0de0337ceebffcdac9e40da91c1ae5a8.ppt
- Количество слайдов: 39

Management of the Bleeding Patient Dr. Alan Tinmouth Director, Adult Regional Hemophilia and Bleeding Disorders Clinic February 1 st, 2005

Outline n Review the mechanism of blood coagulation n Understand the tests used in the investigation of bleeding disorders n Understand therapeutic options in the management of bleeding patients n “Hemostasis” Poker
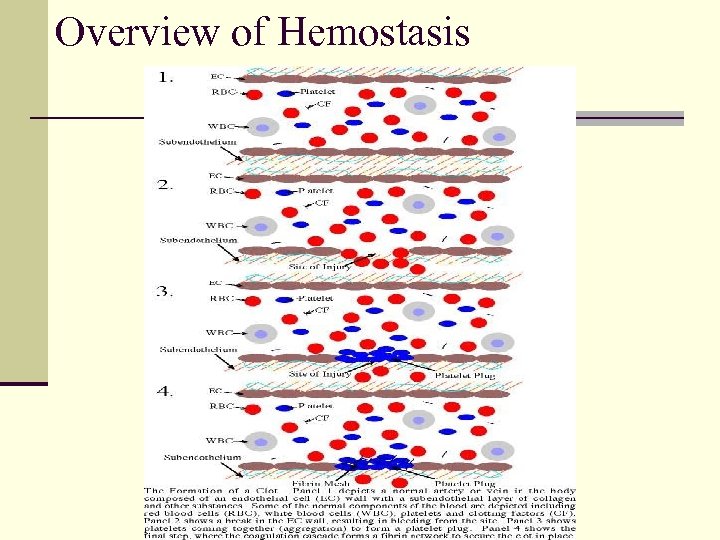
Overview of Hemostasis

Primary Hemostasis: Platelets Adhesion I. n Platelet glycoprotein Ib/V/IX adheres to subendothelium binding is primarily to v. WF Activation II. n n Shape change formation of pseudopods Anionic phospholipids (phospatidylserine and phosphoethanolamine) exposed on external membrane Glycoprotein IIb/IIIa exposed on surface Secretion of platelet granules Aggregation III. n Platelets bind to each other via Gp IIb/IIIa receptor and soluble fibrinogen and v. WF FORMATION OF HEMOSTATIC PLUG
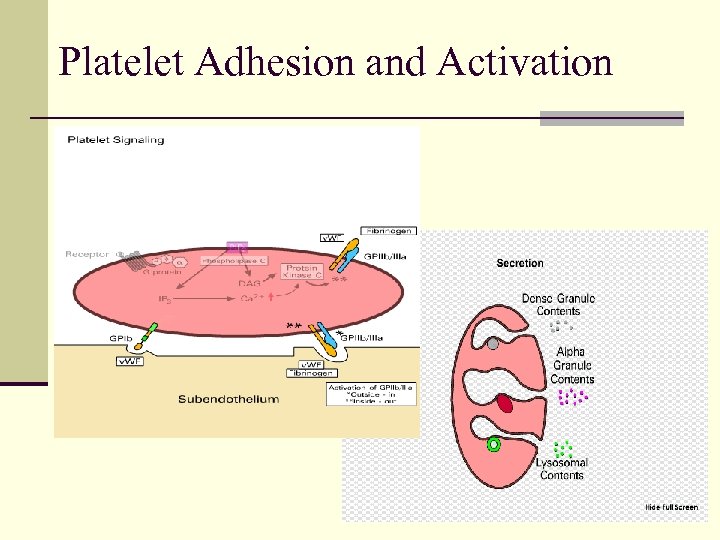
Platelet Adhesion and Activation
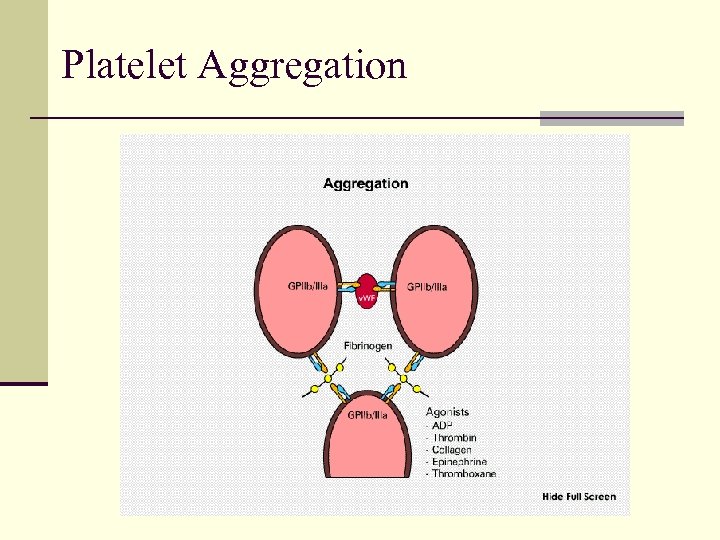
Platelet Aggregation

Secondary Hemostasis: Coagulation Factors n Coagulation factors are proteins that circulate primarily in inactive state (proenzyme), which are converted to active enzyme n Activation of coagulation factors is a stepwise process of one activated factor activating subsequent factor(s) n Historically separated into the intrinsic pathway and extrinsic pathway n n Intrinsic and extrinsic pathways believed to act independently and lead to formation of fibrin clot through separate “coagulation cascades” Model fails to explain many coagulation abnormalities seen clinically
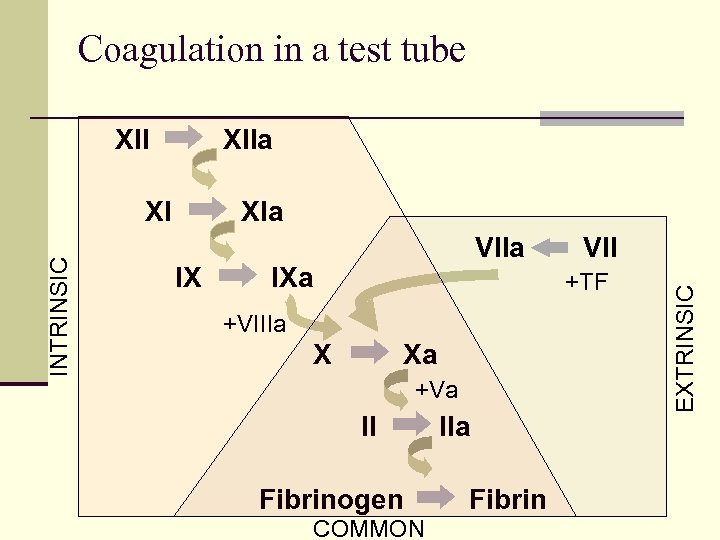
Coagulation in a test tube XIIa XIa IX VIIa IXa VII +TF +VIIIa X Xa +Va II Fibrinogen COMMON IIa Fibrin EXTRINSIC INTRINSIC XI
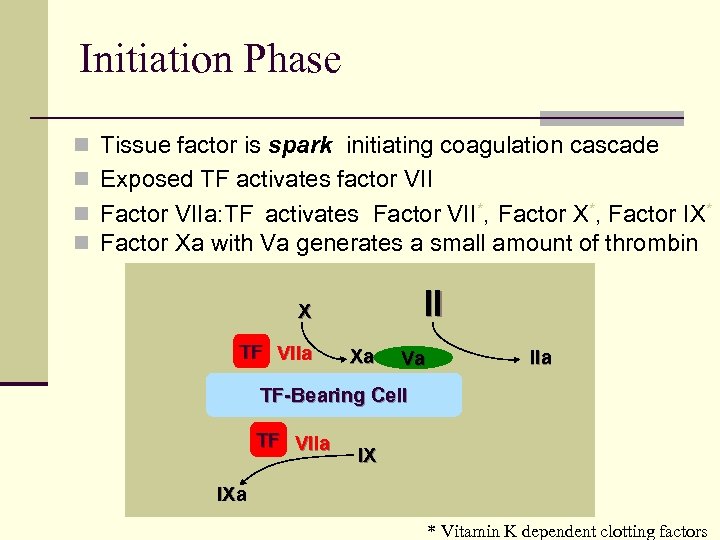
Initiation Phase n Tissue factor is spark initiating coagulation cascade n Exposed TF activates factor VII n Factor VIIa: TF activates Factor VII*, Factor X*, Factor IX* n Factor Xa with Va generates a small amount of thrombin II X TF VIIa Xa Va IIa TF-Bearing Cell TF VIIa IX IXa * Vitamin K dependent clotting factors
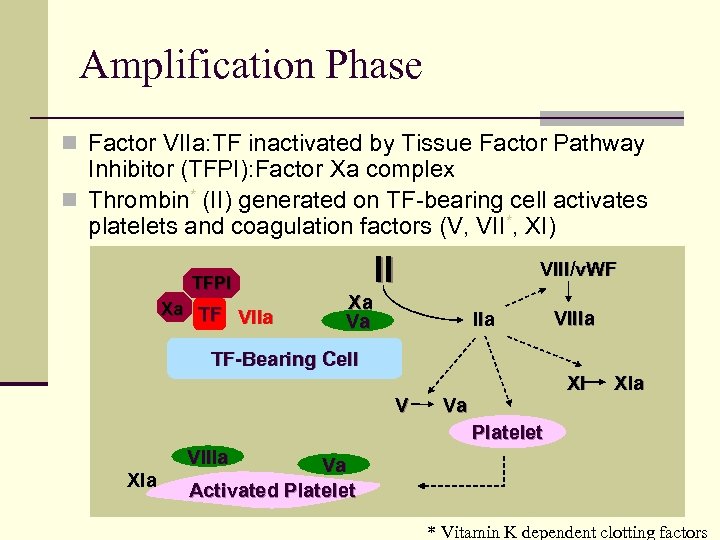
Amplification Phase n Factor VIIa: TF inactivated by Tissue Factor Pathway Inhibitor (TFPI): Factor Xa complex n Thrombin* (II) generated on TF-bearing cell activates platelets and coagulation factors (V, VII*, XI) TFPI Xa TF VIIa II VIII/v. WF Xa Va IIa VIIIa TF-Bearing Cell V XI Va XIa Platelet VIIIa XIa Va Activated Platelet * Vitamin K dependent clotting factors
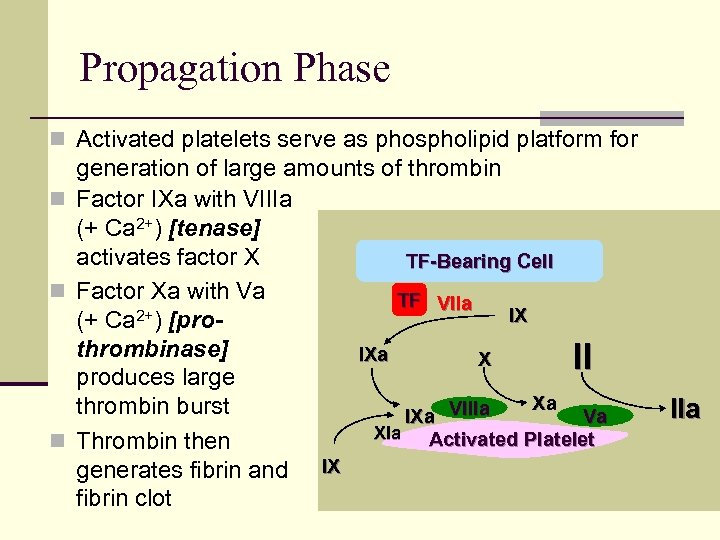
Propagation Phase n Activated platelets serve as phospholipid platform for generation of large amounts of thrombin n Factor IXa with VIIIa (+ Ca 2+) [tenase] activates factor X TF-Bearing Cell n Factor Xa with Va TF VIIa IX (+ Ca 2+) [prothrombinase] IXa X II produces large Xa thrombin burst Va IXa VIIIa XIa Activated Platelet n Thrombin then generates fibrin and IX fibrin clot IIa
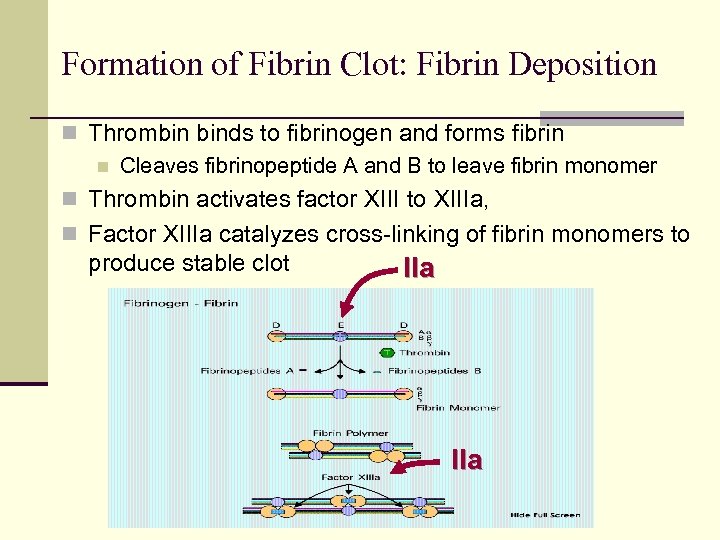
Formation of Fibrin Clot: Fibrin Deposition n Thrombin binds to fibrinogen and forms fibrin n Cleaves fibrinopeptide A and B to leave fibrin monomer n Thrombin activates factor XIII to XIIIa, n Factor XIIIa catalyzes cross-linking of fibrin monomers to produce stable clot IIa
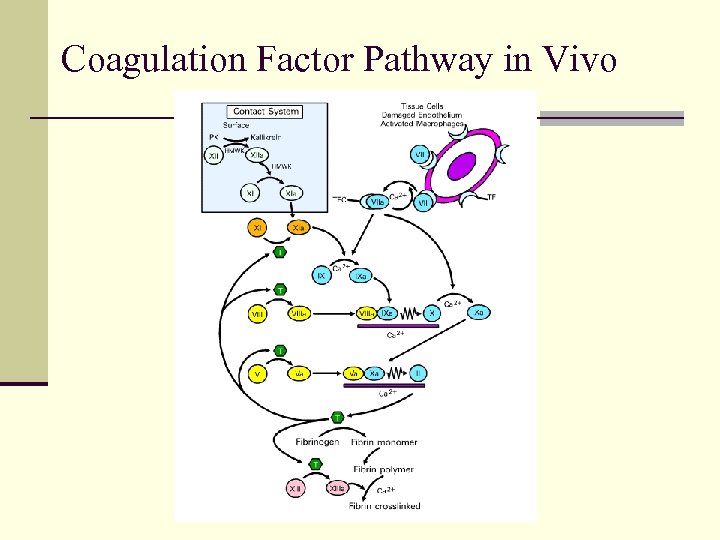
Coagulation Factor Pathway in Vivo

Fibrinolysis n Fibrin clots are temporary scaffolding that allow for cellular wound healing n Dissolution of clots needed to maintain vessel patency n Plasmin (converted from plasminogen) is primary agent of fibrinolysis n Fibrinolysis is controlled by Activators of plasminogen activation n Inhibitors of plasmin n

Fibrinolysis and Plasmin Inhibition Fibrinolysis n Plasminogen and t-PA bind to fibrin lysine sites n Activated plasmin protected from degradation by alpha 2 -antiplasmin n Plasmin optimally positioned to degrade fibrin Plasmin Inhibition n Circulating plasmin is rapidly inactivated by alpha 2 - antiplasmin n Prevents systemic (widespread) fibrinolysis n Thrombin activated fibrinolytic inhibitor (TAFI) removes lysine sites from fibrin to n downregulates fibrinolysis during initial clot formation
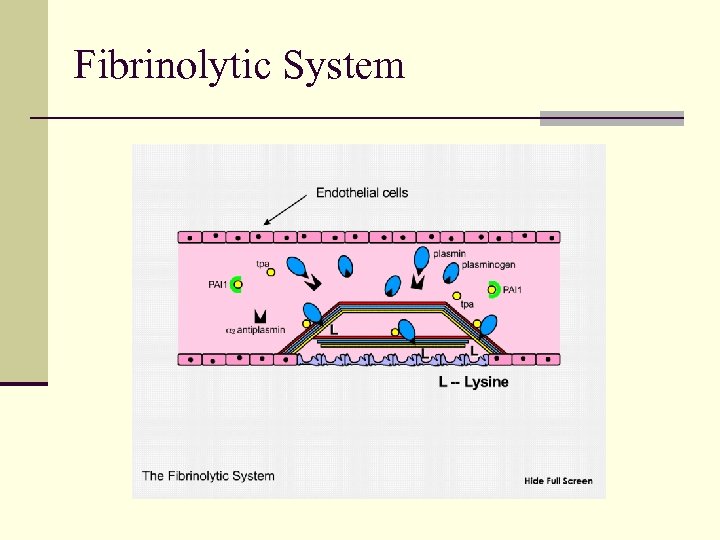
Fibrinolytic System
Laboratory Investigations

Platelet Disorders n Platelet Count n Platelet Morphology (blood film) n Platelet Aggregation / Release n von Willebrand Studies n von Willebrand Antigen n Ristocetin Cofactor n von Willebrand Multimers n Bleeding Time

Coagulation Factor Disorders n Prothrombin Time / International Normalized Ratio n Activated Partial Thromboplastin Time n Thrombin Time n 50: 50 Mixing Studies n Coagulation Factor Assays
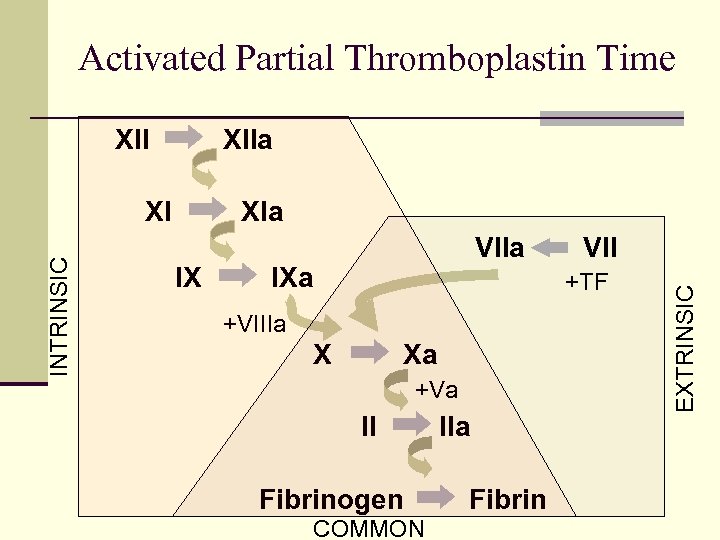
Activated Partial Thromboplastin Time XIIa XIa IX VIIa IXa VII +TF +VIIIa X Xa +Va II Fibrinogen COMMON IIa Fibrin EXTRINSIC INTRINSIC XI
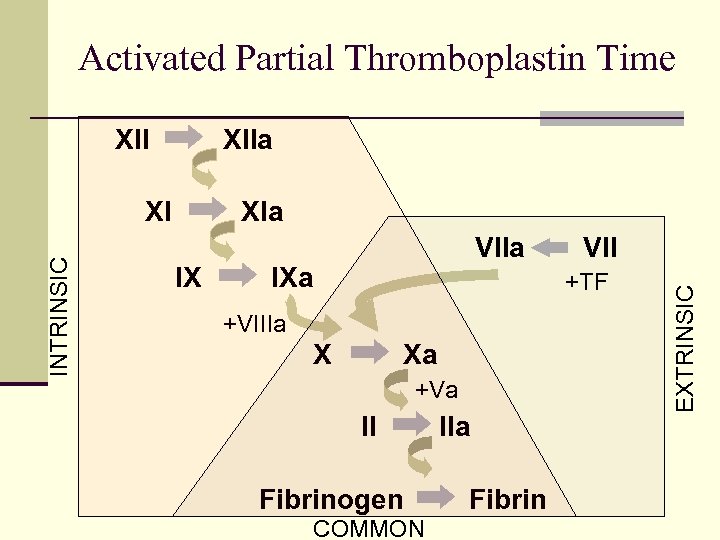
Activated Partial Thromboplastin Time XIIa XIa IX VIIa IXa VII +TF +VIIIa X Xa +Va II Fibrinogen COMMON IIa Fibrin EXTRINSIC INTRINSIC XI
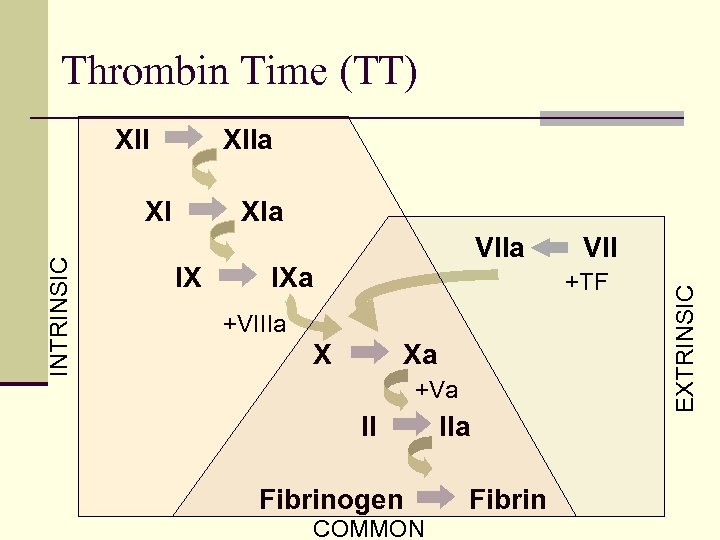
Thrombin Time (TT) XIIa XIa IX VIIa IXa VII +TF +VIIIa X Xa +Va II Fibrinogen COMMON IIa Fibrin EXTRINSIC INTRINSIC XI

Fibrinolytic System n Euglobulin Lysis n Alpha 2 Antiplasmin n Factor XIII levels
Therapy

Platelet Transfusions - Products Random Donor Platelets ü Separated from whole blood donations ü Dose = 5 units (250 -300 mls) ü ABO matched preferable but not mandatory ü Increases platelet ct by 5 -10 x 109/L per unit Single Donor Platelets ü Collected from 1 donor by apheresis ü Equivalent to 5 -6 random donor platelets ü Decrease donor exposure ü Can be matched if patient has identified antibodies to platelets (alloimmune platelet refractoriness)

Indications for Platelet Transfusions Thrombocytopenia Platelet Dysfunction n n Congenital Acquired Therapeutic n n Plat ct < 50 x 109/L Plat dysfunction Prophylactic n n Prior to invasive procedures 9 n Plat ct < 50 -100 x 10 /L Prevent spontaneous bleeding 9 n Plat ct 10 x 10 /L

Fresh Frozen Plasma n n Made from whole blood within 8 hrs of collection Contains all coagulation factors n n n Minimum factor VIII level of 0. 7 IU/ml 200 -250 mls / unit Effect may only last 4 hrs (t 1/2 of factor VII) Indications: INR / PTT > 1. 5 x normal and 1. 2. Bleeding or Emergency procedure or operation

Fresh Frozen Plasma Dose: n 10 -15 ml/kg for bleeding patients n Sufficient to increase all individual coagulation factors by 30% (minimum hemostatic level) n 5 -7 ml/kg may be sufficient for warfarin reversal Alternatives n Vitamin K ü ü 2 mg will correct INR in 12 -24 hrs No effect on PTT (factors VIII, IX, XI) Oral dose more effective than subcutaneous Intravenous associated with anaphylactic reactions

Cryoprecipitate n Precipitate collected from plasma thawed at 40 C n 10 -15 mls/unit n Contains specific clotting factors from plasma ü Factor VIII ü Fibrinogen ü von Willebrand’s Factor ü Factor XIII Indications 1. Fibrinogen < 1. 0 g/L 2. Dysfibrinogenemia

Cryoprecipitate Dose n 1 unit / 5 -10 kg body weight (total 8 -10 units) n t ½ of 3 -5 days Alternatives n Factor VIII or IX Deficiency ü recombinant factor VIII or IX n Von Willebrand’s Disease ü virally inactivated plasma derived factor concentrates n Other factor deficiencies ü recombinant factor concentrates ü virally inactivated plasma derived factor concentrates

DDAVP n Synthetic vasopressin n Release of VIII and v. WF from endothelium n May also help with platelet dysfunction n 2 -3 fold rise in levels n Dose – 0. 3 ug/kg q 12 -24 hours n Tachyphylaxis may occur after 2 -3 doses
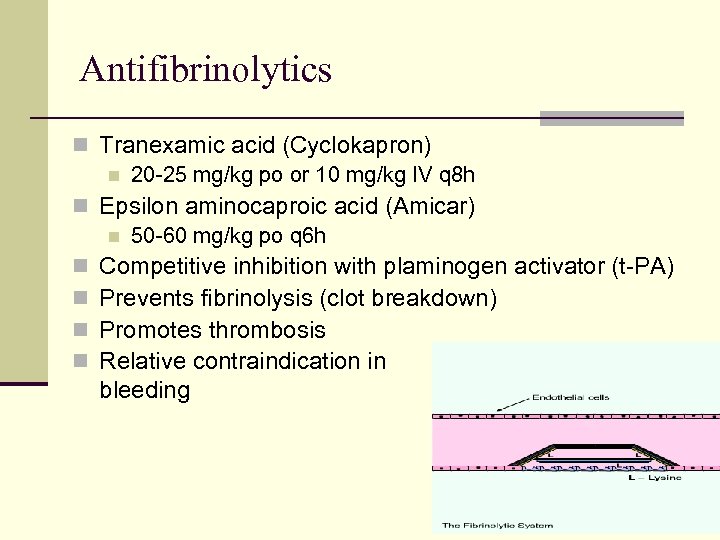
Antifibrinolytics n Tranexamic acid (Cyclokapron) n 20 -25 mg/kg po or 10 mg/kg IV q 8 h n Epsilon aminocaproic acid (Amicar) n 50 -60 mg/kg po q 6 h n Competitive inhibition with plaminogen activator (t-PA) n Prevents fibrinolysis (clot breakdown) n Promotes thrombosis n Relative contraindication in renal bleeding

Recombinant Factor VIIa n Initiates coagulation by interaction with TF n Only approved for treatment of hemophilia with inhibitors n Treat/prevent bleeding in other patient groups? n n n Efficacy not proven Risk of thrombosis? Primary use is bleeding patients refractory to other treatments n Dose for hemophilia 90 ug/kg q 2 -3 h n Lower dose often effective in other patients 30 -40 ug/kg n Vials of 1. 2 mg, 2. 4 mg, 4. 8 mg n Cost ~ $1000/mg
“Hemostasis” Poker
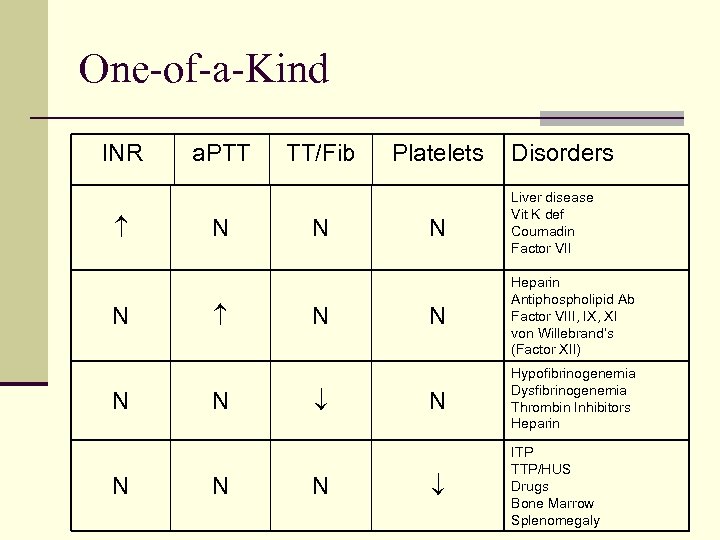
One-of-a-Kind INR N N N a. PTT N N N TT/Fib N N N Platelets Disorders N Liver disease Vit K def Coumadin Factor VII N Heparin Antiphospholipid Ab Factor VIII, IX, XI von Willebrand’s (Factor XII) N Hypofibrinogenemia Dysfibrinogenemia Thrombin Inhibitors Heparin ITP TTP/HUS Drugs Bone Marrow Splenomegaly
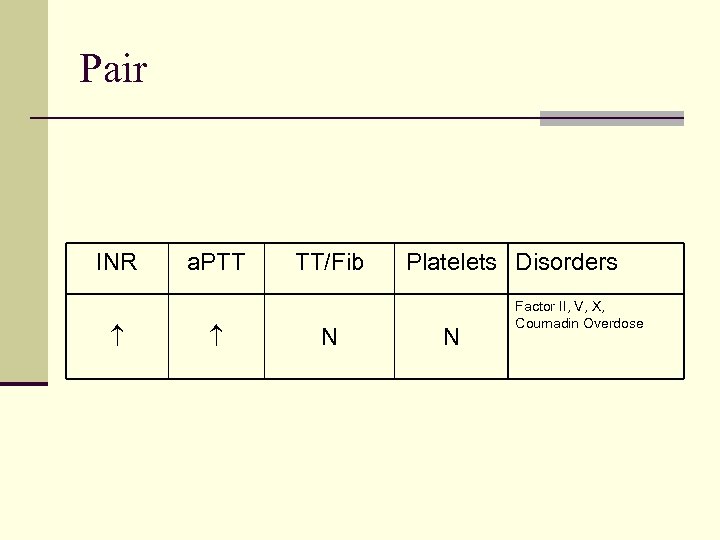
Pair INR a. PTT TT/Fib N Platelets Disorders N Factor II, V, X, Coumadin Overdose
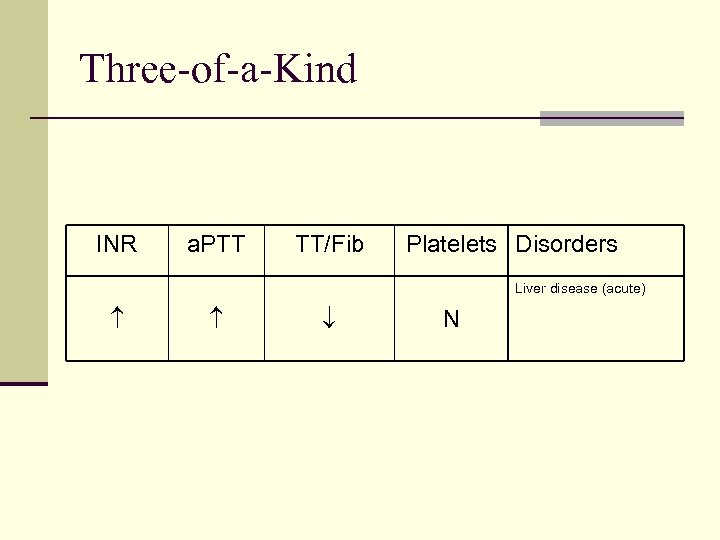
Three-of-a-Kind INR a. PTT TT/Fib Platelets Disorders Liver disease (acute) N
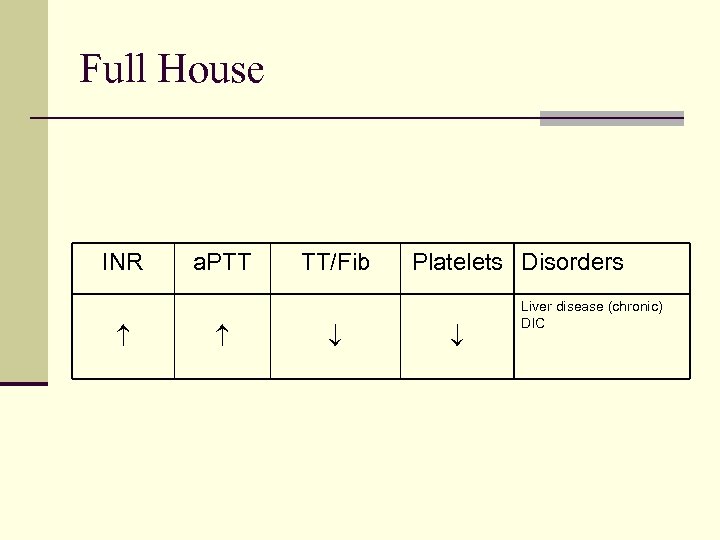
Full House INR a. PTT TT/Fib Platelets Disorders Liver disease (chronic) DIC

Nothing n Von Willebrand’s Disease n Mild Hemophilia A or B n Mild Factor XI deficiency n Platelet Function Disorder n Factor XIII deficiency n Alpha 2 antiplasmin deficiency n Plasminogen Activator Inhibitor deficiency
0de0337ceebffcdac9e40da91c1ae5a8.ppt