0)
 Gonadal agenesis There is no gonadal tissue No other congenital abnormality Phenotype is female Karyotype can be either 46 XX or 46 XY
Gonadal agenesis There is no gonadal tissue No other congenital abnormality Phenotype is female Karyotype can be either 46 XX or 46 XY
 Premature menopause Ovarian failure before the age of 40 years Occurs in 1% of women Maybe due to; autoimmune disease (addison’s disease) viral infection (mumps) cytotoxic drugs post-radiotherapy (for Hodgkin’s disease)
Premature menopause Ovarian failure before the age of 40 years Occurs in 1% of women Maybe due to; autoimmune disease (addison’s disease) viral infection (mumps) cytotoxic drugs post-radiotherapy (for Hodgkin’s disease)
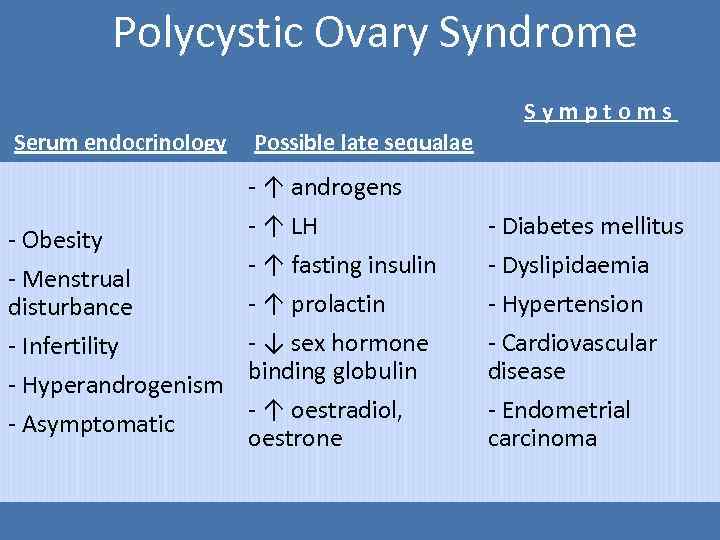 Polycystic Ovary Syndrome Symptoms Serum endocrinology - Obesity - Menstrual disturbance - Infertility - Hyperandrogenism - Asymptomatic Possible late sequalae - ↑ androgens - ↑ LH - ↑ fasting insulin - ↑ prolactin - ↓ sex hormone binding globulin - ↑ oestradiol, oestrone - Diabetes mellitus - Dyslipidaemia - Hypertension - Cardiovascular disease - Endometrial carcinoma
Polycystic Ovary Syndrome Symptoms Serum endocrinology - Obesity - Menstrual disturbance - Infertility - Hyperandrogenism - Asymptomatic Possible late sequalae - ↑ androgens - ↑ LH - ↑ fasting insulin - ↑ prolactin - ↓ sex hormone binding globulin - ↑ oestradiol, oestrone - Diabetes mellitus - Dyslipidaemia - Hypertension - Cardiovascular disease - Endometrial carcinoma
 Disorders of the pituitary
Disorders of the pituitary
 Disorders of the pituitary 1. Pituitary tumours causing hyperprolactinaemia 2. Other causes of hyperprolactinaeima 3. Sheehan’s syndrome
Disorders of the pituitary 1. Pituitary tumours causing hyperprolactinaemia 2. Other causes of hyperprolactinaeima 3. Sheehan’s syndrome
 Pituitary tumours causing hyperprolactinaemia • About 40% of women with hyperprolactinaemia will have a pituitary adenoma • Pituitary fossa X-rays must be taken in all cases of amenorrhoea • If X-rays suggest any abnormality such as - erosion of the clinoid processes - enlargement of the fossa - double flooring of the fossa CT AND MRI SCANNING AND ASSESSMENT OF THE VISUAL FIELDS ARE NECESSARY
Pituitary tumours causing hyperprolactinaemia • About 40% of women with hyperprolactinaemia will have a pituitary adenoma • Pituitary fossa X-rays must be taken in all cases of amenorrhoea • If X-rays suggest any abnormality such as - erosion of the clinoid processes - enlargement of the fossa - double flooring of the fossa CT AND MRI SCANNING AND ASSESSMENT OF THE VISUAL FIELDS ARE NECESSARY
 Bromocriptine Actions - Suppress prolactin secretion - Reduces the size of most prolactinomas Dosage Should be increased slowly over several weeks to minimise the side-effects Side-effects Postural hypotension Role of surgery Removal of tumours is now confined to; - patients with extrasellar manifestations (pressure on the optic chiasma) - patients who do not respond to or can not tolerate dopamine agonist
Bromocriptine Actions - Suppress prolactin secretion - Reduces the size of most prolactinomas Dosage Should be increased slowly over several weeks to minimise the side-effects Side-effects Postural hypotension Role of surgery Removal of tumours is now confined to; - patients with extrasellar manifestations (pressure on the optic chiasma) - patients who do not respond to or can not tolerate dopamine agonist
 Cabergoline - Potent dopamine receptor agonist on D 2 receptors - Second line agent in prolactinomas when bromocriptine is ineffective
Cabergoline - Potent dopamine receptor agonist on D 2 receptors - Second line agent in prolactinomas when bromocriptine is ineffective
 Other causes of hyperprolactinaemia Primary hypothyriodism Chronic renal failure Pituitary stalk compression Drugs (phenothiazines, haloperidol, metoclopramide, cimetidine, methyldopa, antihistamines and morphine) • Idiopathic • •
Other causes of hyperprolactinaemia Primary hypothyriodism Chronic renal failure Pituitary stalk compression Drugs (phenothiazines, haloperidol, metoclopramide, cimetidine, methyldopa, antihistamines and morphine) • Idiopathic • •
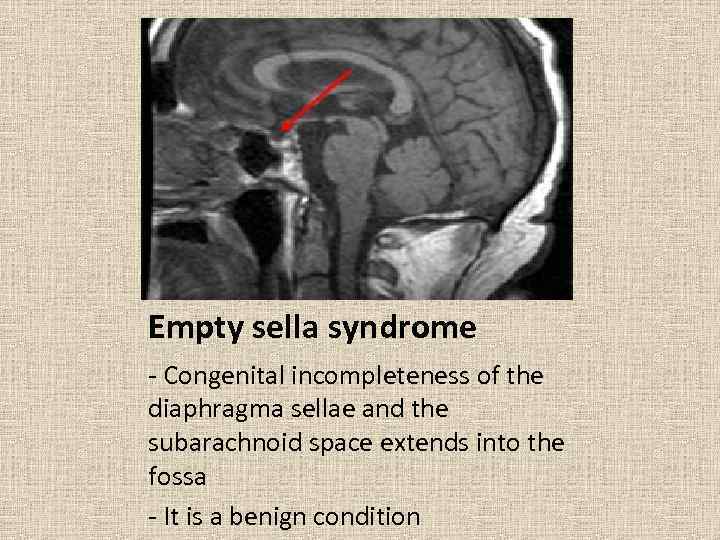 Empty sella syndrome - Congenital incompleteness of the diaphragma sellae and the subarachnoid space extends into the fossa - It is a benign condition
Empty sella syndrome - Congenital incompleteness of the diaphragma sellae and the subarachnoid space extends into the fossa - It is a benign condition
 Disorders of the hypothalamus
Disorders of the hypothalamus
 Disorders of the hypothalamus 1. Weight loss-associated amenorrhoea 2. Kallman’s syndrome 3. Tumours
Disorders of the hypothalamus 1. Weight loss-associated amenorrhoea 2. Kallman’s syndrome 3. Tumours
 Disorders of the hypothalamus • The most common reason for hypogonadotrophic secondary amenorrhoea • Often associated with weight loss, excessive exercise or stress • Diagnosed by exclusion of pituitary lesions • Ovulation induction is not indicated unless the patient wishes to become pregnant • If progestogen challenge test is negative, there is a significant risk of osteoporosis and hormone replacement therapy should be given
Disorders of the hypothalamus • The most common reason for hypogonadotrophic secondary amenorrhoea • Often associated with weight loss, excessive exercise or stress • Diagnosed by exclusion of pituitary lesions • Ovulation induction is not indicated unless the patient wishes to become pregnant • If progestogen challenge test is negative, there is a significant risk of osteoporosis and hormone replacement therapy should be given
 Weight loss-associated amenorrhoea - Loss of more than 10 kg is frequently associated with amenorrhoea - It usually occurs in young women as they become obsessed with their body image and starve themselves
Weight loss-associated amenorrhoea - Loss of more than 10 kg is frequently associated with amenorrhoea - It usually occurs in young women as they become obsessed with their body image and starve themselves
 Weight loss-associated amenorrhoea • Oestrogen levels can be profoundly suppressed • Hypothalamo-pituitary-ovarian function is usually restored when the lost weight is regained • Ovulation induction may be required but should be given only when weight >45 kg to avoid pregnancy risks (pre-term delivery)
Weight loss-associated amenorrhoea • Oestrogen levels can be profoundly suppressed • Hypothalamo-pituitary-ovarian function is usually restored when the lost weight is regained • Ovulation induction may be required but should be given only when weight >45 kg to avoid pregnancy risks (pre-term delivery)
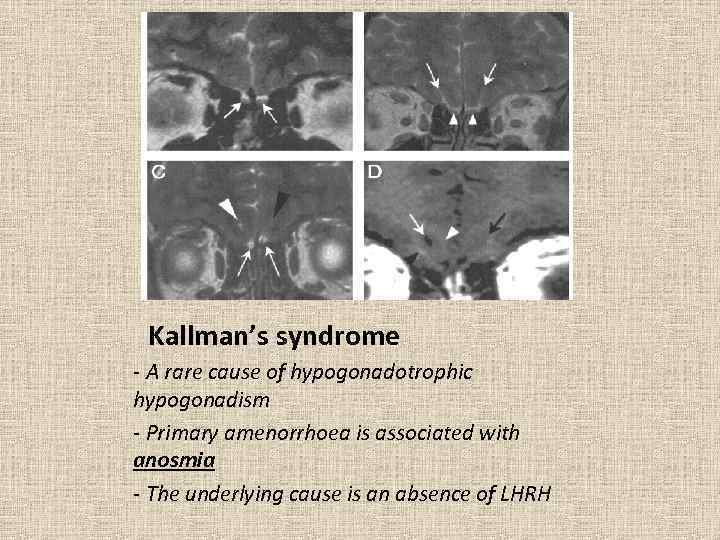 Kallman’s syndrome - A rare cause of hypogonadotrophic hypogonadism - Primary amenorrhoea is associated with anosmia - The underlying cause is an absence of LHRH
Kallman’s syndrome - A rare cause of hypogonadotrophic hypogonadism - Primary amenorrhoea is associated with anosmia - The underlying cause is an absence of LHRH
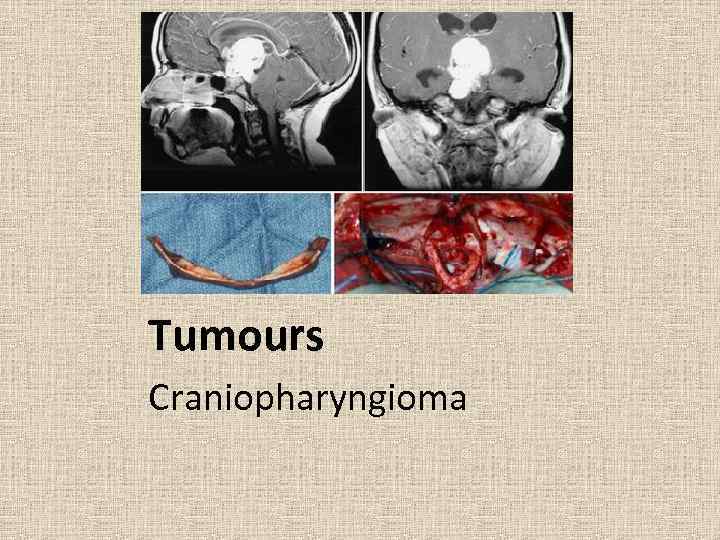 Tumours Craniopharyngioma
Tumours Craniopharyngioma
 Basic investigations of amenorrhoea
Basic investigations of amenorrhoea
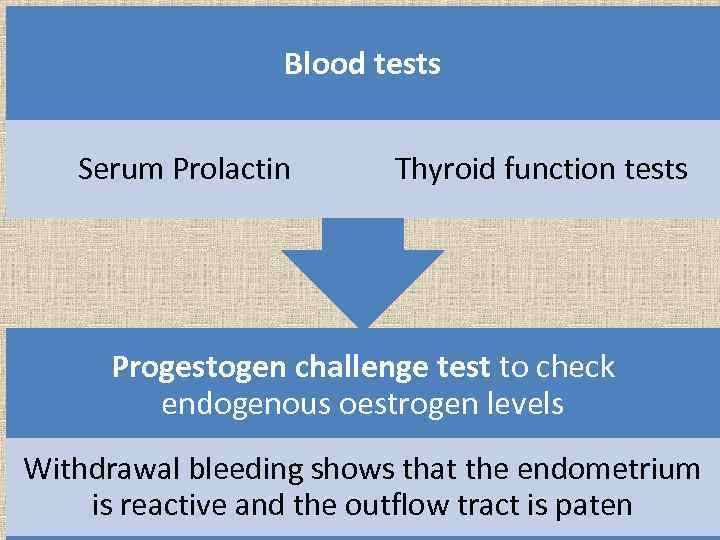 Blood tests Serum Prolactin Thyroid function tests Progestogen challenge test to check endogenous oestrogen levels Withdrawal bleeding shows that the endometrium is reactive and the outflow tract is paten
Blood tests Serum Prolactin Thyroid function tests Progestogen challenge test to check endogenous oestrogen levels Withdrawal bleeding shows that the endometrium is reactive and the outflow tract is paten
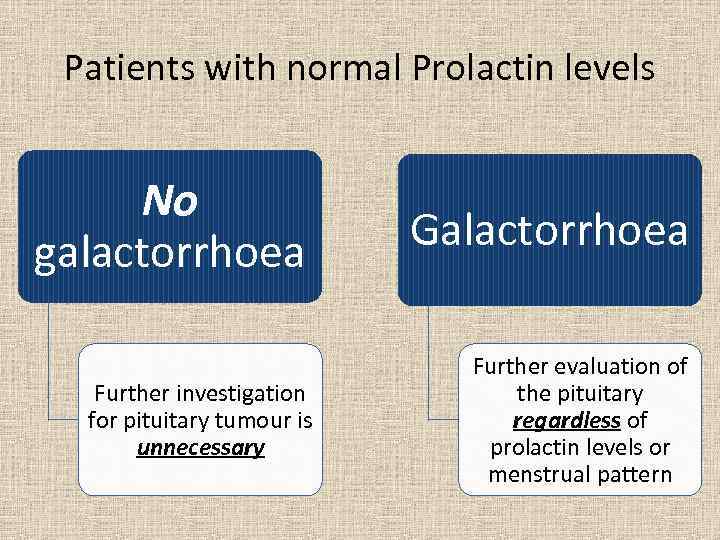 Patients with normal Prolactin levels No galactorrhoea Galactorrhoea Further investigation for pituitary tumour is unnecessary Further evaluation of the pituitary regardless of prolactin levels or menstrual pattern
Patients with normal Prolactin levels No galactorrhoea Galactorrhoea Further investigation for pituitary tumour is unnecessary Further evaluation of the pituitary regardless of prolactin levels or menstrual pattern
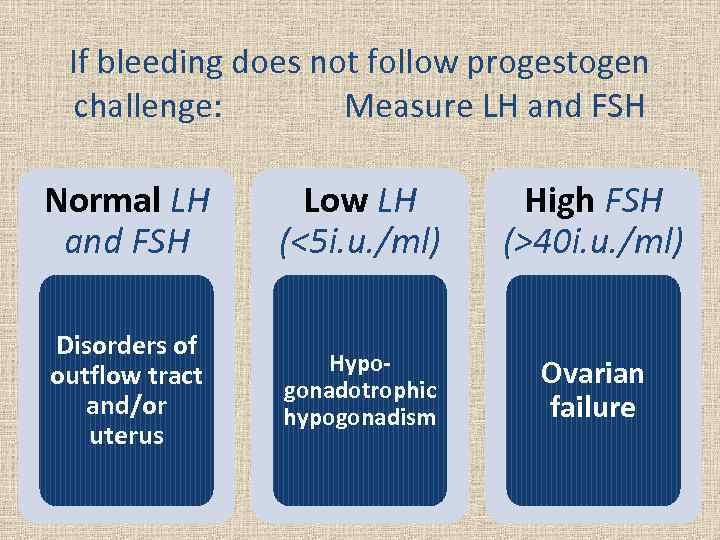 If bleeding does not follow progestogen challenge: Measure LH and FSH Normal LH and FSH Low LH (<5 i. u. /ml) High FSH (>40 i. u. /ml) Disorders of outflow tract and/or uterus Hypogonadotrophic hypogonadism Ovarian failure
If bleeding does not follow progestogen challenge: Measure LH and FSH Normal LH and FSH Low LH (<5 i. u. /ml) High FSH (>40 i. u. /ml) Disorders of outflow tract and/or uterus Hypogonadotrophic hypogonadism Ovarian failure
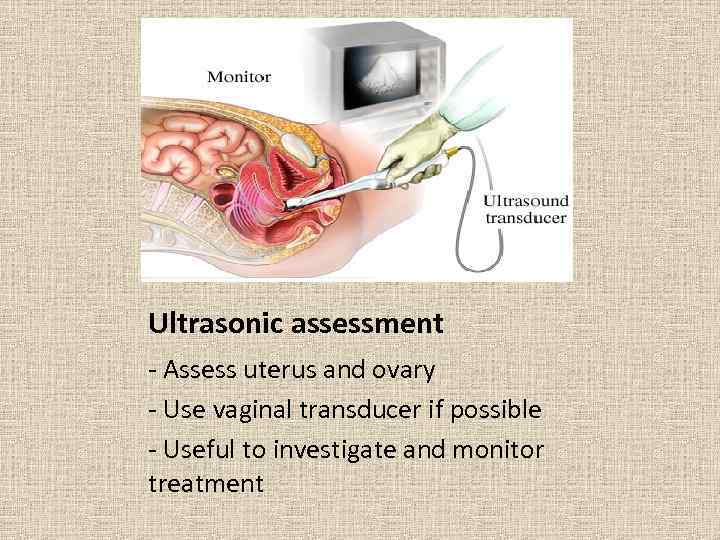 Ultrasonic assessment - Assess uterus and ovary - Use vaginal transducer if possible - Useful to investigate and monitor treatment
Ultrasonic assessment - Assess uterus and ovary - Use vaginal transducer if possible - Useful to investigate and monitor treatment
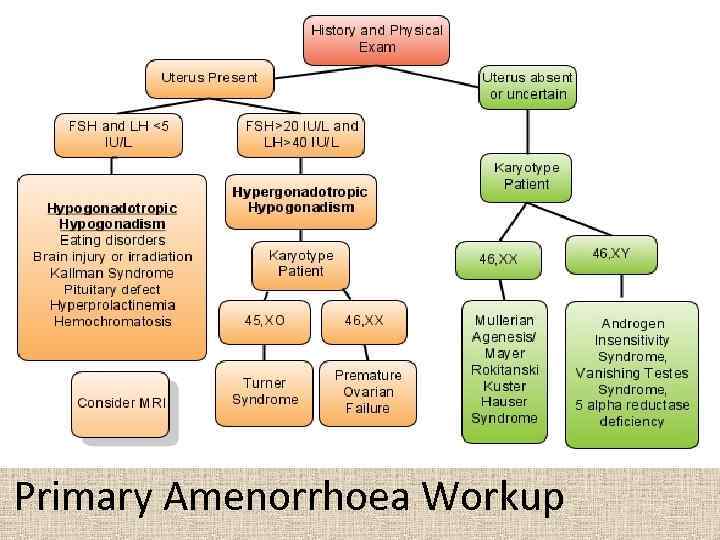 Primary Amenorrhoea Workup
Primary Amenorrhoea Workup
 Thank you
Thank you


