e8de1523ad84b73d823e87c1ff11d0d2.ppt
- Количество слайдов: 44

Intrathecal Baclofen for Spasticity George Jallo MD, Division of Pediatric Neurosurgery Johns Hopkins University

Spasticity Spastikos - “to draw or tug” n n Motor disorder Velocity-dependent increased resistance to passive stretch Exaggerated tendon jerks Hyperexcitability of the stretch reflex

Pathophysiology of Spasticity Theory n n Imbalance between excitatory and inhibitory impulses to the alpha motor neuron Due to a lack of descending inhibitory input to the alpha motor neuron Descending Inhibition Sensory Excitation
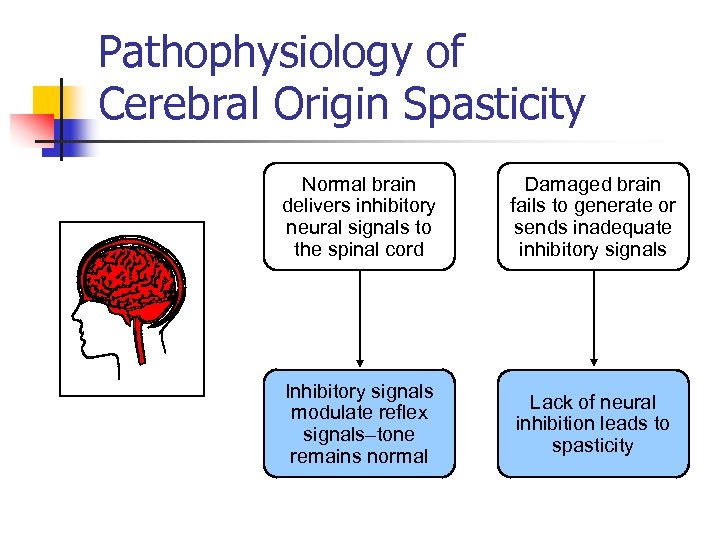
Pathophysiology of Cerebral Origin Spasticity Normal brain delivers inhibitory neural signals to the spinal cord Damaged brain fails to generate or sends inadequate inhibitory signals Inhibitory signals modulate reflex signals–tone remains normal Lack of neural inhibition leads to spasticity
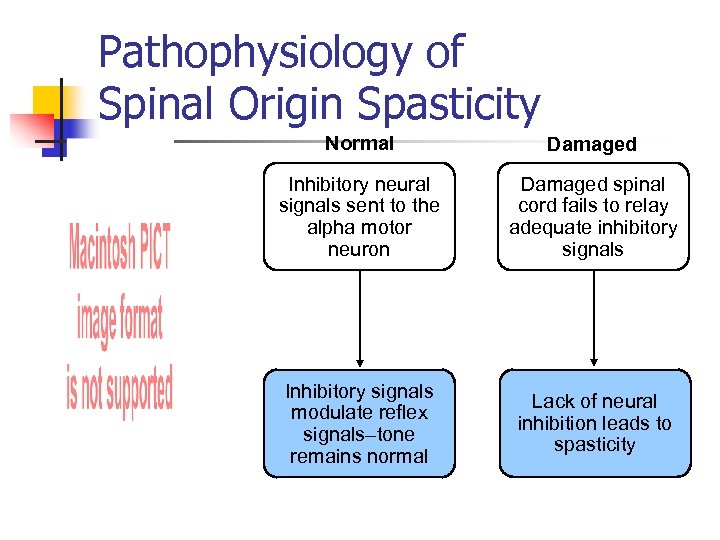
Pathophysiology of Spinal Origin Spasticity Normal Damaged Inhibitory neural signals sent to the alpha motor neuron Damaged spinal cord fails to relay adequate inhibitory signals Inhibitory signals modulate reflex signals–tone remains normal Lack of neural inhibition leads to spasticity

Possible Advantages of Spasticity n n Maintains muscle tone Helps support circulatory function May prevent formation of deep vein thrombosis May assist in activities of daily living

Consequences of Spasticity n n May interfere with mobility, exercise, joint range of motion May interfere with activities of daily living May cause pain and sleep disturbance Can make patient care more difficult

Measuring Spasticity n n Ashworth and Modified Ashworth scales Spasm and reflex scales Passive quantitative tests Active tests of movement

Factors That May Increase Spasticity Uncontrollable n n n n Urinary tract infection Kidney stones Menses Bowel impaction or gas Deep vein thrombosis Pneumonia Wounds or infections Progression of disease Controllable n n n Stress Ingrown nails Restrictive clothing Fatigue Psychological factors Change in temperature or humidity

Spasticity Associated with Cerebral Palsy (CP) n Disorders affecting n n n movement posture balance Injury to the developing brain Permanent and non-progressive Developmental disability

Classifications of Cerebral Palsy n Location of brain lesion n n Type of movement disorder n n pyramidal, extrapyramidal, mixed spastic, dystonic, athetoid, ataxia, mixed Extent and location of limb involvement n monoplegia, diplegia, hemiplegia, paraplegia, tetraplegia

Conditions Associated with Cerebral Palsy n n n n Mental retardation, learning disabilities Seizures Gastrointestinal difficulties Urinary infections Respiratory problems Hearing/vision impairment Orthopedic problems

Goals of Spasticity: Management n n n n Decrease spasticity Improve functional ability and independence Decrease pain associated with spasticity Prevent or decrease incidence of contractures Improve ambulation Facilitate hygiene Ease rehabilitation procedures Save caregivers’ time

Spectrum of Care for Management of Spasticity Prevent Nociception Intrathecal Baclofen (ITB™) Therapy Rehabilitation Therapy Oral Drugs Patient Orthopedic Treatments Injection Therapy Neurosurgery
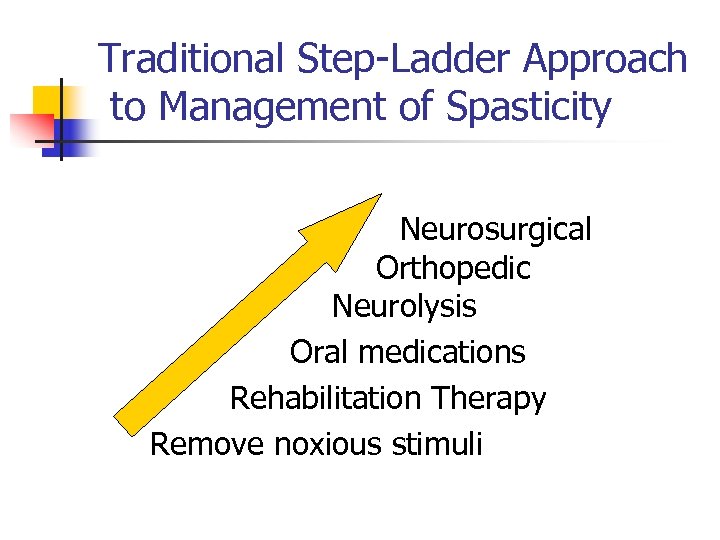
Traditional Step-Ladder Approach to Management of Spasticity Neurosurgical Orthopedic Neurolysis Oral medications Rehabilitation Therapy Remove noxious stimuli
Rehabilitation Therapy n n Stretching Weight bearing Inhibitory casting Vibration of the antagonist n n Pool therapy EMG biofeedback Electrical stimulation Positioning and rotary movements

Oral Medications n n Baclofen Diazepam Dantrolene Sodium Tizanidine
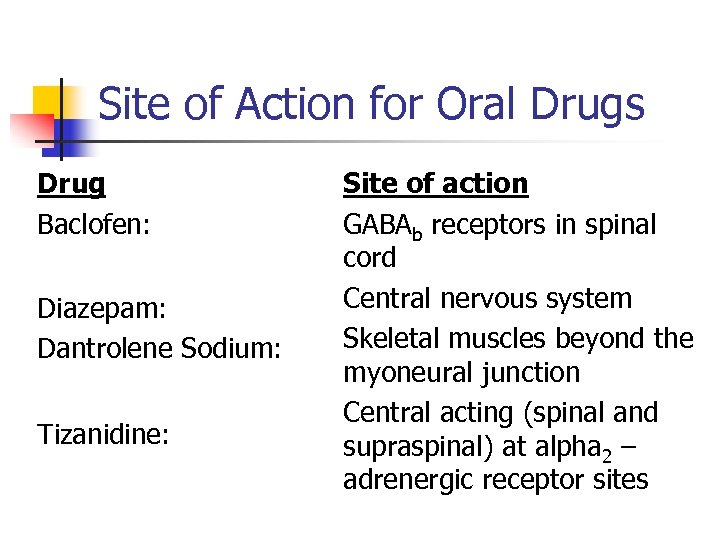

Site of Action for Oral Drugs Drug Baclofen: Diazepam: Dantrolene Sodium: Tizanidine: Site of action GABAb receptors in spinal cord Central nervous system Skeletal muscles beyond the myoneural junction Central acting (spinal and supraspinal) at alpha 2 – adrenergic receptor sites

Neurosurgery Surgical Treatments Neurodestructive Procedures n n n Neurectomy Myelotomy Rhizotomy Cordectomy Selective Dorsal Rhizotomy

Selective Dorsal Rhizotomy Surgical procedure where the dorsal (sensory) nerve roots are severed n Two primary goals: n facilitate patient care n n sitting, dressing, transfers improve function n walking

Orthopedic Surgeries Soft Tissue Procedures n n Tenotomy Tendon lengthening Myotomy Tendon transfers

Why Intrathecal vs. Oral? Baclofen Injection n Baclofen injection is delivered to the CSF and thought to act at GABAb receptor sites at the spinal cord Lower doses than those required orally Potential for fewer systemic side effects Oral Baclofen n Low blood/brain barrier penetration, with high systemic absorption and low CNS absorption Lack of preferential spinal cord distribution Some patients experience unacceptable side effects at effective doses

Advantages of ITB™ Therapy n n n Reversible Potentially fewer systemic side effects Programmable n n allows dose titration to give optimal benefit Effective in reducing spasticity n n upper and lower extremities 1 cerebral and spinal origin

ITB™ Therapy Process n n Stage 1: 2: 3: 4: Patient Selection Screening Test Implant Maintenance

Efficacy in Adults and Children n n 86% cerebral origin (screening test) 97% spinal cord origin (screening test) Upper and lower extremities Both patients with functional goals and patients with goals of improving comfort and ease of care Albright, A. Leland. Baclofen in the Treatment of Cerebral Palsy, J Child Neurol 1996; 11: 77 -83. Becker, R. , Alberti, O. , and Bauer, B. L. Continuous intrathecal baclofen infusion in severe spasticity after traumatic or hypoxic brain injury, J Neurol 1997; 244: 160 -166. Campbell, Susan K. , Almeida, Gil L. , Penn, Richard D. , and Corcos, Daniel M. The Effects of Intrathecally Administered Baclofen on Function in Patients with Spasticity, Phys Ther 1995; 75: 352 -362.

Reported Outcomes in Patients with Spasticity of Cerebral Origin Method n n n 37 patients Spastic quadriplegia ITB Therapy received over a range of 3 - 48 months Results n n 6 and 12 months post implant n muscle tone significantly decreased in lower and upper extremities 25 children capable of self-care at start of study: n significant improvement in n ADL n upper extremity function n hamstring extensibility Albright AL, Barron WB, Fasick MP, et al. Continuous Intrathecal Baclofen Infusion for Spasticity of Cerebral Origin. JAMA 270(20): 2475 -77, Nov 24, 1993.

Reported Outcomes in Patients with Spasticity of Spinal Origin Method n n n 20 patients Diagnosed with spinal cord injury or multiple sclerosis ITB Therapy received over a range of 10 -33 months Results n n n Statistically significant decreases in muscle tone of hip, knee, and ankle musculature n based on Ashworth score Statistically significant decrease in frequency of spasms Functional status tracked in 8 patients (6 months duration): n improved ADL n improved bowel and bladder management programs Parke B, Penn RD, Savoy SM, et al. Functional Outcome after Delivery of Intrathecal Baclofen. Arch Phys Med Rehabil 70: 30 -32, 1989. Penn RD, Savoy SM, Corcos D, et al. Intrathecal Baclofen for Severe Spinal Spasticity N Engl J Med 329: 1517 -21, 1989.
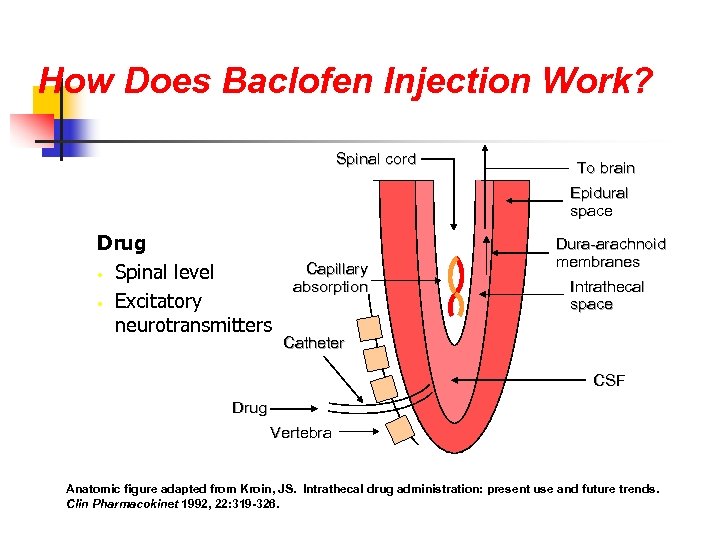
How Does Baclofen Injection Work? Spinal cord To brain Epidural space Drug • Spinal level • Excitatory neurotransmitters Capillary absorption Dura-arachnoid membranes Intrathecal space Catheter CSF Drug Vertebra Anatomic figure adapted from Kroin, JS. Intrathecal drug administration: present use and future trends. Clin Pharmacokinet 1992, 22: 319 -326.

GABA n n Gamma-butyric acid (GABA) n an inhibitory neurotransmitter Baclofen n thought to act as a GABA agonist in the spinal cord, reducing positive input to the alpha motor neuron

Pharmacokinetics of Baclofen Oral n n 60 mg dose: 0. 024 mcg/m. L IT lumbar concentration Half-life 3 -4 hours Intrathecal n n n 600 mcg/day dose: 1. 24 mcg/m. L IT lumbar concentration Lumbar to cervical concentration is 4: 1 Half-life 4 -5 hours

Pharmacodynamics of Baclofen Injection Bolus n n n Onset of action is one-half hour to 1 hour after intrathecal bolus Peak effect at 4 hours after dosing Effects may last from 4 to 8 hours Continuous n n Effects are first seen at 6 to 8 hours after initiation of continuous infusion Maximum effect observed in 24 to 48 hours Onset, peak response, and duration of action may vary

Interdisciplinary Team Assessment n n n Considers all facets of patient’s needs and resources Considers the “whole” person Provides optimal care for the patient

Contraindications of ITB™ Therapy n n Patient has a history of allergy (hypersensitivity) to oral baclofen Infection is present at time of screening or implant

Potential Risks of ITB™ Therapy n n n Common side effects: hypotonia, somnolence, nausea/vomiting, headache, dizziness Overdose, although rare, could lead to respiratory depression, loss of consciousness, reversible coma, and in extreme cases, may be life-threatening Catheter and procedural complications may occur

Causes of Overdose n n n Dosing error Pump malfunction Programming error Injecting catheter access port during refill Filling catheter with syringe during surgery Use of concomitant drugs

Screening Test Flow Chart Bolus: 50 mcg + 24 hrs after Bolus: 75 mcg + + - = Positive Response “Implant” = Negative Response “No Implant” 24 hrs after Bolus: 100 mcg + Intrathecal Baclofen Therapy Clinical Reference Guide for Spasticity Management, Medtronic, Inc. Not a Candidate

Synchro. Med® System Components n n n Pump n infuses drug Catheter n delivers drug to the intrathecal (subarachnoid) space of the spinal cord Programmer n allows for precise dosing n easily adjustable dosing

Synchro. Med® EL Pump n n n Battery life of approximately 7 years Flow rates down to 48 microliters/day Four suture loops Matte finish No changes in clinical procedure or pump programming
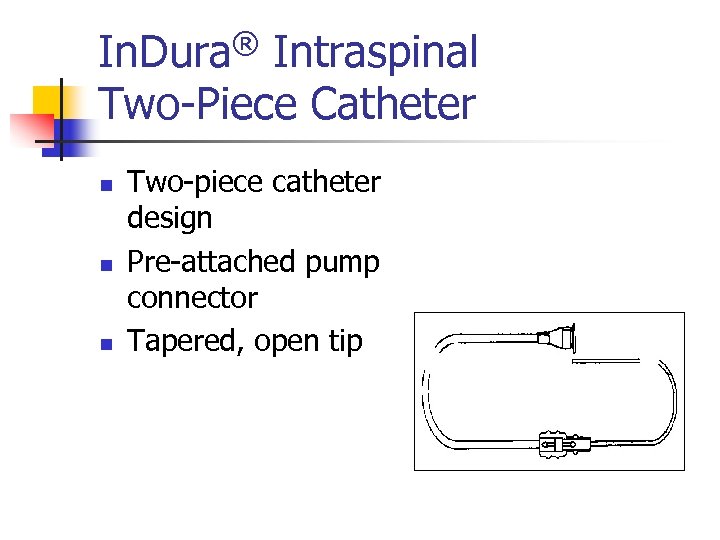
In. Dura® Intraspinal Two-Piece Catheter n n n Two-piece catheter design Pre-attached pump connector Tapered, open tip

Catheter Implant n n Insert the catheter through the introducer needle to the desired level (T 10 -T 12) Verify catheter tip position through use of fluoroscopy and CSF backflow Advancing catheter under fluoroscopy
Pump Implant n Abdominal incision n make a pocket for the pump no deeper than 2. 5 cm or 1 inch

Titration Period After First 24 -Hour Period n n Increase dose slowly Increase only once every 24 hours until desired clinical effect achieved n Adults with spasticity of spinal origin n n Adults with spasticity of cerebral origin n n 10 -30% increments 5 -15% increments Pediatrics n 5 -15% increments

Comparison of Techniques

Conclusions n n n Intrathecal delivery is an alternative to rhizotomy procedures in children Advantages: simple, adjustable, reversible Disadvantages: cost, infection, toxicity
e8de1523ad84b73d823e87c1ff11d0d2.ppt