824370e2e4d83934d4d87be25ac41b6c.ppt
- Количество слайдов: 30

MANAGEMENT OF BLUNT OCULAR TRAUMA SPEAKER : KUMAR SAURABH

BIRMINGHEM EYE TRAUMA TERMINOLOGY SYSTEM (BETTS) * Eye Wall : Sclera and Cornea Closed Globe Injury : No full thickness wound of eye wall. Open Globe Injury : Full thickness wound of eye wall. Contusion : No full thickness wound. Lamellar Laceration : Partial thickness wound of eye wall. Rupture : Full thickness wound of eye wall caused by blunt object. Laceration : Full thickness wound of eye wall caused by sharp object. Penetrating Injury : Entrance wound sans exit wound. Perforating Injury : Entrance wound and exit wounds. *Kuhn F, Morris R, Witherspoon CD, Heimann K, Jaffers JB, Treister G ; Ophthalmology 1996 Feb; 103(2) 240 -3.
LID AND ORBITAL SOFT TISSUE ABRASION : Normal saline irrigation and cleansing of necrotic debris. Documentation with drawings and photographs. Prophylactic topical antibiotics. Tetanus prophylaxis. HEMATOMA : Rule out fracture of orbital roof or basal skull. Ice packs for first 24 hours followed by hot packs. Indications of Incision and Drainage : - Infected Tense Large hematoma.

ORBITAL OEDEMA : WORK UP : Rule out occult globe lacerations, puncture wounds and foreign bodies. Examination : Under topical anaesthesia with two Desmarres retractors. Light perception and pupillary response. Forced Duction Test : To confirm nonspecific limitations of motility, if any. CT Scan : To rule out orbital fracture or major soft tissue injury. TREATMENT : Ice packs : Diminish oedema and minor surface anaesthetic. Oral Corticosteroids : Early resolution of oedema and recovery of motility. Lateral Canthotomy : Elevated intraocular pressure Features of CRAO Central vision loss Orbital Decompression

LID LACERATION : WORK UP : Tetanus toxoid Systemic Antibiotics : Grossly contaminated wound more than 3 hours old. Thorough cleansing with normal saline. Iced saline compress. Preoperative documentation with photographs and drawings. TIMING OF REPAIR : Within 24 hours of trauma ANAESTHESIA : Local anaesthesia for isolated lid laceration General anaesthesia : Associated lacrimal system injury Extensive trauma Associated bony orbital trauma Uncooperative patient

REPAIR OF LID LACERATION v SUPERFICIAL LACERATIONS : Repaired with 6 -0 black silk Sutures removed after 5 days. v LID MARGIN LACERATIONS: Trimming of irregular edges. Realignment of margin with a 6 -0 black silk suture along meibomian gland orifices. Repair of trasal plate with partial thickness 6 -0 Polyglycolic acid (Vicryl) suture. Lash line suture with 6 -0 black silk. Skin closure with 6 -0 black silk interrupted sutures. Suture removal after 7 -10 days. v LACERATION WITH TISSUE LOSS : Small defects : Lateral canthotomy followed by usual repair. Moderate defects : Tenzel semicircular flap procedure Large defects : Mustarde cheek rotation flap Eye lid sharing procedure Glabellar flap procedure
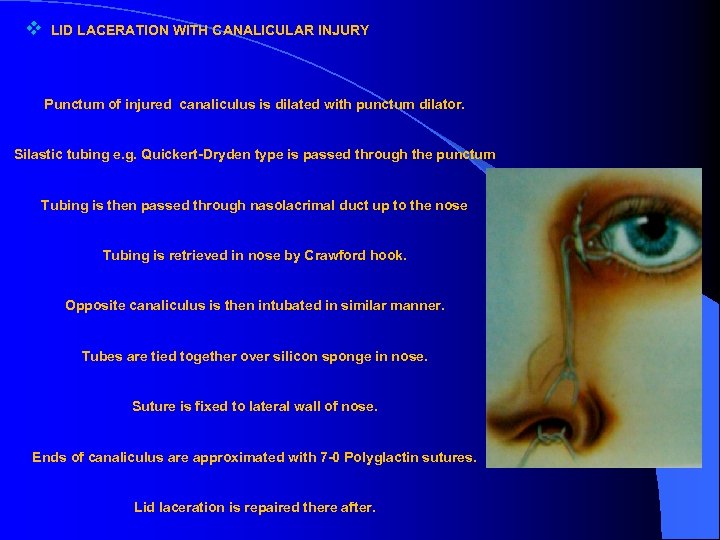
v LID LACERATION WITH CANALICULAR INJURY Punctum of injured canaliculus is dilated with punctum dilator. Silastic tubing e. g. Quickert-Dryden type is passed through the punctum Tubing is then passed through nasolacrimal duct up to the nose Tubing is retrieved in nose by Crawford hook. Opposite canaliculus is then intubated in similar manner. Tubes are tied together over silicon sponge in nose. Suture is fixed to lateral wall of nose. Ends of canaliculus are approximated with 7 -0 Polyglactin sutures. Lid laceration is repaired there after.
CONJUNCTIVAL BLUNT TRAUMA SUBCONJUNCTIVAL : HEMORRHAGE CHEMOSIS : Best treatment is reassurance Tears substitutes Rule out globe injury Subsides spontaneously When Conjunctival prolapse develops – Lubricating ointment Corticosteroid cream SUBCONJUNCTIVAL : EMPHYSEMA CONJUNCTUVAL : FOREIGN BODY Rule out globe rupture or retained foreign body. Treatment of the cause of emphysema. Irrigation with normal saline Sweeping with cotton tipped applicator Removal with fine forceps Topical antibiotic prophylaxis

CORNEAL BLUNT TRAUMA ABRASION : DO’s Topical broad-spectrum antibiotic ointment Cycloplegic eye drop Firm pressure patching -- Controversial Follow up at 24 hours to exclude infection and monitor healing If infection is suspected : Discontinue patching Send corneal swab for culture Fortified antibiotic eye drops Topical antibiotics continued for 1 week after healing. DONT’s Never prescribe topical steroids Never prescribe topical anaesthetics Kaiser P. K. A comparison between pressure patching and no patching for corneal abrasion due to trauma or foreign body removal. Ophthalmology 1997 Feb; 104(2) 169 -70

ACUTE HYDROPS : Sympathy, Empathy and Reassurance Tell patients that “Corneal rupture will not occur” And that “Vision will improve in 3 months time. ” Residual parallel striae/fishmouth breaks do not impair vision.

CORNEAL FORIEGN BODY : PRELIMINARIES : History of circumstances of injury and identification of foreign body Multiple superficial : Irrigation with normal saline Discrete superficial : Foreign body spud or 25 G needle Deep, older than 7 days : Allowed to remain and spontaneously extrude if there is no infiltrate. Deep, large, suspected perforation : Through entry site-- Razor blade knife Through limbal route-- Intra-ocular foreign body forceps MEDICATIONS : Antibiotic eye ointment for 3 -5 days Cycloplegic eye drops Pressure patching -- Controversial Examination of fornices and conjunctiva foreign bodies Kaiser P. K. A comparison between pressure patching and no patching for corneal abrasion due to trauma or foreign body removal. Ophthalmology 1997 Feb; 104(2) 169 -70
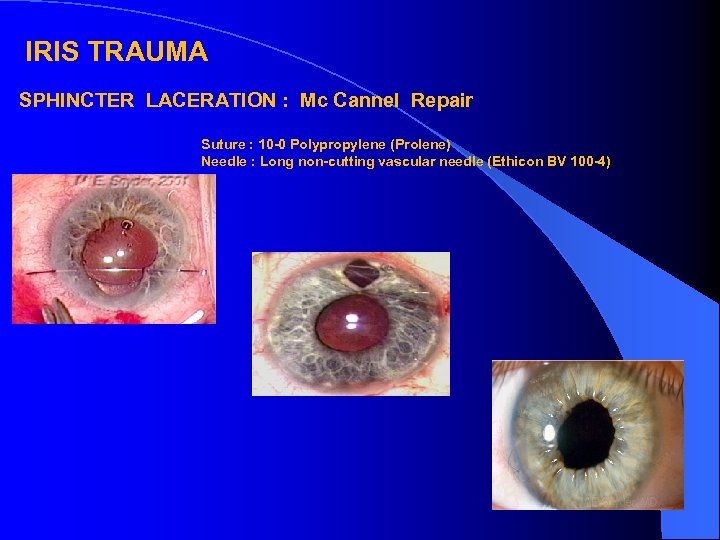
IRIS TRAUMA SPHINCTER LACERATION : Mc Cannel Repair Suture : 10 -0 Polypropylene (Prolene) Needle : Long non-cutting vascular needle (Ethicon BV 100 -4)
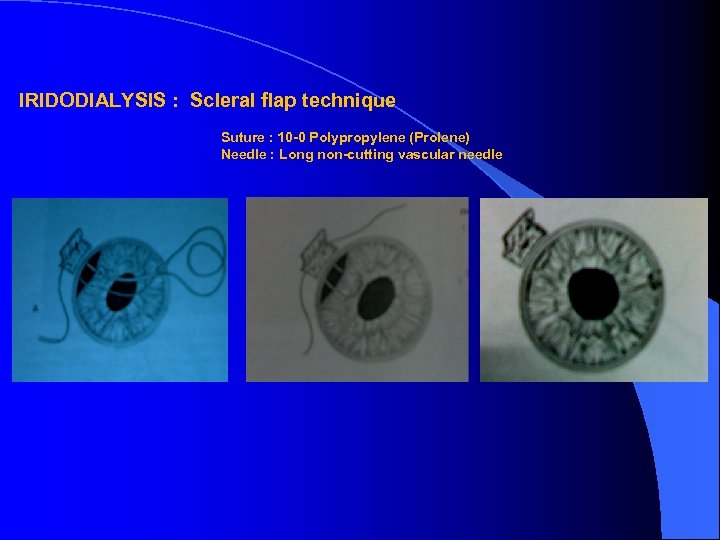
IRIDODIALYSIS : Scleral flap technique Suture : 10 -0 Polypropylene (Prolene) Needle : Long non-cutting vascular needle

TRAUMATIC HYPHEMA HISTORY : Time of sustaining the injury Type of injury sustained Personal or family history of bleeding disorder Drug intake in recent past History of any addiction specially alcohol History of similar episode in recent past

EXAMINATION : All patients with traumatic hyphema should be considered ruptured globe suspects. Vision Size of hyphema Clotted or fresh blood Intra-ocular pressure Corneal blood staining Gonioscopy : 1 month post-injury Ultrasonography LABORATORY TEST : Haemoglobin electrophoresis Liver function test
SUPPORTIVE TREATMENT : Rest with limited daily activities Metal shield to protect the eye ball Head elevation to 30 degree Control of systemic blood pressure MEDICAL MANAGEMENT : Atropine 1% eye drops Topical steroids Oral Aminocaproic acid 50 mg/kg every 4 hours for 5 days Timolol maleate eye drops Laxatives, sleeping pills.
INDICATIONS FOR HYPHEMA DRAINAGE A. Intra-ocular pressure criteria IOP > 50 mm Hg for 5 days or, IOP > 35 mm Hg for 7 days. B. Corneal blood staining criteria At the earliest sign of blood staining IOP > 25 mm Hg for 5 days in total or near-total hyphema C. Duration based criterion Large clot for more than 10 days duration SURGICAL TECHNIQUES Paracentesis and Anterior Chamber Washout : Surgical procedure of choice Clot expression and Limbal Delivery : 4 th to 7 th day Automated Hyphemaectomy

TRAUMATIC GLAUCOMA ACUTE GLAUCOMA : Topical steroids – Reduces inflammation and infiltration of meshwork Avoids/minimises trabecular meshwork scarring. Topical beta adrenergic agonists Oral carbonic anhydrase inhibitors CHRONIC GLAUCOMA : Managed as open angle glaucoma [ANGLE RECESSION GLAUCOMA] Argon Laser Trabeculoplasty Trabeculectomy with Mitomycin C application GHOST CELL GLAUCOMA : Topical beta adrenergic blockers Carbonic anhydrase inhibitors Anterior chamber washout Pars plana vitrectomy
CONTUSION CATARACTS INDICATION OF TREATMENT : Dimness of vision Phacoanaphylactic uveitis Phacolytic glaucoma MEDICAL MANAGEMENT : Miotics – For small off axis opacities causing glare Topical steroids – To control inflammation Antiglaucoma medications SURGICAL MANAGEMENT : Intact posterior capsule No lens displacement No vitreous in AC Anterior Limbal Approach Posterior capsule rupture Dislocated lens Vitreous in AC Pars plana Approach INTRA-OCULAR LENS : Anterior chamber IOL is avoided. PCIOL given if posterior capsule is intact Sulcus fixation lens is safest

GLOBE RUPTURE THINGS TO BE DONE BEFORE STARTING URGENT REPAIR Establish an intravenous line Start broad spectrum prophylactic intravenous antibiotics Tetanus toxoid or tetanus immunoglobulin Antiemetic medications Take sufficient time to obtain cooperation from patient Premium non nocere Apply aluminum shield to avoid pressure on globe Avoid any pressure on ruptured globe Avoid intraocular pressure measurement Avoid ointments or eye drops

Repair is done with 6 -0 or 7 -0 Polyglactin (Vicryl) Peritomy is a must. Place suture as soon as an area of ruptured sclera is discovered Sclera beneath extraocular muscle should be examined. For gaping wound, pass needle completely through one end before making second pass Prolapsed uveal tissue can be reposited by zippering technique Excision of prolapsed uveal tissue should be preceded by cauterization Any tissue removed from eye should be sent for histopathological examination

POST-OPERATIVE MANAGEMENT : 4 day course of intravenous antibiotics Topical and oral corticosteroids Topical antibiotics Topical beta blockers Cycloplegic eye drops Lubricating eye ointment Antiemetic medications
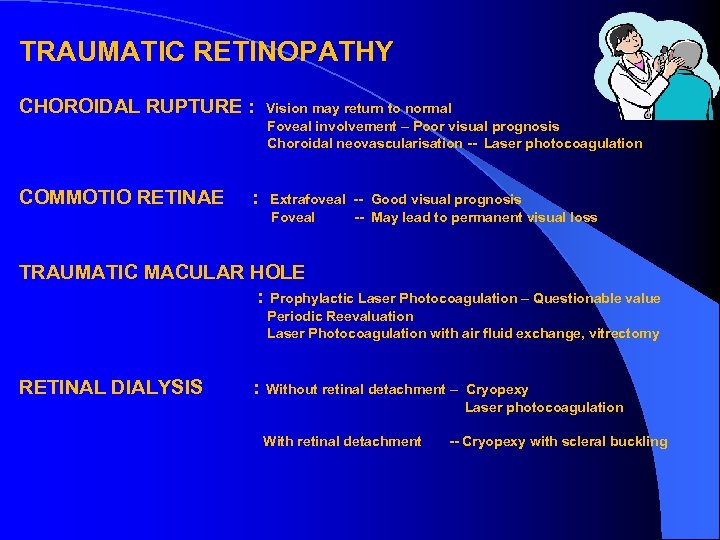
TRAUMATIC RETINOPATHY CHOROIDAL RUPTURE : COMMOTIO RETINAE : Vision may return to normal Foveal involvement – Poor visual prognosis Choroidal neovascularisation -- Laser photocoagulation Extrafoveal -- Good visual prognosis Foveal -- May lead to permanent visual loss TRAUMATIC MACULAR HOLE : Prophylactic Laser Photocoagulation – Questionable value Periodic Reevaluation Laser Photocoagulation with air fluid exchange, vitrectomy RETINAL DIALYSIS : Without retinal detachment – With retinal detachment Cryopexy Laser photocoagulation -- Cryopexy with scleral buckling
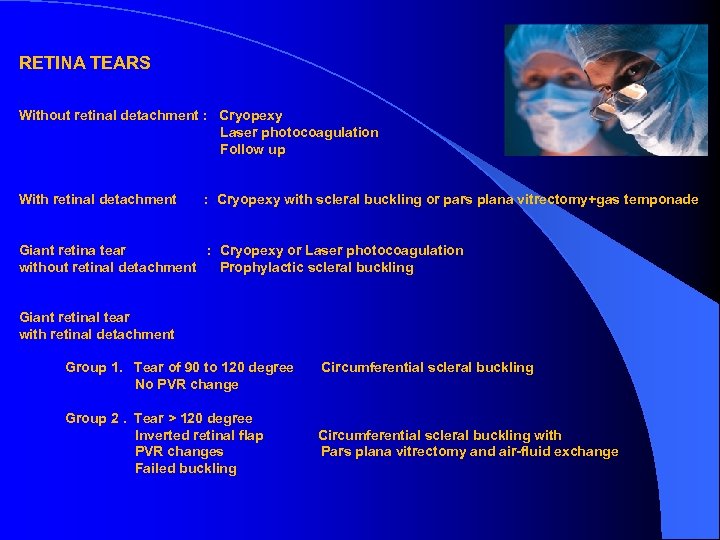
RETINA TEARS Without retinal detachment : Cryopexy Laser photocoagulation Follow up With retinal detachment : Cryopexy with scleral buckling or pars plana vitrectomy+gas temponade Giant retina tear : Cryopexy or Laser photocoagulation without retinal detachment Prophylactic scleral buckling Giant retinal tear with retinal detachment Group 1. Tear of 90 to 120 degree No PVR change Group 2. Tear > 120 degree Inverted retinal flap PVR changes Failed buckling Circumferential scleral buckling with Pars plana vitrectomy and air-fluid exchange
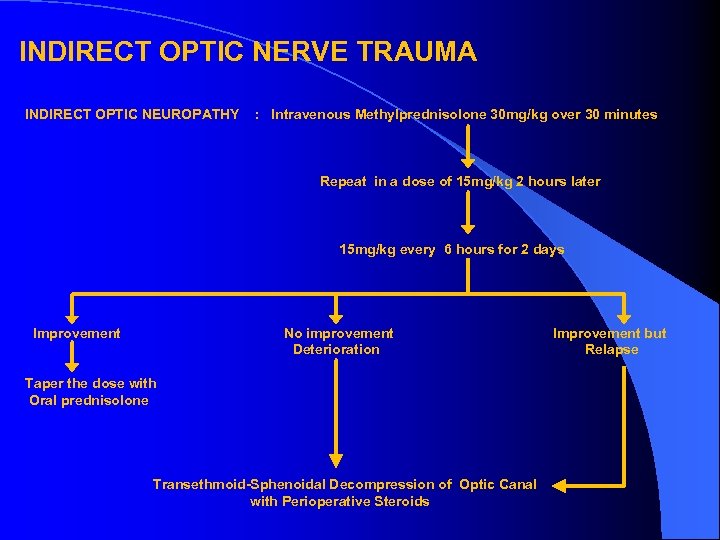
INDIRECT OPTIC NERVE TRAUMA INDIRECT OPTIC NEUROPATHY : Intravenous Methylprednisolone 30 mg/kg over 30 minutes Repeat in a dose of 15 mg/kg 2 hours later 15 mg/kg every 6 hours for 2 days Improvement No improvement Deterioration Taper the dose with Oral prednisolone Transethmoid-Sphenoidal Decompression of Optic Canal with Perioperative Steroids Improvement but Relapse

BLOW OUT FRACTURE OF ORBIT INDICATIONS OF SURGERY Enophthalmos > 3 mm Ocular motility limitation Diplopia TIMING OF SURGERY Within 10 days of fracture PREOPERATIVE STEROID Differentiates true entrapment from oedma Early resolution of diplopia Unmasks enophthalmos SURGERY Repair of orbital floor with strengthening Route -- Inferior fornicial-Lateral canthotomy approach Autologus graft -- Iliac bone, Rib, Calvarium Allograft -- Howmedica Bone Cement Cranioplast RTV Silicon Titanium mesh
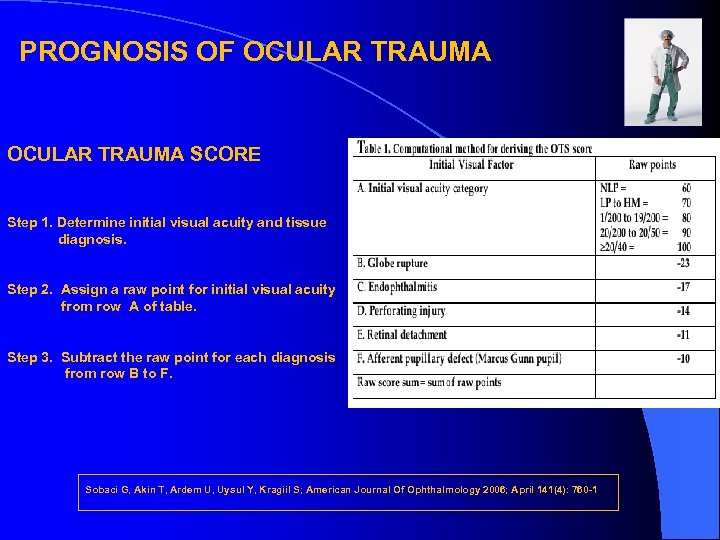

PROGNOSIS OF OCULAR TRAUMA SCORE Step 1. Determine initial visual acuity and tissue diagnosis. Step 2. Assign a raw point for initial visual acuity from row A of table. Step 3. Subtract the raw point for each diagnosis from row B to F. Sobaci G, Akin T, Ardem U, Uysul Y, Kragiil S; American Journal Of Ophthalmology 2006; April 141(4): 760 -1
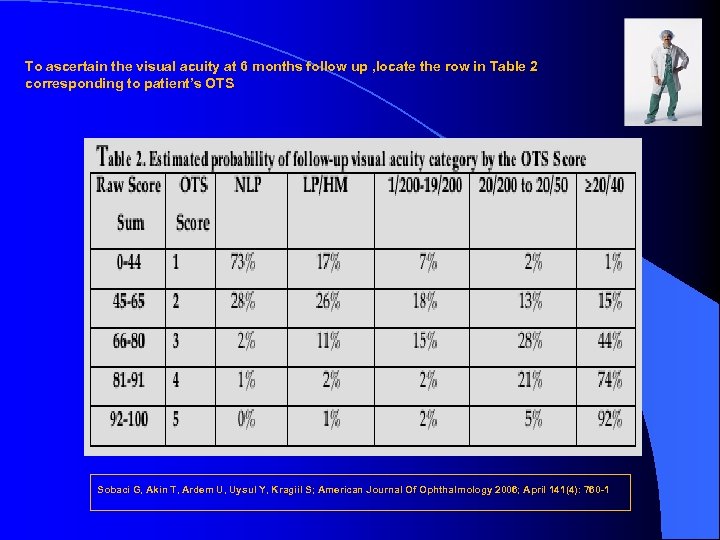
To ascertain the visual acuity at 6 months follow up , locate the row in Table 2 corresponding to patient’s OTS Sobaci G, Akin T, Ardem U, Uysul Y, Kragiil S; American Journal Of Ophthalmology 2006; April 141(4): 760 -1


THANK YOU
824370e2e4d83934d4d87be25ac41b6c.ppt