bipolar.pptx
- Количество слайдов: 38
 INVESTIGATION OF THE MENTAL HUMAN DISORDERS. MANIC-DEPRESSIVE PSYCHOSIS AS A CAUSE OF SUICIDE
INVESTIGATION OF THE MENTAL HUMAN DISORDERS. MANIC-DEPRESSIVE PSYCHOSIS AS A CAUSE OF SUICIDE
 Outline • definition of the manic-depressive illness( bipolar I, bipolar II, cyclothemia, mixed state ) • Ethiology and pathogenesis • The most common theories to manic-depression • Symptomatology and diagnosis • Treatment • Bipolar disorder and suicide • World statistic and interesting factors of risk
Outline • definition of the manic-depressive illness( bipolar I, bipolar II, cyclothemia, mixed state ) • Ethiology and pathogenesis • The most common theories to manic-depression • Symptomatology and diagnosis • Treatment • Bipolar disorder and suicide • World statistic and interesting factors of risk
 Manic depressive disorder refers to mood swings from overly “high” (manic) to overly “low” (depressed). Another name for manic-depressive illness is bipolar disorder. This refers to a person’s mood alternating between “poles” of mania (highs) and depression (lows).
Manic depressive disorder refers to mood swings from overly “high” (manic) to overly “low” (depressed). Another name for manic-depressive illness is bipolar disorder. This refers to a person’s mood alternating between “poles” of mania (highs) and depression (lows).
 Bipolar disorder is a brain disorder that causes unusual changes in the person’s mood, energy, and ability to function. The Bipolar Spectrum ranges from Bipolar I the most severe to Cyclothymia the least severe, in between is Bipolar II and Bipolar NOS which doesn’t fall under any category.
Bipolar disorder is a brain disorder that causes unusual changes in the person’s mood, energy, and ability to function. The Bipolar Spectrum ranges from Bipolar I the most severe to Cyclothymia the least severe, in between is Bipolar II and Bipolar NOS which doesn’t fall under any category.
 Bipolar I This is the most severe and sufferers will experience mania which includes psychotic symptoms such as delusions and hallucinations. The other cycle in the illness is depression although it can be mild, this factor varies with individuals. One episode or mood can last for months sometimes a year.
Bipolar I This is the most severe and sufferers will experience mania which includes psychotic symptoms such as delusions and hallucinations. The other cycle in the illness is depression although it can be mild, this factor varies with individuals. One episode or mood can last for months sometimes a year.
 Bipolar II This is the milder form of Bipolar I, sufferers will experience hypomania which does not include psychotic symptoms and if so they are very mild and rare, hypomania can be very enjoyable and often goes undiagnosed because the sufferers will begin to feel good, have grand ideas, more confident and may seem insightful and life of the party to others. Sufferers may sink into deep depression on the other cycle of the mood; however the severity differs depending on the patient.
Bipolar II This is the milder form of Bipolar I, sufferers will experience hypomania which does not include psychotic symptoms and if so they are very mild and rare, hypomania can be very enjoyable and often goes undiagnosed because the sufferers will begin to feel good, have grand ideas, more confident and may seem insightful and life of the party to others. Sufferers may sink into deep depression on the other cycle of the mood; however the severity differs depending on the patient.
 Cyclothymia This is the mildest form where the individuals suffers from a less severe form of hypomania and mild depression, however it is also a serious illness as their moods cycle frequently e. g. every four weeks with periods of a normal state.
Cyclothymia This is the mildest form where the individuals suffers from a less severe form of hypomania and mild depression, however it is also a serious illness as their moods cycle frequently e. g. every four weeks with periods of a normal state.
 Mixed State This is when a sufferer has depressive and manic symptoms at the same time, the person feeling and mood will be very confusing and difficult and suicide is very likely.
Mixed State This is when a sufferer has depressive and manic symptoms at the same time, the person feeling and mood will be very confusing and difficult and suicide is very likely.
 Manic-depressive illness or bipolar disorder affects both men and women.
Manic-depressive illness or bipolar disorder affects both men and women.
 bipolar disorder can start at any age, it usually begins in late adolescence. Bipolar disorder is found among people of all ages, races, ethnic groups, and social classes. It appears to have a genetic link and tends to run in families. Unfortunately, in addition to affecting the sufferer’s life, this disease also has the potential to devastate the lives of the caregivers and those in the immediate family circle
bipolar disorder can start at any age, it usually begins in late adolescence. Bipolar disorder is found among people of all ages, races, ethnic groups, and social classes. It appears to have a genetic link and tends to run in families. Unfortunately, in addition to affecting the sufferer’s life, this disease also has the potential to devastate the lives of the caregivers and those in the immediate family circle
 Like every mental illness, there is no definitive evidence concerning the etiology of manic-depression, also known as bipolar disorder
Like every mental illness, there is no definitive evidence concerning the etiology of manic-depression, also known as bipolar disorder
 Many scientists have isolated single genes to which they believe manic-depression can be attributed; however, very few agree on which gene it is. Egeland (1987) announced that she and her colleagues had found a gene that provided a strong diathesis toward manic-depression on chromosome 11. Two different groups of researchers (Detera-Wadleigh et al. , 1987 and Hodgkinson et al. , 1987) found no connection between the same gene and manic-depression, which led to theory that more than one gene may be responsible for the disorder. At the same time, Baron et al. (1987) announced they had found a genetic link between manicdepression and a different gene.
Many scientists have isolated single genes to which they believe manic-depression can be attributed; however, very few agree on which gene it is. Egeland (1987) announced that she and her colleagues had found a gene that provided a strong diathesis toward manic-depression on chromosome 11. Two different groups of researchers (Detera-Wadleigh et al. , 1987 and Hodgkinson et al. , 1987) found no connection between the same gene and manic-depression, which led to theory that more than one gene may be responsible for the disorder. At the same time, Baron et al. (1987) announced they had found a genetic link between manicdepression and a different gene.
 In 1993, Bredbechka et al. announced that the gene for manic -depression is on the X-chromosome; the next year Berrettini et al. (1994) reported to have found the gene that contributes to the disorder on chromosome 18 and Straub et al. (1994) reported it to be on chromosome 21. Mc. Mahon et al. (1995) found evidence to suggest that manic -depression was more likely to be inherited from mothers than from fathers, proposing that the gene for the disorder would be different in women and men. At the same time, Stine (1995) published a paper supporting theory that the gene for manic-depression is on chromosome 18
In 1993, Bredbechka et al. announced that the gene for manic -depression is on the X-chromosome; the next year Berrettini et al. (1994) reported to have found the gene that contributes to the disorder on chromosome 18 and Straub et al. (1994) reported it to be on chromosome 21. Mc. Mahon et al. (1995) found evidence to suggest that manic -depression was more likely to be inherited from mothers than from fathers, proposing that the gene for the disorder would be different in women and men. At the same time, Stine (1995) published a paper supporting theory that the gene for manic-depression is on chromosome 18
 Gershon’s research found that cases of manicdepression in which there is a connection to chromosome 18 was not present in cases where the disorder seemed to be inherited from the mother. Stine believes that a predisposition from chromosome 18 is present only if inherited from the father …. .
Gershon’s research found that cases of manicdepression in which there is a connection to chromosome 18 was not present in cases where the disorder seemed to be inherited from the mother. Stine believes that a predisposition from chromosome 18 is present only if inherited from the father …. .
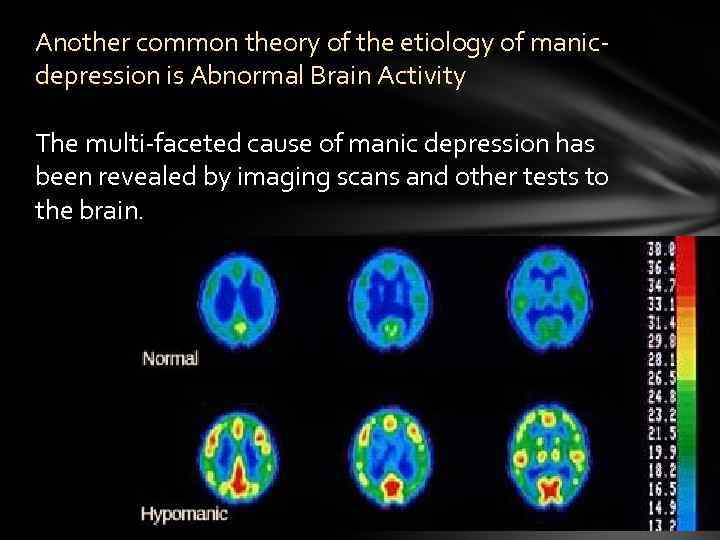 Another common theory of the etiology of manicdepression is Abnormal Brain Activity The multi-faceted cause of manic depression has been revealed by imaging scans and other tests to the brain.
Another common theory of the etiology of manicdepression is Abnormal Brain Activity The multi-faceted cause of manic depression has been revealed by imaging scans and other tests to the brain.
 • Oversecretion of cortisol, a stress hormone • Excessive calcium influx into brain cells • Abnormal hyperactivity in parts of the brain associated with emotion and movement coordination • Low activity in parts of the brain associated with concentration, attention, inhibition, and judgment neurochemical malfunctions in the brain • neurotransmitter dysfunctions
• Oversecretion of cortisol, a stress hormone • Excessive calcium influx into brain cells • Abnormal hyperactivity in parts of the brain associated with emotion and movement coordination • Low activity in parts of the brain associated with concentration, attention, inhibition, and judgment neurochemical malfunctions in the brain • neurotransmitter dysfunctions
 Symptomatology and diagnosis depressive illness or bipolar Manic depressive states are diagnosed as: disorder are classified • Manic episode according to either manic or • Depressive episode depressive episodes. • Mixed bipolar episode The symptoms of manic-
Symptomatology and diagnosis depressive illness or bipolar Manic depressive states are diagnosed as: disorder are classified • Manic episode according to either manic or • Depressive episode depressive episodes. • Mixed bipolar episode The symptoms of manic-
 Diagnosing : Manic episode: A manic episode is diagnosed if elevated mood occurs with 3 or more of the other symptoms most of the day, nearly every day, or for 1 week or longer. If the mood is irritable, 4 additional symptoms must be present. Depressive episode: A depressive episode is diagnosed if 5 or more of these symptoms last most of the day, nearly every day, or for a period of 2 weeks or longer.
Diagnosing : Manic episode: A manic episode is diagnosed if elevated mood occurs with 3 or more of the other symptoms most of the day, nearly every day, or for 1 week or longer. If the mood is irritable, 4 additional symptoms must be present. Depressive episode: A depressive episode is diagnosed if 5 or more of these symptoms last most of the day, nearly every day, or for a period of 2 weeks or longer.
 Mixed bipolar episode: In some people, however, symptoms of mania and depression can occur together in a mixed bipolar state. A person could have a very sad, hopeless mood, while feeling energized at the same time.
Mixed bipolar episode: In some people, however, symptoms of mania and depression can occur together in a mixed bipolar state. A person could have a very sad, hopeless mood, while feeling energized at the same time.
 External environmental and psychological factors are also believed to be involved in the development of bipolar disorder. These external factors are called triggers
External environmental and psychological factors are also believed to be involved in the development of bipolar disorder. These external factors are called triggers
 Triggers can set off new episodes of mania or depression or make existing symptoms worse. However, many bipolar disorder episodes occur without an obvious trigger. Stress – Stressful life events can trigger bipolar disorder in someone with a genetic vulnerability. These events tend to involve drastic or sudden changes–either good or bad–such as getting married, going away to college, losing a loved one, getting fired, or moving. Substance Abuse – While substance abuse doesn’t cause bipolar disorder, it can bring on an episode and worsen the course of the disease. Drugs such as cocaine, ecstasy, and amphetamines can trigger mania, while alcohol and tranquilizers can trigger depression.
Triggers can set off new episodes of mania or depression or make existing symptoms worse. However, many bipolar disorder episodes occur without an obvious trigger. Stress – Stressful life events can trigger bipolar disorder in someone with a genetic vulnerability. These events tend to involve drastic or sudden changes–either good or bad–such as getting married, going away to college, losing a loved one, getting fired, or moving. Substance Abuse – While substance abuse doesn’t cause bipolar disorder, it can bring on an episode and worsen the course of the disease. Drugs such as cocaine, ecstasy, and amphetamines can trigger mania, while alcohol and tranquilizers can trigger depression.
 Medication – Certain medications, most notably antidepressant drugs, can trigger mania. Other drugs that can cause mania include over-the-counter cold medicine, appetite suppressants, caffeine, corticosteroids, and thyroid medication. Seasonal Changes – Episodes of mania and depression often follow a seasonal pattern. Manic episodes are more common during the summer, and depressive episodes more common during the fall, winter, and spring. Sleep Deprivation – Loss of sleep—even as little as skipping a few hours of rest—can trigger an episode of mania.
Medication – Certain medications, most notably antidepressant drugs, can trigger mania. Other drugs that can cause mania include over-the-counter cold medicine, appetite suppressants, caffeine, corticosteroids, and thyroid medication. Seasonal Changes – Episodes of mania and depression often follow a seasonal pattern. Manic episodes are more common during the summer, and depressive episodes more common during the fall, winter, and spring. Sleep Deprivation – Loss of sleep—even as little as skipping a few hours of rest—can trigger an episode of mania.
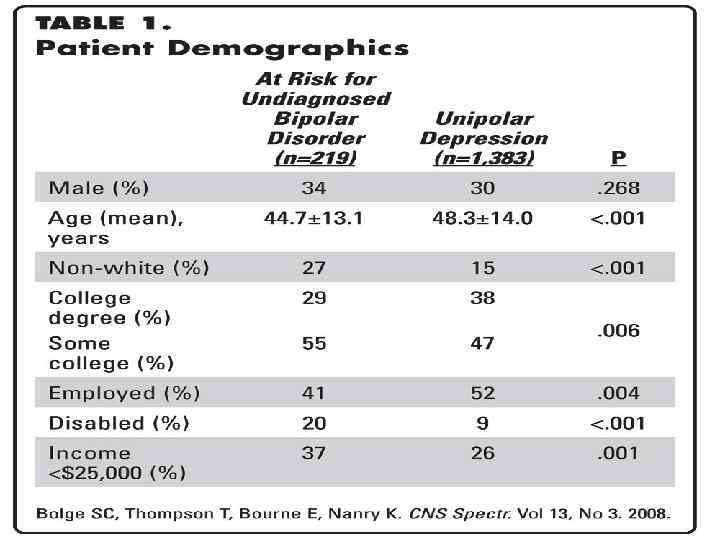
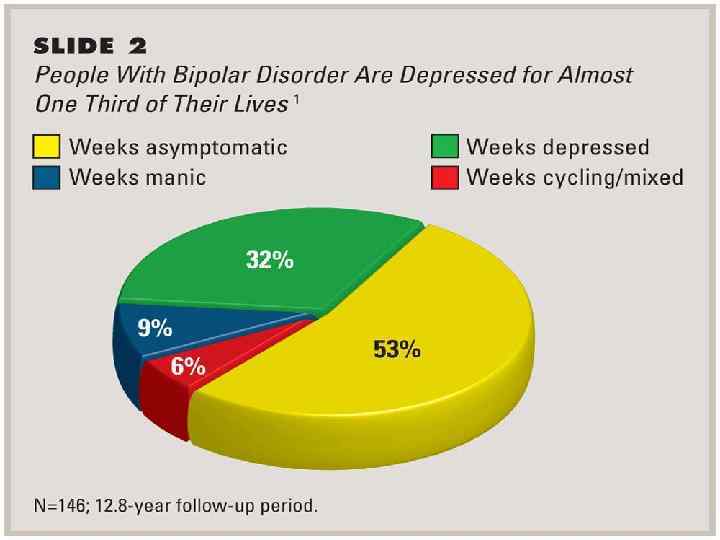
 Treatments : Know your personal triggers: Manic-depressive illness has a recurrent pattern, and continuous treatment is necessary. An adequate amount of sleep and regular sleep times are of primary importance in the treatment of bipolar disorder. Knowing personal triggers such as sleep patterns and life events help in the proper treatment of the disease. Medication: Psychiatrists generally prescribe medications known as “mood stabilizers”. Monitor your thyroid function: People with bipolar disorder often have abnormal thyroid function. Thyroid levels need to be monitored carefully because they affect mood and energy levels. Learn to spot relapses: For a person with manic-depressive illness, understanding the illness and learning to spot relapses is vital to successful treatment. This applies to the person who has the illness as well as family members who often seek treatment.
Treatments : Know your personal triggers: Manic-depressive illness has a recurrent pattern, and continuous treatment is necessary. An adequate amount of sleep and regular sleep times are of primary importance in the treatment of bipolar disorder. Knowing personal triggers such as sleep patterns and life events help in the proper treatment of the disease. Medication: Psychiatrists generally prescribe medications known as “mood stabilizers”. Monitor your thyroid function: People with bipolar disorder often have abnormal thyroid function. Thyroid levels need to be monitored carefully because they affect mood and energy levels. Learn to spot relapses: For a person with manic-depressive illness, understanding the illness and learning to spot relapses is vital to successful treatment. This applies to the person who has the illness as well as family members who often seek treatment.
 BIPOLAR DISORDER AND SUICIDE The relationship between bipolar disorder and suicide is a matter of continuing research…
BIPOLAR DISORDER AND SUICIDE The relationship between bipolar disorder and suicide is a matter of continuing research…
 Many men and women with bipolar disorder are familiar with suicidal thoughts….
Many men and women with bipolar disorder are familiar with suicidal thoughts….
 The depressive phase of bipolar disorder is often very severe, and suicide is a major risk factor. In fact, people suffering from bipolar disorder are more likely to attempt suicide than those suffering from regular depression. Furthermore, their suicide attempts tend to be more lethal.
The depressive phase of bipolar disorder is often very severe, and suicide is a major risk factor. In fact, people suffering from bipolar disorder are more likely to attempt suicide than those suffering from regular depression. Furthermore, their suicide attempts tend to be more lethal.
 The risk of suicide is even higher in people with bipolar disorder who have frequent depressive episodes, mixed episodes, a history of alcohol or drug abuse, a family history of suicide, or an early onset of the disease.
The risk of suicide is even higher in people with bipolar disorder who have frequent depressive episodes, mixed episodes, a history of alcohol or drug abuse, a family history of suicide, or an early onset of the disease.
 The warning signs of suicide include: - Talking about death, self-harm, or suicide - Feeling hopeless or helpless - Feeling worthless or like a burden to others - Acting recklessly, as if one has a “death wish” - Putting affairs in order or saying goodbye - Seeking out weapons or pills that could be used to commit suicide
The warning signs of suicide include: - Talking about death, self-harm, or suicide - Feeling hopeless or helpless - Feeling worthless or like a burden to others - Acting recklessly, as if one has a “death wish” - Putting affairs in order or saying goodbye - Seeking out weapons or pills that could be used to commit suicide
 Important It’s very important to take any thoughts or talk of suicide seriously Bipolar disorder has no single cause. It appears that certain people are genetically predisposed to bipolar disorder. Yet not everyone with an inherited vulnerability develops the illness, indicating that genes are not the only cause. .
Important It’s very important to take any thoughts or talk of suicide seriously Bipolar disorder has no single cause. It appears that certain people are genetically predisposed to bipolar disorder. Yet not everyone with an inherited vulnerability develops the illness, indicating that genes are not the only cause. .
 Some brain imaging studies show physical changes in the brains of people with bipolar disorder. Other research points to neurotransmitter imbalances, abnormal thyroid function, circadian rhythm disturbances, and high levels of the stress hormone cortisol.
Some brain imaging studies show physical changes in the brains of people with bipolar disorder. Other research points to neurotransmitter imbalances, abnormal thyroid function, circadian rhythm disturbances, and high levels of the stress hormone cortisol.
 About 30% of individuals with bipolar disorder have histories of suicide attempts. Other behavior changes often observed in those experiencing depression include increased sleepiness, lack of energy, and irritability. Some may lose interest in things they usually enjoy and have failing grades in school due to lack of concentration. It is often important for family members and mental health experts to help these patients, especially those with a history bipolar disorder and suicide attempts. If patients are not given prompt and proper therapy, their problems can frequently worsen.
About 30% of individuals with bipolar disorder have histories of suicide attempts. Other behavior changes often observed in those experiencing depression include increased sleepiness, lack of energy, and irritability. Some may lose interest in things they usually enjoy and have failing grades in school due to lack of concentration. It is often important for family members and mental health experts to help these patients, especially those with a history bipolar disorder and suicide attempts. If patients are not given prompt and proper therapy, their problems can frequently worsen.
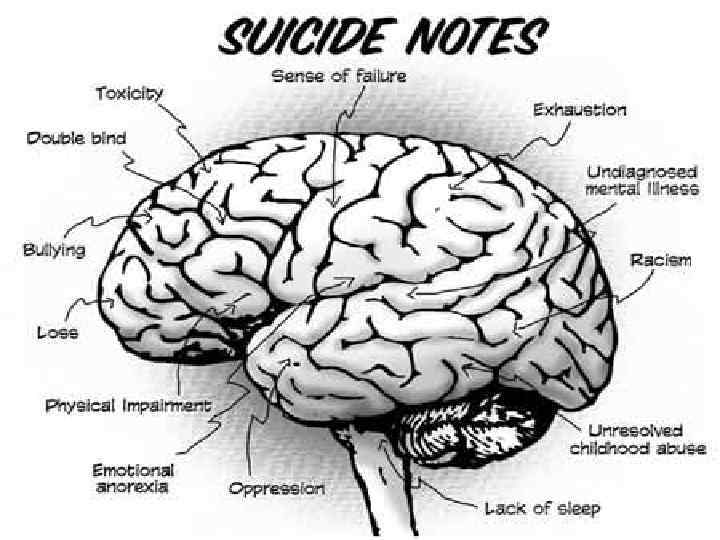
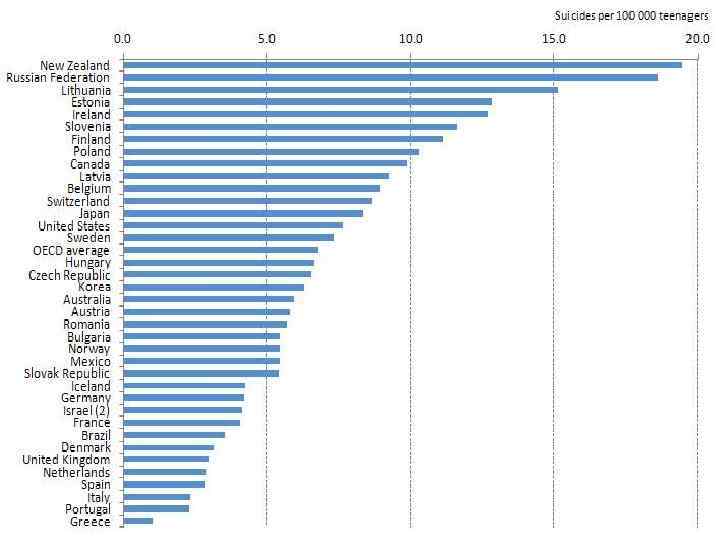
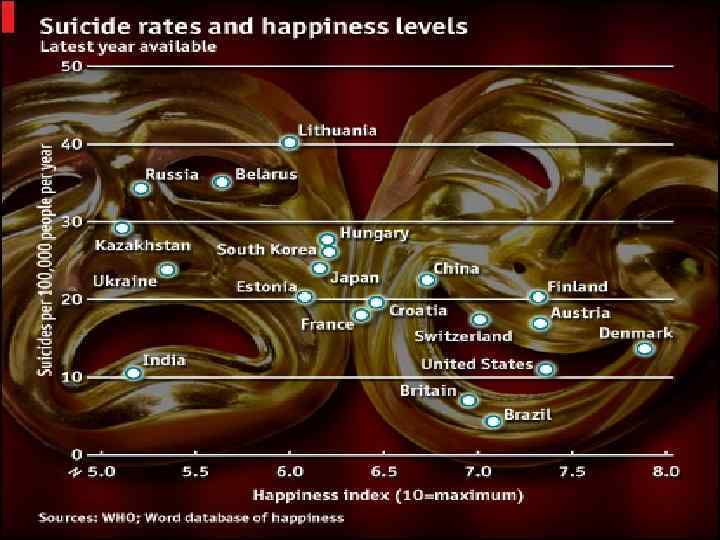
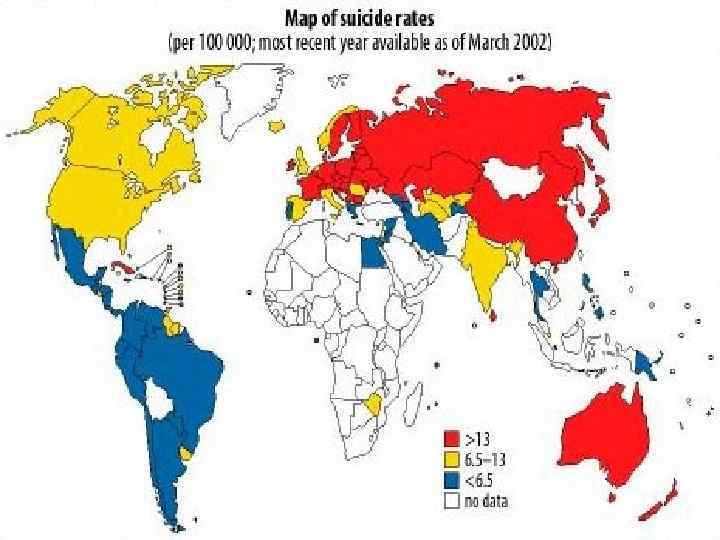
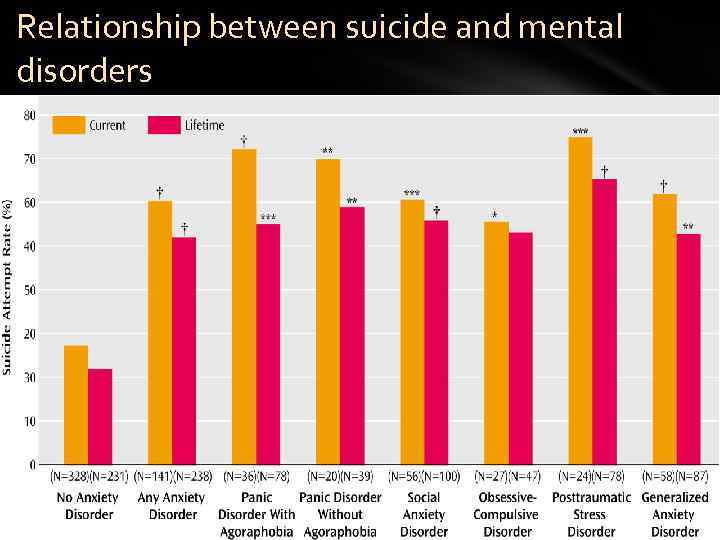 Relationship between suicide and mental disorders
Relationship between suicide and mental disorders