ecde607cd9ef97aaea187475d816e4c4.ppt
- Количество слайдов: 76

ISCHEMIC STROKE, THROMBOLYSIS & TIA Mark Keezer R 3 Neurology August 26 th 2009 Cigarettes and Chocolate Milk

Objectives 1. 2. 3. 4. Background review of stroke Approach to acute ischemic stroke Thrombolysis in acute stroke General management of acute stroke Craniectomy BP 5. for malignant MCA control Approach to TIA.

Synonyms Abound Stroke is currently the most preferred term Cerebrovascular accident (CVA ) Apoplexy (Gr. Being struck down, to suffer a seizure).

Drowning in a Sea of Strokes Dr. Charles Miller Fisher House officers and students learn neurology “stroke by stroke” >50% of neurological admissions 50, 000 new /year in Canada 3 rd most important cause of death after heart disease and cancer Most important cause of adult disability 30% of survivors require daily assistance.

Stroke Definition Acute Focal Neurologic syndrome Secondary to vascular pathology (ie cerebrovascular disease) Exclusions include local pressure effects of aneurysms, vascular headache, CNS vasculitis, elevated ICP. . . Adams et al. Guidelines for the early management of adults with ischemic stroke. A guideline from the AHA/ASA stroke council… Stroke 2007; 38: 1655 -1711.
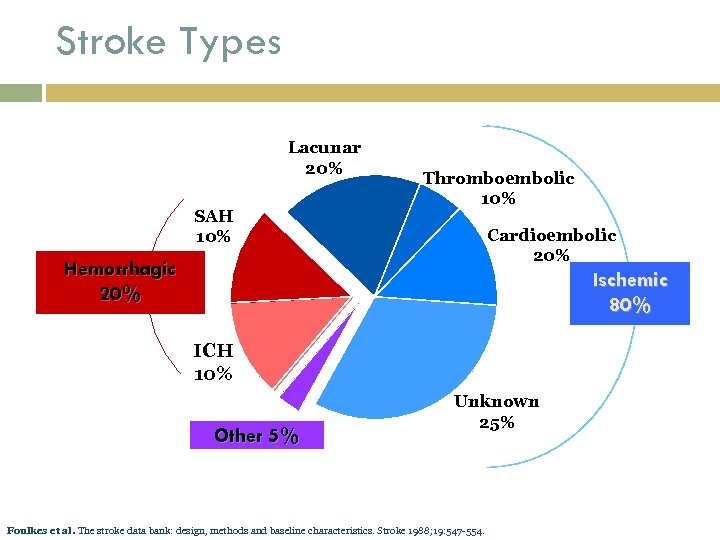
Stroke Types Lacunar 20% SAH 10% Thromboembolic 10% Cardioembolic 20% Hemorrhagic 20% Ischemic 80% ICH 10% Other 5% Unknown 25% Foulkes et al. The stroke data bank: design, methods and baseline characteristics. Stroke 1988; 19: 547 -554.

Risk Factors 1/3 Non-modifiable Age Male gender Ethnicity: African or Asian origin Family history Stroke in first degree relative Genetics MELAS, CADASIL Fabry’s disease Ehler’s Danlos type IV Pseudoxanthoma elasticum Dyslipidemias Vasculopathies Cardiomyopathies.

Risk Factors 2/3 Modifiable : HTN – 4 x DM – 2 x (4 x with HTN) Smoking – 2 x Hyperlipidemia – 1. 5 x CAD Stroke , TIA , stenosis Drugs (cocaine, amphetamines, heroin, Et. OH) A fib – 5 -6 x.
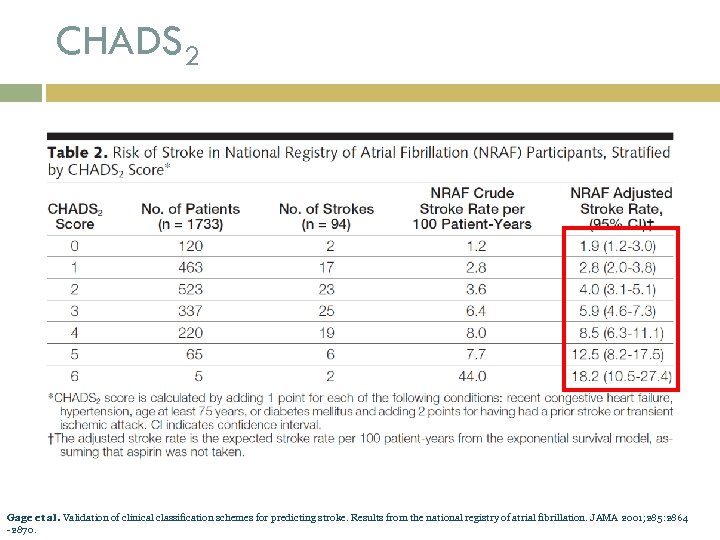
CHADS 2 Gage et al. Validation of clinical classification schemes for predicting stroke. Results from the national registry of atrial fibrillation. JAMA 2001; 285: 2864 -2870.

Risk Factors 3/3 Others: Thrombophilia APL antibodies (lupus anticoagulant, anticardiolipin antibodies) Homocysteine OCP.

Pathophysiology The brain is very metabolically active tissue Normal CBF > 55 ml/min/100 g 15 -20% of cardiac output CBF <23 ml/min/100 g: critical level for impairment of function CBF <10 -12 ml/min/100 g: infarction regardless of duration Complete arrest of flow: 15 sec: suppression of electric activity 2 -4 min: inhibition of synaptic excitability 4 -6 min: inhibition of electric excitability.
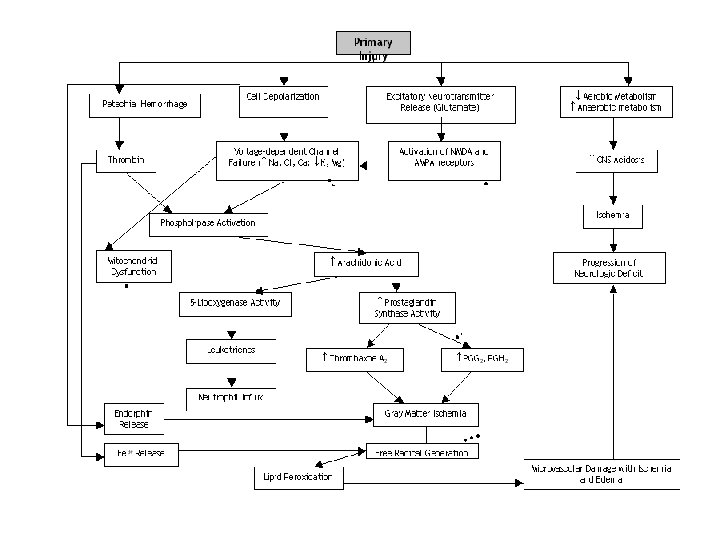

Stroke Syndromes 1/2 ACA MCA (Ant choroidal, Gerstmann) PCA (Alexia without agraphia, Balint, Dejerine-Roussy, Anton) Lacunar (PM, PS, SM, AH, CD and 200 more).

Stroke Syndromes 2/2 Brain stem syndromes Midbrain Pons Weber = PCA = ipsi 3 rd, contra plegia Claude = PCA = contra rubral tremor Benedikt = PCA = ipsi 3 rd, contra plegia and rubral tremor Marie-Foix Syndrome = long circumferential = ipsi ataxia, contra plegia & ST Raymond Syndrome = paramedian branches = ipsi 6 th, contra plegia Millard-Gubler Syndrome (aka Foville) = paramedian branches = ipsi 6 th& 7 th contra plegia Medulla Dejerine = vertebral = ipsi 12 th, contra plegia and ML Wallenberg = PICA > vertebral = ipsi 5 th, 8 th, 9 & 10 th, Horner’s and ataxia; contra ST + singultus.

“Code Stroke!” Now what?

ER Evaluation 1/2 Immediate response! ABC and G (glucose) Concise but pertinent history: WHEN WAS THE PATIENT LAST (& DEFINITELY) SEEN NORMAL ? Resetting the clock? Atypical features H/A, NECK PAIN, SZ Any improvement.

Beware of Mimics! Adams et al. Guidelines for the early management of adults with ischemic stroke. A guideline from the AHA/ASA stroke council… Stroke 2007; 38: 1655 -1711.

ER Evaluation 2/2 Pertinent PMHx Risk factors Dr Minuk’s “ 5 Horseman of the Apocalypse” Recent MI, trauma, surgery, migraines, epilepsy or pregnancy Pertinent Medx Anticoagulants Antiplatelets Antihypertensives Hypoglycemics / insulin. Albrecht Dürer, Four Horsemen of the Apocalypse, 1498.

Φ Vitals (including glucose) Dr Côté checks the BP in both arms Pulse(s) Cardiac murmurs or carotid bruits.

NINDS Stroke Scale
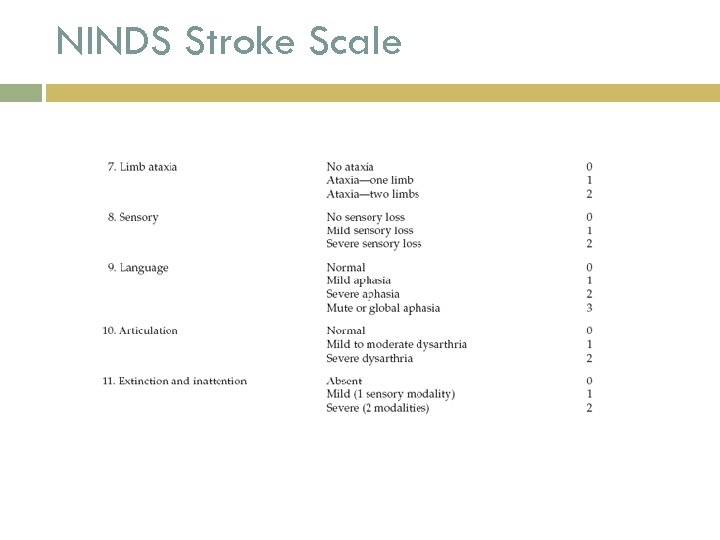

NINDS Stroke Scale

Requisite Initial Interventions Would this pt benefit from IV NS? Dr Wein doesn’t hesitate to give 120 cc/hr Consider a NS Bolus if hypotensive Maintain fi. O 2 ≥ 92%.

Requisite Initial Investigations CBC INR SMA 7 (incl glucose) EKG, troponin +/- CXR (very modest value and can the pt afford the delay? ) Selected patients: toxicology, b-HCG. Adams et al. Guidelines for the early management of adults with ischemic stroke. A guideline from the AHA/ASA stroke council… Stroke 2007; 38: 1655 -1711.
Neuro-imaging in Acute Stroke

Immediate Goal Exclude hemorrhage Exclude mass lesions Assess location & degree of brain injury +/- CTA protocol to identify occluded vessel.

First Step CT scan: Non-contrast Goal is door-to-CT in 25 mins Subtle Loss signs (82% of large vessel occlusions within 6 hrs) of gray-white matter differentiation Sulcal effacement Obscuration of basal ganglia, insula MCA sign (M 1 branch), dot sign (M 2/M 3 branch) Parenchymal hypodensity.
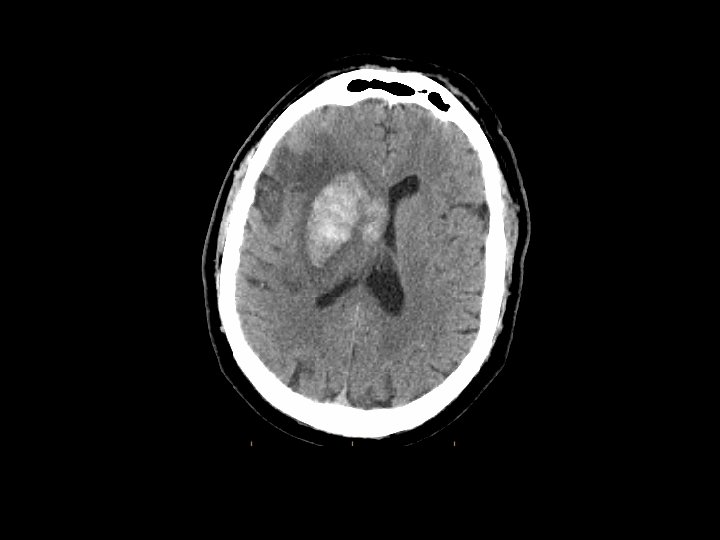
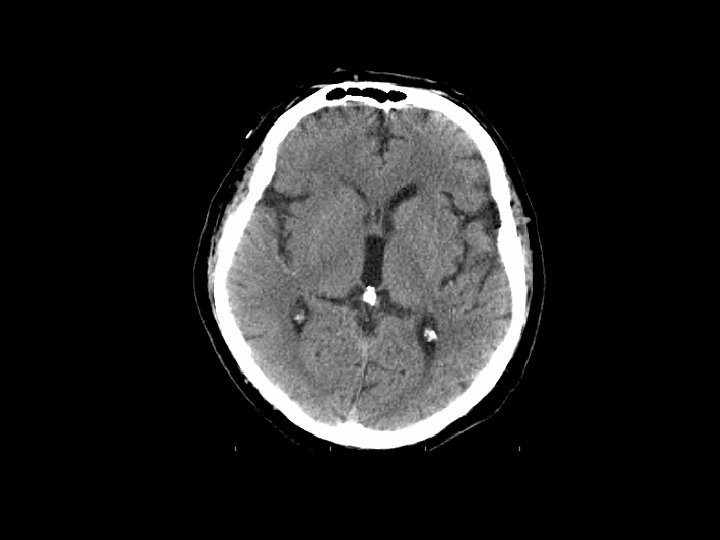
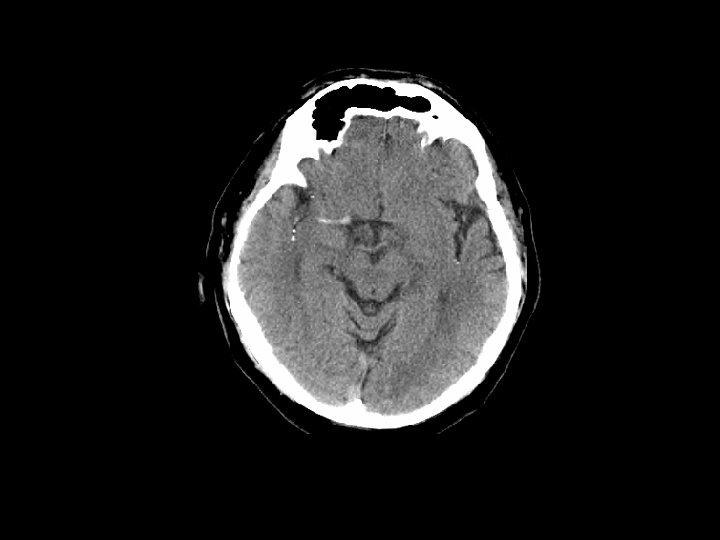
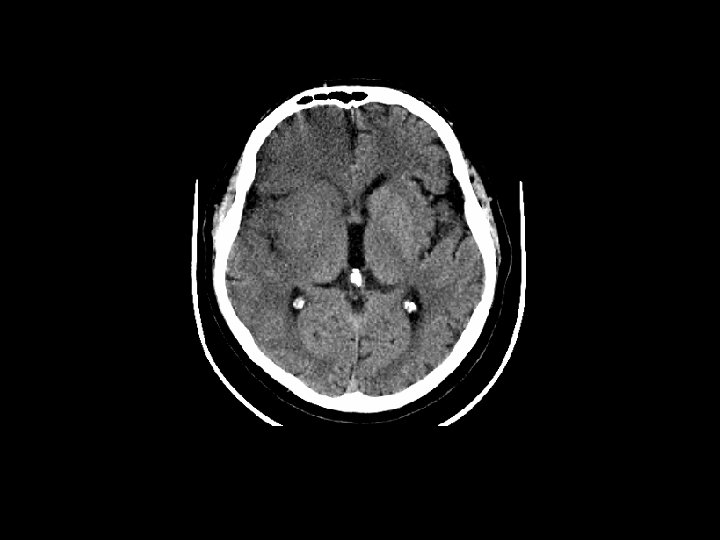
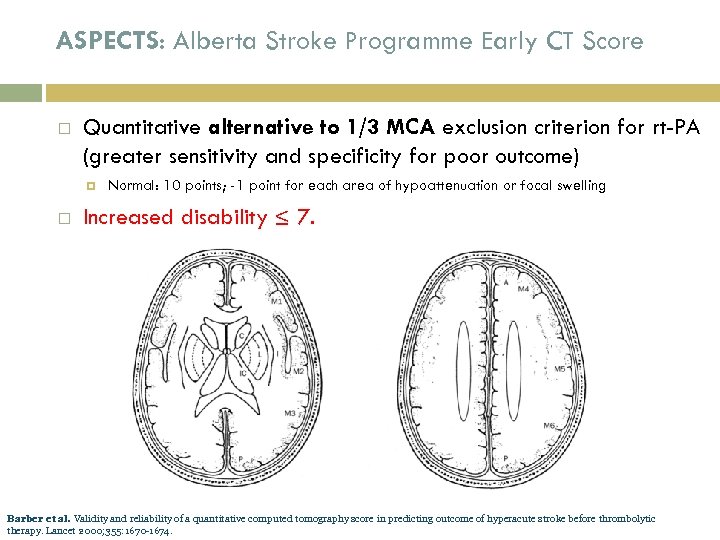
ASPECTS: Alberta Stroke Programme Early CT Score Quantitative alternative to 1/3 MCA exclusion criterion for rt-PA (greater sensitivity and specificity for poor outcome) Normal: 10 points; -1 point for each area of hypoattenuation or focal swelling Increased disability ≤ 7. Barber et al. Validity and reliability of a quantitative computed tomography score in predicting outcome of hyperacute stroke before thrombolytic therapy. Lancet 2000; 355: 1670 -1674.

Thrombolysis!

Indications for rt-PA Intravenous may be given within 4. 5 hours of symptom onset Intra-arterial may be given within 6 hours under the care of a stroke neurologist Intra-arterial may be given within 24 hours (or more? ) for catastrophic posterior fossa event AHA guidelines Do not wait for platelets or INR unless you suspect a possible bleeding diathesis. Adams et al. Guidelines for the early management of adults with ischemic stroke. A guideline from the AHA/ASA stroke council… Stroke 2007; 38: 1655 -1711.

AHA Guideline Criteria 1/2 Adams et al. Guidelines for the early management of adults with ischemic stroke. A guideline from the AHA/ASA stroke council… Stroke 2007; 38: 1655 -1711.

AHA Guideline Criteria 2/2 Adams et al. Guidelines for the early management of adults with ischemic stroke. A guideline from the AHA/ASA stroke council… Stroke 2007; 38: 1655 -1711.
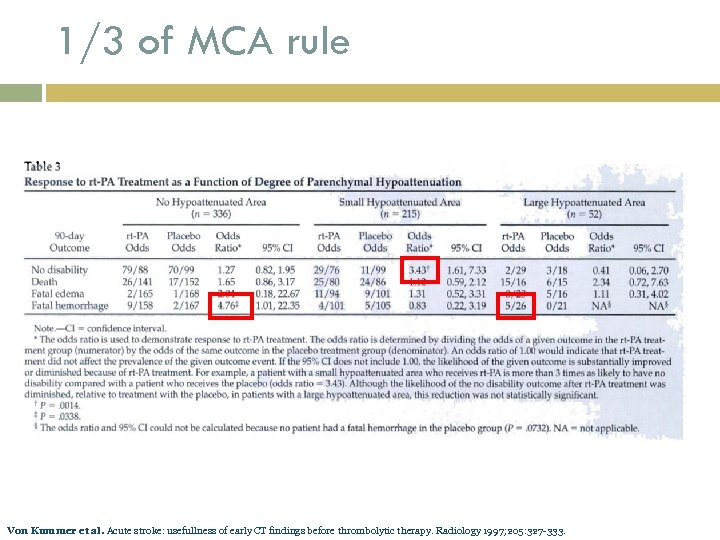
1/3 of MCA rule Von Kummer et al. Acute stroke: usefullness of early CT findings before thrombolytic therapy. Radiology 1997; 205: 327 -333.
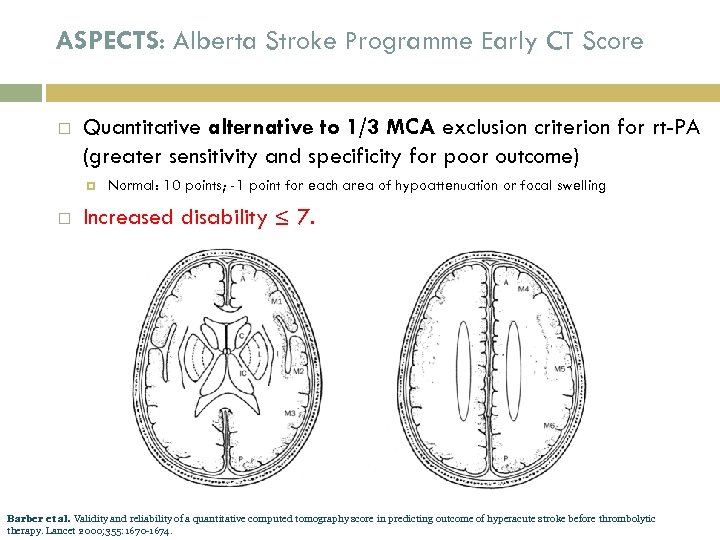
ASPECTS: Alberta Stroke Programme Early CT Score Quantitative alternative to 1/3 MCA exclusion criterion for rt-PA (greater sensitivity and specificity for poor outcome) Normal: 10 points; -1 point for each area of hypoattenuation or focal swelling Increased disability ≤ 7. Barber et al. Validity and reliability of a quantitative computed tomography score in predicting outcome of hyperacute stroke before thrombolytic therapy. Lancet 2000; 355: 1670 -1674.
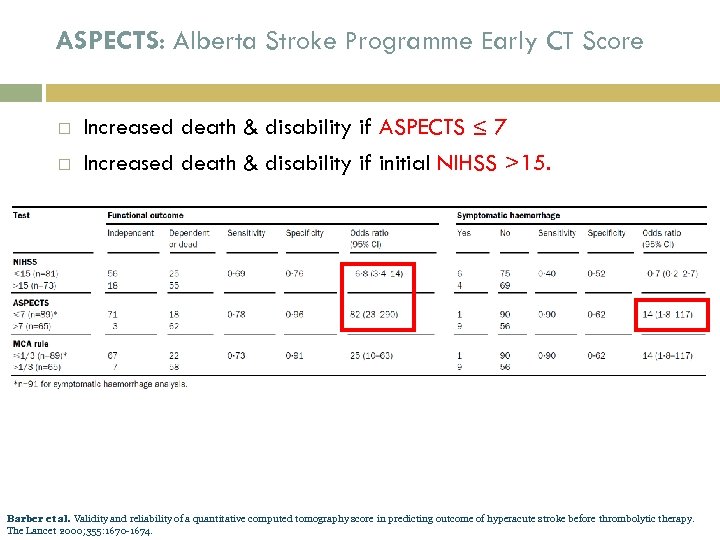
ASPECTS: Alberta Stroke Programme Early CT Score Increased death & disability if ASPECTS ≤ 7 Increased death & disability if initial NIHSS >15. Barber et al. Validity and reliability of a quantitative computed tomography score in predicting outcome of hyperacute stroke before thrombolytic therapy. The Lancet 2000; 355: 1670 -1674.

NINDS rt-PA Stroke Study Group Randomized, double-blind, placebo controlled trial Included only patients within 3 h Permuted block randomization Half within 90 minutes Half between 90 -180 minutes Strict exclusion criteria No stroke severity criteria No ischemic size criteria No myocardial infarction criteria. NINDS rt-PA Stroke Study Group. Tissue plasminogen activator for acute ischemic stroke. NEJM 1995; 333: 1581 -1587.

NINDS rt-PA Stroke Study Group 2 parts Part 1: early improvement 291 pts randomized to rt-PA or placebo Looked at NIHSS improvement ≥ 4 pts at 24 h Part 2 : delayed improvement 333 pts randomized to rt-PA or placebo Primary outcome: pts with minimal or no deficits at 3 months 95 or 100 on Barthel index ≤ 1 on NIHSS ≤ 1 on m. RS 1 on Glasgow outcome scale. NINDS rt-PA Stroke Study Group. Tissue plasminogen activator for acute ischemic stroke. NEJM 1995; 333: 1581 -1587.

NINDS rt-PA Stroke Study Group 12% absolute risk reduction at 3 months NNT = 8 NINDS rt-PA Stroke Study Group. Tissue plasminogen activator for acute ischemic stroke. NEJM 1995; 333: 1581 -1587.
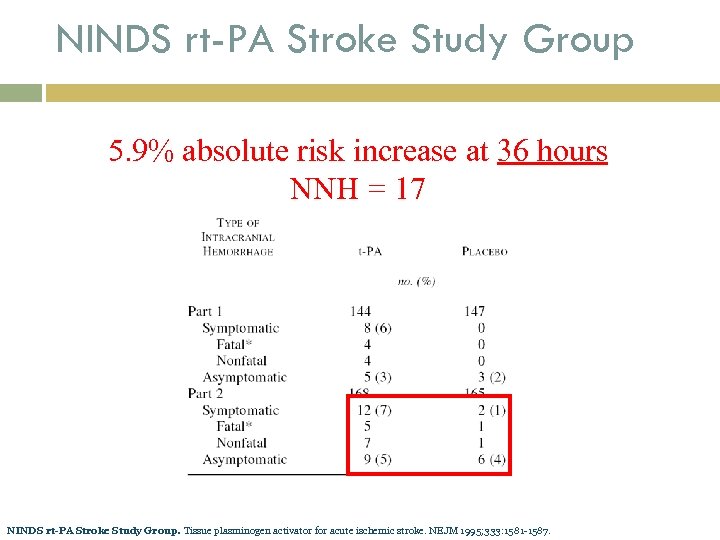
NINDS rt-PA Stroke Study Group 5. 9% absolute risk increase at 36 hours NNH = 17 NINDS rt-PA Stroke Study Group. Tissue plasminogen activator for acute ischemic stroke. NEJM 1995; 333: 1581 -1587.
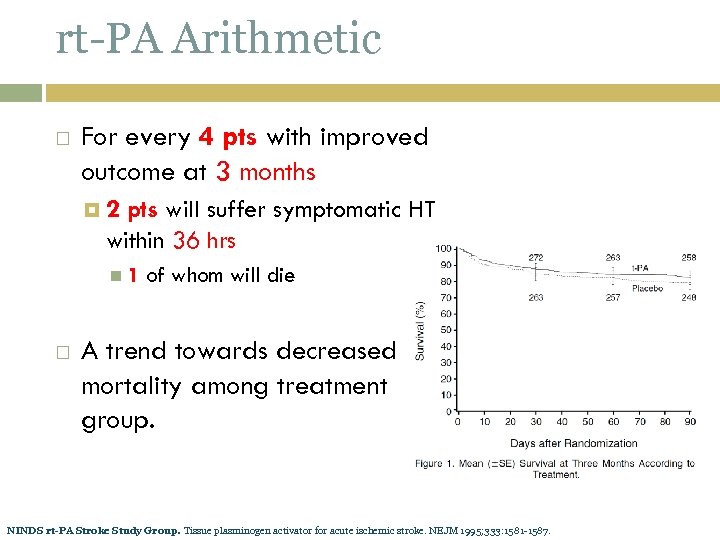
rt-PA Arithmetic For every 4 pts with improved outcome at 3 months 2 pts will suffer symptomatic HT within 36 hrs 1 of whom will die A trend towards decreased mortality among treatment group. NINDS rt-PA Stroke Study Group. Tissue plasminogen activator for acute ischemic stroke. NEJM 1995; 333: 1581 -1587.
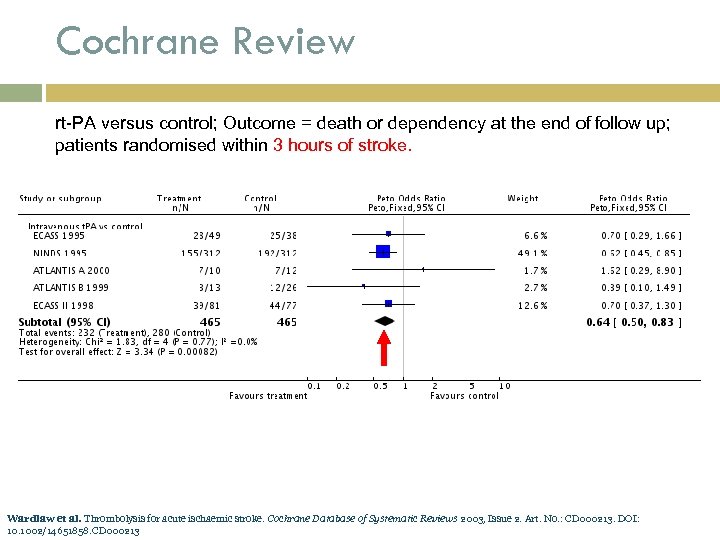
Cochrane Review rt-PA versus control; Outcome = death or dependency at the end of follow up; patients randomised within 3 hours of stroke. Wardlaw et al. Thrombolysis for acute ischaemic stroke. Cochrane Database of Systematic Reviews 2003, Issue 2. Art. No. : CD 000213. DOI: 10. 1002/14651858. CD 000213

European Cooperative Acute Stroke Study (ECASS) III Randomized, double-blind, placebo controlled trial rt-PA from 3 to 4. 5 hrs Primary outcome was m. RS at 3 months Favourable outcome ≤ 1 Exclusion criteria included: Severe stroke (NIHSS ≥ 25 or ≥ 1/3 MCA territory) Combination of previous stroke and diabetes mellitus. Hacke et al. Thrombolysis with alteplase 3 to 4. 5 hours after acute ischemic stroke. NEJM 2008; 359: 1317 -1329.
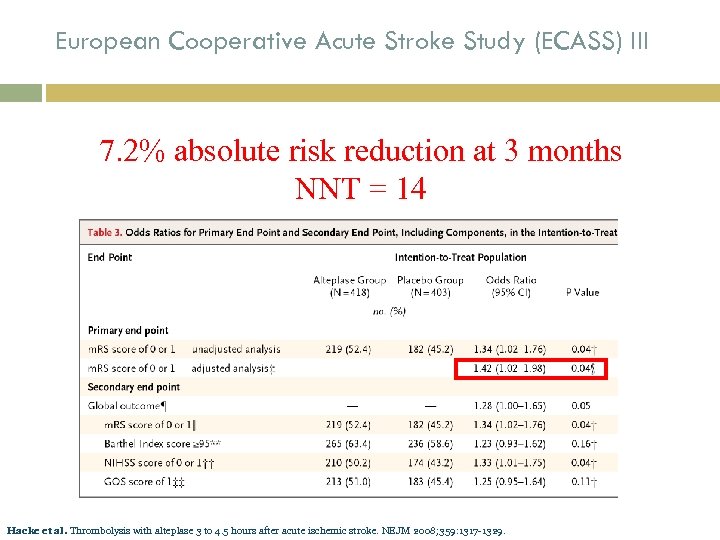
European Cooperative Acute Stroke Study (ECASS) III 7. 2% absolute risk reduction at 3 months NNT = 14 Hacke et al. Thrombolysis with alteplase 3 to 4. 5 hours after acute ischemic stroke. NEJM 2008; 359: 1317 -1329.

European Cooperative Acute Stroke Study (ECASS) III 4. 4% absolute risk increase at 3 months NNH = 23 Hacke et al. Thrombolysis with alteplase 3 to 4. 5 hours after acute ischemic stroke. NEJM 2008; 359: 1317 -1329.

Time is Brain! “Remember that time is money. ” Benjamin Franklin, Advice to a Young Tradesman (1748) Saver JL. Time is brain – quantified. Stroke 2006; 37: 263 -266.
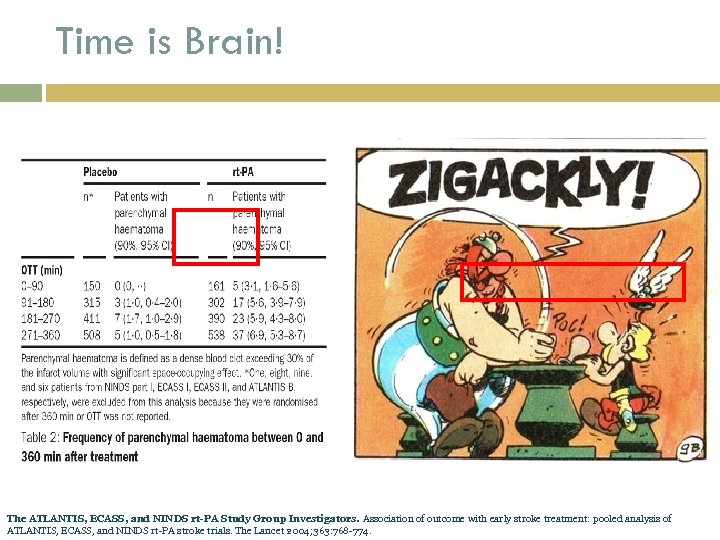

Time is Brain! The ATLANTIS, ECASS, and NINDS rt-PA Study Group Investigators. Association of outcome with early stroke treatment: pooled analysis of ATLANTIS, ECASS, and NINDS rt-PA stroke trials. The Lancet 2004; 363: 768 -774.

Intra-arterial vs. Intravenous PROACT II (JAMA 1999) Pro-urokinase in MCA occlusion @ < 6 hrs 180 patients (121 tx; 59 placebo) ARR 15% but a further 8% with ICH at 24 hrs Intra-arterial may result in greater rates of recanalization (66%!? ) Intravenous remains favoured due to potential delays in delivery. Adams et al. Guidelines for the early management of adults with ischemic stroke. A guideline from the AHA/ASA stroke council… Stroke 2007; 38: 1655 -1711.

Consider Intra-arterial if… Severe neurological deficits (NIHSS ≥ 10) Presentation between 3 and 6 hours Recent major surgery Occlusion of major cervical or intracranial vessels Presence of hyper-dense artery sign? If considering, give bridging rt-PA IV dose while waiting. Adams et al. Guidelines for the early management of adults with ischemic stroke. A guideline from the AHA/ASA stroke council… Stroke 2007; 38: 1655 -1711.

Angioplasty and Stenting Possible acute uses (in conjunction with thrombolysis) ICA occlusion Vertebrobasilar occlusion Anecdotally, >24 hrs post onset! Adams et al. Guidelines for the early management of adults with ischemic stroke. A guideline from the AHA/ASA stroke council… Stroke 2007; 38: 1655 -1711.
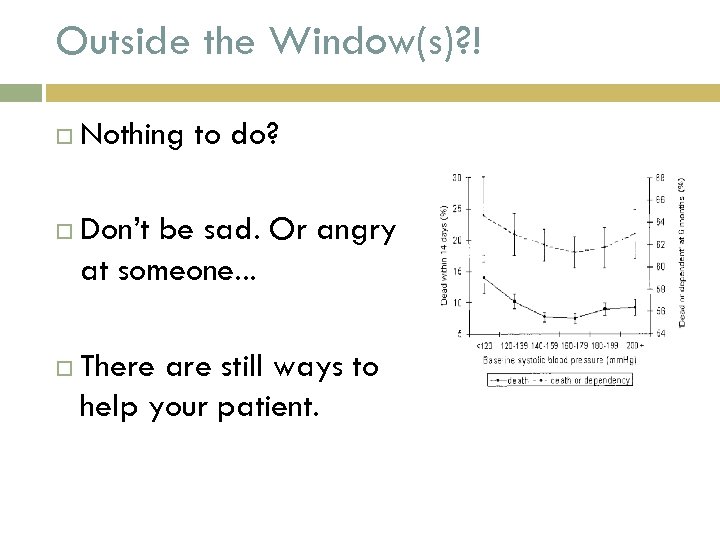
Outside the Window(s)? ! Nothing to do? Don’t be sad. Or angry at someone. . . There are still ways to help your patient.

Early Stroke Management Maintain adequate tissue oxygenation, ≥ 92 % Common: pneumonia, severe dysphagia, atelectasis NPO Elevate HOB? Robinul, atropine 1% eye drops po? Cardiac monitoring MI and arrhythmia frequent after stroke, most often a. fib Arrhythmia associated with insular strokes (right >>left) 24 hour monitoring recommended. Adams et al. Guidelines for the early management of adults with ischemic stroke. A guideline from the AHA/ASA stroke council… Stroke 2007; 38: 1655 -1711.

Early Stroke Management Avoid hyperthermia Treat fever and infections No evidence for cooling and potential risks of hypotension, cardiac arrhythmia and pneumonia Glucose Treat hyperglycemia aggressively, frequent testing, scales and Insulin DVT prophylaxis Frequent complication 5000 U bid or LMWH, safe with ASA. Adams et al. Guidelines for the early management of adults with ischemic stroke. A guideline from the AHA/ASA stroke council… Stroke 2007; 38: 1655 -1711.

Early Stroke Management Seizures: 5 -8 % after stroke, prophylaxis not recommended Incontinence not uncommon in acute stroke Limit use of Foleys to avoid urosepsis Decubitus ulcers in 15% of pts Think of it Positioning, dressings, adequate nutrition. Adams et al. Guidelines for the early management of adults with ischemic stroke. A guideline from the AHA/ASA stroke council… Stroke 2007; 38: 1655 -1711.

BP and Long Term Outcome Leonardi-Bee et al. Blood pressure and clinical outcomes in the International Stroke Trial. Stroke 2002; 33: 1315 -1320.
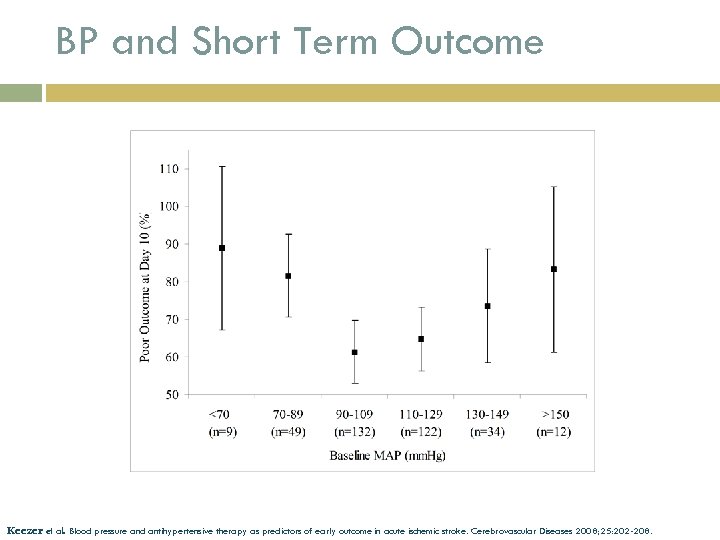
BP and Short Term Outcome Keezer et al. Blood pressure and antihypertensive therapy as predictors of early outcome in acute ischemic stroke. Cerebrovascular Diseases 2008; 25: 202 -208.

Acute Hypertension Management Blood pressure monitoring and higher BP associated with ↑ infarct volume at 7 days Lower AHA guidelines Lower or only if > 220/120 mm. Hg 185/110 for rt-PA Labetalol 10 -20 mg IV q 10 -20 min (or nitroprusside infusion) Goal is 15 -25% reduction within first 24 hrs Otherwise, hold all antihypertensives for first 24 hours! Adams et al. Guidelines for the early management of adults with ischemic stroke. A guideline from the AHA/ASA stroke council… Stroke 2007; 38: 1655 -1711.

Acute Hypertension Management No conclusive data, only expert opinion Hold all antihypertensives 1. Follow the guidelines Continue all antihypertensives 2. If the brain wants hypertension (and the heart can handle it), it will happen Continue some of them 3. Avoid holding those that will give rebound hypertension or tachycardia.
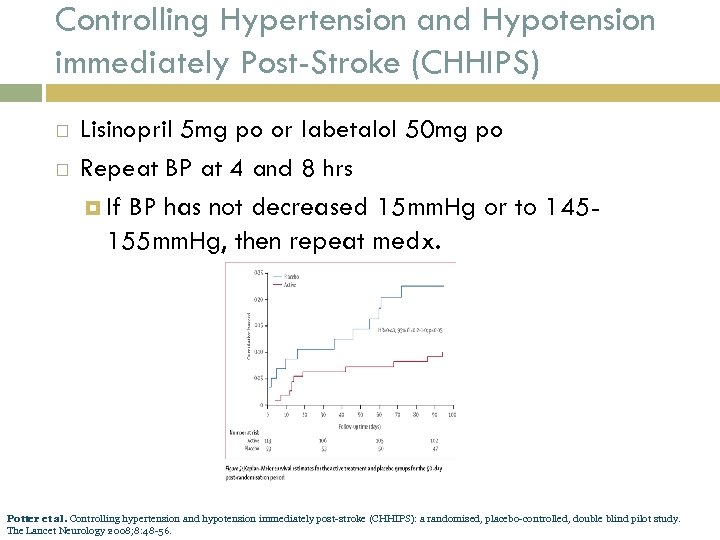
Controlling Hypertension and Hypotension immediately Post-Stroke (CHHIPS) Lisinopril 5 mg po or labetalol 50 mg po Repeat BP at 4 and 8 hrs If BP has not decreased 15 mm. Hg or to 145155 mm. Hg, then repeat medx. Potter et al. Controlling hypertension and hypotension immediately post-stroke (CHHIPS): a randomised, placebo-controlled, double blind pilot study. The Lancet Neurology 2008; 8: 48 -56.
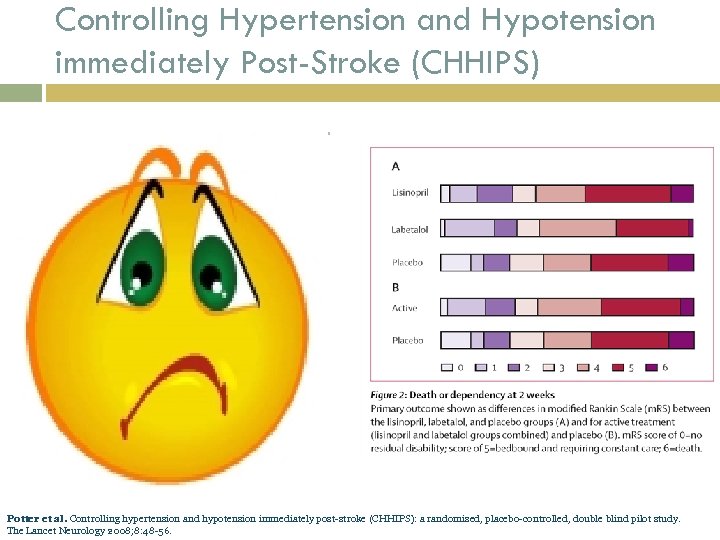
Controlling Hypertension and Hypotension immediately Post-Stroke (CHHIPS) Potter et al. Controlling hypertension and hypotension immediately post-stroke (CHHIPS): a randomised, placebo-controlled, double blind pilot study. The Lancet Neurology 2008; 8: 48 -56.

Acute Hypertension Management I’ve been known to use hydralazine or clonidine if SBP >>200 mm. Hg (not expert opinion ) But remember, impaired auto-regulation is relative If I’ve been walking around for 5 yrs with a BP 210/140, be careful about dropping it too much Maybe I’ll extend my infarct if you drop me to a ~measly 170/100 Use the AHA 15% rule!

Acute Hypotension Management Rare Correct hypovolemia Correct any cardiac arrythmia (ie fast a. fib) Dopamine is proposed by the AHA Little if any data to support their use CHHIPS attempted to look at phenylephrine but suffered from inadequate recruitment Phenylephrine has been favoured because of little cerebral vasoconstriction. Adams et al. Guidelines for the early management of adults with ischemic stroke. A guideline from the AHA/ASA stroke council… Stroke 2007; 38: 1655 -1711. Mistri et al. Pressor therapy in acute ischemic stroke. Systematic review. Stroke 2006; 37: 1565 -1571.

Anticoagulation International Stroke Trial 19, 435 pts ASA (300 mg qd) + uf. H (5000 or 12, 500 U bid) ASA alone uf. H alone Neither Death at 14 days, death or dependency at 6 months Heparin led to fewer recurrent strokes at 14 days (2. 9% vs 3. 8%) Offset by an increase in ICH (1. 2% vs 0. 4%) No significant difference in death or non-fatal recurrent stroke (11. 7% vs 12. 0%) AHA does not recommend its use, even in the setting of worsening stroke. IST Collaborative Group. The IST: a randomised trial of aspirin, subcutaneous heparin, both, or neither among 19 435 patients with acute ischemic stroke. The Lancet 1997; 349: 1569 -1581.

Antiplatelets Effect of early ASA not proven with IST combined with Chinese Acute Stroke Trial (CAST) ASA during first 14 days post-stroke produced 10 fewer deaths or recurrent strokes per 1000 pts 4 more ICH, transfused or fatal extra-cranial bleeds per 1000 pts No data for early clopidogrel or dipyridamole/ASA Currently, none are recommended within first 24 hours. Adams et al. Guidelines for the early management of adults with ischemic stroke. A guideline from the AHA/ASA stroke council… Stroke 2007; 38: 1655 -1711. IST Collaborative Group. The IST: a randomised trial of aspirin, subcutaneous heparin, both, or neither among 19 435 patients with acute ischemic stroke. The Lancet 1997; 349: 1569 -1581.

Decompressive Craniectomy +/- Mannitol HAMLET, DECIMAL, DESTINY 48 hrs Hofmeijer et al. Surgical decompression for space-occupying cerebral infarction (the hemicraniectomy after middle cerebral artery infarction with lifethreatening edema trial [HAMLET]): a multicentre, open, randomised trial. The Lancet Neurology 2009; 8: 326 -333.
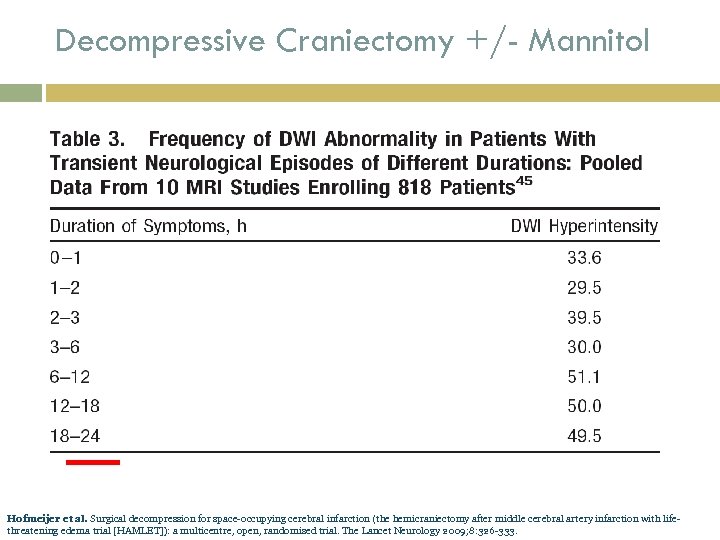
Decompressive Craniectomy +/- Mannitol Hofmeijer et al. Surgical decompression for space-occupying cerebral infarction (the hemicraniectomy after middle cerebral artery infarction with lifethreatening edema trial [HAMLET]): a multicentre, open, randomised trial. The Lancet Neurology 2009; 8: 326 -333.

Transient Ischemic Attack

TIA Classic definition Focal neurological deficits lasting < 24 hours New AHA definition: “Transient episode of neurological dysfunction caused by focal brain, spinal cord, or retinal ischemia, without acute infarction” Most last <1 or 2 hours (if not 5 to 20 mins) It is a stroke that did not finish, yet! Easton et al. Definition and evaluation of transient ischemic attack. A scientific statement for healthcare professionals from the AHA/ASA stroke council… Stroke 2009; 40: 2276 -2293.

Imaging positive TIA Easton et al. Definition and evaluation of transient ischemic attack. A scientific statement for healthcare professionals from the AHA/ASA stroke council… Stroke 2009; 40: 2276 -2293.
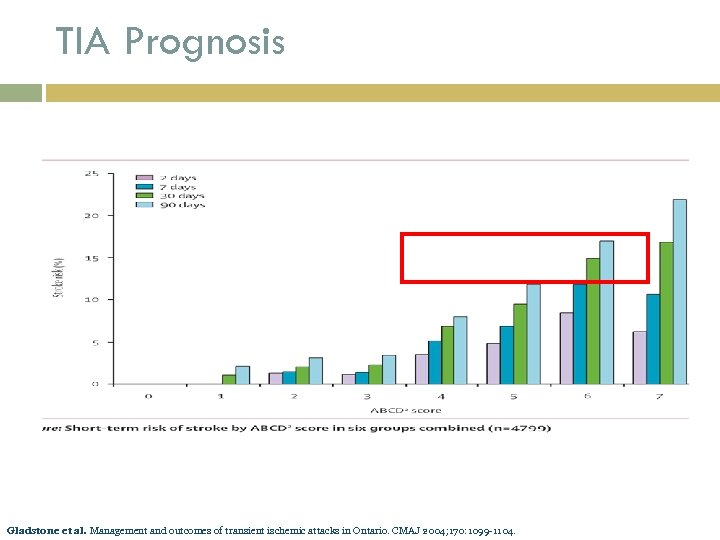
TIA Prognosis Gladstone et al. Management and outcomes of transient ischemic attacks in Ontario. CMAJ 2004; 170: 1099 -1104.
High risk TIA – ABCD 2 score Age > 60 yrs = 1 pt BP >140/90 = 1 pt Clinical Weakness (2 pts) Speech without weakness (1 pt) Other (0 pts) Duration >60 min (2 pts), 10 -59 1 (pt) <10 (0 pts) Diabetes = 1 pt. Johnston et al. Validation and refinement of scores to predict very early stroke risk after transient ischemic attack. The Lancet 2007; 369: 283 -292.
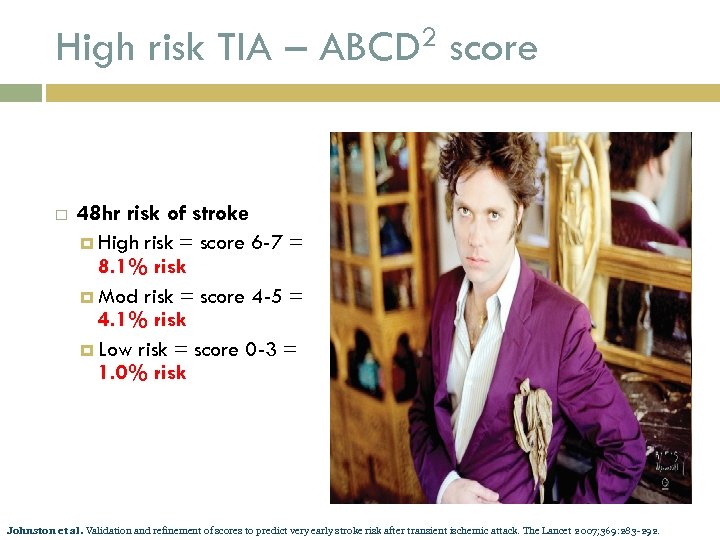

High risk TIA – ABCD 2 score 48 hr risk of stroke High risk = score 6 -7 = 8. 1% risk Mod risk = score 4 -5 = 4. 1% risk Low risk = score 0 -3 = 1. 0% risk Johnston et al. Validation and refinement of scores to predict very early stroke risk after transient ischemic attack. The Lancet 2007; 369: 283 -292.

Evaluation & Management Current AHA guidelines If ABCD 2 ≥ 3 then admit for monitoring In case of urgent need for thrombolysis More rapid investigations Otherwise evaluation and management similar to that of stroke. Easton et al. Definition and evaluation of transient ischemic attack. A scientific statement for healthcare professionals from the AHA/ASA stroke council… Stroke 2009; 40: 2276 -2293.

ON THE SHOULDERS OF GIANTS: MATHIAS ZILLER, MIKE SIDEL, ALEXANDRE POPPE, ADEL ALHAZZANI. Poses Thank you
ecde607cd9ef97aaea187475d816e4c4.ppt