8f6ed6059c343ae0dbf357eb3ef09858.ppt
- Количество слайдов: 21

Lothian Diabetes Managed Clinical Network Nicola Zammitt Secondary care clinical lead MCN CD ECED MCN meeting 24/11/16

Outline • Context – Diabetes Improvement Plan – Quarterly reporting • Refreshed MCN – Staff – Subgroups/workstreams – Meetings • Recent challenges – T 2 D LES

Diabetes Improvement Plan 2014: Context • In last 10 yrs, 1 o care contacts for diabetes risen by 25%. • Diabetes: 10% of total heath resource expenditure in UK. • NHS Scotland Quality Strategy: – Put people at the heart of everything NHS does – Provide best possible care – Improvement in quality of care involves all staff/levels/roles • Route map to the 2020 Vision for health and Social Care: – – Builds on quality strategy Aim for safe, effective and person-centred care. Focus on 12 priority areas of action Diabetes improvement plan priorities are anchored to those of the route map

2020 Vision for Health and Social Care

Diabetes Improvement Plan (2014): 8 priorities

Diabetes Improvement Plan: 8 priorities

Diabetes Improvement Plan: 12 measures 12 Initial measures 1. % people with DM who receive all 9 key indicator measurements: 1. Weight/BMI 2. Urine albumin creatinine ratio 3. Serum creatinine 4. BP 5. Hb. A 1 c 6. Cholesterol 7. Retinopathy screening 8. Foot risk stratification 9. Smoking status

National Diabetes Improvement Plan 2014 12 Initial measures 1. J 2. % persons with an Hb. A 1 c <58 mmol/mol at 1 year post diagnosis 3. % persons with an Hb. A 1 c <58 mmol/mol and >75 mmol/mol 4. % current smokers 5. % people aged 50 -80 with total chol <5 mmol/l AND SBP <140 mm. Hg 6. % of new foot ulcers 7. % of eligible people who got retinopathy screening in last 15 months 8. % of people with diabetes with end stage renal disease or on dialysis 9. % people on insulin pumps 10. % people with BMI ≥ 30 who have lost ≥ 5% body weight in last year 11. % persons who have attended structured education 12. % disengaged from care (no Hb. A 1 c or retinal screening in last 15/12)

Quarterly reporting • From Jan 2016: NHS Boards (through MCNs) provide quarterly report outlining progress against the 12 diabetes quality measures. Section 1 Baseline and Self-Assessment • Use RAG rating to indicate baseline performance for the start of quarter 1 • Self-assessment: consider where focussed action is needed, where current activity will support continued improvement or where no action is required. • Section 1 only completed once at start of reporting year. • Overview and some examples:
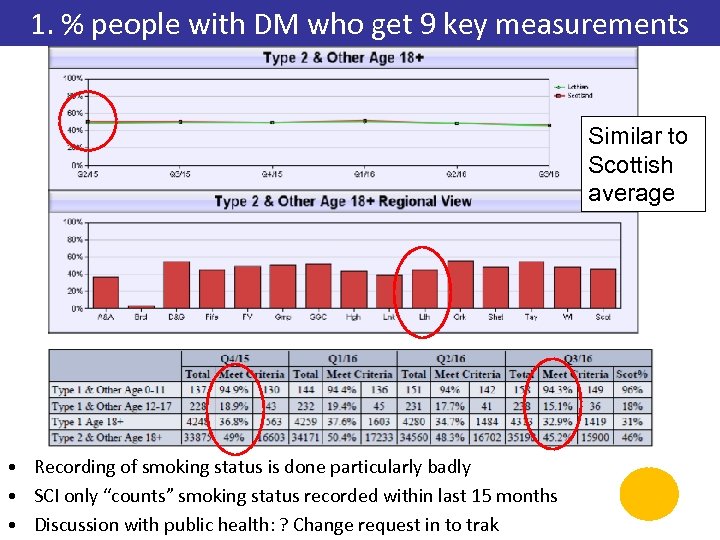
1. % people with DM who get 9 key measurements Similar to Scottish average • Recording of smoking status is done particularly badly • SCI only “counts” smoking status recorded within last 15 months • Discussion with public health: ? Change request in to trak
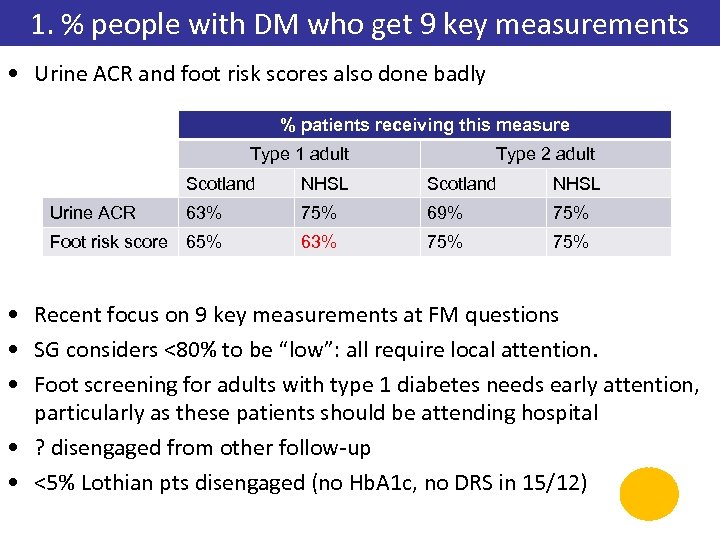
1. % people with DM who get 9 key measurements • Urine ACR and foot risk scores also done badly % patients receiving this measure Type 1 adult Type 2 adult Scotland NHSL Urine ACR 63% 75% 69% 75% Foot risk score 65% 63% 75% • Recent focus on 9 key measurements at FM questions • SG considers <80% to be “low”: all require local attention. • Foot screening for adults with type 1 diabetes needs early attention, particularly as these patients should be attending hospital • ? disengaged from other follow-up • <5% Lothian pts disengaged (no Hb. A 1 c, no DRS in 15/12)
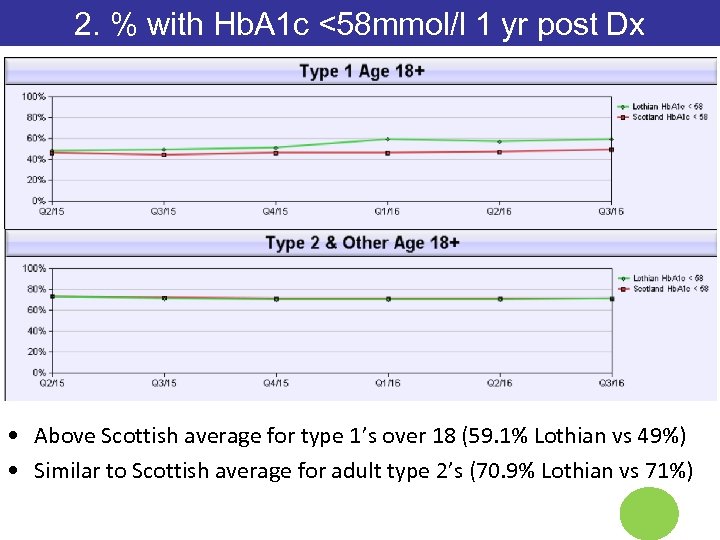
2. % with Hb. A 1 c <58 mmol/l 1 yr post Dx • Above Scottish average for type 1’s over 18 (59. 1% Lothian vs 49%) • Similar to Scottish average for adult type 2’s (70. 9% Lothian vs 71%)
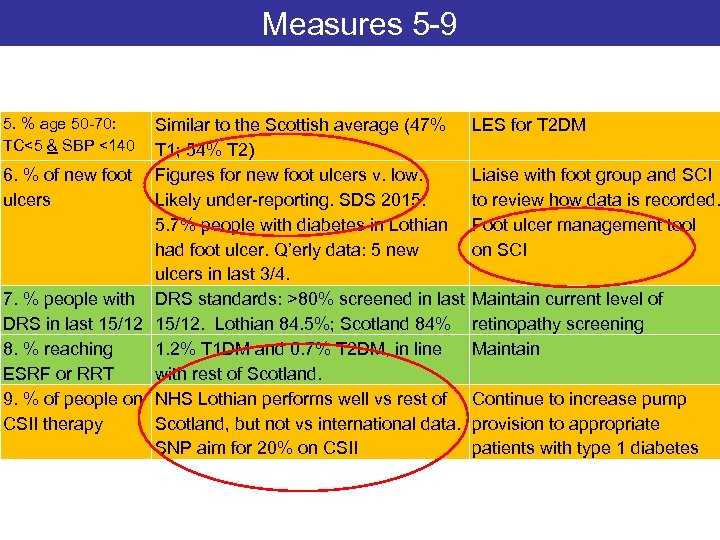
Measures 5 -9 5. % age 50 -70: TC<5 & SBP <140 Similar to the Scottish average (47% T 1; 54% T 2) 6. % of new foot Figures for new foot ulcers v. low. ulcers Likely under-reporting. SDS 2015: 5. 7% people with diabetes in Lothian had foot ulcer. Q’erly data: 5 new ulcers in last 3/4. 7. % people with DRS standards: >80% screened in last DRS in last 15/12. Lothian 84. 5%; Scotland 84% 8. % reaching 1. 2% T 1 DM and 0. 7% T 2 DM, in line ESRF or RRT with rest of Scotland. 9. % of people on NHS Lothian performs well vs rest of CSII therapy Scotland, but not vs international data. SNP aim for 20% on CSII LES for T 2 DM Liaise with foot group and SCI to review how data is recorded. Foot ulcer management tool on SCI Maintain current level of retinopathy screening Maintain Continue to increase pump provision to appropriate patients with type 1 diabetes
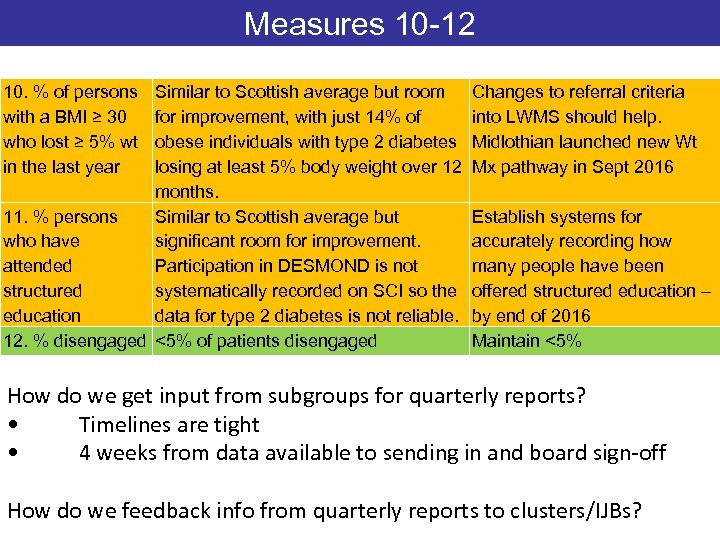

Measures 10 -12 10. % of persons with a BMI ≥ 30 who lost ≥ 5% wt in the last year Similar to Scottish average but room for improvement, with just 14% of obese individuals with type 2 diabetes losing at least 5% body weight over 12 months. 11. % persons Similar to Scottish average but who have significant room for improvement. attended Participation in DESMOND is not structured systematically recorded on SCI so the education data for type 2 diabetes is not reliable. 12. % disengaged <5% of patients disengaged Changes to referral criteria into LWMS should help. Midlothian launched new Wt Mx pathway in Sept 2016 Establish systems for accurately recording how many people have been offered structured education – by end of 2016 Maintain <5% How do we get input from subgroups for quarterly reports? • Timelines are tight • 4 weeks from data available to sending in and board sign-off How do we feedback info from quarterly reports to clusters/IJBs?

Refreshed MCN

Refreshed MCN • • Clinical lead role shared 1 o/2 o care (David Jolliffe, Nicola Zammitt) 2 o care clinical lead is also Diabetes CD New strategic programme manager (Paul Currie → Alyson Cumming) New MCN coordinator (Bonnie Thomson → Marie Mc. Callum) • HSCPS – IJBs. • LTCs – House of Care, multimorbidity hubs, c. DSNs • New public health liaison – Joy Tomlinson → Sarah Wild. Duncan Mc. Cormick to lead DRS • New sub-groups aligned to improvement plan – Time is precious. Need room for new players. – Other autonomous groups link to MCN but not formal sub-groups. SLWGs as necessary • Leaner MCN. Meet quarterly.

Refreshed MCN • New sub-groups aligned to improvement plan – Prevention & early detection (plus public health and ? Prescribing) – T 1 DM – Innovation – In patient diabetes – Education (improving info and supporting/developing staff) • Feet • Threads run thro all groups: Person-centred care, equality of access.
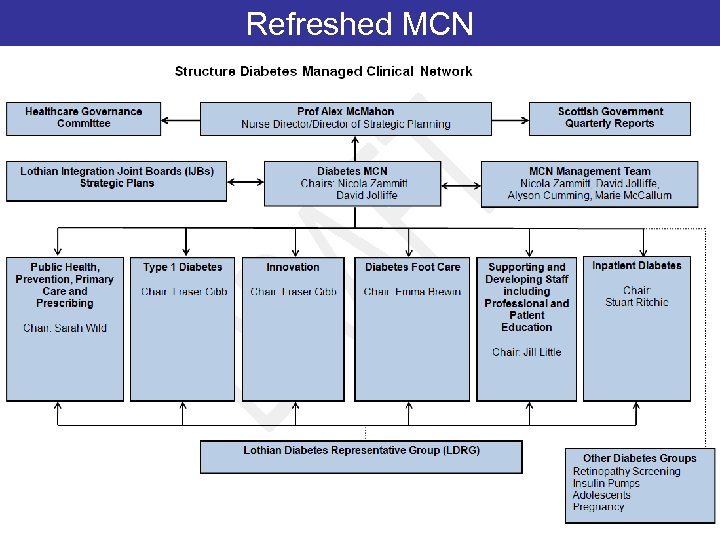
Refreshed MCN

Background to LES • 2012 Diabetes MCN reviewed T 2 pathway • Pathway presented to LMC: T 2 LES to support pathway • 2015 -16: 1 o care investment £ 1 M (non recurring) to support key strategic priorities incl LES. Approved by NHSL Board. • From July 2015: LES funding to GPs to: – Assess and manage new onset patients – Help reflect the rise in prevalence and complexity • 118/125 practices signed up (95%) – engagement fee £ 300 per practice - £ 35, 400 – Practices paid £ 120 per newly diagnosed patient managed • Total cost of LES for 9 months - £ 229, 320

LES going forward • 31/3/16: non-extension of LES funding • After extensive discussions, decision on 14/6/16 to reinstate. Risk sharing approach with IJBs: £ 220 k for rest of financial year • Challenge to identify future funds (? £ 5 M for 1 o care over 5 years) • CMT agreed on 14/11/16 to support LES but IJBs to discuss funding. LES Service outcomes: Named practice lead (GP or Practice nurse) is required to: 1. Keep up to date with current MCN and LJF recommendations on diabetes care, incl indications for referral. 2. Liaise with the Community Diabetes Specialist Nurses (DSN). 3. Ensure that relevant practice staff remain abreast of service developments and referral pathways (incl annual educational update)

LES: what does it cover? Work included in LES (£ 120 per new patient): • Correct coding at diagnosis: populates SCI Diabetes • In house education on diet and lifestyle (GP, nurse, pharmacist, AHP) • Refer to DESMOND or other suitable structured education • CV risk score • Foot assessment +/- referral • Review of all the standard diabetes Qo. F indicators • Work of initial assessment – Identify complications (retinopathy screening automatically triggered) – Initiate diet and medical therapy +/- referral – Establish FU in line with guidelines and MCN recommendations • LES needs refreshing (QOF removed, new T 2 Dx pathway – Hb. A 1 c). • Opportunity to build quality into refresh Eg aim Hb. A 1 c<58 mmol/mol at 1 yr post-Dx (measure 2 on improvement plan)
8f6ed6059c343ae0dbf357eb3ef09858.ppt