11.lung diseases.ppt
- Количество слайдов: 76
 LUNG Diseases
LUNG Diseases
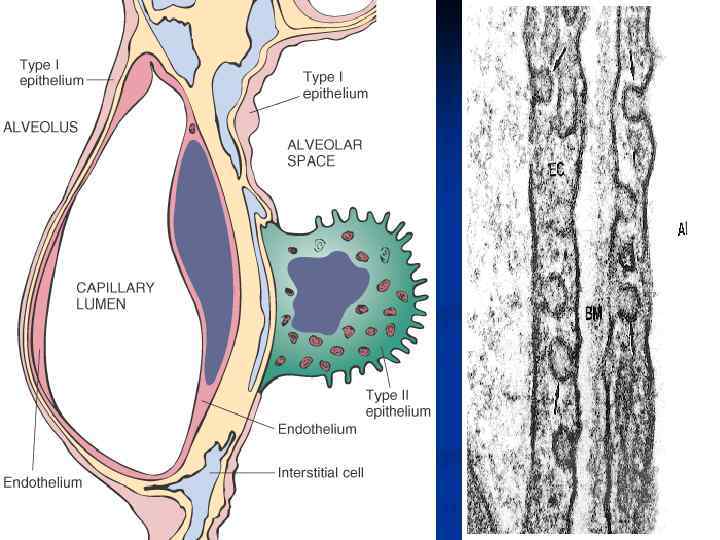
 Function of the Respiratory System · Oversees gas exchanges (oxygen and carbon dioxide) between the blood and external environment · Exchange of gasses takes place within the lungs in the alveoli(only site of gas exchange, other structures passageways · Passageways to the lungs purify, warm, and humidify the incoming air · Shares responsibility with cardiovascular system Slide 13. 2
Function of the Respiratory System · Oversees gas exchanges (oxygen and carbon dioxide) between the blood and external environment · Exchange of gasses takes place within the lungs in the alveoli(only site of gas exchange, other structures passageways · Passageways to the lungs purify, warm, and humidify the incoming air · Shares responsibility with cardiovascular system Slide 13. 2
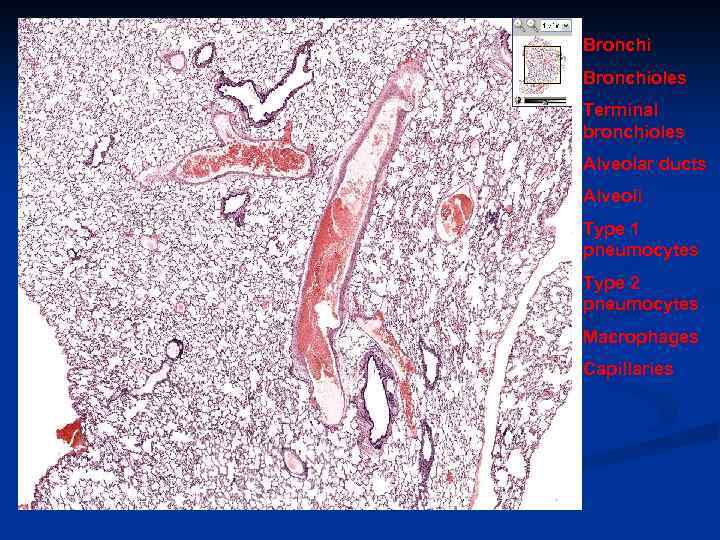 Bronchioles Terminal bronchioles Alveolar ducts Alveoli Type 1 pneumocytes Type 2 pneumocytes Macrophages Capillaries
Bronchioles Terminal bronchioles Alveolar ducts Alveoli Type 1 pneumocytes Type 2 pneumocytes Macrophages Capillaries
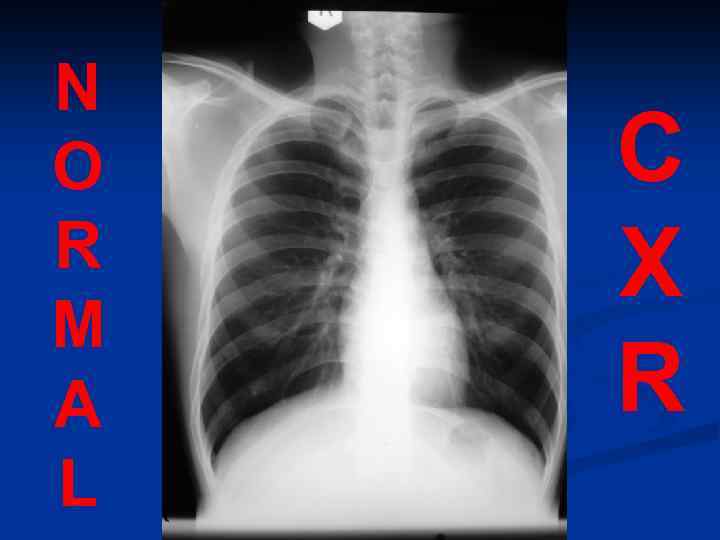 N O R M A L C X R
N O R M A L C X R
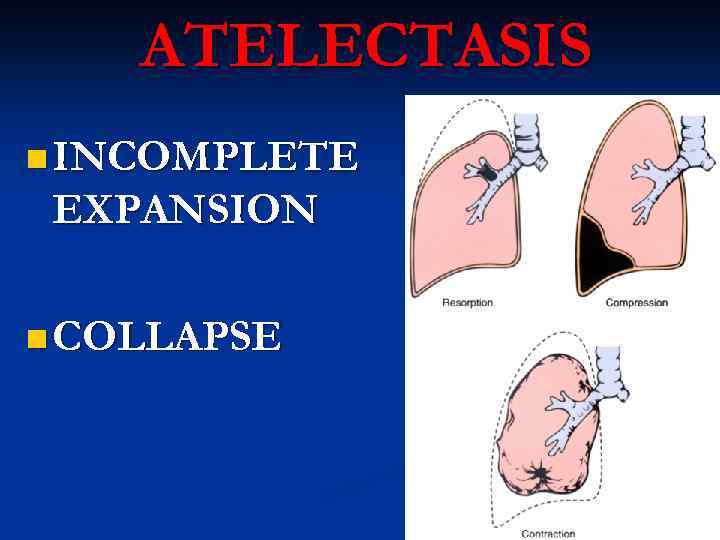 ATELECTASIS n INCOMPLETE EXPANSION n COLLAPSE
ATELECTASIS n INCOMPLETE EXPANSION n COLLAPSE
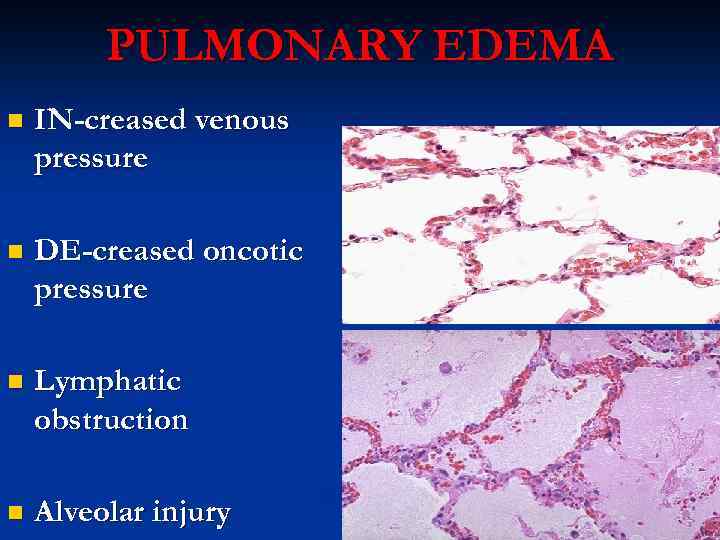 PULMONARY EDEMA n IN-creased venous pressure n DE-creased oncotic pressure n Lymphatic obstruction n Alveolar injury
PULMONARY EDEMA n IN-creased venous pressure n DE-creased oncotic pressure n Lymphatic obstruction n Alveolar injury
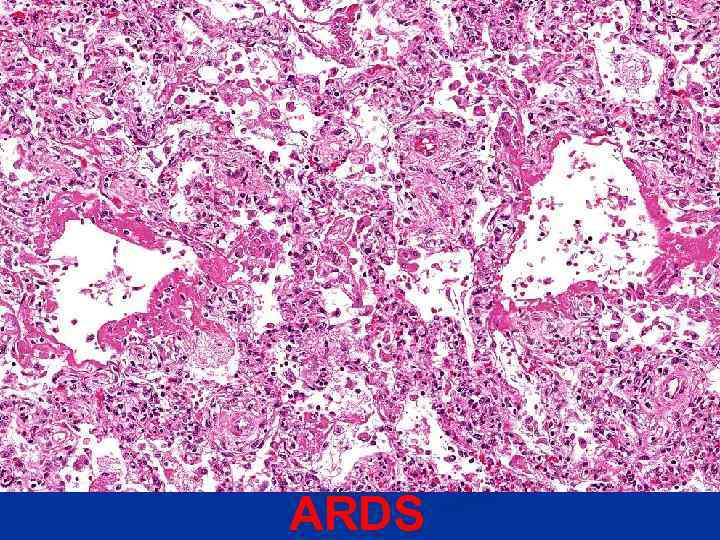 ARDS
ARDS
 ACUTE INTERSTITIAL PNEUMONIA n Think of it as ARDS with NO known etiology!
ACUTE INTERSTITIAL PNEUMONIA n Think of it as ARDS with NO known etiology!
 OBSTRUCTION v. RESTRICTION n OBSTRUCTION • RESTRICTION n Air or blood? Large or small? Inspiration or Expiration? “Compliance” “Infiltrative” n n REDUCED lung n Obstruction is VOLUME, DYSPNEA, SMALL AIRWAY CYANOSIS EXPIRATION obstruction, i. e. , wheezing REDUCED GAS TRANSFER n HYPEREXPANSION on CXR “GROUND GLASS” on CXR
OBSTRUCTION v. RESTRICTION n OBSTRUCTION • RESTRICTION n Air or blood? Large or small? Inspiration or Expiration? “Compliance” “Infiltrative” n n REDUCED lung n Obstruction is VOLUME, DYSPNEA, SMALL AIRWAY CYANOSIS EXPIRATION obstruction, i. e. , wheezing REDUCED GAS TRANSFER n HYPEREXPANSION on CXR “GROUND GLASS” on CXR
 OBSTRUCTION (c. OPD) n. EMPHYSEMA (almost always chronic) n. CHRONIC BRONCHITIS emphysema n. ASTHMA n. BRONCHIECTASIS
OBSTRUCTION (c. OPD) n. EMPHYSEMA (almost always chronic) n. CHRONIC BRONCHITIS emphysema n. ASTHMA n. BRONCHIECTASIS
 EMPHYSEMA COPD, or “END-STAGE” lung disease n Centri-acinar, Pan-acinar, Paraseptal, Irregular n Like cirrhosis, thought of as END-STAGE of multiple chronic small airway obstructive etiologies n NON-specific n IN-creased crepitance, BULLAE (BLEBS) n Clinically linked to recurrent pneumonias, and progressive failure n
EMPHYSEMA COPD, or “END-STAGE” lung disease n Centri-acinar, Pan-acinar, Paraseptal, Irregular n Like cirrhosis, thought of as END-STAGE of multiple chronic small airway obstructive etiologies n NON-specific n IN-creased crepitance, BULLAE (BLEBS) n Clinically linked to recurrent pneumonias, and progressive failure n
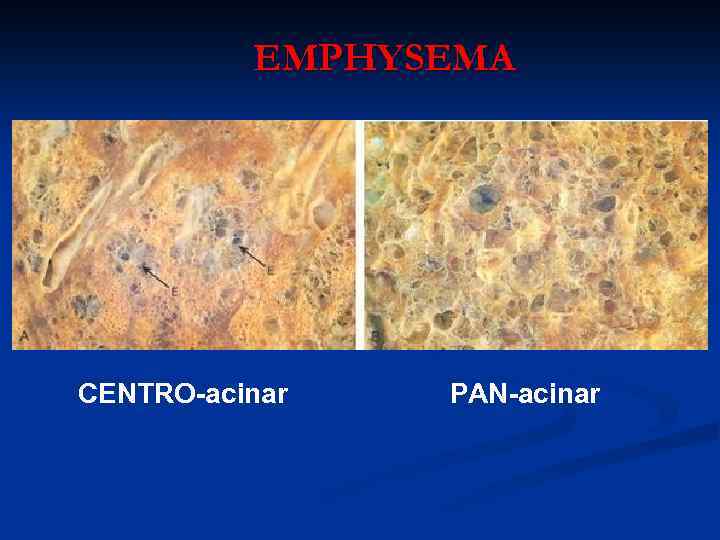 EMPHYSEMA CENTRO-acinar PAN-acinar
EMPHYSEMA CENTRO-acinar PAN-acinar
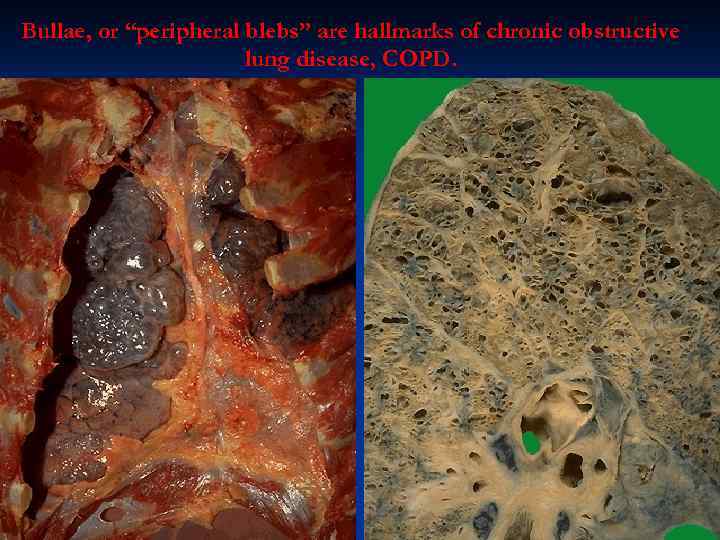 Bullae, or “peripheral blebs” are hallmarks of chronic obstructive lung disease, COPD.
Bullae, or “peripheral blebs” are hallmarks of chronic obstructive lung disease, COPD.
 CHRONIC BRONCHITIS INHALANTS, POLLUTION, CIGARETTES n CHRONIC COUGH n CAN OFTEN PROGRESS TO EMPHYSEMA n MUCUS hypersecretion, early, i. e. goblet cell increase n CHRONIC bronchial inflammatory infiltrate n
CHRONIC BRONCHITIS INHALANTS, POLLUTION, CIGARETTES n CHRONIC COUGH n CAN OFTEN PROGRESS TO EMPHYSEMA n MUCUS hypersecretion, early, i. e. goblet cell increase n CHRONIC bronchial inflammatory infiltrate n
 ASTHMA Similar to chronic bronchitis but: n n n Wheezing is hallmark (bronchospasm, i. e. “wheezing”) STRONG allergic role, i. e. , eosinophils, Ig. E, allergens Often starting in CHILDHOOD ATOPIC (allergic) or NON-ATOPIC (infection) Chronic small airway obstruction and infection 1) Mucus hypersecretion with plugging, 2) lymphocytes/eosinophils, 3) lumen narrowing, 4) smooth muscle hypertrophy
ASTHMA Similar to chronic bronchitis but: n n n Wheezing is hallmark (bronchospasm, i. e. “wheezing”) STRONG allergic role, i. e. , eosinophils, Ig. E, allergens Often starting in CHILDHOOD ATOPIC (allergic) or NON-ATOPIC (infection) Chronic small airway obstruction and infection 1) Mucus hypersecretion with plugging, 2) lymphocytes/eosinophils, 3) lumen narrowing, 4) smooth muscle hypertrophy
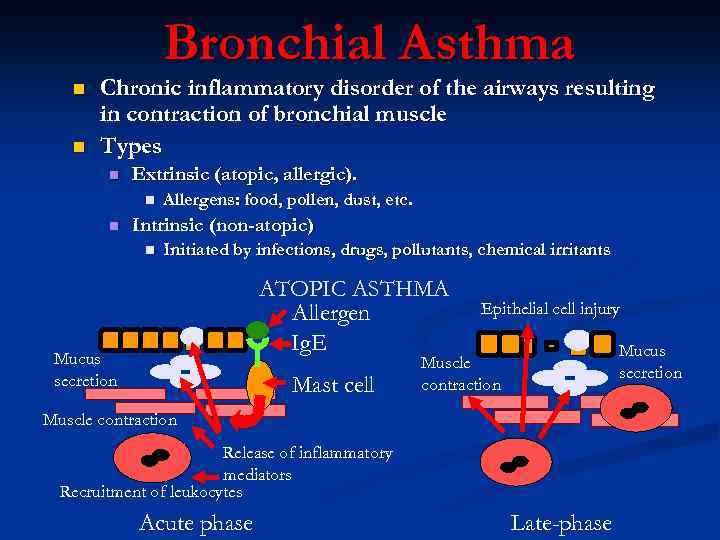 Bronchial Asthma n n Chronic inflammatory disorder of the airways resulting in contraction of bronchial muscle Types n Extrinsic (atopic, allergic). n n Allergens: food, pollen, dust, etc. Intrinsic (non-atopic) n Initiated by infections, drugs, pollutants, chemical irritants ATOPIC ASTHMA Allergen Ig. E Mucus secretion Mast cell Epithelial cell injury Mucus secretion Muscle contraction Release of inflammatory mediators Recruitment of leukocytes Acute phase Late-phase
Bronchial Asthma n n Chronic inflammatory disorder of the airways resulting in contraction of bronchial muscle Types n Extrinsic (atopic, allergic). n n Allergens: food, pollen, dust, etc. Intrinsic (non-atopic) n Initiated by infections, drugs, pollutants, chemical irritants ATOPIC ASTHMA Allergen Ig. E Mucus secretion Mast cell Epithelial cell injury Mucus secretion Muscle contraction Release of inflammatory mediators Recruitment of leukocytes Acute phase Late-phase
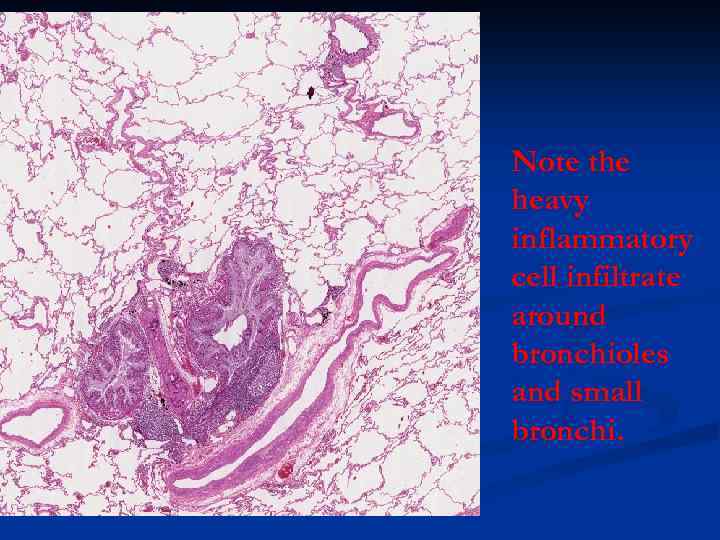 Note the heavy inflammatory cell infiltrate around bronchioles and small bronchi.
Note the heavy inflammatory cell infiltrate around bronchioles and small bronchi.
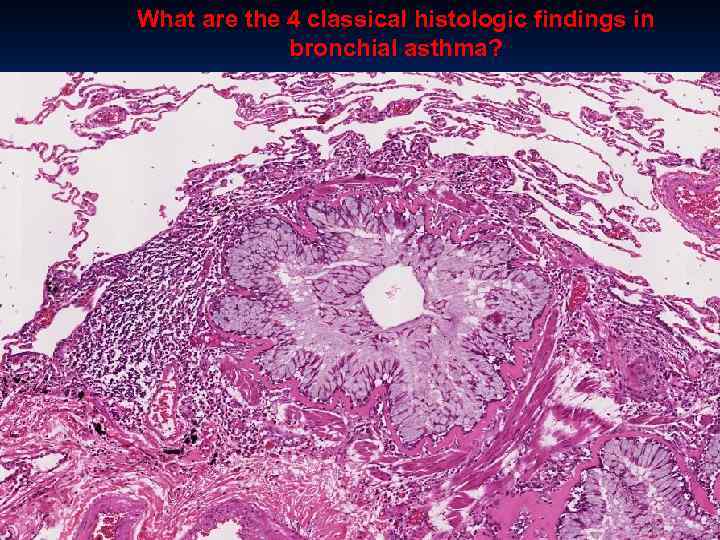 What are the 4 classical histologic findings in bronchial asthma?
What are the 4 classical histologic findings in bronchial asthma?
 BRONCHIECTASIS DILATATION of the BRONCHUS, associated with, often, necrotizing inflammation n CONGENITAL n. TB, other bacteria, many viruses BRONCHIAL OBSTRUCTION (i. e. , LARGE AIRWAY, NOT SMALL AIRWAY) n Rheumatoid Arthritis, SLE, IBD (Inflammatory Bowel Disease) n
BRONCHIECTASIS DILATATION of the BRONCHUS, associated with, often, necrotizing inflammation n CONGENITAL n. TB, other bacteria, many viruses BRONCHIAL OBSTRUCTION (i. e. , LARGE AIRWAY, NOT SMALL AIRWAY) n Rheumatoid Arthritis, SLE, IBD (Inflammatory Bowel Disease) n
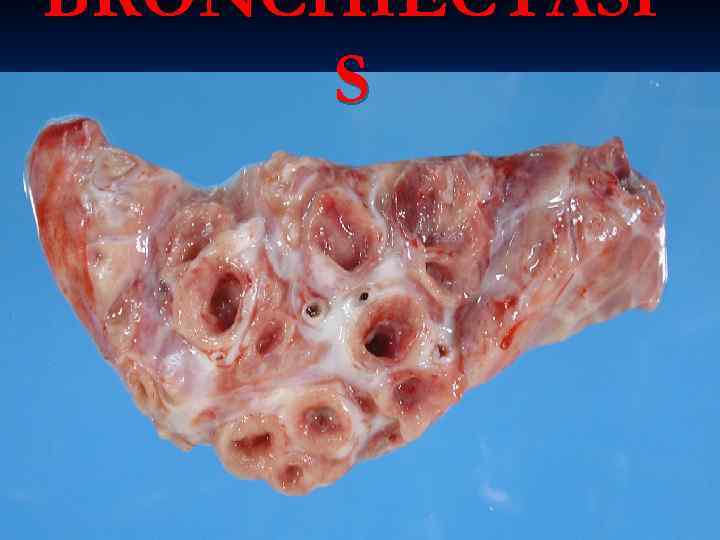 BRONCHIECTASI S
BRONCHIECTASI S
 RESTRICTIVE (INFILTRATIVE) n n n REDUCED COMPLIANCE, reduced gas exchange) Are also DIFFUSE HETEROGENEOUS n FIBROSING n GRANULOMATOUS n EOSINOPHILIC n SMOKING RELATED n PAP (Pulmonary Alveolar Proteinosis
RESTRICTIVE (INFILTRATIVE) n n n REDUCED COMPLIANCE, reduced gas exchange) Are also DIFFUSE HETEROGENEOUS n FIBROSING n GRANULOMATOUS n EOSINOPHILIC n SMOKING RELATED n PAP (Pulmonary Alveolar Proteinosis
 FIBROSING “IDIOPATHIC” PULMONARY FIBROSIS (IPF) n NONSPECIFIC INTERSTITIAL FIBROSIS n “CRYPTOGENIC” ORGANIZING PNEUMONIA n “COLLAGEN” VASCULAR DISEASES n PNEUMOCONIOSES n DRUG REACTIONS n RADIATION CHANGES n
FIBROSING “IDIOPATHIC” PULMONARY FIBROSIS (IPF) n NONSPECIFIC INTERSTITIAL FIBROSIS n “CRYPTOGENIC” ORGANIZING PNEUMONIA n “COLLAGEN” VASCULAR DISEASES n PNEUMOCONIOSES n DRUG REACTIONS n RADIATION CHANGES n
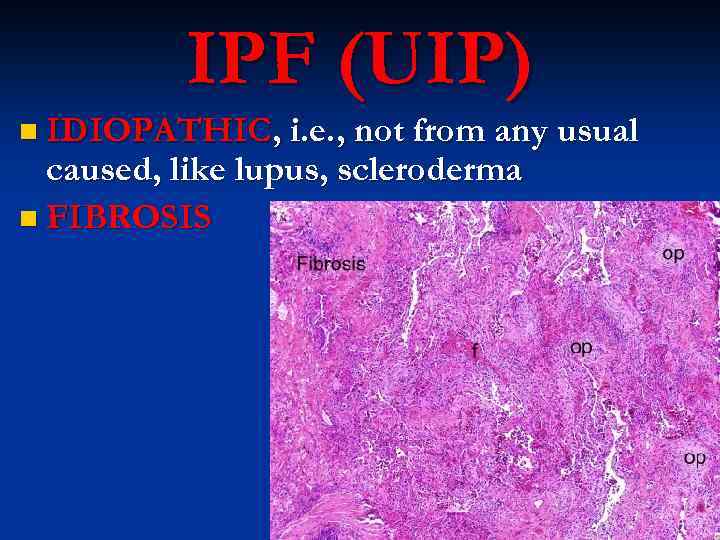 IPF (UIP) n IDIOPATHIC, i. e. , not from any usual caused, like lupus, scleroderma n FIBROSIS
IPF (UIP) n IDIOPATHIC, i. e. , not from any usual caused, like lupus, scleroderma n FIBROSIS
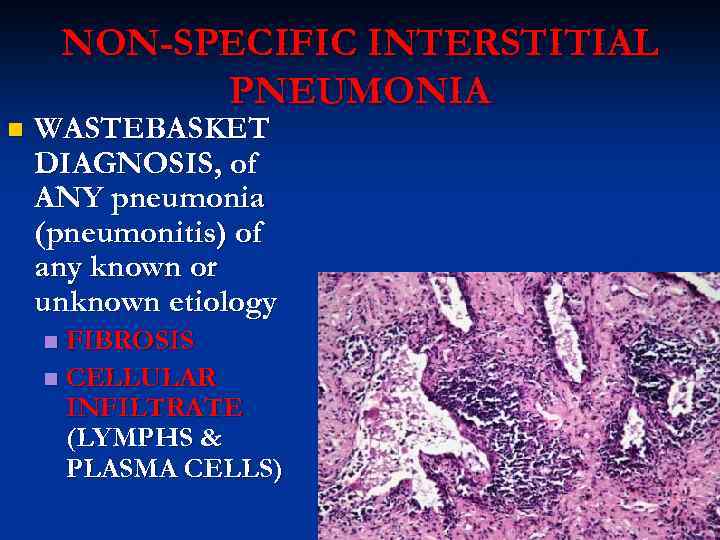 NON-SPECIFIC INTERSTITIAL PNEUMONIA n WASTEBASKET DIAGNOSIS, of ANY pneumonia (pneumonitis) of any known or unknown etiology FIBROSIS n CELLULAR INFILTRATE (LYMPHS & PLASMA CELLS) n
NON-SPECIFIC INTERSTITIAL PNEUMONIA n WASTEBASKET DIAGNOSIS, of ANY pneumonia (pneumonitis) of any known or unknown etiology FIBROSIS n CELLULAR INFILTRATE (LYMPHS & PLASMA CELLS) n
 CRYPTOGENIC ORGANIZING PNEUMONIA (COP) IDIOPATHIC n “BRONCHIOLITIS OBLITERANS” n
CRYPTOGENIC ORGANIZING PNEUMONIA (COP) IDIOPATHIC n “BRONCHIOLITIS OBLITERANS” n
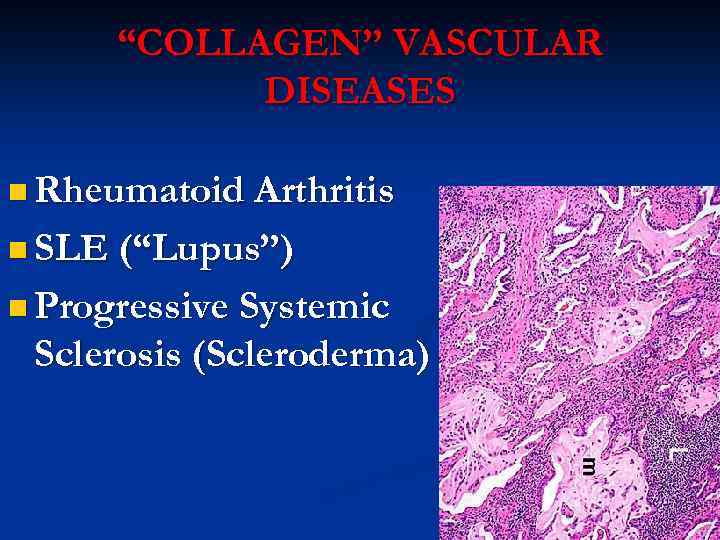 “COLLAGEN” VASCULAR DISEASES n Rheumatoid Arthritis n SLE (“Lupus”) n Progressive Systemic Sclerosis (Scleroderma)
“COLLAGEN” VASCULAR DISEASES n Rheumatoid Arthritis n SLE (“Lupus”) n Progressive Systemic Sclerosis (Scleroderma)
 PNEUMOCONIOSES “OCCUPATIONAL” n “COAL MINERS LUNG” n DUST OR CHEMICALS OR ORGANIC MATERIALS n Coal (anthracosis) n Silica n Asbestos n n Be, Fe. O, Ba. SO 4, CHEMO n HAY, FLAX, BAGASSE, INSECTICIDES, etc.
PNEUMOCONIOSES “OCCUPATIONAL” n “COAL MINERS LUNG” n DUST OR CHEMICALS OR ORGANIC MATERIALS n Coal (anthracosis) n Silica n Asbestos n n Be, Fe. O, Ba. SO 4, CHEMO n HAY, FLAX, BAGASSE, INSECTICIDES, etc.
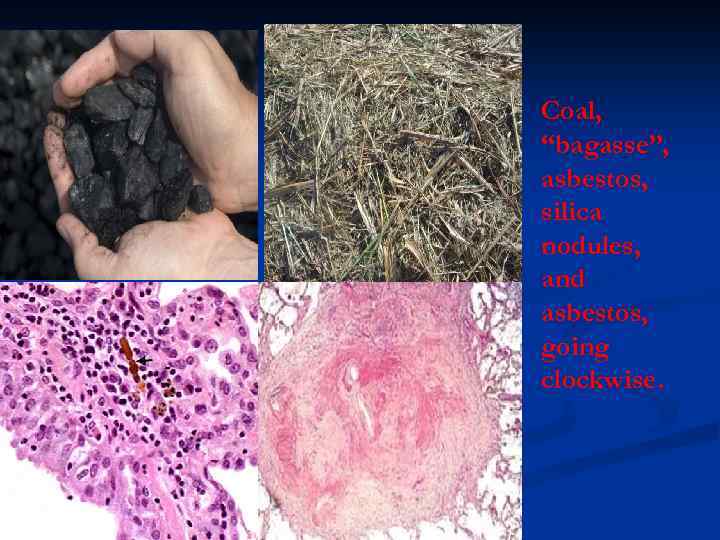 Coal, “bagasse”, asbestos, silica nodules, and asbestos, going clockwise.
Coal, “bagasse”, asbestos, silica nodules, and asbestos, going clockwise.
 GRANULOMATOUS n SARCOIDOSIS, i. e. , NON-caseating granulomas (IDIOPATHIC) n HYPERSENSITIVITY (DUSTS, bacteria, fungi, Farmer’s Lung, Pigeon Breeder’s Lung)
GRANULOMATOUS n SARCOIDOSIS, i. e. , NON-caseating granulomas (IDIOPATHIC) n HYPERSENSITIVITY (DUSTS, bacteria, fungi, Farmer’s Lung, Pigeon Breeder’s Lung)
 SARCOIDOSIS n Mainly LUNG, but eye, skin or ANYWHERE n UNKNOWN ETIOLOGY n IMMUNE, GENETIC factors n F>>M n B>>W n YOUNG ADULT BLACK WOMEN
SARCOIDOSIS n Mainly LUNG, but eye, skin or ANYWHERE n UNKNOWN ETIOLOGY n IMMUNE, GENETIC factors n F>>M n B>>W n YOUNG ADULT BLACK WOMEN
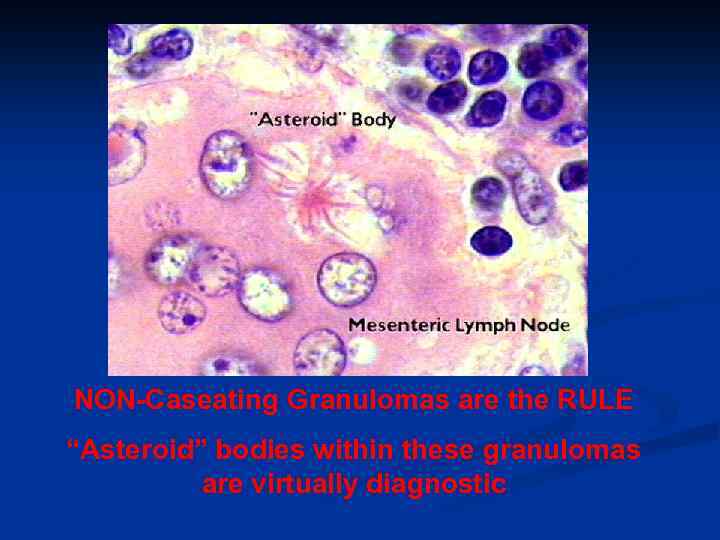 NON-Caseating Granulomas are the RULE “Asteroid” bodies within these granulomas are virtually diagnostic
NON-Caseating Granulomas are the RULE “Asteroid” bodies within these granulomas are virtually diagnostic
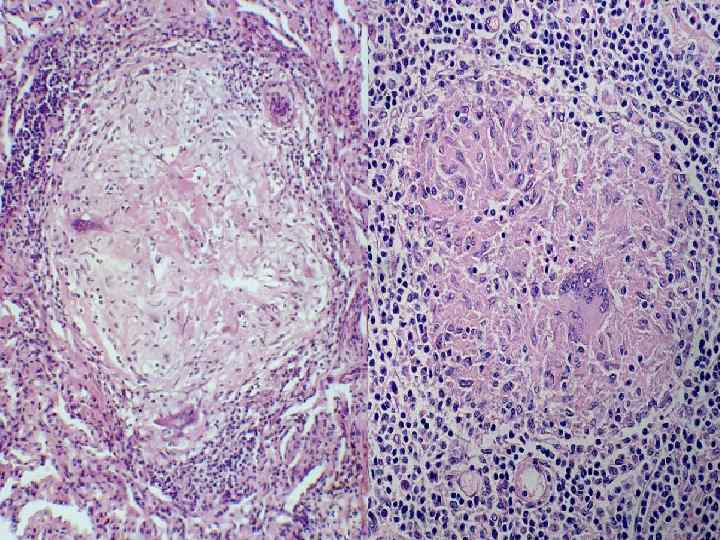
 SMOKING RELATED n DIP (Desquamative Interstitial Pneumonia) M>>F n CIGARETTES n 100% Survival n Alveolar Macrophages
SMOKING RELATED n DIP (Desquamative Interstitial Pneumonia) M>>F n CIGARETTES n 100% Survival n Alveolar Macrophages
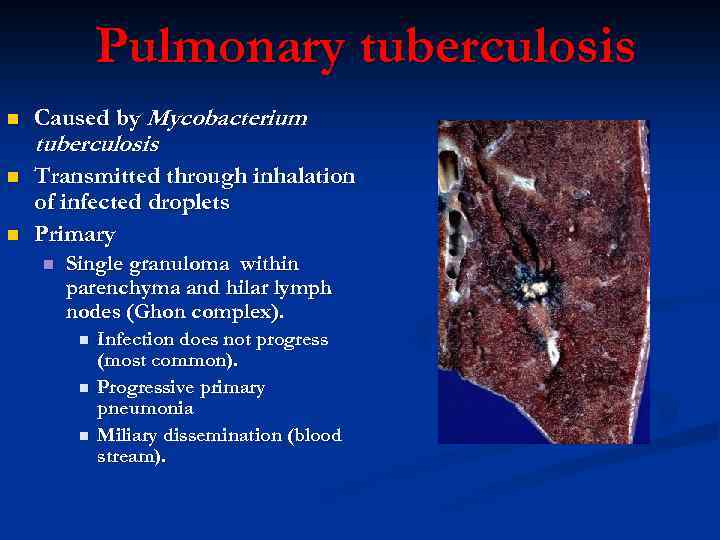 Pulmonary tuberculosis n n n Caused by Mycobacterium tuberculosis. Transmitted through inhalation of infected droplets Primary n Single granuloma within parenchyma and hilar lymph nodes (Ghon complex). n n n Infection does not progress (most common). Progressive primary pneumonia Miliary dissemination (blood stream).
Pulmonary tuberculosis n n n Caused by Mycobacterium tuberculosis. Transmitted through inhalation of infected droplets Primary n Single granuloma within parenchyma and hilar lymph nodes (Ghon complex). n n n Infection does not progress (most common). Progressive primary pneumonia Miliary dissemination (blood stream).
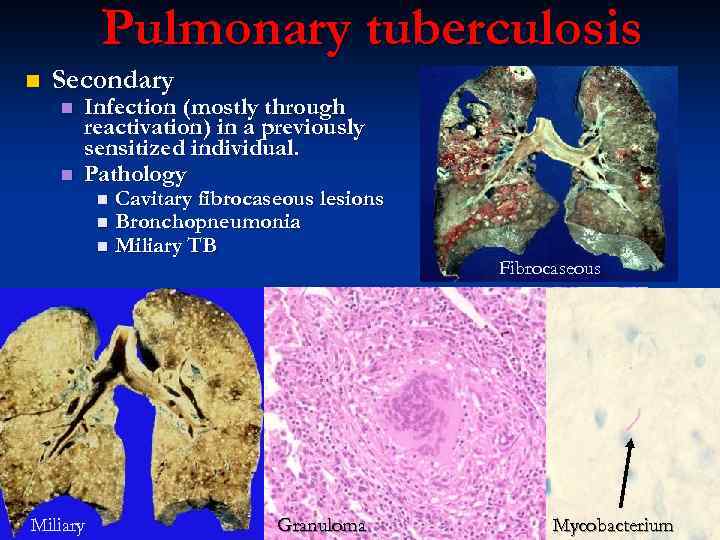 Pulmonary tuberculosis n Secondary n n Infection (mostly through reactivation) in a previously sensitized individual. Pathology n n n Miliary Cavitary fibrocaseous lesions Bronchopneumonia Miliary TB Granuloma Fibrocaseous Mycobacterium
Pulmonary tuberculosis n Secondary n n Infection (mostly through reactivation) in a previously sensitized individual. Pathology n n n Miliary Cavitary fibrocaseous lesions Bronchopneumonia Miliary TB Granuloma Fibrocaseous Mycobacterium
 VASCULAR PULMONARY DISEASES PULMONARY EMBOLISM (with or usually WITHOUT infarction) n PULMONARY HYPERTENSION, leading to cor pulmonale n HEMORRHAGIC SYNDROMES n n GOODPASTURE SYNDROME n HEMOSIDEROSIS, idiopathic n WEGENER GRANULOMATOSIS
VASCULAR PULMONARY DISEASES PULMONARY EMBOLISM (with or usually WITHOUT infarction) n PULMONARY HYPERTENSION, leading to cor pulmonale n HEMORRHAGIC SYNDROMES n n GOODPASTURE SYNDROME n HEMOSIDEROSIS, idiopathic n WEGENER GRANULOMATOSIS
 P. E. n n n n Usually secondary to debilitated states with immobilization, or following surgery Usually deep leg and deep pelvic veins (DVT), NOT superficial veins Follows Virchow’s triad, i. e. , 1) flow problems, 2) endothelial disruption, 3) hypercoagulabilty Usually do NOT infarct, usually ventilate When they DO infarct, the infarct is hemorrhagic Decreased PO 2, acute chest pain, V/Q MIS-match DX: Chest CT, V/Q scan, angiogram RX: short term heparin, then long term coumadin
P. E. n n n n Usually secondary to debilitated states with immobilization, or following surgery Usually deep leg and deep pelvic veins (DVT), NOT superficial veins Follows Virchow’s triad, i. e. , 1) flow problems, 2) endothelial disruption, 3) hypercoagulabilty Usually do NOT infarct, usually ventilate When they DO infarct, the infarct is hemorrhagic Decreased PO 2, acute chest pain, V/Q MIS-match DX: Chest CT, V/Q scan, angiogram RX: short term heparin, then long term coumadin
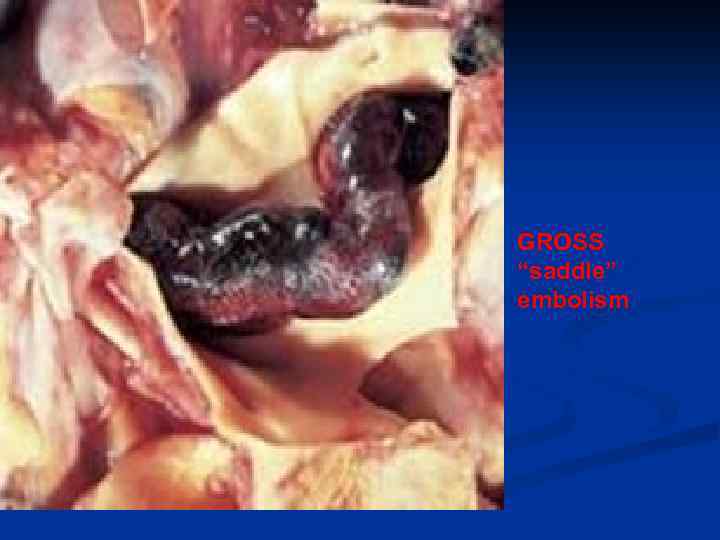 GROSS “saddle” embolism
GROSS “saddle” embolism
 PULMONARY HYPERTENSION n COPD, C”I”PD (vicious cycle) n CHD (Congenital HD, increased left atrial pressure) n Recurrent PEs n Autoimmune, e. g. , PSS (Scleroderma), i. e. , fibrotic pulmonary vasculature
PULMONARY HYPERTENSION n COPD, C”I”PD (vicious cycle) n CHD (Congenital HD, increased left atrial pressure) n Recurrent PEs n Autoimmune, e. g. , PSS (Scleroderma), i. e. , fibrotic pulmonary vasculature
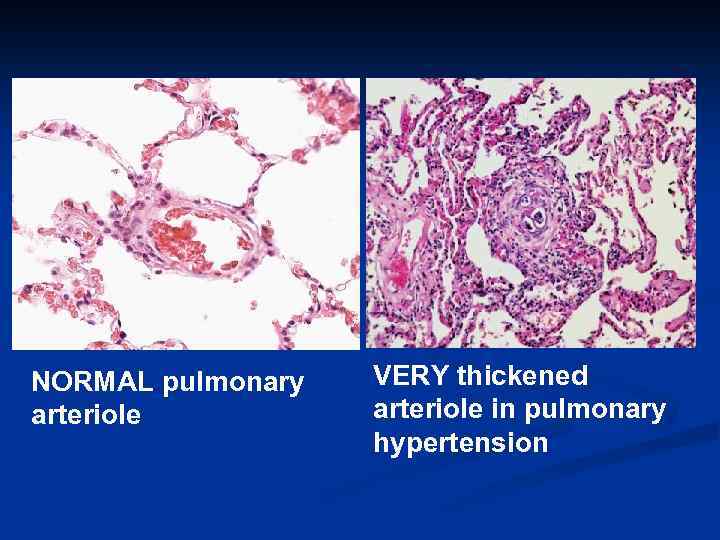 NORMAL pulmonary arteriole VERY thickened arteriole in pulmonary hypertension
NORMAL pulmonary arteriole VERY thickened arteriole in pulmonary hypertension
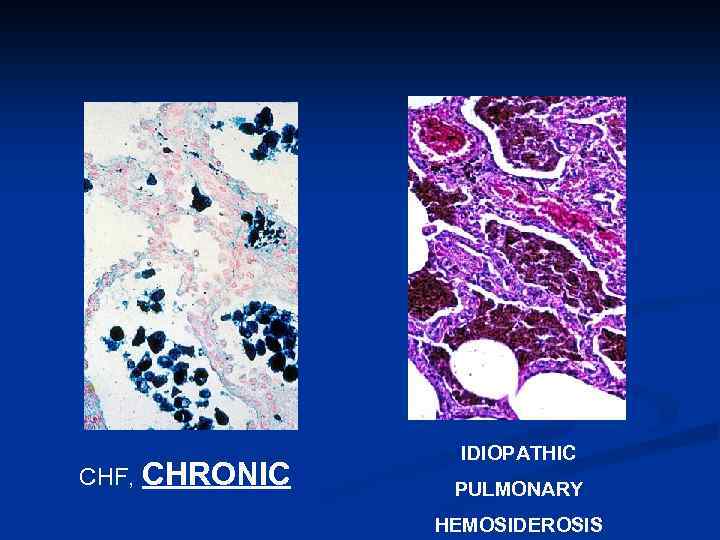 CHF, CHRONIC IDIOPATHIC PULMONARY HEMOSIDEROSIS
CHF, CHRONIC IDIOPATHIC PULMONARY HEMOSIDEROSIS
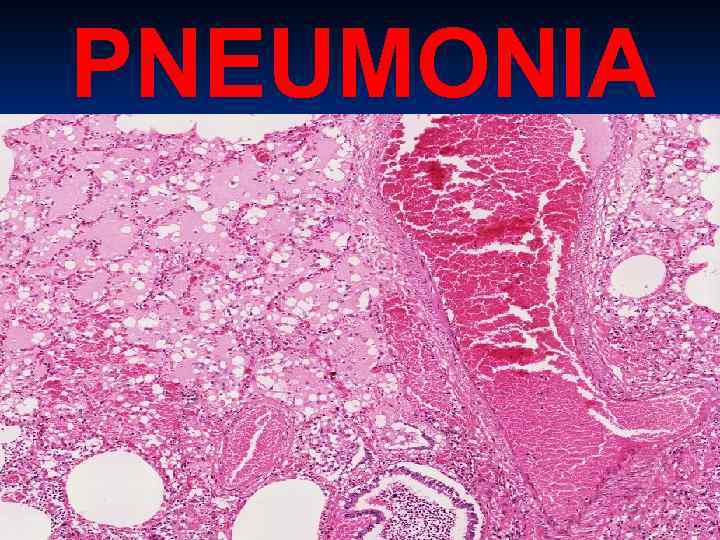 PNEUMONIA
PNEUMONIA
 PULMONARY INFECTIONS COMMUNITY-ACQUIRED BACTERIAL ACUTE PNEUMONIAS Streptococcus Pneumoniae Haemophilus Influenzae Moraxella Catarrhalis Staphylococcus Aureus Klebsiella Pneumoniae Pseudomonas Aeruginosa Legionella Pneumophila COMMUNITY-ACQUIRED ATYPICAL (VIRAL AND MYCOPLASMAL) PNEUMONIAS Morphology. Clinical Course. Influenza Infections Severe Acute Respiratory Syndrome (SARS) NOSOCOMIAL PNEUMONIA ASPIRATION PNEUMONIA LUNG ABSCESS Etiology and Pathogenesis. CHRONIC PNEUMONIA Histoplasmosis, Morphology Blastomycosis, Morphology Coccidioidomycosis, Morphology PNEUMONIA IN THE IMMUNOCOMPROMISED HOST
PULMONARY INFECTIONS COMMUNITY-ACQUIRED BACTERIAL ACUTE PNEUMONIAS Streptococcus Pneumoniae Haemophilus Influenzae Moraxella Catarrhalis Staphylococcus Aureus Klebsiella Pneumoniae Pseudomonas Aeruginosa Legionella Pneumophila COMMUNITY-ACQUIRED ATYPICAL (VIRAL AND MYCOPLASMAL) PNEUMONIAS Morphology. Clinical Course. Influenza Infections Severe Acute Respiratory Syndrome (SARS) NOSOCOMIAL PNEUMONIA ASPIRATION PNEUMONIA LUNG ABSCESS Etiology and Pathogenesis. CHRONIC PNEUMONIA Histoplasmosis, Morphology Blastomycosis, Morphology Coccidioidomycosis, Morphology PNEUMONIA IN THE IMMUNOCOMPROMISED HOST
 n n n BASIC CONSIDERATIONS PNEUMONIA vs. PNEUMONITIS DIFFERENTIATION from INJURIES, OBSTRUCTIVE DISEASES, RESTRICTIVE DISEASES, VASCULAR DISEASES DIFFERENTIATION FROM NEOPLASMS CLASSICAL STAGES of INFLAMMATION LOBAR- vs. BRONCHOINTERSTITIAL vs. ALVEOLAR COMMUNITY vs. NOSOCOMIAL ETIOLOGIC AGENTS vs. HOST IMMUNITY 2 PRESENTING SYMPTOMS 2 DIAGNOSTIC METHODS ANY ORGANISM CAN CAUSE PNEUMONIA!!!
n n n BASIC CONSIDERATIONS PNEUMONIA vs. PNEUMONITIS DIFFERENTIATION from INJURIES, OBSTRUCTIVE DISEASES, RESTRICTIVE DISEASES, VASCULAR DISEASES DIFFERENTIATION FROM NEOPLASMS CLASSICAL STAGES of INFLAMMATION LOBAR- vs. BRONCHOINTERSTITIAL vs. ALVEOLAR COMMUNITY vs. NOSOCOMIAL ETIOLOGIC AGENTS vs. HOST IMMUNITY 2 PRESENTING SYMPTOMS 2 DIAGNOSTIC METHODS ANY ORGANISM CAN CAUSE PNEUMONIA!!!
 PREDISPOSING FACTORS n LOSS OF COUGH REFLEX n DIMINISHED MUCIN or CILIA FUNCTION n ALVEOLAR MACROPHAGE INTERFERENCE n VASCULAR FLOW IMPAIRMENTS n BRONCHIAL FLOW IMPAIRMENTS
PREDISPOSING FACTORS n LOSS OF COUGH REFLEX n DIMINISHED MUCIN or CILIA FUNCTION n ALVEOLAR MACROPHAGE INTERFERENCE n VASCULAR FLOW IMPAIRMENTS n BRONCHIAL FLOW IMPAIRMENTS
 Although pneumonia is one of the most common causes of death, it usually does NOT occur in healthy people spontaneously
Although pneumonia is one of the most common causes of death, it usually does NOT occur in healthy people spontaneously
 Classifications of PNEUMONIAS COMMUNITY ACQUIRED n COMMUNITY ACQUIRED, ATYPICAL n NOSOCOMIAL n ASPIRATION n CHRONIC n NECROTIZING/ABSCESS FORMATION n PNEUMONIAS in IMMUNOCOMPROMISED HOSTS n
Classifications of PNEUMONIAS COMMUNITY ACQUIRED n COMMUNITY ACQUIRED, ATYPICAL n NOSOCOMIAL n ASPIRATION n CHRONIC n NECROTIZING/ABSCESS FORMATION n PNEUMONIAS in IMMUNOCOMPROMISED HOSTS n
 COMMUNITY ACQUIRED STREPTOCOCCUS PNEUMONIAE (i. e. , “diplococcus”) n HAEMOPHILUS INFLUENZAE (“HFlu”) n MORAXELLA n STAPHYLOCOCCUS (STAPH) n KLEBSIELLA PNEUMONIAE n PSEUDOMONAS AERUGINOSA n LEGIONELLA PNEUMOPHILIA n
COMMUNITY ACQUIRED STREPTOCOCCUS PNEUMONIAE (i. e. , “diplococcus”) n HAEMOPHILUS INFLUENZAE (“HFlu”) n MORAXELLA n STAPHYLOCOCCUS (STAPH) n KLEBSIELLA PNEUMONIAE n PSEUDOMONAS AERUGINOSA n LEGIONELLA PNEUMOPHILIA n
 STREPTOCOCCUS n The classic LOBAR pneumonia n Normal flora in 20% of adults n Only 20% of victims have + blood cultures n “Penicillins” are often 100% curative n Vaccines are often 100% preventive
STREPTOCOCCUS n The classic LOBAR pneumonia n Normal flora in 20% of adults n Only 20% of victims have + blood cultures n “Penicillins” are often 100% curative n Vaccines are often 100% preventive
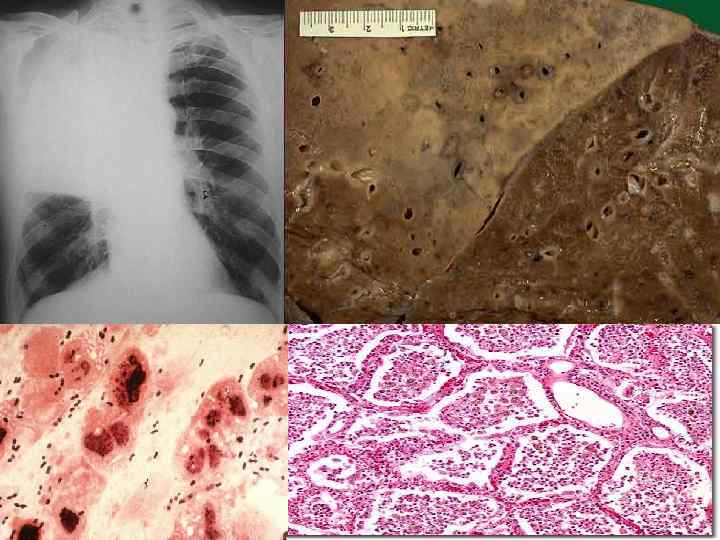
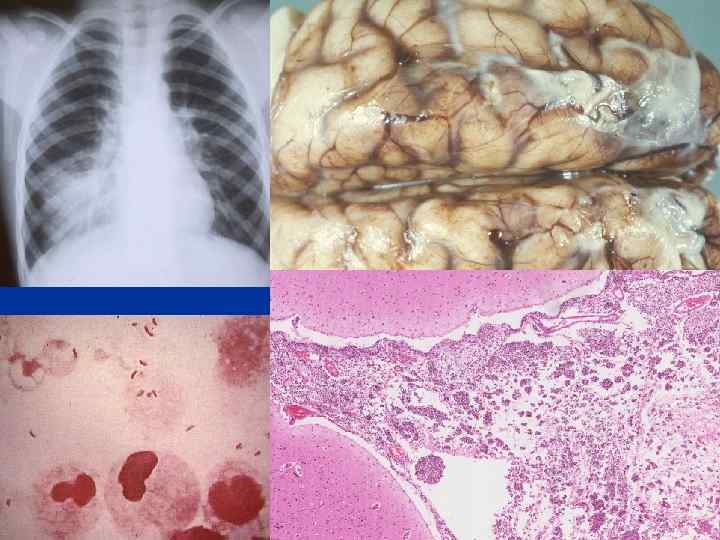
 MORPHOLOGY ACUTE n ORGANIZING n CHRONIC n FIBROSIS vs. FULL RESOLUTION n “HEPATIZATION”, RED vs. GREY n CONSOLIDATION n “INFILTRATE”, XRAY vs. HISTOPATH n Loss of “CREPITANCE” n
MORPHOLOGY ACUTE n ORGANIZING n CHRONIC n FIBROSIS vs. FULL RESOLUTION n “HEPATIZATION”, RED vs. GREY n CONSOLIDATION n “INFILTRATE”, XRAY vs. HISTOPATH n Loss of “CREPITANCE” n
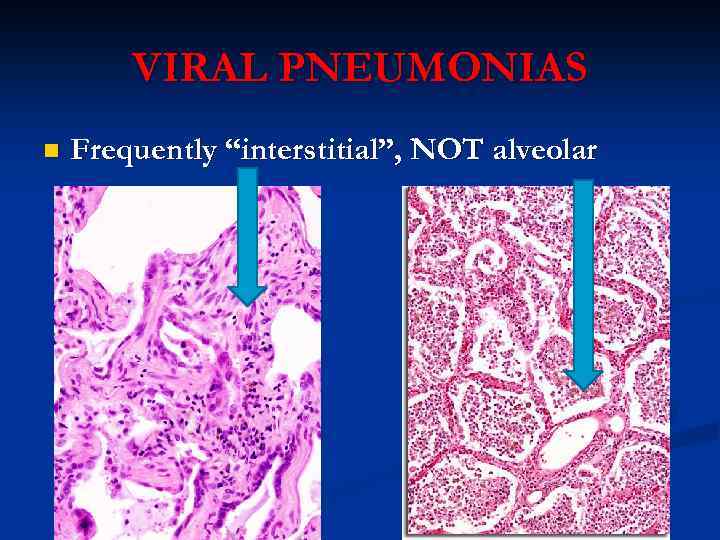 VIRAL PNEUMONIAS n Frequently “interstitial”, NOT alveolar
VIRAL PNEUMONIAS n Frequently “interstitial”, NOT alveolar
 ASPIRATION PNEUMONIAS UNCONSCIOUS PATIENTS n PATIENTS IN PROLONGED BEDREST n LACK OF ABILITY TO SWALLOW OR GAG n USUALLY CAUSED BY ASPIRATION OF GASTRIC CONTENTS n POSTERIOR LOBES (gravity dependent) MOST COMMONLY INVOLVED, ESPECIALLY THE SUPERIOR SEGMENTS of the LOWER LOBES n n Often lead to ABSCESSES
ASPIRATION PNEUMONIAS UNCONSCIOUS PATIENTS n PATIENTS IN PROLONGED BEDREST n LACK OF ABILITY TO SWALLOW OR GAG n USUALLY CAUSED BY ASPIRATION OF GASTRIC CONTENTS n POSTERIOR LOBES (gravity dependent) MOST COMMONLY INVOLVED, ESPECIALLY THE SUPERIOR SEGMENTS of the LOWER LOBES n n Often lead to ABSCESSES
 LUNG ABSCESSES ASPIRATION n SEPTIC EMBOLIZATION n NEOPLASIA n From NEIGHBORING structures: n ESOPHAGUS n SPINE n PLEURA n DIAPHRAGM n n ANY pneumonia which is severe and destructive, and UN-treated enough
LUNG ABSCESSES ASPIRATION n SEPTIC EMBOLIZATION n NEOPLASIA n From NEIGHBORING structures: n ESOPHAGUS n SPINE n PLEURA n DIAPHRAGM n n ANY pneumonia which is severe and destructive, and UN-treated enough
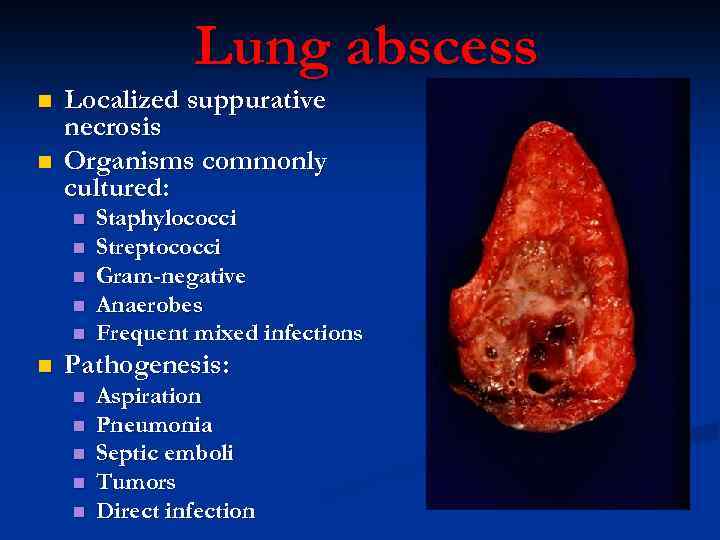 Lung abscess n n Localized suppurative necrosis Organisms commonly cultured: n n n Staphylococci Streptococci Gram-negative Anaerobes Frequent mixed infections Pathogenesis: n n n Aspiration Pneumonia Septic emboli Tumors Direct infection
Lung abscess n n Localized suppurative necrosis Organisms commonly cultured: n n n Staphylococci Streptococci Gram-negative Anaerobes Frequent mixed infections Pathogenesis: n n n Aspiration Pneumonia Septic emboli Tumors Direct infection
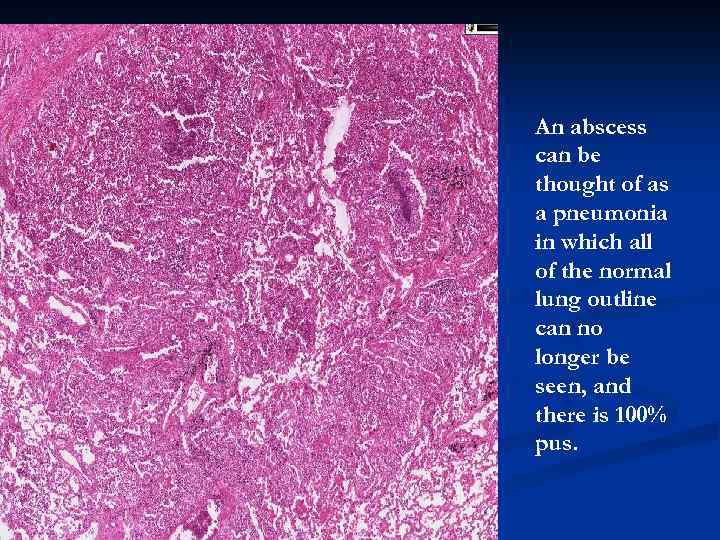 An abscess can be thought of as a pneumonia in which all of the normal lung outline can no longer be seen, and there is 100% pus.
An abscess can be thought of as a pneumonia in which all of the normal lung outline can no longer be seen, and there is 100% pus.
 CHRONIC Pneumonias USUALLY NOT persistences of the community or nosocomial bacterial infections, but CAN BE, at least histologically n Often SYNONYMOUS with the 4 classic fungal n or granulomatous pulmonary infections, i. e. , TB, Histo-, Blasto-, Coccidion If you see pulmonary granulomas, think of a CHRONIC process, often years
CHRONIC Pneumonias USUALLY NOT persistences of the community or nosocomial bacterial infections, but CAN BE, at least histologically n Often SYNONYMOUS with the 4 classic fungal n or granulomatous pulmonary infections, i. e. , TB, Histo-, Blasto-, Coccidion If you see pulmonary granulomas, think of a CHRONIC process, often years
 CHRONIC Pneumonias n. TB n. HISTO-PLASMOSIS n. BLASTO-MYCOSIS n. COCCIDIO-
CHRONIC Pneumonias n. TB n. HISTO-PLASMOSIS n. BLASTO-MYCOSIS n. COCCIDIO-
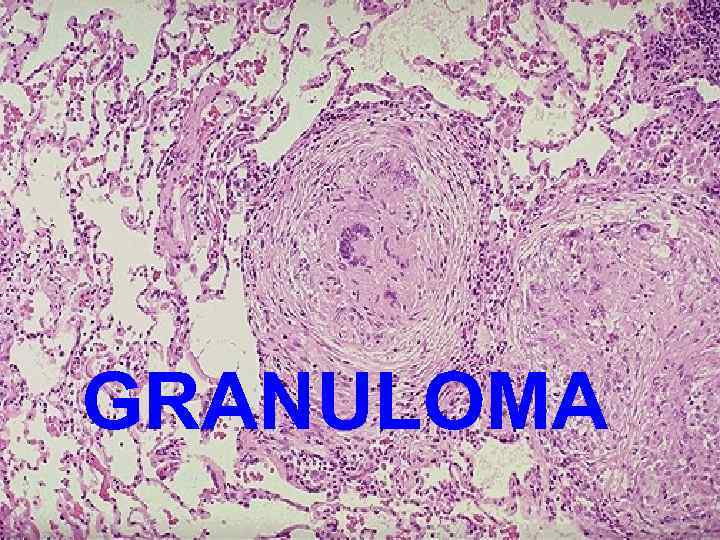 GRANULOMA
GRANULOMA
 LUNG TUMORS Benign, malignant, epithelial, mesenchymal, but 90% are CARCINOMAS n BIGGEST USA killer. Why? Ans: Prevalence not as high as prostate or breast but mortality higher. Only 15% 5 year survival. n n TOBACCO has polycyclic aromatic hydrocarbons, such as benzopyrene, anthracenes, radioactive isotopes n Radiation, asbestos, radon n C-MYC, K-RAS, EGFR, HER-2/neu
LUNG TUMORS Benign, malignant, epithelial, mesenchymal, but 90% are CARCINOMAS n BIGGEST USA killer. Why? Ans: Prevalence not as high as prostate or breast but mortality higher. Only 15% 5 year survival. n n TOBACCO has polycyclic aromatic hydrocarbons, such as benzopyrene, anthracenes, radioactive isotopes n Radiation, asbestos, radon n C-MYC, K-RAS, EGFR, HER-2/neu
 PATHOGENESIS n NORMAL BRONCHIAL MUCOSA n METAPLASTIC/DYSPLASTIC MUCOSA n CARCINOMA-IN-SITU (squamous, adeno) n INFILTRATING (i. e. , “INVASIVE”) cancer
PATHOGENESIS n NORMAL BRONCHIAL MUCOSA n METAPLASTIC/DYSPLASTIC MUCOSA n CARCINOMA-IN-SITU (squamous, adeno) n INFILTRATING (i. e. , “INVASIVE”) cancer
 TWO TYPES n NON-SMALL CELL n SQUAMOUS CELL CARCINOMA n ADENOCARCINOMA n LARGE CELL CARCINOMA n SMALL CELL CARCINOMA
TWO TYPES n NON-SMALL CELL n SQUAMOUS CELL CARCINOMA n ADENOCARCINOMA n LARGE CELL CARCINOMA n SMALL CELL CARCINOMA
 The BIG list n n n Squamous cell carcinoma Small cell carcinoma Combined small cell carcinoma Adenocarcinoma: Acinar, papillary, bronchioloalveolar, solid, mixed subtypes Large cell carcinoma Large cell neuroendocrine carcinoma Adenosquamous carcinoma Carcinomas with pleomorphic, sarcomatoid, or sarcomatous elements Carcinoid tumor: Typical, atypical Carcinomas of salivary gland type Unclassified carcinoma
The BIG list n n n Squamous cell carcinoma Small cell carcinoma Combined small cell carcinoma Adenocarcinoma: Acinar, papillary, bronchioloalveolar, solid, mixed subtypes Large cell carcinoma Large cell neuroendocrine carcinoma Adenosquamous carcinoma Carcinomas with pleomorphic, sarcomatoid, or sarcomatous elements Carcinoid tumor: Typical, atypical Carcinomas of salivary gland type Unclassified carcinoma
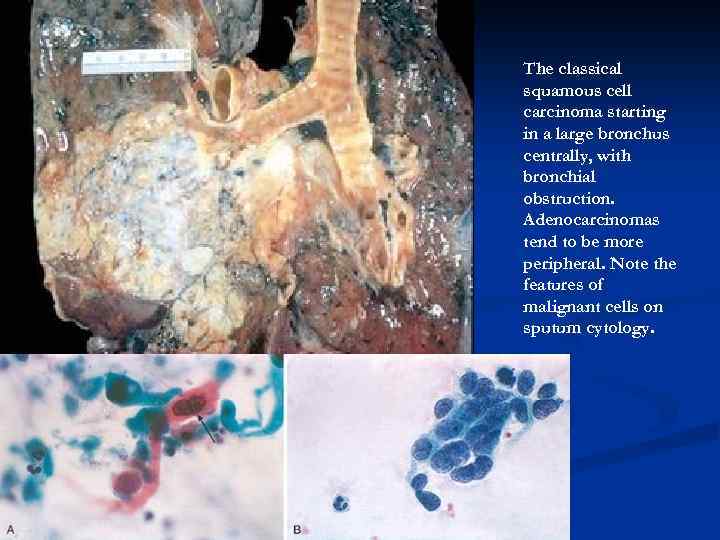 The classical squamous cell carcinoma starting in a large bronchus centrally, with bronchial obstruction. Adenocarcinomas tend to be more peripheral. Note the features of malignant cells on sputum cytology.
The classical squamous cell carcinoma starting in a large bronchus centrally, with bronchial obstruction. Adenocarcinomas tend to be more peripheral. Note the features of malignant cells on sputum cytology.
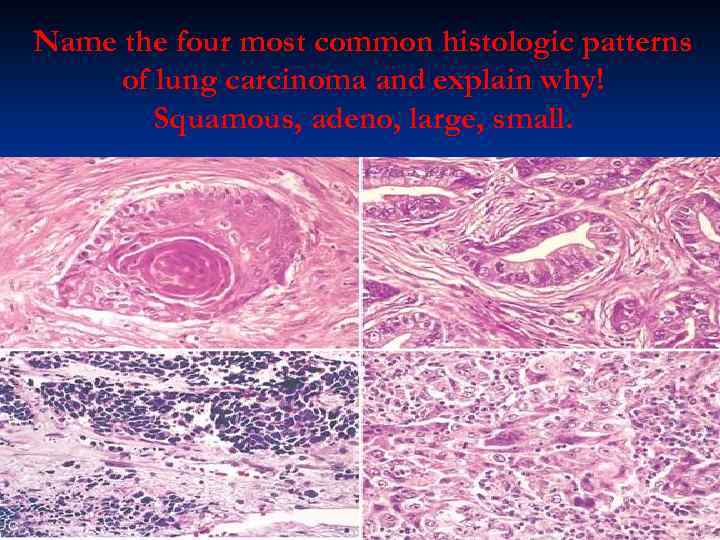 Name the four most common histologic patterns of lung carcinoma and explain why! Squamous, adeno, large, small.
Name the four most common histologic patterns of lung carcinoma and explain why! Squamous, adeno, large, small.
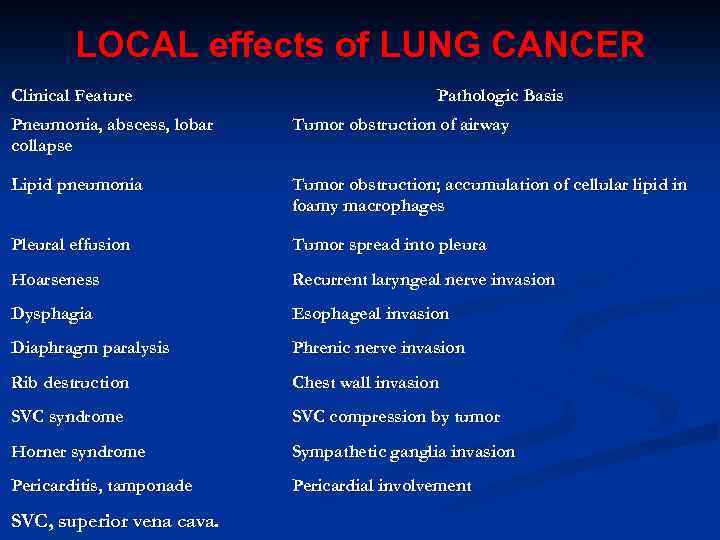 LOCAL effects of LUNG CANCER Clinical Feature Pathologic Basis Pneumonia, abscess, lobar collapse Tumor obstruction of airway Lipid pneumonia Tumor obstruction; accumulation of cellular lipid in foamy macrophages Pleural effusion Tumor spread into pleura Hoarseness Recurrent laryngeal nerve invasion Dysphagia Esophageal invasion Diaphragm paralysis Phrenic nerve invasion Rib destruction Chest wall invasion SVC syndrome SVC compression by tumor Horner syndrome Sympathetic ganglia invasion Pericarditis, tamponade Pericardial involvement SVC, superior vena cava.
LOCAL effects of LUNG CANCER Clinical Feature Pathologic Basis Pneumonia, abscess, lobar collapse Tumor obstruction of airway Lipid pneumonia Tumor obstruction; accumulation of cellular lipid in foamy macrophages Pleural effusion Tumor spread into pleura Hoarseness Recurrent laryngeal nerve invasion Dysphagia Esophageal invasion Diaphragm paralysis Phrenic nerve invasion Rib destruction Chest wall invasion SVC syndrome SVC compression by tumor Horner syndrome Sympathetic ganglia invasion Pericarditis, tamponade Pericardial involvement SVC, superior vena cava.
 METASTATIC TUMORS n LUNG is the MOST COMMON site for all metastatic tumors, regardless of site of origin n It is the site of FIRST CHOICE for metastatic sarcomas for purely anatomic reasons!
METASTATIC TUMORS n LUNG is the MOST COMMON site for all metastatic tumors, regardless of site of origin n It is the site of FIRST CHOICE for metastatic sarcomas for purely anatomic reasons!
 PLEURA n PLEURITIS n PNEUMOTHORAX n EFFUSIONS n HYDROTHORAX n HEMOTHORAX n CHYLOTHORAX n MESOTHELIOMAS
PLEURA n PLEURITIS n PNEUMOTHORAX n EFFUSIONS n HYDROTHORAX n HEMOTHORAX n CHYLOTHORAX n MESOTHELIOMAS
 PLEURITIS n Usual bacteria, viruses, etc. n Infarcts n Lung abscesses, empyema n TB n “Collagen” diseases, e. g. , RA, SLE n Uremia n Metastatic
PLEURITIS n Usual bacteria, viruses, etc. n Infarcts n Lung abscesses, empyema n TB n “Collagen” diseases, e. g. , RA, SLE n Uremia n Metastatic
 PNEUMOTHORAX n SPONTANEOUS, TRAUMATIC, THERAPEUTIC n OPEN or CLOSED n “TENSION” pneumothorax, “valvular” effect n “Bleb” rupture n Perforating injuries n Post needle biopsy
PNEUMOTHORAX n SPONTANEOUS, TRAUMATIC, THERAPEUTIC n OPEN or CLOSED n “TENSION” pneumothorax, “valvular” effect n “Bleb” rupture n Perforating injuries n Post needle biopsy
 EFFUSIONS n TRANSUDATE (HYDROTHORAX) n EXUDATE (HYDROTHORAX) n BLOOD (HEMOTHORAX) n LYMPH (CHYLOTHORAX)
EFFUSIONS n TRANSUDATE (HYDROTHORAX) n EXUDATE (HYDROTHORAX) n BLOOD (HEMOTHORAX) n LYMPH (CHYLOTHORAX)
 MESOTHELIOMAS n “Benign” vs. “Malignant” differentiation does not matter, but a self limited localized nodule can be regarded as benign, and a spreading tumor can be regarded as malignant n Visceral or parietal pleura, pericardium, or peritoneum n Most are regarded as asbestos caused or asbestos “related”
MESOTHELIOMAS n “Benign” vs. “Malignant” differentiation does not matter, but a self limited localized nodule can be regarded as benign, and a spreading tumor can be regarded as malignant n Visceral or parietal pleura, pericardium, or peritoneum n Most are regarded as asbestos caused or asbestos “related”
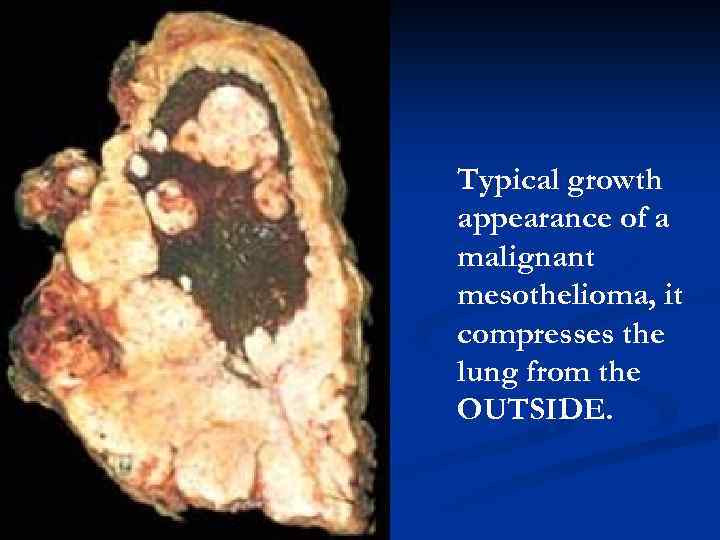 Typical growth appearance of a malignant mesothelioma, it compresses the lung from the OUTSIDE.
Typical growth appearance of a malignant mesothelioma, it compresses the lung from the OUTSIDE.
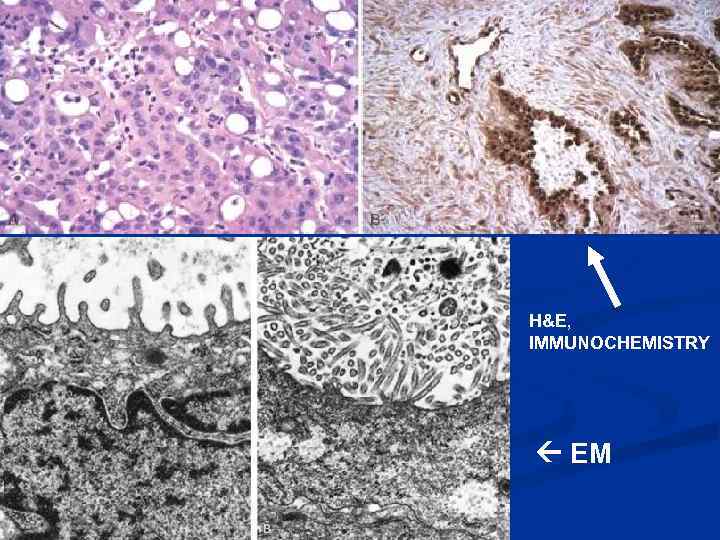 H&E, IMMUNOCHEMISTRY EM
H&E, IMMUNOCHEMISTRY EM


