24769905d641f4eb857ac3251f5f9530.ppt
- Количество слайдов: 33

Medication reconciliation: Public vs. Private - is there are difference? Dr Treasure Mc. Guire 19 November 2014

You have already met Daniel • 60 y. o male presented for day surgery in our Private hospital • Not eligible for High 5 s – < 65 y. o. – Not admitted through the ED to inpatient services – Intention was a hospital stay of < 24 hrs • When he needed to be admitted – Medication Hx - No 2 nd source used • Minimal information from VMO or GP • Patient didn’t bring own medications • Only knew names of his medicines • “Best guess” for doses

Case study cont. Medications charted by cardiologist Dexamphetamine 10 mg po tds (withheld) Allegron® (nortriptyline) 80 mg nocte Paxam® (clonazepam) 20 mg nocte • Only one source: patient recall • Nurse contacted Surgeon for Phone order for evening meds • Patient no dose recall (20 mg vs 10 mg) • VMO – reduced to 10 mg

Next morning Pharmacist conducted BPMH (within 24 h) – Used > one source of Med Hx information • Community pharmacy & patient’s psychiatrist Dexamphetamine 10 mg tds Correct (but may have contributed to tachycardia) Nortriptyline 100 mg nocte NOT 80 mg Unintentional discrepancy Clonazepam 0. 5 mg nocte NOT 20 mg prescribed & 10 mg administered Unintentional discrepancy Outcome 20 x overdose (40 x overdose prescribed)! Clinically – dizzy, drowsy, unsteady on feet Required 2 nights in hospital

Would this misadventure have occurred: § Across the road in our public hospital? § If a BPMH had been taken?

High 5 s Medication Reconciliation project “Assuring medication accuracy at transitions of care” § Evidence-based patient safety solution sponsored by WHO § Lead technical agency - Australian Commission on Safety and Quality in Health Care (ACSQHC) § 10 participating hospitals over the 4 -5 year period (2010 -14) § Most were public hospitals § High 5 s Standard Operating Protocol (SOP) § Consistent with Australian practice § Aligns with APAC Guiding principles to achieve continuity in medication management.

4 Quality Improvement Measures used to evaluate the process & impact of implementing the Med Rec SOP Measure Definition Target 100% MR 1 Percent of Patients with Medications Reconciled within 24 hours of the decision to admit the patient MR 2 Mean Number of Outstanding Undocumented Intentional Medication Discrepancies per Patient 0 -1 MR 3 Mean Number of Outstanding Unintentional Medication Discrepancies per Patient ≤ 0. 3 MR 4 Percent of Patients with at Least One Outstanding Unintentional Discrepancy <40% MR 0 Mean Number of Medication Discrepancies (Intentional + Unintentional) per patient, identified at admission (i. e. prior to BPMH) -

To use these Measures to answer the question Public vs Private Med Rec: is there a difference • Need to understand the variables that underpin Med Rec in both settings
Australian High 5 Sites Mater Health Services South Brisbane Tertiary hospital with public & private beds (total approx 1000 beds) consisting of: • Mater Adult Hospital (Public) • Mater Children’s Hospital (Public & Private) • Mater Mothers’ Hospital (Public & Private) • Mater Private Hospital

Variables impacting on the quality of Med Rec – Public vs Private Patient cohort Medical model MR 0, 1, 2, 3, 4 HP conducting Med Rec Pharmacy model

1. Patient cohort Public vs. Private • Patient cohort – same High 5 s criteria – However • More social issues in Public setting • Potential differences in SES, education levels • Higher use of CAMs

2. HP conducting BPMH § In the Private system – HP may receive minimal information from VMO or GP § Cost-effective BPMH depends on HPs’ § Medication skill base & § Willingness to obtain >1 source of Med Hx § Communication skills In Daniel’s case, – Nursing staff recorded 1 st Med. Hx – relied on only 1 source (patient recall) – Neither Prescriber nor Nurse who administered overdose of clonazepam were familiar with the usual dose range & did not check an information source.

3. Medical model At Mater Private - General reluctance for nursing & medical staff involvement in conducting a BPMH: • In-house survey – “perceived insufficient time” to invest on this activity Nurses • Medication Hx on admission 2 -5 mins vs BPMH (15 -30 min up to an hour for complex patients)

3. Medical model Private VMOs – Less time for writing scripts &/or documenting care plan – vs JMO in Public – Increased reliance on Phone orders • Rely on memory when giving ward staff medn orders – Appreciated Pharmacist BPMH • Stated couldn’t justify time implications • Wanted Pharmacists to complete BPMH before they write up chart (& some would like pharmacists to do that for them too!) If Daniel was in our public system • Pre-admission clinic & BPMH avail during & post surgery (whether intention is to admit or not) • Missing for Private Surgical Day Patients

4. Pharmacy model Pharmacy Mater Public Mater Private Alternate Private model Service Clinical service, with pharmacist in ward 85% of day* Supply on script or chart Location On site, dispensing from ward Remote Pharmacist to bed ratio SHPA guidelines based Script volume based PBS Inpatient LAM Inpatient & Formulary Discharge only Our Pharmacy Model is same for Public and Private: Inpatient & Discharge Ward based clinical service M-F 8 am til 4: 30 pm* and ED in public from 7 am til 11 am Sat/ Sun & public holidays. Central pharmacy until 7: 30 pm M-F and 5: 30 pm Sat/Sun We would still have ‘missed’ Daniel’s first Med Hx!

4. Pharmacy model contd. Mater MHS “Public” MHS Private Alternate Private model Communication methods (of discrepancies) Phone, pager, in person as discrepancy found. Less use of clinical notes Depends on seriousness /level of urgency. More use of clinical notes. Phone for more urgent Phone, pager Transfer of Med Hx (in hospital to community) e-PCP transposed to Med List for discharge e-PCP transposed to Variable Med List for discharge Detail of documentation Variable – moderate Variable – minimal to to excellent e. PCP: Mater’s equivalent of an e. MAP • • In use for almost a decade Electronic, real time data collection & reports May not be accessible by pharmacist
Admissions List
Patient Demographics & Admission Information
‘Drugs on Admission’
Drugs on Admission Summary
Patient-specific tasks
Patient-specific tasks • Series of automatic tasks which appear for all newly admitted patients • BPMH – Completed within 24 hours of admission. – NOT completed within 24 hours of admission – Differs from other documented medication history (Delete if no difference)
Discharge Drugs - Preparation
Drug Profile – Log of ALL Med-related events Admission to D/C
e. PCPs – Electronic Pharmaceutical Care Plans Advantage • Comprehensive Medication profile easily accessed • Able to “import” from meds dispensed & from prev. admissions • Series of automatic tasks appear for all new admissions • ID outstanding tasks/ profiles to be signed off • Once “signed-off” faxed electronically irrespective of medical/ nursing DC summaries Neutral • Only completed by pharmacists • Only 1 profile can be generated on DC. Problem if pt classified as low risk but nurse/ doctor has started a med profile. Disadvantage • Only pharmacy staff can view the majority of content • VMOs can’t access completed e- profiles as yet • No Authorised Form# (ie some get filed, some don’t)

So how did Mater perform on Medication Reconciliation during High 5 – Public vs Private?
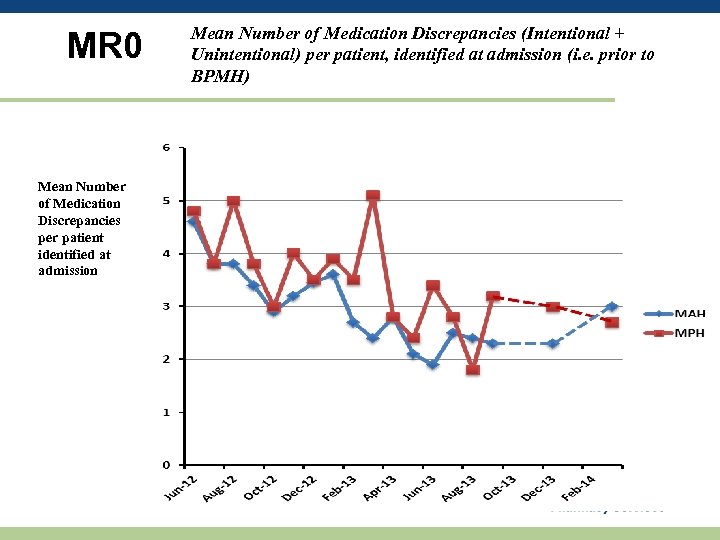
MR 0 Mean Number of Medication Discrepancies per patient identified at admission Mean Number of Medication Discrepancies (Intentional + Unintentional) per patient, identified at admission (i. e. prior to BPMH)
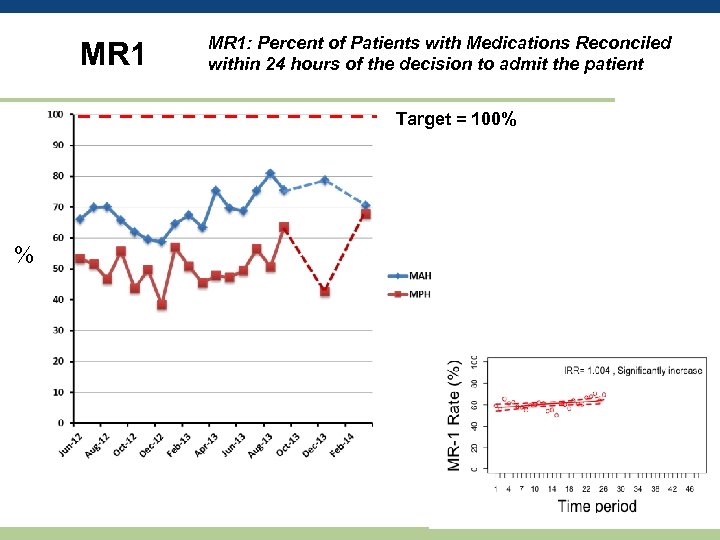
MR 1: Percent of Patients with Medications Reconciled within 24 hours of the decision to admit the patient Target = 100% %
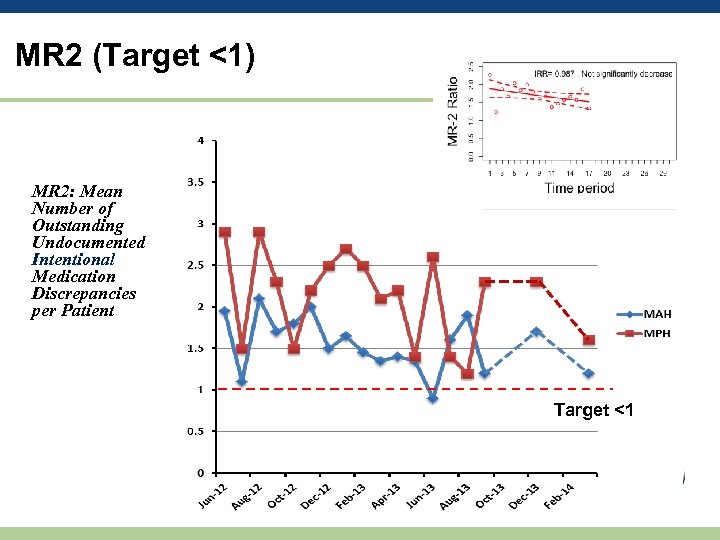
MR 2 (Target <1) MR 2: Mean Number of Outstanding Undocumented Intentional Medication Discrepancies per Patient Target <1
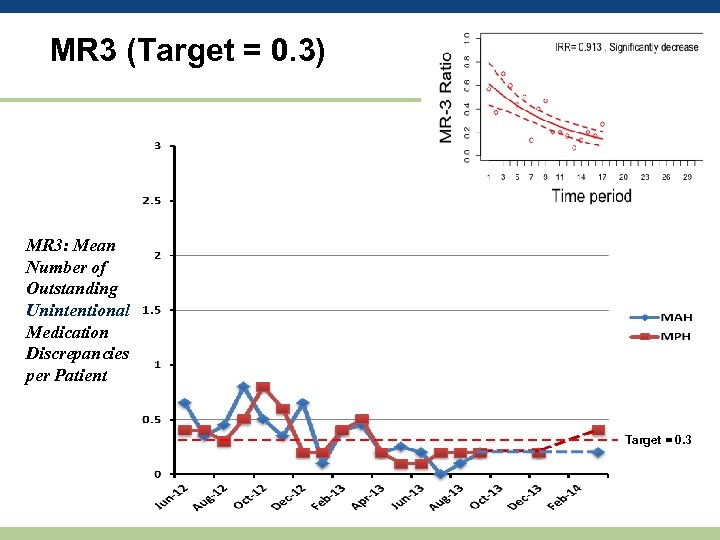
MR 3 (Target = 0. 3) MR 3: Mean Number of Outstanding Unintentional Medication Discrepancies per Patient Target = 0. 3
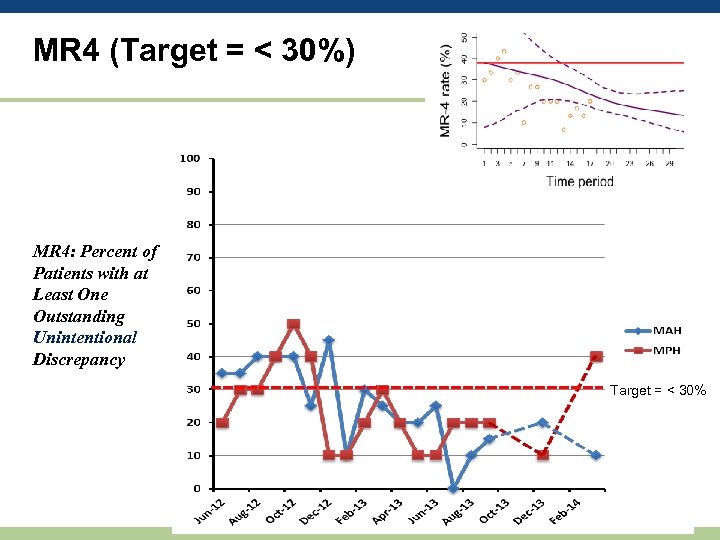
MR 4 (Target = < 30%) MR 4: Percent of Patients with at Least One Outstanding Unintentional Discrepancy Target = < 30%

Limitations – High 5 s SOP Focus was on admissions via ED: § Omitted surgical day care patients admitted with complications Lack of initial consensus (or individual hospital perspective) on the potential for clinical impact from discrepancies wrt: – CAMs – PRN unrelated to episode of care • Sedatives • Eye drops (non Rx) • Topicals e. g. Creams If unrelated to episode of care

Conclusion Mater High 5 statistics § MR 1 slightly higher in Public vs Private (% Med Recs within 24 hrs of adm) § But MR 2, 3, 4 & 0 comparable Public vs Private Med Rec is a feasible model to improve patient safety / QUM, with comparable outcomes in a Private vs Public setting IF 3 CRITERIA SATISFIED: • Model & staff support BPMH • Staff take time to access resources for double check • HP conducting the BPMH in any transition of care has a good working knowledge of not just medication available but their dose forms, strengths & usual doses
24769905d641f4eb857ac3251f5f9530.ppt