a825ace9f7ec78b3ddae79c146f8984a.ppt
- Количество слайдов: 29
 Medical University of Sofia, Faculty of M Department of Pharmacology and Toxico Antiseizure (antiepileptic) drugs (Abstract) Assoc. Prof. Ivan Lambev e-mail: itlambev@mail. bg
Medical University of Sofia, Faculty of M Department of Pharmacology and Toxico Antiseizure (antiepileptic) drugs (Abstract) Assoc. Prof. Ivan Lambev e-mail: itlambev@mail. bg
 EPILEPSY affects 5– 10‰ of the general pop It is due to sudden, excessive depolarizati some or all cerebral neurons. This may be: • localized (focal or partial seizure); • spread to cause a secondary generalized s • may affect all cortical neurons simultaneou (primary generalized seizure).
EPILEPSY affects 5– 10‰ of the general pop It is due to sudden, excessive depolarizati some or all cerebral neurons. This may be: • localized (focal or partial seizure); • spread to cause a secondary generalized s • may affect all cortical neurons simultaneou (primary generalized seizure).
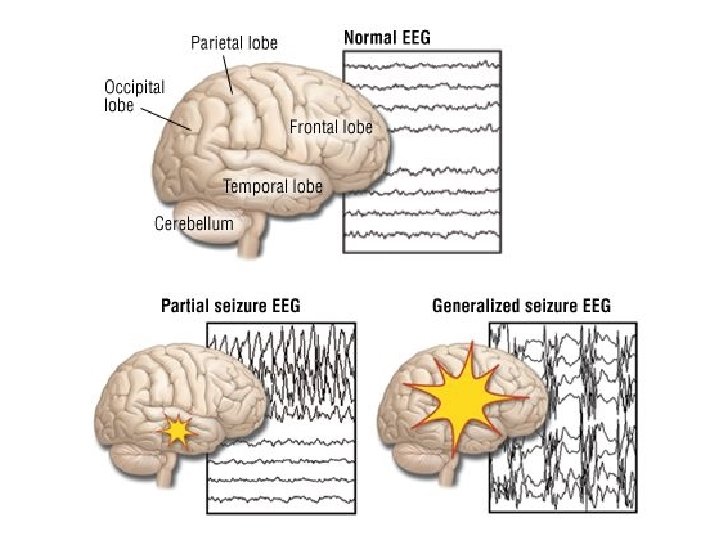
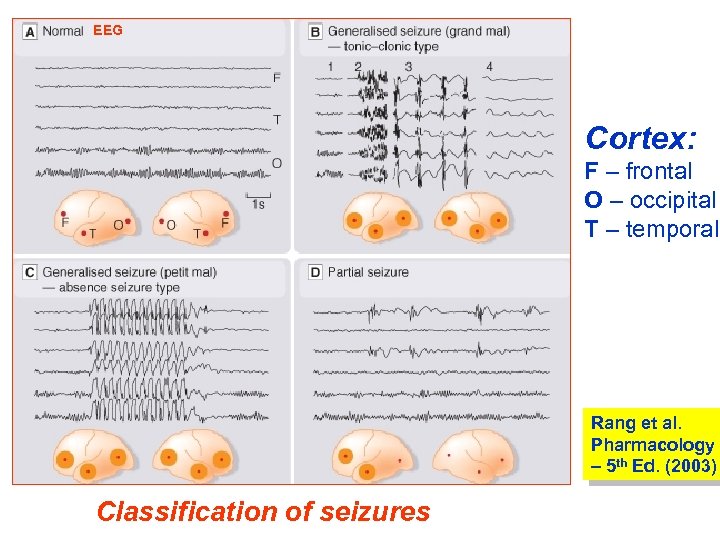 EEG Cortex: F – frontal O – occipital T – temporal Rang et al. Pharmacology – 5 th Ed. (2003) Classification of seizures
EEG Cortex: F – frontal O – occipital T – temporal Rang et al. Pharmacology – 5 th Ed. (2003) Classification of seizures
 HISTORY • Bromides (1857) • Phenobarbital (1912) • Phenytoin (1938) • Later: Ethosiximide, Carbmazepine • New anticonvulsants (in the last 15– 20 ye vigabatrin, gabapentin, lamotrigine, topira oxcarbazepine, levetiracetam, pregabalin
HISTORY • Bromides (1857) • Phenobarbital (1912) • Phenytoin (1938) • Later: Ethosiximide, Carbmazepine • New anticonvulsants (in the last 15– 20 ye vigabatrin, gabapentin, lamotrigine, topira oxcarbazepine, levetiracetam, pregabalin
 ANTISEIZURE DRUGS 1. Carboxamides (enzyme inductors – CYP 450): Carbamazepine (+ neuropathic pain – n. trigeminus postherpetic pain, etc. ), Oxcarbazepine 2. Hydantoins: Phenytoin (enzyme inductor), used in intoxication too 3. Barbiturates (Phenobarbital – enzyme inductors) a analogues (Primidone – prodrug) 4. Succinimides: Ethosuximide (casp. 250 mg – petit m 5. Valproates (enzyme inhibitors): Sodium valproate (D 6. Benzodiazepines: Clonazepam, Clorazepate, Diaze t 1/2 43 h, amp. 10 mg/2 ml i. m. /i. v. , Lorazepam, Nitraz 7. GABA analogues: Gabapentin, Tiagabine 8. Hetereogenic anticonvulsants: Lamotrigine, Levetir Pregabalin (partial seizures, peripheral neuropathic p Topiramate, Vigabatrin
ANTISEIZURE DRUGS 1. Carboxamides (enzyme inductors – CYP 450): Carbamazepine (+ neuropathic pain – n. trigeminus postherpetic pain, etc. ), Oxcarbazepine 2. Hydantoins: Phenytoin (enzyme inductor), used in intoxication too 3. Barbiturates (Phenobarbital – enzyme inductors) a analogues (Primidone – prodrug) 4. Succinimides: Ethosuximide (casp. 250 mg – petit m 5. Valproates (enzyme inhibitors): Sodium valproate (D 6. Benzodiazepines: Clonazepam, Clorazepate, Diaze t 1/2 43 h, amp. 10 mg/2 ml i. m. /i. v. , Lorazepam, Nitraz 7. GABA analogues: Gabapentin, Tiagabine 8. Hetereogenic anticonvulsants: Lamotrigine, Levetir Pregabalin (partial seizures, peripheral neuropathic p Topiramate, Vigabatrin
 MECHANISM OF ACTION OF ANTIEPILEPTIC D Antiepileptics inhibit the neuronal discharge or its spread in o more of the following ways: (1) Enhancing GABA synaptic transmission: barbiturates, diazepines, gabapentin, levetiracetam, tiagabine, vigabatrin, mate, valproate; the result is increased permeability to chlorid which reduces neuronal excitability. Valproate and topiramate GABA transaminase and tiagabine blocks reuptake of GABA (2) Reducing cell membrane permeability to voltage-depe sodium channels: carbamazepine, lamotrigine, oxcarbazep phenytoin, topiramate, valproate. (3) Reducing cell membrane permeability to calcium T-ch valproate, ethosuximide; the result is diminishing of the gene of action potential. (4) Inhibiting excitory neurotransmitter glutamate: lam
MECHANISM OF ACTION OF ANTIEPILEPTIC D Antiepileptics inhibit the neuronal discharge or its spread in o more of the following ways: (1) Enhancing GABA synaptic transmission: barbiturates, diazepines, gabapentin, levetiracetam, tiagabine, vigabatrin, mate, valproate; the result is increased permeability to chlorid which reduces neuronal excitability. Valproate and topiramate GABA transaminase and tiagabine blocks reuptake of GABA (2) Reducing cell membrane permeability to voltage-depe sodium channels: carbamazepine, lamotrigine, oxcarbazep phenytoin, topiramate, valproate. (3) Reducing cell membrane permeability to calcium T-ch valproate, ethosuximide; the result is diminishing of the gene of action potential. (4) Inhibiting excitory neurotransmitter glutamate: lam
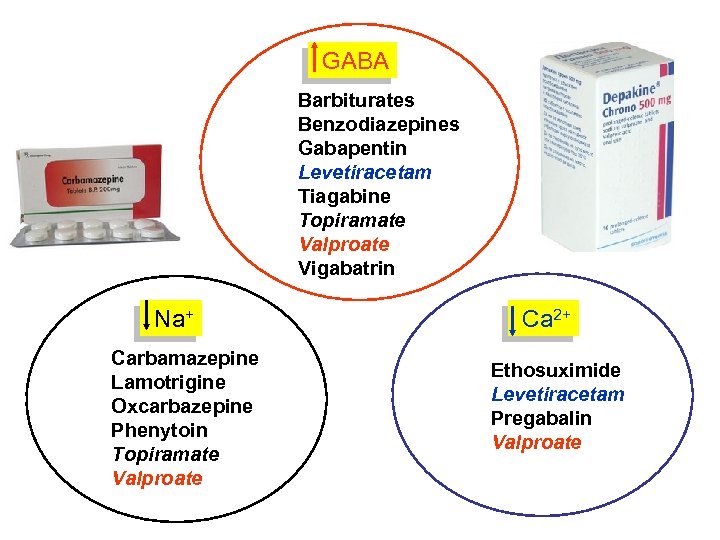 GABA Barbiturates Benzodiazepines Gabapentin Levetiracetam Tiagabine Topiramate Valproate Vigabatrin Na+ Carbamazepine Lamotrigine Oxcarbazepine Phenytoin Topiramate Valproate Ca 2+ Ethosuximide Levetiracetam Pregabalin Valproate
GABA Barbiturates Benzodiazepines Gabapentin Levetiracetam Tiagabine Topiramate Valproate Vigabatrin Na+ Carbamazepine Lamotrigine Oxcarbazepine Phenytoin Topiramate Valproate Ca 2+ Ethosuximide Levetiracetam Pregabalin Valproate
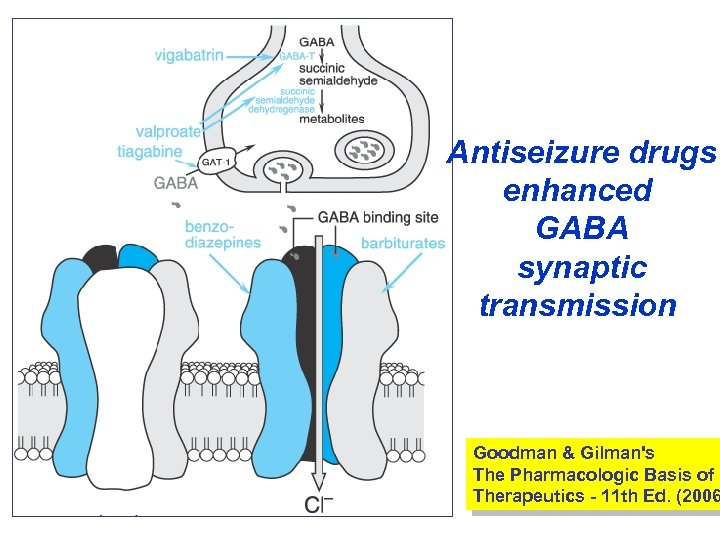 Antiseizure drugs enhanced GABA synaptic transmission Goodman & Gilman's The Pharmacologic Basis of Therapeutics - 11 th Ed. (2006
Antiseizure drugs enhanced GABA synaptic transmission Goodman & Gilman's The Pharmacologic Basis of Therapeutics - 11 th Ed. (2006
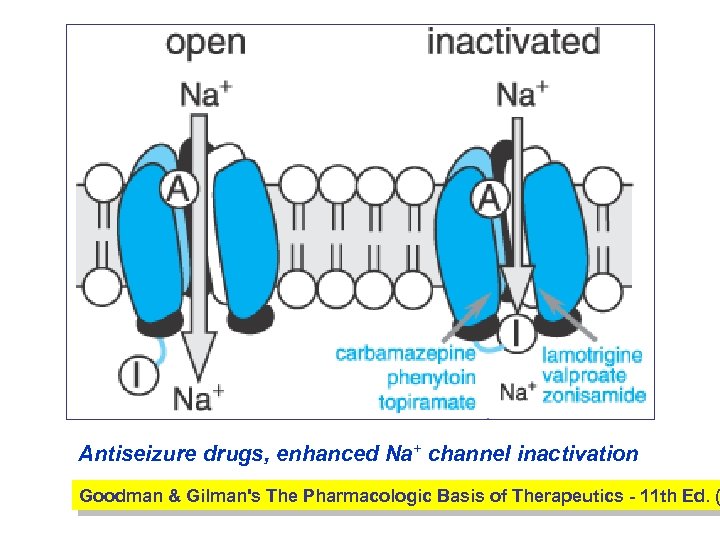 Antiseizure drugs, enhanced Na+ channel inactivation Goodman & Gilman's The Pharmacologic Basis of Therapeutics - 11 th Ed. (
Antiseizure drugs, enhanced Na+ channel inactivation Goodman & Gilman's The Pharmacologic Basis of Therapeutics - 11 th Ed. (
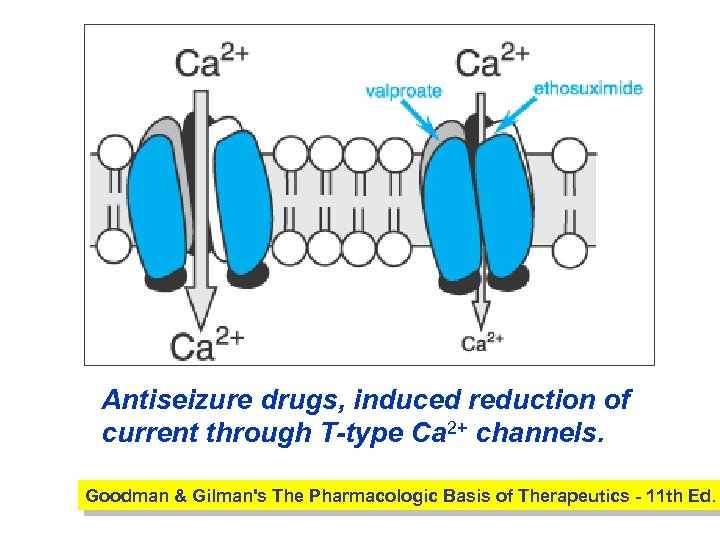 Antiseizure drugs, induced reduction of current through T-type Ca 2+ channels. Goodman & Gilman's The Pharmacologic Basis of Therapeutics - 11 th Ed.
Antiseizure drugs, induced reduction of current through T-type Ca 2+ channels. Goodman & Gilman's The Pharmacologic Basis of Therapeutics - 11 th Ed.
 Goodman & Gilman's The Pharmacologic Basis of Therapeutics – 11 th Ed. ( Effects of three antiseizure drugs on sustained high-frequency firin potentials by cultured neurons. Intracellular recordings were ma neurons while depolarizing current pulses, approximately 0. 75 s in were applied (on-off step changes indicated by arrows). In the abs drug, a series of high-frequency repetitive action potentials fil entire duration of the current pulse. Phenytoin, carbamazepin sodium valproate all markedly reduced the number of action p elicited by the current pulses.
Goodman & Gilman's The Pharmacologic Basis of Therapeutics – 11 th Ed. ( Effects of three antiseizure drugs on sustained high-frequency firin potentials by cultured neurons. Intracellular recordings were ma neurons while depolarizing current pulses, approximately 0. 75 s in were applied (on-off step changes indicated by arrows). In the abs drug, a series of high-frequency repetitive action potentials fil entire duration of the current pulse. Phenytoin, carbamazepin sodium valproate all markedly reduced the number of action p elicited by the current pulses.
 INDIVIDUAL ANTIEPILEPTICS ▼CARBAMAZEPINE blocks voltage-dependent sodium ion reducing membrane excitability. The t 1/2 of the drug falls from 20 h over the first few weeks of therapy due to the induction enzymes that metabolize it as well as other drugs (including corticosteroids, hormonal contraceptives, theophylline and w Standard tablets are taken twice a day. Carbamazepine is a first choice for focal and secondary generalized epileps aggravates myoclonic and absence seizure. It is useful for t treatment of trigeminal neuralgia, postherpetic pains, etc. Adverse reactions (ARs): reversible blurring of vision, diplo dizziness, ataxia, depression of AV conduction, skin rashes kidney dysfunction.
INDIVIDUAL ANTIEPILEPTICS ▼CARBAMAZEPINE blocks voltage-dependent sodium ion reducing membrane excitability. The t 1/2 of the drug falls from 20 h over the first few weeks of therapy due to the induction enzymes that metabolize it as well as other drugs (including corticosteroids, hormonal contraceptives, theophylline and w Standard tablets are taken twice a day. Carbamazepine is a first choice for focal and secondary generalized epileps aggravates myoclonic and absence seizure. It is useful for t treatment of trigeminal neuralgia, postherpetic pains, etc. Adverse reactions (ARs): reversible blurring of vision, diplo dizziness, ataxia, depression of AV conduction, skin rashes kidney dysfunction.
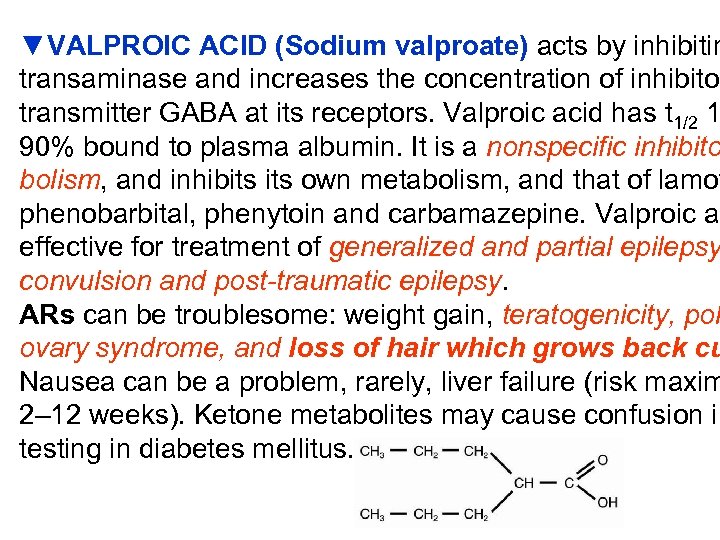 ▼VALPROIC ACID (Sodium valproate) acts by inhibitin transaminase and increases the concentration of inhibitor transmitter GABA at its receptors. Valproic acid has t 1/2 1 90% bound to plasma albumin. It is a nonspecific inhibito bolism, and inhibits own metabolism, and that of lamot phenobarbital, phenytoin and carbamazepine. Valproic ac effective for treatment of generalized and partial epilepsy convulsion and post-traumatic epilepsy. ARs can be troublesome: weight gain, teratogenicity, pol ovary syndrome, and loss of hair which grows back cu Nausea can be a problem, rarely, liver failure (risk maxim 2– 12 weeks). Ketone metabolites may cause confusion in testing in diabetes mellitus.
▼VALPROIC ACID (Sodium valproate) acts by inhibitin transaminase and increases the concentration of inhibitor transmitter GABA at its receptors. Valproic acid has t 1/2 1 90% bound to plasma albumin. It is a nonspecific inhibito bolism, and inhibits own metabolism, and that of lamot phenobarbital, phenytoin and carbamazepine. Valproic ac effective for treatment of generalized and partial epilepsy convulsion and post-traumatic epilepsy. ARs can be troublesome: weight gain, teratogenicity, pol ovary syndrome, and loss of hair which grows back cu Nausea can be a problem, rarely, liver failure (risk maxim 2– 12 weeks). Ketone metabolites may cause confusion in testing in diabetes mellitus.
 ▼PHENYTOIN (t 1/2 6– 24 h) has saturation kinetics. It is exten hydroxylated in the liver and this process becomes saturated a doses needed for therapeutic effect (therapeutic plasma conce range is 10– 20 mg/L). Phenytoin is a potent inducer of hepatic lizing enzymes affecting itself and other drugs (carbamazepine farin, adrenal and gonadal steroids, thyroxine, tricyclic antidep doxycycline, vitamin D, folate). Drugs that inhibit phenytoin me include: valproic acid, cimetidine, co-trimoxazole, isoniazid, ch phenicol, some NSAIDs, disulfiram. Phenytoin is 90% bound t albumin and small changes in binding will result in a higher co tion of free active drug. It is used to prevent all types of partial generalized seizure, and st. epilepticus. It is not used for abse ARs: impairment of cognitive function (which has led many ph prefer carbamazepine and valproate), sedation, hirsutism, skin gum hyperplasia (due to the inhibition of collagen metabolism) hyperglycemia, anaemia, osteomalacia.
▼PHENYTOIN (t 1/2 6– 24 h) has saturation kinetics. It is exten hydroxylated in the liver and this process becomes saturated a doses needed for therapeutic effect (therapeutic plasma conce range is 10– 20 mg/L). Phenytoin is a potent inducer of hepatic lizing enzymes affecting itself and other drugs (carbamazepine farin, adrenal and gonadal steroids, thyroxine, tricyclic antidep doxycycline, vitamin D, folate). Drugs that inhibit phenytoin me include: valproic acid, cimetidine, co-trimoxazole, isoniazid, ch phenicol, some NSAIDs, disulfiram. Phenytoin is 90% bound t albumin and small changes in binding will result in a higher co tion of free active drug. It is used to prevent all types of partial generalized seizure, and st. epilepticus. It is not used for abse ARs: impairment of cognitive function (which has led many ph prefer carbamazepine and valproate), sedation, hirsutism, skin gum hyperplasia (due to the inhibition of collagen metabolism) hyperglycemia, anaemia, osteomalacia.
 Saturation kinetics. Phenytoin is extensively hydroxylated in the liver and this process becomes saturated at about the doses needed for therapeutic effect. Thus phenytoin at low doses exhibits firstorder kinetics but saturation or zero-order kinetics develop as therapeutic plasma concentration range (10– 20 mg/L) is approached, i. e. the dose increments of equal size produce disproportional rise in steady-state plasma concentration.
Saturation kinetics. Phenytoin is extensively hydroxylated in the liver and this process becomes saturated at about the doses needed for therapeutic effect. Thus phenytoin at low doses exhibits firstorder kinetics but saturation or zero-order kinetics develop as therapeutic plasma concentration range (10– 20 mg/L) is approached, i. e. the dose increments of equal size produce disproportional rise in steady-state plasma concentration.
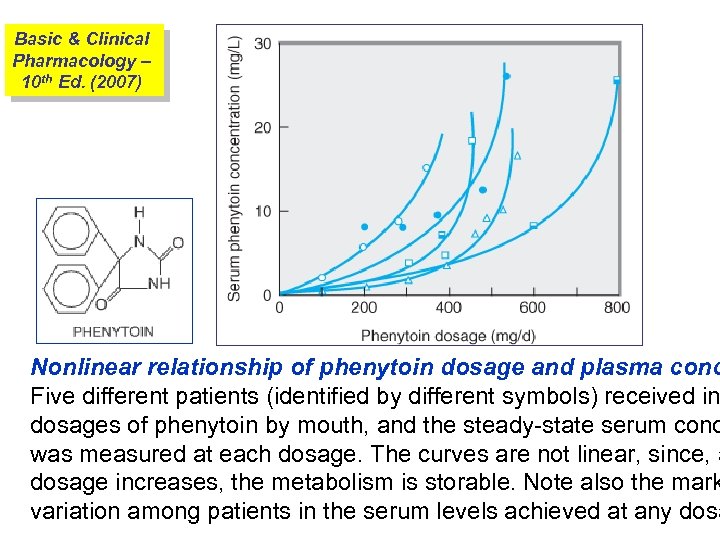 Basic & Clinical Pharmacology – 10 th Ed. (2007) Nonlinear relationship of phenytoin dosage and plasma conc Five different patients (identified by different symbols) received in dosages of phenytoin by mouth, and the steady-state serum conc was measured at each dosage. The curves are not linear, since, a dosage increases, the metabolism is storable. Note also the mark variation among patients in the serum levels achieved at any dosa
Basic & Clinical Pharmacology – 10 th Ed. (2007) Nonlinear relationship of phenytoin dosage and plasma conc Five different patients (identified by different symbols) received in dosages of phenytoin by mouth, and the steady-state serum conc was measured at each dosage. The curves are not linear, since, a dosage increases, the metabolism is storable. Note also the mark variation among patients in the serum levels achieved at any dosa
 ▼BENZODIAZEPINES • Diazepam given intravenously or rectally is highly effect stopping continuous seizure activity, especially generaliz clonic status epilepticus. The drug is occasionally given o a long-term basis, although it is not considered very effec this application, probably because of the rapid developm tolerance. A rectal gel is available for refractory patients acute control of bouts of seizure activity. • Lorazepam appears in some studies to be more effectiv longer-acting than diazepam in the treatment of status ep and is preferred by some experts. • Clonazepam (t 1/2 25 h) is a benzodiazepine used as a second line drug for treatment of primary generalized epi and status epilepticus.
▼BENZODIAZEPINES • Diazepam given intravenously or rectally is highly effect stopping continuous seizure activity, especially generaliz clonic status epilepticus. The drug is occasionally given o a long-term basis, although it is not considered very effec this application, probably because of the rapid developm tolerance. A rectal gel is available for refractory patients acute control of bouts of seizure activity. • Lorazepam appears in some studies to be more effectiv longer-acting than diazepam in the treatment of status ep and is preferred by some experts. • Clonazepam (t 1/2 25 h) is a benzodiazepine used as a second line drug for treatment of primary generalized epi and status epilepticus.
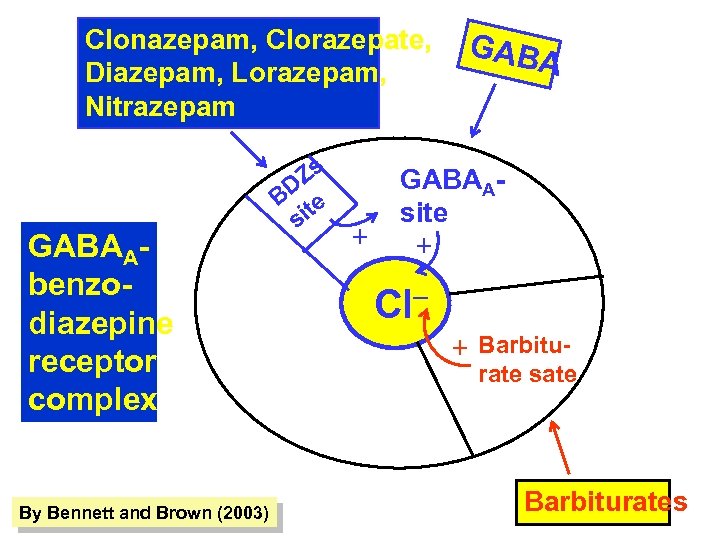 Clonazepam, Clorazepate, Diazepam, Lorazepam, Nitrazepam GABAAbenzodiazepine receptor complex By Bennett and Brown (2003) Zs BD te si + GABAAsite + Cl+ Barbitu- rate sate Barbiturates
Clonazepam, Clorazepate, Diazepam, Lorazepam, Nitrazepam GABAAbenzodiazepine receptor complex By Bennett and Brown (2003) Zs BD te si + GABAAsite + Cl+ Barbitu- rate sate Barbiturates
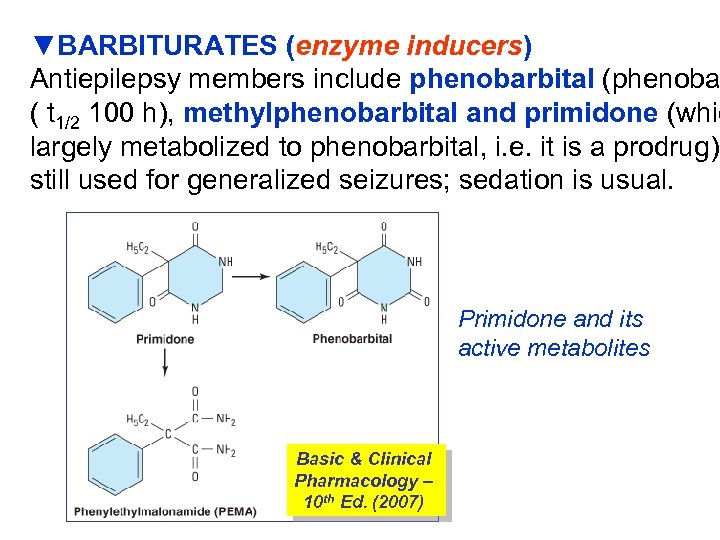 ▼BARBITURATES (enzyme inducers) Antiepilepsy members include phenobarbital (phenoba ( t 1/2 100 h), methylphenobarbital and primidone (whic largely metabolized to phenobarbital, i. e. it is a prodrug). still used for generalized seizures; sedation is usual. Primidone and its active metabolites Basic & Clinical Pharmacology – 10 th Ed. (2007)
▼BARBITURATES (enzyme inducers) Antiepilepsy members include phenobarbital (phenoba ( t 1/2 100 h), methylphenobarbital and primidone (whic largely metabolized to phenobarbital, i. e. it is a prodrug). still used for generalized seizures; sedation is usual. Primidone and its active metabolites Basic & Clinical Pharmacology – 10 th Ed. (2007)
 ▼LAMOTRIGINE (t 1/2 6– 24 h) inhibits excitory neurotran glutamate. Lamotrigine is effective for the treatment of pa secondarily generalized tonic-clonic seizure. It is general tolerated but may cause serious ARs of the skin, includin Stevens–Johnson syndrome and toxic epidermal necroly ▼TOPIRAMATE (t 1/2 21 h) is used as adjunctive treatme partial seizure, with or without secondary generalization. sedation, weight loss, acute myopia, raised intraocular p ▼ETHOSUXIMIDE (t 1/2 55 h) blocks T-type calcium ion channels. It is active in absence seizures (petit mal). ARs: gastric upset, CNS effects and allergic reactions.
▼LAMOTRIGINE (t 1/2 6– 24 h) inhibits excitory neurotran glutamate. Lamotrigine is effective for the treatment of pa secondarily generalized tonic-clonic seizure. It is general tolerated but may cause serious ARs of the skin, includin Stevens–Johnson syndrome and toxic epidermal necroly ▼TOPIRAMATE (t 1/2 21 h) is used as adjunctive treatme partial seizure, with or without secondary generalization. sedation, weight loss, acute myopia, raised intraocular p ▼ETHOSUXIMIDE (t 1/2 55 h) blocks T-type calcium ion channels. It is active in absence seizures (petit mal). ARs: gastric upset, CNS effects and allergic reactions.
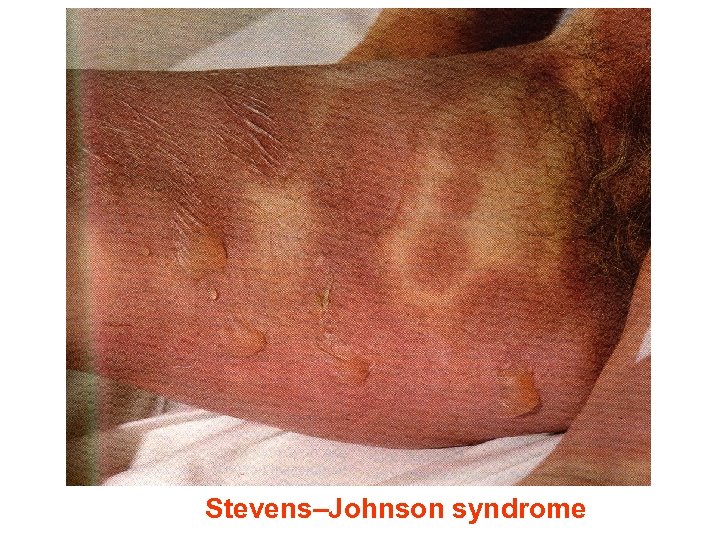 Stevens–Johnson syndrome
Stevens–Johnson syndrome
 PRINCIPLES OF MANAGEMENT (Clinical Parmacology – 9 th Ed. , 2003) • Any causative factor must be treated (cerebral neopla • Educate the patient about the disease, duration of trea and need for compliance. • Avoid precipitating factor (alcohol, sleep deprivation, e stress, and caffeine). • Anticipate natural variation: fits may occur around me periods in women – catamenial (monthly) epilepsy. • Give antiepileptics only if seizure type and frequency (e. g. more than one fit every 6– 12 months).
PRINCIPLES OF MANAGEMENT (Clinical Parmacology – 9 th Ed. , 2003) • Any causative factor must be treated (cerebral neopla • Educate the patient about the disease, duration of trea and need for compliance. • Avoid precipitating factor (alcohol, sleep deprivation, e stress, and caffeine). • Anticipate natural variation: fits may occur around me periods in women – catamenial (monthly) epilepsy. • Give antiepileptics only if seizure type and frequency (e. g. more than one fit every 6– 12 months).
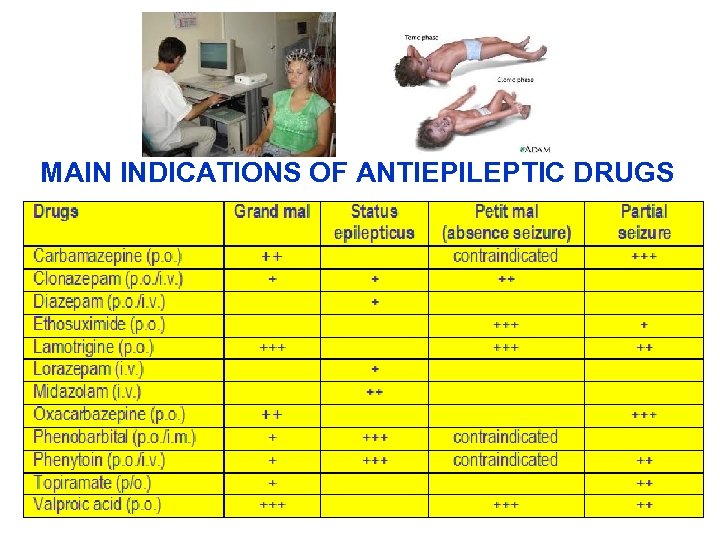 MAIN INDICATIONS OF ANTIEPILEPTIC DRUGS
MAIN INDICATIONS OF ANTIEPILEPTIC DRUGS
 Anticonvulsive drugs of choice Grand mal: I choice – valproate or Lamotrigine Alternative – Carbamazepine, Topiramate or Phenytoin Petit mal: I choice – Ehosuximide or valproate Alternative – Clonazepam or Lamotrigine Partial seizures: I choice – Carbamazepine or valproate Alternative – Phenytoin, Lamotrigine, Vigabatrin, Topiram Status epilepticus: I choice – Diazepam or Lorazep Alternative – Phenobarbital (i. m. /i/v. )
Anticonvulsive drugs of choice Grand mal: I choice – valproate or Lamotrigine Alternative – Carbamazepine, Topiramate or Phenytoin Petit mal: I choice – Ehosuximide or valproate Alternative – Clonazepam or Lamotrigine Partial seizures: I choice – Carbamazepine or valproate Alternative – Phenytoin, Lamotrigine, Vigabatrin, Topiram Status epilepticus: I choice – Diazepam or Lorazep Alternative – Phenobarbital (i. m. /i/v. )
 Treatment of status epilepticus in a Patient in opisthotonus (grand mal)
Treatment of status epilepticus in a Patient in opisthotonus (grand mal)
 GENERAL GUIDE TO ANTIEPILEPSY PHARMACOT (1) The decision whether or not to initiate drug therapy af single seizure remains controversial since approximately of patients may not have another seizure. (2) Therapy should start with a single drug (70% of patien be controlled on one drug (monotherapy). (3) Anticonvulsant drug therapy should be appropriate to of seizure. (4) The choice of drugs is also determined by the patient’ and sex. (5) If the attempt to control epilepsy by use of a single dru unsuccessful, it should be withdrawn and replaced by a s line drug, though these are effective in only 10% of patien
GENERAL GUIDE TO ANTIEPILEPSY PHARMACOT (1) The decision whether or not to initiate drug therapy af single seizure remains controversial since approximately of patients may not have another seizure. (2) Therapy should start with a single drug (70% of patien be controlled on one drug (monotherapy). (3) Anticonvulsant drug therapy should be appropriate to of seizure. (4) The choice of drugs is also determined by the patient’ and sex. (5) If the attempt to control epilepsy by use of a single dru unsuccessful, it should be withdrawn and replaced by a s line drug, though these are effective in only 10% of patien
 There is little evidence that 2 or 3 drugs are better than but more drugs often mean more ARs. (6) Effective therapy must never be stopped suddenly, only gradually. (7) After a period of at least 2– 3 years free from seizure drawal of anticonvulsants can be considered. In genera continuing the antiepileptic drug therapy is associated w about 20% relapse during withdrawal and a further 20% over the following 5 years. It is recommended that the a leptic drug be withdrawn over a period of 6 months. If a occurs during this time, full therapy must begin again un patient has been free from seizure for a further 2– 3 yea
There is little evidence that 2 or 3 drugs are better than but more drugs often mean more ARs. (6) Effective therapy must never be stopped suddenly, only gradually. (7) After a period of at least 2– 3 years free from seizure drawal of anticonvulsants can be considered. In genera continuing the antiepileptic drug therapy is associated w about 20% relapse during withdrawal and a further 20% over the following 5 years. It is recommended that the a leptic drug be withdrawn over a period of 6 months. If a occurs during this time, full therapy must begin again un patient has been free from seizure for a further 2– 3 yea
 Alternative methods for treatment of epileps • Neurosurgery + laser therapy
Alternative methods for treatment of epileps • Neurosurgery + laser therapy


