14ef1df5de2d930e91b4c91bb075cf98.ppt
- Количество слайдов: 40
 Lung Cancer Elin Roddy, Lead Clinician for Lung Cancer at Sa. TH Elin. roddy@sath. nhs. uk @elinlowri
Lung Cancer Elin Roddy, Lead Clinician for Lung Cancer at Sa. TH Elin. roddy@sath. nhs. uk @elinlowri
 Overview • Some depressing statistics • Some possible reasons for the depressing statistics • Brief overview of diagnosis and treatment of lung cancer, explaining why we sometimes take so long • Discussion around potential improvements
Overview • Some depressing statistics • Some possible reasons for the depressing statistics • Brief overview of diagnosis and treatment of lung cancer, explaining why we sometimes take so long • Discussion around potential improvements
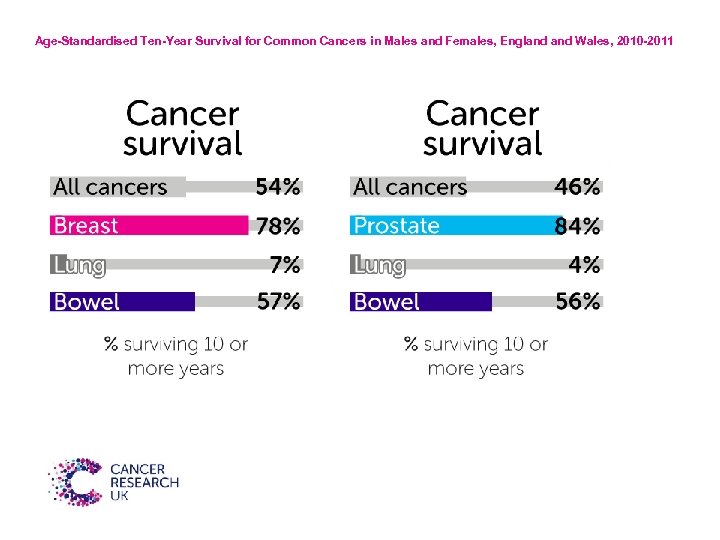 Age-Standardised Ten-Year Survival for Common Cancers in Males and Females, England Wales, 2010 -2011
Age-Standardised Ten-Year Survival for Common Cancers in Males and Females, England Wales, 2010 -2011
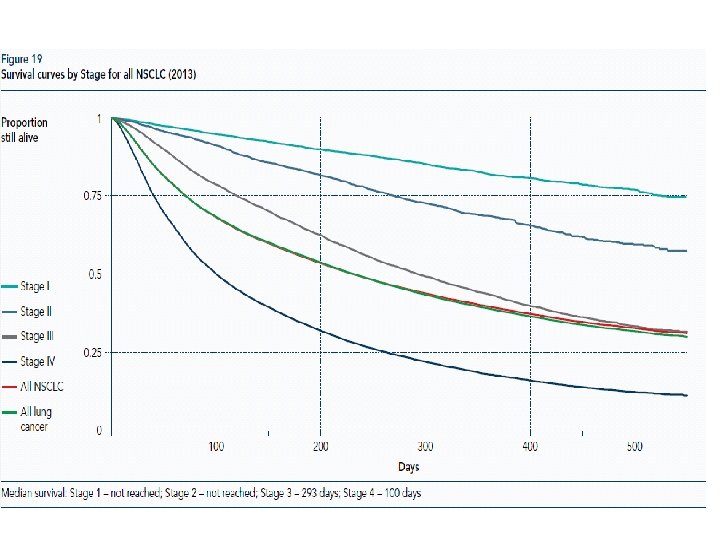
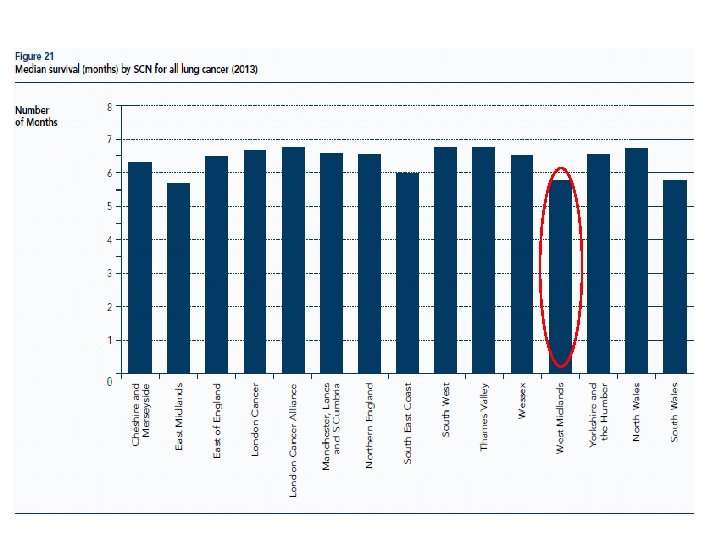
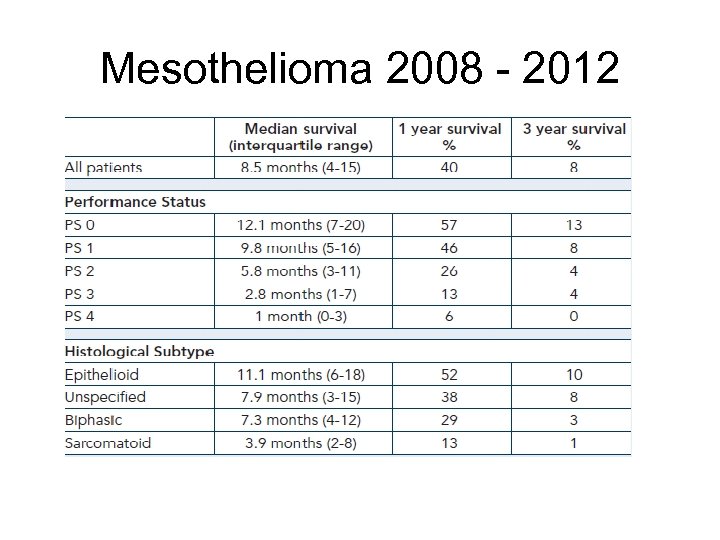 Mesothelioma 2008 - 2012
Mesothelioma 2008 - 2012
 Reasons why lung cancer survival is still variable and poor? • • Late presentation Deprivation (not just smoking, but mainly) Lack of advocacy & research Stigma • Access to staff, diagnostics and treatment
Reasons why lung cancer survival is still variable and poor? • • Late presentation Deprivation (not just smoking, but mainly) Lack of advocacy & research Stigma • Access to staff, diagnostics and treatment
 Late presentation • Late symptoms due to anatomy • Poor differentiation of symptoms by patients • Primary care gate-keeping? • Early diagnosis campaigns not a panacea
Late presentation • Late symptoms due to anatomy • Poor differentiation of symptoms by patients • Primary care gate-keeping? • Early diagnosis campaigns not a panacea
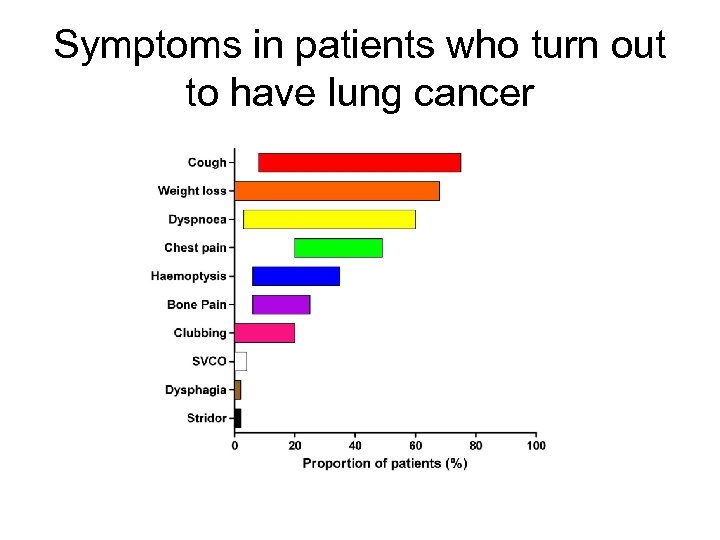 Symptoms in patients who turn out to have lung cancer
Symptoms in patients who turn out to have lung cancer
 Red flags are not always reliable but……NICE says • • Any haemoptysis Three weeks of unexplained clubbing or…. . Cough Breathlessness Chest or shoulder pain Weight loss Hoarseness Chest signs • Or just because smokes and tired? Unclear. But probably. • Don’t wait for antibiotics to work
Red flags are not always reliable but……NICE says • • Any haemoptysis Three weeks of unexplained clubbing or…. . Cough Breathlessness Chest or shoulder pain Weight loss Hoarseness Chest signs • Or just because smokes and tired? Unclear. But probably. • Don’t wait for antibiotics to work
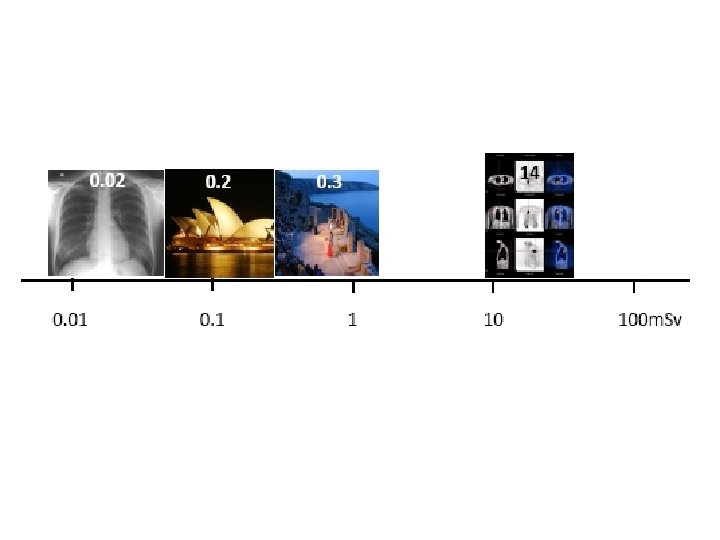
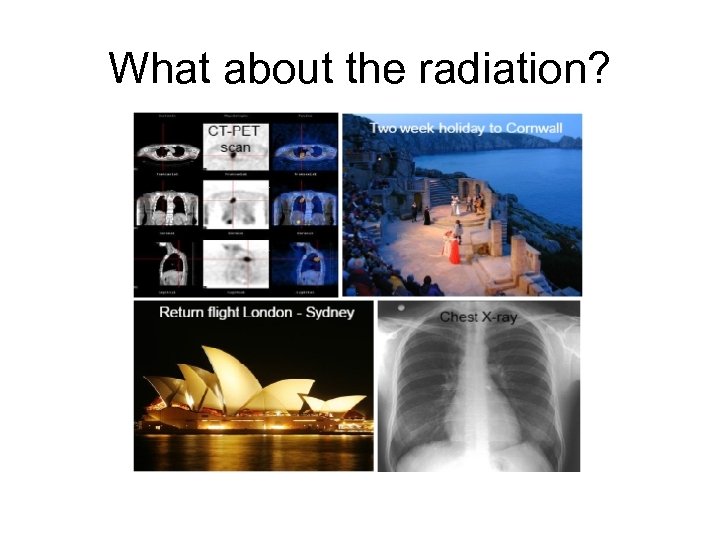 What about the radiation?
What about the radiation?
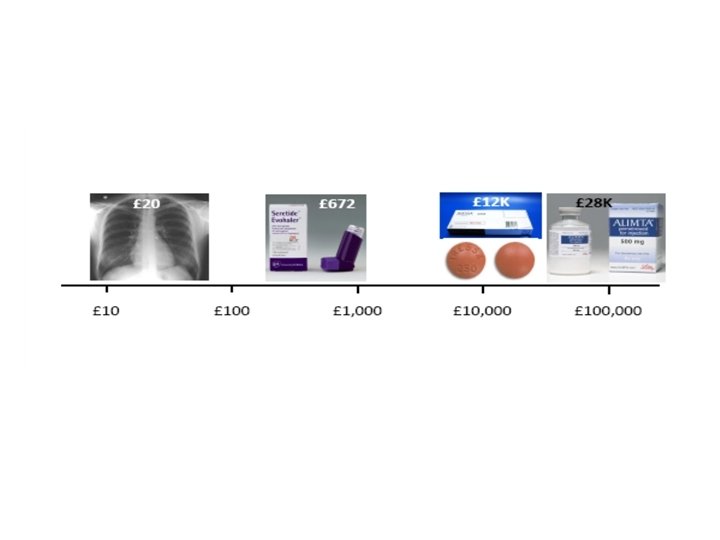
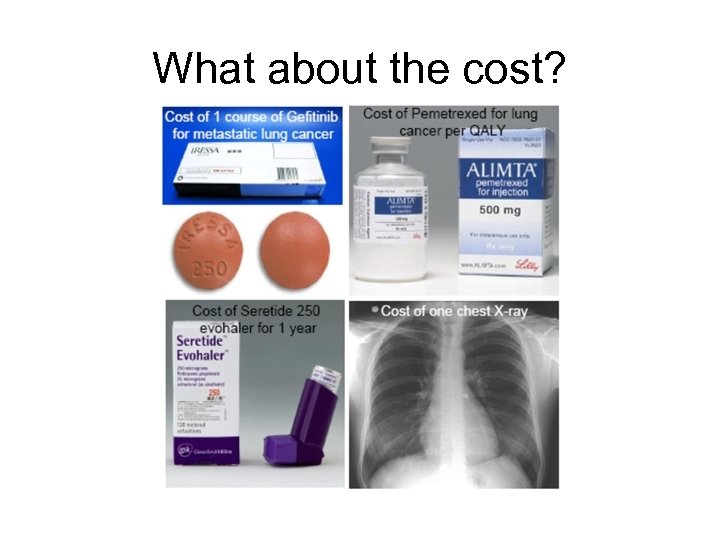 What about the cost?
What about the cost?
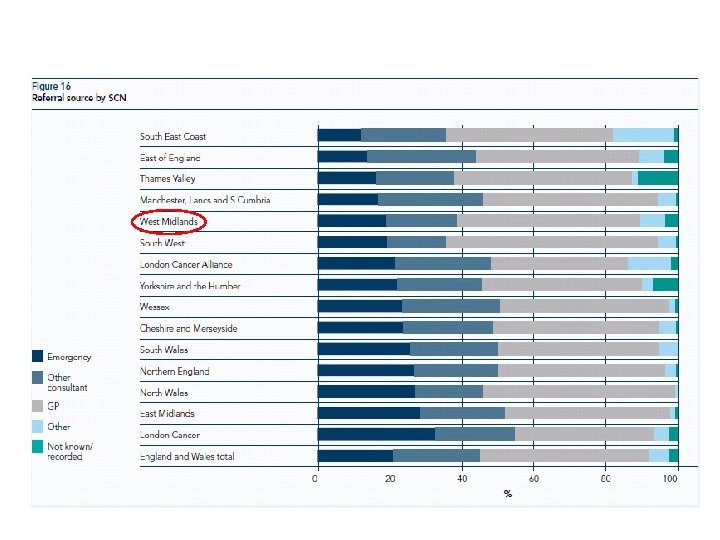
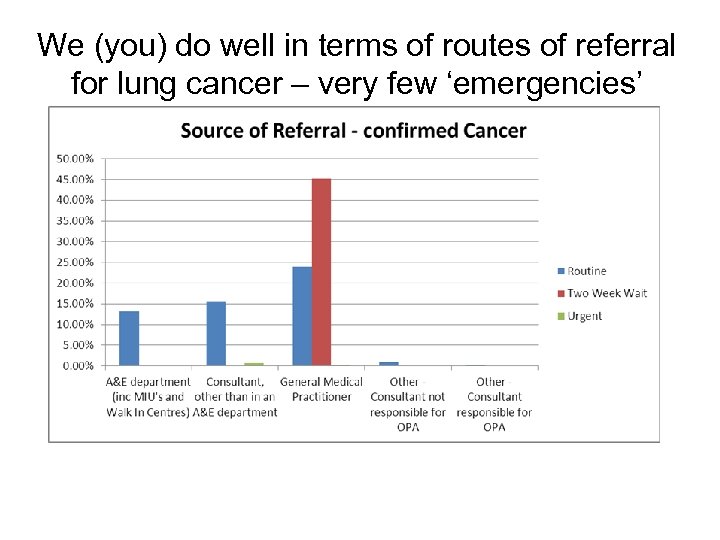 We (you) do well in terms of routes of referral for lung cancer – very few ‘emergencies’
We (you) do well in terms of routes of referral for lung cancer – very few ‘emergencies’
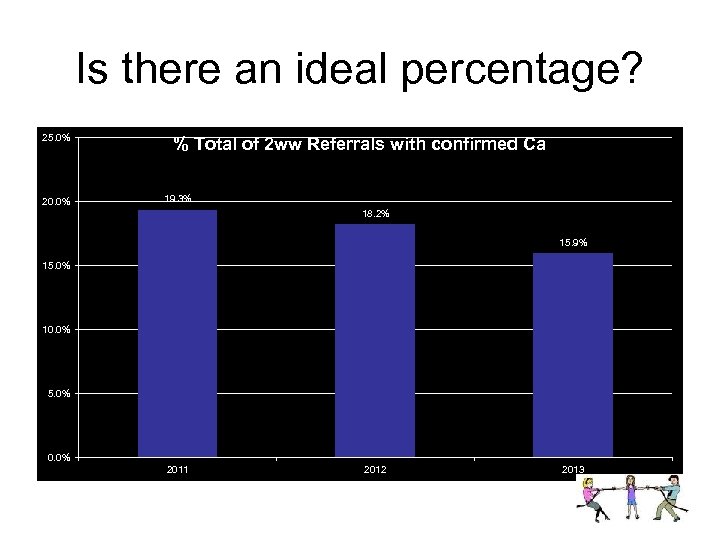 Is there an ideal percentage? 25. 0% 20. 0% % Total of 2 ww Referrals with confirmed Ca 19. 3% 18. 2% 15. 9% 15. 0% 10. 0% 5. 0% 0. 0% 2011 2012 2013
Is there an ideal percentage? 25. 0% 20. 0% % Total of 2 ww Referrals with confirmed Ca 19. 3% 18. 2% 15. 9% 15. 0% 10. 0% 5. 0% 0. 0% 2011 2012 2013
 Lung cancer rates by deprivation quintile
Lung cancer rates by deprivation quintile
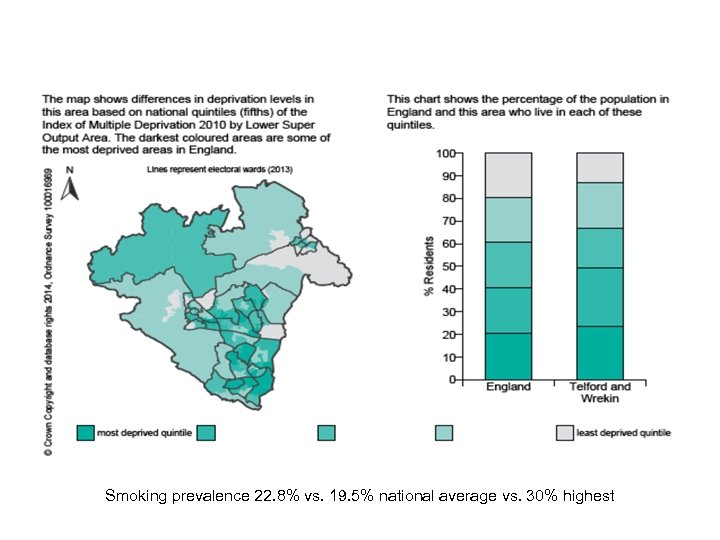 Smoking prevalence 22. 8% vs. 19. 5% national average vs. 30% highest
Smoking prevalence 22. 8% vs. 19. 5% national average vs. 30% highest
 Advocacy, stigma, research • Linked to deprivation and smoking • ‘It’s all my own fault’ • Deserving vs. undeserving cancers • Research spend per annum in the UK: Breast - £ 41 million (£ 3500 per death) Leukaemia - £ 32 million (£ 7000 per death) Lung - £ 15 million (£ 400 per death)
Advocacy, stigma, research • Linked to deprivation and smoking • ‘It’s all my own fault’ • Deserving vs. undeserving cancers • Research spend per annum in the UK: Breast - £ 41 million (£ 3500 per death) Leukaemia - £ 32 million (£ 7000 per death) Lung - £ 15 million (£ 400 per death)


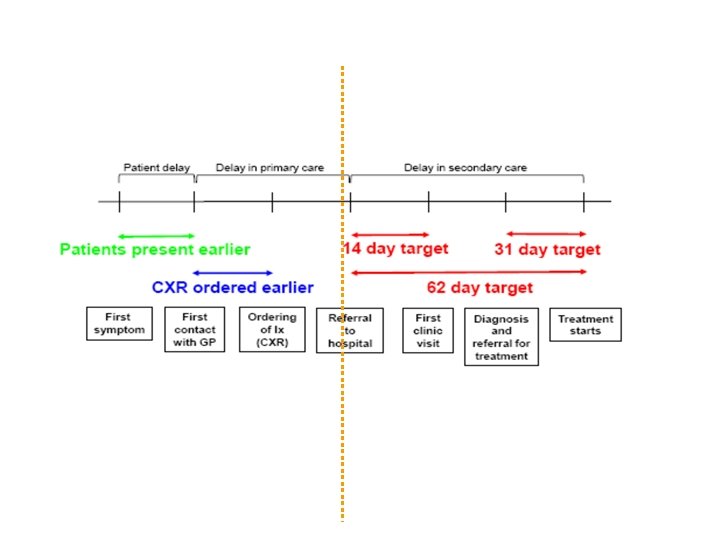
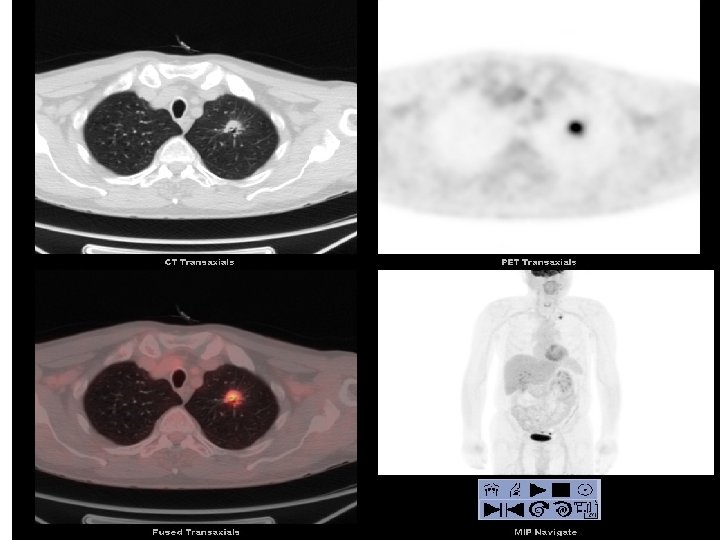
 Diagnosis and Staging • • Accurate diagnosis AND staging is important CT should be before bronchoscopy Most patients should have histology obtained Nodal staging with EBUS is becoming important • ‘Radical’ treatment should be preceded by PET • ‘Open and close rates’ should be <5%
Diagnosis and Staging • • Accurate diagnosis AND staging is important CT should be before bronchoscopy Most patients should have histology obtained Nodal staging with EBUS is becoming important • ‘Radical’ treatment should be preceded by PET • ‘Open and close rates’ should be <5%
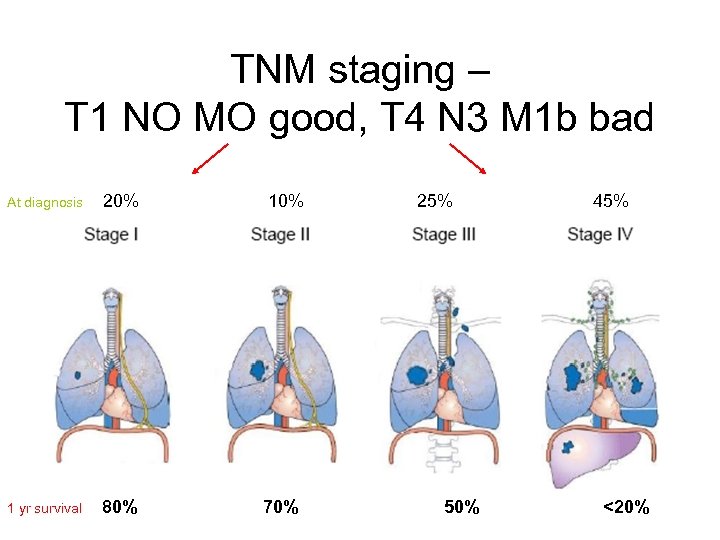 TNM staging – T 1 NO MO good, T 4 N 3 M 1 b bad At diagnosis 20% 1 yr survival 80% 70% 25% 50% 45% <20%
TNM staging – T 1 NO MO good, T 4 N 3 M 1 b bad At diagnosis 20% 1 yr survival 80% 70% 25% 50% 45% <20%
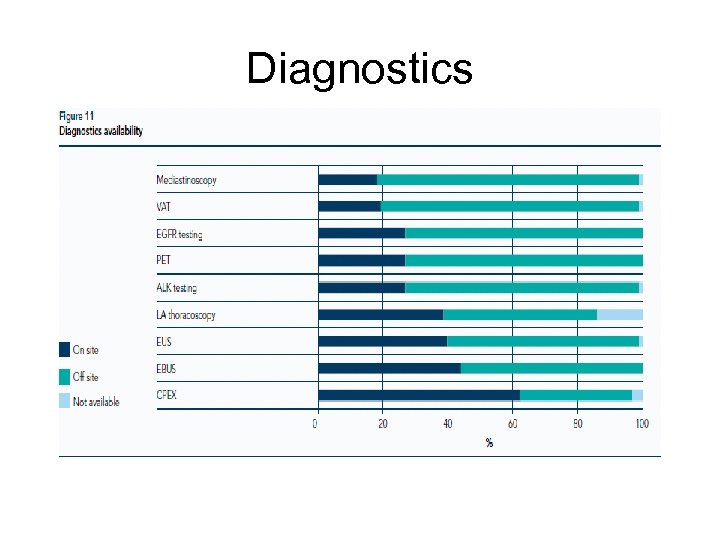 Diagnostics
Diagnostics
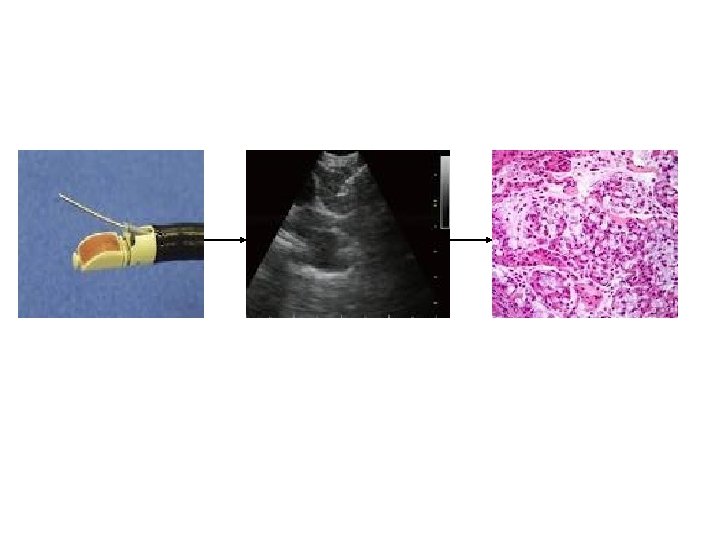
 Treatment • Surgery is preferred radical option • ‘Resectable’ versus ‘operable’ • Radical RT (or SBRT) should be considered even if patient not fit for surgery (‘operable’) • Performance status at diagnosis is crucial: Grade Explanation of activity 0 Fully active, able to carry on all pre-disease performance without restriction 1 Restricted in physically strenuous activity but ambulatory and able to carry out work of a light or sedentary nature, e. g. , light house work, office work 2 Ambulatory and capable of all selfcare but unable to carry out any work activities. Up and about more than 50% of waking hours 3 Capable of only limited selfcare, confined to bed or chair more than 50% of waking hours 4 Completely disabled. Cannot carry on any selfcare. Totally confined to bed or chair 5 Dead
Treatment • Surgery is preferred radical option • ‘Resectable’ versus ‘operable’ • Radical RT (or SBRT) should be considered even if patient not fit for surgery (‘operable’) • Performance status at diagnosis is crucial: Grade Explanation of activity 0 Fully active, able to carry on all pre-disease performance without restriction 1 Restricted in physically strenuous activity but ambulatory and able to carry out work of a light or sedentary nature, e. g. , light house work, office work 2 Ambulatory and capable of all selfcare but unable to carry out any work activities. Up and about more than 50% of waking hours 3 Capable of only limited selfcare, confined to bed or chair more than 50% of waking hours 4 Completely disabled. Cannot carry on any selfcare. Totally confined to bed or chair 5 Dead
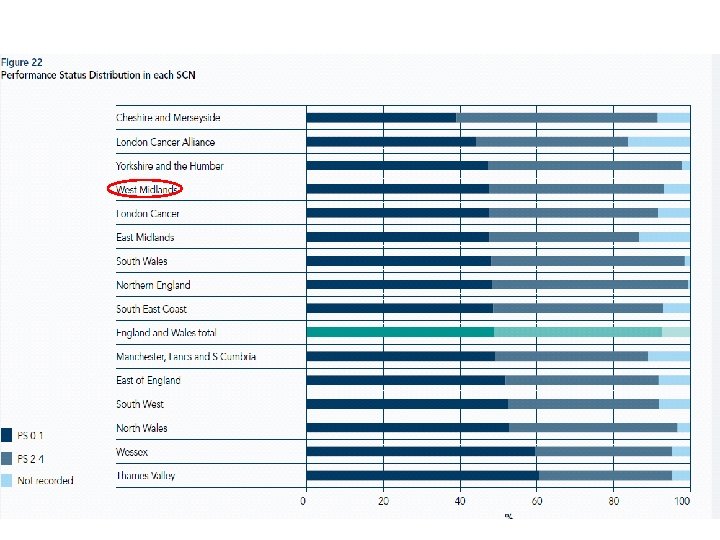
 Things that affect PS • • • Nutrition Pain Continued smoking Low mood Physical activity
Things that affect PS • • • Nutrition Pain Continued smoking Low mood Physical activity
 Surgery
Surgery
 Radiotherapy • Radiotherapy – can be curative, good for pain, brain mets or in combination with chemo • Radical, long course palliative, single fraction • Side effects – skin redness, hair loss, fatigue • Spinal cord and lung damage concerns with higher doses but IMRT reduces risk • Previous RT (eg for breast) may affect current dose
Radiotherapy • Radiotherapy – can be curative, good for pain, brain mets or in combination with chemo • Radical, long course palliative, single fraction • Side effects – skin redness, hair loss, fatigue • Spinal cord and lung damage concerns with higher doses but IMRT reduces risk • Previous RT (eg for breast) may affect current dose
 Chemotherapy • • Neo-adjuvant Adjuvant Palliative – first-line, second-line, maintenance Biologic treatments – gefitinib, erlotinib – oral, fewer side-effects – need receptor testing • • Incremental gains Histological diagnosis more & more important In the future – a panel of receptors tested? Treatment more likely with CNS support
Chemotherapy • • Neo-adjuvant Adjuvant Palliative – first-line, second-line, maintenance Biologic treatments – gefitinib, erlotinib – oral, fewer side-effects – need receptor testing • • Incremental gains Histological diagnosis more & more important In the future – a panel of receptors tested? Treatment more likely with CNS support
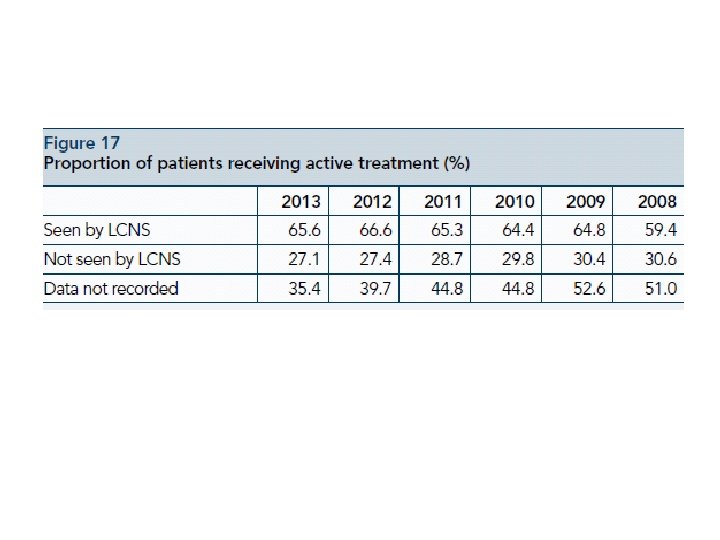 -
-
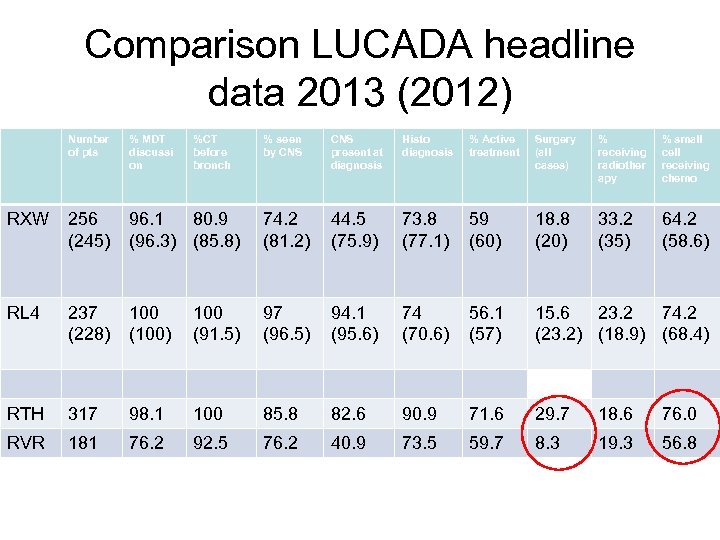 Comparison LUCADA headline data 2013 (2012) Number of pts % MDT discussi on RXW 256 (245) RL 4 %CT before bronch % seen by CNS present at diagnosis Histo diagnosis % Active treatment Surgery (all cases) % receiving radiother apy % small cell receiving chemo 96. 1 80. 9 (96. 3) (85. 8) 74. 2 (81. 2) 44. 5 (75. 9) 73. 8 (77. 1) 59 (60) 18. 8 (20) 33. 2 (35) 64. 2 (58. 6) 237 (228) 100 (100) 100 (91. 5) 97 (96. 5) 94. 1 (95. 6) 74 (70. 6) 56. 1 (57) 15. 6 23. 2 74. 2 (23. 2) (18. 9) (68. 4) RTH 317 98. 1 100 85. 8 82. 6 90. 9 71. 6 29. 7 18. 6 76. 0 RVR 181 76. 2 92. 5 76. 2 40. 9 73. 5 59. 7 8. 3 19. 3 56. 8
Comparison LUCADA headline data 2013 (2012) Number of pts % MDT discussi on RXW 256 (245) RL 4 %CT before bronch % seen by CNS present at diagnosis Histo diagnosis % Active treatment Surgery (all cases) % receiving radiother apy % small cell receiving chemo 96. 1 80. 9 (96. 3) (85. 8) 74. 2 (81. 2) 44. 5 (75. 9) 73. 8 (77. 1) 59 (60) 18. 8 (20) 33. 2 (35) 64. 2 (58. 6) 237 (228) 100 (100) 100 (91. 5) 97 (96. 5) 94. 1 (95. 6) 74 (70. 6) 56. 1 (57) 15. 6 23. 2 74. 2 (23. 2) (18. 9) (68. 4) RTH 317 98. 1 100 85. 8 82. 6 90. 9 71. 6 29. 7 18. 6 76. 0 RVR 181 76. 2 92. 5 76. 2 40. 9 73. 5 59. 7 8. 3 19. 3 56. 8
 Learning points • Smoking and deprivation influence incidence, treatment and outcomes • Improving early diagnosis is complex • X ray early • Aim to maintain PS - including smoking cessation • Surgery preferred treatment option • Accurate staging can be complex and time-consuming • Chemo is improving, individualised • Improving specialist nurse support improves outcomes • Inverse care law – perhaps equal resource not the answer?
Learning points • Smoking and deprivation influence incidence, treatment and outcomes • Improving early diagnosis is complex • X ray early • Aim to maintain PS - including smoking cessation • Surgery preferred treatment option • Accurate staging can be complex and time-consuming • Chemo is improving, individualised • Improving specialist nurse support improves outcomes • Inverse care law – perhaps equal resource not the answer?

 References • British Journal of Cancer (2015) 112, 207– 216. doi: 10. 1038/bjc. 2014. 596 – evaluation of the early diagnosis campaign • http: //www. bbc. co. uk/news/business-22310825 - Robert Peston on funding • http: //www. rcgp. org. uk/clinicalresources/~/media/Files/CIRC/Cancer/Improving. Cancer. Diag nosis • The Patient Paradox by Margaret Mc. Cartney • http: //www. apho. org. uk/resource/item. aspx? RID=142221 – Health Profile for T&W • http: //www. hscic. gov. uk/catalogue/PUB 12719/clin-audi-suppprog-lung-nlca-2013 -rep. pdf
References • British Journal of Cancer (2015) 112, 207– 216. doi: 10. 1038/bjc. 2014. 596 – evaluation of the early diagnosis campaign • http: //www. bbc. co. uk/news/business-22310825 - Robert Peston on funding • http: //www. rcgp. org. uk/clinicalresources/~/media/Files/CIRC/Cancer/Improving. Cancer. Diag nosis • The Patient Paradox by Margaret Mc. Cartney • http: //www. apho. org. uk/resource/item. aspx? RID=142221 – Health Profile for T&W • http: //www. hscic. gov. uk/catalogue/PUB 12719/clin-audi-suppprog-lung-nlca-2013 -rep. pdf


