a07e3643b4dfc9e6cb70f21d9c9ccfea.ppt
- Количество слайдов: 39
 Lifestyle Therapy and Fertility in Women with PCOS Infertility Treatment in PCOS Richard S. Legro, M. D. Penn State College of Medicine Dept of Ob/Gyn Hershey, PA
Lifestyle Therapy and Fertility in Women with PCOS Infertility Treatment in PCOS Richard S. Legro, M. D. Penn State College of Medicine Dept of Ob/Gyn Hershey, PA
 l AUTHORS' CONCLUSIONS: No RCTs were located that assessed the effects of preconception advice on the chance of a live birth or other fertility outcomes in people who perceived that they may be infertile and were investigating the possibility of medical treatment to address subfertility.
l AUTHORS' CONCLUSIONS: No RCTs were located that assessed the effects of preconception advice on the chance of a live birth or other fertility outcomes in people who perceived that they may be infertile and were investigating the possibility of medical treatment to address subfertility.
 There ıs no evidence based schema Hum Reprod. 2008 Mar; 23(3): 462 -77 and Fertil Steril. 2008 Mar; 89(3): 505 -22
There ıs no evidence based schema Hum Reprod. 2008 Mar; 23(3): 462 -77 and Fertil Steril. 2008 Mar; 89(3): 505 -22
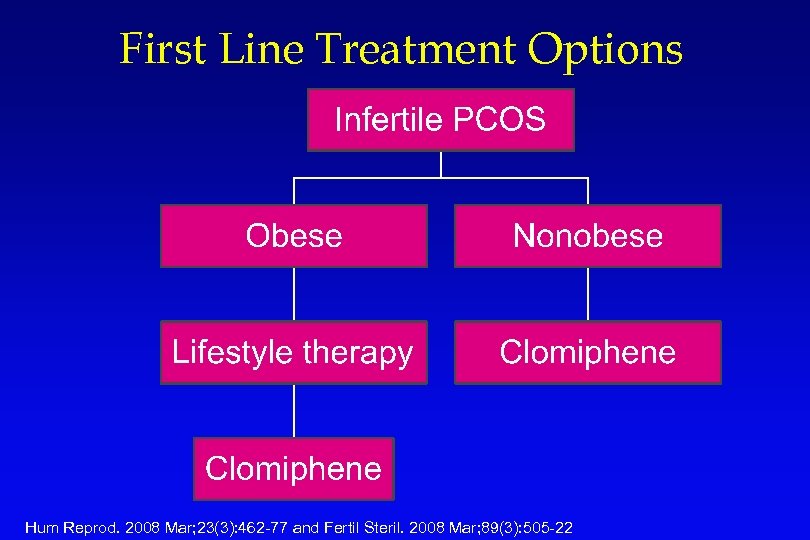 First Line Treatment Options Hum Reprod. 2008 Mar; 23(3): 462 -77 and Fertil Steril. 2008 Mar; 89(3): 505 -22
First Line Treatment Options Hum Reprod. 2008 Mar; 23(3): 462 -77 and Fertil Steril. 2008 Mar; 89(3): 505 -22
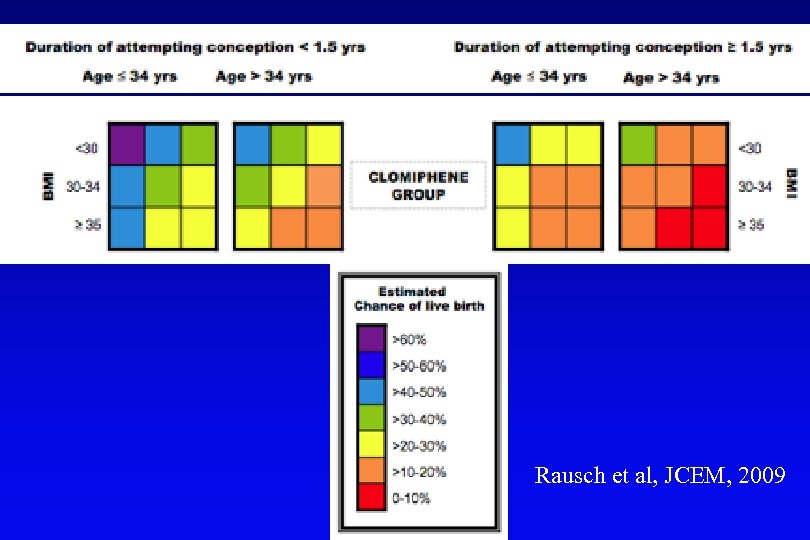 Rausch et al, JCEM, 2009
Rausch et al, JCEM, 2009
 Can we achieve meaningful weight loss which will improve fertility outcomes?
Can we achieve meaningful weight loss which will improve fertility outcomes?
 Limitations of Lifestyle Therapy in Infertility l Dose? u. Is there an ideal rate of weight loss or activity increase l Duration? u. How long should the intervention be instituted l Timing? u. Is the intervention before or during infertility treatment? l Patient Compliance (buy in) u. Will patients be able to follow our instructions
Limitations of Lifestyle Therapy in Infertility l Dose? u. Is there an ideal rate of weight loss or activity increase l Duration? u. How long should the intervention be instituted l Timing? u. Is the intervention before or during infertility treatment? l Patient Compliance (buy in) u. Will patients be able to follow our instructions
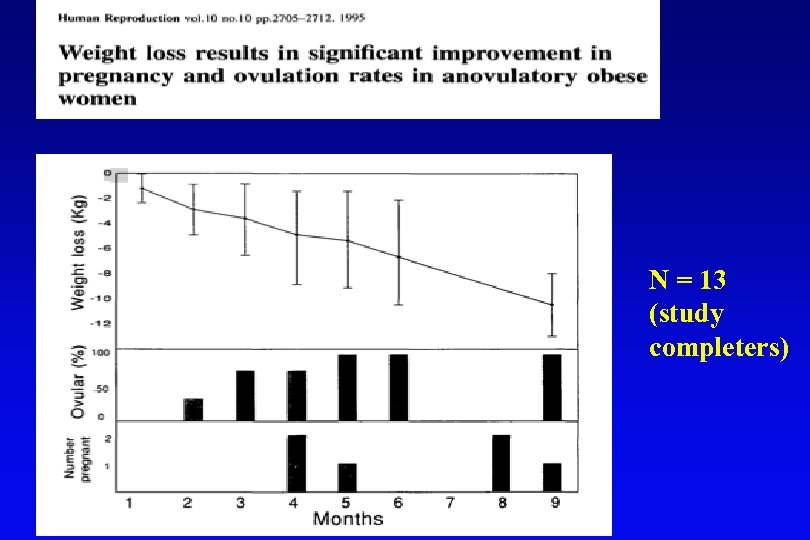 N = 13 (study completers)
N = 13 (study completers)
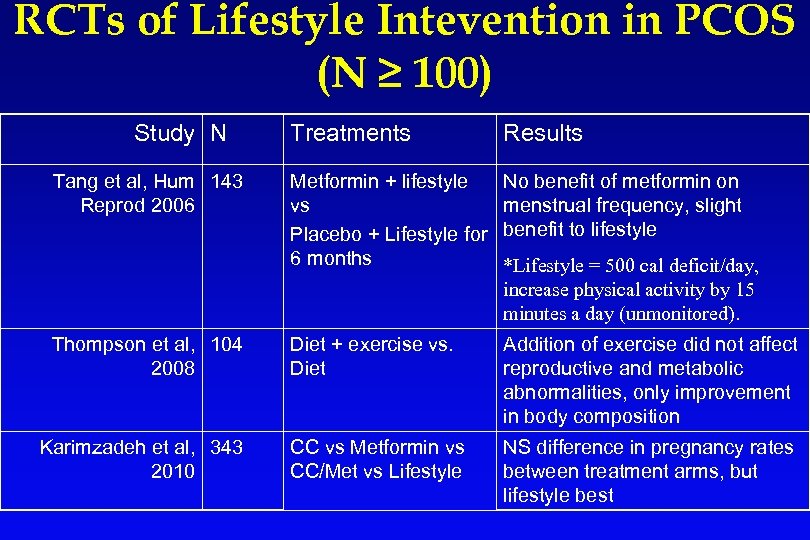 RCTs of Lifestyle Intevention in PCOS (N ≥ 100) Study N Tang et al, Hum 143 Reprod 2006 Thompson et al, 104 2008 Karimzadeh et al, 343 2010 Treatments Results Metformin + lifestyle vs Placebo + Lifestyle for 6 months No benefit of metformin on menstrual frequency, slight benefit to lifestyle Diet + exercise vs. Diet Addition of exercise did not affect reproductive and metabolic abnormalities, only improvement in body composition CC vs Metformin vs CC/Met vs Lifestyle NS difference in pregnancy rates between treatment arms, but lifestyle best *Lifestyle = 500 cal deficit/day, increase physical activity by 15 minutes a day (unmonitored).
RCTs of Lifestyle Intevention in PCOS (N ≥ 100) Study N Tang et al, Hum 143 Reprod 2006 Thompson et al, 104 2008 Karimzadeh et al, 343 2010 Treatments Results Metformin + lifestyle vs Placebo + Lifestyle for 6 months No benefit of metformin on menstrual frequency, slight benefit to lifestyle Diet + exercise vs. Diet Addition of exercise did not affect reproductive and metabolic abnormalities, only improvement in body composition CC vs Metformin vs CC/Met vs Lifestyle NS difference in pregnancy rates between treatment arms, but lifestyle best *Lifestyle = 500 cal deficit/day, increase physical activity by 15 minutes a day (unmonitored).
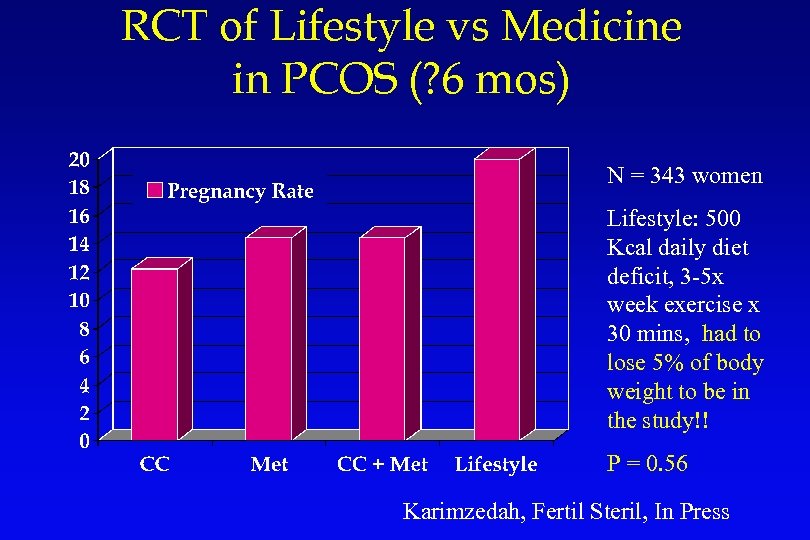 RCT of Lifestyle vs Medicine in PCOS (? 6 mos) N = 343 women Lifestyle: 500 Kcal daily diet deficit, 3 -5 x week exercise x 30 mins, had to lose 5% of body weight to be in the study!! P = 0. 56 Karimzedah, Fertil Steril, In Press
RCT of Lifestyle vs Medicine in PCOS (? 6 mos) N = 343 women Lifestyle: 500 Kcal daily diet deficit, 3 -5 x week exercise x 30 mins, had to lose 5% of body weight to be in the study!! P = 0. 56 Karimzedah, Fertil Steril, In Press
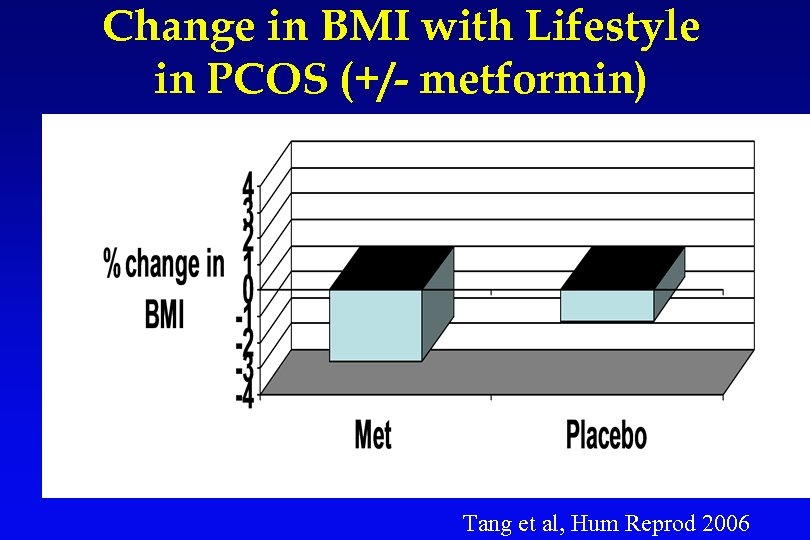 Change in BMI with Lifestyle in PCOS (+/- metformin) Tang et al, Hum Reprod 2006
Change in BMI with Lifestyle in PCOS (+/- metformin) Tang et al, Hum Reprod 2006
 Metformin, Lifestyle Modification or OC treatment in PCOS l l l Pilot trial of 43 obese adolescents with PCOS randomized to metformin, placebo, lifestyle modification or oral contraceptive for 6 months Lifestyle Modification: Combined group start, parent/adolescent 24 class educational session, 500 cal/d deficit, 30 mins/d moderate to intense activity, unmonitored) 9 dropped out ( 3 of 11 in lifestyle) Hoeger, et al JCEM 2008
Metformin, Lifestyle Modification or OC treatment in PCOS l l l Pilot trial of 43 obese adolescents with PCOS randomized to metformin, placebo, lifestyle modification or oral contraceptive for 6 months Lifestyle Modification: Combined group start, parent/adolescent 24 class educational session, 500 cal/d deficit, 30 mins/d moderate to intense activity, unmonitored) 9 dropped out ( 3 of 11 in lifestyle) Hoeger, et al JCEM 2008
 Weight changes by group Hoeger, et al JCEM 2008
Weight changes by group Hoeger, et al JCEM 2008
 Combination therapy for obese PCOS adolescents l l l Follow Up Trial of 36 obese adolescents treated with oral contraceptive (ethinyl estradiol + drosperinone) with metformin or placebo 4 dropped out over the 6 month trial. All received lifestyle modification program as before (parent/adolescent educational program, 500 cal/d deficit/30 mins/d exercise- now monitored, flexible enrollment, email/web support) Hoeger et al JCEM 2008
Combination therapy for obese PCOS adolescents l l l Follow Up Trial of 36 obese adolescents treated with oral contraceptive (ethinyl estradiol + drosperinone) with metformin or placebo 4 dropped out over the 6 month trial. All received lifestyle modification program as before (parent/adolescent educational program, 500 cal/d deficit/30 mins/d exercise- now monitored, flexible enrollment, email/web support) Hoeger et al JCEM 2008
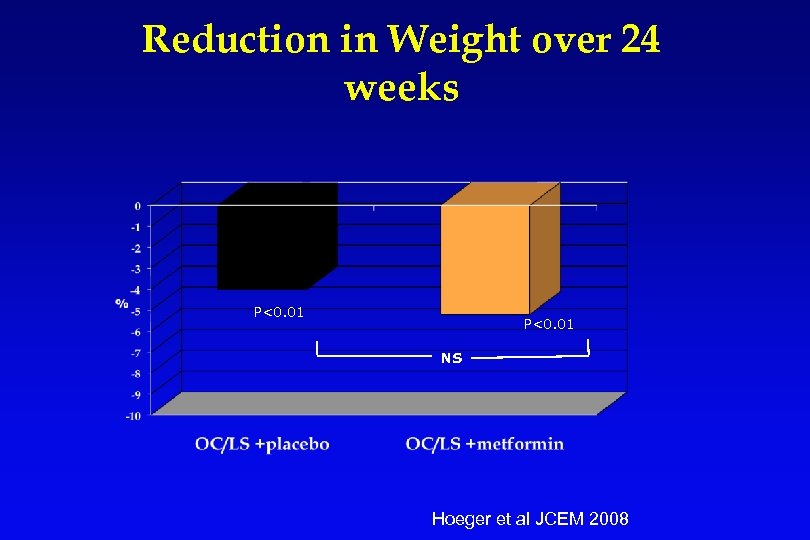 Reduction in Weight over 24 weeks P<0. 01 NS Hoeger et al JCEM 2008
Reduction in Weight over 24 weeks P<0. 01 NS Hoeger et al JCEM 2008
 High Dropout in PCOS Lifestyle Studies 50% Dropout after Randomization Thomson, R. L. et al. J Clin Endocrinol Metab 2008; 93: 3373 -3380
High Dropout in PCOS Lifestyle Studies 50% Dropout after Randomization Thomson, R. L. et al. J Clin Endocrinol Metab 2008; 93: 3373 -3380
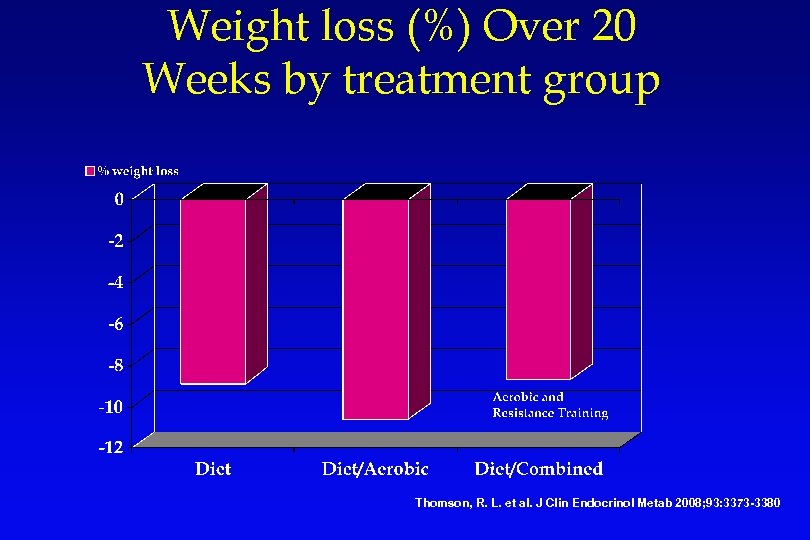 Weight loss (%) Over 20 Weeks by treatment group Thomson, R. L. et al. J Clin Endocrinol Metab 2008; 93: 3373 -3380
Weight loss (%) Over 20 Weeks by treatment group Thomson, R. L. et al. J Clin Endocrinol Metab 2008; 93: 3373 -3380
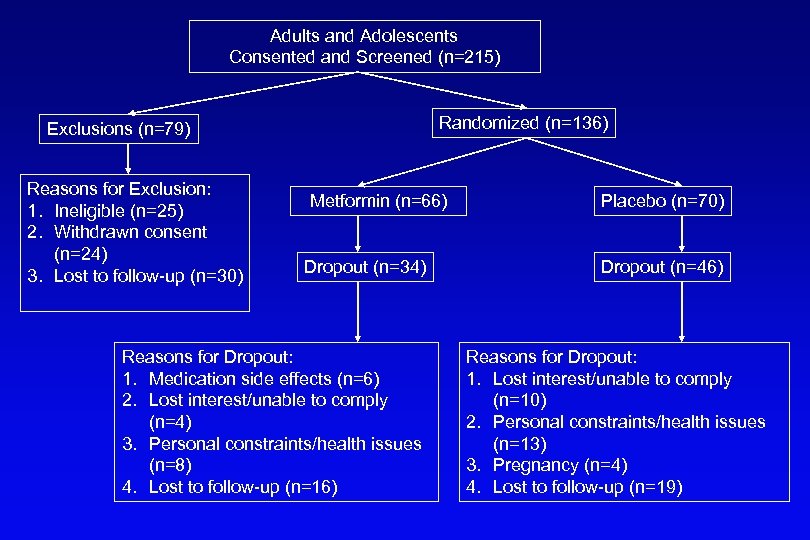 Adults and Adolescents Consented and Screened (n=215) Randomized (n=136) Exclusions (n=79) Reasons for Exclusion: 1. Ineligible (n=25) 2. Withdrawn consent (n=24) 3. Lost to follow-up (n=30) Metformin (n=66) Dropout (n=34) Reasons for Dropout: 1. Medication side effects (n=6) 2. Lost interest/unable to comply (n=4) 3. Personal constraints/health issues (n=8) 4. Lost to follow-up (n=16) Placebo (n=70) Dropout (n=46) Reasons for Dropout: 1. Lost interest/unable to comply (n=10) 2. Personal constraints/health issues (n=13) 3. Pregnancy (n=4) 4. Lost to follow-up (n=19)
Adults and Adolescents Consented and Screened (n=215) Randomized (n=136) Exclusions (n=79) Reasons for Exclusion: 1. Ineligible (n=25) 2. Withdrawn consent (n=24) 3. Lost to follow-up (n=30) Metformin (n=66) Dropout (n=34) Reasons for Dropout: 1. Medication side effects (n=6) 2. Lost interest/unable to comply (n=4) 3. Personal constraints/health issues (n=8) 4. Lost to follow-up (n=16) Placebo (n=70) Dropout (n=46) Reasons for Dropout: 1. Lost interest/unable to comply (n=10) 2. Personal constraints/health issues (n=13) 3. Pregnancy (n=4) 4. Lost to follow-up (n=19)
 Penn State College of Medicine/ Meharry Medical College Demographics l Penn l l l State Rural Primarily Caucasian Located in Hershey PA l Meharry l l l Urban Diverse Located in Nashville TN
Penn State College of Medicine/ Meharry Medical College Demographics l Penn l l l State Rural Primarily Caucasian Located in Hershey PA l Meharry l l l Urban Diverse Located in Nashville TN
 Lifestyle Intervention l Dietary u. Lose 7% of body weight in 6 mos and maintain. u. Hypocaloric diet l Exercise u. Supervised – 1 session/week u. Unsupervised – 1500 -2000 kcal/wk u. Monitor Submaximal VO 2 Max monthly
Lifestyle Intervention l Dietary u. Lose 7% of body weight in 6 mos and maintain. u. Hypocaloric diet l Exercise u. Supervised – 1 session/week u. Unsupervised – 1500 -2000 kcal/wk u. Monitor Submaximal VO 2 Max monthly
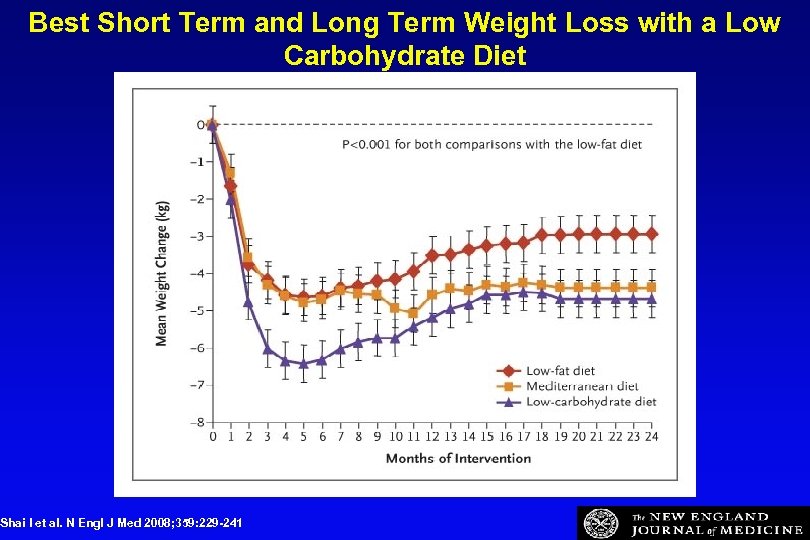 Best Short Term and Long Term Weight Loss with a Low Carbohydrate Diet Shai I et al. N Engl J Med 2008; 359: 229 -241
Best Short Term and Long Term Weight Loss with a Low Carbohydrate Diet Shai I et al. N Engl J Med 2008; 359: 229 -241
 Methods to Encourage Compliance Diet and exercise logs Weekly phone visit Exchange records 2 week visits Pedometer data Heart monitor data Educational modules Supervised exercised sessions
Methods to Encourage Compliance Diet and exercise logs Weekly phone visit Exchange records 2 week visits Pedometer data Heart monitor data Educational modules Supervised exercised sessions
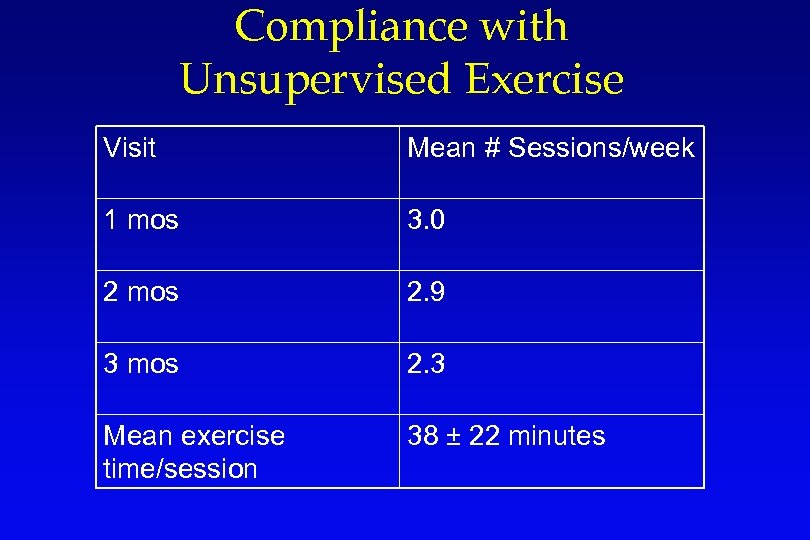 Compliance with Unsupervised Exercise Visit Mean # Sessions/week 1 mos 3. 0 2 mos 2. 9 3 mos 2. 3 Mean exercise time/session 38 ± 22 minutes
Compliance with Unsupervised Exercise Visit Mean # Sessions/week 1 mos 3. 0 2 mos 2. 9 3 mos 2. 3 Mean exercise time/session 38 ± 22 minutes
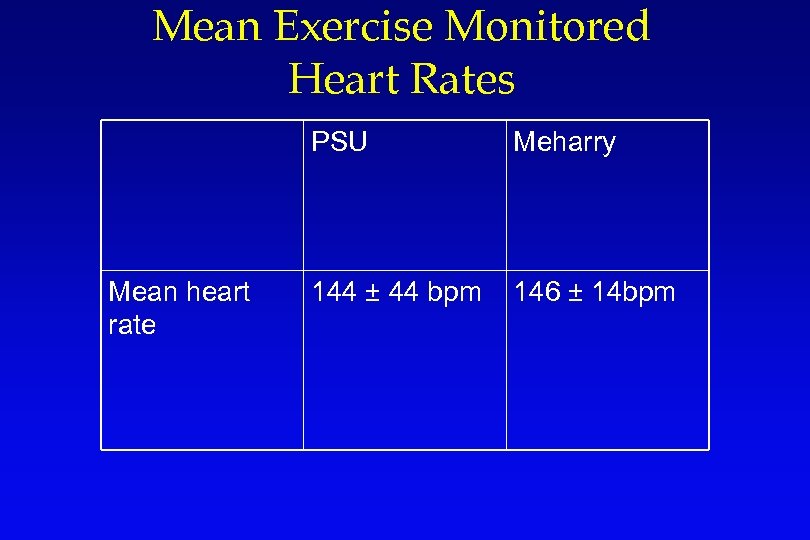 Mean Exercise Monitored Heart Rates PSU Mean heart rate Meharry 144 ± 44 bpm 146 ± 14 bpm
Mean Exercise Monitored Heart Rates PSU Mean heart rate Meharry 144 ± 44 bpm 146 ± 14 bpm
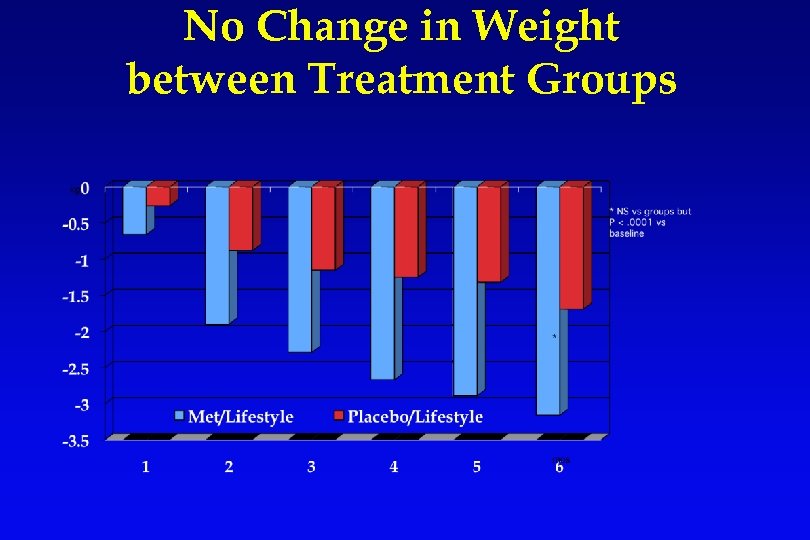 No Change in Weight between Treatment Groups
No Change in Weight between Treatment Groups
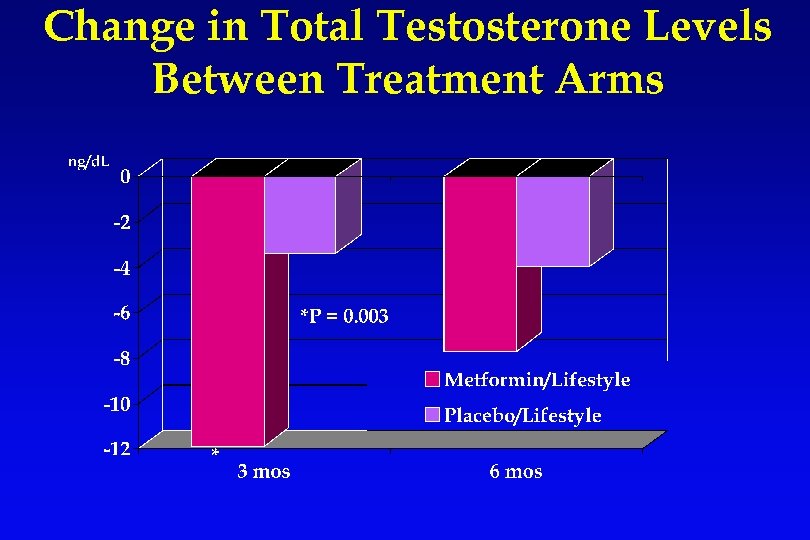 Change in Total Testosterone Levels Between Treatment Arms
Change in Total Testosterone Levels Between Treatment Arms
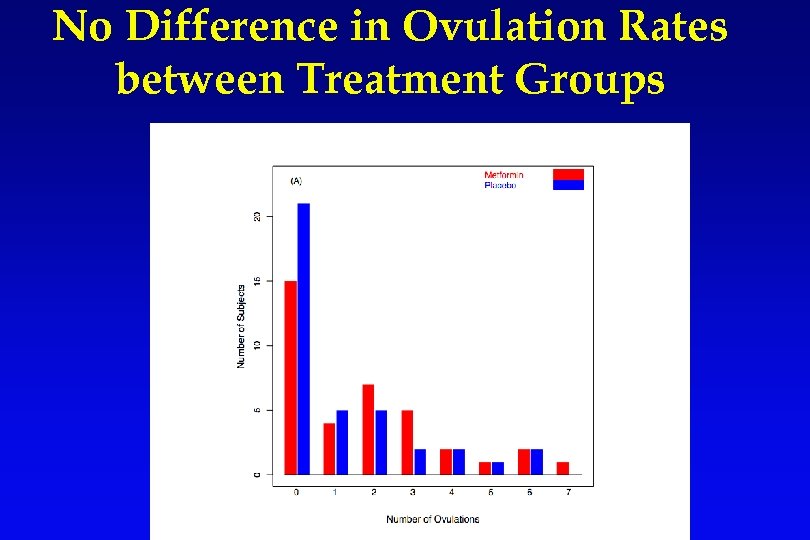 No Difference in Ovulation Rates between Treatment Groups
No Difference in Ovulation Rates between Treatment Groups
 Summary: Lessons Learned l External Validity u. Many will not even attempt a lifestyle intervention u. Most who do will drop out u. Severely obese patients may be poor candidates for such programs u. There will be hurdles to implementing these programs in our current medical system l Best Case Scenario u. Modest Effects, ? Improved outcomes
Summary: Lessons Learned l External Validity u. Many will not even attempt a lifestyle intervention u. Most who do will drop out u. Severely obese patients may be poor candidates for such programs u. There will be hurdles to implementing these programs in our current medical system l Best Case Scenario u. Modest Effects, ? Improved outcomes
 The common resources of the lancet, a garden, a kitchen, fresh air, cool water and exercise will be sufficient to cure all diseases that are at present under the power of medicine Benjamin Rush (1745 -1813)
The common resources of the lancet, a garden, a kitchen, fresh air, cool water and exercise will be sufficient to cure all diseases that are at present under the power of medicine Benjamin Rush (1745 -1813)
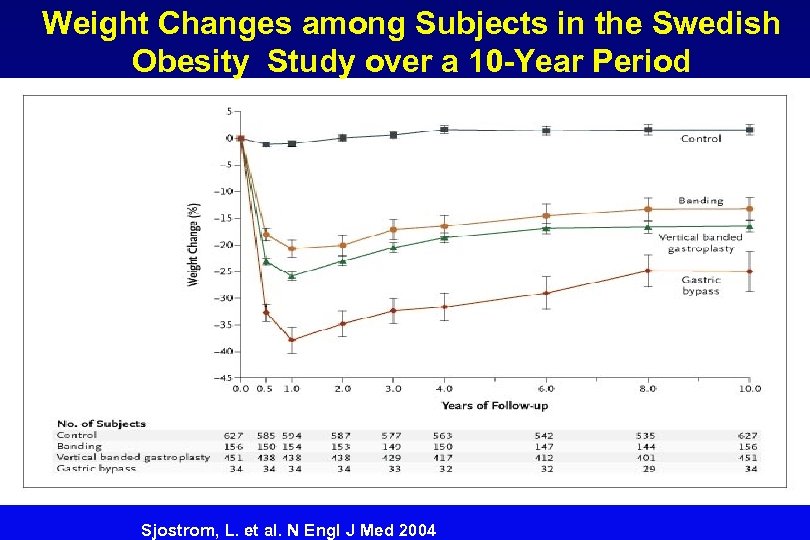 Weight Changes among Subjects in the Swedish Obesity Study over a 10 -Year Period Sjostrom, L. et al. N Engl J Med 2004
Weight Changes among Subjects in the Swedish Obesity Study over a 10 -Year Period Sjostrom, L. et al. N Engl J Med 2004
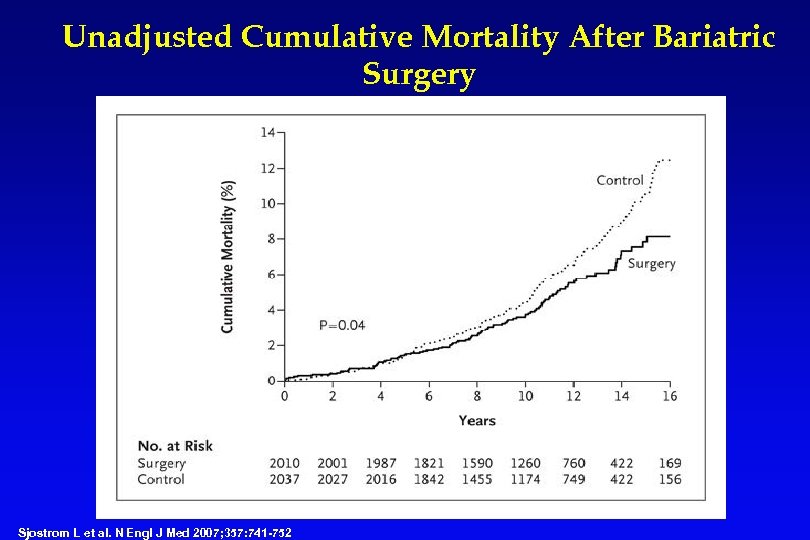 Unadjusted Cumulative Mortality After Bariatric Surgery Sjostrom L et al. N Engl J Med 2007; 357: 741 -752
Unadjusted Cumulative Mortality After Bariatric Surgery Sjostrom L et al. N Engl J Med 2007; 357: 741 -752
 NIH consensus: Indications for Bariatric Surgery BMI > 40 l BMI > 35 with serious medical comorbidities l u. Is PCOS and/or infertility a serious medical comorbidity Malcolm, NEJM, 2009
NIH consensus: Indications for Bariatric Surgery BMI > 40 l BMI > 35 with serious medical comorbidities l u. Is PCOS and/or infertility a serious medical comorbidity Malcolm, NEJM, 2009
 Reproductive Health in Women undergoing Bariatric Surgery l l 1, 538 females having bariatric surgery (NIH-LABS Consortium). PCOS had been diagnosed in 13. 1% of subjects. Women who were obese by 18 years old were more likely to report PCOS and infertility and less likely to have ever been pregnant, compared with women who became obese later in life. Future pregnancy was important to 30. 3% of women younger than 45 years, and overall to 51. 4%. Gosman et al, Fertil Steril, 2009
Reproductive Health in Women undergoing Bariatric Surgery l l 1, 538 females having bariatric surgery (NIH-LABS Consortium). PCOS had been diagnosed in 13. 1% of subjects. Women who were obese by 18 years old were more likely to report PCOS and infertility and less likely to have ever been pregnant, compared with women who became obese later in life. Future pregnancy was important to 30. 3% of women younger than 45 years, and overall to 51. 4%. Gosman et al, Fertil Steril, 2009
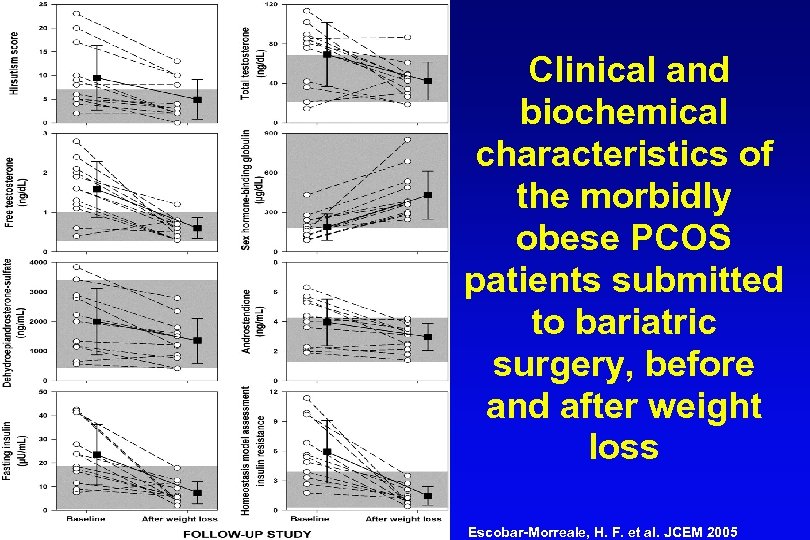 Clinical and biochemical characteristics of the morbidly obese PCOS patients submitted to bariatric surgery, before and after weight loss Escobar-Morreale, H. F. et al. JCEM 2005
Clinical and biochemical characteristics of the morbidly obese PCOS patients submitted to bariatric surgery, before and after weight loss Escobar-Morreale, H. F. et al. JCEM 2005
 Conclusion: Rates of many adverse maternal and neonatal outcomes may be lower in women who become pregnant after having had bariatric surgery compared with rates in pregnant women who are obese; however, further data are needed from rigorously designed studies.
Conclusion: Rates of many adverse maternal and neonatal outcomes may be lower in women who become pregnant after having had bariatric surgery compared with rates in pregnant women who are obese; however, further data are needed from rigorously designed studies.
 Can we achieve meaningful weight loss which will improve fertility outcomes? Only with bariatric surgery!
Can we achieve meaningful weight loss which will improve fertility outcomes? Only with bariatric surgery!
 Funding/Collaborators Supported by NIH grants, K 08 and K 24 grant, The National Cooperative Program for Infertility Research U 54 HD 34449, U 10 38992, Reproductive Medicine Network, 1 R 01 HD 056510 and A General Clinical Research Center grant MO 1 RR 10732 to Penn State Northwestern Andrea Dunaif, M. D. Virginia Commonwealth Jerry Strauss, M. D. , Ph. D. , John Nestler, M. D. University of Pennsylvania Christos Coutifaris, M. D. , Ph. D. Rich Spielman, Ph. D. Anuja Dokras, M. D. , Ph. D. Penn State Jan Mc. Allister, Ph. D. Larry Demers, Ph. D. Bill Dodson, M. D. Rich Zaino, M. D. Peter Lee, M. D. , Ph. D. Alex Vgontzas, M. D. Allen Kunselman Jami Ober Kelly Stamets Rawa Patsy Emily George Sandra Eyer RMN Principal Investigators
Funding/Collaborators Supported by NIH grants, K 08 and K 24 grant, The National Cooperative Program for Infertility Research U 54 HD 34449, U 10 38992, Reproductive Medicine Network, 1 R 01 HD 056510 and A General Clinical Research Center grant MO 1 RR 10732 to Penn State Northwestern Andrea Dunaif, M. D. Virginia Commonwealth Jerry Strauss, M. D. , Ph. D. , John Nestler, M. D. University of Pennsylvania Christos Coutifaris, M. D. , Ph. D. Rich Spielman, Ph. D. Anuja Dokras, M. D. , Ph. D. Penn State Jan Mc. Allister, Ph. D. Larry Demers, Ph. D. Bill Dodson, M. D. Rich Zaino, M. D. Peter Lee, M. D. , Ph. D. Alex Vgontzas, M. D. Allen Kunselman Jami Ober Kelly Stamets Rawa Patsy Emily George Sandra Eyer RMN Principal Investigators
 Reproductive Medicine Network PPCOS Investigators
Reproductive Medicine Network PPCOS Investigators
 OCP vs Weight Loss for Pregnancy in Polycystic Ovary Syndrome OWLPCOS
OCP vs Weight Loss for Pregnancy in Polycystic Ovary Syndrome OWLPCOS


