f545c9be0ed689006037cdc3667852f3.ppt
- Количество слайдов: 21
 Measuring Quality In Health Care Linda K. Shelton Assistant Vice President Product Development
Measuring Quality In Health Care Linda K. Shelton Assistant Vice President Product Development
 Overview • • Who is NCQA Ways We Assess Quality How We Develop Measures What Measurement Can Do
Overview • • Who is NCQA Ways We Assess Quality How We Develop Measures What Measurement Can Do
 • Private, non-profit health care quality oversight organization • Measures and reports on health care quality • Unites diverse groups around common goal: improving health care quality
• Private, non-profit health care quality oversight organization • Measures and reports on health care quality • Unites diverse groups around common goal: improving health care quality
 NCQA Assessment Programs • Managed Care Organizations • Preferred Provider Organizations • Managed Behavioral Healthcare Organizations • Disease Management Organizations • Physician Organizations • Credentials Verification Organizations
NCQA Assessment Programs • Managed Care Organizations • Preferred Provider Organizations • Managed Behavioral Healthcare Organizations • Disease Management Organizations • Physician Organizations • Credentials Verification Organizations
 NCQA Assessment Programs • Privacy Certification for Business Associates • HEDIS Auditors and Software Vendors • Organizations Providing Utilization Management or Credentialing Services • Human Research Protection • Diabetes Physician Recognition
NCQA Assessment Programs • Privacy Certification for Business Associates • HEDIS Auditors and Software Vendors • Organizations Providing Utilization Management or Credentialing Services • Human Research Protection • Diabetes Physician Recognition
 Ways We Assess Quality: Standards On-site surveys: Reviews of the clinical and administrative systems necessary for quality care and service Web-based tools: Readiness evaluations and submissions of documents online, for efficient surveys We grade on performance against standards.
Ways We Assess Quality: Standards On-site surveys: Reviews of the clinical and administrative systems necessary for quality care and service Web-based tools: Readiness evaluations and submissions of documents online, for efficient surveys We grade on performance against standards.
 Ways We Assess Quality: Measures HEDIS ®: Specified, audited key measures of clinical effectiveness for health plans Diabetes Physician Recognition Program: Specified, audited key measures of diabetes care for physicians CAHPS® 3. 0 H: A specified, audited survey used to measure members’ experience with the care and service they receive from health plans We grade on quantitative measures.
Ways We Assess Quality: Measures HEDIS ®: Specified, audited key measures of clinical effectiveness for health plans Diabetes Physician Recognition Program: Specified, audited key measures of diabetes care for physicians CAHPS® 3. 0 H: A specified, audited survey used to measure members’ experience with the care and service they receive from health plans We grade on quantitative measures.
 How We Select Measures • Practice Guidelines • Evidence-based medicine • Minimum 2 years after recommendation to allow time for implementation • Committee on Performance Measurement (CPM): includes industry, health plan, consumer and purchaser representatives • Measurement Advisory Panels (MAPS): population and disease-specific experts
How We Select Measures • Practice Guidelines • Evidence-based medicine • Minimum 2 years after recommendation to allow time for implementation • Committee on Performance Measurement (CPM): includes industry, health plan, consumer and purchaser representatives • Measurement Advisory Panels (MAPS): population and disease-specific experts
 What Makes a Good Measure Relevance Meaningful Health importance Financial importance Cost-effectiveness Strategically important Controllability Scientific Soundness Clinical Evidence Reproducible Valid Accurate Variance among systems Case-mix Adjustment/Risk Adjustment Potential for improvement Comparability of data sources Feasibility Precisely specified Reasonable cost Confidential Logistically feasible Auditable
What Makes a Good Measure Relevance Meaningful Health importance Financial importance Cost-effectiveness Strategically important Controllability Scientific Soundness Clinical Evidence Reproducible Valid Accurate Variance among systems Case-mix Adjustment/Risk Adjustment Potential for improvement Comparability of data sources Feasibility Precisely specified Reasonable cost Confidential Logistically feasible Auditable
 What Measurement Can Do
What Measurement Can Do
 Chaos Gets Headlines. . . But It’s Not the Whole Story
Chaos Gets Headlines. . . But It’s Not the Whole Story
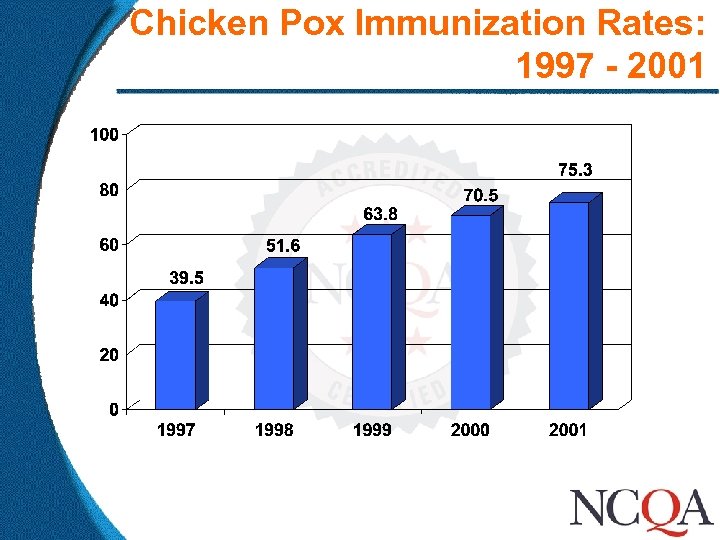 Chicken Pox Immunization Rates: 1997 - 2001
Chicken Pox Immunization Rates: 1997 - 2001
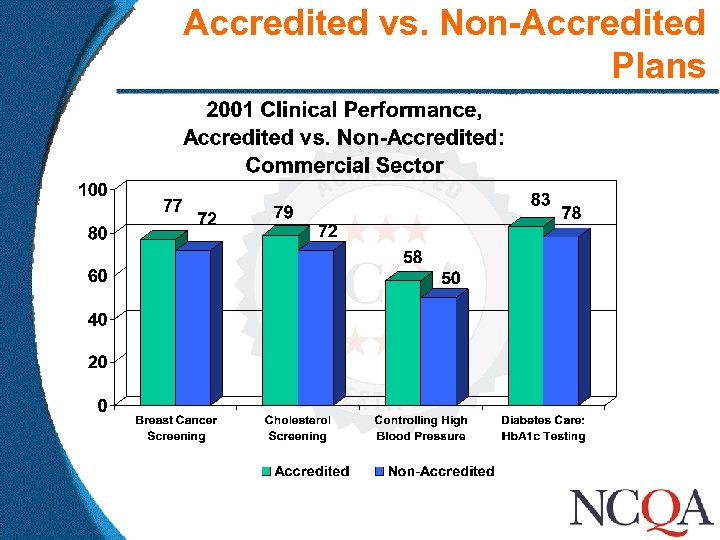 Accredited vs. Non-Accredited Plans
Accredited vs. Non-Accredited Plans
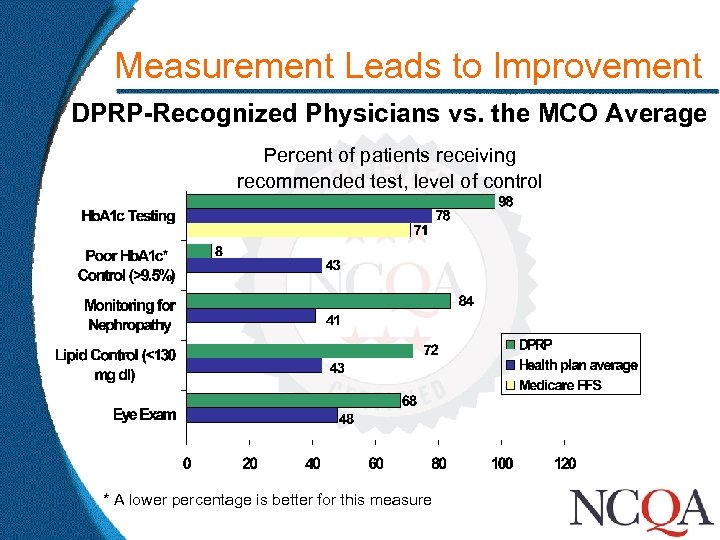 Measurement Leads to Improvement DPRP-Recognized Physicians vs. the MCO Average Percent of patients receiving recommended test, level of control * A lower percentage is better for this measure
Measurement Leads to Improvement DPRP-Recognized Physicians vs. the MCO Average Percent of patients receiving recommended test, level of control * A lower percentage is better for this measure
 Incentives • Public reporting—comparable measures on report cards • Market share—purchasers demanding a level of measurable quality • Financial rewards—direct payments for quality • Competition—within and between organizations
Incentives • Public reporting—comparable measures on report cards • Market share—purchasers demanding a level of measurable quality • Financial rewards—direct payments for quality • Competition—within and between organizations
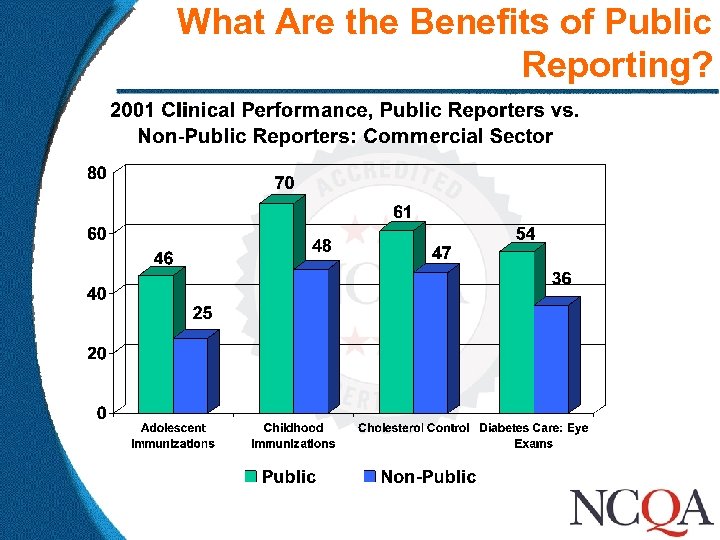 What Are the Benefits of Public Reporting?
What Are the Benefits of Public Reporting?
 Health. Choices™ Health Portal • Easy interface with the corporate intranet • Customized version of the HPRC • Listing of doctors and hospitals affiliated with health plan options • Comprehensive, reliable health content • Specific company benefit information
Health. Choices™ Health Portal • Easy interface with the corporate intranet • Customized version of the HPRC • Listing of doctors and hospitals affiliated with health plan options • Comprehensive, reliable health content • Specific company benefit information
 Health Plan Report Card
Health Plan Report Card
 • Recognized physicians receive: – A certificate of recognition – Performance reports with comparative data – Referrals through 1 -800 -DIABETES; NCQA, ADA Web sites – Preferential reimbursement?
• Recognized physicians receive: – A certificate of recognition – Performance reports with comparative data – Referrals through 1 -800 -DIABETES; NCQA, ADA Web sites – Preferential reimbursement?
 Financial Rewards for Quality • • • Performance guarantees Return on investment Payments from purchasers to Providers Bridges logo here Bonuses from health plans to providers— California Pay for Performance
Financial Rewards for Quality • • • Performance guarantees Return on investment Payments from purchasers to Providers Bridges logo here Bonuses from health plans to providers— California Pay for Performance
 NCQA’s Quality Dividend Calculator • Free, Web-based utility • User enters general information about employee population, overall revenues • Generates projected productivity gains (in terms of sick days, sick wages) from contracting with accredited plans
NCQA’s Quality Dividend Calculator • Free, Web-based utility • User enters general information about employee population, overall revenues • Generates projected productivity gains (in terms of sick days, sick wages) from contracting with accredited plans


