3e4c80f8dc98913edcb8634ba5943465.ppt
- Количество слайдов: 11

Latent TB surveillance in school Children and contact tracing in Matlosana, North West Province, South Africa Katlego Motlhaoleng Perinatal HIV Research Unit 01 October 2014 Research Day – North West Province

Background Matlosana Sub-district in North West Gold and platinum mining area, Four towns/townships Antenatal HIV prevalence in entire district – 37. 0% (SA Do. H 2010) TB burden in entire district 950/100 000 (HST ) TB leading cause of admission and death in Tshepong Hospital – ~90% TB cases Co-infected with HIV (E Variava personal communication ) No recent TB infection surveys outside of Western Cape

Objectives Q: Do children with demonstrable TB infection have an infectious case of TB in their house? To report prevalence of TB infection in 5 year olds and 7 year olds. Assess the proportion of households where a child with TB infection lives with a case of pulmonary TB To record a baseline TB infection prevalence ARVs Better diagnostics Better living conditions

Methods List of primary schools from Do. E and list of Creches from Local Gov Random selection of schools stratified by the four townships – basing numbers on the total number of creches or schools on the list per township Any child aged 5 years or 7 years old Consented by parents Quantiferon Gold in Tube Assay (QGIT)

Methods Children with Positive QGIT – Index TB Infection Referral to exclude active TB Intensified active case finding in contacts of the index children HH census Individually consent each HH member TB sputum for smear and MGIT on everyone able to produce HIV testing Po. C 2 -rapid algorithm or HIV ELISA – Orasure/blood Test CD 4 count for the HIV + Referral for TBs and for HIV with CD 4<350

Results Total 35 Primary Schools and 35 Crèches required 70 out of 95 Schools in the area Low acceptance of study initially Media reports on TB blood tests of no value Concerns that QGIT a disguised HIV test Communication challenges – principals, teachers, parents etc.
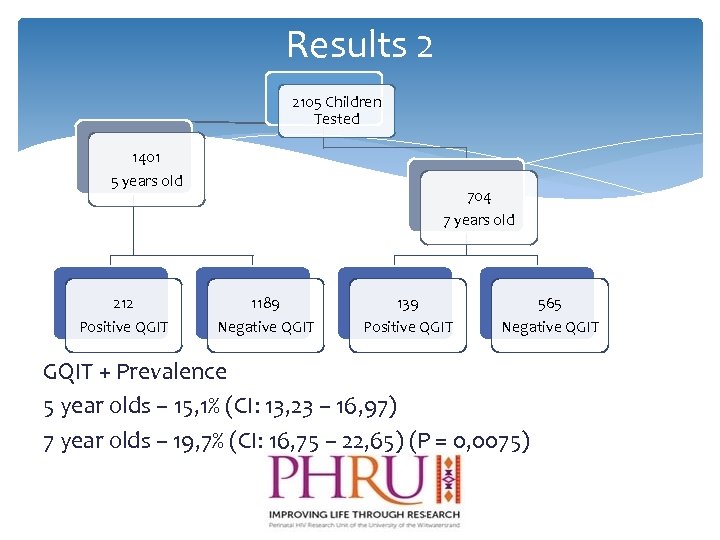
Results 2 2105 Children Tested 1401 5 years old 212 Positive QGIT 704 7 years old 1189 Negative QGIT 139 Positive QGIT 565 Negative QGIT GQIT + Prevalence 5 year olds – 15, 1% (CI: 13, 23 – 16, 97) 7 year olds – 19, 7% (CI: 16, 75 – 22, 65) (P = 0, 0075)

Household contacts Results TB 1215 household contacts screened for TB 7 (2, 4%) – active TB; 3 Newly diagnosed by study team Undetected TB rate 247/100 000 (95%CI: -33– 527) 7/292 Households had a case of active TB HIV 780 household contacts screened for HIV 144 HIV pos, 66 Newly diagnosed by study team 14 (9, 7%) CD 4 below 350, referred for treatment Undetected HIV rate – 5432/100 000 ( 95%CI: 4122 -6740) HIV /TB Co-infection All 3 cases co-infected

Summary Approx 2. 5% increase in TB infection per annum Intensified active case finding identified 247/100 000 cases of undiagnosed TB infection and 5432/100 000 HIV Far lower rate than we expected

Conclusions Children index cases not recommended for active case finding Low detection rate More research on TB genotypes to identify source of infection

Acknowledgements Neil Martinson Richard Chaisson Jonathan Golub Glenda Gray Limakatso Lebina Modiehi Rakgokong ICOHRTA E. Variava P. M. Abraham Tsepong Hospital PHRU Klerksdorp Research Team Do. H North West Do. E North West PEPFAR/USAID
3e4c80f8dc98913edcb8634ba5943465.ppt