ihd-110108065443-phpapp02.pptx
- Количество слайдов: 112

Ischemic Heart Disease By: Ammar Abd El-Rahmann 1 5: 38 AM
Definition Epidemiology What is the problem? Etiology & Risk factors Pathophysiology Lecture in points Clinical presentation Diagnosis Goals of therapy How to deal with the problem? Treatments options Counseling 5: 38 AM Outcome evaluation 2

Definition Synonym: IHD-CAD “Ischemic” refers to a decreased supply of oxygenated blood Narrowing of one or more of the major coronary arteries 5: 38 AM 3
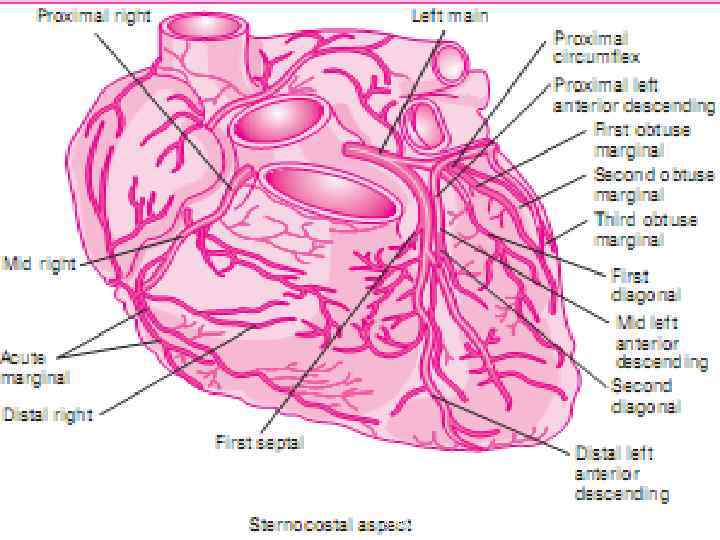
5: 38 AM 4
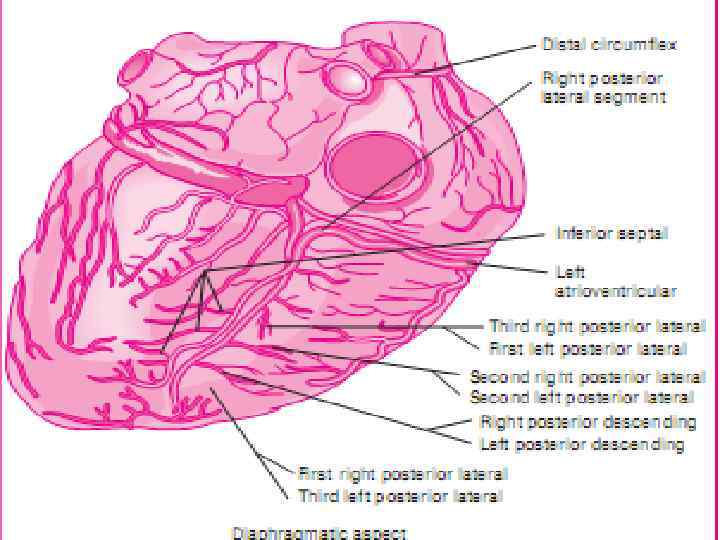
5: 38 AM 5

Angina pectoris Most common symptom of IHD. Angina = discomfort in the chest that occurs when the blood supply to the myocardium is compromised. 5: 38 AM 6

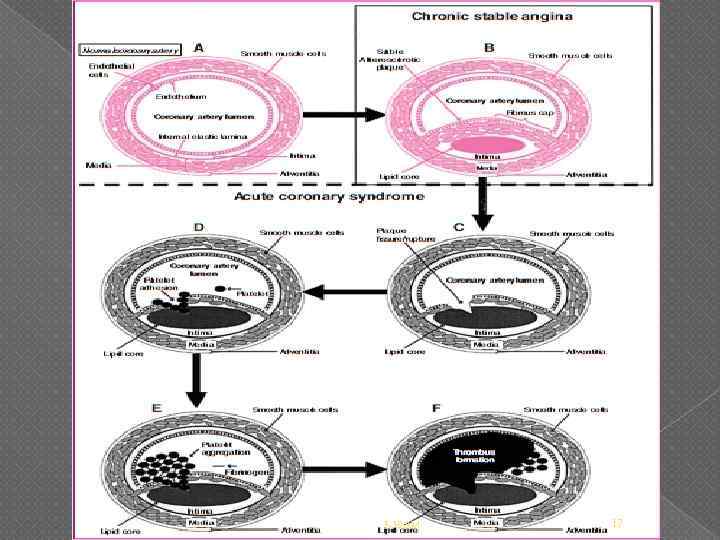
IHD -CAD Chronic stable angina • chronic and predictable occurrence of chest discomfort due to transient myocardial ischemia with physical exertion or other conditions that ↑ oxygen demand Prinzmetal’s or variant angina • spasm or contraction of a normal or diseased coronary artery • generally transient, may persist long enough to infarct the myocardium. 5: 38 AM Acute coronary syndrome • rupture of an atherosclerotic plaque with subsequent platelet adherence, activation , and aggregation, and the activation of the clotting cascade. • Ultimately, a thrombus forms composed of fibrin and platelets. 7
Definition Epidemiology What is the problem? Etiology & Risk factors Pathophysiology Lecture in points Clinical presentation Diagnosis Goals of therapy How to deal with the problem? Treatments options Counseling 5: 38 AM Outcome evaluation 8

Epidemiology The leading cause of death for both men and women in the United States The incidence of IHD is higher in middle-aged men compared to women. However, the rate of IHD ↑s two to three fold in women after menopause. 5: 38 AM 9
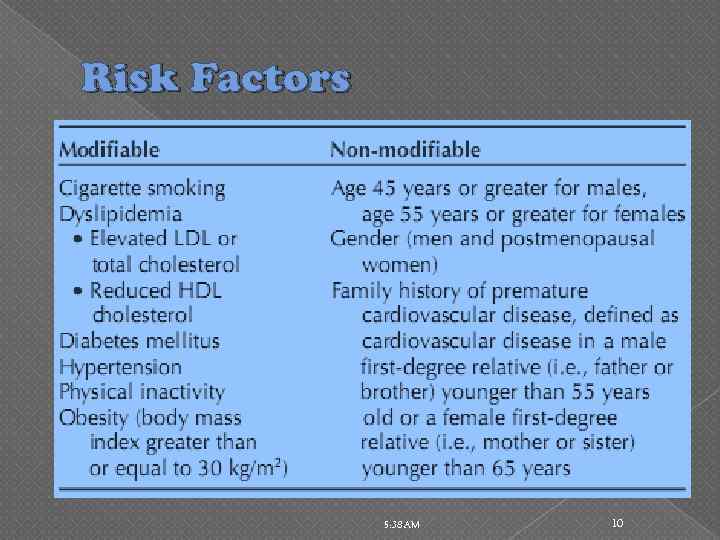

Risk Factors 5: 38 AM 10
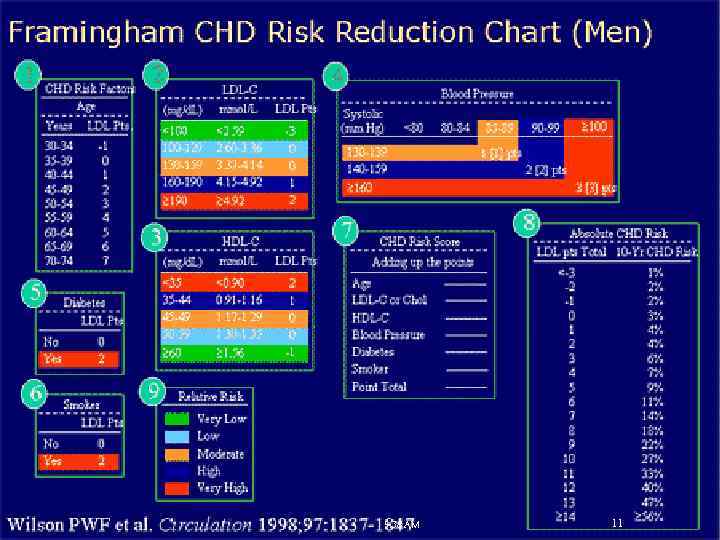
5: 38 AM 11

Metabolic syndrome is a constellation of cardiovascular risk factors related to hypertension, abdominal obesity , dyslipidemia , and insulin resistance. The risk of developing IHD and related complications is two-fold higher in patients with metabolic syndrome. 5: 38 AM 12

↑waist circumference (>40 inches or 102 cm ♂ and >35 inches or 89 cm♀). TG of 150 mg/d. L (1. 70 mmol/L) or greater or active treatment to ↓ TG ↓ HDL-c < 40 mg/d. L or 1. 04 mmol/L ♂ and <50 mg/d. L or 1. 3 mmol/L ♀ or active treatment to ↑ HDL-c BP 130/85 mm Hg or greater or active treatment with anti-HTN therapy. FBG of 100 mg/d. L (5. 55 mmol/L) or greater or active treatment for DM 5: 38 AM 13
Definition Epidemiology Etiology & Risk factors What is the problem? Pathophysiology Lecture in points Clinical presentation Diagnosis Goals of therapy How to deal with the problem? Treatments options Counseling 5: 38 AM Outcome evaluation 14
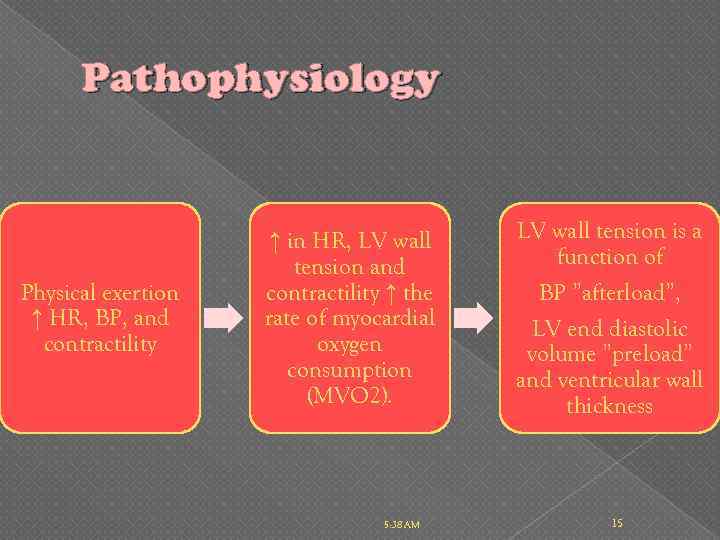
Pathophysiology Physical exertion ↑ HR, BP, and contractility ↑ in HR, LV wall tension and contractility ↑ the rate of myocardial oxygen consumption (MVO 2). 5: 38 AM LV wall tension is a function of BP ”afterload”, LV end diastolic volume ”preload” and ventricular wall thickness 15
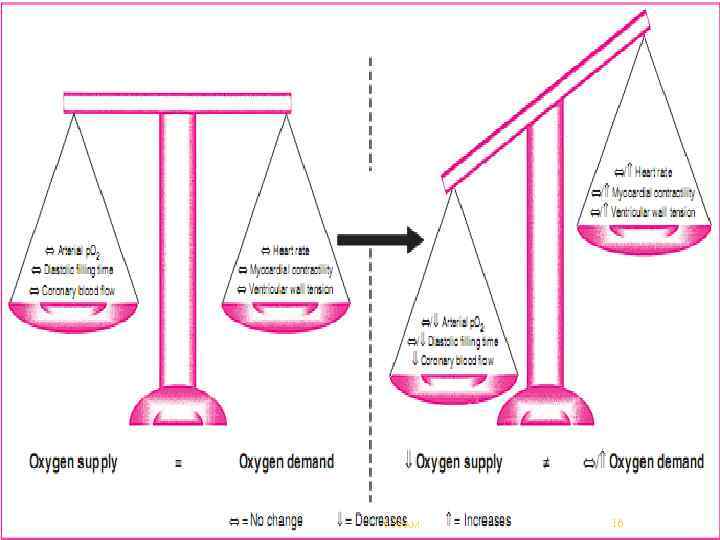
5: 38 AM 16
5: 38 AM 17
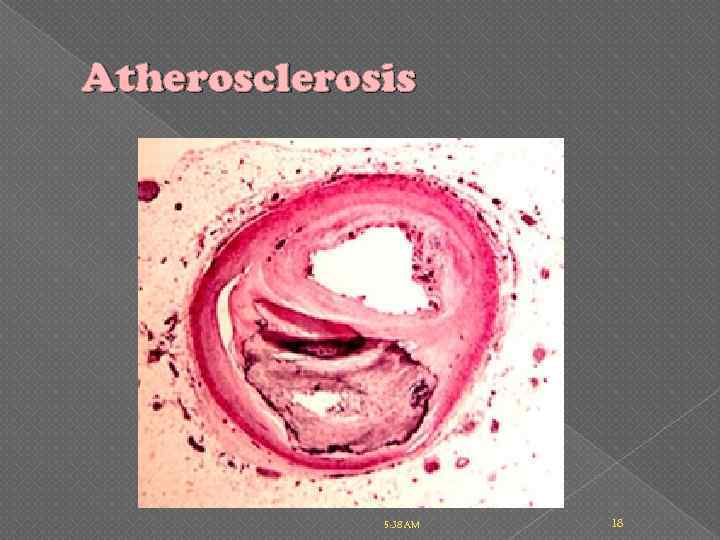
Atherosclerosis 5: 38 AM 18
Definition Epidemiology Etiology & Risk factors What is the problem? Pathophysiology Lecture in points Clinical presentation Diagnosis Goals of therapy How to deal with the problem? Treatments options Counseling 5: 38 AM Outcome evaluation 19
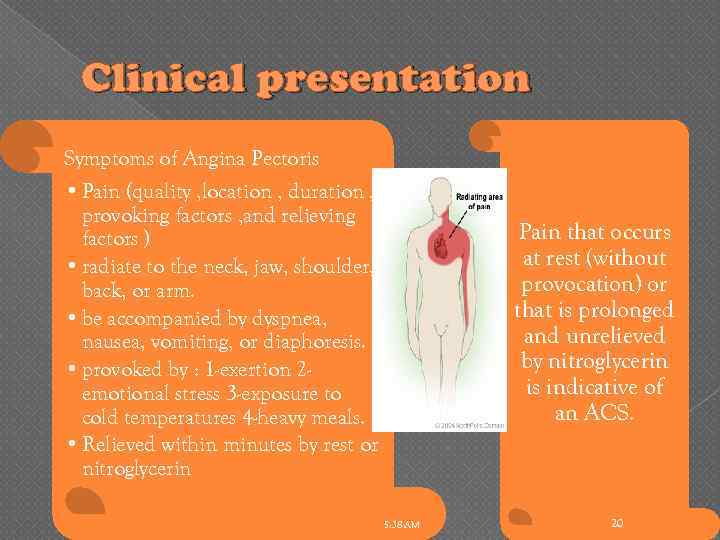
Clinical presentation Symptoms of Angina Pectoris • Pain (quality , location , duration , provoking factors , and relieving factors ) • radiate to the neck, jaw, shoulder, back, or arm. • be accompanied by dyspnea, nausea, vomiting, or diaphoresis. • provoked by : 1 -exertion 2 emotional stress 3 -exposure to cold temperatures 4 -heavy meals. • Relieved within minutes by rest or nitroglycerin Pain that occurs at rest (without provocation) or that is prolonged and unrelieved by nitroglycerin is indicative of an ACS. 5: 38 AM 20

Silent ischemia In some cases , ischemia may not produce any symptoms and is termed “silent ischemia. ” Diabetics may experience associated symptoms as dyspnea and diaphoresis, without having any of the classic chest pain symptoms. 5: 38 AM 21

The Canadian Cardiovascular Society Classification System 5: 38 AM 22

Non-atherosclerotic Conditions that Can Cause Angina-like Symptoms 5: 38 AM 23

Presentation of ACS midline anterior anginal chest discomfort, occur at rest , as a severe new onset, or as an increasing angina that is at least 20 minutes in duration. may radiate to the shoulder , down the left arm , and to the back or to the jaw. Associated symptoms which may accompany the chest discomfort include nausea , vomiting, diaphoresis , or shortness of breath. While similar to stable angina , the duration may be longer and the intensity greater. On physical exam , no specific features are indicative of ACS 5: 38 AM 24
Definition Epidemiology Etiology & Risk factors What is the problem? Pathophysiology Lecture in points Clinical presentation Diagnosis Goals of therapy How to deal with the problem? Treatments options Counseling 5: 38 AM Outcome evaluation 25
Diagnosis Physical examination Coronary angiography Biochemical Markers ECG 5: 38 AM 26

1 - Physical examination Medical history and physical exam 1 - ascertain cardiovascular risk factors 2 - exclude non-ischemic and non-cardiac conditions Cardiac findings on the physical exam are often normal in patients with chronic stable angina. 5: 38 AM 27

Stable Vs Unstable angina Provoked by increase in O 2 demand Sudden decrease in O 2 supply Reproducible with exertion At rest without precipitating factors Reversible Prolonged symptoms (>20 minutes) (relieved by rest & nitroglycerin) Less responsive to rest & medication 5: 38 AM 28
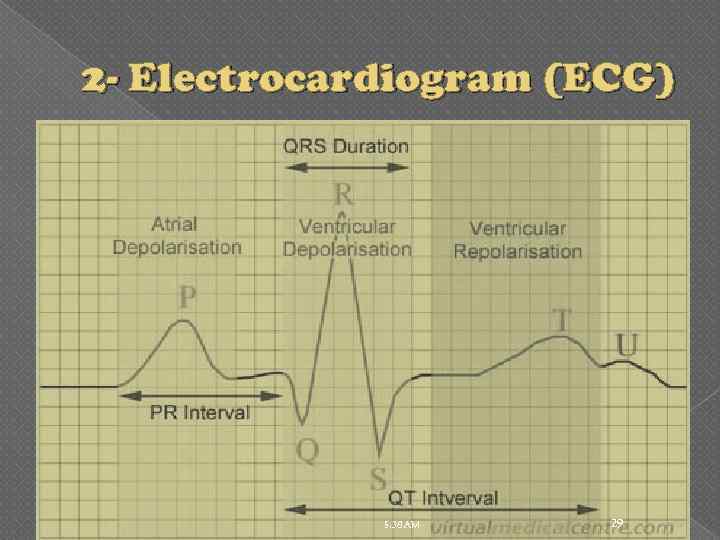
2 - Electrocardiogram (ECG) 5: 38 AM 29
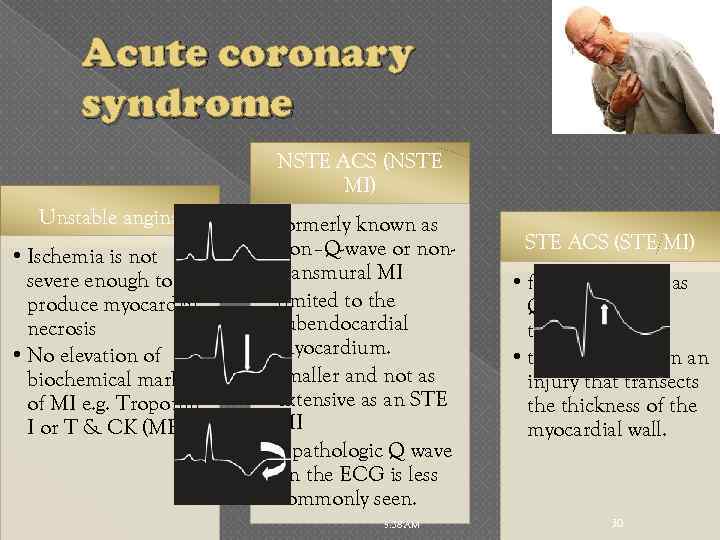
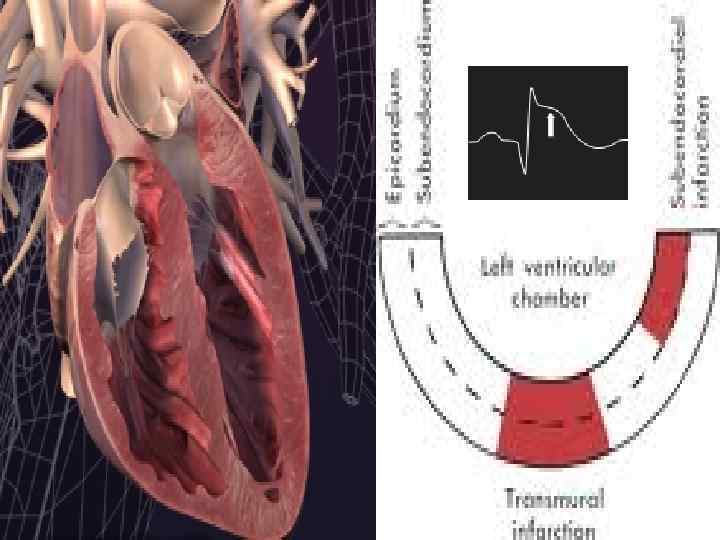
Acute coronary syndrome NSTE ACS (NSTE MI) Unstable angina • Ischemia is not severe enough to produce myocardial necrosis • No elevation of biochemical markers of MI e. g. Troponin I or T & CK (MB) • formerly known as non–Q-wave or nontransmural MI • limited to the subendocardial myocardium. • smaller and not as extensive as an STE MI • a pathologic Q wave on the ECG is less commonly seen. 5: 38 AM STE ACS (STE MI) • formerly known as Q-wave or transmural MI, • typically results in an injury that transects the thickness of the myocardial wall. 30
5: 38 AM 31
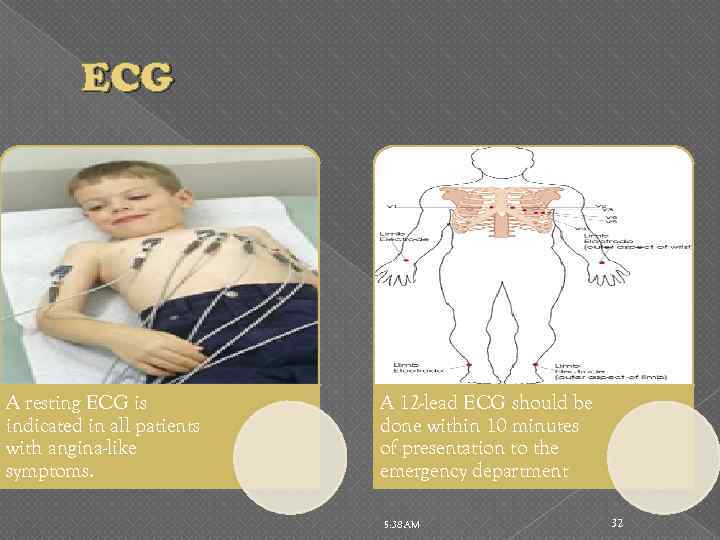
ECG A resting ECG is indicated in all patients with angina-like symptoms. A 12 -lead ECG should be done within 10 minutes of presentation to the emergency department 5: 38 AM 32

Stress testing Exercise ECG testing using either a treadmill (most commonly) or bicycle ergometer is a common non-invasive test A radioactive element (thalium TI 201) selective for heart tissues may be injected for imaging. Pharmacologic stressors are used for patients who are unable to exercise Dobutamine is used with stress echocardiography, adenosine or dipyridamole for nuclear imaging studies 5: 38 AM 33

3 - Coronary angiography (cardiac catheterization or “cardiac cath”) is considered the gold standard for the diagnosis of IHD Indicated when: 1 -stress testing results are abnormal 2 -symptoms of angina are poorly controlled. 5: 38 AM 34
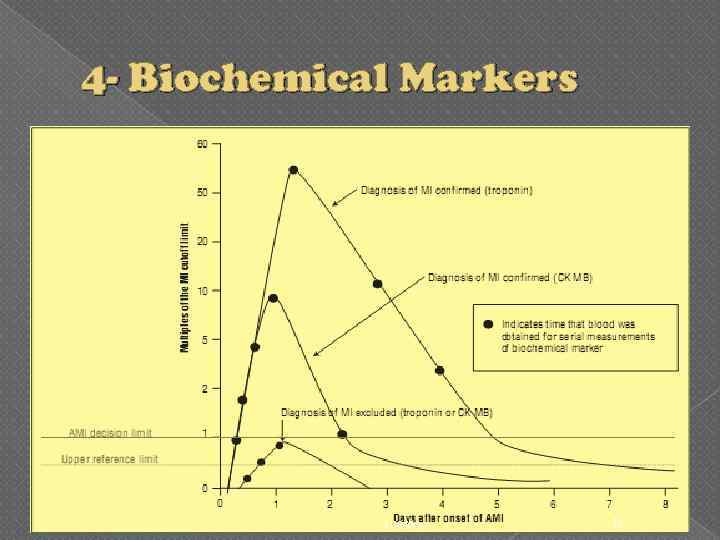
4 - Biochemical Markers 5: 38 AM 35

4 - Biochemical Markers (troponin and CK-MB) Blood is obtained from the patient 3 times: once in the emergency department and two additional times over the next 12 to 24 hours in order to measure. A single measurement of a marker is not adequate to exclude a diagnosis of MI If at least one troponin value is greater than the MI decision limit or two CKMB results are greater than the MI decision limit MI If early reinfarction is suspected , CK-MB is the preferred diagnostic test 5: 38 AM 36
Definition Epidemiology Etiology & Risk factors What is the problem? Pathophysiology Lecture in points Clinical presentation Diagnosis Goals of therapy How to deal with the problem? Treatments options Counseling 5: 38 AM Outcome evaluation 37
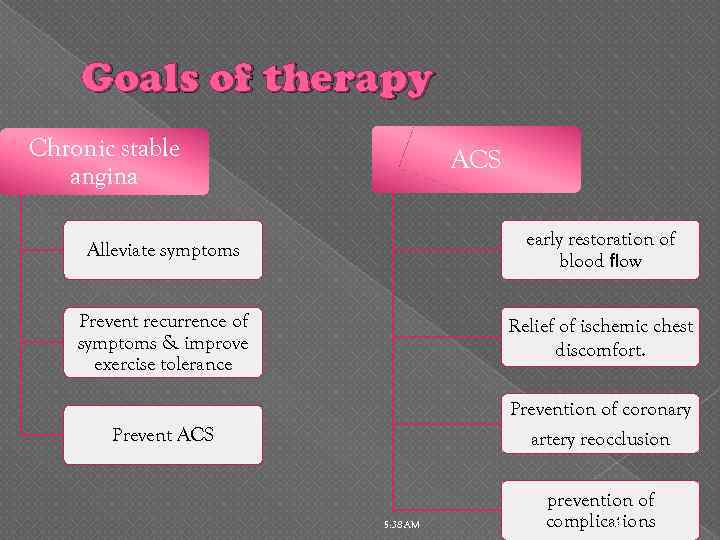
Goals of therapy Chronic stable angina ACS Alleviate symptoms early restoration of blood flow Prevent recurrence of symptoms & improve exercise tolerance Relief of ischemic chest discomfort. Prevention of coronary artery reocclusion Prevent ACS 5: 38 AM prevention of complications 38
Complications of ACS Cardiogenic shock , occurring in approximately 10% of hospitalized MI patients mortality 60%. Heart failure Valvular dysfunction, left ventricular free wall rupture. Ventricular and atrial tachyarrhythmias , bradycardia, heart block Pericarditis Stroke secondary to left ventricular thrombus embolization , Venous thromboembolism 5: 38 AM 39
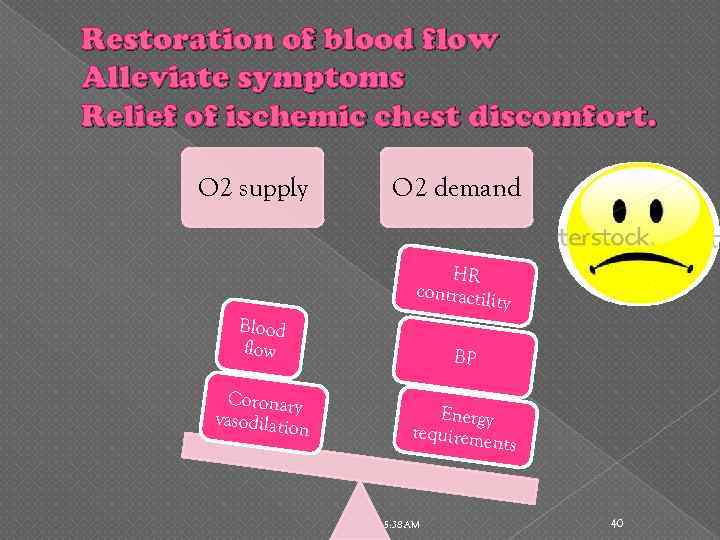
Restoration of blood flow Alleviate symptoms Relief of ischemic chest discomfort. O 2 supply O 2 demand HR contractili ty Blood flow Coronary vasodilatio n BP Energy requireme nts 5: 38 AM 40
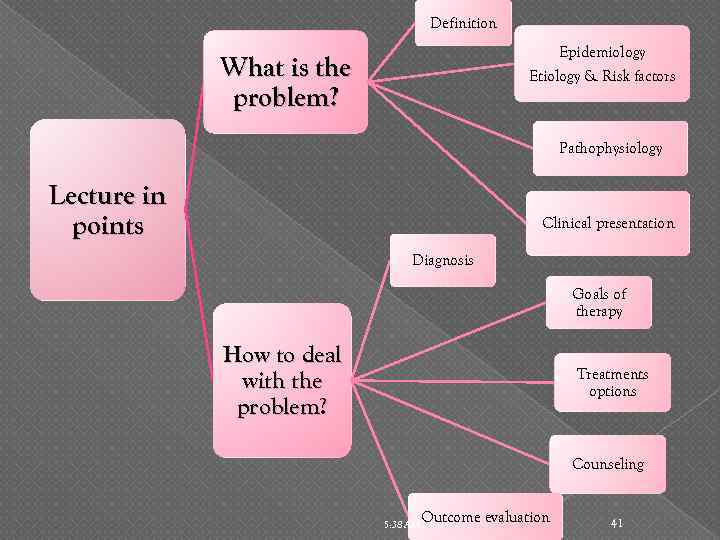
Definition Epidemiology Etiology & Risk factors What is the problem? Pathophysiology Lecture in points Clinical presentation Diagnosis Goals of therapy How to deal with the problem? Treatments options Counseling 5: 38 AM Outcome evaluation 41
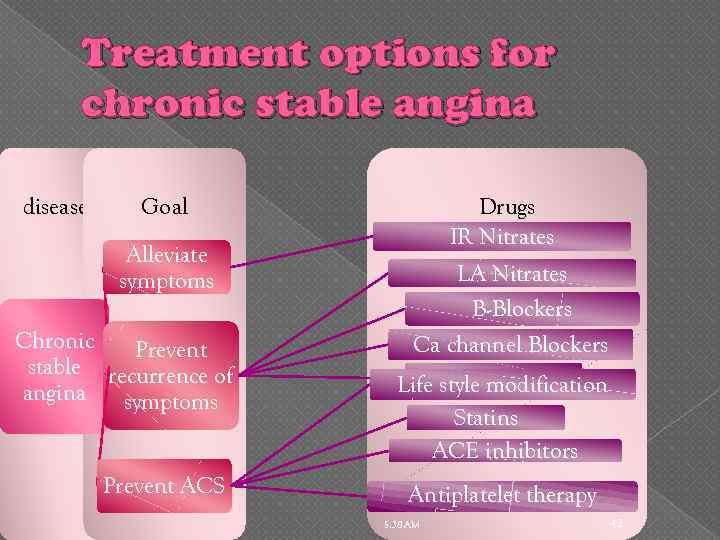
Treatment options for chronic stable angina disease Goal Alleviate symptoms Chronic Prevent stable recurrence of angina symptoms Prevent ACS Drugs IR Nitrates LA Nitrates B-Blockers Ca channel Blockers Ranolazine Life style modification Statins ACE inhibitors Antiplatelet therapy 5: 38 AM 42

IR Nitrates Short acting nitrates Nitroglycerin (NTG) or isosorbide dinitrate (ISDN) Route: sublingual (rapid action –bypass 1 st pass hepatic metabolism) Dosage form: tablet (less expensive) or spray ( easy use –more stable) 5: 38 AM 43
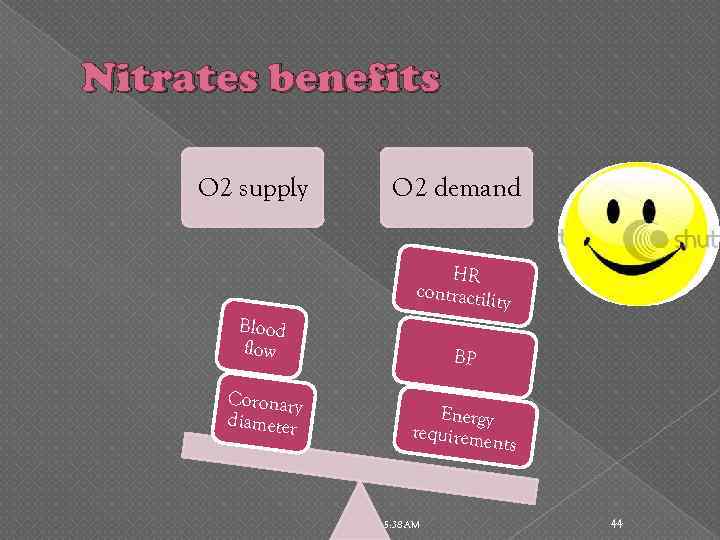
Nitrates benefits O 2 supply O 2 demand HR contractili ty Blood flow Coronary diameter BP Energy requireme nts 5: 38 AM 44
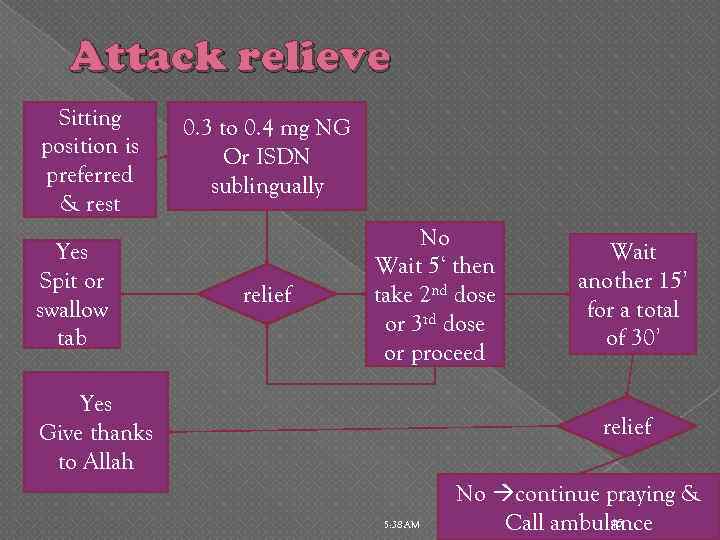
Attack relieve Sitting position is preferred & rest Yes Spit or swallow tab 0. 3 to 0. 4 mg NG Or ISDN sublingually relief No Wait 5‘ then take 2 nd dose or 3 rd dose or proceed Yes Give thanks to Allah Wait another 15’ for a total of 30’ relief 5: 38 AM No continue praying & 45 Call ambulance

Attack prophylaxis sublingual nitroglycerin 2 to 5 minutes prior to an activity known to cause angina (effects last for about 30 ‘ ). sublingual Isosorbide dinitrate longer half-life (effects lasting up to 2 hours. ) 5: 38 AM 46

Phosphodiestrase(PDE) type 5 inhibitors & Nitrates the use of nitrates within 24 hours of sildenafil or vardenafil and within 48 hours of tadalafil is contraindicated. 5: 38 AM 47
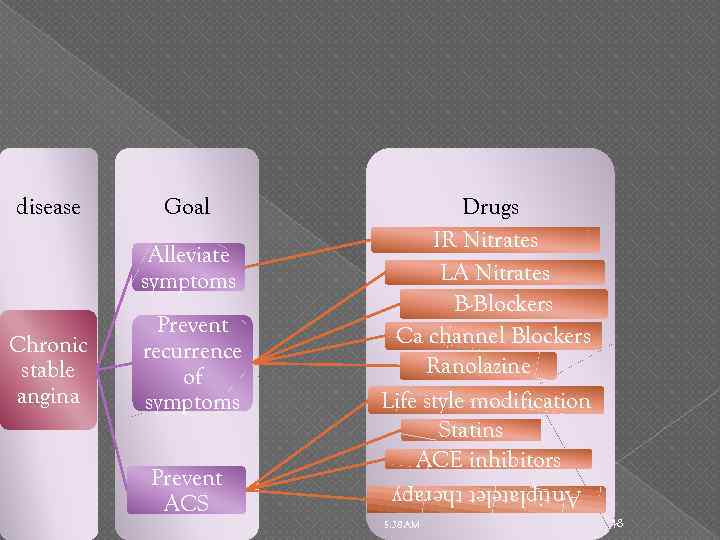
Goal Alleviate symptoms Chronic stable angina Prevent recurrence of symptoms Prevent ACS Drugs IR Nitrates LA Nitrates B-Blockers Ca channel Blockers Ranolazine Life style modification Statins ACE inhibitors Antiplatelet therapy disease 5: 38 AM 48

Long acting nitrates (NTG – ISDN – ISMN) Route & dosage form Nitroglycerin extended-release oral capsules – transdermal film Isosorbide dinitrate tablets slow-release capsules Isosorbide mononitrate tablets – extended-release tablets 5: 38 AM 49

Long acting nitrates use in IHD Monotherapy for the prevention of recurrence of symptoms should be avoided Why? • Reflex increases in sympathetic activity and heart rate may occur. • Patients are unprotected from ischemia during the nitrate-free interval. β-Blockers and calcium channel blockers are dosed to provide 24 -hour protection from ischemia. Monotherapy may be appropriate in patients who have low blood pressure or who experience symptomatic hypotension with low doses of β -blockers or calcium channel blockers. 5: 38 AM 50

Nitrate tolerance The cause of tolerance is unclear , several mechanisms have been proposed: depletion of the sulfhydryl groups necessary for the conversion of nitrates to nitric oxide, activation of neurohormonal systems, increased intravascular volume generation of free radicals that degrade nitric oxide. 5: 38 AM 51

How to avoid tolerance ? allow a daily nitrate-free interval 8 to 12 hrs • interval should occur when the patient is least likely to experience angina (nighttime hours ) 5: 38 AM 52

Common Side effects Headache flushing secondary to venodilation resolves with continued therapy or treated by paracetamol Postural hypotension 5: 38 AM Skin erythema rotating the application site 53
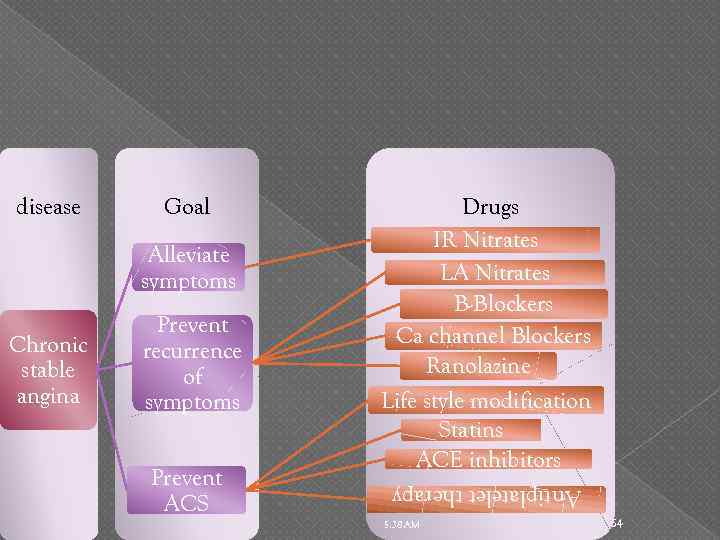
Goal Alleviate symptoms Chronic stable angina Prevent recurrence of symptoms Prevent ACS Drugs IR Nitrates LA Nitrates B-Blockers Ca channel Blockers Ranolazine Life style modification Statins ACE inhibitors Antiplatelet therapy disease 5: 38 AM 54

β-Blockers β 1 selective α 1, β 1, and β 2 & ISA β 2 • (“Acebutolol ISA” Atenolol Bisoprolol Metoprolol ) • (Carvedilol) • (Labetalol) 5: 38 AM non selective • (Nadolol Propranolol “& ISA Pindolol”) 55
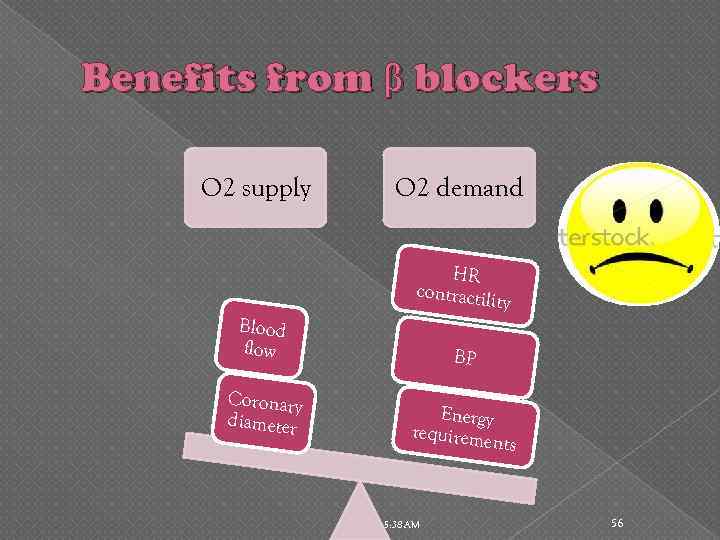
Benefits from β blockers O 2 supply O 2 demand HR contractili ty Blood flow Coronary diameter BP Energy requireme nts 5: 38 AM 56

β blockers use in IHD Doses initiated at the lowest , with titration according to symptom and hemodynamic response β-blocker dose is commonly titrated to achieve the following: • Resting HR between 50 and 60 b/min. • Maximum HR with exercise < 100 b/min or 20 b/min +resting HR. 5: 38 AM 57

β blockers use in IHD β-Blockers are 1 st line for preventing recurrence of symptoms particularly with a history of MI. Why? • May prevent cardiac arrhythmias • May prevent stroke and heart failure , with hypertension • Decrease the risk for reinfarction and improve survival in patients with history of MI. β-blockers with ISA should be avoided in patients with IHD. 5: 38 AM 58

β blockers contraindications 1 - Severe bradycardia (heart rate less than 50 beats per minute) 2 - AV conduction defects in the absence of a pacemaker 5: 38 AM 59

Relative contraindications Asthma , COPD, bronchospastic disease selective β 1 -Blockers preferred peripheral vascular disease Ca channel blockers preferred Variant angina (best avoid β-Blockers) Ca channel blockers preferred severe depression 5: 38 AM 60

β-Blockers use with particular caution in combination with other drugs that depress AV conduction (e. g. , digoxin, verapamil, and diltiazem) Diabetes (mask hypoglycemia –prolong recovery) selective β 1 Blockers preferred Heart failure i. e. , ejection fraction less than 35% (worsen symptoms of HF) start low &titrate slow 5: 38 AM 61

β-blockers adverse effects fatigue, malaise sleep disturbances, depression 5: 38 AM Sexual dysfunction. 62
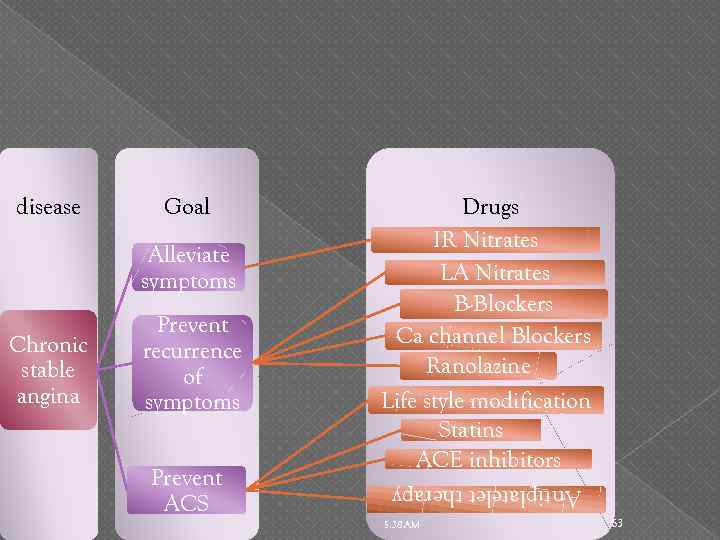
Goal Alleviate symptoms Chronic stable angina Prevent recurrence of symptoms Prevent ACS Drugs IR Nitrates LA Nitrates B-Blockers Ca channel Blockers Ranolazine Life style modification Statins ACE inhibitors Antiplatelet therapy disease 5: 38 AM 63

Ca channel blockers (CCB) Non dihydeopyridines “cardiac selective” Dihydropyridines • (verapamil-diltiazem) • (amlodipine- felodipine nifedipine -nicardipine) 5: 38 AM 64
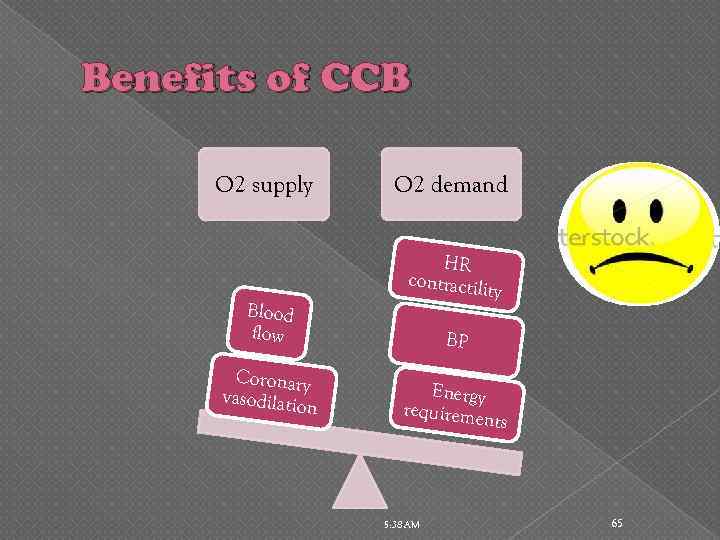
Benefits of CCB O 2 supply Blood flow Coronary vasodilatio n O 2 demand HR contractili ty BP Energy requireme nts 5: 38 AM 65

dihydropyridine calcium channel blockers Cardioselective CCB Verapamil • , nifedipine in • decrease myocardial particular, areand Diltiazem are generally more potent oxygen demand by effective anti-anginal agents vasodilators that can dihydropyridine CCBs slowing cardiac than the cause baroreflexconduction through mediated increases the AV nodes and in sympathetic tone lowering heart rate and heart rate. 5: 38 AM 66

CCB use in IHD Calcium channel blockers are recommended as initial treatment in IHD when ß-blockers are contraindicated or not tolerated. In addition, CCBs may be used in combination with ß-blockers when initial treatment is unsuccessful. 5: 38 AM 67

CCB contraindications Verapamil & diltiazem in severe bradycardia or AV conduction disease. 5: 38 AM 68

CCB use with particular caution Verapamil & diltiazem in combination with other agents that depress AV conduction (e. g. , digoxin, β Blockers ) CCB with –ve inotropic effect left ventricular systolic dysfunction Amlodipine & Felodipine has low –ve inotropic effect so they appear to be safe in left ventricular systolic dysfunction Short-acting CCB (nifedipine and nicardipine) should be avoided in the management of IHD. 5: 38 AM 69
Goal Alleviate symptoms Chronic stable angina Prevent recurrence of symptoms Prevent ACS Drugs IR Nitrates LA Nitrates B-Blockers Ca channel Blockers Ranolazine Life style modification Statins ACE inhibitors Antiplatelet therapy disease 5: 38 AM 70

Ranolazine Enhance Energy Efficiency Exact mechanism is unknown but may involve: • partial inhibition of fatty acid oxidation • enhanced generation of adenosine triphosphate (ATP) 5: 39 AM 71
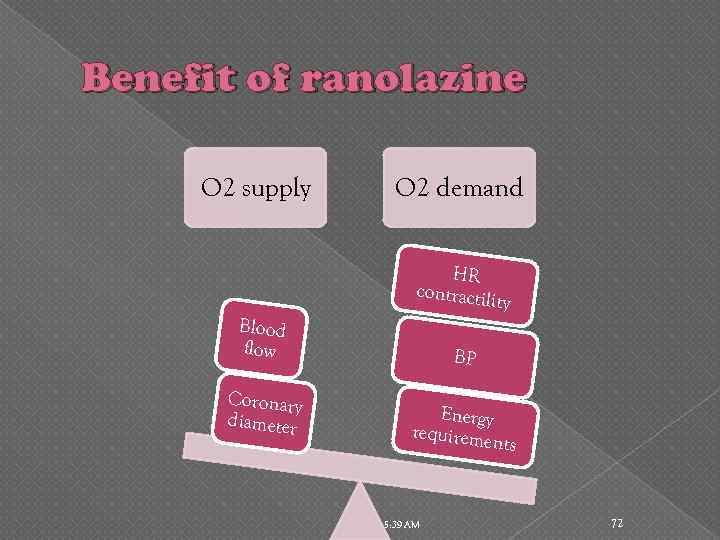
Benefit of ranolazine O 2 supply O 2 demand HR contractili ty Blood flow Coronary diameter BP Energy requireme nts 5: 39 AM 72

Risks & Adverse effects Ranolazine has the potential to prolong the QT interval and increase the risk for the lifethreatening arrhythmia, torsades de pointes. Reserved for patients who do not respond to traditional anti-anginal medications. 5: 39 AM 73
Risks & Adverse effects dizziness headache constipation 5: 39 AM nausea. 74
Goal Alleviate symptoms Chronic stable angina Prevent recurrence of symptoms Prevent ACS Drugs IR Nitrates LA Nitrates B-Blockers Ca channel Blockers Ranolazine Life style modification Statins ACE inhibitors Antiplatelet therapy disease 5: 39 AM 75
Prevent ACS & coronary artery reocclusion Risk factors modifications Stabilize plaques Prevent formation of thrombus 5: 39 AM 76

Life style modifications slow the progression of IHD, and decrease the risk for IHD -related complications. 5: 39 AM 77

Life style modifications Smoking cessation Dietary recommendation Excercise 5: 39 AM 78
Exercise Benefits of exercise: weight loss BP reduction. Increase functional capacity Exertion may induce symptoms? begin a low level of exercise for 20 to 30 minutes at a time, with increases in exercise duration and intensity as symptoms allow. 5: 39 AM 79
Goal Alleviate symptoms Chronic stable angina Prevent recurrence of symptoms Prevent ACS Drugs IR Nitrates LA Nitrates B-Blockers Ca channel Blockers Ranolazine Life style modification Statins ACE inhibitors Antiplatelet therapy disease 5: 39 AM 80

Aspirin & antiplatelet therapy Benefits: platelet adherence activation & aggregation are important steps in thrombus formation & ACS This is mediated by thromboxane ( a mediator synthesized by COX enzyme) Aspirin in doses (75 – 375)mg daily inhibit COX enzyme & have antiplatlet effects In stable or unstable angina, aspirin reduce the risk of major CVS events , particularly MI. Aspirin should be considered for all patients without contraindications, particularly with a history of MI 81 5: 39 AM

Aspirin & antiplatelet therapy Clopidogrel (or other) is indicated if : aspirin is contraindicated (e. g. , aspirin allergy, active peptic ulcer disease , active internal bleeding or ASA) is not tolerated by the patient Combination antiplatelet therapy may be synergistic in reducing the risk of IHD-related events 5: 39 AM 82
Goal Alleviate symptoms Chronic stable angina Prevent recurrence of symptoms Prevent ACS Drugs IR Nitrates LA Nitrates B-Blockers Ca channel Blockers Ranolazine Life style modification Statins ACE inhibitors Antiplatelet therapy disease 5: 39 AM 83

Statins (HMG-Co A Reductase inhibitors) Statins shown to decrease morbidity and mortality associated with IHD include lovastatin, simvastatin, pravastatin, and atorvastatin Not only patients with dyslipidemia , but also patients with “normal” LDL cholesterol derived benefit from statins. 5: 39 AM 84

Statins (HMG-Co A Reductase inhibitors) Additional benefits other than LDL lowering: Shift LDL particle from small, dense, highly atherogenic to larger, less atherogenic. Improve endothelial function. Prevent or inhibit inflammation by lowering C-reactive protein and other inflammatory mediators Possibly improving atherosclerotic plaque stability. 5: 39 AM 85
Goal Alleviate symptoms Chronic stable angina Prevent recurrence of symptoms Prevent ACS Drugs IR Nitrates LA Nitrates B-Blockers Ca channel Blockers Ranolazine Life style modification Statins ACE inhibitors Antiplatelet therapy disease 5: 39 AM 86

ACE inhibitors shown to decrease morbidity and mortality in patients with heart failure or a history of MI Ramipril reduced the risk of death, acute MI, and stroke in patients with IHD by 22% compared to placebo after an average of 5 years of treatment. Similar results have been demonstrated with perindopril 5: 39 AM 87

ACE inhibitors indications IHD patients who also have • diabetes mellitus, • left ventricular dysfunction, • history of myocardial infarction ARBs are alternative for ACEI if they were intolerable ACEI are 1 st line in patients with history of MI 5: 39 AM 88

Percutaneous Coronary Intervention (PCI) When to indicate? • Drug therapy fails • If extensive coronary atherosclerosis is present, one or more critical coronary stenoses (i. e. , greater than 70% occlusion of the coronary lumen) Benefits • restore coronary blood flow • relieve symptoms • prevent major adverse cardiac events 5: 39 AM 89

Percutaneous Coronary Intervention (PCI) Catheter-based interventions : Percutaneous transluminal coronary angioplasty (PTCA); Intracoronary bare metal stent placement; BMS Intracoronary drug-eluting (antiproliferative medications, such as paclitaxel or sirolimus, ) stent placement DES Atherectomy (rotational –directional ) 5: 39 AM 90
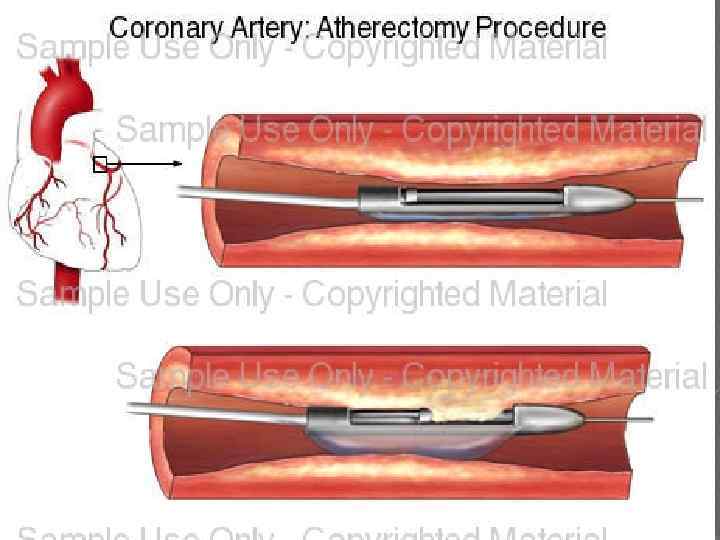
5: 39 AM 91

Coronary Artery Bypass Graft Surgery (CABG) Also known as open-heart surgery When to indicate? • extensive coronary atherosclerosis (generally greater than 70% occlusion ofthree or more coronary arteries) or • refractory to medical treatment Last resort in patients with IHD. 5: 39 AM 92
5: 39 AM 93
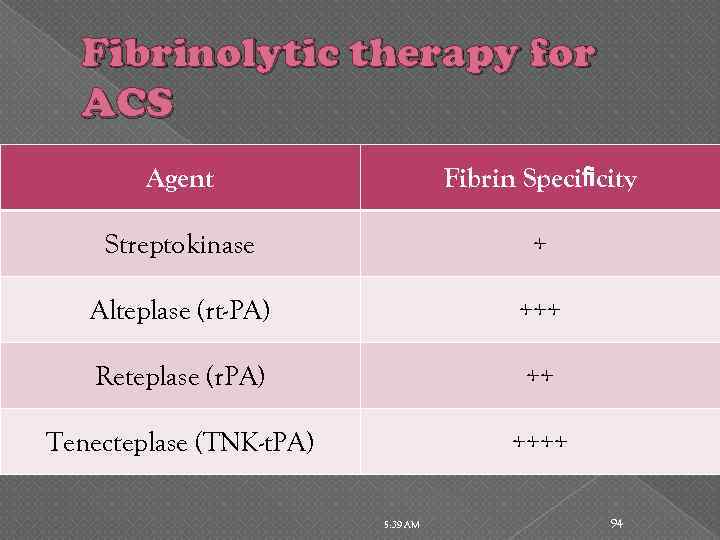
Fibrinolytic therapy for ACS Agent Fibrin Specificity Streptokinase + Alteplase (rt-PA) +++ Reteplase (r. PA) ++ Tenecteplase (TNK-t. PA) ++++ 5: 39 AM 94

Fibrinolytic therapy for ACS Indications ACC/AHA guidlines • Ischemic chest discomfort >20 minutes but <12 hours since symptom onset and ST-segment elevation of > 1 mm in height in 2 or more contiguous leads, or new or presumed new left bundle-branch block • Ongoing ischemic chest discomfort >20 minutes 12– 24 hours since symptom onset and ST-segment elevation of >1 mm in height in two or more contiguous leads It is not necessary to obtain the results of biochemical markers before initiating fibrinolytic therapy. Not indicated for any patient with NSTE ACS 5: 39 AM 95

Fibrinolytic therapy for ACS Absolute Contraindications ACC/AHA guidlines • Active internal bleeding (not including menses) • Previous intracranial hemorrhage at any time; ischemic stroke within 3 months • Known intracranial neoplasm • Known structural vascular lesion (e. g. , arteriovenous malformation) • Suspected aortic dissection • Significant closed head or facial trauma within 3 months 5: 39 AM 96

• Severe, uncontrolled on presentation B. P>180/110 mm hg • History of severe, chronic, poorly controlled hypertension Hypertension Coagulation impairment • Current use of anticoagulants • Known bleeding diathesis • Recent (within 2– 4 weeks) internal bleeding , Active peptic ulcer. Pregnancy • Non-compressible vascular puncture (such as a recent liver biopsy or carotid artery puncture) • Traumatic or prolonged (greater than 10 minutes) CPR or major surgery (less than 3 weeks ago) Relative Contraindications ACC/AHA guidlines Bleeding risk Streptokinase Known intracranial pathology • previous streptokinase use (greater than 5 days) or prior allergic reactions • History of prior ischemic stroke >3 months ago, dementia, or pathology not covered above under absolute contraindications 5: 39 AM 97

Fibrinolytic VS Primary PCI Patients presenting with an absolute contraindication will likely not receive fibrinolytic therapy, as primary PCI is preferred. Patients with a relative contraindication may receive fibrinolytic therapy if the perceived risk of death from the MI is higher than the risk of major hemorrhage 5: 39 AM 98
Definition Epidemiology What is the problem? Etiology & Risk factors Pathophysiology Lecture in points Clinical presentation Diagnosis Goals of therapy How to deal with the problem? Treatments options Counseling 5: 39 AM Outcome evaluation 99

Counseling of chronic stable angina Life style modification should be encouraged , monitored & periodically evaluated Correct use of IR nitates should be assessed Emotional support from health care team, family or other caring institutes is fundamental Warning about adverse effects of drugs and importance of immediate report of their occurrence 5: 39 AM 100

Counseling of Chronic Stable Angina for attack The seated position is generally preferred since the drug may cause dizziness. Close the cap tightly after use of tablets. Repeated use of NTG is not addictive and not result in any long-term side effects. NTG should not be taken with PDE 5 inhibitors 5: 39 AM 101
Definition Epidemiology What is the problem? Etiology & Risk factors Pathophysiology Lecture in points Clinical presentation Diagnosis Goals of therapy How to deal with the problem? Treatments options Counseling 5: 39 AM Outcome evaluation 102
Outcome evaluation Assess effectiveness of therapy Monitor disease progression Monitor adverse effects of drugs 5: 39 AM 103
Assess effectiveness of therapy Assess frequency and intensity of anginal symptoms. Determining the frequency of sublingual nitroglycerin use is helpful 5: 39 AM Assess exercise tolerance of patient 104

Monitor disease progression In case of increasing frequency or intensity, adjust therapy and refer the patient for additional diagnostic testing (e. g. , coronary angiography) and possibly for coronary interventions (e. g. , PCI or CABG surgery). Control risk factors should be assessed regularly. Routine screening for metabolic syndrome Assess the patient for IHD-related complications, such as heart failure. 5: 39 AM 105

Monitor adverse effects of drugs Hemodynamic parameters (BP – HR) should be routinely monitored to assess drug tolerance BP reduction particularly after initiation and dose titration of βblockers with α-blocking effects (e. g. , labetalol and carvedilol). Warn patients that postural hypotension during initiation or uptitration HR: drugs may have negative chronotropic effects (e. g. , bblockers, verapamil, or diltiazem) or may cause reflex tachycardia (e. g. , nitrates or dihydropyridine CCBs). 5: 39 AM 106

Case study A. E. , a 65 -year-old man, has been treated for chronic angina pectoris for 4 years. He refuses cardiac catheterization and revascularization; however, his coronary risk factors include a strong family history of cardiovascular disease and hyperlipoproteinemia. He experienced rheumatic fever at age 12; 5 years ago, his mitral valve was replaced. At that time, he had two-vessel CAD with 80% and 85% occlusion and an LV EF of 30% (normal, 55%). 5: 39 AM 107

1. 2. 3. 4. 5. 6. 7. Current medications include a prescription for: SL nitroglycerin; warfarin 5 mg for 5 days/week and 2. 5 mg for 2 days/week; metoprolol 50 mg every day; enalapril 10 mg every day; digoxin 0. 125 mg/day (serum digoxin concentration drawn 18 hours after the last dose is 0. 7 ng/m. L); oral simvastatin 40 mg every day; and furosemide 40 mg/day. 5: 39 AM 108

At his regular follow-up visit with his cardiologist, A. E. reports an increase in weekly anginal attacks over the last 2 months during his daily routine of working in his yard. Current vital signs include 1. a blood pressure of 110/60 mm. Hg and 2. a resting heart rate of 60 beats/minute. 5: 39 AM 109

What therapeutic options would be available for A. E. for additional control of his chronic stable angina? A. E. is at goal heart rate and his blood pressure is well controlled on his current regimen, but he continues to have anginal symptoms. A –ve inotrope CCB should not be given because A. E. has evidence of poorly controlled heart failure (EF of 30%). A long-acting nitrate is an option, but this could lower his blood pressure more than is desired. A dihydrpyridine (amlodipine &felodipine) may also lower blood pressure of A. E. Because of the lack of hemodynamic effects, ranolazine is a reasonable option for A. E. , in addition to continuing metoprolol. 5: 39 AM 110

References http: //www. theheart. org/article/194187. do http: //cme. medscape. com/viewarticle/474936 http: //www. fda. gov/ohrms/dockets/ac/00/slides /3622 s 2_01_2 -Squibb-cohen/sld 005. htm www. nucleosinc. com www. emedtv. com 5: 39 AM 111

We are the So, you ‘d better stop When it is a Hold your & we hold 5: 39 AM 112
ihd-110108065443-phpapp02.pptx