joint anomalies.ppt
- Количество слайдов: 40
 JOINT ANOMALIES Jesh Talwar
JOINT ANOMALIES Jesh Talwar
![Hip joint anomalies Hip dysplasia, developmental dysplasia of the hip (DDH)[1] or congenital dysplasia Hip joint anomalies Hip dysplasia, developmental dysplasia of the hip (DDH)[1] or congenital dysplasia](https://present5.com/presentation/117303453_64198769/image-2.jpg) Hip joint anomalies Hip dysplasia, developmental dysplasia of the hip (DDH)[1] or congenital dysplasia of the hip (CDH)[2] is a congenital or acquired deformation or misalignment of the hip joint. Forms of the condition Types of misalignments of femur head to socket in hip dysplasia. A: Normal. B: Dysplasia. C: Subluxation. D: Luxa. Hip dysplasia can range from barely detectable to severely malformed / dislocated. The congenital form, teratologic or non-reducible dislocation occurs as part of more complex conditions. The condition can be bilateral or unilateral: If both hip joints are affected one speaks of "bilateral" dysplasia. In this case some diagnostic indicators like
Hip joint anomalies Hip dysplasia, developmental dysplasia of the hip (DDH)[1] or congenital dysplasia of the hip (CDH)[2] is a congenital or acquired deformation or misalignment of the hip joint. Forms of the condition Types of misalignments of femur head to socket in hip dysplasia. A: Normal. B: Dysplasia. C: Subluxation. D: Luxa. Hip dysplasia can range from barely detectable to severely malformed / dislocated. The congenital form, teratologic or non-reducible dislocation occurs as part of more complex conditions. The condition can be bilateral or unilateral: If both hip joints are affected one speaks of "bilateral" dysplasia. In this case some diagnostic indicators like
 Hip joint anomalies asymmetric folds and leg-length inequality do not apply. In unilateral dysplasia only one joint shows deformity, the contralateral side may show resulting effects. In 1979 Dr. John F. Crowe [10] et al. proposed a classification to define the degree of malformation and dislocation. Grouped from least severe Crowe I dysplasia to most severe Crowe IV. [11] This classification is very useful for studying treatment results. Rather than using the Wiberg angle because it makes it difficult to quantify the degree of dislocation they used 3 key elements to determine the degree of subluxation: A reference line at the lower rim of the "teardrop", junction between the femoral head and neck of the respective joint and the height of the pelvis (vertical measurement). They studied anteroposterior pelvic x-rays and drew horizontal lines through the lower rim of a feature called "teardrop". The distance between this line and the middle lines of the junction between femur head and neck gave them a measure of the degree of femur
Hip joint anomalies asymmetric folds and leg-length inequality do not apply. In unilateral dysplasia only one joint shows deformity, the contralateral side may show resulting effects. In 1979 Dr. John F. Crowe [10] et al. proposed a classification to define the degree of malformation and dislocation. Grouped from least severe Crowe I dysplasia to most severe Crowe IV. [11] This classification is very useful for studying treatment results. Rather than using the Wiberg angle because it makes it difficult to quantify the degree of dislocation they used 3 key elements to determine the degree of subluxation: A reference line at the lower rim of the "teardrop", junction between the femoral head and neck of the respective joint and the height of the pelvis (vertical measurement). They studied anteroposterior pelvic x-rays and drew horizontal lines through the lower rim of a feature called "teardrop". The distance between this line and the middle lines of the junction between femur head and neck gave them a measure of the degree of femur
 Hip joint anomalies If the joint is fully dislocated a false acetabulum often forms (often higher up on the pelvis) opposite the dislocated femoral head position. In actetabular dysplasia the acetabulum (socket) is too shallow or deformed. The center-edge angle is measured as described by Wiberg. [8] In coxa vara the femur head grows at too narrow an angle to the shaft, in coxa valga the angle is too wide. A rare type, the "Beukes familial hip dysplasia" is found among Afrikaners that are members of the Beukes family. The femur head is flat and irregular. Sufferers develop osteoarthritis at an early age.
Hip joint anomalies If the joint is fully dislocated a false acetabulum often forms (often higher up on the pelvis) opposite the dislocated femoral head position. In actetabular dysplasia the acetabulum (socket) is too shallow or deformed. The center-edge angle is measured as described by Wiberg. [8] In coxa vara the femur head grows at too narrow an angle to the shaft, in coxa valga the angle is too wide. A rare type, the "Beukes familial hip dysplasia" is found among Afrikaners that are members of the Beukes family. The femur head is flat and irregular. Sufferers develop osteoarthritis at an early age.
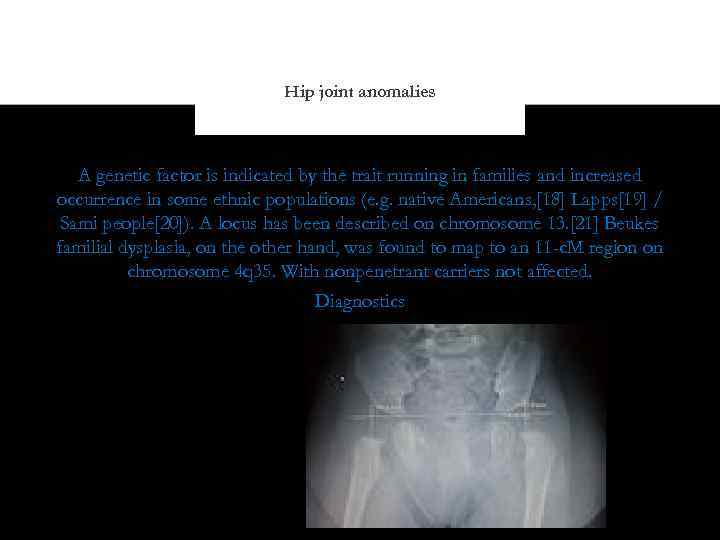 Hip joint anomalies A genetic factor is indicated by the trait running in families and increased occurrence in some ethnic populations (e. g. native Americans, [18] Lapps[19] / Sami people[20]). A locus has been described on chromosome 13. [21] Beukes familial dysplasia, on the other hand, was found to map to an 11 -c. M region on chromosome 4 q 35. With nonpenetrant carriers not affected. Diagnostics
Hip joint anomalies A genetic factor is indicated by the trait running in families and increased occurrence in some ethnic populations (e. g. native Americans, [18] Lapps[19] / Sami people[20]). A locus has been described on chromosome 13. [21] Beukes familial dysplasia, on the other hand, was found to map to an 11 -c. M region on chromosome 4 q 35. With nonpenetrant carriers not affected. Diagnostics
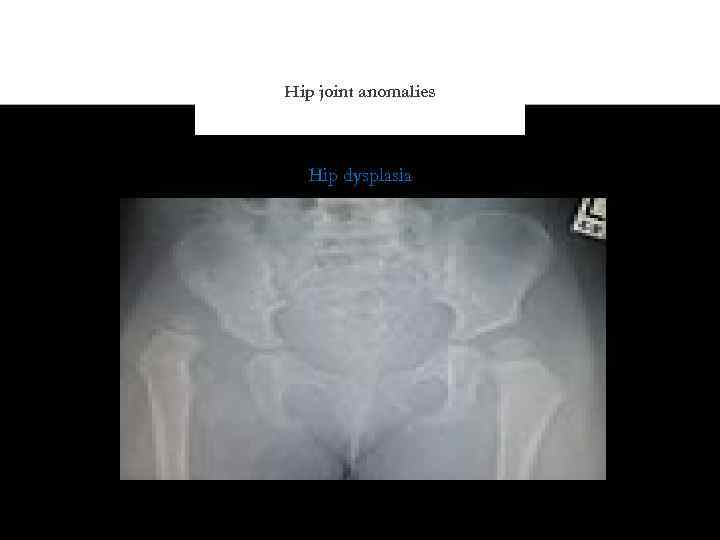 Hip joint anomalies Hip dysplasia
Hip joint anomalies Hip dysplasia
 Hip joint anomalies Surgery In older children the hip abductor and iliopsoas muscles have to be treated surgically because they adapt to the dislocated joint position (contracture). Braces and splints are often used following either of these methods to continue treatment. Although some children "outgrow" untreated mild hip dysplasia[5] and some forms of untreated dysplasia cause little or no impairment of quality of life, studies have as yet been unable to find a method of
Hip joint anomalies Surgery In older children the hip abductor and iliopsoas muscles have to be treated surgically because they adapt to the dislocated joint position (contracture). Braces and splints are often used following either of these methods to continue treatment. Although some children "outgrow" untreated mild hip dysplasia[5] and some forms of untreated dysplasia cause little or no impairment of quality of life, studies have as yet been unable to find a method of
 surgery Treatment requires orthopedic care, which consists initially of repeated cast applications, taping, or use of malleable splints to normalize the foot's position. If casting is not successful and the abnormality is severe, surgery may be required. Optimally, surgery is done before 12 mo, while the tarsal bones are still cartilaginous. Talipes equinovarus may recur as children grow.
surgery Treatment requires orthopedic care, which consists initially of repeated cast applications, taping, or use of malleable splints to normalize the foot's position. If casting is not successful and the abnormality is severe, surgery may be required. Optimally, surgery is done before 12 mo, while the tarsal bones are still cartilaginous. Talipes equinovarus may recur as children grow.
 Hip joint anomalies Crowe II Class Description Dislocation Femur and acetabulum show minimal abnormal development. Less than 50% dislocation The acetabulum shows abnormal development. 50% to 75% dislocation Crowe III The acetabula is developed without a roof. A false acetabulum develops opposite the dislocated femur head position. The joint is fully dislocated. 75% to 100% dislocation Crowe IV The acetabulum is insufficiently developed. Since the femur is positioned high up on the pelvis this class is also known as "high hip dislocation
Hip joint anomalies Crowe II Class Description Dislocation Femur and acetabulum show minimal abnormal development. Less than 50% dislocation The acetabulum shows abnormal development. 50% to 75% dislocation Crowe III The acetabula is developed without a roof. A false acetabulum develops opposite the dislocated femur head position. The joint is fully dislocated. 75% to 100% dislocation Crowe IV The acetabulum is insufficiently developed. Since the femur is positioned high up on the pelvis this class is also known as "high hip dislocation
 Talipes calcaneovalgus : The foot is flat or convex and dorsiflexed with the heel turned outward. The foot can easily be approximated against the lower tibia. Developmental dysplasia of the hip is more common among these children. Early treatment with a cast (to place the foot in the equinovarus position) or with corrective braces is usually successful
Talipes calcaneovalgus : The foot is flat or convex and dorsiflexed with the heel turned outward. The foot can easily be approximated against the lower tibia. Developmental dysplasia of the hip is more common among these children. Early treatment with a cast (to place the foot in the equinovarus position) or with corrective braces is usually successful
 Metatarsus adductus: : The forefoot turns toward the midline. The foot may be supinated at rest. Usually, the foot can be passively abducted and everted beyond the neutral position when the sole is stimulated. Occasionally, an affected foot is rigid, not correcting to neutral. Developmental dysplasia of the hip is more common among these children. The deformity usually resolves without treatment during the first year of life. If it does not, casting or surgery (abductory midfoot osteotomy) is required.
Metatarsus adductus: : The forefoot turns toward the midline. The foot may be supinated at rest. Usually, the foot can be passively abducted and everted beyond the neutral position when the sole is stimulated. Occasionally, an affected foot is rigid, not correcting to neutral. Developmental dysplasia of the hip is more common among these children. The deformity usually resolves without treatment during the first year of life. If it does not, casting or surgery (abductory midfoot osteotomy) is required.
 Metatarsus varus The plantar surface of the foot is turned inward, so that the arch is raised. This deformity usually results from in utero positioning. It typically does not resolve after birth and may require corrective casting.
Metatarsus varus The plantar surface of the foot is turned inward, so that the arch is raised. This deformity usually results from in utero positioning. It typically does not resolve after birth and may require corrective casting.
 Osteoarthritis (OA) also known as degenerative arthritis or degenerative joint disease or osteoarthrosis, is a group of mechanical abnormalities involving degradation of joints, including articular cartilage and subchondral bone. Symptoms may include joint pain, tenderness, stiffness, locking, and sometimes an effusion. A variety of causes—hereditary, developmental, metabolic, and mechanical—may initiate processes leading to loss of cartilage. When bone surfaces become less well protected by cartilage, bone may be exposed and damaged. As a result of decreased movement secondary to pain, regional muscles may atrophy, and ligaments may become more lax.
Osteoarthritis (OA) also known as degenerative arthritis or degenerative joint disease or osteoarthrosis, is a group of mechanical abnormalities involving degradation of joints, including articular cartilage and subchondral bone. Symptoms may include joint pain, tenderness, stiffness, locking, and sometimes an effusion. A variety of causes—hereditary, developmental, metabolic, and mechanical—may initiate processes leading to loss of cartilage. When bone surfaces become less well protected by cartilage, bone may be exposed and damaged. As a result of decreased movement secondary to pain, regional muscles may atrophy, and ligaments may become more lax.
 Classification Osteoarthritis can be classified into either primary or secondary depending on whether or not there is an identifiable underlying cause. Sign and symptom The main symptom is pain, causing loss of ability and often stiffness. "Pain" is generally described as a sharp ache, or a burning sensation in the associate muscles and tendons. OA can cause a crackling noise (called "crepitus") when the affected joint is moved or touched, and patients may experience muscle spasm and contractions in the tendons. Occasionally, the joints may also be filled with fluid. Humid and cold weather increases
Classification Osteoarthritis can be classified into either primary or secondary depending on whether or not there is an identifiable underlying cause. Sign and symptom The main symptom is pain, causing loss of ability and often stiffness. "Pain" is generally described as a sharp ache, or a burning sensation in the associate muscles and tendons. OA can cause a crackling noise (called "crepitus") when the affected joint is moved or touched, and patients may experience muscle spasm and contractions in the tendons. Occasionally, the joints may also be filled with fluid. Humid and cold weather increases
 Sign and symptom OA commonly affects the hands, feet, spine, and the large weight bearing joints, such as the hips and knees, although in theory, any joint in the body can be affected. As OA progresses, the affected joints appear larger, are stiff and painful, and usually feel better with gentle use. but worse with excessive or prolonged use, thus distinguishing it from rheumatoid arthritis.
Sign and symptom OA commonly affects the hands, feet, spine, and the large weight bearing joints, such as the hips and knees, although in theory, any joint in the body can be affected. As OA progresses, the affected joints appear larger, are stiff and painful, and usually feel better with gentle use. but worse with excessive or prolonged use, thus distinguishing it from rheumatoid arthritis.
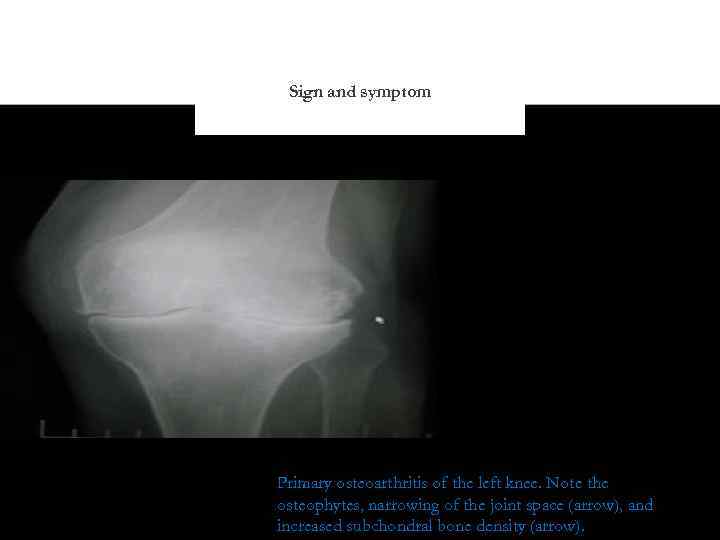 Sign and symptom Primary osteoarthritis of the left knee. Note the osteophytes, narrowing of the joint space (arrow), and increased subchondral bone density (arrow).
Sign and symptom Primary osteoarthritis of the left knee. Note the osteophytes, narrowing of the joint space (arrow), and increased subchondral bone density (arrow).
 treatment Treatment generally involves a combination of exercise, lifestyle modification, and analgesics. If pain becomes debilitating, joint replacement surgery may be used to improve the quality of life. OA is the most common form of arthritis, [2] and the leading cause of chronic disability in the United States. [3] It affects about 8 million people in the United Kingdom and nearly 27 million people in the United States.
treatment Treatment generally involves a combination of exercise, lifestyle modification, and analgesics. If pain becomes debilitating, joint replacement surgery may be used to improve the quality of life. OA is the most common form of arthritis, [2] and the leading cause of chronic disability in the United States. [3] It affects about 8 million people in the United Kingdom and nearly 27 million people in the United States.
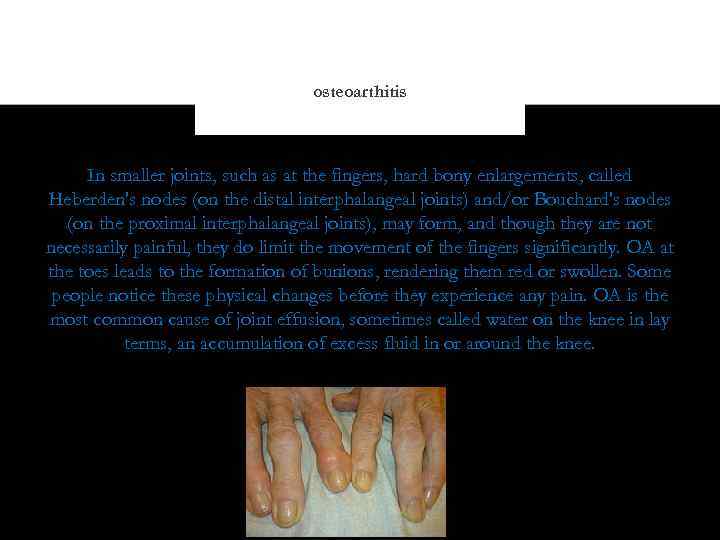 osteoarthitis In smaller joints, such as at the fingers, hard bony enlargements, called Heberden's nodes (on the distal interphalangeal joints) and/or Bouchard's nodes (on the proximal interphalangeal joints), may form, and though they are not necessarily painful, they do limit the movement of the fingers significantly. OA at the toes leads to the formation of bunions, rendering them red or swollen. Some people notice these physical changes before they experience any pain. OA is the most common cause of joint effusion, sometimes called water on the knee in lay terms, an accumulation of excess fluid in or around the knee.
osteoarthitis In smaller joints, such as at the fingers, hard bony enlargements, called Heberden's nodes (on the distal interphalangeal joints) and/or Bouchard's nodes (on the proximal interphalangeal joints), may form, and though they are not necessarily painful, they do limit the movement of the fingers significantly. OA at the toes leads to the formation of bunions, rendering them red or swollen. Some people notice these physical changes before they experience any pain. OA is the most common cause of joint effusion, sometimes called water on the knee in lay terms, an accumulation of excess fluid in or around the knee.
 Causes Some investigators believe that mechanical stress on joints underlies all osteoarthritis, with many and varied sources of mechanical stress, including misalignments of bones caused by congenital or pathogenic causes; mechanical injury; overweight; loss of strength in muscles supporting joints; and impairment of peripheral nerves, leading to sudden or uncoordinated movements that overstress joints. However exercise, including running in the absence of injury, has not been found to increase one's risk of developing osteoarthritis. Nor has cracking ones knuckles been found to play a role.
Causes Some investigators believe that mechanical stress on joints underlies all osteoarthritis, with many and varied sources of mechanical stress, including misalignments of bones caused by congenital or pathogenic causes; mechanical injury; overweight; loss of strength in muscles supporting joints; and impairment of peripheral nerves, leading to sudden or uncoordinated movements that overstress joints. However exercise, including running in the absence of injury, has not been found to increase one's risk of developing osteoarthritis. Nor has cracking ones knuckles been found to play a role.
 Surgery If the above management is ineffective, joint replacement surgery or resurfacing may be required in advanced cases. Arthroscopic surgical intervention for osteoarthritis of the knee however has been found to be no better than placebo at relieving symptoms.
Surgery If the above management is ineffective, joint replacement surgery or resurfacing may be required in advanced cases. Arthroscopic surgical intervention for osteoarthritis of the knee however has been found to be no better than placebo at relieving symptoms.
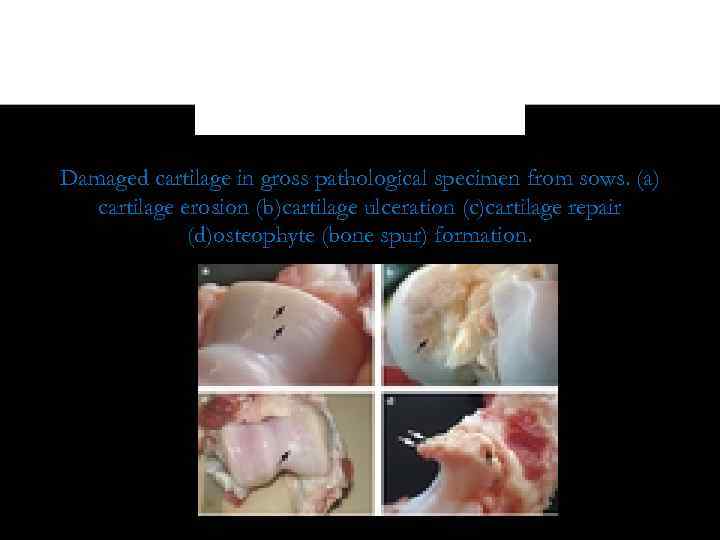 Damaged cartilage in gross pathological specimen from sows. (a) cartilage erosion (b)cartilage ulceration (c)cartilage repair (d)osteophyte (bone spur) formation.
Damaged cartilage in gross pathological specimen from sows. (a) cartilage erosion (b)cartilage ulceration (c)cartilage repair (d)osteophyte (bone spur) formation.
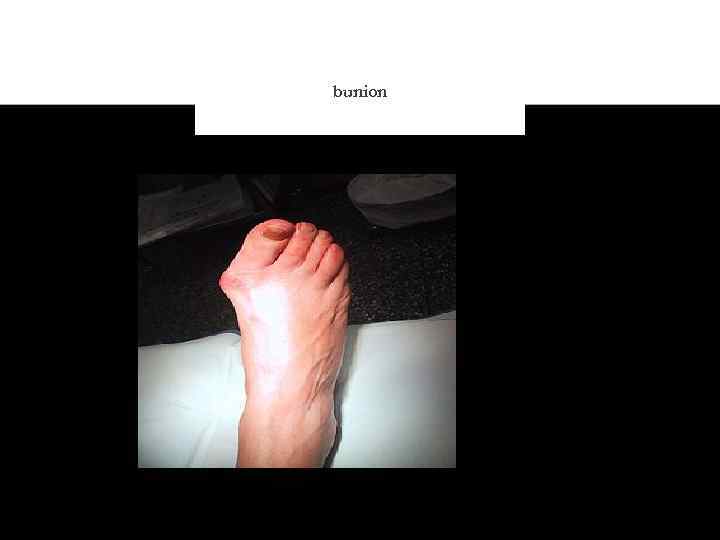
 bunion A bunion (hallux valgus) is a deformity characterized by lateral deviation of the great toe, often erroneously described as an enlargement of bone or tissue around the joint at the head of the big toe (metatarsophalangeal joint). As the great toe (hallux) turns in toward the second toe (angulation) the tissues surrounding the joint may become swollen and tender. The term is used to refer to the pathological bump on the side of the great toe joint. The bump is partly due to the swollen bursal sac and/or an osseous (bony) anomaly on the mesophalangeal joint (where the first metatarsal bone and hallux meet). The larger part of the bump is a normal part of the head of
bunion A bunion (hallux valgus) is a deformity characterized by lateral deviation of the great toe, often erroneously described as an enlargement of bone or tissue around the joint at the head of the big toe (metatarsophalangeal joint). As the great toe (hallux) turns in toward the second toe (angulation) the tissues surrounding the joint may become swollen and tender. The term is used to refer to the pathological bump on the side of the great toe joint. The bump is partly due to the swollen bursal sac and/or an osseous (bony) anomaly on the mesophalangeal joint (where the first metatarsal bone and hallux meet). The larger part of the bump is a normal part of the head of
 bunion
bunion
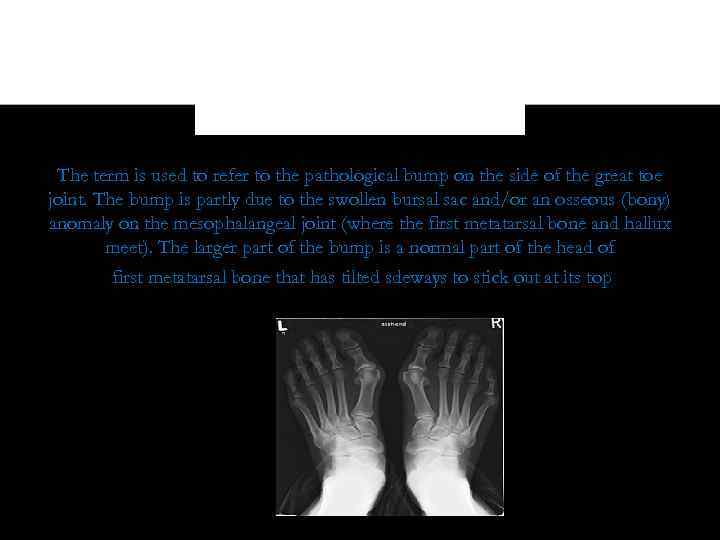 The term is used to refer to the pathological bump on the side of the great toe joint. The bump is partly due to the swollen bursal sac and/or an osseous (bony) anomaly on the mesophalangeal joint (where the first metatarsal bone and hallux meet). The larger part of the bump is a normal part of the head of first metatarsal bone that has tilted sdeways to stick out at its top
The term is used to refer to the pathological bump on the side of the great toe joint. The bump is partly due to the swollen bursal sac and/or an osseous (bony) anomaly on the mesophalangeal joint (where the first metatarsal bone and hallux meet). The larger part of the bump is a normal part of the head of first metatarsal bone that has tilted sdeways to stick out at its top
 Surgery A podiatrist performing surgery to remove the bony enlargement and restore normal alignment of the toe joint. Procedures are designed and chosen to correct a variety of pathologies that may be associated with the bunion. For instance, procedures may address some combination of:
Surgery A podiatrist performing surgery to remove the bony enlargement and restore normal alignment of the toe joint. Procedures are designed and chosen to correct a variety of pathologies that may be associated with the bunion. For instance, procedures may address some combination of:
 surgery removing the abnormal bony enlargement of the first metatarsal, realigning the first metatarsal bone relative to the adjacent metatarsal bone, straightening the great toe relative to the first metatarsal and adjacent toes, realigning the cartilagenous surfaces of the great toe joint, addressing arthritic changes associated with the great toe joint, repositioning the sesamoid bones beneath the first metatarsal bone, shortening, lengthening, raising, or lowering the first metatarsal bone, and correcting any abnormal bowing or misalignment within the great toe.
surgery removing the abnormal bony enlargement of the first metatarsal, realigning the first metatarsal bone relative to the adjacent metatarsal bone, straightening the great toe relative to the first metatarsal and adjacent toes, realigning the cartilagenous surfaces of the great toe joint, addressing arthritic changes associated with the great toe joint, repositioning the sesamoid bones beneath the first metatarsal bone, shortening, lengthening, raising, or lowering the first metatarsal bone, and correcting any abnormal bowing or misalignment within the great toe.
 surgery At present there are many different bunion surgeries for different effects. The age, health, lifestyle, and activity level of the patient may also play a role in the choice of procedure. Bunion surgery can be performed under local, spinal, or general anesthetic. The trend has moved strongly toward using the less invasive local anesthesia over the years. A patient can expect a 6 - to 8 -week recovery period during which crutches are usually required for aid in mobility. An orthopedic cast is much less common today as newer, more stable procedures and better forms of fixation (stabilizing the bone with screws and other hardware) are used. Hardware may even include absorbable pins that perform their function and then broken down by the body over the course of months.
surgery At present there are many different bunion surgeries for different effects. The age, health, lifestyle, and activity level of the patient may also play a role in the choice of procedure. Bunion surgery can be performed under local, spinal, or general anesthetic. The trend has moved strongly toward using the less invasive local anesthesia over the years. A patient can expect a 6 - to 8 -week recovery period during which crutches are usually required for aid in mobility. An orthopedic cast is much less common today as newer, more stable procedures and better forms of fixation (stabilizing the bone with screws and other hardware) are used. Hardware may even include absorbable pins that perform their function and then broken down by the body over the course of months.
 Temporomandibular joint disorder, TMJD (in the medical literature TMD), or TMJ syndrome, is an umbrella term covering acute or chronic pain, especially in the muscles of mastication and/or inflammation of the temporomandibular joint, which connects the mandible to the skull. The primary cause is muscular hyperor parafunction, as in the case of bruxism, with secondary effects on the oral musculoskeletal system, like various types of displacment of the disc in the temporomandibular joint. The disorder and resultant dysfunction can result in significant pain, which is the most common TMD symptom, combined with impairment of function. Because the disorder transcends the boundaries between several health-care disciplines — in particular, dentistry and neurology — there a variety of treatment approaches. The temporomandibular joint is susceptible to many of the conditions that affect other joints in the body, including ankylosis, arthritis, trauma, dislocations, developmental anomalies, neoplasia and reactive lesions.
Temporomandibular joint disorder, TMJD (in the medical literature TMD), or TMJ syndrome, is an umbrella term covering acute or chronic pain, especially in the muscles of mastication and/or inflammation of the temporomandibular joint, which connects the mandible to the skull. The primary cause is muscular hyperor parafunction, as in the case of bruxism, with secondary effects on the oral musculoskeletal system, like various types of displacment of the disc in the temporomandibular joint. The disorder and resultant dysfunction can result in significant pain, which is the most common TMD symptom, combined with impairment of function. Because the disorder transcends the boundaries between several health-care disciplines — in particular, dentistry and neurology — there a variety of treatment approaches. The temporomandibular joint is susceptible to many of the conditions that affect other joints in the body, including ankylosis, arthritis, trauma, dislocations, developmental anomalies, neoplasia and reactive lesions.
 Signs and symptoms of temporomandibular joint disorder vary in their presentation and can be very complex, but are often simple. On average the symptoms will involve more than one of the numerous TMJ components: muscles, nerves, tendons, ligaments, bones, connective tissue, and the teeth. [6] Ear pain associated with the swelling of proximal tissue is a symptom of temporomandibular joint disorder. Symptoms associated with TMJ disorders may be: Biting or chewing difficulty or discomfort Clicking, popping, or grating sound when opening or closing the mouth Dull, aching pain in the face Earache (particularly in the morning) Headache (particularly in the morning) Hearing loss Migraine (particularly in the morning) Jaw pain or tenderness of the jaw Reduced ability to open or close the mouth Tinnitus Neck and shoulder pain Dizziness
Signs and symptoms of temporomandibular joint disorder vary in their presentation and can be very complex, but are often simple. On average the symptoms will involve more than one of the numerous TMJ components: muscles, nerves, tendons, ligaments, bones, connective tissue, and the teeth. [6] Ear pain associated with the swelling of proximal tissue is a symptom of temporomandibular joint disorder. Symptoms associated with TMJ disorders may be: Biting or chewing difficulty or discomfort Clicking, popping, or grating sound when opening or closing the mouth Dull, aching pain in the face Earache (particularly in the morning) Headache (particularly in the morning) Hearing loss Migraine (particularly in the morning) Jaw pain or tenderness of the jaw Reduced ability to open or close the mouth Tinnitus Neck and shoulder pain Dizziness
 Treatment Restoration of the occlusal surfaces of the teeth If the occlusal surfaces of the teeth or the supporting structures have been altered due to inappropriate dental treatment, periodontal disease, or trauma, the proper occlusion may need to be restored. [citation needed] Patients with bridges, crowns, or onlays should be checked for bite discrepancies. These discrepancies, if present, may cause a person to make contact with posterior teeth during sideways chewing motions. These inappropriate contacts are called interferences, and if present, they can cause a patient to subconsciously avoid those motions, as they will provoke a painful response. The result can be excessive strain or even spasms of the chewing muscles. Treatment could include adjusting the restorations or replacing them. (Christensen 1997, A Consumer's Guide to Dentistry).
Treatment Restoration of the occlusal surfaces of the teeth If the occlusal surfaces of the teeth or the supporting structures have been altered due to inappropriate dental treatment, periodontal disease, or trauma, the proper occlusion may need to be restored. [citation needed] Patients with bridges, crowns, or onlays should be checked for bite discrepancies. These discrepancies, if present, may cause a person to make contact with posterior teeth during sideways chewing motions. These inappropriate contacts are called interferences, and if present, they can cause a patient to subconsciously avoid those motions, as they will provoke a painful response. The result can be excessive strain or even spasms of the chewing muscles. Treatment could include adjusting the restorations or replacing them. (Christensen 1997, A Consumer's Guide to Dentistry).
 Intra-aural (ear) device Intra-aural (aural meaning having to do with the ear) device therapy treats TMJ disorder using an appliance worn in the ear canal. The ear canal is in immediate anatomical proximity to the temporomandibular joint (TMJ). "The Clayton Intra. Aural Device (CID) is a hollow, plastic, patented device which rests in the outer third of the ear canal when the jaw is slightly opened. "[20] A randomized controlled clinical trial showed the CID to be a non-invasive, safe and effective therapy for the treatment of temporomandibular joint disorder. [21] Based on data submitted to the FDA the CID was given an indication for use "as an aid in reducing temporomandibular disorder (TMD) pain". [22] The CID is sold under the tradename TMDes (ear system).
Intra-aural (ear) device Intra-aural (aural meaning having to do with the ear) device therapy treats TMJ disorder using an appliance worn in the ear canal. The ear canal is in immediate anatomical proximity to the temporomandibular joint (TMJ). "The Clayton Intra. Aural Device (CID) is a hollow, plastic, patented device which rests in the outer third of the ear canal when the jaw is slightly opened. "[20] A randomized controlled clinical trial showed the CID to be a non-invasive, safe and effective therapy for the treatment of temporomandibular joint disorder. [21] Based on data submitted to the FDA the CID was given an indication for use "as an aid in reducing temporomandibular disorder (TMD) pain". [22] The CID is sold under the tradename TMDes (ear system).
 Splint Occlusal splints (also called night guards or mouth guards) reduce nighttime clenching in some patients, while increasing clenching activity in other patients. [citation needed] Thus, while occlusal splints do prevent loss of tooth enamel from grinding, use of a splint can worsen TMJ disorder symptoms for some people Nighttime biofeedback Nighttime EMG biofeedback (for instance by using a biofeedback headband or biofeedback device) can be used to reduce bruxism and thus reduce or eliminate the ongoing nightly cycle of damage that contributes to the majority of TMJ disorder symptoms. This treatment is non-invasive. The Bruxism Association warns that such devices can disrupt sleep and it does not consider them to be a safe treatment
Splint Occlusal splints (also called night guards or mouth guards) reduce nighttime clenching in some patients, while increasing clenching activity in other patients. [citation needed] Thus, while occlusal splints do prevent loss of tooth enamel from grinding, use of a splint can worsen TMJ disorder symptoms for some people Nighttime biofeedback Nighttime EMG biofeedback (for instance by using a biofeedback headband or biofeedback device) can be used to reduce bruxism and thus reduce or eliminate the ongoing nightly cycle of damage that contributes to the majority of TMJ disorder symptoms. This treatment is non-invasive. The Bruxism Association warns that such devices can disrupt sleep and it does not consider them to be a safe treatment
 Pain relief While conventional analgesic pain killers such as paracetamol (acetaminophen) or NSAIDs provide initial relief for some sufferers, the pain is often more neurologic in nature, which often does not respond well to these drugs. [24] An alternative approach is for pain modification, for which off-label use of lowdoses of Tricyclic antidepressant that have anti-muscarinic properties (e. g. Amitriptyline or the less sedative Nortriptyline) generally prove more effective. [25][26] In TMJD the muscles are unbalanced. Biofeedback using EMG is successful in balancing these muscles. A mirror can be used as a biofeedback device: Draw a vertical line on mirror. Relax the jaw by relaxing as you exhale. See the jaw relax in the midline. Practice the breathing and relaxing daily using the mirror. When the jaw does open midline the symptoms should abate
Pain relief While conventional analgesic pain killers such as paracetamol (acetaminophen) or NSAIDs provide initial relief for some sufferers, the pain is often more neurologic in nature, which often does not respond well to these drugs. [24] An alternative approach is for pain modification, for which off-label use of lowdoses of Tricyclic antidepressant that have anti-muscarinic properties (e. g. Amitriptyline or the less sedative Nortriptyline) generally prove more effective. [25][26] In TMJD the muscles are unbalanced. Biofeedback using EMG is successful in balancing these muscles. A mirror can be used as a biofeedback device: Draw a vertical line on mirror. Relax the jaw by relaxing as you exhale. See the jaw relax in the midline. Practice the breathing and relaxing daily using the mirror. When the jaw does open midline the symptoms should abate
 Prolotherapy There is on-going study of prolotherapy as a treatment option. A preliminary report claims "prolotherapy with 10% dextrose appears promising for the treatment of symptomatic TMJ hypermobility. "
Prolotherapy There is on-going study of prolotherapy as a treatment option. A preliminary report claims "prolotherapy with 10% dextrose appears promising for the treatment of symptomatic TMJ hypermobility. "
 Congenital Glenoid Hypoplasia This malformation is due to failure of formation of the lower and upper glenoid epiphysis. It is characterized in the radiogram by flattening, shallowness, and a denate appeareance of the glenoid cavity. The lower aspect of the clavicle may be hypertrophied into a bony prominence, and there may be spina bifida in the cervical region. Often, the abnormality is bilateral and is encountered as an isolated malformation. It may be hereditary. Samilson reported congenital glenoid hypoplasia in three successive generations of the same family.
Congenital Glenoid Hypoplasia This malformation is due to failure of formation of the lower and upper glenoid epiphysis. It is characterized in the radiogram by flattening, shallowness, and a denate appeareance of the glenoid cavity. The lower aspect of the clavicle may be hypertrophied into a bony prominence, and there may be spina bifida in the cervical region. Often, the abnormality is bilateral and is encountered as an isolated malformation. It may be hereditary. Samilson reported congenital glenoid hypoplasia in three successive generations of the same family.
 Occasionally, it is seen in association with other congenital malformations such as Apert’s syndrome, Hurler’s syndrome, aglossia-adactylia, oculodento-osseous dysplasia, Holt-Oram syndrome, and Cornelia De Lange’s syndrome. Clinically, in the young child the anomaly is usually asymptomatic and may be found incidentally in the radiogram. In the older patients, however, the glenohumeral joint may be unstable and may become dislocated posteriorly. The range of abduction of the shoulder will be restricted, and occasionally it may cause neurovascular embarrassment. In the differential diagnosis, one should consider glenoid hypoplasia secondary to obstetrical brachial plexus palsy or multiple epiphyseal dysplsia.
Occasionally, it is seen in association with other congenital malformations such as Apert’s syndrome, Hurler’s syndrome, aglossia-adactylia, oculodento-osseous dysplasia, Holt-Oram syndrome, and Cornelia De Lange’s syndrome. Clinically, in the young child the anomaly is usually asymptomatic and may be found incidentally in the radiogram. In the older patients, however, the glenohumeral joint may be unstable and may become dislocated posteriorly. The range of abduction of the shoulder will be restricted, and occasionally it may cause neurovascular embarrassment. In the differential diagnosis, one should consider glenoid hypoplasia secondary to obstetrical brachial plexus palsy or multiple epiphyseal dysplsia.
 treatment Management should be individualized. Often no treatment is indicated. In symptomatic posterior dislocation of the shoulder, glenoidplasty with a bone graft may help. Aplasia of Scapula Congenital absence of the scapula is extremely rare. It is usually associated with ipsilateral Amelia. Treatment consists of fitting with an upper limb prosthesis.
treatment Management should be individualized. Often no treatment is indicated. In symptomatic posterior dislocation of the shoulder, glenoidplasty with a bone graft may help. Aplasia of Scapula Congenital absence of the scapula is extremely rare. It is usually associated with ipsilateral Amelia. Treatment consists of fitting with an upper limb prosthesis.
 Torsional Deformity of Glenoid Cavity This deformity will cause posterior or anterior dislocation of the shoulder and can be demonstrated on an axillary radiogram or a computed tomographic torsion study of the glenoid cavity. Treatment consists of osteotomy of the neck of the scapula and insertion of a wedge bone graft to correct the abnormal glenoid torsion.
Torsional Deformity of Glenoid Cavity This deformity will cause posterior or anterior dislocation of the shoulder and can be demonstrated on an axillary radiogram or a computed tomographic torsion study of the glenoid cavity. Treatment consists of osteotomy of the neck of the scapula and insertion of a wedge bone graft to correct the abnormal glenoid torsion.
 Congenital Varus Deformity of Proximal Humerus This malformation may be developmental or secondary to neurofibromatosis or rachitic syndromes.
Congenital Varus Deformity of Proximal Humerus This malformation may be developmental or secondary to neurofibromatosis or rachitic syndromes.
 Torsional Deformity of Humeral Neck Excessive retroversion will cause posterior dislocation of the glenohumeral joint, and excessive anteversion will cause anterior dislocation. Computed axial tomography will show the degree of humeral torsion. When torsion deformity is severe and is causing shoulder joint instability, it is treated by derotation osteotomy.
Torsional Deformity of Humeral Neck Excessive retroversion will cause posterior dislocation of the glenohumeral joint, and excessive anteversion will cause anterior dislocation. Computed axial tomography will show the degree of humeral torsion. When torsion deformity is severe and is causing shoulder joint instability, it is treated by derotation osteotomy.


