26a4ece9e8f1534907aaeed5ab889af5.ppt
- Количество слайдов: 88
 Introduction to Person Centered Planning June 2011 Neal Adams MD MPH California Institute of Mental Health
Introduction to Person Centered Planning June 2011 Neal Adams MD MPH California Institute of Mental Health

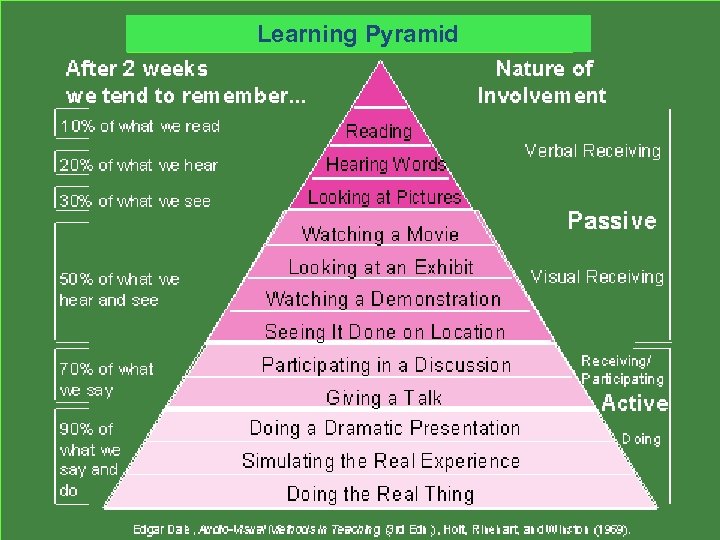 Learning Pyramid
Learning Pyramid
 Warm Up • List typical goals found on current service plans • Write 3 goals/areas of meaning you have for yourself on a piece of paper • Hand that paper to the person sitting next to you
Warm Up • List typical goals found on current service plans • Write 3 goals/areas of meaning you have for yourself on a piece of paper • Hand that paper to the person sitting next to you
 person-centered / directed care …it’s not a straight path from here to there…
person-centered / directed care …it’s not a straight path from here to there…
 Definition of a Recovery Plan • A recovery plan is a document, co-created by the person receiving services and the provider, to outline the steps needed to achieve a particular goal or outcome.
Definition of a Recovery Plan • A recovery plan is a document, co-created by the person receiving services and the provider, to outline the steps needed to achieve a particular goal or outcome.
 The Recovery Plan • It is the work/social “contract”, created by the person and provider.
The Recovery Plan • It is the work/social “contract”, created by the person and provider.
 A Person-Centered Approach to Service Planning • Collaboration and partnership. • The plan prioritizes the person’s desires while including a provider perspective.
A Person-Centered Approach to Service Planning • Collaboration and partnership. • The plan prioritizes the person’s desires while including a provider perspective.
 PCP…Don’t we already do this? ? Ø Making progress but… we DON’T “already do this. ” Ø Not according to consumer/survivors… Ø “old wine…new bottles” Ø and not if you take a close look at concrete implementation strategies Ø Review your current records/plans Treatment Plan Recovery Plan
PCP…Don’t we already do this? ? Ø Making progress but… we DON’T “already do this. ” Ø Not according to consumer/survivors… Ø “old wine…new bottles” Ø and not if you take a close look at concrete implementation strategies Ø Review your current records/plans Treatment Plan Recovery Plan
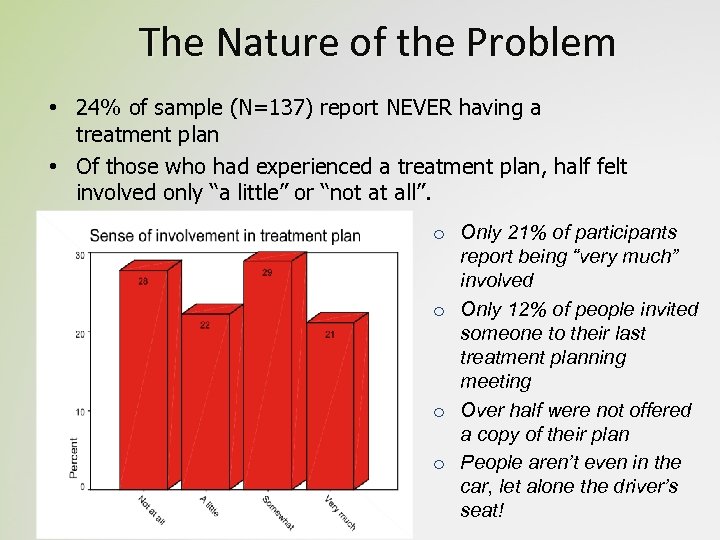 The Nature of the Problem • 24% of sample (N=137) report NEVER having a treatment plan • Of those who had experienced a treatment plan, half felt involved only “a little” or “not at all”. o Only 21% of participants report being “very much” involved o Only 12% of people invited someone to their last treatment planning meeting o Over half were not offered a copy of their plan o People aren’t even in the car, let alone the driver’s seat!
The Nature of the Problem • 24% of sample (N=137) report NEVER having a treatment plan • Of those who had experienced a treatment plan, half felt involved only “a little” or “not at all”. o Only 21% of participants report being “very much” involved o Only 12% of people invited someone to their last treatment planning meeting o Over half were not offered a copy of their plan o People aren’t even in the car, let alone the driver’s seat!
 It Works! • For example, WNYCCP has achieved the following outcomes: • • • 55% decrease in ER visits 58% decrease in inpatient days 66% decrease in suicide attempts 52% decrease in harm to others 18% decrease in arrests • Cost-effective • Over a 3 year period, Medicaid costs per participant decreased 10% compared to an 8% increase for the general population
It Works! • For example, WNYCCP has achieved the following outcomes: • • • 55% decrease in ER visits 58% decrease in inpatient days 66% decrease in suicide attempts 52% decrease in harm to others 18% decrease in arrests • Cost-effective • Over a 3 year period, Medicaid costs per participant decreased 10% compared to an 8% increase for the general population
 The Comprehensive Person-Centered Plan Incorporates Evidence-Based Practices Encourages Peer-Based Services Promotes Cultural Responsiveness Focuses on Natural Supporters/Community Settings Maximizes Self. Determination & Choice Informed by Stages of Change & MI Methods Respects Both Professional & Personal Wellness Strategies Consistent w/ Standards of Fiscal & Regulatory Bodies, e. g. , CMS, JCAHO
The Comprehensive Person-Centered Plan Incorporates Evidence-Based Practices Encourages Peer-Based Services Promotes Cultural Responsiveness Focuses on Natural Supporters/Community Settings Maximizes Self. Determination & Choice Informed by Stages of Change & MI Methods Respects Both Professional & Personal Wellness Strategies Consistent w/ Standards of Fiscal & Regulatory Bodies, e. g. , CMS, JCAHO
 PDP is… • Person Directed Planning is a planning process that is controlled by the person receiving services (family for children) u results in a recovery plan that details the issues important to the person u o u managed in all important aspects by that person with freely chosen support when necessary spells out what will constitute both quality in the execution of the plan as well as specific outcomes 13
PDP is… • Person Directed Planning is a planning process that is controlled by the person receiving services (family for children) u results in a recovery plan that details the issues important to the person u o u managed in all important aspects by that person with freely chosen support when necessary spells out what will constitute both quality in the execution of the plan as well as specific outcomes 13
 Being Person-Centered in Practice • The consumer as a whole person • Sharing power and responsibility • Having a therapeutic alliance • The clinician as person 14
Being Person-Centered in Practice • The consumer as a whole person • Sharing power and responsibility • Having a therapeutic alliance • The clinician as person 14
 Fundamental Principles of PDP • Adheres to the “person-first” concept • Applies to ALL people • Views the recovery process as flexible and non-linear • Promotes self-determination to the maximum extent possible • Focuses on capitalizing strengths • Demands transparency and equal access to information • Facilitates natural supporter involvement
Fundamental Principles of PDP • Adheres to the “person-first” concept • Applies to ALL people • Views the recovery process as flexible and non-linear • Promotes self-determination to the maximum extent possible • Focuses on capitalizing strengths • Demands transparency and equal access to information • Facilitates natural supporter involvement
 The Road to Recovery. . . • Person-centered planning u u u is a collaborative process resulting in a recovery oriented treatment plan is directed by consumers and produced in partnership with care providers for treatment and recovery supports consumer preferences and a recovery orientation Adams/Grieder
The Road to Recovery. . . • Person-centered planning u u u is a collaborative process resulting in a recovery oriented treatment plan is directed by consumers and produced in partnership with care providers for treatment and recovery supports consumer preferences and a recovery orientation Adams/Grieder
 Use of Person-first Language • Not a diagnostic label u Person with schizophrenia, or addiction • not “a schizophrenic” or “an addict” • Not “front-line staff” who are “in the trenches” u direct care staff providing compassionate care • Focus on strengths, successes, talents • Self-determination as a right • Communicate a consistent message of hope 17
Use of Person-first Language • Not a diagnostic label u Person with schizophrenia, or addiction • not “a schizophrenic” or “an addict” • Not “front-line staff” who are “in the trenches” u direct care staff providing compassionate care • Focus on strengths, successes, talents • Self-determination as a right • Communicate a consistent message of hope 17
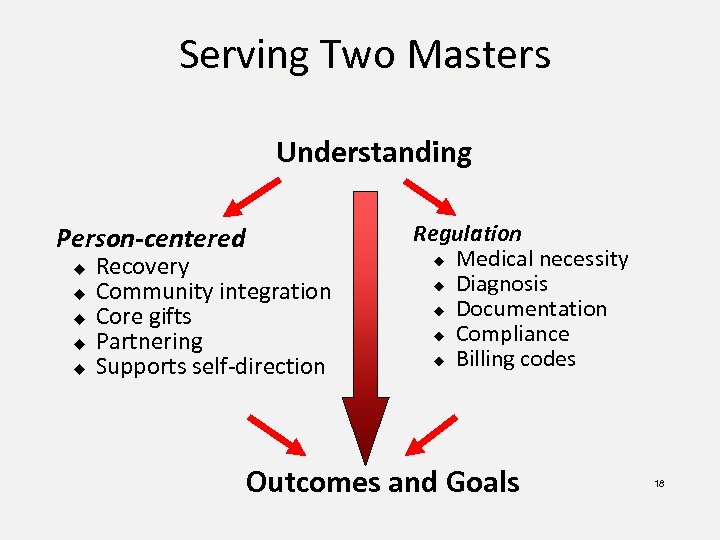 Serving Two Masters Understanding Person-centered u u u Recovery Community integration Core gifts Partnering Supports self-direction Regulation u Medical necessity u Diagnosis u Documentation u Compliance u Billing codes Outcomes and Goals 18
Serving Two Masters Understanding Person-centered u u u Recovery Community integration Core gifts Partnering Supports self-direction Regulation u Medical necessity u Diagnosis u Documentation u Compliance u Billing codes Outcomes and Goals 18
 Medical Necessity • Doing the right thing, at the right time, for the right reason • Standard of service and quality • Five elements u u Indicated Appropriate o u u u consider issues of culture Efficacious Effective Efficient 19
Medical Necessity • Doing the right thing, at the right time, for the right reason • Standard of service and quality • Five elements u u Indicated Appropriate o u u u consider issues of culture Efficacious Effective Efficient 19
 Example • Goal u Decrease depression • Objectives u u u Assess medication needs Improve finances Develop appropriate vocational goals 20
Example • Goal u Decrease depression • Objectives u u u Assess medication needs Improve finances Develop appropriate vocational goals 20
 Example • Goal u Maintain psychiatric stability • Objectives u u Attend appointments with PCP Donna will attend psychiatric appointments 21
Example • Goal u Maintain psychiatric stability • Objectives u u Attend appointments with PCP Donna will attend psychiatric appointments 21
 Example • Goal u Life long sobriety and abstinence • Objectives u u Attend all classes and groups on substance abuse education Complete 4 th step by November 2008 Attend 5 NA/AA meetings per week Weekly individual therapy 22
Example • Goal u Life long sobriety and abstinence • Objectives u u Attend all classes and groups on substance abuse education Complete 4 th step by November 2008 Attend 5 NA/AA meetings per week Weekly individual therapy 22
 Plan Development • Acquired skill / Art form u u u Not often taught in professional training Often viewed as administrative burden and paper exercise Requires flexibility • Opportunity for creative thinking • Integrates information about person served u u Derived from formulation and prioritization Information transformed to understanding • Strategy for managing complexity 23
Plan Development • Acquired skill / Art form u u u Not often taught in professional training Often viewed as administrative burden and paper exercise Requires flexibility • Opportunity for creative thinking • Integrates information about person served u u Derived from formulation and prioritization Information transformed to understanding • Strategy for managing complexity 23
 Service Plan Functions • Specifies intended outcomes / transitions / discharge criteria u Clearly elaborates expected results of services o u includes perspective of person served and family in the context of the person’s culture Promotes consideration and inclusion of alternatives and natural supports / community resources • Establishes role of person served and family in their own recovery / rehabilitation u u Assures that services are person-centered Enhances collaboration between person served and providers 24
Service Plan Functions • Specifies intended outcomes / transitions / discharge criteria u Clearly elaborates expected results of services o u includes perspective of person served and family in the context of the person’s culture Promotes consideration and inclusion of alternatives and natural supports / community resources • Establishes role of person served and family in their own recovery / rehabilitation u u Assures that services are person-centered Enhances collaboration between person served and providers 24
 Service Plan Functions continued • Identifies responsibilities of team members-including person served and family u u Increases coordination and collaboration Decreases fragmentation and duplication Coordinates multidisciplinary interventions Prompts analysis of available time and resources • Provides assurance / documentation of medical necessity u Anticipates frequency, intensity, duration of services • Promotes culturally competent services 25
Service Plan Functions continued • Identifies responsibilities of team members-including person served and family u u Increases coordination and collaboration Decreases fragmentation and duplication Coordinates multidisciplinary interventions Prompts analysis of available time and resources • Provides assurance / documentation of medical necessity u Anticipates frequency, intensity, duration of services • Promotes culturally competent services 25
 Service Plan Functions continued • Supports utilization management u u Services authorization, communication with payers and payment for services Allocation of limited resource • A contract with the people we serve! 26
Service Plan Functions continued • Supports utilization management u u Services authorization, communication with payers and payment for services Allocation of limited resource • A contract with the people we serve! 26
 The Plan…Must it be a heavy burden? “Apparently, Smith’s desk just couldn’t withstand the weight of the paperwork we piled on his desk. ”
The Plan…Must it be a heavy burden? “Apparently, Smith’s desk just couldn’t withstand the weight of the paperwork we piled on his desk. ”
 Elements of a Recovery Plan • The person’s goal: what is the desired outcome of services? • Discharge/transition criteria—establishing and end point • How to overcome barriers? • Objectives – what are the steps to reduce barriers and attain the goal? • Proposed type(s) of interventions – who is going to do what to get there? u u proposed duration– when will things be accomplished? Purpose—what’s to be accomplished relative to the objective?
Elements of a Recovery Plan • The person’s goal: what is the desired outcome of services? • Discharge/transition criteria—establishing and end point • How to overcome barriers? • Objectives – what are the steps to reduce barriers and attain the goal? • Proposed type(s) of interventions – who is going to do what to get there? u u proposed duration– when will things be accomplished? Purpose—what’s to be accomplished relative to the objective?
 A Plan is a Road Map • Provides hope by breaking a seemingly overwhelming journey into manageable steps for both the provider and the person served B C D A E “life is a journey…not a destination”
A Plan is a Road Map • Provides hope by breaking a seemingly overwhelming journey into manageable steps for both the provider and the person served B C D A E “life is a journey…not a destination”
 Building a Plan Outcomes Services Objectives Strengths/Barriers Goals Prioritization Understanding Assessment Request for services
Building a Plan Outcomes Services Objectives Strengths/Barriers Goals Prioritization Understanding Assessment Request for services
 THE ASSESSMENT
THE ASSESSMENT
 Strengths • Environmental factors that will increase the likelihood of success: community supports, family/relationship support/involvement, work • Identifying the person’s best qualities/motivation • Strategies already utilized to help • Competencies/accomplishments • Interests and activities, i. e. sports, art u (Identified by the consumer and/or the provider)
Strengths • Environmental factors that will increase the likelihood of success: community supports, family/relationship support/involvement, work • Identifying the person’s best qualities/motivation • Strategies already utilized to help • Competencies/accomplishments • Interests and activities, i. e. sports, art u (Identified by the consumer and/or the provider)
 Examples of Strengths • • • Motivated to change Has a support system –friends, family Employed/does volunteer work Has skills/competencies: vocational, relational, transportation savvy, activities of daily living Intelligent, artistic, musical, good at sports Has knowledge of his/her disease Sees value in taking medications Has a spiritual program/connected to church Good physical health Adaptive coping skills Capable of independent living
Examples of Strengths • • • Motivated to change Has a support system –friends, family Employed/does volunteer work Has skills/competencies: vocational, relational, transportation savvy, activities of daily living Intelligent, artistic, musical, good at sports Has knowledge of his/her disease Sees value in taking medications Has a spiritual program/connected to church Good physical health Adaptive coping skills Capable of independent living
 Cultural Factors in Assessment • Begin with cultural and demographic factors u Clarify identity u “how do you see yourself? ” o race, ethnicity, sexual orientation, religion, color, disability reference group Specify language o o fluency literacy preference 34
Cultural Factors in Assessment • Begin with cultural and demographic factors u Clarify identity u “how do you see yourself? ” o race, ethnicity, sexual orientation, religion, color, disability reference group Specify language o o fluency literacy preference 34
 Barriers • What is keeping the person from their goals? need for skills development u intrusive or burdensome symptoms u lack of resources u need for assistance / supports u problems in behavior u challenges in activities of daily living u threats to basic health and safety u • Challenges / needs as a result of a mental / alcohol and/or drug disorder 35
Barriers • What is keeping the person from their goals? need for skills development u intrusive or burdensome symptoms u lack of resources u need for assistance / supports u problems in behavior u challenges in activities of daily living u threats to basic health and safety u • Challenges / needs as a result of a mental / alcohol and/or drug disorder 35
 Importance of Understanding • Data collected in assessment is by itself not sufficient for service planning • Formulation / understanding is essential u u Requires clinical skill and experience Moves from what to why Sets the stage for prioritizing needs and goals The role of culture and ethnicity is critical to true appreciation of the person served • Recorded in a chart narrative u Shared with person served 36
Importance of Understanding • Data collected in assessment is by itself not sufficient for service planning • Formulation / understanding is essential u u Requires clinical skill and experience Moves from what to why Sets the stage for prioritizing needs and goals The role of culture and ethnicity is critical to true appreciation of the person served • Recorded in a chart narrative u Shared with person served 36
 Interpretive Summary Bridge • Informative findings based on assessment data and the subsequent recommendations • Perception of the individual on his/her SNAP (strengths, needs, abilities and preferences) • Perception of the provider on individual’s SNARF (strengths, needs, abilities, risk and functional status) • Provider insight into contribution and impact of individual’s psychodynamic, cognitive, familial, environmental and personality traits on current status, service goals and treatment outcomes
Interpretive Summary Bridge • Informative findings based on assessment data and the subsequent recommendations • Perception of the individual on his/her SNAP (strengths, needs, abilities and preferences) • Perception of the provider on individual’s SNARF (strengths, needs, abilities, risk and functional status) • Provider insight into contribution and impact of individual’s psychodynamic, cognitive, familial, environmental and personality traits on current status, service goals and treatment outcomes
 Interpretive Summary, cont. • Provider & individual’s understanding of how illness/condition impacts function • Provider and individual’s speculation and understanding of previous treatment outcomes • Groundwork for recovery vision and future goals • Prioritization of needs for service planning • Individual’s readiness and motivation for change
Interpretive Summary, cont. • Provider & individual’s understanding of how illness/condition impacts function • Provider and individual’s speculation and understanding of previous treatment outcomes • Groundwork for recovery vision and future goals • Prioritization of needs for service planning • Individual’s readiness and motivation for change
 The 10 Ps • • • P ertinent history (brief) P redisposing factors P recipitating factors P erpetuating factors P resent condition / presenting problem P revious treatment and response P rioritization by person served P references of person served P rognosis P ossibilites 39
The 10 Ps • • • P ertinent history (brief) P redisposing factors P recipitating factors P erpetuating factors P resent condition / presenting problem P revious treatment and response P rioritization by person served P references of person served P rognosis P ossibilites 39
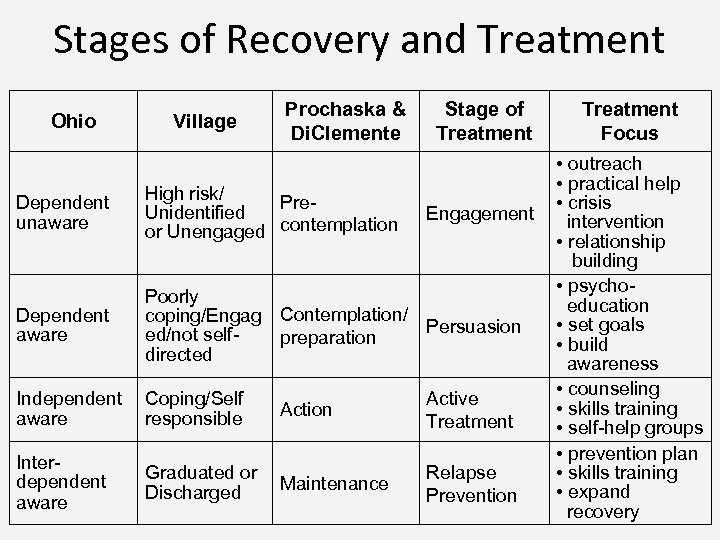 Stages of Recovery and Treatment Ohio Village Prochaska & Di. Clemente Stage of Treatment Dependent unaware High risk/ Pre. Unidentified or Unengaged contemplation Dependent aware Poorly coping/Engag Contemplation/ Persuasion ed/not selfpreparation directed Independent Coping/Self responsible aware Interdependent aware Action Graduated or Maintenance Discharged Engagement Active Treatment Relapse Prevention Treatment Focus • outreach • practical help • crisis intervention • relationship building • psycho- education • set goals • build awareness • counseling • skills training • self-help groups • prevention plan • skills training • expand recovery
Stages of Recovery and Treatment Ohio Village Prochaska & Di. Clemente Stage of Treatment Dependent unaware High risk/ Pre. Unidentified or Unengaged contemplation Dependent aware Poorly coping/Engag Contemplation/ Persuasion ed/not selfpreparation directed Independent Coping/Self responsible aware Interdependent aware Action Graduated or Maintenance Discharged Engagement Active Treatment Relapse Prevention Treatment Focus • outreach • practical help • crisis intervention • relationship building • psycho- education • set goals • build awareness • counseling • skills training • self-help groups • prevention plan • skills training • expand recovery
 The person is… moving beyond… challenging… overwhelmed by… …the disabling power of the illness giving in to… questioning
The person is… moving beyond… challenging… overwhelmed by… …the disabling power of the illness giving in to… questioning

 Vignette--Carmen • 18 year old Latina u u u High school senior o preparing for graduation First generation o parents monolingual Spanish speaking o client bilingual o observant Catholic family Lives in predominantly Anglo-American community 43
Vignette--Carmen • 18 year old Latina u u u High school senior o preparing for graduation First generation o parents monolingual Spanish speaking o client bilingual o observant Catholic family Lives in predominantly Anglo-American community 43
 Vignette continued • Excellent student u u u Active in school and social activities Recently unable to attend school because of distress Graduation from high school and college attendance is core value for Carmen and family • Recent physical problems u Nausea, vomiting, dizziness, headaches • Parents believe she is suffering from susto u Treatment from curandero 44
Vignette continued • Excellent student u u u Active in school and social activities Recently unable to attend school because of distress Graduation from high school and college attendance is core value for Carmen and family • Recent physical problems u Nausea, vomiting, dizziness, headaches • Parents believe she is suffering from susto u Treatment from curandero 44
 Vignette continued • Recent crisis u u u Acute physical distress Admitted to hearing a baby cry while at school Reported feeling sad and blue • Referred to mental health u u Embarrassed and resistant First family member to seek MH services 45
Vignette continued • Recent crisis u u u Acute physical distress Admitted to hearing a baby cry while at school Reported feeling sad and blue • Referred to mental health u u Embarrassed and resistant First family member to seek MH services 45
 Vignette continued • Assessment with Latina provider in Spanish u u Revealed she had a miscarriage a year ago Feeling increasingly guilty and troubled Wants to die and join her baby Relationship with parents has become distant and full of conflict o father refusing to speak with her 46
Vignette continued • Assessment with Latina provider in Spanish u u Revealed she had a miscarriage a year ago Feeling increasingly guilty and troubled Wants to die and join her baby Relationship with parents has become distant and full of conflict o father refusing to speak with her 46
 Vignette Formulation • Identity u u First generation Latina Bilingual • Explanation of Illness u What appeared to be a physical problem is a mental health problem o o somatization is idiom of distress shame, guilt and embarrassment are key themes • Provider relationship u u Spanish preferred More open with Latina clinician 47
Vignette Formulation • Identity u u First generation Latina Bilingual • Explanation of Illness u What appeared to be a physical problem is a mental health problem o o somatization is idiom of distress shame, guilt and embarrassment are key themes • Provider relationship u u Spanish preferred More open with Latina clinician 47
 Vignette Formulation continued • Psychosocial environment u u Lives with family, first generation Some degree of acculturation and distance from parents o difficult and painful • Diagnosis u Consider possibility of culture bound syndrome o u u susto Possible depression with psychotic features Understanding her beliefs may be key to treatment 48
Vignette Formulation continued • Psychosocial environment u u Lives with family, first generation Some degree of acculturation and distance from parents o difficult and painful • Diagnosis u Consider possibility of culture bound syndrome o u u susto Possible depression with psychotic features Understanding her beliefs may be key to treatment 48
 Vignette Formulation continued • Hypothesis u Intergenerational issues of acculturation are a major factor o u u u Age appropriate issues of individuation and separation She is between contemplative and active stage —some ambivalence about help-seeking School completion and education opportunity and advancement are shared values /strengths to build upon Need to help her reconcile feelings of guilt and remorse o Religious and spiritual factors may be significant 49
Vignette Formulation continued • Hypothesis u Intergenerational issues of acculturation are a major factor o u u u Age appropriate issues of individuation and separation She is between contemplative and active stage —some ambivalence about help-seeking School completion and education opportunity and advancement are shared values /strengths to build upon Need to help her reconcile feelings of guilt and remorse o Religious and spiritual factors may be significant 49
 Definition of a Goal “The goal is a broad, general statement that expresses the individual’s and family’s desires for change and improvement in their lives, ideally captured in their own words. ” Source: Adams, N. and Grieder, D. (2005) Treatment Planning for Person-Centered Care. Elsevier Academic Press.
Definition of a Goal “The goal is a broad, general statement that expresses the individual’s and family’s desires for change and improvement in their lives, ideally captured in their own words. ” Source: Adams, N. and Grieder, D. (2005) Treatment Planning for Person-Centered Care. Elsevier Academic Press.
 Definition of a Goal • Goals express the hopes and dreams of the client. • Goals identify the hopedfor destination to be arrived at through the services provided.
Definition of a Goal • Goals express the hopes and dreams of the client. • Goals identify the hopedfor destination to be arrived at through the services provided.
 The Essential Features of Goals • They are BIG u u Long term, global, and broadly stated They are not necessarily measurable • Written in positive terms u u built upon abilities / strengths, preferences and needs embody hope/alternative to current circumstances
The Essential Features of Goals • They are BIG u u Long term, global, and broadly stated They are not necessarily measurable • Written in positive terms u u built upon abilities / strengths, preferences and needs embody hope/alternative to current circumstances
 Key Points about Goals • A good goal inspires the individual to reconnect to their dreams. • Goal development is an essential part of engagement and creating a collaborative working relationship.
Key Points about Goals • A good goal inspires the individual to reconnect to their dreams. • Goal development is an essential part of engagement and creating a collaborative working relationship.
 Collaboration and Goals • Reaching agreement on the goal is essential The provider understands and appreciates the importance of the goal. u The goal has immediate meaning and relevance for the consumer. u The goal becomes a shared vision of success. u
Collaboration and Goals • Reaching agreement on the goal is essential The provider understands and appreciates the importance of the goal. u The goal has immediate meaning and relevance for the consumer. u The goal becomes a shared vision of success. u
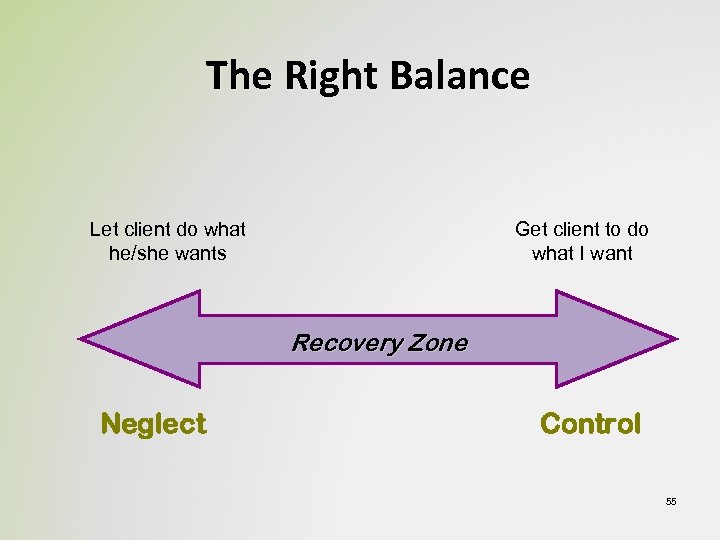 The Right Balance Let client do what he/she wants Get client to do what I want Recovery Zone Neglect Control 55
The Right Balance Let client do what he/she wants Get client to do what I want Recovery Zone Neglect Control 55
 Common Ground • Clients should have the dignity of risk and right of failure • Providers are advocates of client choice • Clients are not abandoned to suffer “the natural consequences” of their choices • Provider or client not a failure if choice results in failure • Use reinforcers to support client choice • Assure true choice over a wide range of options Pat Deegan 56
Common Ground • Clients should have the dignity of risk and right of failure • Providers are advocates of client choice • Clients are not abandoned to suffer “the natural consequences” of their choices • Provider or client not a failure if choice results in failure • Use reinforcers to support client choice • Assure true choice over a wide range of options Pat Deegan 56
 Carmen’s Plan/Action Stage • Goal u “I want to graduate from high school” 57
Carmen’s Plan/Action Stage • Goal u “I want to graduate from high school” 57
 Barriers • What is getting in the way of the person achieving their goal Why can’t they do it tomorrow u Why can’t they do it themselves u • Our focus is removing/reducing/resolving barriers that are a result of the mental illness
Barriers • What is getting in the way of the person achieving their goal Why can’t they do it tomorrow u Why can’t they do it themselves u • Our focus is removing/reducing/resolving barriers that are a result of the mental illness
 Recovery Happens In Small Steps • To be an effective road-map, plans need to clearly identify the smaller steps that get you to your destination. • These markers along the way also offer opportunity to celebrate and acknowledge progress. • Every gain made is additional fuel for the journey!
Recovery Happens In Small Steps • To be an effective road-map, plans need to clearly identify the smaller steps that get you to your destination. • These markers along the way also offer opportunity to celebrate and acknowledge progress. • Every gain made is additional fuel for the journey!
 Defining Objectives • Objectives describe a significant and meaningful change that the individual can see or experience. • Objectives are milestones – they designate the mini-goals along the way. • Well-written objectives create opportunity for success, for seeing that the dream is really possible.
Defining Objectives • Objectives describe a significant and meaningful change that the individual can see or experience. • Objectives are milestones – they designate the mini-goals along the way. • Well-written objectives create opportunity for success, for seeing that the dream is really possible.
 What Do Objectives Do? • Take into account the culture of person served • Divide larger goals into manageable tasks • Provide time frames for assessing progress • These are the action steps the person takes toward their goal
What Do Objectives Do? • Take into account the culture of person served • Divide larger goals into manageable tasks • Provide time frames for assessing progress • These are the action steps the person takes toward their goal
 Objectives and Medical Necessity • Objectives address barriers to the goal. • They also describe changes in behavior, function, or status. u relate back to functional impairments o u how the work we are doing will reduce these barriers identify key changes that the consumer wishes to accomplish
Objectives and Medical Necessity • Objectives address barriers to the goal. • They also describe changes in behavior, function, or status. u relate back to functional impairments o u how the work we are doing will reduce these barriers identify key changes that the consumer wishes to accomplish
 Keep it Focused! • A maximum of two or three objectives per goal is recommended to create focus and reduce the chances of feeling overwhelmed.
Keep it Focused! • A maximum of two or three objectives per goal is recommended to create focus and reduce the chances of feeling overwhelmed.
 Objectives Should Be SMART • • • Simple or Straightforward Measurable Attainable Realistic Time-framed
Objectives Should Be SMART • • • Simple or Straightforward Measurable Attainable Realistic Time-framed
 How to Write an Objective • Subject • Person receiving services • Verb/Action Word • Will demonstrate • What • Ability to use three coping techniques to address anger • When will it be done/timeframe? • Within one month • How will it be measured? • As measured by therapist observation
How to Write an Objective • Subject • Person receiving services • Verb/Action Word • Will demonstrate • What • Ability to use three coping techniques to address anger • When will it be done/timeframe? • Within one month • How will it be measured? • As measured by therapist observation
 Objectives Are Not Interventions • Objectives are the WHAT u What is the next step towards the goal? u What is the next significant milestone? • Interventions are the HOW u How are we going to get there? u Interventions are the action steps taken to achieve the objective.
Objectives Are Not Interventions • Objectives are the WHAT u What is the next step towards the goal? u What is the next significant milestone? • Interventions are the HOW u How are we going to get there? u Interventions are the action steps taken to achieve the objective.
 Carmen’s Plan/Action Stage • Goal u “I want to graduate from high school” • Objective u Carmen will return to class attendance for 5 consecutive full days within a month as reported by Carmen / or support worker 67
Carmen’s Plan/Action Stage • Goal u “I want to graduate from high school” • Objective u Carmen will return to class attendance for 5 consecutive full days within a month as reported by Carmen / or support worker 67
 Interventions • Actions by staff, family, peers, natural supports • Specific to an objective • Respect consumer choice and preference • Specific to the stage of change/recovery • Availability and accessibility of services may be impacted by cultural factors 68
Interventions • Actions by staff, family, peers, natural supports • Specific to an objective • Respect consumer choice and preference • Specific to the stage of change/recovery • Availability and accessibility of services may be impacted by cultural factors 68
 Five Critical Elements • Interventions must specify u u u provider and clinical discipline staff member’s name modality frequency /intensity / duration purpose / intent / impact • Clarifies who does what • Include a task for the family, or other component of natural support system to accomplish 69
Five Critical Elements • Interventions must specify u u u provider and clinical discipline staff member’s name modality frequency /intensity / duration purpose / intent / impact • Clarifies who does what • Include a task for the family, or other component of natural support system to accomplish 69
 The 5 W’s of Interventions • Who u Which member of the team or support system will provide it • What u specifically what service will be provided. • When u How often, how much time and duration • Where u Identify the location of service delivery • Why u Link the intervention back to the desired outcome
The 5 W’s of Interventions • Who u Which member of the team or support system will provide it • What u specifically what service will be provided. • When u How often, how much time and duration • Where u Identify the location of service delivery • Why u Link the intervention back to the desired outcome
 Carmen’s Plan/Action Stage • Interventions u u Psychiatrist to provide weekly to monthly pharmacotherapy management visits for 3 months to relieve acute symptoms of anxiety and depression Social worker to provide one hour of cognitivebehavioral psychotherapy twice a week for 4 weeks to help Carmen resolve feelings of guilt and loss Support worker to meet with Carmen up to 3 hours / week for 4 weeks as required to coordinate / facilitate return to school with school counselors and mental health team Carmen and family to attend weekly sessions with their parish priest to bring about forgiveness and 71 family reconciliation.
Carmen’s Plan/Action Stage • Interventions u u Psychiatrist to provide weekly to monthly pharmacotherapy management visits for 3 months to relieve acute symptoms of anxiety and depression Social worker to provide one hour of cognitivebehavioral psychotherapy twice a week for 4 weeks to help Carmen resolve feelings of guilt and loss Support worker to meet with Carmen up to 3 hours / week for 4 weeks as required to coordinate / facilitate return to school with school counselors and mental health team Carmen and family to attend weekly sessions with their parish priest to bring about forgiveness and 71 family reconciliation.
 Common Mistakes • Assessment u u Do not use all available information resources Not culturally appropriate / sensitive Not sufficiently comprehensive Lack adequate integration / understanding of the person
Common Mistakes • Assessment u u Do not use all available information resources Not culturally appropriate / sensitive Not sufficiently comprehensive Lack adequate integration / understanding of the person
 Common Mistakes • Goals u u u Not global Not directed towards recovery Not responsive to need Not strengths based Too many
Common Mistakes • Goals u u u Not global Not directed towards recovery Not responsive to need Not strengths based Too many
 Common Mistakes • Objectives u u u Don’t support the goal Not measurable or behavioral Interventions become objectives Not time framed Too many simultaneous objectives
Common Mistakes • Objectives u u u Don’t support the goal Not measurable or behavioral Interventions become objectives Not time framed Too many simultaneous objectives
 Common Mistakes • Interventions u Purpose not included u Frequency, intensity, and duration not documented u Too few u Don’t reflect multidisciplinary activity
Common Mistakes • Interventions u Purpose not included u Frequency, intensity, and duration not documented u Too few u Don’t reflect multidisciplinary activity
 Jane • Jane comes in to the mental health clinic for medications that help her with her depression and anxiety. In the past, she has been overwhelmed by sadness and would drink to “numb-out” and her drinking made it impossible for her to function at home or work. Feeling much better, Jane wants to get back into the workforce. She occasionally experiences relapses, but finds that she gets back on her feet more quickly now.
Jane • Jane comes in to the mental health clinic for medications that help her with her depression and anxiety. In the past, she has been overwhelmed by sadness and would drink to “numb-out” and her drinking made it impossible for her to function at home or work. Feeling much better, Jane wants to get back into the workforce. She occasionally experiences relapses, but finds that she gets back on her feet more quickly now.
 Jane’s Goal • Goal: I want to work full-time.
Jane’s Goal • Goal: I want to work full-time.
 Addressing Jane’s Barriers • Objective 1 u Jane will be clean and sober for 30 consecutive days as measured by self-report. • Interventions: u u u Sam Smith, LCSW, will provide dual recovery groups once per week for one year to Jane so she can learn the tools to stay clean. CM will discuss how meetings went with Jane once per week in the community, and reinforce active participation in the group to assist her in achieving sobriety for 3 months. Jane will attend AA meetings 3 x per week for 3 months in order to develop a sober support system
Addressing Jane’s Barriers • Objective 1 u Jane will be clean and sober for 30 consecutive days as measured by self-report. • Interventions: u u u Sam Smith, LCSW, will provide dual recovery groups once per week for one year to Jane so she can learn the tools to stay clean. CM will discuss how meetings went with Jane once per week in the community, and reinforce active participation in the group to assist her in achieving sobriety for 3 months. Jane will attend AA meetings 3 x per week for 3 months in order to develop a sober support system
 Addressing Jane’s Barriers • Objective 2 u Jane will master two stress reduction skills within the next 60 days as measured by her self report of successfully resolving conflicts/problems without self-defeating behavior. • Interventions Peer specialist will meet with Jane every other week in the community to practice stress reduction skills for 2 months u CM will provide skills training on stress management one hour/once per week for 60 u
Addressing Jane’s Barriers • Objective 2 u Jane will master two stress reduction skills within the next 60 days as measured by her self report of successfully resolving conflicts/problems without self-defeating behavior. • Interventions Peer specialist will meet with Jane every other week in the community to practice stress reduction skills for 2 months u CM will provide skills training on stress management one hour/once per week for 60 u
 Barriers / Excuses / Rationales • Medicaid won’t let us do this! u • • OIG audits the forms don’t have the right fields regulations prohibit it consumers aren’t interested/motivated recovery isn’t real u stigma among professionals • lack of time/caseloads too high • “my clients are sicker”
Barriers / Excuses / Rationales • Medicaid won’t let us do this! u • • OIG audits the forms don’t have the right fields regulations prohibit it consumers aren’t interested/motivated recovery isn’t real u stigma among professionals • lack of time/caseloads too high • “my clients are sicker”
 Barriers / Excuses / Rationales social control is our “true” mission professional boundaries funding issues u getting paid for services u no Medicaid reimbursement u dis-incentives u lack of Medicaid funding for EBP’s • “we’re already doing this” • • •
Barriers / Excuses / Rationales social control is our “true” mission professional boundaries funding issues u getting paid for services u no Medicaid reimbursement u dis-incentives u lack of Medicaid funding for EBP’s • “we’re already doing this” • • •
 Provider Role And Contribution • Perception u There isn’t much of a role for providers in the person-centered world • Reality u There is a large but changed role for providers • providers of hope • assessment / formulation • knowledge of the system of care/community • knowledge of the disease and possible solutions • teachers/trainers/coaches
Provider Role And Contribution • Perception u There isn’t much of a role for providers in the person-centered world • Reality u There is a large but changed role for providers • providers of hope • assessment / formulation • knowledge of the system of care/community • knowledge of the disease and possible solutions • teachers/trainers/coaches
 It’s Not Permitted / Reimbursable • Perception u Medicaid regulations and state plans won’t allow for person-centered planning • Reality u Most state plans for Medicaid reimbursement, be they option, clinic option or waiver, speak the language of individualized planning u the person directing the planning, and a strengths based approach to assessment and planning
It’s Not Permitted / Reimbursable • Perception u Medicaid regulations and state plans won’t allow for person-centered planning • Reality u Most state plans for Medicaid reimbursement, be they option, clinic option or waiver, speak the language of individualized planning u the person directing the planning, and a strengths based approach to assessment and planning
 Violates Professional Boundaries • Perception u u This isn’t how I was trained I’m not comfortable with this I know better My licensing board won’t let me do that • Reality u u Providers have not received necessary training and support Established appropriate professional model
Violates Professional Boundaries • Perception u u This isn’t how I was trained I’m not comfortable with this I know better My licensing board won’t let me do that • Reality u u Providers have not received necessary training and support Established appropriate professional model
 Linking Planning With EBP • Perception u EBPs are not person-centered nor Medicaid reimbursable • Reality u u Most evidence based practices / programs are constructed from smaller specific service interventions that can be individualized “De-constructing” EBPs into specific billable services demonstrates medical necessity of each element EBPs provide decision-support point in shareddecision making IMR/IDDT/SE all closely related to PDP
Linking Planning With EBP • Perception u EBPs are not person-centered nor Medicaid reimbursable • Reality u u Most evidence based practices / programs are constructed from smaller specific service interventions that can be individualized “De-constructing” EBPs into specific billable services demonstrates medical necessity of each element EBPs provide decision-support point in shareddecision making IMR/IDDT/SE all closely related to PDP
 Services Are Not Aligned With PCP • Perception u “programs” are not individualized treatment/services and PCP doesn’t fit • Reality u There are opportunities within program structures to provide consumer-centered services o phases/stages of change approach o employing peers as facilitators o budgeting needs to consider moving from services to supports
Services Are Not Aligned With PCP • Perception u “programs” are not individualized treatment/services and PCP doesn’t fit • Reality u There are opportunities within program structures to provide consumer-centered services o phases/stages of change approach o employing peers as facilitators o budgeting needs to consider moving from services to supports
 Consumers Are Too Sick • Perception u Consumers aren’t interested in participating (“old timers”), are “delusional”, have no goals, etc. • Reality u u Need to communicate a message of hope and a belief that their life can be different, or education/training/tools on person-centered planning Need to assess and plan for stage of change
Consumers Are Too Sick • Perception u Consumers aren’t interested in participating (“old timers”), are “delusional”, have no goals, etc. • Reality u u Need to communicate a message of hope and a belief that their life can be different, or education/training/tools on person-centered planning Need to assess and plan for stage of change
 “If you don’t know where you are going, you will probably end up somewhere else. ” Lawrence J. Peter
“If you don’t know where you are going, you will probably end up somewhere else. ” Lawrence J. Peter


