7becf582204ce6df7bbcc58574bcc160.ppt
- Количество слайдов: 20

Investing in Health Systems of the Future Budapest, Hungary 10 – 12 May 2011

Electronic Health Records and Semantic Interoperability: Time to scale up Dipak Kalra Professor of Health Informatics University College London
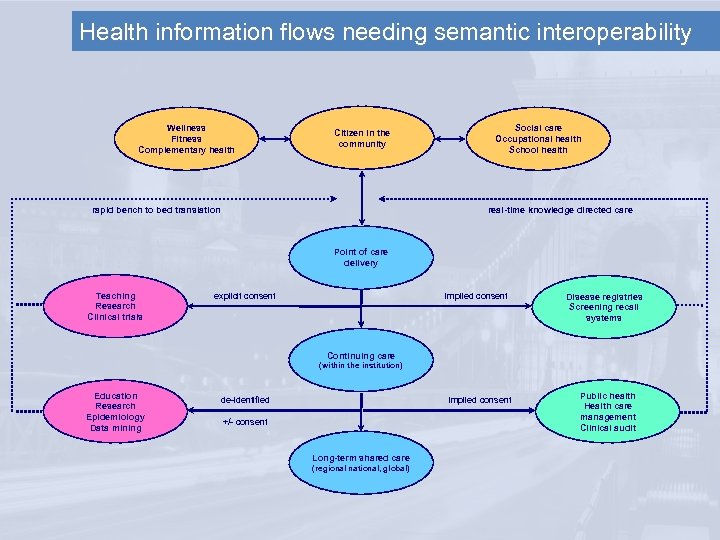
Health information flows needing semantic interoperability Wellness Fitness Complementary health Citizen in the community rapid bench to bed translation Social care Occupational health School health real-time knowledge directed care Point of care delivery Teaching Research Clinical trials explicit consent implied consent Disease registries Screening recall systems Continuing care (within the institution) Education Research Epidemiology Data mining de-identified implied consent +/- consent Long-term shared care (regional national, global) Public health Health care management Clinical audit

Essential needs • • • Guideline and decision support systems, notification and alerting components, and analytic tools need to process integrated health data drawn from multiple EHR systems in a consistent manner Intelligent personal health guidelines interoperating with PHRs and EHRs need to support the centring of care on patients New generation personalised medicine, underpinned by ‘omics sciences and translational research such as the VPH, needs to integrate EHRs with data from research: fundamental biomedical science, clinical and population health research, and clinical trials
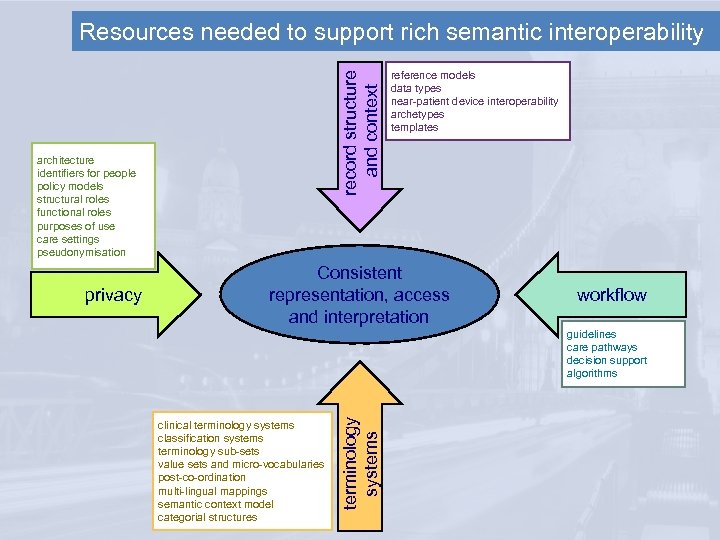
record structure and context Resources needed to support rich semantic interoperability architecture identifiers for people policy models structural roles functional roles purposes of use care settings pseudonymisation reference models data types near-patient device interoperability archetypes templates Consistent workflow guidelines care pathways decision support algorithms clinical terminology systems classification systems terminology sub-sets value sets and micro-vocabularies post-co-ordination multi-lingual mappings semantic context model categorial structures terminology systems privacy Rich EHR representation, access interoperability and interpretation

ARGOS and Semantic Interoperability • • • The ARGOS Transatlantic Observatory for Meeting Global Health Policy Challenges through ICT Enabled Solutions is an international platform for dialogue and collaboration on health policy issues that surround making Health ICT a success Co-ordinated by Euro. Rec, in partnership with AMIA Semantic interoperability is one of the priority themes Experts from the EU and US have met during 2010 -11 and shared understanding of the problem space, solutions found and priority areas to be tackled To be published as a policy brief: co-editor Mark Musen

Semantic interoperability resource priorities • Widespread and dependable access to maintained collections of coherent and quality-assured semantic resources – clinical models, such as archetypes and templates – rules for decision making and monitoring • – workflow logic which are – mapped to EHR interoperability standards – bound to well specified multi-lingual terminology value sets – indexed and correlated with each other via ontologies – referenced from modular (re-usable) care pathway components

Practical issues • • • These resources need to be developed by communities of practice, reflecting real needs This development must include patients, emphasising citizen engagement in self management and health maintenance The resources need to be easily embedded within EHR systems, and within other systems and services that will analyse and interpret EHR data

Semantic interoperability recommendations Eight strategic actions that now need to be championed, as a global mission 1. Establish good practice 2. Scale up semantic resource development 3. Support translations 4. Track key technologies 5. Align and harmonise standardisation efforts 6. Support education 7. Assure quality 8. Design for sustainability 9. Strengthen leadership and governance

1. Establish good practice • • • Develop criteria for assessing the quality of semantic resources Establish projects to develop good practice in the design and validation of clinical models bound to terminologies and ontologies and guideline-based pathway models Ensure projects are well-grounded and practical relevance to the management of clinical conditions of national and international priority – e. g. chronic conditions, like heart failure • – e. g. population health issues, like childhood obesity BUT: still adopting a holistic - not a piecemeal - approach

2. Scale up semantic resource development • • • Develop sustainable approaches to scaling this up across disease areas and stakeholders, importantly with patients Showcase convincing cases: successful pilots Ensure wide-scale clinical engagement during the design and piloting of clinical models and terminology Involve other stakeholders who will create or use health data Address wider health system needs and support future research

3. Support translations • • • Resources need to be multi-lingual to support cross border shared care, cross border health planning and global scale research Specifically consider the challenges of supporting multiple levels of “clinical jargon” for different stakeholders including patients and caregivers Develop and validate mappings amongst the different terminology systems in use by different communities

4. Track key technologies • • Monitor the evolving capability and potential uses of naturallanguage technologies, – including the reliability of such approaches for population-level and patient-level decision making Similarly track technology for automatic encoding of free text or diagrammatic data entry

5. Align and harmonise standardisation efforts • • Having understood the clinical modelling that is really needed. . . conduct a gap analysis of – interoperability standards – informatics tools – knowledge representation formalisms • – clinical content which are needed to support this scaling up, including – embedding such resources within EHR systems – providing formal recommendations to SDOs on the scope and level of detail that is needed and would be usable

6. Support education • Invest in education that enables clinical and patient/citizen acceptance, creation and use of knowledge-rich EHRs – to create good quality (faithful, accurate) and re-usable information – to better trust and use information from external sources • – to take better advantage of semantically interoperable systems and services Grow capacity in health informatics expertise including in semantic interoperability

7. Assure quality • Support research efforts on – what parts of, and how much of, a health record is useful to structure/code/make interoperable: focus on benefits versus effort • – the quality assurance of semantic resources when used together: clinical and technical validation Collaborate across countries on – common conformance criteria for systems and system components – practical methods for testing interoperability (e. g. for vocabularies, ontologies) – validating the correctness and consistent usability of solutions (including human factors)

8. Design for sustainability • • • Develop and align with a business model to justify strategic investments in this field Understand the value propositions (ROI) for key stakeholder groups and decision makers, including – – – – clinicians, patients, residents, caregivers EHR system vendors healthcare provider organisations health authorities insurers academic, bio-science and pharma research standards developers Find win-wins and relevant incentives

9. Strengthen leadership and governance • • Strong leadership within and across all relevant stakeholders will be essential to drive these actions and oversee benefits realisation In the longer term a governance organisation needs to be nominated – to support, co-ordinate and quality manage the future development of semantic interoperability resources for health – to develop an action plan for future research and educational investments

Benefits from rich semantic interoperability • • • Better co-ordination of complex and multi-agency care Improved clinical effectiveness, following guidelines More efficient patient journeys, fewer delays Better informed clinical decision making, better informed patients Reduced duplications, reduced clinical error More cost effective health care Better population health Enhanced opportunity for research and knowledge discovery Faster bench to bedside translation of research

Thank you d. kalra@ucl. ac. uk 10
7becf582204ce6df7bbcc58574bcc160.ppt